Published online Feb 26, 2026. doi: 10.4330/wjc.v18.i2.115528
Revised: November 1, 2025
Accepted: December 17, 2025
Published online: February 26, 2026
Processing time: 113 Days and 17.4 Hours
Hypertensive emergencies, characterized by severe blood pressure elevation (> 180/120 mmHg) with end-organ damage, pose significant risks in patients with coronary artery disease (CAD), where rapid yet safe reduction is crucial to prevent ischemia and complications. Nitroglycerin and labetalol are common intravenous agents, but comparative data in CAD are limited.
To compare efficacy and safety of nitroglycerin vs labetalol in hypertensive emergencies among CAD patients, assessing blood pressure control, reductions, adverse events, outcomes, and utilization.
Retrospective cohort of 563 CAD patients with hypertensive emergency (2018-2024) receiving IV nitroglycerin (n = 282) or labetalol (n = 281). Primary: Time to target blood pressure [systolic blood pressure (SBP) < 160 mmHg, diastolic blood pressure < 100 mmHg]. Secondary: Blood pressure reductions, major adverse cardiovascular event, safety, utilization. Analyzed via t-tests, χ2, multivariable logistic regression adjusting for age, gender, myocardial infarction/heart failure history, diabetes, baseline SBP, chest pain.
Baseline characteristics were balanced. Labetalol achieved target blood pressure faster (25.14 ± 4.92 minutes vs 30.38 ± 5.16 minutes; P < 0.0001), but nitroglycerin yielded greater SBP (50.78 ± 9.45 mmHg vs 45.20 ± 10.46 mmHg; P < 0.0001) and diastolic blood pressure reductions (29.86 ± 8.63 mmHg vs 28.02 ± 7.74 mmHg; P = 0.0079). Nitroglycerin showed trends toward lower major adverse cardiovascular event [adjusted odds ratio (AOR): 0.72; 95% confidence interval (CI): 0.42-1.24], reduced bradycardia (AOR: 0.14; 95%CI: 0.05-0.38), shorter intensive care unit (2.99 ± 1.04 days vs 3.54 ± 1.02 days; P < 0.0001) and hospital stays (6.92 ± 1.93 days vs 7.99 ± 2.06 days; P < 0.0001), lower 30-day readmissions (AOR: 0.49; 95%CI: 0.27-0.88), and smaller biomarker increases (delta troponin: 0.10 ± 0.05 ng/mL vs 0.21 ± 0.10 ng/mL; P < 0.0001).
While labetalol offers faster blood pressure control, nitroglycerin is associated with greater reductions, fewer adverse events like bradycardia, and improved utilization (shorter stays, fewer readmissions) in CAD-associated hypertensive emergencies, supporting its use in ischemic contexts.
Core Tip: This retrospective study uniquely compares intravenous nitroglycerin and labetalol for managing hypertensive emergencies in a large South Asian cohort of patients with established coronary artery disease. Although labetalol achieved target blood pressure more rapidly, nitroglycerin provided greater magnitude of blood pressure reduction, significantly lower rates of bradycardia, smaller rises in cardiac biomarkers, shorter intensive care unit and hospital stays, and reduced 30-day readmissions. These findings highlight nitroglycerin’s potential advantages in ischemic contexts and support its preferential use in high-risk coronary artery disease patients within resource-constrained settings.
- Citation: Chaudhary AJ, Bhat WA, Ul Haq A, Rashid HU, Khan ID, Khan MND, Nawaz HMM, Ali S, Tariq MH. Efficacy of nitroglycerin vs labetalol in hypertensive emergency among patients with a history of coronary artery disease. World J Cardiol 2026; 18(2): 115528
- URL: https://www.wjgnet.com/1949-8462/full/v18/i2/115528.htm
- DOI: https://dx.doi.org/10.4330/wjc.v18.i2.115528
Hypertensive emergency represents a critical medical condition characterized by a severe elevation in blood pressure, typically exceeding 180/120 mmHg, coupled with acute end-organ damage[1]. This differs from hypertensive urgency, where blood pressure is similarly elevated but without immediate organ compromise[1,2]. The prevalence of hyper
The management of hypertensive emergencies requires prompt, controlled blood pressure reduction to mitigate organ damage[5-7]. American Heart Association (AHA) guidelines emphasize tailored therapy based on the clinical presen
Comparative studies on nitroglycerin vs labetalol in hypertensive emergencies are limited, with mixed results[11,12]. One trial in general hypertensive crises found labetalol achieved target blood pressure faster (96% vs 44% at 1 hour) with fewer add-on medications required[11]. However, in specific contexts like pre-eclampsia, nitroglycerin demonstrated superior efficacy (96% vs 87% success rate)[11]. In CAD patients, nitroglycerin’s coronary vasodilatory effects may confer advantages, though direct head-to-head data are scarce[12]. Guidelines suggest nitroglycerin for CAD-associated emergencies to improve myocardial perfusion, while labetalol is a viable alternative for broader use[13]. This gap highlights the need for targeted research.
The present retrospective study aims to evaluate the efficacy of nitroglycerin compared to labetalol in managing hypertensive emergencies among patients with a documented history of CAD. Unlike prior studies in general hypertensive crises or stroke, this research targets CAD patients in a real-world South Asian setting, assessing not only blood pressure control but also biomarkers and utilization to guide ischemic-specific management. By analyzing real-world data, this investigation seeks to provide evidence-based insights to optimize treatment strategies in this high-risk population, potentially informing future guidelines and reducing cardiovascular complications.
This retrospective cohort study was conducted at Northwest General Hospital and Research Centre in Peshawar, Pakistan. We reviewed electronic medical records (EMR) of adult patients (≥ 18 years) admitted with a hypertensive emergency [systolic blood pressure (SBP) > 180 mmHg or diastolic blood pressure (DBP) > 120 mmHg with end-organ damage] from January 1, 2018 to December 31, 2024. Eligible patients had a confirmed history of CAD and received either intravenous nitroglycerin or labetalol as the primary antihypertensive agent within the first hour of presentation. This study included all eligible patients identified from the EMR during the specified period; no formal sample size calculation was performed given the retrospective design. To address potential indication bias (e.g., clinicians selecting nitroglycerin for ischemic presentations or labetalol for tachycardia), multivariable models adjusted for presenting symptoms like chest pain, and baseline characteristics were balanced between groups.
Nitroglycerin was administered as a continuous IV infusion starting at 5 μg/minute, titrated by 5 μg/minute every 3-5 minutes up to 200 μg/minute based on blood pressure response. Labetalol was given as IV boluses of 10-20 mg every 10 minutes (max 300 mg) or infusion at 2 mg/minute, titrated to target. Protocols followed institutional guidelines aligned with AHA recommendations.
A standardized form was used to extract data on baseline demographics, cardiovascular history, comorbidities, and presenting clinical and hemodynamic parameters. Data extraction used a standardized EMR form by two trained reviewers, with inter-rater reliability verified (kappa > 0.8). Blood pressure was measured non-invasively via automated cuff every 5 minutes during initial treatment, verified by nursing records and physician notes. To address potential information bias from EMR data, data extraction was performed by trained reviewers using predefined criteria.
The primary efficacy outcome was the time to achieve target blood pressure (SBP < 160 mmHg and DBP < 100 mmHg). Secondary efficacy outcomes included the magnitude of blood pressure reduction and the proportion of patients achieving target blood pressure within 60 minutes. The primary safety outcome was a composite of major adverse cardiovascular events (MACEs), including all-cause mortality, non-fatal myocardial infarction (MI), non-fatal stroke, and urgent revascularization. Other safety outcomes included the incidence of hypotension (SBP < 90 mmHg), bradycardia (heart rate < 50 bpm), new or worsening heart failure (HF), and acute kidney injury. We also assessed healthcare utilization metrics, such as intensive care unit and hospital length of stay and 30-day readmission rates.
All statistical analyses were performed using R software (version 4.3.1). Continuous variables were presented as means with standard deviations and compared using independent t-tests (assuming normality based on data distribution). Categorical variables were presented as n (%) and analyzed with χ2 or Fisher’s exact tests. To assess the association between treatment and outcomes, both unadjusted (crude) and multivariable-adjusted logistic regression models were constructed. The adjusted models controlled for age, gender, history of MI, history of HF, diabetes mellitus, baseline SBP, and presenting with chest pain. Results are presented as odds ratios with 95% confidence intervals (CIs). Patients with missing data on key variables were excluded from the analysis (complete-case approach); there was no imputation as data were complete post-exclusion. Loss to follow-up for 30-day outcomes was minimal, as readmissions were captured via linked EMR and hospital records. A two-sided P < 0.05 was considered statistically significant.
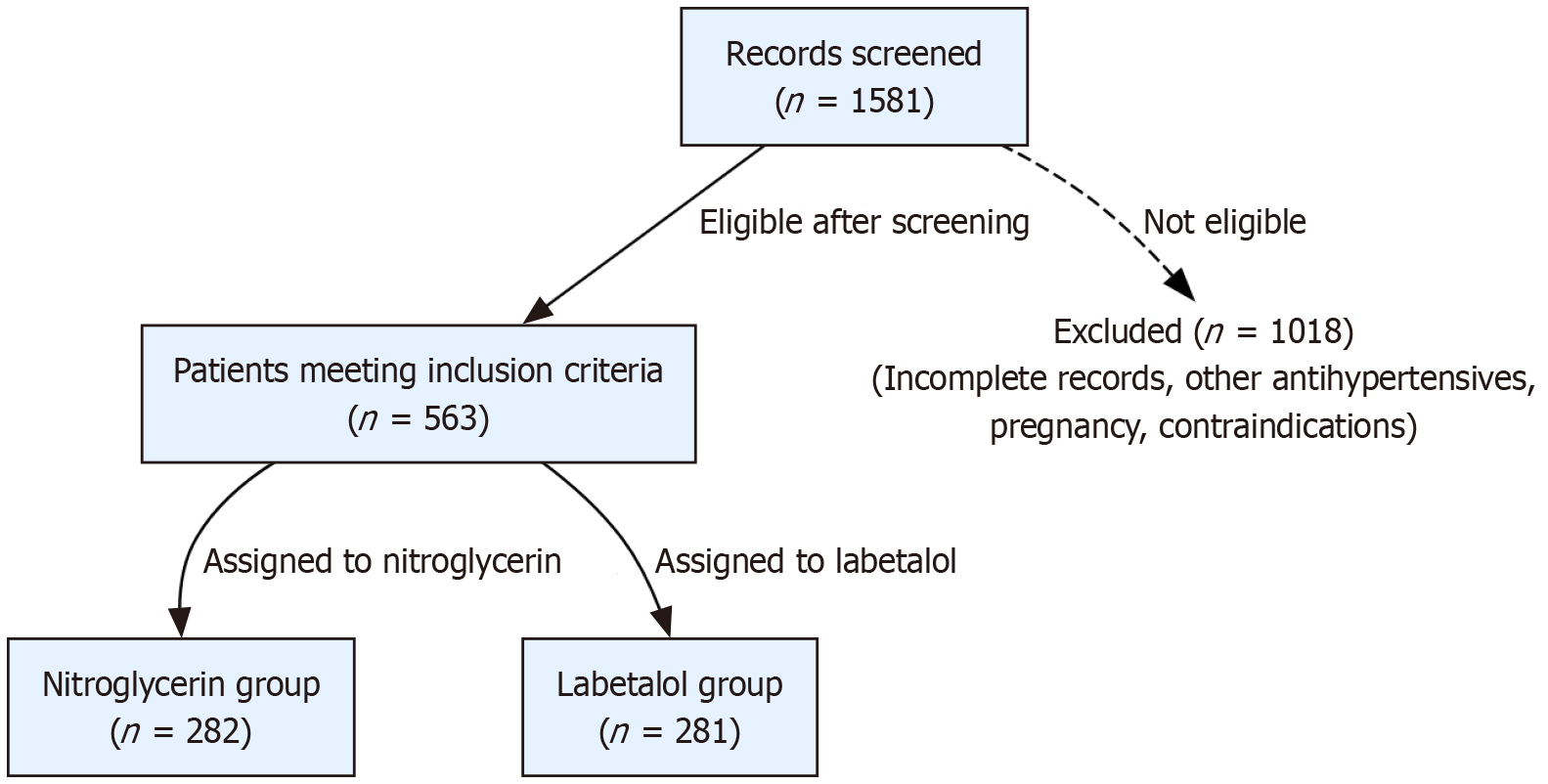
A total of 563 patients were included in the final analysis, with 282 allocated to the nitroglycerin group and 281 to the labetalol group, as detailed in the participant flow diagram (Figure 1). The baseline demographic and clinical characteristics were well-balanced between the two treatment arms (Table 1). There were no missing data for the variables reported. The mean age was 64.79 ± 10.25 years in the nitroglycerin group and 64.52 ± 9.80 years in the labetalol group (P = 0.718). Key cardiovascular comorbidities, including prior MI (38.7% vs 42.0%, P = 0.454) and HF (24.8% vs 20.3%, P = 0.233), were comparable. Baseline hemodynamics were also similar, with a mean initial SBP of 199.20 ± 20.03 mmHg in the nitroglycerin group and 198.54 ± 21.33 mmHg in the labetalol group (P = 0.727). Notably, a significantly higher proportion of patients in the labetalol group presented with chest pain (45.2% vs 36.5%, P = 0.039).
| Variable | Nitroglycerin (n = 282) | Labetalol (n = 281) | P value |
| Age (years) | 64.79 ± 10.25 | 64.52 ± 9.80 | 0.718 |
| Male | 176 (62.4) | 178 (63.3) | 0.847 |
| South Asian | 268 (95.0) | 269 (95.7) | 0.719 |
| History of MI | 109 (38.7) | 118 (42.0) | 0.454 |
| History of PCI/CABG | 94 (33.3) | 85 (30.2) | 0.469 |
| History of HF | 70 (24.8) | 57 (20.3) | 0.233 |
| LVEF (%) | 45.09 ± 9.84 | 45.07 ± 9.79 | 0.978 |
| History of stroke/TIA | 51 (18.1) | 45 (16.0) | 0.545 |
| PAD | 27 (9.6) | 21 (7.5) | 0.413 |
| AF | 58 (20.6) | 60 (21.4) | 0.833 |
| DM | 154 (54.6) | 142 (50.5) | 0.372 |
| eGFR (mL/min/1.73 m2) | 69.48 ± 20.45 | 71.86 ± 18.85 | 0.162 |
| Baseline SBP (mmHg) | 199.20 ± 20.03 | 198.54 ± 21.33 | 0.727 |
| Baseline DBP (mmHg) | 111.21 ± 14.60 | 110.22 ± 15.54 | 0.462 |
| Baseline HR (bpm) | 90.45 ± 14.11 | 90.08 ± 15.12 | 0.771 |
| Chest pain | 103 (36.5) | 127 (45.2) | 0.039 |
| Dyspnea | 92 (32.6) | 75 (26.7) | 0.138 |
| Neurological deficit | 52 (18.4) | 45 (16.0) | 0.494 |
| Initial creatinine (mg/dL) | 1.19 ± 0.52 | 1.19 ± 0.55 | 0.999 |
| Initial troponin (ng/mL) | 0.51 ± 0.32 | 0.53 ± 0.30 | 0.399 |
| ST changes on ECG | 82 (29.1) | 91 (32.4) | 0.443 |
| Home antihypertensives | 205 (72.7) | 187 (66.5) | 0.124 |
| Home antiplatelets | 174 (61.7) | 166 (59.1) | 0.559 |
| Home statins | 154 (54.6) | 142 (50.5) | 0.372 |
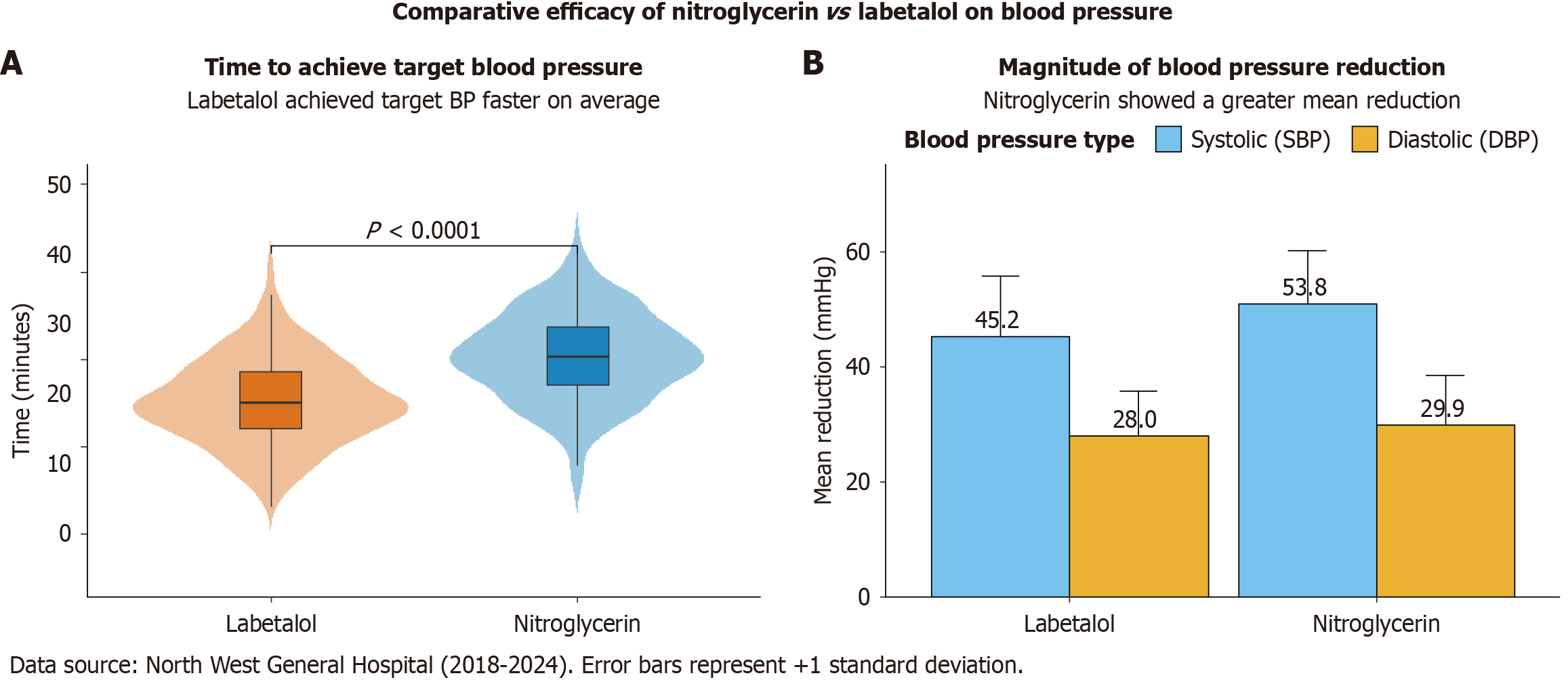
Efficacy of blood pressure control as illustrated in Figure 2A, labetalol was associated with a significantly faster time to achieve target blood pressure compared to nitroglycerin (mean 25.14 ± 4.92 minutes vs 30.38 ± 5.16 minutes, respectively; P < 0.0001). However, as shown in Figure 2B, treatment with nitroglycerin resulted in a greater mean reduction in both SBP (50.78 ± 9.45 mmHg vs 45.20 ± 10.46 mmHg; P < 0.0001) and DBP (29.86 ± 8.63 mmHg vs 28.02 ± 7.74 mmHg; P = 0.0079). The proportion of patients achieving target blood pressure within 60 minutes was similar between the two groups (Table 2).
| Outcome | Nitroglycerin (n = 282) | Labetalol (n = 281) | P value |
| Time to target BP (minute) | 30.38 ± 5.16 | 25.14 ± 4.92 | < 0.0001 |
| Achievement of target BP | 245 (86.9) | 246 (87.5) | 0.9124 |
| SBP reduction (mmHg) | 50.78 ± 9.45 | 45.20 ± 10.46 | < 0.0001 |
| DBP reduction (mmHg) | 29.86 ± 8.63 | 28.02 ± 7.74 | 0.0079 |
| MACE | 27 (9.6) | 35 (12.5) | 0.3384 |
| All-cause mortality | 12 (4.3) | 20 (7.1) | 0.199 |
