Published online Mar 27, 2026. doi: 10.4240/wjgs.v18.i3.115888
Revised: November 27, 2025
Accepted: January 21, 2026
Published online: March 27, 2026
Processing time: 150 Days and 20.8 Hours
Biliary stricture is a common complication after choledochojejunostomy (CJ). In
To evaluate the effectiveness of placing a T-tube at the CJ site to prevent postope
A single-center retrospective study was conducted, involving 68 patients with bile duct diameters < 8 mm who underwent biliary reconstruction surgery in the De
There were no significant differences in age, sex, body mass index, American Society of Anesthesiologists class, preoperative laboratory indices, preoperative hypertension, diabetes history or pathology findings between the two groups. The incidence of postoperative biliary stricture and biliary leakage in the T-tube group was lower than that in the non-T-tube group; in addition, the operation time, intraoperative blood loss and hospital stay in the T-tube group were lower than those in the non-T-tube group. There was no significant difference in postoperative complications such as abdominal infection, pulmonary infection or delayed gastric emptying between the two groups.
The modified T-tube stent external drainage technique effectively reduces the incidence of postoperative biliary stricture, has certain advantages in reducing postoperative biliary leakage, and is worthy of clinical promotion and application.
Core Tip: In this study, a modified choledochojejunostomy (CJ) technique was proposed. A T-tube was placed at the CJ site to support the reconstructed biliary tract, and external drainage was performed during CJ, which effectively reduced the incidence of postoperative biliary stricture. Compared with traditional internal drainage of the CJ, the incidence of biliary complications such as post-operative biliary leakage was significantly lower, length of hospital stay was reduced and patient postoperative quality of life was greatly improved. This technique has high clinical value and is worthy of clinical promotion and application.
- Citation: Liu N, Zhang M, Guo Y, Bian J, Meng XK, Li J. Application of T-tube stent external drainage for the prevention of postoperative biliary stricture during choledochojejunostomy. World J Gastrointest Surg 2026; 18(3): 115888
- URL: https://www.wjgnet.com/1948-9366/full/v18/i3/115888.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i3.115888
Choledochojejunostomy (CJ) is widely performed in hepatobiliary surgery and can be used to treat various diseases, such as intrahepatic and extrahepatic bile duct stones; bile duct stricture, atresia and other bile duct stricture deformities; reconstruction after choledochal cyst resection; reconstruction of the extrahepatic bile duct after tumor resection; repair of iatrogenic bile duct injury; pancreaticoduodenectomy; and bile duct reconstruction in liver transplantation, with its clinical effect well recognized in most studies[1]. However, various postoperative complications, such as anastomotic leakage, biliary bleeding, wound infection, cholangitis and biliary stricture[2-5], severely affect the long-term prognosis of patients; in particular, the incidence of biliary stricture can reach 2%-13%[6-8]. Studies have confirmed that a small dia
Inclusion criteria: (1) Patients aged ≥ 18 years old; (2) Magnetic resonance cholangiopancreatography (MRCP) revealed a bile duct diameter of < 8 mm; (3) The patient underwent CJ in our hospital; (4) Preoperative imaging examination showed no obvious biliary dilatation; (5) Patients with complete clinical data and follow-up time ≥ 2 years; (6) None of the pa
Exclusion criteria: (1) Patients with severe cardiopulmonary dysfunction or systemic organ failure who could not tolerate surgery; (2) Coagulopathy or bleeding tendency; (3) Patients with percutaneous transhepatic cholangial drainage or per
Patients included in this study were hospitalized in the Department of Hepatobiliary Surgery, the Affiliated Hospital of Inner Mongolia Medical University, from January 2021 to October 2023. According to the inclusion criteria, 68 patients were ultimately included. Of these patients, 32 underwent T-tube stent external drainage at the CJ site (T-tube group), and 36 underwent conventional internal drainage of the CJ (non-T-tube group). There were no significant differences in sex, age, body mass index, history of hypertension, history of diabetes, bile duct diameter, proportion of benign and malignant tumors, or preoperative total bilirubin between the two groups (P > 0.05; Table 1). All patients provided written informed consent. The study was approved by the hospital ethics committee.
| T-tube group (n = 32) | Non-T-tube group (n = 36) | t/χ² | P value | |
| Age (years) | 65.07 ± 9.89 | 63.90 ± 7.64 | 0.517 | > 0.05 |
| Sex | ||||
| Male | 13 (40.63) | 16 (44.44) | -0.101 | > 0.05 |
| Female | 19 (59.38) | 20 (55.56) | ||
| Body mass index (kg/m2) | 22.63 ± 2.29 | 22.52 ± 2.70 | 0.173 | > 0.05 |
| Hypertension | 12 (37.50) | 14 (38.89) | 0.014 | > 0.05 |
| Diabetes | 8 (25.00) | 6 (16.67) | 0.720 | > 0.05 |
| Tumor | ||||
| Benign | 13 (40.63) | 17 (47.22) | 0.299 | > 0.05 |
| Malignancy | 19 (59.37) | 19 (52.78) | ||
| Bilirubin (μmol/L) | 63.27 ± 81.37 | 38.72 ± 41.65 | 1.839 | > 0.05 |
| Biliary diameter(mm) | 5.63 ± 2.05 | 5.91 ± 1.21 | -0.675 | > 0.05 |
Traditional CJ: Anastomotic operation: (1) The proximal 1-2 cm of the hilar bile duct was released; (2) The lateral wall of the jejunum was opened; (3) The jejunal mucosa was aligned with the bile duct mucosa; and (4) The anterior wall of the anastomosis was sutured intermittently with 4-0/5-0 absorbable sutures through the jejunum and bile duct.
Seromuscular embedding (using the seromuscular layer of the jejunum to cover the anastomosis) was performed 2-3 cm from the jejunal side of the anastomosis; only the seromuscular layer of the jejunum was sutured with 4-0 absorbable sutures (without penetrating the mucosa), and the seromuscular layer was pulled upward, with the fibrous tissue around the bile duct or liver capsule fixed to cover the CJ.
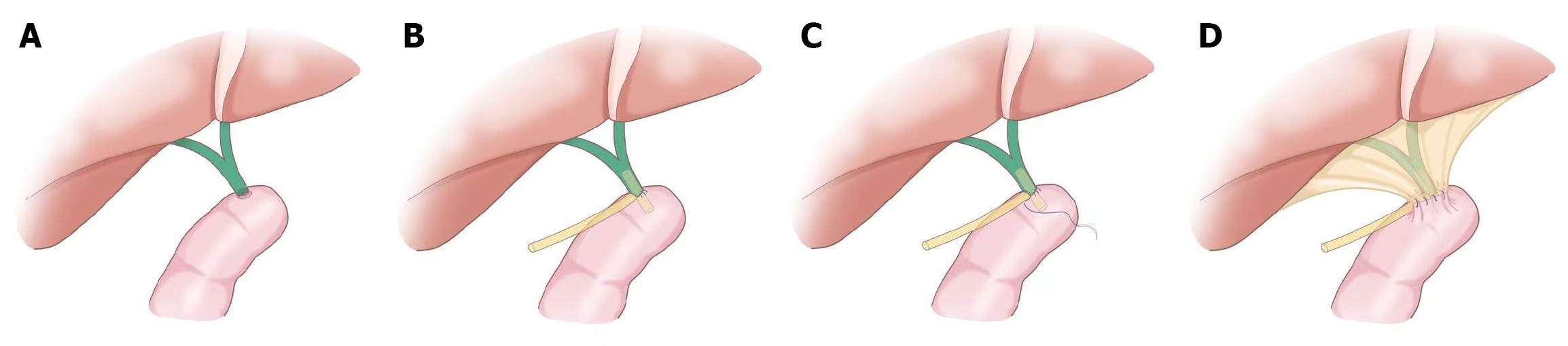
Modified T-tube stent external drainage CJ: (1) Posterior wall anastomosis: 1-2 cm of the proximal hilar bile duct was dissected, meticulous hemostasis was achieved, and an opening on the lateral wall of the jejunum was created. The mucosal layer of the posterior jejunal wall was aligned with that of the posterior bile duct wall. Using 4-0/5-0 absorbable sutures, the needle was inserted from the mucosal surface to the serosal surface of the jejunal wall, and the serosal surface was penetrated to the mucosal surface of the bile duct. After placing 3 interrupted sutures through the posterior walls of the jejunum and bile duct, the knots were tied extra-luminally sequentially to complete the anastomosis of the posterior and partial lateral walls (Figure 1A); (2) T-tube placement and anterior wall anastomosis: Based on the internal diameter of the bile duct, a 14 silicone T-tube was inserted. One end of the transverse arm was positioned in the common hepatic duct and the other end in the jejunum through the lateral jejunal opening (the vertical arm was exteriorized through the abdominal wall postoperatively). Using 4-0/5-0 absorbable sutures, the needle was inserted from the serosal surface to the mucosal surface of the jejunal wall, and the mucosal surface was penetrated to the serosal surface of the bile duct. Suture spacing of approximately 2-3 mm and a margin of 1.5-2 mm (slightly narrower on the bile duct side) was maintained. The knots were tied extra-luminally and the anterior wall anastomosis was completed with interrupted sutures (Figure 1B); (3) Purse-string suture around the T-tube: Using 4-0/5-0 absorbable sutures, the needle was inserted 2-3 mm from the edge of the T-tube and a continuous circumferential full-thickness suture was positioned around the T-tube, encompassing the anterior jejunal wall and anterior bile duct wall. The suture was gently retracted to allow the anterior walls of the jejunum and bile duct to uniformly encircle the T-tube, the suture was then gradually tightened to constrict the jejunal and bile duct tissues around the T-tube before tying the knot (Figure 1C); and (4) Seromuscular burial (covering the anastomosis with the jejunal seromuscular layer): 2-3 cm from the anastomosis on the jejunal side, the seromuscular layer was grasped with atraumatic forceps. Using 4-0 absorbable sutures, only the jejunal seromuscular layer was sutured (without penetrating the mucosa) with a suture spacing of approximately 3-4 mm and a margin of 5-8 mm. The seromuscular layer was retracted upward and secured to the fibrous tissue surrounding the bile duct or the hepatic capsule to cover the CJ anastomosis (Figure 1D).
The T-tube was clamped two weeks after the operation. If the patient had no abnormal conditions, such as abdominal distension, abdominal pain, fever or jaundice, the T-tube was clamped for a long period of time. The patient was reexamined in the outpatient clinic three months after the operation. T-tube angiography was performed for those who could tolerate it, and magnetic resonance MRCP was performed for those who could not. The T-tube was removed after confirming that the biliary tract was unobstructed.
In this study, patients were divided into the T-tube group and the non–T-tube group according to the type of CJ. The two groups of patients were closely observed and followed up after surgery, and the incidence of postoperative biliary complications (including biliary stricture, biliary leakage, and biliary bleeding, etc.) was compared between the two groups.
New onset jaundice continued to increase and was related to the obstruction, as confirmed by postoperative imaging, computed tomography (CT) or MRCP, which showed bile duct dilation consistent with biliary stricture[10,11].
After the operation, high fever, abdominal pain and peritoneal irritation symptoms occurred. B-ultrasound or CT examination revealed effusion around the CJ site or in the abdominal cavity, suggesting the possibility of biliary leakage. Drainage tube fluid was detected around the anastomosis site, and this bile-like fluid was used to diagnose biliary leakage[12,13].
In the T-tube group, biliary bleeding was diagnosed based on blood in fluid drained by the T-tube. In the non-T-tube group, biliary tract bleeding was diagnosed based on postoperative hematochezia, increased heart rate, decreased blood pressure, and decreased hemoglobin, hematocrit and red blood cell count, as determined by laboratory examination, after ruling out gastrointestinal bleeding[14].
The diagnosis of abdominal infection was based on clinical manifestations such as chills, high fever and abdominal distension; laboratory findings showing that the white blood cell count was markedly increased; and the presence of purulent fluid from the abdominal drainage tube[15].
The diagnosis of pulmonary infection was based on clinical manifestations such as fever, cough and expectoration after the operation and laboratory findings showing a markedly increased white blood cell count and increased neutrophil count. Pneumonia was diagnosed by chest CT[16].
The two groups of patients were followed up for 2-4 years after the operation and were reexamined in the outpatient clinic two weeks after the operation and every three months thereafter. The follow-up endpoint was October 2025, with a focus on the occurrence of postoperative biliary stricture and biliary leakage in both groups of patients.
In this study, we used Statistical Package for the Social Sciences 25.0 statistical software. All count data are expressed as frequencies and percentages, and the χ² test or Fisher’s exact probability test was used. For comparisons, measurement data are expressed as the mean ± SD, and an independent sample t-test or analysis of variance was used for comparisons between the groups. P < 0.05 was considered to indicate statistical significance.
There was no significant difference in the occurrence of complications, such as biliary bleeding, abdominal infection or pulmonary infection, between the two groups (P > 0.05; Table 2). No biliary stricture or biliary leakage occurred in the T-tube group; eight cases of biliary stricture and nine cases of biliary leakage occurred in the non-T-tube group (P < 0.05; Table 2). The incidence of postoperative biliary stricture and biliary leakage in the T-tube group was significantly lower than that in the non-T-tube group. Length of hospital stay in the T-tube group was shorter than that in the non-T-tube group.
| T-tube group (n = 32) | Non-T-tube group (n = 36) | F/χ² | Odds ratio (95%CI) | P value | |
| Biliary stricture | 0 (0.00) | 8 (22.22) | - | 19.386 (1.071-350.979) | < 0.05 |
| Biliary leakage | 0 (0.00) | 9 (25.00) | - | 22.455 (1.249-403.547) | < 0.05 |
| Biliary bleeding | 1 (3.12) | 5 (13.89) | 1.285 | > 0.05 | |
| Abdominal infection | 2 (6.25) | 3 (8.33) | 0.019 | > 0.05 | |
| Pulmonary infection | 3 (9.38) | 8 (22.22) | 1.223 | > 0.05 | |
| Days (days) | 21.97 ± 5.12 | 25.47 ± 5.93 | -2.714 | < 0.05 |
The T-tube was placed for three months and T-tube angiography or magnetic resonance imaging was performed before removing the T-tube to confirm that the biliary tract was unobstructed. During the indwelling period of the T-tube, no catheter-related complications, such as catheter breakage, deformation or removal occurred.
There were no statistically significant differences between the two groups in American Society of Anesthesiologists class, operation time, or intraoperative blood loss (P > 0.05; Table 3).
| T-tube group (n = 32) | Non-T-tube group (n = 36) | t/χ² | P value | |
| American Society of Anesthesiologists class | ||||
| II | 22 (68.8) | 25 (69.4) | 0.004 | > 0.05 |
| III | 10 (31.2) | 11(30.6) | ||
| Time (minutes) | 189.94 ± 48.67 | 197.44 ± 20.72 | -0.749 | > 0.05 |
| Blood loss (mL) | 157.81 ± 58.35 | 165.00 ± 51.49 | -0.496 | > 0.05 |
There was no significant difference in serum bilirubin levels between the two groups on the first, fifth and tenth day after the operation (P > 0.05; Table 4).
| T-tube group (n = 32) | Non-T-tube group (n = 36) | t/χ² | P value | |
| 1st day after operation | 56.65 ± 166.78 | 36.47 ± 35.54 | 1.677 | > 0.05 |
| 5th day after operation | 44.90 ± 52.94 | 25.95 ± 22.82 | 2.179 | > 0.05 |
| 10th day after operation | 27.38 ± 30.47 | 19.61 ± 14.22 | 1.550 | > 0.05 |
In clinical hepatobiliary surgery, CJ, a commonly used surgical method, is associated with a high incidence of postopera
In CJ, when the bile duct is dilated due to biliary obstruction, the anastomotic operation is relatively easy to perform, and the risk of postoperative biliary stricture and biliary leakage is also reduced. It has been confirmed that the small diameter and thin wall of the common bile duct are factors inducing postoperative biliary stricture as the bile duct is thin, the surgical anastomosis is difficult, the postoperative biliary tract and anastomotic site are prone to scar stricture, and the increased pressure at the anastomotic site leads to biliary leakage. However, even in non-dilated bile ducts, there is a risk of biliary stricture and biliary leakage after CJ[17,18].
In this study, during CJ, a T-tube was placed at the CJ site, with one short arm inserted into the biliary tract, the other short arm inserted into the jejunum, and the long arm exiting the body through the anastomosis and the skin. The results showed that the incidence of postoperative biliary stricture and biliary leakage in the T-tube group was lower than that in the non-T-tube group (P < 0.05). Notably, among the T-tube group, two patients with post-cholecystectomy biliary stricture and one patient with anastomotic stricture after biliary reconstruction did not experience recurrent stricture following the modified CJ. The reason for this is that the T-tube placed at the CJ site can, on the one hand, support the reconstructed biliary tract and anastomosis, effectively preventing postoperative biliary stricture and anastomotic stricture, and maintain the patency of the biliary tract; on the other hand, postoperatively, a large volume of bile se
In addition, this study also showed that there was no significant difference in intraoperative blood loss or operation time between the T-tube group and the non-T-tube group. This finding indicates that although the T-tube group underwent more surgical steps than the non-T-tube group, due to its simple operation and technology, the T-tube does not increase the operation time or intraoperative blood loss. In contrast, its advantage in reducing complications such as biliary leakage accelerates the postoperative recovery of patients, thus shortening the hospital stay and improving the bed turnover rate. However, the T-tube must be indwelled for at least three months before removal, requiring patients to carry it long-term, which is associated with certain drawbacks. For instance, improper skin care at the T-tube exit site may allow bacterial invasion of subcutaneous tissues or bile leakage into the subcutaneous space, leading to local inflammation characterized by redness, swelling, and pain around the incision. More seriously, retrograde bacterial migration along the T-tube lumen into the biliary tract can result in cholangitis. Additionally, there are risks of T-tube displacement, dislodgement, or fracture, which increase the complexity of nursing care to a certain extent. To address these issues, we propose the following interventions: (1) Regular dressing changes around the T-tube site; (2) Daily replacement of the drainage bag when the tube is unclamped to prevent infection; (3) Adoption of a “double fixation method” for securing the T-tube (i.e., suturing both sides of the T-tube exit site to the skin and fixing the drainage bag to clothing with a safety pin) to avoid traction; and (4) Patient education to avoid strenuous activities and to turn over gently, thereby reducing the risk of T-tube dislodgement. Notably, no such cases occurred in the T-tube group during follow-up in this study.
This study has some limitations. As a single-center retrospective study with a relatively small sample size, it included patients with high heterogeneity (e.g., variations in etiology), which imposes restrictions on the external validity of the results. Additionally, long-term quality of life assessment was lacking. Future research should expand the sample size, conduct stratified analyses for different subgroups (e.g., malignant vs benign lesions), and carry out prospective, multi-center studies with extended follow-up periods. Furthermore, our team plans to perform animal experiments in order to obtain an adequate number of subjects, to ensure statistical test requirements are met. These experiments will exclude clinical confounding factors, reduce experimental errors caused by individual differences, and enhance the reliability and reproducibility of the findings, thereby further validating the efficacy and safety of this modified surgical procedure.
Modified T-tube stenting with an external drainage technique is easy to perform. It can effectively reduce the incidence of postoperative biliary stricture and has clear advantages in reducing postoperative bile leakage, biliary bleeding and hospital stay. This technique enables patients to achieve better postoperative recovery, improves their quality of life and improves the prognosis of this condition. It is an effective modification of CJ in non-dilated bile ducts during biliary surgery and is worthy of clinical promotion and application.
We sincerely acknowledge the entire medical and nursing staff of the Department of Hepatobiliary, Pancreatic and Splenic Surgery and the Department of Anesthesiology at the Affiliated Hospital of Inner Mongolia Medical University for their valuable support in providing surgical procedures and postoperative care for the patients in our research group.
| 1. | Chen D, Zhu A, Zhang Z. Total laparoscopic Roux-en-Y cholangiojejunostomy for the treatment of biliary disease. JSLS. 2013;17:178-187. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 18] [Article Influence: 1.4] [Reference Citation Analysis (1)] |
| 2. | Kadaba RS, Bowers KA, Khorsandi S, Hutchins RR, Abraham AT, Sarker SJ, Bhattacharya S, Kocher HM. Complications of biliary-enteric anastomoses. Ann R Coll Surg Engl. 2017;99:210-215. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 64] [Article Influence: 7.1] [Reference Citation Analysis (1)] |
| 3. | Zafar SN, Khan MR, Raza R, Khan MN, Kasi M, Rafiq A, Jamy OH. Early complications after biliary enteric anastomosis for benign diseases: a retrospective analysis. BMC Surg. 2011;11:19. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 41] [Article Influence: 2.7] [Reference Citation Analysis (1)] |
| 4. | Malgras B, Duron S, Gaujoux S, Dokmak S, Aussilhou B, Rebours V, Palazzo M, Belghiti J, Sauvanet A. Early biliary complications following pancreaticoduodenectomy: prevalence and risk factors. HPB (Oxford). 2016;18:367-374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 70] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 5. | Birgin E, Téoule P, Galata C, Rahbari NN, Reissfelder C. Cholangitis following biliary-enteric anastomosis: A systematic review and meta-analysis. Pancreatology. 2020;20:736-745. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 34] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 6. | Dimou FM, Adhikari D, Mehta HB, Olino K, Riall TS, Brown KM. Incidence of hepaticojejunostomy stricture after hepaticojejunostomy. Surgery. 2016;160:691-698. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 87] [Cited by in RCA: 81] [Article Influence: 8.1] [Reference Citation Analysis (0)] |
| 7. | Zielsdorf SM, Klein JJ, Fleetwood VA, Hertl M, Chan EY. Hepaticojejunostomy for Benign Disease: Long-Term Stricture Rate and Management. Am Surg. 2019;85:1350-1353. [PubMed] |
| 8. | House MG, Cameron JL, Schulick RD, Campbell KA, Sauter PK, Coleman J, Lillemoe KD, Yeo CJ. Incidence and outcome of biliary strictures after pancreaticoduodenectomy. Ann Surg. 2006;243:571-6; discussion 576. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 179] [Cited by in RCA: 146] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 9. | Duconseil P, Turrini O, Ewald J, Berdah SV, Moutardier V, Delpero JR. Biliary complications after pancreaticoduodenectomy: skinny bile ducts are surgeons' enemies. World J Surg. 2014;38:2946-2951. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 66] [Article Influence: 5.5] [Reference Citation Analysis (1)] |
| 10. | Elmunzer BJ, Maranki JL, Gómez V, Tavakkoli A, Sauer BG, Limketkai BN, Brennan EA, Attridge EM, Brigham TJ, Wang AY. ACG Clinical Guideline: Diagnosis and Management of Biliary Strictures. Am J Gastroenterol. 2023;118:405-426. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 94] [Article Influence: 31.3] [Reference Citation Analysis (0)] |
| 11. | Palmucci S, Roccasalva F, Piccoli M, Fuccio Sanzà G, Foti PV, Ragozzino A, Milone P, Ettorre GC. Contrast-Enhanced Magnetic Resonance Cholangiography: Practical Tips and Clinical Indications for Biliary Disease Management. Gastroenterol Res Pract. 2017;2017:2403012. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 12. | Schertz PJ, Mao CA, Derrick KD, Galar F, Ortiz CB, Walker JA, Lopera JE. Biliary Leaks: Multidisciplinary Approach to Diagnosis and Treatment. Radiographics. 2024;44:e230155. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 12] [Reference Citation Analysis (1)] |
| 13. | Nikpour AM, Knebel RJ, Cheng D. Diagnosis and Management of Postoperative Biliary Leaks. Semin Intervent Radiol. 2016;33:307-312. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 33] [Article Influence: 3.3] [Reference Citation Analysis (1)] |
| 14. | Wang C, Wang M, Zhang K, Zhang JX, Liu L, Fan ZN. [Imaging features and therapeutic strategies for lethal iatrogenic hemobilia]. Linchuang Gandanbing Zazhi. 2024;40:2070-2074. [DOI] [Full Text] |
| 15. | Bonomo RA, Humphries R, Abrahamian FM, Bessesen M, Chow AW, Dellinger EP, Edwards MS, Goldstein E, Hayden MK, Kaye KS, Potoski BA, Rodríguez-Baño J, Sawyer R, Skalweit M, Snydman DR, Tamma PD, Donnelly K, Loveless J. 2024 Clinical Practice Guideline Update by the Infectious Diseases Society of America on Complicated Intra-abdominal Infections: Utility of Intra-abdominal Fluid Cultures in Adults, Children, and Pregnant People. Clin Infect Dis. 2024;79:S123-S126. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 16. | Conde M, Lawrence V. Postoperative pulmonary infections. BMJ Clin Evid. 2008;2008:2201. [PubMed] |
| 17. | Kobayashi S, Nakahara K, Umezawa S, Ida K, Tsuchihashi A, Koizumi S, Sato J, Tateishi K, Otsubo T. Benign hepaticojejunostomy strictures after pancreatoduodenectomy. BMC Gastroenterol. 2024;24:293. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 18. | Li K, Ding Y, Liu N, Qi R, Wang Y, Liu J, Shi B. Relationship between postoperative biliary stricture and clinical characteristics of patients with benign and malignant biliary diseases. Wideochir Inne Tech Maloinwazyjne. 2023;18:117-127. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |