Published online Apr 27, 2026. doi: 10.4240/wjgs.v18.i4.116972
Revised: January 8, 2026
Accepted: January 26, 2026
Published online: April 27, 2026
Processing time: 150 Days and 5.7 Hours
Foreign body-associated reactive masses may appear months to decades after abdominal surgery and often present as well-circumscribed lesions on imaging studies. Their radiological features frequently mimic gastrointestinal stromal tumors (GISTs) or other malignant intra-abdominal neoplasms. While most re
A 38-year-old man with a history of open appendectomy 20 years prior was inci
Colonic foreign body-associated reactive masses can mimic GISTs decades after surgery and should be considered in patients with prior abdominal operations.
Core Tip: We report a rare case of a large foreign body-associated reactive mass presenting 20 years after surgery for perforated appendicitis. The lesion mimicked a gastrointestinal stromal tumor on contrast-enhanced computed tomography, leading to diagnostic uncertainty. Surgical resection and histopathological evaluation revealed a chronic foreign body-type inflammatory reaction, in which microscopic foreign materials were identified despite the absence of a grossly identifiable foreign body. This case illustrates a potential diagnostic pitfall and emphasizes the need to consider postoperative inflammatory and foreign body-associated lesions in the differential diagnosis of large intra-abdominal masses.
- Citation: Song SH, Lee SS, Kim DJ. Transverse colon foreign body-associated reactive mass mimicking gastrointestinal stromal tumors: A case report. World J Gastrointest Surg 2026; 18(4): 116972
- URL: https://www.wjgnet.com/1948-9366/full/v18/i4/116972.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i4.116972
Foreign body-associated reactive masses arising in the abdominal cavity are uncommon but clinically significant, as these masses often mimic malignant tumors on cross-sectional imaging[1-4]. Retained surgical materials, such as sponges (gossypiboma or textiloma), account for the majority of reported cases; however, non-textile foreign bodies and chronic postoperative changes, such as organizing hematomas, may generate similar foreign body reactions[5,6]. The true inci
These lesions frequently mimic gastrointestinal stromal tumors (GISTs), soft-tissue sarcomas, ovarian neoplasms, or lymphomas[1-4,7]. Indeed, imaging characteristics, including peripheral enhancement, central necrosis, and well-defined margins, closely resemble those of GISTs, thereby making preoperative diagnosis particularly challenging[1,2,8]. Most reported foreign body-associated reactive masses occur in the small bowel mesentery, pelvis, or retroperitoneum[3,4,6]; involvement of the colon is exceptionally rare[8,9].
We present a unique case of a large transverse colon foreign body-associated reactive mass that developed 20 years after an open appendectomy and strongly mimicked a GIST on contrast-enhanced computed tomography (CT). To our knowledge, reports of colonic foreign body-related reactive masses of this size with such a prolonged latency are exceedingly rare. Thus, this case highlights critical diagnostic pitfalls and underscores the need to consider foreign body reactions in the differential diagnosis of abdominal masses in patients with remote surgical histories.
A 38-year-old man was referred for evaluation of an incidentally detected intra-abdominal mass identified on a chest CT scan performed during routine health screening.
The patient was asymptomatic at the time of detection. He denied abdominal pain, distension, nausea, vomiting, changes in bowel habits, gastrointestinal bleeding, weight loss, fever, or other systemic symptoms. The mass was discovered incidentally, and he remained clinically stable up to the time of surgery.
The patient had no medical comorbidities. His only prior abdominal surgery was an open appendectomy performed 20 years earlier at another hospital for perforated appendicitis complicated by peritonitis.
The patient had no significant personal history of smoking, alcohol use, or occupational exposures. There was no family history of gastrointestinal malignancy or other hereditary diseases.
On physical examination, a firm, palpable mass was noted in the right upper quadrant without tenderness or signs of peritoneal irritation. The abdomen was otherwise soft and nondistended. Vital signs were within normal limits.
