Published online Jun 20, 2026. doi: 10.5662/wjm.v16.i2.115003
Revised: November 19, 2025
Accepted: February 2, 2026
Published online: June 20, 2026
Processing time: 201 Days and 2.7 Hours
Endovascular revascularization for lower limb arteriosclerosis obliterans (ASO) is often limited by long-term restenosis. This study evaluated whether the tradi
To investigate the clinical efficacy of DGSD combined with endovascular revascularization in the treatment of ASO and its impact on patients’ quality of life.
A total of 38 ASO patients treated at Zhangjiajie People’s Hospital from January 2023 to January 2025 were selected and randomly divided into a control group and an experimental group, with 19 patients in each group. The control group received conventional endovascular revascularization and basic treatment, while the experimental group was treated with DGSD in addition to the control group’s treatment. The clinical effectiveness rate, freedom from clinically driven target lesion revascularization, primary patency rate, and quality of life scores were compared between the two groups.
Within one month postoperatively, there was no significant difference in clinical effectiveness between the two groups (experimental group: 78.95% vs control group: 84.21%, P > 0.05), but the improvement in quality of life scores in the expe
DGSD combined with endovascular revascularization can significantly improve the mid-term clinical efficacy in ASO patients, reduce the risk of lower limb arterial re-occlusion, and enhance quality of life, demonstrating sig
Core Tip: This randomized controlled trial demonstrates that adjunctive therapy with Danggui Sini Decoction (DGSD), a classic traditional Chinese medicine formula, significantly enhances the mid-term outcomes of endovascular revascularization for arteriosclerosis obliterans. At six months, the DGSD group showed superior clinical effectiveness (94.74% vs 73.68%) and primary patency rates compared to the control group. The combination therapy also led to a greater impro
- Citation: Fu YB, Yan F, Zhu HJ, Wang C. Clinical efficacy of Danggui Sini Decoction for treatment of lower limb arteriosclerosis obliterans: A randomized controlled trial. World J Methodol 2026; 16(2): 115003
- URL: https://www.wjgnet.com/2222-0682/full/v16/i2/115003.htm
- DOI: https://dx.doi.org/10.5662/wjm.v16.i2.115003
Arteriosclerosis obliterans (ASO) is a chronic progressive disease characterized by the formation of atherosclerotic plaques in the lower extremity arteries, leading to stenosis or occlusion of the arterial lumen, which subsequently causes ischemia and hypoxia in the lower limbs. Its clinical manifestations include intermittent claudication and rest pain, and in severe cases, tissue necrosis may occur[1]. According to statistics, the number of ASO patients worldwide has exceeded 235 million[2]. In China, the incidence of ASO in the population aged 60 years and above is approximately 2.9%, and it is increasing at an annual rate of 5%[3,4]. This not only severely affects patients’ quality of life but also imposes a heavy economic burden on families and society due to the long-term treatment and care requirements. Modern medical treatments for ASO primarily involve antiplatelet medications to inhibit platelet aggregation, vasodilators to expand blood vessels, and interventional therapies to reopen stenotic or occluded arteries. However, the issue of low long-term patency rates remains a significant concern[5-7]. In traditional Chinese medicine (TCM), ASO falls under the categories of “meridian obstruction“ or “yin gangrene“ and is often treated from the perspective of “cold“ and “stasis“. In our center, Danggui Sini Decoction (DGSD)-which functions to warm the meridians, dispell cold, nourish blood, and unblock the vessels-is administered in combination with interventional therapy to restore blood flow in the lower limbs, and this combined regimen has yielded favorable clinical outcomes. The results are reported as follows.
A total of 38 patients with ASO treated at Zhangjiajie People’s Hospital from January 2023 to January 2025 were selected. The patients were randomly assigned in a 1:1 ratio to either an experimental group or a control group. The random allocation sequence was generated by an independent statistician using the random number function in Microsoft Excel. To ensure allocation concealment, this sequence was placed in sequentially numbered, opaque, sealed envelopes. The envelopes were opened by a research nurse only after a patient had provided written informed consent and was formally enrolled in the study. The general information of the patients, including gender, age, time of onset, clinical symptoms, lesion location, and Fontaine stage, is detailed in Table 1. There were no statistically significant differences in any of the general data between the two groups (P > 0.05). This study has obtained informed consent from the patients and was approved by the hospital’s ethics committee.
