Published online Mar 19, 2026. doi: 10.5498/wjp.v16.i3.114588
Revised: November 16, 2025
Accepted: December 15, 2025
Published online: March 19, 2026
Processing time: 136 Days and 23.8 Hours
Patients who undergo lung cancer surgery frequently experience a fear of disease progression (FoP), which can negatively affect their quality of life. Understanding the varying degrees of FoP and related psychological distress experienced by such patients is essential to develop effective interventions. Thus, in this study, we hy
To investigate FoP levels and their association with psychological factors in pati
A sample size was determined with reference to prior research findings and considerations regarding statistical power. Subsequently, 368 patients who had undergone lung cancer surgery were recruited from a university hospital in China for this cross-sectional investigation. Data were obtained through general infor
The total FoP-Q-SF, SAS, and SDS scores were 35.52 ± 6.73, 51.23 ± 6.35, and 54.48 ± 7.15, respectively. Anxiety and depression rates were 62.50% and 59.24%, respectively, among the participants. Marital status, education level, payment method, tumor stage, and SAS and SDS scores independently increased the FoP-Q-SF scores (P < 0.05). The FoP-Q-SF scores were positively correlated with SAS (r = 0.733) and SDS (r = 0.377) scores; physical health factors had stronger associations than social-family factors. Higher anxiety/depression was correlated with higher FoP. The multivariate model, with R2 = 0.773 and an area under the curve value of 0.895, had better predictive effi
Patients post lung cancer surgery have moderate FoP, which is affected by multiple factors and requires targeted psychological intervention.
Core Tip: This study identified levels of fear of disease progression and associated psychological factors in individuals who have undergone lung cancer surgery. Its findings provide a foundation for personalized psychological support to enhance the quality of life of such patients. Furthermore, to our knowledge, it is the first study to comprehensively analyze the multidim
- Citation: Chen MJ, Lei W, Zhou J, Chen LX, Hui T, Lu X. Fear of disease progression and psychological factors in postoperative lung cancer patients. World J Psychiatry 2026; 16(3): 114588
- URL: https://www.wjgnet.com/2220-3206/full/v16/i3/114588.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i3.114588
Lung cancer is a highly prevalent malignant tumor that endangers public health and causes fear of disease progression (FoP) in patients after surgical treatment. FoP refers to persistent concerns regarding disease recurrence, deterioration, and associated consequences[1]. It can reduce treatment compliance, exacerbate psychological distress, and significantly impede the patient’s rehabilitation and quality of life[2].
Previous studies have preliminarily explored relevant factors that influence FoP. Educational level, disease duration, tumor stage, and self-rating anxiety scale (SAS) scores were found to be significantly associated with postoperative FoP; specifically, higher educational levels, shorter disease duration, and early tumor stages were correlated with lower FoP levels[3]. Furthermore, marital status, payment method, and self-rating depression scale (SDS) scores were also sig
However, previous studies have limitations of small sample sizes, single-dimensional factor analysis, and failure to systematically integrate sociodemographic traits, clinical disease markers, and multiple psychological variables, such as the simultaneous inclusion of anxiety and depression. This study aimed to overcome these issues by first expanding the sample size to 368 patients. Second, we analyzed the combined impact of social factors, such as marital status and pay
This study included 368 patients who underwent lung cancer surgery at the Affiliated Zhangjiagang Hospital of Soochow University between June 2023 and May 2025. The inclusion criteria were patients: (1) With pathologically confirmed lung cancer who had undergone surgical treatment; (2) One to six months post-surgery with clear consciousness; and (3) Who voluntarily participated and signed the informed consent form. The exclusion criteria were those who had: (1) Severe mental illness or cognitive impairment; (2) Other malignant tumors; or (3) Incomplete clinical data. This study was revi
This cross-sectional study utilized the fear of progression questionnaire-short form (FoP-Q-SF) scores, a quantitative measure, of postoperative patients with lung cancer, as the core. Based on prior research data[6], the standard deviation (σ) of the total FoP-Q-SF score was 6.60. With α set at 0.05 (Z1 - α/2 = 1.96 for two-tailed test) and an allowable error (δ) of 0.74 points (higher precision standard was adopted to enhance the stability of results), calculations via the formula in
The general information questionnaire obtained participants’ gender, age, marital status, educational attainment, pay
The SAS assesses the frequency of anxiety symptoms experienced by an individual. It consists of 20 items and uses a 4-point rating system, ranging from 1 (no or very little of the time) to 4 (most or all the time). Standard score (total score) is calculated by multiplying the sum of all items by 1.25. A score of 50 or below indicates the absence of anxiety, between 50 and 60 indicates mild anxiety, between 61 and 70 indicates moderate anxiety, and above 70 indicates severe anxiety. The Cronbach’s α of this scale was 0.85 in a previous study[8]. The SDS comprises 20 items scored on a scale from 1 (a little of the time) to 4 (most of the time). Standard score for this scale is calculated by multiplying the sum of all items by 1.25. A score of 50 or below is considered normal, between 50 and 60 indicates mild depression, between 61 and 70 indicates mo
Questionnaires were distributed on-site by trained researchers, who instructed patients to complete them independently and collected the forms immediately. Of the 380 questionnaires distributed, 368 valid ones were received, which resulted in an effective recovery rate of 96.8%.
