Published online Apr 27, 2026. doi: 10.4240/wjgs.v18.i4.116399
Revised: January 7, 2026
Accepted: February 6, 2026
Published online: April 27, 2026
Processing time: 143 Days and 0.8 Hours
Laparoscopic gastrointestinal surgery instruments are complex, and traditional management models rely on nurses’ personal experiences, which can easily lead to intraoperative interruptions. Standardized instrument settings aim to improve team collaboration, efficiency, and surgical safety through a unified process.
To explore the application of an operating room nurse-led standardized laparoscopic instrument setup model to optimize laparoscopic gastrointestinal surgery.
A total of 120 patients undergoing laparoscopic gastrointestinal surgery between June 2022 and June 2025 were divided into observation (n = 60) and control (n = 60) groups using the random number table method. The control group adopted the traditional instrument management model. The observation group imple
Compared with the control group, the observation group showed shorter median operating-room occupancy time (185.6 ± 28.4 minutes vs 205.3 ± 32.1 minutes, P < 0.001), surgical preparation time (18.5 ± 3.2 minutes vs 25.8 ± 4.7 minutes, P < 0.001), and core surgical time (152.7 ± 25.6 minutes vs 168.9 ± 30.3 minutes, P = 0.001). Unplanned interruptions decreased (4.6 ± 1.5 events per case to 1.2 ± 0.8 events per case, P < 0.001), including instrument-related interruptions (2.8 ± 1.1 to 0.5 ± 0.7, P < 0.001) and commu
Nurse-led SIS can significantly operative efficiency, reduce invalid operations and unplanned interruptions, and improve the overall collaborative tacit understanding and work efficiency, supporting further clinical promotion and application.
Core Tip: This study demonstrated that an operating room nurse-led standardized instrument setup (SIS) model significantly enhanced the efficiency of laparoscopic gastrointestinal surgery. Compared to the traditional experience-based approach, the SIS reduced operating room occupancy time, unplanned interruptions, and instrument handover errors, while improving patient outcomes and lowering the cognitive load for surgeons and scrub nurses. This nurse-driven, standardized protocol optimizes workflow and team collaboration and offers a reproducible model for improving surgical safety and efficiency.
- Citation: Tan YZ, Yang M. Standardized instrument setup shortens operating time and reduces interruptions in laparoscopic gastrointestinal surgery: A single-centre randomized control trial. World J Gastrointest Surg 2026; 18(4): 116399
- URL: https://www.wjgnet.com/1948-9366/full/v18/i4/116399.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i4.116399
With the rapid development of minimally invasive surgical techniques, laparoscopic surgery has become a mainstream approach for treating gastrointestinal diseases. It is favored by both patients and surgeons because of its advantages, including minimal trauma, rapid postoperative recovery, and shorter hospital stays[1,2]. However, the successful imple
The traditional management of laparoscopic gastrointestinal surgical instruments relies primarily on the personal work experience, habitual memory, and on-the-spot responsiveness of scrub nurses, representing an experience-based model. In prolonged and high-intensity laparoscopic gastrointestinal surgeries, frequent and rapid instructions from surgeons may overwhelm nurses, leading to unplanned interruptions, including instrument transfer errors, delays, and instrument drops. These issues not only disrupt the surgical rhythm and prolong the operative time but may also increase the in
In recent years, the management philosophy in operating rooms has transitioned from experience-based management to a scientific, systematic, and process-centered approach, with standardization emerging as the core strategy for impro
Based on the above background, this study aimed to explore the application effects of an operating room nurse-led standardized laparoscopic instrument setup model to optimize laparoscopic gastrointestinal surgical processes, improve surgical team collaboration efficiency, and enhance team satisfaction, thereby providing evidence to support refinement and professionalization of operating room nursing management.
Approved by the Ethics Committee of our hospital, a total of 120 patients who underwent laparoscopic gastrointestinal surgery in our hospital from June 2022 to June 2025 were enrolled in the study.
Inclusion criteria: (1) Aged ≥ 18 years; (2) Clear preoperative diagnosis requiring elective laparoscopic radical gastrec
Exclusion criteria: (1) A history of major upper abdominal surgery with expected severe intra-abdominal adhesions; (2) Complicated with severe cardiac, pulmonary, hepatic, or renal dysfunction that could not tolerate surgery; (3) Conversion to open surgery during the operation; and (4) Incomplete clinical data.
Patients were divided into observation and control groups using a random number table method, with 60 patients in each group. There were no statistically significant differences in baseline data (such as age, sex, body mass index, and ASA grade) between the two groups (P > 0.05), indicating comparability (Table 1).
| Group | n | Sex | Age (year) | BMI (kg/m²) | ASA grade | |||
| Male | Female | II | II | IV | ||||
| Observation | 60 | 36 (60.00) | 24 (40.00) | 58.7 ± 10.3 | 23.2 ± 2.8 | 12 (20.00) | 38 (63.33) | 10 (16.67) |
| Control | 60 | 33 (55.00) | 27 (45.00) | 60.1 ± 11.5 | 22.9 ± 3.1 | 15 (25.00) | 35 (58.33) | 10 (16.67) |
| χ2/t | - | 0.309 | 0.702 | 0.577 | 0.536 | |||
| P value | - | 0.578 | 0.484 | 0.565 | 0.765 | |||
Methods for the control group: An traditional, experience-based instrument management model was adopted. Staff training and onboarding were conducted through an apprenticeship-based “follow-the-operation” model. The scrub nurses prepared surgical instruments by type based on their own experiences and habits, without fixed or unified standards for instrument placement. Instrument handover relied on the nurse’s passive response after hearing the surgeon’s instructions. In the case of emergencies, such as instrument malfunctions, handling mainly depended on nurses’ personal on-site responsiveness (Table 2).
| Dimension | Specific plan description | Potential problem analysis |
| Management philosophy | Instrument preparation and management are centered on the scrub nurse’s personal working memory, habits, and preferences | High variability, making it difficult to ensure the stability and consistency of quality |
| Instrument table layout | (1) No zoning planning: Instruments are placed without a fixed functional area division; (2) Disordered placement: Instruments are often piled up by model or type (e.g., all grasping forceps placed together); and (3) Random orientation: Instrument handles face different directions, with mixed front and reverse positions | Increases search time, raises the risk of taking the wrong instrument, and is not ergonomic. This leads to more unnecessary movements and higher fatigue levels for nurses |
| Instrument preparation logic | (1) Classify and place instruments of the same category (e.g., all grasping forceps, all dissecting forceps); and (2) When a specific instrument is needed during surgery, the surgeon gives an instruction, and the nurse then selects, identifies, and passes the instrument from the same category | Response lag and low passing efficiency. Delays are likely to occur during emergency or complex procedures |
| Handover and communication method | (1) Dependence on verbal instructions: Fully relies on the surgeon’s verbal requests (e.g., “Give me that long curved forceps”); (2) No confirmation process: There is usually no verbal confirmation or status check during handover; and (3) Possible communication ambiguity: Instructions may be misunderstood due to environmental noise or inconsistent terminology | High communication costs and high error risks. Surgical noise may mask instructions, leading to handover errors or delays, which affect the surgical rhythm and team morale |
| Staff training and onboarding | (1) Observational learning: New nurses learn by observing the operations of different senior nurses; (2) Diverse habits: Habits and methods of different trainers may conflict with each other; and (3) No standard assessment: Qualification for on-the-job work mainly depends on the subjective judgment of trainers | Long learning curve and unstable training outcomes. New nurses tend to be confused by different habits and find it hard to form a unified and efficient working mode |
| Emergency and special situation handling | When encountering instrument failures, the need for rare instruments, or sudden changes in surgical plans, it fully depends on the scrub nurse's personal experience, memory, and on-site adaptability | Insufficient preparation for emergency situations, making it easy to make mistakes in a hurry and prolong the surgical interruption time |
Methods for the observation group: A SIS protocol formulated under the leadership of operating room nurses was implemented. The specific measures are as follows: (1) Establish an SIS special team: Led by the head nurse, 5 senior scrub nurses proficient in laparoscopic gastrointestinal surgery and 2 surgeons were selected to form the team; (2) Through a literature review, video analysis (recording and replaying previous surgical videos), and brainstorming, each step of laparoscopic gastrointestinal surgery-from pneumoperitoneum establishment, exploration, dissection, transection, anastomosis, and hemostasis to abdominal closure-was systematically decomposed. The specific contents of the in
| Dimension | Specific plan description | Analysis of plan advantages |
| Management philosophy | Process-oriented management centering on the optimized surgical process, solidify best practices into standard operating procedures to ensure stable and reliable instrument management quality for each surgery | Repeatability and stability: Minimize variations caused by human factors to the greatest extent and ensure a baseline for the quality of collaborative work |
