Published online May 19, 2026. doi: 10.5498/wjp.v16.i5.117958
Revised: February 10, 2026
Accepted: March 11, 2026
Published online: May 19, 2026
Processing time: 96 Days and 0.2 Hours
Postoperative headache, dizziness, and depression are intertwined challenges that impede recovery in patients with hypertensive intracerebral hemorrhage (HICH), while conventional care often lacks a systematic approach. The Competency-Opportunity-Motivation-Behavior (COM-B) model, targeting capability, opp
To evaluate a COM-B-based integrated rehabilitation and psychological care inter
A total of 100 HICH patients admitted between January 2023 and January 2025 were enrolled and randomly divided into an observation group and a control group (50 cases each). The control group received routine care, while the observation group received additional COM-B-based holistic rehabilitation training combined with psychological nursing for 8 weeks. Headache, dizziness, depression, sleep quality, neurological/motor function, and daily living ability were compared before and after treatment.
Showed that compared with the control group, the observation group exhibited significantly lower scores on the Visual Analogue Scale, the Dizziness Assessment Rating Scale, the Dizziness Handicap Inventory, the Self-Rating Depression Scale, the Pittsburgh Sleep Quality Index, and the National Institutes of Health Stroke Scale, signi
The COM-B-based integrated rehabilitation and psychological intervention alleviates headache, dizziness, dep
Core Tip: Current rehabilitation research predominantly focuses on cerebral ischemia, while intervention studies targeting hypertensive intracerebral hemorrhage patients remain relatively limited. This study employed an intervention based on the innovative Competency-Opportunity-Motivation-Behavior model, overcoming the limitations of traditional postoperative care. By systematically enhancing patient capabilities, optimizing external support opportunities, and stimulating intrinsic motivation, this model achieves multidimensional rehabilitation support. This study first demonstrates that integrated rehabilitation combined with psychological care guided by the Competency-Opportunity-Motivation-Behavior model not only effectively alleviates symptoms such as headaches, dizziness, and depression but also concurrently promotes neu
- Citation: Zhang HJ, Zhao YF, Wang ZJ, Pang ZL. COM-B-based holistic rehabilitation and psychological care on postoperative headache dizziness and depression in hypertensive intracerebral hemorrhage patients. World J Psychiatry 2026; 16(5): 117958
