Published online Apr 28, 2026. doi: 10.4329/wjr.v18.i4.120706
Revised: March 17, 2026
Accepted: March 30, 2026
Published online: April 28, 2026
Processing time: 49 Days and 14.4 Hours
Adult intussusception is a rare clinical condition. Unlike in pediatric cases, adult intussusception often has a definable lead point, with benign or malignant tumors being the most common etiology. Small intestinal lipoma is a rare cause of adult intussusception. It typically presents with non-specific symptoms and an insi
A 30-year-old man presented with a one-week history of abdominal pain and distension, followed by dark red bloody stools for four days. Physical exami
CT is the modality of choice for diagnosing ileal lipoma-induced intussusception, as it can definitively identify the pathognomonic fat-density lead point. Surgical resection remains the definitive treatment, yielding good outcomes.
Core Tip: Adult intussusception is rare and often tumor-related. This case of ileocolic intussusception in a 30-year-old male underscores the critical diagnostic role of computed tomography (CT). CT not only confirmed the intussusception but, more importantly, identified the pathognomonic fat-density lead point, enabling a preoperative diagnosis of a lipoma. This case highlights that for radiologists and clinicians, recognizing this specific CT feature is key to accurate diagnosis and app
- Citation: Fan JX, Jiang YP, Yao MQ. Adult ileocolic intussusception caused by a terminal ileal lipoma: A case report. World J Radiol 2026; 18(4): 120706
- URL: https://www.wjgnet.com/1949-8470/full/v18/i4/120706.htm
- DOI: https://dx.doi.org/10.4329/wjr.v18.i4.120706
Small intestinal lipoma (SIL) is a clinically uncommon benign tumor[1]. Its manifestations depend on the tumor’s morphology, location, and size. Small SILs are often asymptomatic, whereas larger ones frequently lead to intestinal obstruction or intussusception. SIL has an insidious onset, and the rate of definitive preoperative diagnosis is low[2]. Although SIL is often misdiagnosed as other diseases, particularly other tumors, the use of abdominal computed tomography (CT) has improved diagnostic accuracy. SIL is characterized by a long disease course and slow progression, with malignant transformation being exceedingly rare. The prognosis after surgical resection is favorable.
A patient was admitted to our hospital on September 9, 2025, because of abdominal pain and distension for 1 week and hematochezia for 4 days. Abdominal CT demonstrated intussusception of the colon and ileocecal region with a fat-containing lesion within the lumen. An emergency ileocecal resection was performed. The postoperative diagnosis was an ileal lipoma complicated by intussusception. This case highlights the characteristic CT findings that allowed for a prompt and accurate preoperative diagnosis. By reviewing the relevant literature, we aim to discuss the clinical characteristics, diagnostic value of imaging, and surgical management principles to enhance clinician awareness of this disease.
A 30-year-old male patient presented to our hospital with a one-week history of abdominal pain and distension, followed by four days of dark red bloody stools.
The patient’s symptoms began one week prior to admission with progressive abdominal pain and distension. Four days before presentation, he developed dark red hematochezia. He denied any associated fever, vomiting, diarrhea, or significant weight loss.
The patient has no history of significant past medical conditions.
The patient reported no abnormal past medical or family history.
The patient was conscious and alert, with a height of 163 cm and a weight of 73 kg (body mass index 27.5 kg/m²). Vital signs were stable. Physical examination revealed a distended abdomen with no visible peristalsis. Bowel sounds were present at a rate of five per minute. The abdomen was soft but with tenderness localized to the right lower quadrant; no rebound tenderness or guarding was noted. No definite mass was palpable, and a digital rectal examination revealed no abnormalities.
Laboratory tests showed a mildly elevated white blood cell count of 11.0 × 109/L (reference range: 3.5-9.5 × 109/L) and a C-reactive protein level of 14.9 mg/L (reference range: ≤ 10.0 mg/L). The red blood cell count, hemoglobin, and platelet levels were within normal limits.
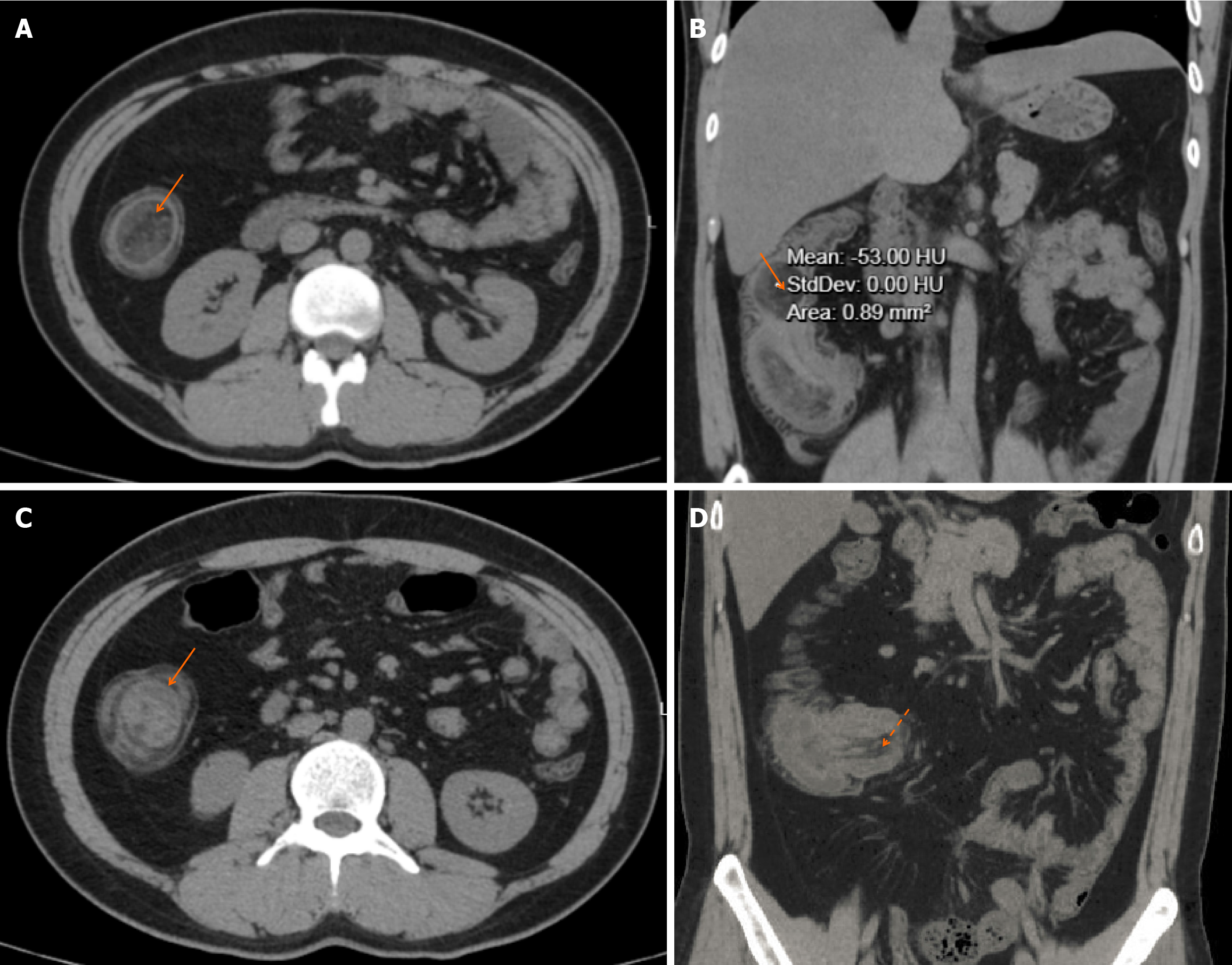
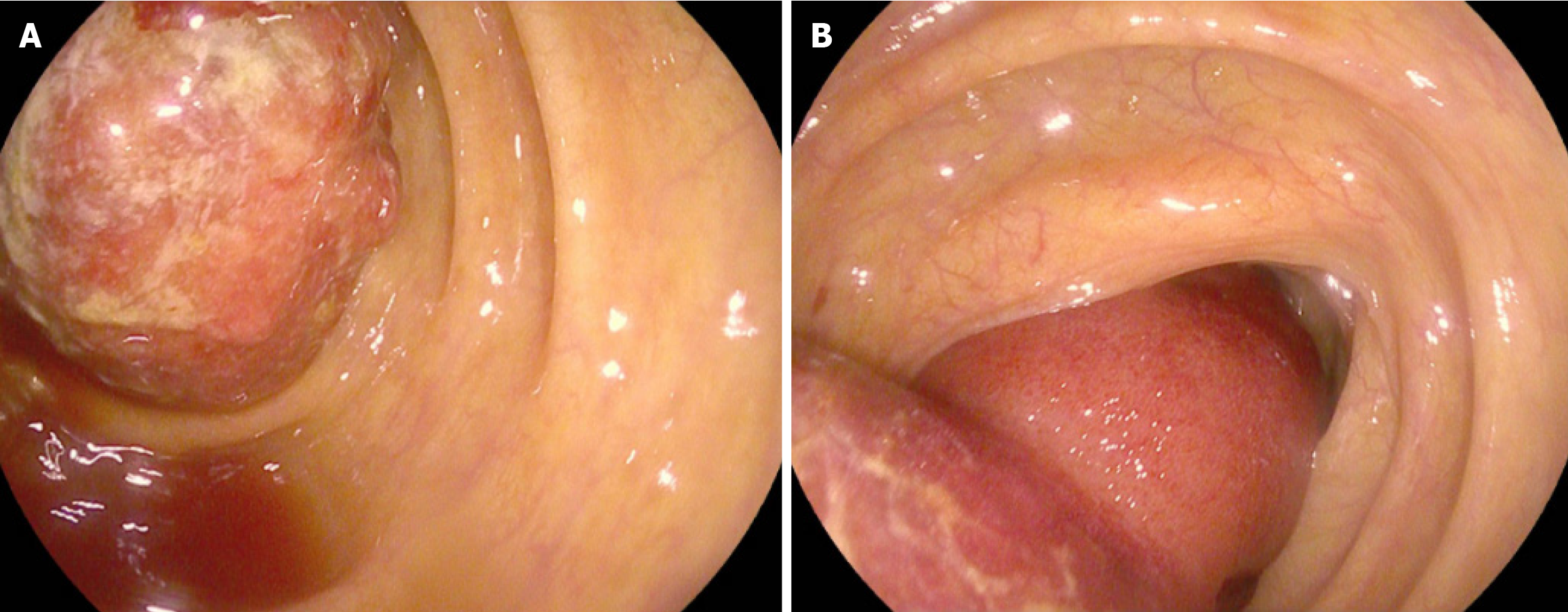
An abdominal CT scan was performed using a 64-row multidetector CT scanner. Non-contrast images were acquired with axial reconstruction at a 2 mm slice thickness, and multiplanar reformations (coronal and sagittal) were generated on the workstation. The CT images demonstrated a classic ileocolic intussusception, with the distal ileum invaginating into the cecum and ascending colon. The intussuscepted segment showed significant concentric wall thickening and edema. A well-defined, oval-shaped mass was identified at the lead point of the intussusception within the ascending colon. This mass exhibited homogeneous fat attenuation, measuring approximately -53 Hounsfield units (HU) (Figure 1A and B), with no evidence of solid soft-tissue components or thick septa, confirming its benign lipomatous nature. Other characteristic signs of intussusception, such as the “target sign” (representing the layered walls of the intussusceptum and intussuscipiens on axial view) (Figure 1C) and the “sausage sign” (representing the elongated intussuscepted bowel loop on coronal view) (Figure 1D), were clearly visualized. There were no CT findings suggestive of bowel ischemia, such as pneumatosis intestinalis or portal venous gas. No pathological lymphadenopathy was observed. A subsequent colonoscopy was performed, which revealed a raised, eroded mass, approximately 4 cm in size, in the ascending colon. This finding represented the lead point of the intussusception (the invaginated terminal ileal segment) that had prolapsed into the colonic lumen, rather than a primary colonic lesion. The mass appeared continuous with the terminal ileum upon deeper insertion (Figure 2).
Ileal lipoma complicated by ileocolic intussusception.
