Published online Mar 9, 2026. doi: 10.5409/wjcp.v15.i1.119008
Revised: January 22, 2026
Accepted: February 26, 2026
Published online: March 9, 2026
Processing time: 49 Days and 16 Hours
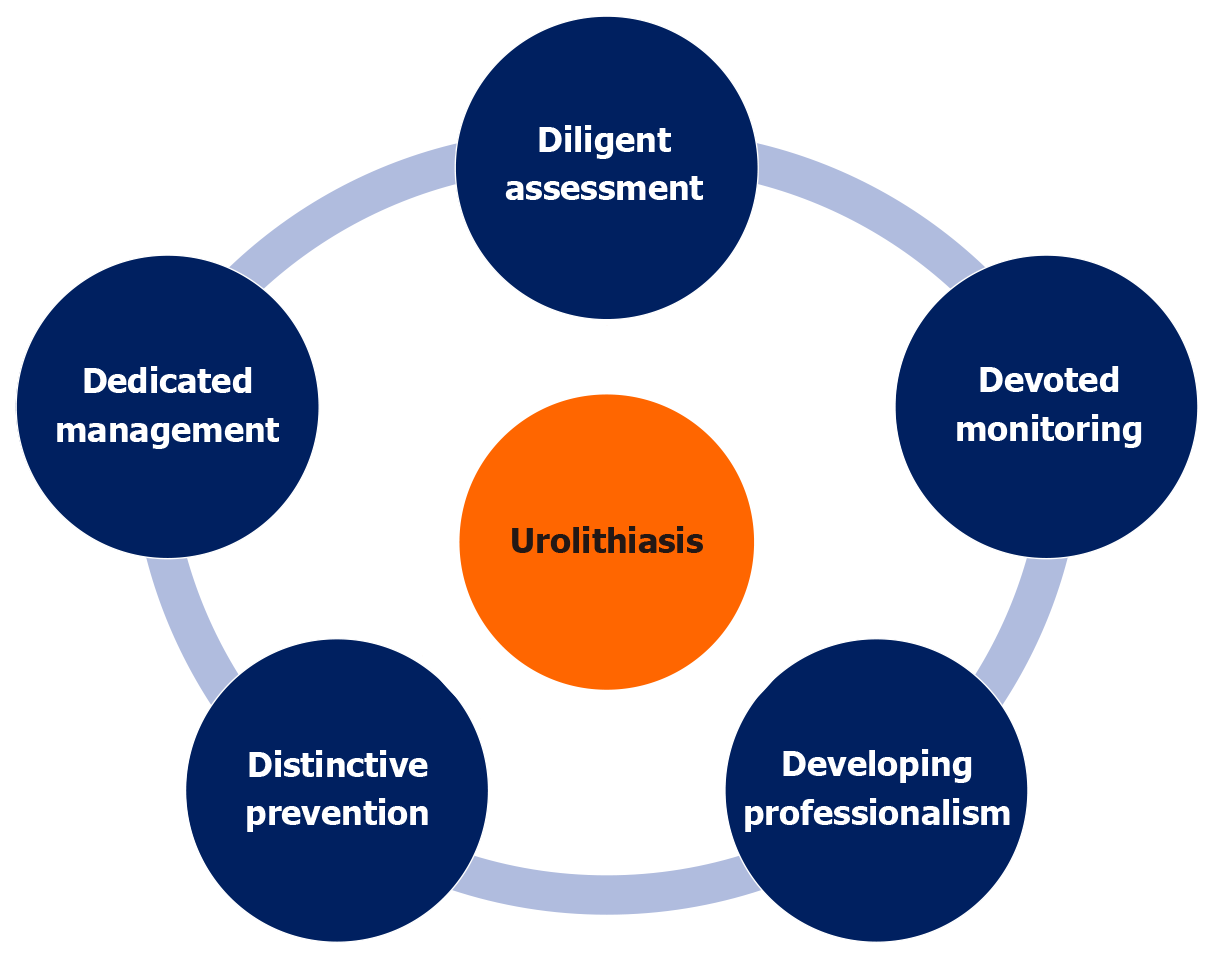
Success and safety of endoscopic ureterolithotripsy (EUL) in pediatric patients has been studied by Khudaybergenov et al in a recent retrospective study. The findings support EUL as a first-line treatment, with careful planning needed for younger children. Urolithiasis is a well-known condition. It can affect any part of the urinary tract. It is quite rare in children (1%-7% of all urinary stones occur during childhood). However, its increasing incidence over last several decades is a cause of concern. Childhood urinary lithiasis is related to genetic, climatic, dietary, and socioeconomic factors. Advancing holistic approach is hope for health for all. Evaluation for aetiopathogenesis to expert management, and energetic prevention requires excellence conceptually. Conceptual frameworks present perspectives about a problem systematically and simplify understanding usefully about how complex things work. We discuss advancements as ‘5Ds’ framework: (1) Diligent assessment: Clinically comprehensive. Investigation should be correct and comprehensive with attention to radiation risks. Results guide rationale methodical management; (2) Dedicated management: Correct intervention guided by best evidence; (3) Devoted monitoring: Immediate and long term; (4) Distinctive prevention: With attention to aetiologies; and (5) Developing professionalism: Expertise development with simulation. Special centres/clinics expertise can guide further refinements. In conclusion, early energetic management ensures cure lifelong.
Core Tip: Urolithiasis is distressing, demanding energetic management. Acute management requires analgesics and antiemetics as needed. Assessment should be for size, location, and aetiology. Stone passage may be spontaneous and medical expulsive therapy can be tried (small ureteral calculi < 4-5 mm). Stone removal becomes necessary for stones that do not pass or are unlikely to pass spontaneously, and if there is evidence of urinary tract infection. Three definitive interventions available are: Shockwave lithotripsy, ureteroscopy, or percutaneous nephrolithotomy. The underlying metabolic disorder should be addressed. Primary prevention should be for all, and includes physiological functioning.
