Published online Mar 27, 2026. doi: 10.4240/wjgs.v18.i3.115767
Revised: November 26, 2025
Accepted: January 12, 2026
Published online: March 27, 2026
Processing time: 154 Days and 5.4 Hours
Intestinal stoma closure can lead to severe gut microbiome dysbiosis, adversely affecting postoperative recovery and quality of life. An integrative approach combining traditional Chinese medicine (TCM) and Western medicine within a multi-disciplinary team (MDT) framework presents a promising strategy to enhance gut health. However, its efficacy has not been systematically evaluated.
To investigate the efficacy of an MDT approach combining TCM and Western medicine in promoting gut microbiome recovery after intestinal stoma closure.
A retrospective study design was employed, analyzing data from patients who underwent intestinal stoma closure between January 2020 and December 2023. Patients were divided into two groups: The control group, which received stan
The study included 251 patients, with 122 in the control group and 129 in the MDT group. Baseline characteristics were similar between the groups. The MDT group showed significantly higher alpha diversity (Shannon index) postoperatively compared with the control group. The MDT group had higher operational taxonomic unit counts for Bacteroidetes and Proteobacteria than the control group, whereas the control group had higher operational taxonomic unit counts for Firmicutes than the MDT group. The MDT group demonstrated lower prevalence rates of abdominal pain, bloating, and diarrhea postoperatively and shorter hospital stays than the control group. Patients in the MDT group reported improvements in chronic condition management, psychological well-being, immunological indicators, and nutritional status. The MDT group exhibited enhanced immune function, improved intestinal permeability, and better quality of life than the control group.
This retrospective study suggests that the MDT approach, combining TCM and Western medicine, has the potential to promote gut microbiome recovery and improve overall outcomes after intestinal stoma closure.
Core Tip: This retrospective study demonstrates that a multi-disciplinary team approach integrating Traditional Chinese medicine with standard Western medicine significantly enhances gut microbiome recovery after intestinal stoma closure. Compared to standard care, the multi-disciplinary team approach improved microbial diversity, reduced gastrointestinal symptoms, shortened hospital stays, and enhanced immunological, nutritional, and psychological outcomes. These findings highlight the potential of integrative medicine to offer a more holistic and effective strategy for improving postoperative recovery in this patient population, providing a novel direction for clinical practice.
- Citation: Zhou Q, Xu JD. Traditional Chinese and Western multidisciplinary team approach for gut microbiome recovery postintestinal stoma closure. World J Gastrointest Surg 2026; 18(3): 115767
- URL: https://www.wjgnet.com/1948-9366/full/v18/i3/115767.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i3.115767
Intestinal stoma closure is a critical surgical intervention performed to reverse the diversion of intestinal contents following procedures, such as ileostomy or colostomy[1]. This closure is necessary for patients to regain normal bowel function and resume a conventional lifestyle[2]. However, this surgical procedure can have crucial implications for the gut microbiome, the complex ecosystem of microorganisms residing in the gastrointestinal tract[3]. The gut microbiome plays a pivotal role in maintaining digestive health, modulating immune responses, and influencing mental well-being[4]. Disturbances to this delicate balance can lead to a range of gastrointestinal symptoms, such as abdominal pain, bloating, and diarrhea, which can impair quality of life and slow recovery[5]. The core challenges following stoma closure extend beyond transient symptoms, often involving persistent gut dysbiosis that conventional Western medical interventions struggle to address fully. Standard postoperative care typically focuses on surgical site healing, pain management, and preventing infection, with little emphasis on actively restoring the microbial ecosystem. While interventions, like probiotics, are used, their efficacy can be inconsistent and may be insufficient to correct the profound alterations caused by surgery. This situation highlights a major limitation in current management protocols, creating a clear research gap for effective and holistic strategies.
Traditional Chinese medicine (TCM), with its rich history and diverse therapeutic modalities, has been increasingly recognized for its potential to affect the gut microbiota positively[6-8]. TCM interventions, including herbal medicine, acupuncture, and dietary therapy, have been shown to have anti-inflammatory and regulatory effects that could be beneficial in restoring gut health after surgery[9]. The multi-disciplinary team (MDT) approach involves collaboration between experts in TCM and Western medicine, each bringing unique diagnostic tools and treatment strategies to the table[10]. By combining TCM’s holistic and individualized assessments with Western medicine’s advanced diagnostic technologies, MDT aims to provide a comprehensive and personalized treatment plan for each patient[11]. This integrative strategy includes TCM interventions, such as herbal formulas tailored to the patient’s specific constitution and symptoms, alongside conventional Western medical treatments, such as medications and dietary advice. This retro
A retrospective study was conducted to evaluate the efficacy of a combined TCM and Western medicine MDT approach in promoting gut microbiome recovery after intestinal stoma closure. The study included patients who underwent intestinal stoma closure between January 2020 and December 2023 at Shijiazhuang People’s Hospital. The patients were divided into two groups: A control group receiving standard Western medical care and an MDT group receiving an integrative MDT approach that combines TCM and Western medicine.