| Non-fatal MI | 9 (3.2) | 17 (6.0) | 0.1571 |
| Non-fatal stroke | 14 (5.0) | 6 (2.1) | 0.1128 |
| Urgent revascularization | 2 (0.7) | 8 (2.8) | 0.1094 |
| Hypotension | 14 (5.0) | 8 (2.8) | 0.2806 |
| Bradycardia | 5 (1.8) | 28 (10.0) | < 0.0001 |
| New/worsening HF | 11 (3.9) | 19 (6.8) | 0.1857 |
| AKI | 17 (6.0) | 19 (6.8) | 0.8546 |
| Intensive care unit LOS (days) | 2.99 ± 1.04 | 3.54 ± 1.02 | < 0.0001 |
| Hospital LOS (days) | 6.92 ± 1.93 | 7.99 ± 2.06 | < 0.0001 |
| 30-day readmission | 20 (7.1) | 36 (12.8) | 0.0335 |
| Delta troponin (ng/mL) | 0.10 ± 0.05 | 0.21 ± 0.10 | < 0.0001 |
| Delta NT-proBNP (pg/mL) | 191.42 ± 101.72 | 287.63 ± 149.26 | < 0.0001 |
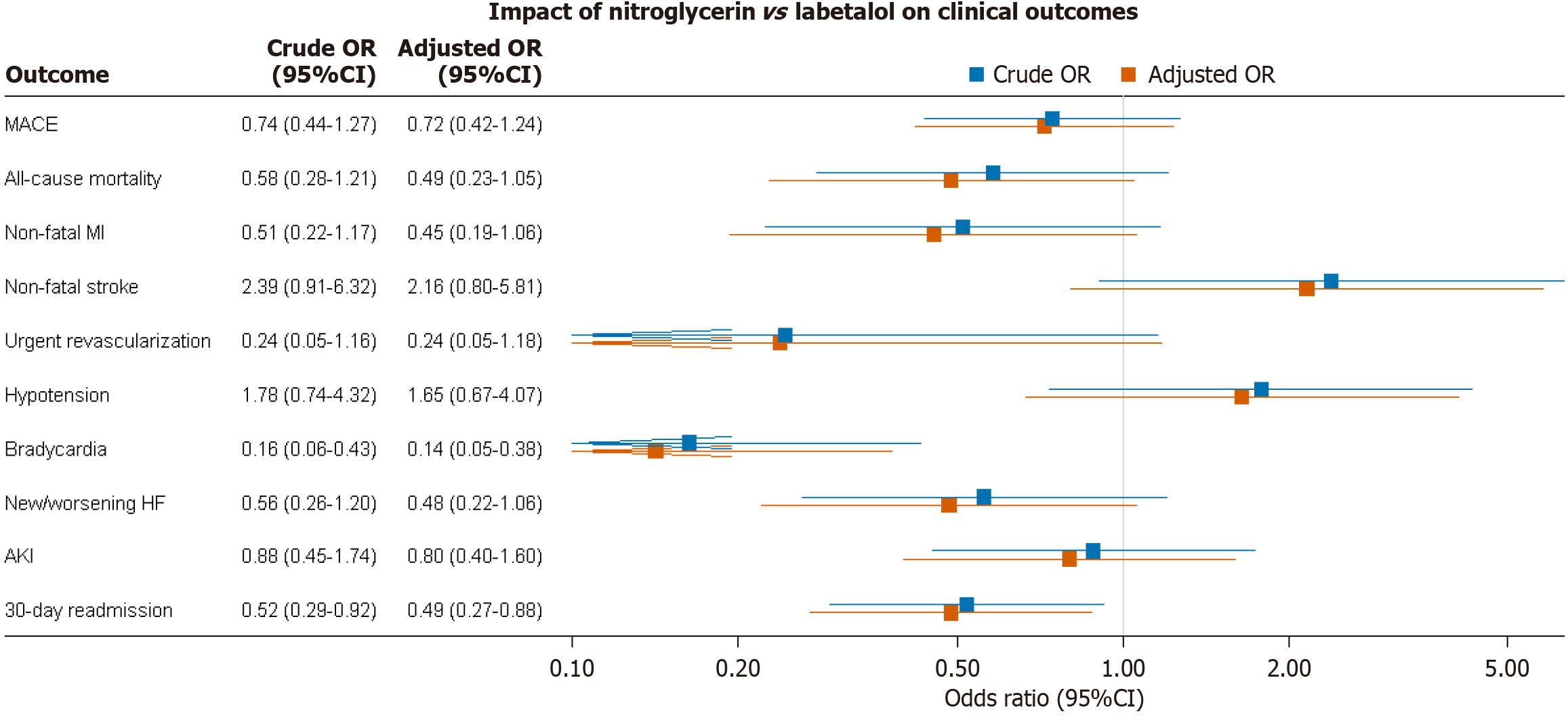
The overall incidence of MACE did not differ significantly between the groups, as detailed in Table 2. After adjusting for baseline covariates, nitroglycerin was associated with a non-significant trend toward lower odds of MACE [adjusted odds ratio (AOR): 0.72; 95%CI: 0.42-1.24], as shown in the forest plot in Figure 3. This trend was driven by numerically lower odds of all-cause mortality (AOR: 0.49; 95%CI: 0.23-1.05) and non-fatal MI (AOR: 0.45; 95%CI: 0.19-1.06), although these findings did not reach statistical significance. Conversely, nitroglycerin use was associated with higher odds of non-fatal stroke compared to labetalol (AOR: 2.16; 95%CI: 0.80-5.81).
Regarding the safety profile, patients receiving labetalol had a significantly higher incidence of bradycardia (10.0% vs 1.8%, P < 0.0001). The adjusted analysis confirmed that treatment with nitroglycerin was strongly protective against bradycardia (AOR: 0.14; 95%CI: 0.05-0.38) (Figure 3). Rates of hypotension, new or worsening HF, and acute kidney injury were not significantly different between the two groups (Table 2).
Patients treated with nitroglycerin had significantly shorter intensive care unit and hospital lengths of stay (Table 2). Furthermore, the 30-day readmission rate was significantly lower in the nitroglycerin group (7.1% vs 12.8%, P = 0.0335), a finding that remained significant after multivariable adjustment (AOR: 0.49; 95%CI: 0.27-0.88) (Figure 3). Treatment with nitroglycerin was also associated with significantly smaller increases in cardiac biomarkers, including delta troponin and delta N-terminal pro-B-type natriuretic peptide (NT-proBNP), compared to labetalol (Table 2).
This retrospective cohort study provides valuable real-world evidence on the comparative efficacy and safety of intravenous nitroglycerin vs labetalol for managing hypertensive emergencies in patients with a history of CAD. This study builds on prior comparisons by focusing on CAD in an underrepresented population, incorporating biomarkers and utilization metrics to highlight nitroglycerin's potential in ischemic emergencies. Analyzing data from 563 patients at a single center in Peshawar, Pakistan, from 2018 to 2024, our findings reveal that labetalol achieves target blood pressure more rapidly (mean 25.14 ± 4.92 minutes vs 30.38 ± 5.16 minutes; P < 0.0001), while nitroglycerin offers greater overall blood pressure reductions (systolic: 50.78 ± 9.45 mmHg vs 45.20 ± 10.46 mmHg, P < 0.0001; diastolic: 29.86 ± 8.63 mmHg vs 28.02 ± 7.74 mmHg, P = 0.0079), MACE rates were similar (9.6% vs 12.5%; P = 0.338), with no significant differences in components after adjustment, fewer bradycardic events (1.8% vs 10.0%, P < 0.0001), lower biomarker elevations (delta troponin: 0.10 ± 0.05 ng/mL vs 0.21 ± 0.10 ng/mL, P < 0.0001; absolute change NT-proBNP: 191.42 ± 101.72 pg/mL vs 287.63 ± 149.26 pg/mL, P < 0.0001), and improved healthcare utilization metrics, including shorter intensive care unit (2.99 ± 1.04 days vs 3.54 ± 1.02 days, P < 0.0001) and hospital lengths of stay (6.92 ± 1.93 days vs 7.99 ± 2.06 days, P < 0.0001) and lower 30-day readmission rates (7.1% vs 12.8%, P = 0.0335). These results underscore the nuanced trade-offs in pharmacologic choices for this vulnerable population, emphasizing the need for individualized therapy to balance expeditious blood pressure control with cardioprotection.
The superior speed of blood pressure reduction with labetalol aligns with its dual alpha- and beta-adrenergic blockade, enabling rapid vasodilation and heart rate modulation without pronounced reflex tachycardia[14]. This finding is consistent with prior comparative trials in general hypertensive crises, where labetalol achieved target blood pressure faster than nitroglycerin (e.g., 96% vs 44% at 1 hour) with minimal additional agents required[15]. In acute stroke settings, labetalol has similarly demonstrated quicker hemodynamic stabilization[16]. In our CAD-focused cohort, this rapidity may be especially pertinent for mitigating immediate end-organ damage in patients presenting with neurological deficits or dyspnea, though the approximately 5-minute difference’s clinical impact remains debatable in resource-constrained environments like Pakistan, where delays in care access could amplify its relevance[17]. Nonetheless, labetalol’s higher bradycardia incidence (AOR: 0.14 for nitroglycerin protection; 95%CI: 0.05-0.38) highlights potential risks in CAD patients with conduction issues or impaired ventricular function, warranting cautious use[18].
In contrast, nitroglycerin’s advantages in blood pressure magnitude and cardioprotective profile stem from its nitric oxide-mediated venodilation, which reduces preload and myocardial oxygen demand while enhancing coronary perfusion - critical in ischemic contexts[19]. MACE rates were similar (9.6% vs 12.5%; P = 0.338), with no significant differences in components after adjustment, as do the attenuated biomarker rises indicative of reduced cardiac strain[20]. These benefits resonate with evidence from perfusion studies showing nitroglycerin preserves peripheral and coronary flow better than labetalol during induced hypotension[21]. Comparable hypotension rates (5.0% vs 2.8%, P = 0.2806) challenge concerns over nitroglycerin’s vasodilatory risks, suggesting tolerability in CAD[22]. However, the numerically elevated non-fatal stroke rate (5.0% vs 2.1%, P = 0.1128; AOR: 2.16, 95%CI: 0.80-5.81) warrants investigation, potentially linked to cerebral autoregulation vulnerabilities or unadjusted confounders like baseline stroke history[23].
From a healthcare perspective, nitroglycerin's association with reduced resource use aligns with literature on agents that optimize myocardial outcomes, potentially lowering costs in low- and middle-income settings amid rising CAD burdens[24]. In Pakistan, where epidemiological shifts exacerbate hypertension-CAD overlap, these efficiencies could guide policy toward preferential nitroglycerin use in cardiac-dominant emergencies[25].
Our findings contextualize within contemporary guidelines. The 2025 AHA/American College of Cardiology guideline advocates individualized therapy, prioritizing nitroglycerin in CAD or acute coronary syndromes for its vasodilatory benefits[26]. The 2024 European Society of Cardiology guideline recommends labetalol for general crises but favors nitroglycerin in ischemia[27], while hypertension Canada’s 2025 updates emphasize lifestyle integration post-emergency to sustain control[28]. Emerging 2025 data on nitroglycerin-labetalol combinations suggest hybrid approaches for enhanced efficacy without compounded risks[29], meriting exploration in CAD.
Strengths include a large, real-world cohort with balanced baselines and multivariable adjustments for confounders like age, gender, and chest pain presentation. Limitations encompass retrospective biases, such as selection (e.g., clinician drug choice) and information inaccuracies from EMRs, despite trained extraction. Single-center design limits generalizability beyond South Asia, and short follow-up precludes long-term insights. Non-significant MACE trends may reflect underpowering, and unmeasured factors (e.g., dosing variations) could introduce residual confounding. Additional limitations include selection bias from retrospective design (e.g., non-randomized drug assignment) and indication bias, where nitroglycerin may have been preferred for chest pain (higher in labetalol group, P = 0.039), potentially con
Future studies should employ prospective, multicenter randomized designs with propensity matching to address biases[30]. Deeper biomarker analyses, including serial troponin/NT-proBNP, could clarify mechanisms[31]. Investigating combinations[29] or alternatives like nicardipine, which systematic reviews show are comparable to labetalol in crises[32], may refine algorithms.
In conclusion, while labetalol excels in speed, nitroglycerin appears preferable for CAD-associated hypertensive emergencies, offering superior reduction, safety, and efficiency. Clinicians should tailor selections to ischemia presence, aligning with guidelines to enhance global cardiovascular care in high-risk groups.
| 1. | Taylor DA. Hypertensive Crisis: A Review of Pathophysiology and Treatment. Crit Care Nurs Clin North Am. 2015;27:439-447. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 20] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 2. | Miller JB, Hrabec D, Krishnamoorthy V, Kinni H, Brook RD. Evaluation and management of hypertensive emergency. BMJ. 2024;386:e077205. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 17] [Article Influence: 8.5] [Reference Citation Analysis (0)] |
| 3. | Desta DM, Wondafrash DZ, Tsadik AG, Kasahun GG, Tassew S, Gebrehiwot T, Asgedom SW. Prevalence of Hypertensive Emergency and Associated Factors Among Hospitalized Patients with Hypertensive Crisis: A Retrospective Cross-Sectional Study. Integr Blood Press Control. 2020;13:95-102. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 17] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 4. | Siddiqi TJ, Usman MS, Rashid AM, Javaid SS, Ahmed A, Clark D 3rd, Flack JM, Shimbo D, Choi E, Jones DW, Hall ME. Clinical Outcomes in Hypertensive Emergency: A Systematic Review and Meta-Analysis. J Am Heart Assoc. 2023;12:e029355. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 33] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 5. | Rosendorff C, Lackland DT, Allison M, Aronow WS, Black HR, Blumenthal RS, Cannon CP, de Lemos JA, Elliott WJ, Findeiss L, Gersh BJ, Gore JM, Levy D, Long JB, O'Connor CM, O'Gara PT, Ogedegbe G, Oparil S, White WB; American Heart Association, American College of Cardiology, and American Society of Hypertension. Treatment of hypertension in patients with coronary artery disease: a scientific statement from the American Heart Association, American College of Cardiology, and American Society of Hypertension. Circulation. 2015;131:e435-e470. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 113] [Cited by in RCA: 99] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 6. | Aronow WS. Treatment of hypertensive emergencies. Ann Transl Med. 2017;5:S5. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 37] [Cited by in RCA: 25] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 7. | Balahura AM, Moroi ȘI, Scafa-Udrişte A, Weiss E, Japie C, Bartoş D, Bădilă E. The Management of Hypertensive Emergencies-Is There a "Magical" Prescription for All? J Clin Med. 2022;11:3138. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 13] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 8. | Nitroglycerin. 2024 Oct 15. In: Drugs and Lactation Database (LactMed®) [Internet]. Bethesda (MD): National Institute of Child Health and Human Development; 2006. [PubMed] |
| 9. | MacCarthy EP, Bloomfield SS. Labetalol: a review of its pharmacology, pharmacokinetics, clinical uses and adverse effects. Pharmacotherapy. 1983;3:193-219. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 148] [Cited by in RCA: 121] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 10. | Sun L, Chen J. Evaluation of the clinical application of information-motivation-behavior model care combined with labetalol pharmacotherapy for patients with hypertensive disorders of pregnancy: a randomized controlled study for improving pregnancy outcomes. Front Med (Lausanne). 2025;12:1627725. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 11. | Sreelal TP, Thulaseedharan JV, Nair S, Ravindran RM, Vijayakumar K, Varma RP. Hypertension control in Kerala, India: A prescription-based study at primary and secondary level health care institutions. Indian Heart J. 2022;74:296-301. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 12. | Ali RM, Salah D. Nitroglycerin versus labetalol to control the blood pressure in acute severe pre-eclampsia. Egypt J Anaesth. 2022;38:453-458. [RCA] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 13. | Rubenstein EB, Escalante C. Hypertensive crisis. Crit Care Clin. 1989;5:477-495. [PubMed] |
| 14. | Chon EM, Middleton RK. Labetalol hepatotoxicity. Ann Pharmacother. 1992;26:344-345. [PubMed] |
| 15. | Booker WA, Siddiq Z, Huang Y, Ananth CV, Wright JD, Cleary KL, DʼAlton ME, Friedman AM. Use of Antihypertensive Medications and Uterotonics During Delivery Hospitalizations in Women With Asthma. Obstet Gynecol. 2018;132:185-192. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 10] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 16. | Liu-Deryke X, Janisse J, Coplin WM, Parker D Jr, Norris G, Rhoney DH. A comparison of nicardipine and labetalol for acute hypertension management following stroke. Neurocrit Care. 2008;9:167-176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 50] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 17. | Jafar TH, Jafary FH, Jessani S, Chaturvedi N. Heart disease epidemic in Pakistan: women and men at equal risk. Am Heart J. 2005;150:221-226. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 86] [Cited by in RCA: 73] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 18. | Richards DA, Prichard BN. Clinical pharmacology of labetalol. Br J Clin Pharmacol. 1979;8:89S-93S. [PubMed] |
| 19. | Sorkin EM, Brogden RN, Romankiewicz JA. Intravenous glyceryl trinitrate (nitroglycerin). A review of its pharmacological properties and therapeutic efficacy. Drugs. 1984;27:45-80. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 36] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 20. | Walker HJ, Geniton DJ. Vasodilator therapy and the anesthetist: a review of nitroprusside, labetalol, hydralazine and nitroglycerin. AANA J. 1989;57:435-444. [PubMed] |
| 21. | Xie C, He M, Xiang Y. Nitroglycerin plus clopidogrel for acute myocardial infarction and the effect on cardiac function indices. Pak J Pharm Sci. 2023;36:973-979. [PubMed] |
| 22. | Peacock WF, Varon J, Baumann BM, Borczuk P, Cannon CM, Chandra A, Cline DM, Diercks D, Hiestand B, Hsu A, Jois-Bilowich P, Kaminski B, Levy P, Nowak RM, Schrock JW. CLUE: a randomized comparative effectiveness trial of IV nicardipine versus labetalol use in the emergency department. Crit Care. 2011;15:R157. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 53] [Cited by in RCA: 46] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 23. | RIGHT-2 Investigators. Prehospital transdermal glyceryl trinitrate in patients with ultra-acute presumed stroke (RIGHT-2): an ambulance-based, randomised, sham-controlled, blinded, phase 3 trial. Lancet. 2019;393:1009-1020. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 167] [Cited by in RCA: 157] [Article Influence: 22.4] [Reference Citation Analysis (0)] |
| 24. | Gaziano TA, Bitton A, Anand S, Weinstein MC; International Society of Hypertension. The global cost of nonoptimal blood pressure. J Hypertens. 2009;27:1472-1477. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 221] [Cited by in RCA: 184] [Article Influence: 10.8] [Reference Citation Analysis (0)] |
| 25. | Peddi NC, Avanthika C, Vuppalapati S, Balasubramanian R, Kaur J, N CD. A Review of Cordocentesis: Percutaneous Umbilical Cord Blood Sampling. Cureus. 2021;13:e16423. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 26. | Writing Committee Members*; Jones DW, Ferdinand KC, Taler SJ, Johnson HM, Shimbo D, Abdalla M, Altieri MM, Bansal N, Bello NA, Bress AP, Carter J, Cohen JB, Collins KJ, Commodore-Mensah Y, Davis LL, Egan B, Khan SS, Lloyd-Jones DM, Melnyk BM, Mistry EA, Ogunniyi MO, Schott SL, Smith SC Jr, Talbot AW, Vongpatanasin W, Watson KE, Whelton PK, Williamson JD. 2025 AHA/ACC/AANP/AAPA/ABC/ACCP/ACPM/AGS/AMA/ASPC/NMA/PCNA/SGIM Guideline for the Prevention, Detection, Evaluation and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Hypertension. 2025;82:e212-e316. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 166] [Cited by in RCA: 140] [Article Influence: 140.0] [Reference Citation Analysis (0)] |
| 27. | McEvoy JW, McCarthy CP, Bruno RM, Brouwers S, Canavan MD, Ceconi C, Christodorescu RM, Daskalopoulou SS, Ferro CJ, Gerdts E, Hanssen H, Harris J, Lauder L, McManus RJ, Molloy GJ, Rahimi K, Regitz-Zagrosek V, Rossi GP, Sandset EC, Scheenaerts B, Staessen JA, Uchmanowicz I, Volterrani M, Touyz RM; ESC Scientific Document Group. 2024 ESC Guidelines for the management of elevated blood pressure and hypertension. Eur Heart J. 2024;45:3912-4018. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1685] [Cited by in RCA: 1416] [Article Influence: 708.0] [Reference Citation Analysis (0)] |
| 28. | Rabi DM, McBrien KA, Sapir-Pichhadze R, Nakhla M, Ahmed SB, Dumanski SM, Butalia S, Leung AA, Harris KC, Cloutier L, Zarnke KB, Ruzicka M, Hiremath S, Feldman RD, Tobe SW, Campbell TS, Bacon SL, Nerenberg KA, Dresser GK, Fournier A, Burgess E, Lindsay P, Rabkin SW, Prebtani APH, Grover S, Honos G, Alfonsi JE, Arcand J, Audibert F, Benoit G, Bittman J, Bolli P, Côté AM, Dionne J, Don-Wauchope A, Edwards C, Firoz T, Gabor JY, Gilbert RE, Grégoire JC, Gryn SE, Gupta M, Hannah-Shmouni F, Hegele RA, Herman RJ, Hill MD, Howlett JG, Hundemer GL, Jones C, Kaczorowski J, Khan NA, Kuyper LM, Lamarre-Cliche M, Lavoie KL, Leiter LA, Lewanczuk R, Logan AG, Magee LA, Mangat BK, McFarlane PA, McLean D, Michaud A, Milot A, Moe GW, Penner SB, Pipe A, Poppe AY, Rey E, Roerecke M, Schiffrin EL, Selby P, Sharma M, Shoamanesh A, Sivapalan P, Townsend RR, Tran K, Trudeau L, Tsuyuki RT, Vallée M, Woo V, Bell AD, Daskalopoulou SS. Hypertension Canada's 2020 Comprehensive Guidelines for the Prevention, Diagnosis, Risk Assessment, and Treatment of Hypertension in Adults and Children. Can J Cardiol. 2020;36:596-624. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 390] [Cited by in RCA: 377] [Article Influence: 62.8] [Reference Citation Analysis (0)] |
| 29. | Yang Z, Zhao J. Effectiveness of placental blood perfusion monitoring of nitroglycerin and labetalol in treatment of women with pregnancy-induced hypertension. Afr J Reprod Health. 2025;29:61-68. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 30. | Austin PC. An Introduction to Propensity Score Methods for Reducing the Effects of Confounding in Observational Studies. Multivariate Behav Res. 2011;46:399-424. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9896] [Cited by in RCA: 8275] [Article Influence: 551.7] [Reference Citation Analysis (5)] |
| 31. | Morrow DA, Antman EM. Evaluation of high-sensitivity assays for cardiac troponin. Clin Chem. 2009;55:5-8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 59] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 32. | Peacock WF 4th, Hilleman DE, Levy PD, Rhoney DH, Varon J. A systematic review of nicardipine vs labetalol for the management of hypertensive crises. Am J Emerg Med. 2012;30:981-993. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 63] [Cited by in RCA: 46] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/