Published online Mar 25, 2026. doi: 10.5527/wjn.v15.i1.114165
Revised: October 2, 2025
Accepted: December 16, 2025
Published online: March 25, 2026
Processing time: 182 Days and 15 Hours
Acute pyelonephritis (APN) is a significant part of the healthcare burden globally. Early risk stratification in APN is crucial to guide intensive care unit (ICU) ad
To assess the accuracy of NEWS2 and qSOFA scores in predicting ICU admission, in-hospital mortality and their role in guiding urological interventions among adults with APN.
A prospective observational study, conducted at a tertiary care centre in South India over two years, on adult patients diagnosed clinically and radiologically with APN. Comprehensive clinical, laboratory, and imaging parameters were re
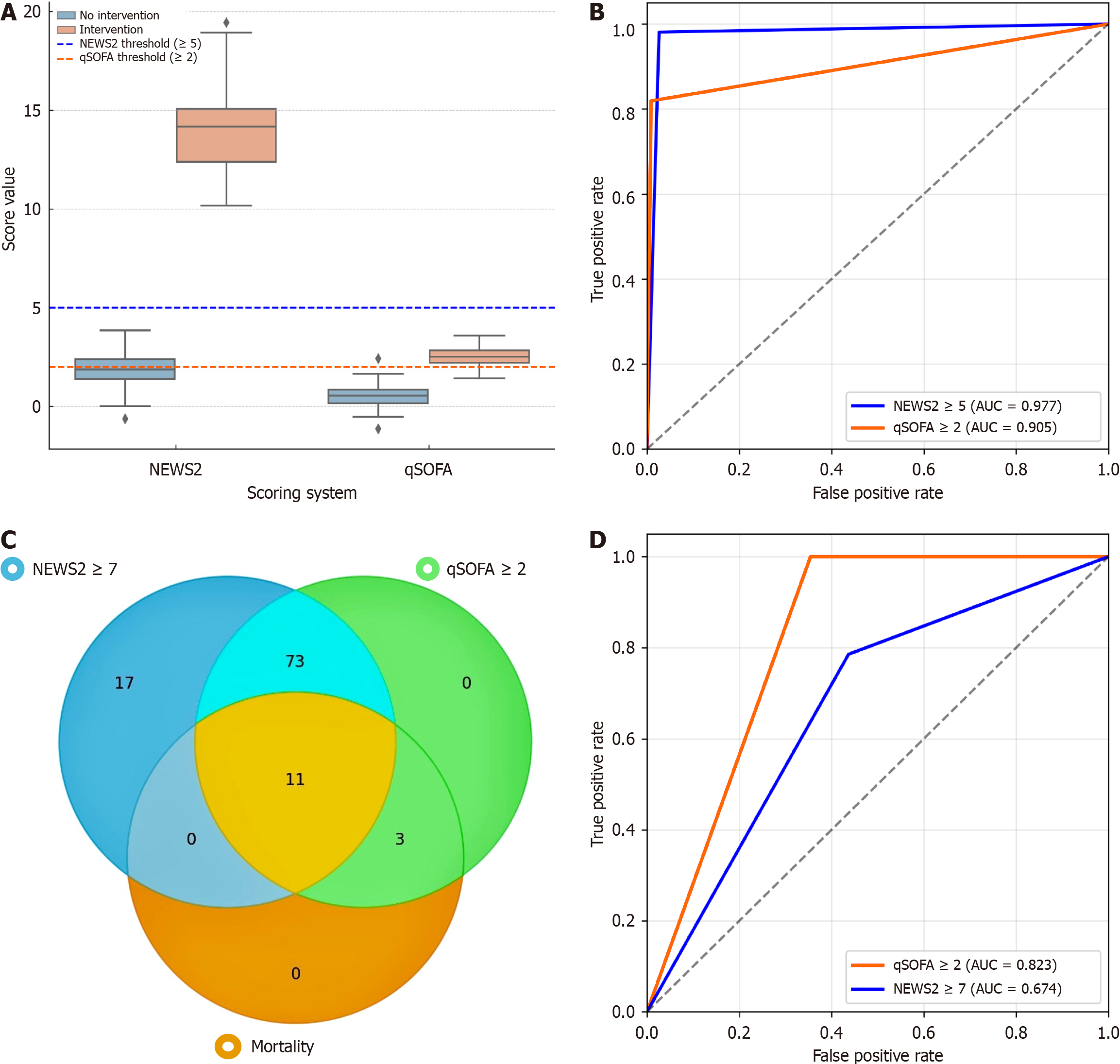
The NEWS2 score ≥ 5 emerged as a robust tool, identifying nearly all patients requiring ICU admission [sensitivity, 98.1%; area under the receiver operating characteristic curve (AUC): 0.977; P < 0.05] and predicting intervention with high accuracy (AUC-0.823; P < 0.05). However, the qSOFA ≥ 2 score proved to be the silent sentinel of mor
In APN, NEWS2 (≥ 5) proved to be a pragmatic trigger for ICU triage, while qSOFA (≥ 2) better flagged in-hospital mortality. Together, they form a complementary framework as a simple, objective, and lifesaving bedside tool.
