Published online Apr 26, 2026. doi: 10.4330/wjc.v18.i4.118431
Revised: January 8, 2026
Accepted: January 28, 2026
Published online: April 26, 2026
Processing time: 103 Days and 19.3 Hours
The release of serum cardiac troponins (cTn) following major non-cardiac surgery (MNCS) is associated with significant adverse postoperative outcomes. This phenomenon comprises myocardial injury after non-cardiac surgery (MINS) or perioperative myocardial infarction that may occur regardless of the presence of obstructive coronary artery disease (CAD). However, there is no consensus on its diagnostic criteria or therapeutic guidelines. The 30-day mortality following MNCS is 2%-6% and more than half of these deaths are attributable to the major adverse cardiovascular events (MACEs). Although MINS is an independent predictor of MACEs, it is not the only prognostic tool. The release of cTn may be secondary to perioperative tachycardia, hypotension, anemia, hypoxia, sepsis, inflammation, and profound stress. In the latter, an adrenergic surge, independent of underlying CAD, can cause a noticeable release of cTn. Even low levels of cTn elevation within the first three days after high-risk surgery are correlated with a significant increase in the short- and long-term mortality rates. Therefore, awa
Core Tip: The Major non-cardiac surgery is associated with a significant risk of perioperative mortality. This adverse outcome relies mainly on the occurrence of myocardial injury in the perioperative settings. Myocardial injury after non-cardiac surgery remains widely unrecognized, partly because there is no universal consensus on its definition and diagnostic criteria. However, a working diagnosis can be established based on an elevated post-operative cardiac troponin level within 30 days of surgery after excluding other non-ischemic causes, regardless of whether the patient has symptoms or electrocardiogram findings. There is growing consensus for proactive surveillance to mitigate the burden of perioperative car
- Citation: El-Menyar A. Unwanted silent crosstalk: Troponinemia and surgeons. World J Cardiol 2026; 18(4): 118431
- URL: https://www.wjgnet.com/1949-8462/full/v18/i4/118431.htm
- DOI: https://dx.doi.org/10.4330/wjc.v18.i4.118431
The major non-cardiac surgery (MNCS) carries a significant risk of mortality and morbidity[1]. It has been reported that one myocardial infarction (MI) may occur in every 100 surgeries[2]. The MI and ischemic myocardial injury that do not fulfil the universal definition of MI comprise a phenomenon called myocardial injury after non-cardiac surgery (MINS), which occurs in up to 20% of patients undergoing MNCS[2-5]. This minireview aims to highlight the importance of detecting MINS in the surgical setting and to address their pathophysiology, diagnosis, and therapy.
Globally, among the 200 million patients who undergo MNCS annually, approximately eight million experience MINS, and one million are projected to die within 30 days, primarily due to major adverse cardiovascular events (MACEs) such as cardiac arrest, congestive heart failure, and stroke[2,3,6]. The 30-day mortality rate following MNCS ranges from 2%-6%, with more than half of these deaths attributable to MACEs[4]. Additionally, most perioperative MIs within one year are linked to high rates of MACEs and all-cause mortality[7,8]. Key determinants of adverse outcomes after MNCS include patient age, comorbidities, physical status, surgical type, and urgency[9]. Some studies have also identified sex differences and blood type as potential risk factors for MINS[10,11].