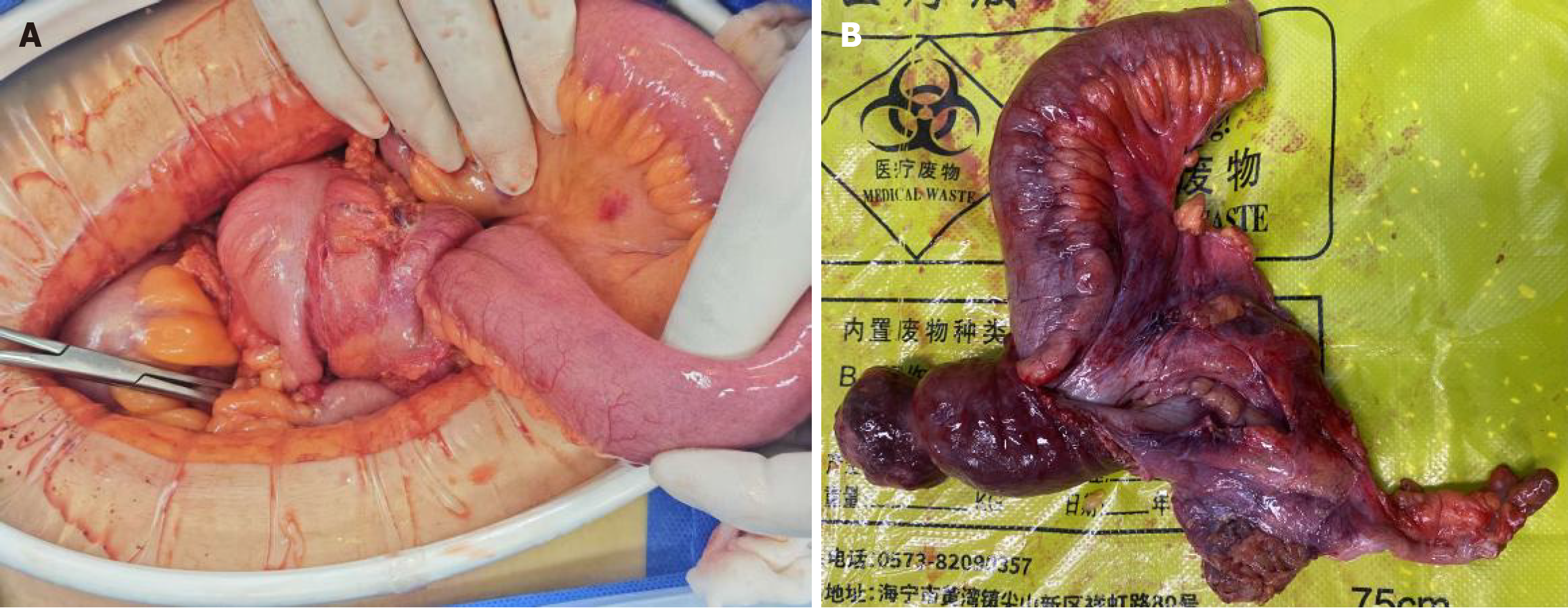
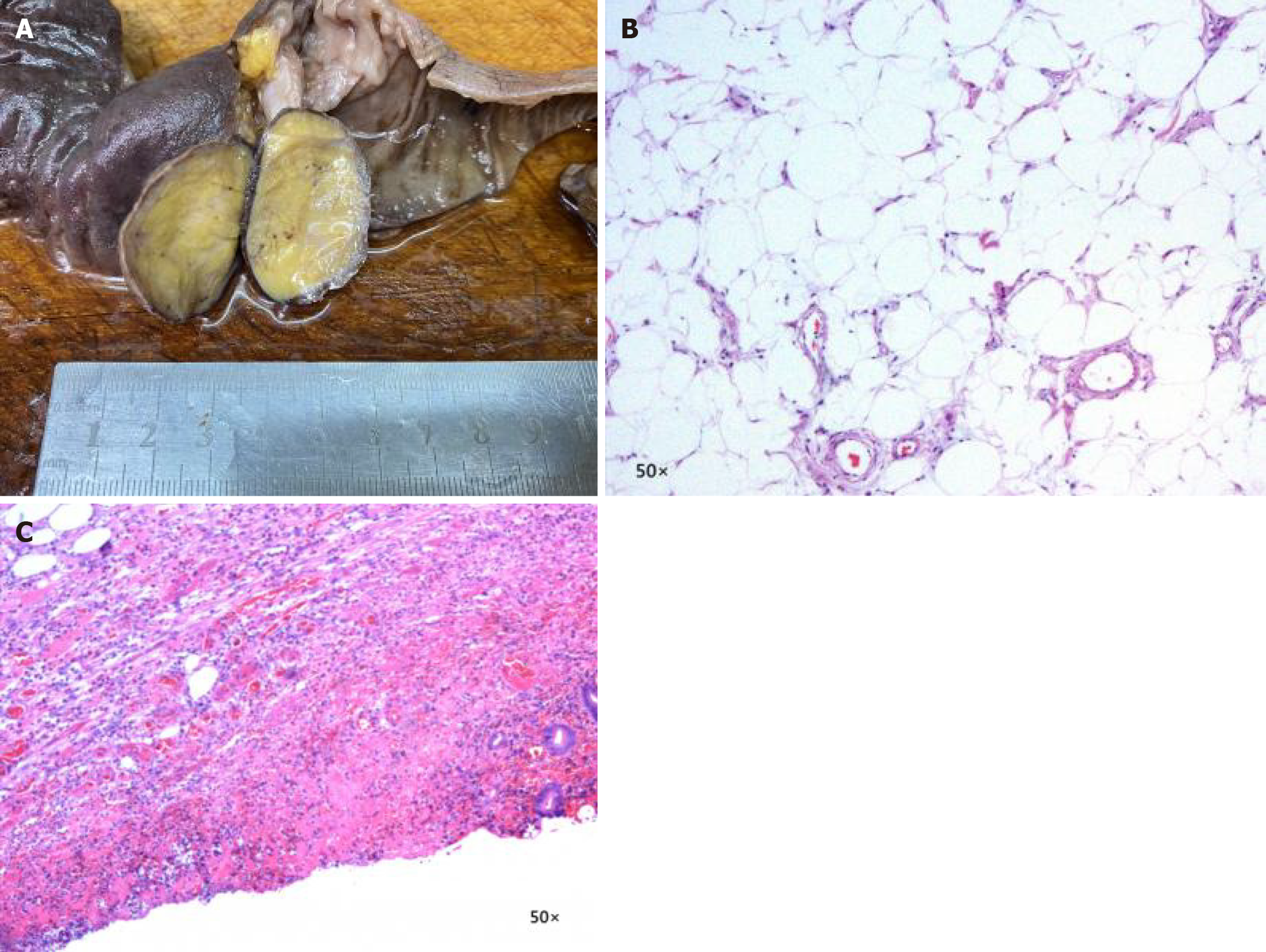
On the day of admission, the patient underwent an emergency exploratory laparotomy under general anesthesia. Intraoperatively, approximately 100 mL of light-yellow ascitic fluid was found in the peritoneal cavity. A segment of the terminal ileum was found to be invaginated into the cecum and ascending colon for approximately 10 cm, causing an ileocolic intussusception (Figure 3). The intussusception was tight, and manual reduction was attempted but unsuccessful due to the degree of edema and impaction. Given the inability to reduce the segment and the clear preoperative imaging suggesting a benign lipoma, an en-bloc ileocecal resection was performed, followed by a side-to-side ileocolic anastomosis. Gross examination of the resected specimen revealed a well-circumscribed, oval-shaped submucosal mass in the ileum, measuring 4.0 cm × 3.0 cm × 2.5 cm, with an intact capsule. The cut surface was pale yellow, solid, and soft (Figure 4A). Histopathological examination confirmed that the tumor was composed of mature adipocytes, consistent with a submucosal lipoma (Figure 4B). The overlying mucosa showed areas of erosion and ulceration (Figure 4C).
The patient developed a postoperative wound infection, which was managed with dressing changes. He was discharged on postoperative day 12 in good condition, with no signs of intestinal obstruction or intra-abdominal bleeding. At the five-month follow-up, the patient reported complete resolution of his presenting symptoms, including abdominal pain, distension, and hematochezia. He remained well with no signs of recurrent intussusception, obstruction, or bleeding.
The patient's clinical course was as follows: He presented to our hospital on day 7 of symptoms with progressive abdominal pain and distension (onset day 1-7) and dark red hematochezia (onset day 4-7). On the day of admission (day 7), abdominal CT and colonoscopy were performed, revealing ileocolic intussusception with a fat-density lead point. Emergency exploratory laparotomy and ileocecal resection were undertaken on the same day. Postoperatively, the patient developed a superficial wound infection, which was managed with dressing changes (day 8-19). He was discharged on postoperative day 12 (day 19 from symptom onset) in good condition, with no signs of intestinal obstruction or intra-abdominal bleeding. At the five-month follow-up, the patient remained asymptomatic with no evidence of recurrence.
The incidence of intussusception is low in adults, accounting for only 1%-5% of all cases of intestinal obstruction. In contrast to the situation in children, 70%-90% of adult intussusception cases have a definitive etiology, such as polyps, tumors, or Meckel’s diverticulum[1,2]. Gastrointestinal tumors are the leading cause of intussusception in adults, with the majority of them being malignant. Among benign causes, lipomas are the most common, accounting for approximately 5% of all benign gastrointestinal tumors. Although these tumors are histologically benign and slow-growing, their rarity and nonspecific presentation often make preoperative diagnosis challenging. They predominantly affect older adults, with a peak incidence seen between 50 years and 70 years of age. Notably, the prevalence is higher in women. Lipomas can occur anywhere in the gastrointestinal tract: Colonic lipomas account for 65%-75%, SILs for 20%-25%, and gastric lipomas for 5%[3,4]. Based on their location within the bowel wall, these tumors are classified as submucosal, intramural, or subserosal. Over 90% are submucosal, most commonly projecting into the lumen, with a very small number being located on the serosal surface. The etiology remains unclear but they may be associated with factors such as abnormal intestinal rotation during embryonic development, inflammatory stimulation, connective tissue degeneration, fatty infiltration around the fibrous trabeculae, disorders of fat metabolism, and Whipple’s disease.
The clinical symptoms of SIL primarily depend on the tumor’s size, morphology, and location. SILs with a maximum diameter of < 1 cm are usually asymptomatic. When the diameter exceeds 2 cm, repeated hematochezia may occur because of erosion or ulceration of the overlying mucosa, and when the maximum diameter is > 4 cm, intussusception often occurs (particularly in those with pedunculated lipomas), leading to varying degrees of intestinal obstruction[5]. Intussusception is the most common complication of SIL. Ileal lipomas often occur in the terminal ileum, where they frequently cause ileocolic intussusception. Therefore, when obstruction of the terminal small intestine is present, the possibility of ileal lipoma-induced intussusception should be considered. Most cases are asymptomatic in their early stages, making early diagnosis extremely difficult; the majority of patients are diagnosed only after developing complications like intussusception, which are typically confirmed through emergency surgery and subsequent pathological examination.
Traditional diagnostic methods (e.g., X-ray, ultrasound, and endoscopy) for SILs have certain limitations. Endoscopically, the tumor surface is smooth and soft, sometimes with erosion and/or ulceration. Because the tumor is usually located in the submucosa and biopsies taken during colonoscopy or enteroscopy often fail to obtain tissue from submucosal lesions, pathological examination may only reveal normal or inflamed mucosa. Abdominal CT is a crucial diagnostic tool for SIL. Because of its characteristic fatty composition, SIL appears on CT images as a well-circumscribed, round or oval, homogeneous fat-density mass within the bowel lumen. The CT findings of intussusception caused by intestinal lipoma are generally similar to those of intussusception resulting from other tumors or non-tumorous causes, such as the “concentric ring sign”, “target sign”, or “sausage sign” formed by the intussusceptum and the intussuscipiens, as well as varying degrees of bowel wall thickening and edema in the intussuscepted segment. The most important trait that differentiates SIL from other causes is the presence of a well-defined fat-density mass at the apex of the intussusception[6].
Radiological differential diagnosis of the lead point is crucial for guiding management. While the presence of a fat-density mass at the apex of the intussusception is pathognomonic for a lipoma, other lead points must be considered. Adenocarcinoma, the most common malignant cause, typically appears as a soft-tissue mass with heterogeneous enhancement, often causing shouldering or annular thickening. Lymphoma can present as a homogeneous, soft-tissue mass with mild enhancement, sometimes associated with bulky lymphadenopathy. Inflammatory masses (e.g., from Crohn’s disease) or a Meckel's diverticulum would show soft-tissue attenuation and associated inflammatory changes in the mesentery. In our case, the diagnosis of a lipoma was favored preoperatively due to the lesion’s pathognomonic homogeneous fat attenuation, smooth, well-circumscribed margins, and the absence of any enhancing soft-tissue component or suspicious lymph nodes. Furthermore, by tracing the intussusceptum back to the distal ileum, CT was able to accurately localize the origin of the lipoma to the terminal ileum, despite the mass being visualized within the colonic lumen on both CT and colonoscopy.
The primary treatment for SIL is surgical resection of the lesion. For smaller tumors, local excision or wedge resection may be performed. For larger tumors, multiple lesions, or cases of intussusception compromising bowel viability, segmental intestinal resection with anastomosis is required. It is reported that SILs can be treated with endoscopic and laparoscopic techniques[7-9]. SILs require no postoperative chemotherapy, and have a good prognosis.
This case underscores several key radiological teaching points for clinicians and radiologists. First, recognizing intussusception on CT is straightforward when classic signs are present: The “target sign” and the “sausage sign” are confirmatory findings. Second, a diligent search for the lead point is mandatory. The presence of a well-defined, homogeneous fat-density mass at the apex of the intussusception is pathognomonic for a lipoma, enabling a confident preoperative diagnosis of a benign etiology. Third, CT is crucial for assessing “red flag” signs that would alter mana
Ileal lipoma is a rare but important cause of adult intussusception, often presenting with nonspecific symptoms that delay diagnosis. Abdominal CT plays a critical role in its preoperative evaluation by accurately localizing the lipoma and delineating the intussusception anatomy. Surgical resection remains the definitive treatment, and timely intervention typically yields favorable outcomes.
| 1. | Chiang JM, Lin YS. Tumor spectrum of adult intussusception. J Surg Oncol. 2008;98:444-447. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 90] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 2. | Mouaqit O, Hasnai H, Chbani L, Benjelloun B, El Bouhaddouti H, Ibn El Majdoub K, Toughrai I, Laalim SA, Oussaden A, Maazaz K, Amarti A, Taleb KA. Adult intussusceptions caused by a lipoma in the jejunum: report of a case and review of the literature. World J Emerg Surg. 2012;7:28. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 15] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 3. | Balmadrid B, Gluck M. Chronic iron deficiency anemia caused by small-bowel lipoma. Gastrointest Endosc. 2014;79:678-679; discussion 679. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 4. | Dong QJ, Tang Y, Zhang CL, Li XG, Chen X, Wang Y. Role of clinical and multidetector computed tomography (MDCT) features in the prediction of patients with intestinal lipoma developing intussusception. Quant Imaging Med Surg. 2024;14:3939-3950. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 5. | Balamoun H, Doughan S. Ileal lipoma - a rare cause of ileocolic intussusception in adults: Case report and literature review. World J Gastrointest Surg. 2011;3:13-15. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 18] [Cited by in RCA: 15] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 6. | Dogra S, Wei J, Wadowski B, Devi-Chou V, Krowsoski L, Shah RR. Terminal Ileum Lipoma Causing Ileocolic Intussusception: A Case Report and Literature Review. Cureus. 2023;15:e49562. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 7. | Shimazaki J, Nakachi T, Tabuchi T, Suzuki S, Ubukata H, Tabuchi T. Laparoscopic management of an octogenarian adult intussusception caused by an ileal lipoma suspected preoperatively: a case report. World J Surg Oncol. 2015;13:75. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 8. | Jiang K, Stephen FO, Jeong D, Pimiento JM. Pancreatic and Gastric Heterotopia with Associated Submucosal Lipoma Presenting as a 7-cm Obstructive Tumor of the Ileum: Resection with Double Balloon Enteroscopy. Case Rep Gastroenterol. 2015;9:233-240. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 13] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 9. | Sun X, Zhao Z, Li R. Endoscopic submucosal dissection of a huge lipoma of ileum assisted with in-vivo traction. Endoscopy. 2025;57:E629-E630. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |