Published online Jul 6, 2025. doi: 10.12998/wjcc.v13.i19.103844
Revised: February 1, 2025
Accepted: February 20, 2025
Published online: July 6, 2025
Processing time: 107 Days and 1.4 Hours
Intraoral honeybee stings are very rare. Stings by these insects occur 25% of the time in the head and neck region. In addition, a stinger intraorally can lead to persistent irritation, inflammation, and secondary infections if not promptly excised.
We report the case of a 52-year-old female patient who was stung in her mouth by a honeybee, causing a local irritation. The patient presented with a one-month history of pain, swelling, and redness in the left buccal mucosa. Inadvertently retained, the stinger was discovered during a clinical evaluation following initial treatment for facial swelling and erythema. After the stinger was removed, the patient’s symptoms resolved without complications.
This case emphasizes the importance of thorough examination and prompt management of insect stings to prevent prolonged discomfort and potential complications.
Core Tip: Stings from honeybees are extremely rare inside the oral cavity. These insects sting in the head and neck area less than 25% of the time compared to other body parts. Furthermore, if a stinger is not removed promptly, it may cause chronic discomfort, inflammation, and secondary infections. We present a 52-year-old female patient who had a local irritation after being stung in the mouth by a honeybee. Shortly after removing the stinger, the patient’s symptoms disappeared without any issues.
- Citation: Aloyouny AY, Albagieh HN, Aleyoni R, Jammali G, Alhuzali K. Unusual foreign body in the buccal mucosa: A case report. World J Clin Cases 2025; 13(19): 103844
- URL: https://www.wjgnet.com/2307-8960/full/v13/i19/103844.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v13.i19.103844
The order Hymenoptera includes many species of bees, wasps, and ants. They usually attack and sting either for defense or to paralyze their prey[1]. Stings by these insects occur 25% of the time in the head and neck region, but the incidence of insect stings intraorally is infrequent. Allergic reaction to insect stings ranges from a minimal response to a life-threatening reaction, depending on the allergic status of the victim, the toxicity and amount of venom injected into the victim’s body, and the site of the sting. Stings within the oral cavity are particularly concerning due to the proximity to vital structures such as the airway, which can lead to severe complications if not promptly and properly managed[2]. The venom from a honeybee sting comprises various toxic and allergenic components, such as melittin, phospholipase A2, hyaluronidase, histamine, and apamin, which contribute to the inflammatory and potentially systemic effects observed following such stings[3,4]. Moreover, a stinger within the oral cavity can lead to persistent irritation, inflammation, and secondary infections if not promptly removed[3]. In this paper, the author presents a rare case of an intraoral bee sting in the left buccal mucosa of an adult female patient with a one-month history of a retained bee stinger. The work has been reported in line with the SCARE criteria[5].
A 52-year-old female patient was referred to the oral medicine clinic for evaluation of painful swelling and redness in the left buccal mucosa.
The patient had a one-month history of localized pain, swelling, and redness in the left buccal mucosa. The patient mentioned that she was visiting a honey hive farm in Egypt. As she was eating soft bread dipped in honey, she experienced an excruciating sting inside her mouth as she opened it wide to take a bite. She reported that she discontinued chewing the bread and spat out the bolus immediately. A few hours later, she had a left facial swelling. The intraoral soreness persisted for a month before the patient sought help.
The patient denied past surgical, medical history or genetic conditions. She also had no allergies, no psychosocial history, and was not taking any treatment.
The patient was not aware of any family health history of inherited conditions.
Extraoral examination: The extraoral examination revealed pain on palpation of the left buccinator muscle area. The left submandibular lymph node was also palpable, firm, and slightly tender on palpation, with no localized warmth, measuring 1 cm × 1 cm in diameter, mobile, and not fixed to the surrounding tissues.