Core Tip: Acute pyelonephritis (APN) is common in urology, but existing studies on early warning scores often mix heterogeneous sepsis cohorts or emphasize stone-related or emphysematous pyelonephritis. Our prospective study is the first to focus exclusively on non-obstructive, non-emphysematous APN, a group frequently overlooked yet clinically challenging. We demonstrate that the National Early Warning Score 2 score reliably identifies patients who require intensive care unit care or urgent intervention, while the quick Sequential Organ Failure Assessment score more accurately predicts mortality. Used together, they provide a complementary dual-score framework for bedside triage and prognostication. This simple approach offers urologists and nephrologists a practical, objective tool to enhance decision-making and improve patient outcomes.
- Citation: Jain PR, Aravind S, K PR, Shekar M, Palaniyandi V, Sekar H, Krishnamoorthy S. Dual-score framework: National Early Warning Score 2 and quick Sequential Organ Failure Assessment scores in acute pyelonephritis. World J Nephrol 2026; 15(1): 114165
- URL: https://www.wjgnet.com/2220-6124/full/v15/i1/114165.htm
- DOI: https://dx.doi.org/10.5527/wjn.v15.i1.114165
Acute pyelonephritis (APN) remains one of the most common urological emergencies encountered in clinical practice. APN is a significant part of the healthcare burden globally. While many patients improve with antibiotics and supportive care, a subset deteriorates quickly, needing intensive care unit (ICU) admission or even succumbing to sepsis. The chal
Several early warning tools have been proposed to guide frontline decision making[3], with the qSOFA and the NEWS2 scores being among the most widely used[4,5]. To date, prior reports evaluating early warning scores predominantly assess the sepsis cohorts presenting to the emergency department in which urinary infection like APN is only a subset or included heterogeneous sepsis populations, such as emphysematous pyelonephritis (EPN), or focused predominantly on severe obstruction secondary to stones[6-8]. These conditions inherently carry high morbidity and inflate ap
This study is among the first prospective effort to directly compare these two scoring systems exclusively in a real-world cohort, designed to bridge that gap by eliminating confounding factors and better reflecting the nuanced presentations of APN seen in routine urological practice. By narrowing the focus to this understudied population, our objective was to evaluate the true clinical value of these scores in early triage, need for intervention and mortality prediction.
This study was conducted at a tertiary care institute in South India.
A prospective observational study.
Adult patients (aged 18 years or older) diagnosed clinically and/or radiologically with APN from January 2023 to January 2025.
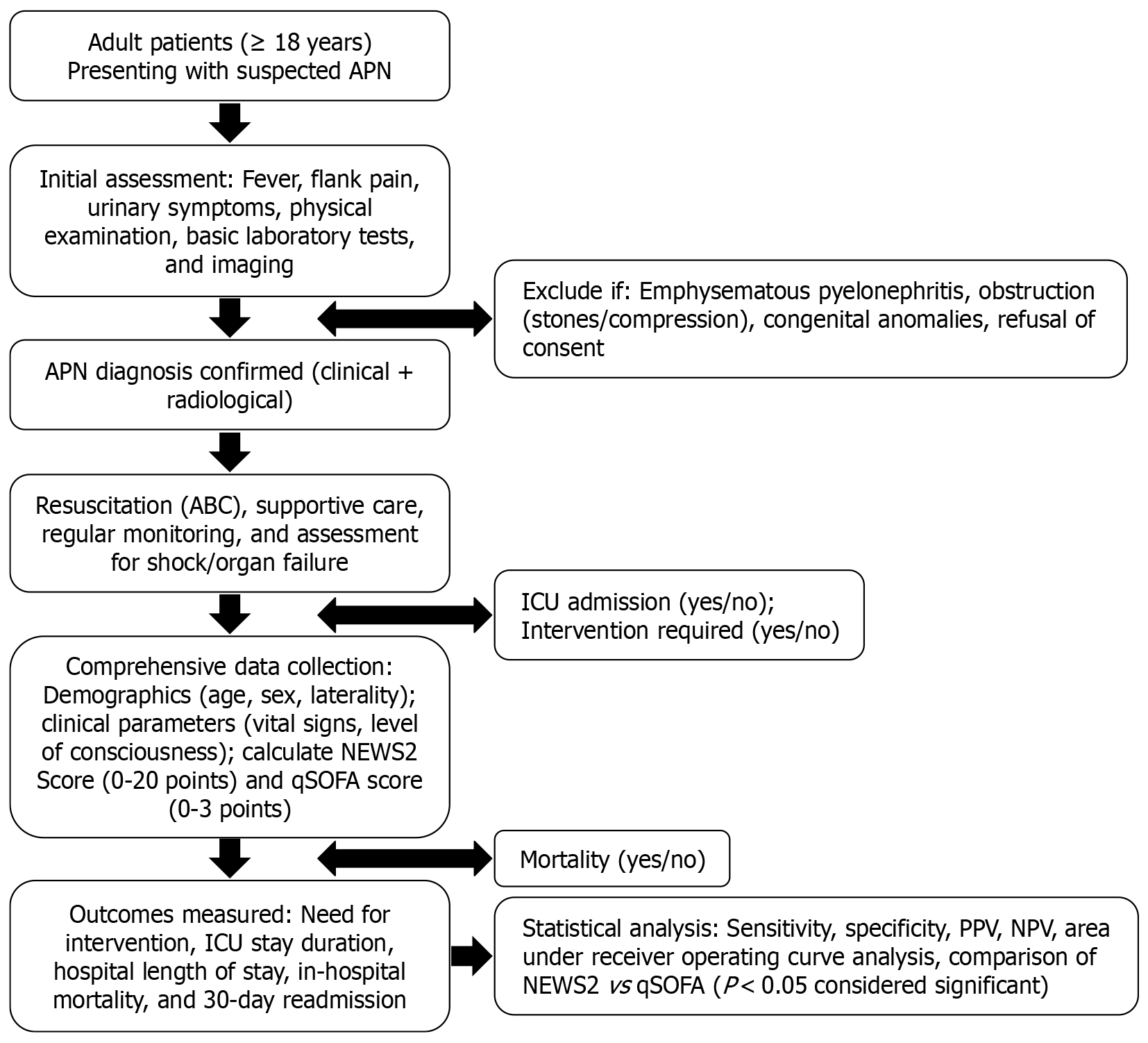
(1) Age ≥ 18 years; and (2) APN suspected at presentation with fever and/or flank pain and/or pyuria and/or costovertebral angle tenderness and/or sepsis, with supportive laboratory and radiological evidence obtained after stabilization.
