©Author(s) (or their employer(s)) 2026.
World J Gastrointest Surg. Feb 27, 2026; 18(2): 116100
Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.116100
Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.116100
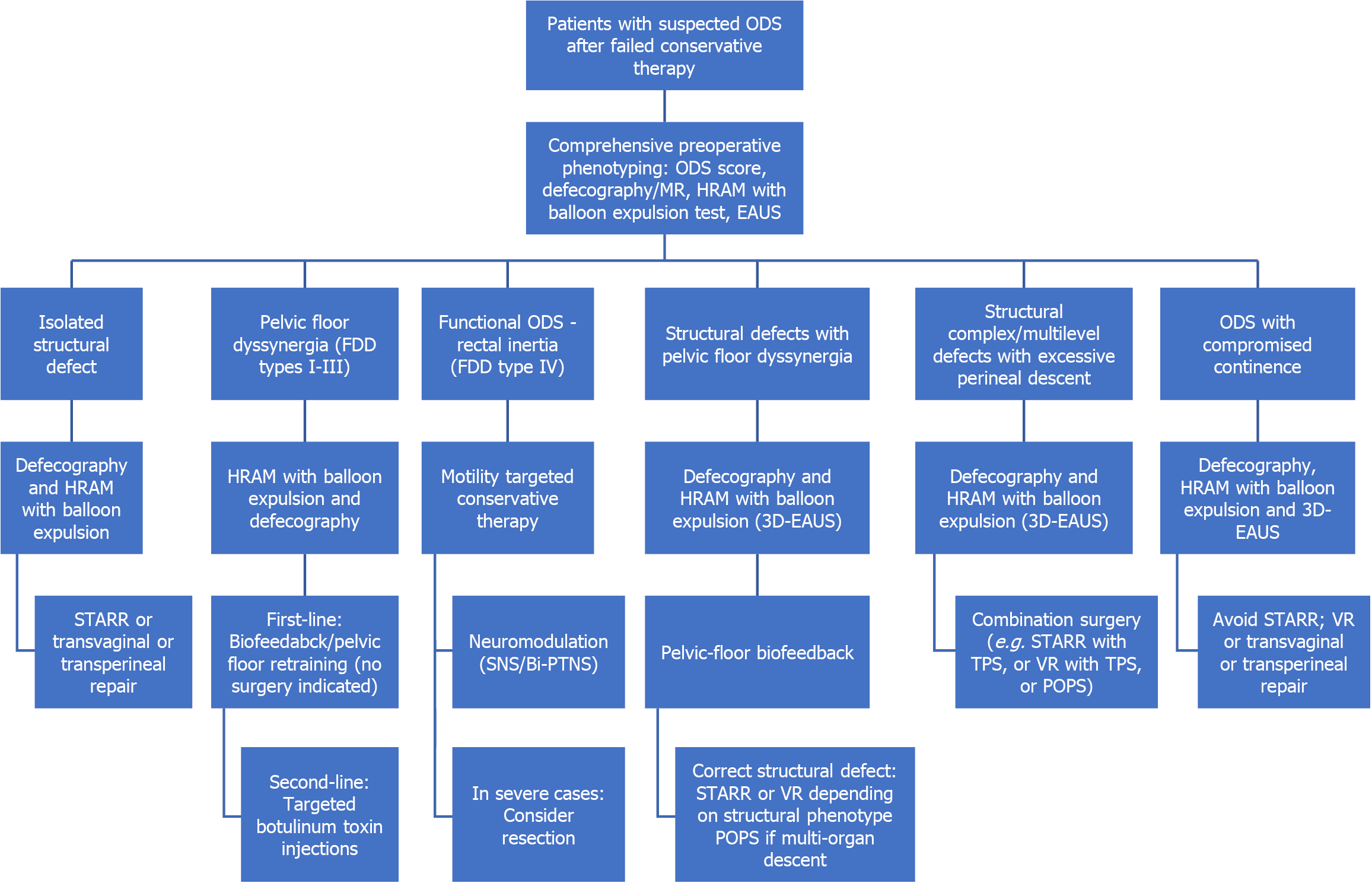
Figure 1 Algorithm for phenotype-guided surgical management of obstructed defecation syndrome.
This algorithm stratifies patients with obstructed defecation syndrome into distinct anatomical and functional phenotypes to guide optimal intervention. Structural phenotypes include isolated anatomical defects, complex multi-compartment prolapse, and high-grade internal intussusception. Functional phenotypes comprise functional defecatory disorders (FDD) types I-IV, based on high-resolution anorectal manometry patterns and balloon expulsion testing. Mixed phenotypes incorporate both anatomical obstruction and pelvic floor dyssynergia. For each subtype, the algorithm outlines preferred first-line and second-line interventions, including stapled transanal rectal resection, ventral rectopexy, pelvic organ prolapse suspension, targeted biofeedback, botulinum toxin for refractory dyssynergia, neuromodulation strategies (sacral neuromodulation, bilateral percutaneous tibial nerve stimulation), and transverse perineal support. The figure highlights the critical principle that suspensive procedures should be avoided in rectal inertia (FDD type IV), where inadequate rectal propulsive pressure is the dominant pathophysiology. ODS: Obstructed defecation syndrome; MR: Magnetic resonance; EAUS: Endoanal ultrasound; HRAM: High-resolution anorectal manometry; STARR: Stapled transanal rectal resection; FDD: Functional defecatory disorder; SNS: Sacral neuromodulation; Bi-PTNS: Bilateral percutaneous tibial nerve stimulation; 3D: Three dimensional; VR: Ventral rectopexy; POPS: Pelvic organ prolapse suspension; TPS: Transverse perineal support.
- Citation: Schiano di Visconte M, Sarnari S. Beyond stapled transanal rectal resection vs ventral rectopexy dichotomy: Toward a phenotype-guided surgical paradigm for obstructed defecation syndrome. World J Gastrointest Surg 2026; 18(2): 116100
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/116100.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.116100