Copyright: ©Author(s) 2026.
World J Nephrol. Mar 25, 2026; 15(1): 114185
Published online Mar 25, 2026. doi: 10.5527/wjn.v15.i1.114185
Published online Mar 25, 2026. doi: 10.5527/wjn.v15.i1.114185
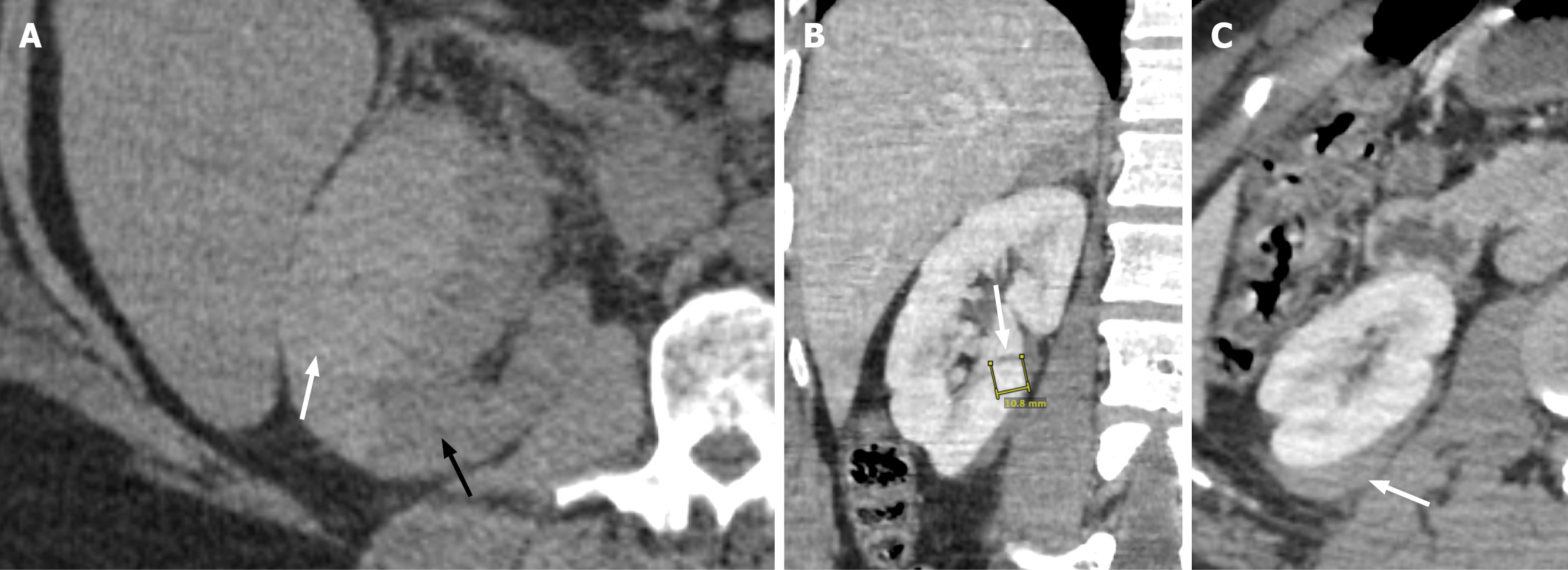
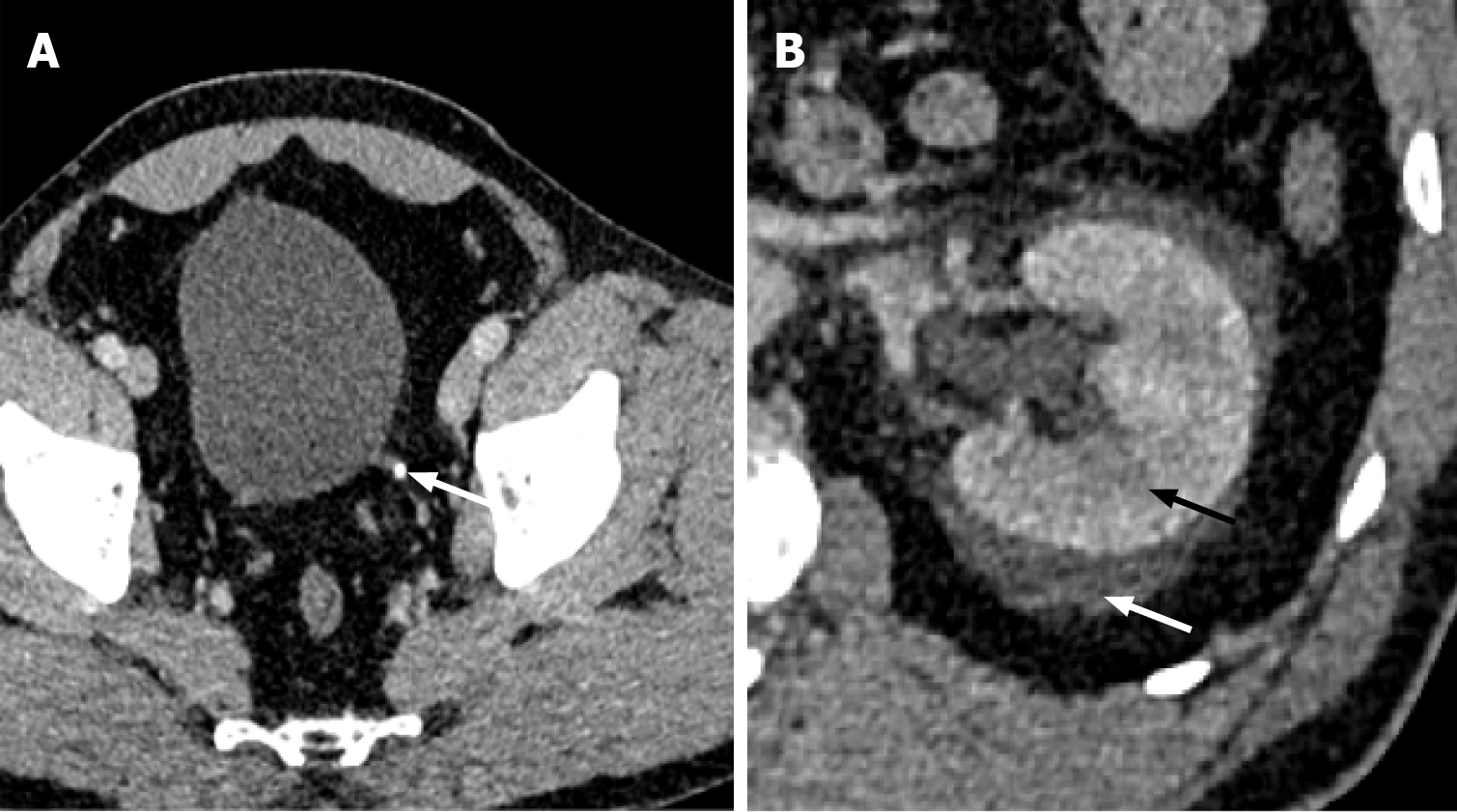
Figure 1 Grade I and II renal Injury.
A: Axial view of the non-contrast enhanced computed tomography of the right kidney demonstrates a lentiform-shaped hyperattenuating subcapsular collection (white arrow) with mass effect on the adjacent renal parenchyma (black arrow), compatible with renal subcapsular hematoma and grade I renal injury; B: Coronal view contrast-enhanced computed tomography of the right kidney demonstrates a linear hypoattenuation (white arrow) measuring > 1 cm in length, consistent with renal laceration; C: The axial view shows a slightly iso- to hyperdense perirenal collection (white arrow), consistent with a perirenal hematoma. The constellation of findings is compatible with grade II renal injury.
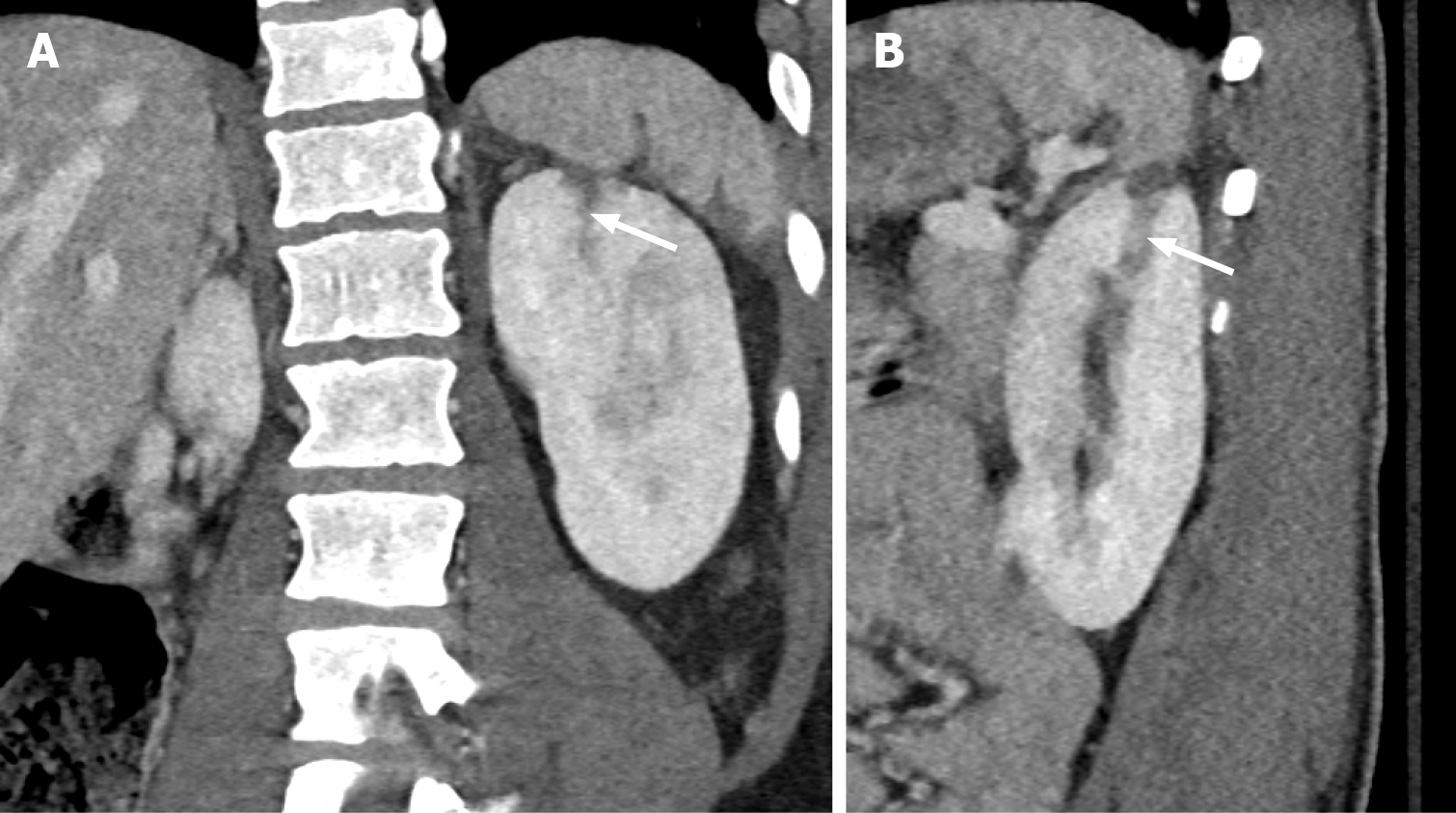
Figure 2 Grade III renal Injury.
A: Coronal view; B: Sagittal view. A linear area of hypoattenuation of 1 cm depth in the left superior renal pole (white arrow), consistent with renal laceration corresponding to grade 3 renal injury.
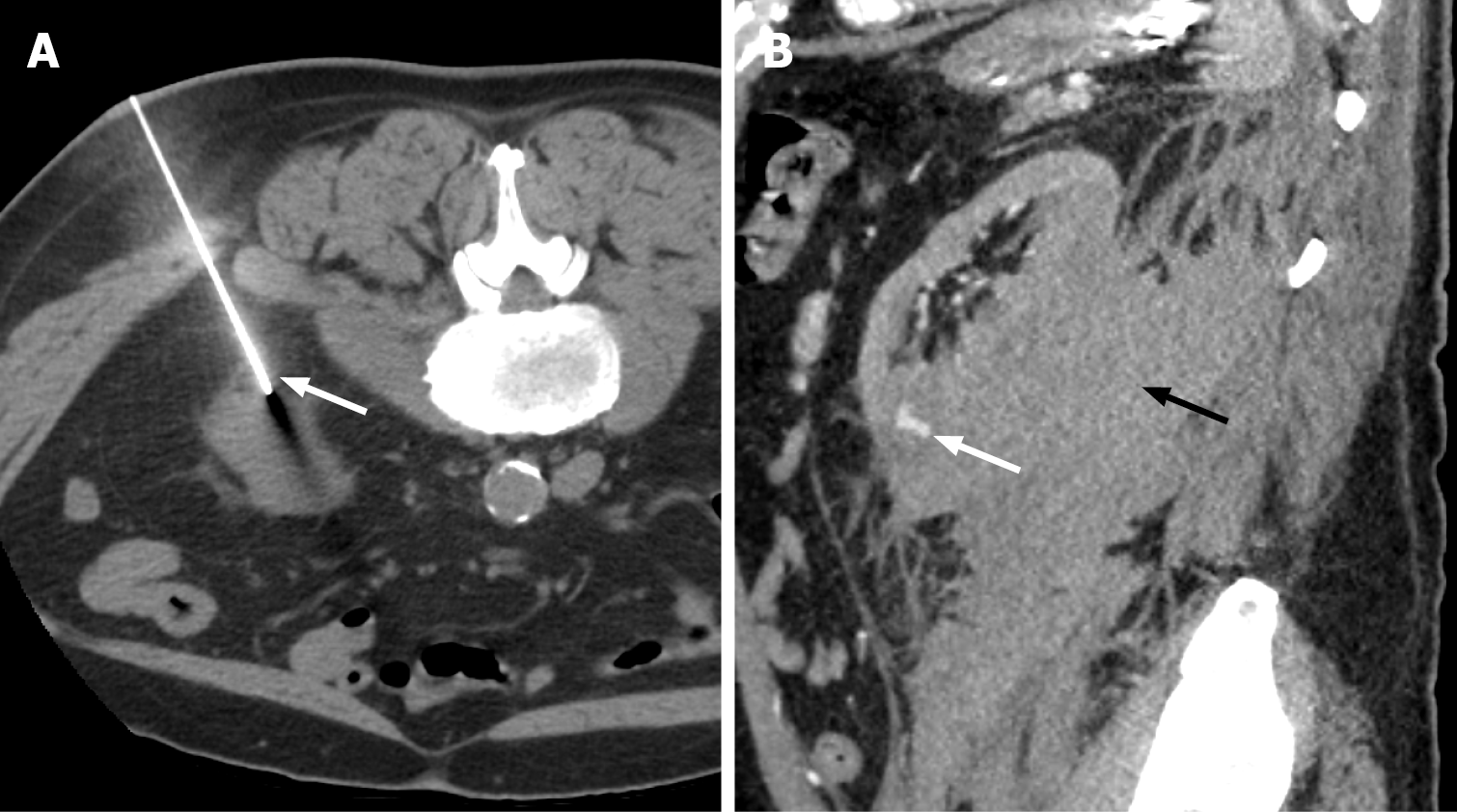
Figure 3 Grade III renal Injury.