(1) Age < 18 years; (2) Pregnancy; (3) Missing core variables required to compute NEWS2 or qSOFA at triage; and (4) EPN, stone related obstructive uropathy, congenital urinary tract abnormalities evidence documented on imaging.
After obtaining ethical clearance from the institutional research ethics committee, a prospective data collection protocol was established. The following data were collected from patients meeting the eligibility criteria using a standardized case record form designed specifically for this study. All enrolled patients were assessed within 24 hours of hospital admission or at first contact.
Demography and comorbidities, signs and symptoms, physiological vital parameters, laboratory and radiological reports, admission records including ICU stay, treatment records with response to treatment (recovery/mortality) were collected. NEWS2 and qSOFA scores were calculated simultaneously at first contact and thereafter as per the triggers reflected for each patient. The scoring was performed by the principal investigator, a resident of the department of urology, with assistance from colleagues of the same grade. Daily review of all entries was conducted by the principal in
All clinical assessments, laboratory investigations, and radiological studies were performed as part of routine clinical care. Data were extracted from direct patient assessment, patient chart reviews, electronic medical records, laboratory information systems, and picture archiving and communication systems. For patients requiring ICU admission, addi
Demographics: Age, sex, laterality of renal involvement.
Symptomatology and its duration: Fever, flank pain, pyuria, hematuria.
Clinical findings: Consciousness, Glasgow Coma Scale (GCS), temperature, pulse, shock [systolic blood pressure (SBP) < 90 mmHg or requiring vasopressors], respiratory rate, oxygen saturation at room air and need for oxygen, costovertebral angle tenderness/tender palpable kidney.
Comorbidities: Diabetes mellitus, hypertension, chronic kidney disease (CKD), and immunocompromised status.
Laboratory parameters: Haemoglobin, total leukocyte count, platelet count, serum creatinine, blood urea nitrogen, urine and blood culture with antibiotic sensitivity pattern.
Imaging: Ultrasonography kidney, ureter, and bladder (KUB) and computed tomography KUB to confirm the diagnosis of APN and exclude cases with obstructive renal or ureteric calculi and EPN. Findings including degree of renal paren
ICU Admission was defined as admission to a monitored intensive care setting at any time during the hospital stay, as per the institutional decision of the treating consultant based on the requirement of one or more organ support, sepsis care. Need for intervention, such as Placement of DJ stent or percutaneous nephrostomy (PCN) performed as part of source control during hospital stay, was at the discretion of the treating consultant based on clinical, laboratory and ra
Mortality was defined as death occurring during the same admission for the APN. Readmission within 30 days was defined as any unplanned readmission with urinary symptoms or sepsis within 30 days of discharge[12].
Scoring was applied at the time of presentation. The decision to stent, admit to the ICU, or escalate care was not influ
Based on these, the total score for the two scoring systems was calculated for each patient.
The NEWS2 score: Scores derived from 6 physiological parameters plus consciousness and oxygen requirement, yielding a total score from 0 to 20.
The qSOFA score: Score based on altered mental status (GCS < 15), SBP ≤ 100 mmHg, and respiratory rate ≥ 22/min, with a total score ranging from 0 to 3.
Data were entered into Microsoft Excel and analyses were conducted using IBM SPSS Statistics for Windows, Version 25.0 (IBM Corp., Armonk, NY, United States). Continuous variables are expressed as mean ± SD, while categorical variables are presented as n (%). Comparisons between groups were performed using independent t-tests for continuous data and χ2 or Fisher’s exact tests for categorical variables. Two-tailed P values < 0.05 were considered statistically significant, and 95% confidence intervals (CI) were reported. Statistical review was performed by a biomedical statis
Univariate analyses were first conducted to identify individual clinical and laboratory features significantly associated with ICU admission and in-hospital mortality. Multivariate logistic regression models to determine independent pre
A total of 220 patients with APN were evaluated, with a median age of 67 years. ICU admission was required in 47.7% of cases. On comparison of baseline demographic, clinical, and laboratory parameters, the median age was 56.3 for ICU-admitted patients and 56.2 for non-ICU admitted patients. Female patients constituted 55.9% of the total cohort, with a slightly higher proportion in the ICU group (58.1%). A total of 70 patients (32%) demonstrated the classical triad of fever, flank pain, and pyuria at presentation, reinforcing the observation that APN may not always follow textbook patterns, and that a high index of suspicion remains essential. Fever was the consistent symptom, present in 75% (n = 162) of the cohort. Hematuria and palpable kidney were relatively uncommon. Shock at presentation was observed in 18.18% overall but was far more common in ICU patients (36.19%) than in non-ICU patients (1.73%). Diabetes mellitus was a significant comorbidity, present in 71.6% of the overall cohort. Notably, this included patients with either acute kidney injury (AKI) (44%) or CKD (11.8%), suggesting that diabetic patients may be at a higher risk of renal compromise during APN epi
| Parameter | Group 1 (n = 105) | Group 2 (n = 115) | 95%CI | P value |
| Age in years (mean ± SD) | 56.3 ± 14 | 56.2 ± 14 | 53.6-59; 53.6-58.8 | 0.96 |
| Female sex | 61 (58.1) | 62 (53.9) | 48.7-67.5; 44.7-63.1 | 0.53 |
| Fever | 105 (100) | 57 (49.6) | 96.5-100; 40.6-58.7 | < 0.001 |
| Flank pain | 67 (63.8) | 22 (19.1) | 54.4-72.5; 12.6-27.1 | < 0.001 |
| Pyuria | 60 (57.1) | 22 (19.1) | 47.4-66.3; 12.6-27.1 | < 0.001 |
| Diabetes | 93 (88.6) | 64 (55.7) | 81.2-93.9; 46.3-64.9 | < 0.001 |
| CKD | 19 (18.1) | 12 (10.4) | 11.5-26.6; 5.5-17.5 | 0.11 |
| AKI | 60 (57.1) | 25 (21.7) | 47.4-66.3; 15-30.2 | < 0.001 |
| Temperature in degrees celsius (mean ± SD) | 38.8 ± 0.6 | 37.7 ± 1.05 | 38.6-38.9; 37.5-37.9 | < 0.001 |
| Pulse in beats/minute (mean ± SD) | 109 ± 15 | 82 ± 7 | 106-112; 81-83 | < 0.001 |
| SBP in mmHg (mean ± SD) | 91 ± 10 | 118 ± 8 | 89-93; 117-120 | < 0.001 |
| RR in breaths/minute (mean ± SD) | 28.3 ± 3.5 | 17.8 ± 2.2 | 27.6-29; 17.4-18.2 | < 0.001 |
| Total WBC count in × 109/L (mean ± SD) | 21 ± 2.3 | 14.8 ± 5.4 | 20.6-21.4; 13.8-15.8 | < 0.001 |
| Platelets in × 109/L (mean ± SD) | 141 ± 39 | 283 ± 77 | 191.2-222.8; 269-297 | < 0.001 |
| BUN in mmol/L (mean ± SD) | 17.3 ± 8.9 | 13.6 ± 7.5 | 16.6-21.7; 9.2-11.3 | < 0.001 |
| Serum creatinine in μmol/L (mean ± SD) | 230 ± 106 | 150 ± 71 | 188-271; 95-117 | < 0.001 |
| NEWS2 score (mean ± SD) | 14.7 ± 3.1 | 1.7 ± 1.3 | 14.1-15.3; 1.46-1.94 | < 0.001 |
| Intervention | 105 (100) | 51 (44.3) | 96.5-100; 35.3-53.7 | < 0.001 |
| Duration of stay in days (mean ± SD) | 9.2 ± 3.1 | 3.5 ± 1.3 | 8.6-9.8; 3.3-3.7 | < 0.001 |
| Mortality | 13 (12.4) | 1 (0.9) | 6.8-20; 0.02-5 | 0.01 |
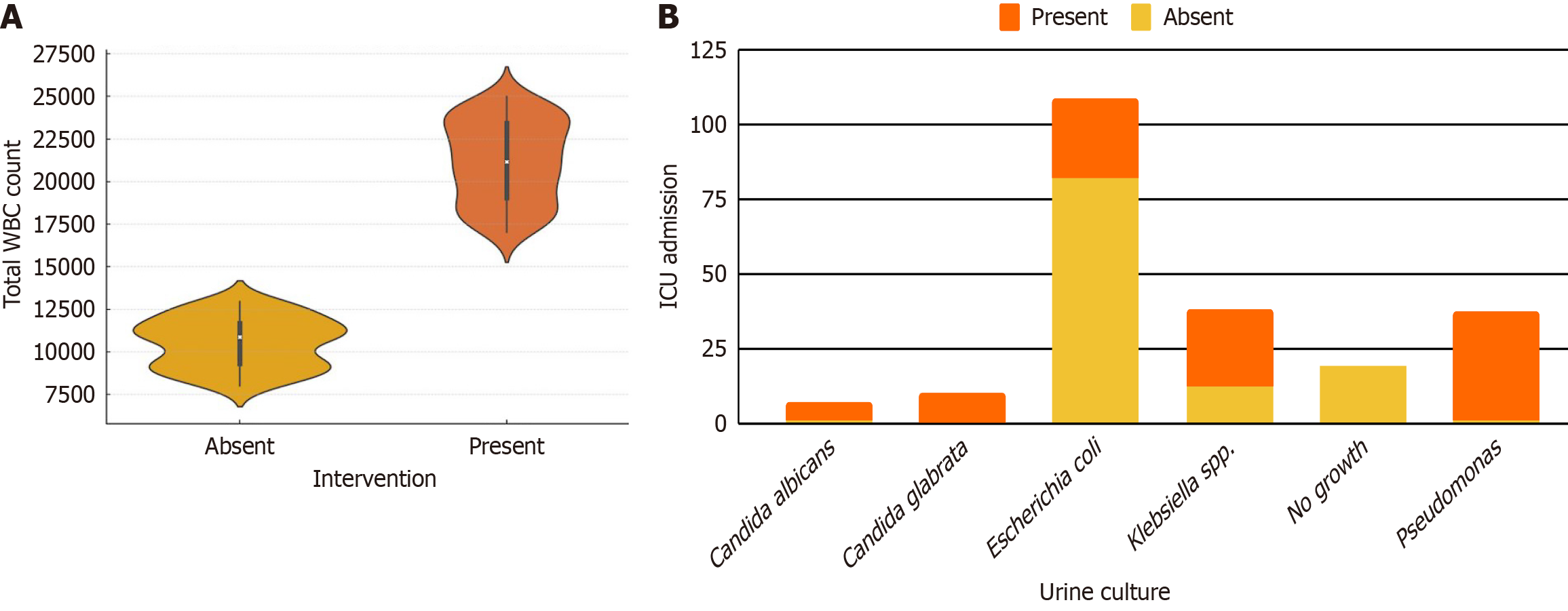
The patients who underwent DJ stenting had significantly higher white blood cell (WBC) counts at admission. The distribution, median, and interquartile ranges of WBC counts among patients who underwent and did not undergo intervention, reflecting an apparent upward shift in total counts among stented patients, with a median value of 21146/mm3. In contrast, the non-stented group had WBC counts predominantly under 12000/mm3. Urine culture revealed predominantly gram-negative colonization (Escherichia coli) in 109 patients across the cohort. Still, Klebsiella spp., Pseudomonas spp., and fungal pathogens, such as Candida species, were predominantly associated with ICU admissions (35%). Suggesting a potential association with more complicated or resistant infections (Figure 2).
The intervention in the form of the DJ stenting or PCN was performed in 70.9% of patients, often in those with ob
Patients who were admitted to the ICU tended to have significantly higher NEWS2 scores, specifically those with a score of 5 and above, which were consistent with progressive physiological compromise, affirming the need for ICU care. The difference in what each score captured became evident during analysis, showing the distribution of NEWS2 scores in patients who were either not admitted to the ICU or shifted later during the course. Those who required late ICU ad
The NEWS2 score appeared to identify early red flags and maintained a better balance of sensitivity and specificity across various thresholds. This makes it more practical in triage, especially in a setting like APN, where a patient can look okay and then deteriorate at a fast pace. Thus, making it the preferred tool for triage and escalation. Variables with cli
The multivariate logistic regression analysis that was performed to identify independent predictors of ICU admission and in-hospital mortality in patients with APN. Notably, classical symptoms such as fever, flank pain, and pyuria were excluded from the final model due to either lack of discriminatory power or collinearity with more robust physiological predictors. For ICU admission, the presence of diabetes mellitus (adjusted OR: 2.75; 95%CI: 1.40-5.38; P = 0.003), AKI at presentation (adjusted OR: 3.21; 95%CI: 1.62-6.38; P = 0.001), shock (SBP < 90 mmHg) at presentation (adjusted OR: 4.68; 95%CI: 2.12-10.33; P < 0.001), respiratory rate ≥ 22/min (adjusted OR: 3.89; 95%CI: 1.91-7.91; P < 0.001), thrombocytopenia with platelet count ≤ 150000/mm3 (adjusted OR: 2.77; 95%CI: 1.34-5.73; P = 0.006), and a NEWS2 score ≥ 5 (adjusted OR: 6.91; 95%CI: 2.84-16.83; P < 0.001) emerged as significant independent predictors. For mortality, shock at admission (adjusted OR: 5.96; 95%CI: 2.03-17.54; P = 0.001), thrombocytopenia (adjusted OR: 3.45; 95%CI: 1.18-10.07; P = 0.024), serum creatinine ≥ 2 mg/dL (adjusted OR: 2.64; 95%CI: 1.01-6.91; P = 0.048), and qSOFA score ≥ 2 (adjusted OR: 7.83; 95%CI: 2.16-28.39; P = 0.002) were independently associated with increased odds of death as depicted in Table 2.
| Parameter | Adjusted OR for ICU admission (95%CI) | P value | Adjusted OR for mortality (95%CI) | P value |
| Age ≥ 60 years | 1.24 (0.78-1.96) | 0.35 | 1.49 (0.72-3.11) | 0.28 |
| Female sex | 1.13 (0.68-1.87) | 0.62 | 0.98 (0.42-2.31) | 0.97 |
| Diabetes mellitus | 2.75 (1.40-5.38) | 0.003 | 1.96 (0.84-4.54) | 0.12 |
| AKI at admission | 3.21 (1.62-6.38) | 0.001 | 2.18 (0.91-5.21) | 0.08 |
| Shock (SBP < 90 mmHg) | 4.68 (2.12-10.33) | < 0.001 | 5.96 (2.03-17.54) | 0.001 |
| RR ≥ 22 breaths/min | 3.89 (1.91-7.91) | < 0.001 | 2.94 (1.02-8.50) | 0.047 |
| Total WBC count ≥ 15 × 109/L | 1.62 (0.89-2.94) | 0.11 | 2.01 (0.78-5.16) | 0.15 |
| Platelets ≤ 150 × 109/L | 2.77 (1.34-5.73) | 0.006 | 3.45 (1.18-10.07) | 0.024 |
| Creatinine ≥ 176.8 μmol/L | 1.98 (0.95-4.14) | 0.07 | 2.64 (1.01-6.91) | 0.048 |
| NEWS2 score ≥ 5 | 6.91 (2.84-16.83) | < 0.001 | 1.65 (0.61-4.48) | 0.32 |
| qSOFA score ≥ 2 | 2.14 (0.88-5.20) | 0.09 | 7.83 (2.16-28.39) | 0.002 |
These findings affirm the utility of integrating score-based and objective clinical parameters for early risk stratification and prognostication in APN. Overall, Trends in scoring, intervention, and outcomes suggest that the NEWS2 score shows a more prominent difference in the lower threshold, supporting its use in triage decisions. Although it lacks granularity in the high-risk group, due to significant clustering with a wide range, it is a comparatively weak predictor of mortality. Hence, both the NEWS2 and the qSOFA score offer value, but in different clinical domains, with the NEWS2 score being better aligned with ICU triage decisions, and the qSOFA score being more predictive of mortality risk.
APN continues to present a clinical challenge, particularly in identifying patients who may progress to severe illness requiring ICU care or those at risk of in-hospital mortality. In the acute setting, especially in urology, where intervention decisions like DJ stenting may be time sensitive, having a reliable, quick bedside scoring system becomes not just helpful but essential. In this study, two rapid scoring systems, NEWS2 and qSOFA were evaluated in patients with APN. The NEWS2 scoring tool was better suited to signal early physiological deterioration and prompt escalation towards ICU admission, consistent with previous literature reports that the NEWS2 scoring tool is preferable for early escalation in acute care settings[13,14]. On the other hand, the qSOFA scoring tool although more specific, lacked the sensitivity re
Importantly, our analysis showed that NEWS2 alone in several patients captured subtle physiological drift and triggered early ICU admission and intervention[15]. These cases highlight the value of a graded scoring system like NEWS2, which can capture mild-to-moderate shifts in physiology and prompt early review by urology or the ICU. On the contrary, qSOFA’s limited scope made it less sensitive to this window of opportunity, even though it aligned well with poor outcomes in patients who eventually deteriorated or were already in advanced stages of systemic illness.
Our multivariate analysis identified that along with NEWS2 score ≥ 5 few other parameters like diabetes mellitus, AKI, shock at presentation, tachypnea (respiratory rate ≥ 22/min), and thrombocytopenia as key independent predictors of ICU admission in patients with APN. These findings underscore the multifactorial nature of disease severity in APN, wherein both systemic inflammatory response and baseline comorbidities contribute to clinical deterioration. Inte
The differing nature of these scores likely explains their performance divergence. The NEWS2 score is continuous, graded, and sensitive to early shifts in physiology-traits ideal for triage and dynamic monitoring. In contrast, the qSOFA score is simpler and binary, focusing on late physiological decompensation markers like hypotension, altered mentation, and tachypnea, which explains its specificity for poor outcomes[16]. For in-hospital mortality, the most salient predictors were shock, elevated serum creatinine (≥ 2 mg/dL), thrombocytopenia, and a qSOFA score ≥ 2. This highlights the prognostic relevance of qSOFA in identifying patients at higher risk of fatal outcomes, aligning with prior literature emphasizing its utility in mortality prediction, particularly in sepsis-related contexts. Collectively, these findings support a dual-score strategy, wherein NEWS2 facilitates early triage and ICU escalation, while qSOFA offers enhanced specificity for predicting adverse outcomes. The independent associations observed affirm that combining clinical judgment with objective scoring metrics can significantly refine risk stratification and guide timely intervention in APN management.
By focusing this study on APN with non-stone obstruction or no anatomical cause, we attempted to reduce the con
Leveraging NEWS2 for escalation and qSOFA for outcome prediction may offer a balanced strategy for managing APN. Thus, integration of both scores, interpreted in the appropriate clinical context, provides a structured and objective framework for decision-making in APN. While numerous studies have validated NEWS2[21] and qSOFA[22] in the general sepsis population, their application to APN has remained superficial. These studies were often diluted by the inclusion of emphysematous cases or stone-induced obstruction that inherently signal clinical severity. These high-risk phenotypes tend to inflate the predictive accuracy of early warning scores, limiting their generalizability.
What sets our study apart is its deliberate exclusion of these extremes to isolate a more clinically ambiguous, yet highly prevalent subset: Non-obstructive, non-emphysematous APN. This “middle-ground” cohort is where the real diagnostic challenge lies. The patients who appear deceptively stable but harbour evolving systemic compromise. Prior literature has largely overlooked this group[23], despite representing a significant proportion of APN admissions. By examining scoring systems in this context, our findings offer a more pragmatic view: NEWS2 proved invaluable in detecting early physiological shifts and prompting escalation before overt decompensation, while qSOFA, although less sensitive upfront, emerged as a potent predictor of mortality once deterioration was underway.
This divergence in performance highlights the importance of aligning the scoring system with the clinical question, specifically triage vs prognosis, rather than treating these tools as interchangeable. In doing so, our study not only fills a critical gap in the current literature but also reframes how clinicians can strategically deploy these scores in the nuanced terrain of urological infections.
To the best of our knowledge, this is the first and largest prospective study in PubMed-indexed literature to systematically evaluate and compare the prognostic performance of the NEWS2 and qSOFA scores exclusively in adult patients with non-obstructive, non-emphysematous APN. Prior research has primarily been limited to retrospective or heterogeneous cohorts, often confounded by emphysematous infections or obstructive uropathy, thereby diminishing the generalizability of findings to the broader APN population.
By deliberately excluding these high-risk phenotypes, our study isolates a clinically challenging yet underrepresented subset of patients who frequently present with deceptively mild symptoms but are at genuine risk of rapid physiological deterioration. Through this focused lens, we demonstrate that the NEWS2 score offers superior sensitivity for early triage and escalation decisions, while the qSOFA score exhibits higher specificity for mortality prediction. Together, these findings fill a critical evidence gap and support a dual-score framework that is both pragmatic and transformative for risk stratification in urological sepsis.
Despite its strengths, this study has certain limitations. First, as a single-centre investigation conducted in a tertiary care setting, the findings may not be fully generalizable to other healthcare environments with differing resource availability and clinical practices. Second, the absence of an external validation cohort limits the ability to confirm the reproducibility of these results across diverse patient populations. Third, while the exclusion of emphysematous and obstructive pyelonephritis was intentional to reduce confounding, it may limit the applicability of the findings to more complex or high-risk cases often encountered in urological practice.
This study highlights that the NEWS2 score, with its broader physiological coverage, more reliably identifies patients with APN who require early ICU admission or intervention, offering a practical edge in triage at an acute care setting. In contrast, the qSOFA score correlates more closely with mortality, reinforcing its role as a specific prognostic indicator. Employing both scores in a complementary manner may enhance clinical decision-making and improve patient outcomes in APN.
| 1. | Angus DC, Seymour CW, Coopersmith CM, Deutschman CS, Klompas M, Levy MM, Martin GS, Osborn TM, Rhee C, Watson RS. A Framework for the Development and Interpretation of Different Sepsis Definitions and Clinical Criteria. Crit Care Med. 2016;44:e113-e121. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 129] [Cited by in RCA: 115] [Article Influence: 11.5] [Reference Citation Analysis (0)] |
| 2. | McGinley A, Pearse RM. A national early warning score for acutely ill patients. BMJ. 2012;345:e5310. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 122] [Cited by in RCA: 107] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 3. | Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA. 2016;315:801-810. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 22160] [Cited by in RCA: 19303] [Article Influence: 1930.3] [Reference Citation Analysis (5)] |
| 4. | Lamontagne F, Harrison DA, Rowan KM. qSOFA for Identifying Sepsis Among Patients With Infection. JAMA. 2017;317:267-268. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 24] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 5. | Pimentel MAF, Redfern OC, Gerry S, Collins GS, Malycha J, Prytherch D, Schmidt PE, Smith GB, Watkinson PJ. A comparison of the ability of the National Early Warning Score and the National Early Warning Score 2 to identify patients at risk of in-hospital mortality: A multi-centre database study. Resuscitation. 2019;134:147-156. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 139] [Cited by in RCA: 114] [Article Influence: 16.3] [Reference Citation Analysis (0)] |
| 6. | Krishnamoorthy S, Zumla A, Sekar H, Muneer A, Thiruvengadam G, Kumaresan N. Prognostic scoring system and risk stratification in patients with emphysematous pyelonephritis: an 11-year prospective study at a tertiary referral centre. BJU Int. 2021;127:418-427. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 7. | Chawla A, Bhaskara SP, Taori R, de la Rosette JJMCH, Laguna P, Pandey A, Mummalaneni S, Hegde P, Rao S, K P. Evaluation of early scoring predictors for expedited care in patients with emphysematous pyelonephritis. Ther Adv Urol. 2022;14:17562872221078773. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 8. | Chen L, Zheng H, Chen L, Wu S, Wang S. National Early Warning Score in Predicting Severe Adverse Outcomes of Emergency Medicine Patients: A Retrospective Cohort Study. J Multidiscip Healthc. 2021;14:2067-2078. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 23] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 9. | Riccalton V, Threlfall L, Ananthakrishnan A, Cong C, Milne-Ives M, Le Roux P, Plummer C, Meinert E. Modifications to the National Early Warning Score 2: a Scoping Review. BMC Med. 2025;23:154. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 10. | Krishnamoorthy S, Thiruvengadam G, Sekar H, Palaniyandi V, Ramadurai S, Narayanasamy S. Modified National Early Warning Score 2, a reliable early warning system for predicting treatment outcomes in patients with emphysematous pyelonephritis. World J Nephrol. 2025;14:103035. [PubMed] [DOI] [Full Text] |
| 11. | Williams B. The National Early Warning Score: from concept to NHS implementation. Clin Med (Lond). 2022;22:499-505. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 122] [Cited by in RCA: 90] [Article Influence: 22.5] [Reference Citation Analysis (0)] |
| 12. | Inada-Kim M. NEWS2 and improving outcomes from sepsis. Clin Med (Lond). 2022;22:514-517. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 12] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 13. | Herwanto V, Shetty A, Nalos M, Chakraborty M, McLean A, Eslick GD, Tang B. Accuracy of Quick Sequential Organ Failure Assessment Score to Predict Sepsis Mortality in 121 Studies Including 1,716,017 Individuals: A Systematic Review and Meta-Analysis. Crit Care Explor. 2019;1:e0043. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 41] [Article Influence: 5.9] [Reference Citation Analysis (1)] |
| 14. | Prasad PA, Fang MC, Abe-Jones Y, Calfee CS, Matthay MA, Kangelaris KN. Time to Recognition of Sepsis in the Emergency Department Using Electronic Health Record Data: A Comparative Analysis of Systemic Inflammatory Response Syndrome, Sequential Organ Failure Assessment, and Quick Sequential Organ Failure Assessment. Crit Care Med. 2020;48:200-209. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 28] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 15. | Tirkkonen J, Karlsson S, Skrifvars MB. National early warning score (NEWS) and the new alternative SpO(2) scale during rapid response team reviews: a prospective observational study. Scand J Trauma Resusc Emerg Med. 2019;27:111. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 12] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 16. | Lo RSL, Leung LY, Brabrand M, Yeung CY, Chan SY, Lam CCY, Hung KKC, Graham CA. qSOFA is a Poor Predictor of Short-Term Mortality in All Patients: A Systematic Review of 410,000 Patients. J Clin Med. 2019;8:61. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 37] [Cited by in RCA: 35] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 17. | Chen CC, Hsieh MS, Hu SY, Huang SC, Tsai CA, Tsai YC. Performance of Scoring Systems in Predicting Clinical Outcomes of Patients with Emphysematous Pyelonephritis: A 14-Year Hospital-Based Study. J Clin Med. 2022;11:7299. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 8] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 18. | Bedoui MA, Saadi A, Zaghbib S, Mokadem S, Boussaffa H, Hermi A, Ayed H, Bouzouita A, Chakroun M, Ben Slama R. Risk factors for sepsis and mortality in patients with emphysematous pyelonephritis : a series of 68 cases (case series). Ann Med Surg (Lond). 2024;86:240-244. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 19. | Myrstad M. Is NEWS2 good news for the early detection of sepsis? Tidsskr Nor Laegeforen. 2023;143. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 20. | Vincent JL, Grimaldi D. Quick sequential organ failure assessment: big databases vs. intelligent doctors. J Thorac Dis. 2016;8:E996-E998. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 21. | Thorén A, Joelsson-Alm E, Spångfors M, Rawshani A, Kahan T, Engdahl J, Jonsson M, Djärv T. The predictive power of the National Early Warning Score (NEWS) 2, as compared to NEWS, among patients assessed by a Rapid response team: A prospective multi-centre trial. Resusc Plus. 2022;9:100191. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 16] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 22. | Fernando SM, Tran A, Taljaard M, Cheng W, Rochwerg B, Seely AJE, Perry JJ. Prognostic Accuracy of the Quick Sequential Organ Failure Assessment for Mortality in Patients With Suspected Infection: A Systematic Review and Meta-analysis. Ann Intern Med. 2018;168:266-275. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 230] [Cited by in RCA: 194] [Article Influence: 24.3] [Reference Citation Analysis (0)] |
| 23. | Jain A, Manikandan R, Dorairajan LN, Sreenivasan SK, Bokka S. Emphysematous pyelonephritis: Does a standard management algorithm and a prognostic scoring model optimize patient outcomes? Urol Ann. 2019;11:414-420. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 28] [Article Influence: 4.0] [Reference Citation Analysis (0)] |