Published online May 19, 2026. doi: 10.5498/wjp.v16.i5.119366
Revised: April 9, 2026
Accepted: April 24, 2026
Published online: May 19, 2026
Processing time: 54 Days and 1.5 Hours
Although protective isolation measures are commonly used to control multidrug-resistant organisms (MDROs) transmission in healthcare settings, reducing social contacts often leads to social alienation for patients under isolation, which may lead to negative emotions and negatively affect recovery. Psychological resilience may protect against these effects; however, the relationship between psychological resilience and social alienation in isolated MDROs patients has not yet been studied. This study was aimed to assess social alienation of MDROs patients undergoing protective isolation and its correlation with psychological resilience.
To address the current situation of social alienation in patients with infected MDROs under protective isolation, and explore its relations to psychological resilience.
This study retrospectively investigated the clinical data and psychological assessment of 289 patients with MDROs infections who were placed on protective isolation in our hospital between January, 2020 and March, 2025. Social alienation was measured with the General Alienation Scale, and psychological resilience was assessed by the Chinese version of Connor-Davidson Resilience Scale. The correlation between social alienation and psychological resilience was evaluated by Pearson correlation analysis, and multiple linear regression analysis was performed to determine the influencing factors of social alienation.
The patients’ total social alienation score (29.87 ± 6.52) was at a moderate level, and 76.47% of the patients reported moderate or higher levels of social alienation. The mean general psychological resilience score was (56.34 ± 15.28). Pearson correlation analysis showed that the total score of social alienation was negatively correlated with the total score of psychological resilience (r = -0.463, P < 0.001), tenacity dimension (r = -0.448), strength dimension (r =
Patients with MDROs infection who underwent protective isolation experienced moderate degrees of social alienation that were negatively correlated with psychological resilience. Between clinical attention to the psychological state of patients with long isolation, fewer family visits and lower educational level and implement methods to improve psychological resilience and reduce social alienation.
Core Tip: Patients with multidrug-resistant organism infections often undergo protective isolation, which may adversely affect their psychosocial well-being. This study demonstrates that social alienation is prevalent among isolated patients and is moderately negatively correlated with psychological resilience. Lower family visit frequency, prolonged isolation, and lower educational level were associated with higher alienation, while greater tenacity and optimism were protective factors. These findings highlight the importance of integrating resilience-enhancing psychological interventions into the care of patients under protective isolation.
- Citation: Song M, Yan FJ, Liu YQ, Shen W, Han J, Mao SY. Correlation between social alienation and psychological resilience in patients with multidrug-resistant organism infections under protective isolation. World J Psychiatry 2026; 16(5): 119366
- URL: https://www.wjgnet.com/2220-3206/full/v16/i5/119366.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i5.119366
Multidrug-resistant organisms (MDROs) infections are a global public health concern[1]. It has been reported that the detection of MDROs is increasing each year, likely related to the widespread use of antimicrobial agents in recent years. Transmission of MDROs, such as methicillin-resistant Staphylococcus aureus (MRSA) and carbapenem-resistant Enterobacteriaceae (CRE), has become a major challenge to nosocomial infection prevention and control especially in healthcare facilities[2]. Protective isolation measures have thus been widely adopted in clinical practice to break the transmission chain of MDROs in hospital settings, commonly through single-room isolation, contact precautions and limiting access to personnel[3]. But, while containment of the infection spread, isolation measures not only had no insignificant negative effects on patients’ psychology[4].
Social alienation is described as a subjective psychological state in which individuals subjectively perceive some distance or disconnection between themselves and their social environment, manifesting feelings of social isolation, meaninglessness and self-alienation[5]. Non-patient studies have shown that patients who are hospitalized and receiving isolation treatment tend to develop increased levels of social alienation due to limitations on physical space, decreased social activities and disease prognosis[6]. Extended periods of alienation can result in negative psychological feelings, such as anxiety and depression[7], which raises concerns about adherence to treatment and development recovery. Psychological resilience is defined as an individual’s ability to show good adaptation in the face of adversity, trauma, or significant stress[8]. Higher levels of psychological resilience enables people to preserve a positive attitude during managing stress or coping with diseases and support mental health[9]. However, the majority of current domestic and international studies on psychological status in patients with MDROs infections mainly focus on evaluating negative emotions, including anxiety and depression[10], while investigation of social alienation in patients under protective isolation and its relationship to psychological resilience is still insufficient[11]. Based on this background, the purpose of this study was to explore the current status of social alienation in MDROs infections patients under protective isolation and its relationship with psychological resilience to provide reference evidence for clinical nursing interventions[12].
This study is built on these three established frameworks: (1) Seeman’s multiform conceptualization of alienation recognizes five key dimensions – powerlessness, meaninglessness, normlessness, social isolation and self-estrangement – all of which can be systematically evoked through the physical and relational restrictions imposed by protective isolation[5]; (2) According to Lazarus and Folkman’s transactional model of stress and coping individual cognitive appraisal processes mediate the association between objective stressors and subjective psychological outcomes; thus, a patient’s appraissal of isolation as threatening vs manageable may greatly explain the degree of alienation experienced[8]; and (3) Richardson’s resilience reintegration theory suggests that people with stronger psychological resilience are more able to reintegrate in an adaptive way following disruption using internal strengths and external resources to restore a sense of meaning and connection[9]. Thus, these frameworks help to create a cohesive conceptual model for why psychological resilience might protective against social alienation in the context of MDROs isolation and provide guidance for the clinical interventions outlined in this study.
We conducted this study as a retrospective analysis using data that were routinely recorded in the hospital’s electronic medical record system and nursing psychological assessment record system to examine if social alienation correlated with psychological resilience in patients with MDROs infections under protective isolation. The Medical Ethics Committee of the hospital approved the study protocol. Since this was a retrospective analysis based on routine clinical assessment records and data were anonymized, the local ethics committee approved the waiver of informed consent.
