Published online Mar 9, 2026. doi: 10.5409/wjcp.v15.i1.116331
Revised: November 25, 2025
Accepted: January 5, 2026
Published online: March 9, 2026
Processing time: 118 Days and 8.3 Hours
Obesity and overweight are major public health challenges and are associated with autonomic imbalance and decreased heart rate variability (HRV), a non-invasive indicator of cardiovascular risk. Omega-3 polyunsaturated fatty acids have shown cardioprotective effects and may modulate autonomic function. Nevertheless, the effect of omega-3 supplementation on HRV in individuals who are overweight or obese remains unclear.
To study the effect of omega-3 supplementation on HRV in overweight and obese individuals and to explore the heterogeneity across different study designs.
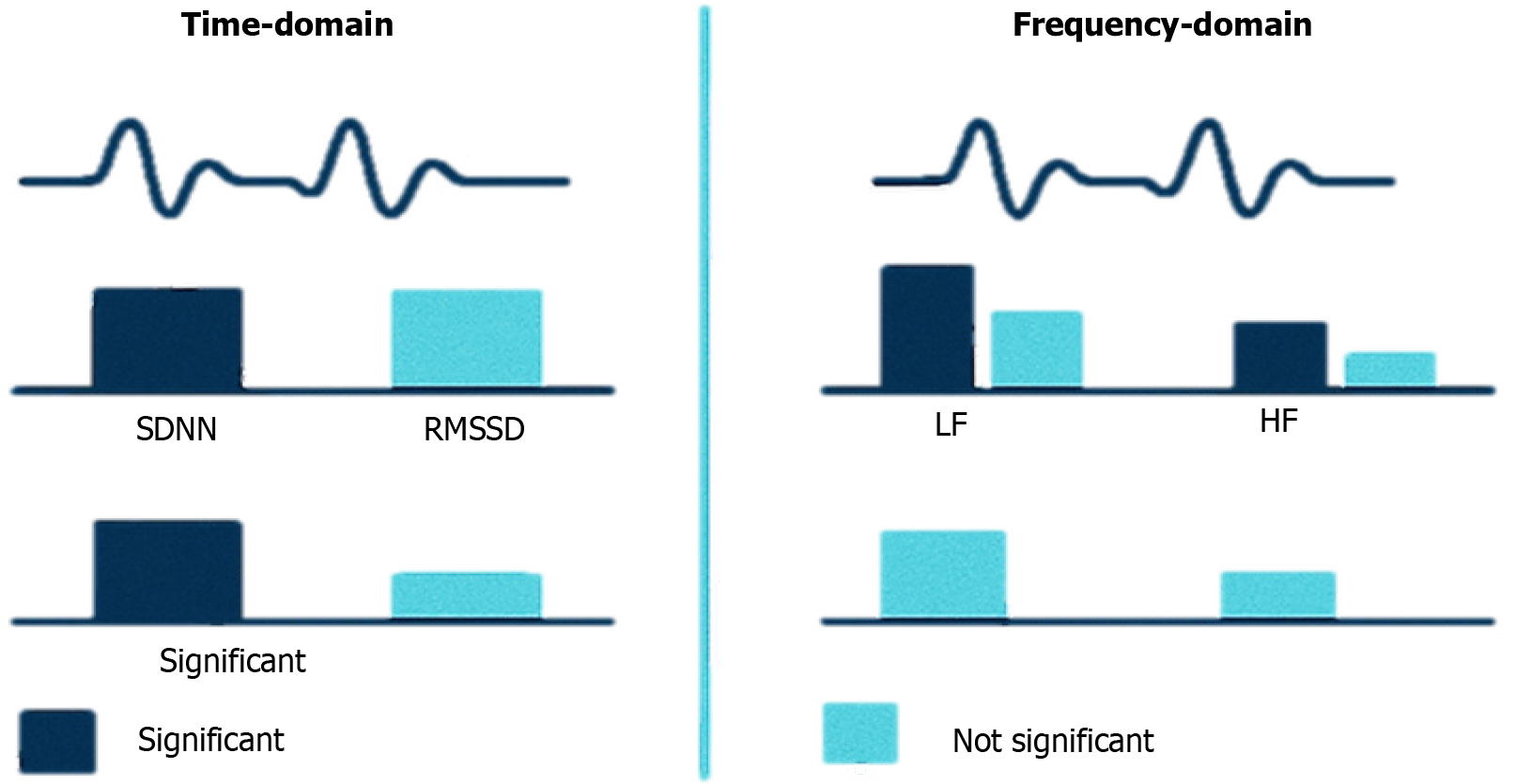
In accordance with PRISMA guidelines, a systematic review and meta-analysis were conducted. PubMed, Science Citation Index, and Scopus were searched for randomized controlled trials (RCTs) assessing the impact of oral omega-3 supplementation on HRV in overweight or obese participants. Primary outcomes were the impacts of omega-3 supplementation on time-domain HRV indices [root mean square of successive differences (RMSSD), standard deviation of normal-to-normal intervals (SDNN), and percentage of successive normal-to-normal intervals differing by more than 50 milliseconds (pNN50%)], and frequency-domain indices [high-frequency (HF) power, low-frequency (LF) power, and LF/HF ratio].
Four RCTs (n = 134 participants) met the inclusion criteria. Two trials compared pre- vs post- omega-3 supplementation, and two compared omega-3 with placebo on HRV in overweight and obese children and adults. In the within-subject analyses, omega-3 supplementation was associated with a significant increase in RMSSD [mean difference (MD) = -11.69 milliseconds, 95%CI: -18.50 to -4.87, P = 0.0008), SDNN (MD = -26.13 milliseconds, 95%CI: -35.84 to -16.42, P < 0.00001), and pNN50% (MD = -9.45, 95%CI: -14.27 to -4.64, P = 0.0001). Between-group comparisons showed that omega-3 supplementation had no significant effect on HF power, LF power, or the LF/HF ratio.
