Published online Jun 20, 2026. doi: 10.5662/wjm.v16.i2.111784
Revised: August 5, 2025
Accepted: December 10, 2025
Published online: June 20, 2026
Processing time: 288 Days and 16.5 Hours
Colovesical fistula (CVF) is an uncommon but serious complication most often linked to diverticular disease of the colon. Its diagnosis can be at times challen
A 65-year-old Indian male was admitted with right lower limb cellulitis and was in septic shock. Despite initial management, he remained oliguric with persistent loose stools. On post-fasciotomy day 4, fecaluria was noted, prompting suspicion of a bowel-urinary tract fistula. Microscopic urine examination confirmed fecal matter. A computed tomography urogram with cystogram revealed a CVF at the sigmoid colon, likely secondary to diverticulitis. Baseline carcinoembryonic anti
CVF should be considered in cases of persistent urinary symptoms or fecaluria, particularly in patients with risk factors such as older age and diverticular disease, even in regions with low incidence of colonic diverticula. Early diagnosis using imaging modalities and prompt surgical management are key to favorable outcomes.
Core Tip: This report highlights a rare presentation of colovesical fistula (CVF) secondary to sigmoid diverticulitis, presenting as lower limb cellulitis with septic shock. Early suspicion, fecaluria recognition, and prompt imaging confirmed CVF. Laparotomy with bladder repair and Hartmann’s procedure ensured a favorable recovery. Clinicians should consider CVF in atypical presentations of sepsis, especially in elderly patients. This case emphasizes the significance of timely diagnosis and surgical planning in managing CVF.
- Citation: Hegde AV, Gupta S, Mohan LN, Rozario A. Unforeseen consequence of colovesical fistula in diverticulitis presenting as septic cellulitis: A case report. World J Methodol 2026; 16(2): 111784
- URL: https://www.wjgnet.com/2222-0682/full/v16/i2/111784.htm
- DOI: https://dx.doi.org/10.5662/wjm.v16.i2.111784
A colovesical fistula (CVF) refers to the abnormal connection between the colon and the bladder. This condition can develop as a consequence of various underlying diseases[1]. Diverticular disease is particularly prevalent in Western societies. Complicated diverticulitis is the leading cause of CVF, accounting for more than two-thirds of cases. In patients with diverticular disease, the likelihood of developing CVF ranges from 2% to 23%. Individuals > 60 years of age have a 30% chance of developing diverticulosis, and this figure increases to approximately 70% for those > 80 years of age[2]. In contrast, the prevalence in individuals < 40 years of age is < 10%[3]. A study has estimated that 15%-25% of people with diverticulosis will develop diverticulitis during their lifetime[4], although a retrospective review in 2013 found a lifetime risk of only 4%[5]. The second most common cause of CVF is malignancy, accounting for 10%-20% of cases, typically involving adenocarcinoma of the colon. Crohn’s colitis is the third most common cause, occurring in 5%-7% of instances and is often linked to chronic disease. Other rare causes of CVF include iatrogenic injuries from surgical procedures, pelvic radiation, abdominal trauma, and tuberculosis[2]. The prognosis for CVF is generally poor owing to the significant risk of severe infection and systemic complications such as uremia, septicemia, and renal failure[1]. Here, we present a case of CVF with diverticulitis in a 65-year-old male Indian patient who presented with right lower limb cellulitis with septicaemia.
Fever, pain, and swelling in the right lower limb.
A 65-year-old man presented to the emergency department with fever, pain, and swelling in the right lower limb extending from foot to thigh.
No similar complaints in the past.
No relevant personal and family history.
He exhibited tachycardia, hypotension, and oliguria, along with an edematous, tender, and erythematous right lower limb, leading to a diagnosis of right lower limb cellulitis and septic shock.
