INTRODUCTION
Over the past two decades, mental health concerns among youths in the United States have increased significantly, so much so that this surge has been declared a public health emergency[1]. In 2021, several professional organizations formally recognized a global mental health crisis in children and adolescents[2-5]. It is estimated that 20%-25% of United States children and adolescents will be diagnosed with a mental health disorder during their lifetime[6,7], and nearly 10% of all hospital admissions for those aged 3 to 20 are directly related to mental health conditions[6,8].
Psychiatric care for children and adolescents is delivered across a broad continuum of settings, beginning with outpatient services (e.g., office visits), and followed by home-based intensive therapy programs such as wraparound services. More intensive levels of care include partial hospitalization programs (PHP), intensive outpatient programs (IOP), inpatient psychiatric hospitalizations, and residential treatment facilities (RTFs)[9]. Inpatient care, the most restrictive level, is typically reserved for youths who are acutely unsafe or unable to engage in less intensive settings[9].
Since the deinstitutionalization movement in the 1960s, psychiatric care in the United States has shifted from long-term hospitalization to short-term, acute models, with marked reductions in inpatient beds[10,11]. Consequently, both psychiatric admissions and readmissions have increased over time[10,12-14]. Between 2006 and 2011, pediatric psychiatric admissions rose by more than 50%, with associated healthcare expenditures reaching approximately 11.6 billion dollars[15]. Notably, hospitalization rates increased nearly fivefold among youths with psychiatric diagnoses compared to those without[16].
Psychiatric readmissions are a significant concern in youth mental health care. Readmission is typically defined as any psychiatric hospitalization that occurs following discharge from a previous inpatient stay. It is estimated that between 33% and 38% of youths are readmitted to a psychiatric unit within 12 months of discharge[17]. Notably, most readmissions occur within the first 90 days after discharge[18]. Psychiatric admissions, and especially readmissions, can significantly disrupt a youth’s social support systems and academic functioning[19,20]. In addition, inpatient stays place substantial strain on families and the healthcare system, particularly in underserved areas where hospitalizations may require long-distance travel[6]. While multiple factors have been suggested and explored as predictors of psychiatric readmissions in youths, the existing literature remains inconclusive. This literature minireview aims to address these gaps by comprehensively examining key predictors of psychiatric readmission in youths, identifying areas for future research, and contributing to the development of clinical strategies to reduce the risk of psychiatric readmissions in this population.
LITERATURE SEARCH
This narrative literature minireview examines the predictors of psychiatric readmissions in children and adolescents. It synthesizes findings from major databases, including PubMed and PsycINFO, using a comprehensive search strategy limited to studies published in the English language. Keywords included readmission, rehospitalization, predictors, children, adolescents, safety, suicide, self-injurious behavior, and aggression. Studies published between 2003 and 2025 were included. In addition, the reference lists of the retrieved articles were reviewed to ensure that all relevant studies were considered. We classified the identified predictors into five domains, psychosocial factors, clinical characteristics, treatment-related factors, system-level factors, and sociodemographic factors. The first section examines psychosocial factors, including childhood adversity and trauma, family factors, and environmental factors. This is followed by clinical characteristics, including diagnostic categories, suicidal ideation and safety concerns, neurodevelopmental disorders, and substance use disorders. In the next section, treatment-related factors are presented, including prior hospitalization, length of stay (LOS) of prior hospitalization, treatment adherence and medication-related factors, discharge and disposition planning, and aftercare services, and system-level variables such as insurance status, and referral and discharge circumstances. Finally, a minireview of sociodemographic variables such as education, age, gender, race and ethnicity was conducted.
PSYCHOSOCIAL FACTORS
Childhood adversity and trauma
Adverse childhood experiences (ACEs), including neglect, physical abuse, and sexual abuse, are strongly associated with long-term negative outcomes such as poor academic performance and psychiatric disorders. These outcomes often follow a dose-response pattern, where greater exposure to ACEs is linked to more severe consequences[21]. Several studies have examined the link between ACEs and psychiatric readmission. In Canada, a retrospective study of adolescents (aged 12-17 years) found that a history of sexual abuse was associated with 29% higher odds of readmission[22]. Similarly, a United States cohort study of 366 youths (aged 11-18 years) reported that trauma exposure tripled the likelihood of readmission within 12 months, while bullying doubled the risk[6].
Evidence regarding “personal loss” as an adverse experience has been more mixed. Eichstadt et al[23] found that loss of a loved one was not significantly associated with readmission among adolescents. In contrast, Bobier and Warwick[24], in a smaller study of 71 inpatients, reported that personal loss, including the end of a romantic relationship or the death of a family member/friend, was negatively associated with readmission, suggesting a potential protective effect. It is likely that such experiences may mobilize support systems or coping mechanisms that buffer against readmission.
Family factors
Parental psychiatric history and family dynamics are important factors influencing psychiatric readmission[22]. In a retrospective study of 1231 youths (aged 5-17 years), 13.4% of readmissions were attributed to caregiver stress and parental psychiatric illness[25]. Similarly, Eichstadt et al[23] found that 52.2% of readmitted adolescents had a parental history of mental illness compared with 37.5% of those not readmitted, with parental psychiatric illness nearly doubling the risk of readmission. Harsh parental discipline and disengaged parent-child relationships have also been linked to higher readmission rates[10,26].
Adolescents cared for by non-parental guardians (e.g., relatives, state-appointed caregivers) are at increased risk of readmission compared with those cared for by parents[13,27-29]. Studies suggest that parental caregiving is generally associated with more favorable post-discharge outcomes[13,23,28]. However, findings are not universal: A Portuguese study reported no significant differences in readmission rates based on the identity of the primary caregiver[30].
Environmental factors
Environmental factors play a critical role in shaping psychiatric outcomes after discharge. Geographic location, housing stability, and neighborhood characteristics influence readmission risk in children and adolescents. Youths residing in underserved or rural areas are at elevated risk of readmission[18,31]. Neighborhood context also appears important: Higher community crime rates have been linked to greater readmission risk[27], although interpersonal relationship difficulties specifically were not significantly associated with readmission[23]. Living arrangements further contribute to risk. Adolescents placed in group homes, assisted care settings, or suburban environments have shown higher readmission rates[22,25]. Conversely, one study reported that youths from upper-middle socioeconomic backgrounds and non-rural areas were more likely to be readmitted, suggesting that socioeconomic advantage does not uniformly confer protection[32]. Among vulnerable populations such as children and adolescents in state custody, environmental context and service availability appear particularly critical. Fewer post-hospital service hours and placement in congregate settings before the index admission predicted higher readmission risk[13]. Similarly, in a large retrospective study of 2445 youths, Stewart et al[22] found that prior police involvement, whether related to violent or nonviolent offenses, was associated with an increased likelihood of readmission.
CLINICAL CHARACTERISTICS
The relationship between specific psychiatric diagnoses and readmission risk has been mixed. Diagnoses such as schizophrenia, bipolar disorder, and other psychotic disorders have consistently been associated with elevated readmission rates[10,32,33], and psychotic disorders appear more predictive of readmission than mood or affective disorders[32]. While somatoform, stress-related, and neurotic disorders were linked to increased 30-day readmissions, psychotic disorders were associated with higher readmission rates within one year[34]. Behavioral problems, particularly severe conduct issues, also increase the risk of readmission[10,26]. Neurodevelopmental disorders, including autism spectrum disorder and intellectual disability, are associated with both longer hospitalizations and higher readmission risk[24,27,31]. Among youths aged 3-17 years, co-occurring psychiatric disorders such as post-traumatic stress disorder and schizophrenia further increase the odds of readmission[10].
However, not all studies find a clear relationship between primary psychiatric diagnosis and readmission. Eichstadt et al[23] did not observe an association between neurocognitive, schizophrenia spectrum, bipolar, or depressive disorders and readmission. Similarly, a study from Portugal[30] and a study from New Zealand[24] found no association between psychiatric comorbidities/diagnoses and risk of readmission. Furthermore, a systematic review found no relationship between functional status, psychiatric comorbidities, and readmission risk[31].
Suicidal ideation and suicide attempts are consistently associated with higher readmission rates[18,23,27,35,36]. Youths with suicidal ideation are readmitted more frequently than those without, and approximately 18% of adolescent readmissions (aged 10-19 years) involve self-poisoning[37]. These findings are supported by evidence indicating that around 73% of readmissions are triggered by illness-related symptom exacerbation due to numerous factors including medication non-compliance and natural course of illness[25].
Substance use disorders also appear to influence readmission risk. Eichstadt et al[23] reported higher readmission rates among youths with substance use disorders, and Bartoli et al[38] identified comorbid substance use as a predictor of early readmission among individuals ≤ 25 years old. Interestingly, a systematic review found that youths with substance use disorders were at lower risk for psychiatric readmission compared with those without such comorbidity, potentially reflecting suboptimal access to psychiatric care or referral to substance use services rather than inpatient psychiatric units[27].
TREATMENT-RELATED FACTORS
Prior hospitalization
A history of psychiatric hospitalization has been consistently identified as a strong predictor of readmission[27,39]. This association has been observed across multiple countries, including Canada[40], Portugal[30], Finland[34], and other European countries such as Italy and Slovenia as part of the “Comparative Effectiveness Research on Psychiatric Hospitalization by Record Linkage of Large Administrative Data Sets” project on predictors of readmission[41]. Furthermore, the relationship between prior hospitalization and subsequent readmission appears to follow a dose-response pattern, with the likelihood of experiencing two or more readmissions increasing proportionally with the number of previous psychiatric hospitalizations[34].
LOS of prior hospitalization
LOS has been identified as a predictor of psychiatric readmission[30]. Across studies, the average LOS ranges from 7.4 days to 21.3 days, depending on the population studied[22]. Youths diagnosed with certain conditions such as schizophrenia or intellectual disability tend to have longer hospitalizations compared with those with other conditions, such as adjustment disorder[22]. Interestingly, both shorter and longer LOS have been associated with increased readmission risk[17,27,31]. For example, LOS shorter than 15 days has been linked to higher readmission rates, particularly among youths with eating disorders[10,42,43]. Conversely, some studies have found that the risk of readmission increases by 1% for every additional five days of hospitalization[32], and in a prospective cohort study, each additional hospital day increased the odds of readmission by 17%, with duration of the initial hospitalization identified as the only significant predictor[19]. However, other research did not find an association between LOS and 30-day readmission risk[34]. Psychiatrist caseload also appears to influence both LOS and readmission. In a Taiwanese study, higher patient volumes were associated with shorter LOS and increased readmission rates[43]. Similarly, Kagabo et al[10] reported that psychiatrists with larger caseloads had patients with both shorter hospitalizations and higher readmission rates.
Treatment adherence and medication-related factors
Treatment non-adherence is a consistent and critical predictor of psychiatric readmission. Readmitted youths consistently demonstrate higher rates of non-compliance with treatment plans compared to non-readmitted peers. For example, one study reported that 47% of readmitted adolescents were noncompliant, compared to 11% of non-readmitted youths, with non-adherence increasing the odds of readmission more than ninefold[23,24]. Similarly, a South African retrospective study found higher rates of non-adherence, measured by outpatient attendance and serum drug levels, among readmitted patients (38.1% vs 10.5%)[23]. A United States Medicaid cohort also observed that medication non-compliance was associated with increased readmission risk[18], and a New Zealand study reported a positive association between non-adherence, defined as discontinuation without professional guidance or failure to take medications as prescribed, and readmission in a small sample of adolescents[24]. In contrast, a prospective study found that 24% of patients who discontinued psychiatric medications after discharge were readmitted compared to 36% who continued treatment; however, this difference was not statistically significant[26]. In addition, polypharmacy, defined as the use of three or more psychiatric medications, and the addition of new drugs to existing regimens have been associated with higher readmission rates, potentially reflecting greater illness severity, poor medication management, or unrecognized non-adherence[31]. The type of medication prescribed during the index hospitalization may also influence outcomes; for example, prescription of an antipsychotic medication has been identified as a risk factor for readmission within one year[25].
Discharge and disposition planning
Residential treatment settings, therapeutic foster care, and varying levels of outpatient support all influence the risk of psychiatric readmission. Readmission rates are significantly higher among patients discharged to other treatment settings, such as long-term placements, compared to those discharged home[27,37]. Youths discharged from RTFs face a substantially higher readmission risk than those leaving nonresidential care[27], particularly if they have a prior history of RTF placement[10,31]. This association may reflect more severe psychopathology or, alternatively, the reinforcement of maladaptive behaviors, as youths in RTFs are often exposed to peers with significant emotional and behavioral challenges[31]. By contrast, therapeutic foster care has demonstrated more favorable outcomes. Retrospective studies show that children in therapeutic foster care exhibit greater improvements in self-esteem and reductions in aggression compared to those in RTFs, with these gains more likely to persist after discharge, leading to lower readmission rates[44]. Similarly, youths readmitted later in the year, rather than within 30 days, were more likely to have been living in RTFs rather than foster care or with their families[25]. Hospitalization often functions as a transitional placement for children in state custody[13]. For these children, inpatient psychiatric care may be driven by factors beyond clinical need, such as the search for a new placement[13]. Notably, a significant proportion of youths referred from RTFs to inpatient care did not meet standard clinical criteria, suggesting that RTFs may operate with a lower threshold for psychiatric admissions[31].
IOP and PHP also show complex relationships with readmission risk. James et al[19] found that neither IOP or PHP alone significantly reduced readmission risk. The effectiveness of these programs may depend on discharge planning and family involvement[19]. Paradoxically, youths who completed only IOT or PHP, as well as those receiving no follow-up support, were more likely to be readmitted. This may reflect the enhanced monitoring inherent in intensive programs, which can identify youths discharged prematurely or unable to maintain symptom stability, resulting in appropriate readmissions[19]. In this context, readmission, though often viewed negatively, can represent an appropriate clinical response when a patient continues to pose a danger to themselves or others.
Aftercare services
High rates of readmission have been linked to inadequate aftercare planning at discharge. A retrospective analysis of national inpatient data found that patients with limited outpatient service availability were at increased risk of readmission[26], and a population-based cohort study estimated that 24% of adolescents had an outpatient appointment (i.e., with psychiatrist or primary care provider) within seven days while 49% had an appointment within 30 days[17]. Despite this gap, the impact of aftercare on readmission has been inconsistent. Some studies indicate a protective effect of aftercare services[13], whereas others report no benefit or even a positive association with readmission[17,18,26,45]. For example, youths who attended an aftercare appointment immediately post-discharge were more likely to be readmitted compared to those who did not, even after adjusting for demographic (e.g., age) and clinical variables (e.g., primary psychiatric diagnosis)[25]. Similarly, adolescents receiving aftercare within 30 days were 22% more likely to have an emergency department visit or readmission overall, and 38% more likely to experience readmission alone[17]. In contrast, a retrospective study reported that greater hours of aftercare services reduced readmission risk, with higher engagement in PHPs associated with lower likelihood of readmission within six months[46]. Overall, both engagement with aftercare services and adherence to post-discharge treatment plans are important predictors of readmission[22,23].
Several demographic and clinical factors influence whether youths receive aftercare. Youths living in urban areas or higher-income neighborhoods, females, patients with prior outpatient treatment, those with comorbid psychiatric conditions (e.g., mood, anxiety, personality, or psychotic disorders), and those with longer inpatient stays were more likely to receive follow-up care[40]. Conversely, youths with substance use or organic disorders, those in rural areas, and patients who left against medical advice were less likely to receive aftercare[40]. Youths referred to medical providers were also more likely to be readmitted than those referred to law enforcement, community-based services, or those discharged without a formal referral[32].
SYSTEM-LEVEL FACTORS
Insurance status
Children and adolescents with public insurance are more likely to experience readmission following psychiatric hospitalization[31,47,48]. In a large retrospective cohort of 253,309 psychiatric admissions among youths aged 5-17 years, children with public insurance had significantly higher 30-day readmission rates compared to those with private insurance[47]. Similarly, Soutullo et al[48] identified public insurance status as a significant predictor of increased readmission risk. Analysis of Medicaid claims data from four states revealed that youths eligible through disability had higher odds of both single and multiple readmissions, likely reflecting greater illness burden[49]. Interestingly, that study also found that youths treated at hospitals with a higher proportion of Medicaid discharges were less likely to be readmitted, suggesting potential institutional or systemic factors influencing readmission risk[49].
Referral and discharge circumstances
The circumstances of admission and discharge can reflect underlying clinical severity, available support systems, and treatment adherence, all of which influence the likelihood of readmission. While one study found no significant differences in mental health service involvement or follow-up between readmitted and non-readmitted youths[30], another reported that system-of-care factors, such as treatment not covered by insurance or inability to access needed services, accounted for only 13% of readmissions, emphasizing the greater role of individual and contextual variables[25]. Youths referred for hospitalization by medical professionals are more likely to be readmitted than those referred by family members or who self-referred. Similarly, patients evaluated in the emergency department prior to admission have a 33% higher likelihood of readmission compared to those admitted directly from outpatient services or clinics. Finally, being discharged against medical advice or transferred to another facility, rather than returning home, has also been associated with increased readmission risk[32].
SOCIODEMOGRAPHIC FACTORS
Education
Higher educational attainment and ongoing school enrollment appear to be protective against psychiatric readmission in youths. A systematic review reported that higher education may reduce readmission risk[41]. In a retrospective cohort of 2445 youths admitted to inpatient psychiatric care, higher educational levels were associated with shorter lengths of stay and lower risk of readmission[22]. Similarly, a South African study of 97 adolescents found that being enrolled in school at discharge and having higher educational attainment were associated with reduce likelihood of readmission[29]. Ongoing school enrollment was also associated with decreased readmission risk in a more recent study[23].
Age
Younger age at initial hospitalization has been identified as a potential predictor of psychiatric readmission in some studies. A retrospective study found that younger age significantly predicted readmission[23]. Similarly, Canadian data reported that younger age was associated with higher readmission risk[22], a trend also observed in a 10-year follow-up study[50]. Youths aged 11 to 15 years have been specifically identified as a high-risk group, coinciding with the typical onset of affective disorders or early-onset psychosis[32,51]. In contrast, several studies found no clear association between age and readmission. A South African study did not observe an age-related effect[29], and a Portuguese study reported no association at either 30 days or 12 months post-discharge[30]. Additional research similarly reported no consistent relationship between age and readmission risk[6,18]. A recent systematic review of studies involving youths aged 21 years or younger concluded that the evidence on age as a predictor of psychiatric readmission remains inconclusive[31].
Gender
Male gender has been associated with an increased likelihood of psychiatric readmission in several studies. A population-based study from Taiwan reported that males were significantly more likely to be readmitted both within 14 days and at longer-term follow-up[43]. Similarly, a United States retrospective cohort found male gender to be a significant predictor of readmission among children and adolescents[10]. Other studies have also identified male gender as a risk factor, even with follow-up extending to one year[32,33]. In contrast, some studies, including research from Finland and South Africa, did not find gender to be a significant predictor of readmission[6,18,23,31,34]. Notably, gender-diverse youths, such as transgender youths, appear to be at higher risk for readmission within 30 days post-discharge compared to cisgender peers[42].
Race and ethnicity
In a retrospective study, Black youths were significantly more likely to be readmitted within 12 months compared to White youths[48]. However, evidence on the role of race and ethnicity in psychiatric readmission remains inconclusive. A systematic review of risk and protective factors in youths reported mixed findings[31], whereas another systematic review and meta-analysis found no evidence that race or ethnicity directly predicted readmission[27].
DISCUSSION
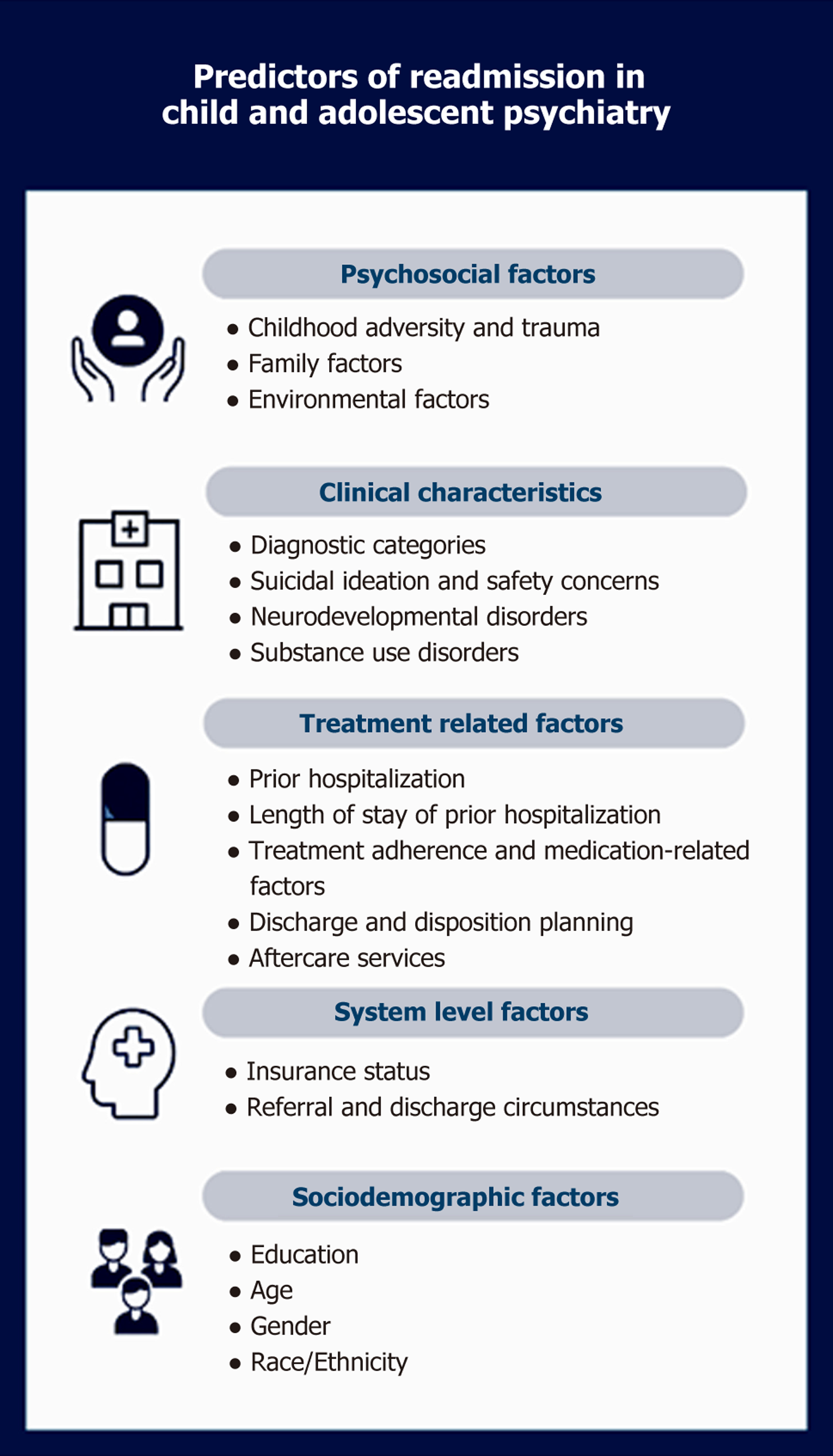
This narrative minireview examined a wide range of factors associated with psychiatric readmissions in children and adolescents. Overall, no single factor independently predicts readmission risk; rather, outcomes are shaped by a complex interplay of clinical, sociodemographic, systemic, and treatment-related variables, with relationships often context-dependent (Figure 1). Psychosocial stressors, including exposure to ACEs, are consistently associated with higher readmission risk. In contrast, sociodemographic factors, such as age, gender, and race, have shown inconsistent associations. Notably, psychosocial factors are often influenced by systemic inequities, including neighborhood income and place of residence, which do not necessarily affect sociodemographic characteristics to the same extent[18,27,31]. Personal loss, such as the death of a loved one, has demonstrated either a protective effect[24] or a neutral effect[23] on readmission risk. These divergent findings may reflect environmental influences, including home stability and social support, as well as cultural factors shaping responses to grief. Suicidality has been consistently associated with higher readmission risk. However, primary psychiatric diagnosis has limited predictive utility due to variable findings across studies. A history of psychiatric hospitalization substantially increases readmission risk, with the likelihood rising proportionally with the number of prior admissions.
Figure 1 Predictors of readmission in child and adolescent psychiatry.
Aftercare services are critical, although evidence regarding their effectiveness is mixed. Engagement with outpatient services and adherence to treatment plans remain essential, as treatment nonadherence consistently predicts increased readmission risk. PHPs are valuable for monitoring high-risk or complex patients post-discharge, identifying those requiring readmission, and reducing inpatient costs[19,52-54]. Telehealth offers a flexible, cost-effective alternative for patients unable to access in-person services due to geographic or scheduling barriers[55-57]. Psychoeducation regarding medication adherence and follow-up[58], along with patient involvement in safety and aftercare planning, can improve compliance and rapport with providers, potentially reducing readmissions[23,59].
Youths with public insurance, particularly Medicaid, consistently face higher readmission risk. This likely reflects both greater clinical complexity and systemic barriers, such as limited access to community resources, poverty, environmental challenges, and family stressors[60]. This finding underscores the need for policy-level interventions aimed at enhancing the capacity of healthcare centers, particularly in underserved areas, to evaluate and treat more patients, as well as increasing funding for case management programs that facilitate outpatient service delivery and improve patient and family compliance.
While most studies identified treatment non-adherence or non-compliance as a predictor for readmission[18,23,24], Blader[26] reported an opposite trend, finding that patients who continued taking their medications after discharge were more likely to be readmitted than those who discontinued them. This counterintuitive finding may reflect illness severity: Patients with more severe symptoms may have remained adherent to medications yet still required readmission, whereas those with milder symptoms could discontinue treatment without requiring readmission. Similarly, the observation that prescription of antipsychotic medications was identified as a risk factor for readmission within a year[25], may also be explained by this disease severity hypothesis, as individuals prescribed antipsychotic medications generally present with more severe psychopathology.
Placement and disposition factors, including discharge to RTFs or state custody, increase readmission risk. Given the more favorable outcomes associated with therapeutic foster care, this option should be considered when clinically appropriate. Robust community programs and social services are needed to ensure stable placements for children involved with child protective services. System-level interventions, including improved access to outpatient psychiatry and psychotherapy, expansion of treatment options such as PHPs, and strengthening school-based mental health programs through increased funding and recruitment of qualified staff, are critical. Telehealth has mitigated some structural and financial barriers, improving appointment adherence and patient-perceived quality of care[55-57].
This minireview also revealed inconsistent and/or contradictory findings across multiple predictor categories such as sociodemographic factors, and the association between primary psychiatric diagnosis and readmission risk. This is likely related to methodological differences of the studies included (e.g., empirical observational studies, quality improvement studies), population heterogeneity (e.g., some studies referred to participants as “youth” while others specified the ages included), variability in the definition of “readmission” as an outcome, and cultural and health care model differences, considering studies from different countries were included.
Specialized interventions, including standardized workflows, checklists, individualized post-discharge plans incorporating dialectical behavioral therapy, follow-up phone calls, conflict management groups, and family education, have demonstrated effectiveness. These interventions led to a 49% reduction in 7-day readmissions and a 36% reduction in 30-day readmissions[61]. Similarly, the Community Advocacy and Resource Engagement Team, a short-term post-discharge program providing case management and therapeutic support, reduced emergency department mental health visits by 58.4%, psychiatric readmissions by 18.7%, and the combined outcome of emergency department mental health visits or psychiatric admissions by 15%[62]. Effective strategies to reduce psychiatric readmissions must be multifaceted. Enhanced outpatient follow-up, structured psychoeducation, and risk assessment models incorporating clinical, psychosocial, and system-level factors are critical[23,52]. Special attention is required for vulnerable populations, including youths in state custody, those with trauma histories, and those from underserved communities who face compounded structural inequities. Efforts should address multiple domains simultaneously.
Policies should prioritize early identification of individuals at risk for readmission through comprehensive screening, alongside community programs providing accessible behavioral health services and school-based interventions. Improved discharge planning, strengthened aftercare, family-focused interventions, culturally responsive care models, enhanced provider continuity, reduced psychiatrist caseloads, and expanded outpatient access are all essential for lowering readmission rates. Future research should systematically examine both risk and protective factors and develop reliable models for predicting readmission. Longitudinal study designs are needed to capture temporal patterns and causal pathways. Additionally, studies should include underrepresented ethnic groups (e.g., Hispanic youths) and compare outcomes across socioeconomic strata (e.g., middle vs low socioeconomic status). This minireview did not differentiate readmission by developmental period, which should also be considered in future investigations.
CONCLUSION
While psychiatric readmission is sometimes clinically necessary to ensure safety and stabilization, it can negatively impact a young person’s social relationships, academic functioning, and overall development. A wide range of factors, including sociodemographic characteristics, psychosocial challenges, clinical presentations, treatment history, and system-level barriers, contribute to readmission risk. Addressing this complex issue requires a multifactorial approach that prioritizes individualized risk assessment, incorporating the unique combination of factors present in each youth. Strengthening mental health services and improving access to comprehensive community-based care are critical steps toward reducing readmission and supporting sustained recovery.
Provenance and peer review: Invited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Psychiatry
Country of origin: United States
Peer-review report’s classification
Scientific Quality: Grade A, Grade B, Grade E
Novelty: Grade B, Grade B, Grade D
Creativity or Innovation: Grade B, Grade B, Grade B
Scientific Significance: Grade B, Grade B, Grade D
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/
P-Reviewer: Avcı M, PhD, Assistant Professor, Türkiye; Awad AA, MD, Researcher, Egypt; Takım U, MD, Assistant Professor, Türkiye S-Editor: Wu S L-Editor: Webster JR P-Editor: Zhang YL