A: Non-contrast computed tomography obtained during biopsy of the left kidney with the patient in the prone position, demonstrating the biopsy needle with the tip abutting the left inferior renal pole (white arrow); B: Follow-up arterial phase computed tomography abdomen 48 hours later demonstrates left subcapsular and retroperitoneal haemorrhage (black arrow) with an area of contrast blush in the inferior renal pole consistent with pseudoaneurysm (white arrow).
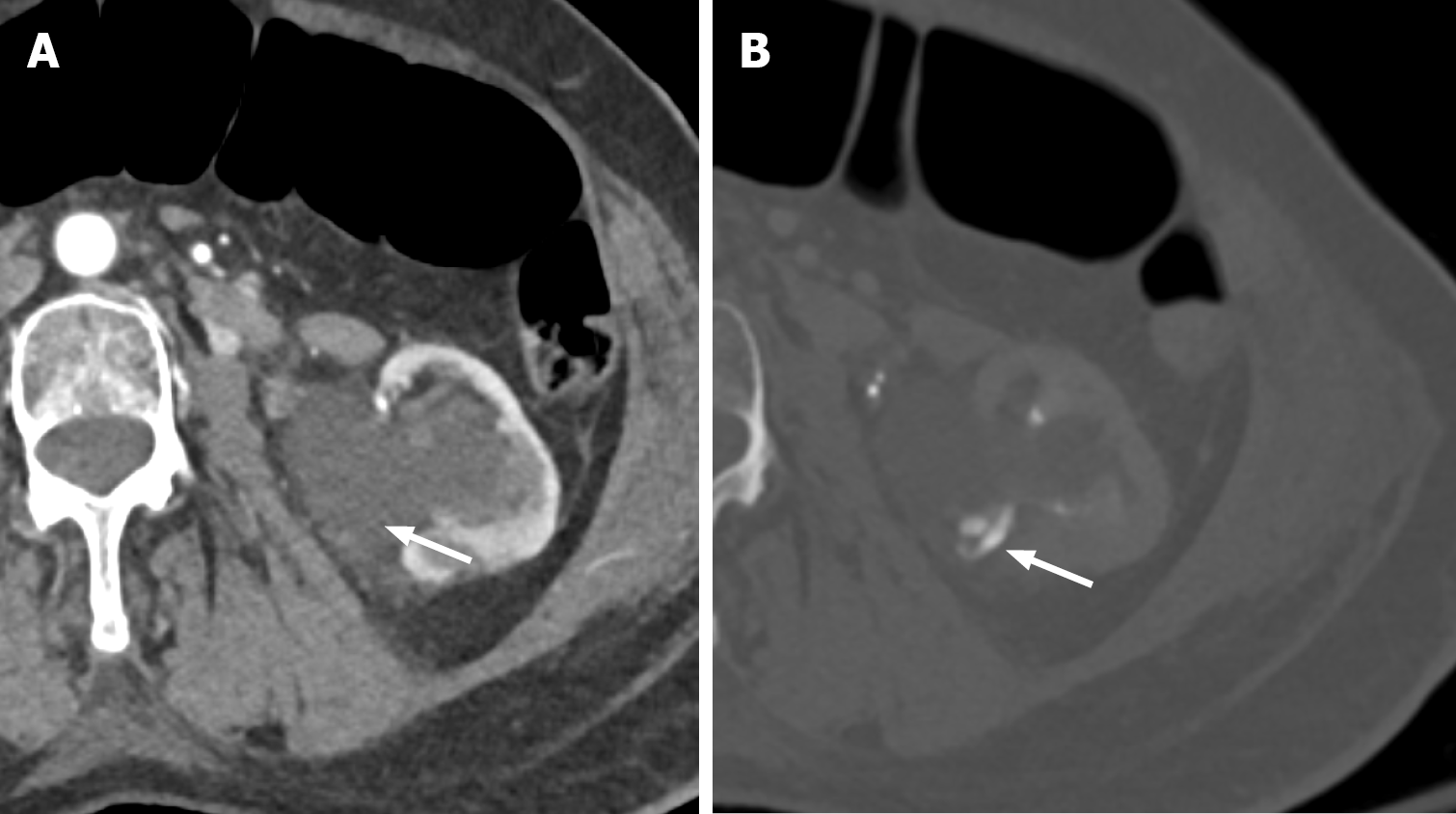
Figure 4 Grade IV renal injury.
A: Axial computed tomography of the abdomen in corticomedullary phase demonstrating renal hilar injury with diffuse hypoattenuating fluid collection in the hilum, concerning for collecting system involvement (white arrow); B: On delayed phase imaging, note the contrast extravasation from the renal collecting system into the hypoattenuating collection consistent with urine extravasation (white arrow). These findings correspond to grade IV renal injury.
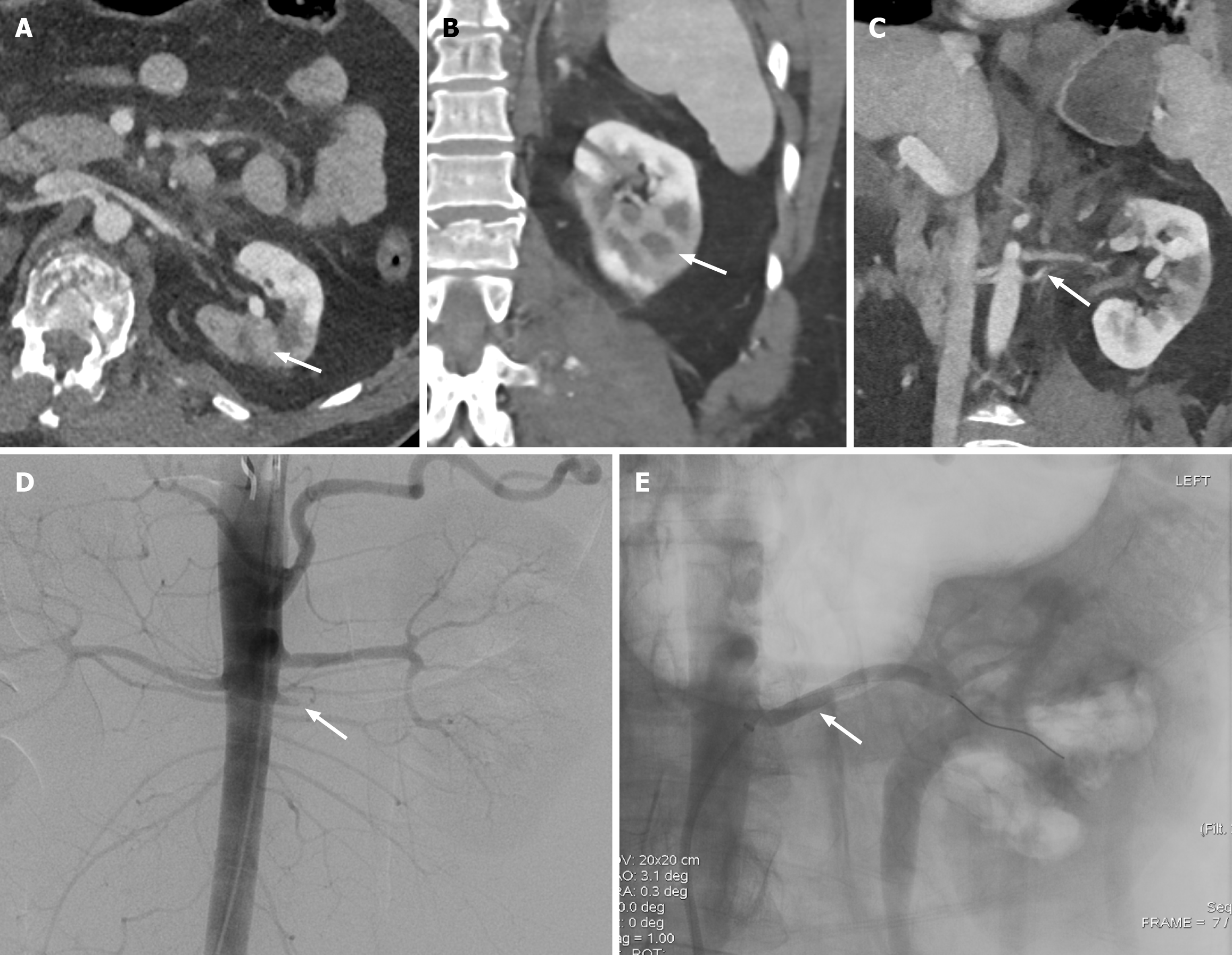
Figure 5 Renal infarct.
A: Axial computed tomography of the abdomen shows segmental absent enhancement of the left kidney (white arrow); B: Coronal computed tomography of the abdomen shows segmental absent enhancement of the left kidney (white arrow); C: The infarction is attributed to the thrombosis of the accessory left renal artery (white arrow). These findings correspond to grade IV renal injury; D: Patient underwent left renal angiogram confirming the thrombotic occlusion of the accessory left renal artery (white arrow); E: Successful deployment of the bare-metal stent with improved flow (white arrow).
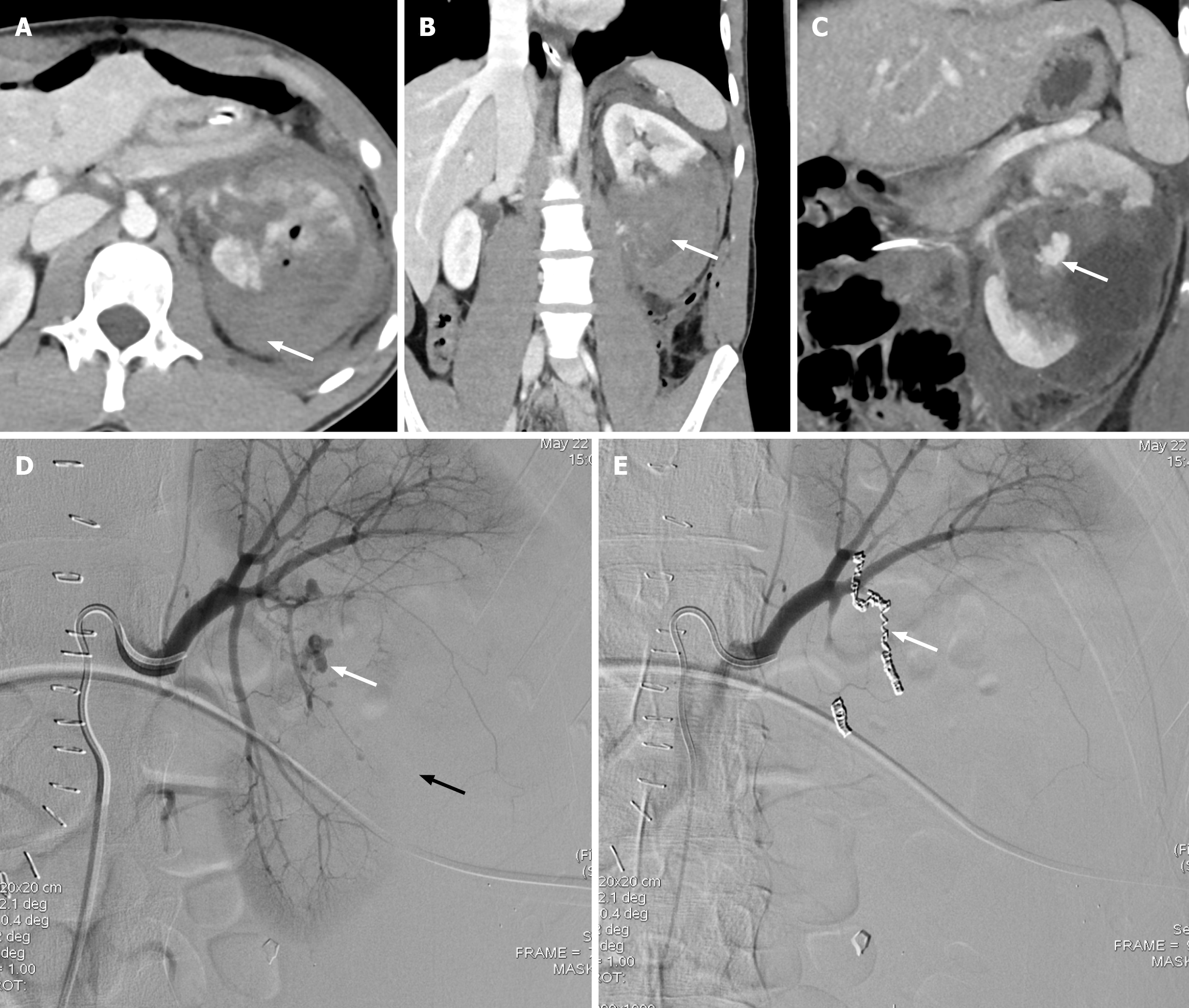
Figure 6 Grade V renal injury.
A: Axial computed tomography (CT) of the abdomen shows a shattered left kidney with foci of air and a large perinephric hematoma (white arrow); B: Coronal CT shows devascularization of the interpolar and inferior pole of the left kidney (white arrow); C: Coronal CT shows contrast blush concerning for active bleeding (white arrow). The patient was immediately taken to the interventional radiology suite; D: Left renal angiogram shows pseudoaneurysm arising from the segmental branch of the renal artery (white arrow). Note the absent perfusion of the interpolar and a part of the inferior pole regions of the left kidney (black arrow); E: Successful coil embolization of the actively bleeding renal artery branches (white arrow).
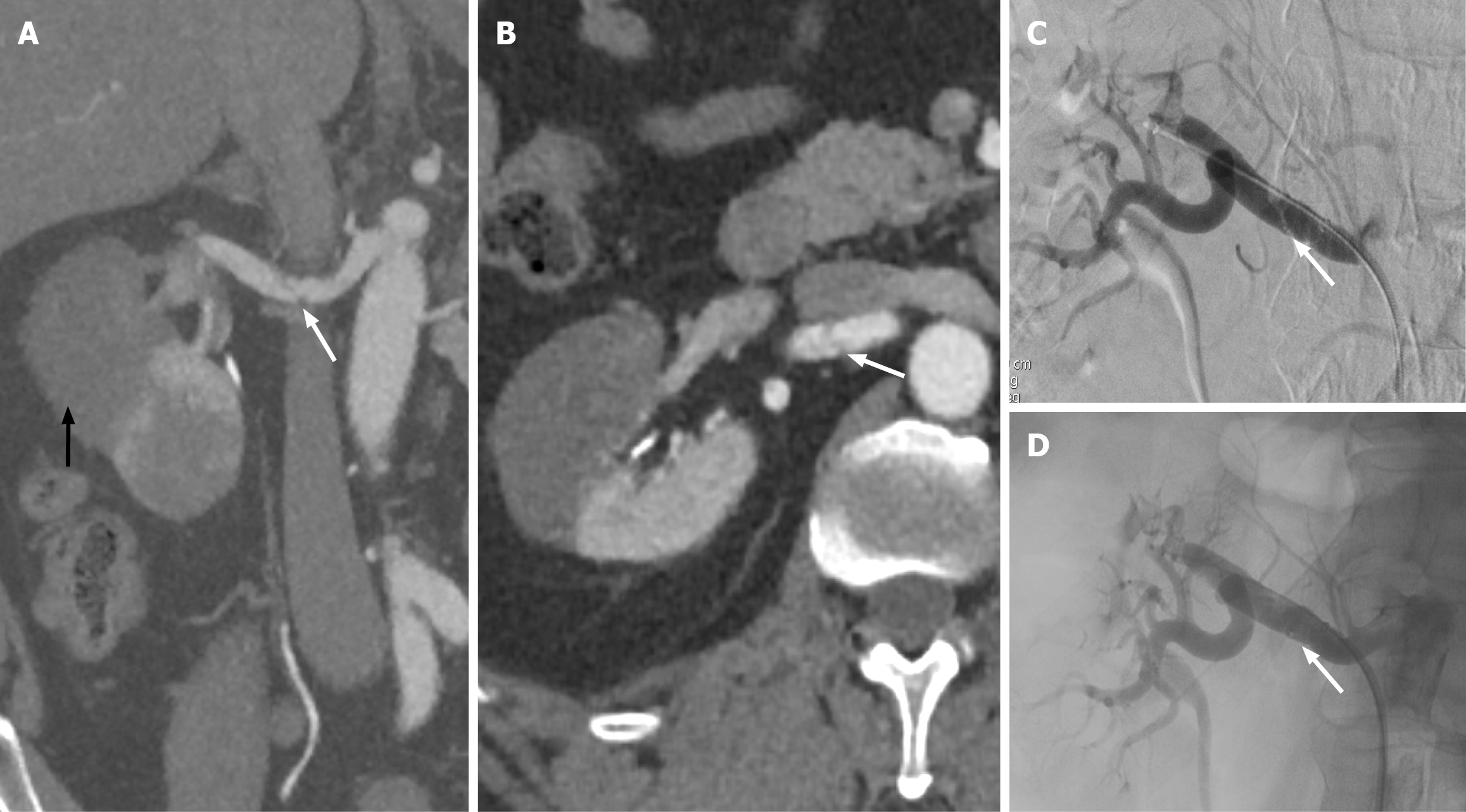
Figure 7 Renal artery dissection.
A: Coronal view computed tomography of the abdomen in arterial phase demonstrates linear hypoattenuation within the right mid renal artery, suggesting dissection (white arrow). Note the infarcted kidney (black arrow); B: Axial view confirming the dissection flap within the right renal artery (white arrow); C: Right renal angiogram demonstrating the dissection flap within the right renal artery (white arrow); D: Successful stenting of the right renal artery (white arrow).
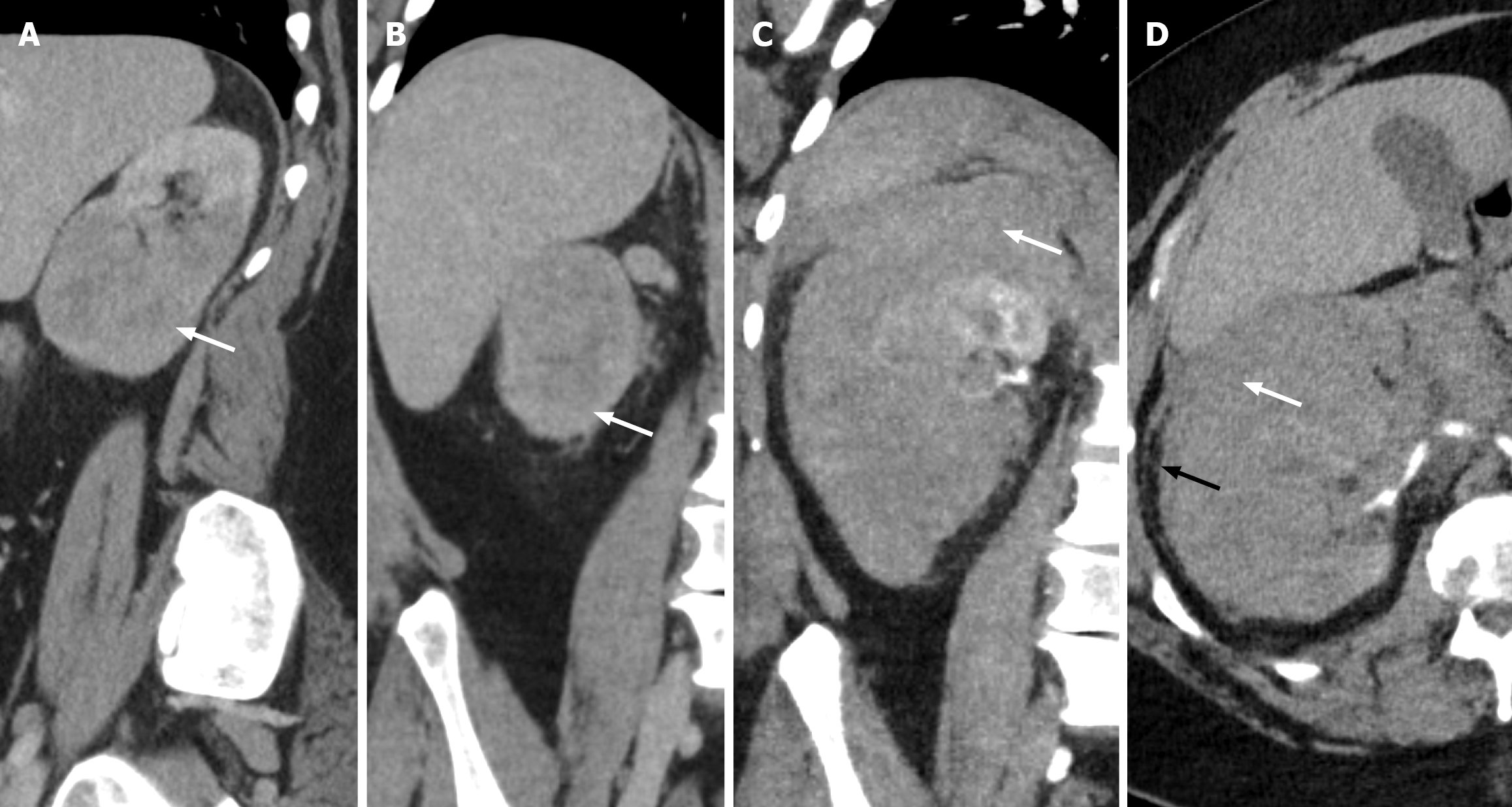
Figure 8 Spontaneous renal hemorrhage.
A and B: Sagittal (A) and (B) computed tomography of the right kidney demonstrating a homogenous hypoattenuating mass infiltrating the inferior portion of the right renal parenchyma, consistent with renal lymphoma (white arrow). A few months later, the patient presented with acute abdominal/right flank pain; C and D: Coronal (C) and (D) axial computed tomography demonstrating a hyperdense subcapsular collection consistent with spontaneous renal haemorrhage and subcapsular hematoma (white arrow) with slight extension into the perinephric space (black arrow).
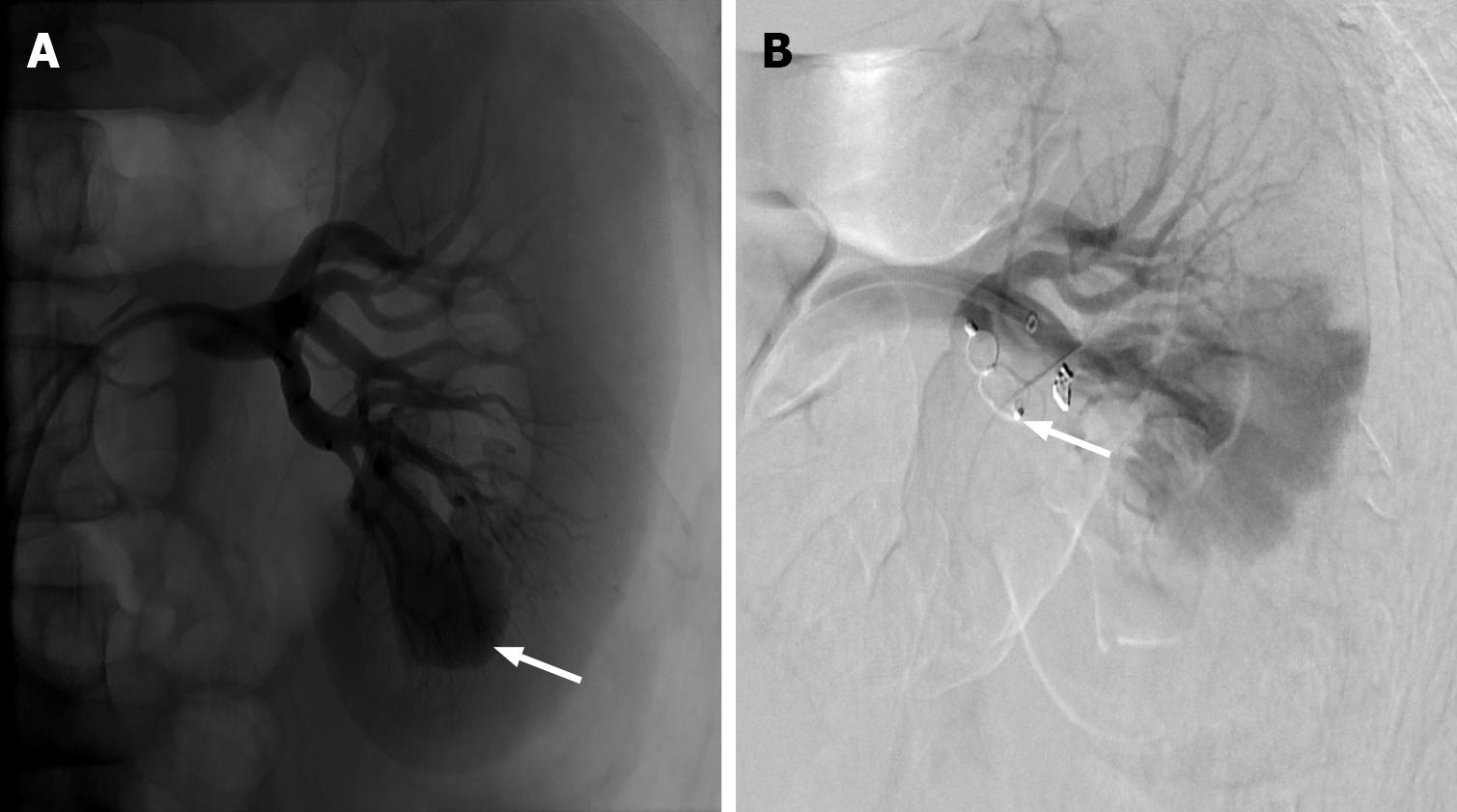
Figure 9 Renal arterio-venous fistula.
A: Left renal artery angiogram demonstrating a large inferior pole pseudoaneurysm (white arrow); B: Subsequent treatment with an Amplatzer plug (white arrow) and a single coil, with successful occlusion of the pseudoaneurysm. Additionally, early venous filling was noted during examination, concerning for traumatic renal arterio-venous fistula.
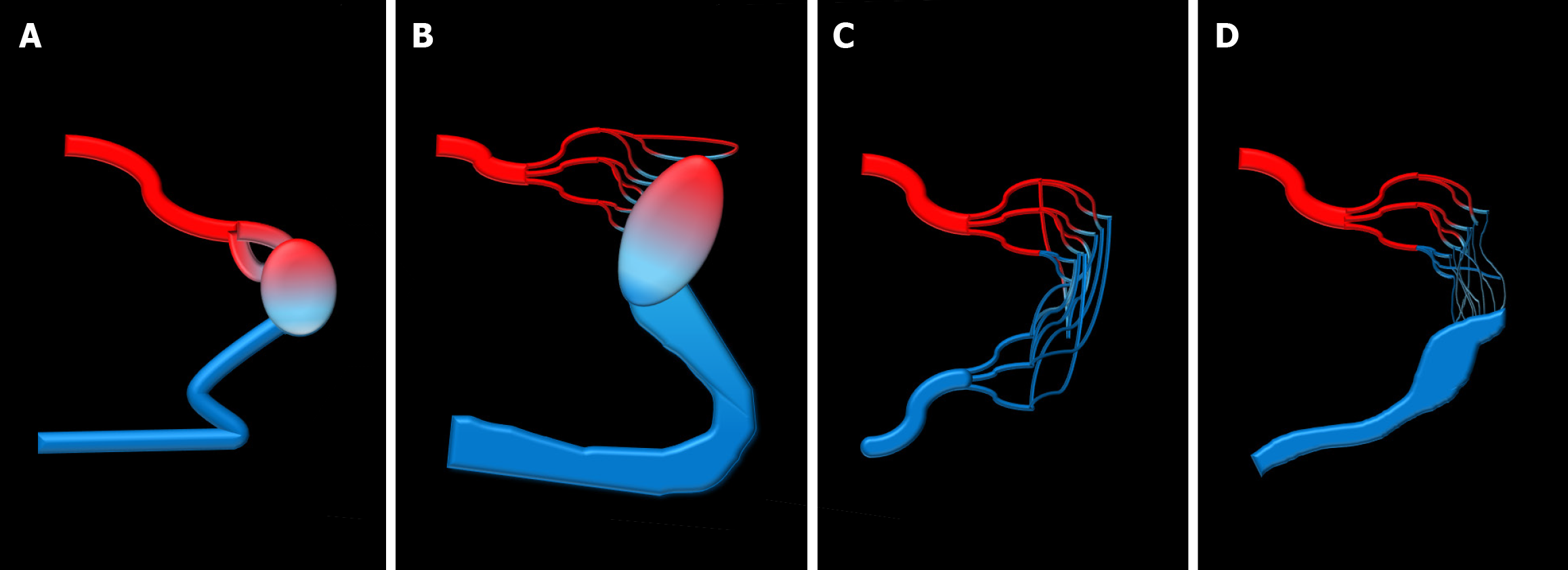
Figure 10 Cho’s classification of arteriovenous malformation.
A: Type 1: Arterio-venous fistula; B: Arterio-venulous fistula; C: Non-dilated arterio-venulous fistula; D: Dilated arterio-venulous fistula.
Figure 11 Obstructive uropathy.
A: Axial computed tomography in portal venous phase demonstrates an obstructing calculus (white arrow) within the left distal ureter close to the ureterovesical junction; B: Axial computed tomography at the level of the kidneys demonstrates a delayed nephrogram (indicated by the black arrow) with perinephric edema (indicated by the white arrow) due to obstructive uropathy.
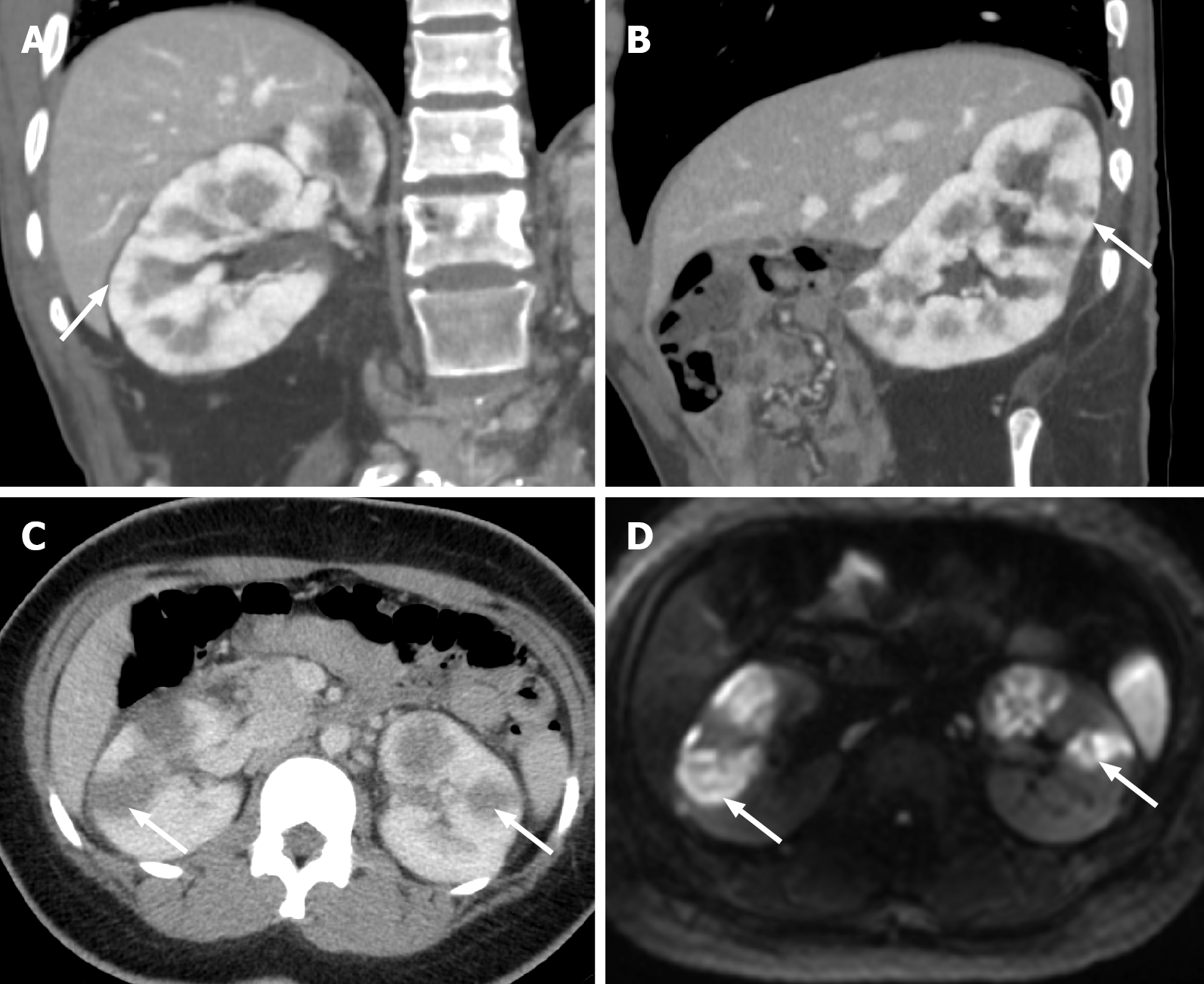
Figure 12 Acute pyelonephritis.
A: Coronal computed tomography in portal venous phase demonstrating striated renal cortical enhancement suggesting acute pyelonephritis (white arrows); B: Sagittal computed tomography in portal venous phase demonstrating striated renal cortical enhancement suggesting acute pyelonephritis (white arrows); C: Axial computed tomography of a different patient with acute pyelonephritis shows multifocal hypoattenuating lesions bilaterally concerning for abscesses (white arrows); D: These findings can be confirmed on magnetic resonance imaging, where the abscesses demonstrate diffusion restriction (indicated by white arrows).
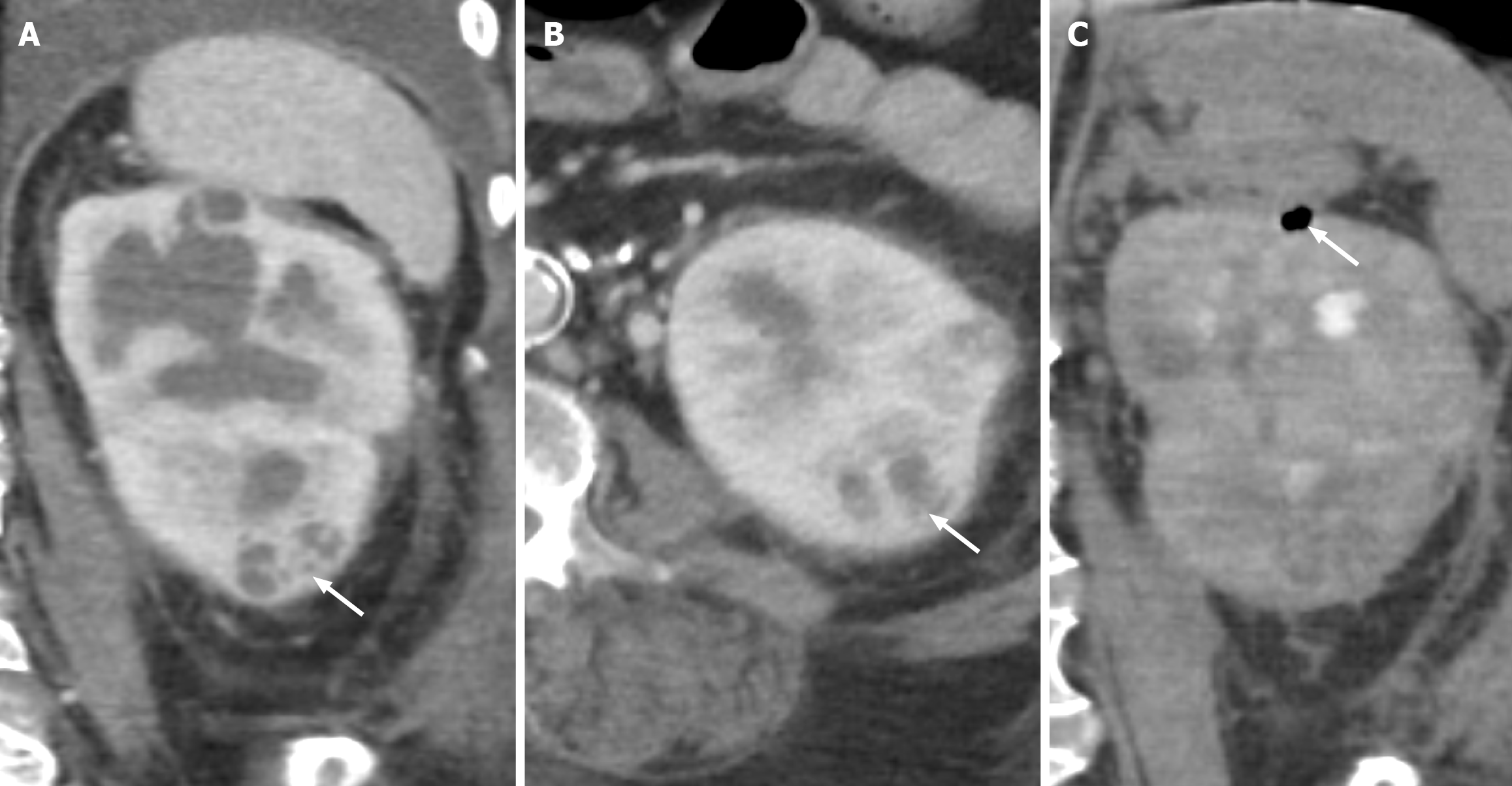
Figure 13 Emphysematous pyelonephritis.
A: Coronal computed tomography of the abdomen demonstrating heterogeneous enhancement of the left kidney with multifocal hypoattenuating renal cortical lesions (white arrow); B: Axial computed tomography of the abdomen demonstrating heterogeneous enhancement of the left kidney with multifocal hypoattenuating renal cortical lesions (white arrow); C: Coronal view demonstrating a focus of cortical air within the left superior renal pole (white arrow). These findings are consistent with emphysematous pyelonephritis, characterized by abscess formation.
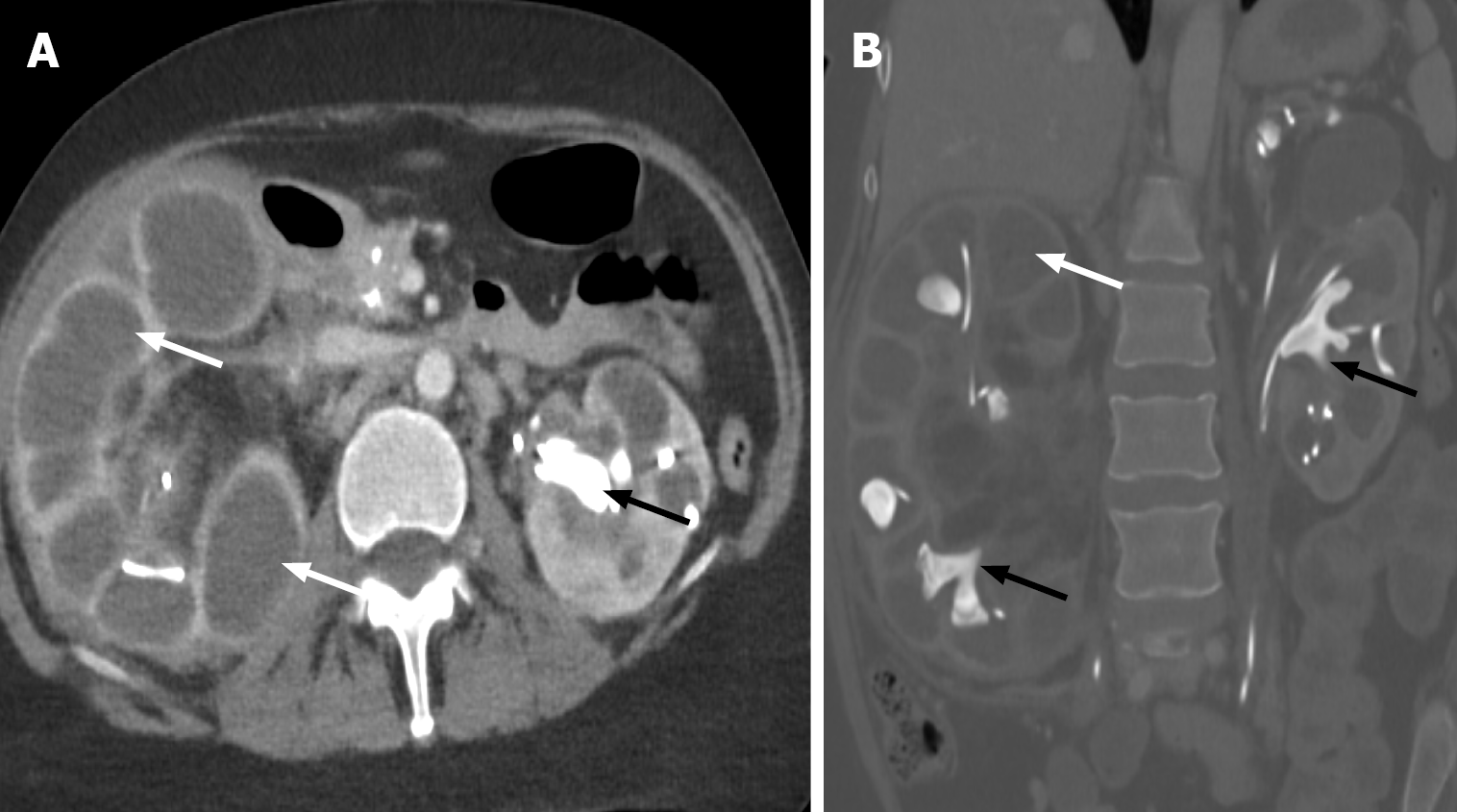
Figure 14 Xanthogranulomatous pyelonephritis.
A and B: Axial (A) and coronal (B) computed tomography demonstrating diffusely dilated renal calyceal system with renal cortical thinning (bear paw sign) (white arrow). Multiple staghorn calculi are filling the calyces (indicated by the black arrow). These findings are consistent with xanthogranulomatous pyelonephritis.
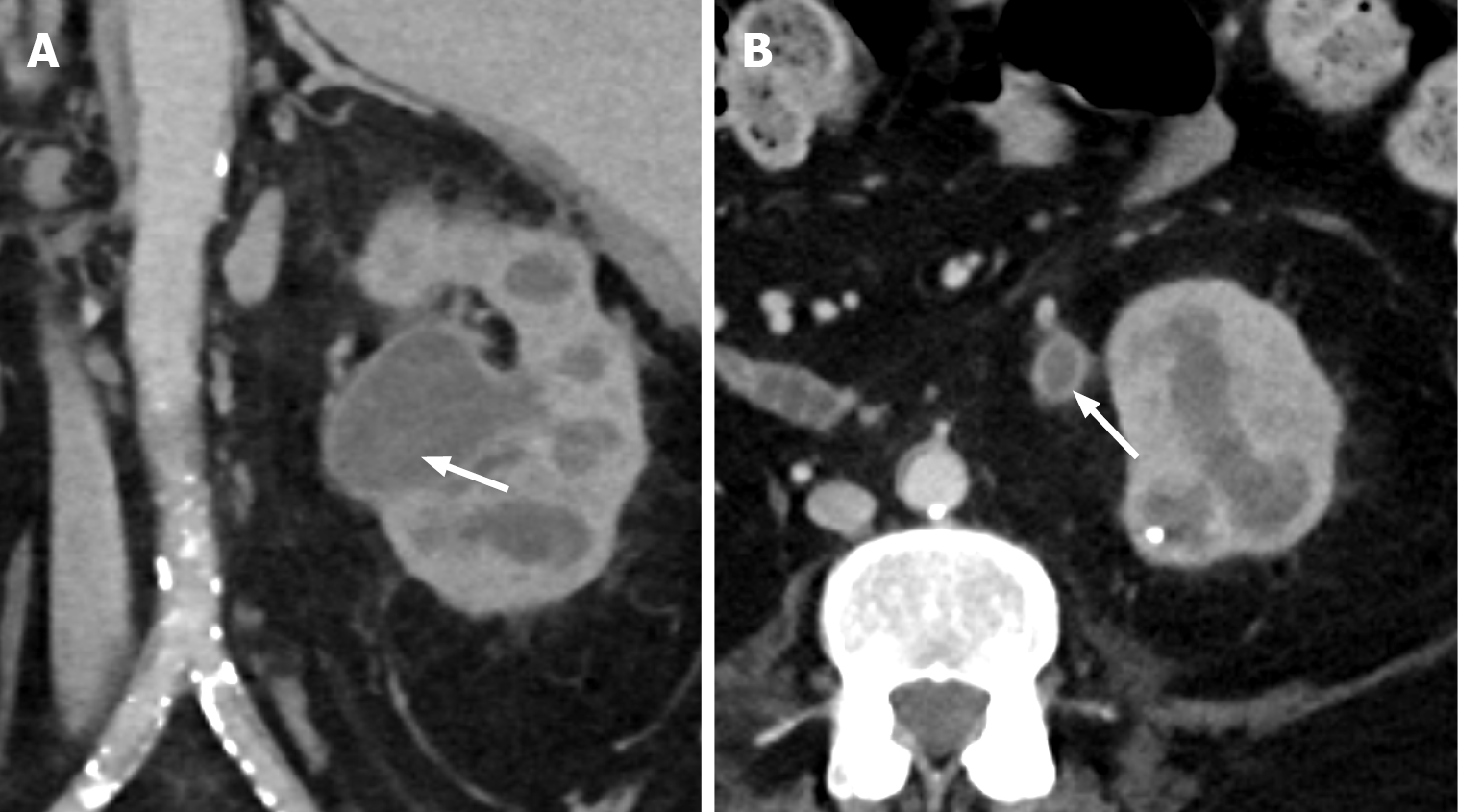
Figure 15 Pyonephrosis.
A and B: Coronal (A) and axial (B) computed tomography in portal venous phase demonstrating dilated left renal pelvis with diffuse urothelial enhancement (white arrows). These findings are consistent with pyonephrosis.
- Citation: Vulasala SSR, Robinson J, Engel C, Zulia Y, Sharma A, Gopireddy DR, Adler G, Virarkar M. Computed tomography of renal emergencies: A comprehensive diagnostic guide for radiology residents. World J Nephrol 2026; 15(1): 114185
- URL: https://www.wjgnet.com/2220-6124/full/v15/i1/114185.htm
- DOI: https://dx.doi.org/10.5527/wjn.v15.i1.114185