Published online Apr 26, 2026. doi: 10.4330/wjc.v18.i4.115113
Revised: November 18, 2025
Accepted: February 9, 2026
Published online: April 26, 2026
Processing time: 188 Days and 9.8 Hours
There is limited data availability regarding safety and feasibility of outpatient percutaneous coronary interventions (PCI).
To evaluate the short- and long-term outcomes of patients undergoing outpatient PCI with special regard to patients with left main and proximal left anterior descending artery disease.
The retrospective, single-center study was conducted in a hemodynamics laboratory dedicated to one-day procedures. We have analyzed short-, medium- and long-term outcomes of the patients undergoing PCI mostly from radial or ulnar access being discharged few hours after procedure.
During the follow-up period, 787 procedures were performed on 444 patients, including 25 procedures in the left main and 115 procedures in the proximal left anterior descending artery. The median time to discharge was 150 minutes. The median time of follow-up in the general group was 587 days. There was no myocardial infarction (MI), death, stroke or emergent bypass within 24 hours after surgery. During the 30 days of major adverse cardiac and cerebrovascular events follow-up, there were 1 MI (0.17%), 7 cases (0.88%) of target vessel revascularization (TVR) and 4 unplanned hospitalizations (0.7%); there were no deaths or strokes. During 720 days of major adverse cardiac and cerebrovascular events follow-up, there were 11 deaths (1.93%), 5 MIs (0.88%), 60 cases of TVR (7.62%), and 1 stroke (0.17%). Cases of repeat revascularization were observed more often in combined group of patients with diabetes or pre-diabetes than in patients without these conditions (P = 0.046). Patients who underwent PCI with femoral access were statistically more likely to undergo repeat revascularization within 2 years after the procedure [19 (21.84%) vs 41 (5.85%) P < 0.001]. There was a statistically significant higher prevalence of TVR within 2 years after the procedure in patients who had more than one lesion treated compared to single lesion procedures [22 (11.70%) vs 38 (6.34%); P = 0.015].
The results of this study suggest that PCIs performed on an outpatient basis with very short discharge times may be safe and feasible. However, as this is a hypothesis- generating study, the present findings should be interpreted with caution and confirmed in future large- scale randomized controlled trials.
Core Tip: A single-center, retrospective study was conducted to evaluate the short- and long-term outcomes of patients undergoing outpatient percutaneous coronary interventions. During the follow-up period, 787 procedures were performed on 444 patients, including 25 procedures in the left main and 115 procedures in the proximal left anterior descending artery. Over the 720 days of major adverse cardiac and cerebrovascular events follow-up, there were 11 deaths (1.93%), 5 myocardial infarctions (0.88%), 60 cases of target vessel revascularization (7.62%), and 1 stroke (0.17%). The results of study suggest that percutaneous coronary interventions performed on an outpatient basis with very short discharge times may be safe and feasible.
- Citation: Klocek K, Gora B, Fischell TA, Kunik P, Janas A, Kiesz RS. Safety and feasibility of outpatient percutaneous coronary interventions with short- and long-term outcomes. World J Cardiol 2026; 18(4): 115113
- URL: https://www.wjgnet.com/1949-8462/full/v18/i4/115113.htm
- DOI: https://dx.doi.org/10.4330/wjc.v18.i4.115113
Percutaneous coronary interventions (PCI) procedures in the United States have been on the rise in recent years. PCI volume in the United States increased by 15.8%, from 550872 in 2013 to 637650 in 2017 and it is still growing[1]. In an aging population, the percentage of people with coronary artery disease is increasing and thus number of patients requiring angioplasty[2]. Developments in the field of cardiology have led to an increased safety of the PCI procedure and allowed the patient to be discharged the same day[3-5]. Discharging the patient on the same day increases patient satisfaction and comfort, reduces hospitalization costs and reduces the risk of typical hospital complications[6-10]. The Amin et al[11], published in 2018, analyzed 672470 PCI procedures performed between 2006 and 2015 at 493 United States hospitals- 62920 patients were discharged on the day of the procedure (9.1%). Discharge on the day of surgery was associated with a savings of $5128 on average. This means that implementing the same-day discharge criteria used by the top 10% of the “top” hospitals analyzed (increasing the number of same-day procedures from 2.2% to 44.5%) would mean a savings of $433828 for the average United States hospital performing 200 elective PCIs per year. The beginnings of a randomized security assessment carried out by Heyde et al[12], who conducted a randomized trial that evaluated complications 24 hours after PCI showed, that same-day discharge after elective PCI is feasible and safe in the majority of patients selected for day-case PCI. Same-day discharge did not lead to additional complications compared with overnight stay. However, there are scarce data evaluating long-term complications in patients discharged early. There is even less safety data on discharging patients on the same day after complex procedures, such as left main coronary artery angioplasty. Gaba et al[13] conducted an EXCEL study, where among 948 patients with left main coronary artery disease assigned to PCI, 935 patients underwent PCI as their first procedure, including 100 (10.7%) performed in the outpatient setting. Patients who underwent outpatient compared with inpatient PCI were less likely to have experienced recent myocardial infarction (MI). Similar results were observed in patients with distal left main bifurcation lesions. In conclusion, in the EXCEL trial, outpatient PCI of patients with left main coronary artery disease was not associated with an excess early or late hazard of major adverse cardiac and cerebrovascular events. However, in this case there is also the lack of studies conducting long-term follow-up.
In order to safely perform the procedure in a single day, special rules must be followed, including the use of an appropriate anticoagulant. Bivalirudin is a direct thrombin inhibitor for intravenous administration and is an alternative to unfractionated heparin. It has a shorter half-life of 25 minutes (57 minutes at glomerular filtration rate < 30 mL/minute) compared to 90 minutes for unfractionated heparin. The anticoagulant effect is virtually abolished 1.5 hours after stopping the infusion. It is not necessary to determine blood clotting times (activated partial thromboplastin time/activated clotting time). A limitation is that anticoagulation cannot be reversed.
The main aim of the study was to evaluate the safety and feasibility of outpatient PCI with short- and long-term outcomes with special regard to patients with left main and proximal left anterior descending (LAD) artery disease. This retrospective, single-center study was conducted in San Antonio Endovascular and Heart Institute - a hemodynamics laboratory dedicated to one-day procedures (ambulatory surgical center/office-based lab), which has experience performing outpatient PCI since 2008. We have analyzed short-, medium- and long-term outcomes (24 hours, 30 days, 180 days, 360 days and 720 days) of the patients undergoing PCI mostly from radial or ulnar access being discharged few hours after procedure. We have paid special attention to major adverse cardiac and cerebrovascular events follow-up (MACE), defined in the study as death, MI, stroke or target vessel revascularization (TVR). Short-term complications, such as the presence of clinically significant hematomas, pseudoaneurysms and unplanned hospitalizations up to 30 days after the procedure were also evaluated. This research focused on evaluating the complications of consecutive performed procedures and paid special attention to certain groups of patients, such as those with left main and proximal LAD coronary artery disease.
The data were collected by an independent investigator not involved in interventions. In order to collect data, we used the system that the facility used on a daily basis for clinical purposes. The study included consecutive PCIs performed in a single Cath-lab on a diverse population of adult patients from 2018 to 2023. Patients were qualified for the procedure based on the presence of symptoms of myocardial ischemia and/or ischemia confirmed by functional imaging studies. All patients gave standard written consent for the procedure. Laboratory tests were performed on the day of surgery, unless they were done up to a week before surgery.
Procedures were performed through radial, ulnar or femoral access. The access was obtained using modified Seldinger technique with ultrasound guidance. Then, in case of radial or ulnar access, the sheath was inserted and flushed with cocktail containing heparin, verapamil and nitroglycerin. At the end of the procedure, the catheter and sheath were removed and TR or Zephyr band with stat seal was applied. The insertion site from the femoral access was closed with an artery closure device: Vascade, Mynx Grip or Celt. All patients received dual antiplatelet therapy and aggressive statin therapy [majority of patients (84.46%) received 40 mg of rosuvastatin] after the procedure, unless contraindications existed. The patient was mobilized according to the protocols for each device. After the intervention, patients were transferred to the post-operative care area, where their vital signs were monitored. If there were no significant complications, and the patient’s clinical condition was satisfactory in the doctor’s opinion, the participant was discharged home. The day after the procedure, the patient reported for dressing changes and to check the proper healing of the arterial puncture site - if any worrisome symptoms were found, a Doppler ultrasound was performed. If no abnormalities were found, the patient was scheduled for a routine follow-up visit to the cardiology outpatient clinic as recommended by the doctor on the discharge card (usually 2-4 weeks after the procedure), followed by routine follow-ups every 3/6 months depending on the indications and clinical condition.
Data were processed with Microsoft Excel and statistical analysis software. Demographics consisted of age, gender, height, weight, body mass index, number of active smokers. Presence of chronic diseases such as obesity, hypertension, diabetes, heart failure, atrial fibrillation, hypothyroidism, chronic obstructive pulmonary disease/asthma, carotid artery disease, peripheral artery disease were analyzed. Also, data such as family history of cardiovascular diseases, history of MI or stroke and underwent procedures such as pacemakers, coronary artery bypass grafting and PCI in the past was collected. The term pre-diabetes referred to individuals without a formal diagnosis of type 2 diabetes who exhibited impaired fasting glucose [fasting plasma glucose level of 100-125 mg/dL (5.6-6.9 mmol/L)] and/or impaired glucose tolerance [2-hour plasma glucose level of 140-199 mg/dL (7.8-11.0 mmol/L) on a 75-g oral glucose tolerance test] according to American Diabetes Association. Medications taken on a regular basis by patients were also evaluated. Additionally, ejection fraction from transthoracic echocardiography, single-photon emission computed tomography images and calcium score were evaluated.
Continuous data with normal distribution (compared with the t-test) are presented as mean ± SD. Whereas, continuous data with skewed distribution were compared with the Mann-Whitney U test and are presented as medians (first to third quartile). Statistical significance was considered for P < 0.05. The exclusion criteria for participation in this research was incomplete documentation of the procedure performed or follow-up visits. The study received approval from the Bioethics Committee dated February 7, 2024 (approval No. 20240401).
Study established a registry of patients and divided them into several groups for safety and efficacy analyses. During the follow-up period, 787 procedures were performed on 444 patients with 571 unique follow-ups, including 25 procedures in the left coronary artery trunk and 115 procedures in the proximal LAD, 768 (97.59%) of the treatments were successful. The criterion for success was dilatation of the target artery and restoration of normal flow at the thrombolysis in myocardial infarction III level. Of 223 (50.23%) patients had single vessel disease, 142 (31.98%) had two coronary vessels involved, 51 (11.49%) had triple vessel disease, while 28 (6.3%) patients had more than 3 vessels involved. There were 204 (25.92%) cases of 2 lesions targeted, while 23 (2.92%) procedures were performed on at least 3 lesions. The characteristics of the study group in terms of demographics and concomitant diseases are shown below (Table 1).
| All procedures = 787 | Median | n | % |
| Age (years) | 66 | ||
| Weight (kg) | 89.13 | ||
| Height (cm) | 172.72 | ||
| BMI | 30.48 | ||
| Number of males | 313 | 70.50 | |
| Obesity | 220 | 49.55 | |
| Hypertension | 374 | 84.23 | |
| Hyperlipidemia | 390 | 87.84 | |
| Diabetes mellitus | 274 | 61.71 | |
| Heart failure | 27 | 6.08 | |
| Active smoker | 72 | 16.22 | |
| Atrial fibrillation | 23 | 5.18 | |
| Hypothyroidism | 50 | 11.26 | |
| Chronic obstructive pulmonary disease/asthma | 28 | 6.31 | |
| Pacemaker in history | 15 | 3.38 | |
| Carotid artery atherosclerosis | 5 | 1.13 | |
| Cancer in history | 38 | 8.56 | |
| Chronic kidney disease | 82 | 18.47 | |
| Peripheral artery disease | 68 | 15.32 | |
| MI in history | 70 | 15.77 | |
| Stroke/TIA in history | 18 | 4.05 |
The majority of patients undergoing procedure: 436 (55.4%) in terms of symptoms fell into the Canadian Cardio
| All procedures = 787 | n | % |
| PCI LM | 25 | 2.83 |
| PCI LAD | 332 | 37.60 |
| PCI diagonal | 35 | 3.96 |
| PCI Cx | 101 | 11.44 |
| PCI OM | 96 | 10.87 |
| PCI ramus | 20 | 2.27 |
| PCI PDA | 54 | 6.12 |
| PCI RCA | 202 | 22.88 |
| PCI posterolateral | 15 | 1.70 |
| PCI graft to RCA | 1 | 0.11 |
| PCI LIMA | 2 | 0.23 |
| All PCI | 883 | 100 |
| BA LAD | 25 | 15.53 |
| BA diagonal | 46 | 28.57 |
| BA Cx | 15 | 9.32 |
| BA OM | 27 | 16.77 |
| BA ramus | 4 | 2.48 |
| BA RCA | 14 | 8.70 |
| BA posterolateral | 7 | 4.35 |
| BA PDA | 21 | 13.04 |
| BA LIMA | 2 | 1.24 |
| All BA | 161 | 100 |
In the total patient population the median time to discharge was 150 minutes: The longest was 523 and the shortest was 65 minutes. The median time of follow-up in the general group was 587 days. Time to discharge was defined as the interval between the start of the procedure and the patient’s discharge from the ambulatory surgical center. Short-term complications assessed 24 hours after surgery are shown in the table below (Table 3). There was no MI, deaths, strokes or emergent bypass within 24 hours after the surgery. There was no need to transfer any of the patients to 24-hour hospital care for overnight observation. None of the patients were hospitalized within 24 hours after the procedure.
| Complications 24 hours after surgery | n | % |
| Haematoma | 15 | 1.91 |
| Pseudoaneurysm | 2 | 0.25 |
| Minor bruising/pain/swelling | 42 | 5.34 |
| Total occlusion of radial/ulnar artery | 1 | 0.13 |
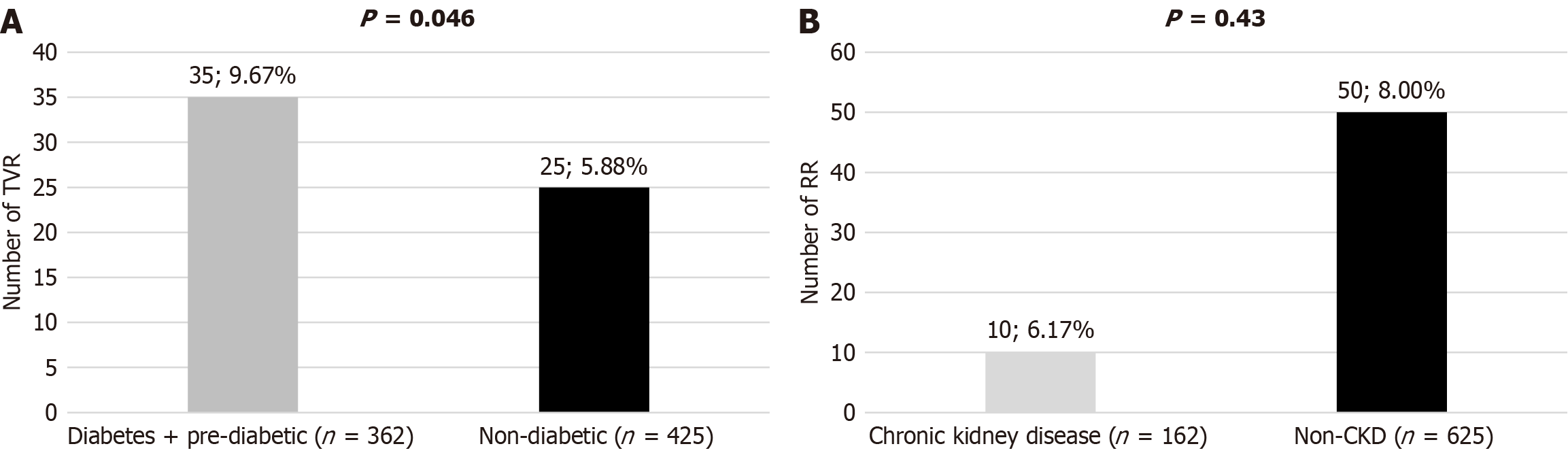
The study focused on cases of major cardiovascular events and evaluated them at different time points. In the main group, during the 30 days of MACE follow-up, there were 1 MI, 7 cases of TVR and 4 unplanned hospitalizations for cardiovascular reasons; there were no deaths or strokes. During 720 days of MACE follow-up, there were 11 deaths, 5 MIs, 60 cases of TVR, and 1 stroke. The summed cases at each time point are shown in the table below. Data on unplanned hospitalizations were collected only up to 30 days after surgery, because data beyond this timeframe were not accessible (Table 4). Cases of repeat revascularization were observed more often in combined group of patients with diabetes or pre-diabetes than in patients without these conditions (P = 0.046) (Figure 1A). The presence of chronic kidney disease did not affect the increased need for repeat revascularization (P = 0.43) (Figure 1B).
| MACE | 0-30 days | % | 6 months | % | 12 months | % | 24 months | % |
| Death | 0 | 0 | 1 | 0.17 | 6 | 1.02 | 11 | 1.93 |
| MI | 1 | 0.17 | 2 | 0.35 | 3 | 0.52 | 5 | 0.85 |
| TVR | 7 | 0.89 | 15 | 1.9 | 34 | 4.32 | 60 | 7.62 |
| Stroke | 0 | 0 | 1 | 0.17 | 1 | 0.17 | 1 | 0.17 |
| Unplanned hospitalization | 4 | 0.7 |
In the group of patients who underwent repeat revascularization, there were no statistically significant differences in the incidence of obesity, hypertension, heart failure or hypothyroidism. On the other hand, we observed a statistically significant higher percentage of patients with hyperlipidemia and a history of stroke [respectively 58 (96.67%) vs 640 (87.79%), P = 0.03; 7 (11.67%) vs 30 (4.12%), P = 0.007]. Patients who underwent repeat revascularization within two years had a significantly longer time to discharge than patients without this complication (168 minutes vs 150 minutes, P = 0.025).
The vast majority of procedures (n = 700; 88.95%) were performed from the wrist with radial or ulnar access. The median follow-up time in this group was 594 days, while the median time to discharge was 150 minutes. In this group, there were 41 (5.85%) cases of TVR, 8 (1.14%) deaths, 4 (0.57%) MIs and not a single stroke during the 2-year observation period. On the other hand, 87 PCIs from femoral access were performed from 2018 to 2023. The median follow-up time in this group was 608 days, and the median time to discharge was 150 minutes. During the two years of follow-up in this group, there were 19 (21.84%) TVRs, 3 (3.45%) deaths, 1 (1.14%) stroke and 1 (1.14%) MI. Patients in the femoral access group had a statistically significant higher incidence of TVR, during 2 years of follow-up [19 (21.84%) vs 41 (5.85%), P < 0.001], while there was no statistical significance in terms of death and MI (P = 0.084, P = 0.52). The groups were homogeneous in terms of prevalence of obesity, hypertension, hyperlipidemia, heart failure, atrial fibrillation, pulmonary disease, history of cancer, lower extremity atherosclerosis, history of stroke and family history of cardiovascular disease. However, the femoral access group was shown to have significantly more type 2 diabetes [53 (60.92%) vs 309 (44.14%); P = 0.003], chronic kidney disease [31 (35.63%) vs 131 (18.71%); P = 0.0002], history of MI [27 (31.03%) vs 128 (18.29%); P = 0.0048] and history of PCI [62 (71.26%) vs 351 (50.14%); P = 0.00019] and coronary artery bypass grafting [27 (31.03%) vs 55 (7.86%); P < 0.00001].
All procedures were performed using drug eluting stents. A variety of stents were used during follow-up, but the most commonly used devices were selected for comparison. The table below shows the percentage of the four most popular stents used in the procedures. A comparison was made between these groups in terms of the incidence of stent related complications. The rate of TVR and MI did not depend on the type of stent used (P = 0.96, P = 0.56) (Table 5).
| Stent | n | % | TVR | MI |
| Xience DES | 558 | 63.19 | 37 (6.63) | 3 (0.53) |
| Orsiro DES | 155 | 17.55 | 11 (7.1) | 0 |
| EluNIR DES | 58 | 6.57 | 3 (5.17) | 0 |
| Resolute Onyx DES | 54 | 6.12 | 4 (7.4) | 1 (1.85) |
Radiation parameters and the amount of contrast given is presented in the table below (Table 6). From 2018 to 2023 in this centre 25 procedures were performed on left main artery, including 10 in ostial part of left main a 15 in mid/distal part with median time of follow-up of 782 days. Median time to discharge was respectively 180 minutes and 175 minutes. During follow-up, there were no serious short- or long-term complications in these groups. There were 2 (8%) cases of TVR in mid/distal left main group. However, they were not a statistically significant difference compared to the ostial group (P = 0.94).
| Procedure details | mean | SD | Median |
| Fluoroscopy time (minute) | 9.99 | 6.87 | 8.1 |
| DAP (mGyCm2) | 81626.4 | 61324.91 | 64241 |
| AK (mGy) | 1290.59 | 861.94 | 1068.5 |
| Contrast volume (mL) | 107.05 | 64.76 | 95 |
| Angiomax bolus (mL) | 13.64 | 2.99 | 13.5 |
| Angiomax drip (mL/hour) | 30.82 | 8.4 | 31.5 |
| Nitroglicerin (μg) | 256.09 | 134.23 | 250 |
332 procedures were performed in the LAD, including 115 in the proximal part and 217 in the mid/distal. Median follow-up for proximal LAD group was 463 days. During 2 years of follow-up, there was no cases of stroke, major bleeding or unplanned hospitalization for cardiovascular reasons. The observed cases of MACE are shown in the table below- the overall number of MACE was low and did not differ compared to the general group (Table 7). There were no statistically significant differences between the proximal LAD and mid/distal LAD groups (Table 8).
| Complication | LAD (n = 332) | General group (n = 787) | P value |
| TVR | 21 (6.33) | 60 (7.62) | 0.44 |
| MI | 3 (0.90) | 5 (0.64) | 0.63 |
| Death | 5 (1.51) | 11 (1.40) | 0.89 |
| Complication | Proximal LAD | LAD | P value |
| TVR | 7 (6.08) | 14 (6.45) | 0.89 |
| MI | 1 (0.86) | 2 (0.92) | 0.96 |
| Death | 2 (1.74) | 3 (1.38) | 0.89 |
The decision to fix several lesions during one procedure or to stage the patient was up to the doctor. Comparisons were made in terms of complications after procedures in which more than one intervention was performed (n = 188; 23.89%) vs procedures on a single lesion (n = 599; 76.11%). Median time to discharge was respectively 145 minutes and 150 minutes and it did not differ significantly (P = 0.78). There was a statistically significant higher prevalence of TVR within 2 years after the procedure in patients who had more than one lesion treated compared to single lesion procedures [22 (11.70%) vs 38 (6.34%); P = 0.015] (Table 9).
| Complication | Single vessel (n = 599) | % | Multivessel (n = 188) | % | P value |
| Death | 9 | 1.50 | 2 | 1.06 | 0.65 |
| MI | 5 | 0.83 | 0 | 0.00 | 0.67 |
| TVR | 38 | 6.34 | 22 | 11.70 | 0.015 |
| Stroke | 1 | 0.17 | 0 | 0.00 | 0.38 |
| Haematoma | 13 | 2.17 | 2 | 1.06 | 0.33 |
| Pseudoaneurysm | 2 | 0.33 | 0 | 0.00 | 0.7 |
| Minor bruising/pain/swelling | 35 | 5.84 | 7 | 3.72 | 0.25 |
| Total occlusion of radial artery | 1 | 0.17 | 0 | 0.00 | 0.38 |
Although it was not a center specializing in chronic total obstruction, during the course of observation, 30 chronic total obstructions were attempted, of which 21 (70%) were successful. The median time to discharge in this group was 142 minutes. Complications were counted for the group of procedures successfully completed. One hematoma and one case of minor bruising were observed. During 2 years of follow-up, there were 3 (14.29%) cases of repeat revascularization and 1 (4.76%) case of MI, which did not differ statistically significantly from the general group (respectively P = 0.26, P = 0.08).
To date, there is a lack of studies describing the long-term effects of PCI performed on an outpatient basis, so we have attempted to address this topic. Our study demonstrates the safety of performing PCI in stable patients on a same-day basis, even with very early discharge (median time to discharge from the start of the procedure was 150 minutes) after percutaneous coronary angioplasty. This type of management is not associated with an increased risk of short-term as well as long-term complications. The results are consistent with findings from other studies on outpatient PCI, which also demonstrated safety in the short-term[14-17].