| Experimental group | Control group | t/χ2 | P value | ||
| Age (years) | 66.84 ± 7.98 | 66.32 ± 10.87 | 0.17 | 0.87 | |
| Gender | Male | 12 (63.16) | 10 (52.63) | 0.43 | 0.51 |
| Female | 7 (36.84) | 9 (47.37) | |||
| Smoking | 7 (36.84) | 6 (31.58) | 0.12 | 0.73 | |
| Comorbidities | Hypertension | 8 (42.11) | 7 (36.84) | 0.11 | 0.74 |
| Diabetes | 7 (36.84) | 6 (31.58) | 0.12 | 0.73 | |
| Coronary heart disease | 5 (26.32) | 4 (21.05) | 0.15 | 0.70 | |
| Chronic renal insufficiency | 8 (42.11) | 5 (26.32) | 1.05 | 0.31 | |
| Fontaine stage | Stage I | 0 | 0 | ||
| Stage II | 6 (31.58) | 5 (26.32) | 0.13 | 0.72 | |
| Stage III | 8 (42.11) | 10 (52.63) | 0.42 | 0.52 | |
| Stage IV | 5 (26.32) | 4 (21.05) | 0.15 | 0.70 | |
| Ankle-brachial-pressure-index | 0.26 ± 0.22 | 0.30 ± 0.23 | -0.54 | 0.59 | |
| Lesion location | Iliac artery | 4 (21.05) | 7 (36.84) | 1.15 | 0.28 |
| Femoropopliteal artery | 13 (68.42) | 7 (36.84) | 3.8 | 0.051 | |
| Infrapopliteal artery | 9 (47.37) | 13 (68.42) | 1.73 | 0.19 |
The diagnostic criteria required patients to conform to the diagnostic and efficacy criteria for ASO (draft) established by the Peripheral Vascular Disease Professional Committee of the Chinese Association of Integrative Medicine, with the TCM pattern matching the cold-dampness obstructing the collaterals pattern as defined in the criteria.
Eligible patients were required to have symptoms such as intermittent claudication, rest pain, or gangrene in the lower limbs, along with physical signs including decreased skin temperature and weakened or absent arterial pulses in the lower limbs. Additionally, color Doppler ultrasound or computed tomography angiography had to demonstrate stenosis or occlusion of the lower limb arteries.
Patients were excluded if their lower limb symptoms (pain, ulcers, or gangrene) were attributable to non-vascular etiologies. Patients complicated with severe primary diseases such as cancer, or cardiac, cerebral, hepatic, or hema
General treatment: All patients received treatments including glucose-lowering, antihypertensive, lipid-regulating, and antiplatelet aggregation therapies to control relevant risk factors. All patients also underwent walking exercises or rehabilitation therapy.
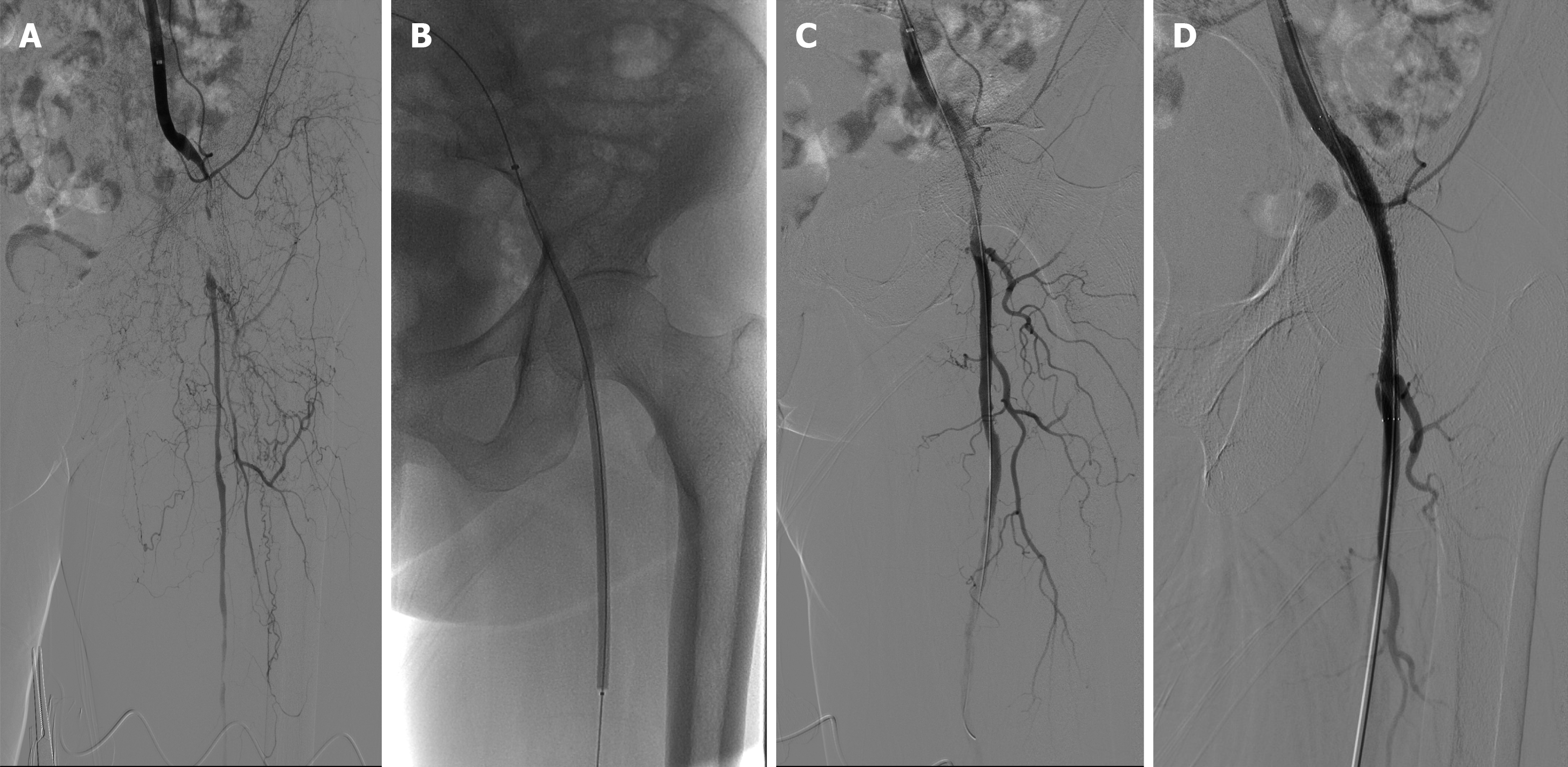
Control group: In addition to the aforementioned basic treatment, patients in this group underwent endovascular revascularization of the affected lower limb. Following routine disinfection and local anesthesia in the groin area, the femoral artery was punctured antegradely or retrogradely to place a vascular sheath. After systemic heparinization, angiography was performed to define the lesion extent (Figure 1A). Subsequently, under roadmap guidance, a guidewire and catheter were used to slowly cross the lesion segment. Based on pre-operative computed tomography angiography images, the vascular preparation method was determined: (1) If the lesion was primarily considered thrombotic, a thrombolysis catheter (Shanghai Meichuang Medical Device Co., Ltd.) was placed, and urokinase (Wuhan Humanwell Pharmaceutical Co., Ltd., National Medicine Permit No. H42021792) was