Copyright: ©Author(s) 2026.
World J Gastrointest Endosc. May 16, 2026; 18(5): 119587
Published online May 16, 2026. doi: 10.4253/wjge.v18.i5.119587
Published online May 16, 2026. doi: 10.4253/wjge.v18.i5.119587
Figure 1 Gadgets used during Endoscopic retrograde cholangiopancreatography to dilate the strictures.
A: Soehendra dilators of various sizes; B: Biliary dilatation balloons of various sizes.
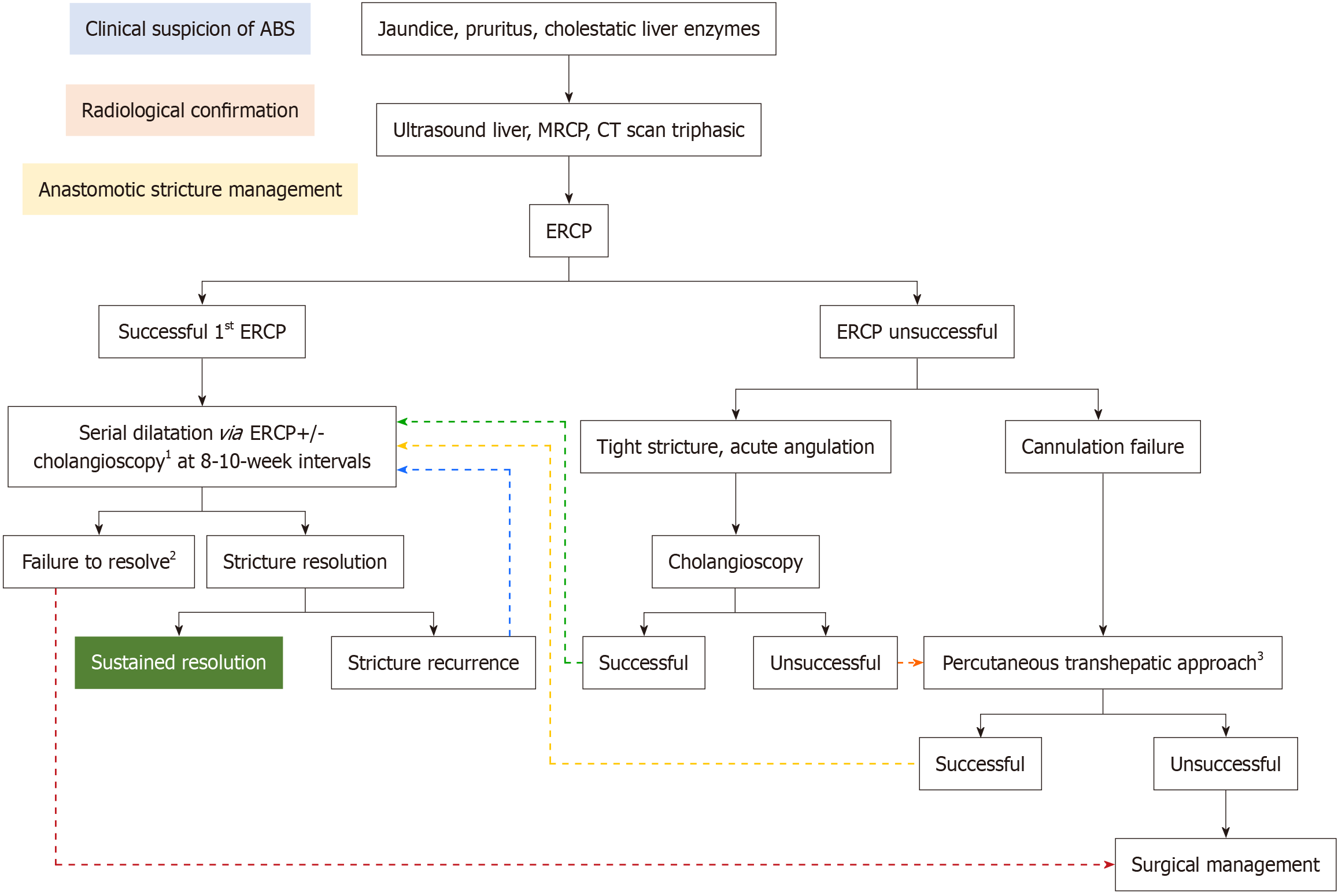
Figure 2 Management algorithm for anastomotic biliary strictures.
1Cholangioscopy was utilized to facilitate traversal of acutely angulated strictures, enable drainage of sectoral branches, and confirm stricture resolution. 2Failure of stricture resolution was defined as the persistence of the stricture despite 12 months of endoscopic therapy. 3Percutaneous transhepatic cholangiography was employed in cases where primary endoscopic retrograde cholangiopancreatography or cholangioscopy failed, as well as for sectoral duct strictures that were not amenable to endoscopic management. ABS: Anastomotic biliary strictures; ERCP: Endoscopic retrograde cholangiopancreatography.
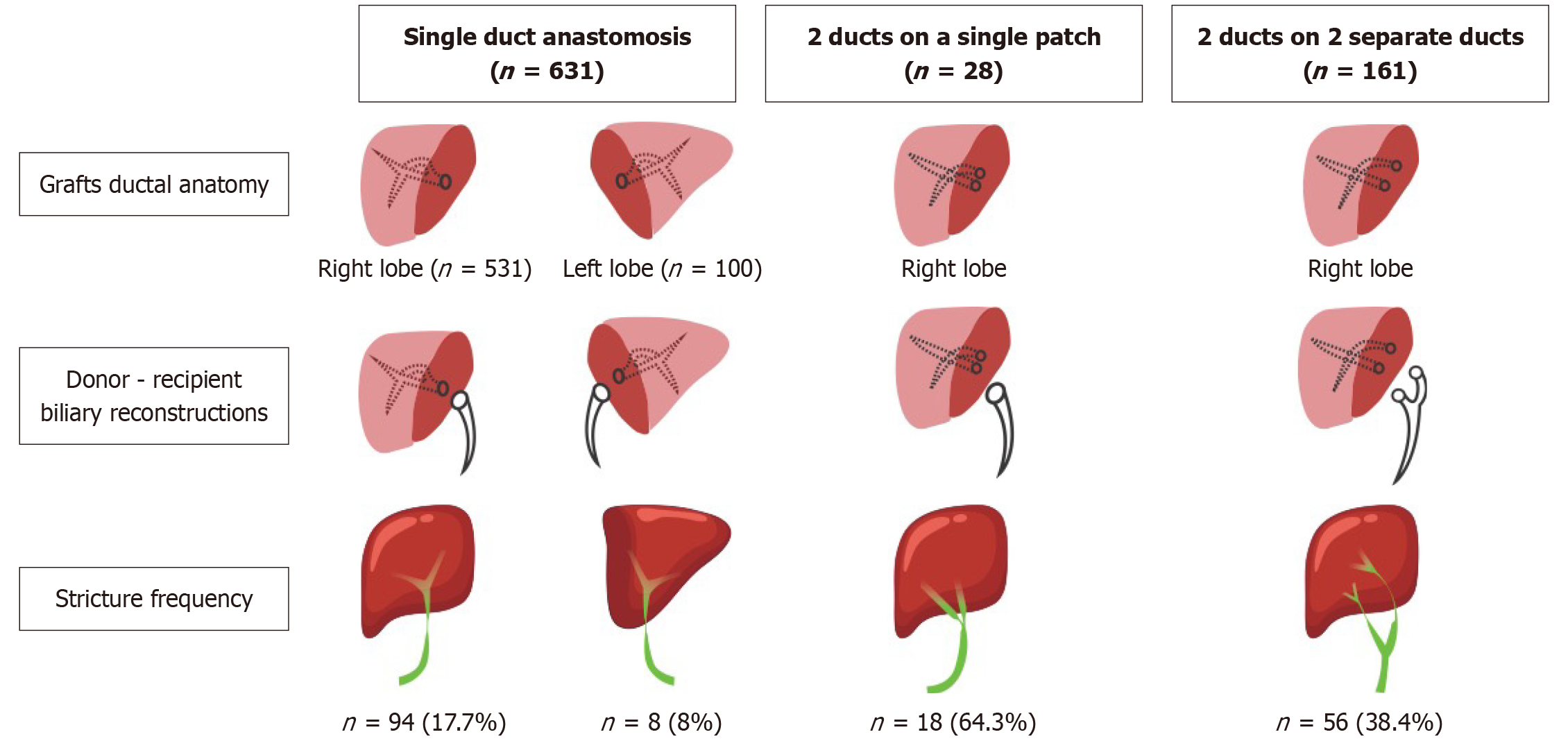
Figure 3 Incidence of biliary strictures across different reconstruction techniques.
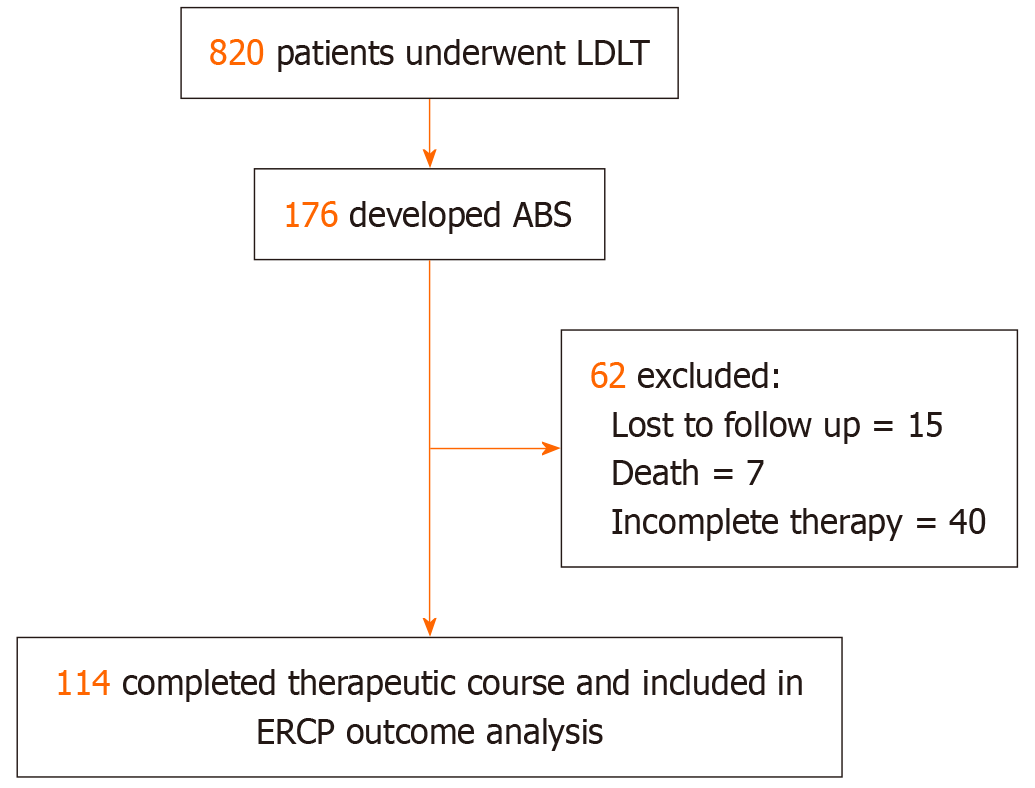
Figure 4 Participant flow diagram.
LDLT: Living donor liver transplantation; ABS: Anastomotic biliary strictures; ERCP: Endoscopic retrograde cholangiopancreatography.
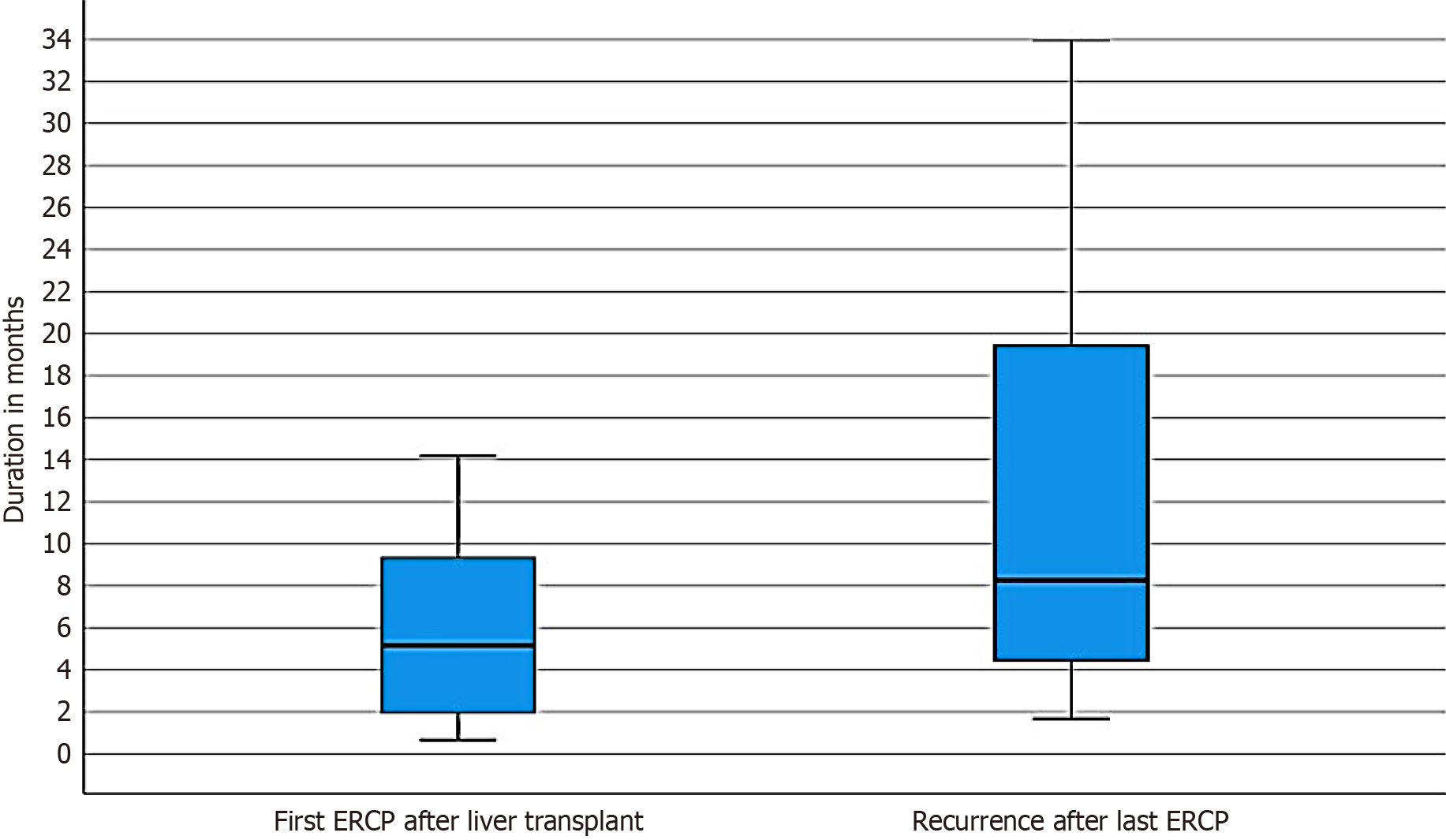
Figure 5 Timelines between liver transplant to first endoscopic retrograde cholangiopancreatigraphy and post-resolution stricture recurrence.
ERCP: Endoscopic retrograde cholangiopancreatography.
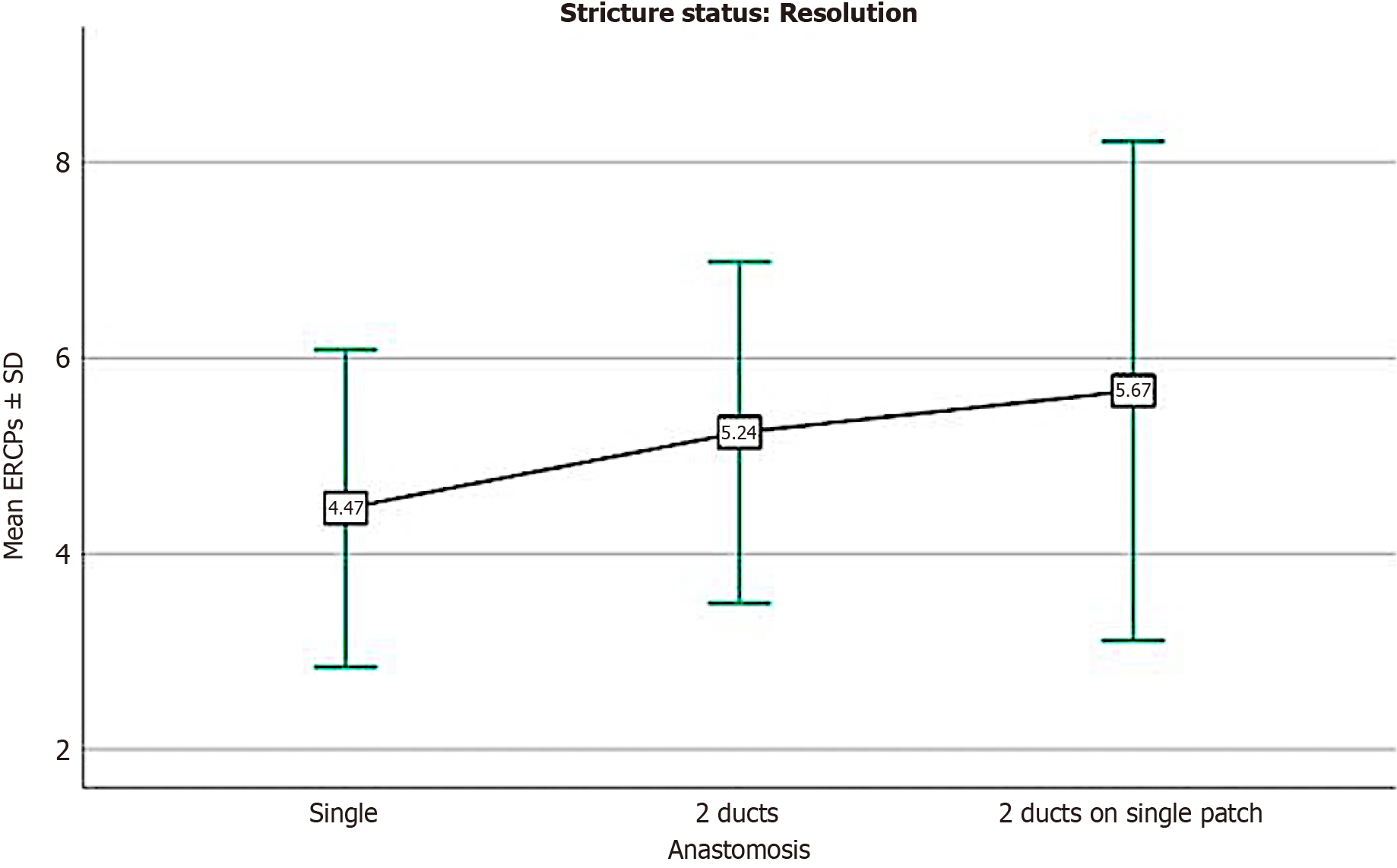
Figure 6 Comparison of endoscopic retrograde cholangiopancreatography sessions required to achieve resolution for various types of biliary reconstructions.
ERCP: Endoscopic retrograde cholangiopancreatography.
- Citation: Aujla UI, Syed IA, Malik AK, Khan MMZ, Rafi K, Dar FS. Endoscopic management of post-living donor liver transplant anastomotic biliary strictures: A quaternary care transplant center experience. World J Gastrointest Endosc 2026; 18(5): 119587
- URL: https://www.wjgnet.com/1948-5190/full/v18/i5/119587.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i5.119587