Copyright: ©Author(s) 2026.
World J Cardiol. Mar 26, 2026; 18(3): 116789
Published online Mar 26, 2026. doi: 10.4330/wjc.v18.i3.116789
Published online Mar 26, 2026. doi: 10.4330/wjc.v18.i3.116789
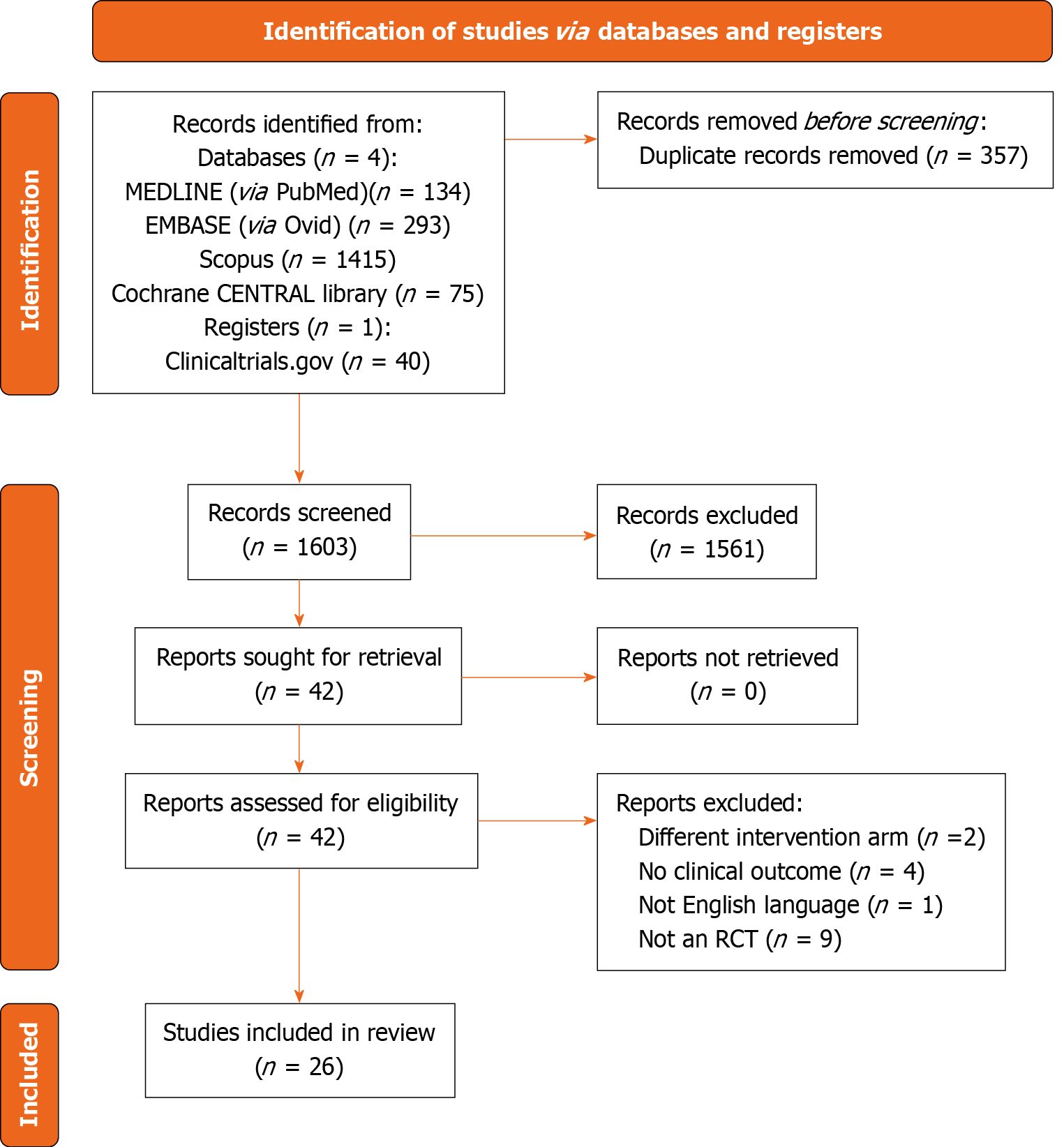
Figure 1 PRISMA flow diagram.
RCT: Randomized controlled trial.
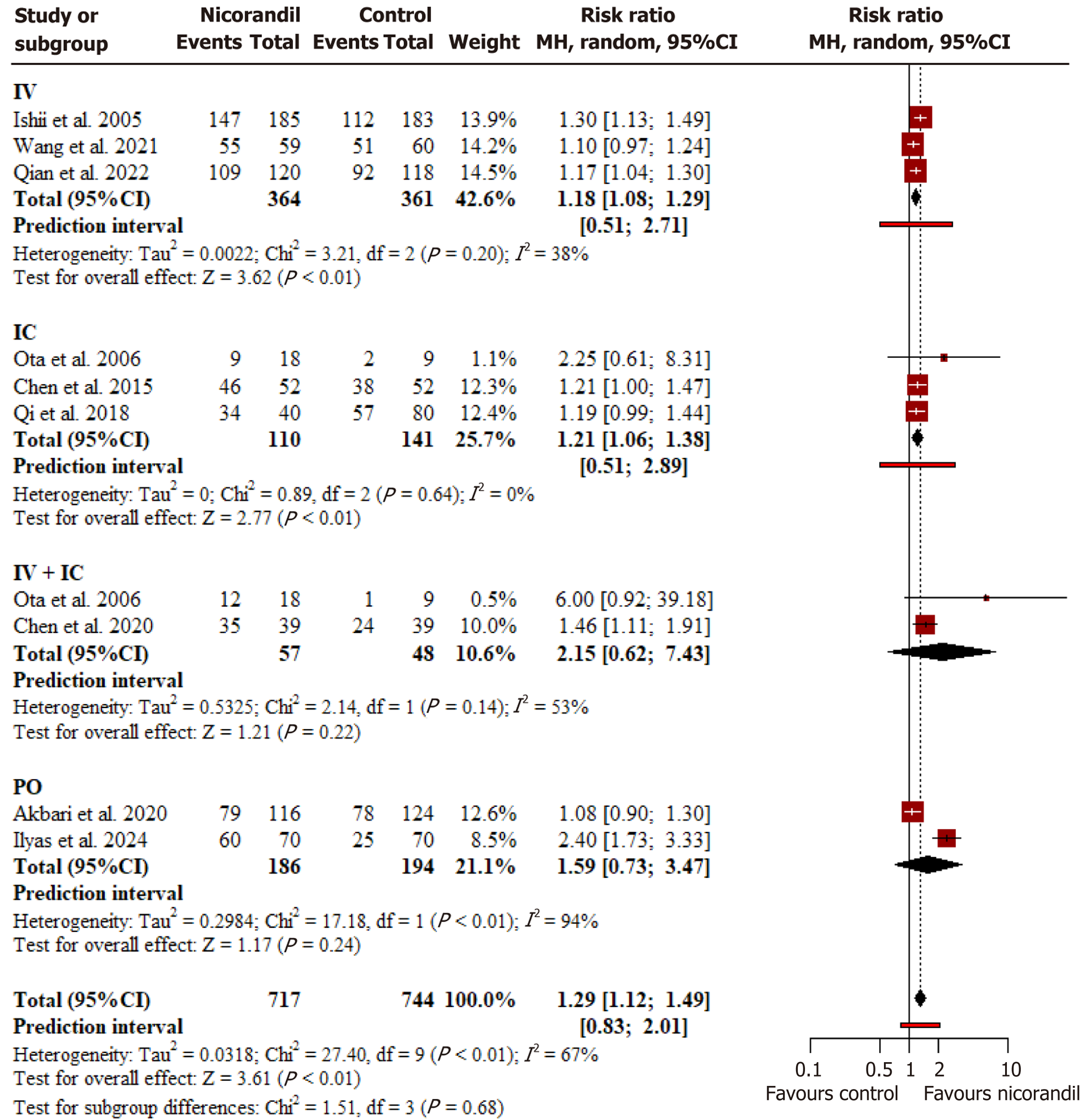
Figure 2 Forest plot for ST-segment resolution following percutaneous coronary intervention.
The overall pooled analysis demonstrated a significantly higher rate of complete ST-segment resolution with nicoranadil compared with control. Subgroup analysis stratified by route of administration showed no statistically significant difference. MH: Mantel-Haenszel; CI: Confidence interval; IV: Intravenous; IC: Intracoronary; PO: Per orem.
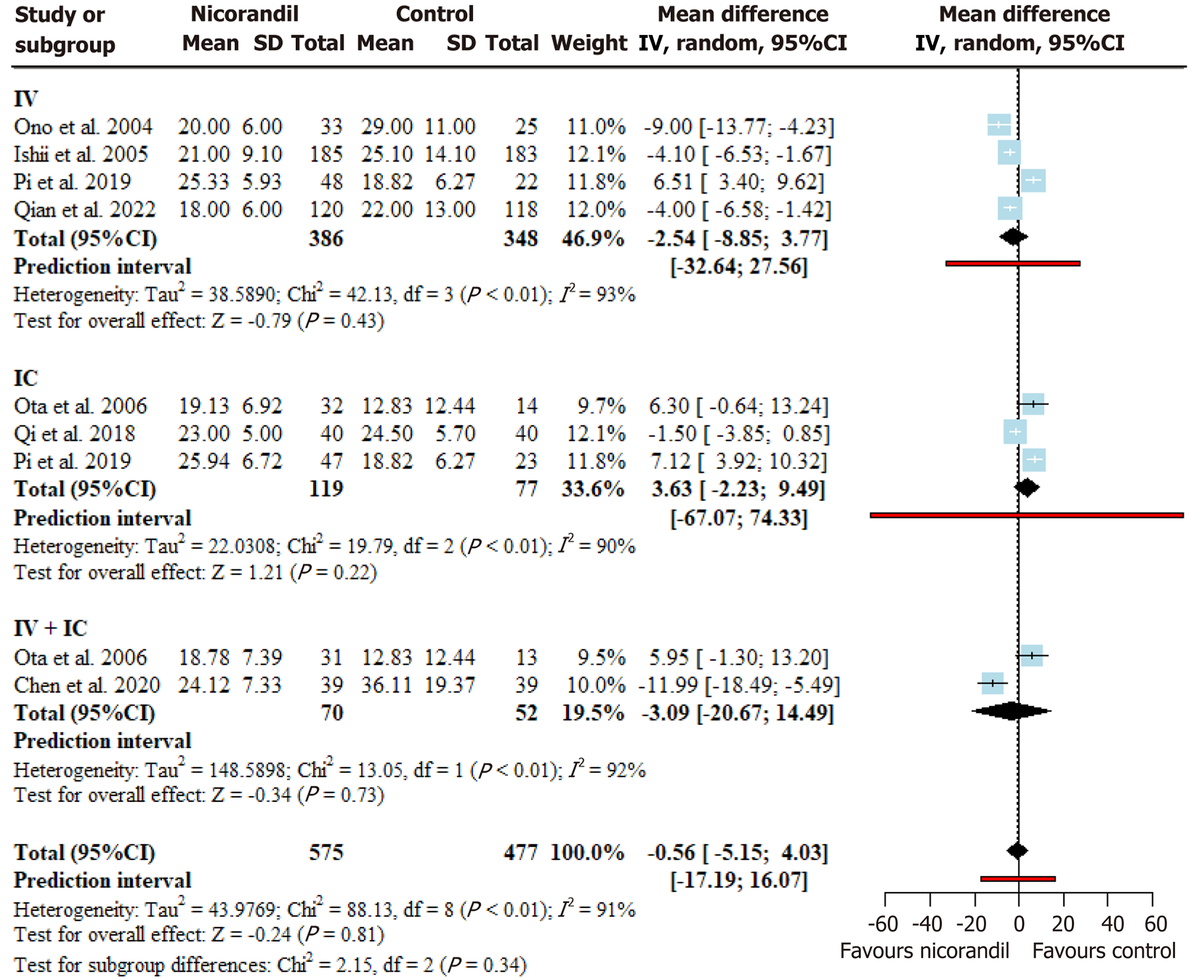
Figure 3 Forest plot for corrected Thrombolysis in Myocardial Infarction frame count.
The pooled and subgroup analysis showed no significant difference between nicoranadil and the control group. Substantial heterogeneity was noted in the overall and subgroup analyses. CI: Confidence interval; IV: Intravenous; IC: Intracoronary.
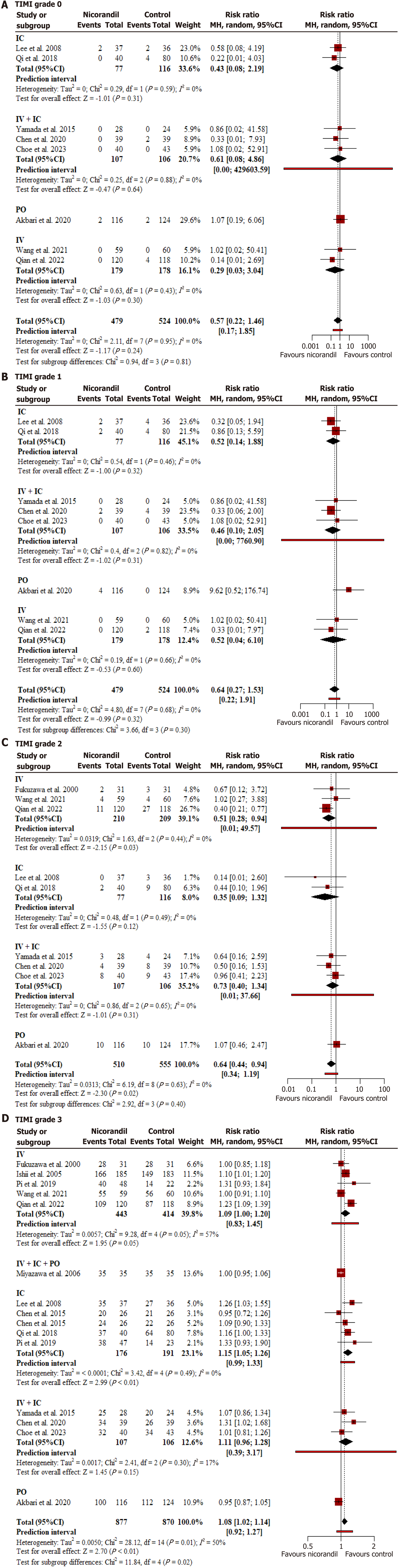
Figure 4 Forest plot for Thrombolysis in Myocardial Infarction grades (0, 1, 2, and 3).
A: Thrombolysis in Myocardial Infarction (TIMI) grades 0; B: TIMI grades 1; C: TIMI grades 2; D: TIMI grades 3. Nicorandil was associated with a higher incidence of TIMI grade 3 and a lower incidence of TIMI grade 2, while no statistically significant differences were observed for TIMI grades 0 or 1. Subgroup analysis for TIMI grade 3 demonstrated significant differences by route of administration. MH: Mantel-Haenszel; CI: Confidence interval; IV: Intravenous; IC: Intracoronary; PO: Per orem.
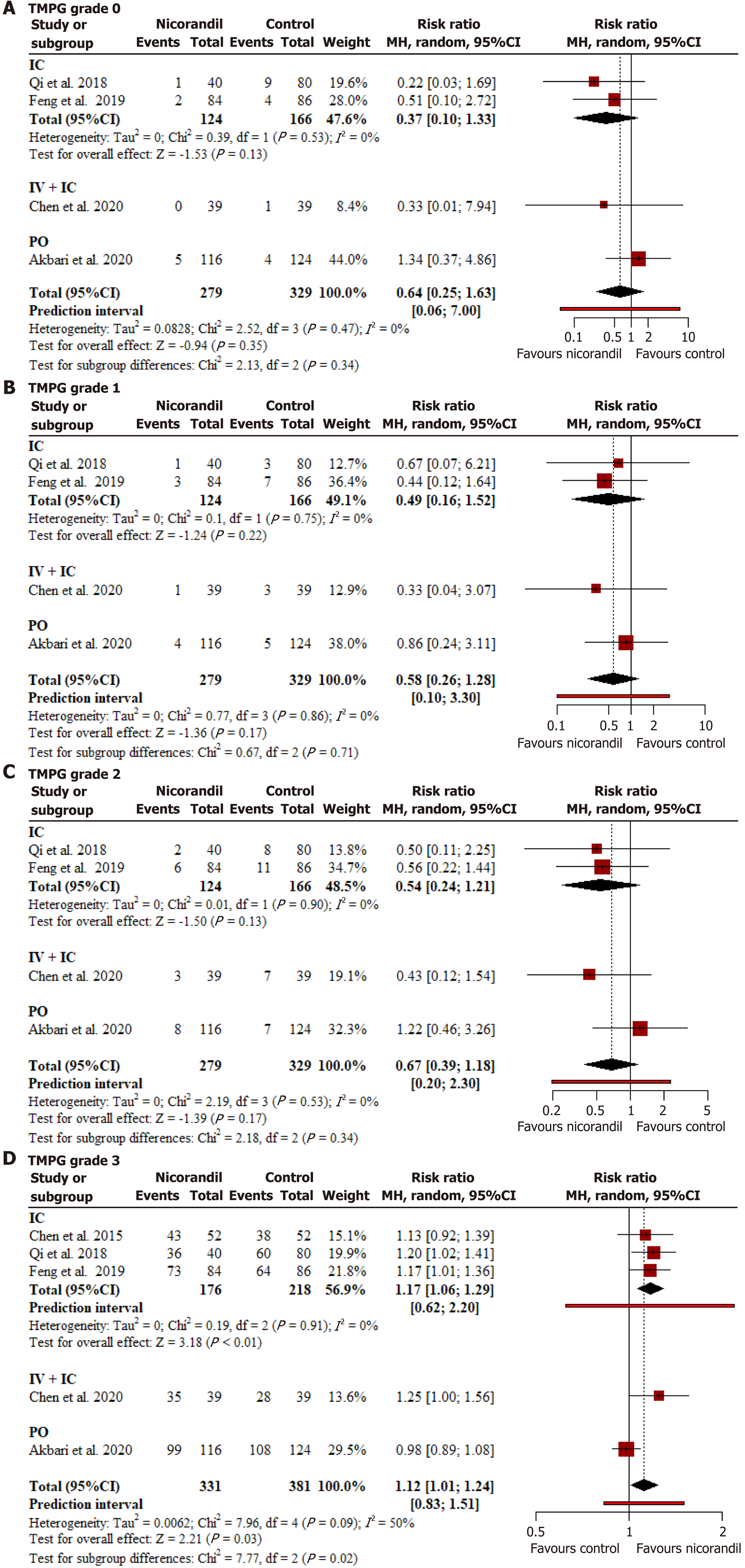
Figure 5 Forest plot for Thrombolysis in Myocardial Infarction Myocardial Perfusion Grades (0, 1, 2, and 3).
A: Thrombolysis in Myocardial Infarction Myocardial Perfusion Grades (TMPG) grades 0; B: TMPG grades 1; C: TMPG grades 2; D: TMPG grades 3. Nicorandil significantly increased the incidence of TMPG 3 following percutaneous coronary intervention, while no such differences were observed for TMPG 0,1 and 2. Subgroup analysis showed a statistically significant difference for TMPG 3 when stratified by route of administration. MH: Mantel-Haenszel; CI: Confidence interval; IV: Intravenous; IC: Intracoronary; PO: Per orem.
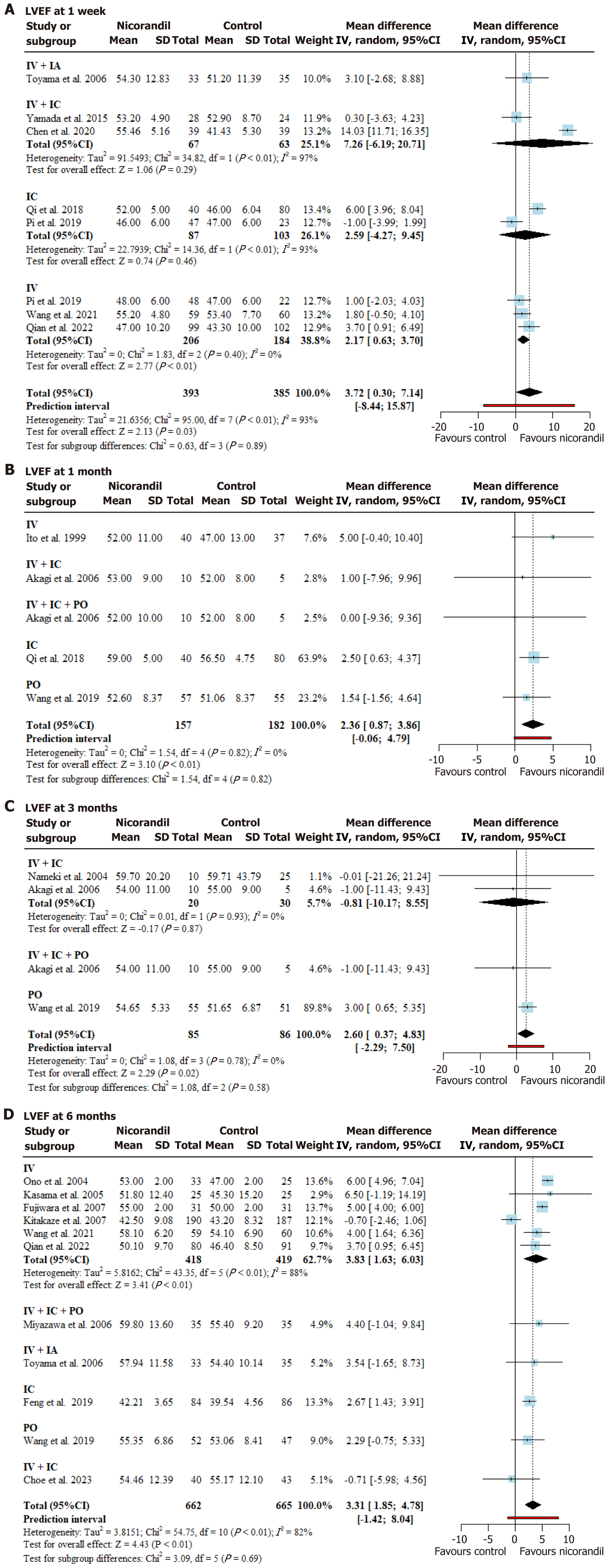
Figure 6 Forest plot for left ventricular ejection fraction following percutaneous coronary intervention in ST-segment elevation myo
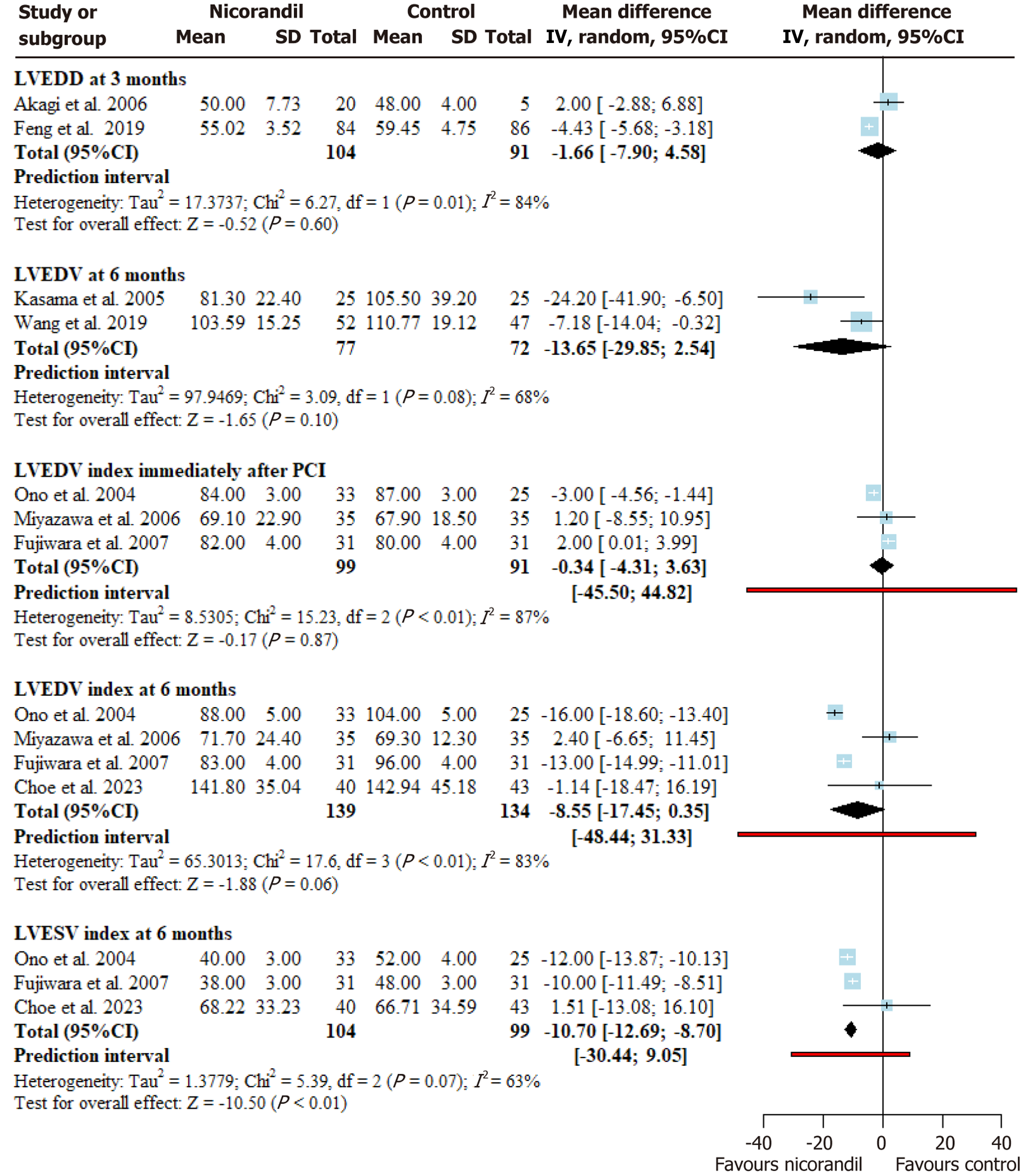
Figure 7 Forest plot for left ventricular functions (left ventricular end-diastolic diameter at 3 months, left ventricular end-diastolic volume at 6 months, left ventricular end-dia
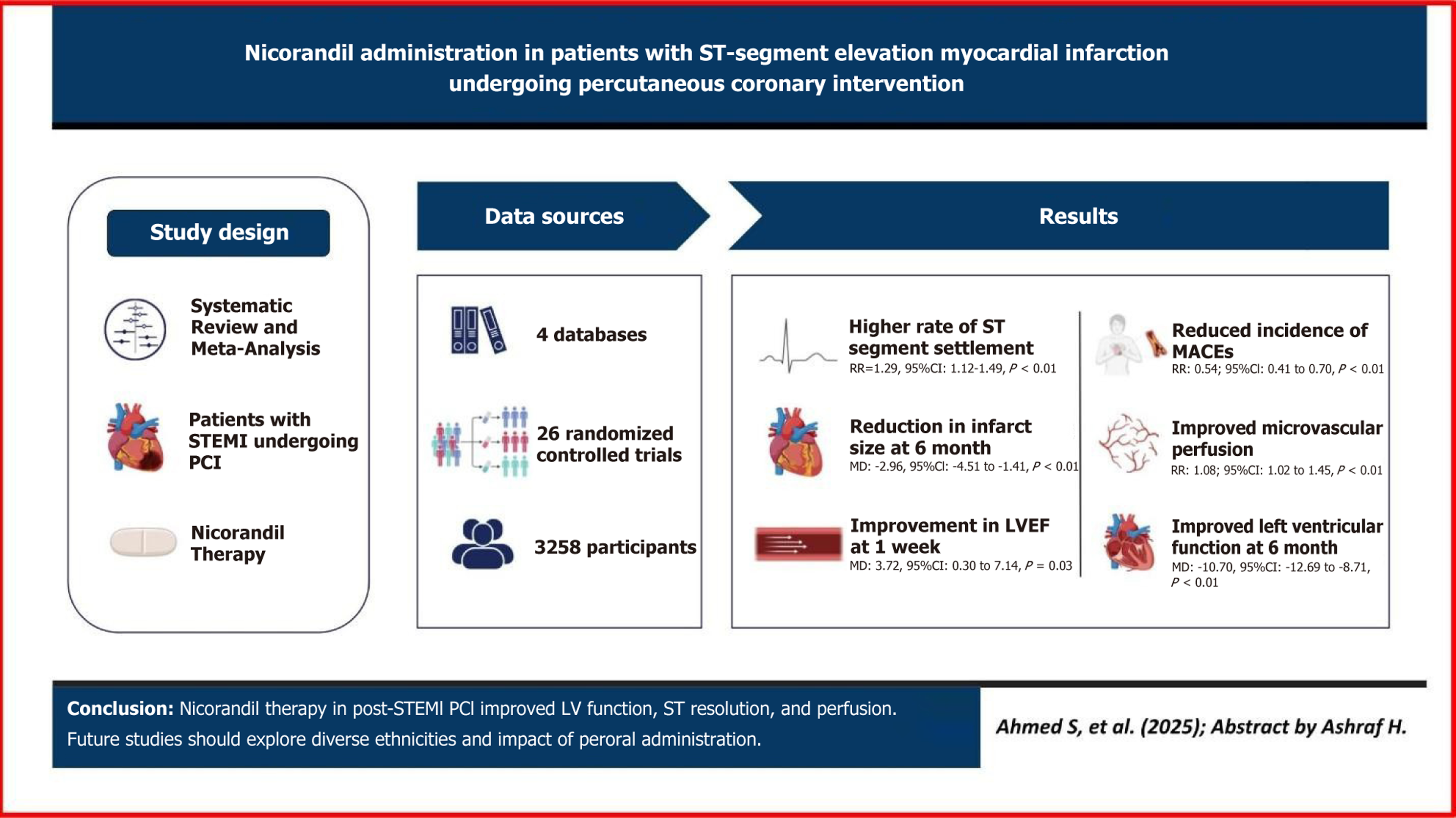
Figure 8 Graphical abstract.
STEMI: ST-elevation myocardial infarction; PCI: Percutaneous coronary intervention; LVEF: Left ventricular ejection fraction; RR: Risk ratio; CI: Confidence interval; MACE: Major adverse cardiovascular event; MD: Mean difference.
- Citation: Ahmed S, Ahmad E, Ashraf H, Ain HU, Ahmad S, Akram U, Basit J, Hassan IN, Ullah I, Ahmed R, Fonarow GC, Cortese B. Nicorandil in ST-segment elevation myocardial infarction patients undergoing percutaneous coronary intervention: A systematic review and meta-analysis. World J Cardiol 2026; 18(3): 116789
- URL: https://www.wjgnet.com/1949-8462/full/v18/i3/116789.htm
- DOI: https://dx.doi.org/10.4330/wjc.v18.i3.116789