Published online Apr 19, 2026. doi: 10.5498/wjp.v16.i4.111713
Revised: November 10, 2025
Accepted: December 22, 2025
Published online: April 19, 2026
Processing time: 202 Days and 1 Hours
Anxiety and depression adversely affect clinical outcomes in children with bron
To clarify the relationship between emotional state, treatment compliance, and symptom improvement in children with bronchopneumonia.
A total of 306 children with bronchopneumonia (January 2022 to January 2025) were included. Clinical data on emotional state (the Depression Self-Rating Scale for Children and the Screen for Child Anxiety Related Emotional Disorders), treatment compliance, and symptom improvement (time to wheezing, fever, lung rales, and cough resolution) were collected. Anxiety/depression status across different clinical characteristics was assessed, and its correlation with treatment compliance and symptom improvement was analyzed.
Depression Self-Rating Scale for Children and Screen for Child Anxiety Related Emotional Disorders scores were significantly higher in children with a disease duration > 4 days and moderate illness but showed no significant correlation with gender or age. Anxious or depressed children showed markedly lower overall compliance, with longer symptom-resolution times.
In pediatric bronchopneumonia, adverse emotional states are closely associated with poorer treatment compliance and slower symptom improvement. Reducing anxiety or depression may enhance compliance and alleviate sym
Core Tip: In 306 children with bronchopneumonia, emotional state was evaluated in relation to treatment compliance and symptom improvement. Anxiety/depression was strongly associated with lower compliance and slower symptom recovery, supporting targeted clinical psychological intervention to enhance children’s compliance and consequently accelerate rehabilitation. The findings of this study provide an important breakthrough for the rapid recovery of children with bron
- Citation: Ai CL, Xu D, Guan XF. Association of emotional state with treatment compliance and clinical symptom improvement in pediatric bronchopneumonia patients. World J Psychiatry 2026; 16(4): 111713
- URL: https://www.wjgnet.com/2220-3206/full/v16/i4/111713.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i4.111713
Bronchopneumonia is a common pediatric respiratory tract infectious disease caused by invasion of peripheral lung tissue or bronchi by pathogens (e.g., pneumococcus, adenovirus, protozoa, and chlamydia)[1,2]. Its pathogenesis is complex and may involve lung injury and inflammation mediated by the 3-phosphoinositide-dependent protein kinase 1/NOD-like receptor family pyrin domain-containing 3 axis[3]. Early symptoms post-infection are often subtle due to decreased lung capacity, weak cough reflex, relatively weak respiratory musculature, and low respiratory function[4], leading to delayed diagnosis and intervention, disease aggravation (e.g., marked lung rales)[5], greater treatment difficulty, and a higher risk of complications[6]. Meanwhile, bronchopneumonia-affected children commonly experience asthma, fever, cough, lung pain, and dyspnea, which significantly threaten health[7,8]. Due to the heavy disease burden, fear of treatment, and unfamiliar hospital environments, children’s emotional state is prone to anxiety and depression[9], which may decrease treatment compliance and impede symptom improvement[10,11].
To clarify the association between emotional state, treatment compliance, and symptom improvement, this study analyzed 306 children with bronchopneumonia to provide reliable evidence for optimizing clinical management. Existing research in this area remains limited, and this study offers clinically relevant findings that may guide refinement of treatment experience for affected children. Most children were aged 8-12 years for three reasons: First, this group has sufficient cognitive ability to complete the selected emotional assessment scales, supporting assessment effectiveness; second, this range helps minimize confounding from adolescent psychological and physiological factors; third, treatment compliance behaviors are obvious in this age range, facilitating observation of the correlation between emotion and cooperation.
A total of 306 children with bronchopneumonia admitted to Zhumadian Central Hospital from January 2022 to January 2025 were included.
Eligibility criteria: (1) Bronchopneumonia diagnosis confirmed by clinical and diagnostic evaluation[12]; (2) Age 8-12 years; age-appropriate cognitive and intellectual development; (3) Treatment-naive for bronchopneumonia; no preadmission history of psychiatric disorders (e.g., depression, mania, or schizophrenia); (4) No prior tuberculosis or respiratory tract infections; and (5) Complete case records available.