Laboratory evaluation revealed no abnormalities. Complete blood count, liver function tests, renal function tests, and routine blood biochemistry were all within normal ranges.
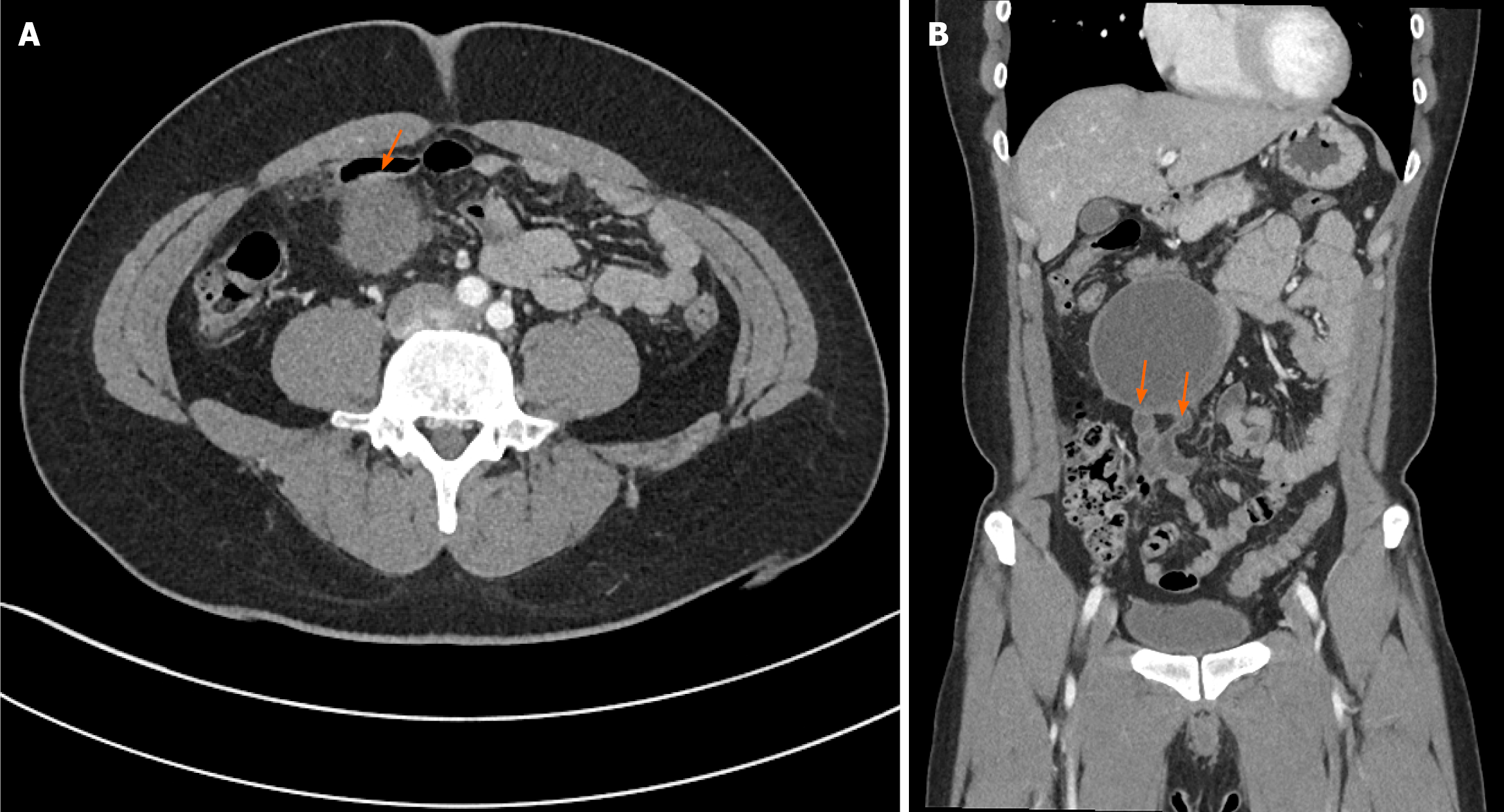
An abdominal contrast-enhanced CT revealed a well-circumscribed mass of approximately 10 cm located in the small bowel mesentery (Figure 1). The lesion demonstrated markedly low attenuation in the central portion with a solid, enhancing peripheral rim, creating a radiological appearance highly suggestive of a GIST. The mass was tightly abutting adjacent ileal loops, raising suspicion of a mural or mesenteric origin. There were no associated liver lesions, ascites, or lymphadenopathy, and no other abnormal intra-abdominal findings were identified.