- URL: https://www.wjgnet.com/2220-3206/full/v16/i5/117958.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i5.117958
Hypertensive intracerebral hemorrhage (HICH) is caused by the rupture of cerebral blood vessels due to hypertension, resulting in intracranial hemorrhage. It is characterized by rapid onset, critical condition, high mortality and disability rate. Postoperative patients not only experience symptoms such as limb dysfunction, headache, and dizziness, but also often have depressive symptoms such as low mood, insomnia, and changes in appetite[1,2]. Studies have shown that persistent physical symptoms can exacerbate psychological distress, while depressive mood can reduce patients’ wil
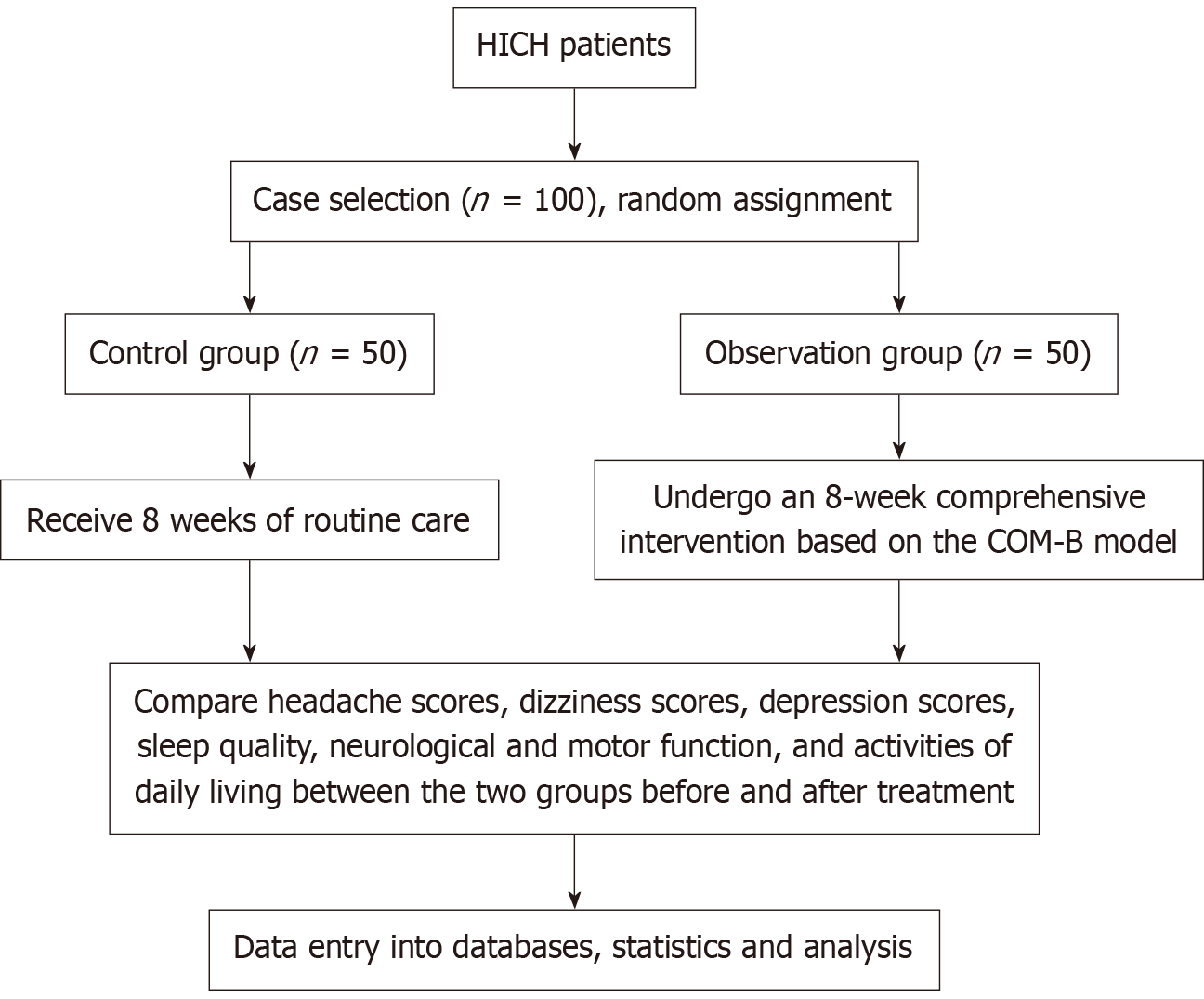
A total of 100 patients with HICH admitted to our hospital between January 2023 and January 2025 were selected as study subjects. Patients were randomly assigned using a computer-generated random number sequence to form an observation group and a control group, each comprising 50 cases. After randomization, all baseline variables (Table 1) were tested for balance between groups, confirming no statistically significant differences (all P > 0.05). This study employed a blinded evaluator design, ensuring that evaluators remained unaware of group assignments throughout the data collection process. The research intervention flowchart is shown in Figure 1.
| Variable | Control group (n = 50) | Observation group (n = 50) | χ2/t | P value |
| Gender | 0.226 | 0.635 | ||
| Male | 29 (58.00) | 27 (54.00) | ||
| Female | 21 (42.00) | 23 (46.00) | ||
| Age (year), mean ± SD | 55.91 ± 6.19 | 56.07 ± 6.23 | 0.152 | 0.880 |
| Marriage | 1.841 | 0.398 | ||
| Unmarried | 3 (6.00) | 2 (4.00) | ||
| Married | 43 (86.00) | 45 (90.00) | ||
| Divorced or widowed | 4 (8.00) | 3 (6.00) | ||
| Education level | 4.703 | 0.095 | ||
| Primary school and below | 10 (18.00) | 12 (24.00) | ||
| Junior high to high school | 29 (58.00) | 31 (62.00) | ||
| College degree or above | 11 (24.00) | 7 (14.00) | ||
| Duration of hypertension (in years), mean ± SD | 6.78 ± 1.37 | 6.85 ± 1.44 | 0.314 | 0.754 |
| Cerebral hemorrhage volume (mL), mean ± SD | 43.55 ± 6.07 | 43.70 ± 6.11 | 0.086 | 0.931 |
Inclusion criteria: (1) Diagnosed with HICH by imaging examination; (2) First-time onset and the time interval between onset and surgery < 12 hours; (3) Stable vital signs and clear consciousness after surgery; and (4) Signed an informed consent form voluntarily.
Exclusion criteria: (1) Complicated with systemic immune diseases or malignant tumors; (2) Complicated with severe liver and kidney dysfunction or hematological diseases; (3) Having mental, hearing, linguistic, or cognitive impairments that prevent them from participating in the study; (4) Complicated with ischemic stroke, traumatic brain injury or other brain lesions; and (5) Suffering from other musculoskeletal diseases that affect limb movement.
Patients in the control group received routine care for 8 weeks, including close monitoring of vital signs, maintenance of limb positioning, and low-flow oxygen support. Nursing staff regularly turned and percussed patients’ backs to ensure airway patency and administered dehydrating, hemostatic, and antihypertensive medications as prescribed. Oral care and dietary guidance were strengthened, and nebulized medication was administered to patients with difficulty expectorating to promote expectoration. Patients were guided to perform appropriate limb rehabilitation exercises throughout the nursing process. Before discharge, patients received discharge instructions, including a reasonable diet, appropriate exercise, adherence to medication, and regular follow-up examinations. After discharge, monthly telephone follow-ups were conducted to assess medication adherence and disease recovery, and targeted answers and guidance were pro
The observation group received holistic rehabilitation training based on the COM-B model combined with psychological nursing care, in addition to the treatment given to the control group. The intervention lasted for 8 weeks. The team comprises a neurosurgery chief physician, a rehabilitation medicine attending physician, a psychological counselor, rehabilitation therapists, and neurosurgery specialty nurses. A research nurse manager oversees overall coordination. The neurosurgery chief physician is responsible for assessing and authorizing patient medical safety; the rehabilitation medicine attending physician collaborates with rehabilitation therapists to develop and supervise physical and functional training programs; The psychological counselor implements motivational interviewing and cognitive behavioral therapy sessions, while also providing foundational supportive skills training to nurses. The neurosurgery specialty nurse serves as the primary liaison, handling daily health education, organizing family meetings, assisting with group activities, and maintaining patient rehabilitation journals. All team members undergo 12 hours of standardized training covering the COM-B model theory, intervention protocols, and role-specific professional competencies. A standardized intervention manual is distributed post-training. Quality control is implemented through: Weekly team meetings to report and discuss typical cases; and random selection of 10% of intervention sessions (e.g., training sessions, counseling) by a researcher independent of the intervention team for audio/video recording and compliance review against a predefined checklist. Competence: Refers to the patient's physical and mental abilities to understand and perform rehabilitation training, including knowledge about headaches and dizziness, physical conditions for vestibular and balance training, and psychological skills for managing emotions. Opportunity: Refers to external environmental factors that motivate patients to engage in rehabilitation and adhere to symptom management, including professional equipment setup, family and social support, and a suitable rehabilitation environment. Motivation: Refers to the patient's intrinsic willingness and belief in actively participating in rehabilitation and overcoming difficulties, as well as their positive expectations for rehabilitation outcomes. Specific details are as follows.
Through illustrated manuals and videos, systematically explain to patients and their families the pathogenesis, expected course of the disease, and importance of overall rehabilitation of headache and dizziness after HICH surgery. Help patients identify the causes of headache and explain the relationship between depressive mood and physical symptoms. Twice a week, 20 minutes each time. Under the guidance of a rehabilitation therapist, conduct personalized vestibular rehabilitation training, including: Brandt-Daroff habituation, eye movement control training, optomotor training, and balance training. Develop a progressive walking endurance training plan, such as gradually transitioning from slow indoor walking to short outdoor walking, to improve activity limitation caused by dizziness, once a week, 30-40 minutes each time. Under the guidance of a specialist nurse, practice relaxation techniques such as abdominal breathing and progressive muscle relaxation, and introduce the concept of simple cognitive behavioral therapy to help patients improve negative thinking, once a week, 15-20 minutes each time.
Assess the ward and home environment, and instruct patients and their families to avoid stimuli such as strong light and noise that may aggravate headaches and dizziness; discuss with patients and their families to establish a regular daily routine to ensure sufficient rest and orderly rehabilitation training. Instruct patients to perform slow changes in body position, such as following the principle of “sitting up for 30 seconds, standing for 30 seconds” before walking; instruct family members to master the correct assistance methods, such as balance training and emotional support skills with accompaniment, and encourage family members to become active rehabilitation partners. Encourage patients to cultivate hobbies and interests, participate in group interest activities, and increase the frequency and time of daily social com
One-on-one interviews are conducted by a psychological counselor. At the beginning of the interview, the counselor introduces himself, states the purpose and significance of the interview, and establishes a trust relationship through brief general conversation. During the interview, the counselor guides the patient to express the conflicting feelings and concerns in the rehabilitation process, strengthens the rehabilitation motivation, and works with the patient to set specific and achievable short-term rehabilitation goals. Establish a rehabilitation group after cerebral hemorrhage and invite patients to join so that they can ask questions and communicate at any time; organize experience sharing sessions regularly and invite patients with significant rehabilitation results to share their experiences. By setting examples, giving praise and encouragement, patients’ confidence in rehabilitation is enhanced and their self-management compliance is improved. Once a week, 60 minutes each time. Follow up with patients by telephone and WeChat to understand the implementation of rehabilitation training and the management effect of symptoms such as headache and dizziness, answer questions in a timely manner and provide targeted guidance. Guide patients to reflect on the weak links in the rehabilitation process, and at the same time fully affirm their efforts in adhering to rehabilitation training and actively managing their health. Once every two weeks, 15 minutes to 20 minutes each time.
Environmental and emotional regulation method: Optimize the ward environment to ensure it is clean, comfortable and quiet, thereby actively regulating the patient's psychological and emotional state.
Regular psychological assessment and guidance: Conduct psychological assessments at 8 pm every day, assist patients in reviewing their rehabilitation experience of the day, address negative emotions and treatment concerns in a targeted manner, and listen to the patient’s rational treatment suggestions.
Social and peer support method: Encourage family members to increase their time with the patient, actively participate in and assist the patient’s various rehabilitation trainings, and guide family members to put themselves in the patient’s shoes. At the same time, actively create opportunities to promote communication among patients and encourage them to actively share their treatment experiences and insights.
Compare general information between the two groups: Gender, age, marital status, education level, duration of hyper
Headache score: Visual analog scale (VAS) score: Total score of 10 points. Instruct patients to score according to the degree of pain; the more severe the pain, the higher the score. Headache duration scoring: An average monthly attack duration exceeding 48 hours scores 6 points; An average monthly attack duration of 12 hours to 48 hours scores 4 points; An average monthly attack duration of 12 hours or less scores 2 points; no attacks scores 0 point. Headache frequency scoring: Monthly headache frequency > 5 times is 6 points; monthly headache frequency 3 times to 4 times is 4 points; monthly headache frequency < 2 times is 2 points; no attacks are 0 points.
Vertigo score: Patients’ level of vertigo is assessed using the vertigo assessment rating scale (DARS) and vertigo disorder rating scale (DHI). The overall DARS score, which assesses the extent of vertigo symptom improvement, is 68 points. The better the recovery of vertigo symptoms, the lower the score. The DHI assesses the degree of functional, emotional, and physical disability and has a total score of 100. The degree of vertigo increases with the score.
Depression score: Before and after treatment, the patient’s depression is assessed using the self-rating depression scale (SDS). The 20 items on the scale cover the person's subjective depressive symptoms. Ten of the items have positive ratings, while ten have bad ratings. A scale of 1 to 4 is used to score each item. The severity of the depression symptoms increases with the score.
Sleep quality: The patients’ sleep quality was evaluated using the Pittsburgh Sleep Quality Index (PSQI). The measure has 19 self-report items over 7 dimensions, totaling 21 points. The lower the quality of sleep, the higher the score.
