Published online Mar 9, 2026. doi: 10.5409/wjcp.v15.i1.110584
Revised: July 7, 2025
Accepted: October 21, 2025
Published online: March 9, 2026
Processing time: 270 Days and 0.7 Hours
Pediatric complex regional pain syndrome (CRPS) is a debilitating chronic condition that affects the quality of life and psychosocial development of children and adolescents. Despite increasing recognition, significant diagnostic and the
To evaluate current diagnostic and therapeutic practices in pediatric CRPS, id
Physiotherapists who had treated at least one pediatric CRPS case in the past two years were surveyed. The online questionnaire included 40 questions divided into three sections: Professional knowledge, therapeutic approaches, and personal perceptions. Data were analyzed using descriptive statistics and χ2 tests.
Most participants worked in private clinics (71%) and collaborated with other healthcare professionals. About 53% had specific training in pediatric pain, while 40% had training in CRPS. Only 13% had received training in cognitive-behavioral therapy (CBT). The use of the Budapest criteria was limited, primarily applied during the diagnostic suspicion phase. The most common therapeutic strategies included mirror therapy (40%) and relaxation techniques (80%). The main reported challenges were the lack of specific clinical guidelines (60%) and insufficient professional training (47%).
Physical therapists are key contributors to multidisciplinary diagnosis and play a central role in managing pediatric CRPS in most cases, adopting a collaborative and largely non-pharmacological approach. However, the absence of stand
Core Tip: Pediatric complex regional pain syndrome is a complex condition that significantly impacts children’s well-being, yet diagnostic and treatment challenges remain due to the lack of pediatric-specific criteria. This study surveyed physiotherapists to assess current practices and knowledge gaps. Limited use of diagnostic tools and the absence of standardized guidelines were major barriers identified. The findings highlight the need for tailored protocols and improved training in psychological therapies.
- Citation: Moutafakir R, Strilinsky-Pérez OD, Zamora-Tortosa J, Raya-Benítez J, Benítez-Feliponi Á, Valenza MC, Granados-Santiago M. Beliefs, attitudes, knowledge, and behaviours of physical therapists towards pediatric complex regional pain syndrome. World J Clin Pediatr 2026; 15(1): 110584
- URL: https://www.wjgnet.com/2219-2808/full/v15/i1/110584.htm
- DOI: https://dx.doi.org/10.5409/wjcp.v15.i1.110584
Pediatric complex regional pain syndrome (CRPS) is a chronic and disabling pain condition that primarily affects children and adolescents. It has a profound impact on quality of life, physical function, and psychosocial development[1]. The syndrome is characterized by persistent pain that is often disproportionate to the initial injury, along with sensory disturbances such as allodynia and hyperalgesia, autonomic chan
The pathophysiology of pediatric CRPS remains incompletely understood but is believed to involve peripheral and central sensitization, inflammation, and cortical reorganization[4]. In pediatric population, the condition frequently follows minor trauma or occurs without a clear trigger, most commonly affecting the lower limbs[5].
Early diagnosis is critical, as delayed intervention can lead to chronic disability, school absenteeism, and significant emotional distress, including anxiety and depression[6]. However, diagnostic challenges persist due to the lack of definitive biomarkers and reliance on clinical criteria, which may not fully capture pediatric presentations[7].
Management today relies on a comprehensive, multidisciplinary approach involving physical therapy, psychological support, and medication to enhance function and manage symptoms[8]. Emerging evidence supports the use of graded motor imagery, mirror therapy, and desensitization techniques to reestablish normal sensory-motor integration[9]. According to a scoping review[10], integrating cognitive-behavioral therapy (CBT) with physiotherapy education can support a holistic biopsychosocial approach and lead to better patient outcomes. Nevertheless, treatment responses vary, and relapse rates remain concerning, highlighting the need for personalized, evidence-based strategies[11].
New approaches like sensory testing and thermography may facilitate earlier detection and more effective monitoring[12]. Additionally, innovative therapies like transcranial magnetic stimulation and virtual reality-based rehabilitation are being explored to target maladaptive neural pathways[13]. Despite these developments, disparities in access to specialized care and inconsistent adherence to clinical guidelines continue to hinder optimal outcomes[14].
