Copyright: ©Author(s) 2026.
World J Radiol. Apr 28, 2026; 18(4): 118196
Published online Apr 28, 2026. doi: 10.4329/wjr.v18.i4.118196
Published online Apr 28, 2026. doi: 10.4329/wjr.v18.i4.118196
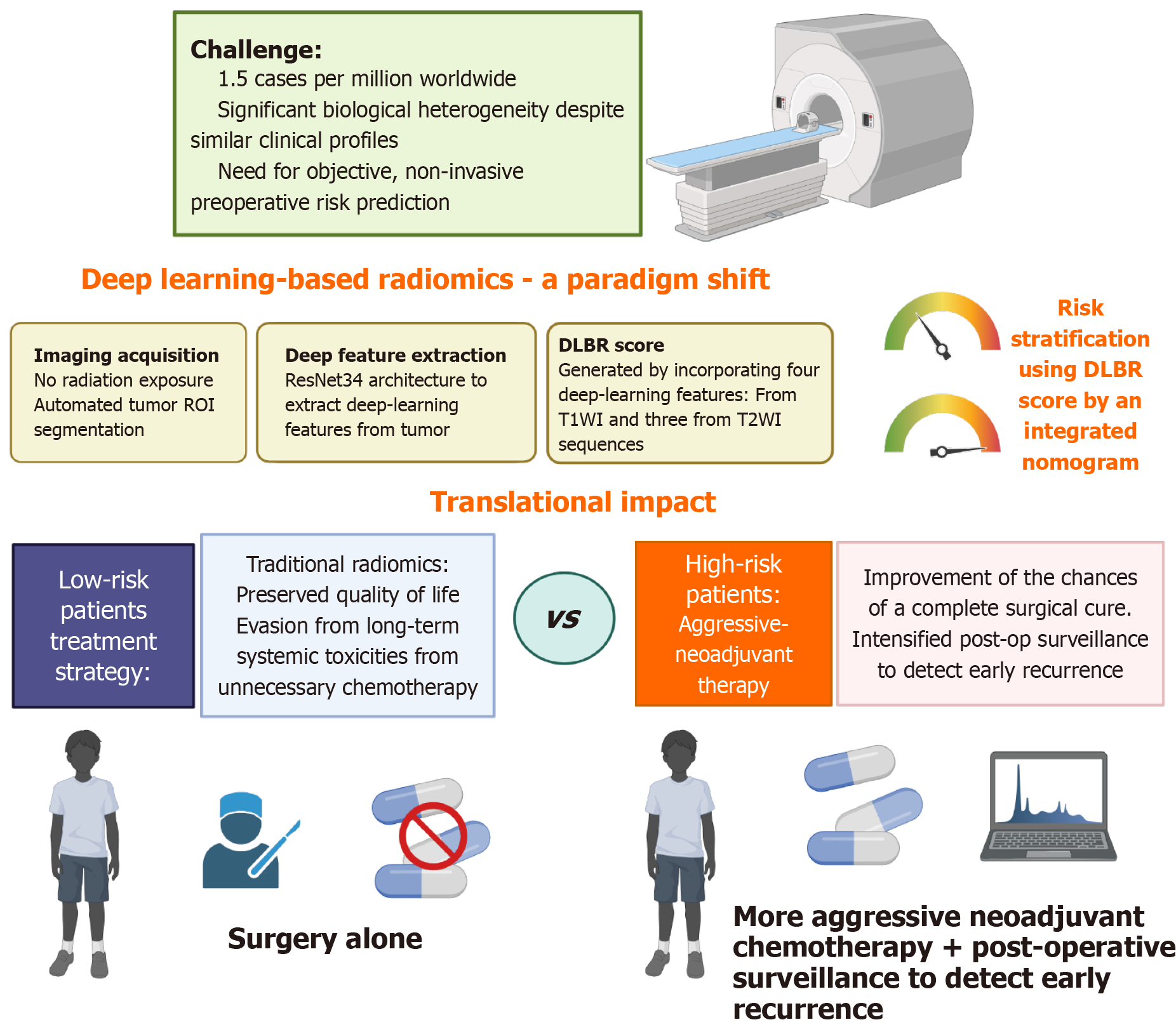
Figure 1 Based on the study results, the figure illustrates a diagnostic paradigm shift where a magnetic resonance imaging derived deep-learning radiomics score, calculated from four key T1/T2 characteristics via ResNet34, provides a quantitative biological signature of hepatoblastoma heterogeneity.
When integrated with traditional markers like AFP and PRETEXT stage into a prognostic nomogram, the model identifies high-risk patients requiring aggressive neoadjuvant therapy and intensified surveillance, while conversely identifying low-risk candidates for surgery alone to avoid adjuvant chemotherapy causing cardio or ototoxicities. Created in https://BioRender.com/di4ajz9.
- Citation: Chowdhury U, Mahajan AA, Kavitha MS, Rajendran RL, Gangadaran P, Ahn BC. Letter to the Editor: Magnetic resonance imaging-based deep learning radiomics for preoperative risk stratification in pediatric hepatoblastoma. World J Radiol 2026; 18(4): 118196
- URL: https://www.wjgnet.com/1949-8470/full/v18/i4/118196.htm
- DOI: https://dx.doi.org/10.4329/wjr.v18.i4.118196