| Instrument table layout | Standardized zoned positioning layout: (1) High-frequency operation area: The area closest to the nurse directly in front, where high-frequency instruments (e.g., main operating trocar, atraumatic grasping forceps, dissecting forceps, electric hook/ultrasonic scalpel) are placed; (2) Medium-Frequency operation area: The areas on both sides of the high-frequency area, where medium-frequency instruments (e.g., needle holders, scissors, suction devices, Hem-o-lok forceps) are placed; (3) Low-frequency/standby area: The distal end of the instrument table, where special and standby instruments (e.g., stapler components, special retractors) are placed; and (4) Uniform orientation: All instrument handles face the nurse, and the functional jaws are oriented in the same direction, maintained in a “ready for handover” state | Fixed positioning and ergonomic compliance: Greatly shorten the search path and decision-making time, reduce unnecessary movements such as turning around and bending over, lower the nurse’s workload, and improve handover speed |
| Instrument preparation logic | Process-specific kits: (1) Pneumoperitoneum establishment kit: Pneumoperitoneum needle, first trocar, laparoscope, pneumoperitoneum tube; (2) Dissection and anatomy kit: Ultrasonic scalpel, dissecting forceps, atraumatic grasping forceps, suction device; (3) Anastomosis preparation kit: Stapler, cutting stapler, needle holder, suture thread; and (4) Predictive preparation: Nurses, based on the surgical progress, place the PSK for the next stage within easy reach before the current stage is about to end | Concurrent engineering and proactive preparation: Transform “passively waiting for instructions” into “proactively anticipating needs” to achieve the state of “instruments waiting for the surgeon”. Fundamentally reduce waiting-related interruptions during surgery and ensure extremely smooth processes |
| Handover and communication method | Standardized passing protocol: (1) Silent tacit handover: For high-frequency instruments (e.g., ultrasonic scalpel, dissecting forceps), form a conditioned reflex through training where the nurse hands over the instrument as soon as the surgeon reaches out; (2) Verbal confirmation handover (ticket-style): When handing over special or valuable instruments, clearly report the name and status (e.g., linear cutting stapler, green staple cartridge installed), and the surgeon must give a brief confirmation (e.g., Okay) upon receipt; and (3) Closed-loop communication: Ensure instructions are clearly received and correctly executed | Noise reduction, efficiency improvement, and safety enhancement: Reduce noise interference and the risk of mishearing caused by verbal instructions. Closed-loop communication significantly improves the accuracy and safety of information transmission. Silent tacit understanding greatly enhances team cohesion and surgical rhythm |
| Staff training and onboarding | Systematic training and certification: (1) Theoretical training: Learn the concept of the SIS plan, layout diagrams, PSK lists, and SPP processes; (2) Simulation drills: Conduct high-intensity, repetitive drills in a simulated operating room until muscle memory is formed; and (3) Assessment and certification: Formulate objective scoring criteria (e.g., preparation time, handover accuracy), and only those who achieve a 100% passing rate in the assessment are eligible for on-the-job qualification | Shortened growth cycle: Enable new nurses to get rid of dependence on specific trainers, quickly reach a qualified level through standardized training, and ensure the homogenization and high level of the overall collaborative quality of the team |
| Emergency and special situation handling | Standardized emergency procedures: (1) Instrument malfunction: Immediately activate standby instruments, move the malfunctioning instrument to a specific area, and handle it uniformly after the surgery; (2) Additional instrument request: Circulating nurses quickly locate and hand over instruments according to the pre-set “Instrument List” to avoid blind searching on the sterile table; and (3) Surgical procedure change: Initiate the pre-determined “expanded instrument kit” procedure | Note: The original table lacks content for “analysis of plan advantages” in this dimension. It is recommended to supplement relevant advantages based on actual scenarios, such as “clear response guidelines: Ensure rapid, orderly, and error-free handling of emergencies, minimize surgical delays caused by unexpected situations, and enhance the team’s ability to respond to risks” |
(1) Operating room occupancy time: Total time from the patient’s entry into the operating room to their departure; (2) Surgical preparation time: Time from the patient’s entry into the operating room to the surgical skin incision; (3) Core surgical time: Time from skin incision to completion of skin suture; (4) Intraoperative unplanned interruptions: Total number of events causing surgical process suspension for more than 10 seconds, their causes, and interruption duration; and (5) Instrument handover efficiency: Number of instrument handovers from scrub nurses to surgeons in a single operation, effective handover rate, and average handover time.
The recorded indicators included intraoperative blood loss, incidence of intraoperative adverse events, length of post
Complications included postoperative fever, surgical site infection, pulmonary infection, anastomotic leakage, intestinal obstruction, and deep vein thrombosis.
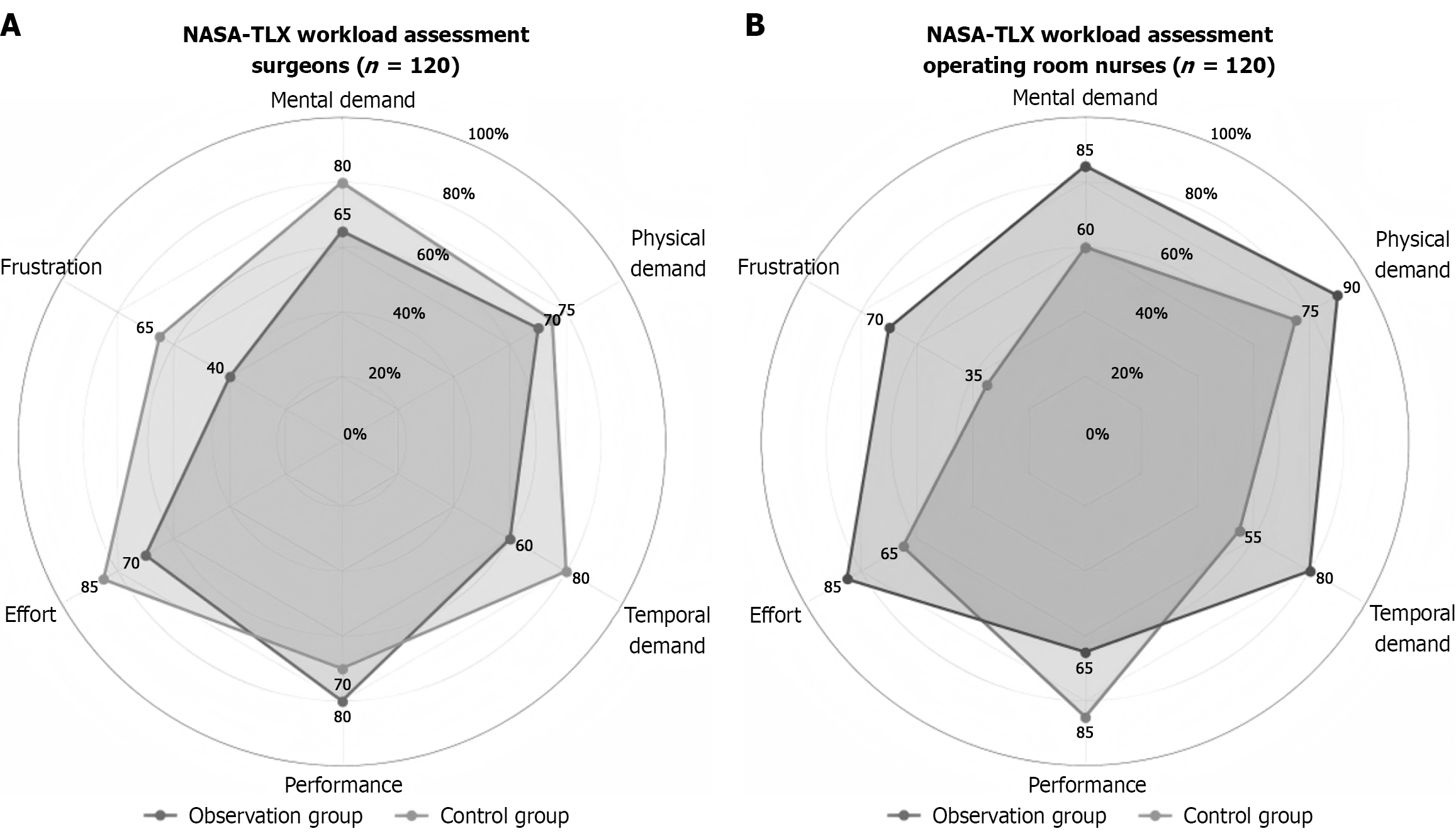
The NASA Task Load Index (NASA-TLX) was used to assess the subjective cognitive load of surgeons and scrub nurses during surgery. It comprises six dimensions: Mental, physical, temporal, performance, effort, and frustration. The scores range from 0 to 100, with higher scores indicating a heavier cognitive load.
SPSS software (version 26.0) was used for the data analysis. Measurement data were expressed as mean ± SD, and count data were expressed as n (%). Inter-group comparisons were conducted using the independent samples t-test and χ2 test, respectively. Statistical significance was set at P value < 0.05.
The surgical efficiency in the observation group was significantly higher than that in the control group. Specifically, the operating room occupancy time (185.6 ± 28.4 minutes vs 205.3 ± 32.1 minutes, P < 0.001), surgical preparation time (18.5 ± 3.2 minutes vs 25.8 ± 4.7 minutes, P < 0.001), and core surgical time (152.7 ± 25.6 minutes vs 168.9 ± 30.3 minutes, P = 0.001) were all significantly shorter in the observation group.
Furthermore, the observation group exhibited fewer intraoperative disruptions than the control group. The total number of unplanned interruptions was markedly lower in the observation group (1.2 ± 0.8 times vs 4.6 ± 1.5 times, P < 0.001), with reductions seen in both instrument-related (0.5 ± 0.7 times vs 2.8 ± 1.1 times, P < 0.001) and communication-related interruptions (0.3 ± 0.5 times vs 1.1 ± 0.8 times, P < 0.001). Consequently, the average interruption duration was also shorter in the observation group (15.3 ± 5.2 seconds vs 28.7 ± 10.4 seconds, P < 0.001).