Previous reviews[10,15,16] have highlighted the importance of a multidisciplinary approach while also noting the absence of pediatric-specific diagnostic tools, which contributes to delays and variability in treatment. Accordingly, this study aims to assess current diagnostic and therapeutic practices in pediatric CRPS, identifying barriers to timely intervention and gaps in provider knowledge. By examining clinical decision-making, the application of protocols, and the integration of emerging technologies, this research aims to improve multidisciplinary care and long-term outcomes, promote more consistent practice, and address existing deficiencies in clinical management. Ultimately, enhancing early recognition and evidence-based management may mitigate the profound physical and emotional burdens imposed by pediatric CRPS.
A cross-sectional study was carried out to examine the beliefs, attitudes, knowledge, and behaviors of physical therapists towards differential diagnostic and therapeutic practices in pediatric CRPS. The study was performed according to the ethical principles of the Declaration of Helsinki. It was carried out between October 2024 and January 2025 in France.
Participants were licensed physiotherapists (≥ 18 years) who have treated at least one child or adolescent diagnosed with CRPS within the past two years in hospitals, private practices, clinics, or rehabilitation centers. Participants should have an adequate understanding of the language in which the questionnaire is written to ensure that their responses are accurate and meaningful. Access to an internet connection is required for participation.
Physiotherapists not practicing in France, undergraduate physical therapy students, trainees, and individuals without professional experience in this field were excluded from participation. Furthermore, physiotherapists who do not complete the entire questionnaire will not be included in the study.
A convenience sample of physiotherapists was recruited to participate voluntarily in the study. Participants provided informed consent before beginning the questionnaire, after reviewing the consent statement. The survey was conducted in accordance with France’s personal data protection regulations, which adapts the GDPR legal framework and ensure the anonymity and confidentiality of the participants.
The questionnaire was distributed through several channels, including the national health insurance physiotherapists’ directory, various professional and training networks for physiotherapists (such as 'réseau kinepediatrie', 'Kiné pédia PACA', 'kine-pédiatrie', 'MedOrtho', 'Superkiné pédiatrie', 'kiné pédia 2020-2021', 'kinésithérapie', 'superkiné parisien', 'le réseau des kinés', and 'le monde des kinés'), as well as social media platforms (Linkedln®, Facebook®, and Instagram®; Menlo Park, CA, United States), to maximize participation among physiotherapists in private practice in France.
The platform “Eval and Go” was used to design the questionnaire. Previously, physiotherapists were contacted through various social media networks, and those who responded positively to the invitation subsequently received the URL link to access the questionnaire.
The questionnaire includes 40 questions divided into three sections: (1) “Knowledge and characteristics of the professionals in the sample population”, consists of four questions that explore the setting of care (such as “In what type of facility have you treated patients with CRPS?”), multidisciplinary collaboration, specific knowledge acquired by professionals, and diagnostic modalities of paediatric CRPS; (2) “Therapeutic approach of paediatric CRPS”, includes nine questions focused on the use of Budapest criteria (standard diagnostic criteria), initial assessment (such as “What treatments do you primarily use to manage pain in pediatric patients with CRPS?”), consideration of CRPS phase in pain management, recommendations during the acute phase, recommendations during the chronic phase, therapeutic education and cognitive-behavioural therapy (CBT) [such as “Do you incorporate cognitive-behavioral therapy (CBT) as part of your treatment?”], pain treatments in CRPS and associated treatments received by patients; and (3) “Professionals' own perceptions”, includes difficulties in the management of pediatric patients with CRPS (such as “What difficulties have you encountered in the management of pediatric CRPS patients?”).
The questionnaire comprised multiple-choice questions developed from existing literature to ensure structured and focused responses; with no open-ended questions included.
All questionnaire responses were collected directly through the application and subsequently exported to Microsoft Excel for processing. Statistical analyses were conducted using SPSS Version 23.0 statistical software (SPSS Inc., Chicago, IL, United States). Summary descriptive statistics, including mean values with 95% confidence intervals, were calculated for the socio-demographic data of the participants. Descriptive analyses of study variables were performed using absolute and relative frequencies (%). For categorical variables, frequencies and proportions were calculated to describe the distribution of the main characteristics of the population included. Results are presented in tables. The χ2 test of independence was used to assess associations between categorical variables.
A total of 15 physiotherapists with experience in treating CRPS in the paediatric population were surveyed. The professionals’ characteristics and knowledge are presented in Table 1.
| Overall (n = 15) | |||
| Variable | % | ||
| Setting of care | Private clinics | 71 | |
| Hospitals and specialised centres | 24 | ||
| Home care services | 6 | ||
| Multidisciplinary collaboration | With other healthcare professionals | Doctors/pain team | 27 |
| Psychologists | 20 | ||
| Specific knowledge | Paediatric pain | 53 | |
| Chronic pain and CRPS | 40 | ||
| CBT | 13 | ||
| Without specific knowledge | 7 | ||
| Diagnostic modalities of paediatric CRPS | Doctor | 38 | |
| Physiotherapist | 48 | ||
| Informal diagnosis | 14 | ||
As for the setting of care, the majority of physiotherapist worked in private clinics (71%), followed by those based in hospitals or specialised centres (24%) and home care services (6%).
A high level of collaboration with other healthcare professionals was observed (60%), with the pain team (27%) and psychologists (20%) being the most contacted.
In terms of specific knowledge, 53% had received training in paediatric pain, 40% in chronic pain or CRPS, and 13% in CBT. A total of 7% of the professionals reported having received no specific knowledge in any of these areas.
Regarding the diagnostic modalities to paediatric CRPS, a relatively balanced distribution was observed between medical professionals (38%) and physiotherapists (48%) as those responsible for the diagnosis, while 14% reported that the diagnosis is not clearly established within the medical field.
Therapeutic approaches of paediatric CRPS are included in Table 2.
| Overall (n = 15) | ||
| Variable | % | |
| Use of Budapest criteria | Do not use Budapest criteria | 33 |
| Used when CRPS is suspected (pre-diagnostic phase) | 40 | |
| Used during confirmed diagnosis (evaluation or treatment phase) | 13 | |
| Unfamiliar with Budapest criteria | 7 | |
| Initial assessment | Pain and function | 93 |
| Functional impact | 53 | |
| Quality of life | 46 | |
| Psychological aspect | 40 | |
| Recommendations during the acute phase of CRPS | Rest and splint use | 31 |
| Analgesic use | 34 | |
| Regular physical activity | 21 | |
| Warm baths | 14 | |
| Combination of strategies | 40 | |
| Recommendations during the chronic phase of CRPS | Removal of supportive splint | 47 |
| Regular physical activity | 67 | |
| Increasing of intensity and frequency of physical activity | 53 | |
| Analgesics no recommended | 100 | |
| Therapeutic education | Relaxation techniques/stress management | 80 |
| Behavioral education/emotional support | 53 | |
| parent-focused intervention | 47 | |
| CBT | Find CBT useful | 73 |
| Unable to apply CBT | 20 | |
The use of the Budapest diagnostic criteria was limited: 33% of participants reported not using them, 40% used them only when CRPS was clinically suspected, and 13% applied them during assessment or treatment. Notably, 7% indicated they were unfamiliar with the criteria.
Initial assessment focused primarily on pain and function (93%), followed by functional impact (53%), quality of life (46%), and psychological factors (40%).
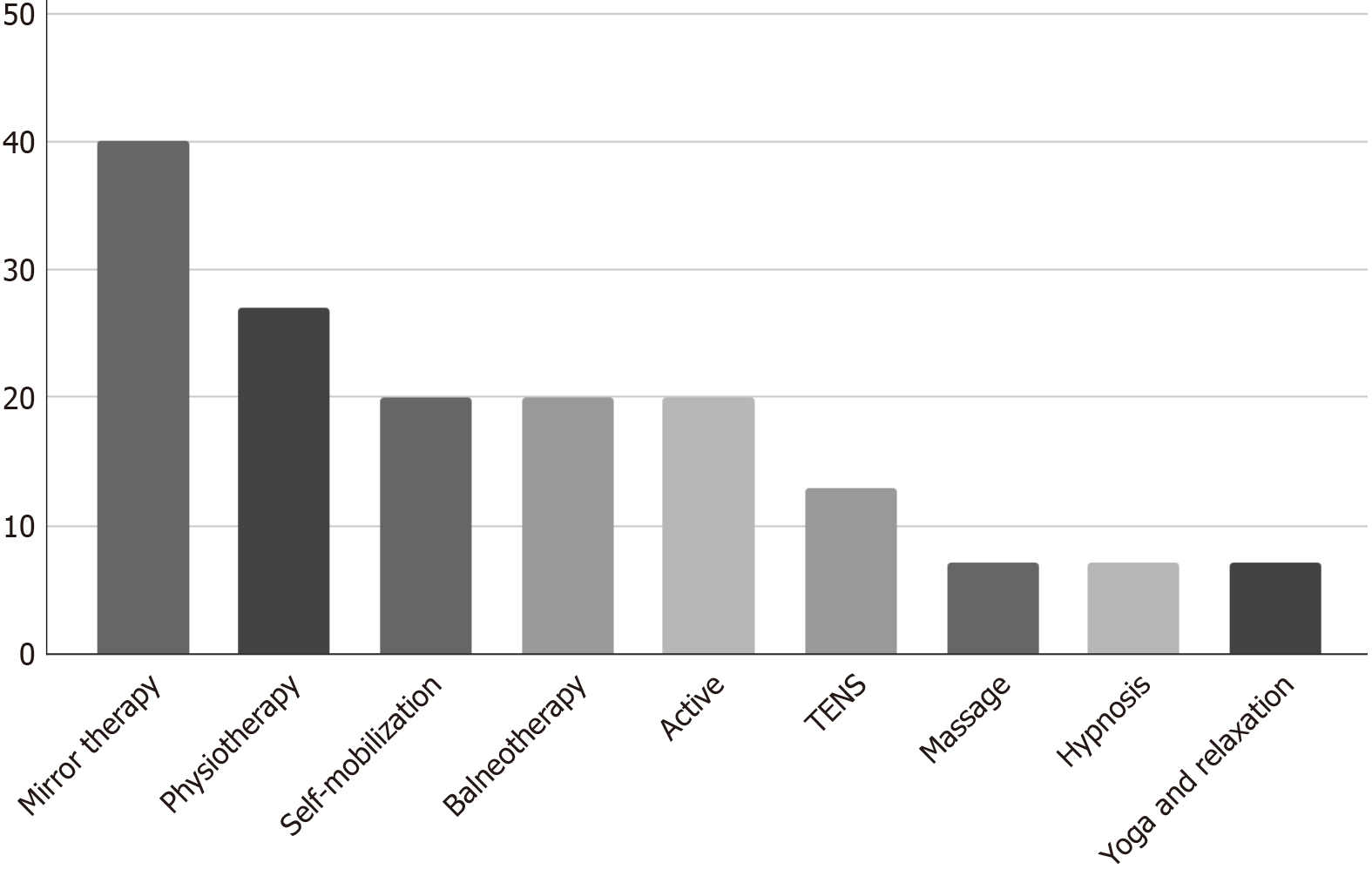
Figure 1 shows that pain management is mainly based on mirror therapy (40%) and physiotherapy (27%). Physical approaches such as self-mobilisation, balneotherapy, and active movement strategies were employed in 20% of cases. Transcutaneous electrical nerve stimulation was used in 13% of cases. In contrast, massage, yoga, and hypnosis were integrated in 7% of the cases.
During this acute (“hot”) phase, the most common therapeutic recommendations included the use of analgesics (34%), rest and splinting (31%), and regular physical activity (21%), while 40% reported employing a combination of strategies. In contrast, during the chronic (“cold”) phase, there was greater consensus: 100% of professionals discouraged the use of analgesics, and most promoted regular physical activity (67%).
Therapeutic education was widely implemented, with over 80% of professionals incorporating psychoeducation and stress management techniques. However, only 53% included behavioural education or emotional support, and 47% actively involved parents in the therapeutic process.
As for CBT, 73% of respondents considered it a useful tool, although only 33% reported actively integrating it into their clinical practice. Twenty per cent stated they lacked the necessary knowledge for its implementation.
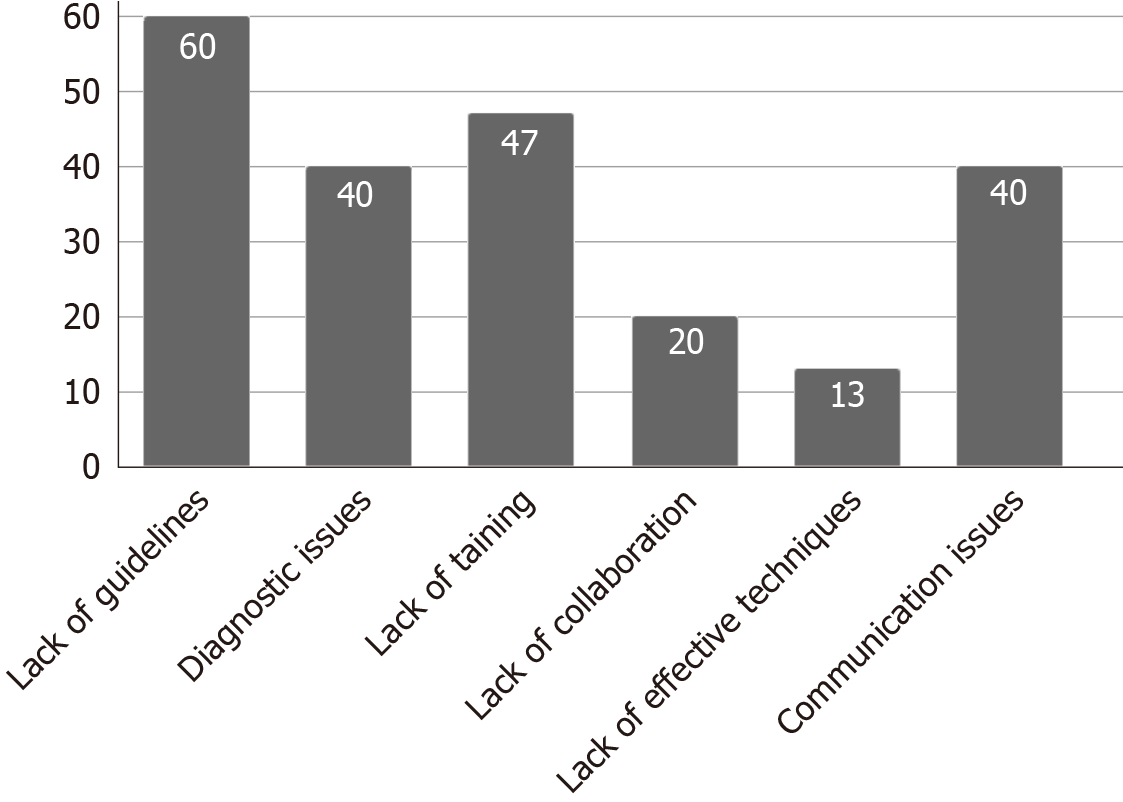
Professionals' own perceptions. Figure 2 shows the professionals' own perceptions regarding the difficulties in managing pediatric patients with CRPS.
The main difficulties identified included the lack of specific guidelines (60%), diagnostic issues (40%), lack of training (47%), lack of collaboration (20%), communication issues with other professionals (40%), and the perceived absence of effective techniques (13%).
This study aimed to evaluate current diagnostic and therapeutic approaches to pediatric CRPS. We found that physiotherapists made most of the diagnoses, care was primarily delivered in private clinics, and professionals often had specialized training in pediatric pain and preferred to work collaboratively with others healthcare professionals. Additionally, the Budapest criteria were primarily applied when a diagnosis of pediatric CRPS was suspected. Initial evaluations focused on pain and functional assessment. Mirror therapy and relaxation techniques or stress management strategies (particularly CBT) were commonly used and found to be helpful. The acute phase involved a combination of treatments, whereas in the chronic phase, analgesics were not recommended, and physical activity was promoted. Finally, a major issue identified in the management of pediatric CRPS was the lack of standardized clinical guidelines.
Prior research evaluated the physiotherapy professional’s perception and the diagnosis and treatment of children[17] and adults[18] chronic illness.
Our findings highlight that physiotherapists play a central role in diagnosing pediatric CRPS, with care predominantly delivered in private clinics by professionals trained in pediatric pain management. Emerging evidence suggests that diagnostic criteria developed for adults may lack sufficient sensitivity when applied to pediatric populations. A systematic review[19] identified four main diagnostic tools: The Veldman criteria, the International Association for the Study of Pain criteria, Budapest Criteria, and the Budapest Research Criteria. However, none of these tools have been validated for use in pediatric CRPS. Recent literature emphasizing the importance of multidisciplinary collaboration in CRPS care, particularly for children, where early intervention improves outcomes[10]. The predominant use of the Budapest criteria for diagnosis reflects current guidelines[20], though their adaptation for pediatric populations remains debated. While these criteria improve diagnostic specificity in adults, children often present with atypical symptoms[21], suggesting a need for pediatric-specific modifications. Our finding that pain and functional assessments dominate initial evaluations is consistent with the biopsychosocial approach recommended for pediatric pain[22,23]. Future studies are needed to develop a diagnostic tool tailored to pediatric populations.
According to our findings, mirror therapy and CBT are the recommended options in the management of pediatric CPRS[10]. Although 73% of participants considered CBT to be useful intervention for pediatric CRPS, only 33% reported incorporating it into their clinical practice. This gap may be attributed to physiotherapists’ limited formal training or lack of confidence in applying psychological strategies[24].
Besides, there are preferences for non-pharmacological therapies aligned with recent studies to minimize opioid use in pediatric pain[25]. For example, a review[26] reported high recovery rates when physical and behavioral strategies were combined. Similarly, a descriptive study[27] found that physiotherapy and psychological support were included in approximately threequarters of treatment protocols, whereas pharmacological interventions were used less frequently. These findings indicate that nonpharmacological approaches (particularly those addressing both physical and psychosocial aspects) play a central role in therapeutic decision-making and may provide age-appropriate benefits compared to pharmacotherapy, which has limited evidence and carries potential side effects in children.
Future research should focus on developing consensus guidelines that integrate physical, psychological, and non-pharmacological approaches for managing pediatric CRPS. Although expert consensus and commonly accepted treatment protocols are strongly recommended to optimize outcomes in pediatric chronic pain management[10,28], specific guidelines for pediatric CRPS remain lacking, as highlighted by our study.
Several limitations should be acknowledged. First, the small sample size represents a major limitation and restricts the generalizability of the findings. It also does not provide sufficient empirical breadth to support the development of a robust graded intervention algorithm. Additionally, the lack of formal validation of the online questionnaire constitutes a significant limitation, and the results should be interpreted with caution. The study also relied on self-reported data from participants which may introduce response bias and social desirability bias[29], which may affect the reliability and generalizability of the results. Moreover, the absence of multivariate analyses further limits the findings. Future research should aim to validate the questionnaire, conduct larger multicenter studies before proposing a definitive clinical flowchart, and exploring alternative methods to obtain more reliable data.
Physiotherapists play a central role in the multidisciplinary diagnosis and management of pediatric CRPS, primarily adopting a collaborative, non-pharmacological approach in private practice settings. Although strategies such as the Budapest criteria and physical activity are commonly implemented, the lack of standardized clinical guidelines remain a significant limitation. Future research should aim to develop standardized diagnostic and treatment protocol for pediatric CRPS to improve clinical outcomes in this population. Moreover, the development of a clinical guideline that consider the heterogeneity of this population is recommended, together with practical dissemination strategies to ensure accessibility in rural or resource-limited areas.
| 1. | Logan DE, Carpino EA, Chiang G, Condon M, Firn E, Gaughan VJ, Hogan M, Leslie DS, Olson K, Sager S, Sethna N, Simons LE, Zurakowski D, Berde CB. A day-hospital approach to treatment of pediatric complex regional pain syndrome: initial functional outcomes. Clin J Pain. 2012;28:766-774. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 128] [Cited by in RCA: 120] [Article Influence: 8.6] [Reference Citation Analysis (0)] |
| 2. | Weissmann R, Uziel Y. Pediatric complex regional pain syndrome: a review. Pediatr Rheumatol Online J. 2016;14:29. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 66] [Cited by in RCA: 76] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 3. | Low AK, Ward K, Wines AP. Pediatric complex regional pain syndrome. J Pediatr Orthop. 2007;27:567-572. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 111] [Cited by in RCA: 92] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 4. | Bruehl S. Complex regional pain syndrome. BMJ. 2015;351:h2730. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 310] [Cited by in RCA: 254] [Article Influence: 23.1] [Reference Citation Analysis (1)] |
| 5. | Harden RN, Oaklander AL, Burton AW, Perez RS, Richardson K, Swan M, Barthel J, Costa B, Graciosa JR, Bruehl S; Reflex Sympathetic Dystrophy Syndrome Association. Complex regional pain syndrome: practical diagnostic and treatment guidelines, 4th edition. Pain Med. 2013;14:180-229. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 331] [Cited by in RCA: 318] [Article Influence: 24.5] [Reference Citation Analysis (1)] |
| 6. | Finniss DG, Murphy PM, Brooker C, Nicholas MK, Cousins MJ. Complex regional pain syndrome in children and adolescents. Eur J Pain. 2006;10:767-770. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 13] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 7. | Abu-Arafeh H, Abu-Arafeh I. Complex regional pain syndrome in children: a systematic review of clinical features and movement disorders. Pain Manag. 2017;7:133-140. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 18] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 8. | Birklein F, Schlereth T. Complex regional pain syndrome-significant progress in understanding. Pain. 2015;156 Suppl 1:S94-S103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 105] [Cited by in RCA: 120] [Article Influence: 10.9] [Reference Citation Analysis (0)] |
| 9. | Goebel A, Bisla J, Carganillo R, Frank B, Gupta R, Kelly J, McCabe C, Murphy C, Padfield N, Phillips C, Sanders M, Serpell M, Shenker N, Shoukrey K, Wyatt L, Ambler G. Low-Dose Intravenous Immunoglobulin Treatment for Long-Standing Complex Regional Pain Syndrome: A Randomized Trial. Ann Intern Med. 2017;167:476-483. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 38] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 10. | Vescio A, Testa G, Culmone A, Sapienza M, Valenti F, Di Maria F, Pavone V. Treatment of Complex Regional Pain Syndrome in Children and Adolescents: A Structured Literature Scoping Review. Children (Basel). 2020;7:245. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 11] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 11. | Maihöfner C, Seifert F, Markovic K. Complex regional pain syndromes: new pathophysiological concepts and therapies. Eur J Neurol. 2010;17:649-660. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 123] [Cited by in RCA: 97] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 12. | Marinus J, Moseley GL, Birklein F, Baron R, Maihöfner C, Kingery WS, van Hilten JJ. Clinical features and pathophysiology of complex regional pain syndrome. Lancet Neurol. 2011;10:637-648. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 418] [Cited by in RCA: 451] [Article Influence: 30.1] [Reference Citation Analysis (0)] |
| 13. | Li WW, Guo TZ, Shi X, Birklein F, Schlereth T, Kingery WS, Clark JD. Neuropeptide regulation of adaptive immunity in the tibia fracture model of complex regional pain syndrome. J Neuroinflammation. 2018;15:105. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 37] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 14. | Bruehl S, Maihöfner C, Stanton-Hicks M, Perez RS, Vatine JJ, Brunner F, Birklein F, Schlereth T, Mackey S, Mailis-Gagnon A, Livshitz A, Harden RN. Complex regional pain syndrome: evidence for warm and cold subtypes in a large prospective clinical sample. Pain. 2016;157:1674-1681. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 91] [Article Influence: 9.1] [Reference Citation Analysis (0)] |
| 15. | Mesaroli G, Ruskin D, Campbell F, Kronenberg S, Klein S, Hundert A, Stinson J. Clinical Features of Pediatric Complex Regional Pain Syndrome: A 5-Year Retrospective Chart Review. Clin J Pain. 2019;35:933-940. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 17] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 16. | Baerg K, Tupper SM, Chu LM, Cooke N, Dick BD, Doré-Bergeron MJ, Findlay S, Ingelmo PM, Lamontagne C, Mesaroli G, Oberlander TF, Poolacherla R, Spencer AO, Stinson J, Finley GA. Canadian surveillance study of complex regional pain syndrome in children. Pain. 2022;163:1060-1069. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 13] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 17. | Kashif D, Tariq DES. Pain Assessment and Management of Neurologic Impairments by Pediatric Physical Therapists; A Cross-Sectional Survey. Healer J Phys Ther Rehabil Sci. 2022;2:97-103. [DOI] [Full Text] |
| 18. | Vigier-Fretey CS, Granados-Santiago M, Raya-Benitez J, Zamora-Tortosa J, Heredia-Ciuro A, Valenza MC. Beliefs, Attitudes, Knowledge, and Behaviors of Physical Therapists Towards Differential Diagnosis in Chronic Neck Pain Etiology. Hospitals. 2025;2:7. [DOI] [Full Text] |
| 19. | Mesaroli G, Hundert A, Birnie KA, Campbell F, Stinson J. Screening and diagnostic tools for complex regional pain syndrome: a systematic review. Pain. 2021;162:1295-1304. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 29] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 20. | Harden NR, Bruehl S, Perez RSGM, Birklein F, Marinus J, Maihofner C, Lubenow T, Buvanendran A, Mackey S, Graciosa J, Mogilevski M, Ramsden C, Chont M, Vatine JJ. Validation of proposed diagnostic criteria (the "Budapest Criteria") for Complex Regional Pain Syndrome. Pain. 2010;150:268-274. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 977] [Cited by in RCA: 830] [Article Influence: 51.9] [Reference Citation Analysis (0)] |
| 21. | Mesaroli G, McLennan L, Friedrich Y, Stinson J, Sethna N, Logan D. Signs and symptoms of pediatric complex regional pain syndrome - type 1: A retrospective cohort study. Can J Pain. 2023;7:2179917. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 22. | Vetter TR, McGwin G Jr, Bridgewater CL, Madan-Swain A, Ascherman LI. Validation and clinical application of a biopsychosocial model of pain intensity and functional disability in patients with a pediatric chronic pain condition referred to a subspecialty clinic. Pain Res Treat. 2013;2013:143292. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 14] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 23. | Greenough MJ, Jibb L, Lewis KB, Bucknall T, Lamontagne C, Demery Varin M, Sokalski A, Squires JE. A systematic review of the biopsychosocial dimensions affected by chronic pain in children and adolescents: identifying reliable and valid pediatric multidimensional chronic pain assessment tools. Pain Rep. 2023;8:e1099. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 24. | Alexanders J, Anderson A, Henderson S. Musculoskeletal physiotherapists' use of psychological interventions: a systematic review of therapists' perceptions and practice. Physiotherapy. 2015;101:95-102. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 119] [Article Influence: 9.9] [Reference Citation Analysis (0)] |
| 25. | Wren AA, Ross AC, D'Souza G, Almgren C, Feinstein A, Marshall A, Golianu B. Multidisciplinary Pain Management for Pediatric Patients with Acute and Chronic Pain: A Foundational Treatment Approach When Prescribing Opioids. Children (Basel). 2019;6:33. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 58] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 26. | Katholi BR, Daghstani SS, Banez GA, Brady KK. Noninvasive treatments for pediatric complex regional pain syndrome: a focused review. PM R. 2014;6:926-933. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 14] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 27. | Broman J, Weigel C, Hellmundt L, Persson A. A descriptive study on the treatment of pediatric CRPS in the Nordic countries and Germany. Paediatr Neonatal Pain. 2021;3:163-169. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 28. | Birnie KA, Ouellette C, Do Amaral T, Stinson JN. Mapping the evidence and gaps of interventions for pediatric chronic pain to inform policy, research, and practice: A systematic review and quality assessment of systematic reviews. Can J Pain. 2020;4:129-148. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 30] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 29. | Althubaiti A. Information bias in health research: definition, pitfalls, and adjustment methods. J Multidiscip Healthc. 2016;9:211-217. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 875] [Cited by in RCA: 1943] [Article Influence: 194.3] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/