We retrospectively collected clinical data and psychological assessment records of patients with infections caused by MDROs who had been hospitalized and received protective isolation in our hospital from January 2020 to March 2025. All patients who met the inclusion criteria during the study period were included using consecutive sampling.
Inclusion criteria: (1) Age ≥ 18 years; (2) Diagnosed MDROs infection according to the bacterial culture and antimicrobial susceptibility testing, including MRSA, CRE, vancomycin-resistant enterococci, multidrug-resistant Pseudomonas aeruginosa, and multidrug-resistant Acinetobacter baumannii; (3) Protective isolation measures performed per the hospital infection management regulations with an isolation time of ≥ 72 hours; (4) Clear conscious state as assessed by Glasgow Scale Coma score ≥ 15, normal cognitive functions based on Mini-Mental State Examination score ≥ 24 point, and able to cooperate in completing questionnaires; and (5) Finally for criterion No. five being complete medical records with psych
Inclusion criteria: (1) Patients who completed the questionnaire independently and signed informed consent; (2) Patients aged between 18 years and 75 years; and (3) Patients who had been admitted to the department for at least one week.
Exclusion criteria: (1) Patients with severe mental disorders confirmed by psychiatric consultation (including schizophrenia, acute episodes of bipolar disorder, major depressive disorder, etc.); (2) Critically ill patients with unstable vital signs; (3) Questionnaire data missing more than 20% or showing obvious patterns of responses (e.g., selecting the same option for subsequent ≥ 10 questions ); and (4) Patients transferred to intensive care unit due to disease deterioration during hospitalization. Ultimately, 289 patients were included.
General information questionnaire: The general information questionnaire was developed based on the relevant literature and reviewed by five experts in nursing science and infectious diseases. The contents included demographic data (age, sex, marital status, educational level, employment status) and disease-related data (MDROs type and infection site; isolation duration; length of hospital stay; number of underlying diseases; whether it was the first MDROs infection in this patient; frequency of family visits). Frequency of family visit was classified into: (1) No visits (0 times/week); (2) Occasional visits (1-2 times/week); (3) Frequent visits (3-4 times/week); and (4) Daily visits (≥ 5 times/week).
General Alienation Scale: General Alienation Scale is designed to assess the extent of alienation regarding their terrestrial social environment, as well as from components such as social isolation, meaninglessness, powerlessness and self-alienation. The scale consists of 12 items on a 4-point Likert scale (1 = strongly disagree, 2 = disagree, 3 = agree, and 4 = strongly agree), in which the reverse-scored items are: (1) Item 2; (2) Item 4; (3) Item 7; and (4) Item 10. The total score can go from 12 to 48 and a higher score means more social alienation. Total scores were divided into as follows: (1) Low alienation (12-23); (2) Moderate alienation (24-35); and (3) High alienation (36-48).
Psychological Resilience Scale: Data were collected using the Chinese version of the Connor-Davidson Resilience Scale. This scale includes 25 items comprising three dimensions: (1) Tenacity (13 items); (2) Strength (8 items); and (3) Optimism (4 items). A 5-point Likert scale is employed (0 = never, 1 = rarely, 2 = sometimes, 3 = often, 4 = almost always), and the total scores may range from 0 to a maximum score of 100. Higher values indicate greater psychological resilience.
Using SPSS 26.0 statistical software to analyze data. Continuous variables were assessed for normality using the Shapiro-Wilk test. Normally distribution continuous variables were presented as mean ± SD with intergroup comparison by independent samples t-test or one-way analysis of variance. Continuous variables that did not conform to a normal distribution were presented as median with interquartile range, and the comparison between groups was based on either Mann-Whitney U test or Kruskal-Wallis H test. Categorical variables were presented as n (%) and differences between groups were compared with the χ2 test. We explored the correlation between social alienation and psychological resilience using Pearson correlation analysis or Spearman rank correlation analysis. Absolute values of correlation coefficient r were classified according to the following: (1) < 0.3 weak correlation; (2) 0.3 ≤ |r| < 0.5 moderate correlation; and (3) |r| ≥ 0.5 strong correlation. Multiple linear regression analysis was conducted in which total score of social alienation was taken as dependent variable, and the variables with P < 0.05 in univariate analysis and scores of each psychological resilience dimension were taken as independent variables to determine influencing factors for social alienation. F-test was used to test the overall regression equation, while t-test was used to test the significance of individual coefficients for inde
All patients who received MDROs infections during protective isolation from the ward were included (full-final analysis, aged 18-89 years old with mean age of 58.43 ± 14.76 years). Of them, 167 (57.79%) were male and 122 (42.21%) were female. The most prevalent type of MDROs found in this study was MRSA, which was present in 98 (33.91%) cases, followed by CRE with 72 (24.91%) cases, multidrug-resistant Acinetobacter baumannii with 56 (19.38%) cases, Multidrug-Resistant Pseudomonas aeruginosa with 41 (14.19%) cases and vancomycin-resistant enterococci with 22 (7.61%) cases as shown in Table 1. Most of the infections were localized to the respiratory tract (112 cases, 38.75%) length of isolation varied from 3 days to 42 days with 12.58 ± 6.34 days mean period of isolation. Hospitalization period ranged from 7 days to 68 days (mean: 21.73 ± 10.52). The other general characteristics are shown in Table 2.
