Published online Mar 19, 2026. doi: 10.5498/wjp.v16.i3.116166
Revised: January 10, 2026
Accepted: February 2, 2026
Published online: March 19, 2026
Processing time: 94 Days and 23.9 Hours
Clinical psychological nursing plays a vital role in clinical practice, and “mental health nurses” face greater stress than general nurses. Assessing the stress responses of “psychological nurses” during the implementation of psychological care and developing corresponding stress reduction strategies will enhance their capacity for stress management.
To explore the effect of pressure adjustment on mental health nurses in graded psychological nursing departments of general hospitals and to enhance their stress-coping ability through the Stress Management and Resiliency Training-clinical (SMART-C) program.
A total of 40 mental health nurses engaged in graded psychological nursing assessment and implementation in a hospital-wide pilot department from January 2019 to June 2020 were enrolled. The SMART-C stress management training was implemented, and stressors and psychosomatic responses were compared before and after the intervention.
Before mental health nursing participated in group training, the psychological stressor assessment results showed that “task” stress was significantly higher than “responsibility” stress, and “interpersonal” stress was close to the domestic norm. After 8 weeks of SMART-C stress management training, the “responsibility” and “task” stress decreased significantly. Before the implementation of the plan, stomachaches, headaches, and sleep issues were the three most severe physical symptoms troubling mental health nurses. The self-rated psychological stress and somatic symptom scores among the mental health nurses decreased significantly following SMART-C training.
SMART-C stress management training can improve stress-adjustment ability and reduce adverse somatic reactions in mental health nurses.
Core Tip: Clinical nurses often face great stress in clinical practice. Managing work stress is crucial for nurses’ physical and mental health. Stress Management and Resiliency Training program conduct corresponding training and adjustments for a series of psychological reaction during acute and chronic stress. This study is aim to access the change of psychological status of mental health nurse after stress intervention programs.
- Citation: Deng J, Xiao YX, Wang L, Bao AZ. Impact of stress management and resilience training-clinical program on stress adjustment in clinical graded psychological nursing nurses. World J Psychiatry 2026; 16(3): 116166
- URL: https://www.wjgnet.com/2220-3206/full/v16/i3/116166.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i3.116166
Stress in the workplace is commonly referred to as “occupational stress”. The fundamental principle underlying this concept is that the work environment imposes certain demands, and the inability to meet these demands may lead to illness or psychological distress[1]. With the continuous advancement of medical technology and increasing workload, healthcare workers face growing pressure[2]. Reports indicate that nurses' stress primarily stems from heavy workloads, poor working conditions, and complex interpersonal relationships[3]. Previous studies have found that the greatest sources of stress for nurses are nursing workload, management issues, and occupational conflicts. In China, nurses are overburdened with work and often unable to complete tasks on time during clinical care[4]. Long term job stress can affect disease, fatigue, injury and mental health. Research also indicates that individual work stress impacts psychological well-being, turnover rates, and physical and mental health. Prolonged stress has led to a declining trend in nurses’ health status[5,6]. Therefore, managing work stress is crucial for nurses’ physical and mental health.
Stress Management and Resiliency Training-clinical (SMART-C) program is based on stress management and resilience training developed by the Benson-Henry Institute for Mind Body Medicine, Massachusetts General Hospital, Harvard Medical School, United States. From psychological and physiological perspectives, SMART-C provides targeted training and adjustment for several psychological and physiological responses associated with acute and chronic stress. The programs aim to enhance stress-coping capacity, improve emotional regulation, and thereby increase psychosomatic resilience, defined as the dynamic psychological and behavioral response of individuals to environmental change. This adaptive state evolves with environmental demands and supports the maintenance of both mental and physical health. SMART-C has been successfully applied among medical staff at Massachusetts General Hospital, McLean Hospital, and other institutions. The program was later localized in China to address stress characteristics specific to Chinese popu
At the same time, mental health nurses bear greater psychological pressure than ordinary nurses. To reduce the emotional and physical burden associated with graded psychological nursing, the stress responses of mental health nurses during psychological nursing implementation were evaluated, and corresponding decompression programs were developed to strengthen their stress management capacity. The present study reports these findings.
