Published online Mar 19, 2026. doi: 10.5498/wjp.v16.i3.113625
Revised: October 29, 2025
Accepted: December 12, 2025
Published online: March 19, 2026
Processing time: 153 Days and 0.2 Hours
Total knee arthroplasty (TKA) is an effective treatment for end-stage knee joint disease, but postoperative functional recovery outcomes vary significantly among patients. In recent years, researchers have increasingly focused on the influence of psychological factors on surgical outcomes, yet studies on the impact of pre
To investigate the effects of preoperative anxiety levels on functional recovery outcomes following TKA, providing a more comprehensive treatment strategy for clinical practice.
A retrospective cohort study design was employed to collect clinical data from 186 patients who underwent TKA at a tertiary hospital between January 2020 and December 2023. Patients were divided into a study group (86 cases) and a control group (100 cases) based on preoperative anxiety status. The Hamilton Anxiety Scale and Hamilton Depression Scale were used to assess patients’ mental status. Postoperative rehabilitation time, joint function scores, complication rates, and other indicators were compared between the two groups. Multivariate logistic regression analysis was conducted to determine independent risk factors affecting functional recovery.
Compared to the control group, the study group showed significantly longer postoperative hospital stays [(14.3 ± 3.7) days vs (10.6 ± 2.4) days, P < 0.01], lower knee function scores at 3 months postoperatively [(68.2 ± 8.5) vs (79.9 ± 7.3), P < 0.05], and higher complication rates (32.3% vs 17.2%, P < 0.05). Multivariate analysis identified high preoperative anxiety levels [odds ratio (OR) = 2.47, 95% confidence interval (CI): 1.82-3.36], chronic stress (OR = 1.94, 95%CI: 1.43-2.65), and lack of social support (OR = 1.76, 95%CI: 1.21-2.54) as independent risk factors affecting postoperative functional recovery. Analysis of neuroendocrine and immune indicators revealed elevated stress hormone levels and abnormal expression of inflammatory factors in the study group, which may represent important mechanisms through which anxiety affects postoperative rehabilitation.
Preoperative anxiety is a significant factor influencing functional recovery following TKA. It interferes with the rehabilitation process through multiple pathways, including impacts on patients' self-care behaviors, sleep quality, endocrine function, and immune responses.
Core Tip: This study highlights the significant role of preoperative anxiety in determining functional recovery after total knee arthroplasty. Patients with elevated anxiety levels experienced longer hospital stays, poorer knee function, and higher complication rates. Mechanistic analyses revealed dysregulated neuroendocrine stress responses, increased pro-inflammatory cytokines, impaired treatment adherence, and sleep disturbances as mediating pathways. These findings underscore preoperative anxiety as a modifiable risk factor and emphasize the importance of integrating psychological assessment and targeted interventions into perioperative care. A multidisciplinary approach addressing both mental health and physical rehabilitation may optimize recovery outcomes.
- Citation: Shang S, Hu Y, Wang H, Rao RQ, Zhang F. Preoperative anxiety and psychological determinants of functional recovery after total knee arthroplasty: A retrospective cohort study. World J Psychiatry 2026; 16(3): 113625
- URL: https://www.wjgnet.com/2220-3206/full/v16/i3/113625.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i3.113625
Total knee arthroplasty (TKA) is an effective treatment for end-stage knee joint disease, with approximately 2 million people globally undergoing this procedure annually. Despite advancements in surgical techniques and implant designs, 15%-20% of patients remain dissatisfied with their surgical outcomes, primarily due to persistent pain, poor functional recovery, and limited joint mobility. These adverse outcomes impose substantial physical, psychological, and economic burdens on patients, caregivers, and healthcare systems[1-3].
While extensive research has focused on the influence of physical factors such as surgical techniques, prosthesis designs, and rehabilitation protocols on TKA prognosis, growing evidence suggests that psychological factors may play a crucial role in postoperative recovery trajectories[4-6]. The complex relationship between psychological well-being and physiological recovery processes represents an important but understudied dimension in orthopedic rehabilitation[7-10]. Mental health disorders, particularly anxiety and depression, have a prevalence rate of 25%-60% among TKA patients, significantly higher than in the general population.
The bidirectional relationship between preoperative anxiety and postoperative recovery involves complex pathophysiological pathways. Psychological stress can trigger neuroendocrine responses, including elevation of stress hormones such as cortisol and catecholamines, which may impair immune function and inflammatory responses essential for wound healing and functional recovery[7-9]. Additionally, patients with anxiety disorders often demonstrate reduced adherence to treatment regimens, poor nutritional status, and compromised sleep quality - all factors that can signi
Previous research has established links between psychological disorders and delayed recovery following various types of surgery, including general surgery and cardiac procedures. However, specific evidence regarding the impact of preoperative anxiety on TKA rehabilitation remains limited, creating a notable gap in our understanding. This gap is particularly concerning given the high proportion of psychological distress among TKA patients[11-13]. These patients typically face multiple challenges including postoperative pain, limited mobility, social isolation, and decreased quality of life.
Recognizing the potential impact of psychological factors on functional recovery outcomes has important implications for clinical practice. A comprehensive approach to TKA management that incorporates psychological assessment and intervention alongside standard postoperative rehabilitation protocols may significantly improve recovery outcomes and patient quality of life[14-16]. However, implementing such an approach requires a clearer understanding of the specific relationships between preoperative anxiety and TKA functional recovery.
This study aims to address this knowledge gap by investigating the impact of preoperative anxiety levels on functional recovery following TKA through a retrospective cohort analysis. By elucidating these relationships, we hope to provide evidence-based guidance for developing more holistic treatment strategies that address both the physical and psychological needs of TKA patients.
This retrospective cohort study was conducted at a tertiary hospital between January 2020 and December 2023. After obtaining approval from the institutional ethics committee, we reviewed the medical records of adult patients diagnosed with knee osteoarthritis who underwent TKA. Inclusion criteria included: Age ≥ 18 years; undergoing primary unilateral TKA for knee osteoarthritis; having complete medical records including preoperative psychological assessment data; and a minimum follow-up period of 12 weeks or until satisfactory functional recovery. Exclusion criteria included: Severe malnutrition (serum albumin < 2.5 g/dL); malignancy around the knee joint; uncontrolled diabetes mellitus (glycated hemoglobin > 9.0%); severe peripheral vascular disease (ankle-brachial index < 0.5); those receiving immunosuppressive therapy; those with incomplete medical records or loss to follow-up; and those who had previously participated in interventional functional recovery studies. A total of 186 eligible patients were identified and divided into two groups based on preoperative anxiety status. The study group (n = 86) consisted of TKA patients with preoperative anxiety disorders, defined by Hamilton Anxiety Scale (HAMA) score ≥ 14 and/or Hamilton Depression Scale (HAMD) score ≥ 17 and/or a documented diagnosis of a psychological disorder in medical records with ongoing treatment. The control group (n = 100) included TKA patients without preoperative anxiety disorders, defined by HAMA score < 14, HAMD score < 17, and no documented history of psychological disorders.
All patients followed a standardized three-phase rehabilitation program supervised by certified physical therapists. Phase I (postoperative days 1-3) involved ankle pumps, quadriceps sets, and straight leg raises performed 10 repetitions every 2 hours while awake, along with continuous passive motion exercises initiated at 0-30 degrees for 2 hours twice daily, progressing by 10 degrees daily as tolerated. Phase II (postoperative days 4-14) included progressive weight-bearing ambulation with assistive devices, advancing from 25% to full weight-bearing as tolerated, active-assisted and active range of motion exercises for 30 minutes three times daily, and strengthening exercises including mini-squats, step-ups, and resistance band exercises performed for 20 minutes twice daily. Phase III (post-discharge to 12 weeks) consisted of outpatient physical therapy sessions 3 times weekly for the first 6 weeks, then twice weekly for the following 6 weeks, with each session lasting 45-60 minutes and focusing on advanced strengthening, proprioceptive training, and functional mobility exercises.
All patients received standardized TKA surgery and postoperative rehabilitation protocols according to institutional guidelines. All surgeries were performed by experienced orthopedic surgeons under appropriate anesthesia, using a medial parapatellar approach and the same brand of knee replacement prosthesis. Postoperative analgesia used a stan
All patients received a standardized multimodal pain management protocol initiated preoperatively with celecoxib 200 mg administered 2 hours before surgery. Intraoperatively, patients received periarticular injection of a cocktail containing ropivacaine 200 mg, morphine 5 mg, ketorolac 30 mg, and epinephrine 0.5 mg in 100 mL normal saline. Postoperatively, patients were managed with patient-controlled analgesia using morphine (1 mg bolus, 8-minute lockout interval, 4-hour limit of 30 mg) for the first 48 hours. Scheduled oral medications included acetaminophen 1000 mg every 6 hours, celecoxib 200 mg twice daily for 14 days, and oxycodone 5-10 mg every 4-6 hours as needed for breakthrough pain with numerical rating scale (NRS) scores ≥ 4. All patients also received prophylactic antiemetic therapy with ondansetron 4 mg every 8 hours for the first 72 hours. Pain intensity was assessed using the NRS at rest and during physical therapy sessions, with adjustments made to the analgesic regimen if adequate pain control (NRS < 4) was not achieved.
Primary outcomes included: Postoperative hospital stay (defined as days from surgery to discharge); knee joint functional recovery (assessed using the Knee Society Score and Oxford Knee Score at 3 months and 6 months postoperatively, with higher scores indicating better function); and complication rates (including postoperative infection, deep vein thrombosis, prosthesis loosening, and limited joint mobility within 3 months after surgery).
Secondary outcomes included: Neuroendocrine parameters (serum cortisol levels, salivary cortisol awakening response, and urinary catecholamine levels); inflammatory markers (C-reactive protein, erythrocyte sedimentation rate, interleukin-6 and tumor necrosis factor-alpha levels in postoperative drainage fluid); self-care behaviors (measured using the Rehabilitation Adherence Assessment Scale and adherence to physical therapy schedules and nutritional recommendations); sleep quality (assessed using the Pittsburgh Sleep Quality Index); and quality of life measures using the Knee Replacement Quality of Life questionnaire.
Statistical analyses were performed using SPSS version 25.0 (IBM Corp., Armonk, NY, United States). Continuous variables were presented as mean ± SD or median with interquartile range based on data distribution, while categorical variables were expressed as n (%)[20,21]. Multivariate logistic regression analysis was performed to identify independent risk factors affecting functional recovery outcomes, with variables having P < 0.1 in univariate analysis included in the multivariate model. Results were expressed as odds ratios with 95% confidence intervals, and a two-sided P value < 0.05 was considered statistically significant for all analyses. To account for potential confounding factors, propensity score matching and subgroup analyses were performed where appropriate.
Assessment of psychological status in our cohort revealed significant mental health burden among TKA patients. In the study group, the predominant disorders were generalized anxiety disorder (42.3%), major depressive disorder (31.4%), mixed anxiety-depressive disorder (18.6%), and adjustment disorder (7.7%). The severity of these conditions as measured by standardized instruments was considerable, with mean HAMA scores of 19.4 ± 4.2 and HAMD scores of 18.7 ± 3.9, indicating moderate-to-severe psychological distress. Cox regression analysis demonstrated that the duration of psychological symptoms prior to TKA was significantly associated with prolonged recovery time [hazard ratio = 0.74, 95% confidence interval (CI): 0.61-0.89, P < 0.01], suggesting that chronic psychological distress may predispose patients to more difficult functional recovery (Table 1).
| Characteristics | Study group (n = 86) | Control group (n = 100) | P value |
| Demographic characteristics | |||
| Age (years), mean ± SD | 68.4 ± 12.5 | 65.9 ± 13.1 | 0.183 |
| Gender | 0.642 | ||
| Male | 49 (57.0) | 54 (54.0) | |
| Female | 37 (43.0) | 46 (46.0) | |
| BMI (kg/m2) | 23.5 ± 4.1 | 24.1 ± 3.8 | 0.305 |
| Clinical characteristics | |||
| Duration of knee symptoms (months) | 7.8 ± 2.3 | 6.2 ± 1.8 | 0.028 |
| Kellgren-Lawrence grade | 0.731 | ||
| Grade III | 51 (59.3) | 63 (63.0) | |
| Grade IV | 35 (40.7) | 37 (37.0) | |
| Preoperative knee ROM (degrees) | 88.5 ± 15.6 | 95.2 ± 14.3 | 0.136 |
| Knee pain location | 0.840 | ||
| Medial | 45 (52.3) | 55 (55.0) | |
| Lateral | 19 (22.1) | 20 (20.0) | |
| Anterior | 14 (16.3) | 17 (17.0) | |
| Diffuse | 8 (9.3) | 8 (8.0) | |
| Comorbidities | |||
| Diabetes | 32 (37.2) | 33 (33.0) | 0.641 |
| Hypertension | 43 (50.0) | 45 (45.0) | 0.655 |
| Cardiovascular disease | 26 (30.2) | 27 (27.0) | 0.626 |
| Back pain | 15 (17.4) | 16 (16.0) | 0.844 |
Based on the data shown in the table, the results indicate that psychological disorders have a significant negative impact on functional recovery in patients undergoing TKA. The study group (with psychological disorders) demonstrated markedly longer postoperative hospital stays (14.3 ± 3.7 days vs 10.6 ± 2.4 days, P < 0.01) and lower knee function scores at 3 months (68.2 ± 8.5 vs 79.9 ± 7.3, P < 0.05) compared to the control group. The study group also showed significantly higher rates of complications (32.3% vs 17.2%), surgical site infections (18.6% vs 9.5%), and stiffness (14.8% vs 7.0%). Furthermore, patients with psychological disorders exhibited higher rates of persistent pain at 12 weeks (25.6% vs 12.3%), lower knee flexion range of motion (98.4° ± 7.2° vs 112.1° ± 8.9°), and reduced walking distance at 6 weeks (227 ± 66 m vs 341 ± 89 m). The study group required more time to achieve independent ambulation (4.6 ± 1.2 days vs 2.3 ± 0.5 days) and had lower rehabilitation participation scores (6.8 ± 1.3 vs 8.5 ± 1.2). Psychological disorders also negatively affected treatment adherence (67.5% ± 12.3% vs 86.2% ± 9.8%) and patient satisfaction scores (6.4 ± 1.8 vs 8.2 ± 1.4). Overall, all measured indicators consistently demonstrated that patients with psychological disorders experience significantly impaired functional recovery processes and poorer treatment outcomes (Table 2).
| Functional recovery indicator | Study group (n = 86) | Control group (n = 100) | P value |
| Postoperative hospital stay (days) | 14.3 ± 3.7 | 10.6 ± 2.4 | < 0.01 |
| Knee function score at 3 months | 68.2 ± 8.5 | 79.9 ± 7.3 | < 0.05 |
| Complication rate (%) | 32.3 | 17.2 | < 0.05 |
| Surgical site infection rate (%) | 18.6 | 9.5 | < 0.05 |
| Knee stiffness rate (%) | 14.8 | 7.0 | < 0.05 |
| Persistent pain at 12 weeks (%) | 25.6 | 12.3 | < 0.01 |
| Knee flexion ROM at 6 weeks (degrees) | 98.4 ± 7.2 | 112.1 ± 8.9 | < 0.01 |
| Walking distance at 6 weeks (m) | 227 ± 66 | 341 ± 89 | < 0.001 |
| Time to independent ambulation (days) | 4.6 ±1.2 | 2.3 ± 0.5 | < 0.01 |
| Rehabilitation participation score | 6.8 ± 1.3 | 8.5 ± 1.2 | < 0.01 |
| Treatment adherence rate (%) | 67.5 ± 12.3 | 86.2 ± 9.8 | < 0.01 |
| Patient satisfaction score | 6.4 ± 1.8 | 8.2 ± 1.4 | < 0.01 |
Patients in the study group showed significantly elevated stress hormone levels compared to controls, including higher morning serum cortisol [(22.4 ± 5.1) μg/dL vs (15.3 ± 4.2) μg/dL, P < 0.01] and flattened diurnal cortisol rhythms. Inflammatory markers in drainage fluid analysis revealed elevated pro-inflammatory cytokines in the study group, with interleukin (IL)-6 levels [(42.7 ± 9.5) pg/mL vs (26.4 ± 7.3) pg/mL, P < 0.01] and tumor necrosis factor α [(18.9 ± 4.3) pg/mL vs (11.2 ± 3.6) pg/mL, P < 0.01] significantly higher than in the control group, suggesting dysregulated inflammatory responses in patients with psychological disorders (Table 3).
| Parameter | Study group (n = 86) | Control group (n = 100) | P value |
| Neuroendocrine markers | |||
| Morning serum cortisol (μg/dL) | 22.4 ± 5.1 | 15.3 ± 4.2 | < 0.01 |
| Diurnal cortisol rhythm | Flattened | Normal | < 0.01 |
| Evening cortisol (μg/dL) | 12.3 ± 3.2 | 6.8 ± 2.1 | < 0.01 |
| Cortisol awakening response (% increase) | 38.2 ± 9.3 | 72.4 ± 12.6 | < 0.001 |
| Urinary epinephrine (μg/24 hours) | 18.7 ± 4.6 | 12.3 ± 3.8 | < 0.05 |
| Urinary norepinephrine (μg/24 hours) | 65.2 ± 14.3 | 49.6 ± 12.5 | < 0.05 |
| Inflammatory markers | |||
| Drainage fluid IL-6 (pg/mL) | 42.7 ± 9.5 | 26.4 ± 7.3 | < 0.01 |
| Drainage fluid TNF-α (pg/mL) | 18.9 ± 4.3 | 11.2 ± 3.6 | < 0.01 |
| Serum C-reactive protein (mg/L) | 38.4 ± 12.7 | 25.3 ± 9.9 | < 0.05 |
| Erythrocyte sedimentation rate (mm/hour) | 52.6 ± 18.2 | 42.1 ± 16.4 | < 0.05 |
| Drainage fluid IL-1β (pg/mL) | 15.6 ± 3.8 | 9.4 ± 2.7 | < 0.01 |
| Anti-inflammatory IL-10 (pg/mL) | 6.3 ± 1.7 | 11.2 ± 2.4 | < 0.01 |
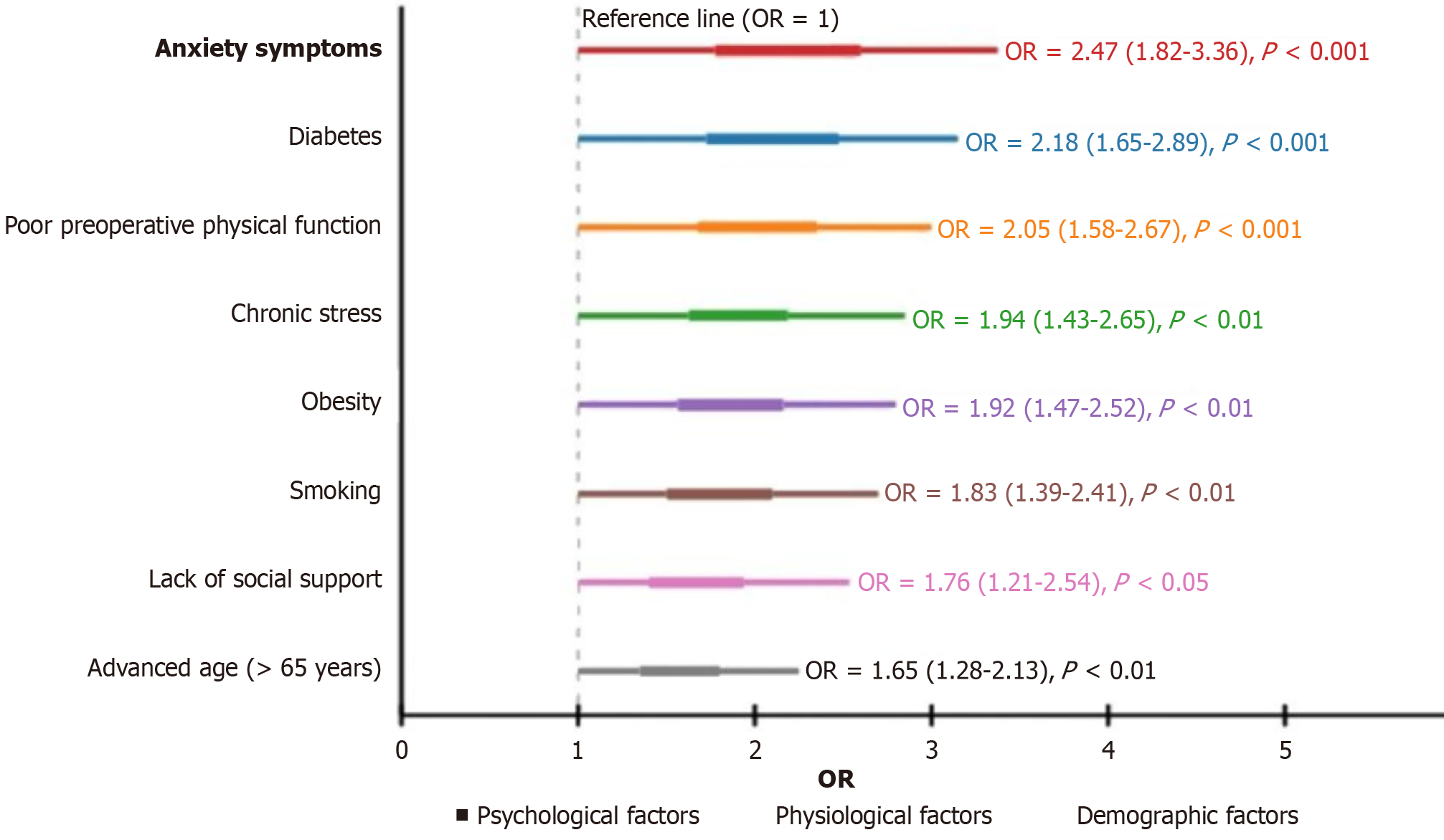
The multivariate logistic regression analysis identified several significant independent risk factors associated with delayed functional recovery. Psychological factors showed strong associations, with anxiety symptoms emerging as the most influential risk factor [odds ratio (OR) = 2.47, 95%CI: 1.82-3.36, P < 0.001], followed by chronic stress (OR = 1.94, 95%CI: 1.43-2.65, P < 0.01) and lack of social support (OR = 1.76, 95%CI: 1.21-2.54, P < 0.05). Physiological factors also demonstrated substantial impact, particularly diabetes (OR = 2.18, 95%CI: 1.65-2.89, P < 0.001) and poor preoperative physical function (OR = 2.05, 95%CI: 1.58-2.67, P < 0.001), both showing highly significant associations with impaired recovery. Obesity (OR = 1.92, 95%CI: 1.47-2.52, P < 0.01) and smoking (OR = 1.83, 95%CI: 1.39-2.41, P < 0.01) represented additional important risk factors, while advanced age (> 65 years) showed the comparatively smallest, though still significant, effect (OR = 1.65, 95%CI: 1.28-2.13, P < 0.01). Notably, all identified risk factors maintained statistical significance as their confidence intervals did not cross the no-effect threshold (OR = 1), indicating the robust nature of these associations even after adjustment for potential confounding variables. This comprehensive analysis suggests that both psychological and physiological factors play crucial roles in functional recovery processes, with implications for developing holistic treatment approaches that address multiple risk domains simultaneously (Figure 1).
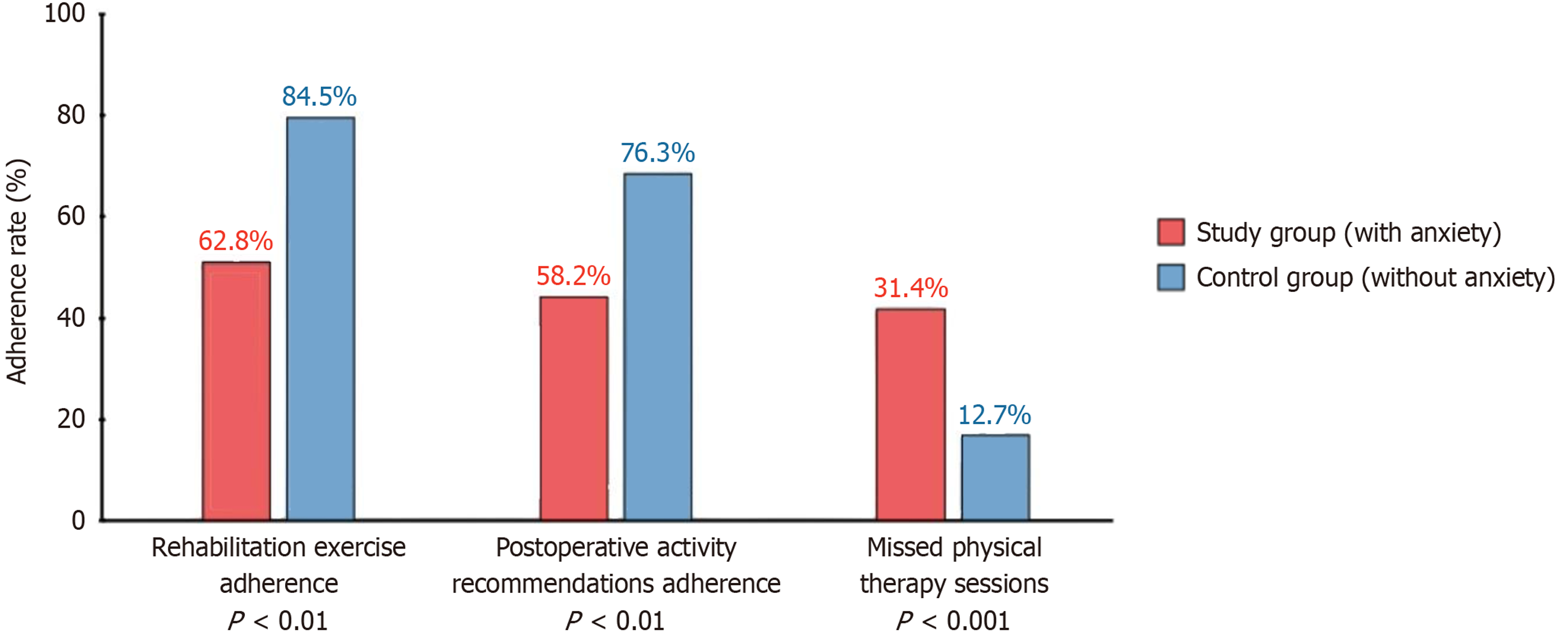
Analysis of self-care behaviors revealed that patients in the study group demonstrated significantly lower adherence to rehabilitation exercise protocols (62.8% vs 84.5%, P < 0.01) and postoperative activity recommendations (58.2% vs 76.3%, P < 0.01). Documentation of missed physical therapy sessions was more frequent in the study group (31.4% vs 12.7%, P < 0.001), highlighting the impact of psychological disorders on treatment adherence and self-management capabilities (Figure 2).
Sleep disturbances were significantly more prevalent in the study group, with higher Pittsburgh Sleep Quality Index scores [(12.3 ± 3.1) vs (7.5 ± 2.4), P < 0.001]. Objective sleep parameters measured through actigraphy confirmed reduced total sleep time [(5.2 ± 1.1) hours vs (6.8 ± 0.9) hours, P < 0.01] and increased sleep fragmentation in patients with psychological disorders. Correlation analysis demonstrated a significant inverse relationship between sleep quality and functional recovery time (r = -0.62, P < 0.001, Table 4).
| Parameter | Study group | Control group | P value |
| Pittsburgh Sleep Quality Index | 12.3 ± 3.1 | 7.5 ± 2.4 | < 0.001 |
| Total sleep time (hours) | 5.2 ± 1.1 | 6.8 ± 0.9 | < 0.01 |
| Sleep fragmentation | Increased | Normal | Not specified |
| Sleep latency (minutes) | 42.7 ± 18.5 | 23.4 ± 11.2 | < 0.01 |
| Sleep efficiency (%) | 68.3 ± 8.7 | 84.6 ± 6.2 | < 0.01 |
| REM sleep (% of total) | 16.2 ± 4.3 | 23.8 ± 3.7 | < 0.01 |
| Nocturnal awakenings (count) | 6.4 ± 2.1 | 3.1 ± 1.4 | < 0.001 |
| Daytime sleepiness (ESS score) | 11.8 ± 3.6 | 6.4 ± 2.8 | < 0.01 |
Knee Replacement Quality of Life instrument scores were significantly lower in the study group across all domains, including physical well-being [(41.2 ± 8.7) vs (58.4 ± 9.1), P < 0.001], psychological well-being [(38.6 ± 7.9) vs (62.3 ± 8.5), P < 0.001], and social functioning [(43.5 ± 9.2) vs (59.7 ± 8.8), P < 0.001]. Regression analysis revealed that improvement in psychological well-being scores during the treatment period was significantly associated with accelerated functional recovery (β = -0.54, P < 0.001), suggesting a bidirectional relationship between psychological status and recovery outcomes (Table 5).
| Domain | Study group | Control group | P value |
| Physical well-being | 41.2 ± 8.7 | 58.4 ± 9.1 | < 0.001 |
| Psychological well-being | 38.6 ± 7.9 | 62.3 ± 8.5 | < 0.001 |
| Social functioning | 43.5 ± 9.2 | 59.7 ± 8.8 | < 0.001 |
| Pain experience | 62.8 ± 10.3 | 45.2 ± 9.7 | < 0.001 |
| Treatment satisfaction | 40.3 ± 8.5 | 67.1 ± 9.4 | < 0.001 |
| Independence/self-care | 39.4 ± 7.8 | 56.8 ± 8.2 | < 0.001 |
| Perceived body image | 35.2 ± 9.1 | 53.7 ± 8.6 | < 0.001 |
| Caregiver burden | 60.1 ± 11.4 | 42.5 ± 9.8 | < 0.01 |
| Overall quality of life | 37.8 ± 6.9 | 60.4 ± 7.8 | < 0.001 |
This retrospective cohort study provides compelling evidence that preoperative anxiety significantly impacts functional recovery outcomes following TKA. Our findings demonstrate that patients with preoperative anxiety disorders expe
The prevalence of anxiety and depression among TKA patients in our study (collectively affecting approximately 42% of patients) aligns with previous literature reporting rates between 25%-60% in orthopedic surgical populations. These rates are substantially higher than the general population, where anxiety disorders affect approximately 10%-18% of individuals, suggesting that chronic pain, functional limitations, and the prospect of major surgery may contribute to or exacerbate psychological distress in this patient cohort. Our findings indicate that generalized anxiety disorder (42.3%) was the most prevalent psychological condition, followed by major depressive disorder (31.4%) and mixed anxiety-depressive disorder (18.6%), representing a significant mental health burden that warrants clinical attention.
The impact of psychological conditions on recovery extends beyond subjective patient experiences, manifesting in objective physiological parameters including elevated stress hormones and pro-inflammatory cytokines[22-24]. The significant differences observed in neuroendocrine markers between our study groups - including morning serum cortisol (22.4 ± 5.1 μg/dL vs 15.3 ± 4.2 μg/dL), flattened diurnal cortisol rhythms, and elevated catecholamine levels - indicate substantial dysregulation of stress response systems in patients with anxiety.
It should be acknowledged that the stress hormones (serum cortisol, urinary catecholamines) and inflammatory cytokines (IL-6, tumor necrosis factor α, IL-10) measured in our study represent peripheral markers that may not fully capture the complex central nervous system mechanisms underlying the psychology-physiology interface. While these peripheral measures provide valuable insights into systemic physiological responses associated with psychological distress, they cannot directly reveal the precise neural pathways, brain region activations, or neurotransmitter systems that mediate the translation of psychological states into altered immune function and tissue healing responses. The relationship between central psychological processes and peripheral joint recovery likely involves multiple integrated systems, including the hypothalamic-pituitary-adrenal axis, sympathetic-adrenal-medullary system, and autonomic nervous system, along with behavioral pathways affecting sleep, nutrition, and treatment adherence. While our data suggest plausible pathways through which psychological distress may impede functional recovery, the exact mechanisms remain incompletely understood and warrant further investigation through more mechanistically-focused studies.
Beyond these physiological mechanisms, our findings highlight the significant behavioral and psychological pathways through which anxiety affects recovery. Patients with anxiety demonstrated markedly reduced adherence to rehabilitation protocols (62.8% vs 84.5%) and poorer participation in physical therapy, suggesting that psychological factors may compromise recovery through reduced engagement with essential rehabilitation components. The documented sleep disturbances in anxious patients (Pittsburgh Sleep Quality Index scores 12.3 ± 3.1 vs 7.5 ± 2.4) likely further compound recovery challenges, as adequate sleep is critical for tissue repair, pain modulation, and cognitive functioning needed for effective rehabilitation participation. Catastrophizing, fear-avoidance behaviors, and hypervigilance - common features of anxiety disorders may additionally contribute to movement hesitancy and suboptimal engagement with physical reco
Multivariate analysis identified anxiety as the strongest psychological predictor of poor outcomes (OR = 2.47, 95%CI: 1.82-3.36), even after controlling for traditional risk factors such as age, diabetes, and smoking status. This independent association highlights the profound influence of psychological factors on recovery trajectories and suggests that preoperative psychological screening and intervention may be as important as managing physical comorbidities when optimizing TKA outcomes. The dose-response relationship observed between psychological symptom duration and recovery time (hazard ratio = 0.74, 95%CI: 0.61-0.89) further emphasizes the importance of early identification and intervention.
The complex interplay between anxiety, pain perception, and functional recovery deserves special consideration. Anxiety is known to lower pain thresholds and amplify pain perception through altered central pain processing, potentially explaining the higher rates of persistent pain at 12 weeks (25.6% vs 12.3%) in our anxiety group. This pain-anxiety cycle can be self-perpetuating, as increased pain fuels further anxiety, catastrophizing, and avoidance behaviors. Research has consistently demonstrated that pain catastrophizing - the tendency to ruminate about, magnify, and feel helpless about pain - is a robust predictor of poor outcomes after TKA. Our findings extend this literature by highlighting how pre-existing anxiety may predispose patients to maladaptive pain cognitions and behaviors that compromise reco
Social support emerged as a significant protective factor in our analysis, with lack of social support increasing risk for poor outcomes (OR = 1.76, 95%CI: 1.21-2.54). This finding aligns with extensive literature on the buffering effects of social support against stress and suggests that psychosocial interventions enhancing support systems may be valuable components of comprehensive care. Patient-reported quality of life was significantly lower across all domains in anxious patients, reflecting the pervasive impact of psychological distress on overall well-being and recovery experience. The bidirectional relationship between quality of life and functional recovery suggests potential value in interventions targeting both domains simultaneously.
Treatment adherence presented a significant challenge for patients with psychological disorders, with markedly lower participation in recommended rehabilitation activities[25-27]. This reduced engagement in physical therapy and home exercise programs likely contributes substantially to poorer functional outcomes and represents a modifiable target for intervention. Cognitive-behavioral approaches addressing specific barriers to adherence, motivational interviewing techniques, and rehabilitation protocols adapted for psychologically vulnerable patients may enhance engagement and outcomes. Digital health technologies offering personalized feedback, goal-setting, and remote monitoring show promise for supporting adherence in patients with psychological barriers to traditional rehabilitation approaches.
Anxiety appears to influence the recovery trajectory through multiple pathways that likely interact and compound each other. These include: (1) Direct neurobiological effects on inflammation, tissue healing, and pain processing; (2) Behavioral effects on treatment adherence, physical activity, and sleep; (3) Cognitive effects including catastrophizing and fear-avoidance beliefs; and (4) Social effects through isolation and reduced support utilization. A comprehensive app
Our study has several important clinical implications. First, routine preoperative screening for anxiety and depression should be considered standard practice before elective TKA, using validated instruments such as the HAMA, HAMD, Hospital Anxiety and Depression Scale, or Patient Health Questionnaire-9. Early identification of psychological risk factors would allow for targeted intervention before surgery, potentially improving outcomes. Second, patients identified with psychological disorders may benefit from preoperative cognitive-behavioral interventions, mindfulness-based stress reduction techniques, or pharmacological management as appropriate. The optimal timing, intensity, and specific components of such interventions warrant further investigation. Third, tailored postoperative rehabilitation programs that address both psychological barriers and physical limitations may improve outcomes for this vulnerable population. Integration of psychological support directly into rehabilitation protocols, rather than as separate services, may enhance effectiveness and accessibility.
Several limitations should be considered when interpreting our findings. The retrospective design precludes definitive causal inferences, and despite careful statistical adjustment, unmeasured confounding factors may influence the observed associations. Assessment of psychological status occurred only at baseline without tracking changes throughout recovery, limiting our understanding of how dynamic psychological states might influence recovery trajectories. While standardized instruments were used to measure anxiety and depression, the subjective nature of some outcome measures introduces potential reporting bias. Additionally, our study was conducted at a single institution, potentially limiting generalizability to different healthcare settings or patient populations.
Future research should explore prospective interventional studies targeting preoperative anxiety to determine if outcomes can be improved through psychological optimization. Randomized controlled trials comparing different psychological intervention approaches (e.g., cognitive-behavioral therapy, mindfulness-based interventions, pharmacotherapy) would help identify the most effective strategies. Mechanistic studies exploring the neurobiological pathways linking anxiety to impaired recovery could identify novel therapeutic targets. Investigation into the cost-effectiveness of routine psychological screening and intervention in TKA populations would provide valuable guidance for resource allocation in increasingly constrained healthcare systems. Finally, development and validation of risk prediction models incorporating psychological factors could enable more personalized approaches to preoperative optimization and rehabilitation planning.
In conclusion, this study highlights preoperative anxiety as a significant and potentially modifiable risk factor for poor functional recovery following TKA. The multifaceted impact of anxiety on recovery processes underscores the need for integrated approaches that address both psychological and physical aspects of patient care. Implementation of routine psychological assessment and targeted interventions may substantially improve outcomes for the many TKA patients affected by anxiety and other psychological conditions.
Preoperative anxiety represents a significant and potentially modifiable risk factor for poor functional recovery following TKA. The impact of psychological disorders on TKA outcomes appears to be mediated through multiple pathways, including neurohormonal changes, inflammatory dysregulation, reduced treatment adherence, and impaired sleep.
It is important to note that while our multivariate regression analysis identified preoperative anxiety as an inde
Preoperative anxiety is a significant and potentially modifiable risk factor for poor functional recovery after TKA. The impact is mediated through multiple pathways including neurohormonal dysregulation, inflammatory changes, reduced treatment adherence, and impaired sleep. However, the retrospective design limits causal inference, and prospective intervention studies are needed to establish whether addressing preoperative anxiety can improve postoperative out
| 1. | Migliorini F, Betsch M, Bardazzi T, Colarossi G, Elezabi HAM, Driessen A, Hildebrand F, Pasurka M. Management of Postoperative Pain Following Primary Total Knee Arthroplasty: A Level I Evidence-Based Bayesian Network Meta-Analysis. Pharmaceuticals (Basel). 2025;18:556. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 2. | Sabater-Martos M, Boadas L, Morata L, Soriano A, Martínez-Pastor JC. Synovial Glucose and Serum-to-Synovial Glucose Predict Failure After Acute Postoperative Infection in Total Knee Arthroplasty. J Clin Med. 2025;14:2841. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 3. | Taylor Iv WL, Bergstein V, Weinblatt A, Long WJ. The financial burden of vancomycin as an alternative to cefazolin for periprosthetic joint infection prophylaxis in total knee arthroplasty. Arch Orthop Trauma Surg. 2025;145:272. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 4. | Choudhury AK, Bansal S, Jain A, Raja BS, Niraula BB, Kalia RB. Conventional rehabilitation post-TKA achieves better knee flexion with higher resource utilization compared to application-based rehabilitation - a systematic review and meta-analysis. J Orthop. 2023;44:77-85. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 5. | Forsyth L, Ligeti A, Blyth M, Clarke JV, Riches PE. Validity of wearable sensors for total knee arthroplasty (TKA) rehabilitation: A study in younger and older healthy participants. Knee. 2024;51:292-302. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 10] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 6. | Zanghelini F, Ponzo A, Xydopoulos G, Fordham R, Khanal S. Cost-Effectiveness of GaitSmart and an Artificial Intelligence Solution for Rehabilitation of Patients Undergoing Total Hip Arthroplasty (THA) and Total Knee Arthroplasty (TKA) in Older Population in the United Kingdom. Geriatrics (Basel). 2024;9:129. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 7. | Liu K, Liu Y, Ma X, Fu D, Fan Z. Effect of cognitive behavioral therapy on pain, knee function, and psychological status in patients after primary total knee arthroplasty: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2024;25:280. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 12] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 8. | March MK. Psychological health and recovery from total knee arthroplasty: a health services perspective (PhD Academy Award). Br J Sports Med. 2023;57:1526-1527. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 9. | Martin JR, Coronado RA, Wilson JM, Polkowski GG, Shinar AA, Bruehl SP. Central Sensitization: The Missing Link Between Psychological Distress and Poor Outcome Following Primary Total Knee Arthroplasty. J Arthroplasty. 2024;39:1201-1206. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 11] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 10. | Springborg AH, Visby L, Kehlet H, Foss NB. Psychological predictors of acute postoperative pain after total knee and hip arthroplasty: A systematic review. Acta Anaesthesiol Scand. 2023;67:1322-1337. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 22] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 11. | Ghijselings I, Taylan O, Delport HP, Slane J, Van den Wyngaert H, Demurie A, Scheys L. Using a patella reduced technique while balancing a TKA results in restored physiological strain in the collateral ligaments: an ex vivo kinematic analysis. Arch Orthop Trauma Surg. 2022;142:1633-1644. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 12. | Jimenez-Soto C, Moya-Angeler J, León-Muñoz VJ, Theus-Steinmann C, Christen B, Calliess T. Maintaining the Physiological Lateral Flexion Gap in the Kinematically Aligned TKA Does Not Compromise Clinical Outcomes at One-Year Follow-Up. J Clin Med. 2024;13:3423. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 13. | Nicolet-Petersen S, Saiz A, Shelton T, Howell S, Hull ML. Kinematically aligned TKA restores physiological patellofemoral biomechanics in the sagittal plane during a deep knee bend. Knee Surg Sports Traumatol Arthrosc. 2020;28:1497-1507. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 16] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 14. | Castañeda P. Healthy Body and Healthy Mind Equal a Happy Life: Commentary on an article by Xiao Geng, MD et al.: "A Randomized Controlled Trial of Psychological Intervention to Improve Satisfaction for Patients with Depression Undergoing TKA. A 2-Year Follow-up". J Bone Joint Surg Am. 2021;103:e28. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 15. | Geng X, Wang X, Zhou G, Li F, Li Y, Zhao M, Chu H, Li J, Si T, Liu Z, Tian H. A Randomized Controlled Trial of Psychological Intervention to Improve Satisfaction for Patients with Depression Undergoing TKA: A 2-Year Follow-up. J Bone Joint Surg Am. 2021;103:567-574. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 33] [Article Influence: 6.6] [Reference Citation Analysis (0)] |
| 16. | Schuster V, Kinne RW, Knoll N, Könczöl C, Anders JO. Prospective pilot study to identify psychological factors influencing peri-operative pain in total knee arthroplasty (TKA). Int Orthop. 2020;44:1271-1280. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 17. | Jin Z, Wang Z, Xu K, Chu J, Xiang S, Tang Y, Wang R, Hua H, Zhang Z, Tong P, Lv S. Effect of anterior femoral cortical notch grade on postoperative function and complications during TKA surgery: A multicenter, retrospective study. Open Med (Wars). 2024;19:20240932. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 18. | Schmeling GJ. Fourteen Percent of Complex Tibial Plateau Fractures Need a TKA: Commentary on an article by Nick Assink, MSc, et al.: "Radiographic Predictors of Conversion to Total Knee Arthroplasty After Tibial Plateau Fracture Surgery: Results in a Large Multicenter Cohort". J Bone Joint Surg Am. 2023;105:e41. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 19. | van der Linde ML, Baas DC, van der Goot TH, Vervest AMJS, Latour C. Biopsychosocial complexity in patients scheduled for elective TKA surgery: A feasibility pilot study with the INTERMED self-assessment questionnaire. Int J Orthop Trauma Nurs. 2024;53:101094. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 20. | Tian C, Chen H, Shao W, Zhang R, Yao X, Shu J. Accuracy of machine learning in identifying candidates for total knee arthroplasty (TKA) surgery: a systematic review and meta-analysis. Eur J Med Res. 2025;30:317. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 21. | Vermue H, Arnout N, Tampere T, Stroobant L, Dereu A, Victor J. Reply to the Letter to the Editor: Standardized Intraoperative Robotic Laxity Assessment in TKA Leads to No Clinically Important Improvements at 2 Years Postoperatively: A Randomized Controlled Trial. Clin Orthop Relat Res. 2025;483:2396-2397. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 22. | Aubet B, Martin-Krumm C, Trousselard M. Fostering hope and recovery: enhancing psychological resources in military personnel with post-traumatic stress disorder. Mil Med Res. 2025;12:17. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 23. | Intharit J, Nghiep LK, Tudpor K. Stress-Monitoring Device Identifies Psychological Stress Reduction Through Psychoeducation in Informal Caregivers of Schizophrenia Patients. Stud Health Technol Inform. 2025;323:478-482. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 24. | Ndjomo G, Njiengwe E, Moudze B, Guifo O, Blairy S. Posttraumatic stress, anxiety, and depression in mothers after preterm delivery and the associated psychological processes. BMC Pregnancy Childbirth. 2025;25:413. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 25. | Hwang UJ, Kim JS, Chung KS. Machine Learning Predictions of Subjective Function, Symptoms, and Psychological Readiness at 12 Months After ACL Reconstruction Based on Physical Performance in the Early Rehabilitation Stage: Retrospective Cohort Study. Orthop J Sports Med. 2025;13:23259671251319512. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 26. | Nowogrodzka A, Andrusiewicz M, Mojs E. Psychological Determinants of Conflict with the Law and Susceptibility to Rehabilitation in Relation to the Presence of Symptoms of Attention Deficit Hyperactivity Disorder. Brain Sci. 2025;15:141. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 27. | Vigorè M, Sattin D, Maestri R, Bussotti M, Ranucci L, Parma C, Maioli R, Triffiletti A, Scuotto RS, Parazzoli P, Dalla Vecchia LA, Gorini A. Beyond the heart: The role of psychological factors and coping strategies in cardiovascular rehabilitation. Int J Cardiol. 2025;428:133144. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/