Published online Apr 18, 2026. doi: 10.5312/wjo.v17.i4.116076
Revised: November 19, 2025
Accepted: January 28, 2026
Published online: April 18, 2026
Processing time: 159 Days and 22.6 Hours
Tibial plateau fractures (TPFs), although comprising only 1% of all fractures, pose significant diagnostic and management challenges due to their frequent as
To evaluate the diagnostic accuracy of preoperative quantitative CT parameters in predicting meniscal and cruciate ligament injuries associated with TPFs.
A systematic review was conducted per the PRISMA guidelines. Two databases (PubMed and Scopus) were searched up to October 2024. Studies were included if they involved skeletally mature patients with TPFs, reported at least one CT parameter predictive of soft tissue injury, and used arthroscopy or open surgery as the diagnostic gold standard. A risk of bias assessment was conducted using the Quality Assessment of Diagnostic Accuracy Studies 2 tool, and meta-analyses were performed where appropriate, using the random-effects model.
Lateral plateau depression (LPD) and lateral plateau widening (LPW) were the most commonly assessed parameters. Pooled analysis revealed that LPD and LPW were significantly higher in patients with lateral meniscus injuries (mean difference, 5.23 mm and 1.37 mm, respectively; P < 0.00001 and P = 0.02). No significant associations were found for medial plateau depression or LPD with medial meniscus or posterior cruciate ligament injuries. Lateral area of depression and LPW were reported in a single study to be predictive of anterior cruciate ligament injuries.
Preoperative CT parameters, particularly LPD and LPW, provide a strong predictive value for lateral meniscus injuries in TPFs, potentially aiding in early diagnosis and management. However, their utility in predicting cruciate or medial meniscus injuries remains limited. CT scan remains a valuable first-line tool, especially where magnetic resonance imaging is inaccessible, and can guide further investigation or intraoperative planning.
Core Tip: Although magnetic resonance imaging remains the gold standard for detecting meniscal and ligamentous injuries, it may not always be available in the acute trauma setting. This systematic review examined the predictive value of pre
- Citation: Hassan AAA, Khalifa AA, Villalon AR, Hauri D, Zhu TY. Predictive value of preoperative computed tomography parameters for meniscal and cruciate ligament injuries in tibial plateau fractures: Meta-analysis. World J Orthop 2026; 17(4): 116076
- URL: https://www.wjgnet.com/2218-5836/full/v17/i4/116076.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i4.116076
Although tibial plateau fractures (TPFs) comprise only 1% of all fractures, they are considered one of the most challenging fractures to manage[1]. In contrast to other fractures, the main challenge lies in achieving an anatomical reduction and stable fixation, while addressing associated soft-tissue injuries and impaired knee function[2]. Concomitant meniscal and cruciate ligamentous injuries are very commonly encountered in the context of TPFs, with an overall incidence of 22.5% to 99% and 16.7% to 57%, respectively[3,4].
As the orthopaedic practice continues to evolve, it has become clear that, in addition to restoring articular surface and leg alignment, identifying and managing associated meniscal and ligamentous injuries are the linchpin to a good clinical outcome[5-7]. Leaving these injuries unaddressed leads to the development of early post-traumatic osteoarthritis as a result of increased contact stress of the knee joint and impaired stability[8].
Pre-operative identification of these injuries can be performed via either radiological or clinical examination. Clinical examinations rely on symptoms of pain, swelling, and limited range of motion at the time of injury and are subject to the levels of personal skills and experience. Therefore, the main burden of their diagnosis lies in radiological examination[9].
Several studies have reported that soft tissue injuries occur more frequently with increasing tibial plateau displacement, which can be evaluated on computed tomography (CT) scan images using lateral plateau depression (LPD) and lateral plateau widening (LPW) measurements[9-13].
Gardner et al[14] attempted to predict soft-tissue injuries by measuring LPD on plain radiographs. Still, these studies were later refuted because these measures cannot be reliably performed on plain radiographs due to the normal tibial slope, leading to underestimation of the measurements compared with CT scans[11,15].
On the other hand, magnetic resonance imaging (MRI) has unique advantages in diagnosing meniscus and ligamentous injuries of the knee joint[16]. However, due to the high costs, lengthy examination time, and difficulties with appointment scheduling, MRI is still not widely used as the first-line imaging modality for evaluating these injuries, especially in non-tertiary hospitals[10].
Thus, nowadays, preoperative X-ray and CT examinations are still the primary imaging tools for the majority of patients with TPFs. Although access to MRI is more limited than CT scan, most surgeons still consider MRI as the only acceptable imaging modality for the assessment of meniscal and ligamentous injuries associated with TPFs.
By far, there is no consensus on the use of quantitative CT scan parameters for diagnosing soft-tissue injuries associated with TPFs. Given this, we aimed to systematically review the available evidence on the accuracy of different preoperative quantitative CT parameters in evaluating these soft tissue injuries (meniscus and cruciate ligaments in particular) to enhance diagnostic and management decisions.
This systematic review and meta-analysis were conducted within the Cochrane Back and Neck Group framework[17], and reported according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines[18]. The protocol was registered in PROSPERO (CRD42022316270).
We included all types of study designs (published in English), except for case reports and review articles that fulfilled all following criteria: (1) Reporting on TPFs in skeletally mature patients (older than 18 years old); (2) At least one quantitative CT parameter to diagnose meniscal or ligamentous injuries was reported; and (3) Arthroscopy or open surgery was used as the reference procedure to diagnose such injuries. Cadaveric or animal studies and those reported on pathological fractures were excluded.
Two databases were used for an electronic search, namely PubMed and Scopus libraries, using both controlled vocabularies and free-texts, and the search was performed from databases inception till October 2024: For PubMed (((Tibial Fractures/diagnostic imaging[mh]) OR (tibial plateau fracture)) AND (((CT[tw]) OR (Tomography, X-Ray Computed[mh])) OR (computed tomography))) AND (((((((((ligament*[tw]) OR (menisc*[tw])) OR (Tibial Meniscus Injuries/diagnosis[mh])) OR (Anterior Cruciate Ligament[mh])) OR (Anterior Cruciate Ligament Injuries[mh])) OR (Collateral Ligaments[mh])) OR (Soft Tissue Injuries/diagnosis[mh])) OR (posterior cruciate ligament[mh])) OR (meniscus[mh])); for Scopus: (“tibial plateau” AND fractur*) AND (CT AND scan OR CT OR comput* AND tomography) AND (menisc* AND injur* OR ligamnet* AND injur*). Furthermore, we performed backward and forward snowballing of the articles that were finally included to retrieve as many relevant studies as possible. (The search was repeated before the final data analysis on September 10, 2024 to capture any published studies after the original search was performed).
All search results were combined, and duplicates were removed using EndNote X9®. Two authors independently screened and selected articles against the inclusion and exclusion criteria. The initial screening involved the titles and abstracts of the identified articles. In case of disagreement between the two reviewers, the article was included in the full-text assessment.
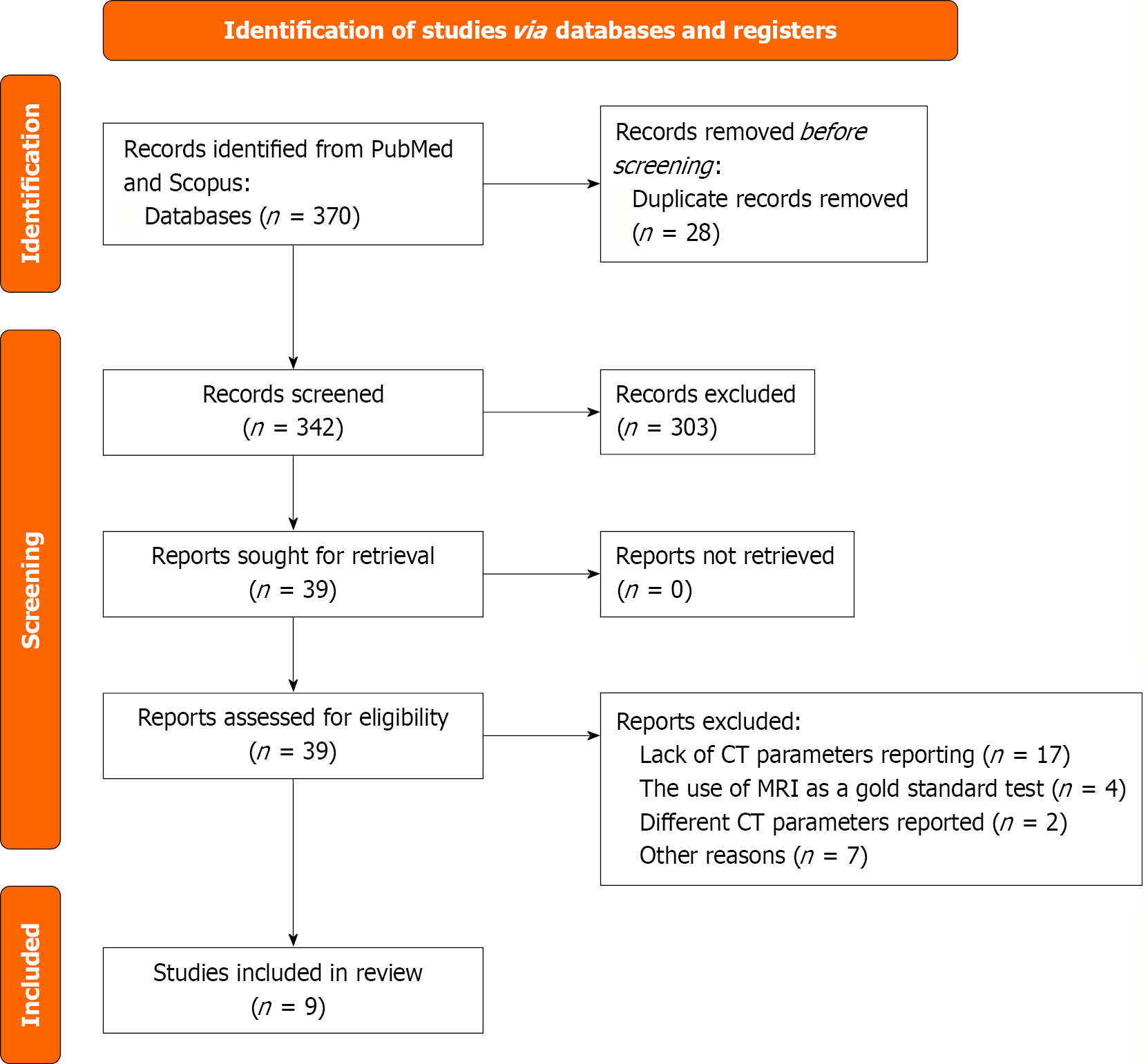
For the provisionally included articles, full texts were obtained and assessed. In the event of disagreement between the two reviewers during the full-text assessment, the article was reassessed by a third author, who made the final decision. The articles that were finally included were forward and backward snowballed by two authors to identify any additional eligible articles. The number of articles identified, included, and excluded at each step of the screening, along with the reasons for exclusions, was presented according to the PRISMA flowchart (Figure 1).
Two authors performed data extraction independently into an Excel spreadsheet, where the following data were extracted: Study characteristics (authors, country of origin, type of study, and year of publication), patient characteristics (basic demographic information and fracture-related information such as fracture classification and associated soft tissue injuries), details of the assessment protocols (including the CT scan parameters and the reference assessment tools for example, arthroscopy). In cases of discrepancies, these were either resolved through discussion between the two authors, or a third author was consulted.
The following were the variables assessed in CT scans: LPD and medial plateau depression (MPD): Measured as the maximum amount of articular depression calculated from the intact plateau line (parallel to the femoral condyles) to the lowest point of the depressed subchondral bone[3]. LPW and medial plateau widening (MPW): Using the femoral condyle as a reference, it was measured as the distance between the tangential line to the respective femoral epicondyle (perpendicular to the femoral condyles) and the most displaced point of the tibial plateau[3]. Lateral area of depression (LAD) and medial area of depression: These were calculated on the CT scan coronal reformatted images; the area of depression could be located anteriorly or posteriorly; the appropriate section could be easily identified to calculate the depression area using the freehand region of interest tool[3].
The risk of bias of the included studies was assessed independently by two authors using the Quality Assessment of Diagnostic Accuracy Studies-2 tool. The Quality Assessment of Diagnostic Accuracy Studies-2 tool is recommended for use in systematic reviews of diagnostic accuracy by the Agency for Healthcare Research and Quality, Cochrane Collaboration, and the National Institute for Health and Clinical Excellence[19].
A synthesis of qualitative and quantitative results was performed when feasible. The qualitative data synthesis involved tabulating the data extracted from the included articles to summarize studies and patient characteristics, assessment parameters, assess soft tissue structures, and risk of bias results. If two or more articles reported the same outcomes and were similarly analyzed, a quantitative synthesis (meta-analysis) was conducted. The calculated effect sizes were visualized in forest plots using the random effect model.
The data were checked for heterogeneity using the I2 statistic; furthermore, a leave-one-out sensitivity analysis was planned to assess the influence of individual studies on outcomes with substantial heterogeneity. RevMan 5.4® was used for statistical analysis. Publication bias was evaluated using an Egger’s regression test and visual inspection of a funnel plot. The significance level was considered if the P < 0.05.
The initial search yielded 370 eligible articles, of which nine were included (seven case series and two cohort studies)[3,8,10,12,13,20-23]. The PRISMA flow chart shows the search strategy and article selection process (Figure 1).
The nine studies included 883 patients (909 fractures) with an average age of 46.72 years (ranging from 52.4 years to 43.9 years), comprising 60.6% males and 39.4% females (Table 1). The most commonly included fracture was type II (58.97%). The assessed soft tissue injuries were only lateral meniscus (LM) in six studies[8,10,13,20-22], LM and medial meniscus (MM) in one study[12], LM, MM, and posterior cruciate ligament (PCL) in one study[23], and LM, MM, PCL, and anterior cruciate ligament in one study[3].
| Ref. | Country | Type of study | Number of patients | Sex (male/female) | Age, mean ± SD (range) | Fracture classification (according to Schatzker classification) | Studied structures | Reported CT parameters | Reference procedure |
| Chang et al[3], 2018 | China | Prospective | 100 | 77/23 | 44.6 ± 13.28 (18 to 72) | 4 type I, 33 type II, 12 type III, 20 type IV, 18 type V and 15 type VI | LM, MM, ACL, and PCL | LPD, LPW, MPD, MPW, LAD and MAD | Arthroscopy (performed after fracture fixation) |
| Salari et al[20], 2021 | United States | Retrospective | 70 | 49/21 | 45.1 ± 12.9 | 12 type I and 58 type II | LM | LPD | Sub-meniscal arthrotomy |
| Jain et al[12], 2020 | United Kingdom | Retrospective | 88 | 58/30 | 45.25 ± 16.5 | 1 type I, 50 type II, 19 type IV, and 18 type VI | LM and MM | LPD and LPW | Open surgery |
| Kim et al[21], 2022 | South Korea | Retrospective | 42 | 26/16 | 47.2 ± 9.6 (17 to 63) | 39 type II and 3 type III | LM | LPD | Arthroscopy (the authors performed ARIF) |
| Liu et al[22], 2023 | China | Retrospective | 60 | 35/25 | Injured: 45.8 ± 18.2; intact: 44.5 ± 16.5 | 60 type IV | LM | LPD and LPW | Open surgery |
| Pu et al[10], 2022 | China | Prospective | 296 | 174/122 | 44.9 ± 15.6; injured: 46.0 ± 16.0; intact: 43.8 ± 15.2 | 296 type II | LM | LPD and LPW | They performed both open surgery evaluation (mainly for the anterior horn and body of the LM) and arthroscopic assessment of the remaining soft tissue structures |
| Ringus et al[13], 2010 | United States | Retrospective | 85 | 50/35 | 45.0 ± 17.6 (8 to 85); injured: 40.9 ± 15.1 (20 to75); intact: 46.9 ± 18.5 (18 to 85) | 2 type I, 21 type II, 9 type III, 1 type IV, 35 type V and 16 type VI | LM | LPD | Open surgery |
| Tang et al[8], 2017 | Taiwan | Retrospective | 132 | 60/72 | 45.7 ± 13.1 (18 to 75) | 4 type I, 25 type II, 20 type III, 8 type IV, 52 type V and 23 type VI | LM | LPD and LPW | Arthroscopy (the authors performed ARIF |
| Thamyongkit et al[23], 2018 | Thailand | Prospective | 10 | 6/4 | 52.4 ± 12.5 (35 to 80) | 1 type I, 1 type II, 3 type IV, 2 type V and 3 type VI | LM, MM, and PCL | LPD, LPW, MPD and MPW | Arthroscopy |
The primary source of bias in most studies (6 out of 9) was in the patient selection domain, as the studies did not show consecutive patient selection[10,13,20-23] (Table 2). Additionally, there was no clear temporal relationship between the time of trauma and the time of surgical/arthroscopic intervention. However, all the studies demonstrated good applicability in patient selection, the index procedure, and the reference method used.
| Ref. | Risk of Bias | Applicability | |||||
| Patient selection | Index test | Reference standard | Flow and timing | Patient selection | Index test | Reference standard | |
| Chang et al[3], 2018 | Low | Low | Low | Unclear | Low | Low | Low |
| Salari et al[20], 2021 | High | Low | Low | Unclear | Low | Low | Low |
| Jain et al[12], 2020 | Low | Low | Low | Unclear | Low | Low | Low |
| Liu et al[22], 2023 | High | Low | Low | Low | Low | Low | Low |
| Ringus et al[13], 2010 | High | Low | Low | Unclear | Low | Low | Low |
| Kim et al[21], 2022 | High | Low | Low | Unclear | Low | Low | Low |
| Thamyongkit et al[23], 2018 | High | Unclear | Unclear | Unclear | Low | Low | Low |
| Pu et al[10], 2022 | High | Low | Low | Unclear | Low | Low | Low |
| Tang et al[8], 2017 | Unclear | Low | Low | High | Low | Low | Low |
The following CT parameters were evaluated: LPD and LPW in four studies[8,10,12,22], only LPD in three[13,20,21], LPD, LPW, MPD, MPW, LAD and medial area of depression in one[3], and LPD, LPW, MPD and MPW in one[23]. In all studies, the authors reported the details of CT parameter values for knees with injured and intact soft tissue structures. However, in the studies by Jain et al[12] and Kim et al[21], the authors did not separately report the measurements for the injured and non-injured soft tissue structures. The details are reported in Table 3.
| Ref. | LM | MM | ACL | PCL | ||||
| Injured | Intact | Injured | Intact | Injured | Intact | Injured | Intact | |
| Chang et al[3], 2018 | LPW: 7 ± 7.4 mm; LPD: 11 ± 7.9 mm; LAD: 433.7 ± 229.1 mm2; MPW: 0.1 ± 0.8 mm; MPD: 0.3 ± 1.5 mm; MAD: 9.9 ± 61 mm2 | LPW: 4.6 ± 4.3 mm; LPD: 6 ± 6.3 mm; LAD: 258.6 ± 250.9 mm2; MPW: 0.2 ± 1 mm; MPD: 0.4 ± 1.5 mm; MAD: 20.5 ± 83.7 mm2 | LPW: 5.9 ± 6.8 mm; LPD: 5.9 ± 6.8 mm; LAD: 366.8 ± 289 mm2; MPW: 0.4 ± 1.5 mm; MPD: 0.7 ± 1.8 mm; MAD: 15.4 ± 77.5 mm2 | LPW: 5.1 ± 4.7 mm; LPD: 8.8 ± 7.6 mm; LAD: 203 ± 242.2 mm2; MPW: 0.1 ± 0.7 mm; MPD: 0.3 ± 1.4 mm; MAD: 15.7 ± 46.1 mm2 | LPW: 5.9 ± 6.8 mm; LPD: 5.9 ± 6.8 mm; LAD: 203 ± 242.2 mm2; MPW: 0.4 ± 1.5 mm; MPD: 0.7 ± 1.8 mm; MAD: 15.7 ± 46.1 mm2 | LPW: 5.1 ± 4.7 mm; LPD: 8.8 ± 7.6 mm; LAD: 366.8 ± 289 mm2; MPW: 0.1 ± 0.7 mm; MPD: 0.3 ± 1.4 mm; MAD: 15.4 ± 77.5 mm2 | LPW: 4.7 ± 4.1 mm; LPD: 8 ± 9.8 mm; LAD: 252.79.7 mm2; MPW: 1.1 ± 2.4 mm; MPD: 0.4 ± 1.4 mm; MAD: 17.1 ± 54.2 mm2 | LPW: 5.9 ± 5.6 mm; LPD: 8.4 ± 7.3 mm; LAD: 291.1 ± 30.3 mm2; MPW: 0.1 ± 0.4 mm; MPD: 0.3 ± 1.5 mm; MAD: 15.2 ± 75.6 mm2 |
| Salari et al[20], 2021 | LPD: 12.48 ± 7.17 mm | LPD: 6.4 ± 4.3 mm | NR | NR | NR | NR | NR | NR |
| Jain et al[12], 2020 | NR | NR | NR | NR | NR | NR | NR | NR |
| Kim et al[21], 2022 | NR | NR | NR | NR | NR | NR | NR | NR |
| Liu et al[22], 2023 | LPD: 15.3 ± 3.5 mm; LPW: 9.4 ± 1.8 mm | LPD: 8.4 ± 3.4 mm; LPW: 6.9 ± 0.9 mm | NR | NR | NR | NR | NR | NR |
| Pu et al[10], 2022 | LPW: 8 ± 1.4 mm; LPD: 14.8 ± 10.2 mm | LPW: 6.8 ± 1.6 mm; LPD: 9.3 ± 8.1 mm | NR | NR | NR | NR | NR | NR |
| Ringus et al[13], 2010 | LPD: 15.9 ± 8.4 mm | LPD: 9.5 ± 6.7 mm | NR | NR | NR | NR | NR | NR |
| Tang et al[8], 2017 | LPW: 2.9 ± 3.4 mm; LPD: 14.8 ± 10.2 mm | LPW: 3.5 ± 4.8 mm; LPD: 9.3 ± 8.1 mm | NR | NR | NR | NR | NR | NR |
| Thamyongkit et al[23], 2018 | LPD: 5.36 ± 3.56 mm; MPD: 1.78 ± 2.24 mm | LPD: 1.33 ± 2.17 mm; MPD: 2.44 ± 0.89 mm | LPD: 2.93 ± 4.19 mm; MPD: 3.38 ± 1.22 mm | LPD: 3.62 ± 3.06 mm; MPD: 1.26 ± 1.49 mm | NR | NR | LPD: 3.32 ± 2.29 mm; MPD: 3.29 ± 0.43 mm2 | LPD: 3.35 ± 3.83 mm; MPD: 1.82 ± 1.81 mm |
LPD to predict lateral meniscus injury[10,13,20-22]: The cut-off values ranged from 11 mm to 4.3 mm, with a sensitivity range from 40.4% to 100%, a specificity range from 29% to 94.12%, and an area under the curve range from 0.678 to 0.898 (Table 4).
| Ref. | ROC analysis (cut-off point, sensitivity, specificity, and AUC) | Regression analysis (OR, 95%CI) |
| Chang et al[3], 2018 | LMi-LPW: 6.3 mm, 75.5%, 58.5%, 0.7; LMi-LAD: 112.9 mm2, 83.7%, 43.4%, 0.67; ACLi-LPW: 5.7 mm, 75.5%, 58.5%, 0.68; ACLi-LAD: 209.5 mm2, 66.7%, 65.5%, 0.66 | LMi-LPD: 4.35 (1.86-10.17); ACLi-LPW: 9.22 (2.33-36.54); ACLi-LAD: 6.81 (1.8-25.76) |
| Salari et al[20], 2021 | LMi-LPD: 4.3 mm, 100%, 29%, 0.75 | NR |
| Jain et al[12], 2020 | NR | LMi-LPW: 0.25 (0.06-1.05); LMi-LPD: 0.19 (0.04-0.97) |
| Kim et al[21], 2022 | LMi-LPD: 10.62 mm, 40.4%, 94.12%, 0.678 | LMi-LPD: 9 (1.018-79.545) |
| Liu et al[22], 2023 | LMi-LPW: 7.9 mm, 75%, 90%, 0.897; LMi-LPD: 8.4 mm, 95%, 85%, 0.898 | LMi-LPW: 6.25 (1.59-24.55); LMi-LPD: 1.52 (1.148-2.016) |
| Pu et al[10], 2022 | LMi-LPW: 7.5 mm, 70%, 70.6%, 0.724; LMi-LPD: 7.9 mm, 95%, 58.5%, 0.818 | NR |
| Ringus et al[13], 2010 | LMi-LPD: 10 mm, 79%, 67%, 0.74 | LMi-LPD: 7.89 (2.64-23.59) |
| Tang et al[8], 2017 | LMi-LPD: 11 mm, 70.3%, 61.8% | NR |
| Thamyongkit et al[23], 2018 | NR | NR |
LPW to predict lateral meniscus injury[3,10,22]: The cut-off values ranged from 6.3 mm to 7.9 mm, with a sensitivity range from 70% to 75.5%, a specificity range from 58.5% to 90%, and an area under the curve range from 0.7 to 0.897.
Predicting anterior cruciate ligament injury: Chang et al[3], was the only one to report cut-off values considering the LPW and LAD for anterior cruciate ligament injury (ACLi) prediction, which were 5.7 mm and 209.5 mm2, respectively.
The odds ratio (OR) for lateral meniscus injury (LMi) in the presence of LPD ranged from 0.19 to 9[3,12,13,22]. While the OR for LMi in the presence of LPW was 0.25 and 6.25[12,22]. Lastly, the OR for ACLi were 9.22 and 6.81 for LPW and LAD, respectively (Table 4)[3].
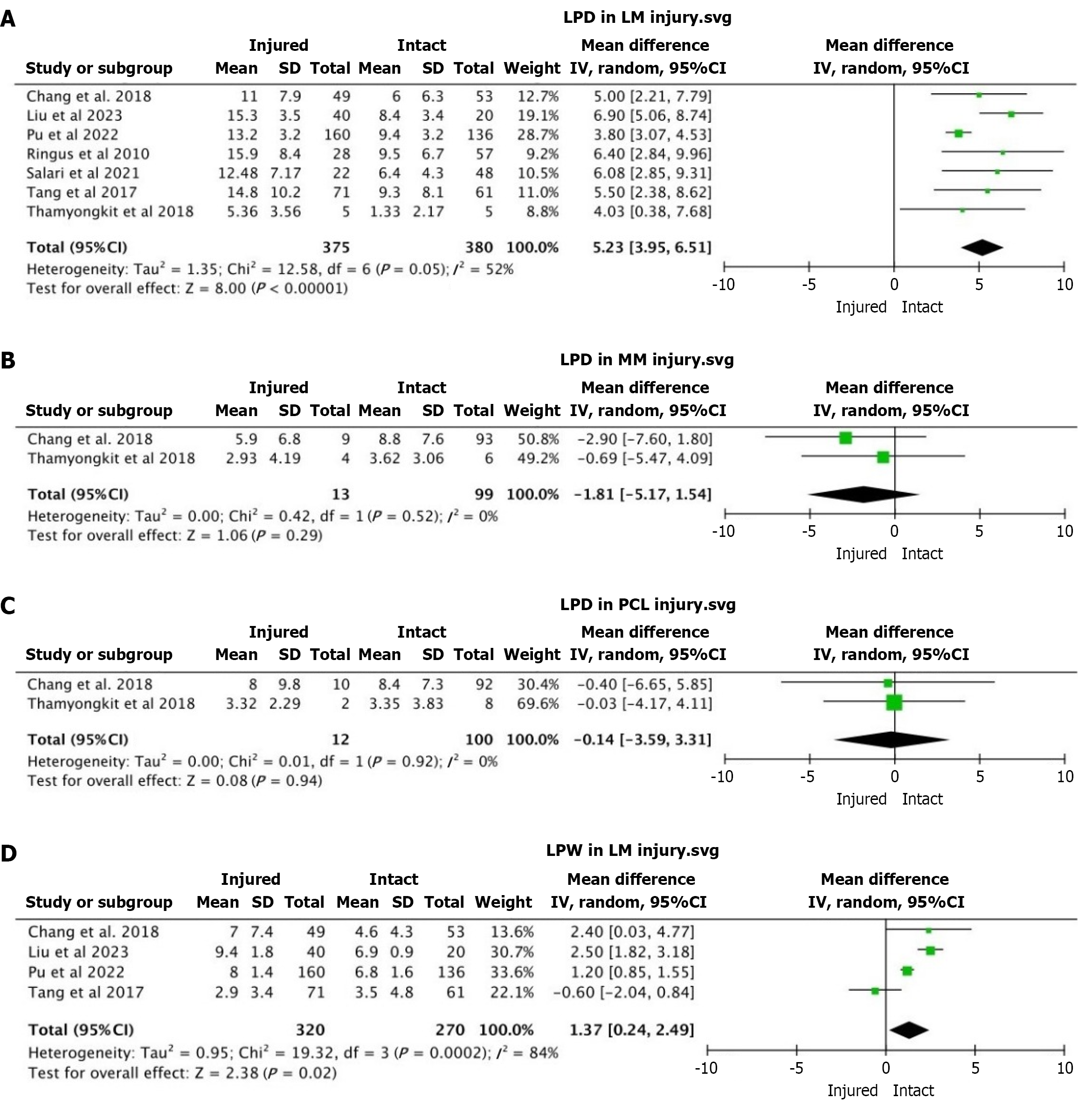
LPD in LMi: A statistically significant LPD increase was found in LMi patients compared to those with intact menisci, with a pooled mean difference of 5.23 [95% confidence interval (CI): 3.95-6.51, P < 0.00001]. Although moderate heterogeneity was observed (I2 = 52%), the consistency of individual study results supports the robustness of this conclusion (Figure 2A).
LPD in MM injuries: There was no statistically significant difference in LPD in patients with MM injuries (MMi) compared to those with intact menisci, with a pooled mean difference of -1.81 (95%CI: -5.17 to 1.54, P = 0.29). The low heterogeneity (I2 = 0%) reflects consistency among the included studies (Figure 2B).
LPD in PCL injuries: The analysis revealed no statistically significant difference in LPD between patients with PCL injuries (PCLi) and those with intact PCLs, with a pooled mean difference of -0.14 (95%CI: -3.59 to 3.31, P = 0.94). The absence of heterogeneity (I2 = 0%) indicates high consistency among the included studies (Figure 2C).
LPW in LMi: There was a statistically significant difference in LPW between LMi patients compared to those with intact menisci, with a pooled mean difference of 1.37 (95%CI: 0.24-2.49, P = 0.02). However, substantial heterogeneity was observed (I2 = 84%), suggesting variability among the included studies. Furthermore, the leave-one-out sensitivity analysis showed that the statistical significance of the pooled estimate was sensitive to the exclusion of individual studies. Specifically, upon removal of the study by Liu et al[22], the effect was no longer statistically significant. Furthermore, the substantial heterogeneity (I2 = 84%) was almost entirely attributable to the study by Tang et al[8], which reported an effect in the opposite direction (Table 5) (Figure 2D).
| Study omitted | Pooled MD (95%CI) | I2 | Tau2 | Conclusion |
| Overall analysis | 1.37 (0.24-2.49) | 84% | 0.95 | Original significant finding |
| Chang et al[3], 2018 | 1.18 (0.01-2.36) | 86% | 1.07 | Effect remains significant while point estimate decreases slightly |
| Liu et al[22], 2023 | 0.95 (-0.17 to 2.07) | 82% | 0.79 | Effect loses statistical significance (P > 0.05) |
| Pu et al[10], 2022 | 1.65 (0.22-3.08) | 88% | 1.43 | Effect remains significant while point estimate increases |
| Tang et al[8], 2017 | 1.94 (1.33-2.55) | 0% | 0.00 | Effect remains significant and heterogeneity is eliminated |
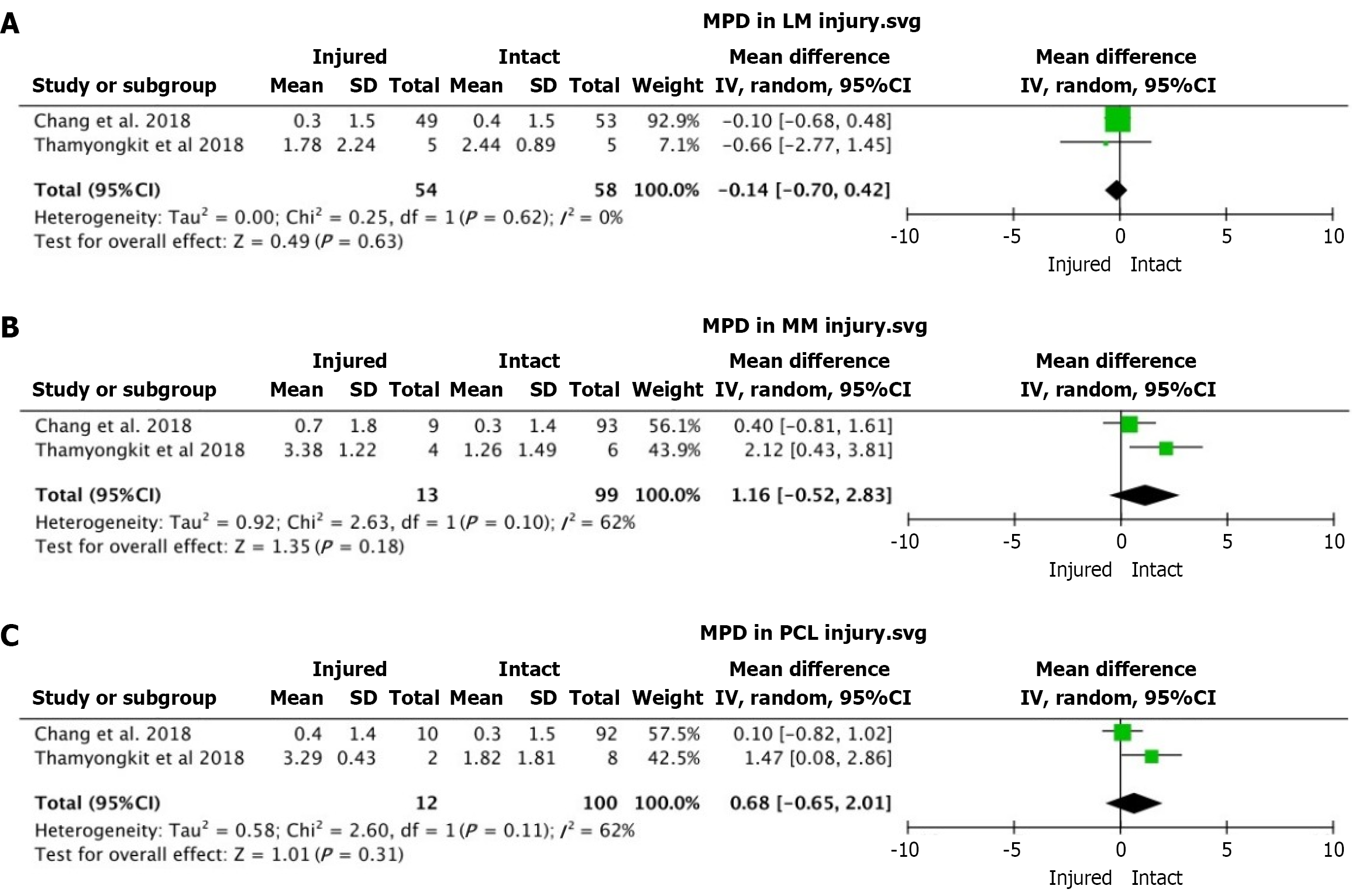
MPD in LMi: There was no statistically significant difference in MPD between LMi patients compared to those with intact menisci, with a pooled mean difference of -0.14 (95%CI: -0.70 to 0.42, P = 0.63). There was no significant heterogeneity among the included studies (I2 = 0%, P = 0.62), indicating consistency in the results across studies (Figure 3A).
MPD in MMi: There was no statistically significant difference in MPD between MMi patients compared to those with intact menisci, with a pooled mean difference of 1.16 (95%CI: -0.52 to 2.83, P = 0.18). Moderate heterogeneity was observed (I2 = 62%, P = 0.10) (Figure 3B).
MPD in PCLi: There was no significant difference in MPD between patients with PCLi and those with intact PCLs, with a pooled mean difference of 0.68 (95%CI: -0.65 to 2.01, P = 0.31). Moderate heterogeneity (I2 = 62%) indicates some inconsistency among the included studies (Figure 3C).
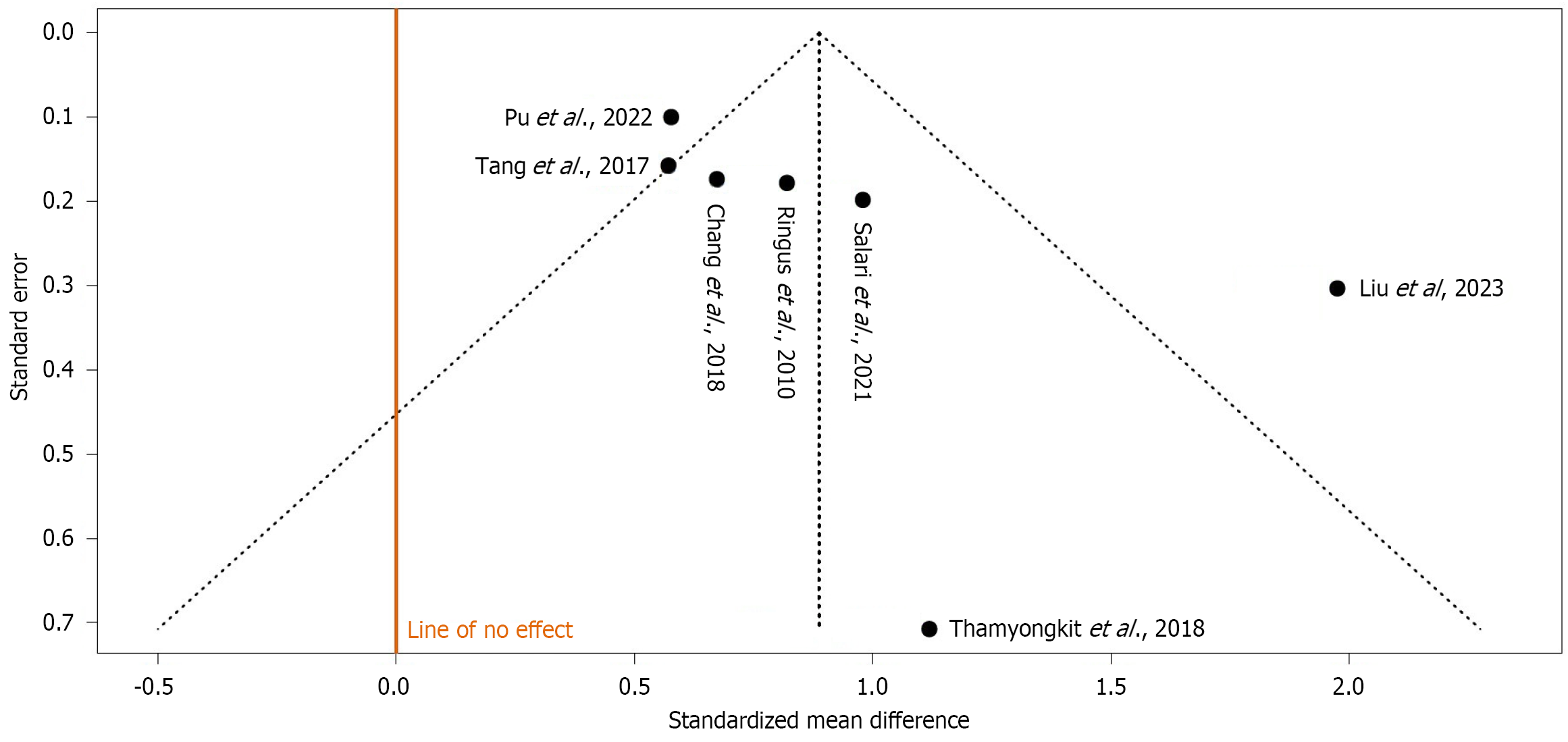
A funnel plot was constructed for the pooled analysis of LPD as a predictor of LMi as reported in seven studies[3,8,10,13,20,22,23]. The funnel plot (Figure 4) does not indicate potential publication bias. The Egger’s test does not support the presence of funnel plot asymmetry (intercept: 2.61, 95%CI: 0.14-5.07, t: 2.075, P = 0.093).
Although the management protocol for TPFs is well-documented in the literature, this only applies to bony injuries[24-26]; there is still no consensus among trauma surgeons regarding the optimal approach to diagnose and manage soft tissue injuries associated with TPFs[2,27]. Up to 93% of TPFs have associated soft tissue injuries[27], and their proper identification before fracture fixation enables surgeons to manage such injuries, leading to better outcomes and fewer complications[2,26,28-32]. Furthermore, some authors have proposed the need to include soft-tissue injuries in TPF classification systems[33].
The estimated incidence of soft tissue injuries accompanying TPFs ranges from 39% to 99% for meniscal injuries and 16.7% to 57% for ligamentous injuries[3,27,34,35]. The incidence increases as fracture severity and displacement increase[11,36]. Surgeons will not treat injuries they do not see, while diagnosed injuries will mostly be surgically addressed if required[2].
For most trauma surgeons, obtaining a CT scan to diagnose and determine the management plan for TPFs is the gold standard practice after preliminary plain radiographs; furthermore, most classification systems for TPFs rely on the CT scan configuration of the fracture. Measurable CT scan parameters can potentially predict soft-tissue injuries, as highlighted in the current systematic review, in which LMi was the most commonly studied injury and could be predicted by measuring LPD and LPW. Although it was evaluated in one study, ACLi could be predicted by assessing the LPD and LPW. However, none of the measured parameters could significantly predict MMi or PCLi.
Some authors have suggested additional diagnostic approaches to define and locate soft-tissue injuries associated with TPFs, namely, MRI imaging and direct evaluation via knee arthroscopy or arthrotomy[2,27]. Although some reports have suggested the beneficial role of the above-mentioned approaches, we believe that a CT scan remains the most suitable tool for most surgeons.
Stephens et al[2] evaluated 18 studies assessing diagnostic approaches (MRI vs arthroscopy vs arthrotomy) for soft-tissue injuries. The studies included 884 patients with TPFs. In eight studies, MRI was obtained preoperatively, which diagnosed between 32% and 60% of concomitant LMi. In six studies, arthrotomy was utilized (exclusively for LMi associated with lateral TPFs); unfortunately, arthrotomy during lateral TPFs provides inadequate exposure of the rest of the knee to inspect the cruciate and MM. Furthermore, 12 studies utilized intraoperative arthroscopy, which provided better visualization and identification of the lesion, with the advantage of concomitant management of the soft-tissue injuries and confirming the fracture reduction quality[2]. However, intraoperative arthroscopy carries some disadvantages: The technique is not mastered by all trauma surgeons, potentially increasing the operative time, the fluid extravasation through the fracture could lead to increased compartment pressure, the visibility could be reduced owing to the fracture hematoma, and in some fractures, the knee manipulation is restricted which limits the visualization and access to all soft tissue structures[2,37].
In a systematic review by Thürig et al[27] evaluating the role of MRI in diagnosing TPFs associated soft tissue injuries, they evaluated 878 fractures from 18 studies; the authors reported that the included studies in their systematic review are inconsistent regarding the incidence of soft tissue injuries; furthermore, precise information guiding the surgical intervention to manage these soft tissue injuries was lacking, which obviously indicates that even obtaining MRI could not lead to a conclusive diagnosis and would not help in the management plan. A further drawback of MRI is that it could consider old degenerative meniscus lesions as fresh traumatic injuries, leading to a false positive diagnosis[3].
Schatzker and Kfuri[24] emphasized the importance of diagnosing associated soft-tissue injuries concurrent with TPFs to understand the injury mechanism better, leading to a more precise diagnosis and, ultimately, a more effective management plan. To achieve these goals, they recommended obtaining a preoperative MRI in addition to the gold standard CT scans. However, Stephens et al[2] concluded from their review that they cannot recommend the routine use of MRI, arthroscopy, or even arthrotomy for diagnosing associated soft tissue injuries.
The medial and lateral menisci serve essential functions to maintain the integrity of the knee joint; they increase articular surface congruency, act as shock absorbers, transmit load while walking, and contribute to knee joint stability[38]. Meniscal injury will affect these functions, leading to early derangement of the knee joint and the possibility of early osteoarthritis development[29,39,40].
The meniscal lesions associated with TPFs can be described as simple contusions (no noticeable tear), radial, peripheral, horizontal, flap, and bucket-handle tears[40,41]. Furthermore, meniscus degenerative changes could be found and misdiagnosed as traumatic tears (as reported in some studies using MRI as a diagnostic tool)[3].
Proper identification of possible meniscus injuries and efficient management in cases of TPFs provide better outcomes and lower chances of posttraumatic osteoarthritis development. Furthermore, meniscus injury repair during open reduction and internal fixation of TPFs results in better functional outcomes[12,42].
The LMi was the most commonly evaluated soft tissue injury in the studies included in the current review, in which an LPD of 1.6 mm to 4.3 mm could predict LMi, with sensitivities and specificities up to 100% and 94%, respectively (OR of 0.19-7.89). Meanwhile, LPW of 6.3 mm to 7.9 mm has a lower sensitivity and specificity of nearly 75% for both (OR 0.25-6.25). Furthermore, CT scans poorly predict MMi.
It is worth noting that, owing to the higher heterogeneity detected regarding LPW in predicting LMi, while the association is still significant, it should not be considered an analysis flaw; however, it highlights that the relationship between LPW and LMi could be more complex and affected by other possible variables, rather than a simple LPW value. Moreover, the sensitivity analysis showed that omitting a single study had an effect; however, the point estimate remained positive across all scenarios, indicating a consistent leaning towards a larger LPW being associated with LMi.
The location of the maximum articular impaction/displacement could be a more precise clue to the soft tissue injury location, images obtained from CT scans could be further divided into quadrants as reported by Salari et al[20], who investigated LMi in cases presented with lateral TPFs comparing the CT findings to those obtained during arthrotomy, the authors divided the lateral tibial plateau into anterolateral, anteromedial (AM), posterolateral (PL) and posteromedial in the axial cuts. They reported that if the articular impaction/displacement is located in the anterolateral or AM zones, the OR for LMi is 7.3 and 5.6, respectively, compared with other zones. The authors indicated that in anterior zones, the amount of depression required to cause LMi was lower than in posterior zones.
Liu et al[22] exclusively included TPFs involving the medial plateau (type IV); however, the authors further divided this fracture according to the location of the fracture line as suggested by Wahlquist et al[43], into subtypes A, B, and C fractures, where type IVC is when the fracture line is located on the lateral side of the tibial eminence, making this particular type more susceptible to have LMi (mostly entrapment)[44].
It is obvious that anterior cruciate ligament or PCL avulsions from their attachment can be easily identified in CT scan images; however, mid-substance tears can be challenging to diagnose. Chang et al[3] reported an incidence of cruciate ligament injury of 22.5% (14.7% ACLi and 9.8% PCLi); these injuries were classified into either avulsion fractures (the most commonly occurring, accounting for 9.8% of all fractures) or partial or complete tears. In the systematic review by Thürig et al[27], the authors reported incidences of ACLi and PCLi of 36.8% and 14.8%, respectively.
In the current systematic review, Chang et al[3] were the only study to evaluate the ACLi and its predictors. They indicated that LAD and LPW were significant predictors for ACLi, and they set cut-off values of 209.5 mm2 (66.7% sensitivity and 65.5% specificity) and 5.7 mm (75.5% sensitivity and 58.5% specificity) for both parameters, respectively.
In the study by Tang et al[8], the authors reported a significant association between MPD and ACLi, with a threshold of 3 mm (P = 0.014), yielding a positive predictive value of 49.2% and a negative predictive value of 74.6%. Furthermore, the authors classified the fractures based on the three-column concept; they found that TPFs involving the AM and PL columns had a higher risk of concomitant ACLi (avulsion fractures), the incidence was 50.7% with AM and 45.2% with PL; furthermore, the OR with AM involvement was 4.11 (P = 0.012), and with PL involvement was 3.61 (P = 0.015).
Some studies have found an increased incidence of ACLi with certain types of fractures. Stannard et al[45] reported that ACLi occurred more commonly in their patients with high-energy TPFs (Schatzker types IV-VI). Tang et al[8] reported that ACLi (specifically, avulsion fractures) occurred more frequently in younger patients and with higher-energy TPF patterns (48.2% in Schatzker type IV-VI fractures vs 18.4% in Schatzker type I-III, P = 0.001).
In contrast, Chang et al[3] reported no significant correlation between TPF classification and ACLi. The same was reported by Jain et al[12], who found no effect of TPF classification on the soft tissue injury type. Furthermore, in an MRI-based study by Gardner et al[35] evaluating 103 TPFs, the authors reported no differences in ACLi incidence across fracture classifications.
Regarding PCLi, it was evaluated in two studies[3,23], although Chang et al[3] reported a significant difference between MPW in patients diagnosed with PCLi and those without (1.1 ± 2.4 mm2 vs 0.1 ± 0.4 mm2; P = 0.005), the pooled analysis from the current systematic review found neither MPW nor LPD had a significant difference between PCLi and being intact.
The current systematic review has some limitations. First, although we acknowledged substantial heterogeneity among the included studies (I2 = 84%) regarding LPW in predicting LMi, it is worth noting that such a heterogeneity might be attributed to differences in the demographic data of the included patients between studies, possible associated other soft tissue injuries, flaws and inconsistency in obtaining the CT images and performing the measurements among different studies, and from a statistical point of view, if the included studies are few, the estimate of between-study variance (Tau2) is less stable, which might inflate the I2 value making it less precise or trustable. Second, the included studies focused on meniscal and cruciate ligament injuries; however, other soft-tissue structures, such as the synovium, capsule, articular cartilage, and collateral ligaments, were not evaluated. Third, measuring CT scan parameters is an indirect method for predicting soft-tissue injuries without a clear diagnosis of their nature, and it cannot provide a precise indication of which structure should be addressed. However, CT scans that predict soft-tissue injuries may indicate the need for an MRI for further delineation. Fourth, the included studies lack assessment and prediction of cruciate ligament injuries. Fourth, most studies did not report the precise location of the fracture lines or the depression, which could affect the location and type of soft-tissue injury, as noted by Salari et al[20].
Lastly, we only included two databases: PubMed and Scopus. Although they provide extensive indexing of TPF-related studies, the exclusion of additional databases, such as EMBASE, Web of Science, and the Cochrane Library, as well as other sources, including grey literature and trial registries, may have led to unintentional omissions of relevant studies. Future studies should include a broader database search strategy to further minimize potential publication and indexing bias.
Until there is a consensus regarding which diagnostic tool is best for diagnosing soft tissue injuries associated with TPFs, CT scans, which are obtained by default for all TPF cases, may provide sufficient data to suspect or diagnose associated meniscus or cruciate ligament injuries. Furthermore, identifying possible soft-tissue injury patterns based on CT scan parameters enables the surgeon to modify the management decision to either obtain an MRI to further delineate the injuries or proceed with arthroscopically assisted fracture fixation.
| 1. | Tornetta P, Ostrum RF, McKee MD, Ollivere BJ, de Ridder VA. Rockwood and Green's fractures in adults. Riverwoods, IL: Lippincott Williams and Wilkins, 2024. |
| 2. | Stephens A, Searle H, Carlos W, Gomindes A, Pilarski A, Syed F, Smith N, Khatri C. Diagnostic impacts on management of soft tissue injuries associated with tibial plateau fractures: A narrative review. Injury. 2024;55:111546. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 3. | Chang H, Zheng Z, Shao D, Yu Y, Hou Z, Zhang Y. Incidence and Radiological Predictors of Concomitant Meniscal and Cruciate Ligament Injuries in Operative Tibial Plateau Fractures: A Prospective Diagnostic Study. Sci Rep. 2018;8:13317. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 30] [Article Influence: 3.8] [Reference Citation Analysis (1)] |
| 4. | Behrendt P, Berninger MT, Thürig G, Dehoust J, Christensen J, Frosch KH, Krause M, Hartel MJ. Nanoscopy and an extended lateral approach can improve the management of latero-central segments in tibial plateau fractures: a cadaveric study. Eur J Trauma Emerg Surg. 2023;49:1433-1439. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 11] [Reference Citation Analysis (1)] |
| 5. | Ruiz-Ibán MÁ, Diaz-Heredia J, Elías-Martín E, Moros-Marco S, Cebreiro Martinez Del Val I. Repair of meniscal tears associated with tibial plateau fractures: a review of 15 cases. Am J Sports Med. 2012;40:2289-2295. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 36] [Article Influence: 2.6] [Reference Citation Analysis (1)] |
| 6. | Stahl D, Serrano-Riera R, Collin K, Griffing R, Defenbaugh B, Sagi HC. Operatively Treated Meniscal Tears Associated With Tibial Plateau Fractures: A Report on 661 Patients. J Orthop Trauma. 2015;29:322-324. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 42] [Article Influence: 3.8] [Reference Citation Analysis (1)] |
| 7. | Wang Y, Wang L, Zhu T, Liu Z, Liu G. Open reduction and internal fixation in a one-stage anterior cruciate ligament reconstruction surgery for the treatment of tibial plateau fractures: A case report and literature review. Injury. 2018;49:1215-1219. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 8. | Tang HC, Chen IJ, Yeh YC, Weng CJ, Chang SS, Chen AC, Chan YS. Correlation of parameters on preoperative CT images with intra-articular soft-tissue injuries in acute tibial plateau fractures: A review of 132 patients receiving ARIF. Injury. 2017;48:745-750. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 27] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 9. | Kolb JP, Regier M, Vettorazzi E, Stiel N, Petersen JP, Behzadi C, Rueger JM, Spiro AS. Prediction of Meniscal and Ligamentous Injuries in Lateral Tibial Plateau Fractures Based on Measurements of Lateral Plateau Widening on Multidetector Computed Tomography Scans. Biomed Res Int. 2018;2018:5353820. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 18] [Article Influence: 2.3] [Reference Citation Analysis (2)] |
| 10. | Pu Y, Lei Z, Wenge D, Yue X, Xiaowei J, Kejie W, Yiwen Z, Zhihui H, Xiaoyu D. Correlation between CT images of lateral plateau and lateral meniscus injuries in patients with Schatzker II tibial plateau fractures:a retrospective study. BMC Musculoskelet Disord. 2022;23:9. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 11. | Spiro AS, Regier M, Novo de Oliveira A, Vettorazzi E, Hoffmann M, Petersen JP, Henes FO, Demuth T, Rueger JM, Lehmann W. The degree of articular depression as a predictor of soft-tissue injuries in tibial plateau fracture. Knee Surg Sports Traumatol Arthrosc. 2013;21:564-570. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 42] [Article Influence: 3.2] [Reference Citation Analysis (1)] |
| 12. | Jain A, Iliopoulos E, Trompeter A. Widening is a predictive factor of bucket handle tear in tibial plateau fractures. Eur J Orthop Surg Traumatol. 2020;30:695-699. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 13. | Ringus VM, Lemley FR, Hubbard DF, Wearden S, Jones DL. Lateral tibial plateau fracture depression as a predictor of lateral meniscus pathology. Orthopedics. 2010;33:80-84. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 24] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 14. | Gardner MJ, Yacoubian S, Geller D, Pode M, Mintz D, Helfet DL, Lorich DG. Prediction of soft-tissue injuries in Schatzker II tibial plateau fractures based on measurements of plain radiographs. J Trauma. 2006;60:319-23; discussion 324. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 56] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 15. | Mustonen AO, Koivikko MP, Lindahl J, Koskinen SK. MRI of acute meniscal injury associated with tibial plateau fractures: prevalence, type, and location. AJR Am J Roentgenol. 2008;191:1002-1009. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 36] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 16. | Hashemi SA, Ranjbar MR, Tahami M, Shahriarirad R, Erfani A. Comparison of Accuracy in Expert Clinical Examination versus Magnetic Resonance Imaging and Arthroscopic Exam in Diagnosis of Meniscal Tear. Adv Orthop. 2020;2020:1895852. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 15] [Article Influence: 2.5] [Reference Citation Analysis (1)] |
| 17. | Furlan AD, Malmivaara A, Chou R, Maher CG, Deyo RA, Schoene M, Bronfort G, van Tulder MW; Editorial Board of the Cochrane Back, Neck Group. 2015 Updated Method Guideline for Systematic Reviews in the Cochrane Back and Neck Group. Spine (Phila Pa 1976). 2015;40:1660-1673. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 597] [Cited by in RCA: 549] [Article Influence: 49.9] [Reference Citation Analysis (0)] |
| 18. | Moher D, Liberati A, Tetzlaff J, Altman DG; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol. 2009;62:1006-1012. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9572] [Cited by in RCA: 8817] [Article Influence: 518.6] [Reference Citation Analysis (5)] |
| 19. | Whiting PF, Rutjes AW, Westwood ME, Mallett S, Deeks JJ, Reitsma JB, Leeflang MM, Sterne JA, Bossuyt PM; QUADAS-2 Group. QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med. 2011;155:529-536. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11012] [Cited by in RCA: 10550] [Article Influence: 703.3] [Reference Citation Analysis (5)] |
| 20. | Salari P, Busel G, Watson JT. A radiographic zone-based approach to predict meniscus injury in lateral tibial plateau fracture. Injury. 2021;52:1539-1543. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 11] [Article Influence: 2.2] [Reference Citation Analysis (1)] |
| 21. | Kim SH, Lee SH, Gwak H, Kim KI, Lee SH. Clinical and radiographic results after arthroscopic repair of lateral meniscus tear in lateral-depression tibial plateau fracture. Arch Orthop Trauma Surg. 2022;142:263-270. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 6] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 22. | Liu Y, Fang R, Tu B, Zhu Z, Zhang C, Ning R. Correlation of preoperative CT imaging shift parameters of the lateral plateau with lateral meniscal injury in Schatzker IV-C tibial plateau fractures. BMC Musculoskelet Disord. 2023;24:793. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 23. | Thamyongkit S, Sa-Ngasoongsong P, Kulachote N, Ruangchaijatuporn T, Saengpetch N, Limitlaohaphan C, Kijkunasathian C (2018). Association between preoperative CT findings and meniscal injury in the fracture of tibial plateau: A preliminary report. J Med Assoc Thai. 2018;101:S1-S8. |
| 24. | Schatzker J, Kfuri M. Revisiting the management of tibial plateau fractures. Injury. 2022;53:2207-2218. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 45] [Article Influence: 11.3] [Reference Citation Analysis (1)] |
| 25. | Rosteius T, Rausch V, Pätzholz S, Lotzien S, Königshausen M, Schildhauer TA, Geßmann J. Factors influencing the outcome after surgical reconstruction of OTA type B and C tibial plateau fractures: how crucial is the restoration of articular congruity? Arch Orthop Trauma Surg. 2023;143:1973-1980. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 26] [Article Influence: 8.7] [Reference Citation Analysis (1)] |
| 26. | Snoeker B, Turkiewicz A, Magnusson K, Frobell R, Yu D, Peat G, Englund M. Risk of knee osteoarthritis after different types of knee injuries in young adults: a population-based cohort study. Br J Sports Med. 2020;54:725-730. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 160] [Article Influence: 22.9] [Reference Citation Analysis (1)] |
| 27. | Thürig G, Korthaus A, Frosch KH, Krause M. The value of magnetic resonance imaging in the preoperative diagnosis of tibial plateau fractures: a systematic literature review. Eur J Trauma Emerg Surg. 2023;49:661-679. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 19] [Reference Citation Analysis (1)] |
| 28. | Verona M, Marongiu G, Cardoni G, Piras N, Frigau L, Capone A. Arthroscopically assisted reduction and internal fixation (ARIF) versus open reduction and internal fixation (ORIF) for lateral tibial plateau fractures: a comparative retrospective study. J Orthop Surg Res. 2019;14:155. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 30] [Article Influence: 4.3] [Reference Citation Analysis (1)] |
| 29. | Weber J, Koch M, Angele P, Zellner J. The role of meniscal repair for prevention of early onset of osteoarthritis. J Exp Orthop. 2018;5:10. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 53] [Article Influence: 6.6] [Reference Citation Analysis (1)] |
| 30. | Warner SJ, Garner MR, Schottel PC, Fabricant PD, Thacher RR, Loftus ML, Helfet DL, Lorich DG. The Effect of Soft Tissue Injuries on Clinical Outcomes After Tibial Plateau Fracture Fixation. J Orthop Trauma. 2018;32:141-147. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 42] [Article Influence: 5.3] [Reference Citation Analysis (1)] |
| 31. | Bird ML, Chenard KE, Gonzalez LJ, Konda SR, Leucht P, Egol KA. A Comparative Study of Clinical Outcomes and Functional Status after Knee Fracture and Knee Fracture Dislocation. J Knee Surg. 2023;36:695-701. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 32. | Cinque ME, Godin JA, Moatshe G, Chahla J, Kruckeberg BM, Pogorzelski J, LaPrade RF. Do Tibial Plateau Fractures Worsen Outcomes of Knee Ligament Injuries? A Matched Cohort Analysis. Orthop J Sports Med. 2017;5:2325967117723895. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 18] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 33. | Tuncez M, Akan I, Seyfettinoğlu F, Çetin Tunçez H, Dirim Mete B, Kazımoğlu C. Is It Necessary To Add Soft Tissue Injury to the Classification in Tibial Plateau Fracture Management? Cureus. 2022;14:e22236. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 34. | Shepherd L, Abdollahi K, Lee J, Vangsness CT Jr. The prevalence of soft tissue injuries in nonoperative tibial plateau fractures as determined by magnetic resonance imaging. J Orthop Trauma. 2002;16:628-631. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 59] [Article Influence: 2.5] [Reference Citation Analysis (1)] |
| 35. | Gardner MJ, Yacoubian S, Geller D, Suk M, Mintz D, Potter H, Helfet DL, Lorich DG. The incidence of soft tissue injury in operative tibial plateau fractures: a magnetic resonance imaging analysis of 103 patients. J Orthop Trauma. 2005;19:79-84. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 156] [Cited by in RCA: 154] [Article Influence: 7.3] [Reference Citation Analysis (1)] |
| 36. | Wang J, Wei J, Wang M. The distinct prediction standards for radiological assessments associated with soft tissue injuries in the acute tibial plateau fracture. Eur J Orthop Surg Traumatol. 2015;25:913-920. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 20] [Article Influence: 1.8] [Reference Citation Analysis (1)] |
| 37. | Shamrock AG, Khazi Z, Gulbrandsen TR, Duchman KR, Willey MC, Karam MD, Hogue MH, Marsh JL. Trends and Complications of Arthroscopic-Assisted Tibial Plateau Fracture Fixation: A Matched Cohort Analysis. Arthrosc Sports Med Rehabil. 2020;2:e569-e574. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 38. | Greis PE, Bardana DD, Holmstrom MC, Burks RT. Meniscal injury: I. Basic science and evaluation. J Am Acad Orthop Surg. 2002;10:168-176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 281] [Cited by in RCA: 252] [Article Influence: 10.5] [Reference Citation Analysis (1)] |
| 39. | Matar HE, Duckett SP, Raut V. Degenerative meniscal tears of the knee: evaluation and management. Br J Hosp Med (Lond). 2019;80:46-50. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 10] [Article Influence: 1.4] [Reference Citation Analysis (1)] |
| 40. | Bhan K. Meniscal Tears: Current Understanding, Diagnosis, and Management. Cureus. 2020;12:e8590. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 57] [Article Influence: 9.5] [Reference Citation Analysis (1)] |
| 41. | Shiraev T, Anderson SE, Hope N. Meniscal tear - presentation, diagnosis and management. Aust Fam Physician. 2012;41:182-187. [PubMed] |
| 42. | Park HJ, Lee HD, Cho JH. The Efficacy of Meniscal Treatment Associated with Lateral Tibial Plateau Fractures. Knee Surg Relat Res. 2017;29:137-143. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 17] [Article Influence: 1.9] [Reference Citation Analysis (1)] |
| 43. | Wahlquist M, Iaguilli N, Ebraheim N, Levine J. Medial tibial plateau fractures: a new classification system. J Trauma. 2007;63:1418-1421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 26] [Article Influence: 1.4] [Reference Citation Analysis (1)] |
| 44. | Yan B, Sun J, Yin W. The prevalence of soft tissue injuries in operative Schatzker type IV tibial plateau fractures. Arch Orthop Trauma Surg. 2021;141:1269-1275. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 28] [Article Influence: 5.6] [Reference Citation Analysis (1)] |
| 45. | Stannard JP, Lopez R, Volgas D. Soft tissue injury of the knee after tibial plateau fractures. J Knee Surg. 2010;23:187-192. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 82] [Article Influence: 5.1] [Reference Citation Analysis (1)] |