The study population consisted of 251 patients who underwent intestinal stoma closure between January 2020 and December 2023 at Shijiazhuang People’s Hospital. The patients were divided into two groups on the basis of their treatment approach: The control (n = 122) and MDT (n = 129) groups.
Inclusion criteria: (1) Patients aged > 18 years; (2) Patients who underwent intestinal stoma closure surgery during the study period; (3) Patients with a complete set of medical records available for review; and (4) Patients who provided informed consent for their medical data to be used in this retrospective study.
Exclusion criteria: (1) Patients with advanced cancer, severe liver or kidney dysfunction, or other systemic diseases; (2) Patients who had previous major abdominal surgery that could affect the results of the current study; (3) Patients with a history of allergic reactions to TCM herbs or other components of the integrative treatment protocol; and (4) Patients who were lost to follow-up or whose data were incomplete for analysis.
Medical records were reviewed to collect data on patient demographics [age, gender, and body mass index (BMI)]; clinical characteristics (stoma type, stoma duration, previous surgery count, and chronic conditions); and pre- and postoperative gut microbiome composition, diversity, and functionality. Gut microbiome analysis was performed by using 16S ribosomal ribonucleic acid gene sequencing. Additionally, data on gastrointestinal symptoms, hospital stay duration, psychological well-being, and immunological and nutritional status indicators were collected.
Experts in TCM and Western medicine collaborated during the diagnostic phase, merging TCM's comprehensive evaluations (inspection, auscultation, inquiry, and palpation) with Western medicine’s sophisticated diagnostic tools to achieve precise diagnoses. A unified treatment strategy was developed, incorporating TCM treatments and moxibustion with Western medical interventions, such as medications and surgery, customized to the specific needs of each patient. Throughout the treatment journey, regular consultations between TCM and Western medicine practitioners occurred, enabling timely modifications to the treatment plan in response to the patient’s feedback and progress. A holistic rehabilitation program, which involved TCM’s health maintenance techniques along with Western medical rehabilitation exercises to aid in recovery and deter recurrence, was devised following treatment. TCM and Western medicine practitioners were also involved in health education, providing insights into maintaining well-being and preventing illness, thereby equipping patients with effective self-care tactics.
The control group received standard Western medical care, which included: (1) Postoperative medications, such as prophylactic antibiotics as needed, analgesics for pain management, and antiemetics for nausea; (2) Standard dietary advice, involving a gradual progression from clear liquids to a soft, low-residue diet to support healing; and (3) Physical therapy to aid in mobility and strength restoration as deemed necessary by the primary care team. By contrast, the MDT group received an integrative treatment approach that combined the above standard Western medical care with personalized TCM interventions. These interventions were formulated by a certified TCM practitioner within the MDT and included the following: (1) Herbal medicine: Patients were prescribed a modified version of the Jian Pi Li Chang Decoction (Spleen-Strengthening and Intestine-Regulating Decoction), administered orally once daily. The formula was tailored to each patient’s specific TCM pattern diagnosis (e.g., Spleen Qi Deficiency and Damp Heat in the Large Intestine) and aimed to reduce inflammation, promote gut motility, and restore digestive function; (2) Acupuncture and moxibustion: Daily sessions of acupuncture were performed at key acupoints known to regulate gastrointestinal function. These acupoints included Zusanli (ST36), Tianshu (ST25), and Shangjuxu (ST37). Moxibustion was applied to enhance warming and tonifying effects; and (3) TCM dietary therapy: In addition to standard dietary advice, patients received personalized guidance based on TCM principles, such as consuming warm, cooked foods (e.g., congee and steamed vegetables) and avoiding cold, raw, or greasy foods to protect the Spleen and Stomach qi.
Statistical analysis was performed by using SPSS software (Version 26.0). For continuous variables, data were presented as mean ± SD. Differences between the two groups were evaluated by using the independent samples t-test for normally distributed data and the Mann-Whitney U test for nonnormally distributed data. For categorical variables, frequencies, n (%) were presented, and associations were compared by using the χ2 test. For gut microbiome analysis, alpha diversity was calculated by employing the Shannon index, and beta diversity was analyzed through principal coordinates analysis. Statistical significance was set at P < 0.05.
A total of 251 patients participated in the study, with 122 patients and 129 patients allocated to the control and MDT groups, respectively. Upon comparison, no statistically significant differences were observed between the two study groups in terms of demographic profiles and health-related factors (Table 1).
| Baseline characteristics | Control group (n = 122) | MDT group (n = 129) | P value | |
| Age (years), mean ± SD | 55.2 ± 10.1 | 54.9 ± 9.8 | 0.723 | |
| Gender | 0.845 | |||
| Male | 67 (55.0) | 68 (52.7) | ||
| Female | 55 (45.0) | 61 (47.3) | ||
| BMI (kg/m²), mean ± SD | 23.4 ± 3.1 | 23.6 ± 3.0 | 0.652 | |
| Duration of stoma (months), mean ± SD | 8.5 ± 2.6 | 8.4 ± 2.5 | 0.876 | |
| Type of stoma | 0.789 | |||
| Ileostomy | 72 (58.9) | 75 (58.1) | ||
| Colostomy | 50 (41.1) | 54 (41.9) | ||
| Previous surgery count, mean ± SD | 1.2 ± 0.4 | 1.3 ± 0.5 | 0.462 | |
| Chronic conditions | 0.521 | |||
| DM | 17 (13.9) | 16 (12.4) | ||
| HTN | 15 (12.3) | 15 (11.6) | ||
| Asthma | 11 (9.0) | 13 (10.1) | ||
| CKD | 9 (7.4) | 8 (6.2) | ||
| Heart disease | 7 (5.7) | 8 (6.2) | 0.371 | |
| Preoperative Gut Symptom Score, mean ± SD | 6.2 ± 1.5 | 6.3 ± 1.4 | 0.425 | |
| Psychological State Score, mean ± SD | 3.1 ± 0.8 | 3.0 ± 0.7 | 0.538 | |
| Gut microbiome diversity, mean ± SD | 3.5 ± 0.6 | 3.6 ± 0.5 | ||
| Gut microbiome function, mean ± SD | 2.8 ± 0.7 | 2.9 ± 0.6 | 0.614 | |
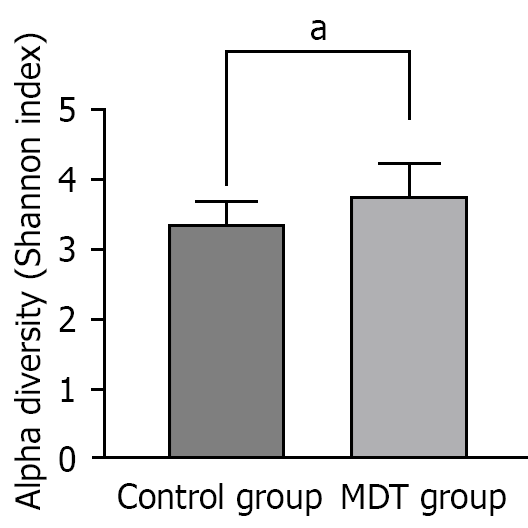
As shown in Figure 1, the MDT group showed a significantly higher alpha diversity postoperatively than the control group (P < 0.05). Furthermore, gut microbiome analysis revealed significant compositional differences (Table 2). The MDT group had higher operational taxonomic unit counts for Bacteroidetes and Proteobacteria than the control group (all P < 0.05), whereas the control group showed higher operational taxonomic unit counts for Firmicutes than the MDT group (P < 0.05).
| Gut microbiome characteristics | Control group (n = 122) | MDT group (n = 129) | P value |
| OTUs of Bacteroidetes | 1.2 × 108 ± 5.0 × 107 | 1.4 × 108 ± 4.8 × 107 | 0.001 |
| OTUs of Firmicutes | 1.8 × 108 ± 6.3 × 107 | 1.7 × 108 ± 5.9 × 107 | 0.033 |
| OTUs of Proteobacteria | 6.1 × 107 ± 4.1 × 106 | 7.3 × 107 ± 3.7 × 106 | < 0.001 |
As detailed in Table 3, the MDT group demonstrated a significantly lower prevalence of abdominal pain, bloating, and diarrhea postoperatively than the control group (all P < 0.05). Additionally, the MDT group had a shorter hospital stay, with 58.9% of its patients discharged within five days, than the control group, with 36.9% of its patients discharged within five days (P = 0.002).
| Outcome measure | Control group (n = 122) | MDT group (n = 129) | P value |
| Number of patients reporting | |||
| Abdominal pain | 38 (31.1) | 20 (15.5) | 0.003 |
| Bloating | 52 (42.6) | 30 (23.3) | 0.001 |
| Diarrhea | 29 (23.8) | 12 (9.3) | 0.014 |
| Constipation | 15 (12.3) | 5 (3.9) | 0.032 |
| Postoperative hospital stay (days) | |||
| ≤ 5 days | 45 (36.9) | 76 (58.9) | 0.002 |
| > 5 days | 77 (63.1) | 53 (41.1) | 0.002 |
The integrative MDT approach also appeared beneficial in managing chronic conditions (Table 4). The MDT group experienced a significantly higher rate of medication reduction for diabetes mellitus, hypertension, and chronic kidney disease postoperatively compared with the control group (all P < 0.05).
| Chronic condition management | Control group (n = 122) | MDT group (n = 129) | P value |
| Medication reduction for DM | 10 (8.2) | 22 (17.1) | 0.011 |
| Medication reduction for HTN | 12 (9.8) | 25 (19.4) | 0.019 |
| Medication reduction for CKD | 7 (5.7) | 16 (12.4) | 0.027 |
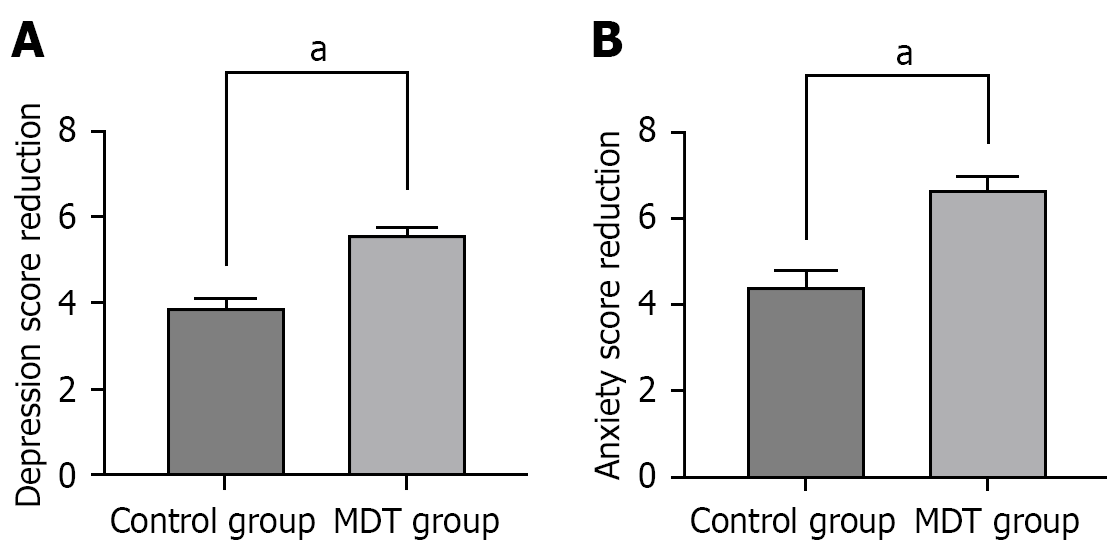
As illustrated in Figure 2, the patients in the MDT group reported better psychological well-being, with a significant reduction in depression (Figure 2A) and anxiety (Figure 2B) scores compared with the control group (all P < 0.05).
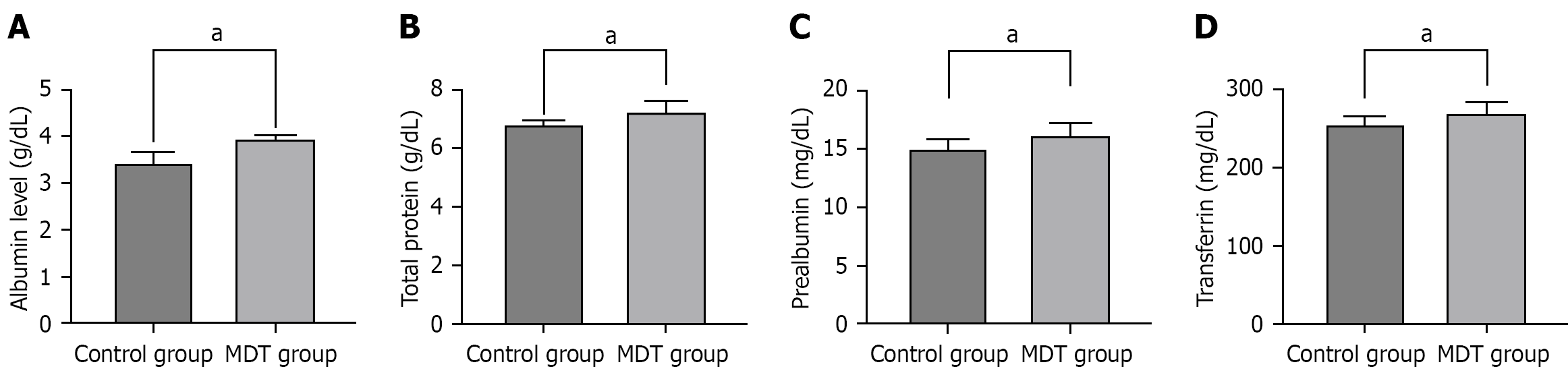
Figure 3 presents a comparison of key immunological indicators. The results showed that the MDT group had signi
The MDT group demonstrated significant improvements in nutritional status across multiple markers, as shown in Table 5. These improvements included a small negative change in BMI; reduced malnutrition prevalence; and signi
| Nutritional status indicators | Control group (n = 122) | MDT group (n = 129) | P value |
| BMI change | -1.2 ± 0.4 | -0.8 ± 0.3 | 0.009 |
| Malnutrition prevalence | 27 (22.1) | 12 (9.3) | 0.016 |
| Serum sodium (mmol/L) | 135 ± 3 | 137 ± 2 | 0.012 |
| Serum potassium (mmol/L) | 3.9 ± 0.4 | 4.1 ± 0.3 | 0.028 |
| Serum calcium (mg/dL) | 8.7 ± 0.6 | 9.0 ± 0.5 | 0.031 |
| Vitamin B12 (pg/mL) | 200 ± 40 | 220 ± 35 | 0.036 |
| Vitamin D (ng/mL) | 20 ± 5 | 25 ± 4 | 0.019 |
| Daily caloric intake (kcal) | 1800 ± 200 | 2000 ± 150 | 0.026 |
| Protein intake (g/day) | 60 ± 10 | 65 ± 8 | 0.017 |
| Fiber intake (g/day) | 20 ± 5 | 25 ± 4 | 0.024 |
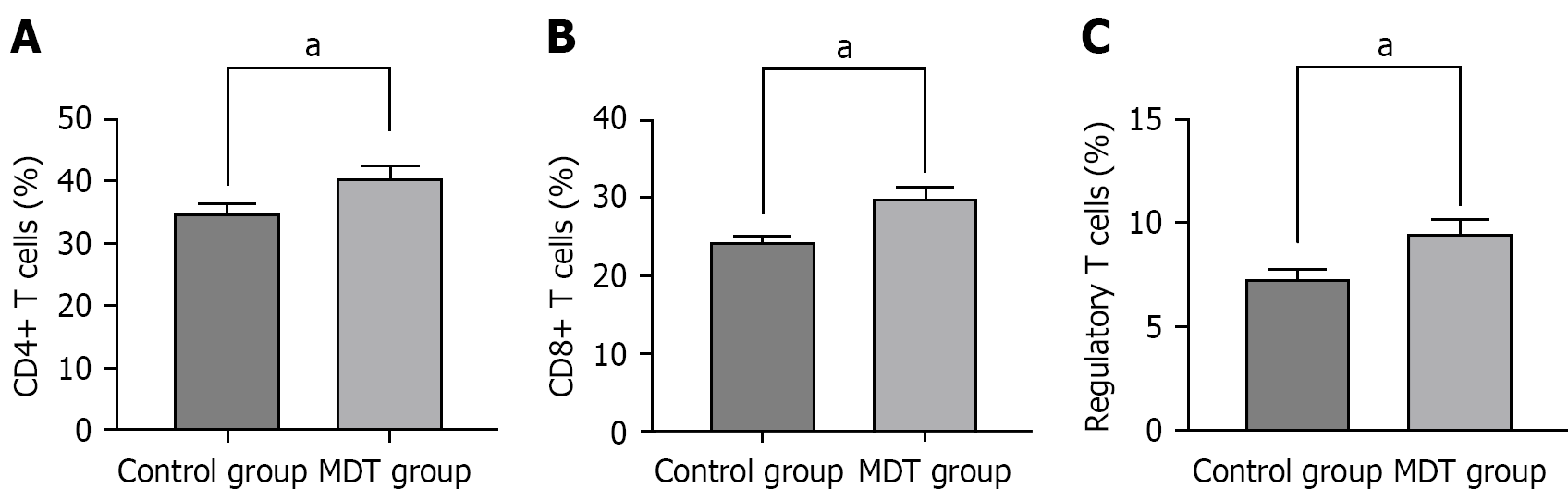
The MDT group exhibited enhanced immune function, as detailed in Figure 4. This enhancement was evidenced by the significantly increased percentages of CD4+ (Figure 4A), CD8+ (Figure 4B), and regulatory (Figure 4C) T cells, indicating a robust and balanced immune response (all P < 0.05).
Finally, as illustrated in Table 6, the MDT group experienced significant improvements in intestinal permeability, as reflected by a reduced lactulose: Mannitol ratio (P < 0.05). This change was accompanied with notable enhancements in quality of life, with the MDT group scoring higher in physical functioning, mental health, and social functioning compared with the control group (all P < 0.05).
| Outcome measures | Control group (n = 122) | MDT group (n = 129) | P value |
| Intestinal permeability - lactulose/mannitol ratio | 0.12 ± 0.03 | 0.09 ± 0.02 | 0.015 |
| Quality of life - physical functioning (SF-36) | 68.9 ± 8.4 | 77.5 ± 7.3 | 0.022 |
| Quality of life - mental health (SF-36) | 62.1 ± 9.2 | 70.4 ± 8.6 | 0.031 |
| Quality of life - social functioning (SF-36) | 73.2 ± 10.1 | 81.5 ± 9.4 | 0.029 |
In recent years, integrative medicine has gained remarkable traction within the healthcare community as healthcare providers increasingly recognize the synergistic advantages of blending traditional and complementary therapeutic strategies with conventional Western medical interventions[12-14]. At the heart of this integrative approach lies the MDT methodology, which leverages the collective expertise of professionals from diverse medical specialties to provide com
The results of this retrospective study indicate that the MDT approach, which combines TCM and Western medicine, has the potential to promote gut microbiome recovery effectively following intestinal stoma closure. This integrative strategy not only improved the composition, diversity, and functionality of the gut microbiome but also resulted in a reduction in gastrointestinal symptoms and a shortened hospital stay. The improvement in gut microbiome diversity, as evidenced by the higher Shannon index in the MDT group than in the control group, is particularly encouraging. This increased diversity may reflect a healthy gut ecosystem, which is crucial for the maintenance of overall health. The gut microbiome plays a pivotal role in various physiological processes, including digestion, metabolism, immune function, and even mental health[18-20]. Therefore, the positive changes observed in the MDT group could have wide-ranging implications for the well-being of patients after intestinal stoma closure. The gut microbiome analysis also revealed significant differences in the abundance of certain bacterial taxa between the two groups. The MDT group exhibited higher counts of Bacteroidetes and Proteobacteria compared with the control group, whereas the control group had higher counts of Firmicutes compared with the MDT group. These differences suggest that the integrative approach may influence the gut microbiome in a way that promotes a balanced and resilient microbial community. This balance is important because dysbiosis, or an imbalance in the gut microbiota, has been associated with various health issues, including gastrointestinal disorders, metabolic diseases, and immune dysregulation[21].
The reduction in gastrointestinal symptoms in the MDT group is another key finding. Abdominal pain, bloating, and diarrhea are common postoperative complications following intestinal stoma closure[22]. The fact that the MDT group experienced fewer of these symptoms relative to the control group suggests that the integrative approach may help mitigate the postoperative impact on the gut microbiome and improve digestive function. This effect could be due to the anti-inflammatory and regulatory effects of TCM interventions, which may help restore gut health and reduce inflammation. The shortened hospital stays in the MDT group are an additional benefit of the integrative approach. This finding not only improves patient satisfaction but also has economic implications by reducing healthcare costs. The reasons for the shortened stays are likely multifactorial, including reduced gastrointestinal symptoms, improved gut barrier function, and enhanced overall recovery. These factors may contribute to a rapid return to normal activities and an improved quality of life for patients.
The MDT approach also had a positive influence on chronic condition management. Patients with chronic conditions, such as diabetes mellitus, hypertension, and chronic kidney disease, reported improvements in their condition manage
The nutritional status improvements in the MDT group are another noteworthy finding. The reductions in BMI change and malnutrition prevalence, as well as the increased levels of key serum markers and dietary intake, indicate that the integrative approach may help improve nutrient absorption and utilization, which is crucial for recovery and overall health. Proper nutrition is essential for wound healing, immune function, and energy production, and the findings suggest that the integrative approach may offer considerable benefits in this regard[25]. The enhanced immune function in the MDT group, as evidenced by the increased percentages of CD4+, CD8+, and regulatory T cells, is particularly encouraging. These cells are critical for maintaining a balanced immune response, and their high levels in the MDT group suggest that the integrative approach may help improve immune function, which is important for postoperative recovery and overall health. A robust immune system can help prevent infections and other complications, leading to rapid and complete recovery[26]. The improvements in intestinal permeability and quality of life in the MDT group are also important findings. The reduced lactulose: Mannitol ratio in the MDT group suggests improved gut barrier function, which is crucial for preventing the entry of harmful substances into the bloodstream. The enhanced quality of life, particularly in physical functioning, mental health, and social functioning, as measured by the SF-36 scale, with the MDT group demonstrating better outcomes than the control group, indicates that the integrative approach may offer considerable benefits in this regard.
While the results of this study are promising, acknowledging the limitations of its retrospective design is important. The retrospective nature of this work may introduce selection bias, and the findings may not be generalizable to all patient populations. Furthermore, this study relied on medical records, which may be incomplete or inaccurate, for data collection. Future research should aim to validate these findings in large, prospective studies with rigorous methodology and standardized data collection
This study demonstrates the potential benefits of a combined TCM and Western MDT approach in promoting gut microbiome recovery and overall health following intestinal stoma closure. This integrative strategy not only improved the composition, diversity, and functionality of the gut microbiome but also resulted in a reduction in gastrointestinal symptoms, shortened hospital stays, and improved recovery outcomes. Its findings suggest that the MDT approach offers a promising strategy for optimizing postoperative recovery and improving patient outcomes in this patient population.
| 1. | Allart K, Sabbagh C, Demouron M, Brazier F, Regimbeau JM. Natural history of anastomotic leakage after elective stoma closure. J Visc Surg. 2023;160:96-100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 2. | Hajibandeh S, Hajibandeh S, Maw A. Purse-string skin closure versus linear skin closure in people undergoing stoma reversal. Cochrane Database Syst Rev. 2024;3:CD014763. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 14] [Reference Citation Analysis (0)] |
| 3. | Farhad T, Sarwar MKA, Chowdhury MZ, Walid A, Sadia A, Chowdhury TK. Fast Track versus Conventional Perioperative Care Protocols in Paediatric Intestinal Stoma Closure ‒ A Randomised Study. Afr J Paediatr Surg. 2024;21:123-128. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 4. | Kuziel GA, Rakoff-Nahoum S. The gut microbiome. Curr Biol. 2022;32:R257-R264. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 160] [Cited by in RCA: 124] [Article Influence: 31.0] [Reference Citation Analysis (1)] |
| 5. | Dhopatkar N, Keeler JL, Mutwalli H, Whelan K, Treasure J, Himmerich H. Gastrointestinal symptoms, gut microbiome, probiotics and prebiotics in anorexia nervosa: A review of mechanistic rationale and clinical evidence. Psychoneuroendocrinology. 2023;147:105959. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 36] [Reference Citation Analysis (1)] |
| 6. | Li Z, Feiyue Z, Gaofeng L. Traditional Chinese medicine and lung cancer--From theory to practice. Biomed Pharmacother. 2021;137:111381. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 175] [Article Influence: 35.0] [Reference Citation Analysis (1)] |
| 7. | Zhang YL, Wang YL, Yan K, Li H, Zhang X, Essola JM, Ding C, Chang K, Qing G, Zhang F, Tan Y, Peng T, Wang X, Jiang M, Liang XJ, Hua Q. Traditional Chinese Medicine Formulae QY305 Reducing Cutaneous Adverse Reaction and Diarrhea by its Nanostructure. Adv Sci (Weinh). 2024;11:e2306140. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 36] [Cited by in RCA: 30] [Article Influence: 15.0] [Reference Citation Analysis (1)] |
| 8. | Zhang S, Wang W, Pi X, He Z, Liu H. Advances in the Application of Traditional Chinese Medicine Using Artificial Intelligence: A Review. Am J Chin Med. 2023;51:1067-1083. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 34] [Reference Citation Analysis (1)] |
| 9. | Wang XQ, Li H, Li XN, Yuan CH, Zhao H. Gut-Brain Axis: Possible Role of Gut Microbiota in Perioperative Neurocognitive Disorders. Front Aging Neurosci. 2021;13:745774. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 21] [Article Influence: 5.3] [Reference Citation Analysis (1)] |
| 10. | Reddy D, Bedi N, Dudderidge T. Focal therapy, time to join the multi-disciplinary team discussion? Transl Androl Urol. 2020;9:1526-1534. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 11. | Ibrahim H, Harhara T, Athar S, Nair SC, Kamour AM. Multi-Disciplinary Discharge Coordination Team to Overcome Discharge Barriers and Address the Risk of Delayed Discharges. Risk Manag Healthc Policy. 2022;15:141-149. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 24] [Article Influence: 6.0] [Reference Citation Analysis (1)] |
| 12. | Parker J, Gupta S, Shenbagaraj L, Harborne P, Ramaraj R, Karandikar S, Mottershead M, Barbour J, Mohammed N, Lockett M, Lyons A, Vega R, Torkington J, Dolwani S. Outcomes of complex colorectal polyps managed by multi-disciplinary team strategies-a multi-centre observational study. Int J Colorectal Dis. 2023;38:28. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 6] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 13. | Abnett H, Tuckwell R, Evans L. Early introduction of the multi-disciplinary team through student Schwartz Rounds: a mixed methodology study. BMC Med Educ. 2022;22:523. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 8] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 14. | Lewis H, Biesecker B, Lee SS, Anderson K, Joseph G, Jenkins CL, Bulkley JE, Leo MC, Goddard KAB, Wilfond BS. Promoting equity, inclusion, and efficiency: A team science approach to the development of authorship guidelines for a multi-disciplinary research team. J Clin Transl Sci. 2023;7:e265. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 15. | Merker L, Conroy S, El-Wakeel H, Laurence N. Streamlining the Multi-Disciplinary Team Meeting: The Introduction of Robust Pre-Preparation Methods and Its Effect on the Length of Case Discussions. J Multidiscip Healthc. 2023;16:613-622. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (1)] |
| 16. | Zhang T, Gao G, Kwok LY, Sun Z. Gut microbiome-targeted therapies for Alzheimer's disease. Gut Microbes. 2023;15:2271613. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 95] [Reference Citation Analysis (1)] |
| 17. | Beamish EL, Johnson J, Shih B, Killick R, Dondelinger F, McGoran C, Brewster-Craig C, Davies A, Bhowmick A, Rigby RJ. Delay in loop ileostomy reversal surgery does not impact upon post-operative clinical outcomes. Complications are associated with an increased loss of microflora in the defunctioned intestine. Gut Microbes. 2023;15:2199659. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 9] [Reference Citation Analysis (1)] |
| 18. | Kraimi N, Ross T, Pujo J, De Palma G. The gut microbiome in disorders of gut-brain interaction. Gut Microbes. 2024;16:2360233. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 37] [Reference Citation Analysis (1)] |
| 19. | Brown EM, Clardy J, Xavier RJ. Gut microbiome lipid metabolism and its impact on host physiology. Cell Host Microbe. 2023;31:173-186. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 371] [Cited by in RCA: 299] [Article Influence: 99.7] [Reference Citation Analysis (1)] |
| 20. | Wiertsema SP, van Bergenhenegouwen J, Garssen J, Knippels LMJ. The Interplay between the Gut Microbiome and the Immune System in the Context of Infectious Diseases throughout Life and the Role of Nutrition in Optimizing Treatment Strategies. Nutrients. 2021;13:886. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 405] [Cited by in RCA: 311] [Article Influence: 62.2] [Reference Citation Analysis (1)] |
| 21. | Sorboni SG, Moghaddam HS, Jafarzadeh-Esfehani R, Soleimanpour S. A Comprehensive Review on the Role of the Gut Microbiome in Human Neurological Disorders. Clin Microbiol Rev. 2022;35:e0033820. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 211] [Cited by in RCA: 360] [Article Influence: 90.0] [Reference Citation Analysis (1)] |
| 22. | Yang S, Tang G, Zhang Y, Wei Z, Du D. Meta-analysis: loop ileostomy versus colostomy to prevent complications of anterior resection for rectal cancer. Int J Colorectal Dis. 2024;39:68. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 16] [Article Influence: 8.0] [Reference Citation Analysis (1)] |
| 23. | Koc MA, Akyol C, Gokmen D, Aydin D, Erkek AB, Kuzu MA. Effect of Prehabilitation on Stoma Self-Care, Anxiety, Depression, and Quality of Life in Patients With Stomas: A Randomized Controlled Trial. Dis Colon Rectum. 2023;66:138-147. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 20] [Article Influence: 6.7] [Reference Citation Analysis (1)] |
| 24. | Chakraborty B, Byemerwa J, Krebs T, Lim F, Chang CY, McDonnell DP. Estrogen Receptor Signaling in the Immune System. Endocr Rev. 2023;44:117-141. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 197] [Cited by in RCA: 168] [Article Influence: 56.0] [Reference Citation Analysis (1)] |
| 25. | Wickramasinghe K, Mathers JC, Wopereis S, Marsman DS, Griffiths JC. From lifespan to healthspan: the role of nutrition in healthy ageing. J Nutr Sci. 2020;9:e33. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 50] [Article Influence: 8.3] [Reference Citation Analysis (1)] |
| 26. | Buonacera A, Stancanelli B, Colaci M, Malatino L. Neutrophil to Lymphocyte Ratio: An Emerging Marker of the Relationships between the Immune System and Diseases. Int J Mol Sci. 2022;23:3636. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 284] [Cited by in RCA: 640] [Article Influence: 160.0] [Reference Citation Analysis (1)] |