| Variable | Category | n | Social alienation score | t/F value | P value |
| Sex | Male | 167 | 29.56 ± 6.38 | 1.024 | 0.307 |
| Female | 122 | 30.29 ± 6.71 | |||
| Age (years) | 18-44 | 52 | 27.35 ± 5.89 | 5.672 | 0.001 |
| 45-59 | 78 | 29.18 ± 6.24 | |||
| 60-74 | 104 | 30.76 ± 6.58 | |||
| ≥ 75 | 55 | 31.84 ± 6.73 | |||
| Marital status | Unmarried | 31 | 31.42 ± 6.87 | 4.358 | 0.014 |
| Married | 198 | 29.23 ± 6.31 | |||
| Divorced/widowed | 60 | 31.48 ± 6.82 | |||
| Educational level | Primary school or below | 67 | 32.16 ± 6.74 | 7.893 | < 0.001 |
| Junior high school | 82 | 30.45 ± 6.28 | |||
| High school/technical secondary school | 74 | 29.12 ± 6.19 | |||
| College or above | 66 | 27.24 ± 5.96 | |||
| Employment status | Employed | 89 | 29.13 ± 6.27 | 1.842 | 0.161 |
| Retired | 132 | 30.38 ± 6.64 | |||
| Unemployed/other | 68 | 29.82 ± 6.53 | |||
| MDROs type | Methicillin-resistant Staphylococcus aureus | 98 | 29.54 ± 6.42 | 0.756 | 0.555 |
| Carbapenem-resistant Enterobacteriaceae | 72 | 30.18 ± 6.67 | |||
| Multidrug-resistant Acinetobacter baumannii | 56 | 30.32 ± 6.58 | |||
| Multidrug-resistant Pseudomonas aeruginosa | 41 | 29.46 ± 6.34 | |||
| Vancomycin-resistant enterococci | 22 | 30.64 ± 6.89 | |||
| Infection site | Respiratory tract | 112 | 30.12 ± 6.54 | 0.423 | 0.792 |
| Urinary tract | 68 | 29.68 ± 6.37 | |||
| Bloodstream | 43 | 30.26 ± 6.78 | |||
| Skin and soft tissue | 38 | 29.34 ± 6.42 | |||
| Other | 28 | 29.82 ± 6.56 | |||
| Isolation duration (days) | 3-7 | 82 | 27.64 ± 5.86 | 12.348 | < 0.001 |
| 8-14 | 118 | 29.72 ± 6.24 | |||
| ≥ 15 | 89 | 32.36 ± 6.78 | |||
| Length of hospital stay (days) | 7-14 | 76 | 27.82 ± 5.92 | 8.965 | < 0.001 |
| 15-28 | 131 | 29.64 ± 6.28 | |||
| ≥ 29 | 82 | 32.18 ± 6.86 | |||
| Number of underlying diseases | 0-1 | 54 | 27.52 ± 5.94 | 6.873 | 0.001 |
| 2-3 | 137 | 29.68 ± 6.32 | |||
| ≥ 4 | 98 | 31.54 ± 6.82 | |||
| First MDROs infection | Yes | 196 | 29.24 ± 6.28 | -2.316 | 0.021 |
| No | 93 | 31.19 ± 6.84 | |||
| Frequency of family visits | No visits | 34 | 34.56 ± 6.92 | 14.726 | < 0.001 |
| Occasional visits | 87 | 31.42 ± 6.47 | |||
| Frequent visits | 102 | 28.76 ± 5.98 | |||
| Daily visits | 66 | 26.58 ± 5.64 |
| Variable | Category | n | Percentage |
| Sex | Male | 167 | 57.79 |
| Female | 122 | 42.21 | |
| Age (years) | 18-44 | 52 | 17.99 |
| 45-59 | 78 | 26.99 | |
| 60-74 | 104 | 35.99 | |
| ≥ 75 | 55 | 19.03 | |
| Marital status | Unmarried | 31 | 10.73 |
| Married | 198 | 68.51 | |
| Divorced/widowed | 60 | 20.76 | |
| Educational level | Primary school or below | 67 | 23.18 |
| Junior high school | 82 | 28.37 | |
| High school/technical secondary school | 74 | 25.61 | |
| College or above | 66 | 22.84 | |
| Employment status | Employed | 89 | 30.8 |
| Retired | 132 | 45.67 | |
| Unemployed/other | 68 | 23.53 | |
| MDROs type | Methicillin-resistant Staphylococcus aureus | 98 | 33.91 |
| Carbapenem-resistant Enterobacteriaceae | 72 | 24.91 | |
| Multidrug-resistant Acinetobacter baumannii | 56 | 19.38 | |
| Multidrug-resistant Pseudomonas aeruginosa | 41 | 14.19 | |
| Vancomycin-resistant enterococci | 22 | 7.61 | |
| Infection site | Respiratory tract | 112 | 38.75 |
| Urinary tract | 68 | 23.53 | |
| Bloodstream | 43 | 14.88 | |
| Skin and soft tissue | 38 | 13.15 | |
| Other | 28 | 9.69 | |
| Isolation duration (days) | 3-7 | 82 | 28.37 |
| 8-14 | 118 | 40.83 | |
| ≥ 15 | 89 | 30.8 | |
| Length of hospital stay (days) | 7-14 | 76 | 26.3 |
| 15-28 | 131 | 45.33 | |
| ≥ 29 | 82 | 28.37 | |
| Number of underlying diseases | 0-1 | 54 | 18.69 |
| 2-3 | 137 | 47.4 | |
| ≥ 4 | 98 | 33.91 | |
| First MDROs infection | Yes | 196 | 67.82 |
| No | 93 | 32.18 | |
| Frequency of family visits | No visits | 34 | 11.76 |
| Occasional visits (1-2 times/week) | 87 | 30.1 | |
| Frequent visits (3-4 times/week) | 102 | 35.29 | |
| Daily visits (≥ 5 times/week) | 66 | 22.84 |
The social alienation total score of the 289 patients with MDROs infections under protective isolation was 29.87 ± 6.52, and item mean score was 2.49 ± 0.54. Total 68 Urban patients (23.53%) had low alienation, 178 patients (61.59%) had moderate alienation and 43 patients (14.88%) had high alienation. The mean score of the psychological resilience scale was 56.34 ± 15.28. Results for each dimension are displayed in Table 3.
| Scale/dimension | Number of items | Score range | Actual score | Item mean score |
| Total social alienation score | 12 | 12-48 | 29.87 ± 6.52 | 2.49 ± 0.54 |
| Total psychological resilience score | 25 | 0-100 | 56.34 ± 15.28 | 2.25 ± 0.61 |
| Tenacity | 13 | 0-52 | 28.96 ± 8.43 | 2.23 ± 0.65 |
| Strength | 8 | 0-32 | 18.52 ± 5.17 | 2.32 ± 0.65 |
| Optimism | 4 | 0-16 | 8.86 ± 2.94 | 2.22 ± 0.74 |
The results of univariate analysis indicated a statistically significant differences in social alienation scores among patients from different groups, including age, marital status, educational level, isolation duration, hospitalization duration, number of underlying diseases, first MDROs infection or not and frequency of family visits (P < 0.05). Patients with different sex, employment status, MDROs type and infection site had similar social alienation scores (P > 0.05). Details are shown in Table 1.