Neurological function, motor function, and daily living ability: Prior to and during the intervention, the two patient groups’ neurological impairments were evaluated using the National Institutes of Health Stroke Scale (NIHSS). There are fifteen components on the scale, and the total score ranges from 0 point to 42 points. The degree of neurological function impairment increases with the score. Prior to and during the intervention, the patients’ limb motor function was evaluated using the Fugl-Meyer Motion Scale (FMA). Scores range from 0 to 66 for the upper limb portion and from 0 to 34 for the lower limb portion. The better the recovery of limb motor function, the higher the overall score. Patients’ daily functioning abilities were evaluated using the Barthel Index (BI). Ten evaluation items make up the scale, and the overall score ranges from 0 to 100. The patient's functional independence and capacity for self-care in day-to-day living are stronger when the score is higher.
SPSS 21.0 was used for statistical analysis: Normality of measurement data was assessed using the Shapiro-Wilk test. Data meeting normality criteria were expressed as mean ± SD, and intergroup comparisons were performed using the independent samples t-test. Data not meeting normality criteria were compared using the Mann-Whitney U test; Count data were expressed as number of cases n (%), and χ2 tests were used to analyze differences in distribution between groups. P < 0.05 was considered statistically significant.
In this study, 100 HICH patients were split into two groups at random: A control group and an observation group, each consisting of 50 patients. Comparability was demonstrated by the lack of statistically significant differences (P > 0.05) between the two groups’ general characteristics (Table 1).
Following treatment, the observation group’s VAS score, headache duration, and headache frequency were significantly lower than those of the control group (P < 0.05); similarly, both groups’ VAS scores, headache duration, and headache frequency were significantly lower than those of the pre-treatment group (P < 0.05) (Table 2).
| Group | VAS (points) | Headache duration (minutes) | Frequency of headaches (minutes) | |||
| Before treatment | After treatment | Before treatment | After treatment | Before treatment | After treatment | |
| Control group (n = 50) | 6.83 ± 1.08 | 2.37 ± 0.66a | 4.15 ± 1.23 | 2.06 ± 0.44a | 4.84 ± 0.59 | 2.84 ± 0.61a |
| Observation group (n = 50) | 6.91 ± 1.11 | 2.08 ± 0.47a | 4.20 ± 1.16 | 1.88 ± 0.51a | 4.77 ± 0.55 | 2.43 ± 0.49a |
| t | 0.058 | 2.144 | 0.193 | 2.384 | 0.994 | 2.569 |
| P value | 0.953 | 0.034 | 0.848 | 0.018 | 0.322 | 0.012 |
Compared with the control group, the DARS and DHI scores of the observation group were significantly reduced after treatment (P < 0.05); compared with before treatment, the DARS and DHI scores of both groups were significantly reduced after treatment (P < 0.05) (Table 3).
The observation group’s SDS and PSQI scores were significantly lower after treatment (P < 0.05) when compared to the control group; similarly, both groups’ SDS and PSQI scores were significantly lower after treatment (P < 0.05) when compared to before treatment (Table 4).
The observation group’s FMA and BI scores significantly increased and the NIHSS score significantly decreased after treatment (P < 0.05) when compared to the control group; both groups’ FMA and BI scores significantly increased and the NIHSS score significantly decreased after treatment (P < 0.05) when compared to before treatment (Table 5).
| Group | NIHSS (points) | FMA (points) | BI (points) | |||
| Before treatment | After treatment | Before treatment | After treatment | Before treatment | After treatment | |
| Control group (n = 50) | 27.51 ± 3.57 | 17.77 ± 4.28a | 35.48 ± 5.19 | 58.64 ± 6.11a | 47.50 ± 5.48 | 64.94 ± 5.69a |
| Observation group (n = 50) | 27.72 ± 3.64 | 13.47 ± 4.67a | 35.60 ± 5.06 | 63.12 ± 5.79a | 47.39 ± 5.41 | 68.36 ± 6.08a |
| t | 0.678 | 5.802 | 0.002 | 4.193 | 0.182 | 3.481 |
| P value | 0.499 | < 0.001 | 0.998 | < 0.001 | 0.856 | 0.001 |
With the increasing aging of the population and changes in people’s lifestyles, the incidence of HICH is rising year by year, accounting for about one-third of all cerebrovascular diseases, and its mortality rate is the highest[12-14]. In recent years, minimally invasive treatment techniques for HICH have emerged, such as minimally invasive puncture hematoma drainage and small bone window hematoma evacuation. Compared with traditional craniotomy, minimally invasive treatment can significantly reduce surgical trauma and effectively reduce the risk of related complications[15-17]. However, patients often need to go through a long recovery process after surgery. Affected by factors such as limb dysfunction and decline in daily living ability, coupled with the lack of understanding of the disease among most patients, there are generally varying degrees of negative emotions such as tension, anxiety and depression. These pro
This study aims to improve patients’ postoperative symptoms and functional status by introducing holistic rehabilitation training based on the COM-B model combined with psychological nursing, and systematically promoting behavioral changes from three dimensions: Ability, opportunity and motivation. In the postoperative rehabilitation stage, headache and dizziness are mostly caused by direct damage to brain tissue from hematoma, stimulation from surgical operation, intracranial pressure fluctuations and cerebral vascular autoregulation dysfunction[21,22]. If the cerebral hemorrhage lesion involves the frontal lobe-limbic system and other emotional regulation pathways, it can further induce or aggravate emotional disorders[23]. At the same time, the psychological stress of sudden illness, functional impairment and future life also significantly increases the risk of post-stroke depression[24]. The results of this study show that the observation group has significant improvement in headache, dizziness and depression compared with the control group, indicating that this comprehensive intervention model has good clinical effect. On the one hand, holistic rehabilitation training based on the COM-B model enhances patients’ physical function and neuromodulation ability, improves cerebral blood flow and vestibular function, thereby alleviating headaches and dizziness[25,26]. On the other hand, psychological care enhances patients' self-management ability and coping confidence in symptoms through cognitive behavioral intervention and emotional support, thereby enhancing treatment compliance[27,28]. The COM-B model emphasizes the core role of motivation in behavior change. This study enhances patients' initiative and self-efficacy in participating in rehabilitation through individualized psychological counseling, positive incentives and social support. At the same time, relaxation techniques and attention diversion methods integrated into the holistic rehabilitation training also help alleviate anxiety and depression and improve overall psychological adaptability. In addition, the improvement in sleep quality may further alleviate the frequency and intensity of anxiety and depression[29,30]. In terms of neurological function and motor rehabilitation, the NIHSS score of the observation group decreased significantly, while the FMA and BI scores increased significantly. This may be due to the synergistic effect of “ability” and “opportunity” in the COM-B model. Rehabilitation training not only improved the patient’s muscle strength, balance and coordination, but also created social and physical conditions for continuous practice through environmental adaptation and family par
This study still has several limitations. First, no sample size estimation was conducted in the preliminary phase. Although the results indicate significant intergroup differences, interpretation should be approached with caution. Second, the intervention period was relatively short, making it impossible to assess the sustainability of long-term efficacy. To further validate the generalizability of the findings, subsequent studies should conduct multicenter, large-sample investigations with extended follow-up periods.
In conclusion, patients following HICH surgery benefit from holistic rehabilitation training based on the COM-B model in conjunction with psychological nursing intervention. This helps with headaches, depression, and dizziness as well as improving sleep, promoting the recovery of neurological and motor functions, and improving daily living abilities. This model offers a theoretical foundation and useful reference for thorough postoperative rehabilitation, and it is very clinically feasible.
| 1. | Zhang J, Liu X, Zhang Z. The trajectory and influencing factors of disability acceptance in patients with hypertensive intracerebral haemorrhage: a protocol for prospective longitudinal cohort study in Heyuan City, China. BMJ Open. 2024;14:e076314. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 2. | Feng L, Zhu L, Wang B. Psychological and neurological benefits of high-quality nursing for postoperative hypertensive intracranial hemorrhage patients. Front Neurol. 2025;16:1627446. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 3. | Castello JP, Pasi M, Kubiszewski P, Abramson JR, Charidimou A, Kourkoulis C, DiPucchio Z, Schwab K, Anderson CD, Gurol ME, Greenberg SM, Rosand J, Viswanathan A, Biffi A. Cerebral Small Vessel Disease and Depression Among Intracerebral Hemorrhage Survivors. Stroke. 2022;53:523-531. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 38] [Article Influence: 9.5] [Reference Citation Analysis (0)] |
| 4. | Zhang YZ, Zhang CY, Tian YN, Xiang Y, Wei JH. Cerebral arterial blood flow, attention, and executive and cognitive functions in depressed patients after acute hypertensive cerebral hemorrhage. World J Clin Cases. 2024;12:3815-3823. [PubMed] [DOI] [Full Text] |
| 5. | Tan X, Liu T, Li Y. Impact of perioperative care and cognitive training on neurological recovery and life ability in hypertensive intracerebral hemorrhage patients undergoing minimally invasive hematoma evacuation. Am J Transl Res. 2024;16:5038-5048. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 6. | Michie S, van Stralen MM, West R. The behaviour change wheel: a new method for characterising and designing behaviour change interventions. Implement Sci. 2011;6:42. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4491] [Cited by in RCA: 7716] [Article Influence: 514.4] [Reference Citation Analysis (0)] |
| 7. | Whittal A, Störk S, Riegel B, Herber OR. Applying the COM-B behaviour model to overcome barriers to heart failure self-care: A practical application of a conceptual framework for the development of complex interventions (ACHIEVE study). Eur J Cardiovasc Nurs. 2021;20:261-267. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 24] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 8. | Wu J, Zhu X, Wu Q, Xiao F. Interdisciplinary collaborative care model combined with family empowerment in patients with comorbid hypertension and diabetes: A study on blood pressure/glucose control and psychosocial adaptation based on the COM-B model. Clin Exp Hypertens. 2025;47:2570212. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 9. | Kavuran E, Özalp C, Ay E. The impact of a walking program on self-management, anxiety, stress, depression, quality of life, and seizure frequency in patients with epilepsy: A mixed methods approach using the COM-B behaviour change model. Epilepsy Behav. 2025;162:110149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 10. | Asim M, Hameed W, Khan B, Saleem S, Avan BI. Applying the COM-B Model to Understand the Drivers of Mistreatment During Childbirth: A Qualitative Enquiry Among Maternity Care Staff. Glob Health Sci Pract. 2023;11:e2200267. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 11. | Wang WX, Qiu J, Kong LN, Yang J, Chen L, Zhao Y, Wang TT. Effects of an exercise intervention based on the COM-B model among community-dwelling prefrail older adults with diabetes: study protocol for a randomised controlled trial. BMJ Open. 2025;15:e098945. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 12. | Li W, Wu LX, Huang BS, Yang LJ, Huang JQ, Li ZS, Jiao J, Cheng T, Li D, Xiong Y. A pilot study: Gut microbiota, metabolism and inflammation in hypertensive intracerebral haemorrhage. J Appl Microbiol. 2022;133:972-986. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 14] [Reference Citation Analysis (0)] |
| 13. | Mei L, Fengqun M, Xiaozhuo L, Qing W, Mingming F, Zhengyao Z, Dongpo S, Qian H, Tong C. Effect Western Medicines Combined With Nao-Xue-Shu in Patients With Hypertensive Intracerebral Hemorrhage: A Network Meta-Analysis. Front Pharmacol. 2022;13:892904. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 14. | Wu R, Bao J, Zhang J, Wang Z, Zhang X, Yun Q. Clinical effects of neuroendoscopic hematoma evacuation for hypertensive intracerebral hemorrhage. Am J Transl Res. 2022;14:1084-1091. [PubMed] |
| 15. | Xu X, Zhang H, Zhang J, Luo M, Wang Q, Zhao Y, Gan Z, Xu B, Chen X; MISICH study team. Minimally invasive surgeries for spontaneous hypertensive intracerebral hemorrhage (MISICH): a multicenter randomized controlled trial. BMC Med. 2024;22:244. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 47] [Reference Citation Analysis (0)] |