Elfandi and Safirstein[18] has performed the literature review and evaluated the studies regarding the same day discharge after transradial PCI over the last 17 years. This research concluded, that outpatient PCI from radial access for appropriately selected patients will be the standard of care in the future. The rate of repeat revascularization was significantly influenced by the presence of diabetes and pre-diabetic status. This indicates the need for good glycemic control in these patients and for a randomized trial to determine the impact of glycemic control on patients’ long-term outcomes after rapid discharge. Hyperlipidemia as a known risk factor for coronary artery disease was significantly more common in patients who underwent repeat revascularization, which also indicates the need to control lipid profile according to the guidelines. The risk of bleeding when performing elective procedures is low [according to the National Cardiovascular Data Registry Percutaneous Coronary Intervention via Cardiac Catheterization (CathPCI) 2017 registry of more than 600000 procedures, the rate of major bleeding within 72 hours after the procedure was 1.4%]. In our study, there was not a single case of serious bleeding during this period. During follow-up, there was one case of major bleeding within 6 months after the procedure- a patient experienced gastrointestinal bleeding, and no correlation was found between PCI and this incident. The results of our study are comparable to the large Same-day TransRadial Intervention and Discharge Evaluation trial[19], where the investigators did not observe any significant adverse effects of percutaneous coronary angioplasty that could be avoided by having the patient stay longer. Tamez et al’s study[20] was conducted on 653304 patients from CathPCI registry, with 10.2% (in-stent restenosis) PCI and 89.8% de novo lesion PCI, with a median duration of follow-up of 825 days. In this research the frequency of MACE (55.6% vs 45.0%; P < 0.001), all-cause mortality (27.8% vs 25.5%; P < 0.001), MI (19.0% vs 12.3%; P < 0.001), repeat revascularization (31.9% vs 18.6%; P < 0.001), TVR (22.4% vs 8.0%; P < 0.001), and stroke (8.8% vs 8.3%; P = 0.005) was higher after in-stent restenosis PCI. Data from our study show lower or comparable percentages of MACE among elective outpatient PCI compared to the data from CathPCI registry. Referring to the results comparing access site, the femoral access group included higher-risk patients. The higher rate of TVR in this group may reflect patient characteristics rather than access site itself- hence the need for further research in this area.
The precise prediction of a patient’s duration of stay in the ward is advantageous not solely from a medical viewpoint, but also from an organizational angle. Procedures carrying a higher risk of extended stays can be prioritized earlier in the day, facilitating the optimal utilization of the medical facility’s operational hours.
The main limitation of our study is its retrospective and single-center nature. Despite the fact that records were kept in a very thorough manner, this study has several weaknesses. The most significant limitation of this study is the absence of a comparator group- a direct comparison between patients discharged on the same day and those discharged the following day would have provided much stronger evidence. A very important component of same-day discharge is high patient satisfaction, so expanding the study to include this aspect would be very beneficial. It would also be important to determine the impact of diabetes control and hypercholesterolemia on long-term outcomes in patients after early discharge.
The results of this study suggest that PCIs performed on an outpatient basis with very short discharge times may be safe and feasible. However, as this is a hypothesis-generating study, the present findings should be interpreted with caution and confirmed in future large-scale randomized controlled trials.
| 1. | Inohara T, Kohsaka S, Spertus JA, Masoudi FA, Rumsfeld JS, Kennedy KF, Wang TY, Yamaji K, Amano T, Nakamura M. Comparative Trends in Percutaneous Coronary Intervention in Japan and the United States, 2013 to 2017. J Am Coll Cardiol. 2020;76:1328-1340. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 140] [Cited by in RCA: 128] [Article Influence: 21.3] [Reference Citation Analysis (0)] |
| 2. | Khalid N, Haider S, Abdullah M, Asghar S, Laghari MA, Rajeswaran Y. Trends and disparities in coronary artery disease prevalence among U.S. adults from 2019 to 2022. Curr Probl Cardiol. 2024;49:102645. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 12] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 3. | Bertrand OF, Larose E, De Larochellière R, Proulx G, Nguyen CM, Déry JP, Gleeton O, Barbeau G, Noël B, Rouleau J, Boudreault JR, Roy L, Rodés-Cabau J. Outpatient percutaneous coronary intervention: Ready for prime time? Can J Cardiol. 2007;23 Suppl B:58B-66B. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 13] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 4. | Khater M, Zureikat H, Alqasem A, Alnaber N, Alhaddad IA. Contemporary outpatient percutaneous coronary intervention: feasible and safe. Coron Artery Dis. 2007;18:565-569. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 5. | Caputo RP, Levine RL. I'll Take My PCI to Go. Cardiovasc Revasc Med. 2020;21:1374-1376. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 6. | Singletary D. Evaluation of the safety and efficacy of same-day discharge following outpatient surgery in a US hospital. Nurs Manag (Harrow). 2016;23:34-38. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 7. | Koshy SKG, George LK, Das P. Cost-effectiveness and Outcomes with Early or Same-Day Discharge After Elective Percutaneous Coronary Intervention. Curr Cardiol Rep. 2020;22:42. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 8. | Hyasat K, Femia G, Alzuhairi K, Ha A, Kamand J, Hasche E, Rajaratnam R, Lo S, Almafragy H, Liou K, Chiha J, Asrress K. Safety, Feasibility and Economic Analysis of Same Day Discharge Following Elective Percutaneous Coronary Intervention. Clin Med Insights Cardiol. 2022;16:11795468221116852. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 9. | Krishnaswamy A, Isogai T, Brilakis ES, Nanjundappa A, Ziada KM, Parikh SA, Rodés-Cabau J, Windecker S, Kapadia SR. Same-Day Discharge After Elective Percutaneous Transcatheter Cardiovascular Interventions. JACC Cardiovasc Interv. 2023;16:1561-1578. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 19] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 10. | Gilchrist IC. Same day discharge after elective percutaneous coronary intervention. Curr Cardiol Rep. 2014;16:470. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 11. | Amin AP, Pinto D, House JA, Rao SV, Spertus JA, Cohen MG, Pancholy S, Salisbury AC, Mamas MA, Frogge N, Singh J, Lasala J, Masoudi FA, Bradley SM, Wasfy JH, Maddox TM, Kulkarni H. Association of Same-Day Discharge After Elective Percutaneous Coronary Intervention in the United States With Costs and Outcomes. JAMA Cardiol. 2018;3:1041-1049. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 88] [Cited by in RCA: 76] [Article Influence: 9.5] [Reference Citation Analysis (0)] |
| 12. | Heyde GS, Koch KT, de Winter RJ, Dijkgraaf MG, Klees MI, Dijksman LM, Piek JJ, Tijssen JG. Randomized trial comparing same-day discharge with overnight hospital stay after percutaneous coronary intervention: results of the Elective PCI in Outpatient Study (EPOS). Circulation. 2007;115:2299-2306. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 155] [Cited by in RCA: 132] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 13. | Gaba P, Serruys PW, Karmpaliotis D, Lembo NJ, Banning AP, Zhang Z, Morice MC, Kandzari DE, Gershlick AH, Ben-Yehuda O, Sabik JF 3rd, Kappetein AP, Stone GW. Outpatient Versus Inpatient Percutaneous Coronary Intervention in Patients With Left Main Disease (from the EXCEL Trial). Am J Cardiol. 2021;143:21-28. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 14. | Chia J, Wilson A, Law D, Kelly M, Lambert B. The safety of same-day discharge following percutaneous coronary intervention in regional Australia. Intern Med J. 2024;54:1821-1826. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 15. | Córdoba-Soriano JG, Jiménez-Mazuecos J, Rivera Juárez A, Gutiérrez-Díez A, Gutiérrez Ibañes E, Samaniego-Lampón B, Lozano I, Gallardo-López A, Díaz L, Sanz-Ruiz R, Melehi D, Barrionuevo-Sánchez MI, Rondán-Murillo J, Vegas-Valle JM, Elízaga J. Safety and Feasibility of Outpatient Percutaneous Coronary Intervention in Selected Patients: A Spanish Multicenter Registry. Rev Esp Cardiol (Engl Ed). 2017;70:535-542. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 16. | Ginete WL, Groth NA, Rudeck MN, Renier CM, Benziger CP. Outcomes of same-day discharge following percutaneous coronary intervention in a rural population. Catheter Cardiovasc Interv. 2023;102:472-480. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 17. | Brandt MC, Alber H, Berger R, Binder RK, Mascherbauer J, Niessner A, Schmid M, Wernly B, Frick M; Austrian working group of interventional cardiology. Same-day discharge after percutaneous coronary procedures-Structured review and comprehensive meta-analysis. Wien Klin Wochenschr. 2024;136:44-60. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 18. | Elfandi A, Safirstein JG. Transradial PCI and Same Day Discharge. Curr Treat Options Cardiovasc Med. 2018;20:10. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 19. | Jabara R, Gadesam R, Pendyala L, Chronos N, Crisco LV, King SB, Chen JP. Ambulatory discharge after transradial coronary intervention: Preliminary US single-center experience (Same-day TransRadial Intervention and Discharge Evaluation, the STRIDE Study). Am Heart J. 2008;156:1141-1146. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 74] [Cited by in RCA: 65] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 20. | Tamez H, Secemsky EA, Valsdottir LR, Moussa ID, Song Y, Simonton CA, Gibson CM, Popma JJ, Yeh RW. Long-term outcomes of percutaneous coronary intervention for in-stent restenosis among Medicare beneficiaries. EuroIntervention. 2021;17:e380-e387. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 63] [Article Influence: 12.6] [Reference Citation Analysis (0)] |