Published online Apr 18, 2026. doi: 10.5312/wjo.v17.i4.116107
Revised: November 7, 2025
Accepted: January 8, 2026
Published online: April 18, 2026
Processing time: 158 Days and 21.6 Hours
Iatrogenic ipsilateral femoral neck fractures are rare but significant complications associated with intramedullary nailing of femoral shaft fractures. These injuries may occur intraoperatively due to technical errors or be diagnosed postopera
To identify etiological factors contributing to iatrogenic femoral neck fractures during femoral shaft nailing and to propose a structured management algorithm for prevention and treatment.
A retrospective analysis was conducted on 1342 femoral interlocking nail procedures performed between 2017 and 2021. Eighteen cases (1.3%) of iatrogenic femoral neck fractures were identified. Clinical data, imaging findings, surgical techniques, and fixation methods were reviewed. Fractures were classified based on timing of diagnosis (intraoperative vs postoperative) and displacement status.
The most common causes included erroneous entry points (6 cases), inadvertent jig hammering (5 cases), misdirected nail manipulation (3 cases), and hoop stress-related fractures (3 cases). Fourteen fractures were diagnosed intraoperatively, while four were identified postoperatively. Fixation strategies included long proximal femoral nails (10 cases), cannulated cancellous screws (6 cases), and salvage techniques such as hemiarthroplasty (1 case). Delayed diagnosis correlated with increased operative time and poorer outcomes (P < 0.05), though union rates at 6 months and 12 months were statistically comparable across fixation methods.
Iatrogenic femoral neck fractures during femoral nailing are preventable with meticulous technique, appropriate implant selection, and vigilant intraoperative imaging. A standardized preoperative and intraoperative protocol can reduce incidence and improve outcomes.
Core Tip: Iatrogenic femoral neck fractures, though rare, are a notable complication during or after femoral shaft fixation with interlocking nails. This study highlights key technical errors-erroneous entry points, misdirected nail manipulation, and forceful jig hammering-as primary causes. Early recognition and adherence to surgical precision can prevent such fractures. Timely diagnosis and appropriate fracture management are essential to optimize patient outcomes and reduce postoperative morbidity.
- Citation: Nallakumarasamy A, Vetrivel VN, Balaji VP, Yadav R, Jeyaraman N, Muthu S, Jeyaraman M. Management and prevention of iatrogenic ipsilateral femoral neck fracture during intramedullary nailing of femoral shaft. World J Orthop 2026; 17(4): 116107
- URL: https://www.wjgnet.com/2218-5836/full/v17/i4/116107.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i4.116107
Intramedullary nailing is the most commonly employed surgical procedure for managing fractures of the femoral shaft in adults[1,2]. Nailing is a technically demanding technique that must be performed appropriately to prevent complications. An iatrogenic femoral neck fracture is a rare preventable complication following a femur interlocking nail procedure[3,4]. It can occur primarily due to improper surgical techniques, such as erroneous entry or hammering the awl while making the entry point, the improper introduction or manipulation of the nail, the inadequate reaming and or inadvertent hammering of the nail[5,6].
The other entity is the presence of a subclinical occult fracture that may get missed preoperatively; hence, it mandates preoperative computed tomography (CT) assessment in high-velocity double impact injuries or highly suspicious cases[7,8]. It may help us get informed consent to avoid medicolegal issues and effectively plan surgical management. The neck fracture and the avascular necrosis of the femoral head are the preventable devastating complications following the interlock nailing procedure[9-11]. Most of the iatrogenic neck fractures are diagnosed within the intraoperative period of operating femoral shaft fracture[12,13]. However, the inadequate intraoperative screening at the end of the surgery increases the incidence of delayed diagnosis of such fractures.
This study aims to systematically identify and classify the etiological factors contributing to iatrogenic ipsilateral femoral neck fractures during intramedullary nailing of femoral shaft fractures, and to evaluate their impact on surgical outcomes. Importantly, this study proposes a practical algorithm for early detection and tailored intervention, addressing a clinically underreported complication.
This retrospective study was conducted at a tertiary trauma center between January 2017 and December 2021, following institutional ethical committee approval (No. Dr. MGR-ERI/SLMCH/2025/005 dated March 5, 2025). The study aimed to identify the incidence, etiological factors, and management strategies for iatrogenic ipsilateral femoral neck fractures occurring during or after intramedullary nailing of femoral shaft fractures.
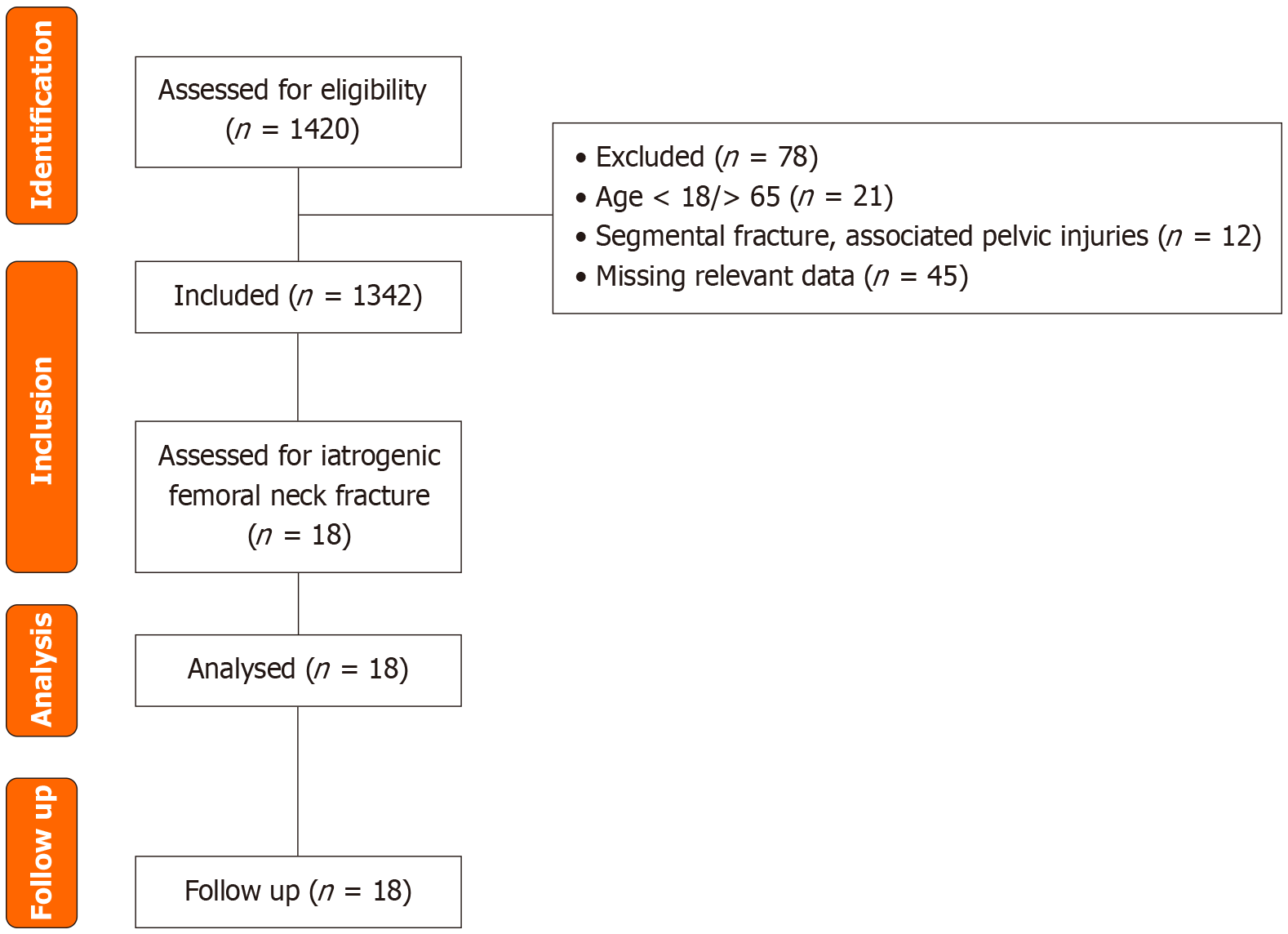
A total of 1342 adult patients who underwent closed antegrade intramedullary nailing for femoral shaft fractures were included. Inclusion criteria comprised skeletally mature individuals with isolated femoral shaft fractures treated with interlocking nails. Patients with pre-existing femoral neck fractures, pathological fractures, or polytrauma involving the pelvis or acetabulum were excluded. The flow of selection of patients in the study is given in Figure 1.
Clinical records, operative notes, and imaging archives were reviewed to identify cases of iatrogenic femoral neck fractures. Fractures were classified based on timing of diagnosis (intraoperative vs postoperative), displacement status (displaced vs undisplaced), and fixation method. Preoperative imaging included standard anteroposterior and lateral pelvic radiographs. In suspicious cases, additional fluoroscopic views or CT scans were performed to exclude occult neck fractures.
All procedures were performed on a fracture table under fluoroscopic guidance. The piriformis fossa was used as the standard entry point. Reaming was performed with incremental sizing, maintaining a 1.5 mm clearance over the intended nail diameter. Nail insertion was performed under controlled impaction, avoiding excessive force. Intraoperative imaging was used to confirm reduction and detect any proximal femoral complications.
Iatrogenic neck fractures were diagnosed either intraoperatively (via fluoroscopy) or postoperatively (via radiographs within six weeks). Etiological factors were categorized as: (1) Erroneous entry point; (2) Misdirected nail manipulation; (3) Inadvertent jig hammering; (4) Hoop stress-related fractures; and (5) Unexplained causes. Each case was reviewed for surgical technique, implant type, and intraoperative events.
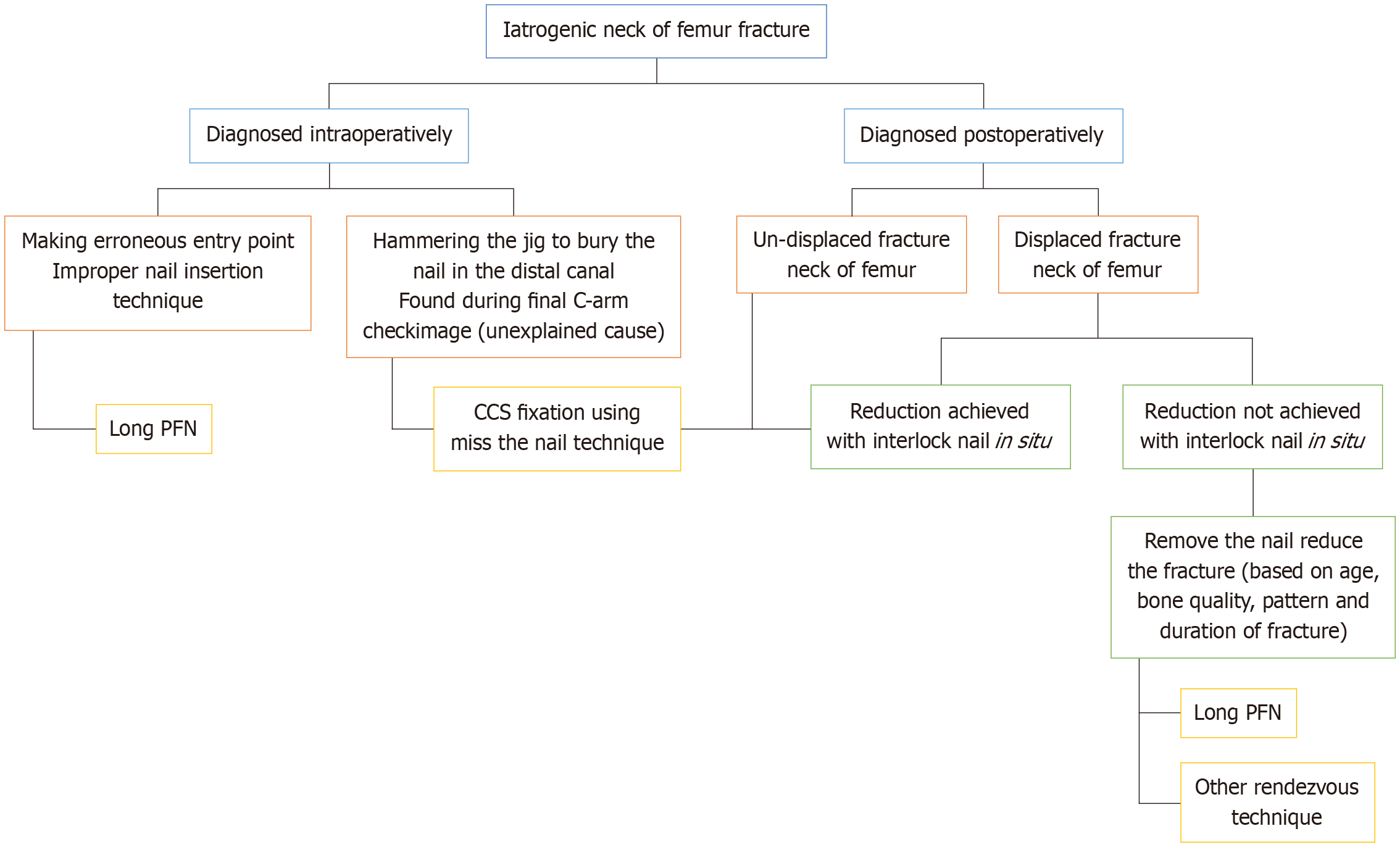
Fracture management was individualized based on displacement, timing of diagnosis, and implant status as illustrated in Figure 2. Undisplaced fractures diagnosed intraoperatively were managed with long proximal femoral nails. Displaced fractures diagnosed after nail insertion were treated using cannulated cancellous screws via the “miss-the-nail” technique. In select cases with poor bone quality or delayed diagnosis, salvage procedures such as hemiarthroplasty were employed. Postoperative follow-up included radiographic assessment at 6 weeks, 3 months, 6 months, and 12 months.
Descriptive statistics were used to summarize demographic and clinical variables. Statistical analysis was performed using descriptive and inferential methods to evaluate associations between fracture characteristics, timing of diagnosis, fixation strategies, and clinical outcomes. Categorical variables such as fracture etiology, displacement status, and fixation method were analyzed using the χ2 test, while Fisher’s exact test was applied when expected cell counts were below five to ensure validity in small sample comparisons. Continuous variables, including surgical duration, were assessed using independent samples t-tests to determine their impact on fracture union and complication rates. A P value of less than 0.05 was considered statistically significant.
Out of 1342 patients who underwent closed antegrade intramedullary nailing for femoral shaft fractures, 18 cases (1.3%) of iatrogenic ipsilateral femoral neck fractures were identified. The cohort included 14 males and 4 females, with a mean age of 41.6 years (range: 19-63 years). All patients had preoperative pelvic radiographs of acceptable diagnostic quality; however, none revealed a pre-existing femoral neck fracture. In six cases with high clinical suspicion, additional fluoroscopic views or preoperative CT scans were performed to exclude occult fractures.
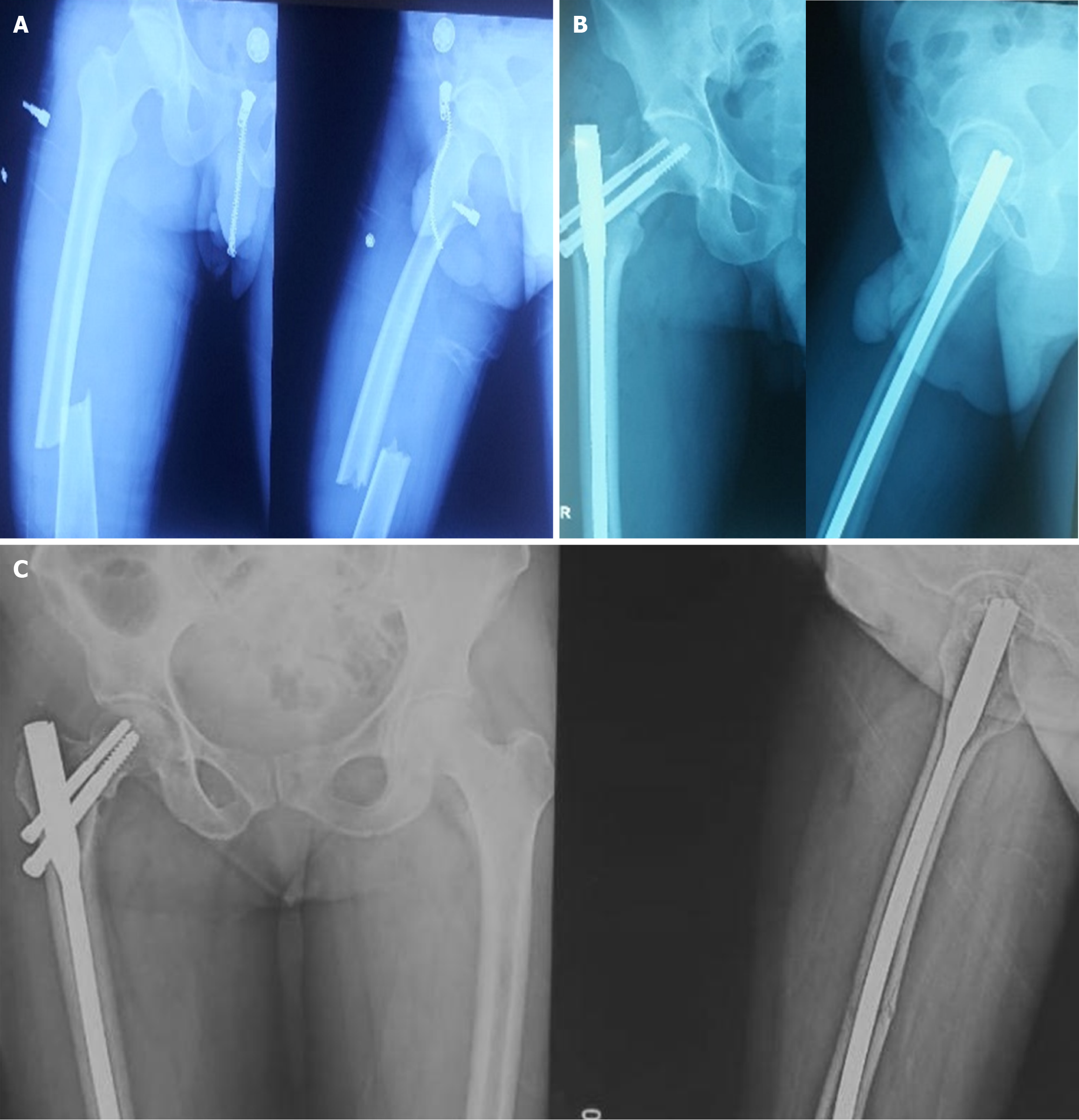
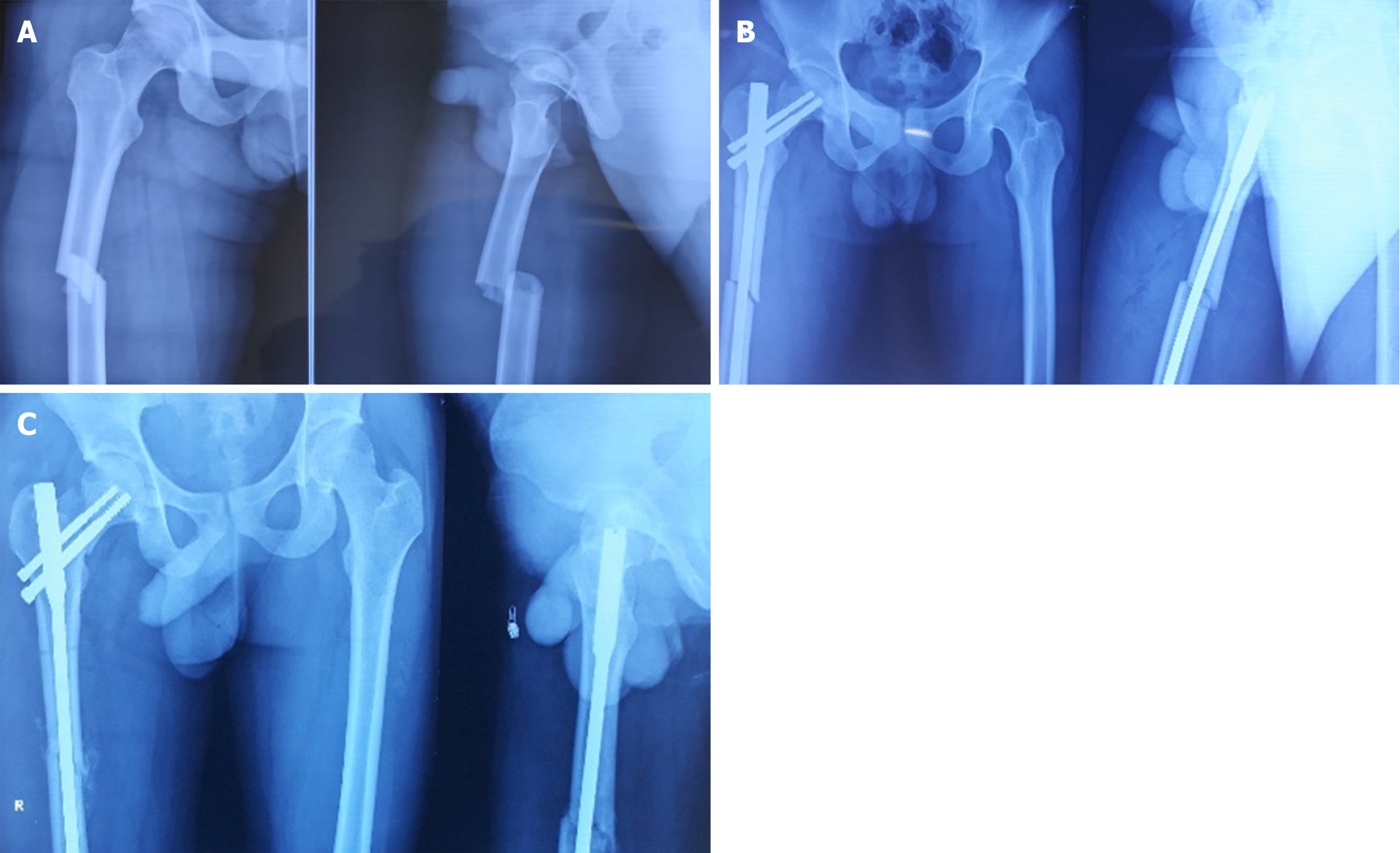
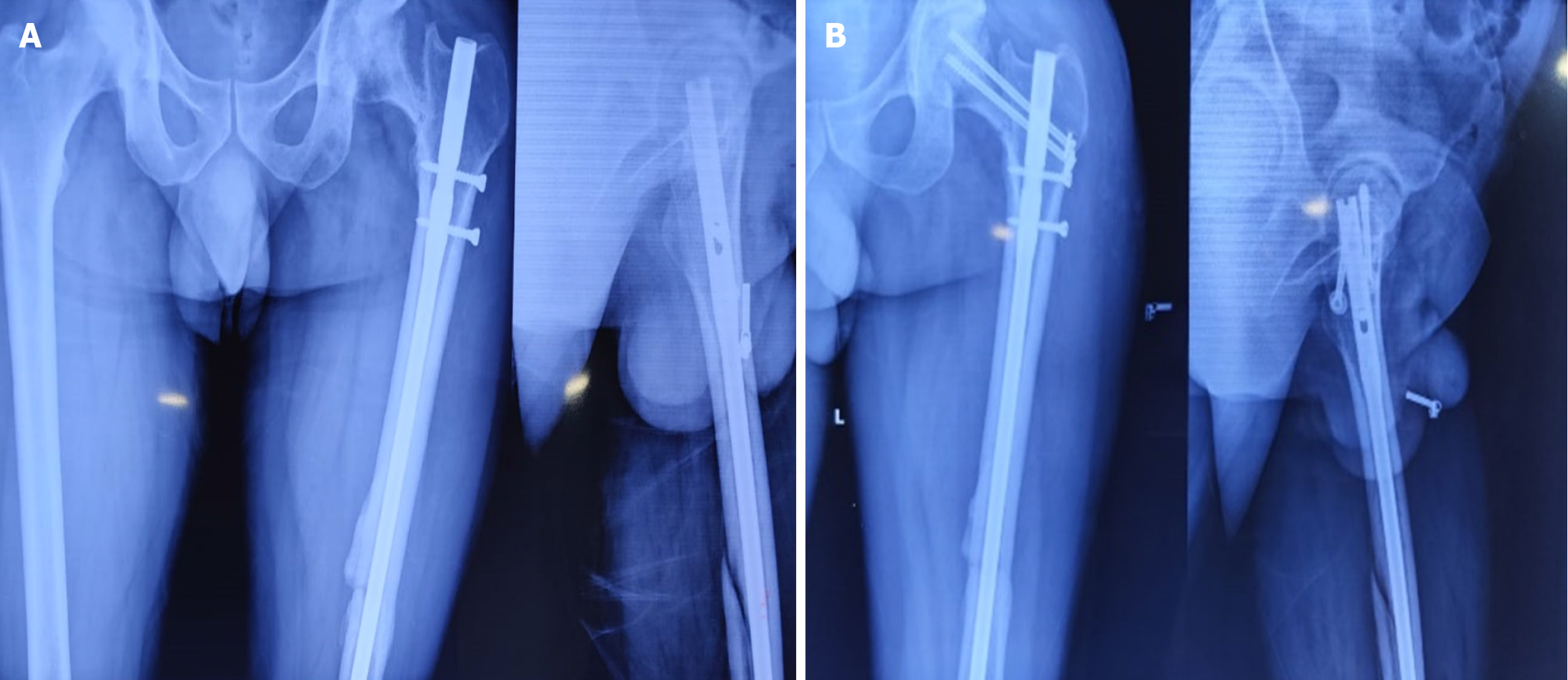
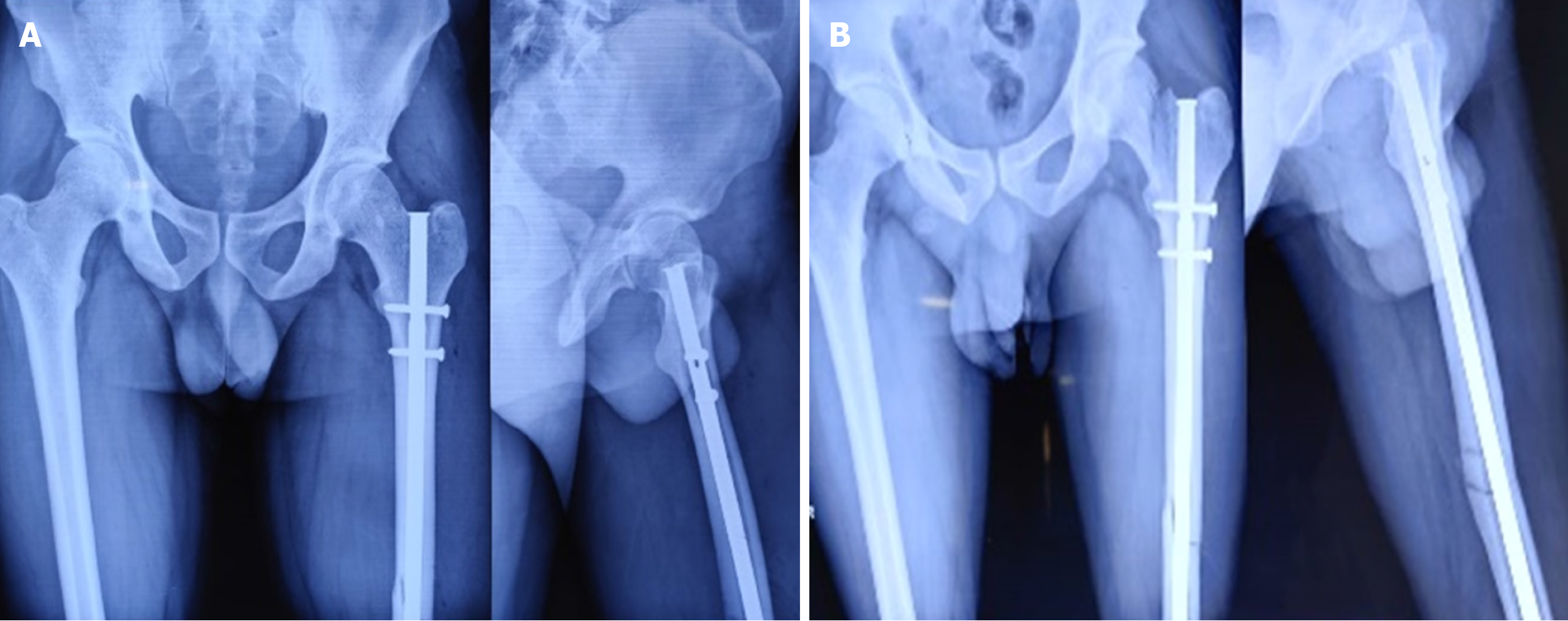
Fractures were diagnosed intraoperatively in 14 cases, immediately postoperatively in 1 case, and during follow-up (within 4 weeks) in 3 cases. The etiological breakdown included erroneous entry point (6 cases) as shown in Figure 3, inadvertent jig hammering (5 cases) as shown in Figure 4, misdirected nail manipulation (3 cases), hoop stress-related fractures (3 cases) as shown in Figure 5, and one case of unexplained origin. Intraoperative fractures were typically identified during final fluoroscopic checks, while postoperative fractures were detected on follow-up radiographs without intervening trauma Figure 6. The list of eitiologies contributing to iatrogenic fractures during femoral nailing is listed in Table 1.
| Etiology | Number of cases | Timing of diagnosis | Displacement status | Fixation method used |
| Erroneous entry point | 6 | Intraoperative | 4 undisplaced, 2 displaced | Long PFN (5), CCS (1) |
| Inadvertent jig hammering | 5 | Intraoperative | 3 undisplaced, 2 displaced | Long PFN (3), CCS (2) |
| Misdirected nail manipulation | 3 | Intraoperative | 2 undisplaced, 1 displaced | Long PFN (2), CCS (1) |
| Hoop stress-related fracture | 3 | Postoperative (≤ 4 weeks) | 1 undisplaced, 2 displaced | CCS (2), hemiarthroplasty (1) |
| Unexplained origin | 1 | Immediate postoperative | Displaced | CCS (1) |
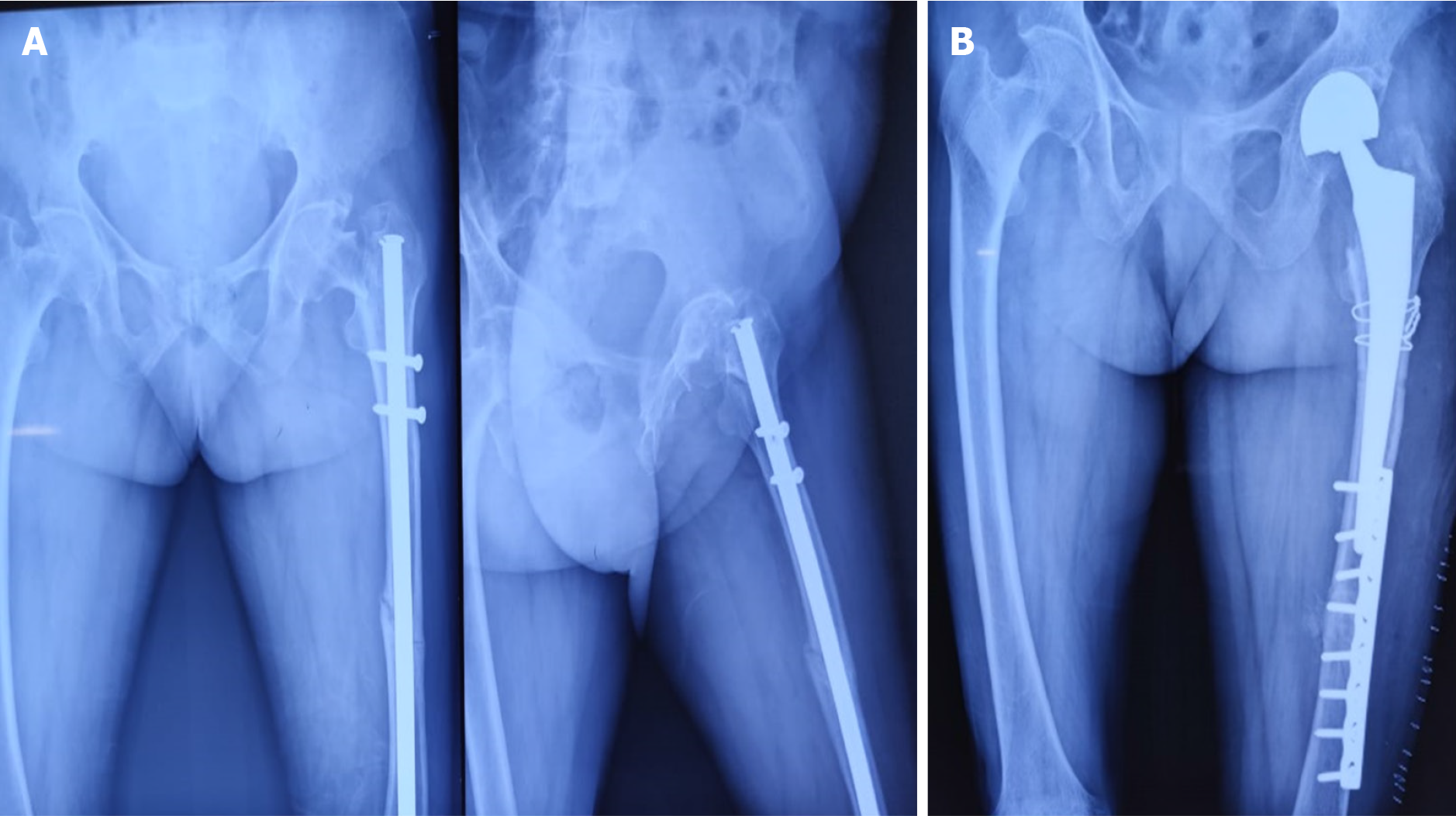
Among the 18 cases, 11 were undisplaced and 7 were displaced. Fixation methods included long proximal femoral nails (10 cases), cannulated cancellous screws (6 cases) as shown in Figure 6, bipolar hemiarthroplasty (1 case) as shown in Figure 7, and dual implant technique with limited contact dynamic compression plate (1 case) as shown in Figure 7. The “miss-the-nail” technique was employed in cases where the interlock nail remained in situ and removal was deemed risky due to potential displacement as shown in Figure 5 and Table 2.
| Timing of diagnosis | Number of cases | Common fixation method(s) | Mean surgical duration (minute) | Union achieved at 12 months |
| Intraoperative | 14 | Long PFN, CCS | 110 ± 15 | 12/14 (85.7) |
| Immediate post-operation | 1 | CCS | 125 | 1/1 (100) |
| Delayed post-operation (≤ 4 weeks) | 3 | CCS, hemiarthroplasty | 145 ± 20 | 1/3 (33.3) |
Immediate postoperative imaging confirmed stable fixation in 15 cases and unstable fixation in 3 cases. Radiographic union of both shaft and neck fractures was achieved in 14 cases by 12 months. Four cases showed delayed union or incomplete healing at the neck site, including one requiring salvage hemiarthroplasty due to poor bone quality and late diagnosis. The average neck-shaft angle was 125° ± 10°, with no significant difference between fixation groups (P = 0.342) as shown in Table 3.
| Fixation method | Number of cases | Displacement status | Union at 6 months | Union at 12 months | Complications observed |
| Long proximal femoral nail | 10 | 6 undisplaced, 4 displaced | 9/10 | 9/10 | 1 delayed union |
| Cannulated cancellous screws | 6 | 4 undisplaced, 2 displaced | 5/6 | 5/6 | 1 superficial infection |
| Hemiarthroplasty + plate | 1 | Displaced | NA | NA | No AVN, satisfactory function |
Union rates at 6 months and 12 months were not significantly associated with fracture etiology, timing of diagnosis, or fixation method (P > 0.05). However, delayed diagnosis and inappropriate implant selection were significantly associated with increased operative time and poorer functional outcomes (P < 0.05). The mean surgical duration was notably higher in cases requiring implant exchange or salvage procedures as shown in Table 4.
| Variable | P value | Interpretation |
| Timing of diagnosis vs union | > 0.05 | Not statistically significant |
| Fixation method vs union | > 0.05 | No significant difference in union rates |
| Surgical duration vs outcome | < 0.05 | Longer duration is associated with poorer outcomes |
| Displacement status vs AVN | NA | No AVN observed during follow-up |
No cases of avascular necrosis were documented during the follow-up period, although longer-term surveillance is warranted. One patient developed superficial wound infection, managed conservatively. The study highlighted that technical errors, particularly medialized entry points and forceful jig hammering, were preventable contributors to iatrogenic neck fractures. The use of intraoperative fluoroscopy and adherence to reaming protocols were critical in early detection and prevention.
The standard treatment for femoral shaft fractures is intramedullary interlocking nailing of the femur. The prevalence of ipsilateral shaft and neck fracture is about 2.5%-6% out of all femoral shaft fractures[14]. According to researchers, delayed diagnosis of this association ranges from 19% to 31%[15,16]. On the initial survey, these fractures are diagnosed using X-rays, but occult or undisplaced fractures may not be evident on X-rays. Hence, CT scan is needed to detect such fractures when there is strong suspicion. A femoral neck fracture while doing or after intramedullary nailing has been considered an iatrogenic complication, and it is rarely reported in the literature[3,17-19]. In our series, all cases had preop X-rays of good quality in both views and a new anteroposterior and axial view under fluoroscopy to rule out the presence of a femoral neck fracture.
The pioneer of femoral nailing, Gerhard Küntscher, warned about iatrogenic femoral neck fractures and recommended a lateral-based greater trochanter entry point[20]. Later, Winquist et al[21] described the piriformis fossa entry point for antegrade femoral nails. Subsequently, multiple authors have reported the potential for iatrogenic femoral neck fractures associated with a piriformis starting point, with a 1% incidence[4,22].
Harper and Henstorf[23] stated that iatrogenic neck fracture could be produced due to a misdirected introduction of the nail into the proximal canal, resulting in violation of the medial cortex of the femoral neck. Christie and Court-Brown[24] insist on the importance of avoiding an oblique insertion of the nail. The Kuntscher, Grosse-Kempf, and Russell-Taylor nails were of straight-line nail designs, so the optimal entry in these cases was the piriformis fossa. Also, the rigidity of these nails could be a contributing factor to this unusual complication. However, the nails with lateral bend should be inserted laterally or over the tip of the trochanter[25].
Tornetta et al[26] suggest a preoperative protocol that includes an anteroposterior internal rotation X-ray of the hip, a fine cut (2-mm) CT scan through the femoral neck, and an intraoperative fluoroscopic lateral view of the hip before the procedure. Further, an anteroposterior and lateral X-ray of the hip should be obtained after proximal interlocking screw fixation before shifting from the fracture table. At follow-up, anteroposterior and lateral radiographs should be done, and the patient should be clinically assessed about hip pain with any concerning findings or suspicious in X-ray; the patient is subjected to repeat computed tomography. The results of the study appear to be promising, with improved sensitivity and a significant reduction in delay of diagnosis by more than 90%.
The iatrogenic neck fracture diagnosed before the complete insertion of interlock nail should be managed with long proximal femoral nail[4]. However, once the interlock nail has been fully inserted, the diagnosed neck fracture should be fixed as early as possible using the cannulated cancellous screw since removing the nail may displace the neck fracture and increase the risk of avascular necrosis of the head. Also, the use of the long proximal femoral nail in this scenario may results in significant malreduction of the neck fracture[27]. It has been found that postoperatively diagnosed iatrogenic neck femur fracture can be managed effectively with cannulated cancellous screws but delay in such diagnosis adversely affect the outcome[6,27]. Doing proximal femur nailing in such cases increases the operative time, blood loss, infection rate and may also disturb the primary shaft fracture union while removing the interlocking nail. We must consider the various options of rendezvous dual implanting techniques based upon the fracture pattern, the time elapsed since fracture, and patient risk factors[22].
The preventive measures include making an appropriate entry point with the bone awl under C-arm guidance, which should be confirmed in both views. The internal rotation of the proximal fragment using Steinmann pin visualizes the entire neck morphology and the entry site clearly. The awl should be advanced with rotatory movement, trajected towards the medullary canal without hammering it. The reamer size should be increased consecutively with an increasing trend of 0.5 mm size, and it should start with a minimal size of 8 mm. The entire medullary canal should be reamed with a size of 1.5 mm, more incredible than that of the desired nail size. The nail should be inserted only after adequate reduction and appropriate reaming; the manipulation with the nail to achieve the reduction should be avoided. If hammering is needed, the nail must be advanced 1-1.5 cm into the canal on each impaction with the hammer. During hammering, the degree of the nail advancing should be monitored. If it is not advancing, one should check the reamer size or decrease the nail diameter of the next lesser size, and it should be alternating with rotating the jig 180°, thereby reducing the stress at the nail-bone interface at the entry site. Proximal part of the femur should be reamed with the appropriate size reamer, which depends on the thickness of the proximal part of the nail. This appropriate reaming will avoid the hammering process and prevent nail hoop stress.
This study has several limitations inherent to its retrospective and descriptive design. First, the relatively small number of iatrogenic femoral neck fracture cases (n = 18) limits the statistical power to detect significant associations between specific etiological factors and clinical outcomes. Second, the absence of a control group precludes comparative analysis with patients who underwent uneventful femoral nailing, thereby restricting causal inference. Third, the classification of fracture mechanisms was based on intraoperative documentation and postoperative imaging, which may be subject to reporting bias or interobserver variability. Additionally, the study did not employ a standardized radiological protocol across all cases, and the use of preoperative CT was selective rather than routine, potentially underestimating the incidence of occult pre-existing neck fractures. Finally, the follow-up duration was insufficient to assess long-term complications such as avascular necrosis of the femoral head. Future prospective studies with larger cohorts, uniform imaging protocols, and extended follow-up are warranted to validate these findings and refine preventive strategies.
Iatrogenic ipsilateral femoral neck fractures during intramedullary nailing of femoral shaft fractures, though uncommon, represent a preventable surgical complication with significant implications for patient outcomes. This study highlights key technical errors, medialized entry points, misdirected nail manipulation, and forceful jig hammering, as primary contributors. Early intraoperative recognition, adherence to precise surgical technique, and appropriate implant selection are critical to minimizing risk. The proposed management algorithm offers a structured approach to timely diagnosis and tailored fixation strategies, including the use of long proximal femoral nails and “miss-the-nail” screw techniques. While union rates were not significantly affected by fracture etiology or timing of diagnosis, delayed recognition was associated with increased operative time and complexity. Preoperative imaging protocols, intraoperative fluoroscopic vigilance, and postoperative radiographic scrutiny should be integral to femoral nailing workflows. Ultimately, heightened awareness and surgical discipline, especially among early-career surgeons, can reduce iatrogenic morbidity and improve the safety profile of femoral shaft fracture fixation.
| 1. | Ryan-Coker MFD, Batura R, Kubai H, Forde MYE, Perdomo-Lizarraga JC, Marenah K, Haghparast-Bidgoli H. Outcomes of intramedullary nailing for traumatic adult femoral shaft fractures in low-and-middle-income countries; a systematic review. OTA Int. 2025;8:e434. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 2. | Rodrigues FL, Ferrari ALM, Faria FF, Pinto RLE, Lopes MF, Santos MEA, Varela EC, Filho MJL, Cecyn MN, Oliveira NHC. Intramedullary Nailing in Femoral Diaphyseal Fractures: A Retrospective Multicenter Cohort Study. Life (Basel). 2025;15:540. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 3. | Castellanos J, Garcia-Nuño L, Cavanilles-Walker JM, Roca J. Iatrogenic femoral neck fracture during closed nailing of the femoral shaft fracture. Eur J Trauma Emerg Surg. 2009;35:479-481. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 4. | Wang JH, Chuang HC, Su WR, Chang WL, Kuan FC, Hong CK, Hsu KL. The characteristics and influence of iatrogenic fracture comminution following antegrade interlocking nailing for simple femoral shaft fractures, a retrospective cohort study. BMC Musculoskelet Disord. 2022;23:456. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 5. | Joo YB, Jeon YS, Lee WY, Chung HJ. Risk Factors Associated with Intraoperative Iatrogenic Fracture in Patients Undergoing Intramedullary Nailing for Atypical Femoral Fractures with Marked Anterior and Lateral Bowing. Medicina (Kaunas). 2023;59:735. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 6. | Apivatthakakul T, Arpornchayanon O. Iatrogenic femoral neck fracture caused by mal-insertion of a curved intramedullary nail. Injury. 2001;32:727-729. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 7. | Lucenti L, Sodano A, Panvini FMC, Vescio A, Papotto G, Testa G, Pavone V. Does Preoperative CT Improve Outcomes in Femoral Neck Fracture Fixation? A Retrospective Study. J Clin Med. 2025;14:5917. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 8. | Park YC, Um KS, Hong SP, Oh CW, Kim S, Yang KH. Preoperative "Computed tomography capsular sign" for the detection of occult ipsilateral femoral neck fractures associated with femoral shaft fractures. Injury. 2020;51:1051-1056. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 11] [Article Influence: 1.8] [Reference Citation Analysis (1)] |
| 9. | Gomaa HR, Buanq AA, Hazeem AM, Daoud SM, Almajed AH. Avascular Necrosis of the Femoral Head Following Intramedullary Nailing of a Femoral Shaft Fracture in a Skeletally Mature Adult: A Case Report. Cureus. 2024;16:e53357. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 10. | Tsarouhas A, Hantes ME, Karachalios T, Bargiotas K, Malizos KN. Reconstruction nailing for ipsilateral femoral neck and shaft fractures. Strategies Trauma Limb Reconstr. 2011;6:69-75. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 12] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 11. | Labza S, Fassola I, Kunz B, Ertel W, Krasnici S. Delayed recognition of an ipsilateral femoral neck and shaft fracture leading to preventable subsequent complications: a case report. Patient Saf Surg. 2017;11:20. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 6] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 12. | Khan FA, Ikram MA, Badr AA, al-Khawashki H. Femoral neck fracture: a complication of femoral nailing. Injury. 1995;26:319-321. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 26] [Article Influence: 0.8] [Reference Citation Analysis (3)] |
| 13. | Klima ML. Mechanical Complications After Intramedullary Fixation of Extracapsular Hip Fractures. J Am Acad Orthop Surg. 2022;30:e1550-e1562. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 24] [Reference Citation Analysis (1)] |
| 14. | Watson JT, Moed BR. Ipsilateral femoral neck and shaft fractures: complications and their treatment. Clin Orthop Relat Res. 2002;78-86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 70] [Article Influence: 2.9] [Reference Citation Analysis (1)] |
| 15. | Wolinsky PR, Johnson KD. Ipsilateral femoral neck and shaft fractures. Clin Orthop Relat Res. 1995;81-90. [PubMed] |
| 16. | Singh R, Rohilla R, Magu NK, Siwach R, Kadian V, Sangwan SS. Ipsilateral femoral neck and shaft fractures: a retrospective analysis of two treatment methods. J Orthop Traumatol. 2008;9:141-147. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 31] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 17. | Grala P, Mańkowski B, Kierzynka G. Femoral neck fracture following intramedullary nailing with misplacement of an end cup: report of two cases. J Orthop Traumatol. 2009;10:35-38. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 18. | Papadakis SA, Zalavras C, Mirzayan R, Shepherd L. Undetected iatrogenic lesions of the anterior femoral shaft during intramedullary nailing: a cadaveric study. J Orthop Surg Res. 2008;3:30. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 2] [Article Influence: 0.1] [Reference Citation Analysis (1)] |
| 19. | Hsu KL, Kuan FC, Chang WL, Liu YF, Hong CK, Yeh ML, Su WR. Interlocking nailing of femoral shaft fractures with an extremely narrow medullary canal is associated with iatrogenic fractures. Injury. 2019;50:2306-2311. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 20. | Bick EM. The intramedullary Nailing of Fractures by G. Küntscher. Translation of article in Archiv für Klinische Chirurgie, 200:443, 1940. Clin Orthop Relat Res. 1968;60:5-12. [PubMed] |
| 21. | Winquist RA, Hansen ST Jr, Clawson DK. Closed intramedullary nailing of femoral fractures. A report of five hundred and twenty cases. J Bone Joint Surg Am. 1984;66:529-539. [PubMed] |
| 22. | McDonald LS, Tepolt F, Leonardelli D, Hammerberg EM, Stahel PF. A cascade of preventable complications following a missed femoral neck fracture after antegrade femoral nailing. Patient Saf Surg. 2013;7:16. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 17] [Article Influence: 1.3] [Reference Citation Analysis (1)] |
| 23. | Harper MC, Henstorf J. Fractures of the femoral neck associated with technical errors in closed intramedullary nailing of the femur. Report of two cases. J Bone Joint Surg Am. 1986;68:624-626. [PubMed] |
| 24. | Christie J, Court-Brown C. Femoral neck fracture during closed medullary nailing: brief report. J Bone Joint Surg Br. 1988;70:670. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 26] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 25. | Bharti DS, Goyal DN, Chavan DR. Trochanteric entry VS piriformis entry in case of antegrade nailing of femoral shaft fracture treatment: A prospective randomised comparative study. Int J Orthop Sci. 2019;5:1016-1022. [DOI] [Full Text] |
| 26. | Tornetta P 3rd, Kain MS, Creevy WR. Diagnosis of femoral neck fractures in patients with a femoral shaft fracture. Improvement with a standard protocol. J Bone Joint Surg Am. 2007;89:39-43. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 45] [Article Influence: 2.4] [Reference Citation Analysis (1)] |
| 27. | Bedi A, Karunakar MA, Caron T, Sanders RW, Haidukewych GJ. Accuracy of reduction of ipsilateral femoral neck and shaft fractures--an analysis of various internal fixation strategies. J Orthop Trauma. 2009;23:249-253. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 37] [Article Influence: 2.2] [Reference Citation Analysis (1)] |