continuously infused at a dose of 400000-600000 IU daily for 2 days. This was followed by staged balloon angioplasty using conventional balloons (Boston Scientific) (Figure 1B); and (2) If the lesion was primarily considered stenosis caused by plaque, direct staged balloon angioplasty was performed using conventional balloons (Boston Scientific). The procedure was concluded if no flow-limiting dissection or residual stenosis < 30% was present post-balloon angioplasty. If flow-limiting dissection (Figure 1C) or residual stenosis ≥ 30% occurred, a bare-metal stent was implanted to improve blood flow (Figure 1D). Post-intervention, patients received antiplatelet therapy with Rivaroxaban (Jilin Province Boda Pharmaceutical Co., Ltd., National Medicine Permit No. H20213352) 2.5 mg twice daily combined with Aspirin (Chenxin Pharmaceutical Co., Ltd., National Medicine Permit No. H20113013) 100 mg once daily for 6 months. All procedures across both study groups were conducted under the same standardized protocol by the same surgical team to ensure consistency and minimize operator bias.
Experimental group: Patients in the experimental group underwent the same standardized endovascular revascularization procedure as the control group, performed by the same surgical team. Additionally, they were administered DGSD. The prescription composition was: (1) Angelicae Sinensis Radix (Dang Gui); (2) Cinnamomi Ramulus (Gui Zhi); (3) Paeoniae Radix Rubra (Chi Shao) 15 g each; (4) Asari Radix et Rhizoma (Xi Xin) 3 g; (5) Tetrapanacis Medulla (Tong Cao) 10 g; (6) Dipsaci Radix (Xu Duan) 10 g; (7) Achyranthis Bidentatae Radix (Niu Xi) 10 g; (8) Spatholobi Caulis (Ji Xue Teng) 10 g; and (9) Jujubae Fructus (Da Zao) 5 pieces. One dose was decocted daily in water to obtain approximately 300 mL of decoction, divided into three warm doses taken orally. This constituted one treatment course lasting 4 weeks, and patients com
Postoperative assessments included monitoring for complications, perioperative mortality, and early postoperative occlusion. Patients returned for a follow-up visit at 1 month postoperatively to evaluate clinical efficacy and complete the Vascular Quality of Life (VascuQol) questionnaire. The VascuQol is a validated, disease-specific instrument for patients with peripheral arterial disease, consisting of 25 items grouped into 5 domains: (1) Pain (4 items); (2) Symptoms (4 items); (3) Activities (8 items); (4) Social function (3 items); and (5) Emotional status (6 items). Each item is rated on a 7-point Likert scale, where 1 represents the worst and 7 the best possible status. Domain scores and a global total score were calculated as the mean of the respective item scores. For more intuitive clinical interpretation, the mean scores were transformed to a 0-100 scale, with higher scores indicating better quality of life. The primary quality of life outcome was the change in the VascuQol total score (postoperative score minus preoperative score). A telephone follow-up was conducted at 6 months to assess clinical efficacy, limb salvage rate, and freedom from clinically driven target lesion revascularization.
