Published online May 19, 2026. doi: 10.5498/wjp.v16.i5.114680
Revised: December 30, 2025
Accepted: February 2, 2026
Published online: May 19, 2026
Processing time: 148 Days and 0 Hours
Patients with early liver cancer (eLC) commonly experience substantial psychological burden during treatment. High-quality nursing support provision may alle
To check how the clinical nursing pathway (CNP) + psychological nursing imp
Total 230 patients with eLC surgery were allocated to the control (routine nursing) and observation (CNP + psychological nursing) groups. We conducted compa
Postcare, the scores (points) of the GAD-7 [8.00 (5.00-10.00) vs 10.00 (8.00-12.75)], PHQ-9 [8.00 (6.00-11.00) vs 13.00 (11.00-16.00)], NRS [4.00 (3.00-5.00) vs 4.50 (3.00-5.75)], and SF-MPQ-2 (35.70 ± 5.22 vs 39.63 ± 5.96) scales, as well as the proportion of moderate (34.43% vs 61.11%) and severe (0.82% vs 5.56%) CRF patients, were notably lower in the observation group than in controls. Regarding the CD-RISC scores (points), the observation group scored higher in tenacity [34.00 (31.00-38.00) vs 28.00 (26.00-31.00)], strength [22.00 (18.75-25.00) vs 18.00 (16.00-21.00)], and optimism [10.00 (8.00-12.00) vs 7.00 (5.00-9.00)] domains; the number of patients with absent (15.57% vs 4.63%) or mild (49.18% vs 28.70%) CRF was also greater in the observation cohort, along with higher treatment compliance (95.08% vs 75.00%) and nursing satisfaction (95.08% vs 78.70%).
The above results demonstrate the effectiveness of CNP plus psychological nursing in mitigating anxiety, dep
Core Tip: Conventional care is unable to meet the detailed health needs and psychological support requirements of perioperative patients. This study proposed applying clinical nursing pathways and psychological nursing interventions for patients undergoing early liver cancer (eLC) surgery. This nursing model had significant clinical advantages over conventional nursing, as it significantly alleviated patients’ negative emotions, pain, and cancer-related fatigue and exerted a significant improvement effect on patients’ psychological resilience, treatment compliance, and nursing satisfaction. These results pro
- Citation: Zhang T, Liang HX, Cao LD, Hu SS. Clinical nursing pathways and psychological care in early liver cancer surgery patients: Effects on anxiety, depression, and pain. World J Psychiatry 2026; 16(5): 114680
- URL: https://www.wjgnet.com/2220-3206/full/v16/i5/114680.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i5.114680
Liver cancer (LC) is a liver malignancy with a highly heterogeneous pathophysiological process and a 5-year mortality rate of nearly 80%, with most cases belonging to hepatocellular carcinoma (90%)[1]. Relevant reports indicate LC-associated burden of approximately 12.53 million disability-adjusted life years and nearly 500000 related fatalities[2]. Despite overall downward trends in age-standardized LC incidence and mortality rates, regional differences persist. The situation in the Americas and Southeast Asia remains worrying[3]. Currently, early LC (eLC) can be treated through surgical resection and local ablation. Although possessing a certain clinical effect, these modalities show varied curative effects due to the high heterogeneity of patients’ conditions[4]. Due to postoperative pain, fear of unknown disease development, worries about potential postoperative complications, and the present role of being a patient, eLC-affected individuals often develop great psychological stress during treatment and are prone to anxiety, depression, and fatigue[5,6]. Therefore, providing nursing support to surgically treated eLC patients may help change the above situation. Conventional nursing, mainly providing physiological care and technical operation support, is difficult to meet the detailed health needs and psychological support requirements of perioperative patients[7]. The clinical nursing pathway (CNP), being people-oriented, is a personalized and detailed comprehensive care process designed to address the potential medical and physiological needs of perioperative patients, which can maximize the effectiveness of nursing[8]. Gou et al[9] reported that applying CNP to liver cirrhosis and LC patients undergoing interventional treatment effectively improved quality of life and survival outcomes. Another systematic review and meta-analysis indicated CNP capability to effectively alleviate negative emotions while reducing treatment-related side effects in LC patients undergoing interventional therapy[10]. Psychological care is a nursing model that emphasizes patients’ psychological changes and needs, with the primary objective of reducing patients’ negative emotions and accelerating their smooth recovery as much as possible[11]. Psychological care in cancers, including LC, proves effective in negative psychology (depression, anxiety, hopelessness, etc.) alleviation while fostering positive psychology (e.g., self-esteem, self-efficacy, optimism, resilience, happiness, meaning in life)[12]. Moreover, psychological care for lung cancer chemotherapy patients reduces negative psychological symptoms, effectively alleviates pain, enhances treatment confidence, and improves nursing sati
This study, by combining CNP with psychological care, attempts to further optimize the nursing model to minimize anxiety, depression, and pain among individuals undergoing surgery for eLC. Limited relevant research underscores the substantial clinical implications of these results for patient-centered oncology care.