With regard to instrument handover, the observation group demonstrated higher efficiency. The total number of handovers was lower (85.6 ± 12.4 times vs 112.3 ± 18.9 times, P < 0.001), while the effective handover rate was higher (99.1 ± 0.9% vs 95.2 ± 2.3%, P < 0.001). The average time required per handover was also significantly shorter (1.5 ± 0.3 seconds vs 2.8 ± 0.6 seconds, P < 0.001) (Tables 4 and 5).
| Group | Operating room occupancy time (minutes) | Surgical preparation time (minutes) | Core surgical time (min) | Total number of unplanned interruptions (times) | Instrument-related interruptions (times) |
| Observation group (n = 60) | 185.6 ± 28.4 | 18.5 ± 3.2 | 152.7 ± 25.6 | 1.2 ± 0.8 | 0.5 ± 0.7 |
| Control group (n = 60) | 205.3 ± 32.1 | 25.8 ± 4.7 | 168.9 ± 30.3 | 4.6 ± 1.5 | 2.8 ± 1.1 |
| t value | 3.628 | 10.117 | 3.278 | 7.112 | 6.854 |
| P value | < 0.001 | < 0.001 | 0.001 | < 0.001 | < 0.001 |
| Group | Communication-related interruptions (times) | Average interruption duration (seconds) | Total number of instrument handovers (times) | Effective handover rate (%) | Average handover time (seconds) |
| Observation group (n = 60) | 0.3 ± 0.5 | 15.3 ± 5.2 | 85.6 ± 12.4 | 99.1 ± 0.9 | 1.5 ± 0.3 |
| Control group (n = 60) | 1.1 ± 0.8 | 28.7 ± 10.4 | 112.3 ± 18.9 | 95.2 ± 2.3 | 2.8 ± 0.6 |
| t value | 5.123 | 6.225 | 9.458 | 12.341 | 15.327 |
| P value | < 0.001 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
The clinical outcomes of the patients in the observation group were more favorable. Intraoperative blood loss was lower (105.6 ± 20.8 mL vs 115.3 ± 22.1 mL, P = 0.015), and the incidence of intraoperative adverse events was reduced (5.0% vs 13.3%, P < 0.05).
Postoperatively, patients in the observation group recovered rapidly. Their hospital stay was shorter (8.2 ± 1.2 days vs 9.3 ± 1.4 days, P < 0.001), time to first ambulation occurred earlier (24.6 ± 3.1 hours vs 28.3 ± 3.6 hours, P < 0.001), and time to first anal exhaust was also accelerated (60.7 ± 7.2 hours vs 66.2 ± 8.5 hours, P < 0.001) (Table 6).
| Group | Intraoperative blood loss (mL) | Postoperative hospital stay (days) | Time to first ambulation (hours) | Time to first anal exhaust (hours) |
| Observation group (n = 60) | 105.6 ± 20.8 | 8.2 ± 1.2 | 24.6 ± 3.1 | 60.7 ± 7.2 |
| Control group (n = 60) | 115.3 ± 22.1 | 9.3 ± 1.4 | 28.3 ± 3.6 | 66.2 ± 8.5 |
| t value | 2.475 | 4.619 | 6.032 | 3.824 |
| P value | 0.015 | < 0.001 | < 0.001 | < 0.001 |
The overall postoperative complication rate in the observation group was significantly lower than that in the control group [10.00% (6/60) vs 25.00% (15/60), χ² = 4.675, P = 0.031]. This difference was primarily reflected in lower rates of surgical site infections (3.33% vs 5.00%) and pulmonary infections (1.67% vs 5.00%) in the observation group (Table 7).
| Group | Postoperative fever | Surgical site infection | Anastomotic leak | Pulmonary infection | Intestinal obstruction | Deep vein thrombosis | Total complications |
| Observation group (n = 60) | 2 (3.33) | 2 (3.33) | 1 (1.67) | 1 (1.67) | 0 (0.00) | 0 (0.00) | 6 (10.00) |
| Control group (n = 60) | 4 (6.67) | 3 (5.00) | 2 (3.33) | 3 (5.00) | 2 (3.33) | 1 (1.67) | 15 (25.00) |
| χ² | - | - | - | - | - | - | 4.675 |
| P value | - | - | - | - | - | - | 0.031 |
Assessment using the NASA-TLX scale revealed that the SIS model reduced the subjective cognitive load of both surgeons and scrub nurses. In the observation group, the scores for mental demand, temporal demand, effort, and frustration, as well as the total score, were significantly lower than those in the control group (all P < 0.05). Conversely, the performance score, which reflected perceived task accomplishment, was significantly higher in the observation group (P < 0.05) (Figure 1).
