©The Author(s) 2021.
World J Clin Cases. Dec 16, 2021; 9(35): 10792-10804
Published online Dec 16, 2021. doi: 10.12998/wjcc.v9.i35.10792
Published online Dec 16, 2021. doi: 10.12998/wjcc.v9.i35.10792
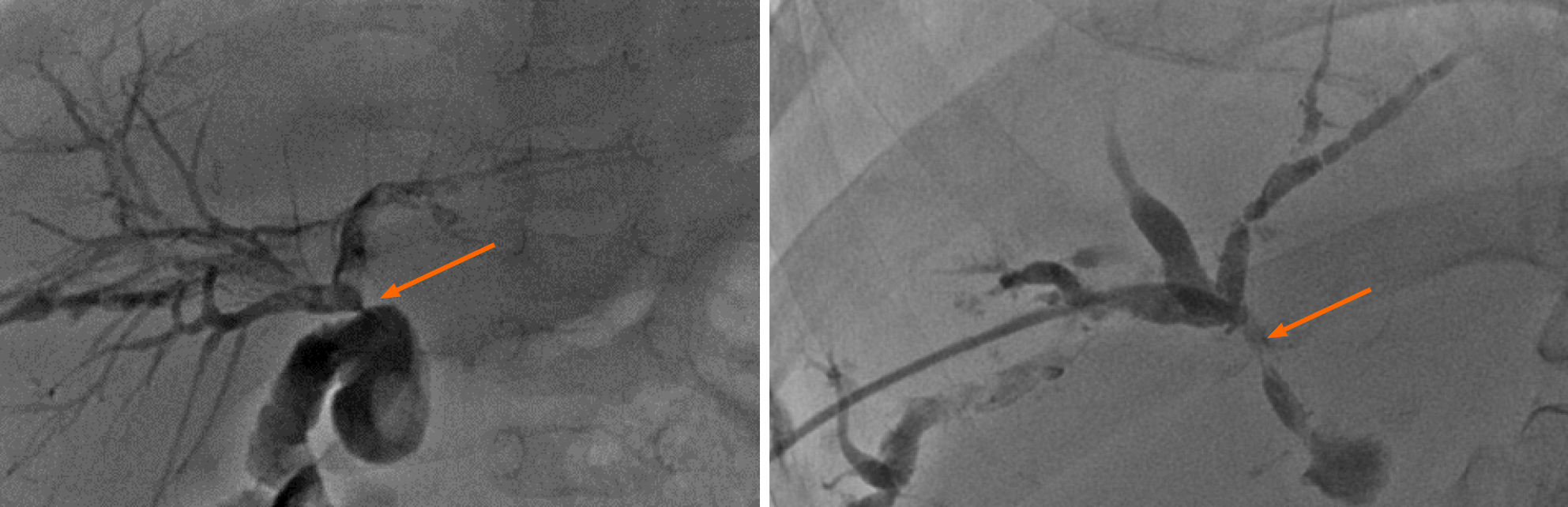
Figure 1 Endoscopic cholangiogram showing anastomotic strictures after liver transplantation.
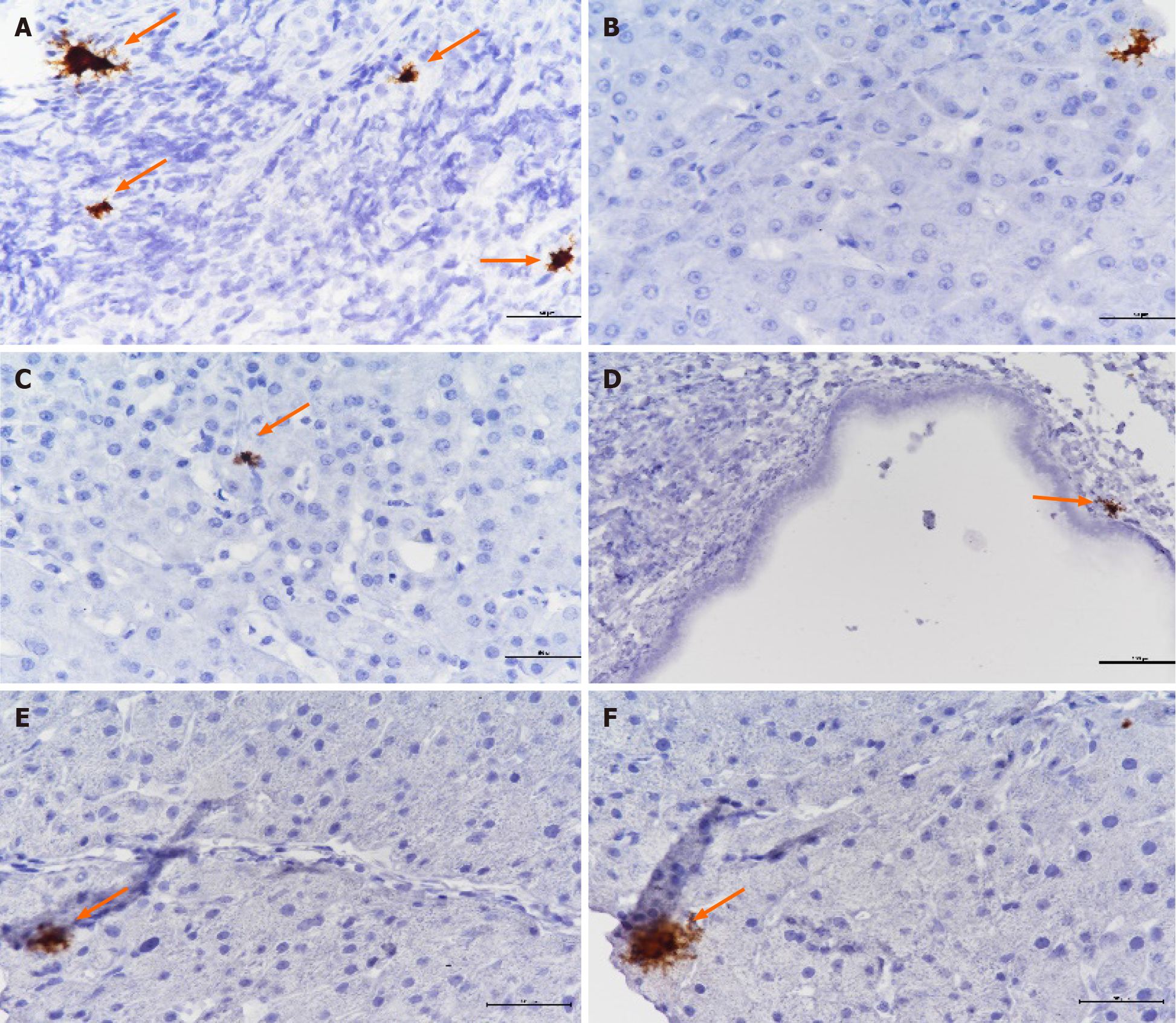
Figure 2 RNAscope in situ hybridization tests for the presence of cytomegalovirus in paraffin-embedded liver tissue samples.
A: Positive control; B-D: Patient 3, Patient 6, Patient 10; E and F: Patient 13. We used RNAscope in situ hybridization to test for the presence of cytomegalovirus in paraffin-embedded liver sections from 8 patients who tested positive for biliary cytomegalovirus-DNA. Four patients tested positive using RNAscope technology.
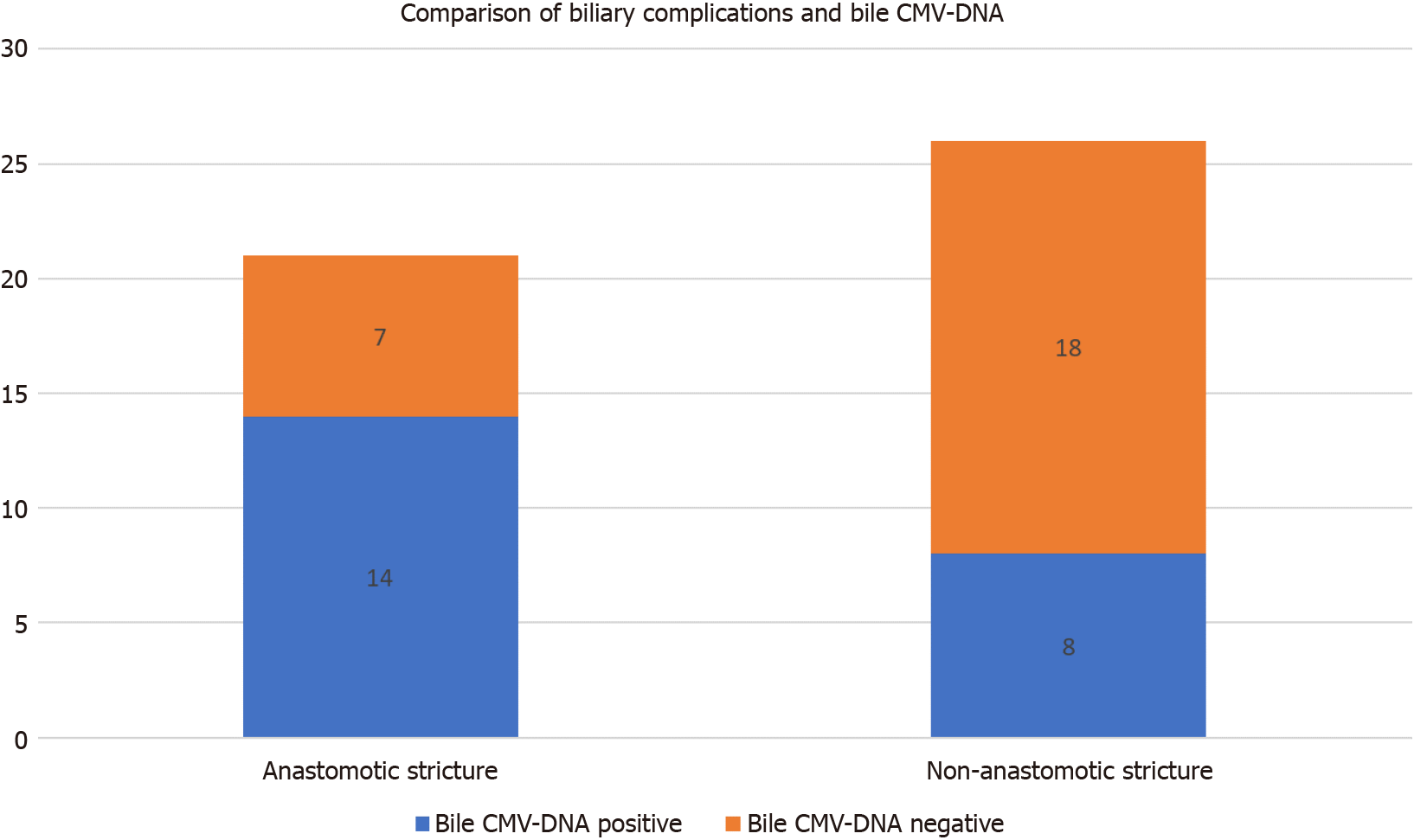
Figure 3 Comparison of biliary complications and bile cytomegalovirus-DNA.
In 21 patients with anastomotic stricture, 66.7% (14/21) of patients had positive bile cytomegalovirus (CMV)-DNA. In 26 patients with other biliary complications, 30.8% (8/26) of patients had positive bile CMV-DNA. These results showed that biliary anastomotic stricture was more relevant to biliary CMV infection in this study.
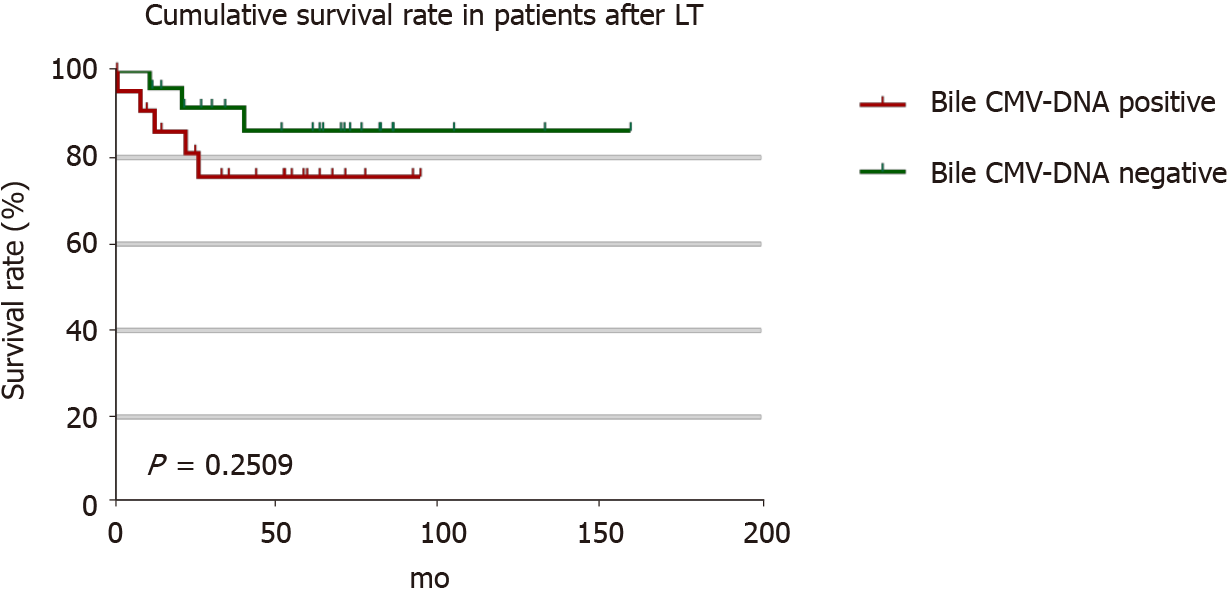
Figure 4 Cumulative survival rate in patients after liver transplantation.
In patients with negative cytomegalovirus (CMV)-DNA bile, 1-year cumulative survival rate was 96.0%, 3-year cumulative survival rate was 91.6%, and 5-year cumulative survival rate was 86.2%. In patients with CMV-DNA positive bile, 1-year cumulative survival rate was 90.9%, and the cumulative 3- and 5-year survival rates were 75.7%. Occult CMV infection is a risk factor for chronic graft failure and mortality after liver transplant.
- Citation: Liu JY, Zhang JR, Sun LY, Zhu ZJ, Wei L, Qu W, Zeng ZG, Liu Y, Zhao XY. Impact of cytomegalovirus infection on biliary disease after liver transplantation - maybe an essential factor. World J Clin Cases 2021; 9(35): 10792-10804
- URL: https://www.wjgnet.com/2307-8960/full/v9/i35/10792.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v9.i35.10792