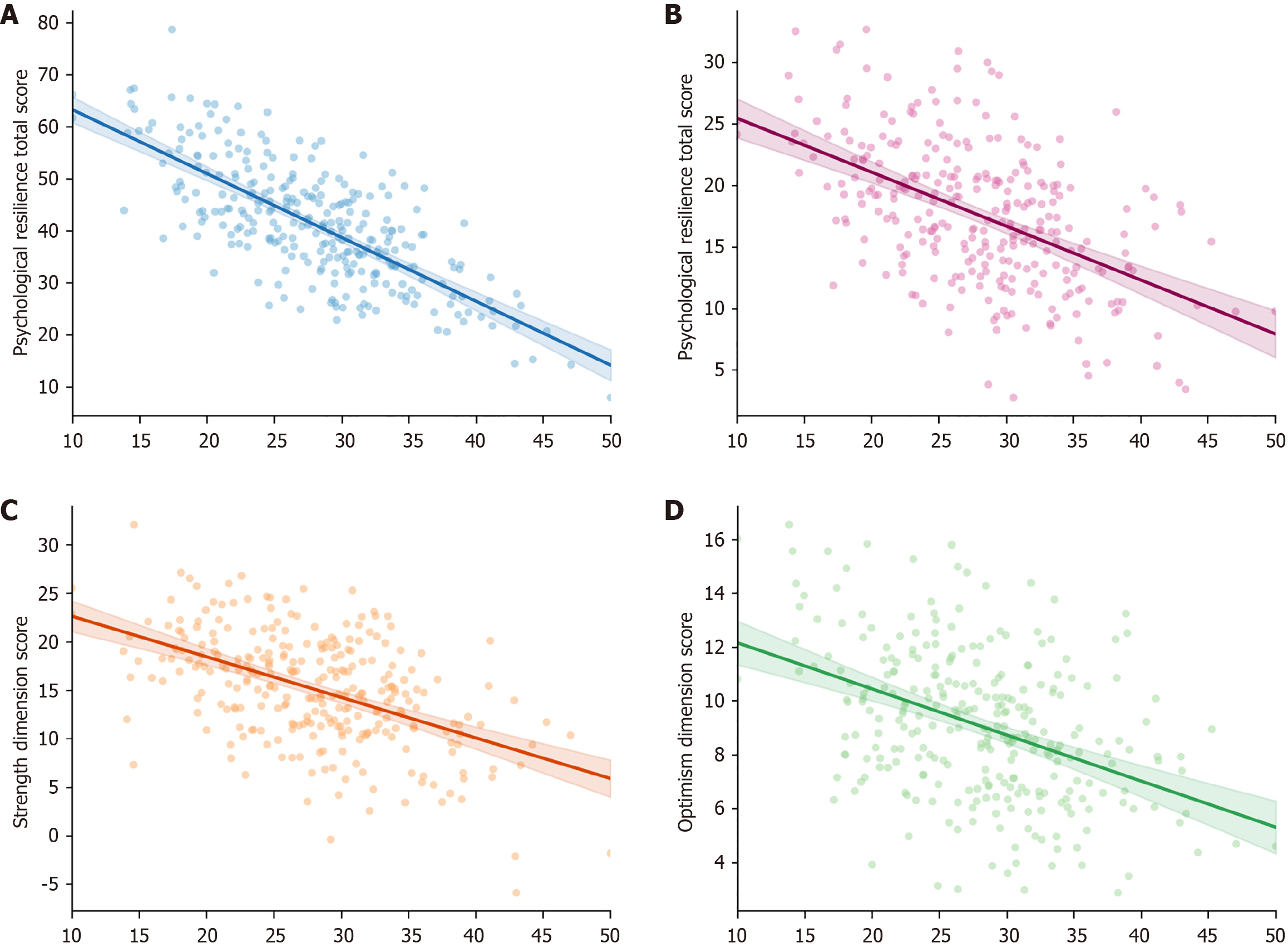
Pearson correlation analysis results showed that the total social alienation score of patients with MDROs infections under protective isolation was negatively correlated with the total psychological resilience score and scores of all dimensions (P < 0.001). The total social alienation score showed moderate negative correlation with total psychological resilience score (r = -0.463), moderate negative correlation with tenacity dimension (r = -0.448), moderate negative correlation with strength dimension (r = -0.421), and moderate negative correlation with optimism dimension (r = -0.386) (Table 4, Figure 1).
With total social alienation score as the dependent variable, variables with statistical significance in univariate analysis (age, marital status, educational level, isolation duration, length of hospital stay, number of underlying diseases, whether first MDROs infection, and frequency of family visits) and scores of each psychological resilience dimension were entered as independent variables in multiple linear regression analysis. The assignment method for independent variables is shown in Table 5.
| Independent variable | Assignment method |
| Age | 18-44 years = 1, 45-59 years = 2, 60-74 years = 3, ≥ 75 years = 4 |
| Marital status | Married = 1, unmarried = 2, divorced/widowed = 3 |
| Educational level | College or above = 1, high school/technical secondary school = 2, junior high school = 3, primary school or below = 4 |
| Isolation duration | 3-7 days = 1, 8-14 days = 2, ≥ 15 days = 3 |
| Length of hospital stay | 7-14 days = 1, 15-28 days = 2, ≥ 29 days = 3 |
| Number of underlying diseases | 0-1 = 1, 2-3 = 2, ≥ 4 = 3 |
| First multidrug-resistant organisms infection | Yes = 0, no = 1 |
| Frequency of family visits | Daily visits = 1, frequent visits = 2, occasional visits = 3, no visits = 4 |
| Tenacity | Original value entered |
| Strength | Original value entered |
| Optimism | Original value entered |
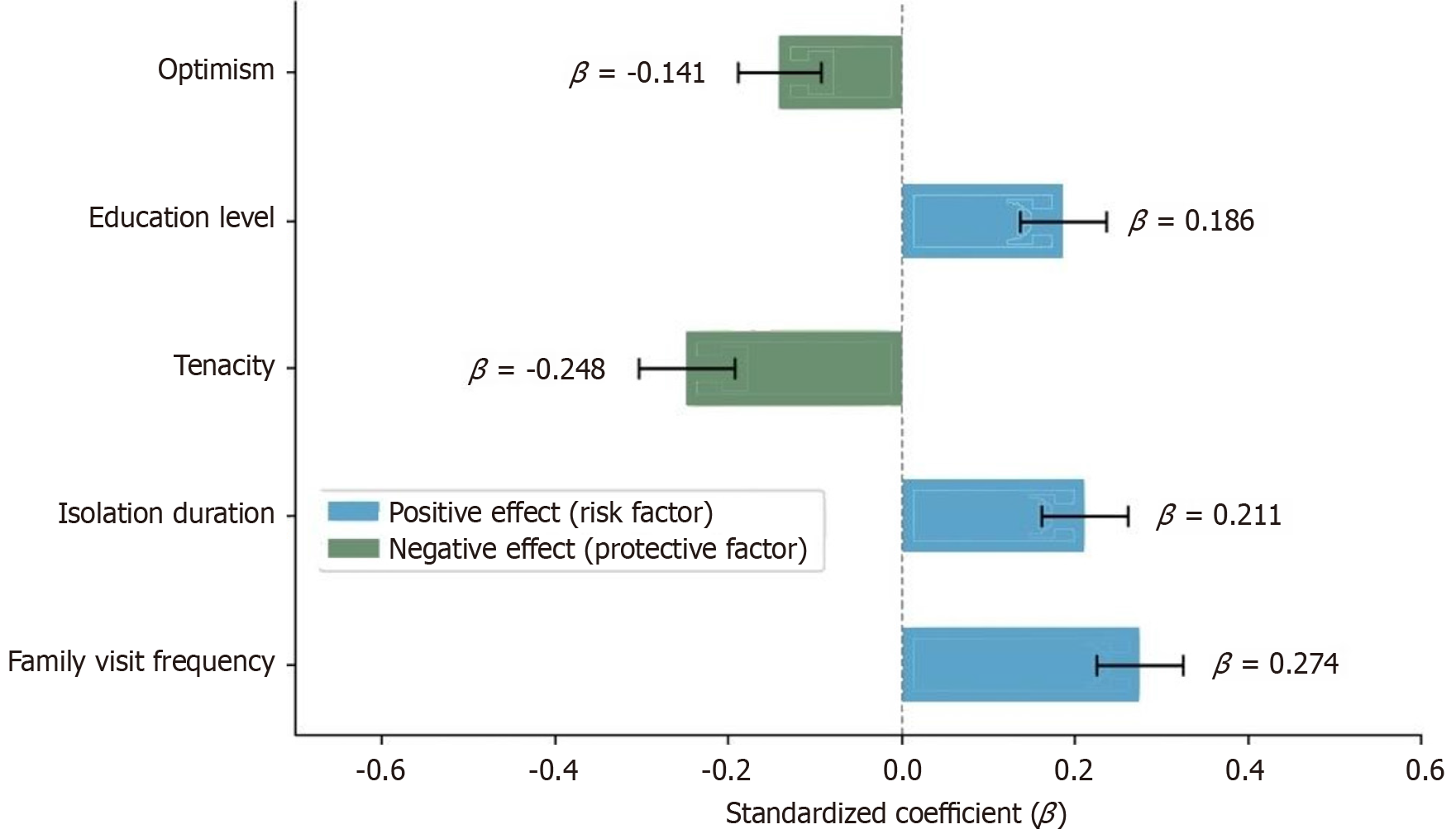
Multiple linear regression analysis results showed that frequency of family visits, isolation duration, tenacity, educational level, and optimism were independent factors influencing social alienation in patients with MDROs infections under protective isolation (P < 0.05), explaining 49.8% of the total variance in social alienation (Table 6, Figure 2).
| Variable | B | SE | β | t value | P value | 95%CI |
| Constant | 36.842 | 2.054 | - | 17.936 | < 0.001 | 32.798-40.886 |
| Frequency of family visits | 1.924 | 0.302 | 0.274 | 6.371 | < 0.001 | 1.330-2.518 |
| Isolation duration | 1.586 | 0.308 | 0.211 | 5.149 | < 0.001 | 0.980-2.192 |
| Tenacity | -0.192 | 0.038 | -0.248 | -5.053 | < 0.001 | -0.267 to -0.117 |
| Educational level | 0.968 | 0.218 | 0.186 | 4.44 | < 0.001 | 0.539-1.397 |
| Optimism | -0.312 | 0.084 | -0.141 | -3.714 | < 0.001 | -0.477 to -0.147 |
The total score of social alienation of patients with MDROs infections in protective isolation was 29.87 ± 6.52. Moderate level, and 76.47% of patients were moderate or more alienation. The sanity showed that this population social alienation is serious generally. These findings are comparable with domestic survey results on isolated infectious disease patients[13] but indicate higher alienation than those noted in general hospitalized patients[14]. The reasons are probably the patients with MDROs infections not only suffer from the physical and psychological stress brought about by the infectious disease itself but also experience limited social contact due to isolation environment. Healthcare workers with personal protective equipment when entering the patient rooms might also unconsciously augment patients’ feelings of being “isolated”[15]. Moreover, some patients may have cognitive biases regarding MDROs infection, fearing to be judged as the “source of infection”, which creates illness-related stigma and worsens their experience of social alienation[16].
The finding of 76.47% moderate-to-high social alienation among the patients has significant clinical and ethical implications that need to be discussed explicitly. From a clinical standpoint, this prevalence rate indicates that social alienation is not an occasional or minority experience but rather a nearly universal psychological cost of the burden in this group, one that requires systematic – as opposed to discretionary – psychosocial support. Routine alienation screening and proactive psychological support should be integrated as non-negotiable aspects of care within standard MDROs isolation protocols. From an ethical perspective, the data illuminate a tension inherent to protective isolation: A protocol aimed at protecting both the individual patient and larger ward community from infectious transmission simultaneously places measurable and systematic psychological burdens on the very patients whom that protocol aims to protect. Healthcare institutions have an obligation to do no harm according to the bioethical principle of non-maleficence, and therefore a duty of care exists to monitor and combat this unintended harm. Practically, this requires infection control committees to formally evaluate the psychological effects of isolation protocols as part of routine policy reviews; ward-level psycho
This study showed that patients’ social alienation was strongly correlated with the frequency of visits by family members. The social alienation score of patients without visits were significantly higher than daily visiting ones, which is consistent with the theory of social support[17]. Besides offering emotional comfort, family visits also serve a major function in preserving patients’ connectivity as they venture further into the external world, knowing that they were still being cared for and belonged[18]. Nevertheless, protective isolation measures objectively hinder visits, and some family members decrease frequency of visits out of the worry to become infected[19]. Hence, we recommend a flexible policy to visitation XXXractices in healthcare institutions while infection prevention and control measures are applied at all times strictly; for instance moderate increased visit frequency is acceptable with trained family members them about the rules of protective suggestions conducted uniformly and using video calls as an alternative for face-to-face conversation[20].
There was a significantly positive relationship between the duration of infection isolation and social alienation i.e., longer duration of infection isolation for patients was associated with stronger social alienation feeling. This outcome matches conclusions of earlier research[21]. Long-term restrictions of social roles in a closed environment lead to interference with daily life cycles, and making them more vulnerable to meaninglessness and powerlessness feelings[22]. The social alienation scores were significantly higher in patients whose isolation time was more than or equal to 15 days, which indicated that clinicians should pay attention on the psychological changes of patients who had a long duration of isolation (Table 1). They recommend that health care providers intensify psychological screening among those isolated beyond 2 weeks, identify and treat high-risk patients[23].
Lower educational patients were more socially alienated. This may be associated with their health literacy levels[23], as patients with lower educational levels have a relatively lack of knowledge on MDROs infection and isolation measures, making them more likely to fall into fear and confusion[24]. At the same time, this population has relatively constrained options to access information and emotional support, along with lower cognitive resources to cope with stress[25]. Thus, nursing personnel should emphasize the use of “easy to understand” language in health education and use illustrated materials to help patients further comprehend the necessity and temporary nature of isolation, which can reduce their psychological burden[26].
The main finding of the current study was a significant moderate negative correlation between social alienation with psychological resilience. Both the total score of psychological resilience and all three dimensions, i.e., tenacity, strength, and optimism were negatively correlated with social alienation; specifically, tenacity and optimism emerged as independent protective factors against social alienation in the regression equation. Tenacity indicates a person’s persistence and adaptability when confronting challenges[27]; therefore, patients with high tenacity are more likely to interpret isolation as a temporary phase in the course of treatment rather than a permanent divorce from society. Op
The regression model presented In”this’analysis explains 49.8% of the total variance in social alienation, which suggests that close to 50% of the variance arises from other unaccounted for factors. Previous literature implicates nurse-patient relationship quality, comfort of ward environment and back to the fellow patients in room interaction[32] that may also modulate psychological experience in grouped patients even isolation[4]. Moreover, this study was a single-center retrospective study so that the sample representativeness would be limited[33]. The current study has several other limitations that deserve explicit acknowledgment. First, the retrospective design and exclusion of patients who could not complete psychological assessments because of serious illness, unstable vital signs, or cognitive impairment may have created a systematic selection bias in favor of those with better clinical and cognitive status. These excluded people are probably a particularly vulnerable subgroup – those with higher disease burden and, for that reason, likely greater levels of social alienation – whose psychological patterns cannot be gleaned from the current analysis. As a result, the results of this study may not accurately represent both the prevalence and severity of social alienation in the wider MDROs iso
Several directions for future research are indicated by the findings and limitations of the current study. First, multicenter prospective cohort studies with larger, more representative samples including patients who are currently excluded due to cognitive impairment or critical illness are needed to establish the generalizability of the observed associations and to capture the full spectrum of psychological burden in this population. Second, randomized controlled trials evaluating specific resilience-enhancing intervention programs such as acceptance and commitment therapy, positive psychology-based nursing protocols, or digitally delivered mindfulness training – in MDROs isolation patients are needed to move from correlation to causation and to provide the evidence base required for guideline development.
In summary, social alienation in patients with MDROs infections under protective isolation is at a moderate level. Low frequency of family visits, prolonged isolation duration, and low educational level are risk factors for social alienation, while higher levels of tenacity and optimism are protective factors. Clinical nursing should focus on the psychological status of patients with prolonged isolation, lack of family support, and low educational levels, while emphasizing the cultivation of psychological resilience to alleviate patients’ social alienation experience and promote physical and psychological recovery.
| 1. | Asokan GV, Ramadhan T, Ahmed E, Sanad H. WHO Global Priority Pathogens List: A Bibliometric Analysis of Medline-PubMed for Knowledge Mobilization to Infection Prevention and Control Practices in Bahrain. Oman Med J. 2019;34:184-193. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 96] [Cited by in RCA: 252] [Article Influence: 36.0] [Reference Citation Analysis (0)] |
| 2. | Weiner-Lastinger LM, Pattabiraman V, Konnor RY, Patel PR, Wong E, Xu SY, Smith B, Edwards JR, Dudeck MA. The impact of coronavirus disease 2019 (COVID-19) on healthcare-associated infections in 2020: A summary of data reported to the National Healthcare Safety Network. Infect Control Hosp Epidemiol. 2022;43:12-25. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 228] [Article Influence: 57.0] [Reference Citation Analysis (0)] |
| 3. | Teerawattanapong N, Kengkla K, Dilokthornsakul P, Saokaew S, Apisarnthanarak A, Chaiyakunapruk N. Prevention and Control of Multidrug-Resistant Gram-Negative Bacteria in Adult Intensive Care Units: A Systematic Review and Network Meta-analysis. Clin Infect Dis. 2017;64:S51-S60. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 64] [Cited by in RCA: 96] [Article Influence: 12.0] [Reference Citation Analysis (0)] |
| 4. | Vuichard-Gysin D, Nueesch R, Fuerer RL, Dangel M, Widmer A. Measuring perception of mental well-being in patients under isolation precautions: a prospective comparative study. BMJ Open. 2022;12:e044639. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 5. | Diao K, Wang J, Zhang Y, Huang Y, Shan Y. The mediating effect of personal mastery and perceived social support between emotional intelligence and social alienation among patients receiving peritoneal dialysis. Front Public Health. 2024;12:1392224. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 6. | Zhu B, Wu H, Lv S, Xu Y. Association between illness perception and social alienation among maintenance hemodialysis patients: The mediating role of fear of progression. PLoS One. 2024;19:e0301666. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 7. | Andersen BL, Lacchetti C, Ashing K, Berek JS, Berman BS, Bolte S, Dizon DS, Given B, Nekhlyudov L, Pirl W, Stanton AL, Rowland JH. Management of Anxiety and Depression in Adult Survivors of Cancer: ASCO Guideline Update. J Clin Oncol. 2023;41:3426-3453. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 220] [Cited by in RCA: 182] [Article Influence: 60.7] [Reference Citation Analysis (0)] |
| 8. | Troy AS, Willroth EC, Shallcross AJ, Giuliani NR, Gross JJ, Mauss IB. Psychological Resilience: An Affect-Regulation Framework. Annu Rev Psychol. 2023;74:547-576. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 372] [Cited by in RCA: 228] [Article Influence: 76.0] [Reference Citation Analysis (0)] |
| 9. | Tarsitani L, Pinucci I, Tedeschi F, Patanè M, Papola D, Palantza C, Acarturk C, Björkenstam E, Bryant R, Burchert S, Davisse-Paturet C, Díaz-García A, Farrel R, Fuhr DC, Hall BJ, Huizink AC, Lam AIF, Kurt G, Leijen I, Mittendorfer-Rutz E, Morina N, Panter-Brick C, Purba FD, Quero S, Seedat S, Setyowibowo H, van der Waerden J, Pasquini M, Sijbrandij M, Barbui C. Resilience of people with chronic medical conditions during the COVID-19 pandemic: a 1-year longitudinal prospective survey. BMC Psychiatry. 2022;22:633. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 10. | Azizi A, Achak D, Saad E, Hilali A, Youlyouz-Marfak I, Marfak A. Post-COVID-19 mental health and its associated factors at 3-months after discharge: A case-control study. Clin Epidemiol Glob Health. 2022;17:101141. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 13] [Reference Citation Analysis (0)] |
| 11. | Hoang P, King JA, Moore S, Moore K, Reich K, Sidhu H, Tan CV, Whaley C, McMillan J. Interventions Associated With Reduced Loneliness and Social Isolation in Older Adults: A Systematic Review and Meta-analysis. JAMA Netw Open. 2022;5:e2236676. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 59] [Cited by in RCA: 171] [Article Influence: 42.8] [Reference Citation Analysis (0)] |
| 12. | Thompson C, Halcomb E, Masso M. The contribution of primary care practitioners to interventions reducing loneliness and social isolation in older people-An integrative review. Scand J Caring Sci. 2023;37:611-627. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 13] [Reference Citation Analysis (0)] |
| 13. | Hao H, Du M, Yue J. Social isolation, loneliness, and subjective wellbeing among Chinese older adults during the COVID-19 pandemic. Front Public Health. 2024;12:1425575. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 14. | Röhr S, Wittmann F, Engel C, Enzenbach C, Witte AV, Villringer A, Löffler M, Riedel-Heller SG. Social factors and the prevalence of social isolation in a population-based adult cohort. Soc Psychiatry Psychiatr Epidemiol. 2022;57:1959-1968. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 91] [Article Influence: 22.8] [Reference Citation Analysis (0)] |