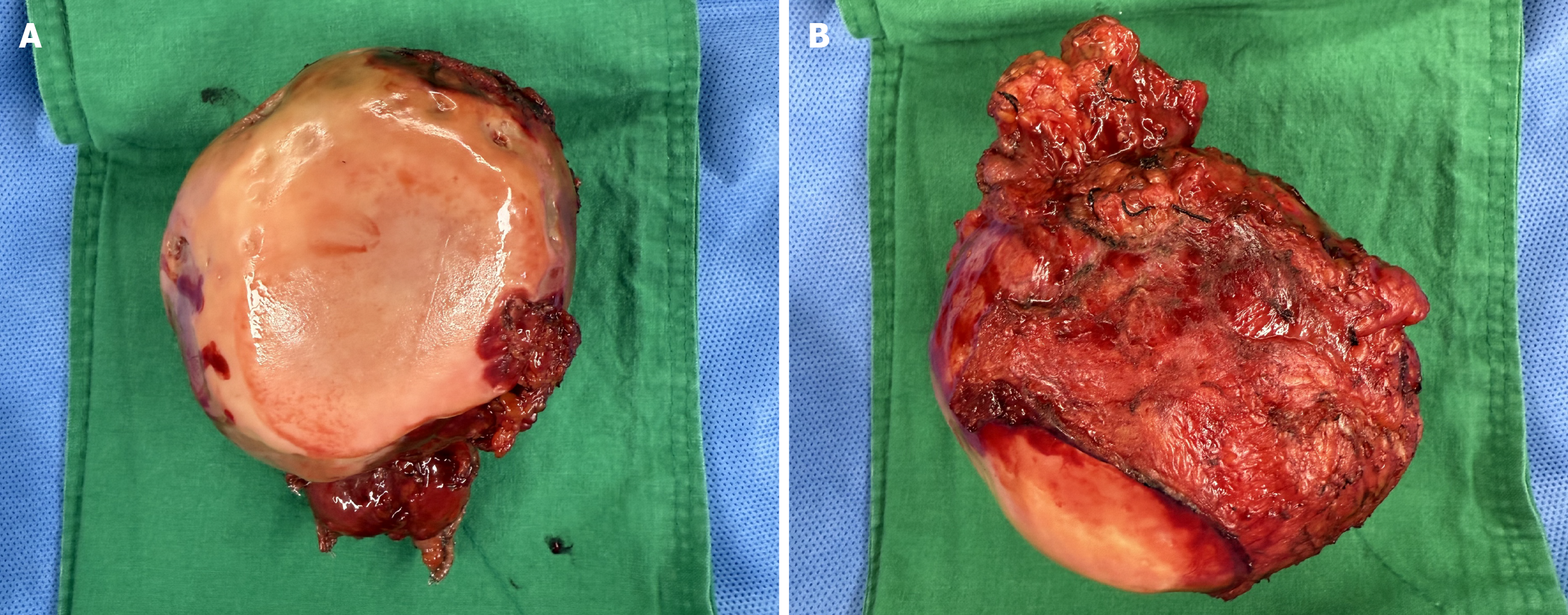
Gross examination of the resected specimen revealed a well-circumscribed subserosal mass arising from the transverse colon, measuring 9.7 cm × 8.0 cm × 7.5 cm (Figure 2A). The external surface of the mass was smooth and glistening with a pale tan appearance, with focal areas of discoloration consistent with old hemorrhage. On the opposite aspect, the mass showed irregular nodularity and dense fibrotic tissue firmly adherent to the adjacent colonic wall and mesentery, correlating with the marked adhesions observed intraoperatively (Figure 2B). No grossly identifiable foreign material was detected on initial inspection.