Data were analyzed using SPSS version 26.0. Measurement data were expressed as mean ± SD, with comparisons across groups performed via t-test or analysis of variance. Count data were presented as n (%), while inter-group comparisons were analyzed via the χ2 test. Pearson’s correlation analysis was used to assess correlations between the variables. Mul
Of the 368 patients, 201 were male (54.6%) and 167 were female (45.4%). Their ages ranged from 35-78 (mean 53.43 ± 7.96) years. Furthermore, 292 were married (79.3%) and 76 were unmarried, divorced, or widowed (20.7%). Regarding their educational level, 58 patients (15.8%) had received primary school education or below, 124 (33.7%) had received junior high school education, 102 (27.7%) had received senior high school education, and 84 (22.8%) had received junior college education or higher school education. Regarding medical insurance, 186 patients were covered by employee medical insurance (50.5%), 122 by resident medical insurance (33.2%), and 60 paid out-of-pocket (16.3%). Regarding the tumor stage, 230 patients were at stage I-II (62.5%) and 138 were at stage III-IV (37.5%) (Table 1).
| Indicators | Categories | n (%) |
| Gender | Male | 201 (54.6) |
| Female | 167 (45.4) | |
| Age (years) | < 50 | 118 (32.07) |
| 50-65 | 200 (54.35) | |
| > 65 | 50 (13.59) | |
| Marital status | Married | 292 (79.3) |
| Unmarried/divorced/widowed | 76 (20.7) | |
| Educational level | Primary school and below | 58 (15.8) |
| Junior high school | 124 (33.7) | |
| Senior high school/technical secondary school | 102 (27.7) | |
| College degree and above | 84 (22.8) | |
| Payment method | Employee medical insurance | 186 (50.5) |
| Resident medical insurance | 122 (33.2) | |
| Self-payment | 60 (16.3) | |
| Tumor stage | Stage I-II | 230 (62.5) |
| Stage III-IV | 138 (37.5) |
The overall FoP-Q-SF score was 35.52 ± 6.73 points. It comprised 18.30 ± 5.97 points and 17.19 ± 3.33 points for the physical health and social-family factors, respectively. Standard SAS score was 51.23 ± 6.35 points, and the anxiety incidence was 62.50% (230 out of 368). Standard SDS score was 54.48 ± 7.15 points, and the depression incidence was 59.24% (218 out of 368) (Table 2).
| Scale | Total score | Factor score | Abnormality rate |
| FoP-Q-SF | 35.52 ± 6.73 | Physical health factor: 18.30 ± 5.97 | - |
| Social-family factor: 17.19 ± 3.33 | - | ||
| SAS | 51.23 ± 6.35 | - | 230 (62.50) |
| SDS | 54.48 ± 7.15 | - | 218 (59.24) |
Gender: Male (n = 201, 35.94 ± 6.67) vs female (n = 167, 35.02 ± 6.77), P = 0.192. Age: < 50 years (n = 118, 34.64 ± 6.41), 50 years to 65 years (n = 200, 36.10 ± 6.78), > 65 years (n = 50, 35.28 ± 7.00), P = 0.166. Marital status: Married (n = 292, 33.77 ± 6.13) vs others (n = 76, 42.22 ± 4.28), P < 0.001. Educational level: Primary school and below (n = 58, 43.17 ± 4.20) > junior high school (n = 124, 37.94 ± 5.80) > senior high school/technical secondary school (n = 102, 33.18 ± 4.76) > college degree and higher (n = 84, 29.51 ± 4.14), P < 0.001. Payment method: Self-payment (n = 60, 42.72 ± 4.34) > resident medical insurance (n = 122, 37.58 ± 5.63) > employee medical insurance (n = 186, 31.84 ± 5.45), P < 0.001. Tumor stage: Stage III-IV (n = 138, 38.73 ± 6.00) > stage I-II (n = 230, 33.59 ± 6.40), P < 0.001. Anxiety status: With anxiety (n = 230, 39.25 ± 4.73) > without anxiety (n = 138, 29.30 ± 4.65), P < 0.001. Depression status: With depression (n = 218, 37.53 ± 6.13) > without depression (n = 150, 32.60 ± 6.49), P < 0.001 (Table 3).
| Indicators | Categories | n | FoP-Q-SF scores (points) | t | P value |
| Gender | Male | 201 | 35.94 ± 6.67 | 1.308 | 0.192 |
| Female | 167 | 35.02 ± 6.77 | |||
| Age (years) | < 50 | 118 | 34.64 ± 6.41 | 1.802 | 0.166 |
| 50-65 | 200 | 36.10 ± 6.78 | |||
| > 65 | 50 | 35.28 ± 7.00 | |||
| Marital status | Married | 292 | 33.77 ± 6.13 | 11.320 | < 0.001 |
| Unmarried/divorced/widowed | 76 | 42.22 ± 4.28 | |||
| Educational level | Primary school and below | 58 | 43.17 ± 4.20 | 105.700 | < 0.001 |
| Junior high school | 124 | 37.94 ± 5.80 | |||
| Senior high school/technical secondary school | 102 | 33.18 ± 4.76 | |||
| College degree and above | 84 | 29.51 ± 4.14 | |||
| Payment method | Employee medical insurance | 186 | 31.84 ± 5.45 | 107.400 | < 0.001 |
| Resident medical insurance | 122 | 37.58 ± 5.63 | |||
| Self-payment | 60 | 42.72 ± 4.34 | |||
| Tumor stage | Stage I-II | 230 | 33.59 ± 6.40 | 7.634 | < 0.001 |
| Stage III-IV | 138 | 38.73 ± 6.00 | |||
| Anxiety status | With anxiety | 230 | 39.25 ± 4.73 | 19.660 | < 0.001 |
| Without anxiety | 138 | 29.30 ± 4.65 | |||
| Depression status | With depression | 218 | 37.53 ± 6.13 | 7.401 | < 0.001 |
| Without depression | 150 | 32.60 ± 6.49 |
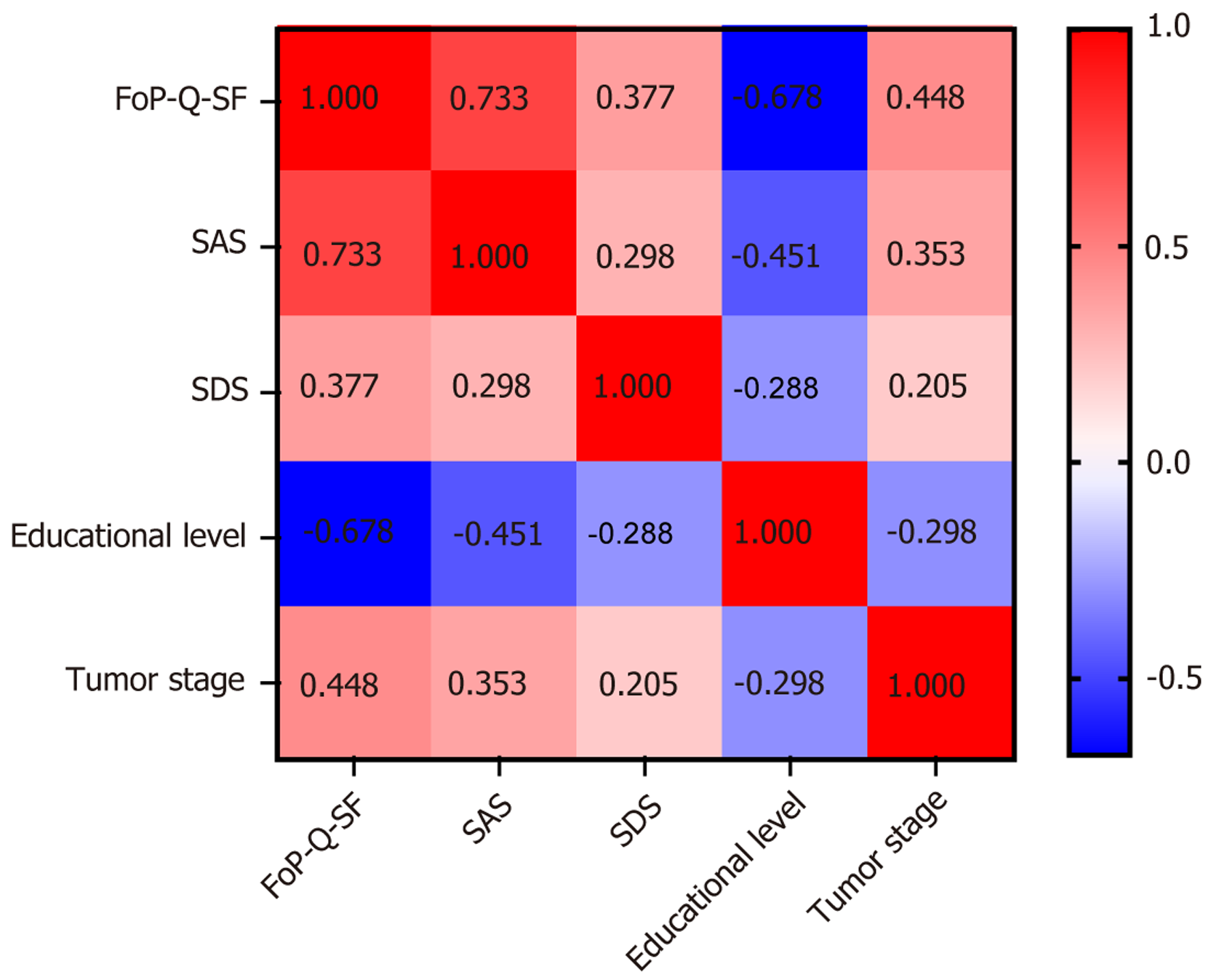
The FoP-Q-SF scores were positively correlated with SAS (r = 0.733, P < 0.001) and SDS scores (r = 0.377, P < 0.001) and negatively correlated with educational level (r = -0.678, P < 0.001). Furthermore, they were positively associated with tumor stage (r = 0.448, P < 0.001). Additionally, SAS scores were negatively correlated with educational level (r = -0.451, P < 0.001) and positive correlated with tumor stage (r = 0.353, P < 0.001) (Figure 1).
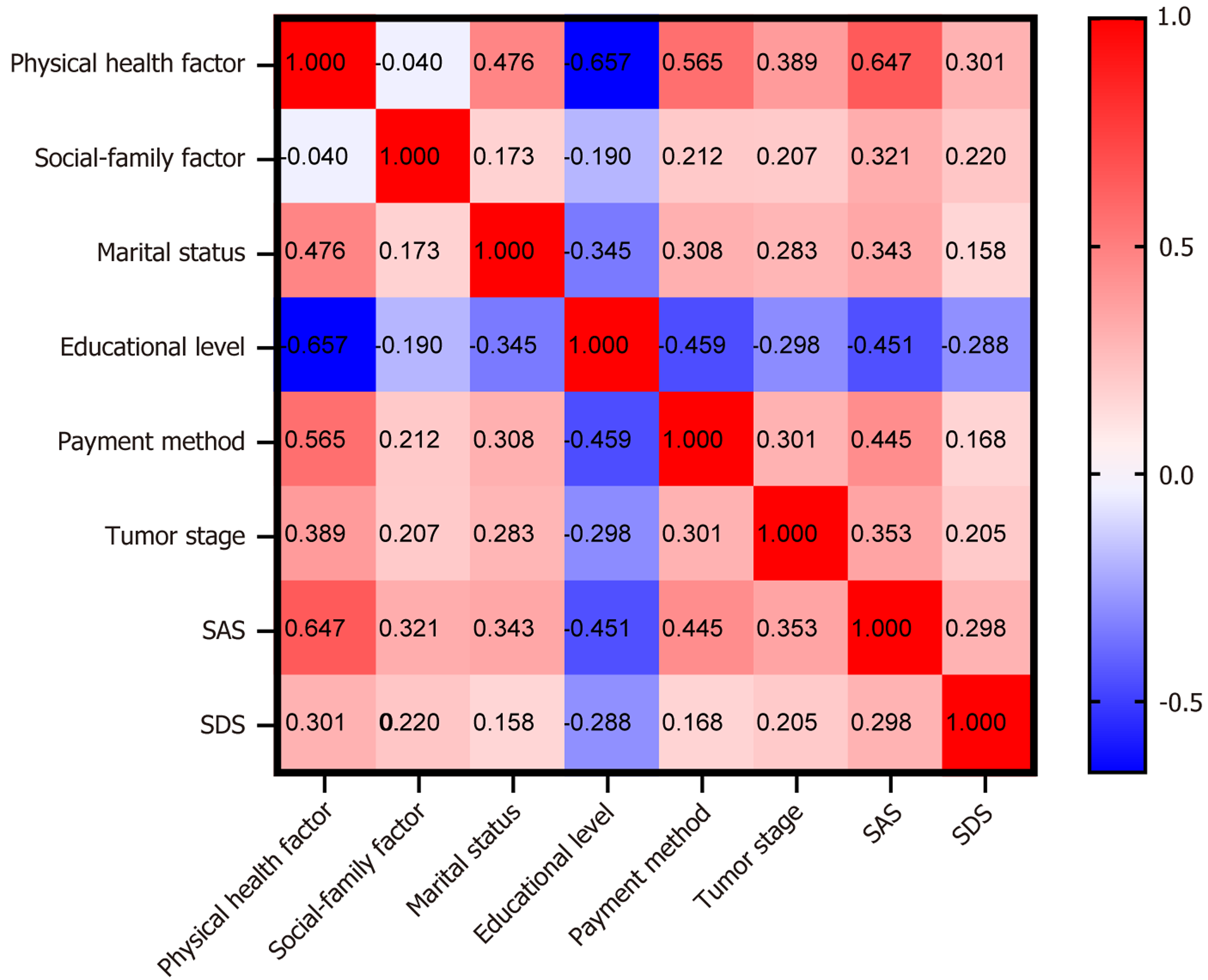
We conducted an association analysis on the physical health and social-family factors of the FoP-Q-SF. Results revealed that the associations of the physical health factor with marital status, educational level, payment method, tumor stage, SAS, and SDS (r = 0.476, -0.657, 0.565, 0.389, 0.647, and 0.301 respectively; all P < 0.001) were notably greater compared with those of the social-family factor (r = 0.173, -0.190, 0.212, 0.207, 0.321, and 0.220 respectively; all P < 0.001) (Figure 2).
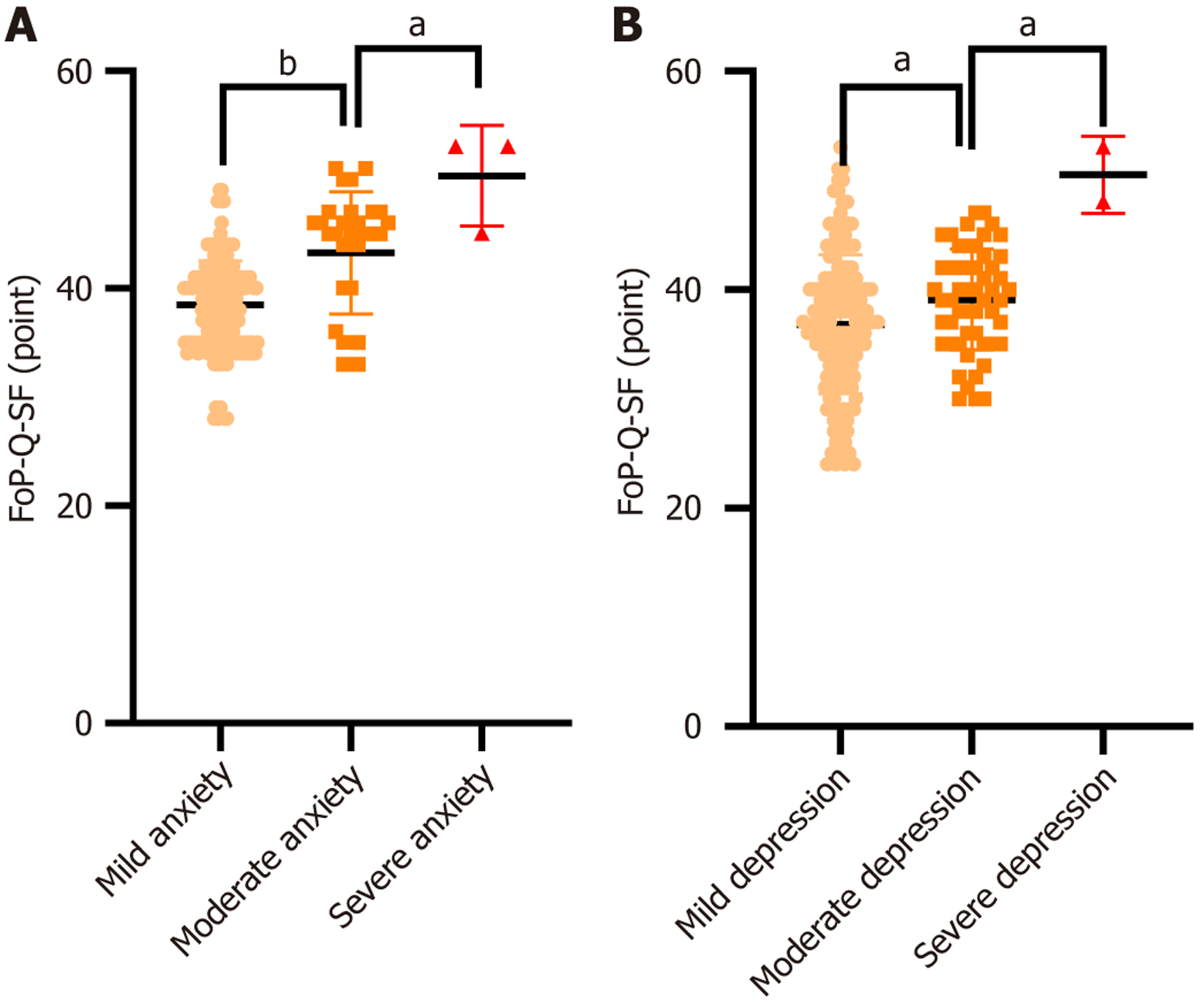
SAS standard scores were categorized into mild (50-59 points, n = 197), moderate (60-69 points, n = 30), and severe anxiety (≥ 70 points, n = 3). Corresponding FoP-Q-SF scores were 38.47 ± 4.04 points, 43.27 ± 5.53 points, and 50.33 ± 3.77 points, respectively. All groups differed significantly (P < 0.001), and scores increased linearly with the severity of anxiety experienced (F = 26.840, P < 0.001). SDS standard scores were classified into mild (53-62 points, n = 162), moderate (63-72 points, n = 54), and severe depression (≥ 73 points, n = 2), with the corresponding FoP-Q-SF scores being 36.85 ± 6.33 points, 39.09 ± 4.60 points, and 50.50 ± 2.50 points respectively. Similar significant gradient differences were observed (F = 7.699, P < 0.001) (Figure 3).
We used the total FoP-Q-SF score as the outcome variable and incorporated variables with significant univariate associations (marital status, educational level, payment method, tumor stage, and SAS and SDS scores) into the regression model. Results indicated that being unmarried, divorced, or widowed (β = 0.156), having a low educational level (β =
| Variable | Assignment | Unstandardized coefficient β (95%CI) | Standardized coefficient β | SE | t | P value |
| Constant | - | 9.554 (5.316-13.792) | - | 2.155 | 4.434 | < 0.001 |
| Marital status | 0 = married; 1 = unmarried/divorced/widowed | 2.805 (1.894-3.717) | 0.169 | 0.464 | 6.051 | < 0.001 |
| Educational level | 1 = Primary school and below; 2 = junior high school; 3 = senior high school/technical secondary school; 4 = college degree and above | -1.972 (-2.376 to -1.569) | -0.295 | 0.205 | -9.615 | < 0.001 |
| Payment method | 1 = employee medical insurance; 2 = resident medical insurance; 3 = self-payment | 1.819 (1.284-2.354) | 0.201 | 0.272 | 6.69 | < 0.001 |
| Tumor stage | 1 = stage I; 2 = stage II; 3 = stage III; 4 = stage IV | 0.606 (0.255-0.957) | 0.094 | 0.178 | 3.392 | 0.001 |
| SAS | Actual value | 0.415 (0.350-0.479) | 0.391 | 0.033 | 12.659 | < 0.001 |
| SDS | Actual value | 0.090 (0.040-0.139) | 0.095 | 0.025 | 3.552 | < 0.001 |
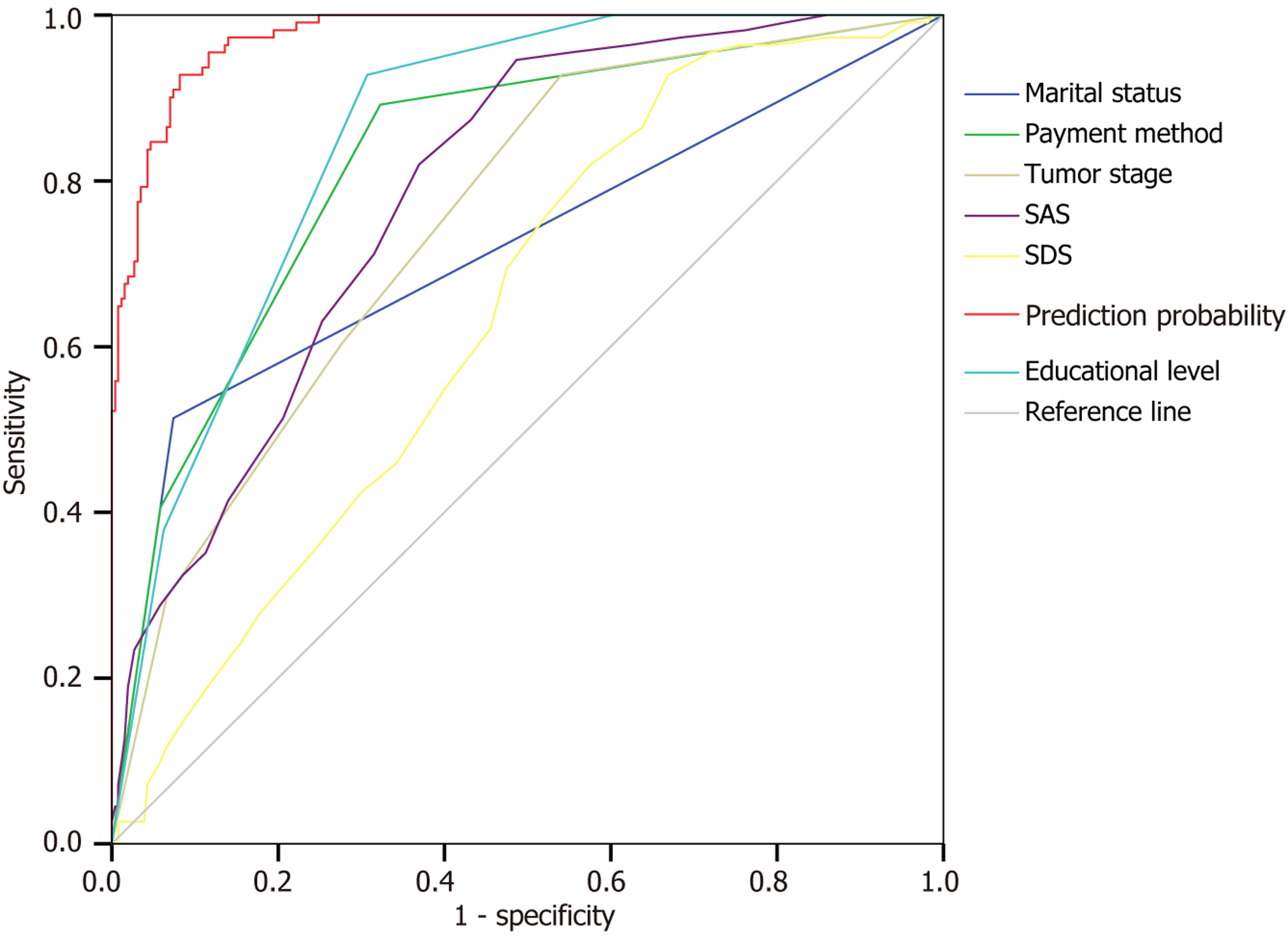
