©Author(s) (or their employer(s)) 2026.
World J Gastrointest Surg. Feb 27, 2026; 18(2): 113021
Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.113021
Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.113021
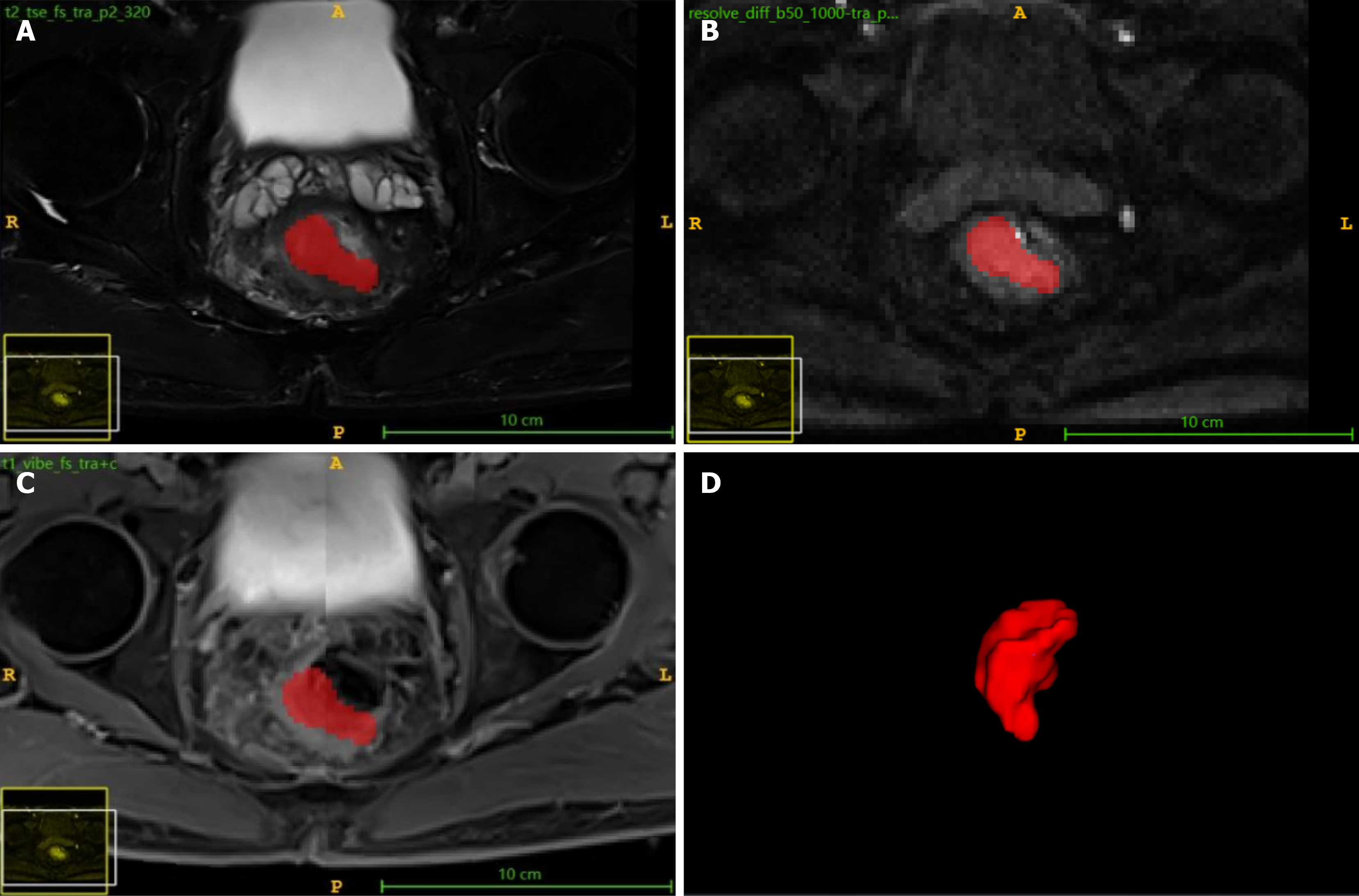
Figure 1 Region of interest delineation of rectal cancer lesion area.
A: Region of interest (ROI) delineation on axial fat-suppressed T2-weighted imaging; B: ROI delineation on diffusion-weighted imaging; C: ROI delineation on axial fat-suppressed T1-weighted contrast-enhanced imaging; D: Volume of rectal cancer region of interest based on single-slice ROI fusion.
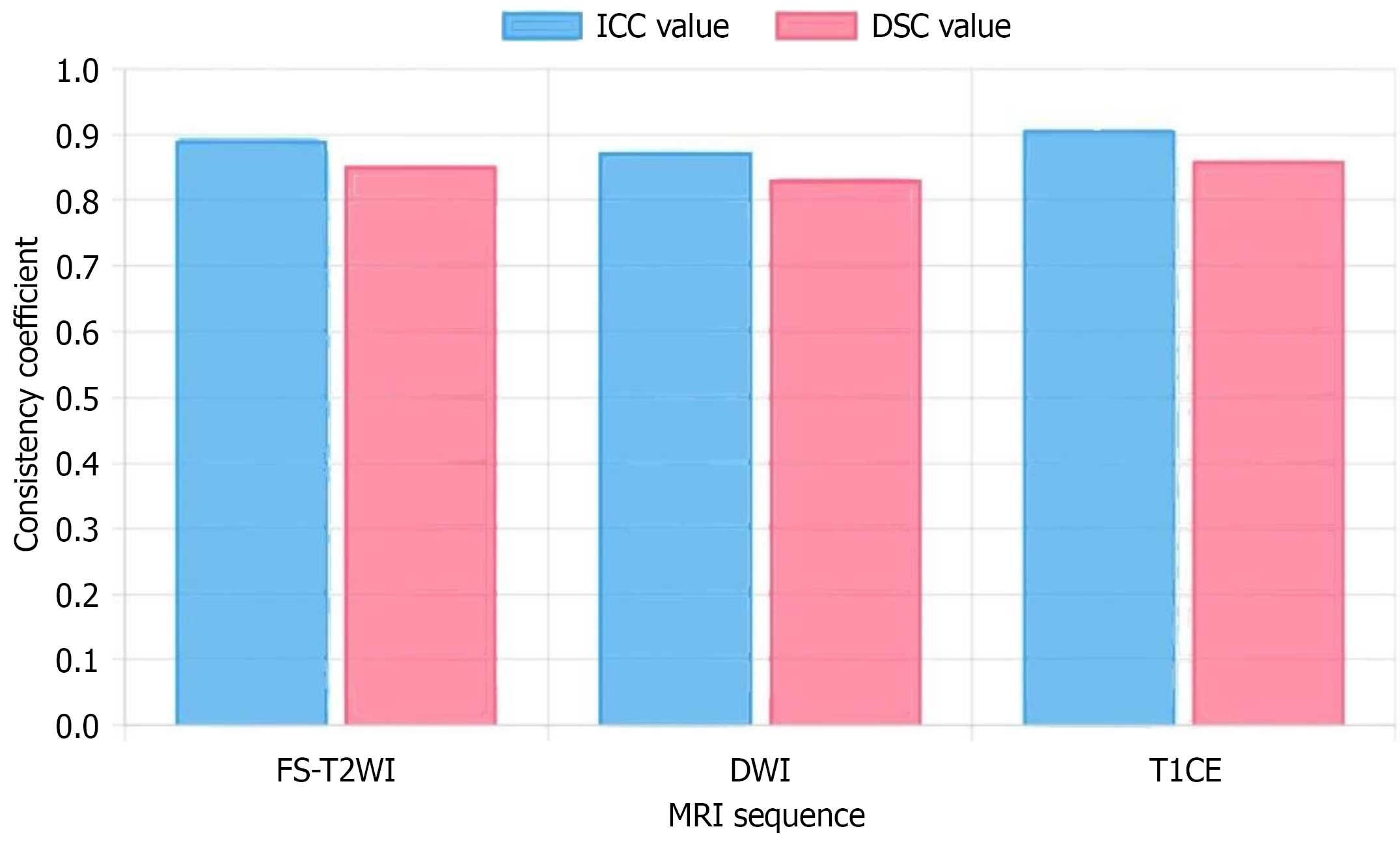
Figure 2 Inter-observer consistency assessment results.
Comparison of intraclass correlation coefficient and Dice similarity coefficient values across magnetic resonance imaging sequences (fat-suppressed T2-weighted imaging, diffusion-weighted imaging, T1-weighted contrast-enhanced imaging). ICC: Intraclass correlation coefficient; DSC: Dice similarity coefficient; FS-T2WI: Fat-suppressed T2-weighted imaging; DWI: Diffusion-weighted imaging; T1CE: T1-weighted contrast-enhanced imaging; MRI: Magnetic resonance imaging.
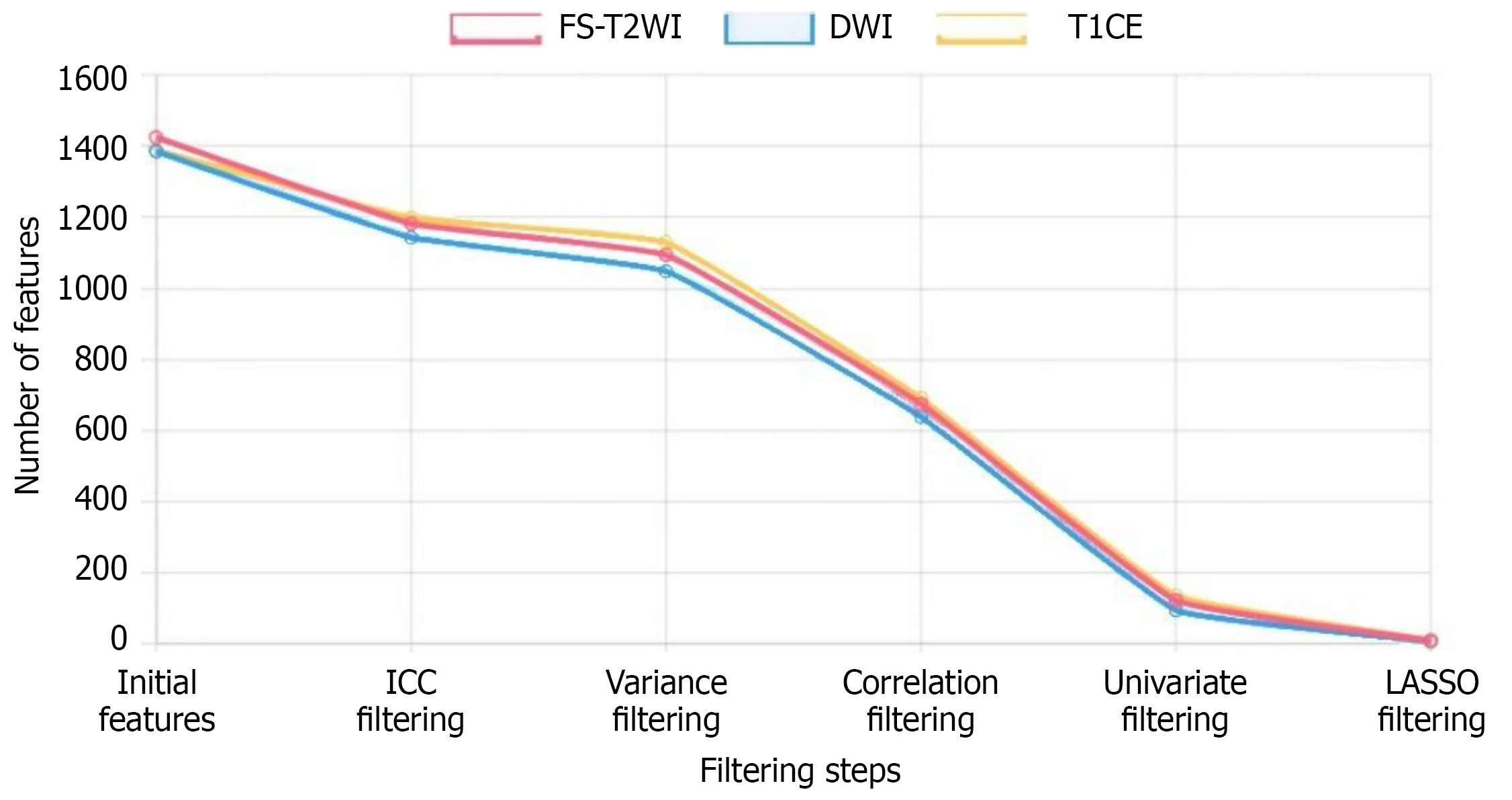
Figure 3 Radiomics feature selection process.
Feature-reduction pipeline across three magnetic resonance imaging sequences (fat-suppressed T2-weighted imaging, diffusion-weighted imaging, T1-weighted contrast-enhanced imaging). Bars show the number of radiomic features remaining after each filtering step: Initial extraction, intraclass correlation coefficient thresholding, variance filtering, correlation filtering, univariate selection, and least absolute shrinkage and selection operator regression. FS-T2WI: Fat-suppressed T2-weighted imaging; DWI: Diffusion-weighted imaging; T1CE: T1-weighted contrast-enhanced imaging; ICC: Intraclass correlation coefficient; LASSO: Least absolute shrinkage and selection operator.
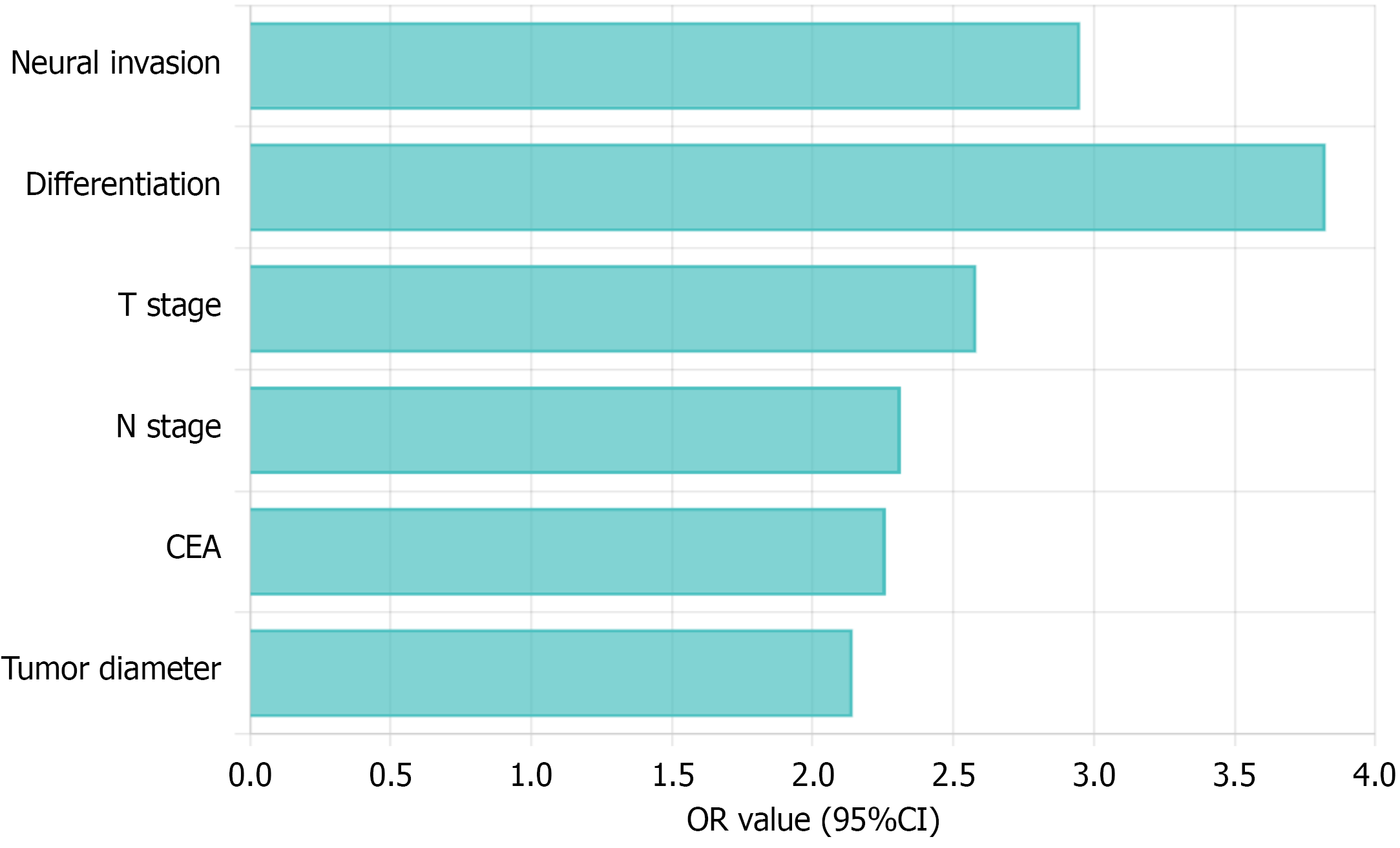
Figure 4 Forest plot of independent predictors for lymphovascular invasion.
Forest plot of clinicopathologic predictors of neural invasion. Horizontal lines represent odds ratio with 95% confidence intervals; vertical reference line at odds ratio = 1. OR: Odds ratio; CI: Confidence interval; CEA: Carcinoembryonic antigen.
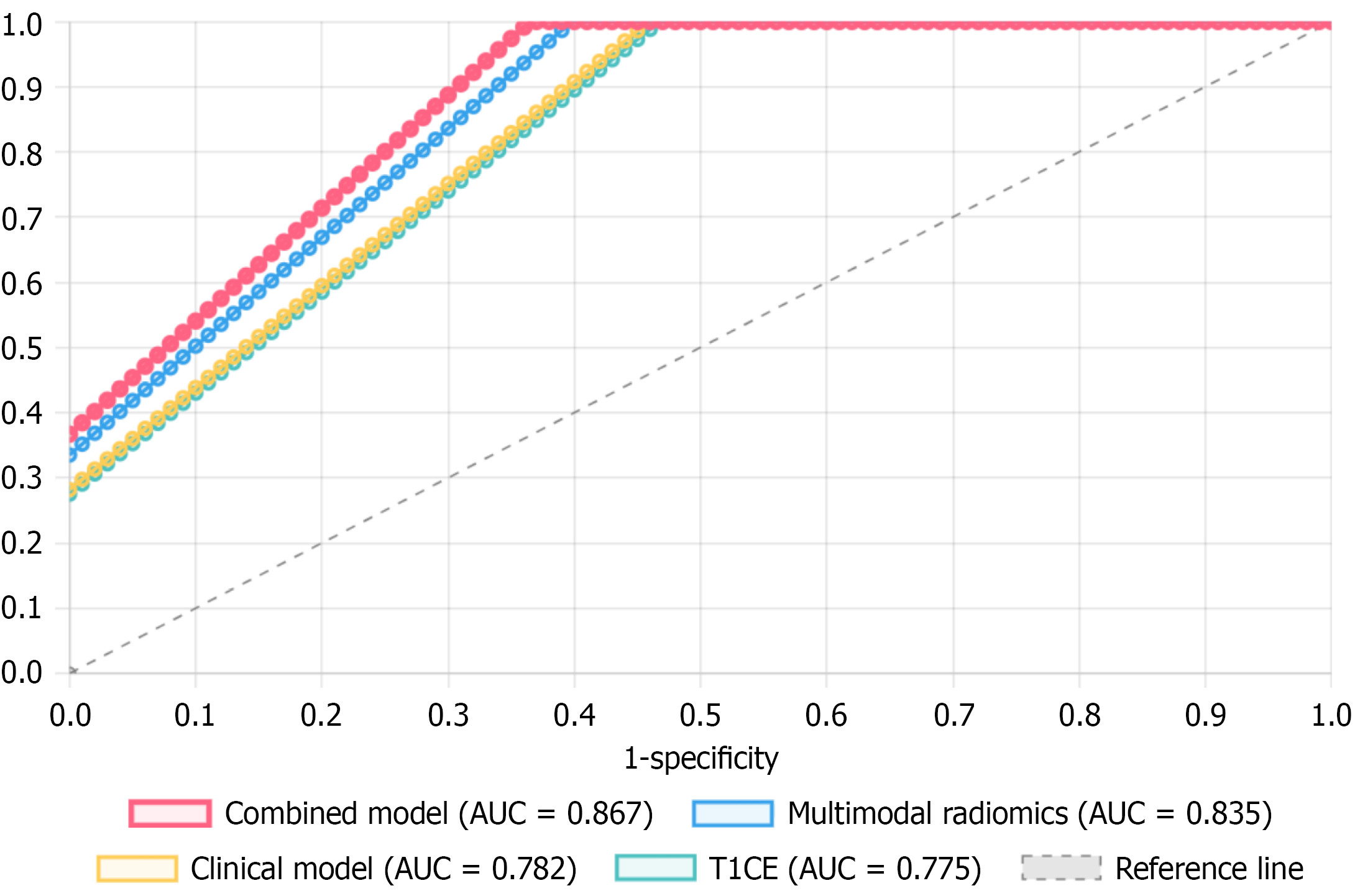
Figure 5 Receiver operating characteristic curve comparison of different models (test set).
Receiver operating characteristic curves comparing the diagnostic performance of the combined model [area under the curve (AUC) = 0.867], multimodal radiomics (AUC = 0.835), clinical model (AUC = 0.782) and T1-weighted contrast-enhanced imaging alone (AUC = 0.775) for predicting neural invasion. The dashed diagonal indicates the reference line (AUC = 0.5). AUC: Area under the curve; T1CE: T1-weighted contrast-enhanced imaging.
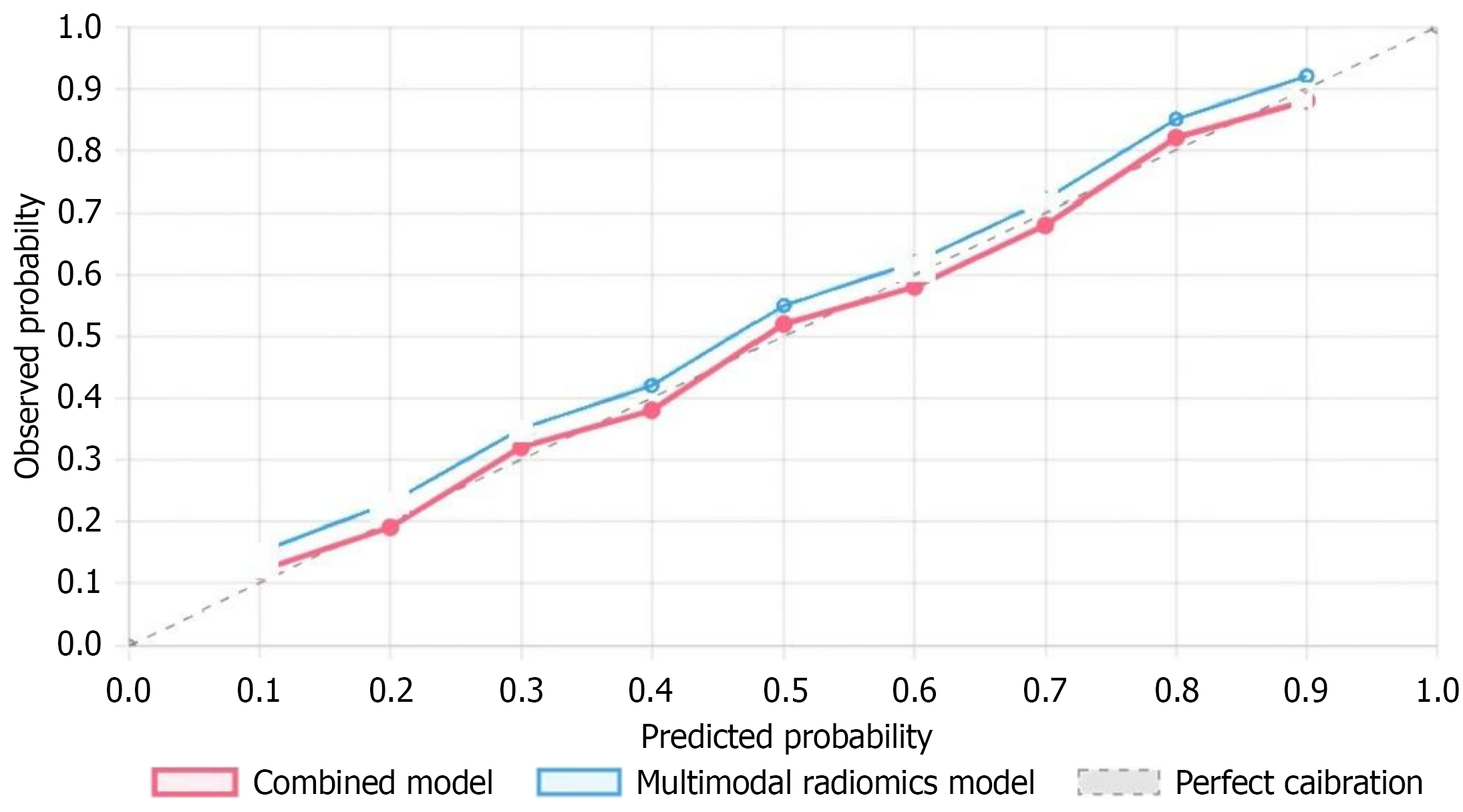
Figure 6 Model calibration curves (test set).
Calibration plot of the combined model: Predicted vs observed probabilities of neural invasion. The solid gray line indicates perfect calibration; closeness of the model’s curve to this line demonstrates good agreement.
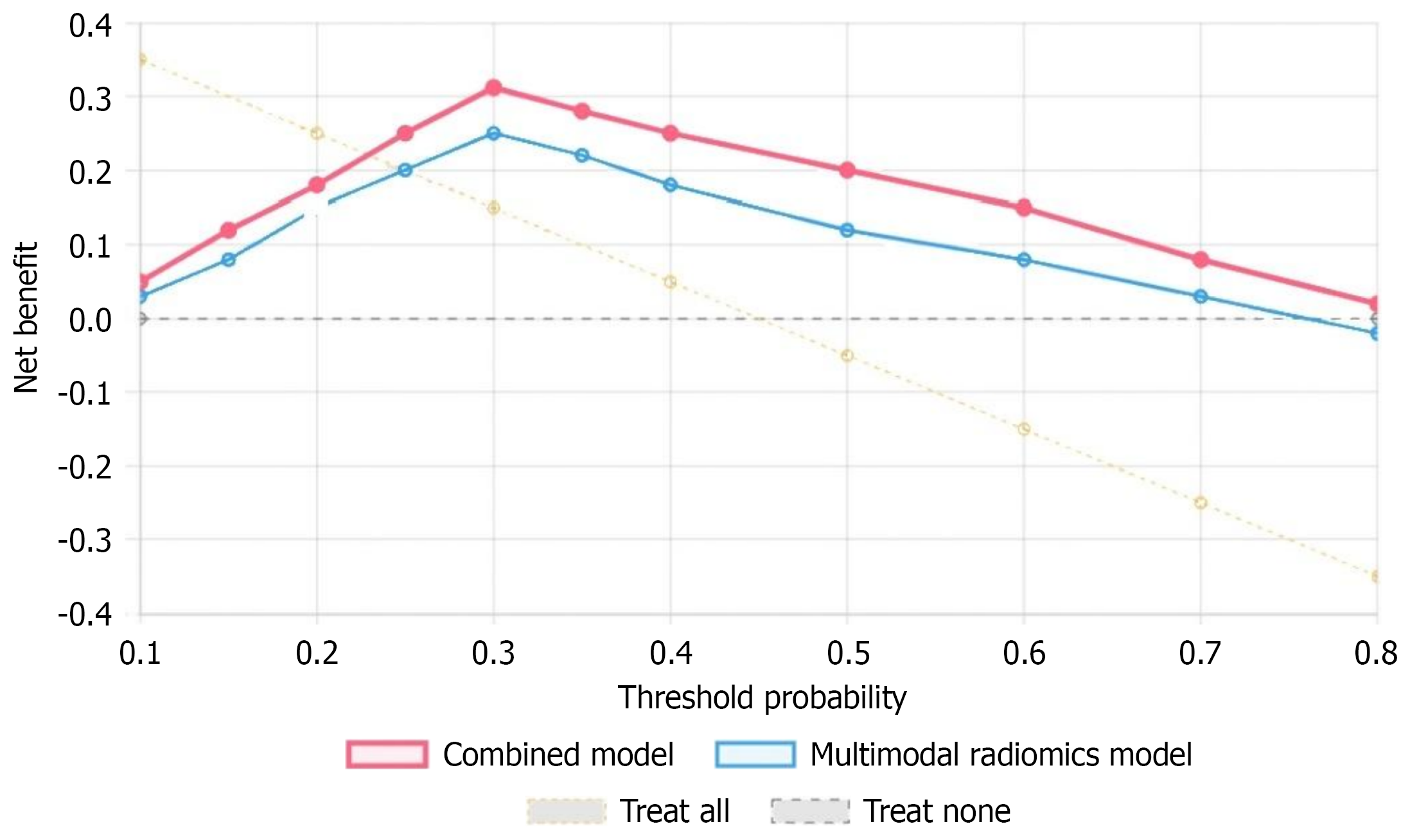
Figure 7 Decision curve analysis.
Decision curve analysis for the combined model vs the radiomics model and extreme strategies (treat-all, treat-none). The combined model displays the highest net benefit across the entire range of threshold probabilities, indicating superior clinical utility.
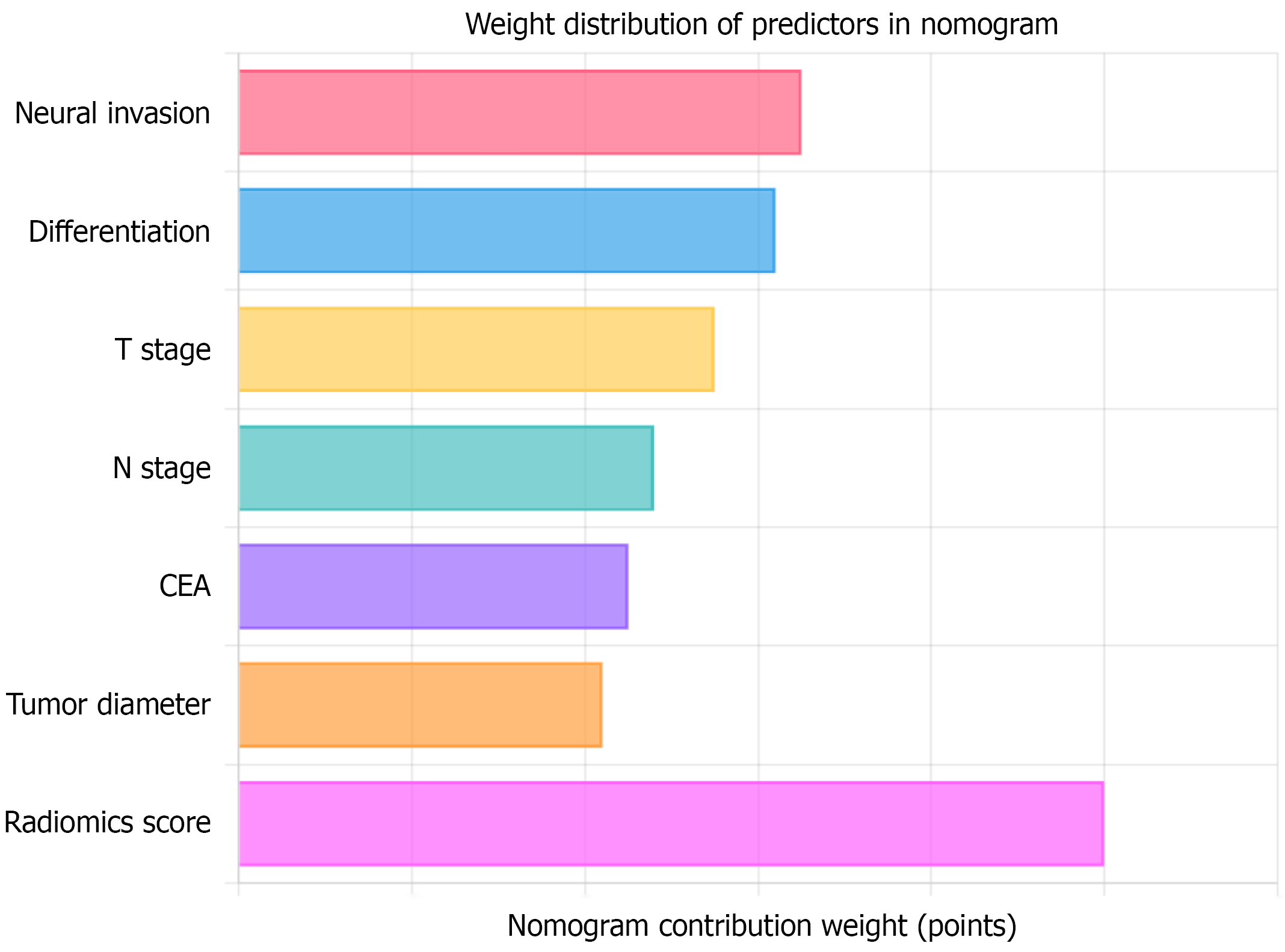
Figure 8 Lymphovascular invasion prediction nomogram.
Relative contribution (points) of each predictor within the nomogram for estimating the risk of neural invasion. Longer bars denote greater influence on the final probability, with radiomics score, differentiation, and T stage providing the highest weights. CEA: Carcinoembryonic antigen.
- Citation: Zhu ZH, Liang Y, Shi M. Prediction of lymphovascular invasion in rectal cancer based on multimodal magnetic resonance imaging radiomics model. World J Gastrointest Surg 2026; 18(2): 113021
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/113021.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.113021