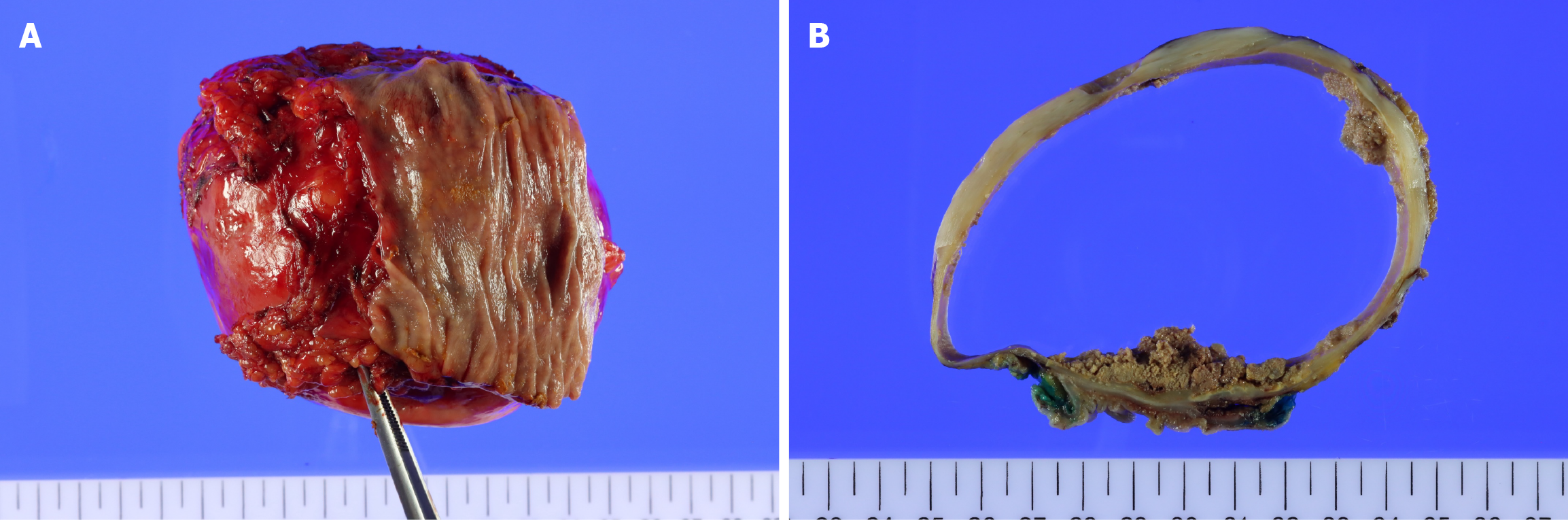
On gross examination of the opened specimen, the colonic mucosa was intact, and a large subserosal mass measuring approximately 10 cm in maximal diameter was identified (Figure 3A). On sectioning, the mass was revealed as a unilocular cyst with a thick fibrous capsule, filled with yellowish, friable, dirty materials adherent to the inner wall (Figure 3B).