Omega-3 supplementation represents a promising and low-cost strategy for enhancing autonomic balance and potentially reducing cardiovascular risk in overweight and obese populations, as it improves time-domain HRV measures.
Core Tip: Overweight and obesity have become serious global health concerns that frighteningly impact both adults and children. Obesity is intimately linked to decreased heart rate variability (HRV), which is considered a non-invasive indicator of cardiovascular risk. Omega-3 fatty acids supplementation acts as a promising adjuvant cardio-protective therapy that may improve time-domain HRV in the overweight and obese individuals.
- Citation: Atef Abdelsattar Ibrahim H, Gouda Kamal K, Zid MKAMA, Ashraf Hamad A, Kuraishi A, Taha M. Effects of omega-3 fatty acid supplementation on heart rate variability. World J Clin Pediatr 2026; 15(1): 116331
- URL: https://www.wjgnet.com/2219-2808/full/v15/i1/116331.htm
- DOI: https://dx.doi.org/10.5409/wjcp.v15.i1.116331
Obesity has become a serious global health concern, affecting both adults and children at alarming rates[1]. Beyond its association with metabolic diseases such as type 2 diabetes and dyslipidemia, obesity profoundly impacts the autonomic nervous system (ANS) function, often manifesting as altered cardiac autonomic regulation. One of the most widely accepted non-invasive markers of ANS balance is heart rate variability (HRV), which reflects the interaction between parasympathetic and sympathetic activity[2]. HRV is a readily available, non-invasive, and reliable independent indicator of ANS function. Since reduced HRV has been linked to ANS dysregulation, impaired stress reactivity, increased cardiometabolic risk, and premature death, regular HRV monitoring is becoming more common in adults as a means of assessing ANS activity[3]. Reduced HRV is strongly associated with increased cardiovascular morbidity and mortality, making it a valuable prognostic indicator in populations at cardiometabolic risk, including individuals with obesity[4].
Nutritional interventions have been increasingly studied as strategies to improve autonomic function and reduce cardiovascular risk. Among these, Omega-3 polyunsaturated fatty acids (PUFAs) have attracted particular interest due to their cardioprotective properties, including decreasing triglyceride levels, minimizing inflammation, and enhancing endothelial function[5]. Importantly, omega-3 PUFAs are hypothesized to beneficially modulate autonomic tone, potentially improving HRV and reducing the risk of arrhythmias[6]. Observational studies suggest that habitual fish consumption is associated with a reduced resting heart rate and improved HRV[7]; however, intervention trials in humans have produced inconsistent results, particularly in overweight or obese populations.
To date, no systematic review has specifically synthesized the evidence on omega-3 supplementation and HRV outcomes in overweight and obese populations. Given the rising prevalence of obesity across all age groups and the prognostic importance of HRV in cardiovascular health, a critical appraisal of the literature is warranted. Accordingly, this systematic review aims to evaluate the effects of omega-3 supplementation on HRV and resting heart rate in overweight and obese individuals, as well as to explore heterogeneity across study designs and dosing regimens (Figure 1).
This review adhered to Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) 2009 guidelines and was prospectively registered in PROSPERO (CRD420251149899). The protocol was finalized prior to data extraction and analysis.
We used the population, intervention, comparator, outcomes (PICO) framework to define eligibility:
Population: Studies involving overweight or obese individuals (adults or children)[8-11]
Intervention: Oral omega-3 supplementation.
Control: Obese patients who did not receive omega-3 supplementation were studied to evaluate differences in the frequency-domain measures of HRV[8,9]. Regarding time-domain measures of HRV, only one study used obese participants as controls[11], which was insufficient for the meta-analysis. Therefore, baseline data were used as controls[10,11]. Contact with the corresponding author was made whenever essential data for this review was not reported.
Outcomes: Primary outcomes were time-domain HRV measures; root mean square of successive differences (RMSSD), standard deviation of normal-to-normal intervals (SDNN), and the percentage of successive normal-to-normal intervals differing by more than 50 milliseconds (pNN50%). Secondary outcomes included resting heart rate and frequency-domain measures: High-frequency (HF) power, low-frequency (LF) power, and low-to-high-frequency (LF/HF) ratio.
Study design: Randomized controlled trials (RCTs) (parallel or crossover) and pre-post intervention studies published in peer-reviewed journals.
Three major databases, PubMed, Scopus, and Clarivate Web of Science, were systematically searched to identify all relevant studies. The search strategy was designed to be broad and combined the terms omega-3 and HRV. For example, the PubMed search strategy included: ("Fatty Acids, Omega-3"[Mesh] OR "Fish Oils"[Mesh] OR omega-3 OR EPA OR DHA) AND ("Heart Rate"[Mesh] OR "Heart Rate Variability"[Mesh] OR HRV).
EndNote X8 was used to import all received records, and duplicate studies were removed. Titles, abstracts, and the full texts of potential studies were filtered using the PICO framework. Study selection was carried out independently by two reviewers. After merging search results and removing duplicates, we screened abstracts and titles, followed by a thorough assessment of the complete texts of possibly eligible research. Any disputes that arose during this process were handled through discussion.
A standardized data-extraction format was used, including research identifiers, settings, sample sizes, event counts, outcomes, and notes. One reviewer extracted the data, and the other verified the accuracy.
Meta-analyses were carried out with Review Manager (RevMan, Version 5.4, The Cochrane Collaboration, 2020). For continuous outcomes, we calculated the mean difference and 95% confidence interval (CI) when all studies used the same scale. The standardized mean difference was used for outcomes reported in different units (e.g., normalized units vs absolute power for HF).
We employed a random-effects model for all analyses, as we anticipated clinical heterogeneity due to variations in study populations and intervention methods. The I2 statistic was used to measure heterogeneity, with a value above 50% indicating significant heterogeneity. The χ2 test (Cochran’s Q) was also used, with a significance level of P < 0.10 indicating significant heterogeneity. Because the number of papers (< 10) for each outcome, assessment of publication bias using funnel plots was not feasible.
Using the Cochrane Risk of Bias tool (ROB 2.0), two reviewers independently assessed the risk of bias in the included RCTs. This tool evaluates bias across five domains: (1) Randomization process; (2) Deviations from intended interventions; (3) Missing outcome data; (4) Measurement of the outcome; and (5) Selection of the reported result. Each study was judged to have a “low risk”, “some concerns”, or “high risk” of bias for each domain. The overall risk of bias judgment for each article was then calculated. A summary of the risk of bias across domains is illustrated in Table 1.
| Ref. | Domain 1: Randomization process | Domain 2: Deviations from intended interventions | Domain 3: Missing outcome data | Domain 4: Measurement of the outcome | Domain 5: Selection of reported results | Overall risk of bias (auto) |
| Ninio et al[8], 2008 | Low risk | Low risk | Low risk | Low risk | Low risk | Low risk |
| Sjoberg et al[9], 2009 | Low risk | Low risk | Low risk | Low risk | Low risk | Low risk |
| Baumann et al[10], 2018 | High risk | Some concerns | Low risk | Some concerns | Low risk | High risk |
| Ibrahim et al[11], 2025 | Low risk | Low risk | Low risk | Low risk | Low risk | Low risk |
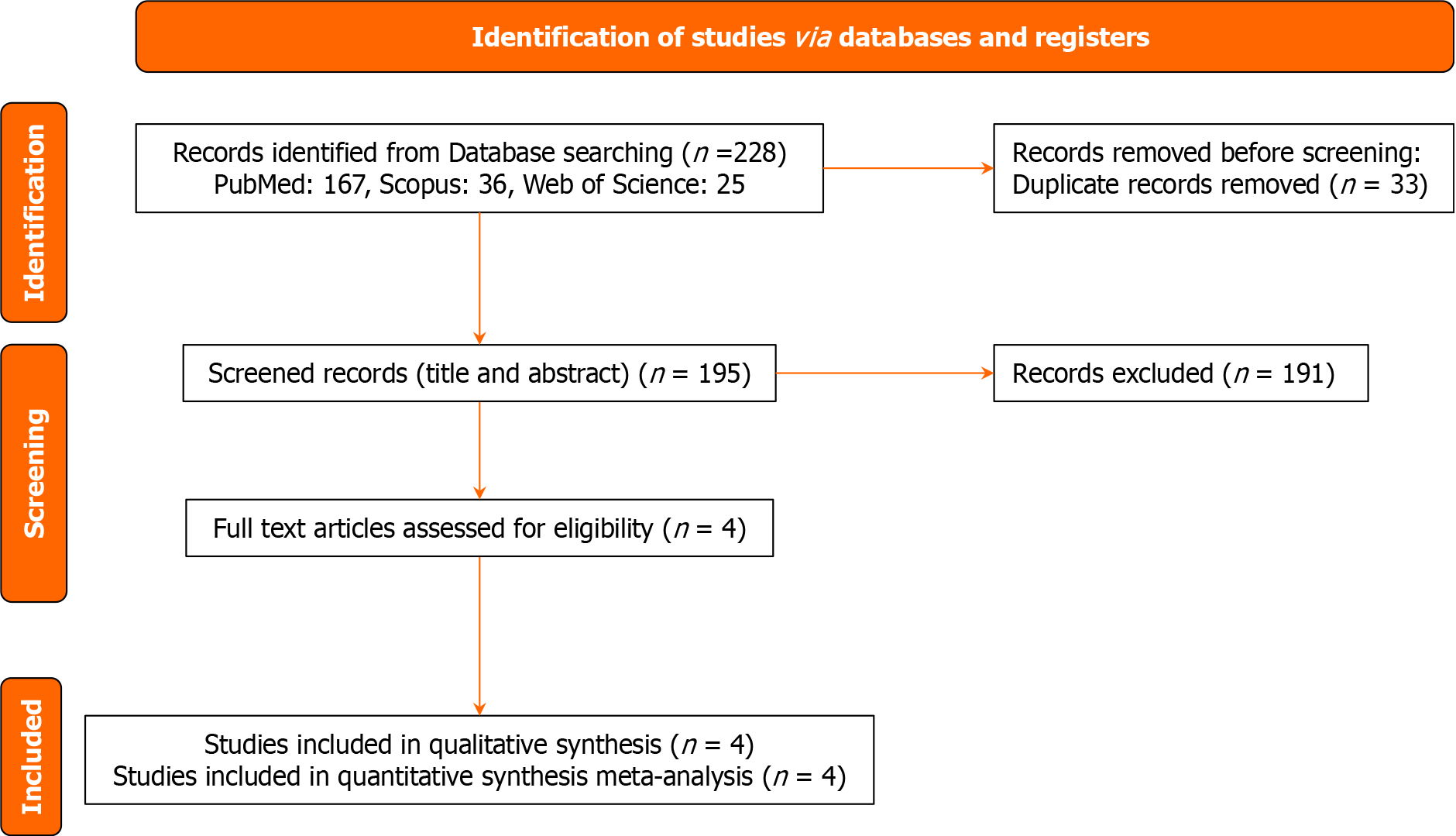
Our initial systematic search of PubMed, Scopus, and Clarivate yielded 228 records. After eliminating 33 duplicates, we reviewed the abstracts and titles of 195 distinct studies. The vast majority (n = 191) were excluded because they did not meet the eligibility criteria. This left four studies for full-text review[8-11]. All four were deemed suitable for inclusion and were subsequently used in qualitative synthesis and meta-analysis (Figure 2).
We used the ROB 2.0 tool to evaluate the methodological quality of the included RCTs. The risk of bias was deemed low for three studies[8,9,11]. These trials demonstrated robust randomization protocols, minimal variations from the intended interventions, and thorough outcome data reporting.
The four included RCTs, published between 2008 and 2025, enrolled a total of 134 participants. Of these, 90 were assigned to omega-3 supplementation groups and 94 to control groups (placebo or standard care). Table 2 presents the socio-demographic criteria of the enrolled studies.
| Ref. | Country | Study design | Population/sample size | Intervention/exposure | Comparator | Outcome(s) | Duration | Main findings | Type and dose of omega-3 fatty acid, mg/day |
| Ninio et al[8], 2008 | Australia | A randomized, double-blind, parallel trial | Fifty overweight, sedentary adults with risk factors for coronary disease | DHA-rich fish oil 6 g/day (providing 1.56 g DHA + 0.36 g EPA) (n = 23) | Sunflower seed oil (placebo) (n = 27) | Resting heart rate, heart rate during submaximal exercise, and HRV parameters (high-frequency and low-frequency power) | 12 weeks | DHA-rich fish oil significantly increased high-frequency power (indicative of enhanced parasympathetic/vagal tone). Resting heart rate and heart rate during exercise were significantly reduced compared with placebo | DHA-rich fish oil: Approximately 1560 mg DHA/day and approximately 360 mg EPA/day (total 6 g fish oil) |
| Sjoberg et al[9], 2009 | Australia | A randomized, double-blind, placebo-controlled, parallel dose-response supplementation trial | Thirty-four overweight or obese adults | DHA-rich fish oil (n = 17) | Placebo (6 g/day of sunola oil) (n = 17) | HRV, specifically the low frequency, high frequency, and (LF/HF) ratio | 12 weeks | The LF/HF ratio of HRV decreased with increasing doses of fish oil. The changes in these biomarkers may reflect that fish oil-induced improvements in arterial function and cardiac autonomic regulation | The 2, 4, and 6 g/day doses of fish oil provided 0.52, 1.04, and 1.56 g DHA/day, respectively |
| Baumann et al[10], 2018 | Germany | A parallel randomized interventional control trial | 20 obese children/adolescents (BMI > 95th percentile) | Daily omega-3 fatty acid supplementation (fish oil capsules) | Same obese subjects before supplementation | Time-domain HRV parameters (SDNN, RMSSD, pNN50) | At least 3 months, average of approximately 214 days (≈ 7 months) between baseline and follow-up ECG in the obese group | Omega-3 fatty acid supplementation may be used for cardiovascular prophylaxis in obese children and adolescents | Fish oil capsules containing at least 400 mg EPA and 120 mg DHA per day |
| Ibrahim et al[11], 2025 | Egypt | A parallel randomized interventional control trial | 30 overweight and obese children | Omega-3 supplementation | Same obese children before supplementation | HRV differences in RMSSD, SDNN, pNN50%, and lipid profiles | 3 months | Significant increases in HRV measures (RMSSD, SDNN, pNN50) in the omega-3 group compared to controls. Significant improvements in lipid profile: Decreased triglycerides and increased HDL in the omega-3 group | 400 mg EPA and 200 mg DHA daily for 3 months was taken (the ratio of EPA to DHA to 2:1) |
Heart rate variability parameters: This part of the meta-analysis included data from two studies[10,11], involving 50 participants in the omega-3 group and 50 in the control group.
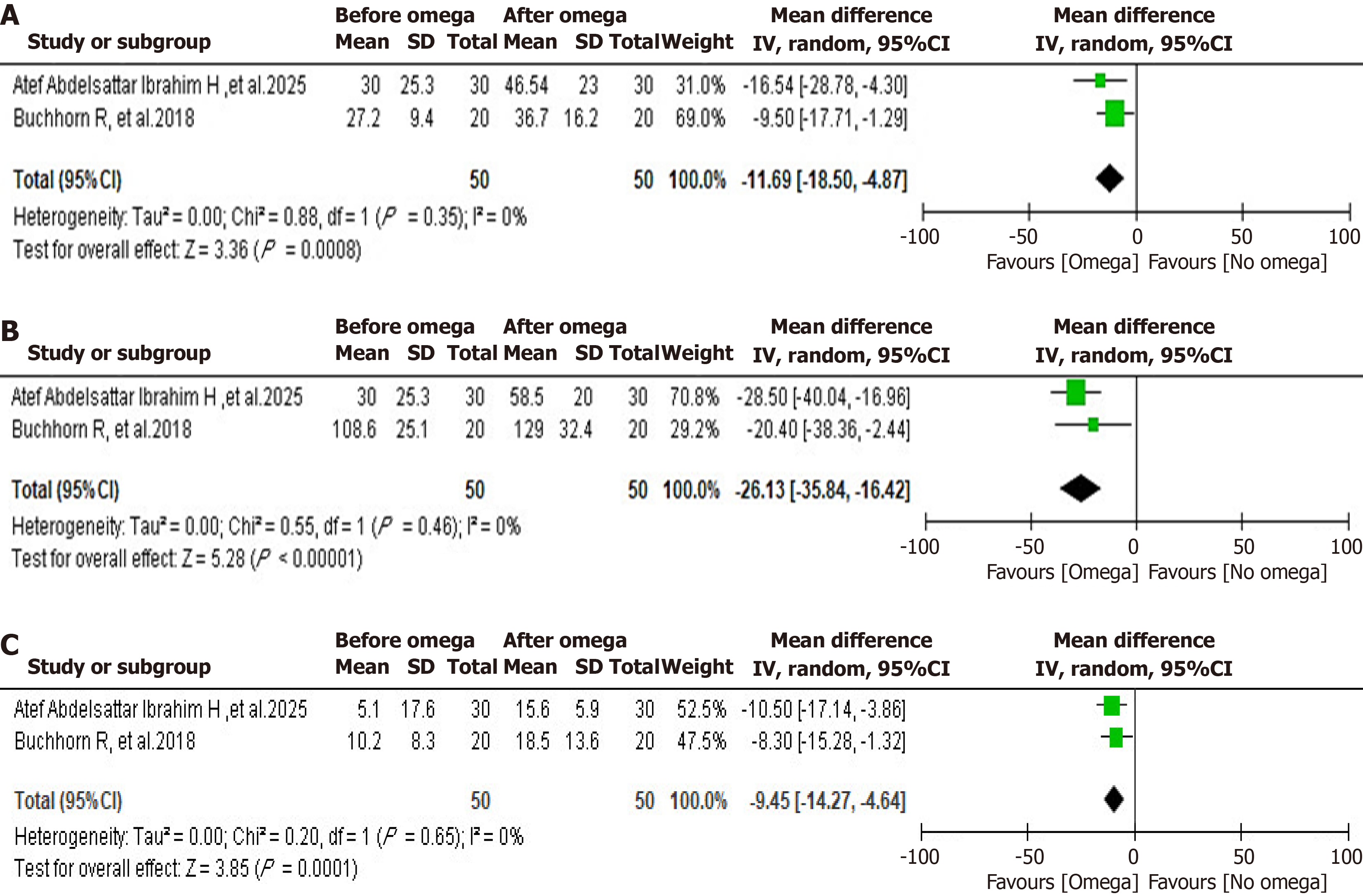
RMSSD: A meta-analysis of RMSSD demonstrated a significant improvement in parasympathetic activity following omega-3 supplementation. The forest plot showed a statistically significant increase in RMSSD compared to the baseline with a mean difference (pre-post) of -11.69 (95%CI: -18.50 to -4.87; P = 0.0008). The random effects model (I2 = 0%, τ2 = 0.00, χ2 = 0.88, P = 0.35), which denoted a low heterogeneity (Figure 3A).
SDNN: A meta-analysis of SDNN revealed a significant increase in the omega-3 group compared to the baseline, with a pooled mean difference (pre-post) of -26.13 (95%CI: -35.84 to -16.42, P < 0.00001). Heterogeneity was low (I2 = 0%, τ2 = 0.00, χ2 = 0.55, P = 0.46), Figure 3B.
pNN50%: A meta-analysis of pNN50% demonstrated a statistically significant improvement in parasympathetic activity following omega-3 supplementation. The pooled mean difference favored the omega-3 group with a mean difference (pre-post) of -9.45 (95%CI: -14.27 to -4.64, P = 0.0001). Heterogeneity across studies was negligible (I2 = 0%, τ2 = 0.00, χ2 = 0.20, P = 0.65), indicating consistency of effect across trials (Figure 3C).
This finding complements the improvements observed in RMSSD, SDNN, and pNN50%, collectively reinforcing the beneficial effect of omega-3 supplementation on vagal-mediated cardiac modulation in overweight and obese individuals.
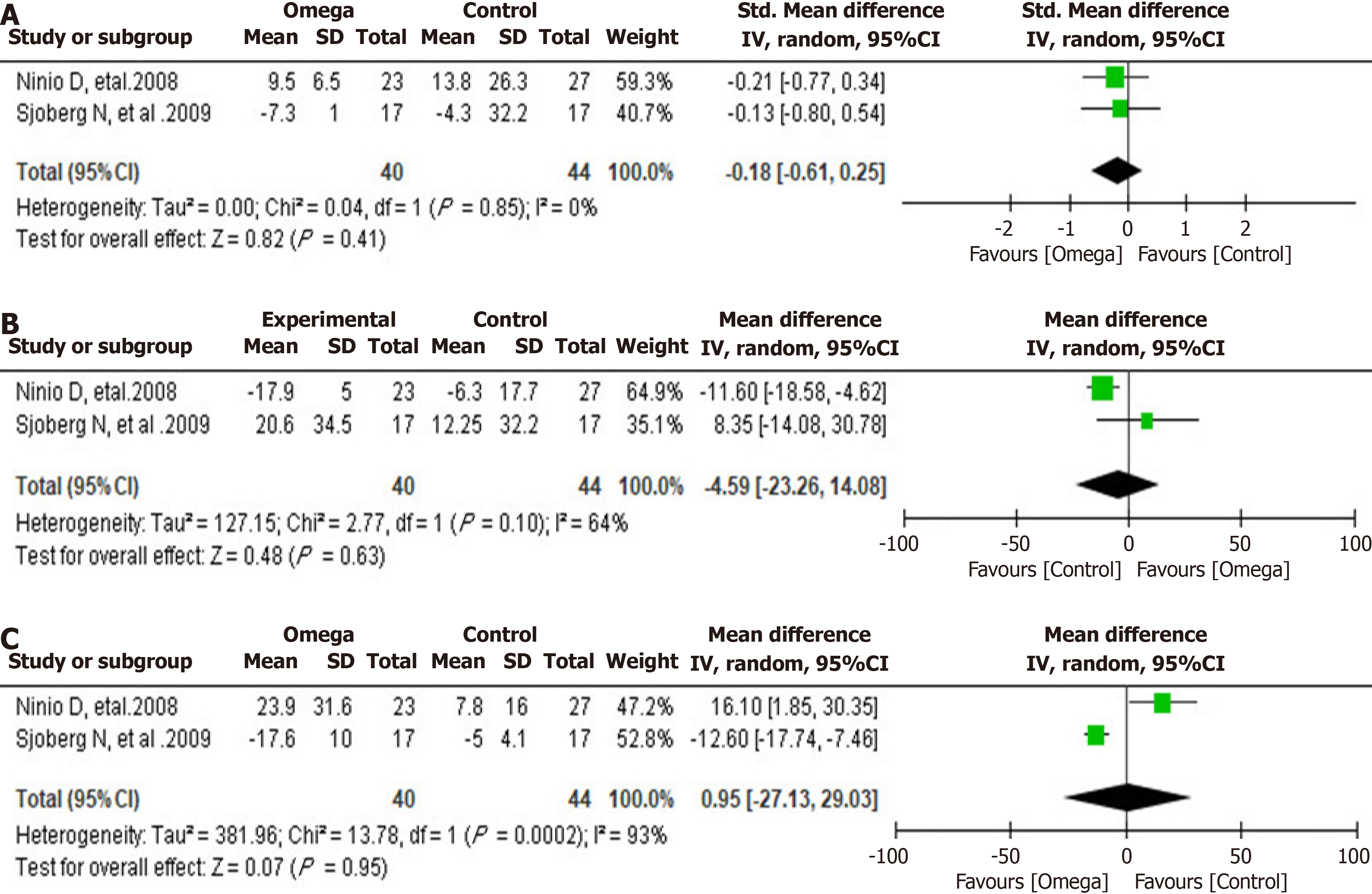
This part of the meta-analysis included two studies[8,9], with 40 individuals in the omega-3 group and 44 individuals in the control group. Analysis of HF Power, LF Power, and LF/HF ratio showed no significant difference between groups, with mean differences of -0.18 (95%CI: -0.61 to 0.25, P = 0.41), -4.59 (95%CI: -23.26 to 14.08, P = 0.63), and 0.95 (95%CI:
Subgroup analyses by comparator type and sensitivity analyses excluding pilot trials were pre-specified but could not be conducted due to only three RCTs. Publication bias was not assessed because of the small number of articles.
This systematic review and meta-analysis demonstrate that omega-3 supplementation significantly improves time-domain HRV measures (SDNN, RMSSD, and pNN50%) and lowers resting heart rate in overweight and obese individuals. These changes suggest an enhanced parasympathetic (vagal) tone and improved autonomic balance. The effects of omega-3 supplementation on the frequency-domain measures were mixed, with little overall evidence of improvement. Omega-3 PUFAs, therefore, show promise as a safe, low-cost intervention to enhance cardiac autonomic regulation in obesity.
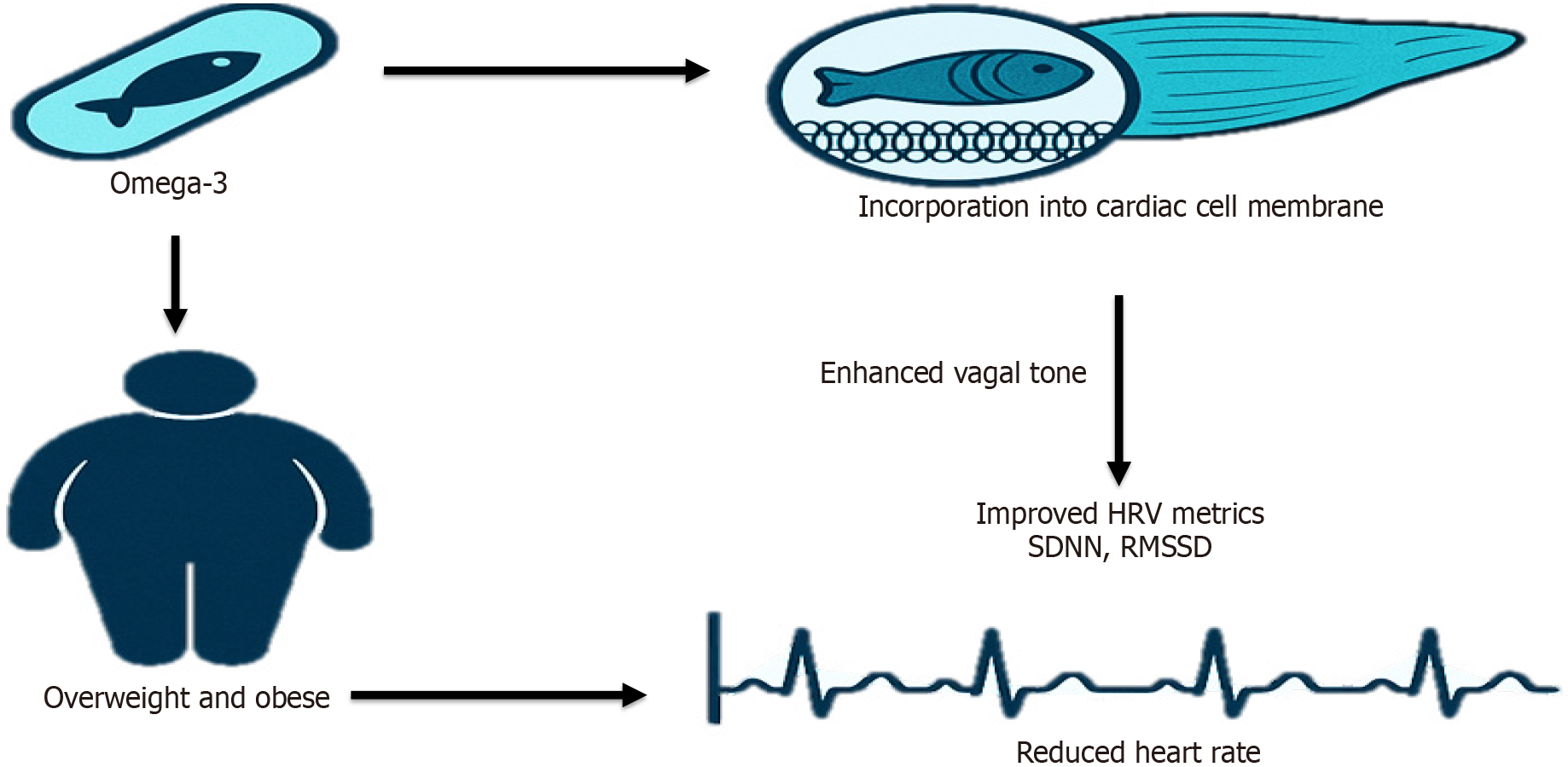
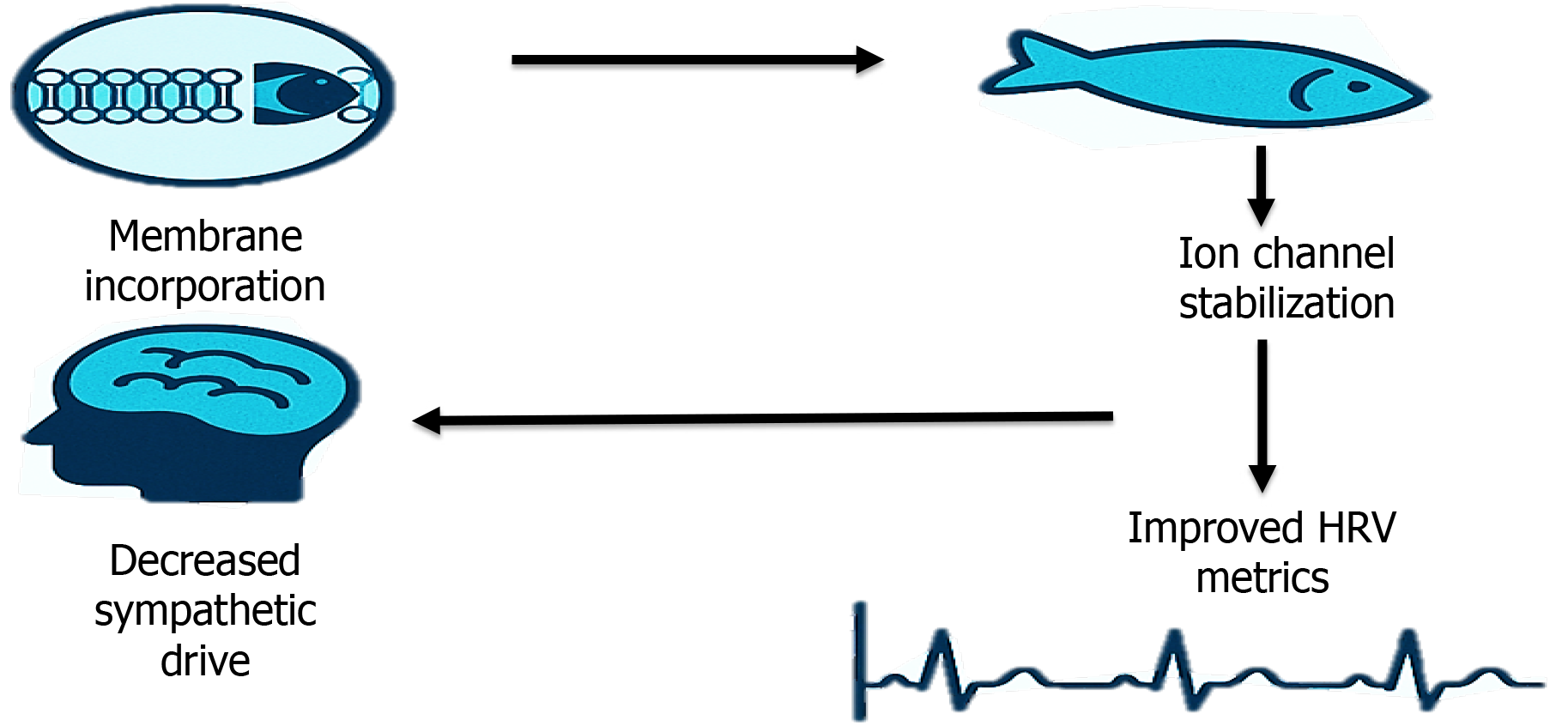
Omega-3 fatty acids can affect cardiac autonomic function through incorporation into cell membranes, altering ion channel function and membrane fluidity, thereby stabilizing cardiac electrophysiology. They may suppress sympathetic activity and enhance vagal tone by modulating sodium and calcium channel currents and reducing inflammation. The proposed mechanisms are illustrated in Figure 6. Clinically, fish-oil intake is linked to lower resting heart rate and improved HRV. In the dose-response trial, reductions in the LF/HF ratio were accompanied by increased arterial compliance and higher erythrocyte eicosapentaenoic acid (EPA) levels, suggesting vascular and anti-inflammatory effects as mediators. Improved lipid profiles observed in adolescents may further support autonomic regulation.