Currently, the concept of modern operating room management is undergoing a transformation from experience-based management to “process-centered” scientific and systematic management. Against this backdrop, standardization has become a core strategy for improving surgical quality and ensuring patient safety[9-11]. As departments within hospitals feature high technology intensity, complex processes, and extremely strict requirements for multidisciplinary colla
In operating rooms, the standardized setup of instruments serves as a key entry point for process optimization. Estab
The study results showed that, compared with the control group adopting traditional experience-based management, the observation group implementing standardized management exhibited significant advantages in multiple surgical efficiency indicators. In the SIS protocol, from establishing a special task force and decomposing surgical steps, to designing a standardized layout, establishing PSK and SPP, and further formulating systematic training and emergency procedures, all aspects reflect the initiative and professionalism of nursing practice. These findings are consistent with those reported by Pan and Yi[17], who explored the impact of refined management on the surgical efficiency of laparoscopic radical resection for colon cancer. Di Saverio et al[18] conducted in-depth reflections on the process of emergency laparoscopic surgery during the coronavirus disease 2019 pandemic and proposed that standardized algorithmic mana
The operating room occupancy time, surgical preparation time, and core surgical time in the observation group were all significantly shortened (P < 0.05), indicating that the SIS protocol effectively reduced non-value-added time consump
The SIS protocol emphasizes “process-specific instrument kits” and “predictive preparation”, which changes the traditional serial model of “surgeon’s instruction-nurse’s response”. It fully embodies the application of the “concurrent engineering” concept in surgical processes, realizes the parallel advancement of instrument preparation and surgical progress, and makes “instruments waiting for the surgeon” possible, thereby substantially reducing waiting-related interruptions. Through the combination of a standardized layout (zoned positioning), PSK and SPP, workflow inter
Meanwhile, the study results showed that in the observation group, intraoperative blood loss, incidence of intraoperative adverse events, postoperative hospital stay, time to first ambulation, time to first anal exhaust/defecation, and overall complication rate were lower than those in the control group (P < 0.05). The improvement in these results is closely related to the inherent benefits of optimizing the surgical process. First, reducing unplanned interruptions and instrument handover delays means less interference with the core steps of surgery, enabling surgeons to perform delicate operations in a more focused and continuous manner, thereby reducing tissue damage and bleeding. Secondly, efficient and accurate instrument collaboration reduces the risk of technical errors caused by incorrect instruments or delays, thereby further reducing the incidence of intraoperative adverse events. Furthermore, a smooth surgical process helps to shorten the duration of anesthesia and surgical stress, which may alleviate the patient's physiological trauma stress response. This is inherently consistent with the findings of Zeng et al[23] regarding perioperative comfort care, which reduced patients' stress responses.
The improvement in postoperative recovery indicators is directly related to the reduction of surgical trauma and stress and conforms to the concept of enhanced recovery after surgery (ERAS). Chen et al[24] showed that ERAS nursing can promote the recovery of gastrointestinal function and improve sleep quality in patients after laparoscopic appendectomy. The results of this study indicate that the standardization of instrument management, as an important optimization in the operating room nursing process, has a positive cascading effect on promoting the postoperative recovery of patients. This can be regarded as a specific manifestation of the process optimization and efficiency improvement principles advocated by ERAS in the context of instrument management. Cao et al[25] also found in their study of elderly patients undergoing laparoscopic total gastrectomy for gastric cancer that implementation of the ERAS protocol can improve patient prog
In addition, the results showed that for surgeons and instrument nurses in the observation group, the scores of the mental demand, temporal demand, effort, and frustration dimensions of the NASA-TLX scale, as well as the total score, were all lower than those in the control group, whereas the score of the performance dimension was higher than that of the control group (P < 0.05). This indicates that standardized management significantly reduces the mental stress and workload of surgical team members. The standardized table layout and PSK model shifted instrument nurses from a passive state of relying on memory and on-site response to an active state of proactive preparation in accordance with predetermined processes. This reduces the dependence on high-intensity working memory and the uncertainty of decision making, thereby lowering the mental load and perceived frustration[26].
Geubbels et al[27] pointed out that simulation training on basic laparoscopic surgical skills could improve the attitudes of operating room nursing students. However, the SIS protocol in this study directly enhanced the work experience and sense of efficacy of in-service nurses by constructing a standardized practical work model. For surgeons, stable and predictable instrument support reduces the time pressure caused by waiting and communication corrections, allowing them to focus more on surgical operations and enhancing their subjective perception of surgical performance. Reduction in team cognitive load and improvement in performance perception are of far-reaching significance for maintaining the morale of the surgical team, reducing occupational burnout, and promoting long-term collaborative rapport[28,29]. Ramzan et al[30] showed that quantitative operating room nursing combined with psychological interventions could improve patients’ stress responses and mental states. The value of this study lies in reducing the factors that cause stress among team members by optimizing the work process itself, further confirming the clinical application advantages of the SIS protocol.
This study has some limitations. First, this was a single-center study with a relatively small sample size (n = 120), which may have limited the statistical power and potentially increased the risk of type II errors. Second, the study population was confined to patients undergoing elective laparoscopic gastrointestinal surgeries (e.g., radical gastrectomy and colorectal cancer surgery), and the conclusions may not be fully generalizable to emergency surgeries, other types of laparoscopic procedures (e.g., hepatobiliary and urological procedures), or open surgeries. Third, the implementation of the SIS protocol was conducted within a specific team and hospital environment, and its effectiveness and feasibility in other institutions with varying resource levels, staff training systems, or cultural contexts warrants further validation through multicenter studies. Future studies should aim to expand the sample size, include diverse surgical types and settings, and employ longer follow-up periods to comprehensively evaluate the long-term impact and broader applicability of the standardized management model.
In conclusion, a nurse-led, SIS in the operating room can significantly optimize the laparoscopic gastrointestinal surgery process, reduce ineffective operations and unplanned interruptions, and improve the overall collaborative rapport and work efficiency of the surgical team. These findings support broader clinical implementation of this approach.
| 1. | Aydal P, Uslu Y, Ulus B. The Effect of Preoperative Nursing Visit on Anxiety and Pain Level of Patients After Surgery. J Perianesth Nurs. 2023;38:96-101. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 17] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 2. | Odogwu S, Morris S, Addison S, Abbott S. Laparoscopic cholecystectomy performed by a surgical care practitioner: a review of outcomes. Ann R Coll Surg Engl. 2024;106:724-728. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 11] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 3. | Wang P, Ma S, Yu L. Study on the application effect of personalized nursing in the operating room of laparoscopic cholecystectomy for gallstone. Panminerva Med. 2022;64:302-303. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 4. | Zhang J, Deng L, Wang X, Song F, Hou H, Qiu Y. Effect of Forced-Air Warming Blanket on Perioperative Hypothermia in Elderly Patients Undergoing Laparoscopic Radical Resection of Colorectal Cancer. Ther Hypothermia Temp Manag. 2022;12:68-73. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 14] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 5. | Ng SSM, Chan SKC, Ng MHL, Lee JFY, Lai PBS. Fast-track versus traditional perioperative care for laparoscopic colorectal surgery: a prospective randomised trial (abridged secondary publication). Hong Kong Med J. 2020;26 Suppl 8:18-21. [PubMed] |
| 6. | Woldehana NA, Jung A, Parker BC, Coker AM, Haut ER, Adrales GL. Clinical Outcomes of Laparoscopic vs Robotic-Assisted Cholecystectomy in Acute Care Surgery. JAMA Surg. 2025;160:755-762. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 20] [Cited by in RCA: 19] [Article Influence: 19.0] [Reference Citation Analysis (0)] |
| 7. | Klein J, Lemma M, Prabhakaran K, Rafieezadeh A, Kirsch JM, Rodriguez G, Blazar I, Jose A, Zangbar B. Robotic versus Laparoscopic Emergency and Acute Care Surgery: Redefining Novelty (RLEARN): feasibility and benefit of robotic cholecystectomy for acute cholecystitis at a level 1 trauma center. Trauma Surg Acute Care Open. 2024;9:e001522. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 8. | Tica VI, Tica AA, De Wilde RL. The Future in Standards of Care for Gynecologic Laparoscopic Surgery to Improve Training and Education. J Clin Med. 2022;11:2192. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 9] [Reference Citation Analysis (0)] |
| 9. | Nassar A, Hobeika C, Lamer C, Beaussier M, Sarran A, Yamazaki S, Sanou Y, Bonnet S, Gayet B, Fuks D. Relevance of blood loss as key indicator of the quality of surgical care in laparoscopic liver resection for colorectal liver metastases. Surgery. 2020;168:411-418. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 8] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 10. | Kouhestani Z, Aboutalebi MS, Izadan M, Aarabi A, Mosleh S. Compliance with care standards and professional knowledge of operating theatre personnel before, during and after laparoscopic bariatric surgery: A study in public hospitals in Iran. J Perioper Pract. 2024;17504589241300274. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 11. | Qian M, Ye Y, Zhou J. Effect of thermal insulation on preventing hypothermia during laparoscopic radical resection for colorectal cancer. Am J Transl Res. 2024;16:2158-2165. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 12. | Hasegawa M, Ogino T, Sekido Y, Takeda M, Hata T, Hamabe A, Miyoshi N, Uemura M, Doki Y, Eguchi H. Surgical approach for a refractory enterocutaneous fistula by combining laparoscopic surgery and a planned open conversion: a case report. Surg Case Rep. 2024;10:186. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 13. | Gurusamy KS, Koti R, Davidson BR. Routine abdominal drainage versus no abdominal drainage for uncomplicated laparoscopic cholecystectomy. Cochrane Database Syst Rev. 2013;CD006004. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 38] [Cited by in RCA: 44] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 14. | Ochoa-Ortiz LI, Cervantes-Pérez E, Ramírez-Ochoa S, Gonzalez-Ojeda A, Fuentes-Orozco C, Aguirre-Olmedo I, De la Cerda-Trujillo LF, Rodríguez-Navarro FM, Navarro-Muñiz E, Cervantes-Guevara G. Risk Factors and Prevalence Associated With Conversion of Laparoscopic Cholecystectomy to Open Cholecystectomy: A Tertiary Care Hospital Experience in Western Mexico. Cureus. 2023;15:e45720. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 15. | Ghimire R, Pudasaini P, Acharya BP, Limbu Y, Regmee S. Previous Abdominal Scars among Patients Undergoing Laparoscopic Cholecystectomy in a Tertiary Care Centre. JNMA J Nepal Med Assoc. 2023;61:647-650. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 16. | Yan RC, Shen SQ, Chen ZB, Lin FS, Riley J. The role of prophylactic antibiotics in laparoscopic cholecystectomy in preventing postoperative infection: a meta-analysis. J Laparoendosc Adv Surg Tech A. 2011;21:301-306. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 45] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 17. | Pan Y, Yi M. Effect of refined management in operating room nursing on surgical efficiency and nursing satisfaction during laparoscopic radical resection of colon cancer. Am J Transl Res. 2024;16:506-514. [PubMed] [DOI] [Full Text] |
| 18. | Di Saverio S, Khan M, Pata F, Ietto G, De Simone B, Zani E, Carcano G. Laparoscopy at all costs? Not now during COVID-19 outbreak and not for acute care surgery and emergency colorectal surgery: A practical algorithm from a hub tertiary teaching hospital in Northern Lombardy, Italy. J Trauma Acute Care Surg. 2020;88:715-718. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 78] [Cited by in RCA: 82] [Article Influence: 13.7] [Reference Citation Analysis (0)] |
| 19. | Egan P, Pierce A, Flynn A, Teeling SP, Ward M, McNamara M. Releasing Operating Room Nursing Time to Care through the Reduction of Surgical Case Preparation Time: A Lean Six Sigma Pilot Study. Int J Environ Res Public Health. 2021;18:12098. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 15] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 20. | Yan T, Li HX, Sun YL, Liu Y, Chen R, Peng RH, Zheng ZX, Qu SN, Wang F, Tang W, Zhang L, Wei SJ, Wang BN, Sun L, Zheng H. Preventing pulmonary complications after laparoscopic colorectal surgery: a lung-protective protocol vs. standard care: A randomised controlled trial. Eur J Anaesthesiol. 2025;42:826-839. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 21. | Ray U, Dhar R. A Retrospective Analysis of Short-Term Outcomes of Robotic and Laparoscopic Cholecystectomy: An Indian Tertiary Care Comparative Experience. Cureus. 2024;16:e69295. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 22. | Yan W, Xu X, Cui H, Li W. Application of the concept of rapid rehabilitation in the operating room nursing of laparoscopic gastrointestinal surgery. Panminerva Med. 2021;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 23. | Zeng Q, Yang J, Jiang L, Deng Y, Luo X, Yang J. The Impact of Perioperative Comfort Nursing Combined With Targeted Operating Room Nursing on Postoperative Stress Response and Nursing Satisfaction in Colorectal Cancer Patients. Ann Ital Chir. 2025;96:1089-1102. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 24. | Chen SS, Gao YM, Yao XF, Zhang QQ, Yang KL, Xia Q, Ding J. Effect of rapid rehabilitation surgical nursing on patients' gastrointestinal function recovery and sleep quality after laparoscopic appendectomy. World J Gastrointest Surg. 2025;17:102681. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 25. | Cao S, Zheng T, Wang H, Niu Z, Chen D, Zhang J, Lv L, Zhou Y. Enhanced Recovery after Surgery in Elderly Gastric Cancer Patients Undergoing Laparoscopic Total Gastrectomy. J Surg Res. 2021;257:579-586. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 40] [Article Influence: 6.7] [Reference Citation Analysis (1)] |
| 26. | Haldeniya K, R KS, Raghavendra A, Singh PK. Laparoscopic subtotal cholecystectomy in difficult gallbladder: Our experience in a tertiary care center. Ann Hepatobiliary Pancreat Surg. 2024;28:214-219. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 27. | Geubbels N, Evren I, Acherman YIZ, Bruin SC, van de Laar AWJM, Hoen MB, de Brauw LM. Randomized clinical trial of an enhanced recovery after surgery programme versus conventional care in laparoscopic Roux-en-Y gastric bypass surgery. BJS Open. 2019;3:274-281. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 30] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 28. | Qiu Y, Ouyang X, Luo M, Feng L, Zheng C, Li G. Application of a surgical nursing cooperation program in laparoscopic pancreaticoduodenectomy. Gland Surg. 2020;9:1530-1534. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 29. | Krishna A, Rai SK, Jain M, Prakash O, Misra MC, Kumar S, Bansal VK. Outcomes of various bailout strategies for managing different categories of difficult laparoscopic cholecystectomy - An experience of over two decades from a single surgical unit at a tertiary care teaching hospital. J Minim Access Surg. 2025;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 30. | Ramzan M, Javaid MU, Hussain A. Reconsidering the Scalpel: A Comparative Reflection on Endoscopic Sleeve Gastroplasty and Laparoscopic Sleeve Gastrectomy as Diverging Pathways in Modern Bariatric Care. Asian J Endosc Surg. 2025;18:e70083. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |