Published online Apr 16, 2026. doi: 10.4253/wjge.v18.i4.118361
Revised: January 21, 2026
Accepted: February 11, 2026
Published online: April 16, 2026
Processing time: 104 Days and 11.3 Hours
Endoscopic retrograde cholangiopancreatography (ERCP) is a crucial treatment modality for biliary and pancreatic obstruction carrying significant technical challenges and high complication rate. Although rare, complication of perforation can lead to significant morbidity and mortality if not promptly recognized and managed appropriately.
To investigate the incidence, patterns of diagnosis and management and out
This study is a post-hoc analysis of a prospectively collected database of ERCP procedures carried out in a referral center in Lithuania between 2010 and 2019.
In the period between 2010 and 2019 years 5462 ERCP procedures were per
ERCP associated perforation is a rare but potentially fatal procedural complication, necessitating prompt diagnosis, thorough workup and a multidisciplinary management plan.
Core Tip: Endoscopic retrograde cholangiopancreatography (ERCP) is a mainstay minimally invasive treatment modality for biliary and pancreatic duct obstruction. Despite rapid advances in endoscopic techniques ERCP remains one of the most complication-prone interventions. Although rare, ERCP associated perforations can lead to significant morbidity and mortality if not promptly recognized and managed appropriately. This article provides detailed insight into the diagnostic and clinical pathways of managing ERCP associated perforations in a high-volume center, crucial decision-making aspects and promising facets to consider for improved patient outcomes. The results underpin the significance of prompt diagnosis and the importance of multidisciplinary approach when managing ERCP associated perforations.
- Citation: Dieninyte E, Pliuskute K, Jarasunas J, Stanaitis J, Poskus T. Endoscopic retrograde cholangiopancreatography associated perforations: 10-year experience of a large volume center. World J Gastrointest Endosc 2026; 18(4): 118361
- URL: https://www.wjgnet.com/1948-5190/full/v18/i4/118361.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i4.118361
Endoscopic retrograde cholangiopancreatography (ERCP) is a pivotal minimally invasive therapeutic intervention in the management of biliary and pancreatic duct obstruction. Even with the advancements in endoscopic techniques, it remains one of the most technically challenging and complication-prone endoscopic interventions. The main complications of ERCP are post-ERCP pancreatitis, bleeding, cholangitis, cholecystitis, with perforation being among the most perilous adverse events. ERCP associated perforation is the rarest of ERCP related complications with the overall incidence reported from 0.08% to 0.6%[1-3], compared to the most common-post-ERCP-pancreatitis, with the overall incidence of 3% to 10%[4,5], perforations can lead to significant morbidity and mortality if not promptly recognized and managed appropriately[6,7].
There are several mechanisms of ERCP associated perforations: Luminal perforation due to manipulation of the endoscope, extension of sphincterotomy cut beyond the intramural bile duct and extramural passage of guidewires or stent migration.
The risk factors for ERCP associated perforations, such as sphincterotomy, precut techniques, difficult cannulation, and anatomical variations such as periampullary diverticula or altered surgical anatomy, have been identified and necessitate even more measured ERCP technique[8-10]. The Stapfer classification, introduced in 2000, remains the most widely accepted system for categorizing ERCP associated perforations, guiding both diagnosis and management. This classification distinguishes perforations based on anatomical localization and mechanism into four types, each with distinct clinical implications and prognostic significance[7,11].
Despite advances in imaging and endoscopic techniques, the mortality associated with ERCP related perforation remains substantial. Population-based studies report overall ERCP mortality as high as 0.14%, with perforation-specific mortality ranging from 2% to over 20%, depending on the timing of diagnosis, the type of perforation, and the chosen management strategy[6,7]. Timely identification and early intervention are critical to improving outcomes. Recent evidence suggests that intra-procedural diagnosis and endoscopic closure techniques may significantly reduce the need for surgery and shorten hospital stay[6,12].
This study aims to investigate the incidence, patterns of diagnosis, management and outcomes of ERCP associated perforations in a high-volume center in the span of 10 years and reviews 2 illustrative clinical cases.
