Copyright: ©Author(s) 2026.
World J Nephrol. Mar 25, 2026; 15(1): 115252
Published online Mar 25, 2026. doi: 10.5527/wjn.v15.i1.115252
Published online Mar 25, 2026. doi: 10.5527/wjn.v15.i1.115252
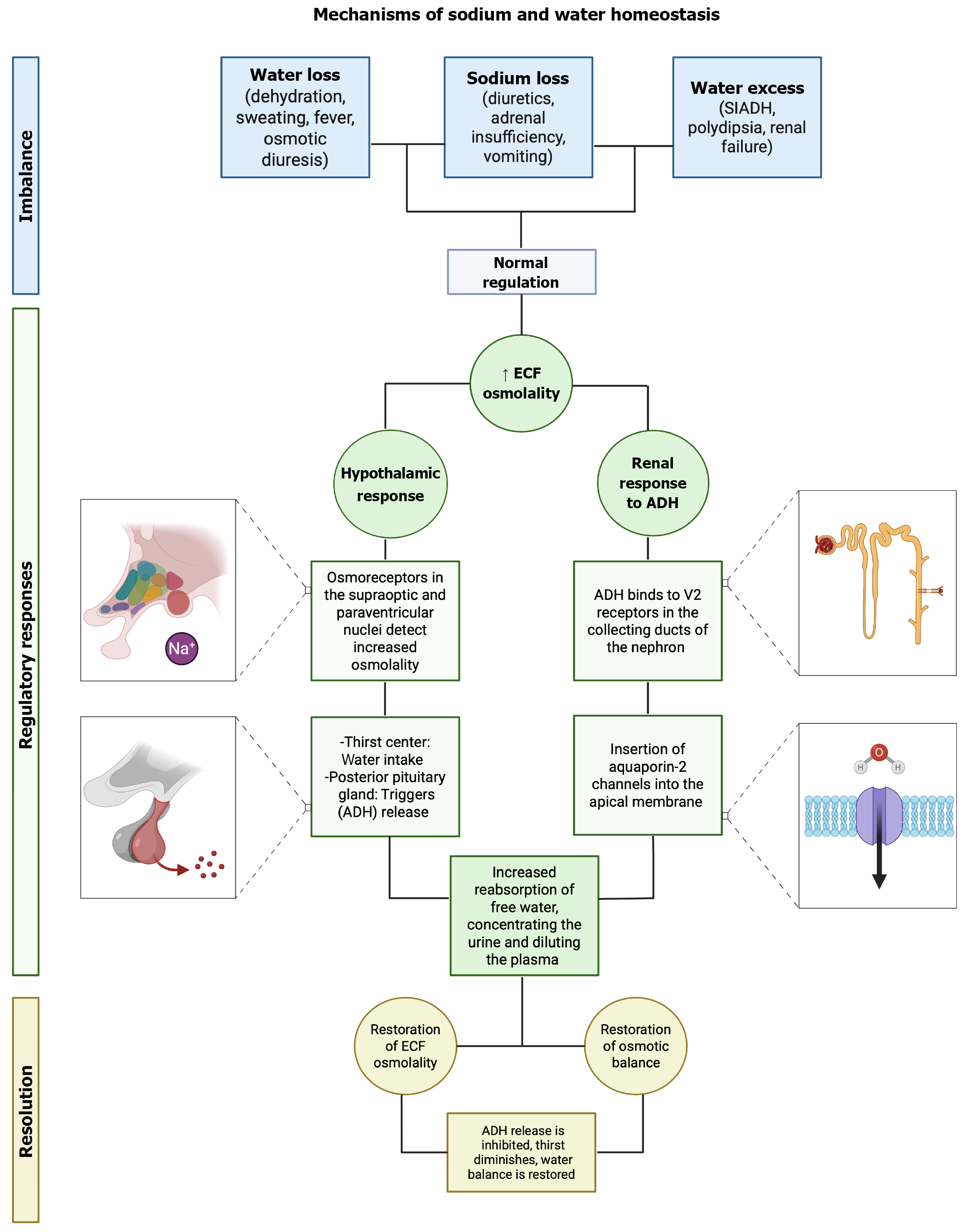
Figure 1 Mechanisms of sodium and water homeostasis.
Schematic representation of the physiological regulation of sodium and water balance under conditions of water loss, sodium loss, or water excess. Osmoreceptor activation in the hypothalamus and subsequent vasopressin (antidiuretic hormone) release from the posterior pituitary increase renal water reabsorption via V2 receptors and aquaporin-2 channel insertion, restoring extracellular fluid osmolality and osmotic equilibrium. SIADH: Syndrome of inappropriate antidiuretic hormone; ECF: Extracellular fluid; ADH: Antidiuretic hormone.
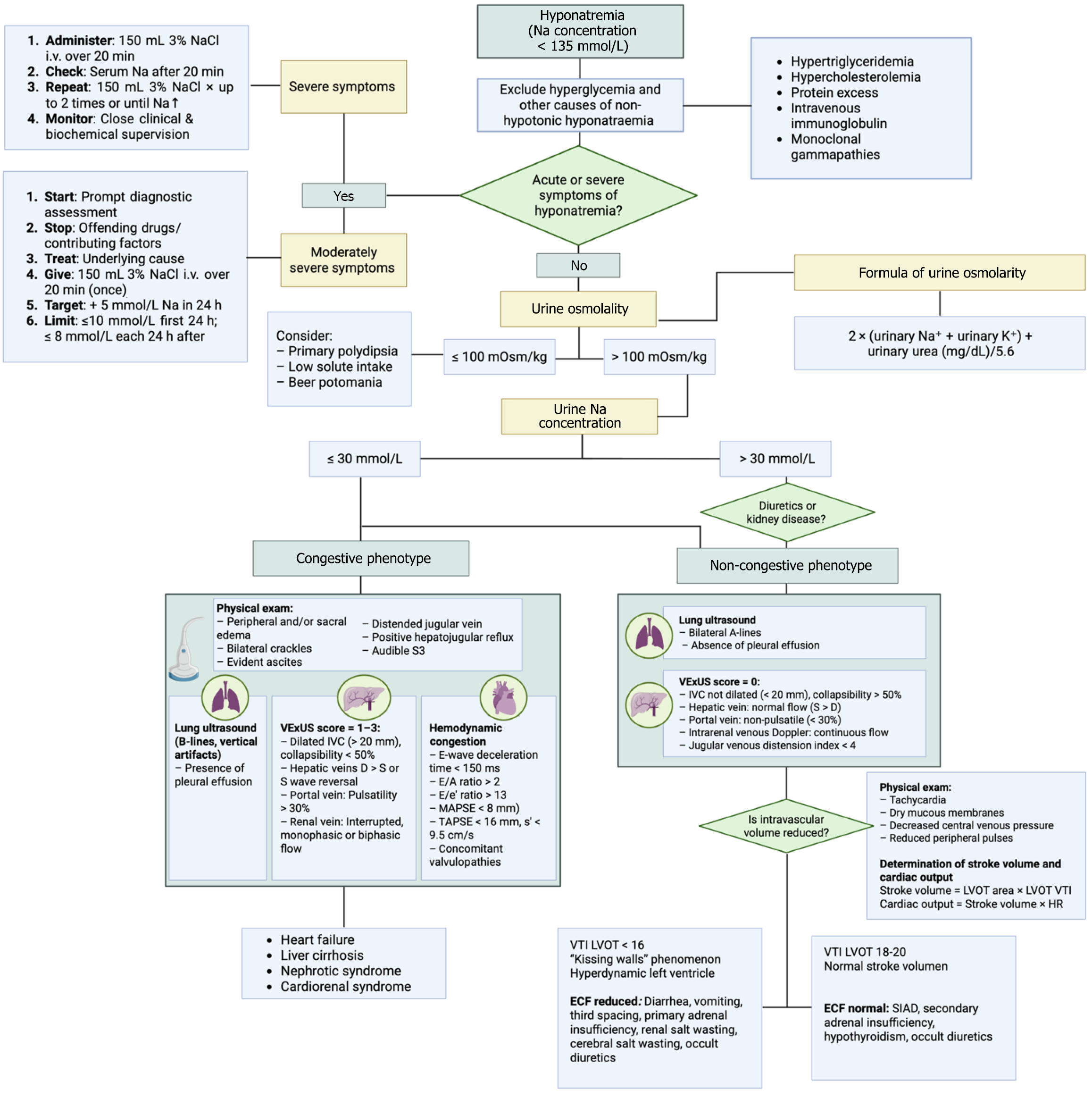
Figure 2 Diagnostic approach and phenotypic classification of hyponatremia.
Adapted from Eljazzar et al[38]. Algorithm outlining the stepwise evaluation of hyponatremia based on clinical severity, urine osmolality, and urine sodium concentration. A urinary sodium ≤ 30 mmol/L typically suggests low effective arterial volume; however, this does not always equate to true venous congestion. Differentiating congestive from non-congestive phenotypes requires a comprehensive assessment of volemic status, where point-of-care ultrasound plays a critical role in identifying hemodynamic congestion through evaluation of the inferior vena cava, hepatic, portal, and intrarenal venous flow patterns. IV: Intravenous; VExUS: Venous excess ultrasound; IVC: Inferior vena cava; E/A: Early to late diastolic transmitral flow velocity ratio; E/e’: Eatio of early mitral inflow velocity to early diastolic mitral annular velocity; MAPSE: Mitral annular plane systolic excursion; TAPSE: Tricuspid annular plane systolic excursion; LVOT: Left ventricular outflow tract; VTI: Velocity time integral; HR: Heart rate; ECF: Extracellular fluid; SIAD: Syndrome of inappropriate antidiuresis.