| 15. | Judd BK, Whelehan DF, Baysari MT, Baillie AJ. The Impact of Personal Protective Equipment on Cognitive and Emotional Aspects of Health Care Work. J Occup Environ Med. 2024;66:174-178. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 16. | Thornicroft G, Sunkel C, Alikhon Aliev A, Baker S, Brohan E, El Chammay R, Davies K, Demissie M, Duncan J, Fekadu W, Gronholm PC, Guerrero Z, Gurung D, Habtamu K, Hanlon C, Heim E, Henderson C, Hijazi Z, Hoffman C, Hosny N, Huang FX, Kline S, Kohrt BA, Lempp H, Li J, London E, Ma N, Mak WWS, Makhmud A, Maulik PK, Milenova M, Morales Cano G, Ouali U, Parry S, Rangaswamy T, Rüsch N, Sabri T, Sartorius N, Schulze M, Stuart H, Taylor Salisbury T, Vera San Juan N, Votruba N, Winkler P. The Lancet Commission on ending stigma and discrimination in mental health. Lancet. 2022;400:1438-1480. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 227] [Cited by in RCA: 374] [Article Influence: 93.5] [Reference Citation Analysis (0)] |
| 17. | An J, Zhu X, Shi Z, An J. A serial mediating effect of perceived family support on psychological well-being. BMC Public Health. 2024;24:940. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 45] [Article Influence: 22.5] [Reference Citation Analysis (0)] |
| 18. | Wenn P, Meshoyrer D, Barber M, Ghaffar A, Razka M, Jose S, Zeltser R, Makaryus AN. Perceived Social Support and its Effects on Treatment Compliance and Quality of Life in Cardiac Patients. J Patient Exp. 2022;9:23743735221074170. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 15] [Reference Citation Analysis (0)] |
| 19. | Tacchini-Jacquier N, Monnay S, Bonvin E, Dubuis J, Verloo H. Relatives' experiences of visiting restrictions during the COVID-19 pandemic's first wave: a PREMs study in Valais Hospital, Switzerland. BMC Health Serv Res. 2023;23:1008. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 20. | Kebapcı A, Türkmen E. The effect of structured virtual patient visits (sVPVs) on COVID-19 patients and relatives' anxiety levels in intensive care unit. J Clin Nurs. 2022;31:2900-2909. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 21. | Hossain MM, Sultana A, Purohit N. Mental health outcomes of quarantine and isolation for infection prevention: a systematic umbrella review of the global evidence. Epidemiol Health. 2020;42:e2020038. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 333] [Cited by in RCA: 311] [Article Influence: 51.8] [Reference Citation Analysis (0)] |
| 22. | Iovino P, Vellone E, Cedrone N, Riegel B. A Middle-Range Theory of Social Isolation in Chronic Illness. Int J Environ Res Public Health. 2023;20:4940. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 47] [Article Influence: 15.7] [Reference Citation Analysis (0)] |
| 23. | Crider K, Williams J, Qi YP, Gutman J, Yeung L, Mai C, Finkelstain J, Mehta S, Pons-Duran C, Menéndez C, Moraleda C, Rogers L, Daniels K, Green P. Folic acid supplementation and malaria susceptibility and severity among people taking antifolate antimalarial drugs in endemic areas. Cochrane Database Syst Rev. 2022;2:CD014217. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 20] [Cited by in RCA: 24] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 24. | Zhao Y, Xu Y, Yao D, Wu Q, Chen H, Hu X, Huang Y, Zhang X. Changes in Infectious Disease-Specific Health Literacy in the Post-COVID-19 Pandemic Period: Two-Round Cross-Sectional Survey Study. JMIR Public Health Surveill. 2024;10:e52666. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 25. | Ingadottir B, Bragadottir B, Zoëga S, Blondal K, Jonsdottir H, Hafsteinsdottir EJG. Sense of security during COVID-19 isolation improved with better health literacy - A cross-sectional study. Patient Educ Couns. 2023;114:107788. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 26. | Galmarini E, Marciano L, Schulz PJ. The effectiveness of visual-based interventions on health literacy in health care: a systematic review and meta-analysis. BMC Health Serv Res. 2024;24:718. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 72] [Article Influence: 36.0] [Reference Citation Analysis (0)] |
| 27. | Han P, Duan X, Jiang J, Zeng L, Zhang P, Zhao S. Experience in the development of nurses' personal resilience: A meta-synthesis. Nurs Open. 2023;10:2780-2792. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 42] [Reference Citation Analysis (0)] |
| 28. | Xiao C, Wu A, Wang Y, Li T, Duan Y, Jiang Y, Shi L, Hong X, Geng W, Li J, Du J, Hu J, Cao J, Wei J. Development and psychometric validation of the hospitalized patients' expectations for treatment scale-patient version. Front Psychiatry. 2023;14:1201707. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 29. | Schäfer SK, von Boros L, Schaubruch LM, Kunzler AM, Lindner S, Koehler F, Werner T, Zappalà F, Helmreich I, Wessa M, Lieb K, Tüscher O. Digital interventions to promote psychological resilience: a systematic review and meta-analysis. NPJ Digit Med. 2024;7:30. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 55] [Cited by in RCA: 31] [Article Influence: 15.5] [Reference Citation Analysis (0)] |
| 30. | Sánchez-Ortega MA, Lluch-Canut MT, Roldán-Merino J, Agüera Z, Hidalgo-Blanco MA, Moreno-Poyato AR, Tinoco-Camarena J, Moreno-Arroyo C, Puig-Llobet M. Nursing Intervention to Improve Positive Mental Health and Self-Care Skills in People with Chronic Physical Health Conditions. Int J Environ Res Public Health. 2022;20:528. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 31. | Vernmark K, Hursti T, Blom V, Asplund RP, Nathanson E, Engelro L, Radvogin E, Andersson G. The Effects of Mindfulness-Focused Internet-Based Cognitive Behavioral Therapy on Elevated Levels of Stress and Symptoms of Exhaustion Disorder: A Randomized Controlled Trial. Clin Psychol Eur. 2024;6:e12899. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 32. | Coelho J, Moreno Poyato A, Roldán Merino J, Sequeira C, Sampaio F. Perspectives of adult patients with mental health disorders on the relationship with nurses: a focus group study. BMC Nurs. 2024;23:9. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 33. | Kim YR, Chung SW, Kim MJ, Choi WM, Choi J, Lee D, Lee HC, Shim JH. Limited Generalizability of Retrospective Single-Center Cohort Study in Comparison to Multicenter Cohort Study on Prognosis of Hepatocellular Carcinoma. J Hepatocell Carcinoma. 2024;11:1235-1249. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 23] [Reference Citation Analysis (0)] |