Clinical efficacy was graded into the following three levels: (1) Markedly effective: The patient’s Fontaine stage decreased by one grade, the claudication distance significantly increased in patients with pre-existing intermittent claudication, or ulcers healed in patients with pre-existing ulcer formation; (2) Ineffective: The patient’s Fontaine stage remained unchanged, claudication distance showed no increase, or ulcers failed to heal; and (3) Deteriorated: The patient’s Fontaine stage increased by one grade.
Statistical analyses were performed using SPSS software (version 26.0). Measurement data, presented as the mean ± SD, were analyzed using the t-test. Count data, described by n (%), were analyzed using the χ2 test. P < 0.05 was considered statistically significant. GraphPad Prism software was used to plot the primary patency rate curve after surgery.
Lower limb revascularization was successfully performed in all 38 patients. The clinical effectiveness rate was 78.95% in the experimental group, with an ineffectiveness rate of 21.10%; in the control group, the clinical effectiveness rate was 84.21%, with an ineffectiveness rate of 15.79%. The patients for whom treatments were ineffective were all those with unhealed foot ulcers. The difference in clinical effectiveness rates between the two groups was not statistically significant (P > 0.05). There were no perioperative deaths in either group. In the experimental group, one patient developed a pseudoaneurysm at the right femoral artery puncture site, which was successfully treated with ultrasound-guided compression and resolved prior to discharge. In the control group, two patients experienced lower limb ischemia-reperfusion injury, manifesting as localized swelling and pain. Both were managed conservatively with mannitol (for dehydration), edaravone (as a neuroprotective agent), and limb elevation, leading to complete resolution of symptoms within 3-5 days. All complications improved after symptomatic treatment, and there was no statistically significant difference in the complication rate between the two groups (P > 0.05). The postoperative VascuQol scores were significantly higher than the preoperative scores in both groups. Furthermore, the difference between pre-operative and post-operative scores in the experimental group was greater than that in the control group, and this difference was statistically significant (P < 0.05). Specific data are detailed in Table 2. Despite successful randomization, a baseline imbalance was noted in the distribution of femoropopliteal artery lesions (68.42% vs 36.84%, P = 0.051). A post hoc subgroup analysis revealed that the primary patency rate remained significantly higher in the experimental group among patients with femoropopliteal lesions (84.6% vs 42.9%, P < 0.05), indicating that the superior outcomes associated with DGSD are independent of this baseline characteristic. The change in VascuQol score represents the difference between postoperative and preoperative total scores (on a transformed 0-100 scale).
| Experimental group | Control group | χ2 | P value | |
| Clinical effectiveness rate | 15 (78.95) | 16 (84.21) | 0.18 | 0.67 |
| Complications | 1 (5.26) | 2 (10.53) | 0.36 | 0.55 |
| Change in VascuQol score (postoperative - preoperative) | 46.11 ± 17.07 | 24.74 ± 8.61 | 4.87 | 0.001 |
At 6 months, the clinical effectiveness rate was 94.74% in the experimental group, with an ineffectiveness rate of 5.26% (attributed to patients with unhealed ulcers). In the control group, the clinical effectiveness rate was 73.68%, with an ineffectiveness rate of 26.32%; among the ineffective cases, 4 were due to re-occlusion of the lower limb arteries and 1 due to an unhealed ulcer. The clinical effectiveness rate in the experimental group was superior to that in the control group, and the difference was statistically significant (P < 0.05). No amputation events occurred in either group. In the control group, 3 patients underwent re-intervention due to re-occlusion of the lower limb arteries. Based on available imaging, these re-occlusions were primarily due to in-stent restenosis within the femoropopliteal segments. Specific data are detailed in Table 3.
| Experimental group | Control group | χ2 | P value | |
| Clinical effectiveness rate | 18 (94.74) | 14 (73.68) | 4.38 | 0.04 |
| Limb salvage rate | 19 (100) | 19 (100) | ||
| Freedom from target lesion revascularization | 19 | 16 (84.21) | 3.26 | 0.07 |
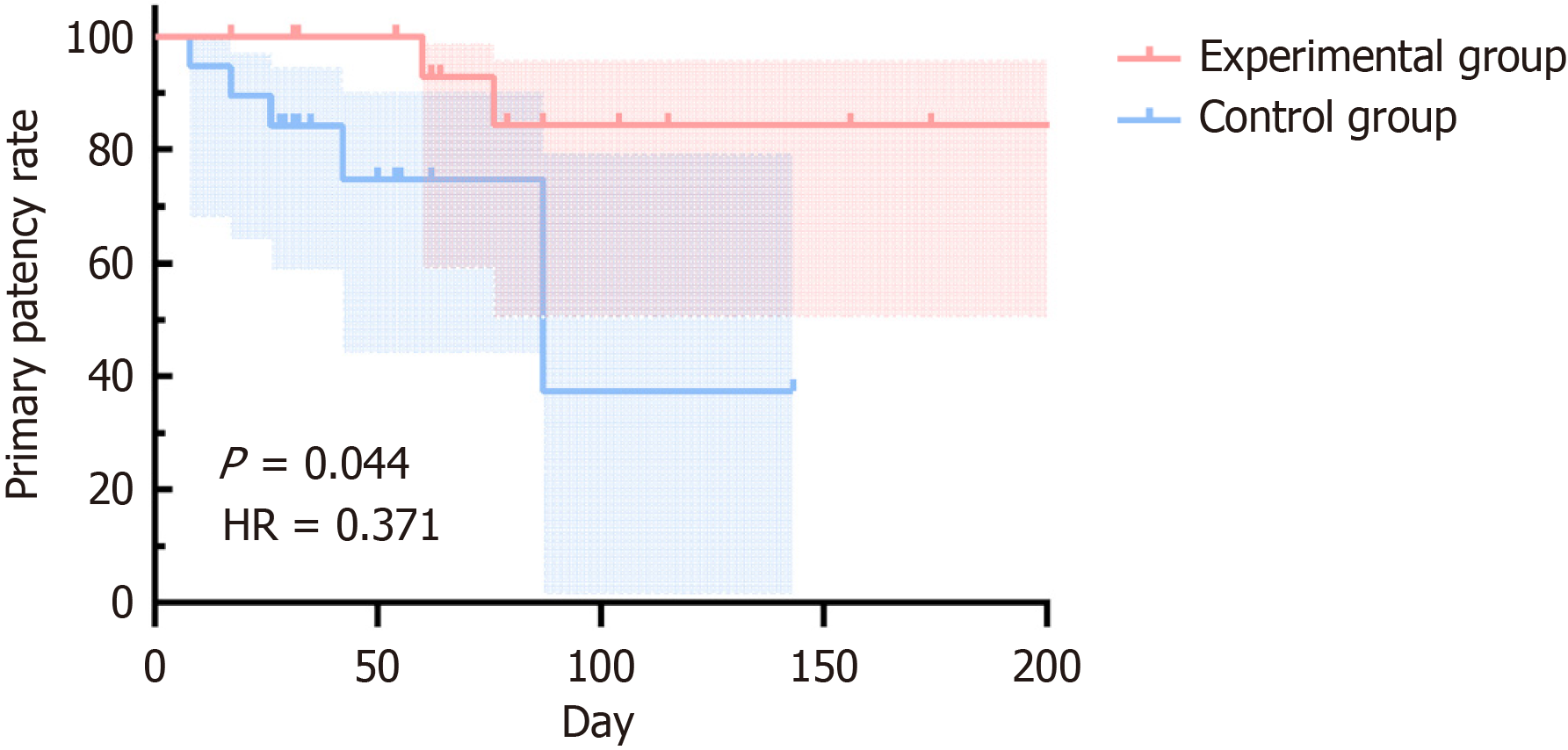
The primary patency rate at 6 months in the experimental group was significantly higher than that of the control group. Comparison of the Kaplan-Meier curves by the log-rank test confirmed a statistically significant difference between the groups (P = 0.044). Details are shown in Figure 2.
ASO is a localized manifestation of systemic atherosclerosis in the lower limbs. Its incidence and disability rates are particularly prominent in the elderly population, making early and active intervention crucial. Although modern medicine, through pharmacological treatment and interventional procedures, can alleviate clinical symptoms to some extent, the issue of low long-term vascular patency rates remains unresolved. Within the theoretical framework of TCM, ASO falls under the categories of "meridian obstruction" (Mai Bi) and "yin gangrene" (Yin Ju). Related records can be traced back to the "Lingshu Yong Ju Chapter": "When it occurs on the toes, it is called gangrene (Tuo Yong); if it appears red-black, it is fatal and incurable; if not red-black, it is not fatal. If it does not subside, it should be urgently amputated, otherwise death will occur." In recent years, TCM has achieved significant results in treating ASO, fully demonstrating its unique advantages and potential[8-10]. Based on this, our study adopted an integrated Chinese and Western medicine approach, focusing on exploring the effect of DGSD on improving clinical symptoms and vascular patency in ASO patients, aiming to provide a more optimized treatment strategy for clinical practice.
In recent years, the rapid development of interventional techniques has established them as a first-line treatment option for ASO patients[11,12]. Among them, percutaneous balloon angioplasty combined with provisional stenting is a classic procedure, widely used in clinical practice due to its minimally invasive nature, cost-effectiveness, and confirmed efficacy. For instance, in this study, the one-month clinical effectiveness rates were 78.95% and 84.21% in the experimental and control groups, respectively; the postoperative VascuQol scores were significantly higher than preoperative scores in both groups. Symptoms improved markedly in all patients with intermittent claudication and rest pain. The ineffective cases were primarily patients with large pre-existing foot ulcers that had not healed within one month post-surgery. However, the long-term patency rate of this procedure is often low due to the tendency for in-stent restenosis. For example, a study by Gouëffic et al[13], involving 775 ASO patients, reported a 1-year primary patency rate of only 74.3% for the balloon angioplasty with provisional stenting group. Similarly, a study by Suzuki et al[14], involving 1505 ASO patients treated with the same procedure, found the 2-year primary patency rate further decreased to 55%-67%. Although various drug-eluting devices are now available that can improve long-term patency rates[15], their high cost limits widespread clinical application. In our study, the Kaplan-Meier estimate for the control group (balloon angioplasty with provisional stenting alone) projected a 1-year primary patency rate of 68%, consistent with the findings mentioned above. In contrast, the experimental group (DGSD combined with balloon angioplasty and provisional stenting) achieved a significantly higher projected 1-year primary patency rate of 82%. It is important to note that these are estimates based on 6-month data, and actual long-term patency requires verification with longer follow-up.
DGSD originates from the "Treatise on Cold Damage Diseases", specifically the chapter on differentiating and treating Shaoyin disease patterns. The text states: "For cold limbs and a faint, thin pulse, DGSD is indicated." It is used for patients with blood deficiency accompanied by cold, leading to poor circulation of Qi and blood resulting in cold limbs and a thin, weak pulse. The formula functions to nourish blood, dispel cold, and warm the meridians. ASO patients often present with cold pain and aversion to cold in the lower limbs, symptoms that worsen at night or upon exposure to cold. This clinical picture highly corresponds to the pattern of blood deficiency with cold congelation targeted by DGSD. The formula comprises Angelicae Sinensis Radix (Dang Gui), Cinnamomi Ramulus (Gui Zhi), Paeoniae Radix (Shao Yao), Asari Radix et Rhizoma (Xi Xin), Tetrapanacis Medulla (Tong Cao), Jujubae Fructus (Da Zao), and Glycyrrhizae Radix Praeparata (Zhi Gan Cao). Within the formula, Paeoniae Radix and Angelicae Sinensis Radix work together to nourish blood and harmonize the nutrient system, while Cinnamomi Ramulus and Asari Radix et Rhizoma dispel cold and warm the channels. To the classic formula that warms channels and dispels cold, we added Achyranthis Bidentatae Radix (Niu Xi) to guide the formula’s action downward to the lower limbs[16] and Spatholobi Caulis (Ji Xue Teng) to intensify blood activation and collateral unblocking, directly addressing the stasis inherent in ASO[17]. This enhanced focus on resolving stasis and targeting the affected region likely contributed to the improved primary patency and quality of life, underscoring the benefit of tailoring classic formulations to specific disease pathologies. Modern clinical research suggests that DGSD plays a significant role in improving blood circulation, relieving pain, and repairing nerve function. Angelicae Sinensis Radix (Dang Gui) and Paeoniae Radix Rubra (Chi Shao), the core drug pair for nourishing blood and harmonizing the nutritive level, have demonstrated profound anti-inflammatory effects beyond their traditional applications. Modern research, particularly in rheumatology, has elucidated that active compounds such as paeoniflorin and caffeic acid from this pair can significantly inhibit the PI3K/AKT/NF-κB signaling pathway[18]. The suppression of this critical pathway leads to the downregulation of key pro-inflammatory cytokines, including tumor necrosis factor-alpha, interleukin-1 beta, and interleukin-6. Given that the progression of atherosclerotic plaques in ASO is driven by a similar chronic inflammatory milieu, this targeted anti-inflammatory mechanism is crucial for stabilizing the vascular lesion and mitigating the ischemic insult, thereby providing a modern pharmacological basis for their use in this formula. Cinnamomi Ramulus (Gui Zhi), known for dispelling cold, contains cinnamaldehyde which acts as a vasodilator, improving peripheral blood flow and countering vasospasm[19]. In our trial, the experimental group not only had a significantly higher long-term patency rate than the control group but also showed a greater improvement in the pre-operative and postoperative VascuQol score difference. This may be related to DGSD’s effects on improving lower limb nerve function and alleviating lower limb pain.
In summary, DGSD demonstrates definite clinical efficacy in the treatment of ASO, significantly improving vascular patency rates at the 6-month follow-up and enhancing health-related quality of life. However, this study has several limitations that should be acknowledged. First, the relatively small sample size may limit the statistical power of the analysis, increasing the risk of a type II error. For instance, the observed trend towards a higher freedom from clinically driven target lesion revascularization in the experimental group may have reached statistical significance with a larger cohort. Second, the 6-month follow-up period is insufficient to evaluate true long-term efficacy and durability, as restenosis in ASO often occurs beyond this time frame, typically between 12 months and 24 months post-intervention. Therefore, our findings, while promising, represent mid-term outcomes and should be interpreted with caution. Future large-scale, multi-center randomized controlled trials with extended follow-up times of at least 1-2 years are warranted to confirm the long-term clinical value of DGSD for ASO patients.
The authors would like to express their sincere gratitude to all the patients who participated in this study. We also thank the nursing staff and clinical colleagues at Zhangjiajie People’s Hospital for their support in patient care and data collection.
| 1. | Gornik HL, Aronow HD, Goodney PP, Arya S, Brewster LP, Byrd L, Chandra V, Drachman DE, Eaves JM, Ehrman JK, Evans JN, Getchius TSD, Gutiérrez JA, Hawkins BM, Hess CN, Ho KJ, Jones WS, Kim ESH, Kinlay S, Kirksey L, Kohlman-Trigoboff D, Long CA, Pollak AW, Sabri SS, Sadwin LB, Secemsky EA, Serhal M, Shishehbor MH, Treat-Jacobson D, Wilkins LR; Peer Review Committee Members. 2024 ACC/AHA/AACVPR/APMA/ABC/SCAI/SVM/SVN/SVS/SIR/VESS Guideline for the Management of Lower Extremity Peripheral Artery Disease: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2024;149:e1313-e1410. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 361] [Cited by in RCA: 378] [Article Influence: 189.0] [Reference Citation Analysis (0)] |
| 2. | Song P, Rudan D, Zhu Y, Fowkes FJI, Rahimi K, Fowkes FGR, Rudan I. Global, regional, and national prevalence and risk factors for peripheral artery disease in 2015: an updated systematic review and analysis. Lancet Glob Health. 2019;7:e1020-e1030. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1121] [Cited by in RCA: 929] [Article Influence: 132.7] [Reference Citation Analysis (0)] |
| 3. | Sheng CS, Li Y, Huang QF, Kang YY, Li FK, Wang JG. Pulse Waves in the Lower Extremities as a Diagnostic Tool of Peripheral Arterial Disease and Predictor of Mortality in Elderly Chinese. Hypertension. 2016;67:527-534. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 30] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 4. | Shilian H, Jing W, Cui C, Xinchun W. Analysis of epidemiological trends in chronic diseases of Chinese residents. Aging Med (Milton). 2020;3:226-233. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 28] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 5. | Micari A, Vadalà G, Castriota F, Liso A, Grattoni C, Russo P, Marchese A, Pantaleo P, Roscitano G, Cesana BM, Cremonesi A. 1-Year Results of Paclitaxel-Coated Balloons for Long Femoropopliteal Artery Disease: Evidence From the SFA-Long Study. JACC Cardiovasc Interv. 2016;9:950-956. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 64] [Cited by in RCA: 68] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 6. | Sufali G, Teraa M. Randomized trial comparing a stent-avoiding with a stent-preferred strategy in complex femoropopliteal lesions. Cardiovasc Diagn Ther. 2024;14:1011-1014. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 7. | Lammer J, Zeller T, Hausegger KA, Schaefer PJ, Gschwendtner M, Mueller-Huelsbeck S, Rand T, Funovics M, Wolf F, Rastan A, Gschwandtner M, Puchner S, Ristl R, Schoder M. Heparin-bonded covered stents versus bare-metal stents for complex femoropopliteal artery lesions: the randomized VIASTAR trial (Viabahn endoprosthesis with PROPATEN bioactive surface [VIA] versus bare nitinol stent in the treatment of long lesions in superficial femoral artery occlusive disease). J Am Coll Cardiol. 2013;62:1320-1327. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 192] [Cited by in RCA: 213] [Article Influence: 16.4] [Reference Citation Analysis (0)] |
| 8. | Cheng S, Xu JX, Long WJ. Advances in the management of arteriosclerosis of the lower extremity: Integrating Western and Chinese medicine approaches. World J Clin Cases. 2024;12:6871-6876. [PubMed] [DOI] [Full Text] |
| 9. | Zhang L, Yuan JQ, Song FC, Zhu MD, Li Q, Liu SH, Zhao K, Zhao C. Ameliorative effects of the traditional Chinese medicine formula Qing-Mai-Yin on arteriosclerosis obliterans in a rabbit model. Pharm Biol. 2020;58:785-795. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 10] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 10. | Li YP, Su T, Xue XL, Shi HR, Su ZH, Li J. Application of buried auricular point combined with Wenjing Sanhan prescription in arteriosclerosis obliterans patients with resting pain. World J Clin Cases. 2024;12:5558-5567. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 11. | Müller AM, Löhn-Kannengießer L, Bradaric C, Dirschinger R, Koppara T, Bergmann K, Kehl V, Cassese S, Xhepa E, Kastrati A, Laugwitz KL, Ibrahim T. Outcomes of endovascular treatment for popliteal artery disease. Vasa. 2023;52:386-393. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 12. | Criqui MH, Matsushita K, Aboyans V, Hess CN, Hicks CW, Kwan TW, McDermott MM, Misra S, Ujueta F; American Heart Association Council on Epidemiology and Prevention; Council on Arteriosclerosis, Thrombosis and Vascular Biology; Council on Cardiovascular Radiology and Intervention; Council on Lifestyle and Cardiometabolic Health; Council on Peripheral Vascular Disease; and Stroke Council. Lower Extremity Peripheral Artery Disease: Contemporary Epidemiology, Management Gaps, and Future Directions: A Scientific Statement From the American Heart Association. Circulation. 2021;144:e171-e191. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 323] [Cited by in RCA: 551] [Article Influence: 110.2] [Reference Citation Analysis (1)] |
| 13. | Gouëffic Y, Torsello G, Zeller T, Esposito G, Vermassen F, Hausegger KA, Tepe G, Thieme M, Gschwandtner M, Kahlberg A, Schindewolf M, Sapoval M, Diaz-Cartelle J, Stavroulakis K; EMINENT Investigators. Efficacy of a Drug-Eluting Stent Versus Bare Metal Stents for Symptomatic Femoropopliteal Peripheral Artery Disease: Primary Results of the EMINENT Randomized Trial. Circulation. 2022;146:1564-1576. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 88] [Cited by in RCA: 77] [Article Influence: 19.3] [Reference Citation Analysis (0)] |
| 14. | Suzuki K, Takahara M, Shintani Y, Tanaka A, Soga Y, Yamaoka T, Tosaka A, Sasaki S, Kawasaki D, Tsuchiya T, Kozuki A, Iida O. Retrospective Multicenter Comparison of S.M.A.R.T. CONTROL and MISAGO Stents in Treatment of Femoropopliteal Lesions. J Vasc Interv Radiol. 2016;27:1642-1649. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 15. | Varcoe RL, DeRubertis BG, Kolluri R, Krishnan P, Metzger DC, Bonaca MP, Shishehbor MH, Holden AH, Bajakian DR, Garcia LA, Kum SWC, Rundback J, Armstrong E, Lee JK, Khatib Y, Weinberg I, Garcia-Garcia HM, Ruster K, Teraphongphom NT, Zheng Y, Wang J, Jones-McMeans JM, Parikh SA; LIFE-BTK Investigators. Drug-Eluting Resorbable Scaffold versus Angioplasty for Infrapopliteal Artery Disease. N Engl J Med. 2024;390:9-19. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 82] [Article Influence: 41.0] [Reference Citation Analysis (0)] |
| 16. | Wu L, Hao Y, Dai C, Zhang Z, Ijaz M, Ibrahim SM, Murtaza G, Yao Z. Network Pharmacological Study of Achyranthis bidentatae Radix Effect on Bone Trauma. Biomed Res Int. 2021;2021:5692039. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 17. | Pan Y, Luo X, Gong P. Spatholobi caulis: A systematic review of its traditional uses, chemical constituents, biological activities and clinical applications. J Ethnopharmacol. 2023;317:116854. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 15] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 18. | Li J, Zhang X, Guo D, Shi Y, Zhang S, Yang R, Cheng J. The mechanism of action of paeoniae radix rubra-angelicae sinensis radix drug pair in the treatment of rheumatoid arthritis through PI3K/AKT/NF-κB signaling pathway. Front Pharmacol. 2023;14:1113810. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 12] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 19. | Liu J, Zhang Q, Li RL, Wei SJ, Huang CY, Gao YX, Pu XF. The traditional uses, phytochemistry, pharmacology and toxicology of Cinnamomi ramulus: a review. J Pharm Pharmacol. 2020;72:319-342. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 51] [Article Influence: 7.3] [Reference Citation Analysis (0)] |