Copyright: ©Author(s) 2026.
World J Cardiol. Mar 26, 2026; 18(3): 117821
Published online Mar 26, 2026. doi: 10.4330/wjc.v18.i3.117821
Published online Mar 26, 2026. doi: 10.4330/wjc.v18.i3.117821
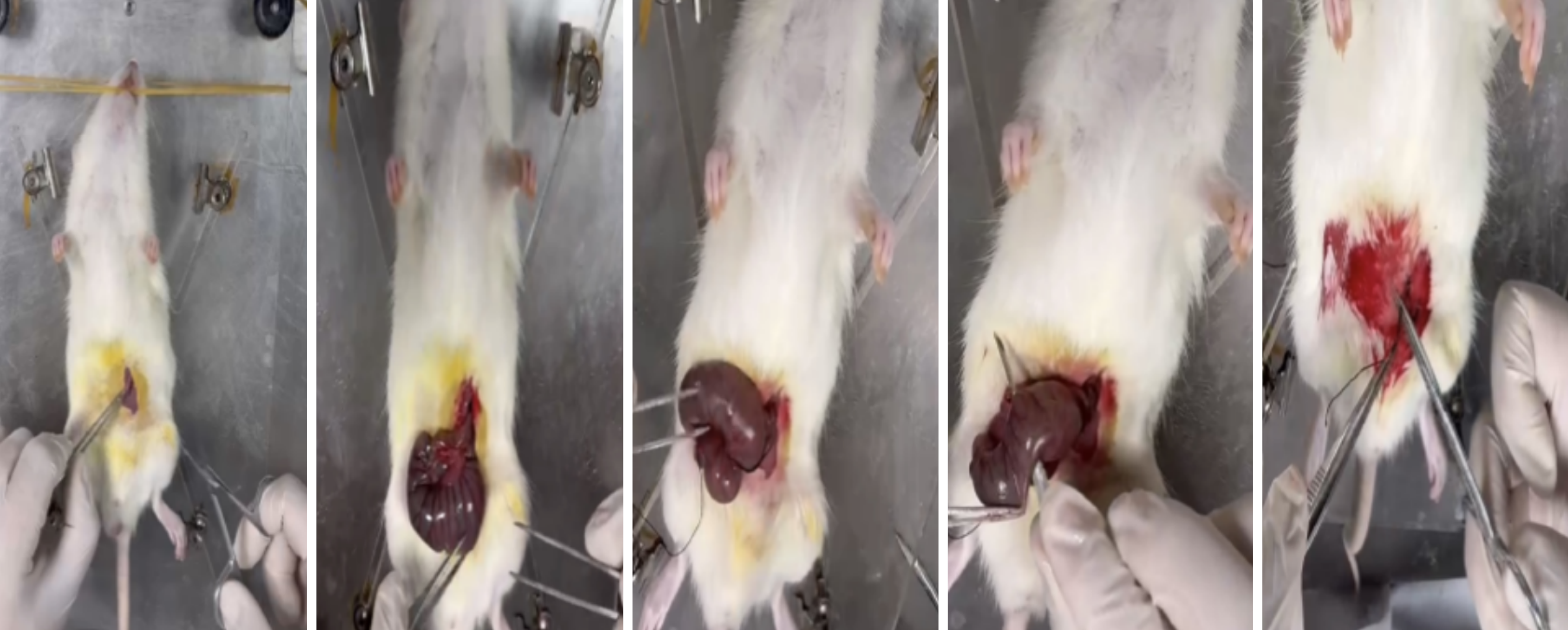
Figure 1 Schematic diagram of the rat sepsis model protocol.
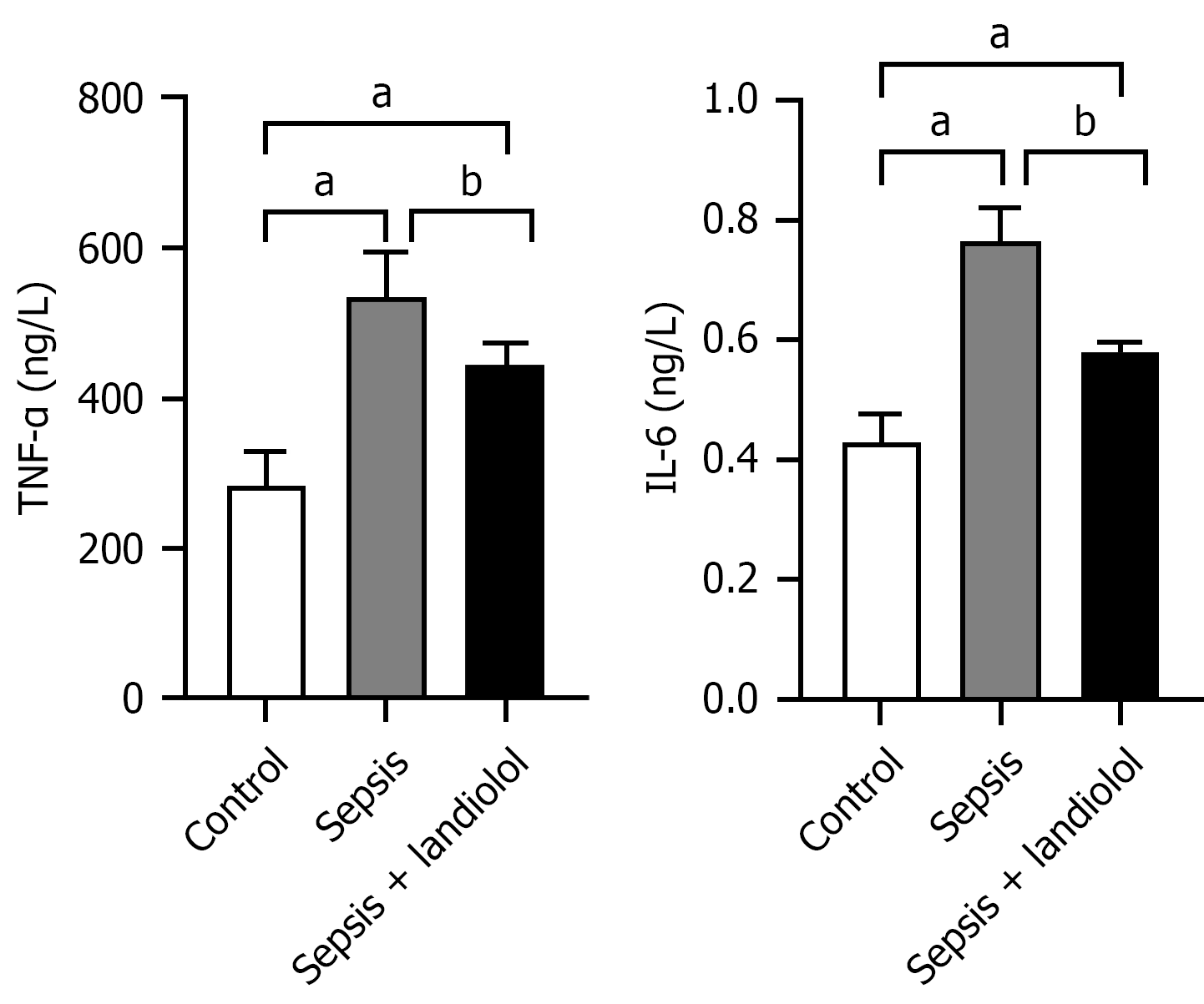
Figure 2 Comparison of tumor necrosis factor-α and interleukin-6 expression levels among the three groups.
aP < 0.05 vs control, bP < 0.05 vs sepsis group, n = 8. TNF-α: Tumor necrosis factor-α; IL-6: Interleukin-6.
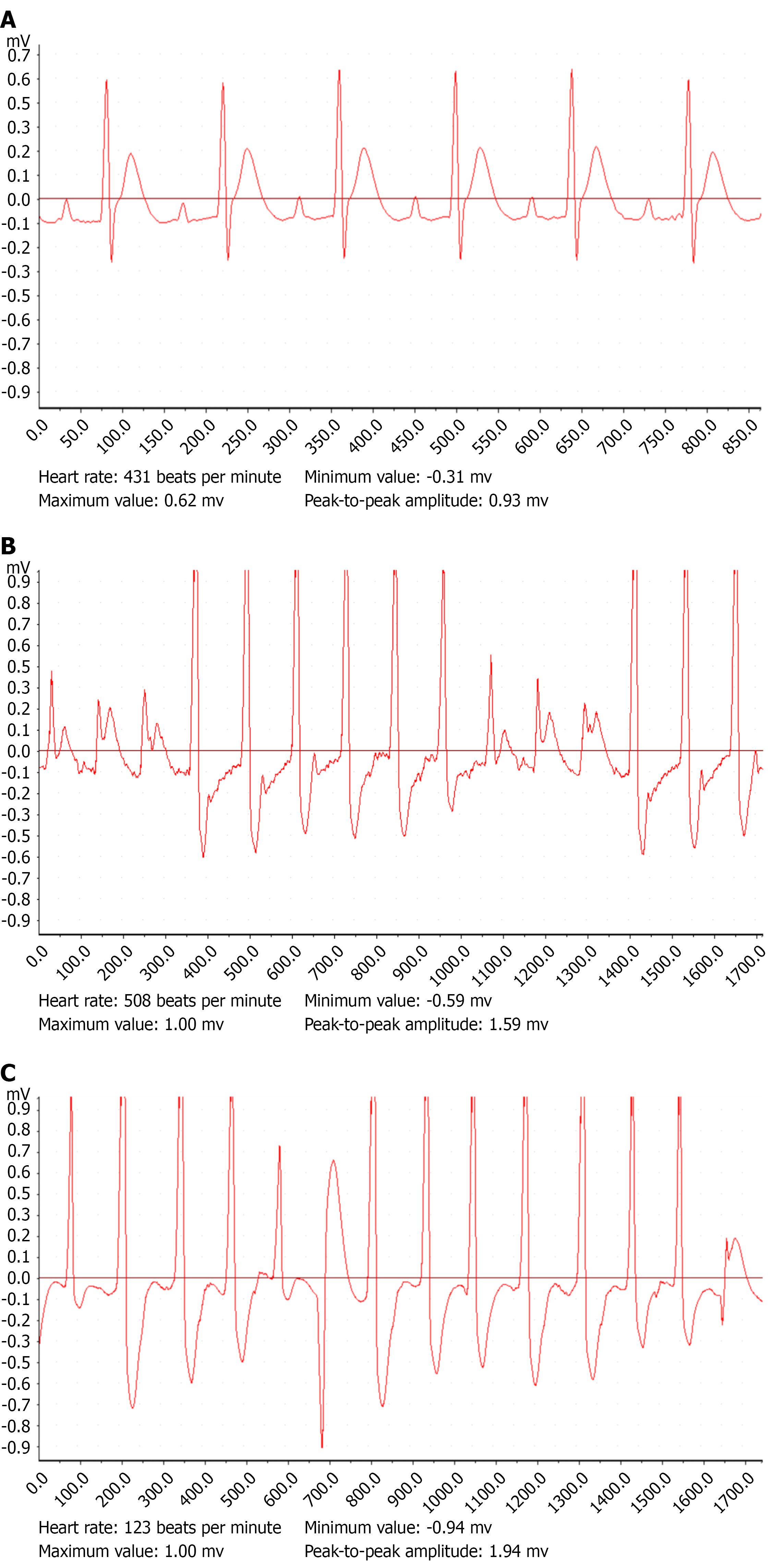
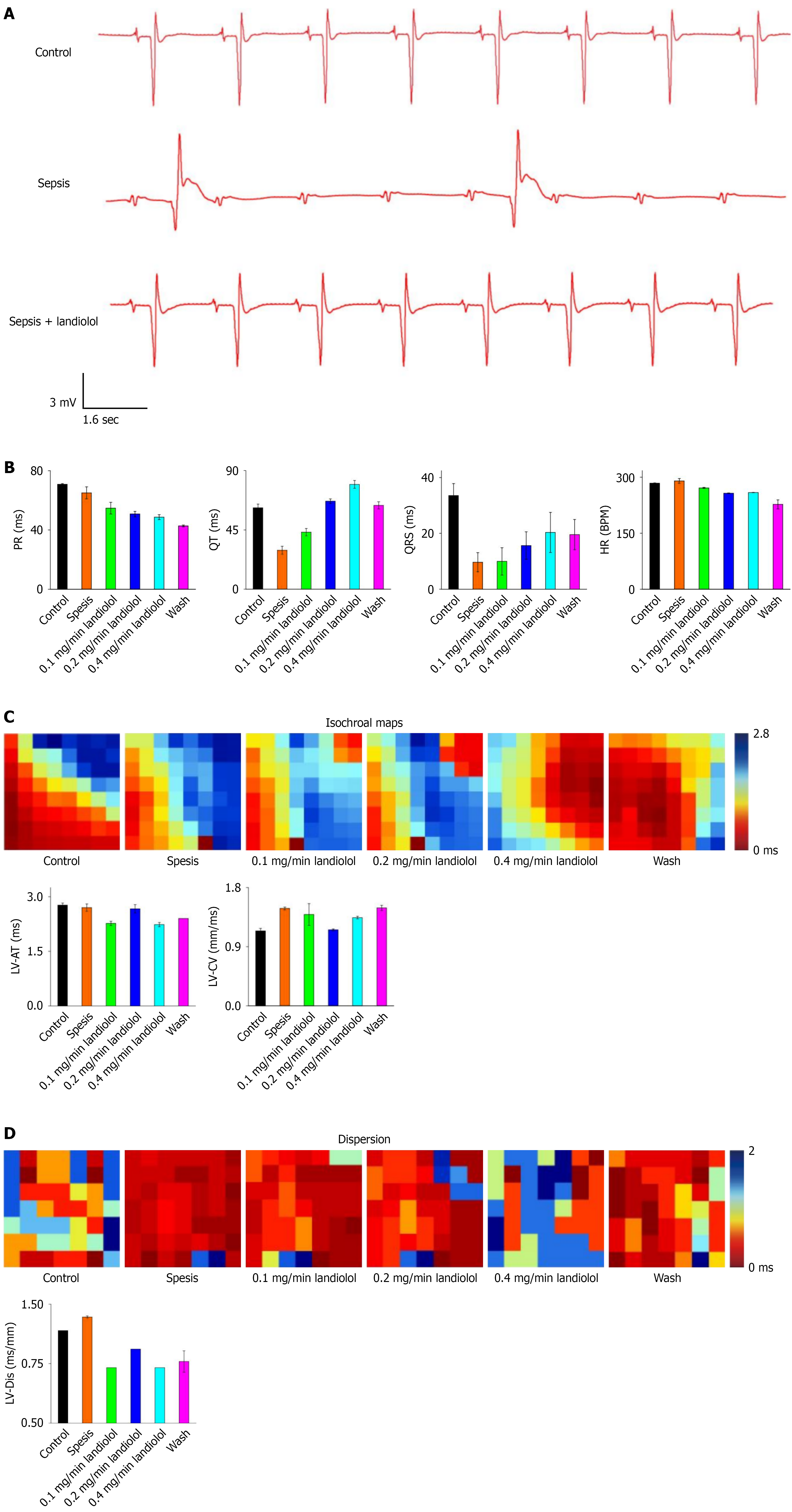
Figure 3 Comparison of the electrocardiogram in the three groups.
A: Control group; B: Sepsis model group; C: Sepsis model + landiolol group.
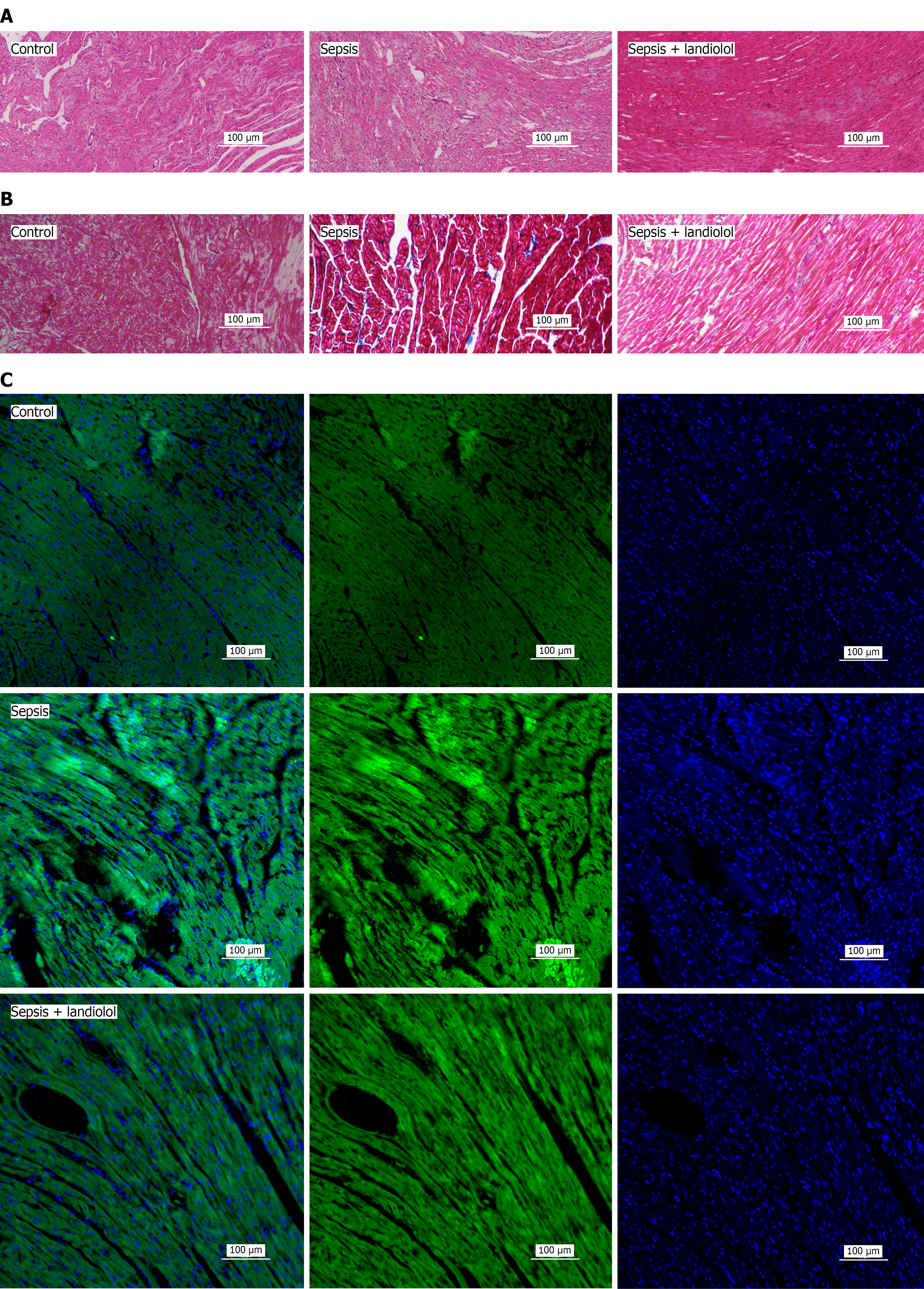
Figure 4 Landiolol inhibits the production of inflammatory cells in the ventricular myocardium of sepsis rats and reduces myocardial cell apoptosis, thereby inhibiting fibrosis.
A: Comparison of hematoxylin and eosin staining results in rat hearts; B: Quantitative comparison of Masson-stained myocardial fibrosis degree in the different experimental groups; C: Subcellular alterations in myocardial cells observed by confocal microscopy. From left to right in each column: Full-field view → FITC channel (green, target protein) → 4’-6-diamidino-2-phenylindole channel (blue, nuclei). Original magnification: 20 ×, n = 3.
Figure 5 Landiolol reverses the abnormal conduction velocity of ventricular myocytes in septic rats, and significantly reduces con
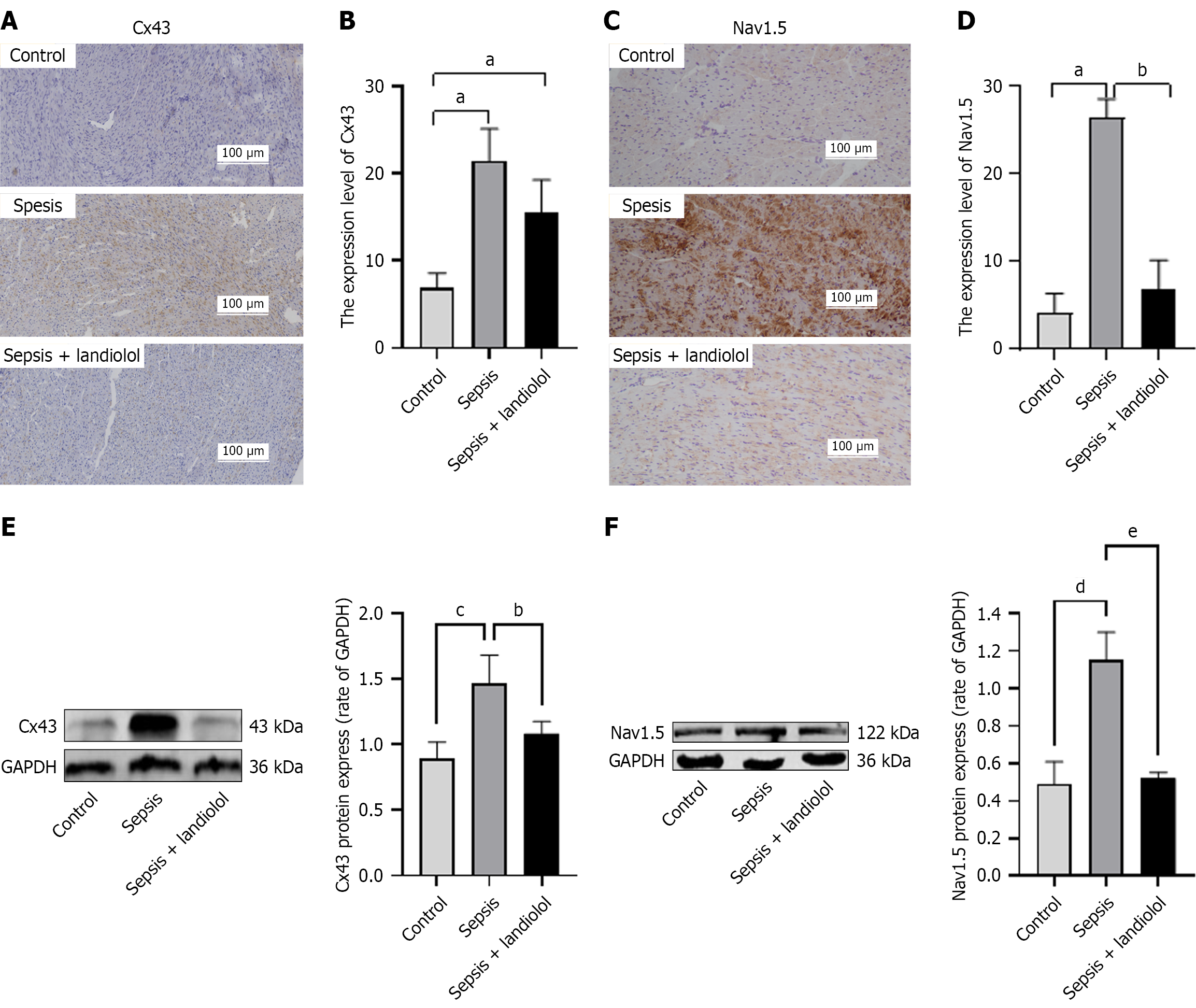
Figure 6 Comparative analysis of connexin-43 expression via immunohistochemistry across the experimental groups.
A: Immuno
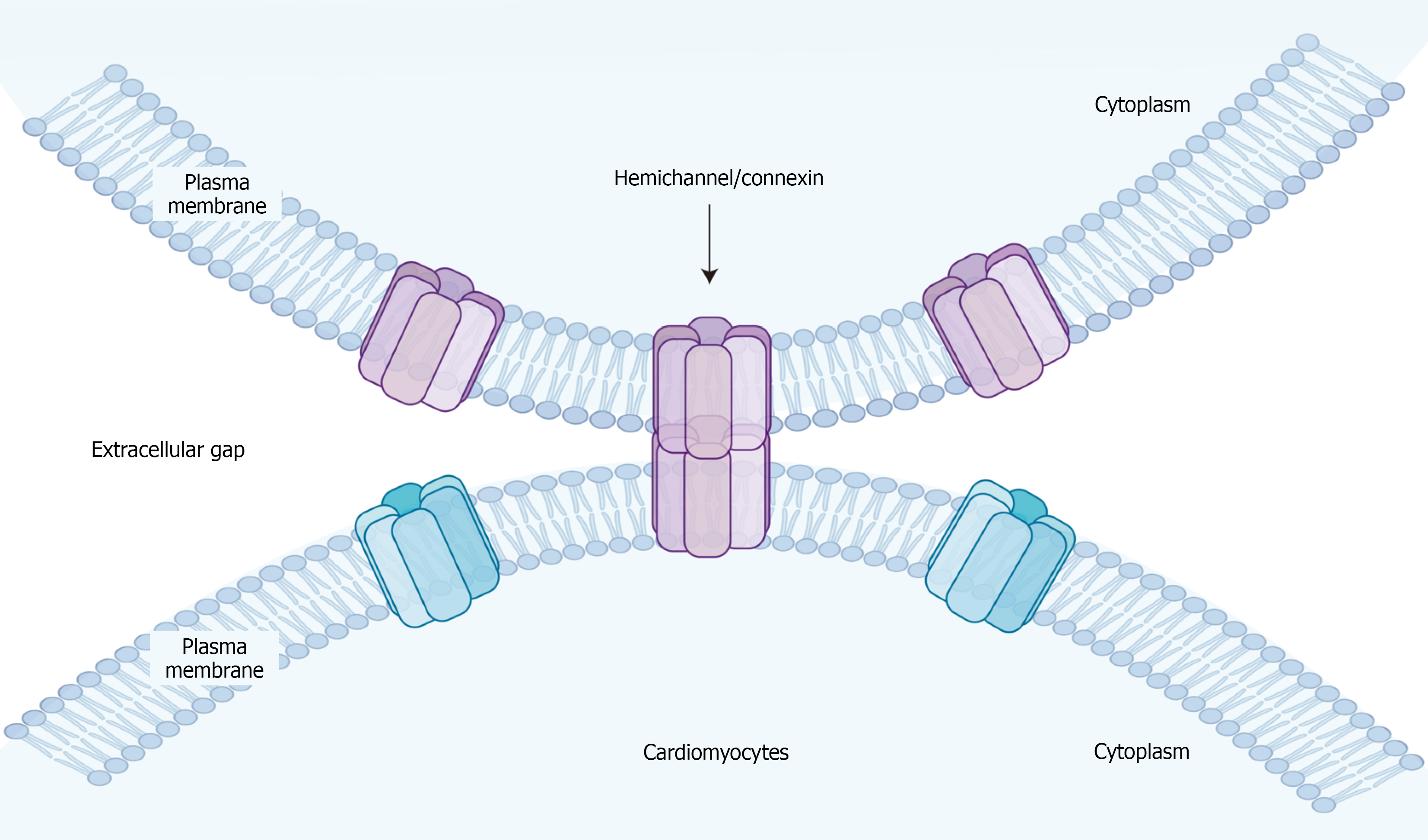
Figure 7 Schematic representation of gap junctions between myocardial cells.
The cell membrane contains a hemichannel composed of six connexins, with the left and right sides remaining unconnected hemichannels, while the central portion consists of two hemichannels that interconnect to form a complete gap junction channel. This channel allows direct molecular passage, facilitating the transfer of substances between adjacent cells.
- Citation: Hu PF, Bai LY, Zhao M, Ma KY, Xuan LY, Qi X. Landiolol modulates sodium 1.5 ion and connexin-43 to reduce sepsis ventricular arrhythmias. World J Cardiol 2026; 18(3): 117821
- URL: https://www.wjgnet.com/1949-8462/full/v18/i3/117821.htm
- DOI: https://dx.doi.org/10.4330/wjc.v18.i3.117821