Laboratory examinations are listed in Table 1.
| Investigations | Values |
| Hemoglobin | 9.6 g/dL |
| Total leukocyte count | 19670 cells/μL |
| Platelet count | 1.32 cells/µL |
| Sodium/potassium | 128/5.7 mmol/L |
| Creatinine | 6.6 mg/dL |
| Creatinine after hemodialysis | 2.1 mg/dL |
| Creatinine at discharge | 1.4 mg/dL |
| Urine culture | Polymicrobial growth |
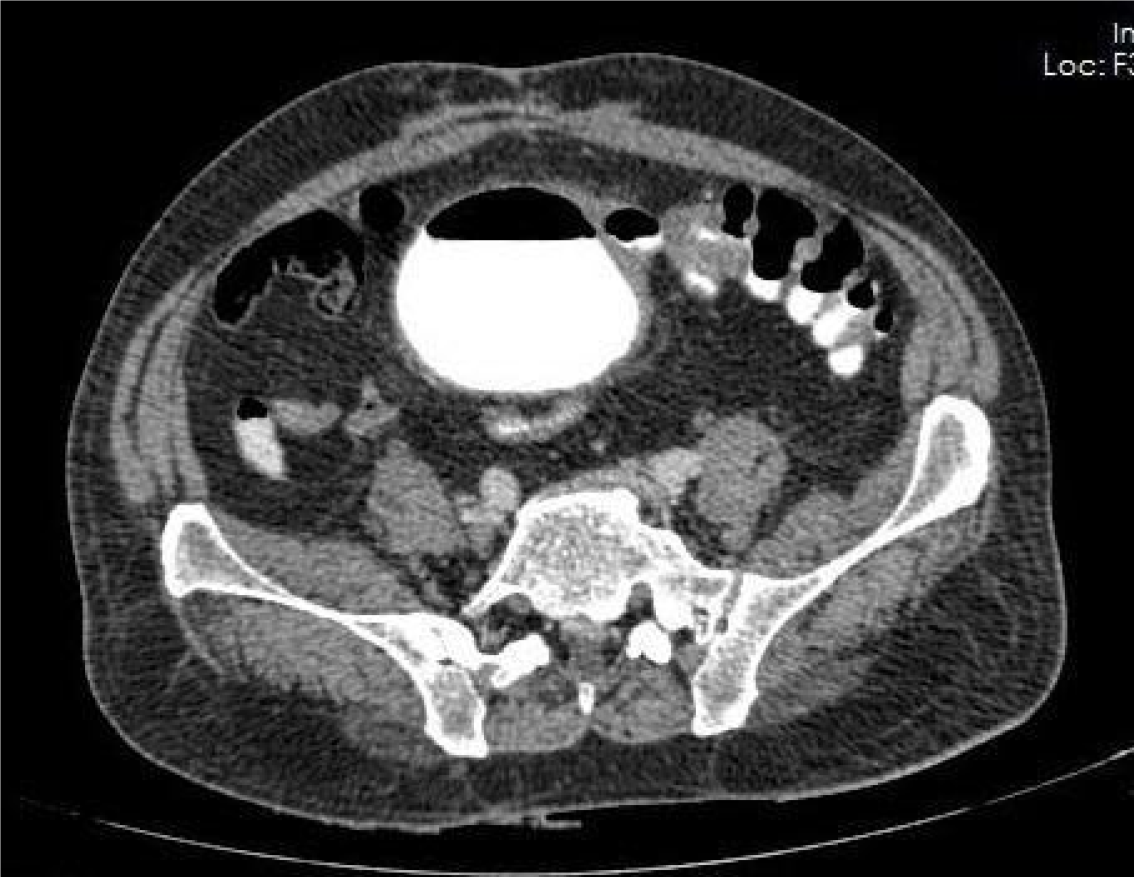
A computed tomography (CT) urogram with cystogram was performed, revealing a CVF at the sigmoid colon owing to diverticulitis (Figure 1), necessitating the exclusion of malignancy.
A urology consultation was obtained, and the patient was scheduled for laparotomy.
Colovesical fistula in diverticulitis with septic cellulitis.
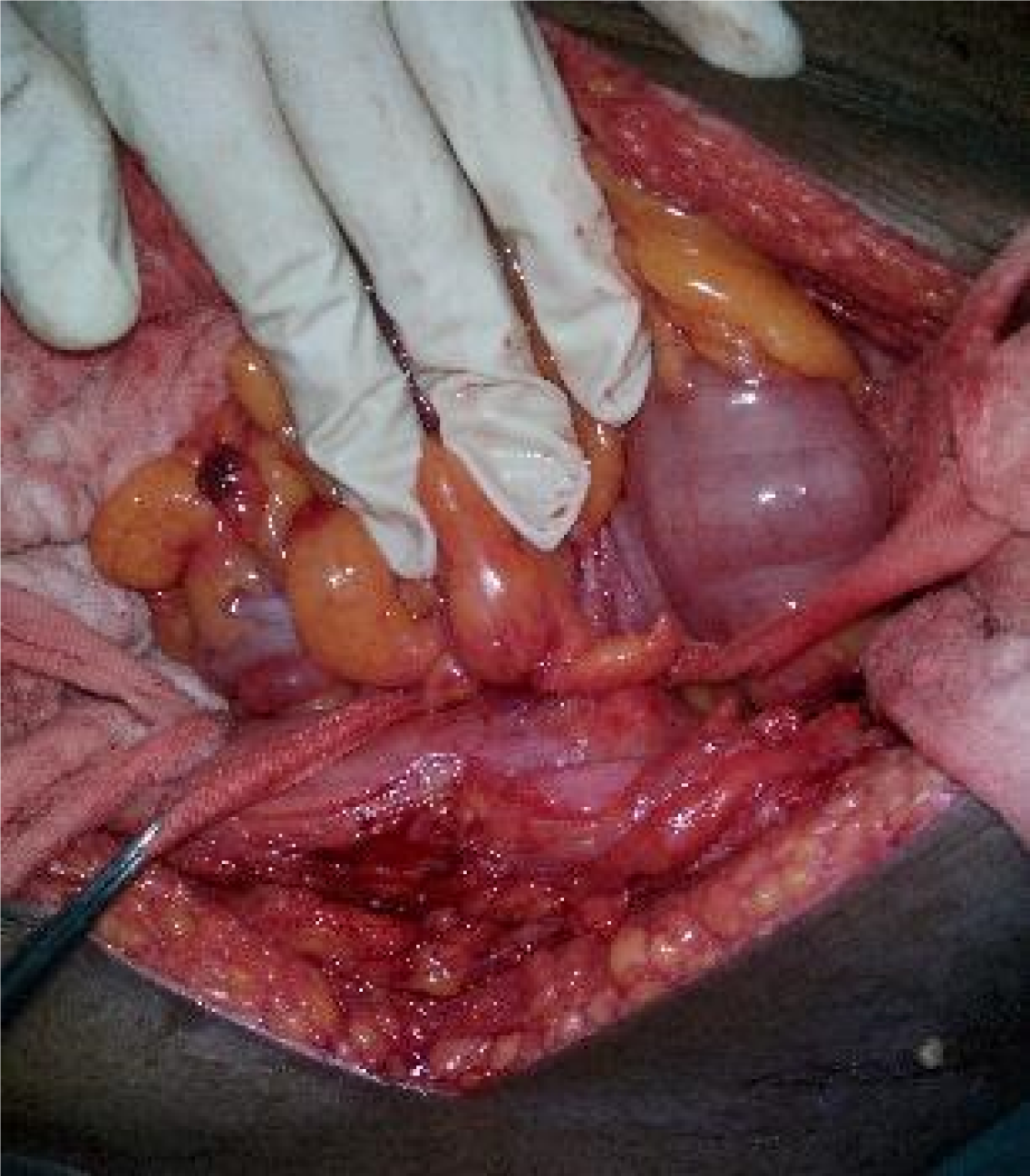
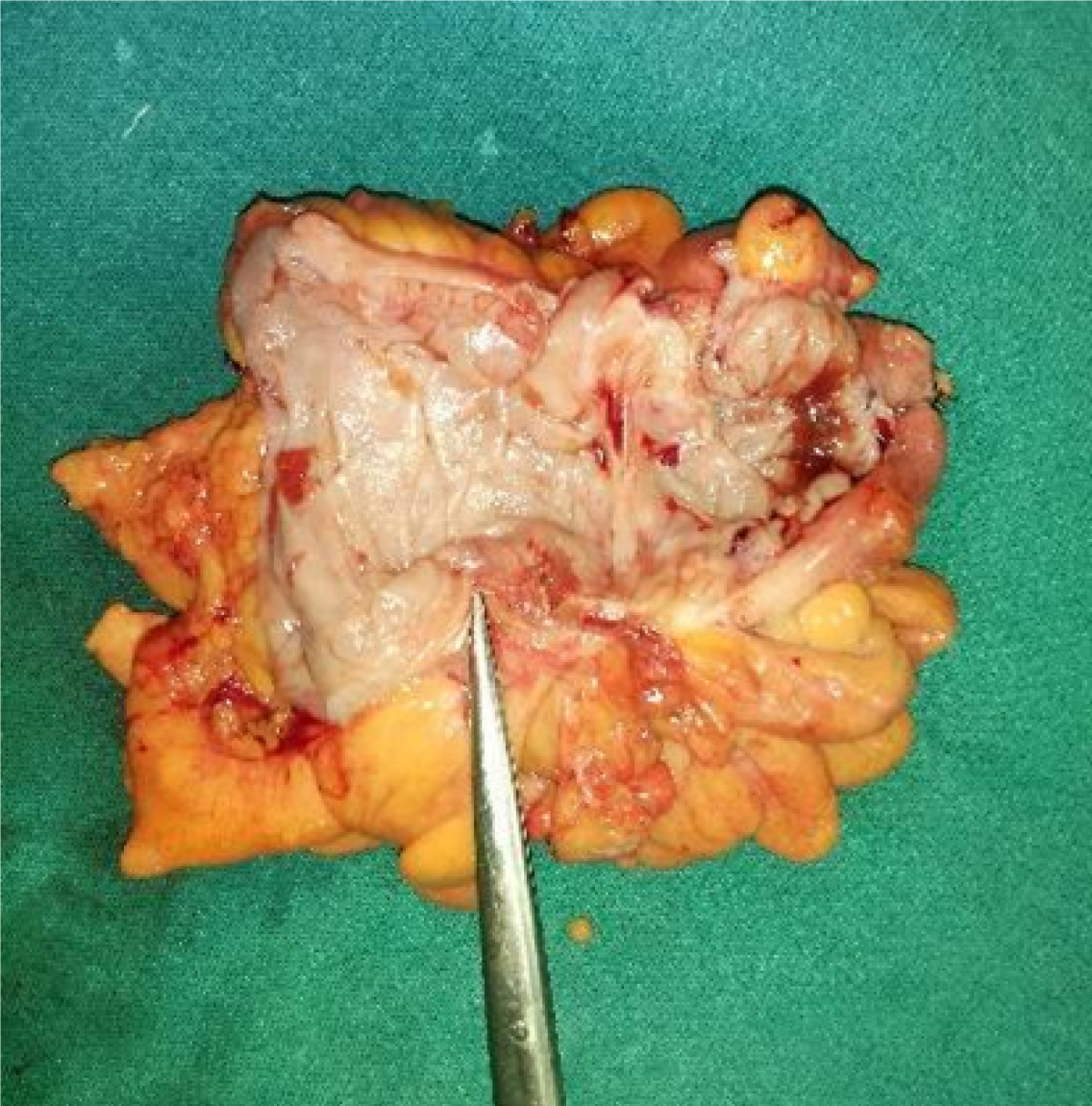
Following stabilization, he was admitted to the intensive care unit and underwent a fasciotomy. The patient reported frequent episodes of loose stools from postoperative day 2. Supportive care was continued, but both oliguria and loose stools persisted. On post-fasciotomy day 4, a bladder wash was performed, yielding scant return, while oliguria continued. The team suspected fecal debris in the urosac bag and requested microscopic analysis of the urine sample, which indicated the presence of stool, suggesting a potential fistulous connection. A wide-bore Foley catheter was inserted, and the bladder wash returned feculent fluid. The combination of persistent oliguria despite hydration, along with new-onset loose stools, with feculent return in the foleys raised suspicion of a fistulous communication. Dense adhesions were identified between the sigmoid colon and the left posterolateral surface of the bladder and were carefully separated during surgery (Figure 2). The fistulous connection was excised and sent for frozen section analysis, which did not reveal any malignant cells. Subsequently, a two-layer bladder repair was performed along with resection of the affected segment of the sigmoid colon and Hartmann’s procedure, following multiple clear bladder washes (Figure 3).
The patient remained hemodynamically labile intraoperatively, with mean arterial pressure fluctuating around 60-65 mmHg despite vasopressor support, supporting the decision for Hartmann’s procedure over primary anastomosis was made. A pelvic drain was placed, and the abdomen was closed in layers. Postoperatively, the patient resumed oral feeding on day 2; the urine output improved, and loose stools stopped. He was discharged on postoperative day 8 after the drain was removed on day 7. The final biopsy confirmed sigmoid diverticulosis with diverticulitis. Two months after the procedure, the stoma was reversed, and the patient was doing well at the 6-month follow-up.
A CVF is an abnormal connection between the urinary bladder epithelium and a section of the large intestine, typically the sigmoid colon. This unusual fistulous link is often attributed to various inflammatory or neoplastic conditions[6]. Cripps initially identified this condition in 1888 as a complication of diverticulitis[7], a finding that has been confirmed in subsequent studies[8,9]. Other factors known to cause CVF include colon cancer, bladder cancer, radiation therapy, Crohn’s disease, and a ruptured appendix[6]. A recent single-center study from Virginia reported that diverticulitis (80.5%) was the commonest cause of CVF, followed by colon cancer (7.3%)[6]. Similar observations were made in a recent systematic review from Italy, wherein colonic diverticulitis was found to be the most common etiology of CVF[10].
Although acute diverticulitis is a common condition, the development of CVF as a complication is quite rare, occurring in < 5% of cases[3]. Only six cases of CVF have been documented in the literature from India, of which the etiology was diverticulitis in three cases[11-14], adenocarcinoma of the sigmoid colon in one case[15], Crohn’s disease in one case[16], and in one case, the patient was a renal allograft recipient[17]. In Western countries, diverticular disease predominantly affects the sigmoid colon, and this segment is also the most common source of fistulas, as observed in our case. The leading types of fistulas are colovesical (65%) and colovaginal (25%), followed by coloenteric (7%), colouterine (3%), and colocutaneous fistulas, as well as complex fistulas involving multiple pelvic organs (10%)[12]. The typical age of patients presenting with CVF is 55-75 years. Although the exact incidence rate of CVF arising from diverticulitis is not clearly defined, a male predominance of 2-3:1 has been reported in the literature, likely due to the protective role of the uterus against inflammation of the sigmoid colon in women[10,12]. In our case, the patient was a 65-year-old man of Indian origin.
Patients with recurrent diverticulitis often report lower abdominal pain and a history of constipation. Furthermore, they exhibit symptoms of urinary tract infections, such as increased frequency, urgency, fever, or chills[3]. Nonetheless, atypical presentations, such as those in our patient, can occur without prior abdominal pain. In this case, the patient presented with an erythematous right lower limb and fever, leading to a diagnosis of cellulitis and septic shock, intensive care unit admission, stabilization, and fasciotomy. Patients with CVF generally present with pneumaturia and/or fecaluria, with pneumaturia being more common. Approximately 70%-90% of these patients exhibit pneumaturia, 50%-70% may experience fecaluria, and 87.5% present with either symptom[3,18]. In our case, the persistence of oliguria and loose stools on postoperative day 4, despite supportive care, raised suspicion of fecal debris in the urosac bag. Urine microscopy confirmed the presence of stool, leading to the insertion of a wide-bore Foley catheter for bladder irrigation, which yielded feculent fluid.
Diagnosing a CVF can be challenging owing to the limitations of conventional imaging techniques, which often fail to adequately visualize small fistula tracks. Several clinical studies recommend the use of CT scanning as a primary diagnostic tool owing to its high sensitivity in identifying a CVF and demonstrating its association with adjacent soft tissue structures[6,19,20]. Specifically, CT scans of the abdomen using both oral and intravenous contrast can detect fistulas in approximately 76% of cases and identify underlying causes in approximately 94%. In our case, a CT urogram with cystogram revealed a CVF at the sigmoid colon, attributed to diverticulitis. CT findings indicative of acute diverticulitis include localized bowel wall thickening (> 4 mm) and increased soft tissue density in the pericolonic fat, resulting from inflammation. Signs of a CVF on CT include contrast extravasation into the urinary bladder or the presence of gas in the bladder, particularly in the absence of recent catheterization[3,11,18]. Colonoscopy is highly ef
The primary treatment for CVF is surgical intervention. However, if a patient is clinically unstable owing to an untreated infection, it should be addressed prior to fistula repair, as was done in our case. A single-stage resection with primary anastomosis is often acceptable for benign CVF. Nevertheless, a multistage approach may be necessary for patients at risk of anastomotic leaks or those unable to endure prolonged surgeries[3]. Laparoscopic resection of CVF resulting from diverticulitis is feasible in experienced hands, as seen in our case, where a laparotomy was performed. Prompt recognition and management of acute diverticulitis and its complications are especially crucial in patients < 50 years of age as research indicates that they often experience a more aggressive disease course[3,21]. This group is more prone to recurrent diverticulitis, exacerbating the risk of complications such as perforation and CVF formation. The patient in our case has been under follow-up for 6 months post-procedure and is currently symptom-free.
Recent literature on CVF highlights several key themes. Diagnosis remains a challenge, with CT imaging and the poppy seed test serving as valuable tools for identification. A growing body of evidence supports the use of minimally invasive surgical techniques, particularly robotic-assisted surgery, which appears to have a lower conversion rate to open procedures than conventional laparoscopy. Although surgical resection is regarded as the definitive treatment, conservative approaches using antibiotics and urinary drainage might be suitable for certain patients at high risk for surgery or who have limited life expectancy. Finally, for complex malignant CVF, the use of neoadjuvant chemotherapy before surgery is being explored to reduce the tumor size and improve surgical outcomes. The management of CVF continues to focus on transitioning to minimally invasive surgical methods. While laparoscopic surgery is well-established and has been shown to be safe and effective with favorable outcomes, robotic-assisted surgery is gaining attention as a promising alternative. The enhanced dexterity and superior visualization of the robotic platform may lead to a lower conversion rate to open surgery, especially in technically challenging dissections with dense adhesions. Moreover, robotic surgery has been associated with shorter hospital stays and improved recovery, although the operative times may be longer. The choice between laparoscopic and robotic approaches often depends on the surgeon’s experience and the complexity of the individual case.
CVF, regardless of its etiology, presents a complex and challenging clinical issue for diagnosis and management. Limited research has been conducted on the incidence of CVF within the Indian population. Overall, diverticular disease is relatively uncommon among Indians, and only a small number of these cases present as CVF. This case highlights the importance of considering CVF in patients with atypical presentations, even in the absence of a prior history of abdo
| 1. | Dong C, Pan X, Wei L, Man X, Zhou Z, Huang Y, Wang X, Qi L, Xue F, Li Y. Colon cancer with colovesical fistula: A report of four cases and a literature review. Oncol Lett. 2023;25:158. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 2. | Seeras K, Qasawa RN, Akbar H, Lopez PP. Colovesical Fistula. 2023 Jul 16. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan. [PubMed] |
| 3. | Dufera RR, Tolu-Akinnawo O, Maliakkal BJ. Colovesical Fistula Complicating the First Symptomatic Episode of Acute Diverticulitis in a Young Adult. Cureus. 2023;15:e35082. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 4. | Scarpignato C, Barbara G, Lanas A, Strate LL. Management of colonic diverticular disease in the third millennium: Highlights from a symposium held during the United European Gastroenterology Week 2017. Therap Adv Gastroenterol. 2018;11:1756284818771305. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 40] [Cited by in RCA: 27] [Article Influence: 3.4] [Reference Citation Analysis (4)] |
| 5. | Shahedi K, Fuller G, Bolus R, Cohen E, Vu M, Shah R, Agarwal N, Kaneshiro M, Atia M, Sheen V, Kurzbard N, van Oijen MG, Yen L, Hodgkins P, Erder MH, Spiegel B. Long-term risk of acute diverticulitis among patients with incidental diverticulosis found during colonoscopy. Clin Gastroenterol Hepatol. 2013;11:1609-1613. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 359] [Cited by in RCA: 322] [Article Influence: 24.8] [Reference Citation Analysis (4)] |
| 6. | Keller-Biehl L, Yu KR, Smith-Harrison L, Timmerman W, Rivers J, Miller T. Colovesical Fistula: A 28 year experience at a major United States Department of Veterans Affairs Medical Center. Surg Pract Sci. 2022;11:100100. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 7. | Cripps H. The Passage of Air and Fæces from the Urethra. Edinb Med J. 1888;33:1026-1027. |
| 8. | Martinolich J, Croasdale DR, Bhakta AS, Ata A, Chismark AD, Valerian BT, Canete JJ, Lee EC. Laparoscopic Surgery for Diverticular Fistulas: Outcomes of 111 Consecutive Cases at a Single Institution. J Gastrointest Surg. 2019;23:1015-1021. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 30] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 9. | Gilshtein H, Yellinek S, Maenza J, Wexner SD. Surgical management of colovesical fistulas. Tech Coloproctol. 2020;24:851-854. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 10. | Zizzo M, Tumiati D, Bassi MC, Zanelli M, Sanguedolce F, Porpiglia F, Fiori C, Campobasso D, Castro Ruiz C, Bergamaschi FA, Maestroni UV, Carrieri G, Cormio L, Biolchini F, Palicelli A, Soriano A, Sassatelli R, Ascani S, Annessi V, Giunta A. Management of colovesical fistula: a systematic review. Minerva Urol Nephrol. 2022;74:400-408. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 19] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 11. | Ramakrishnan R, Kapoor P, Ravindrakumar C. Colovesical fistula: A case report and review of literature. Sri Ramachandra J Med. 2013;6:24-26. |
| 12. | Di Buono G, Bonventre G, Buscemi S, Randisi B, Romano G, Agrusa A. The colovescical fistula in diverticular disease: Laparoscopic approach in two different cases. Int J Surg Case Rep. 2020;77S:S112-S115. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 13. | Ranjan N, Ahmed A, Rohit K, Singh M, Tiwary R, Kumar V. Colovesical Fistulae Due to Diverticular Disease of a Sigmoid Colon: A Case Report. UroToday Int J. 2013;6:art 61. [DOI] [Full Text] |
| 14. | Jain M, Wagh S, Balsarkar DJ. Colovesical fistula: a rare complication of diverticulitis in young male. J Clin Diagn Res. 2015;9:PD17-PD18. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 15. | Kumar R, Pradhan U, Agarwal PN, Singh GJ, Verma I. An unusual case of colovesical fistula. Sch J Med Case Rep. 2020;8:971-973. [DOI] [Full Text] |
| 16. | Kadam S, Kundargi VS, Patil S, Patil B, Guru N, Jain A. Colovesical Fistula: A Rare Cause Of Recurrent Urinary Tract Infection In Young Male Managed Conservatively. Indian J Case Rep. 2019;5:252-253. [DOI] [Full Text] |
| 17. | Narayanaswamy S, Goradia R, Bhujbal S, Patwardhan S. Unique case of colovesical fistula in a renal allograft recipient. BMJ Case Rep. 2023;16:e254534. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 18. | El-Haddad HM, Kassem MI, Sabry AA, Abouelfotouh A. Surgical protocol and outcome for sigmoidovesical fistula secondary to diverticular disease of the left colon: A retrospective cohort study. Int J Surg. 2018;56:115-123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 15] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 19. | Ing A, Lienert A, Frizelle F. Medical image. CT colonography for colovesical fistula. N Z Med J. 2008;121:105-108. [PubMed] |
| 20. | Golabek T, Szymanska A, Szopinski T, Bukowczan J, Furmanek M, Powroznik J, Chlosta P. Enterovesical fistulae: aetiology, imaging, and management. Gastroenterol Res Pract. 2013;2013:617967. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 113] [Cited by in RCA: 108] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 21. | Khan A, Hawkins AT. Challenging Surgical Dogma: Controversies in Diverticulitis. Surg Clin North Am. 2021;101:967-980. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (0)] |