©The Author(s) 2023.
World J Stem Cells. Jul 26, 2023; 15(7): 687-700
Published online Jul 26, 2023. doi: 10.4252/wjsc.v15.i7.687
Published online Jul 26, 2023. doi: 10.4252/wjsc.v15.i7.687
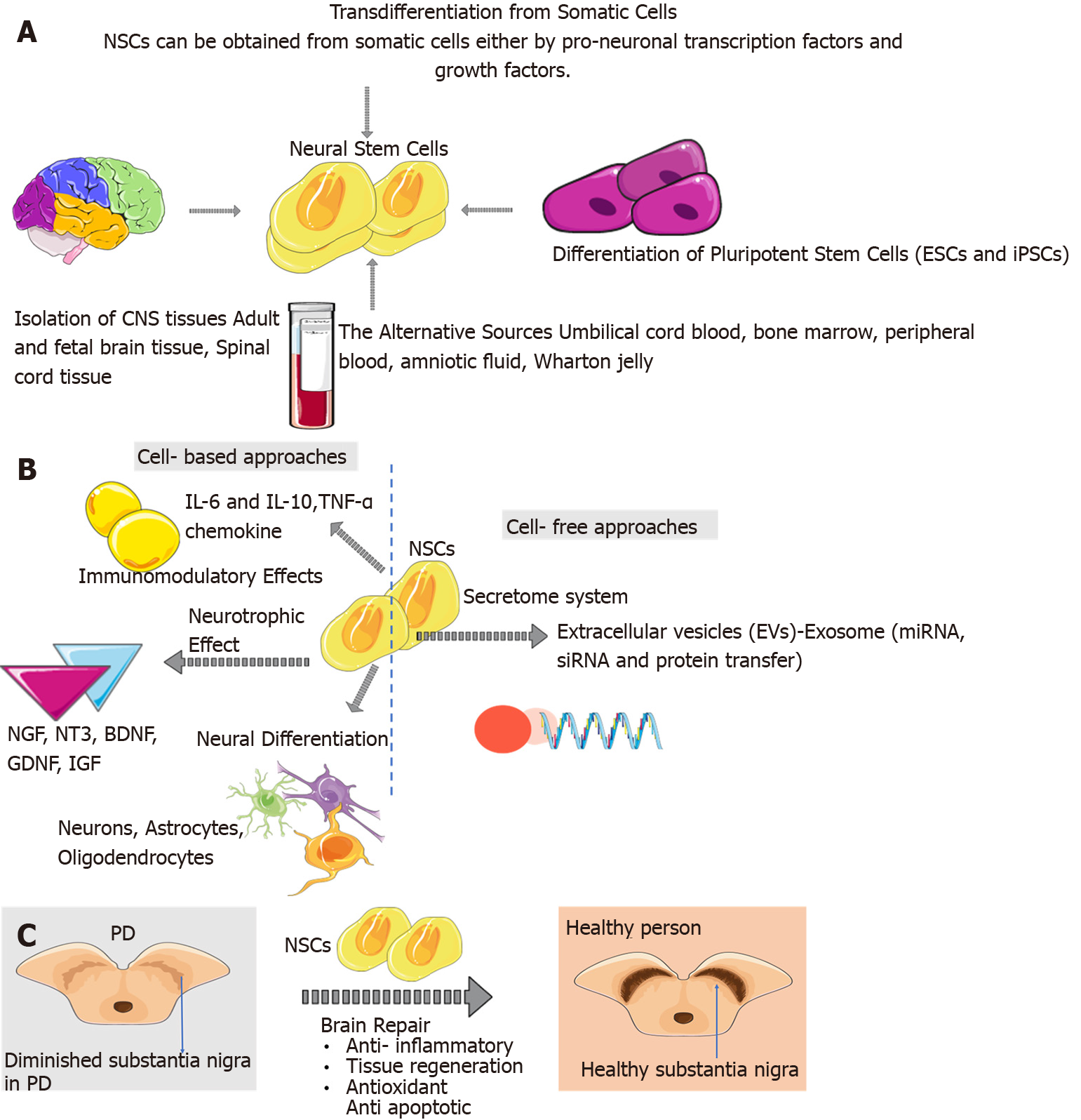
Figure 1 Emergence of neural stem cells in the adult brain and alternative sources of neural stem cells.
A: The sources of neural stem cells (NSCs) are embryonic stem cells and induced pluripotent stem cells, adult/foetal brain tissue and spinal cord tissue. Also, NSCs can be obtained from somatic cells either by transcription factors and growth factors. The alternative sources of NSCs are foetal and adult nervous systems, umbilical cord blood, bone marrow, peripheral blood, amniotic fluid, Wharton jelly; B: NSCs can have immunomodulatory effects such as cytokine, chemokines, and chemokine receptors secretion and T cell proliferation inhibition. NSCs can have neurotrophic effects such as nerve growth factor, neurotrophin-3, brain-derived neurotrophic factor, and glial cell line-derived neurotrophic factor. NSCs can target secretome and paracrine effects via extracellular vesicles like exosomes. Also, NSCs play a role in neural differentiation; C: NSCs after their transplantation, could migrate, survive, and proliferate in specific brain sites. And NSCs play a role in brain repair mechanisms such as antiapoptotic, anti-inflammatory, and antioxidant. CNS: Central nervous system; BDNF: Brain-derived neurotrophic factor; ESCs: Embryonic stem cells; EVs: Extracellular vesicles; GDNF: Glial cell line-derived neurotrophic factor; iPSCs: Induced pluripotent stem cells; NGF: Nerve growth factor; NT-3: Neurotrophin-3; NSCs: Neural stem cells; TFs: Transcription factors; PD: Parkinson’s disease; TGF: Transforming growth factor. Citation: The parts of the figures were drawn using pictures from Servier Medical Art. Servier Medical Art by Servier is licensed under a Creative Commons Attribution 3.0 Unported License (https://creativecommons.org/Licenses/by/3.0/).
Figure 2 Application of nanomaterials in stem cell therapy of Parkinson’s disease.
Preoperative preparation: Nanomaterials, with their small size, unique physicochemical properties, and capability for surface functionalisation, offer the potential for designed manipulating cell behaviour. A promising strategy is that fabricating the extracellular matrix with biocompatible nanomaterial-based scaffolds with topology simulating the microenvironment. Preoperative phase: nanomaterials capable of suppressing oxidative stress, neuroinflammation, and toxic protein aggregation can act as bioactive nanomedicines addressing the limitations of cell-based therapy for Parkinson’s disease. Moreover, “intelligent” nano-drug delivery systems functionalised by targeting ligands with the controlled release of loaded molecules like growth factor aims to support and expand stem cells for brain repair. At the postoperative stage, nanomaterials, with their unique optical properties, cellular uptake, surface functionalisation, and good biocompatibility, are promising candidates for cell tracking and imaging. MRI: Magnetic resonance imaging. Citation: The parts of the figures were drawn using pictures from Servier Medical Art. Servier Medical Art by Servier is licensed under a Creative Commons Attribution 3.0 Unported License (https://creativecommons.org/Licenses/by/3.0/).
- Citation: Oz T, Kaushik A, Kujawska M. Neural stem cells for Parkinson’s disease management: Challenges, nanobased support, and prospects. World J Stem Cells 2023; 15(7): 687-700
- URL: https://www.wjgnet.com/1948-0210/full/v15/i7/687.htm
- DOI: https://dx.doi.org/10.4252/wjsc.v15.i7.687