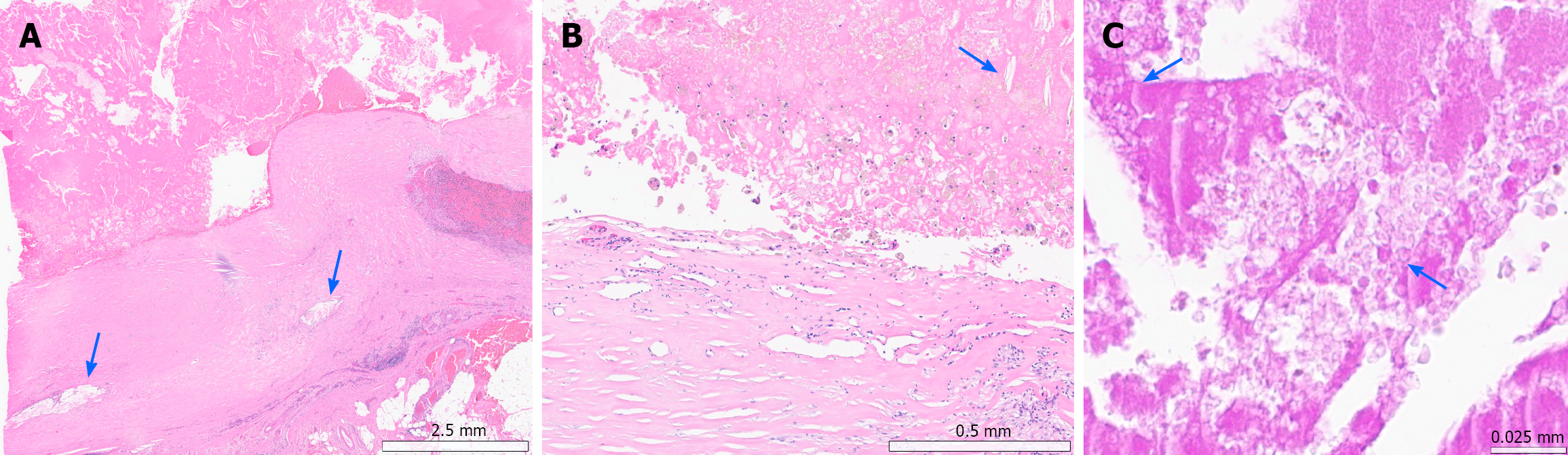
Microscopically, low-power examination demonstrated a thick fibrous cyst wall located within the subserosal layer and attached to the pericolic adipose tissue (Figure 4A). The cyst lacked an epithelial lining, and the wall was composed of densely hyalinized collagen with mild chronic inflammatory cell infiltration, including lymphocytes and histiocytes. Scattered cholesterol crystals were identified within the cyst wall and intracystic contents, accompanied by a foreign-body-type granulomatous reaction. High-power examination revealed dense fibrosis with focal infiltration of macro
A midline laparotomy was first performed by a gastrointestinal surgeon, who encountered extensive intra-abdominal adhesions. Upon exploration, a firm and heterogeneous mass measuring approximately 10 cm was identified in the right upper quadrant. The lesion was densely adherent to the omentum, small bowel mesentery, and retroperitoneum, making dissection difficult. As adhesiolysis progressed, the tumor was found to originate from the transverse colon rather than the small bowel, prompting intraoperative consultation with the colorectal surgery team.
Following identification of the mass as colonic in origin, the colorectal surgeon formally assumed responsibility for the procedure and proceeded with the definitive resection. After confirming the operative field, the ascending colon was mobilized, during which dense adhesions likely related to the prior appendectomy on the patient were encountered and meticulously released. A segmental resection of the transverse colon, including the mass, was then performed. The bowel was divided approximately 5 cm proximal and distal to the lesion using an 80 mm linear stapler, and a functional end-to-end stapled anastomosis was created. Minor intraluminal bleeding along the stapler line was controlled with sutures, and the enterotomy was closed in two layers using a monofilament absorbable suture, with additional seromuscular reinforcement as needed. A drain was placed in the right paracolic gutter for postoperative monitoring.