- Citation: Jain S, Jain PK. Paediatric urolithiasis: Medical & surgical management & sophistication. World J Clin Pediatr 2026; 15(1): 119008
- URL: https://www.wjgnet.com/2219-2808/full/v15/i1/119008.htm
- DOI: https://dx.doi.org/10.5409/wjcp.v15.i1.119008
Urolithiasis is a common distressing costly problem! It is a major health care burden to the society today. It is a common cause of visits to the emergency department. Urolithiasis is quite rare in children, with 1%-7% of all urinary stones occurring during childhood[1,2]. Its increasing incidence over last several decades is a cause of concern. It can affect any part of the urinary tract.
Childhood urinary lithiasis is related to genetic, climatic, dietary, and socioeconomic factors. The factors responsible for increasing prevalence are (1) Westernization of lifestyle habits (e.g., dietary changes, increasing body mass index); and (2) Global warming.
Medical management and advancements in technology for advancing tact for stone removal least invasively need to be put in perspective for practice & progress. The international alliance of urolithiasis is working wonderfully[3].
Advancing holistic approach is hope for health for all. Evaluation for aetiopathogenesis to expert management, and energetic prevention requires excellence conceptually. Conceptual frameworks represent ways of thinking about a problem and ways of representing how complex things work[4,5]. We discuss advancements as ‘5Ds’ framework, Figure 1.
Assessment is for current status, complete management plan, including recurrence prevention. Clinical symptoms and signs are important. Children with urolithiasis have hematuria, which may be gross or microscopic. The presentation of calculus causing ureteral or renal pelvic obstruction is severe flank pain (renal colic) or abdominal pain. Calculus in the distal ureter causes irritative symptoms of dysuria, urgency, and frequency. Calculus at the ureterovesical junction causes pain that typically radiates anteriorly to the scrotum or labia. Calculus in the urethra causes dysuria and difficulty in voiding, particularly in males. In very young children non-specific symptoms (e.g., irritability, vomiting) are common.
The common stones in children are: (1) Calcium stones (calcium oxalate/phosphate); (2) Cystine stones; (3) Struvite stones (magnesium ammonium phosphate); (4) Uric acid stones; and (5) Other stones: Indinavir stones; melamine; nephrocalcinosis.
The American Urological Association recommendation for the initial imaging modality in children is ultrasound (US), as it avoids radiation[6]. As US has high specificity (97%) but only moderate sensitivity (67%) in urolithiasis diagnosis, computed tomography (CT) should be considered when clinical suspicion for stones is high, but US is negative.
A non-contrast helical CT scanning is useful. Thin-section helical imaging (spiral CT scan) is advantageously safe and gives multiplanar reformatted images quickly[7]. It detects stones as small as 1 mm. These may be missed by other imaging modalities. A plain radiograph is not recommended as it cannot identify obstruction and rarely visualizes renal calculi < 3 mm. Radiation risks should be taken into consideration because children are more vulnerable because of multiple reasons[8].
Metabolic factors are more common in pediatric urolithiasis as compared to adults[9]. In all children a metabolic evaluation for the most common predisposing risk factors should be undertaken. Chemical analysis of stones is often helpful in defining the underlying cause.
The basic laboratory studies should include: (1) Serum: Calcium, phosphorus, magnesium, uric acid, electrolytes and anion gap, creatinine, alkaline phosphatase; and (2) Urine: Urinalysis, urine culture, spot test for cystinuria, stone analysis, creatinine clearance/creatinine, calcium, phosphate, oxalate, uric acid, citrate, dibasic amino acids (if cystine spot test result is positive). The results guide specifically for correction of metabolic abnormality.
Pain is managed with nonsteroidal anti-inflammatory drugs (NSAIDS). Uncommonly severe pain may necessitate opiates use. It should be noted that the effectiveness of parenterally administered NSAIDS (e.g., ketorolac) is just similar to opioids in relieving symptoms, and these have fewer side effects. Antiemetics should be given as necessary. Adequate fluid intake and the use of salt restriction to daily allowance range should be ensured. Specific medical treatment against the detected metabolic abnormalities is required.
Small ureteral calculi (< 4-5 mm) often pass spontaneously, although the child might experience severe renal colic. Calculus passage can also be aided by placement a ureteral stent past the stone endoscopically[10].
Medical expulsive therapy has been found useful in two pediatric meta-analyses[11,12]. An α-adrenergic blocker, e.g., tamsulosin, facilitates stone passage. Mechanism of action is (1) Decreasing ureteral pressure below the stone; and (2) Decreasing the frequency of the peristaltic contractions of the obstructed ureter.
Stone removal becomes necessary for stones that do not pass or are not likely to pass spontaneously, and if urinary tract infection evidence is present. Surgical success requires distinctive diligence[13]. Three definitive interventions available are: Shockwave lithotripsy (SWL), ureteroscopy, or percutaneous nephrolithotomy (PCNL).
Ureterorenoscopy is the treatment of choice. Lithotripsy is a common non-invasive procedure for bladder, ureteral, and small renal pelvic calculi. Different lithotripsy techniques, including ultrasonic, pneumatic and laser lithotripsy can be used. The holmium laser through a flexible or rigid ureteroscope is quite effective, with enhanced stone fragmentation and dusting capabilities. Khudaybergenov et al’s study[14] shows that laser and pneumatic lithotripsy have similar efficacy, with laser having slightly shorter operative times.
Extracorporeal shock wave lithotripsy (ESWL) is another option. It can be used in children with renal and ureteral stones. Its success rate is > 75%. The predictive factor for ESWL success is the Hounsfield unit (HU) of stone on non-contrast CT. SWL likely to be more successful in stones with HU < 600-1000[15]. Calcium oxalate monohydrate, cystine, and calcium phosphate stones are relatively resistant to ESWL. However, the variable compositions of these stones often render them susceptible to fragmentation by lithotripsy[16].
PCNL is another alternative. In this the renal collecting system is accessed percutaneously, and calculi breaking is carried out using ultrasonic lithotripsy.
Laparoscopic removal is resorted if the above modalities are not successful. The da Vinci robot can be utilized for this procedure[7].
Urological advances in approaches and instruments have almost eliminated the need for open surgical procedures like ureterolithotomy or pyelolithotomy.
Ureterorenoscopy complications possible include ureteral injury or stricture. Studies reporting the use of endoscopy for ureteric stones in children have all clearly demonstrated that there is no significant risk of ureteric strictures[15]. The finding of 92.1% stone free rates (SFR) by Khudaybergenov et al[14] is encouraging.
ESWL complications are subcapsular or perinephric renal hematoma and ureteral obstruction by stone fragments (“Steinstrausse”). ESWL advantage is an outpatient procedure with less procedure time and shorter hospital stay. However, disadvantages are that it has a lower SFR and higher retreatment rate than PCNL[17].
In children with urolithiasis, the underlying metabolic disorder should be addressed. The European Association of Urology advises that metabolic risk should be determined in high-risk individuals with 24-hour urine sample ex
With acute stone event memory fading, return to old habits (e.g., insufficient fluid intake) is likely. Thus, the need for long-term follow-up, including repeat 24-hour urine collections typically annually, is important. All this will make sure that the preventive regimen is followed, and is resulting in the desired reduction in the risk of new stone formation.
Longitudinal monitoring furthermore identifies patients becoming refractory to therapy and aids more timely ad
Primary prevention should be for all, and includes physiological functioning. Proper balanced diet, salt restriction to permitted intakes, adequate hydration are important. Increased consumption of salty, processed foods by children is leading to increased dietary sodium intake significantly! The high sodium intake is harmful by increasing urinary excretion of calcium and may result in hypocitraturia. Thus, increasing stone incidence in children. Thus, it is important to restrict salt intake. Adequate hydration should be ensured, especially in summers. Diet rich in vegetables is advantageous in reducing the recurrence of stoines by increasing the urine pH[19].
Secondary prevention depends upon stone type and the results of metabolic evaluation. Dietary management is guided by the calculus’ chemical analysis, with modifications in the consumption of purities, oxalates or calcium, and pho
In many Asian countries, especially in China, rise in the prevalence and incidence of urolithiasis has been mainly due to high-fat and high-sugar diet becoming more and more popular[20].
Public awareness and advanced professional advice for lifestyle modification efforts can reduce urolithiasis’ impact on populations[21].
Clinical skills are important for early diagnosis. Correct investigations need to be directed by competent doctors. Excellence & competency ensures correct treatment, free from errors and side effects[22]. Continuing education about latest developments is desirable, as medical and surgical sciences are constantly evolving.
Surgery practice rise has been attributable largely due to tactfully refined tools and advanced manual aspects of the craft[23]. New instrumentation and imaging techniques continue to evolve for the good. Surgical skills should be of highest professional standards. Surgeons should perfect their skills, and embrace and master new techniques[24]. Tech
Research refines practices and progresses professionalism. The ‘7Ps’ priorities should be (1) Precision urolithiasis management: Targeted therapies based on metabolic & genetic data; (2) Progression in technology: Thulium fibre laser, robotic ureteroscopy, miniaturization of PCNL sheaths; (3) Pertinent novel biochemical markers (e.g., metabolomics-derived urine signatures for early risk stratification); (4) Prediction models: Refining risks with genetic markers and metabolic evaluation protocols integration; (5) Prevention of long-term metabolic consequences of pediatric stones (e.g., renal tubular dysfunction); (6) Perfection with artificial intelligence, as it provides insights better and besides the traditional statistical approaches; and (7) Progressive prevention with understanding of intricasies of the connection between urolithiasis and dietary and lifestyle decisions in populations.
Urolithiasis presentation pain is worst of all pains. Acute management has to be compassionate. Cure for life with scientific management, suitable follow-up, and stimulating always healthy lifestyle for all is best workings for success. Acute symptomatology distressing, management scientific relieving, research for precise medical and surgical care designing, intricacies for curing for lifelong healthy living.
The authors are thankful to the creators of all references cited as well as the formulators of all guidelines and policies.
| 1. | Carlo HND, Crigger CB. Urinary Lithiasis. In: Kliegman RM, St. Geme III JW, Blum NJ, Tasker RC, Wilson KM, Schuh AM, Mack CL. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia: Elsevier, 2024: 3311-3316. |
| 2. | Strohmaier WL. [Current aspects in pediatric urolithiasis treatment]. Urologe A. 2020;59:289-293. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 3. | Zeng G, Zhu W, Somani B, Choong S, Straub M, Maroccolo MV, Kamal W, Ibrahim TAA, Cho A, Mazzon G, Chai CA, Ferretti S, Zhong W, Onal B, Mohamed O, Saulat S, Jurkiewicz B, Sezer A, Liu Y, Zeng T, Wang W, Gauhar V, Elderwy AA, Zaidi Z, Duvdevani M, Hamri SB, Kumar N, Kartalas-Goumas L, Gadzhiev N, Kraft K, Sepulveda F, Halinski A, Marietti S, Al-Anazi NAS, Santos LS, Vaddi CM, Jia J, Li J, Kuang X, Ye Z, Sarica K. International Alliance of Urolithiasis (IAU) guidelines on the management of pediatric urolithiasis. Urolithiasis. 2024;52:124. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 4. | Rougas S, Berry A, Bierer SB, Blanchard RD, Cianciolo AT, Colbert-Getz JM, Han H, Lipner K, Teal CR. Applying Conceptual and Theoretical Frameworks to Health Professions Education Research: An Introductory Workshop. MedEdPORTAL. 2022;18:11286. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 5. | Bordage G. Conceptual frameworks to illuminate and magnify. Med Educ. 2009;43:312-319. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 260] [Cited by in RCA: 276] [Article Influence: 16.2] [Reference Citation Analysis (0)] |
| 6. | Pearle MS, Matlaga BR, Antonelli JA, Chi T, Hsi RS, Kim SK, Kirkby E, Knudsen B, Koo K, Maalouf NM, Pais VM Jr, Paris A, Penniston KL, Scotland KB, Souter LH, Streeper N, Tasian G, Wood KD, Ziemba JB. Surgical Management of Kidney and Ureteral Stones: AUA Guideline (2026) Part I: Evaluation and Treatment of Patients With Kidney and/or Ureteral Stones. J Urol. 2026;215:113-123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 6.0] [Reference Citation Analysis (1)] |
| 7. | Jain S. 'Children Kidney Care Centers': Rationale, requirements and recommendations for best facilities and better future. World J Nephrol. 2023;12:10-20. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 2] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 8. | Jain S. Radiation in medical practice & health effects of radiation: Rationale, risks, and rewards. J Family Med Prim Care. 2021;10:1520-1524. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 52] [Cited by in RCA: 26] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 9. | Sharma AP, Filler G. Epidemiology of pediatric urolithiasis. Indian J Urol. 2010;26:516-522. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 39] [Cited by in RCA: 47] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 10. | Bernasconi V, Tozzi M, Pietropaolo A, De Coninck V, Somani BK, Tailly T, Bres-Niewada E, Mykoniatis I, Gregori A, Talso M. Comprehensive overview of ureteral stents based on clinical aspects, material and design. Cent European J Urol. 2023;76:49-56. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 12] [Reference Citation Analysis (0)] |
| 11. | Velázquez N, Zapata D, Wang HH, Wiener JS, Lipkin ME, Routh JC. Medical expulsive therapy for pediatric urolithiasis: Systematic review and meta-analysis. J Pediatr Urol. 2015;11:321-327. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 38] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 12. | George A, Montag S, Cubillos J, Gitlin J, Palmer LS. The effect of tamsulosin on ureterolithiasis in the pediatric population. J Urol. 2011;185:e552-e553. [RCA] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 13. | Jain CS, Chandra LCN, Thapar CRK. Pediatric surgery experiences of a tertiary referral hospital: International Classification of Diseases spectrum for teaching, planning, and scaling up services. Indian J Child Health. 2019;6:313-319. [DOI] [Full Text] |
| 14. | Khudaybergenov U, Shomarufov A, Abdukarimov O, Nadjimitdinov Y. Efficacy and safety of semirigid ureterolithotripsy in pediatric urolithiasis: Retrospective analysis from a tertiary center. World J Clin Pediatr. 2026;15:115147. [RCA] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 15. | Radmayr C, Bogaert G, Burgu B, Dogan HS, Nijman JM, Quaedackers J, Rawashdeh YFH, Silay MS, Stein R, Tekgül S. EAU Guidelines. Edn. presented at the EAU Annual Congress Amsterdam 2022. Available from: http://uroweb.org/guidelines/compilations-of-all-guidelines/. |
| 16. | Manzoor H, Leslie SW, Saikali SW. Extracorporeal Shockwave Lithotripsy. 2024 Oct 18. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. [PubMed] |
| 17. | He Q, Xiao K, Chen Y, Liao B, Li H, Wang K. Which is the best treatment of pediatric upper urinary tract stones among extracorporeal shockwave lithotripsy, percutaneous nephrolithotomy and retrograde intrarenal surgery: a systematic review. BMC Urol. 2019;19:98. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 28] [Cited by in RCA: 41] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 18. | Türk C, Petřík A, Sarica K, Seitz C, Skolarikos A, Straub M, Knoll T. EAU Guidelines on Diagnosis and Conservative Management of Urolithiasis. Eur Urol. 2016;69:468-474. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 417] [Cited by in RCA: 574] [Article Influence: 52.2] [Reference Citation Analysis (0)] |
| 19. | Kamal W, Azhar RA, Hamri SB, Alathal AH, Alamri A, Alzahrani T, Abeery H, Noureldin YA, Alomar M, Al Own A, Alnazari MM, Alharthi M, Awad MA, Halawani A, Althubiany HH, Alruwaily A, Violette P. The Saudi urological association guidelines on urolithiasis. Urol Ann. 2024;16:1-27. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 20. | Liu Y, Chen Y, Liao B, Luo D, Wang K, Li H, Zeng G. Epidemiology of urolithiasis in Asia. Asian J Urol. 2018;5:205-214. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 132] [Cited by in RCA: 229] [Article Influence: 28.6] [Reference Citation Analysis (0)] |
| 21. | Alhubaishy BA, Bokhary OA, Alhuzali MA, Bokhary HA. Prevalence of urolithiasis in Saudi Arabia: A systematic literature review. Urol Ann. 2024;16:261-265. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 22. | Jain S, Kamal Jain B, Kamal Jain P, Singh Kushwaha A. Prevention Strategies for Patient Safety in Hospitals: Methodical Paradigm, Managerial Perspective, and Artificial Intelligence Advancements. In: Salen PN, Stawicki SP, editors. Contemporary Topics in Patient Safety - Volume 2. London: IntechOpen, 2023. [DOI] [Full Text] |
| 23. | Rutkow I. The Rise of Modern Surgery: An Overview. In: Townsend CM, Beauchamp RD Jr, Evers BM, Mattox KL, editors. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. 21st ed. Missouri: Elsevier, 2022; 2-19. |
| 24. | Jain S, Puranik A. General Surgery: Requirements, Rationale, and Robust Results. Surg J (NY). 2022;8:e342-e346. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 25. | Jain S, Jain BK, Jain PK, Marwaha V. "Technology Proficiency" in Medical Education: Worthiness for Worldwide Wonderful Competency and Sophistication. Adv Med Educ Pract. 2022;13:1497-1514. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 26. | Hameed BMZ, Somani S, Keller EX, Balamanigandan R, Mahapatra S, Pietropaolo A, Tonyali Ş, Juliebø-Jones P, Naik N, Mishra D, Kumar S, Chlosta P, Somani BK. Application of Virtual Reality, Augmented Reality, and Mixed Reality in Endourology and Urolithiasis: An Update by YAU Endourology and Urolithiasis Working Group. Front Surg. 2022;9:866946. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 23] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/