Eligible participants must: (1) Meet eLC diagnostic criteria[14] through pathological and clinical assessment; (2) Be suitable candidates for hepatic procedures; (3) Be neurologically intact with preserved communication abilities and cognitive function; and (4) Have complete medical records. Exclusion criteria included: (1) Terminal cases with a life expectancy of < 3 months; (2) Major organ dysfunction (cardiac, hepatic, renal, or splenic); (3) The presence of additional malignancies or metastatic disease; (4) Gastrointestinal obstruction; (5) Pregnancy or lactation; (6) With a history of immune or psychiatric disorders (including depression or anxiety); and (7) Audio-visual impairments.
We enrolled 230 surgically managed eLC patients at our institution (May 2023-Jan 2025) who met strict eligibility criteria for retrospective analysis. They were divided into groups nonrandomly based on the specific nursing plans they received: A control group with 108 cases receiving routine nursing and an observation group with 122 cases undergoing CNP + psychological care. No statistically significant disparities existed in the general characteristics between groups (P > 0.05), confirming their suitability for clinical comparisons.
In the control group, routine nursing was given. After admission, oral health knowledge education, psychological intervention, postoperative symptomatic care, and daily schedule guidance were carried out.
CNP plus psychological care was implemented in the observation group. Table 1 outlines the details of these measures.
| Item | Intervention details |
| Admission guidance | Medical staff set up health files for patients and briefed them on the ward layout, assigned medical staff, and available amenities. Patients received advice on smoking cessation and alcohol avoidance, as well as guidance regarding nutrition, rest, and breathing exercises. On the day preceding surgery, instructions were provided for an 8-hour preoperative fast and a 2-hour water restriction. Furthermore, discontinuation of oral anticoagulants was confirmed |
| Preoperative preparation guidance | Patients received education on surgery-related information and preparatory exercises such as fist-clenching, ankle pumps, hip raises, deep breathing, and effective coughing. Preoperative personal item preparation and item removal like jewelry and metallic items were also informed |
| Intraoperative care | Patients’ anxiety and fear were eased through communication and tactile reassurance upon their entry into the operating room. Intraoperative procedures include maintaining continuous monitoring of vital signs and taking measures to avoid hypothermia. During the communication process, the medical staff tried their best to empathize with the patients, gained their trust, and established a good nurse-patient relationship. Besides, they adjusted the nursing procedures in a timely manner according to the individual circumstances of the patients, striving to meet their reasonable needs and positively guiding them. They also briefly and clearly explained the relevant knowledge about the disease to the patients, and elaborated on the available treatment options and prognosis. When necessary, they provided suggestive therapy to guide patients to correctly deal with their own diseases and correct their wrong perceptions, thus prompting them accept treatment and care work with a positive and proactive attitude |
| Postoperative care | Patients were instructed to start a low-fat semi-liquid diet on the second day after surgery while also administering oral nutritional powder (2-3 times a day, 50-100 mL each time). Increased intakes of vegetables and fruits were also encouraged. On the fourth day, a low-fat regular diet was provided, and on the fifth day, the amount of food intake was gradually increased. The patients were assisted in early ambulation. During bed rest, exercises related to limb mobilization on the bed, like fist clenching and elbow bending and extending, were instructed, 5-10 sets per time, 3-4 times a day. Regular dressing changes were carried out. Instructions were given to the patients and their families on how to perform skin cleaning and care, emphasizing the need to protect the surgical wounds. The ward was kept clean, well-ventilated, and regularly disinfected, with the lighting at night being soft and comfortable. Warming decorations were allowed to be added to the ward. According to the doctor's advice, the patient was given pain relief measures such as a patient-controlled analgesia pump; the patient was instructed to divert their attention from the pain by combining breathing exercises, watching TV, etc.; the nursing staff comforted the patient while understanding their behavioral reactions when experiencing pain, selected beautiful music to relieve pain, and helped the patient relax as much as possible; massage and hot compress methods were used to alleviate the patient's pain level |
| Discharge guidance | On the 6th day after surgery, the patient was given education on activities, diet, and abnormal conditions after discharge, and the patient and his/her family were asked to elaborate on the relevant precautions |
Presurgical guidance: Each participant was created with a personal health profile and received detailed dietary and daily routine guidance. No anticoagulant drug administration 72 hours preoperatively and fasting for 24 hours preoperation were ensured.
Intraoperative care: Upon entry into the operating room, the patient was provided with anxiety and fear alleviation via verbal counseling plus gentle touch. Dynamic hemodynamic monitoring and insulation measures for hypothermia pre
Postoperative care: A step-by-step diet reintroduction plan was formulated for the patient, encouraging more intake of fruits and vegetables. Additionally, necessary assistance was provided to encourage early ambulation; during bed rest, exercises related to limb mobilization on the bed were instructed. In addition, regular dressing changes were carried out. Instructions were given to the patients and their families on how to perform skin cleaning and care, emphasizing the need to protect surgical wounds. The ward was kept clean, well-ventilated, and regularly disinfected, with the lighting at night being soft and comfortable. Warming decorations were allowed to be added to the ward.
Pain care: According to the doctor’s advice, the patient was given pain relief measures such as a patient-controlled analgesia pump; the patient was instructed to divert their attention from the pain by combining breathing exercises, watching TV, etc.; the nursing staff comforted the patient while understanding their behavioral reactions when experiencing pain, selected beautiful music to relieve the pain, and helped the patient relax as much as possible; massage and hot compress methods were used to alleviate the patient’s pain level.
Psychological care: During communication and interaction, medical staff fully demonstrate their empathetic awareness. Medical staff built a bridge of trust between doctors and patients through nonverbal signals such as friendly facial expressions, focused eye contact, and appropriate gestures. In addition, they specially adjusted the nursing process according to patients’ individual needs, ensuring that their reasonable demands were fully met while providing constructive health guidance. They also briefly and clearly explained the relevant knowledge about the disease to the patients, and elaborated on the available treatment options and prognosis. When necessary, they provided suggestive therapy to guide patients to correctly deal with their own diseases and correct their wrong perceptions, thus prompting them to accept treatment and care work with a positive and proactive attitude.
Emotional distress: The patients underwent anxiety and depression assessments with the Generalized Anxiety Disorder-7 (GAD-7) and the Patient Health Questionnaire-9 (PHQ-9) pre- and postcare, respectively. GAD-7 has 7 items and is scored on a 0-3 scale with a score range of 0-21; PHQ-9 has 9 items and is scored on a 0–3 scale with a score range of 0-27. Both have a critical value of 5 (indicating the presence of negative emotions); worse symptoms are indicated by higher scores[15].
Psychological resilience: Patients were assessed with the 25-item Connor-Davidson Resilience Scale (CD-RISC) for psychological adaptation and recovery ability postcare, covering tenacity (total score: 52 points), strength (32 points), and optimism (16 points) domains. The Likert 5-point scoring method (0 = “Not at all”, 4 = “Almost all the time”) was adopted, with a total score of 100. A higher score suggests stronger resilience. Among them, tenacity reflects an individual’s persistence and control ability in difficult situations, strength reflects the tendency to learn and grow from experiences, and optimism indicates the trait of having positive expectations for the future[13,16].
Pain intensity: Before and after nursing, we adopted the Numeric Rating Scale (NRS) and the Short-Form McGill Pain Questionnaire-2 (SF-MPQ-2) to assess patients’ pain. Among them, the NRS scale is a single-item self-assessment tool. Patients circle the number on a numerical scale ranging from 0 (no pain) to 10 (the most intense imaginable pain), which represents their pain intensity. The SF-MPQ-2 contains 22 descriptive items, covering sensory, affective, evaluative, and total dimensions; scored on a scale of 0-10, it has a total score (range 0-220) correlating positively with the complexity and intensity of the patient’s pain experience[17].
Cancer-related fatigue: The Cancer Fatigue Scale (CFS) was used for the evaluation. According to the total score, cancer-related fatigue (CRF) was judged as none, mild, moderate, or severe. A higher total score signifies heightened CRF[18].
Treatment adherence: Evaluation criteria: Well cooperative: The patient obeys medical staff instructions and diligently follows various medical orders; Fairly cooperative: The patient is occasionally uncooperative and partially fails to follow medical orders, but is cooperative after persuasion; Uncooperative: The patient fails to follow most medical orders and displays obvious negative emotions. Treatment cooperation is the sum of well-cooperative cases and fairly cooperative cases as a percentage of the total cases[19].
Nursing satisfaction: Nursing satisfaction was surveyed using a self-designed, patient-rated satisfaction questionnaire (max score: 100 points). There are three levels based on the score, with 80-100 being very satisfied, 60-79 being satisfied, and 0-59 being dissatisfied. The total patient satisfaction rate is the percentage of cases where the satisfaction level is either "very satisfied" or "satisfied" out of the total number of cases[20].
In this study, both measurement and counting data were imported into SPSS 20.0 for statistical analysis. The normality of the measurement data was evaluated using the Kolmogorov-Smirnov test. If normally distributed, the measurement data were described using the mean ± SD; the t-test was used for between-group comparisons, and the paired t-test was used for within-group comparisons before and after care. Otherwise, the median (M) and interquartile range were used to represent the data, with the non-parametric test and the Wilcoxon signed-rank test employed for between-group and pre- vs post-care nursing comparisons, respectively. The counting data were expressed by the rate n (%), and the comparison between the two groups of counting data was made by the χ2 test. A P value < 0.05 denotes statistical significance.
Table 2 displays the pretreatment characteristics across both patient groups. No significant differences were observed regarding sex, age, American Society of Anesthesiologists classification, tumor pathology, disease stage, or liver function Child-Pugh classification (P > 0.05).
| Indicators | Observation group (n = 122) | Control group (n = 108) | χ2/t | P value |
| Sex | 0.604 | 0.437 | ||
| Male | 73 (59.84) | 70 (64.81) | ||
| Female | 49 (40.16) | 38 (35.19) | ||
| Age (years) | 59.07 ± 7.72 | 59.15 ± 7.17 | 0.081 | 0.935 |
| ASA classification (grade) | 4.679 | 0.096 | ||
| I | 24 (19.67) | 11 (10.19) | ||
| II | 85 (69.67) | 80 (74.07) | ||
| III | 13 (10.66) | 17 (15.74) | ||
| Tumor pathology | 4.582 | 0.101 | ||
| Hepatocellular carcinoma | 98 (80.33) | 90 (83.33) | ||
| Bile duct cell carcinoma | 24 (19.67) | 15 (13.89) | ||
| Mixed cell carcinoma | 0 (0.00) | 3 (2.78) | ||
| Clinical staging | 0.108 | 0.743 | ||
| I | 76 (62.30) | 65 (60.19) | ||
| II | 46 (37.70) | 43 (39.81) | ||
| Child-Pugh classification | 3.224 | 0.073 | ||
| A | 63 (51.64) | 43 (39.81) | ||
| B | 59 (48.36) | 65 (60.19) |
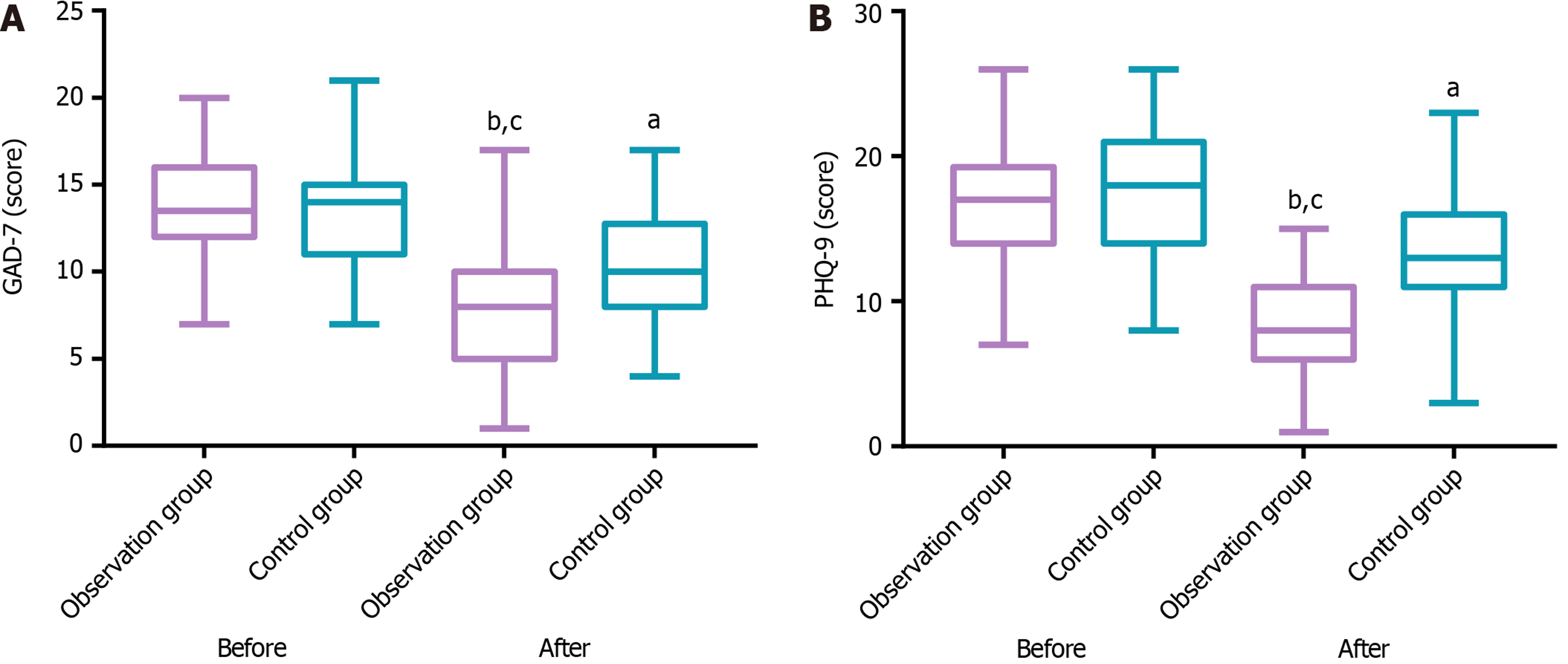
Figure 1 shows the comparative psychological assessments measured by the GAD-7 (anxiety) and PHQ-9 (depression) scales. No baseline inter-group differences existed in psychological status [GAD-7: 13.50 (12.00-16.00) points vs 14.00 (11.00-15.00) points]; PHQ-9: 17.00 (14.00-19.25) points vs 18.00 (14.00-21.00) points; P > 0.05. Postintervention, marked reductions were observed in both groups’ scale scores, with the observation group exhibiting significantly lower values on both GAD-7 and PHQ-9 measures compared to controls [GAD-7: 8.00 (5.00-10.00) points vs 10.00 (8.00-12.75) points]; PHQ-9: 8.00 (6.00-11.00) points vs 13.00 (11.00-16.00) points; P < 0.05.
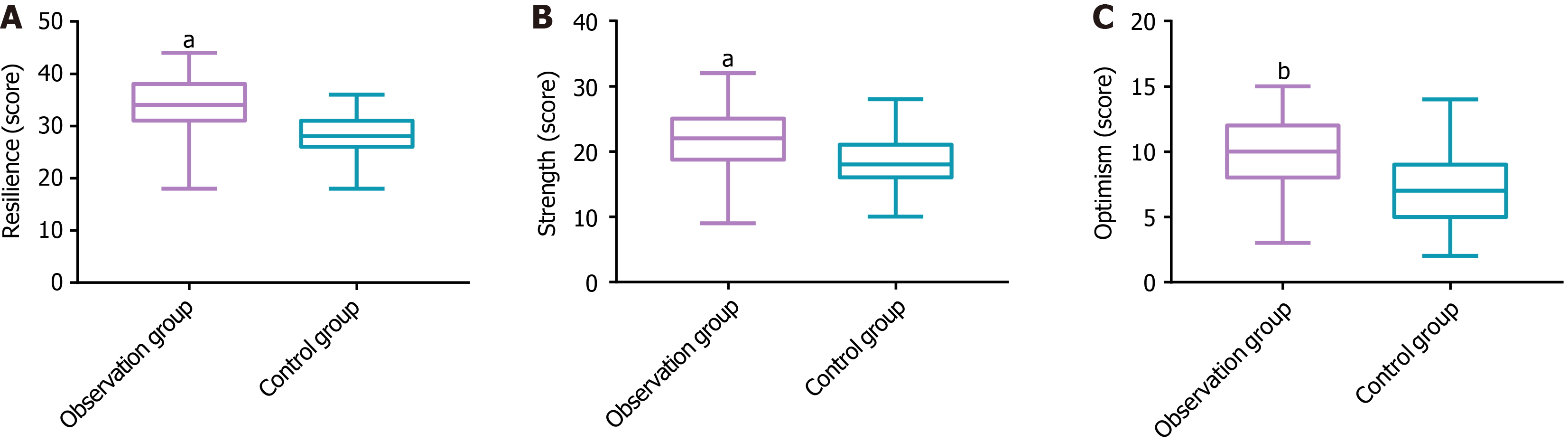
Figure 2 illustrates the comparative CD-RISC measurements evaluating patients’ psychological resilience components. Patients in the observation group outperformed their counterparts in the control group on all measured CD-RISC subscales [tenacity: 34.00 (31.00-38.00) points vs 28.00 (26.00-31.00) points]; strength: 22.00 (18.75-25.00) points vs 18.00 (16.00-21.00) points; optimism: 10.00 (8.00-12.00) points vs 7.00 (5.00-9.00) points.
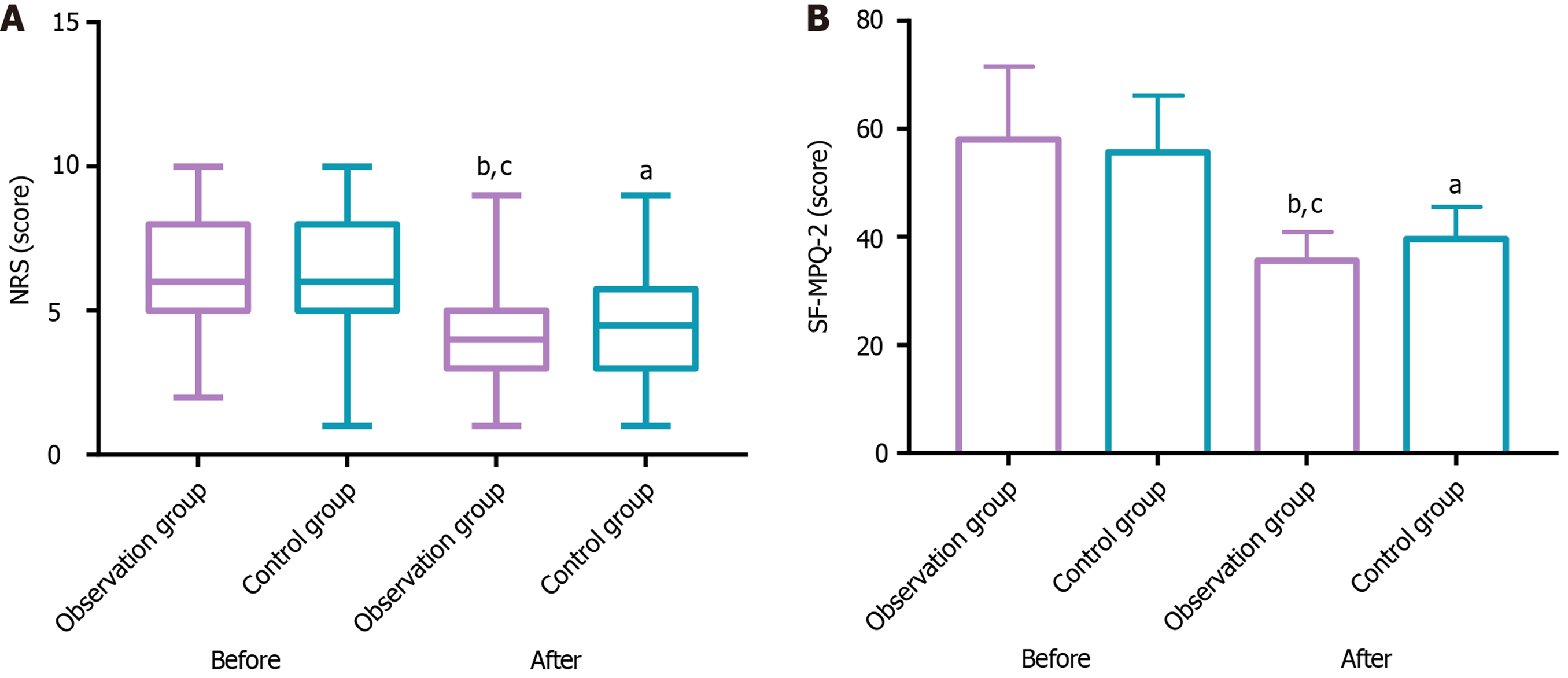
Figure 3 shows pain intensity evaluated using NRS and SF-MPQ-2. Baseline scores did not differ significantly between groups [NRS: 6.00 (5.00-8.00) points vs 6.00 (5.00-8.00) points]; SF-MPQ-2: (58.09 ± 13.42) points vs (55.73 ± 10.45) points; P > 0.05. Postintervention, pain scores decreased markedly in both groups, with the observation group displaying lower values than the control group [NRS: 4.00 (3.00-5.00) points vs 4.50 (3.00-5.75) points]; SF-MPQ-2: (35.70 ± 5.22) points vs (39.63 ± 5.96) points; P < 0.05.
Table 3 presents the CRF assessment using the CFS scale in both patient groups. The observation group exhibited substantially more patients with absent (19 vs 5) and mild (60 vs 31) fatigue than controls, together with fewer moderate (42 vs 66) and intense (1 vs 6) cases (all P < 0.05).
| Indicators | Observation group (n = 122) | Control group (n = 108) | χ2 | P value |
| Absent | 19 (15.57) | 5 (4.63) | 7.342 | 0.007 |
| Mild | 60 (49.18) | 31 (28.70) | 10.046 | 0.002 |
| Moderate | 42 (34.43) | 66 (61.11) | 16.378 | < 0.001 |
| Intense | 1 (0.82) | 6 (5.56) | 4.354 | 0.037 |
Patient compliance with treatment protocols is summarized in Table 4. There were 116 patients in the observation group who cooperated with the treatment, compared to 81 in the control group. The treatment compliance rate was notably higher in the observation group compared to the control cohort (95.08% vs 75.00%; P < 0.001).
| Adherence assessment | Observation group (n = 122) | Control group (n = 108) | χ2 | P value |
| Good | 55 (45.08) | 32 (29.63) | ||
| Fair | 61 (50.00) | 49 (45.37) | ||
| Poor | 6 (4.92) | 27 (25.00) | ||
| Therapeutic adherence | 116 (95.08) | 81 (75.00) | 18.799 | < 0.001 |
Table 5 presents the nursing care satisfaction rates for both patient groups. 116 cases in the observation group and 85 cases in the control group were satisfied with the care, with the satisfaction rate reaching statistical inter-group signi
| Indicators | Observation group (n = 122) | Control group (n = 108) | χ2 | P value |
| Highly satisfied | 62 (50.82) | 40 (37.04) | ||
| Generally satisfied | 54 (44.26) | 45 (41.67) | ||
| Dissatisfied | 6 (4.92) | 23 (21.30) | ||
| Nursing satisfaction | 116 (95.08) | 85 (78.70) | 13.946 | < 0.001 |
In this study of 230 resectable eLC cases, the implementation of CNP supplemented with psychological care was compared with routine care to evaluate the potential clinical benefits. First, we determined significantly better anxiety (GAD-7) and depression (PHQ-9) mitigation outcomes achieved by CNP plus psychological interventions than by traditional nursing measures. This may be attributed to the professional psychological care provided for patients in the combined nursing model. Through empathy and careful listening, patients’ psychological changes can be tracked, allowing for timely psychological intervention and the provision of a series of relaxation measures to minimize their psychological pressure. Consistently, Zhang et al[21] reported effective anxiety and depression alleviation in LC patients receiving intensive nursing.
Xi et al[22] reported that applying CNP combined with psychological nursing in liver transplantation patients effectively relieved anxiety and depression and helped ameliorate insomnia, complementing our findings. According to the CD-RISC scoring results, CNP + psychological nursing led to enhanced resilience in surgically treated eLC patients across domains (tenacity, strength, optimism) compared with conventional nursing. This may be related to the psychological care provided by this study to effectively control patients’ adverse mood, as well as the use of suggestion therapy, all of which assisted patients in establishing correct cognition and a positive attitude. Supporting our findings, Yi et al[23] reported effective resilience enhancement in lung cancer patients undergoing thoracoscopic radical surgery via the CNP + psychological nursing model. Liu et al[24] noted that cognitive behavioral and psychological intervention for nasop
The evaluation of NRS and SF-MPQ-2 showed that CNP + psychological nursing could relieve patients’ pain level more effectively than conventional nursing. The application of CNP plus psychological nursing in LC patients undergoing surgery and interventional therapy has been indicated to effectively reduce postoperative pain and psychological burden. It suggests that the effectiveness of this nursing model in terms of pain relief and alleviation of psychological distress can be extended to patients undergoing interventional treatment for LC[25]. The evaluation of the CFS scale found that the CRF of patients undergoing eLC surgery was effectively ameliorated under the intervention of CNP + psychological nursing. This may be related to the meticulous and high-quality care given to perioperative patients in all aspects under the combined nursing mode in this study, including operation and medication guidance, negative emotion relief, effective pain management, comfortable environment maintenance, etc. Wang et al[26] reported that CNP combined with psychological nursing effectively reduced fatigue severity and improved nursing satisfaction, mirroring our observations. Finally, we also found that the surgically treated eLC patients had higher treatment cooperation and nursing satisfaction under the intervention of CNP + psychological nursing, similar to what was reported by Zhang et al[27], namely, CNP plus psychological nursing contributes to effective treatment compliance and nursing satisfaction enhancement in lung cancer patients after chemoradiotherapy.
This study has several limitations that require further improvement: First, the samples, single-center sourced, may be underrepresented, so the multicenter sample size should be included in the future to improve the accuracy of the research results; second, nursing efficacy-associated determinants were not deeply explored; relevant analysis can be performed to further optimize this nursing model; finally, the economic benefits of the two nursing models are yet to be analyzed to justify the promotion of the combined model. In the future, this study will gradually improve from the above aspects.
CNP + psychological care for surgically treated eLC patients has far better clinical advantages than conventional nursing, which can significantly reduce patients’ anxiety, depression, pain, and CRF, while enhancing their resilience, treatment cooperation, and nursing satisfaction.
| 1. | Donne R, Lujambio A. The liver cancer immune microenvironment: Therapeutic implications for hepatocellular carcinoma. Hepatology. 2023;77:1773-1796. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 524] [Cited by in RCA: 478] [Article Influence: 159.3] [Reference Citation Analysis (5)] |
| 2. | Oh JH, Jun DW. The latest global burden of liver cancer: A past and present threat. Clin Mol Hepatol. 2023;29:355-357. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 103] [Reference Citation Analysis (0)] |
| 3. | Tan EY, Danpanichkul P, Yong JN, Yu Z, Tan DJH, Lim WH, Koh B, Lim RYZ, Tham EKJ, Mitra K, Morishita A, Hsu YC, Yang JD, Takahashi H, Zheng MH, Nakajima A, Ng CH, Wijarnpreecha K, Muthiah MD, Singal AG, Huang DQ. Liver cancer in 2021: Global Burden of Disease study. J Hepatol. 2025;82:851-860. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 135] [Cited by in RCA: 114] [Article Influence: 114.0] [Reference Citation Analysis (0)] |
| 4. | Yoon JH, Choi SK. Management of early-stage hepatocellular carcinoma: challenges and strategies for optimal outcomes. J Liver Cancer. 2023;23:300-315. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 22] [Reference Citation Analysis (0)] |
| 5. | Gao L, Chen W, Qin S, Yang X. The impact of preoperative interview and prospective nursing on perioperative psychological stress and postoperative complications in patients undergoing TACE intervention for hepatocellular carcinoma. Medicine (Baltimore). 2024;103:e35929. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 6. | Wang B, Li B, Tan S, Zhai J, Chen M. Risk factors for anxiety and depression in Chinese patients undergoing surgery for endometrial cancer. Can J Physiol Pharmacol. 2020;98:1-5. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 7. | Ruiz Hernández C, Gómez-Urquiza JL, Pradas-Hernández L, Vargas Roman K, Suleiman-Martos N, Albendín-García L, Cañadas-De la Fuente GA. Effectiveness of nursing interventions for preoperative anxiety in adults: A systematic review with meta-analysis. J Adv Nurs. 2021;77:3274-3285. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 57] [Article Influence: 11.4] [Reference Citation Analysis (0)] |
| 8. | Lin DX, Li X, Ye QW, Lin F, Li LL, Zhang QY. Implementation of a fast-track clinical pathway decreases postoperative length of stay and hospital charges for liver resection. Cell Biochem Biophys. 2011;61:413-419. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 69] [Cited by in RCA: 69] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 9. | Gou Y, Yi J, Jiang M, Cao C. Analysis on Effects of Comprehensive Nursing Care Applied in Interventional Therapy for Patients with Liver Cirrhosis and Liver Cancer. Iran J Public Health. 2019;48:494-500. [PubMed] |
| 10. | Zhang S, Li N, Mao X, Yang D. Effect of comprehensive nursing care for the liver cancer patients undergoing interventional therapy in China: A systematic review and meta-analysis. Int J Nurs Pract. 2024;30:e13243. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 11. | Li DX, Ye W, Yang YL, Zhang L, Qian XJ, Jiang PH. Enhanced recovery nursing and mental health education on postoperative recovery and mental health of laparoscopic liver resection. World J Gastrointest Surg. 2023;15:1728-1738. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 12. | Tian X, Zhou X, Sun M, Yu NX, Peng Y, Zheng X, Xiao W. The effectiveness of positive psychological interventions for patients with cancer: A systematic review and meta-analysis. J Clin Nurs. 2024;33:3752-3774. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 31] [Article Influence: 15.5] [Reference Citation Analysis (0)] |
| 13. | Yu J, Huang T, Xu J, Xiao J, Chen Q, Zhang L. Effect of Nursing Method of Psychological Intervention Combined with Health Education on Lung Cancer Patients Undergoing Chemotherapy. J Healthc Eng. 2022;2022:2438612. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 19] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 14. | Zhou J, Sun H, Wang Z, Cong W, Zeng M, Zhou W, Bie P, Liu L, Wen T, Kuang M, Han G, Yan Z, Wang M, Liu R, Lu L, Ren Z, Zeng Z, Liang P, Liang C, Chen M, Yan F, Wang W, Hou J, Ji Y, Yun J, Bai X, Cai D, Chen W, Chen Y, Cheng W, Cheng S, Dai C, Guo W, Guo Y, Hua B, Huang X, Jia W, Li Q, Li T, Li X, Li Y, Li Y, Liang J, Ling C, Liu T, Liu X, Lu S, Lv G, Mao Y, Meng Z, Peng T, Ren W, Shi H, Shi G, Shi M, Song T, Tao K, Wang J, Wang K, Wang L, Wang W, Wang X, Wang Z, Xiang B, Xing B, Xu J, Yang J, Yang J, Yang Y, Yang Y, Ye S, Yin Z, Zeng Y, Zhang B, Zhang B, Zhang L, Zhang S, Zhang T, Zhang Y, Zhao M, Zhao Y, Zheng H, Zhou L, Zhu J, Zhu K, Liu R, Shi Y, Xiao Y, Zhang L, Yang C, Wu Z, Dai Z, Chen M, Cai J, Wang W, Cai X, Li Q, Shen F, Qin S, Teng G, Dong J, Fan J. Guidelines for the Diagnosis and Treatment of Primary Liver Cancer (2022 Edition). Liver Cancer. 2023;12:405-444. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 388] [Cited by in RCA: 345] [Article Influence: 115.0] [Reference Citation Analysis (7)] |
| 15. | Fortini S, Costanzo E, Rellini E, Amore F, Mariotti SP, Varano M, Parravano M, Virgili G, Bandello F, Rizzo S, Turco S. Use of the Patient Health Questionnaire-9 (PHQ-9) and Generalized Anxiety Disorder-7 (GAD-7) questionnaires for clinical decision-making and psychological referral in ophthalmic care: a multicentre observational study. BMJ Open. 2024;14:e075141. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 16. | Li M, Yu B, He H, Li N, Gao R. Impact of psychological resilience and social support on psycho-social adjustment in postoperative patients with primary hepatocellular carcinoma: mediating effects of fear of progression. Front Psychol. 2024;15:1461199. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 13] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 17. | Zhou Y, Sun W, Fu Y, Wang J, Fan J, Liang Y, Jia W, Han R. Effect of esketamine combined with pregabalin on acute postsurgical pain in patients who underwent resection of spinal neoplasms: a randomized controlled trial. Pain. 2024;165:e96-e105. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 18. | Yang XM, Yang XY, Wang XY, Gu YX. Influence of transcatheter arterial embolization on symptom distress and fatigue in liver cancer patients. World J Gastrointest Oncol. 2024;16:810-818. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 19. | Lao Q, Wu X, Zheng X, Hu J, Huang S, Li D, Du Y, Yang N, Zhu H. Effect of Tacrolimus Time in Therapeutic Range on Postoperative Recurrence in Patients Undergoing Liver Transplantation for Liver Cancer. Ther Drug Monit. 2024;46:42-48. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 20. | Yuan C, Ting C, Guo X. Application effect of "six heart" nursing model intervention in combination with comfort nursing in patients with primary liver cancer undergoing radiotherapy. Biotechnol Genet Eng Rev. 2024;40:1218-1229. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 21. | Zhang Q, Wan R, Liu C. The impact of intense nursing care in improving anxiety, depression, and quality of life in patients with liver cancer: A systematic review and meta-analysis. Medicine (Baltimore). 2020;99:e21677. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 29] [Article Influence: 4.8] [Reference Citation Analysis (2)] |
| 22. | Xi SM, Gu YM, Guo HM, Liu X, Zheng YL, Li GM, Zhang LL. Effect of a Nursing Program on Anxiety, Depression, and Insomnia in Patients After Liver Transplantation: A Randomized Controlled Trial. Ann Transplant. 2025;30:e947351. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 23. | Yi M, Pan Y. Effects of "Timing It Right" nursing on clinical outcome and psychological resilience for lung cancer patients undergoing radical thoracoscopic surgery. Am J Transl Res. 2024;16:179-189. [PubMed] [DOI] [Full Text] |
| 24. | Liu X, Wang C, Li Y, Wang Y. Effects of cognitive behavioral and psychological intervention on social adaptation, psychological resilience and level of hope in patients with nasopharyngeal carcinoma in radiotherapy. Pak J Med Sci. 2024;40:95-100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 25. | Chen P, Zhang L, Sun J, Xing Q, Shi D. Pre- and post-operative comprehensive nursing care versus conventional nursing care: An evaluation of quality of life, postoperative pain, adverse effects, and treatment satisfaction of patients who underwent surgeries and interventional therapies for liver cancer. Medicine (Baltimore). 2023;102:e34643. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (1)] |
| 26. | Wang XB, Sun LF, Niu ME, Cai JZ, Wang HF. The Effect of Nursing Management of Patients Undergoing Interventional Therapy for Liver Cancer Compared with Standard Care on Patient-Reported Outcomes. Clin Nurs Res. 2022;31:1100-1106. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 6] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 27. | Zhang T, Lu J, Fan Y, Wang L. Evidence-based nursing intervention can improve the treatment compliance, quality of life and self-efficacy of patients with lung cancer undergoing radiotherapy and chemotherapy. Am J Transl Res. 2022;14:396-405. [PubMed] |