The patient recovered uneventfully and was discharged on postoperative day 7. He was readmitted the following day with nausea and vomiting; a subsequent abdominal radiography suggested postoperative ileus. Conservative manage
| Time point | Event | Details |
| 20 years prior | Open appendectomy | Performed for perforated appendicitis with peritonitis; no subsequent symptoms for two decades |
| Screening period | Screening chest CT | Incidentally detected a 9-10 cm intra-abdominal mass; patient asymptomatic |
| Diagnostic evaluation | Contrast-enhanced abdominal CT | Well-circumscribed mass with central low attenuation and peripheral enhancement, strongly suggestive of a GIST |
| Day of surgery | Exploratory laparotomy | Dense adhesions present; mass originated from the transverse colon rather than the small bowel |
| Same operation | Segmental transverse colectomy | Mass and involved colon resected; stapled functional end-to-end anastomosis performed |
| Postoperative day 7 | Initial discharge | Early recovery uneventful |
| Postoperative day 8 | Readmission | Nausea and vomiting; imaging suggested postoperative ileus; managed conservatively |
| Postoperative day 13 | Final discharge | Symptoms resolved; no further complications |
| Postoperative pathology | Final diagnosis | Well-circumscribed 9.7 cm × 8.0 cm × 7.5 cm subserosal mass arising from the transverse colon; unilocular cystic lesion with a thick fibrous capsule, containing necrotic debris and old hemorrhage. No epithelial lining or neoplastic cells identified. Histology demonstrated cholesterol crystals and chronic foreign body-type inflammatory reaction, with PAS-positive irregular foreign materials detected microscopically, despite no grossly identifiable foreign material |
Foreign body-associated reactive masses represent an important yet underrecognized postoperative complication, as their clinical and radiological features often mimic intra-abdominal malignancies. Retained surgical textiles, including gossypiboma or textiloma, are the most frequently reported etiology. The largest multi-case series identified 15 cases among more than 45000 abdominal operations, with considerable morbidity and a mortality rate of 13.3%[5]. Compara
A characteristic feature of foreign body-associated reactions is their wide latency spectrum. While some series report symptom onset within months to years, multiple case reports describe delays of several decades, including jejunal gossypiboma 20 years after cesarean section, hepatic textiloma nearly 30 years after cholecystectomy, and suture granuloma more than 50 years after appendectomy[1,5,7,8]. The 20-year interval observed in our patient is consistent with these reports and underscores the importance of considering remote surgical history as a potential cause of late-presenting reactive masses.
Radiologically, foreign body-associated reactive masses are particularly deceptive. CT frequently demonstrates a well-defined mass with peripheral rim enhancement and heterogeneous or low-attenuation central change-features highly suggestive of GISTs or other soft-tissue malignancies[2,3,10]. While GISTs typically appear as predominantly solid enhancing masses with exophytic growth from the bowel wall, foreign body-associated granulomas more commonly demonstrate a cystic or necrotic center with a thick fibrous capsule; however, extensive adhesion to adjacent bowel loops may obscure the true site of origin, as in the present case. Magnetic resonance imaging may further show thick, irregular peripheral enhancement and T2 heterogeneity mimicking sarcoma, whereas positron emission tomography-CT may demonstrate variable fluorodeoxyglucose uptake related to chronic inflammatory activity, raising suspicion of recurrence or metastatic disease[6,7]. Consequently, such lesions have frequently been misinterpreted as GISTs, ovarian teratomas, lymphomas, or sarcoma-like reactions associated with embolic material[1,2,4,8,11]. These recurring diagnostic pitfalls are summarized in Table 2.
| Ref. | Age (year)/sex | Symptoms | Preoperative imaging | Initial suspected diagnosis | Surgical method | Prior surgery and interval |
| Papaoikonomou et al[1] | 42/female | Incidental finding | CT | GIST | Mass resection | Cesarean section, approximately 20 years |
| Han et al[2] | 33/female | Vomiting | CT | Jejunal tumor (GIST) | Laparoscopy-assisted resection | Cesarean section, 7 years |
| Gaylard et al[7] | Adult | Asymptomatic PET-positive lesion | PET-CT | Lymphoma recurrence | Excisional resection | Appendectomy, 56 years |
| Itoh et al[6] | 74/male | Incidental nodules | CT, PET-CT | Peritoneal metastasis | Liver + peritoneal nodule resection | Low anterior resection, 1.5 years |
| Celik et al[3] | Adult | Abdominal/pelvic mass | CT | Soft-tissue tumor | Laparotomy + mass excision | Abdominal surgery (unknown interval) |
| Hajri et al[8] | 65/female | Nausea, vomiting | CT | GIST | Segmental hepatectomy | Cholecystectomy, 29 years |
| Zhang et al[4] | Female | Adnexal mass symptoms | CT | Ovarian teratoma | Mass excision + bowel resection | Abdominal surgery (unknown interval) |
| Oran et al[10] | 28/female | Epigastric mass | CT | Serous cystadenocarcinoma | Laparotomy + mass removal | Cholecystectomy, 3 years |
| Oran et al[10] | 36/female | Abdominal mass | CT | Ovarian/adnexal tumor | Laparotomy + mass removal | Cesarean section, (unknown interval) |
| Eken et al[9] | 62/female | Abdominal discomfort | CT, MRI | Mesenchymal tumor | Mass resection | Prior abdominal surgery (unknown interval) |
| Fumimoto et al[11] | 77/male | Asymptomatic | CT | Lymphoma vs sarcoma | Image-guided biopsy → conservative | NBCA embolization, 12 months |
Postoperative inflammatory pseudocyst (PIP) is an important differential diagnosis, as it is a chronic cystic lesion characterized by a fibrous wall, absence of epithelial lining, and intracystic necrotic debris following abdominal surgery or peritonitis[7,12]. These features were present in our case, and the history of perforated appendicitis supports a postoperative inflammatory background. However, the identification of irregular PAS-positive foreign materials within the necrotic contents, together with cholesterol crystals and a foreign body-type reaction, favors a chronic foreign body–associated process rather than conventional PIP[6,8]. Although no gross foreign material was identified, long-standing foreign substances may fragment over time and persist only as microscopic remnants[1,10]. Accordingly, this lesion is best classified as a foreign body-associated reactive mass within the postoperative inflammatory spectrum.
Ingestion-related foreign body reactions were also considered, as sharp objects such as fish bones or toothpicks may perforate the colon and form tumor-like inflammatory masses[12-15]. These lesions typically occur in older patients with diverticulosis and most commonly involve the sigmoid colon or cecum. In the present case, an ingestion-related mecha
This case highlights that foreign body-associated reactive masses may present decades after abdominal surgery and closely mimic GISTs or other solid tumors. Although ingestion-related foreign body reactions should be considered, large colonic masses lack reliable nonsurgical methods to exclude malignancy. Awareness of these diagnostic limitations is essential, and patients should be counseled regarding the need for surgical resection and the possibility of benign pathology despite suspicious imaging findings.
We report an exceptionally rare case of a transverse colon foreign body-associated reactive mass mimicking a GIST, presenting two decades after appendectomy. Although preoperative imaging strongly suggested a neoplastic process, the lesion proved benign. Surgeons should retain a high index of suspicion for foreign body-related reactive masses in patients with any history of abdominal surgery and be mindful that large masses of this nature ultimately require sur
| 1. | Papaoikonomou MA, Michailidou E, Pogiatzis C, Michailidi ME, Panselinas G. Jejunal Gossypiboma Mimicking a Gastrointestinal Stromal Tumor: A Case of a Rare Iatrogenic Complication and Review of the Literature. Cureus. 2024;16:e75651. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 2. | Han Y, Yang W, Dai W, Ma Q, Yuan T, Yang Y, Lu Y, Zhang B, Zhang M. Case Report: Laparoscopy-assisted resection for intra-abdominal gossypiboma masquerading as a jejunal tumor (with video). Front Oncol. 2023;13:1326032. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (1)] |
| 3. | Celik H, Akin IB, Altay C, Bisgin T, Obuz F. Giant gossypiboma presenting as a pelvic mass. Radiol Case Rep. 2021;16:3308-3310. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 4. | Zhang H, Jiang Y, Wang Q, Liu J. Lower abdominal gossypiboma mimics ovarian teratoma: a case report and review of the literature. World J Surg Oncol. 2017;15:6. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 5. | Tchangai B, Tchaou M, Kassegne I, Simlawo K. Incidence, root cause, and outcomes of unintentionally retained intraabdominal surgical sponges: a retrospective case series from two hospitals in Togo. Patient Saf Surg. 2017;11:25. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 8] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 6. | Itoh N, Takayama G, Kitamura G, Shimauchi Y, Mizutani T, Hikami S, Aratani K, Ujiie K, Yoneda M, Nakamura Y, Takemura M, Koike H, Kakihara N, Ikawa O, Okano S. [A Resected Case of Intraperitoneal Foreign Body Granuloma Mimicking Peritoneal Dissemination]. Gan To Kagaku Ryoho. 2023;50:1501-1503. [PubMed] |
| 7. | Gaylard A, Goai XY, Du Guesclin A, Hodgson R. PET-positive suture granuloma of abdominal wall 56 years post-appendicectomy mimicking recurrence of lymphoma. BMJ Case Rep. 2023;16:e254413. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 8. | Hajri A, Touimi KB, El Berni Y, Erguibi D, Boufettal R, Rifki Jai S, Chehab F. Abdominal textiloma mimicking as gastrointestinal stromal tumor: A case report. Ann Med Surg (Lond). 2021;70:102795. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 9. | Eken H, Soyturk M, Balci G, Firat D, Cimen O, Karakose O, Somuncu E. Gossypiboma Mimicking a Mesenchymal Tumor: A Report of a Rare Case. Am J Case Rep. 2016;17:27-30. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 7] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 10. | Oran E, Yetkin G, Aygün N, Celayir F, Uludağ M. Intraabdominal gossypiboma: Report of two cases. Turk J Surg. 2018;34:77-79. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 11. | Fumimoto M, Kohno S, Oka S, Someya Y, Ishikura R, Nakamura K, Yamashita D, Ueda H, Ando K. Foreign Body Granuloma After Embolization of Internal Iliac Artery Aneurysm Using N-Butyl-2-Cyanoacrylate: A Case Report. Cureus. 2024;16:e60187. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 12. | Fosi S, Altobelli S, Bindi A, Villa M, De Sanctis F, Montuori M, Ricciardi E, Rossi P, Petrella G, Simonetti G. Gradual colonic impaction of a chicken bone associated with inflammatory pseudotumor formation and nonocclusive colon ischemia. Case Rep Radiol. 2014;2014:215465. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 13. | Sibanda T, Pakkiri P, Ndlovu A. Fish bone perforation mimicking colon cancer: A case report. SA J Radiol. 2020;24:1885. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 7] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 14. | Herrera Hernández D, Barragán Jiménez EM, Cano Cabrera P, Flores García PP, Paternina Gonzalez IY, Páramo Hernández DL, Burciaga Castañeda R, Treviño Flores JC. Perforation of the Large Intestine by a Fish Bone Mimicking Cancer: A Rare Case Report. Cureus. 2025;17:e85867. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 15. | Lovece A, Asti E, Sironi A, Bonavina L. Toothpick ingestion complicated by cecal perforation: case report and literature review. World J Emerg Surg. 2014;9:63. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 15] [Article Influence: 1.3] [Reference Citation Analysis (0)] |