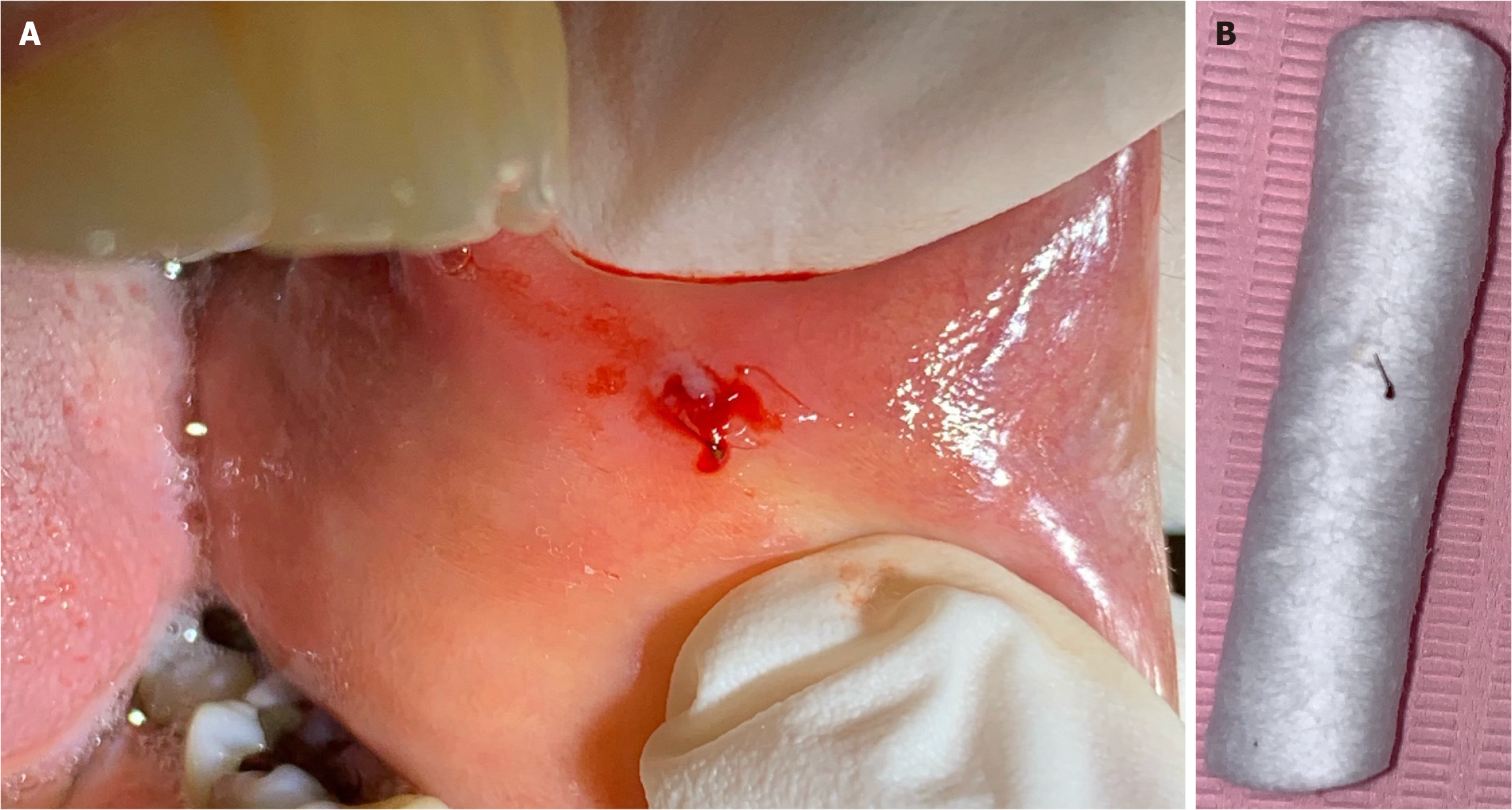
Intraoral examinations: Intraoral examination revealed a solitary, yellowish-white, 0.2 cm × 0.2 cm vesicle on the left anterior buccal mucosa surrounded by a red halo; the lesion was painful and tender to palpation (Figure 1A).
The blood test revealed normal results: A red blood cell count of 3.9 × 106/mL, a hemoglobin count of 13.2 g/dL, a platelet count of 448 × 103/mL, a white blood cell count of 16.7 × 103/mL, segmented neutrophil 42%, and lymphocytes 71%.
An orthopantomogram radiographic imaging was taken, which showed normal bony structures. The patient refused to go through fine needle aspiration for the involved lymph node. In addition, the excisional biopsy procedure was not accepted by the patient.
As part of the foreign body detection workup, diagnostic procedures were carried out to reach the definitive diagnosis. The foreign body was analyzed under the microscope; it was determined to be the honeybee’s stinger (Figure 2). The final diagnosis of the oral vesicle is an intraoral localized infection caused by a long-standing foreign body in the left buccal mucosa.
The patient signed a consent form before starting the treatment. The procedure was performed by an oral medicine consultant who identified as a diplomate in the American Board of Oral Medicine. After the anesthetic solution was applied around the vesicle, a small incision was performed through the blister to release the entrapped pus. Surprisingly, a 2-mm black, long, thin foreign body came out with the pus and blood (Figure 1A). The area was checked and washed with normal saline to remove any other irritants. Finally, the incision was stitched with one resorbable suture. After investigation, and based on the patient’s history, the foreign body turned to be a honeybee stinger (Figure 1B). The patient was unaware of the bee sting because she had not observed the bee before or shortly after feeling the pinch in her mouth. Moreover, she only knew about the bee sting when the stinger was removed in the oral medicine clinic. Luckily, no other sites of the body were affected, there was only one sting in the oral cavity and no evidence of earlier reactions to bee stings.
At one-week and then four-week recall visits, the facial swelling completely resolved, and the sting site healed well without any clinical signs of complications.
Local irritation in the oral cavity is not uncommon; it can be induced by different materials such as food, toys, graphite, dental materials, and oral care goods. However, a foreign body from a living organism inside the mouth is rare[6]. For instance, a retained insect part in the buccal mucosa is unexpected. Honeybee insects belong to the Hymenoptera order and are commonly found in nature. Honeybee stings are common because these insects possess a stinging part at the tail end of the body, which can only move forward because of its complex anatomy. Moreover, the honeybee can deliver around 50 ng of venom[3,4]. The venom toxicity increases when the stinging bee apparatus remains longer and deeper in the victim’s tissue[7]. Usually, the insect’s venom contains histamine, acetylcholine, dopamine, serotonin, numerous enzymes, polypeptide toxins, and kinins[1]. Most bee stings heal with no complications. However, a few cases present with either slight local irritation (measuring < 5 cm in diameter), which results in discomfort and pruritic urticarial lesion, or significant local irritation (measuring > 5 cm in diameter) that lasts for more than one day. Bee stings may also cause a mild systemic reaction, including erythema, urticaria, nausea, or diarrhea; a severe systemic response may lead to anaphylactic shock. Bee stings might cause immediate hypersensitivity reaction within two hours after the sting or delayed hypersensitivity reactions that occur two hours after the insect attack[8].
When dealing with these cases, it is important to assure the patient and take a thorough history and examination. First, immediate management should involve removing the local irritant, which is the bee stinger. Pharmacological treatment should be prescribed depending on the case. Antihistamines can reduce allergic reactions and minimize swelling, while corticosteroids could be administered to reduce severe inflammation and prevent airway compromise[2]. Analgesics should be given to manage pain, and antibiotics might be prescribed if there is evidence of secondary infection or if the patient is at high risk of infection[7]. There should be follow-up with the patient to monitor the healing process and ensure no complications arise. In this case report, the patient had a sizeable local irritation caused by a delayed-hypersensitivity reaction that included the left side of the face, albeit without airway obstruction; the swelling lasted for six days and subsided with therapy. Consequently, it was found that the patient had a retained bee stinger whose extraction was delayed for a month due to impaired visualization. A slight local irritation around the foreign body inside the mouth continued until it was extracted at the oral medicine clinic.
Bee stings inside the oral cavity are exceedingly rare. Usually, patients are aware of insect stings when they happen or shortly after the incident. In this case, the patient reported that she was at a honey hive farm when she opened her mouth wide to take a bite and felt a searing sting inside her mouth. Facial swelling immediately followed intraoral soreness, which was probably caused by an allergic reaction to something in the environment. In this instance, the likelihood of getting stung by bees is increased when visiting a honey hive farm without adopting any safety measures. We urge dentists to take a complete patient history and make a thorough clinical examination during each dental visit for any suspicious lesions.
| 1. | Smoley BA. Oropharyngeal hymenoptera stings: a special concern for airway obstruction. Mil Med. 2002;167:161-163. [PubMed] |
| 2. | Gruchalla RS. Immunotherapy in allergy to insect stings in children. N Engl J Med. 2004;351:707-709. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 12] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 3. | Truskinovsky AM, Dick JD, Hutchins GM. Fatal infection after a bee sting. Clin Infect Dis. 2001;32:E36-E38. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 16] [Article Influence: 0.6] [Reference Citation Analysis (1)] |
| 4. | Ellis AK, Day JH. Clinical reactivity to insect stings. Curr Opin Allergy Clin Immunol. 2005;5:349-354. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 22] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 5. | Agha RA, Borrelli MR, Farwana R, Koshy K, Fowler AJ, Orgill DP; SCARE Group. The SCARE 2018 statement: Updating consensus Surgical CAse REport (SCARE) guidelines. Int J Surg. 2018;60:132-136. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1948] [Cited by in RCA: 2081] [Article Influence: 260.1] [Reference Citation Analysis (0)] |
| 6. | Yamamoto K, Nakayama Y, Matsusue Y, Kurihara M, Yagyuu T, Kirita T. A Foreign Body Granuloma of the Buccal Mucosa Induced by Honeybee Sting. Case Rep Dent. 2017;2017:7902978. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 7. | Alemán Navas RM, Martínez Mendoza MG, Herrera H, Herrera HP. Floor of the nose mucosa lysis and labial abscess caused by a bee sting. Braz Dent J. 2009;20:249-253. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 8. | Tome R, Somri M, Teszler CB, Fradis M, Gaitini LA. Bee stings of children: when to perform endotracheal intubation? Am J Otolaryngol. 2005;26:272-274. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/