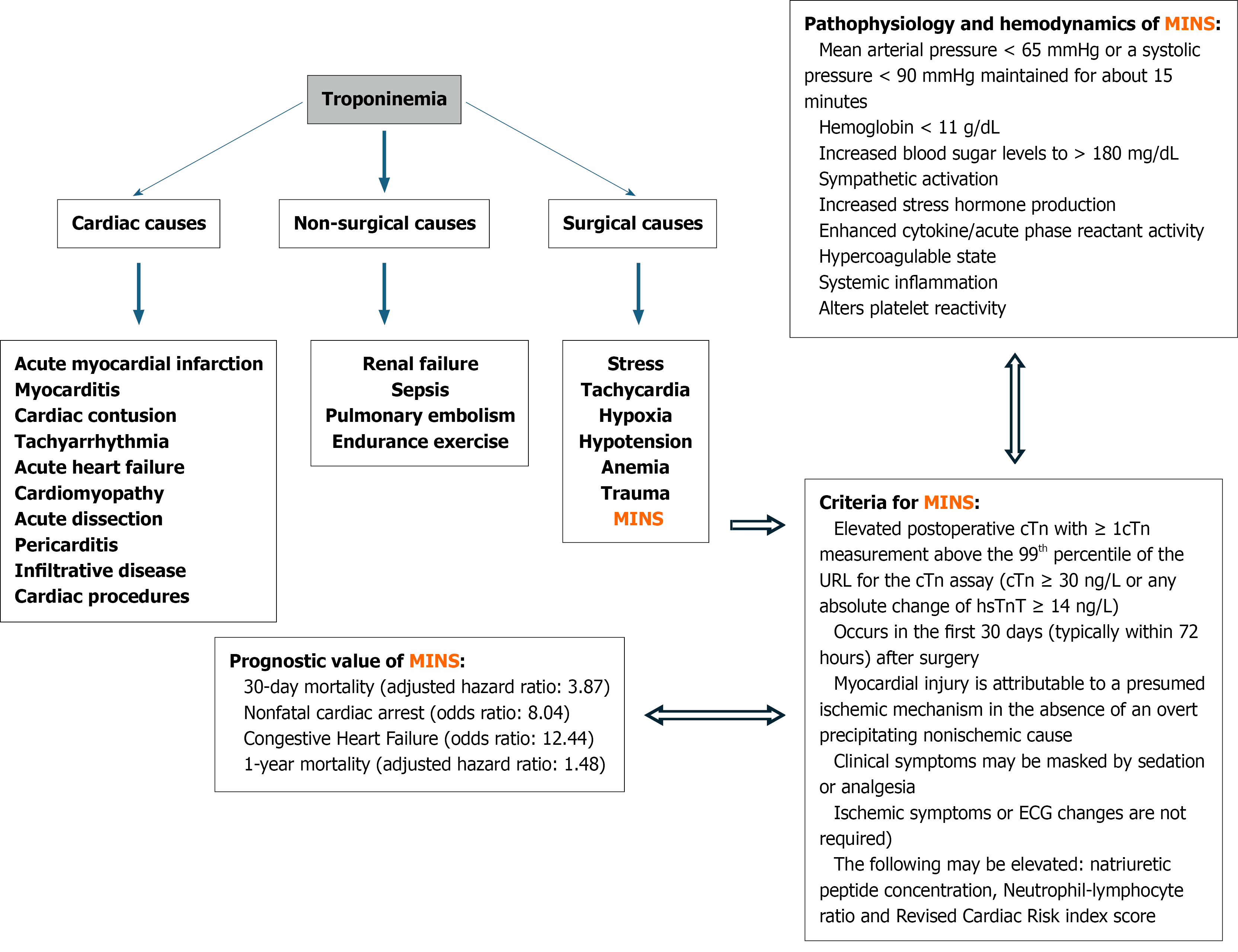
The characteristics of perioperative conditions that contribute to the occurrence of MINS include several factors such as: A mean arterial pressure < 65 mmHg or low systolic blood pressure (< 90 mmHg) maintained for at least 15 minutes, low blood hemoglobin (< 11 g/dL), high blood sugar (> 180 mg/dL), sympathetic activation, systemic inflammation, increased stress hormone production, enhanced cytokine/acute phase reactant activity, hypercoagulable state, altered platelet reactivity, and procoagulant production (Figure 1)[1,2,4]. The frequency, duration, and severity of hypotensive episodes, early or during MNCS, along with other risk factors, are key determinants of MINS development[12]. Mo
MINS is a crucial independent predictor of MACEs, but not the only one (Figure 1)[2-4,14]. Identifying these events in the perioperative period is notoriously difficult. This is because MINS could occur in the absence of obstructive coronary artery disease (CAD) in approximately 30% of patients, and only up to 40% of these injuries meet the standard criteria for MI[6,12]. MINS remains widely unrecognized. However, a working diagnosis can be established based on an elevated post-operative cardiac troponin (cTn) level within 30 days of surgery after excluding other non-ischemic causes[8].
Perioperatively, analgesics frequently mask classic ischemic cardiac symptoms, and electrocardiogram (ECG) ischemic changes are often subtle or transient, complicating the clinical picture of MINS[7]. Moreover, the diagnostic value of perioperative cardiac biomarkers is controversial in this setting. There are several factors that can affect the interpretation of these biomarkers. The release of cTn from cardiomyocytes could be induced by perioperative systemic conditions such as sepsis, inflammation, and profound stress. For instance, the adrenergic surge during surgery, independent of un
Even a low level of cTn elevation (e.g., 0.02 ng/mL) within the first three days after MNCS is associated with a significant increase in the five-year mortality rate[15]. It has been noticed that the absolute risk of 30-day mortality varies with cTn value (i.e., 1.0% for a cTn value ≤ 0.01 ng/mL; 4.0% for a value of 0.02 ng/mL; and 16.9% for a value ≥ 0.30 ng/mL)[16]. Of note, an isolated elevation in cTn is an independent predictor of mortality within a year following MNCS[8,15]. This cTn elevation correlated with a six-fold increase in the risk of death[17]. Supporting this, the VISION study confirmed the relationship between peak postoperative cTn levels and 30-day mortality[17,18]. Moreover, the interval between the peak cTn measurement and death was generally 1 to 2 weeks, suggesting a potential window for clinical intervention to reduce mortality risk[15,18]. The relationship between cTn elevation and mortality risk was also directly related to the magnitude of its increase[17,18]. Yet, it remained independent of preoperative risk factors typically associated with postoperative death (i.e., the Revised Cardiac Risk Index)[8,15,19].
A key unresolved issue is whether cTn measurement should be implemented routinely or only in high-risk surgical populations. Coric and Smith[20] reported that abnormal cTn has high sensitivity (86%) but low specificity (32%) for detecting MACEs, resulting in a 56% false-positive rate. Patients with abnormal cTn levels have a 23% risk of MACEs, and the “number needed to measure” to detect one patient with MACE is 4.4[20]. Incorporating additional biomarkers, such as serum NT-pro-BNP alongside cTn, may enhance predictive and discriminative capacity for improved risk stratification[21].
The pathophysiology of MINS is heterogeneous. Table 1 outlines the criteria for the universal definition of MI and myocardial injury[22]. Only one quarter to one third of MINS cases are attributable to coronary thrombosis (type I MI), while the majority result from a supply-demand mismatch (type II MI), often due to tachycardia, hypotension, anemia, or hypoxia[12]. Other perioperative conditions, including pulmonary embolism, sepsis, trauma, and renal failure, can also elevate serum cTn levels. Consequently, clinicians require additional tools to differentiate ischemia-related cTn elevations from other causes of “troponinemia” in surgical settings[6,14].
| Variable | Definition |
| Myocardial injury | Detection of an elevated cTn value above the 99th percentile URL. The injury is considered acute if there is a rise and/or fall of cTn values |
| Type 1 MI | Detection of a rise and/or fall of cTn values with at least 1 value above the 99th percentile URL and with at least 1 of the below mentioned findings1. Identification of a coronary thrombus by angiography including intracoronary imaging or by autopsy |
| Type 2 MI | Detection of a rise and/or fall of cTn values with at least 1 value above the 99th percentile URL, requiring at least 1 of the below mentioned findings1. Identification of an imbalance between myocardial oxygen supply and demand unrelated to acute coronary atherothrombosis |
| Type 3 MI | Sudden cardiac death, with symptoms suggestive of myocardial ischemia accompanied by presumed new ischemic ECG changes or ventricular fibrillation but die before blood samples for biomarkers can be obtained, or before increases in cardiac biomarkers can be identified, or MI is detected by autopsy examination |
| Type 4 MI (cardiac procedural-related) | An increases of cTn values (> 99th percentile URL) in patients with normal baseline values (≤ 99th percentile URL) or a rise of cTn values > 20% of the baseline value when it is above the 99th percentile URL but it is stable or falling. Type 4 MI can be further classified into three subgroups |
| Type 5 MI (CABG-related MI) | An elevation of cTn values > 10 times the 99th percentile URL in patients with normal baseline cTn values In patients with elevated preprocedure cTn in whom cTn levels are stable (≤ 20% variation) or falling, the postprocedure cTn must rise by > 20%. The absolute postprocedural value still must be > 10 times the 99th percentile URL. In addition to one of these elements: Development of new pathological Q waves, angiographic documented new graft occlusion or new native coronary artery occlusion, imaging evidence of new loss of viable myocardium or new regional wall motion abnormality in a pattern consistent with an ischemic etiology |
Postoperative cTn elevation is a strong predictor of 30-day and one-year mortality [odds ratio (OR) = 3.52 and adjusted OR = 2.53], respectively[17]. After major abdominal surgery, a doubling of postoperative cTn compared to baseline is a robust predictor of 30-day complications and prolonged hospitalization[16,23]. Elevated cTn is a powerful predictor of MACEs and mortality within one year following non-cardiac, non-vascular surgery, with risk levels similar to those observed after major vascular surgery[8,17]. Moreover, in orthopedic surgery, elevated cTn is associated with a one-year mortality OR of 2.14[17].
The VISION study, which measured cTn at 5 post-surgery time points (6-72 hours), found that even cTn levels in the upper normal range, below the diagnostic threshold of 0.04 ng/mL, were associated with increased mortality[18,20]. The study reported 8% of patients who experienced MINS. Only 16% of MINS patients exhibited ischemic symptoms, and two-thirds lacked ischemic ECG findings. The presence of ischemic symptoms further increased mortality risk by 55%[12]. In the POISE trial, two-thirds of patients with perioperative MI were asymptomatic. Since cardiac markers were measured only on the third postoperative day, additional asymptomatic MIs may have been missed[24,25], highlighting the importance of timely cTn measurement in the perioperative period.
The use of high-sensitivity troponin T (hs-TnT) assays has revealed a greater disease burden and provides more relevant prognostic values than that have been detected with a conventional cTn[18]. Mortality rates increase substantially with higher hs-TnT levels, rising from 3% at 20-65 ng/L to 29% at levels above 1000 ng/L[18,19,26]. The incidence of MINS detected increases from 8%-19% with conventional cTn assays to 20%-30% with hs-TnT assays[26,27]. Con
Given this evidence, physicians should consider monitoring cTn levels during the postoperative period in at-risk patients. This monitoring can help identify vulnerable patients who could benefit from cardiovascular optimization. For patients diagnosed with MINS who are not at high risk of bleeding, prescribing dabigatran, low-dose aspirin, and statins could be considered[3,12,28]. However, the rates of mortality and major cardiovascular and cerebrovascular events in patients with unrecognized MINS are high even with aspirin-statin therapy and specialized clinic follow-up[29]. The POISE trial showed that while beta-blockers were associated with a decrease in the post-operative MI, they also increased the incidence of stroke, indicating a need for careful risk-benefit analysis[24].
Following MINS, coronary angiography (CAG) should be considered in patients who have recurrent events and those with heart failure, though currently only a small number of patients with perioperative MI (21%) or MINS (8%) undergo CAG[12,24]. The risk of CAG with stenting (percutaneous coronary intervention) must be weighed cautiously in patients shortly after surgery, as withdrawing antiplatelet therapy can lead to catastrophic in-stent thrombosis[12,28]. Therefore, unnecessary CAG and overtreatment should be avoided, as both have diverse pathophysiological mechanisms and impact unrelated to the primary condition itself.
Major cardiology societies emphasize the importance of early detection of MINS. The American Heart Association recommends measuring cTn within the first 2-3 days postoperatively in high-risk patients. The European Society of Cardiology advises both preoperative and postoperative hsTnT testing for 2-3 days, along with NT-pro-BNP testing, in high-risk individuals undergoing intermediate- or high-risk non-cardiac surgery. The Canadian Cardiovascular Society similarly recommends daily postoperative cTn testing for 2-3 days in high-risk patients[1,3]. This consensus underscores the necessity for proactive surveillance to reduce the burden of perioperative cardiovascular complications. Involving a cardiologist in MINS management has been shown to significantly reduce 30-day mortality compared with those without cardiologist involvement (hazard ratio 0.62)[30].
Recently, machine learning algorithms have shown promise by continuously updating the probabilities of myocardial injury and death during the perioperative period. These tools could be integrated with alarm systems and decision support platforms to guide interventions and potentially reduce complications[31].
Awareness of the phenomenon of MINS is of utmost value for better perioperative management and prognostication. The patient, surgery (type, duration, and urgency), and cTn (timing, type, and frequency) should be considered in MINS identification and interpretation. Appropriate management requires a high index of suspicion and a stepwise, mul
| 1. | Bello C, Rössler J, Shehata P, Smilowitz NR, Ruetzler K. Perioperative strategies to reduce risk of myocardial injury after non-cardiac surgery (MINS): A narrative review. J Clin Anesth. 2023;87:111106. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 26] [Reference Citation Analysis (1)] |
| 2. | Kashlan B, Kinno M, Syed M. Perioperative myocardial injury and infarction after noncardiac surgery: a review of pathophysiology, diagnosis, and management. Front Cardiovasc Med. 2024;11:1323425. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 3. | Ruetzler K, Smilowitz NR, Berger JS, Devereaux PJ, Maron BA, Newby LK, de Jesus Perez V, Sessler DI, Wijeysundera DN. Diagnosis and Management of Patients With Myocardial Injury After Noncardiac Surgery: A Scientific Statement From the American Heart Association. Circulation. 2021;144:e287-e305. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 210] [Cited by in RCA: 169] [Article Influence: 33.8] [Reference Citation Analysis (1)] |
| 4. | Kuthiah N, Er C. Myocardial injury in non-cardiac surgery: complexities and challenges. Singapore Med J. 2020;61:6-8. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 5. | Biccard BM, Scott DJA, Chan MTV, Archbold A, Wang CY, Sigamani A, Urrútia G, Cruz P, Srinathan SK, Szalay D, Harlock J, Tittley JG, Rapanos T, Elias F, Jacka MJ, Malaga G, Abraham V, Berwanger O, Montes FR, Heels-Ansdell DM, Hutcherson MT, Chow CK, Polanczyk CA, Szczeklik W, Ackland GL, Dubois L, Sapsford RJ, Williams C, Cortés OL, Le Mananch Y, Devereaux PJ. Myocardial Injury After Noncardiac Surgery (MINS) in Vascular Surgical Patients: A Prospective Observational Cohort Study. Ann Surg. 2018;268:357-363. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 62] [Article Influence: 8.9] [Reference Citation Analysis (1)] |
| 6. | Verbree-Willemsen L, Grobben RB, van Waes JA, Peelen LM, Nathoe HM, van Klei WA, Grobbee DE. Causes and prevention of postoperative myocardial injury. Eur J Prev Cardiol. 2019;26:59-67. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 23] [Article Influence: 3.3] [Reference Citation Analysis (1)] |
| 7. | Grobben RB, van Klei WA, Grobbee DE, Nathoe HM. The aetiology of myocardial injury after non-cardiac surgery. Neth Heart J. 2013;21:380-388. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 16] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 8. | Puelacher C, Gualandro DM, Glarner N, Lurati Buse G, Lampart A, Bolliger D, Steiner LA, Grossenbacher M, Burri-Winkler K, Gerhard H, Kappos EA, Clerc O, Biner L, Zivzivadze Z, Kindler C, Hammerer-Lercher A, Filipovic M, Clauss M, Gürke L, Wolff T, Mujagic E, Bilici M, Cardozo FA, Osswald S, Caramelli B, Mueller C; BASEL-PMI Investigators. Long-term outcomes of perioperative myocardial infarction/injury after non-cardiac surgery. Eur Heart J. 2023;44:1690-1701. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 77] [Article Influence: 25.7] [Reference Citation Analysis (1)] |
| 9. | Nuttall GA, Merren MP, Naranjo J, Portner ER, Ambrose AR, Rihal CS. Perioperative Mortality: A Retrospective Cohort Study of 75,446 Noncardiac Surgery Patients. Mayo Clin Proc Innov Qual Outcomes. 2024;8:435-442. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 10. | Li J, Li W, Li L, Yang S, Zhao G, Li K. Association between blood groups and myocardial injury after non-cardiac surgery: a retrospective cohort study. Sci Rep. 2024;14:14028. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 11. | Kwon JH, Park J, Lee SH, Hyun CW, Kim J, Yang K, Min JJ, Lee JH, Lee SM, Choi JH, Lee SC, Gwon HC, Her S, Kim K, Ahn J. Sex differences in myocardial injury after non-cardiac surgery and postoperative mortality. Perioper Med (Lond). 2023;12:7. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 12. | Park J, Lee JH. Myocardial injury in noncardiac surgery. Korean J Anesthesiol. 2022;75:4-11. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (1)] |
| 13. | Okamoto K, Ishii M, Ishigami K, Oka K, Yoshida Y, Minami K, Doi K, Yoshizawa T, Ide Y, Fujino A, Iguchi M, Masunaga N, Abe M, Akao M. Predictors of Myocardial Injury after Non-Cardiac Surgery (MINS): a retrospective single-center cohort study. Eur Heart J. 2025;46 Suppl 1:ehaf784.2142. |
| 14. | Christenson E, Christenson RH. The role of cardiac biomarkers in the diagnosis and management of patients presenting with suspected acute coronary syndrome. Ann Lab Med. 2013;33:309-318. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 19] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 15. | van Waes JA, Nathoe HM, de Graaff JC, Kemperman H, de Borst GJ, Peelen LM, van Klei WA; Cardiac Health After Surgery (CHASE) Investigators. Myocardial injury after noncardiac surgery and its association with short-term mortality. Circulation. 2013;127:2264-2271. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 209] [Cited by in RCA: 247] [Article Influence: 19.0] [Reference Citation Analysis (1)] |
| 16. | Vascular Events In Noncardiac Surgery Patients Cohort Evaluation (VISION) Study Investigators; Devereaux PJ, Chan MT, Alonso-Coello P, Walsh M, Berwanger O, Villar JC, Wang CY, Garutti RI, Jacka MJ, Sigamani A, Srinathan S, Biccard BM, Chow CK, Abraham V, Tiboni M, Pettit S, Szczeklik W, Lurati Buse G, Botto F, Guyatt G, Heels-Ansdell D, Sessler DI, Thorlund K, Garg AX, Mrkobrada M, Thomas S, Rodseth RN, Pearse RM, Thabane L, McQueen MJ, VanHelder T, Bhandari M, Bosch J, Kurz A, Polanczyk C, Malaga G, Nagele P, Le Manach Y, Leuwer M, Yusuf S. Association between postoperative troponin levels and 30-day mortality among patients undergoing noncardiac surgery. JAMA. 2012;307:2295-2304. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 888] [Cited by in RCA: 749] [Article Influence: 53.5] [Reference Citation Analysis (1)] |
| 17. | Writing Committee for the VISION Study Investigators; Devereaux PJ, Biccard BM, Sigamani A, Xavier D, Chan MTV, Srinathan SK, Walsh M, Abraham V, Pearse R, Wang CY, Sessler DI, Kurz A, Szczeklik W, Berwanger O, Villar JC, Malaga G, Garg AX, Chow CK, Ackland G, Patel A, Borges FK, Belley-Cote EP, Duceppe E, Spence J, Tandon V, Williams C, Sapsford RJ, Polanczyk CA, Tiboni M, Alonso-Coello P, Faruqui A, Heels-Ansdell D, Lamy A, Whitlock R, LeManach Y, Roshanov PS, McGillion M, Kavsak P, McQueen MJ, Thabane L, Rodseth RN, Buse GAL, Bhandari M, Garutti I, Jacka MJ, Schünemann HJ, Cortes OL, Coriat P, Dvirnik N, Botto F, Pettit S, Jaffe AS, Guyatt GH. Association of Postoperative High-Sensitivity Troponin Levels With Myocardial Injury and 30-Day Mortality Among Patients Undergoing Noncardiac Surgery. JAMA. 2017;317:1642-1651. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 419] [Cited by in RCA: 618] [Article Influence: 68.7] [Reference Citation Analysis (1)] |
| 18. | Chapalain X, Huet O. Post-operative high sensitivity troponin T (hsTnT): toward an extending use for diagnosis and management of myocardial injury after noncardiac surgery? J Thorac Dis. 2017;9:2231-2234. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 19. | Ekeloef S, Alamili M, Devereaux PJ, Gögenur I. Troponin elevations after non-cardiac, non-vascular surgery are predictive of major adverse cardiac events and mortality: a systematic review and meta-analysis. Br J Anaesth. 2016;117:559-568. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 91] [Cited by in RCA: 83] [Article Influence: 8.3] [Reference Citation Analysis (3)] |