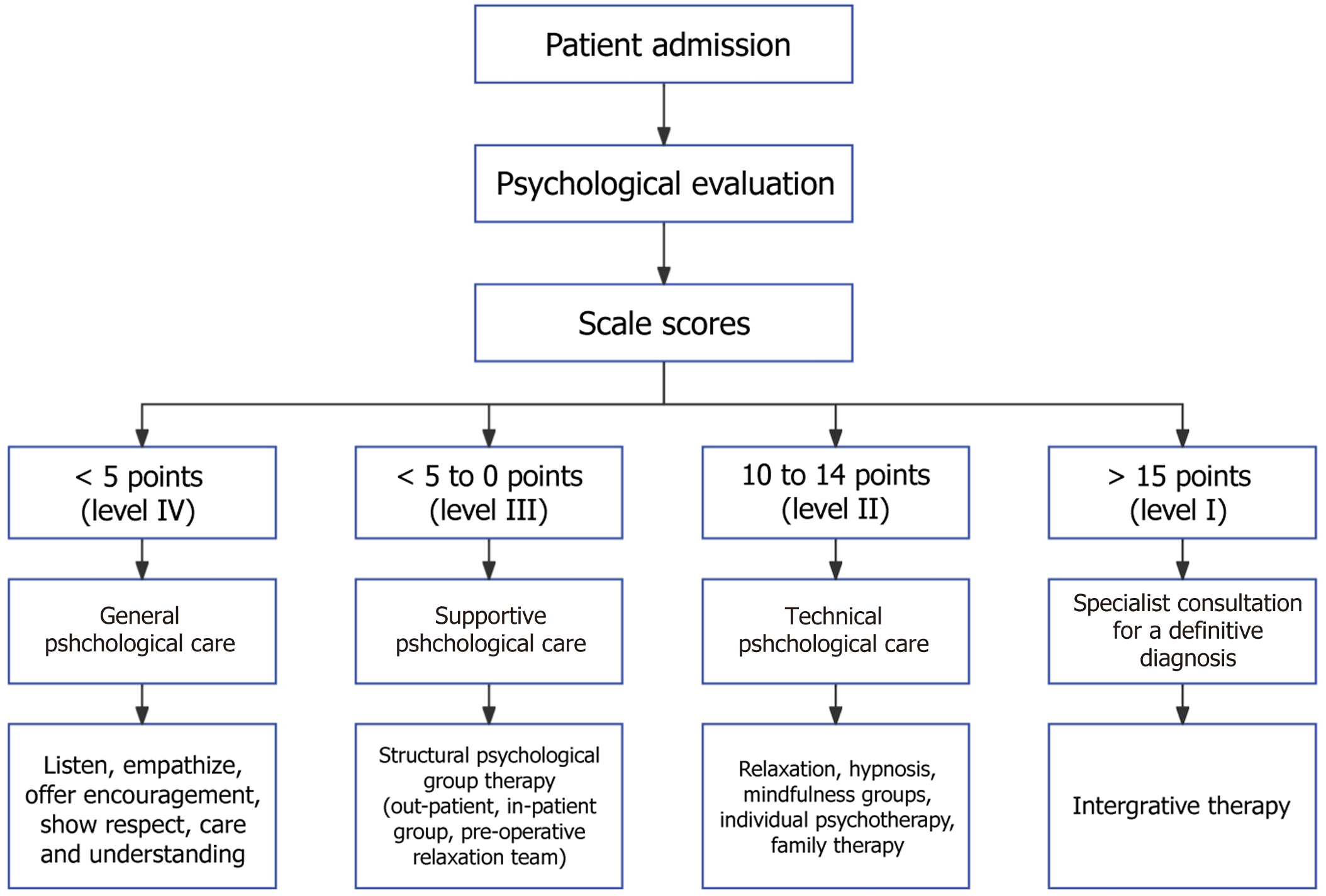
Hierarchical psychological nursing model: Experts with more than 10 years of clinical experience in nursing, psychotherapy, psychiatry, and nursing management in general hospitals were selected based on their professional expertise and extensive experience in psychological nursing practice. Using the Delphi method, a four-level psychological nursing framework was established based on scores from the Generalized Anxiety Disorder-7 and patient Health Questionnaire-9. The specific measures were defined as follows: Level IV: Provision of encouragement, respect, concern, and under
Training of mental health nurses: The Nursing Department of our hospital established the Mental Health Workshop in 2015 in response to patient service needs and staff emotional well-being. A total of 80 nurses with intermediate professional titles or above were selected from 40 clinical departments of the hospital to participate in the workshop training. The training program comprised three stages, namely: (1) External psychological counselor training stage: Completion required certification as a second- or third-level psychological counseling instructor; (2) Internal mental health workshop training stage: Completion required participation in one year of theoretical and practical training, including emotion recognition and awareness, emotion management, sleep management, and baring special group psychotherapy. Asse
40 mental health nurses engaged in the evaluation and implementation of graded psychological nursing in the hospital-pilot department from January 2019 to June 2020 were selected as the research objects. Among them, seven held post
At baseline, the Psychological Emergency Source Scale and the Patient Health Questionnaire-15 (PHQ-15) somatic symptom scale were administered to all 40 mental health nurses. Based on the evaluation results, participants then underwent an eight-week SMART-C psychosomatic stress management training intervention. After completion of the intervention, the two scales were administered again to evaluate intervention effectiveness.
Psychological emergency source scale for medical staff: This study adopted the Psychological Emergency Source Scale for Medical Staff developed by Wang et al[11] which was based primarily on Davis’ Job Stressors Questionnaire. The Crumbach’s α coefficient of the scale was 0.909, and the Spearman-Brown split-half reliability was 0.845. The Crumbach’s α coefficients for the task, responsibility, and interpersonal dimensions were 0.848, 0.847, and 0.786, respectively. Reliability and validity testing demonstrated that the scale can effectively assess psychological stress status and characteristics in medical staff. The scale consists of three dimensions - task, responsibility, and interpersonal relationships - with a total of 25 items. A four-point Likert scoring method is used, with higher scores indicating greater stress intensity.
PHQ-15 somatic symptom scale: The PHQ-15 is a screening tool for somatization disorders developed by Kroenke et al[12] and published in the Journal of the American Medical Association in 1999. The scale contains 15 items, each rated on a three-point scale (0 = no distress, 1 = little distress, 2 = a lot of distress). Total scores are interpreted as follows: 0-4, no somatic problems; 5-9, mild; 10-14, moderate; and ≥ 15, severe somatic symptoms.
SMART-C stress management psychosomatic training implementation: After receiving training from weekly SMART-C sessions. Training was conducted every Wednesday from 19:00 pm to 20:30 pm in accordance with the SMART-C pro
| Time-to-C | Theme | Form | Hour length |
| 1st time | Feeling the pressure | Lecture + experience | 1.5 hours |
| 2nd time | Cognitive boost | Lectures + experiences | 1.5 hours |
| 3rd time | Relaxation training | Lectures + experiences | 1.5 hours |
| 4th time | Supervision and feedback | Practice + sharing | 1.5 hours |
| 5th time | Focus on the moment | Lecture + experience | 1.5 hours |
| 6th time | Awaken the passion | Lectures + experiences | 1.5 hours |
| 7th time | Integrate work and life | Lectures + experiences | 1.5 hours |
| 8th time | Supervision and feedback | Practice + sharing | 1.5 hours |
SPSS version 22.0 was used for data analysis. Quantitative variables described using descriptive statistics, and between-group comparisons were conducted using independent-samples t-tests. Categorical variables were expressed as n (%), and group comparisons were performed using the χ2 test.
Before participation in group training, the psychological stressor assessment showed that “task” stress among mental health nurses was significantly higher than “responsibility” stress, while “interpersonal” stress was close to the domestic norm[13]. After eight weeks of SMART-C stress management training, both “responsibility” and “task” stress scores decreased significantly. The results are presented in Table 2.
| Dimension | Scoring range | Pre-implementation | After implementation | t value | P value |
| Duties | 9-36 | 24.64 ± 3.13 | 10.75 ± 0.48 | 4.623 | 0.001 |
| Accountability | 8-32 | 18.80 ± 3.15 | 11.43 ± 0.52 | 4.166 | 0.001 |
| Interhuman | 8-32 | 15.48 ± 2.95 | 10.21 ± 0.54 | 3.775 | 0.001 |
| Total points | 25-100 | 58.92 ± 9.23 | 32.46 ± 0.51 | 5.412 | 0.001 |
Before the stress intervention, 90% of the mental health nurses reported varying degrees of somatic symptoms, including 57.5% with moderate symptoms and 32.5% with mild symptoms. After eight weeks of SMART-C stress management psychosomatic training, the number of mental health nurses reporting somatic symptoms decreased to 75%. Among them, 52.5% reported mild symptoms, 22.5% reported moderate symptoms, and 25% reported no physical symptoms. The results are shown in Table 3.
| Dimensionality | Before implementation | After implementation | t value | P value | ||||
| Number of people | Self-rated score | Percentage | Number of people | Self-rated score | Percentage | |||
| No body issues | 4 | 2.75 ± 0.48 | 10% | 10 | 1.32 ± 0.61 | 25% | 2.11 | < 0.05 |
| Mild somatic problems | 13 | 7.43 ± 0.52 | 32.50% | 21 | 5.84 ± 0.44 | 52.50% | 2.25 | < 0.05 |
| Moderate body problem | 23 | 13.21 ± 0.54 | 57.50% | 9 | 10.69 ± 0.75 | 22.50% | 2.33 | < 0.05 |
| Severe somatic problems | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
Item-level analysis before and after program implementation indicated that stomach pain, headache, and sleep problems were the three most serious somatic symptoms among mental health nurses. After eight weeks of SMART-C stress mana
| Item | 0: No hassles | 1: Slightly troubled | 2: A lot of trouble | |||
| Pre-implementation | After implementation | Before implementation | After implementation | Before implementation | After implementation | |
| Stomach pain | 13 | 39 | 19 | 1 | 8 | 0 |
| Back pain | 35 | 39 | 2 | 1 | 0 | 0 |
| Pain in the arm, leg, or joint | 31 | 38 | 6 | 0 | 4 | 2 |
| Menstrual pain or other menstrual-related problems (only for women) | 23 | 36 | 10 | 3 | 7 | 1 |
| Headache | 6 | 27 | 26 | 5 | 8 | 2 |
| Chest pain | 38 | 40 | 2 | 0 | 0 | 0 |
| Stun | 36 | 40 | 4 | 0 | 0 | 0 |
| Faint occasionally | 40 | 40 | 0 | 0 | 0 | 0 |
| Feel your heart pounding or beating very fast | 23 | 37 | 9 | 3 | 0 | 0 |
| Breathless | 35 | 38 | 3 | 1 | 2 | 1 |
| Pain or problems during intercourse | 39 | 40 | 1 | 0 | 0 | 0 |
| Constipation, loose stools, or diarrhea | 27 | 37 | 8 | 1 | 5 | 2 |
| Nausea, gas, or indigestion | 24 | 36 | 15 | 4 | 1 | 0 |
| Feeling tired or listless | 20 | 31 | 13 | 5 | 7 | 4 |
| Sleep problems | 11 | 28 | 20 | 10 | 9 | 2 |
Psychological stressor assessment indicated that mental health nurses experienced greater stress related to “responsibility” and “task” demands than “interpersonal” factors. Responsibility-related stress was particularly associated with concerns about accurately identifying patient’s psychosomatic conditions. Previous studies have reported that 30% of outpatients in general hospitals present with organic diseases, 30% with neuroses, and 30% with psychosomatic disorders closely related to psychological factors. A survey conducted in cardiology departments in China reported anxiety and depression prevalence rates of 42.5%[14]. Despite the high prevalence of psychosomatic conditions, recognition rates for anxiety and depression among physicians in general hospitals remain low[15]. A survey of 2345 medical staff from 19 district and county general hospitals in Shanghai reported an average awareness rate of mental health knowledge of 58.33%, while the average awareness rate of depression among 447 nurses from four hospitals in Beijing was 43.02%[16]. Following professional training, mental health nurses often place higher expectations on themselves regarding the identification of psychosomatic disorders. This pressure is particularly pronounced in oncology, chronic disease, and other high-burden departments, where patients’ emotional states are strongly influenced by disease progression and crisis events may occur unexpectedly. Consequently, mental health nurses experience heightened responsibility-related stress due to concerns that failure to recognize emotional changes could lead to adverse outcomes, as well as anxiety about their ability to respond effectively to emergencies. Task-related stress is derived from the implementation of graded psychological nursing. Mental health nurses engage in more frequent communication with patients to establish trust, and patients are often more willing to share discomfort and emotional distress with them. Consequently, activities such as active listening and empathic engagement require substantial time investment. Because routine clinical nursing work
Researchers believe that experiences of work stress have adverse effects on the health of employees, communities, and organizations. Several researchers have documented numerous detrimental physiological, psychological, emotional, and behavioral consequences of work stress[17]. In recent years, a growing body of scientific evidence has shown that specific training methods, such as psychosomatic interventions, can positively affect stress and stress-related diseases from genetic and neuroscience perspectives. Psychosomatic therapy has become an important component of stress mana
As shown in Table 4, stomach pain, headache, and sleep problems were the most prominent physical symptoms affecting mental health nurses. In 2002, the World Congress of Gastroenterology developed a new classification system for gastrointestinal motility disorders, and the concept of the brain–gut axis provides a theoretical framework for understanding the influence of psychological factors on gastrointestinal pathophysiology. Psychological abnormalities are considered not only potential triggers of gastrointestinal diseases but also manifestations of such disorders. Accordingly, psychological treatment, as an adjunctive approach for functional gastrointestinal diseases, has received increasing att
However, this study still have some limitations. This study employed a small sample size. To validate the value of the training program, a large-scale study is required. Additionally, we did not establish a control group to control for in
In summary, the Psychological Emergency Source Scale for Medical Staff was used to identify primary psychological stressors among mental health nurses in our hospital, and SMART-C stress management psychosomatic strengthening training was implemented to improve psychological adaptability and reduce adverse psychosomatic reactions. In the next phase, our hospital will continue to strengthen training in psychosomatic disease identification and nursing practice, apply psychological principles to improve nursing quality and patient satisfaction, and ensure adequate personnel support for the continued development and external promotion of graded psychological nursing. In addition, the “Mental Health Square” will continue to organize mental health activities for nursing staff to support emotional balance, enhance work focus, and establish a sustainable framework for psychological well-being.
| 1. | Bui T, Zackula R, Dugan K, Ablah E. Workplace Stress and Productivity: A Cross-Sectional Study. Kans J Med. 2021;14:42-45. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 39] [Cited by in RCA: 10] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 2. | Dall'Ora C, Ball J, Reinius M, Griffiths P. Burnout in nursing: a theoretical review. Hum Resour Health. 2020;18:41. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 749] [Cited by in RCA: 533] [Article Influence: 88.8] [Reference Citation Analysis (0)] |
| 3. | Goudarzian AH, Nikbakht Nasrabadi A, Sharif-Nia H, Farhadi B, Navab E. Exploring the concept and management strategies of caring stress among clinical nurses: a scoping review. Front Psychiatry. 2024;15:1337938. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 36] [Cited by in RCA: 27] [Article Influence: 13.5] [Reference Citation Analysis (0)] |
| 4. | Yang T, Jin X, Shi H, Liu Y, Guo Y, Gao Y, Deng J. Occupational stress, distributive justice and turnover intention among public hospital nurses in China: A cross-sectional study. Appl Nurs Res. 2021;61:151481. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 32] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 5. | Manchana V. Job demands and job resources for job satisfaction and quality health outcomes among nurses during COVID-19: A cross-sectional study in Indian health settings. J Educ Health Promot. 2022;11:347. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 6. | Wang H, Xu G, Liang C, Li Z. Coping with job stress for hospital nurses during the COVID-19 crisis: The joint roles of micro-breaks and psychological detachment. J Nurs Manag. 2022;30:2116-2125. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 22] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 7. | Zhang WY, Nan N, He Y, Zuo HJ, Song XT, Zhang M, Zhou Y. Prevalence of depression and anxiety symptoms and their associations with cardiovascular risk factors in coronary patients. Psychol Health Med. 2023;28:1275-1287. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 13] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 8. | Haftgoli N, Favrat B, Verdon F, Vaucher P, Bischoff T, Burnand B, Herzig L. Patients presenting with somatic complaints in general practice: depression, anxiety and somatoform disorders are frequent and associated with psychosocial stressors. BMC Fam Pract. 2010;11:67. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 57] [Cited by in RCA: 47] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 9. | Guo S, Xiong J, Liu F, Su Y. Mental Health Literacy Levels of Medical Staff in China: An Assessment Based on a Meta-Analysis. Front Psychiatry. 2021;12:683832. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 8] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 10. | Shao Y, Li WHC, Zhou R, Cheung AT. The Effects of Psychological Interventions on Fostering Resilience in Family Members of Pediatric Cancer Patients: A Systematic Review and Meta-analysis. Cancer Nurs. 2025;48:490-500. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 11. | Wang WJ, Xu HS, Zhu Lin, Deng T, Xuan L. [The development of the Psychological Stressor Scale for Medical Staff]. Zhongguo Jiankang Xinlixue Zazhi. 2014;22:518-520. [DOI] [Full Text] |
| 12. | Kroenke K, Spitzer RL, Williams JB. The PHQ-15: validity of a new measure for evaluating the severity of somatic symptoms. Psychosom Med. 2002;64:258-266. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2750] [Cited by in RCA: 2362] [Article Influence: 98.4] [Reference Citation Analysis (3)] |
| 13. | Lu J, Xu P, Ge J, Zeng H, Liu W, Tang P. Analysis of Factors Affecting Psychological Resilience of Emergency Room Nurses Under Public Health Emergencies. Inquiry. 2023;60:469580231155296. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 14. | Zhang YN, Jin C, Ning L, Gong S, Xiao Y, Yu GL. [Clinical characteristics and related factors of somatization symptoms in outpatients with psychiatric disorders of the department of cardiology in general hospitals]. Zhonghua Xin Xue Guan Bing Za Zhi. 2019;47:907-912. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 15. | Yan ZY, Gu MJ, Zhong BL, Wang C, Tang HL, Ling YQ, Yu XW, Li MQ. Prevalence, risk factors and recognition rates of depressive disorders among inpatients of tertiary general hospitals in Shanghai, China. J Psychosom Res. 2013;75:65-71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 26] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 16. | Yin H, Wardenaar KJ, Xu G, Tian H, Schoevers RA. Mental health stigma and mental health knowledge in Chinese population: a cross-sectional study. BMC Psychiatry. 2020;20:323. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 152] [Cited by in RCA: 106] [Article Influence: 17.7] [Reference Citation Analysis (0)] |
| 17. | Niebuhr F, Borle P, Börner-Zobel F, Voelter-Mahlknecht S. Healthy and Happy Working from Home? Effects of Working from Home on Employee Health and Job Satisfaction. Int J Environ Res Public Health. 2022;19:1122. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 108] [Cited by in RCA: 34] [Article Influence: 8.5] [Reference Citation Analysis (0)] |
| 18. | Zhang X, Tian W, Tang X, Jia L, Meng X, Shi T, Zhao J. Mediating role of resilience on burnout to well-being for hospital nursing staff in Northeast China: a cross-sectional study. BMJ Open. 2024;14:e081718. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 19. | Du S, Zhang L, Chen Y, Zhang Q, Chen B, Chen S. Exploring the Mechanisms of Gastroesophageal Reflux Disease Based on the Brain-Gut Axis Theory. Int J Gen Med. 2025;18:6833-6845. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 20. | Hölzel BK, Carmody J, Vangel M, Congleton C, Yerramsetti SM, Gard T, Lazar SW. Mindfulness practice leads to increases in regional brain gray matter density. Psychiatry Res. 2011;191:36-43. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1333] [Cited by in RCA: 819] [Article Influence: 54.6] [Reference Citation Analysis (4)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/