| 16. | Wei JH, Tian YN, Zhang YZ, Wang XJ, Guo H, Mao JH. Short-term effect and long-term prognosis of neuroendoscopic minimally invasive surgery for hypertensive intracerebral hemorrhage. World J Clin Cases. 2021;9:8358-8365. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 17. | Liu J, Cheng J, Zhou H, Deng C, Wang Z. Efficacy of minimally invasive surgery for the treatment of hypertensive intracerebral hemorrhage: A protocol of randomized controlled trial. Medicine (Baltimore). 2021;100:e24213. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 18. | Li CX, Li L, Zhang JF, Zhang QH, Jin XH, Cai GJ. Tripartite intensive intervention for prevention of rebleeding in elderly patients with hypertensive cerebral hemorrhage. World J Clin Cases. 2021;9:10106-10115. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 1] [Cited by in RCA: 8] [Article Influence: 1.6] [Reference Citation Analysis (15)] |
| 19. | Lu ND, Zhou JJ, Huang F. Cox health behavior intervention combined with psychological care for patients with hypertensive cerebral hemorrhage and mental disorders. World J Psychiatry. 2025;15:106904. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 20. | Chen R, Guo Y, Kuang Y, Zhang Q. Effects of home-based exercise interventions on post-stroke depression: A systematic review and network meta-analysis. Int J Nurs Stud. 2024;152:104698. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 28] [Article Influence: 14.0] [Reference Citation Analysis (0)] |
| 21. | Man Chan Y, Wong Y, Khalid N, Wastling S, Flores-Martin A, Frank LA, Koohi N, Arshad Q, Davagnanam I, Kaski D. Prevalence of acute dizziness and vertigo in cortical stroke. Eur J Neurol. 2021;28:3177-3181. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 20] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 22. | Luo JX, Meng ZZ, Gao ZB, Hu X, Wang ZJ, Liu XY, Chen C, Zhang SY, Sun PJ, Lv XN, Shen J, Li Q. Clinical features and outcomes of intracerebral hemorrhage patients with dizziness: a multi-center cohort study. Neurol Sci. 2025;46:5903-5911. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 23. | Zhou L, Wang T, Yu Y, Li M, Sun X, Song W, Wang Y, Zhang C, Fu F. The etiology of poststroke-depression: a hypothesis involving HPA axis. Biomed Pharmacother. 2022;151:113146. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 81] [Article Influence: 20.3] [Reference Citation Analysis (0)] |
| 24. | Guo J, Wang J, Sun W, Liu X. The advances of post-stroke depression: 2021 update. J Neurol. 2022;269:1236-1249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 325] [Cited by in RCA: 260] [Article Influence: 65.0] [Reference Citation Analysis (0)] |
| 25. | Sana V, Ghous M, Kashif M, Albalwi A, Muneer R, Zia M. Effects of vestibular rehabilitation therapy versus virtual reality on balance, dizziness, and gait in patients with subacute stroke: A randomized controlled trial. Medicine (Baltimore). 2023;102:e33203. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 34] [Article Influence: 11.3] [Reference Citation Analysis (0)] |
| 26. | Yeo SS, Park SY, Cho IH. Injury of the vestibulocerebellar tract in a patient with intracerebral hemorrhage: A case report. Neurosci Lett. 2022;783:136723. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 27. | Gu P, Ding Y, Ruchi M, Feng J, Fan H, Fayyaz A, Geng X. Post-stroke dizziness, depression and anxiety. Neurol Res. 2024;46:466-478. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 11] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 28. | Zhang L, Shen T, Zhou Y, Xie X, Wang J, Gao H. Multidisciplinary management based on clinical nursing pathway model for the treatment of hypertensive intracerebral hemorrhage: A randomized controlled trial. Medicine (Baltimore). 2024;103:e37644. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 29. | Niu S, Liu X, Wu Q, Ma J, Wu S, Zeng L, Shi Y. Sleep Quality and Cognitive Function after Stroke: The Mediating Roles of Depression and Anxiety Symptoms. Int J Environ Res Public Health. 2023;20:2410. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 18] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 30. | Xiao M, Huang G, Feng L, Luan X, Wang Q, Ren W, Chen S, He J. Impact of sleep quality on post-stroke anxiety in stroke patients. Brain Behav. 2020;10:e01716. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 37] [Cited by in RCA: 29] [Article Influence: 4.8] [Reference Citation Analysis (0)] |