Leveraging the results of multiple linear regression analysis, we deduced a regression equation: Total FoP-Q-SF score = 9.554 + 2.805 × marital status + (-1.972) × educational level + 1.819 × payment method + 0.606 × tumor stage + 0.415 × SAS score + 0.090 × SDS score (variable assignments aligned with Table 4). We utilized an internal validation approach (10-fold cross-validation) to assess the predictive capability of the multiple regression model. Results demonstrated that the model’s coefficient of determination (R2) was 0.773 and root mean square error was 3.237. Considering a total FoP-Q-SF score of ≥ 40 as the threshold for high fear status (determined via the Youden index), we plotted the receiver operating characteristic curve of the model’s predicted values, and obtained an AUC of 0.895 [95% confidence interval (95%CI): 0.80-0.96]. Optimal predictive threshold corresponded to a model score of 41, which featured a sensitivity and specificity of 92.8% and 91.8%, respectively. AUC values for models that included only SAS (0.786, 95%CI: 0.739-0.832) and SDS scores (0.638, 95%CI: 0.581-0.696) were markedly lower than those of the full model (Z = 2.119, P = 0.013; Z = 1.262, P = 0.032). Hence, the combined multifactor model possessed superior predictive efficacy (Figure 4).
A survey of postoperative patients with lung cancer revealed that their total FoP-Q-SF score was 35.52 ± 6.73, which reflects a moderate level of FoP. The incidence rates of anxiety and depression were 62.50% and 59.24%, respectively, among the patients. Significant differences were observed in the FoP-Q-SF scores among patients with distinct characteristics. Marital status, educational level, payment method, tumor stage, and anxiety and depression status were all cor
Many recent studies have focused on FoP and related psychological factors in patients with lung cancer. Tao et al[10] reported that FoP in patients with lung cancer was linked to various factors, with anxiety being a key factor. This aligns with our finding that the FoP-Q-SF scores had a significant positive association with SAS scores, which further verifies the role of anxiety in worsening patients’ FoP. Borg et al[11] found that patients with lung cancer and lower educational levels tended to experience more difficulties in coping with the disease and exhibited higher FoP levels, which is con
Mechanisms of psychological factors: Anxiety is associated with FoP and may amplify it by altering patients’ cognitive patterns and coping strategies. Patients in an anxious state may tend to overly concentrate on negative information related to the disease and magnify the perceived risk of disease progression[15-17]. This study observed that patients with anxiety had markedly higher FoP-Q-SF scores than those without anxiety; furthermore, scores increased with the severity of anxiety experienced. This implies that anxiety could be a key psychological factor impacting FoP. Moreover, anxiety can disturb aspects of daily life, such as sleep and diet, which can further weaken one’s psychological ability to cope and create a vicious cycle[18-21]. Regarding the association between depression and FoP, depressive conditions lower psychological resilience, which can lead to pessimistic future expectations[22]. Psychological resilience refers to an individual’s capacity to adapt effectively amid adversity, trauma, tragedy, threats, or other major stressors[23,24]. Studies reveal that psychological resilience regulates the relationships among depression, anxiety, and well-being[25]. Hence, pessimism may heighten FoP, as evidenced by the elevated FoP-Q-SF scores among patients with depression in this study. Depression may also reduce patients’ motivation to participate in rehabilitation, which can increase the risk of dis
Mechanisms of sociodemographic factors: Patients with lower educational levels may struggle to access and comp
Mechanisms underlying disease-related factors: Patients with advanced stages of lung cancer (III-IV) have more serious disease conditions, higher risk of tumor metastasis, and worse prognosis[29]. Their direct awareness of disease pro
This study has some limitations. First, we only enrolled postoperative lung cancer patients from a single region. Hence, our sample lacked sufficient geographical representativeness and possibly failed to accurately mirror the actual situation of patients with lung cancer in various regions. Regional differences in factors, such as medical resources and cultural background, may affect patients’ psychological states and the intensity of their FoP. Future studies should broaden the sample scope to include patients from diverse regions to enhance the generalizability of the findings. Second, we adopted a cross-sectional survey design. Hence, we cannot clarify the causal relationships between variables. Although multiple factors were associated with FoP, whether these factors cause such fear or are arising consequences remains unclear. Subsequent studies should use prospective cohort designs to thoroughly explore the causal mechanisms between the factors. Third, although we utilized widely used scales, such as the FoP-Q-SF, SAS, and SDS, these may not fully capture patients’ complex psychological states or all the influencing factors. Some patients may have unique psychological experiences and unrecognized influencing factors that are not covered by the scales. Future research should consider combining qualitative research methods to comprehensively understand patients’ feelings and improve the assessment of relevant factors.
FoP in postoperative patients with lung cancer was impacted by psychological aspects, such as anxiety and depression, in addition to marital status, educational attainment, payment mode, and tumor stage. Physical health factors had more notable associations with FoP. Furthermore, the multiple regression model had favorable predictive ability. Our results suggest that psychological assessments should be prioritized. Interventions, such as cognitive-behavioral therapy, may help patients with anxiety and depression. Health education should be improved for patients with low educational levels using easy-to-understand language to convey disease-related information. In addition, social support should be enhanced to focus on unmarried, divorced, or widowed patients and reduce financial strain for self-paying patients. Patients’ psy
| 1. | Lakhiani A, Cummins C, Kumar S, Long J, Arora V, Balega J, Broadhead T, Duncan T, Edmondson R, Fotopoulou C, Glasspool R, Kolomainen D, Manchanda R, McNally O, Morrison J, Mukhopadhyay A, Naik R, Wood N, Sundar S. Analysis of Anxiety, Depression and Fear of Progression at 12 Months Post-Cytoreductive Surgery in the SOCQER-2 (Surgery in Ovarian Cancer-Quality of Life Evaluation Research) Prospective, International, Multicentre Study. Cancers (Basel). 2023;16:75. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 2. | Du L, Cai J, Zhou J, Yu J, Yang X, Chen X, Xu X, Zhang X. Current status and influencing factors of fear disease progression in Chinese primary brain tumor patients: A mixed methods study. Clin Neurol Neurosurg. 2024;246:108574. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 3. | Lu Q, Liu Q, Fang S, Ma Y, Zhang B, Li H, Song L. Relationship between fear of progression and symptom burden, disease factors and social/family factors in patients with stage-IV breast cancer in Shandong, China. Cancer Med. 2024;13:e6749. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 11] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 4. | Liu Y, Li J, Liang G, Fang F, Wang S. The mediating effect of dyadic coping between illness perception and fear of disease progression in bladder cancer patients: A cross-sectional survey. Medicine (Baltimore). 2025;104:e44520. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 5. | Xuan YJ, Ye Q, Ren Y, Yao YH, Wang Z, Feng XQ. Fear of cancer recurrence among caregivers of adolescents with malignant bone tumors in China: a cross-sectional survey. Front Public Health. 2025;13:1608217. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 6. | Hu S, Fang A. Dynamic Changes and Influencing Factors for the Quality of Life in Nursing Care after Lung Cancer Resection. Contrast Media Mol Imaging. 2022;2022:1162218. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 7. | Jrad AIS, Yi Y, Yoon B, Cho E, Cho IK, Lee D, Kim J, Chung S, Kim JH. Dysfunctional Self-Focus and Fear of Progression in Cancer Patients Mediated by Depression, Anxiety, and Dysfunctional Sleep Beliefs. Psychiatry Investig. 2024;21:506-512. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 8. | Tan VS, Tjong MC, Chan WC, Yan M, Delibasic V, Darling G, Davis LE, Doherty M, Hallet J, Kidane B, Mahar A, Mittmann N, Parmar A, Tan H, Wright FC, Coburn NG, Louie AV. A population-based analysis of the management of symptoms of depression among patients with stage IV non-small cell lung cancer (NSCLC) in Ontario, Canada. Support Care Cancer. 2024;32:381. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 9. | Xu F, Xie S, Li Q, Zhong X, Zhang J. The impact of depression on the quality of life of lung cancer patients undergoing chemotherapy: mediating effects of perceived social support. Front Psychiatry. 2025;16:1526217. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 10. | Tao XQ, Wu QC, Wei X, Zhang W, Zhou Y, Qiu H. Fear of Progression and Its Associated Factors Among Patients With Positive Lung Cancer Screening Results: A Latent Profile Analysis. Nurs Health Sci. 2025;27:e70176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 11. | Borg M, Løkke A, Henriksen M, Wen SWC, Ibsen R, Hilberg O. Educational attainment and employment status in lung cancer patients: a nationwide study. Clin Transl Oncol. 2025. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 12. | Kolsteren EEM, Kwakkenbos L, Prins JB, Davis L, van der Lee M, Poort H, Servaes P, Sharpe L, Lebel S, Custers JAE. Identification of features of fear of progression in people with advanced cancer and systemic treatment: an international modified Delphi study. J Psychosoc Oncol Res Pract. 2024;6:135. [DOI] [Full Text] |
| 13. | Manzoor Z, Suleman M, Hussain A. Stigmatization and Fear of Death Predicted Psychological Burden of Cancer Patients. Bull Bus Econ. 2024;13. [DOI] [Full Text] |
| 14. | Zhang Q, Chen F, Xiao Z, Li S, Deng Y, Knobf MT, Li J, Ye Z. Self-perceived burden, fear of progression and psychological flexibility in cervical cancer survivors: A moderated network analysis. Asia Pac J Oncol Nurs. 2025;12:100762. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 15. | Curran L, Sharpe L, MacCann C, Butow P. Testing a model of fear of cancer recurrence or progression: the central role of intrusions, death anxiety and threat appraisal. J Behav Med. 2020;43:225-236. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 52] [Article Influence: 8.7] [Reference Citation Analysis (0)] |
| 16. | Sun L, Li W, Qiu Q, Hu Y, Yang Z, Xiao S; Alzheimer's Disease Neuroimaging Initiative. Anxiety adds the risk of cognitive progression and is associated with axon/synapse degeneration among cognitively unimpaired older adults. EBioMedicine. 2023;94:104703. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 39] [Cited by in RCA: 34] [Article Influence: 11.3] [Reference Citation Analysis (0)] |
| 17. | Susini RM, Ciufia N, Marinangeli AL, Alonso R, Eizaguirre MB. Anxiety and Cognition in Multiple Sclerosis: A Narrative Review. Int J MS Care. 2025;27:63-73. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 18. | Peng A, Ji S, Lai W, Hu D, Wang M, Zhao X, Chen L. The bidirectional relationship between sleep disturbance and anxiety: Sleep disturbance is a stronger predictor of anxiety. Sleep Med. 2024;121:63-68. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 42] [Article Influence: 21.0] [Reference Citation Analysis (0)] |
| 19. | Lee S, Almeida D. Dynamic Interplay Between Stress and Poor Sleep and Their Consequences on Daily Well-Being. Innov Aging. 2023;7:587. [RCA] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 20. | Yiyue Y, Kaiqi G, Rujie W, Honghong L, Xu M, Yingxue F, Yijing P, Yu C, Yuanyuan J, Jing M, Dongxiao L, Yue L, Jing L. Effects of sleep quality on suicide risk in COVID-19 patients: The chain mediating of anxiety and depressive symptoms. Heliyon. 2023;9:e15051. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 21. | Zhyvotovska A, Boiko D, Bodnar L, Kozar Y, Martynenko Y, Isakov R. The relationship between sleep disorders, level of psychological stress and state-trait anxiety in patients with anxiety disorders. Acta Fac Med Naiss. 2024;41:344-354. [DOI] [Full Text] |
| 22. | Mei Y, Yang X, Liu C, Li Y, Gui J, Zhang L. The impact of psychological resilience on chronic patients' depression during the dynamic Zero-COVID policy: the mediating role of stigma and the moderating role of sleep quality. BMC Psychol. 2023;11:213. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 23. | Kerkez M, Şanli ME. Mediating role of spirituality in the relationship of anxiety, stress and depression with resilience in individuals exposed to earthquakes in Türkiye. Int J Disaster Risk Reduct. 2024;104:104347. [DOI] [Full Text] |
| 24. | Wang J, Li S, Hu Y, Ren L, Yang R, Jiang Y, Yu M, Liu Z, Wu Y, Dong Z, Zhang C, Dong W, Yao Y. The moderating role of psychological resilience in the relationship between falls, anxiety and depressive symptoms. J Affect Disord. 2023;341:211-218. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 20] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 25. | Chuning AE, Durham MR, Killgore WDS, Smith R. Psychological Resilience and Hardiness as Protective Factors in the Relationship Between Depression/Anxiety and Well-Being: Exploratory and Confirmatory Evidence. Pers Individ Dif. 2024;225:112664. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 15] [Article Influence: 7.5] [Reference Citation Analysis (0)] |
| 26. | Reijnders T, Schuler M, Wittmann M, Jelusic D, Troosters T, Janssens W, Stenzel NM, Schultz K, von Leupoldt A. The impact of disease-specific fears on outcome measures of pulmonary rehabilitation in patients with COPD. Respir Med. 2019;146:87-95. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 31] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 27. | Jassem Z, Ashour I. Correlation between health literacy and level of education in hemodialysis patients: A cross-sectional study. Rawal Med J. 2023;48:843. [DOI] [Full Text] |
| 28. | Cheng X, Liu L, Ni S, Li C, Zhang H, Mao B, Zeng J. Dualistic perspectives on illness coping experiences of individuals with depression and their spouses: a qualitative study. Int J Qual Stud Health Well-being. 2025;20:2503565. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 29. | Zhu J, Branstetter S, Lazarus P, Muscat JE. Smoking, Lung Cancer Stage, and Prognostic Factors-Findings from the National Lung Screening Trial. Int J Environ Res Public Health. 2024;21:400. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 30. | Yang L, Liu J, Liu Q, Wang Y, Yu J, Qin H. The relationships among symptom experience, family support, health literacy, and fear of progression in advanced lung cancer patients. J Adv Nurs. 2023;79:3549-3558. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 31. | Kroll JL, Jones M, Chen AB, Yang CC, Carmack CL, Cohen L, Bruera E, Milbury K. End-of-Life Care, Symptom Burden, and Quality of Life in Couples Facing Stage IV Lung Cancer: The Role of Patient and Spousal Psychospirituality and Discussions Around Fear of Death and Disease Progression. J Palliat Med. 2023;26:690-696. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 32. | Liu Y, Wu W, Li S, Wang X, Zhang L. Exploring psychological distress among lung cancer patients through the stress system model. Sci Rep. 2025;15:27253. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/