Our results align with previous meta-analyses showing that omega-3 supplementation modestly reduces resting heart rate and may enhance parasympathetic modulation. However, earlier reviews often focused on post-myocardial infarction or dialysis patients. By concentrating on overweight and obese populations, this review extends the evidence base and quantifies improvements in time-domain HRV measures. The inconsistent frequency-domain findings mirror mixed results across the broader literature.
Supplementing with omega-3 fatty acids, specifically docosahexaenoic acid (DHA)-rich fish oil, showed positive benefits on cardiac autonomic function in the four trials. DHA supplementation in overweight and obese adults improved HRV indices and arterial compliance in a dose-dependent manner. It also improved heart rate responses and recovery after exercise. Similarly, omega-3 fatty acids supplementation significantly enhanced HRV measures in obese children and adolescents, normalizing them toward levels seen in healthy controls, indicating better autonomic balance and vagal tone. Collectively, these data support the possible benefit of omega-3 fatty acids in enhancing cardiovascular autonomic regulation and reducing cardiovascular risk in obese and overweight populations[8-11].
Strengths of this study include an extensive search across several databases, a prospectively registered protocol, rigorous risk of bias assessment, and inclusion of both pediatric and adult populations.
Limitations of this study include the small number of eligible studies, modest sample sizes, and heterogeneity in dosing, duration, and HRV measurement methods. One pre-post study lacked randomization, and the short intervention durations preclude assessment of long-term effects.
Given its favorable safety profile, omega-3 supplementation could be considered an adjunct strategy to improve autonomic function in overweight and obese individuals. Doses ≥ 1 g/day of combined DHA + EPA and at least three months of treatment may be needed to observe meaningful changes. Future research should include larger, multicenter RCTs with longer follow-up, explore dose-response relationships and EPA: DHA ratios, standardize HRV assessment, and investigate mechanistic pathways. Combining omega-3 supplementation with lifestyle interventions, such as exercise, may yield synergistic benefits.
This systematic review and meta-analysis provide evidence regarding the positive effects of omega-3 fatty acid supplementation on HRV indices, specifically the time-domain measures, in obese and overweight populations.
| 1. | Tomar A, Ahluwalia H, Ramkumar S, Pattnaik S, Nandi D, Raturi P. The interplay of heart rate variability and ventricular repolarization parameters in the obese state: a review. Cardiovasc Endocrinol Metab. 2025;14:e00323. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 2. | Stathori G, Vlahos NF, Charmandari E, Valsamakis G. Obesity- and High-Fat-Diet-Induced Neuroinflammation: Implications for Autonomic Nervous System Dysfunction and Endothelial Disorders. Int J Mol Sci. 2025;26:4047. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 10] [Reference Citation Analysis (1)] |
| 3. | Speer KE, Naumovski N, McKune AJ. Heart rate variability to track autonomic nervous system health in young children: Effects of physical activity and cardiometabolic risk factors. Physiol Behav. 2024;281:114576. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 4. | Sinha MK, K V, Maiya AG, K N S, U S, N RS. Association of physical activity and heart rate variability in people with overweight and obesity: A systematic review. F1000Res. 2023;12:156. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 12] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 5. | Shen S, Gong C, Jin K, Zhou L, Xiao Y, Ma L. Omega-3 Fatty Acid Supplementation and Coronary Heart Disease Risks: A Meta-Analysis of Randomized Controlled Clinical Trials. Front Nutr. 2022;9:809311. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 40] [Article Influence: 10.0] [Reference Citation Analysis (1)] |
| 6. | Baumgartner P, Reiner MF, Wiencierz A, Coslovsky M, Bonetti NR, Filipovic MG, Aeschbacher S, Kühne M, Zuern CS, Rodondi N, Oberle J, Moschovitis G, Lüscher TF, Camici GG, Osswald S, Conen D, Beer JH; SWISS‐AF Investigators. Omega-3 Fatty Acids and Heart Rhythm, Rate, and Variability in Atrial Fibrillation. J Am Heart Assoc. 2023;12:e027646. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 7. | Macartney MJ, Ghodsian MM, Noel-Gough B, McLennan PL, Peoples GE. DHA-Rich Fish Oil Increases the Omega-3 Index in Healthy Adults and Slows Resting Heart Rate without Altering Cardiac Autonomic Reflex Modulation. J Am Nutr Assoc. 2022;41:637-645. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 8. | Ninio DM, Hill AM, Howe PR, Buckley JD, Saint DA. Docosahexaenoic acid-rich fish oil improves heart rate variability and heart rate responses to exercise in overweight adults. Br J Nutr. 2008;100:1097-1103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 41] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 9. | Sjoberg NJ, Milte CM, Buckley JD, Howe PR, Coates AM, Saint DA. Dose-dependent increases in heart rate variability and arterial compliance in overweight and obese adults with DHA-rich fish oil supplementation. Br J Nutr. 2010;103:243-248. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 41] [Article Influence: 2.4] [Reference Citation Analysis (1)] |
| 10. | Baumann C, Rakowski U, Buchhorn R. Omega-3 Fatty Acid Supplementation Improves Heart Rate Variability in Obese Children. Int J Pediatr. 2018;2018:8789604. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 12] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 11. | Ibrahim HAA, Sobhi R, Khaled Farouk N, Mohamed AbdelAziz F. Omega and heart rate variability in overweight and obese schoolchildren. Pediatr Res. 2025;98:957-965. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/