Exclusion criteria: (1) Drug allergy to medications used in this study; (2) Serious congenital disease (e.g., congenital heart disease); (3) Allergic diseases in active stage (e.g., allergic rhinitis and eczema); (4) Tuberculosis, respiratory infection, or respiratory failure before admission; (5) Serious liver, kidney, or other major organ disease; (6) Immune deficiency, malignancy; and (7) Autism or attention deficit hyperactivity disorder.
Emotional status: Depressive and anxiety symptoms were assessed using the Depression Self-Rating Scale for Children (DSRSC) and the Screen for Child Anxiety Related Emotional Disorders (SCARED), respectively[13]. The DSRSC includes 18 items with three response options, yielding a total score of 0-36; a score of > 15 indicates depression. The SCARED includes 41 items scored on three options, yielding a total score of 0-82; scores > 23 indicate anxiety.
Treatment compliance: Total treatment compliance = (full compliance + partial compliance) cases/total cases × 100%. Compliance was evaluated at treatment completion according to the following behavioral standards: (1) Full compliance: Quiet, fully cooperative, no crying, and no resistance behavior; (2) Partial compliance: Mild resistance and crying, relieved after appeasement, and adequate cooperation; and (3) Noncompliance: Marked resistance and persistent crying, and no cooperation.
Symptom improvement: Time to disappearance of wheezing, fever, lung rales, and cough post-treatment was recorded.
mean ± SD was used for describing continuous variables. Between-group comparisons used independent sample t-tests; within-group pre-post comparisons used paired t-tests. Counting data [n (%)] were analyzed using χ2 tests. Data were processed using SPSS version 22.0, with P < 0.05 indicating statistically significant differences.
Clinical data for 306 pediatric bronchopneumonia cases are summarized in Table 1. Among them, 160 were male (52.29%), with a mean age of 9.96 ± 1.38 years and a disease duration of 5.10 ± 2.13 days. Mild cases were 171 (55.88%). The DSRSC score was 14.92 (SD = 4.33) points and the SCARED score was 22.89 (SD = 5.89) points.
| Data | n = 306 |
| Sex | |
| Male | 160 (52.29) |
| Female | 146 (47.71) |
| Age (years) | 9.96 ± 1.38 |
| Illness duration (day) | 5.10 ± 2.13 |
| Disease severity | |
| Mild | 171 (55.88) |
| Moderate | 135 (44.12) |
| DSRSC (points) | 14.92 ± 4.33 |
| ≤ 15 | 173 (56.54) |
| > 15 | 133 (43.46) |
| SCARED (points) | 22.89 ± 5.89 |
| ≤ 23 | 174 (56.86) |
| > 23 | 132 (43.14) |
As shown in Table 2, DSRSC and SCARED scores did not differ significantly by gender or age (P > 0.05). Children with disease duration > 4 days and moderate severity had significantly higher DSRSC and SCARED scores (P < 0.05).
| Variable | DSRSC (points) | t value | P value | SCARED (points) | t value | P value |
| Sex | 0.787 | 0.432 | 0.311 | 0.756 | ||
| Male (n = 160) | 14.73 ± 4.17 | 22.99 ± 6.27 | ||||
| Female (n = 146) | 15.12 ± 4.50 | 22.78 ± 5.45 | ||||
| Age (years) | 0.975 | 0.330 | 0.102 | 0.919 | ||
| ≤ 10 (n = 127) | 14.63 ± 4.23 | 22.93 ± 6.09 | ||||
| > 10 (n = 179) | 15.12 ± 4.40 | 22.86 ± 5.75 | ||||
| Illness duration (day) | 2.016 | 0.045 | 6.921 | < 0.001 | ||
| ≤ 4 (n = 129) | 13.22 ± 3.98 | 20.35 ± 5.19 | ||||
| > 4 (n = 177) | 16.15 ± 4.16 | 24.74 ± 5.68 | ||||
| Disease severity | 4.050 | < 0.001 | 4.784 | < 0.001 | ||
| Mild (n = 171) | 14.05 ± 4.32 | 21.51 ± 5.70 | ||||
| Moderate (n = 135) | 16.02 ± 4.10 | 24.64 ± 5.66 |
Depression (Table 3) and anxiety (Table 4) were then assessed in relation to treatment compliance. We identified 133 children with depression (DSRSC > 15) vs 173 without depression, and 132 with anxiety vs 174 without anxiety. Overall compliance was higher in nondepressed children than in depressed children (95.38% vs 86.47%, P = 0.006), and in non-anxious vs anxious children (94.25% vs 87.88%, P = 0.048).
| Treatment compliance | Depression group (n = 133) | Non-depression group (n = 173) | χ2 value | P value |
| Complete compliance | 58 (43.61) | 95 (54.91) | ||
| Partial compliance | 57 (42.86) | 70 (40.46) | ||
| Non-compliance | 18 (13.53) | 8 (4.62) | ||
| Total compliance | 115 (86.47) | 165 (95.38) | 7.677 | 0.006 |
| Treatment compliance | Anxiety group (n = 132) | Non-anxiety group (n = 174) | χ2 value | P value |
| Complete compliance | 55 (41.67) | 98 (56.32) | ||
| Partial compliance | 61 (46.21) | 66 (37.93) | ||
| Non-compliance | 16 (12.12) | 10 (5.75) | ||
| Total compliance | 116 (87.88) | 164 (94.25) | 3.922 | 0.048 |
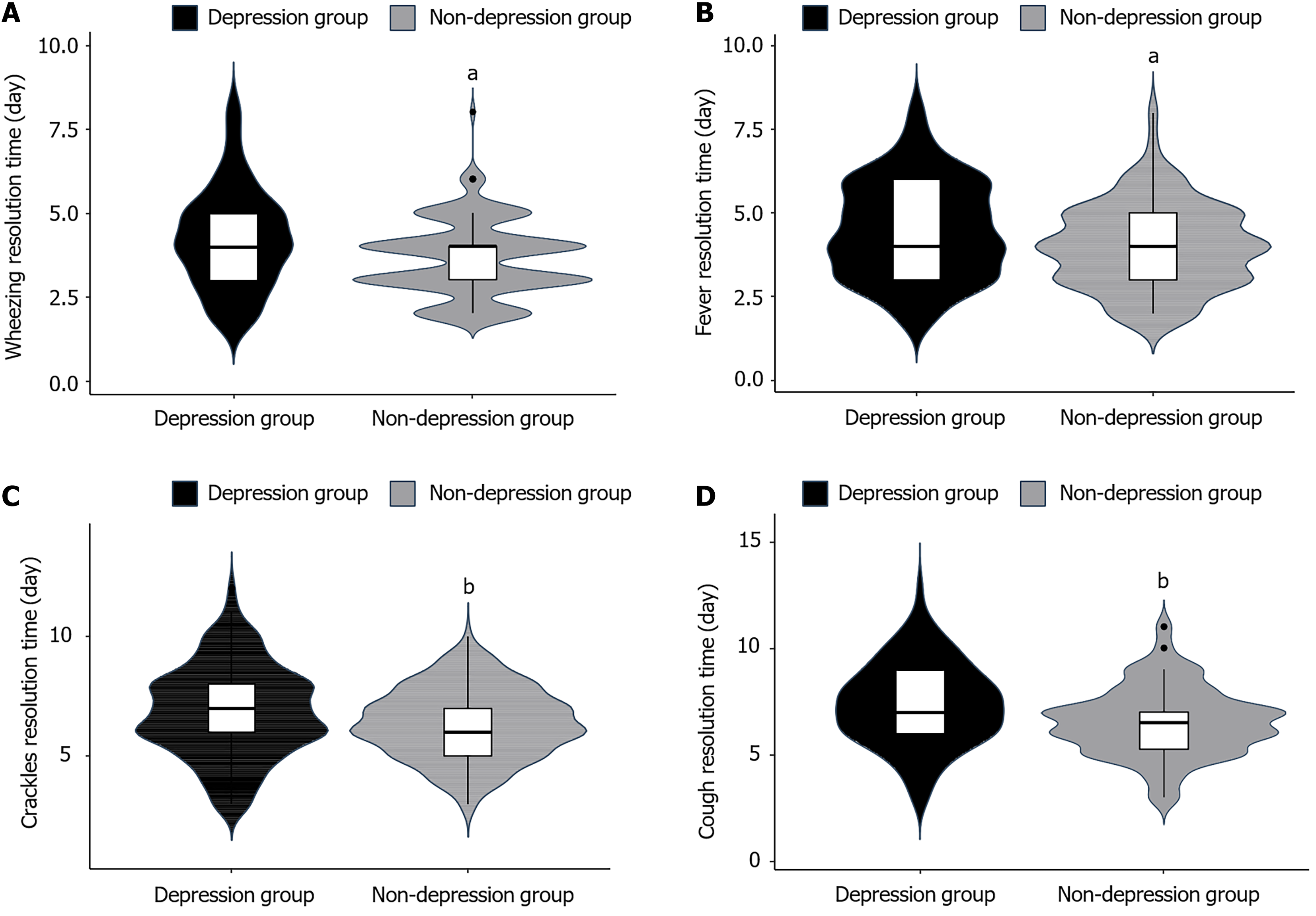
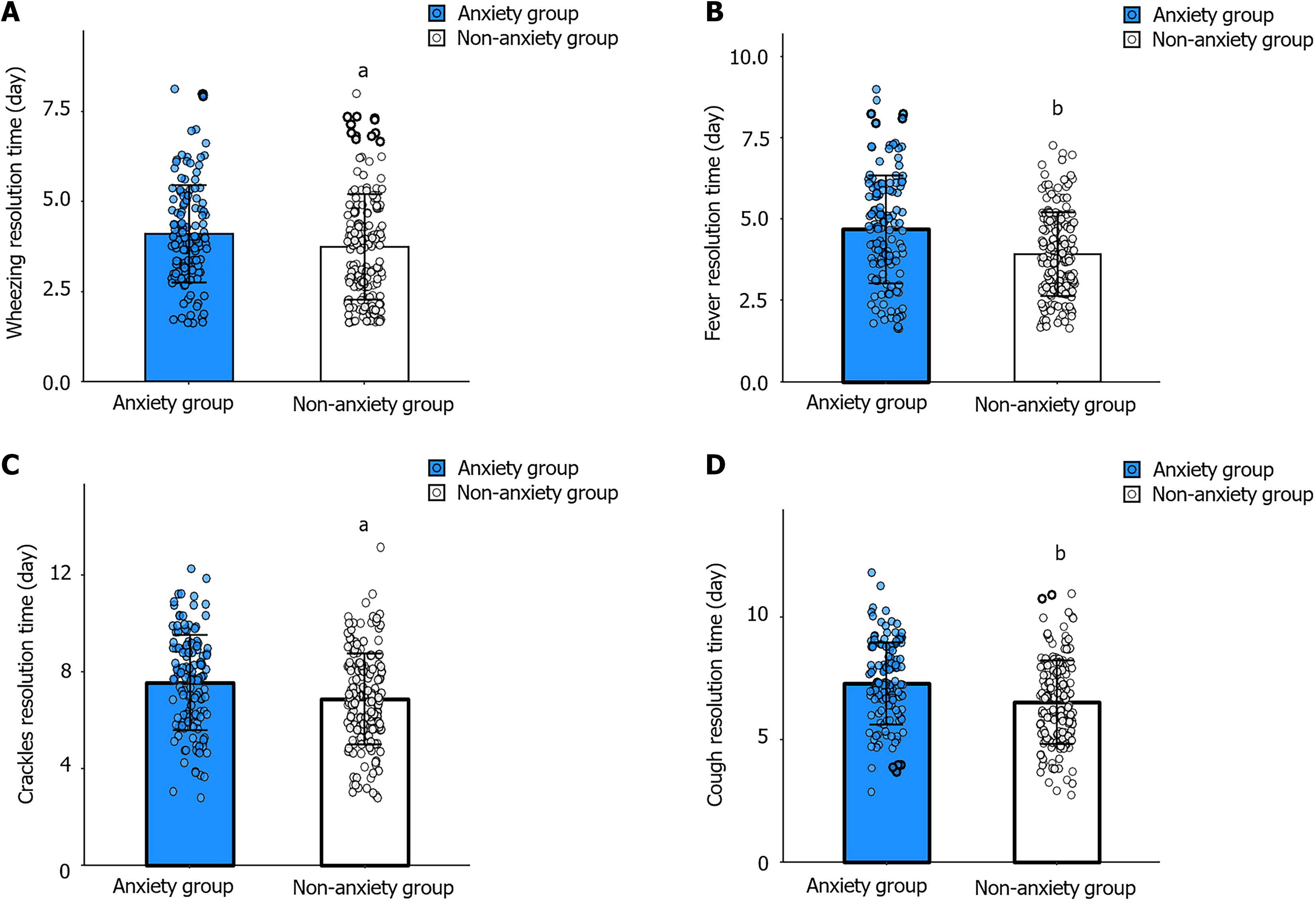
We further evaluated the relationship between depression/anxiety and symptom improvement (Figures 1 and 2). Times to resolution of wheezing, fever, lung rales, and cough were shorter in non-depression/non-anxiety groups than in their corresponding adverse emotion groups (P < 0.05).
Bronchopneumonia is a common pediatric pneumonia characterized by purulent pulmonary inflammation and substantial disease burden and cost[14,15]. This study demonstrates that emotional state in affected children is closely linked to treatment compliance and symptom improvement, underscoring the need to address depression/anxiety in clinical care.
We first compared DSRSC and SCARED scores across clinical characteristics. Neither score correlated with gender or age, but both were higher children with disease duration > 4 days and with moderate severity. Higher DSRSC and SCARED scores reflect more severe depression/anxiety[16]. Depression and anxiety in children with bronchopneumonia may involve the activation of the medial prefrontal cortex-lateral habenula circuit and the dorsal raphe subcortical projection subpopulation, respectively[17]. Longer disease duration (> 4 days) may amplify psychological burden due to prolonged disease-related discomfort symptoms[18], and greater severity may intensify stress, uncertainty, and functional restriction[19], thereby increasing susceptibility to negative emotions[20,21]. Consistent with this, Liu et al[22] reported that longer disease duration is associated with higher anxiety/depression risk in Chinese adults.
Additionally, depression and anxiety in pediatric bronchopneumonia correlated significantly with lower overall treatment compliance, declining from 95.38%/94.25% to 86.47%/87.88%. This indicates that depression and anxiety in such children are detrimental to overall compliance. Targeted psychological support may therefore help alleviate negative emotions and improve treatment compliance. Volpato et al[23] similarly reported lower medication compliance in patients with chronic obstructive pulmonary disease who suffer from depression, consistent with our findings. Sun et al[24] also demonstrated that heterogeneity of adolescent depression/anxiety symptoms correlates with executive dysfunction, where negative emotional states impair working memory and task completion. Together, these findings partially explain why depression and anxiety reduce treatment compliance in pediatric bronchopneumonia.
Our results also show that depression/anxiety symptoms in pediatric bronchopneumonia correlate with delayed resolution of wheezing, fever, pulmonary rales, and cough. Improving emotional state may therefore facilitate smooth recovery of related clinical symptoms, thus helping to shorten the recovery process. Depressive and anxiety symptoms have been associated with both blunted and exaggerated cortisol responses to stress, and dysregulated cortisol may disturb systemic inflammatory balance and delay lung function recovery[25,26].
This study has several limitations. First, although 306 cases were included, all were enrolled at a single center, possibly limiting representativeness. Future multicenter sampling from varied regions may improve result accuracy. Second, this study did not verify the causality between emotional state and treatment compliance or symptom improvement. Analyses addressing causal direction are needed. Third, potential family and environmental contributors to emotional state require further investigation to construct more comprehensive explanatory models and guide multidimensional psychological intervention design.
Emotional state in pediatric bronchopneumonia is strongly associated with treatment compliance and symptom improvement. Children with negative emotional symptoms typically exhibit reduced treatment compliance and longer recovery times. Proactive psychological care customized to these patients’ needs is therefore warranted to mitigate emotional distress and support more effective clinical recovery.
| 1. | Zhao D, Chen M, Shi K, Ma M, Huang Y, Shen J. A long short-term memory-fully connected (LSTM-FC) neural network for predicting the incidence of bronchopneumonia in children. Environ Sci Pollut Res Int. 2021;28:56892-56905. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 12] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 2. | Febbo J, Revels J, Ketai L. Viral Pneumonias. Radiol Clin North Am. 2022;60:383-397. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 3. | Yang M, Li L. Remimazolam attenuates inflammation in bronchopneumonia through the inhibition of NLRP3 activity by PDPK1 ubiquitination. Chem Biol Drug Des. 2024;103:e14438. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 4. | Ho SY, Zhou YT, Ho SY, Hu YL, Yen TY, Huang KA, Lu CY, Huang LM, Chang LY. Clinical Characteristics and Severity Predictors of Pediatric Adenovirus Infections. J Med Virol. 2025;97:e70248. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 5. | Fan F, Lv J, Yang Q, Jiang F. Clinical characteristics and serum inflammatory markers of community-acquired mycoplasma pneumonia in children. Clin Respir J. 2023;17:607-617. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 97] [Cited by in RCA: 79] [Article Influence: 26.3] [Reference Citation Analysis (0)] |
| 6. | Yao W, Zhang X, Xu F, Cao C, Liu T, Xue Y. The therapeutic effects of naringenin on bronchial pneumonia in children. Pharmacol Res Perspect. 2021;9:e00825. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 28] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 7. | Ling Y, Yang D, Yang S. Clinical characteristics, early blood biochemical indicators, and prognostic status of children with bronchopneumonia. Medicine (Baltimore). 2023;102:e36162. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 8. | Zar HJ, Barnett W, Myer L, Nicol MP. Childhood pneumonia - the Drakenstein Child Health Study. S Afr Med J. 2016;106:642-643. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 14] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 9. | Gao J, Fan J, Zhou H, Jit M, Wang P. Health-related quality of life and economic burden of childhood pneumonia in China: a multiregion study. BMJ Paediatr Open. 2023;7:e002031. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 10. | Wisman MA, Emmelkamp J, Dekker JJM, Christ C. Internet-based emotion-regulation training added to CBT in adolescents with depressive and anxiety disorders: A pilot randomized controlled trial to examine feasibility, acceptability, and preliminary effectiveness. Internet Interv. 2023;31:100596. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 14] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 11. | Bogart K, Hemmesch A, Barnes E, Blissenbach T, Beisang A, Engel P; Chloe Barnes Advisory Council on Rare Diseases. Healthcare access, satisfaction, and health-related quality of life among children and adults with rare diseases. Orphanet J Rare Dis. 2022;17:196. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 94] [Cited by in RCA: 71] [Article Influence: 17.8] [Reference Citation Analysis (0)] |
| 12. | Dangor Z, Lala S, Verwey C, Reubenson G, White D, Moore D, Jeena P, Masekela R, Zar H. Bronchiolitis versus bronchopneumonia: navigating antibiotic use within the LRTI spectrum. S Afr Med J. 2023;113:20-23. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 13. | Sun R, Zhang Y, Cheng F, Zhao Y. Effect of pulmonary rehabilitation nursing approach with integrated traditional Chinese and western medicine in children with Mycoplasma Pneumonia after Bronchoalveolar Lavage. Pak J Med Sci. 2025;41:1105-1109. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 14. | Listiarini D, Desai D, Hidayat YW, Handoko KA. Understanding the Correlation between Blood Profile and the Duration of Hospitalization in Pediatric Bronchopneumonia Patients: A Cross-Sectional Original Article. J Crit Care Med (Targu Mures). 2024;10:254-260. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 15. | Ebeledike C, Ahmad T. Pediatric Pneumonia. 2023 Jan 16. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025. [PubMed] |
| 16. | Wang Y, Li L, Qu A, Wang J. Effects of Child-Friendly Music Nursing in the Ward on Mental Health of Children with Henoch-Schönlein Purpura Nephritis: A Retrospective Study. Noise Health. 2025;27:20-25. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 17. | Guo B, Zhang M, Hao W, Wang Y, Zhang T, Liu C. Neuroinflammation mechanisms of neuromodulation therapies for anxiety and depression. Transl Psychiatry. 2023;13:5. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 311] [Cited by in RCA: 263] [Article Influence: 87.7] [Reference Citation Analysis (0)] |
| 18. | Li HM, Wan LL, Jin CX, Zhang GY, Yang H, Zhang XY. Risk factors of peripheral venous catheter-related complication and infection in children with bronchopneumonia. BMC Infect Dis. 2023;23:603. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 19. | Shen D, Lin L, Fan Y, Zhan L, Dong C. Research on Depression in Children with Severe Bronchial Asthma: The Impact of Alexithymia and Somatic Symptoms. Alpha Psychiatry. 2024;25:362-368. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 20. | Pahwa K, Acharya R, Bhalla K, Yadav D. Burden of depression and anxiety among caregivers of children having structural epilepsy. J Family Med Prim Care. 2024;13:3309-3312. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 21. | Soni P, Cheriathu J. Exploring long-term psychological effects of bronchiolitis and influenza in school-aged children. Front Pediatr. 2025;13:1536571. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 22. | Liu X, Cao H, Zhu H, Zhang H, Niu K, Tang N, Cui Z, Pan L, Yao C, Gao Q, Wang Z, Sun J, He H, Guo M, Guo C, Liu K, Peng H, Peng W, Sun Y, Xie Y, Li B, Shan G, Zhang L. Association of chronic diseases with depression, anxiety and stress in Chinese general population: The CHCN-BTH cohort study. J Affect Disord. 2021;282:1278-1287. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 74] [Cited by in RCA: 52] [Article Influence: 10.4] [Reference Citation Analysis (0)] |
| 23. | Volpato E, Toniolo S, Pagnini F, Banfi P. The Relationship Between Anxiety, Depression and Treatment Adherence in Chronic Obstructive Pulmonary Disease: A Systematic Review. Int J Chron Obstruct Pulmon Dis. 2021;16:2001-2021. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 77] [Article Influence: 15.4] [Reference Citation Analysis (0)] |
| 24. | Sun J, Wang S, Mu G, Liu J, Su R, Zhang X, Fang J, Wang Y. Symptoms of depression and anxiety in Chinese adolescents: heterogeneity and associations with executive function. BMC Psychiatry. 2023;23:410. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 11] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 25. | Fiksdal A, Hanlin L, Kuras Y, Gianferante D, Chen X, Thoma MV, Rohleder N. Associations between symptoms of depression and anxiety and cortisol responses to and recovery from acute stress. Psychoneuroendocrinology. 2019;102:44-52. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 229] [Cited by in RCA: 182] [Article Influence: 26.0] [Reference Citation Analysis (0)] |
| 26. | Du YJ, Yang CJ, Li B, Wu X, Lv YB, Jin HL, Cao YX, Sun J, Luo QL, Gong WY, Zhang HY, Liu BJ, Wu JF, Dong JC. Association of pro-inflammatory cytokines, cortisol and depression in patients with chronic obstructive pulmonary disease. Psychoneuroendocrinology. 2014;46:141-152. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 38] [Article Influence: 3.2] [Reference Citation Analysis (0)] |