Published online Apr 26, 2026. doi: 10.4330/wjc.v18.i4.118546
Revised: January 28, 2026
Accepted: February 25, 2026
Published online: April 26, 2026
Processing time: 99 Days and 12 Hours
Vascular rings are rare congenital anomalies of the aortic arch system that encircle and compress the trachea and esophagus, leading to respiratory and feeding symptoms that may mimic more common pediatric conditions. Delayed diagnosis remains a challenge, particularly in patients presenting beyond the neonatal pe
To describe the clinical presentation, diagnostic approach, anatomical characteristics, surgical management, and postoperative outcomes of pediatric patients diagnosed with complete and incomplete vascular rings at a tertiary referral center.
We conducted a retrospective study of patients diagnosed with vascular rings at the Children’s Heart Center of the American University of Beirut Medical Center between January 2010 and December 2025. All patients underwent transthoracic echocardiography and computed tomography angiography for diagnostic confirmation and surgical planning.
Eight patients were identified, of whom three (37.5%) were male. The mean age at time of procedure was 17.5 months (range: 8 days to 38 months). Feeding difficulties and chronic respiratory symptoms were the most common presenting features (both 75%). Three patients (37.5%) had associated intracardiac anomalies. Double aortic arch was the most frequent anatomical subtype (50%), followed by right aortic arch with aberrant left subclavian artery (37.5%). All patients underwent surgical repair, with cardiopulmonary bypass required in two cases. There were no operative or in-hospital deaths. Two neonates developed postoperative tracheomalacia. During a mean follow-up of 32 months, complete symptom resolution was observed in 50% of patients, while the remainder demonstrated significant clinical improvement.
Vascular rings remain an important but often underrecognized cause of airway and esophageal compression in infants and young children. Delayed presentation was common in this cohort, underscoring the need for hei
Core Tip: Vascular rings are rare congenital aortic arch anomalies that frequently present with nonspecific respiratory and feeding symptoms, leading to delayed diagnosis. This single-center retrospective study provides a comprehensive clinical and surgical overview of pediatric vascular rings, distinguished by extensive multimodal imaging. High-quality transthoracic echocardiography, three-dimensional computed tomography angiography, and selective angiography clearly demonstrate anatomical subtypes and airway relationships. These detailed visual findings, combined with favorable surgical outcomes, emphasize the diagnostic value of advanced imaging and reinforce the importance of early recognition and timely intervention.
- Citation: Abdul Khalek J, Kanbar K, Zareef R, Alzein MH, El-Rassi I, Bitar FF, Arabi MT. Vascular rings in a tertiary care center: A retrospective review of clinical presentations and interventions. World J Cardiol 2026; 18(4): 118546
- URL: https://www.wjgnet.com/1949-8462/full/v18/i4/118546.htm
- DOI: https://dx.doi.org/10.4330/wjc.v18.i4.118546
Vascular rings are a group of rare congenital anomalies of the aortic arch system in which the trachea and esophagus are encircled by vascular structures, leading to varying degrees of airway and esophageal compression[1]. These anomalies arise from abnormal regression or persistence of embryonic aortic arches during fetal development[2]. The resulting compression can cause respiratory distress, stridor, chronic cough, recurrent respiratory infections, dysphagia, and feeding difficulties[3]. Because these symptoms often mimic more common pediatric conditions such as asthma or gastroesophageal reflux disease, diagnosis may be delayed or overlooked[4].
The true incidence of vascular rings is estimated to be less than 1% of all congenital heart defects[5]. Despite their rarity, they represent an important cause of airway obstruction in infants and young children. The severity of symptoms depends on the specific anatomical subtype, with double aortic arch (DAA) and right aortic arch (RAA) with aberrant left subclavian artery (LSA) being the most common variants.
Accurate diagnosis requires a high index of suspicion and the use of modern imaging modalities. Transthoracic echocardiography (TTE) is often the initial diagnostic tool, while computed tomography (CT) angiography provides detailed anatomical visualization necessary for surgical planning[6]. Bronchoscopy may also be useful in assessing the degree of tracheal compression or associated tracheomalacia[7]. Surgical correction remains the cornerstone of ma
This study reviews the clinical presentation, diagnostic evaluation, and management of vascular rings, highlighting their anatomical diversity and underscoring the importance of timely recognition and multidisciplinary assessment in optimizing patient outcomes.
This retrospective study was conducted at the Children’s Heart Center of the American University of Beirut Medical Center. The study protocol was approved by the Institutional Review Board of the American University of Beirut Medical Center (Approval No: BIO-2025-0296).
Medical records of patients diagnosed with vascular rings between January 2010 and December 2025 were re
Data were extracted from electronic medical records, operative reports, and institutional imaging archives. Collected variables included demographic characteristics, age at surgery, clinical manifestations, associated cardiac and extracardiac anomalies, diagnostic modalities, anatomical subtype of vascular ring, surgical approach, perioperative details, and postoperative outcomes.
All patients underwent initial evaluation with TTE as a screening modality. CT angiography (CTA) was performed in all cases for definitive anatomical delineation of the vascular ring and its relationship to the trachea and esophagus.
Surgical repair was performed via left thoracotomy or median sternotomy, depending on vascular anatomy and the presence of associated intracardiac lesions requiring concomitant repair. Cardiopulmonary bypass was employed in cases necessitating correction of associated cardiac defects.
Postoperative outcomes assessed included duration of mechanical ventilation, length of hospital stay, and the occurrence of complications, including persistent respiratory symptoms or tracheomalacia. Resolution of symptoms was assessed retrospectively through review of clinical documentation in follow-up clinic notes. Resolution of respiratory symptoms was defined as the absence of previously documented respiratory complaints, including stridor, wheezing, recurrent respiratory tract infections, or respiratory distress, with no ongoing requirement for bronchodilator therapy or respiratory-related hospitalizations. Resolution of feeding symptoms was defined as the absence of dysphagia, choking, or aspiration as documented in follow-up visits, with tolerance of age-appropriate oral intake and clinical improvement in feeding-related concerns, accompanied by stabilization or improvement in growth parameters when available.
Descriptive statistical analysis was performed using Microsoft Excel. Categorical variables are presented as frequencies and percentages, while continuous variables are reported as means with ranges.
Over the study period, eight patients were diagnosed with vascular rings. Demographic and clinical characteristics are summarized in Table 1. Three patients (37.5%) were male. The mean age for surgery was 17.5 months (range: 8 days to 38 months), with most patients presenting beyond the neonatal period. Feeding difficulties were the most common presenting symptom (n = 6, 75%), followed by chronic respiratory symptoms (n = 6, 75%) and failure to thrive (n = 4, 50%). One patient had chronic wheezing, and another had been diagnosed with asthma. Associated intracardiac anomalies were identified in three patients (37.5%). None of the patients had a recognized genetic syndrome, dysmorphic features, or associated extracardiac congenital malformations. The absence of recognized genetic or syndromic conditions in this cohort was based on clinical evaluation and no patients demonstrated features prompting further genetic investigation.
| Patient | Sex | Age at surgery | Primary diagnosis | Weight at surgery (kg) | Associated intracardiac lesions | Feeding difficulties | Failure to thrive | Other pertinent symptoms | Tracheal/esophageal position at presentation |
| 1 | M | 38 months | DAA | 16 | None | No | No | Asthma, recurrent RTI including PNA at birth requiring 3-day ICU admission, breath-holding spells | Midline- an external indentation on the right side of the trachea with mild narrowing |
| 2 | F | 17 months | RAA with aberrant LSA from DA, left retroesophageal ligamentum arteriosum | 7 | ASD, VSD | Yes | Yes | Voice hoarseness | Midline- no deviation; mild indentation of proximal esophagus |
| 3 | F | 8 days | DAA | 2.92 | Large PFO | Yes | No | Recurrent RTI, stridor, perioral cyanosis | Significant tracheal narrowing with a minimum transverse tracheal diameter of 2 mm. Impression on proximal esophagus |
| 4 | F | 1 month | RAA with aberrant LSA from DA, with diverticulum of Kommerell, a tiny left ductus arteriosus originating from aberrant LSA | 2.8 | VSD, small PFO | No | No | Recurrent RTI, stridor | Right upper lobe bronchus arising from the trachea; impingement of the right pulmonary artery along the distal carina; mild narrowing of the trachea |
| 5 | F | 3 years | DAA | 13 | None | Yes | Yes | Chronic cough, GERD, stridor, chronic wheezing | Impression on the right side of the trachea |
| 6 | F | 16 months | RAA with aberrant LSA from DA and left ligamentum arteriosum | 8 | ASD | Yes | Yes | Easy fatigability, perioral cyanosis | Midline - no deviation or narrowing |
| 7 | M | 5 months | LAA with aberrant RSA from DA, and left ligamentum arteriosum | 6.3 | None | Yes | No | Recurrent aspiration, GERD, cyanosis | Midline - no deviation |
| 8 | M | 21 months | DAA | 11.4 | None | Yes | Yes | Recurrent RTI requiring multiple hospitalizations, stridor, dysphagia | Midline - significant tracheal narrowing |
Delayed diagnosis was inferred based on the presence of persistent respiratory and/or feeding symptoms affecting quality of life and the absence of early definitive diagnosis during routine clinical or cardiac evaluation. Overall, 6 of 8 patients (75%) presented beyond the neonatal period, and 5 patients (62.5%) were diagnosed after one year of age. Prior to definitive diagnosis, 5 patients (62.5%) experienced recurrent respiratory tract infections, pneumonia, or repeated pulmonary symptoms, with 2 patients (25%) requiring multiple hospital admissions or neonatal intensive care. Symptom attribution to alternative diagnoses was common, including asthma-like symptoms or wheezing in 2 patients (25%) and gastroesophageal reflux–related symptoms in 2 patients (25%). Notably, markers of significant airway or feeding compromise were present prior to diagnosis, including stridor in 3 patients (37.5%), cyanosis or perioral cyanosis in 3 patients (37.5%), and aspiration in 1 patient (12.5%), underscoring the clinical impact of delayed recognition.
All patients underwent surgical repair. DAA was the most common anatomical subtype (n = 4, 50%), followed by RAA with aberrant LSA arising from the descending aorta (n = 3, 37.5%). Two patients required surgical intervention during the neonatal period, one at 8 days of life due to severe symptoms and another at 28 days, while one patient underwent repair during infancy. The remaining five patients were operated on after one year of age.
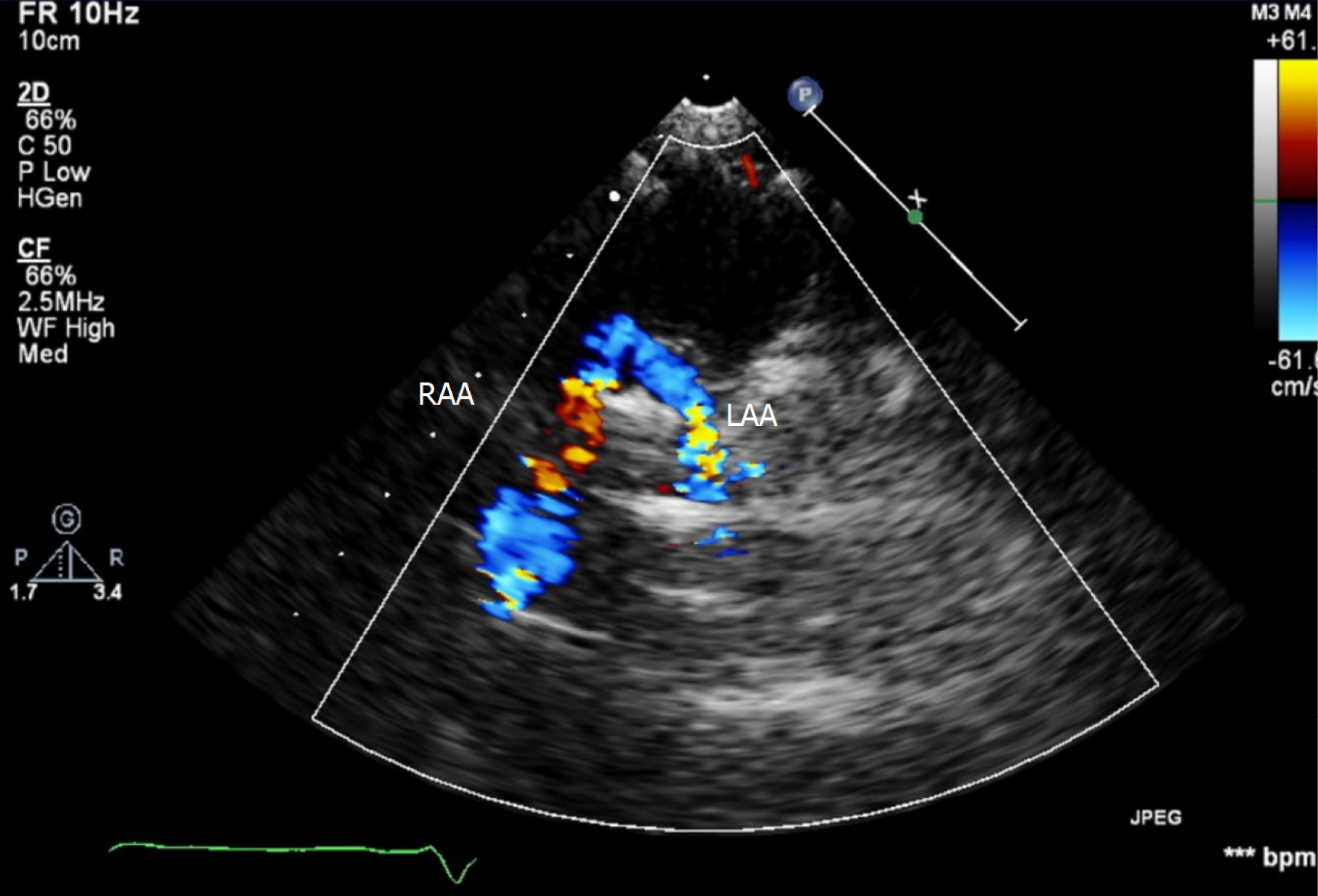
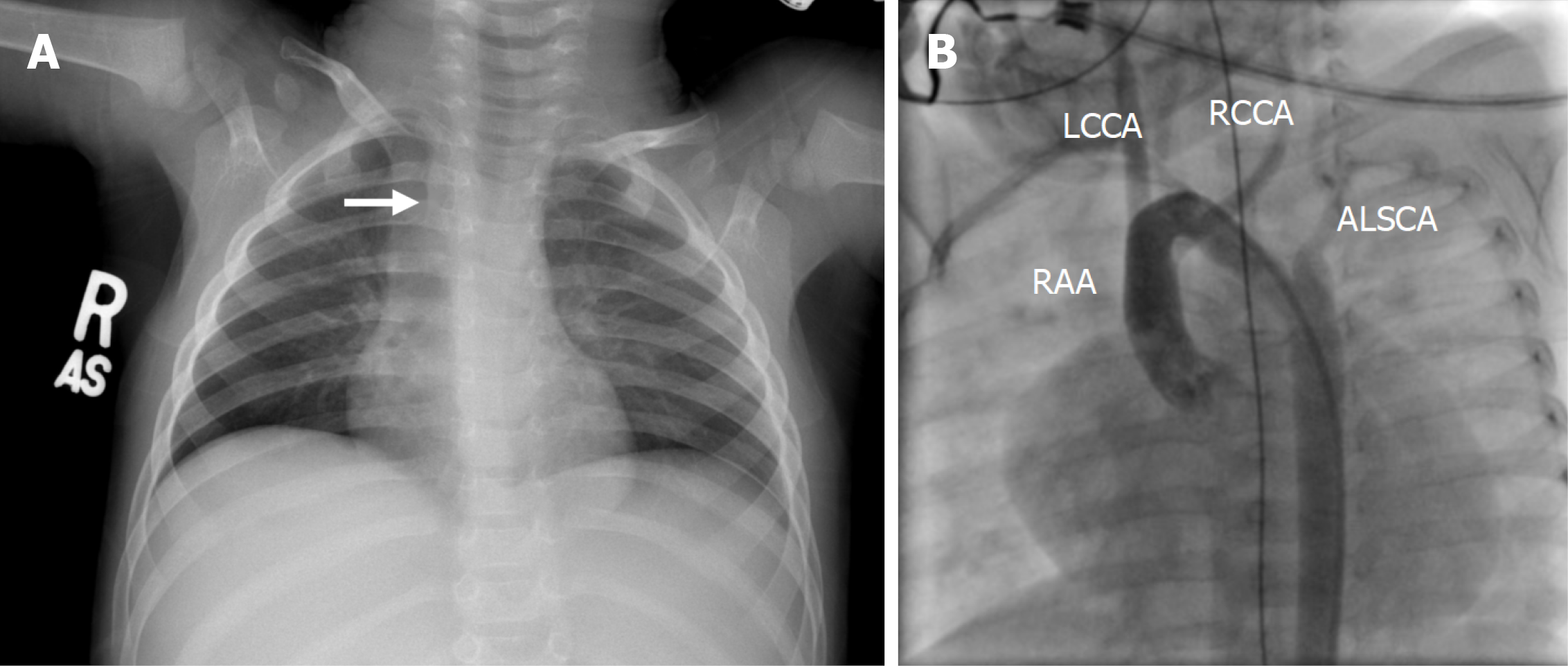
Figure 1 illustrates the echocardiographic findings of a 38-month-old patient with DAA, and Figure 2A shows the corresponding chest radiograph. Notably, this patient had previously been diagnosed with asthma and experienced recurrent respiratory infections requiring multiple antibiotic courses and repeated hospitalizations prior to definitive diagnosis.
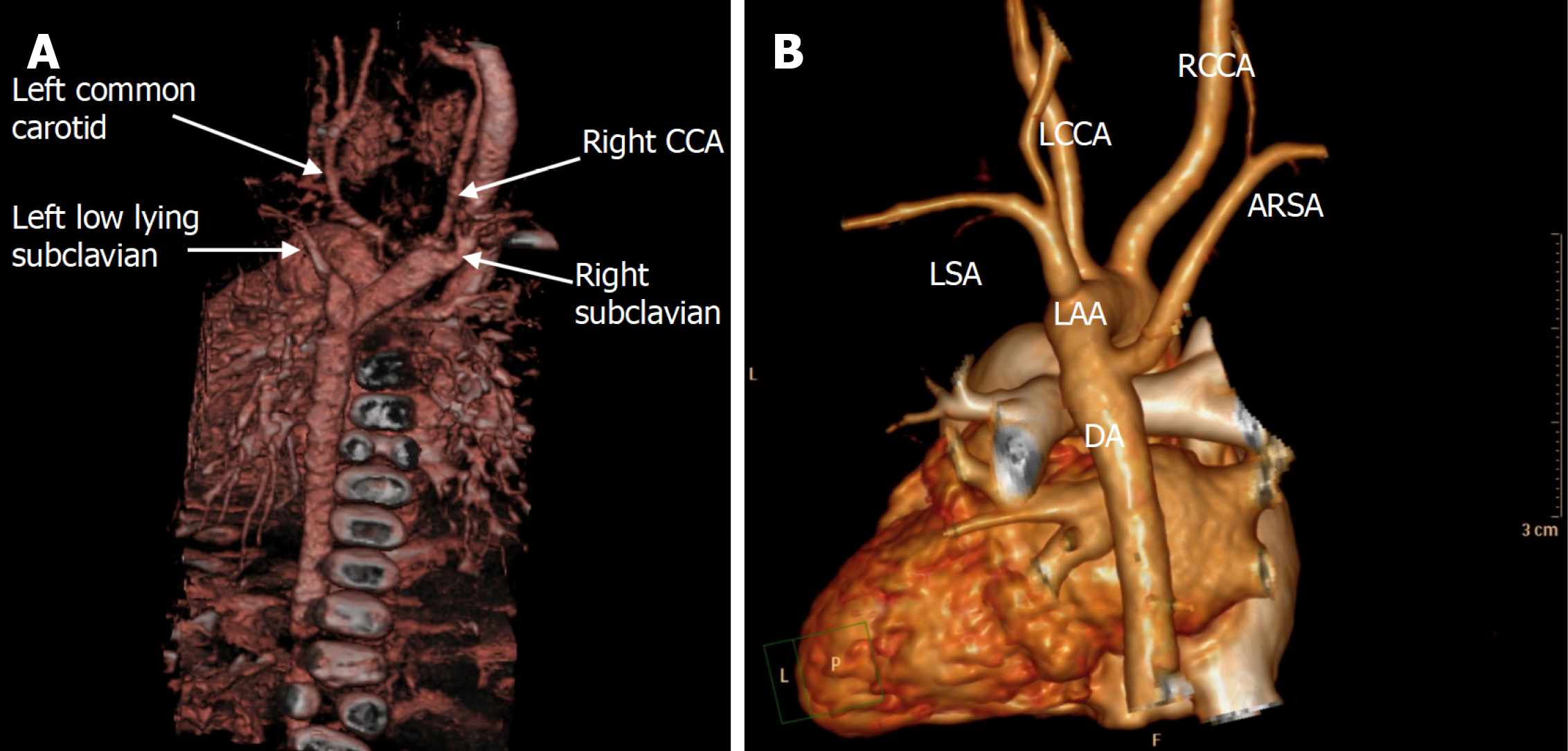
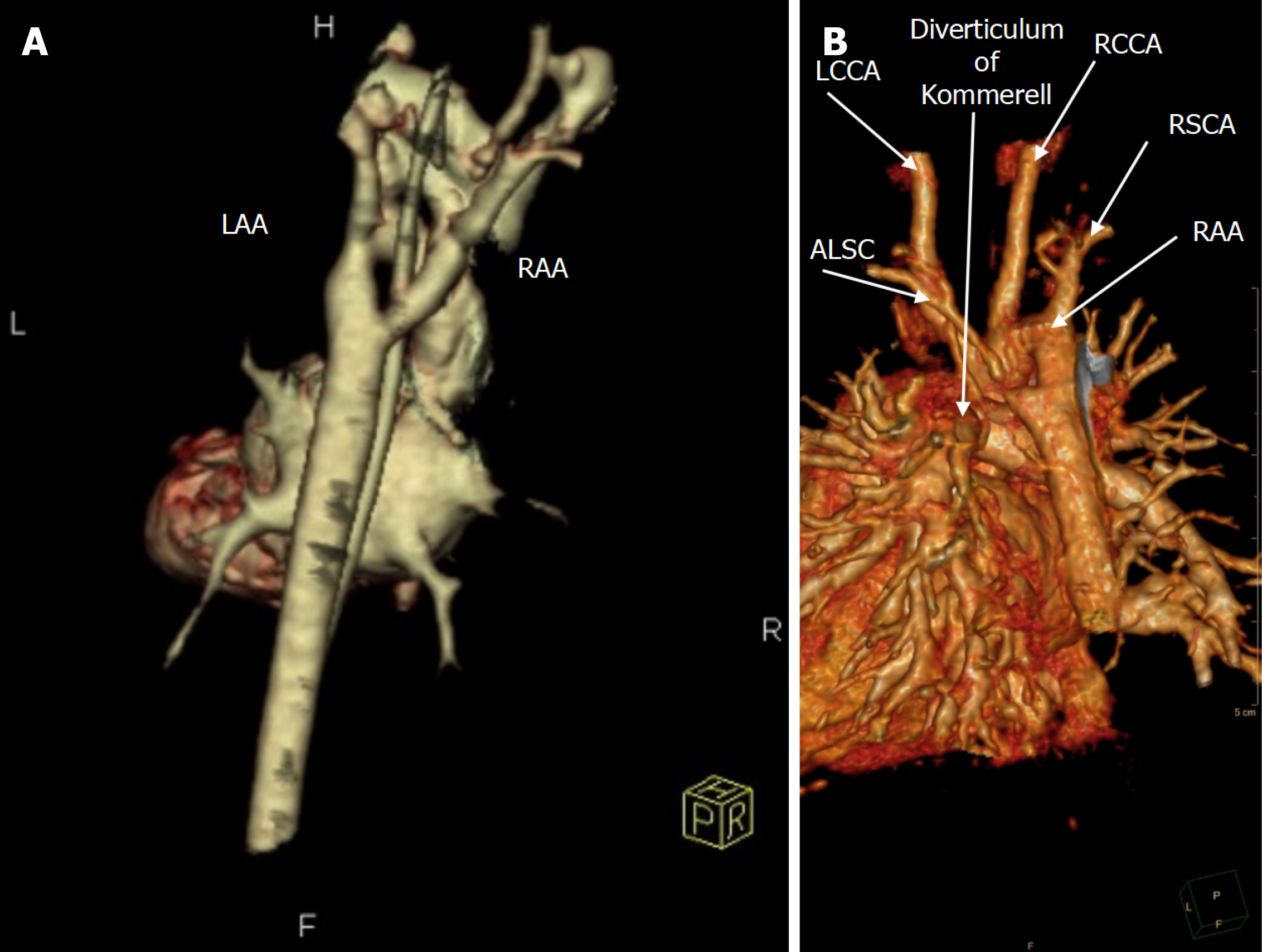
All patients underwent preoperative TTE and CTA for anatomical delineation (Figures 3 and 4). One patient additionally underwent diagnostic cardiac catheterization (Figure 2B).
Operative and postoperative outcomes are summarized in Table 2. Cardiopulmonary bypass was required in three patients (37.5%) to facilitate repair of associated intracardiac defects. Among patients with DAA, transection of the nondominant arch was performed in all cases. In patient 7 [left aortic arch (LAA) with retroesophageal aberrant right subclavian artery (ARSA)], right subclavian artery translocation to the right carotid artery was performed to eliminate the compressive retroesophageal course and address the patient’s significant aerodigestive symptoms. There were no operative or in-hospital deaths. Two neonates developed postoperative tracheomalacia; both were severely symptomatic at presentation and required early surgical intervention. All patients were extubated on the day of surgery.
| Patient | Surgical technique | Dominant arch (for DAA) | Cardiopulmonary bypass used | Hospital stays (day) | Persistent feeding difficulties | Persistent respiratory symptoms |
| 1 | Left posterolateral thoracotomy with division of the ligamentum arteriosum and ligation/division of LAA after delineation of both arches | Right | No | 9 | No | Yes |
| 2 | Median sternotomy with ligation and transection of a long PDA (originating from the aberrant subclavian); banding of main pulmonary artery | Right | Yes | 19 | No | No |
| 3 | Left posterolateral thoracotomy with division of ligamentum arteriosum and ligation/division of abnormal posterior aortic arch | N/A | No | 19 | No | Yes |
| 4 | Median sternotomy with ligation and transection of a long PDA (originating from the aberrant subclavian), and main pulmonary artery banding. Airway was mobilized (trachea/proximal bronchi) after ring release | N/A | No | 20 | Yes | Yes |
| 5 | Left thoracotomy with ligation/transection of the fibrotic PDA followed by transection of the left arch/isthmus (below LSA), with stump management (pleural coverage and posterior fixation of distal stump away from the trachea) | N/A | No | 5 | No | No |
| 6 | Median sternotomy with cardiopulmonary bypass; division/transection of ligamentum arteriosum to relieve the vascular ring, with concomitant ASD closure | Right | Yes | 18 | No | No |
| 7 | Median sternotomy with ligation and transection of the fibrotic PDA to improve exposure and facilitate repair, followed by mobilization, division at origin, and translocation of the aberrant right subclavian artery with end-to-side anastomosis to the right common carotid; the proximal stump was tucked laterally to minimize risk of residual esophageal compression | N/A | No | 7 | No | No |
| 8 | Left posterolateral thoracotomy with transection of the nondominant LAA segment to relieve the vascular ring | Right | Yes | 7 | No | Yes |
Postoperative outcomes were assessed descriptively based on clinical follow-up documentation with a mean follow-up period of 32 months. Overall, complete resolution of all presenting symptoms was observed in 4 of 8 patients (50%), while the remaining patients demonstrated partial but clinically meaningful improvement. Persistent respiratory symptoms at follow-up were documented in 4 of 8 patients (50%). Among patients with complete vascular rings (DAA, n = 4), persistent respiratory symptoms were observed in 3 patients (75%), whereas among those with incomplete vascular rings (n = 4), persistent respiratory symptoms were present in 1 patient (25%). Persistent feeding difficulties were uncommon and were documented in 1 of 8 patients (12.5%) overall. This patient belonged to the incomplete vascular ring group, corresponding to 1-4 patients (25%) with incomplete rings, while no patients with complete vascular rings (0 of 4, 0%) had persistent feeding symptoms at follow-up. Patients who underwent surgical repair during the neonatal or early infant period (n = 2) demonstrated persistent postoperative respiratory symptoms in both cases (100%), whereas among patients operated on later in infancy or early childhood (n = 6), persistent respiratory symptoms were observed in 2 patients (33%). Persistent feeding difficulties were observed in 1 neonate and in no patients operated on at older ages.
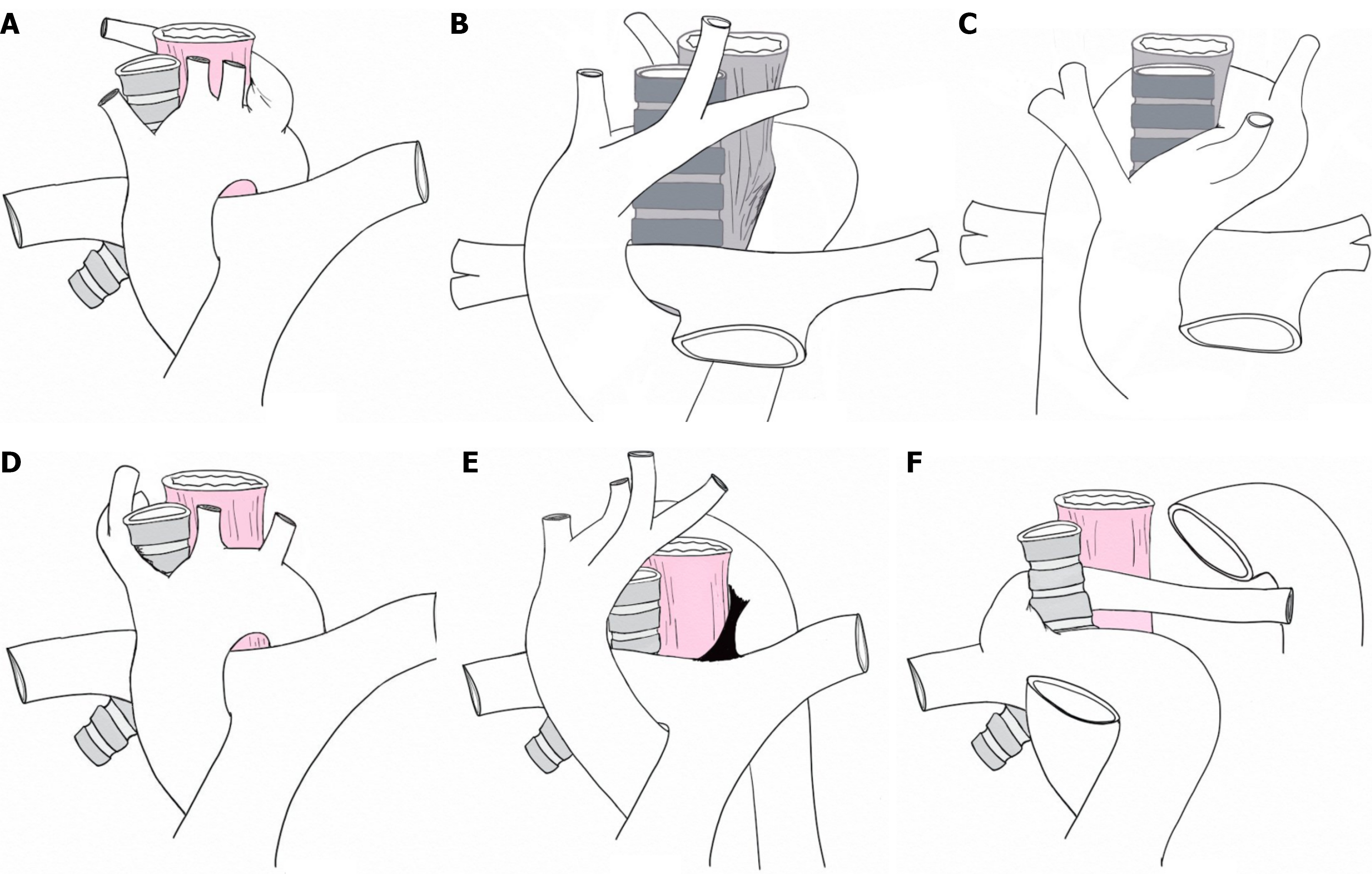
In this study, we described our single-center experience with managing vascular rings in children. Vascular rings are broadly classified into complete and incomplete rings based on the anatomical configuration of the aortic arch and the position of the ligamentum arteriosum or ductus arteriosus (Figure 5). Complete vascular rings include DAA and RAA with left ligamentum arteriosum, both of which fully encircle the airway and esophagus. Incomplete rings, such as LAA with retroesophageal ARSA, pulmonary artery sling, partially encircle these structures and may have a more variable clinical presentation. Variants like RAA with mirror-image branching and retroesophageal ligamentum arteriosum, LAA with right descending thoracic aorta and right ligamentum arteriosum, and left arch with anomalous right brachiocephalic artery represent less common but important subtypes that can form complete or partial rings depending on ligamentum position.
The anatomical distribution in our cohort, with DAA (50%) and RAA with aberrant LSA (37.5%), aligns with the predominant patterns reported in recent literature, where DAA and RAA variants account for the majority of vascular ring cases[8,9]. The incidence of associated intracardiac anomalies in our cohort (37.5%) is slightly higher than reported in the literature, which may reflect regional differences or selection biases[10,11]. Also, the absence of syndromic associations in our cohort contrasts with studies indicating that a significant proportion of vascular ring cases are associated with genetic syndromes[12]. In our cohort, the mean age at surgery was 17.5 months, with surgical repairs performed between 8 days and 38 months of age. This is notably higher than previously reported series in which the median or mean age at repair typically ranges from approximately 3.7 months to 1.04 years[13-15]. This suggests a trend toward later diagnosis and intervention, which may reflect differences in symptom recognition, referral patterns, or healthcare access.
Many patients experienced prolonged respiratory and/or feeding symptoms prior to diagnosis, often with recurrent or progressive manifestations that affected quality of life and led to repeated healthcare encounters. Symptoms were frequently attributed to more common conditions such as asthma, recurrent infections, or gastroesophageal reflux, contributing to diagnostic delay. In several cases, clinically significant airway or feeding compromise was present before definitive diagnosis, highlighting the consequences of delayed recognition and the need for earlier consideration of vascular ring anomalies in children with persistent aerodigestive symptoms.
Respiratory manifestations predominated at presentation, with 75% of patients exhibiting symptoms such as stridor, recurrent respiratory tract infections, or wheezing. This finding is consistent with the literature range, suggesting that respiratory involvement remains the most frequent clinical presentation across published series[10,16]. However, the incidence of feeding difficulties (75%) and failure to thrive (50%) in our cohort was slightly higher than that reported in most published studies, a difference that may be attributable to sample size or delayed presentation or more pronounced esophageal compression at diagnosis.
In terms of follow-up, in our study cohort, 50% of patients achieved complete resolution of their presenting symptoms, while the remainder experienced marked clinical improvement with no reported postoperative mortality. These findings align with existing literature, whereby a meta-analysis for post-operative outcomes in vascular rings reports moderate rates of symptom resolution post-surgery, whereby 33%-40% have persistent symptoms at last follow-up, depending on the type of anomaly[16]. Another more recent study reported similar findings, whereby up to 32% of patients reported persistent respiratory or swallowing difficulties at follow-up a year later[8]. These data underscore the need for continued evaluation of strategies to further reduce residual symptoms and optimize long-term outcomes. In contrast, a recent cohort study of 515 patients reported complete symptom resolution in 94.7% of cases post-surgery, with a low 10-year reoperation rate of 9.6%, a finding not noted in our study[10]. Furthermore, persistent postoperative respiratory symptoms were more frequently observed in patients with complete vascular rings and in those undergoing repair during the neonatal or early infant period. This pattern likely reflects more severe circumferential airway compression and longer-standing preoperative airway compromise in these patients, including the development of tracheomalacia, rather than inadequate surgical relief. In contrast, feeding-related symptoms resolved in the majority of patients, suggesting greater reversibility of esophageal compression following surgical repair.
This study is limited by its small sample size and single-center, retrospective design, reflecting the rarity of vascular rings and precluding meaningful subgroup or comparative analyses by anatomy or age at surgery.
Vascular rings, although rare, represent an important underdiagnosed potential cause of respiratory and feeding difficulties in infants and young children. Our experience highlights a tendency toward delayed presentation, un
| 1. | Umapathi KK, Bokowski JW. Vascular Aortic Arch Ring. 2023 Jul 19. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. [PubMed] |
| 2. | Bae SB, Kang EJ, Choo KS, Lee J, Kim SH, Lim KJ, Kwon H. Aortic Arch Variants and Anomalies: Embryology, Imaging Findings, and Clinical Considerations. J Cardiovasc Imaging. 2022;30:231-262. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 24] [Reference Citation Analysis (0)] |
| 3. | Porcaro F, Ciliberti P, Petreschi F, Secinaro A, Allegorico A, Coretti A, Cutrera R. Long term respiratory morbidity in patients with vascular rings: a review. Ital J Pediatr. 2023;49:24. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 13] [Reference Citation Analysis (0)] |
| 4. | Ceneri NM, Desai MH, Christopher AB, Gerhard EF, Staffa SJ, Zurakowski D, Ramakrishnan K, Donofrio MT. Narrowing Down the Symptomatology of Isolated Vascular Rings in Children. Pediatr Cardiol. 2024;45:416-425. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (1)] |
| 5. | Ruiz-Solano E, Mitchell M. Rings and Slings: Not Such Simple Things. Curr Cardiol Rep. 2022;24:1495-1503. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 6. | Ganie IS, Amod K, Reddy D. Vascular rings: a radiological review of anatomical variations. Cardiovasc J Afr. 2016;27:30-36. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 7. | Yang D, Cascella M. Tracheomalacia. 2023 Jun 26. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. [PubMed] |
| 8. | Farje D, Young A, Stein E, Eltayeb OM, Ghadersohi S, Hazkani I. Persistence of aerodigestive symptoms after vascular ring repair. Am J Otolaryngol. 2024;45:104147. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 9. | François K, Panzer J, De Groote K, Vandekerckhove K, De Wolf D, De Wilde H, Marchau F, De Caluwe W, Benatar A, Bové T. Early and late outcomes after surgical management of congenital vascular rings. Eur J Pediatr. 2017;176:371-377. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 22] [Article Influence: 2.4] [Reference Citation Analysis (1)] |
| 10. | Gikandi A, Chiu P, Crilley N, Brown J, Cole L, Emani S, Fynn Thompson F, Zendejas B, Baird C. Outcomes of Patients Undergoing Surgery for Complete Vascular Rings. J Am Coll Cardiol. 2024;84:1279-1292. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 13] [Reference Citation Analysis (1)] |
| 11. | Said SM, Marey G, Knutson S, Rodgers N, Richtsfeld M, Joy B, Griselli M. Outcomes of Surgical Repair of Vascular Rings and Slings in Children: A Word for the Asymptomatic. Semin Thorac Cardiovasc Surg. 2021;33:492-500. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 17] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 12. | McElhinney DB, Clark BJ 3rd, Weinberg PM, Kenton ML, McDonald-McGinn D, Driscoll DA, Zackai EH, Goldmuntz E. Association of chromosome 22q11 deletion with isolated anomalies of aortic arch laterality and branching. J Am Coll Cardiol. 2001;37:2114-2119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 192] [Cited by in RCA: 185] [Article Influence: 7.4] [Reference Citation Analysis (1)] |
| 13. | Binsalamah ZM, Ibarra C, John R, Zea-Vera R, Adachi I, Imamura M, McKenzie ED, Fraser CD Jr, Mery CM, Heinle JS. Contemporary Midterm Outcomes in Pediatric Patients Undergoing Vascular Ring Repair. Ann Thorac Surg. 2020;109:566-572. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 24] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 14. | Yu D, Guo Z, You X, Peng W, Qi J, Sun J, Wu K, Li X, Mo X. Long-term outcomes in children undergoing vascular ring division: a multi-institution experience. Eur J Cardiothorac Surg. 2022;61:605-613. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 23] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 15. | Wang C, Chen B, Chen J, Luo J, Yang G, Yi L, Deng X. Surgical treatment of double aortic arch in infants. Front Pediatr. 2025;13:1622525. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 16. | Rato J, Zidere V, François K, Boon M, Depypere A, Simpson JM, Speggiorin S, Vigneswaran TV. Post-operative Outcomes for Vascular Rings: A Systematic Review and Meta-analysis. J Pediatr Surg. 2023;58:1744-1753. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |