Published online Apr 18, 2026. doi: 10.5312/wjo.v17.i4.114143
Revised: October 20, 2025
Accepted: January 13, 2026
Published online: April 18, 2026
Processing time: 210 Days and 10.3 Hours
Segmental bone loss caused by an open fracture is a challenging entity to treat, particularly when it is complicated by an infection. Combining bone reconstru
A 30-year-old male with a history of open tibial shaft fractures complicated by infections presented with a segmental bone defect of 13 cm and a soft-tissue defect measuring 10 cm × 15 cm. The patient was treated with radical debridement, anterolateral thigh free flap coverage, and trifocal bone transport with a circular Ilizarov fixator. A secondary correction of a mechanical axis deformity and sub
Trifocal bone transport combined with free flap coverage was effective and safe for treating critical tibial defects caused by post-traumatic infection. This tech
Core Tip: This case highlighted the successful treatment of a 13 cm tibial defect complicated by infections with trifocal bone transport combined with free flap coverage. The combined strategy allowed both soft-tissue coverage and skeletal res
- Citation: Miranda Cárdenas JE. Reconstruction of a massive tibial defect using trifocal bone transport and free flap: A case report. World J Orthop 2026; 17(4): 114143
- URL: https://www.wjgnet.com/2218-5836/full/v17/i4/114143.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i4.114143
Segmental bone defects in the lower limbs can be caused by high-energy trauma, radical debridement, and/or infection. Segmental bone defects are one of the greatest challenges for orthopedic and reconstructive surgeons because both bone and soft-tissue loss must be addressed simultaneously. Post-traumatic infections are treated by thorough debridement of nonviable tissue followed by soft-tissue coverage and skeletal reconstruction to achieve successful limb salvage. Several reconstructive techniques have been described, including distraction osteogenesis, vascularized fibular grafts, and the Masquelet technique[1,2]. These techniques yield comparable consolidation and infection recurrence rates. However, additional advantages have been observed after treatment with multilevel bone transport (trifocal) because it accelerates consolidation, reduces external fixation time, and minimizes complications related to prolonged frame use[3,4]. Herein, the case of a critical 13-cm tibial defect that was managed successfully with trifocal bone transport and free flap hi
Limb salvage in the presence of infection and extensive bone and soft-tissue loss remains a demanding reconstructive problem. The Ilizarov method provides stable fixation, gradual deformity correction, and bone regeneration through distraction osteogenesis, while microsurgical free flap coverage-performed by a plastic surgeon-ensures durable soft-tissue restoration. The combination of both methods has proven reliable for managing critical-sized tibial defects[5-7].
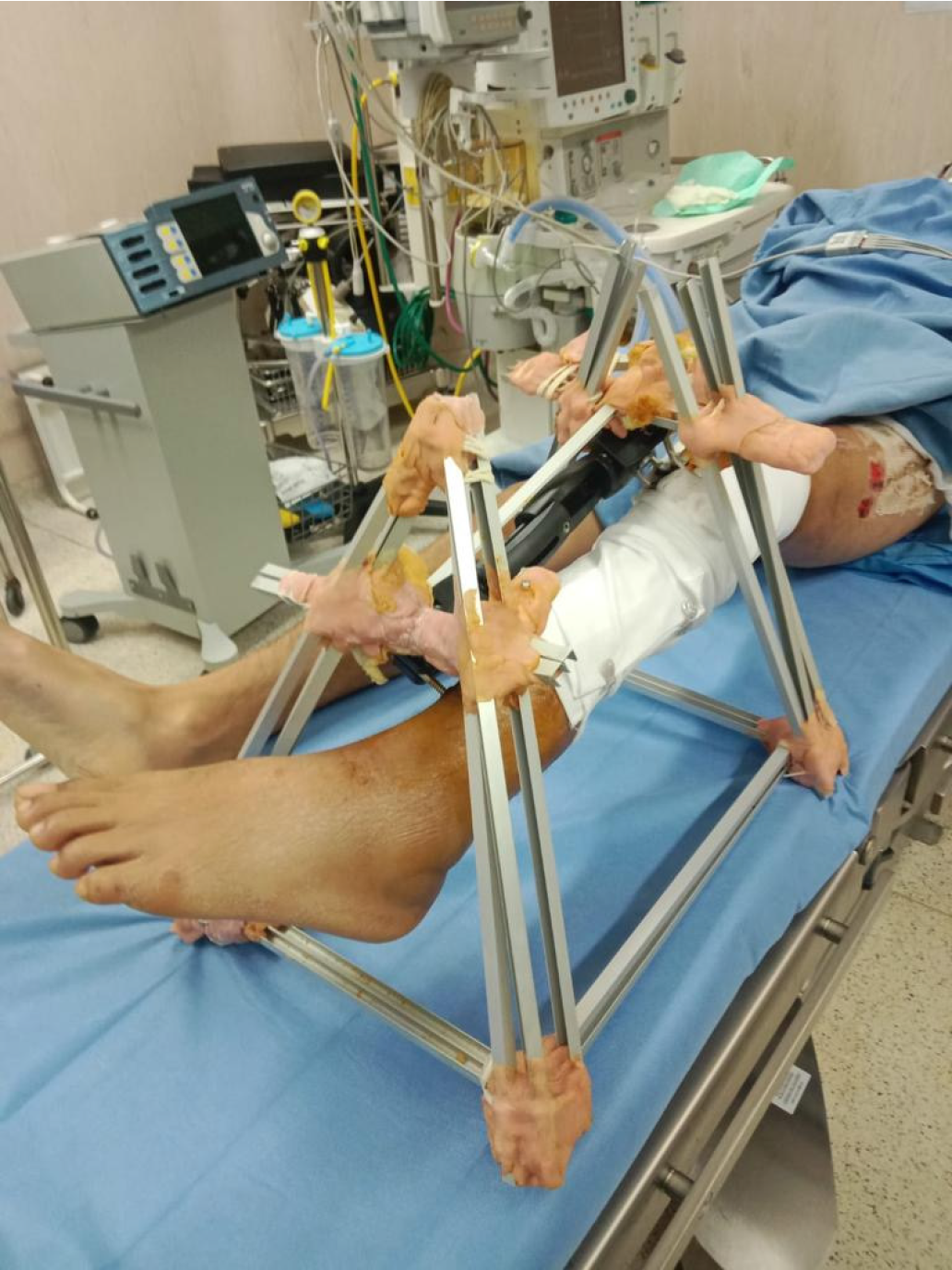
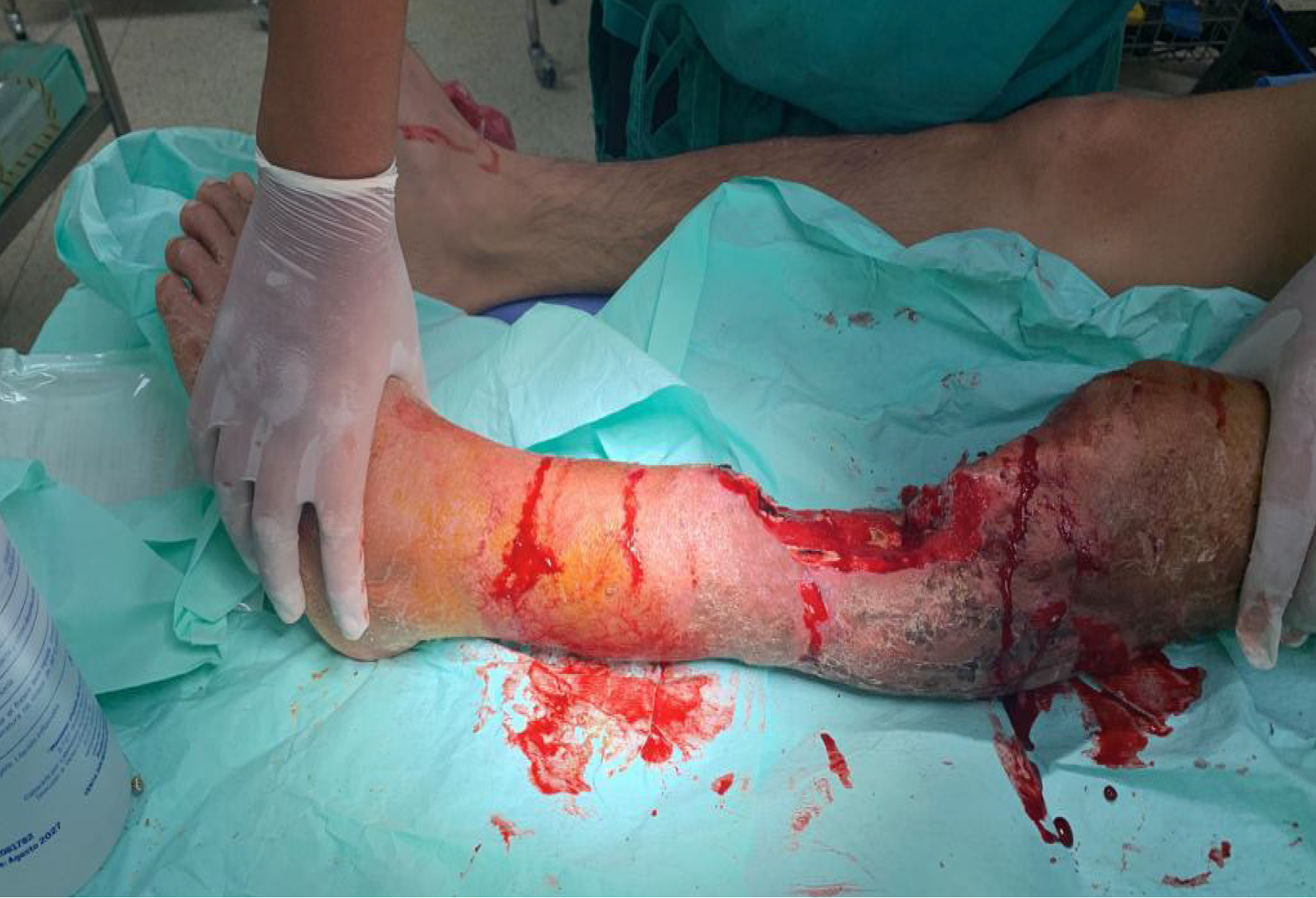
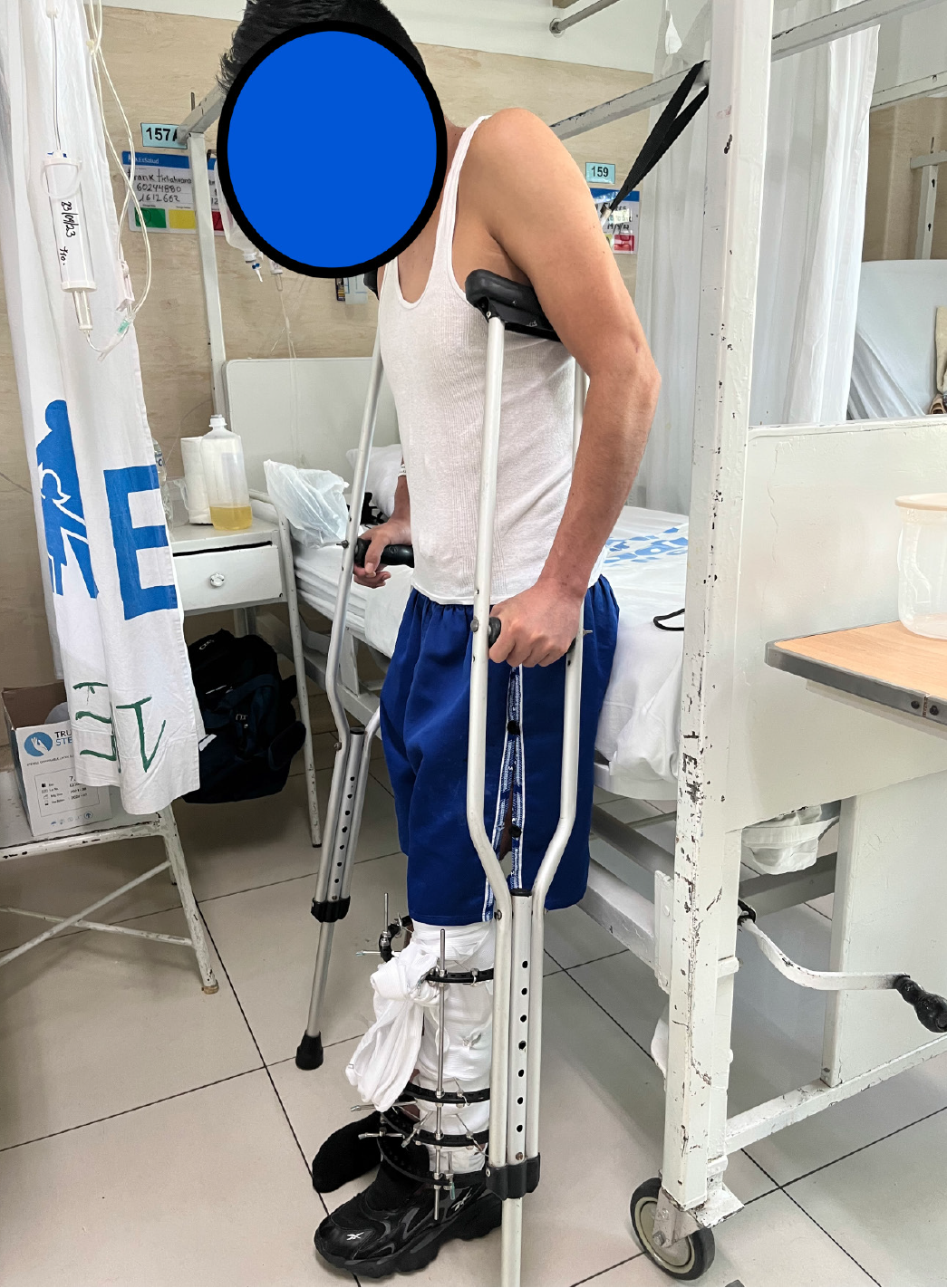
A 30-year-old male presented with an infection, a bone defect measuring 13 cm, and a soft-tissue defect measuring 10 cm × 15 cm in the anteromedial leg (Figures 1 and 2).
The patient had sustained an open tibial shaft fracture in December 2022 that was initially treated with external fixation and multiple debridements.
The patient had no relevant past medical history.
There was no significant personal nor family medical history.
Upon physical examination a segmental defect with soft-tissue loss was observed. There was no indication of vascular compromise nor neurovascular compromise.
The patient’s laboratory results were within normal ranges and were used to guide surgical timing. At admission the C-reactive protein level was below 0.3 mg/dL (normal: < 0.3 mg/dL). The erythrocyte sedimentation rate remained within normal limits (normal: ≤ 15 mm/hour for males). These markers were monitored throughout the patient’s follow-up and remained normal. Inflammatory markers were monitored to guide the timing of the reconstruction.
Imaging (angio-computed tomography and Doppler ultrasound) indicated that there was no vascular injury.
A multidisciplinary team including an orthopedic surgeon, a reconstructive plastic and microsurgeon, and an infectious disease specialist discussed the case and established the management strategy. The orthopedic surgeon performed the bone stabilization procedure and trifocal bone transport using the Ilizarov circular fixator. The plastic and microsurgeon carried out the free flap procedure for soft-tissue coverage. The infectious disease specialist supervised the antibiotic regimen and infection control throughout the treatment.
Fracture-related infection of the tibia with a 13 cm diaphyseal defect and soft-tissue loss.
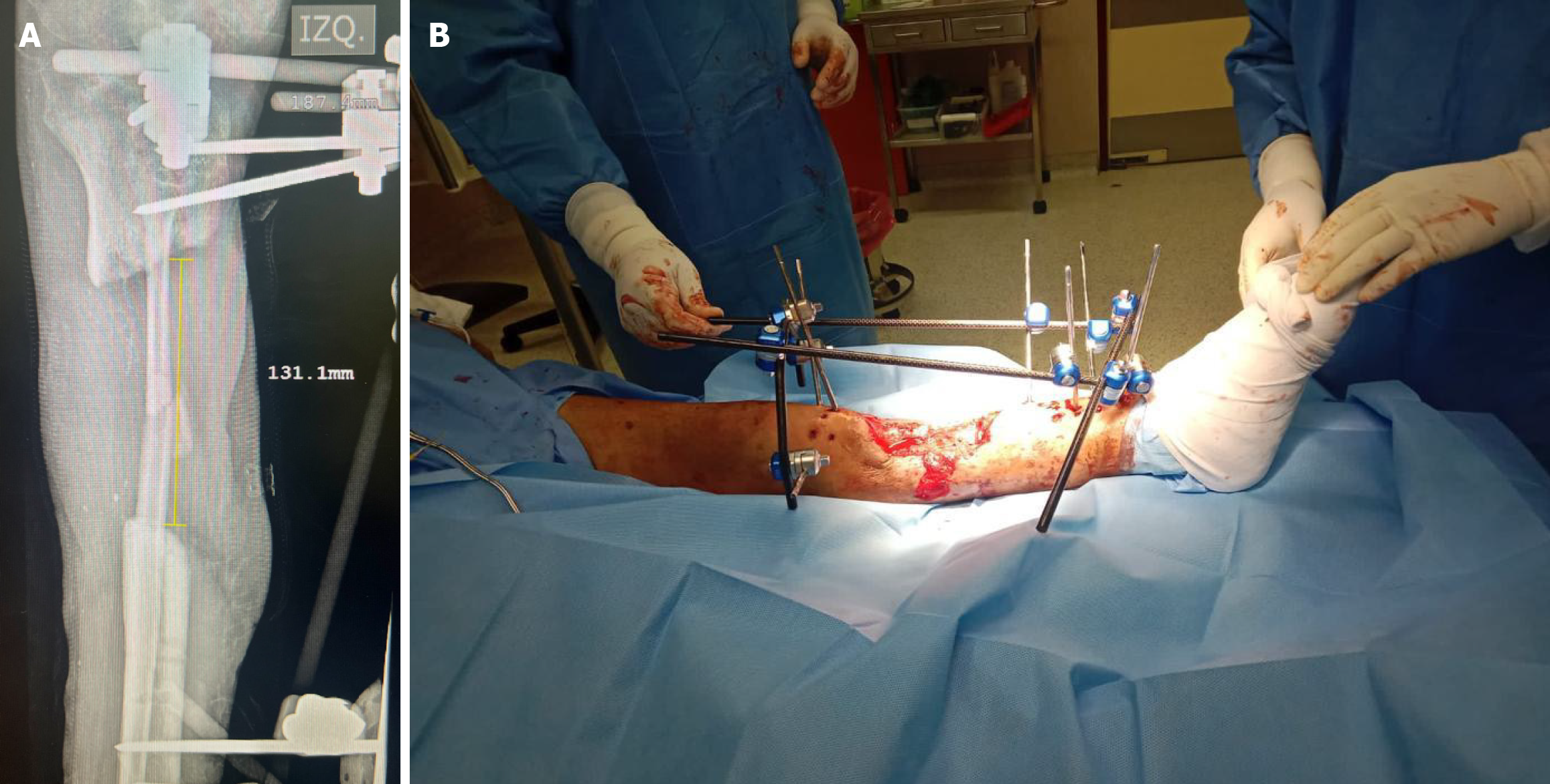
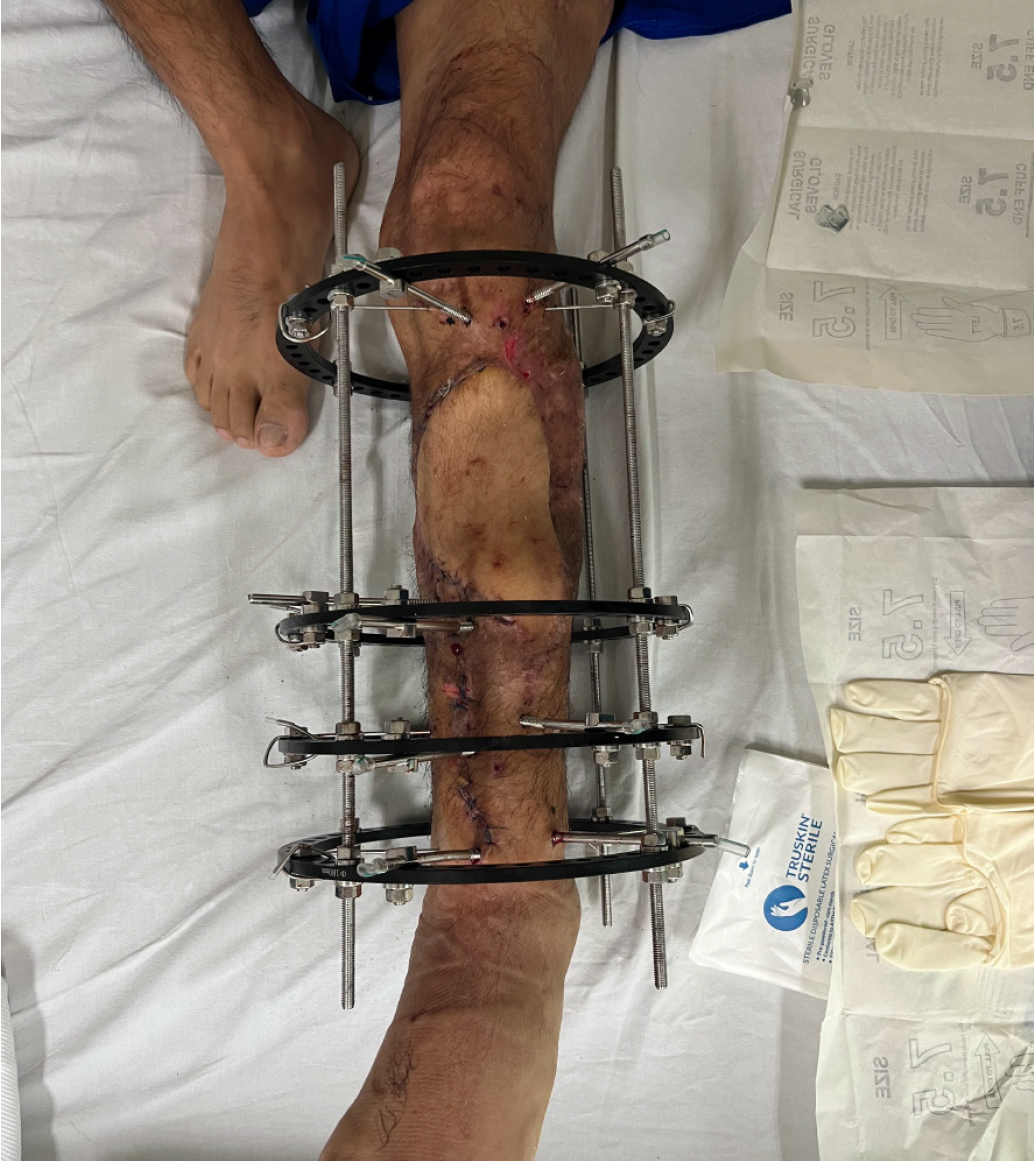
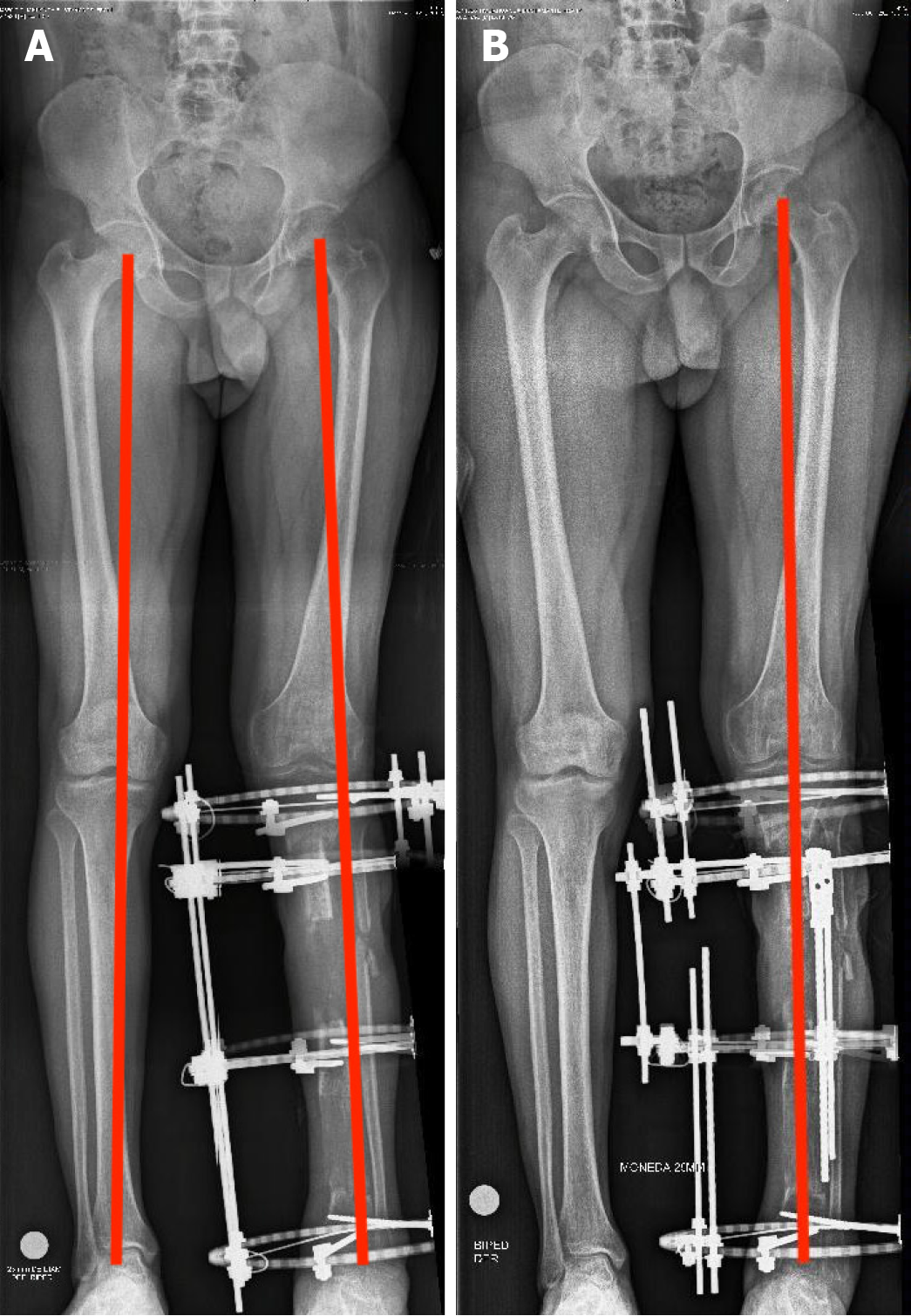
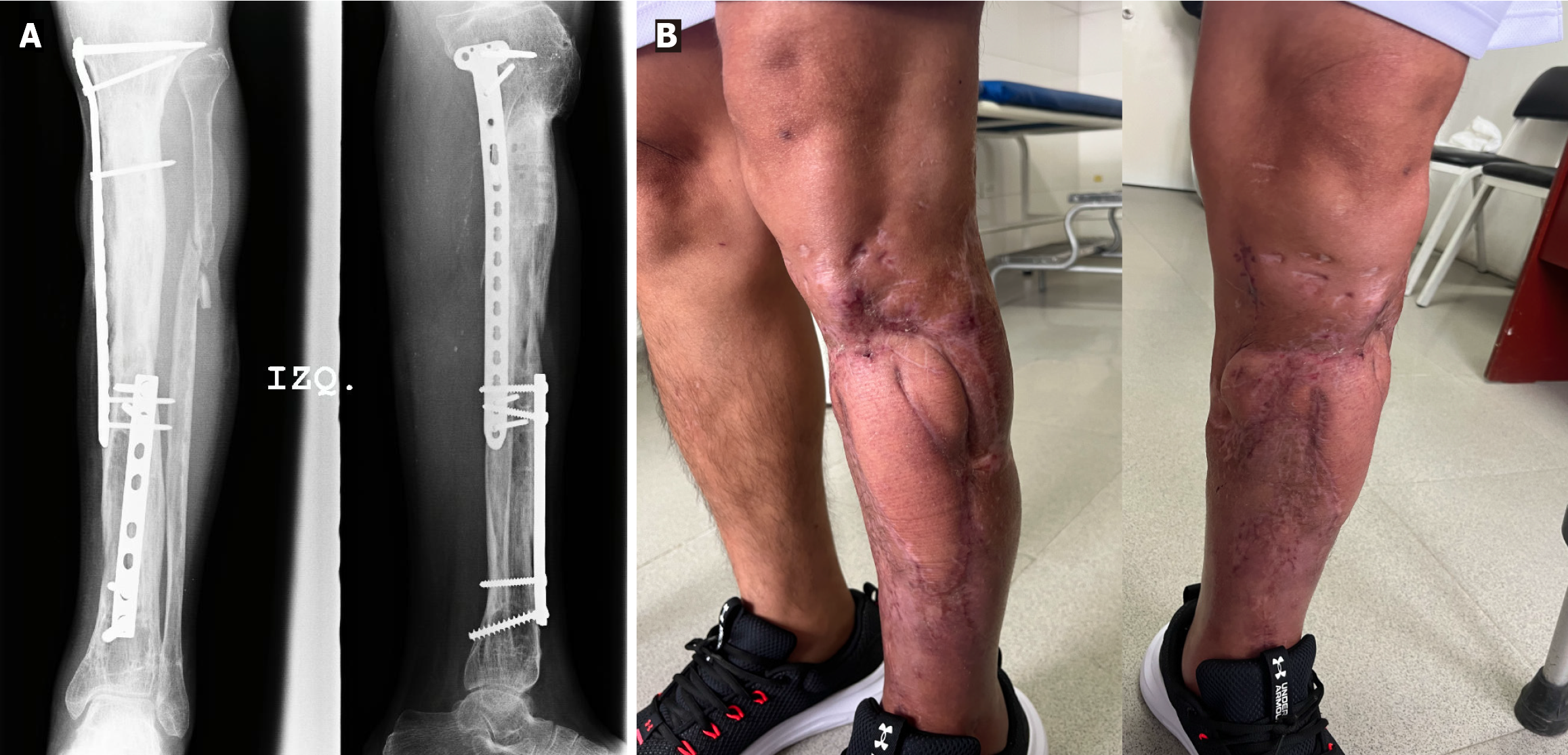
The patient underwent radical debridement of nonviable bone and soft tissue (Figure 3), and he received negative pressure therapy. An anterolateral thigh free flap was used for the reconstruction of the soft-tissue defect. An 8-week course of antibiotic therapy was administered, consisting of intravenous cefazolin (1 g every 8 hours) combined with gentamicin (80 mg every 8 hours) for the first 5 weeks, followed by cefazolin (500 mg every 6 hours) for an additional 3 weeks. Trifocal bone transport was performed with a circular Ilizarov fixator (Figures 4 and 5). The axis deformity was corrected simultaneously (Figure 6). Locking compression plates were applied to protect the bone regeneration after removal of the external fixation (Figure 7).
After 17 months bone regeneration and corticalization was observed. Six months after the frame removal, the patient was asymptomatic with no pain or infections. The patient had also returned to work. Functional recovery was confirmed by excellent Association for the Study and Application of the Method of Ilizarov bone and functional scores.
Massive tibial defects complicated by infection require a staged, multidisciplinary treatment approach that includes radical debridement, vascularized or local flap coverage, and definitive skeletal reconstruction. Comparable outcomes have been observed for various techniques including distraction osteogenesis, vascularized fibula, and the Masquelet technique. There is no consensus on the best option, but management strategies must be individualized to the patient.
Trifocal bone transport is particularly useful for massive defects (> 6 cm) because it reduces the duration of external fixation and accelerates consolidation[3,4]. Patients undergoing trifocal bone transport have reported some complications including pin site infections, soft-tissue invagination, deformity, and the psychological burden of long external fixation durations. Sequential conversion to locking plates enhances corticalization and prevents refracture[5]. We also observed these outcomes in our patient.
Comparable studies have reported satisfactory limb salvage and functional recovery using similar strategies of bone transport combined with microsurgical soft-tissue reconstruction[6,7]. In the present case, the multidisciplinary co
Fractures in the lower limb that are complicated by infection are severe complications requiring radical debridement, vascularized soft-tissue coverage, and skeletal reconstruction. Trifocal bone transport effectively reduces external fixation time, allows axis correction, and promotes corticalization. This staged and multidisciplinary approach is appropriate for limb preservation in massive tibial defects to avoid amputation and restore functional independence.
The multidisciplinary management involving orthopedic, plastic, and infectious disease specialists was crucial for achieving a stable, infection-free reconstruction and favorable functional recovery, with the patient regaining inde
The author would like to thank the plastic and reconstructive microsurgery team and the infectious disease department for their valuable collaboration in the multidisciplinary management of this case. Their coordinated expertise contributed to the successful functional recovery of the patient.
| 1. | Bezstarosti H, Metsemakers WJ, van Lieshout EMM, Voskamp LW, Kortram K, McNally MA, Marais LC, Verhofstad MHJ. Management of critical-sized bone defects in the treatment of fracture-related infection: a systematic review and pooled analysis. Arch Orthop Trauma Surg. 2021;141:1215-1230. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 91] [Article Influence: 18.2] [Reference Citation Analysis (0)] |
| 2. | Corona PS, Carbonell-Rosell C, Vicente M, Serracanta J, Tetsworth K, Glatt V. Three-stage limb salvage in tibial fracture related infection with composite bone and soft-tissue defect. Arch Orthop Trauma Surg. 2022;142:3877-3887. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 3. | Liu K, Zhang H, Maimaiti X, Yusufu A. Bifocal versus trifocal bone transport for the management of tibial bone defects caused by fracture-related infection: a meta-analysis. J Orthop Surg Res. 2023;18:140. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 11] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 4. | Liu K, Jia Q, Wang X, Bahesutihan Y, Ma C, Ren P, Liu Y, Yusufu A. Complications associated with single-level bone transport for the treatment of tibial bone defects caused by fracture-related infection. BMC Musculoskelet Disord. 2023;24:514. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 5. | Kadier X, Liu K, Shali A, Hamiti Y, Wang S, Yang X, Keremu A, Yusufu A. Locking compression plate as a sequential external fixator following the distraction phase for the treatment of tibial bone defects caused by fracture-related infection: experiences from 22 cases. BMC Musculoskelet Disord. 2024;25:1088. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 6. | Moore TJ, Barron J, Hutchinson F 3rd, Golden C, Ellis C, Humphries D. Prosthetic usage following major lower extremity amputation. Clin Orthop Relat Res. 1989;219-224. [PubMed] [DOI] [Full Text] |
| 7. | Masquelet AC, Begue T. The concept of induced membrane for reconstruction of long bone defects. Orthop Clin North Am. 2010;41:27-37; table of contents. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 508] [Cited by in RCA: 585] [Article Influence: 36.6] [Reference Citation Analysis (0)] |