Copyright: ©Author(s) 2026.
World J Gastroenterol. Apr 14, 2026; 32(14): 116415
Published online Apr 14, 2026. doi: 10.3748/wjg.v32.i14.116415
Published online Apr 14, 2026. doi: 10.3748/wjg.v32.i14.116415
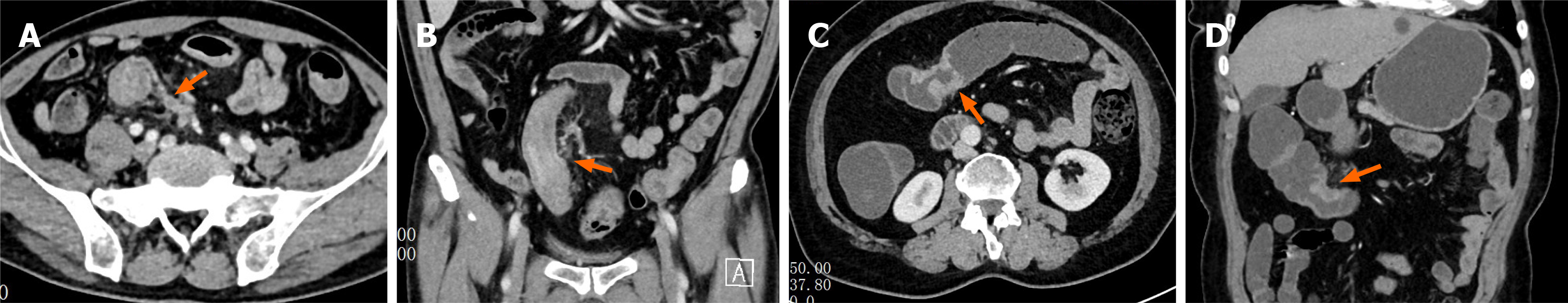
Figure 1 Computed tomography-detected extramural vascular invasion assessment of colon cancer patients.
A: Venous-phase axial computed tomography (CT) image demonstrates focal thickening of the sigmoid colon wall with blurred surrounding fat planes, enlarged adjacent extramural vessels with irregular contours, and intraluminal filling defects (arrow); B: Corresponding venous-phase coronal reconstructed image shows marked thickening of the sigmoid colon wall (arrow) and dilated, irregular extramural vessels containing intraluminal filling defects, consistent with CT-detected extramural vascular invasion-positive findings; C: Venous-phase axial CT image shows thickening of the transverse colon wall (arrow) with preserved surrounding fat planes; D: Corresponding venous-phase coronal reconstructed image demonstrates wall thickening of the transverse colon (arrow) without enlargement or irregularity of adjacent extramural vessels and without abnormal intraluminal density, consistent with CT-detected extramural vascular invasion-negative findings.
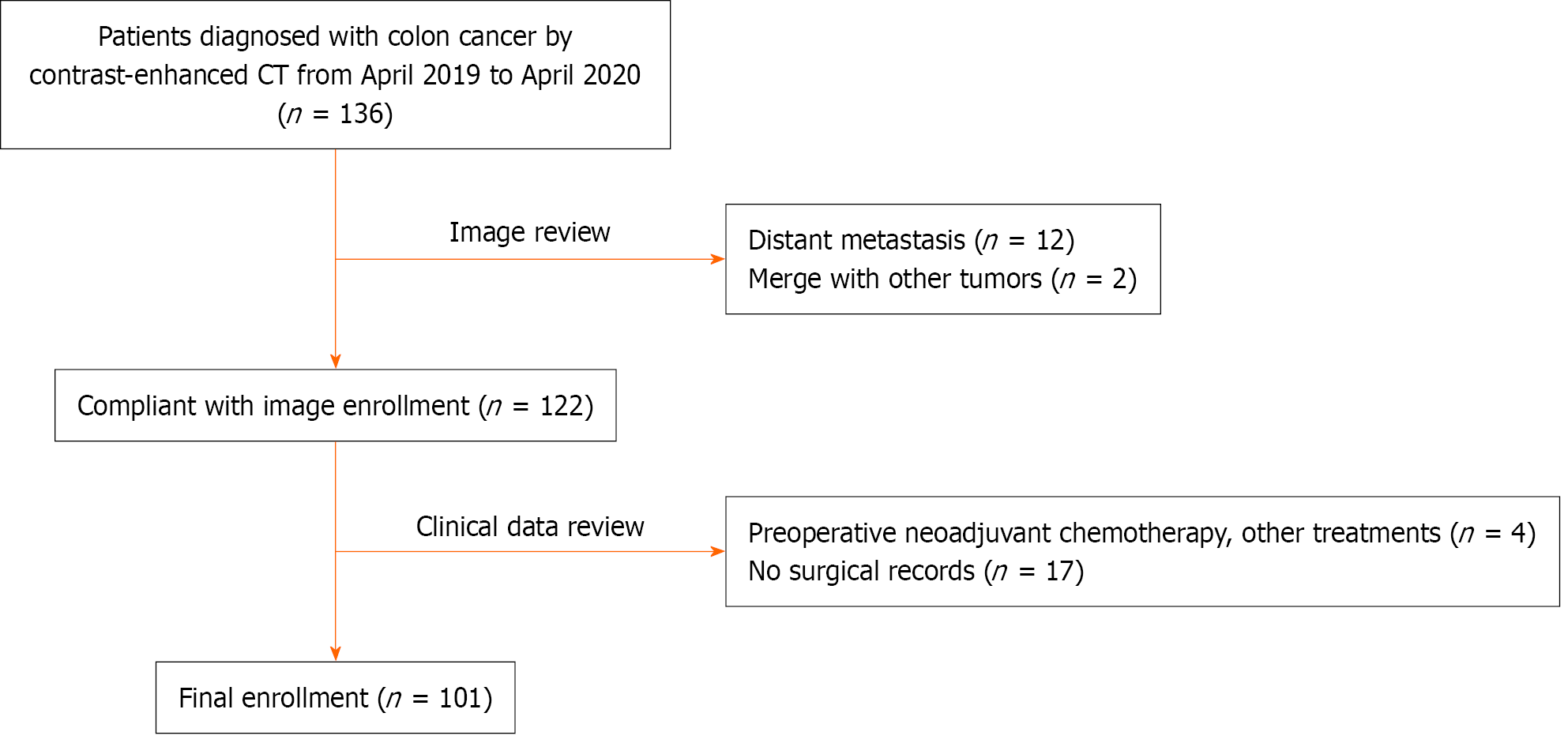
Figure 2 Selection processes for included patients.
CT: Computed tomography.
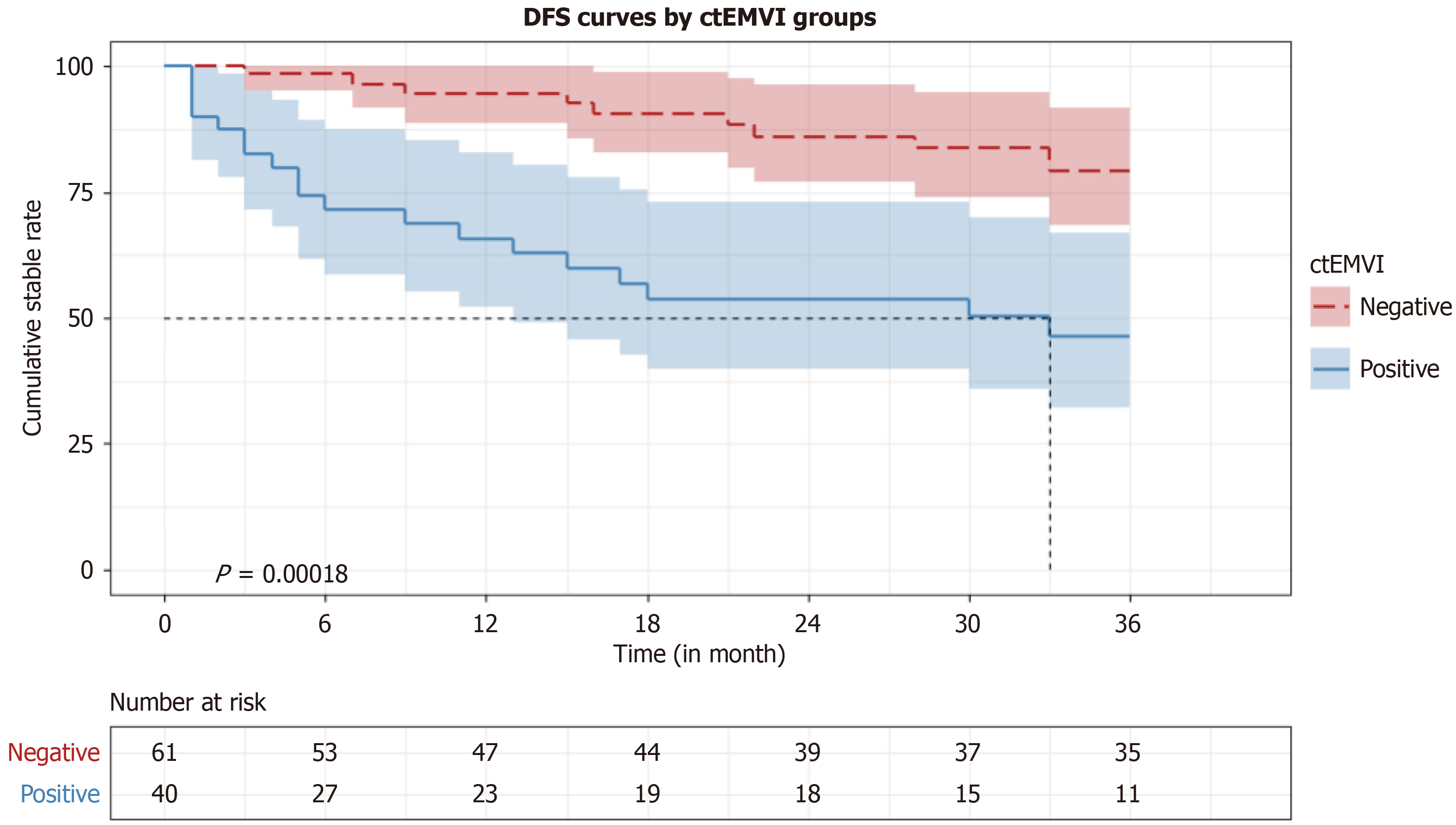
Figure 3 Kaplan-Meier survival curve for disease-free survival.
According to the Kaplan-Meier survival curve, the disease-free survival rate in the computed tomography-detected extramural vascular invasion -positive group was lower than that in the computed tomography-detected extramural vascular invasion-negative group (χ² = 13.991, P = 0.00018). ctEMVI: Computed tomography-detected extramural vascular invasion; DFS: Disease-free survival.
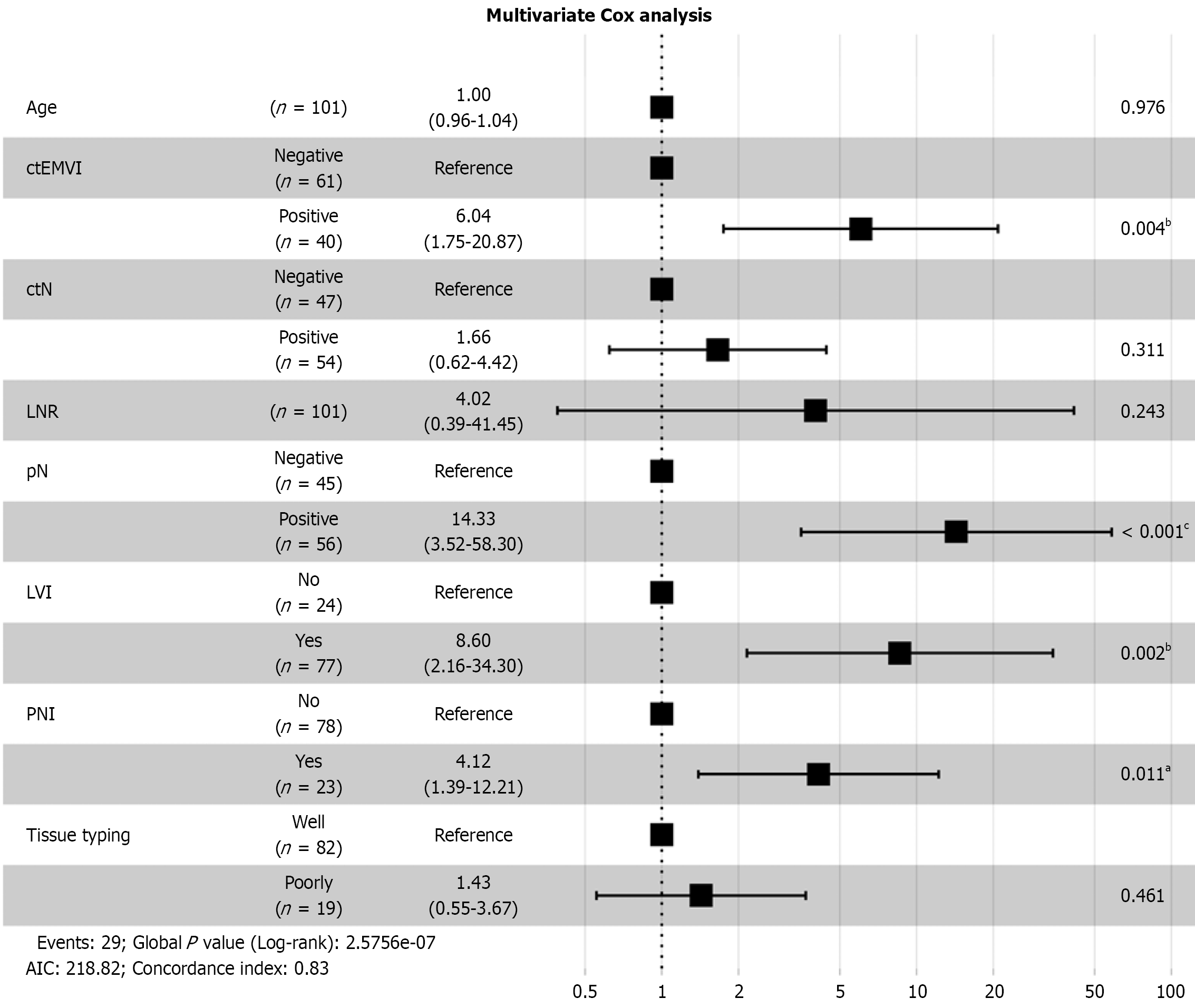
Figure 4 Forest plot of the multi-Cox regression analysis.
aP < 0.05, bP < 0.01, cP < 0.001. AIC: Akaike information criterion; ctEMVI: Computed tomography-detected extramural vascular invasion; ctN: Lymph node status determined by computed tomography; LNR: Lymph node ratio; LVI: Lymphovascular invasion; pN: Pathological nodal status; PNI: Perineural invasion.
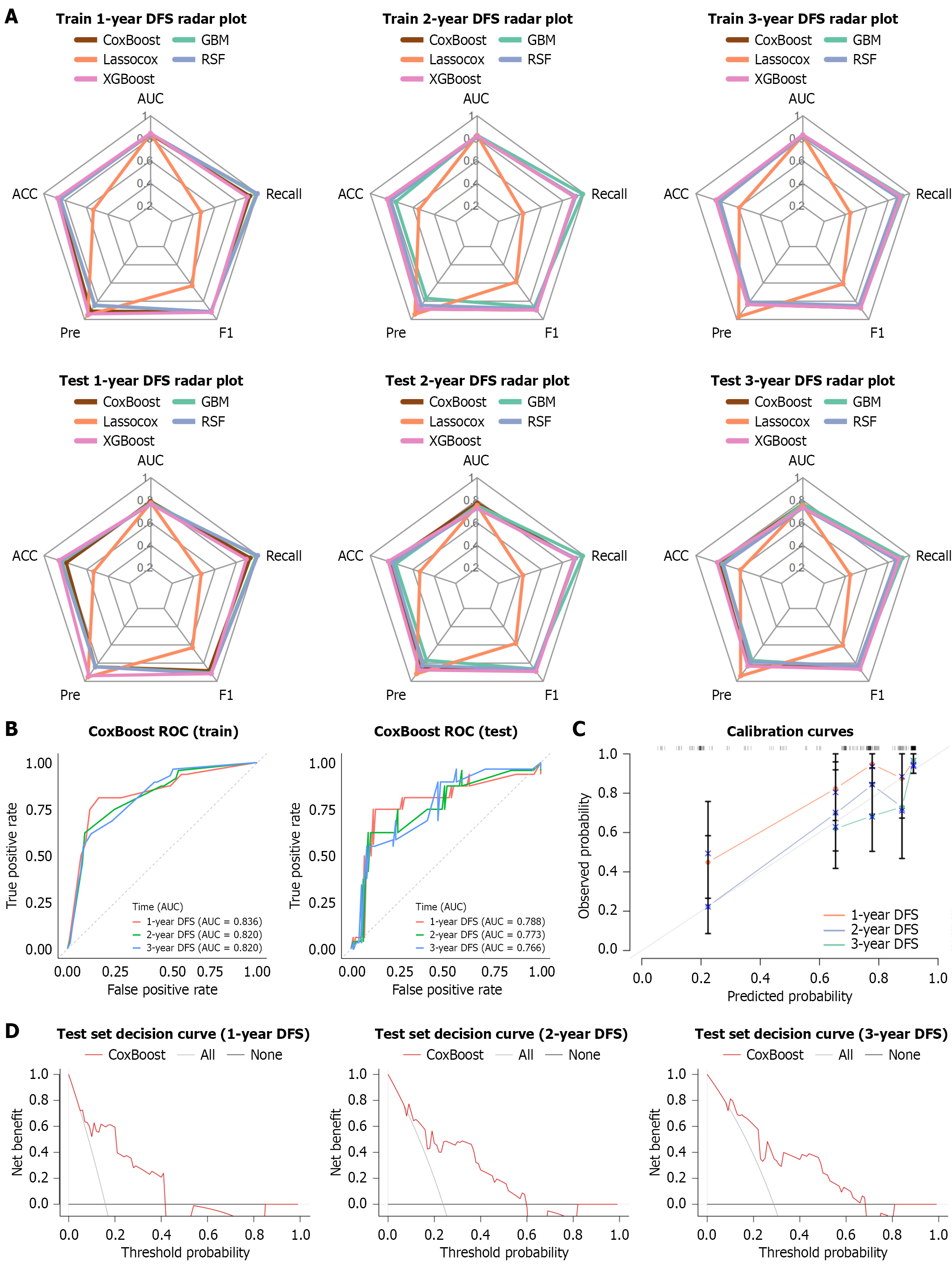
Figure 5 Construction and evaluation of different machine-learning models.
A: The performance comparison of the five machine learning models on the training and test set was presented using radar plots; B: Receiver operating characteristic used to evaluate the CoxBoost model; C: Calibration curve of the CoxBoost model on the train set; D: Decision curve of the CoxBoost model on the train set. ACC: Accuracy; AUC: Area under the receiver operating characteristic curve; DFS: Disease-free survival; GBM: Gradient boosting machine; LASSO: Least absolute shrinkage and selection operator; Pre: Precision; ROC: Receiver operating characteristic; RSF: Random survival forest.
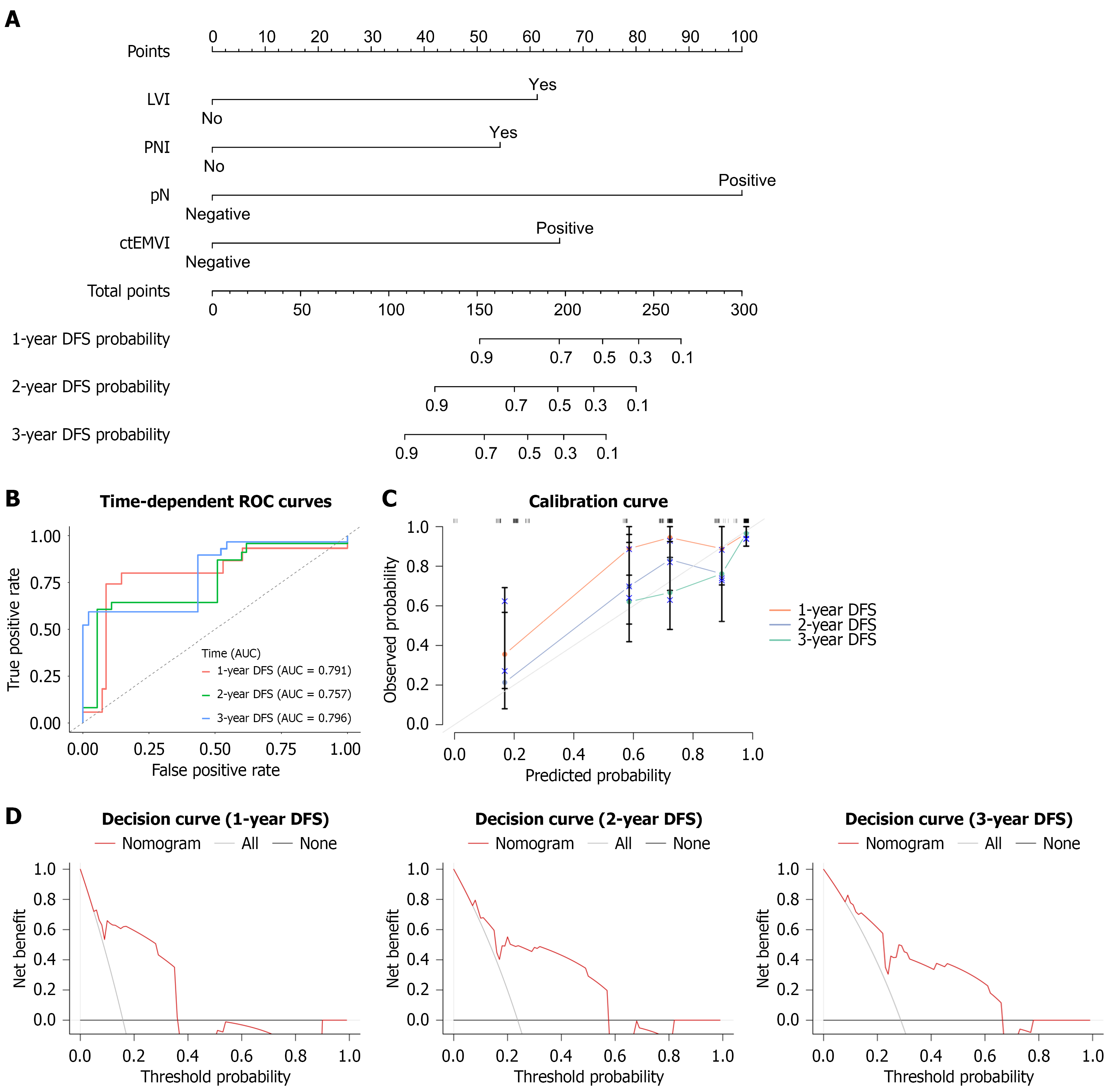
Figure 6 Construction and evaluation of the nomogram model.
A: Nomogram model constructed based on independent prognostic factors; B: Receiver operating characteristic used to evaluate the nomogram model; C: Calibration curve of the nomogram model; D: Decision curve of the nomogram model. AUC: Area under the receiver operating characteristic curve; ctEMVI: Computed tomography-detected extramural vascular invasion; DFS: Disease-free survival; LVI: Lymphovascular invasion; pN: Pathological nodal status; PNI: Perineural invasion; ROC: Receiver operating characteristic.
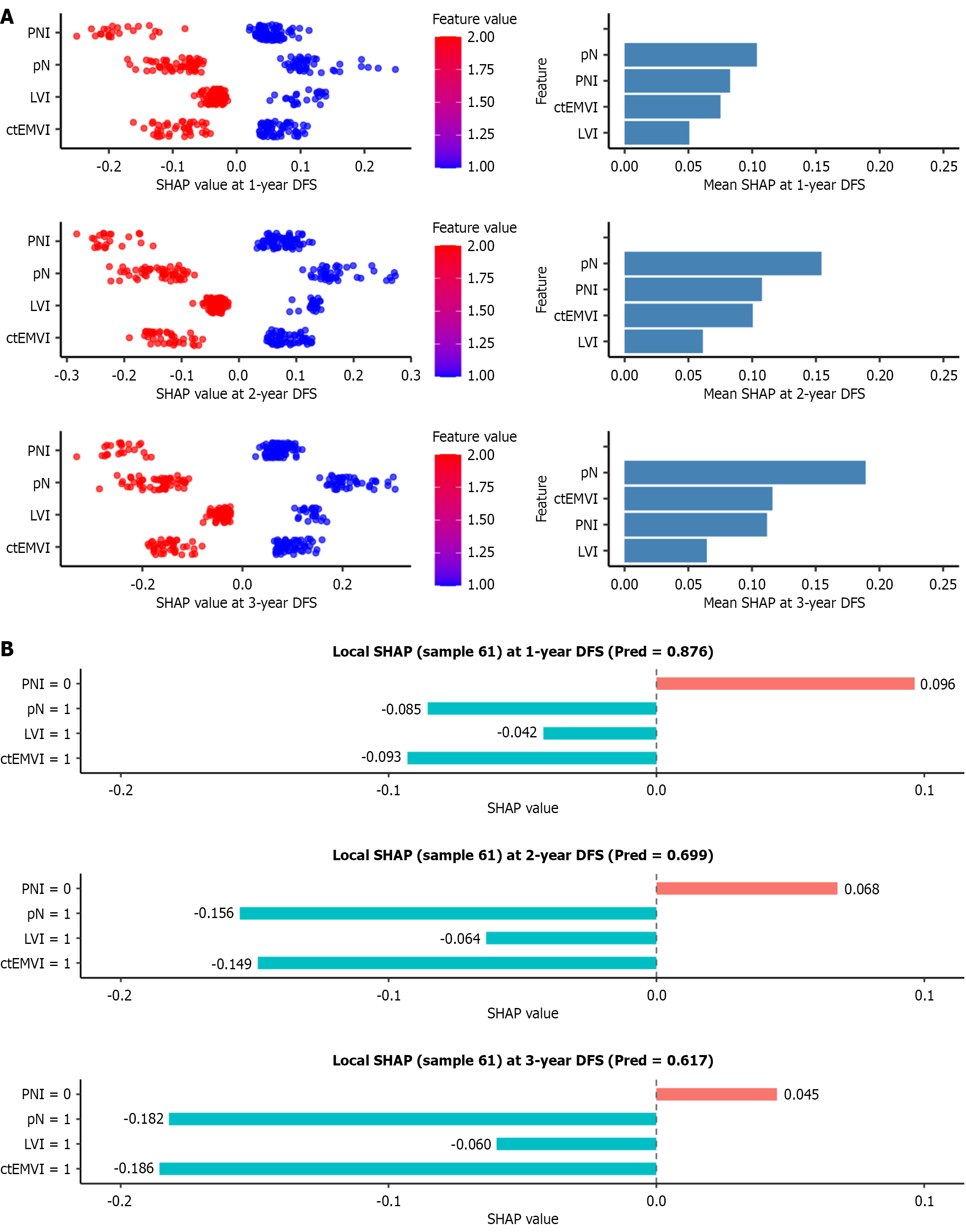
Figure 7 SHapley Additive exPlanations interprets the model.
A: Attributes of characteristics in SHapley Additive exPlanations. The scatter plot on the left shows the distribution of SHapley Additive exPlanations values for each case with respect to the given feature. The bar chart on the right displays the overall importance ranking of the features in disease-free survival (DFS) prediction; B: Individual efforts by patients with DFS after surgery. The predicted probabilities of DFS at 1-year, 2-year, and 3-year are 0.876, 0.699, and 0.617, respectively. In the figure, red features indicate an increase in the predicted probability, while blue features indicate a decrease in the predicted probability. ctEMVI: Computed tomography-detected extramural vascular invasion; DFS: Disease-free survival; LVI: Lymphovascular invasion; pN: Pathological nodal status; PNI: Perineural invasion; SHAP: SHapley Additive exPlanations.
- Citation: Wang MR, Zheng LF, Yang F, Gu XY, Yang JS, Chen FX, Liu JM, He BS. Development and validation of prognostic models for colon cancer incorporating extramural vascular invasion assessed by contrast-enhanced computed tomography. World J Gastroenterol 2026; 32(14): 116415
- URL: https://www.wjgnet.com/1007-9327/full/v32/i14/116415.htm
- DOI: https://dx.doi.org/10.3748/wjg.v32.i14.116415