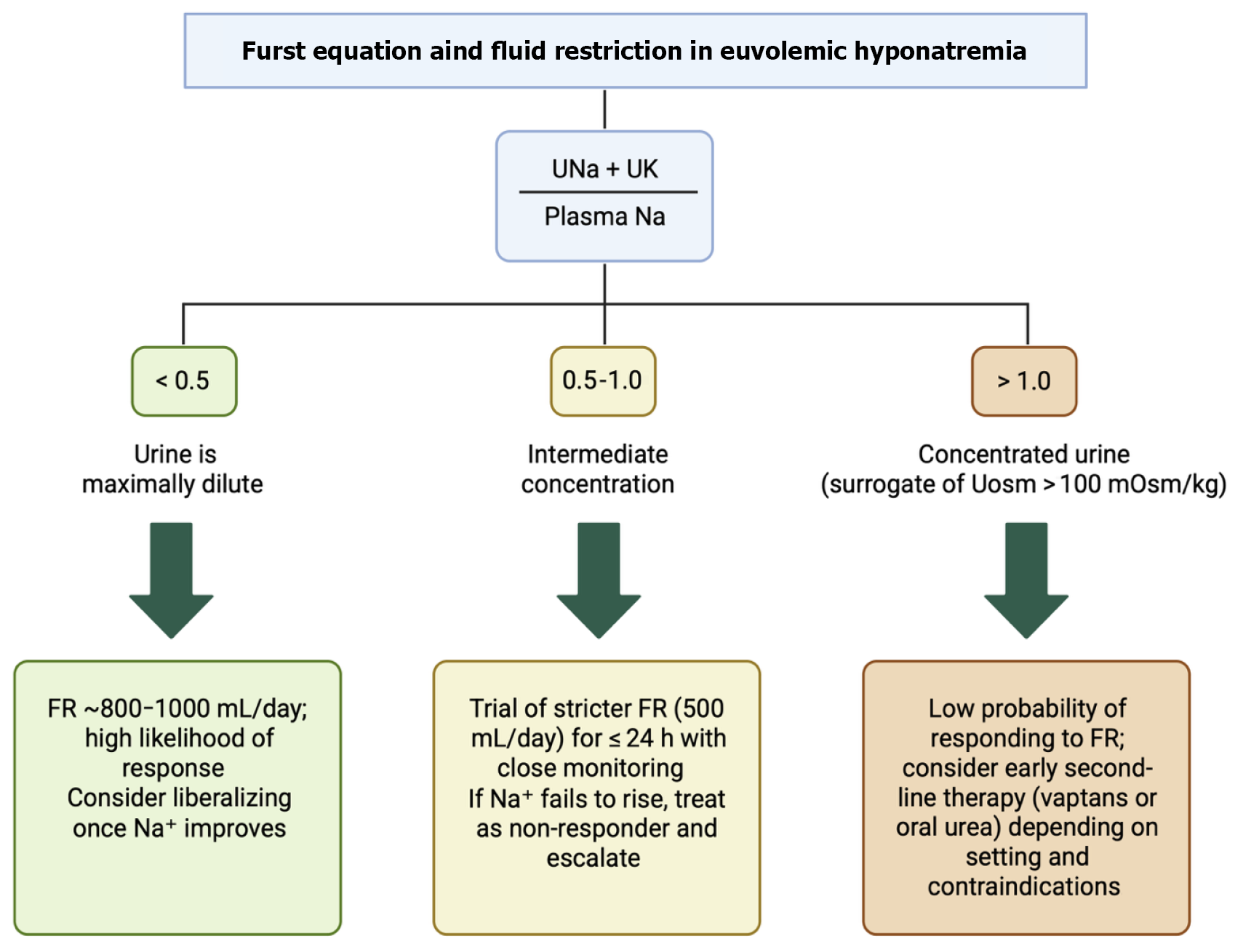
Figure 3 Furst equation and fluid restriction strategy in euvolemic hyponatremia.
The Furst equation provides a practical estimation of urine tonicity relative to plasma sodium concentration and helps anticipate the likelihood of response to fluid restriction (FR). A value < 0.5 indicates maximally dilute urine and high probability of correction with standard FR (approximately 800-1000 mL/day). Intermediate values (0.5-1.0) suggest partial concentration and warrant a stricter trial of FR (approximately 500 mL/day) under close monitoring. Ratios > 1.0 reflect concentrated urine (surrogate for urine osmolality > 100 mOsm/kg), indicating poor response to FR and the need for early consideration of second-line therapies (urea or vasopressin receptor antagonists). Una: Urinary sodium concentration; Uk: Urinary potassium concentration; FR: Fluid restriction.
- Citation: Martínez-Sánchez FD, Gutierrez-Rosas LE, Barranco-Hernandez LH, Gonzalez-Alvarez G, Bastida-Castro LA, Rocha-Haro A, Barrientos-Cabrera G, Martínez-Cabrera CF, Balderas-Juarez J, Salinas-Ramirez MA, Hernandez-Castillo JL. Hyponatremia: Evolving diagnostics and emerging therapeutics in clinical practice. World J Nephrol 2026; 15(1): 115252
- URL: https://www.wjgnet.com/2220-6124/full/v15/i1/115252.htm
- DOI: https://dx.doi.org/10.5527/wjn.v15.i1.115252