A large prospectively collected database of ERCP procedures carried out between 2010 and 2019 was analyzed for ERCP associated perforations. All patients with a diagnosis of ERCP associated perforation were included in the analysis. Permission by the Vilnius regional bioethics committee for the study was obtained (No. 2023/10-1539-1006). The study was conducted in accordance with the principles of the Declaration of Helsinki. Patients whose ERCP procedures were complicated by intraprocedural perforations were identified and demographic data, data regarding diagnostic workup and management of the perforations was collected. Incidences are provided as counts and percentages, whereas continuous data are presented as averages or medians for normally and non-normally distributed data, respectively.
In the period between 2010 and 2019 years 5462 ERCP procedures were performed. 2665 ERCP procedure were carried out with an intention of biliary stent placement resulting in 20 perforations (0.75%). The average age of patients with ERCP related perforations was 73.2 ± 11.9 years, 7 of them being male (35%). All of the patients had risk factors for procedure associated perforation (n = 20, 100%), and in 13 patients cannulation of the biliary tract was classified as “difficult” (65%). Perforations most often occurred in biliary tract (n = 8, 40%). The most common perforation type was type III according to Stapfer (n = 9, 45%) and type III according to Howard (n = 10, 50%). Half of the patients with diagnosed ERCP associated perforation underwent surgical interventions (n = 10, 50%). Median duration of hospitalization for patients with ERCP related perforations was 16.5 days and a quarter of the patients died (n = 5, 25%).
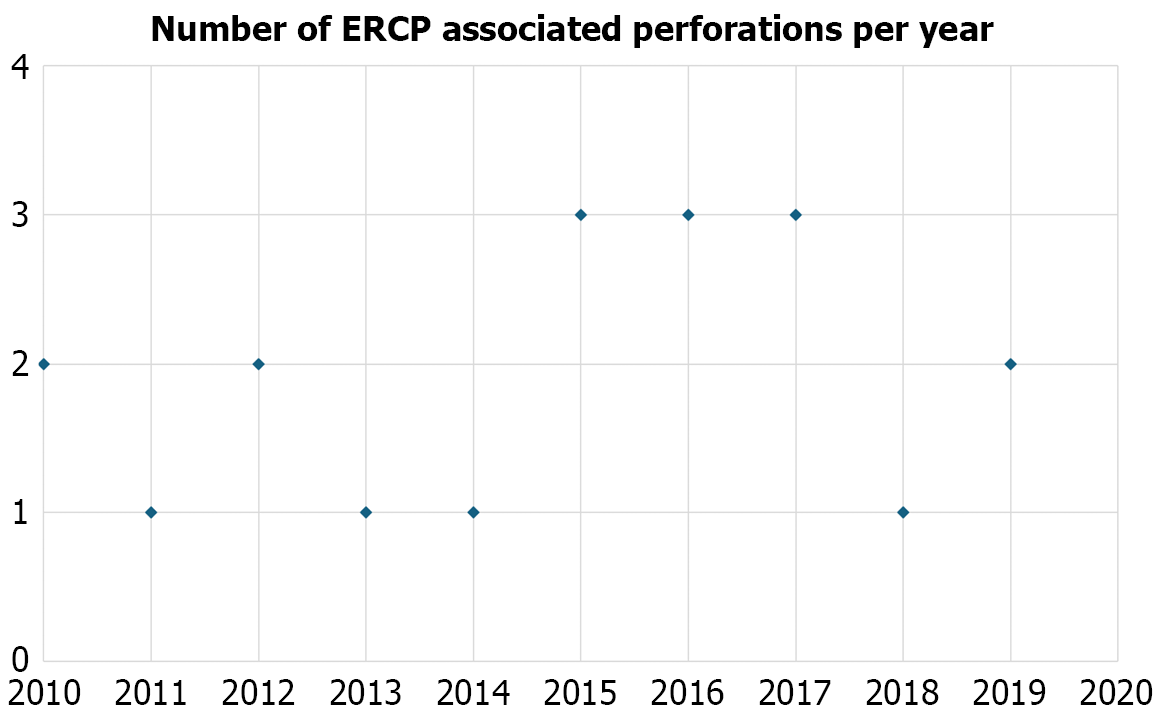
During the period of the study, ERCP procedures were performed by 6 HPB-procedure dedicated endoscopist, 3 of whom performed ERCP procedures during the entirety of analyzed period. There was no significant time trend of decline in incidence of ERCP associated perforations, that would suggest accumulating experience and remained in the range of 1 to 3 per year (Figure 1).
Out of 20 patients with ERCP associated perforations, the complication was diagnosed during ERCP in 6 patients (30%), in the next 24 hours post the procedure in 10 (50%) and after 24 hours post the procedure in 4 (20%). In 13 patients (65%) principal complaint after the ERCP was severe pain and 9 (45%) developed clinical signs of peritonitis. In addition to ERCP associated perforation, 13 patients (65%) were also diagnosed with post-ERCP pancreatitis.
In 5 patients (25%) ultrasound was the only and definitive imaging modality to diagnose an ERCP associated perforation and guide further management. To establish definitive diagnosis 9 patients (45%) underwent contrast-enhanced computerized tomography (CT) and in all the cases the results were conclusive. In none of the cases X-ray was sufficient to identify free air in the abdomen.
Out of 20 patients with ERCP associated perforations, all patients had clinical symptoms of perforations. For 12 patients (60%) primary endoscopic management (stenting or clipping) was sufficient to resolve the perforation when noticed during the index procedure. Of note, all of the patients with successful primary endoscopic closure of perforation 7 (35%) (either clipping or stenting), had complete resolution of perforation and avoided additional interventions.
Four patients (20%) had to undergo surgical intervention, and 2 patients (10%) underwent combined endoscopic and surgical treatment. After careful evaluation of clinical status, laboratory and imaging work-up, 2 patients (10%) were observed with conservative management and had spontaneous resolution despite clinical and radiological signs of ERCP associated perforation.
Twelve patients (60%) were admitted to intensive care unit (ICU) due to the ERCP associated perforation for a median time of 6 days. For 5 patients (25%) ERCP associated perforation resulted in death. For all of the patients with lethal outcomes of ERCP associated perforations primary treatment modality of perforation closure was unsuccessful (5, 100%). Details of patient specific characteristics regarding clinical course of ERCP associated perforation, diagnostic pathway and outcomes are provided in Table 1.
| Patient | Localization of the perforation1 | Perforation type according to Stapfer | Imaging performed | Modality of imaging confirming perforation | Primary treatment, effectiveness | Surgery performed | Hospitalization in ICU | Clavien-Dindo grade | Hospitalization time (days) |
| 1 | 3 | 1 | Endoscopic, yes | + | 3b | 13 | |||
| 2 | 2 | 3 | Endoscopic, no | Laparotomy | + | 3b | 33 | ||
| 3 | 3 | 1 | + | CT | Surgery, no | Laparotomy | + | 5 | 5 |
| 4 | 3 | 4 | + | CT | Observation, yes | 1 | 9 | ||
| 5 | 1 | 3 | + | CT | Endoscopic, no | + | 5 | 4 | |
| 6 | 1 | 3 | + | CT | Endoscopic + surgical, no | Laparoscopy | + | 5 | 26 |
| 7 | 1 | 4 | + | Ultrasound | Observation, yes | 3b | 17 | ||
| 8 | 3 | 1 | + | CT | Surgery, no | Laparotomy | + | 5 | 5 |
| 9 | 2 | 3 | + | CT | Endoscopic, no | Laparotomy | + | 4b | 32 |
| 10 | 1 | 3 | + | Ultrasound | Endoscopic, no | Laparoscopy | + | 3b | 70 |
| 11 | 1 | 3 | + | CT | Endoscopic, yes | + | 3b | 24 | |
| 12 | 3 | 2 | + | CT | Endoscopic, no | Laparotomy | + | 5 | 8 |
| 13 | 2 | 3 | Endoscopic, yes | 1 | 13 | ||||
| 14 | 3 | 1 | + | Ultrasound | Surgery, yes | Laparotomy | 3b | 20 | |
| 15 | 3 | 3 | Endoscopic, yes | 2 | 23 | ||||
| 16 | 3 | 1 | + | Ultrasound | Endoscopic, yes | 3b | 15 | ||
| 17 | 1 | 2 | Endoscopic, yes | 1 | 7 | ||||
| 18 | 1 | 2 | Endoscopic, yes | 3b | 5 | ||||
| 19 | 3 | 1 | + | CT | Endosopic + surgical, yes | Laparotomy | + | 3b | 168 |
| 20 | 1 | 3 | + | Ultrasound | Surgery, yes | Laparotomy | + | 3b | 22 |
One instance of an immediate identification and successful primary endoscopic closure of an ERCP associated perforation is the case of patient N1, a 76-year-old male, who underwent an ERCP for choledocholithiasis. During the procedure, multiple common bile duct (CBD) stones and a suspected distal CBD stricture were visualized. After performing sphincterotomy, balloon dilation of the distal part of CBD was carried out. After extracting the majority of CBD stones with Dormia basket, mechanical lithotripsy for the remaining impacted stone was attempted. A perforation in the second part of duodenum occurred during mechanical lithotripsy and was successfully clipped with 3 endoscopic clips. A 12Fr plastic biliary stent was placed for the possible distal CBD stricture.
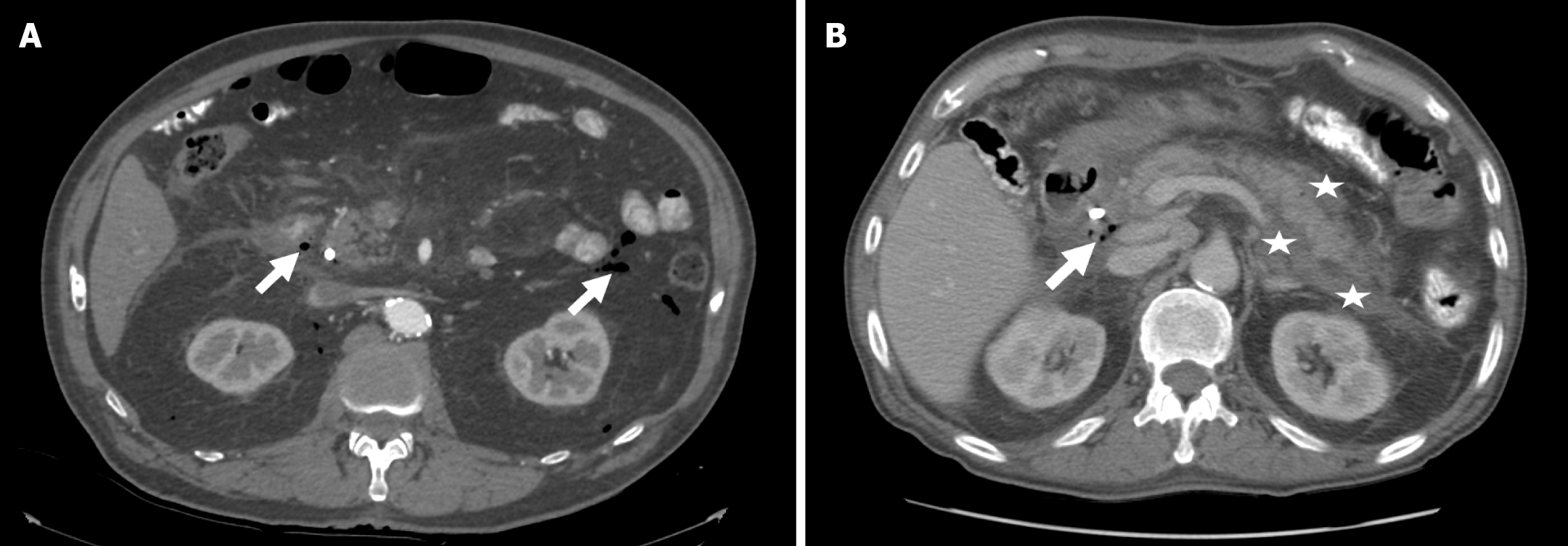
The patient was admitted to ICU for observation and conservative management. One day after the procedure a contrast-enhanced CT showed minor amount of free air in the retroperitoneal space with no further complications (Figure 2A). 3 days after the initial procedure the patient underwent a second look ERCP that showed adequate closure of the perforation and an enteral tube below the perforation was placed for enteral nutrition.
The patient was discharged 12 days after the initial procedure with no further complications. After two months a follow-up ERCP with biliary stent removal was performed, showing no signs of a CBD stricture. The patient underwent a cholecystectomy with no further biliary complications for the remainder of the follow-up.
A much less straightforward diagnostic pathway and complex management of ERCP associated perforation is evident considering patient N15, a 71-year-old male with a history of gallbladder carcinoma, cholecystectomy and liver resection, who underwent an ERCP for suspected mechanical cholestasis due to lymphadenopathy. During the procedure an opacity defect in bifurcation region was identified with a slight dilation of the left hepatic duct. A sphincterotomy was performed and a plastic biliary stent in the left hepatic duct above the bifurcation was placed.
In the post-procedural period, the patient remained in pain, laboratory workup revealed elevation of α-amylase activity in the serum and post-ERCP pancreatitis was diagnosed.
Two days after the procedure a contrast-enhanced CT was performed that showed malignant hilar infiltration, intrahepatic cholestasis, and perihilar free fluid and air (Figure 2B).
Given the poor prognosis of an advanced malignant disease and no evidence of peritonitis, conservative treatment with broad-spectrum antibiotics, enteral nutrition via duodenal tube was commenced. Due to persistent elevation of inflammatory markers and intermittent febrility, 2 weeks after the initial ERCP the patient underwent a second contrast-enhanced CT. CT revealed multiple minute cystic lesions on the left liver lobe and peripancreatic infiltration. It was decided to continue with a conservative treatment, and the antibiotic therapy was escalated. In a course of one week the patient became afebrile, jaundice and inflammatory markers decreased. The patient was discharged 22 days after the index ERCP for palliative care and lost to follow-up.
Our analysis into a high-volume center’s prospectively collected database regarding ERCP associated perforations provides additional evidence with respect to incidence, diagnosis, management and outcomes of a rare, although potentially lethal procedural complication.
Our observed incidence of ERCP related perforations (0.75%) is well within the reported bounds as low as 0.39% in a meta-analysis of 142847 patients by Bishay et al[1] to as high as 0.9% reported in a study by Bray et al[10]. The varying data of the reported incidence of ERCP associated perforations might arise due to differing numbers of ERCP performed in centers, as procedural volume is directly linked to the ERCP related complications[13]. However, the annual ERCP volume and resulting ERCP associated perforations rate remained similar during the duration of the study. Considering our results, it should also be taken into account that only ERCP procedures resulting in biliary stenting were analyzed and the incidence of ERCP associated perforations in an overall cohort might be lower and all patients had at least one risk factor for ERCP associated perforation[14].
In half of the patients in our study (n = 10, 50%) ERCP associated perforation was diagnosed in the first 24 hours after the index procedure and in 4 (20%) after 24 hours with the main complaint being severe abdominal pain prompting further diagnostic workup.
Although the preferred modality for diagnosis of ERCP associated perforation is CT scan with peroral contrast due to the highest sensitivity and specificity[15,16], interestingly, in our cohort, in 20% of the patients, ERCP associated perforation was diagnosed definitively by the means of ultrasound prompting emergency surgery without further imaging studies. The reported ultrasound features of suspected perforation were free fluid or air around duodenal wall, periduodenal fat stranding. This underlines the importance of operator-dependent expertise to detect free air in the abdominal cavity utilizing widely available and fast imaging modality.
In our cohort of patients, the most common type of perforation was type III (distal bile duct) according to Stapfer (n = 9). This is in contrast to the published data reporting type II ERCP associated perforations (periampullary, sphincterotomy-related) to be the most common type. A pooled analysis of 562 perforations by Vezakis et al[17] reported the incidence of II type perforations to be as high as 46% and a systematic review of 14045 ERCPs by Bill et al[18] reported the incidence of type II perforations to be 38.1%[18]. This could be explained by a long-standing tradition in our center to initiate treatment even of perihilar (Bismuth-Corlette type III and IV) mechanical obstruction by endoscopic means resulting in more difficult biliary access, hence, more perforations in biliary tract. Another explanation could be the repeated use of guidewires that become stiffer after the process of sterilization.
Interestingly, for 2 patients (10%), close clinical observation, repeated laboratory work-up and imaging was successful management plan that helped to avoid unnecessary interventional procedures. It could be hypothesized that diagnosis of perforation could have resulted from false-negative imaging findings when during an ERCP procedure air bubbles can sometimes move intramuscularly and simulate signs of perforation. However, both patients were symptomatic with mildly elevated inflammatory markers. Due to no overt signs of peritonitis, overall condition of the patients, cautious observation and treatment with broad-spectrum antibiotics, fasting and intravenous fluids was the chosen management approach. This is in accordance with The American Society for Gastrointestinal Endoscopy recommendations for initial conservative management for ERCP associated perforations without peritoneal signs or systemic inflammatory response[19]. In carefully selected cases of ERCP associated perforations, close clinical observation and repeated evaluation helps to prevent unnecessary interventional procedures, early surgery and associated complications[20]. The importance of careful management plan has been proposed and assessed by Kumbhari et al[21], suggesting diagnostic and management algorithm in cases of Stapfer I and Stapfer II perforations. According to the findings of the study, out of 55 patients with postprocedural diagnosis of Stapfer II type perforation, only 4 patients (7%) failed medical management and required surgery, underpinning the importance of careful evaluation of clinical symptoms and evidence of systemic inflammation to avoid needless and potentially harmful interventions.
All of the patients with perforations diagnosed intra-procedurally were successfully treated with endoscopic means and later discharged concurring with the results of a large multicenter study by Emori et al[6], emphasizing the importance of early detection and minimally invasive treatment options for better outcomes. In our study successful closure of a perforation was performed by the means of either clipping or placing a plastic biliary stent depending on perforation type. Unfortunately, for 7 patients (35%) the primary endoscopic closure was unsuccessful, and patients were referred to surgery. During the period of our study newer modalities for perforation closure, such as over-the-scope clips and fully-covered metal stents were unavailable. Based on the recent evidence, it is reasonable to hypothesize, that having more advanced modalities for perforation closure could have led to better outcomes[22,23].
Unfortunately, 5 (25%) patients with ERCP associated perforations in our cohort had lethal outcomes. This is congruent to the reported data from the studies carried out in similar time frame such as Swedish GallRiks study (52140 ERCPs, 0.72% of perforations, 20% mortality)[7]. Recent studies, such as Emori et al[6], report mortality rate as low as 2%, that might be explained by the advances in minimally invasive treatment modalities, such as over-the-scope clips.
There are several limitations to our study. Firstly, due to the nature of retrospective analysis of the collected database some important factors, pertinent to the patient management and outcomes might have been not accounted for. Secondly, due to the rarity of ERCP associated perforations, only 20 patients encountering this complication, clinical course was analyzed. However, we believe that detailed overview of diagnostic and management pathways provides additional and beneficial knowledge to clinical practice.
ERCP associated perforation is a rare but potentially fatal procedural complication, necessitating prompt diagnosis, thorough workup and a multidisciplinary management plan. Emerging endoscopic management modalities provide possibilities for more efficacious intra-procedural treatment and careful post-procedural evaluation in cases of suspected ERCP associated perforations with multidisciplinary approach lead to better patient outcomes.
| 1. | Bishay K, Meng ZW, Khan R, Gupta M, Ruan Y, Vaska M, Iannuzzi J, O'Sullivan DE, Mah B, Partridge ACR, Henderson AM, Guo H, Samnani S, DeMarco M, Yuan Y, Elmunzer BJ, Keswani RN, Wani S, Smith ZL, Bridges RJ, Heitman SJ, Hilsden RJ, Brenner DR, Leontiadis GI, Forbes N. Adverse Events Associated With Endoscopic Retrograde Cholangiopancreatography: Systematic Review and Meta-Analysis. Gastroenterology. 2025;168:568-586. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 43] [Article Influence: 43.0] [Reference Citation Analysis (1)] |
| 2. | Cotton PB, Garrow DA, Gallagher J, Romagnuolo J. Risk factors for complications after ERCP: a multivariate analysis of 11,497 procedures over 12 years. Gastrointest Endosc. 2009;70:80-88. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 563] [Cited by in RCA: 476] [Article Influence: 28.0] [Reference Citation Analysis (7)] |
| 3. | Masci E, Toti G, Mariani A, Curioni S, Lomazzi A, Dinelli M, Minoli G, Crosta C, Comin U, Fertitta A, Prada A, Passoni GR, Testoni PA. Complications of diagnostic and therapeutic ERCP: a prospective multicenter study. Am J Gastroenterol. 2001;96:417-423. [PubMed] [DOI] [Full Text] |
| 4. | Andriulli A, Loperfido S, Napolitano G, Niro G, Valvano MR, Spirito F, Pilotto A, Forlano R. Incidence rates of post-ERCP complications: a systematic survey of prospective studies. Am J Gastroenterol. 2007;102:1781-1788. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 904] [Cited by in RCA: 788] [Article Influence: 41.5] [Reference Citation Analysis (6)] |
| 5. | Kochar B, Akshintala VS, Afghani E, Elmunzer BJ, Kim KJ, Lennon AM, Khashab MA, Kalloo AN, Singh VK. Incidence, severity, and mortality of post-ERCP pancreatitis: a systematic review by using randomized, controlled trials. Gastrointest Endosc. 2015;81:143-149.e9. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 430] [Cited by in RCA: 361] [Article Influence: 32.8] [Reference Citation Analysis (3)] |
| 6. | Emori T, Yamasaki T, Itonaga M, Bamba S, Kitagawa K, Maruyama H, Ueyama S, Fujita K, Doi T, Iemoto T, Shiomi H, Sawai Y, Ogura T, Shimatani M, Nakanishi F, Uza N, Uenoyama Y, Asai S, Mandai K, Azuma S, Kitano M, Takenaka M. Management of ERCP-related perforation: a large multicenter study. Gastrointest Endosc. 2025;102:97-105.e3. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 7] [Article Influence: 7.0] [Reference Citation Analysis (1)] |
| 7. | Langerth A, Isaksson B, Karlson BM, Urdzik J, Linder S. ERCP-related perforations: a population-based study of incidence, mortality, and risk factors. Surg Endosc. 2020;34:1939-1947. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 35] [Article Influence: 5.0] [Reference Citation Analysis (2)] |
| 8. | Weiser R, Pencovich N, Mlynarsky L, Berliner-Senderey A, Lahat G, Santo E, Klausner JM, Nachmany I. Management of endoscopic retrograde cholangiopancreatography-related perforations: Experience of a tertiary center. Surgery. 2017;161:920-929. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 19] [Article Influence: 2.1] [Reference Citation Analysis (1)] |
| 9. | A Al Manasra ARA, Mesmar Z, Manasreh T, Hammouri HM, Husein A, Jadallah K, Bani Hani M, Abu Farsakh N, K Shahwan S, Al-Qaoud D, Fataftah J. ERCP-induced perforation: review and revisit after half a century. F1000Res. 2023;12:612. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 10. | Bray MS, Borgert AJ, Folkers ME, Kothari SN. Outcome and management of endoscopic retrograde cholangiopancreatography perforations: A community perspective. Am J Surg. 2017;214:69-73. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 17] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 11. | Stapfer M, Selby RR, Stain SC, Katkhouda N, Parekh D, Jabbour N, Garry D. Management of duodenal perforation after endoscopic retrograde cholangiopancreatography and sphincterotomy. Ann Surg. 2000;232:191-198. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 326] [Cited by in RCA: 250] [Article Influence: 9.6] [Reference Citation Analysis (2)] |
| 12. | Shi D, Guo S, Bao Y, Wang Q, Pan W. Diagnosis and management of type II endoscopic retrograde cholangiopancreatography-related perforations: a multicenter retrospective study. BMC Gastroenterol. 2024;24:241. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 13. | Dumonceau JM, Kapral C, Aabakken L, Papanikolaou IS, Tringali A, Vanbiervliet G, Beyna T, Dinis-Ribeiro M, Hritz I, Mariani A, Paspatis G, Radaelli F, Lakhtakia S, Veitch AM, van Hooft JE. ERCP-related adverse events: European Society of Gastrointestinal Endoscopy (ESGE) Guideline. Endoscopy. 2020;52:127-149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 729] [Cited by in RCA: 629] [Article Influence: 104.8] [Reference Citation Analysis (5)] |
| 14. | Enns R, Eloubeidi MA, Mergener K, Jowell PS, Branch MS, Pappas TM, Baillie J. ERCP-related perforations: risk factors and management. Endoscopy. 2002;34:293-298. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 228] [Cited by in RCA: 175] [Article Influence: 7.3] [Reference Citation Analysis (2)] |
| 15. | Avgerinos DV, Llaguna OH, Lo AY, Voli J, Leitman IM. Management of endoscopic retrograde cholangiopancreatography: related duodenal perforations. Surg Endosc. 2009;23:833-838. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 85] [Cited by in RCA: 60] [Article Influence: 3.5] [Reference Citation Analysis (1)] |
| 16. | Morgan KA, Fontenot BB, Ruddy JM, Mickey S, Adams DB. Endoscopic retrograde cholangiopancreatography gut perforations: when to wait! When to operate! Am Surg. 2009;75:477-483; discussion 483. [PubMed] |
| 17. | Vezakis A, Fragulidis G, Polydorou A. Endoscopic retrograde cholangiopancreatography-related perforations: Diagnosis and management. World J Gastrointest Endosc. 2015;7:1135-1141. [PubMed] [DOI] [Full Text] |
| 18. | Bill JG, Smith Z, Brancheck J, Elsner J, Hobbs P, Lang GD, Early DS, Das K, Hollander T, Doyle MBM, Fields RC, Hawkins WG, Strasberg SM, Hammill C, Chapman WC, Edmundowicz S, Mullady DK, Kushnir VM. The importance of early recognition in management of ERCP-related perforations. Surg Endosc. 2018;32:4841-4849. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 17] [Article Influence: 2.1] [Reference Citation Analysis (1)] |
| 19. | ASGE Standards of Practice Committee; Chandrasekhara V, Khashab MA, Muthusamy VR, Acosta RD, Agrawal D, Bruining DH, Eloubeidi MA, Fanelli RD, Faulx AL, Gurudu SR, Kothari S, Lightdale JR, Qumseya BJ, Shaukat A, Wang A, Wani SB, Yang J, DeWitt JM. Adverse events associated with ERCP. Gastrointest Endosc. 2017;85:32-47. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 703] [Cited by in RCA: 606] [Article Influence: 67.3] [Reference Citation Analysis (6)] |
| 20. | Plecic N, Malenkovic A, Begovic A, Pavlovic A, Bulajic M, Bulajic M, Đukic V, Milanovic M, Savic P, Panic N. Management of ERCP-Related Perforations: A Single-Center Experience. J Clin Med. 2024;14:1. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 21. | Kumbhari V, Sinha A, Reddy A, Afghani E, Cotsalas D, Patel YA, Storm AC, Khashab MA, Kalloo AN, Singh VK. Algorithm for the management of ERCP-related perforations. Gastrointest Endosc. 2016;83:934-943. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 47] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 22. | Saeed A, Yousuf S, Zain A, Imran H, Tariq M, Fazal MI, Shah J, Radlinski M, Gamboa A, Xiao Y, Kumar A, Schlachterman A, Kowalski T, Adler DG, Kamal F. Efficacy of fully covered self-expandable metal stents and comparison with conventional management for ERCP-related type II perforations: a systematic review and meta-analysis. Gastrointest Endosc. 2025;102:738-742.e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 6.0] [Reference Citation Analysis (1)] |
| 23. | Iwasa Y, Iwashita T, Uemura S, Mita N, Iwata K, Yoshida K, Mukai T, Yasuda I, Shimizu M. The Efficacy of Over-the-Scope Clip Closure for Gastrointestinal Iatrogenic Perforation During Endoscopic Ultrasound and Endoscopic Retrograde Cholangiopancreatography for Pancreaticobiliary Diseases. Surg Laparosc Endosc Percutan Tech. 2020;30:257-262. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (4)] |