| 20. | Coric D, Smith NA. Postoperative troponin measurement as a screening tool for adverse cardiac events in adult patients undergoing moderate or major non-cardiac surgery. Anaesth Intensive Care. 2017;45:683-687. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 21. | Vernooij LM, van Klei WA, Moons KG, Takada T, van Waes J, Damen JA. The comparative and added prognostic value of biomarkers to the Revised Cardiac Risk Index for preoperative prediction of major adverse cardiac events and all-cause mortality in patients who undergo noncardiac surgery. Cochrane Database Syst Rev. 2021;12:CD013139. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 33] [Article Influence: 6.6] [Reference Citation Analysis (2)] |
| 22. | Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, White HD; Executive Group on behalf of the Joint European Society of Cardiology (ESC)/American College of Cardiology (ACC)/American Heart Association (AHA)/World Heart Federation (WHF) Task Force for the Universal Definition of Myocardial Infarction. Fourth Universal Definition of Myocardial Infarction (2018). J Am Coll Cardiol. 2018;72:2231-2264. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3166] [Cited by in RCA: 2798] [Article Influence: 349.8] [Reference Citation Analysis (1)] |
| 23. | Noordzij PG, van Geffen O, Dijkstra IM, Boerma D, Meinders AJ, Rettig TC, Eefting FD, van Loon D, van de Garde EM, van Dongen EP. High-sensitive cardiac troponin T measurements in prediction of non-cardiac complications after major abdominal surgery. Br J Anaesth. 2015;114:909-918. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 72] [Article Influence: 6.5] [Reference Citation Analysis (1)] |
| 24. | POISE Study Group; Devereaux PJ, Yang H, Yusuf S, Guyatt G, Leslie K, Villar JC, Xavier D, Chrolavicius S, Greenspan L, Pogue J, Pais P, Liu L, Xu S, Málaga G, Avezum A, Chan M, Montori VM, Jacka M, Choi P. Effects of extended-release metoprolol succinate in patients undergoing non-cardiac surgery (POISE trial): a randomised controlled trial. Lancet. 2008;371:1839-1847. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1808] [Cited by in RCA: 1288] [Article Influence: 71.6] [Reference Citation Analysis (2)] |
| 25. | Devereaux PJ, Guyatt G, Yusuf S. Perioperative Myocardial Infarction in Patients Undergoing Noncardiac Surgery. Ann Intern Med. 2011;. [DOI] [Full Text] |
| 26. | Sayed Masri SNN, Basri F, Yunus SN, Cheah SK. Cardiac Troponin as a Prognostic Indicator for Major Adverse Cardiac Events in Non-Cardiac Surgery: A Narrative Review. Diagnostics (Basel). 2025;15:1061. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 27. | Rostagno C, Craighero A. Postoperative Myocardial Infarction after Non-Cardiac Surgery: An Update. J Clin Med. 2024;13:1473. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 28. | Devereaux PJ, Szczeklik W. Myocardial injury after non-cardiac surgery: diagnosis and management. Eur Heart J. 2020;41:3083-3091. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 153] [Cited by in RCA: 129] [Article Influence: 21.5] [Reference Citation Analysis (1)] |
| 29. | Beltrán de Heredia S, Mases A, Recasens L, Sabaté S, Núñez M, Bosch L, Roman L, Rueda M, Alonso E, Gallart L. Mortality and incidence of cardiovascular events in patients treated with aspirin and statins at one year after myocardial injury in noncardiac surgery: a prospective observational study. Minerva Anestesiol. 2023;89:415-424. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 30. | Park J, Oh AR, Kwon JH, Kim S, Kim J, Yang K, Choi JH, Kim K, Ahn J, Sung J, Lee SH. Association between cardiologist evaluation and mortality in myocardial injury after non-cardiac surgery. Heart. 2022;108:695-702. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 27] [Article Influence: 5.4] [Reference Citation Analysis (1)] |
| 31. | Nolde JM, Schlaich MP, Sessler DI, Mian A, Corcoran TB, Chow CK, Chan MTV, Borges FK, McGillion MH, Myles PS, Mills NL, Devereaux PJ, Hillis GS. Machine learning to predict myocardial injury and death after non-cardiac surgery. Anaesthesia. 2023;78:853-860. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |