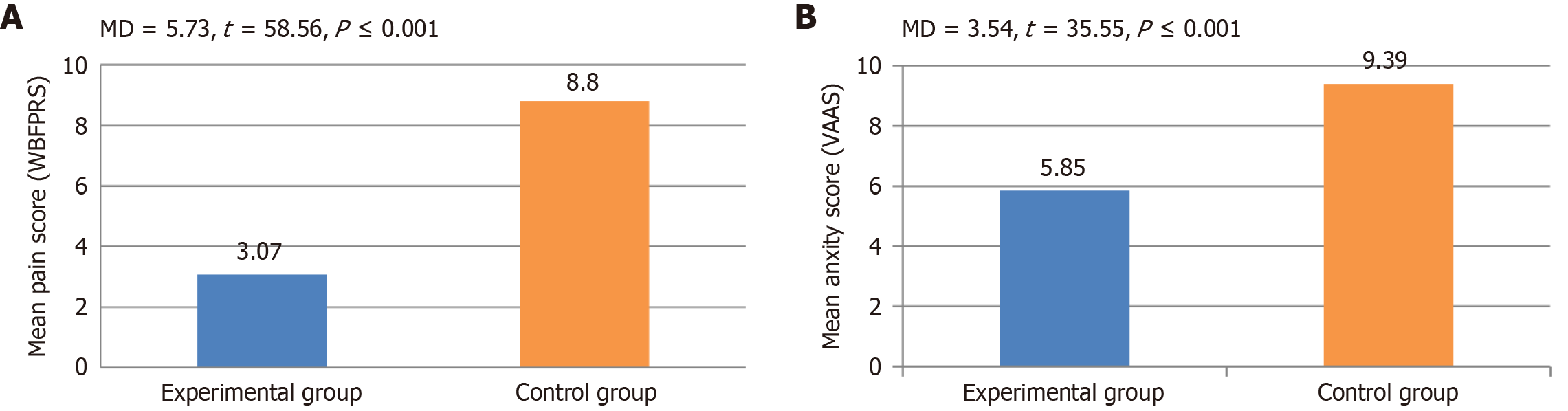Published online Mar 9, 2026. doi: 10.5409/wjcp.v15.i1.111388
Revised: July 27, 2025
Accepted: October 29, 2025
Published online: March 9, 2026
Processing time: 251 Days and 3.9 Hours
Hospitalization and intravenous (IV) procedures are known to provoke significant pain and anxiety in preschool children, potentially leading to long-term psychological distress. Despite growing evidence supporting distraction techniques, practical, low-cost interventions suited for resource-limited settings remain underutilized.
To determine the effectiveness of a nurse-led multimodal distraction intervention – comprising balloon blowing, art therapy, and kaleidoscope use – in reducing pain and anxiety during IV therapy among hospitalized preschool children.
A posttest-only controlled observational study was conducted at Shri Vinoba Bhave Civil Hospital, India. A total of 600 hospitalized preschoolers (aged 3-6 years) were randomly allocated to either an experimental group (n = 300; dis
Children in the experimental group had significantly lower pain scores [mean ± SD (3.07 ± 1.39)] than the control group (8.80 ± 1.01) (t = 58.56, P < 0.00001). Anxiety levels were also reduced in the experimental group (5.85 ± 1.56 mm) compared to controls (9.39 ± 0.73 mm) (t = 35.55, P < 0.00001). A moderate positive correlation was found between pain and anxiety in both groups (experimental: r = 0.67; control: r = 0.66; P < 0.05). Significant associations were also found between pain levels and variables such as age, IV site, cannula size, and medication type (P < 0.05).
This study demonstrates that a simple, low-cost, nurse-led multimodal distraction strategy can significantly reduce pain and anxiety in preschool children undergoing IV therapy. Its ease of use and scalability make it highly suitable for immediate integration into pediatric care, especially in low-resource healthcare settings.
Core Tip: This study highlights the effectiveness of a low-cost, multimodal distraction approach – combining balloon blowing, art therapy, and kaleidoscope use – in reducing pain and anxiety among preschool children undergoing intravenous therapy. Using validated tools like the Wong-Baker Faces Pain Rating Scale and Visual Analogue Anxiety Scale, the intervention showed significant impact. It offers a scalable, nurse-led solution for procedural pain management in low-resource settings, where expensive technologies like virtual reality are often impractical.
- Citation: Wilson LP, Khan Z, Patil PN, Konnur RG, Sriram N. Multimodal distraction reduces intravenous cannulation pain and anxiety in preschoolers: Controlled prospective study. World J Clin Pediatr 2026; 15(1): 111388
- URL: https://www.wjgnet.com/2219-2808/full/v15/i1/111388.htm
- DOI: https://dx.doi.org/10.5409/wjcp.v15.i1.111388
Children constitute one-third of the global population and represent humanity’s most vital future resource. Their health and well-being are therefore of utmost importance. Preschool children (aged 3-6 years) experience rapid developmental growth during which they gain independence in basic tasks and begin transitioning toward school readiness. This developmental stage is characterized by concrete and egocentric thinking, which limits their ability to comprehend complex events such as illness and hospitalization[1].
Hospitalization is inherently stressful for children of all ages. Preschoolers are especially vulnerable because of the immaturity of their physical, intellectual, and immune systems, which contributes to frequent hospital admissions. Such experiences disrupt their routines, separate them from familiar caregivers and environments, and expose them to unfamiliar and often frightening situations[2].
Pain is a universal and highly distressing aspect of pediatric hospitalization. In preschool children, pain perception is complex and affected by developmental stage, temperament, prior experiences, and emotional state (e.g., fear and anxiety). They often struggle to express their pain effectively. When left untreated, pain can result in immediate beha
Globally, more than 50% of hospitalized children experience significant procedural distress, with preschoolers being especially vulnerable due to limited coping mechanisms. In India, where pediatric hospitalizations exceed 12 million annually, over 70% of preschoolers exhibit severe anxiety during needle-related procedures. Several demographic and clinical variables affect the severity of pain and anxiety in this age group. Consistent with our findings, younger age, male sex, and rural residence are associated with increased procedural distress. Clinically, the use of larger cannulae, IV placement in the dorsal hand instead of the cephalic vein, and the administration of antibiotic infusions tend to intensify pain responses[4,8,9].
Younger age and developmental stage are consistently associated with higher levels of post-procedural pain and anxiety in preschoolers. This relationship is supported by Makhlouf et al[10] who identified age as a key factor affecting pediatric pain responses and caregiver pain management strategies. Cultural influences, such as language barriers and parental beliefs, further complicate this issue, leading to variability in pain expression and treatment effectiveness within this population. In a large observational study, Stevens et al[11] found that 78% of hospitalized children underwent at least one painful procedure per day; however, only 28% received documented pain management interventions.
Assessing pain in preschoolers presents distinct challenges. Although self-reporting is ideal, it requires tools tailored to the child’s cognitive abilities. The Wong-Baker FACES Pain Rating Scale (WBFPRS) is widely recommended for children aged 3-7 years[12]. In cases where self-reporting is difficult, observational methods, such as monitoring facial expressions, crying, and withdrawal, along with physiological indicators such as changes in heart rate, serve as essential components of a comprehensive pain assessment[13].
Pharmacological pain management carries limitations and risks in young children. Thus, effective nonpharmacological interventions are essential. Distraction techniques utilize the brain’s limited capacity to attend to multiple stimuli simultaneously, thereby redirecting attention away from painful procedures. These techniques may be passive (e.g., watching television) or active (e.g., interactive play). Research supports the effectiveness of specific active distractions, such as balloon blowing, art therapy, and kaleidoscope use, during procedures such as IV insertion. These methods are relatively simple, cost-effective, and capable of reducing perceived pain and anxiety without significant side effects[14,15].
Several epidemiological surveys have consistently indicated that up to 74% of hospitalized children receive inadequate pain management, despite advances in knowledge and available treatments. In India, a recent survey conducted across 20 tertiary hospitals revealed that only 15% employed evidence-based distraction tools; the majority relied on less effective methods such as verbal reassurance[16-19].
Nurses play a pivotal role in reducing the trauma of hospitalization for preschool children. They are primarily responsible for anticipating, assessing, and managing pain and anxiety. This includes fostering a supportive environment, educating children and families using age-appropriate explanations, applying validated pain assessment tools, and implementing both pharmacological and nonpharmacological interventions, such as distraction techniques. Effective nursing care is essential to minimizing the physical and psychological impacts of hospitalization and painful procedures on this vulnerable population[14]. In resource-rich settings, advanced technologies such as virtual reality (VR) are often used to reduce children’s pain and anxiety during medical procedures. However, these high-cost solutions are not scalable in low-resource environments. In developing countries such as India, pediatric care is constrained by low nurse-to-child ratios (approximately 1:40), severe time limitations, and the absence of standard protocols. These challenges highlight the urgent need for simple, affordable, nurse-led distraction methods that can be feasibly implemented in such settings[20,21].
We chose this topic because IV procedures in preschoolers are frequently associated with high levels of distress, and advanced tools such as VR are often impractical in resource-constrained environments. By introducing a simple multimodal distraction bundle, comprising balloon blowing, art engagement, and kaleidoscope use, our study aims to enhance patient comfort, reduce procedural trauma, and improve the quality of pediatric care in low-resource clinical settings.
This study used a posttest-only control group design. Participants were randomly assigned to one of two groups: (1) An experimental group that received a structured distraction-based intervention; and (2) A control group that received standard nursing care during IV medication administration. The study was conducted in the pediatric ward of Shri Vinoba Bhave Civil Hospital in Silvassa, Dadra and Nagar Haveli and Daman and Diu, India.
A total of 600 preschool children, aged 3-6 years and admitted for IV therapy, were enrolled in the study. Using a lottery method, 300 children were assigned to the experimental group and 300 to the control group. All eligible participants consented to take part, resulting in a 100% response rate with no caregiver refusals.
The sample size for the present study was calculated using a standard formula for estimating population size based on desired confidence and precision levels. Using a standardized value (Z) of 1.96 corresponding to a 95%CI, a sample standard deviation (SD) of 0.444 obtained from a pilot study, and an acceptable margin of error (E) of 0.05, the required sample size (n) was calculated as follows: n = (Z × SD/E)2 = (1.96 × 0.444/0.05)2 = 297.49.
Based on this calculation, the final sample comprised 600 preschool children, with 300 participants each assigned to the experimental and control groups.
The study included preschool children aged 3-6 years who were admitted to the pediatric ward and scheduled to undergo IV cannulation in the hand. Both male and female children were eligible for inclusion, provided they were conscious, cooperative, and had obtained informed consent from their mothers or primary caregivers. Children with chronic illnesses or those whose caregivers declined to provide consent were excluded from the study.
Children in the experimental group received three nonpharmacological interventions: (1) Balloon blowing before IV insertion; (2) Art therapy after the procedure; and (3) Kaleidoscope distraction during the procedure. The kaleidoscope used was a handheld optical instrument, approximately 15 cm in length, containing colored beads and mirrors that formed symmetrical patterns when rotated. During IV insertion, children looked through the eyepiece to observe the shifting patterns. After each procedure, the kaleidoscope was disinfected by wiping the exterior surfaces with 70% isopropyl alcohol for 30 seconds, followed by air-drying in accordance with World Health Organization infection control guidelines.
The intervention was structured into three phases and delivered once daily for three consecutive days surrounding the IV procedure. In the pre-procedure phase, which lasted 5 minutes, children participated in simple art activities such as coloring and were taught how to blow balloons. During IV insertion, they were encouraged to blow balloons while simultaneously viewing the kaleidoscope, which was held by the investigator to help divert their attention. In the post-procedure phase, which also lasted 5 minutes, children continued engaging with the kaleidoscope or resumed the art activity to support relaxation and emotional recovery.
On the third day, pain and anxiety levels were assessed in both the experimental and control groups. Following each session, infection control measures were strictly observed. Used balloons were discarded in biohazard containers, kaleidoscopes were disinfected with alcohol, and art books were given to the children to provide continued engagement and comfort. The control group received standard nursing care without any distraction-based interventions.
Data were collected between November 8, 2022, and February 18, 2023, using a concise, child-friendly process that required approximately five minutes per participant. First, caregivers completed a 12-item demographic questionnaire, which took about three minutes. Children then self-reported their pain using the WBFPRS, a single-item tool that required roughly one minute to complete. Finally, anxiety was assessed using a single-item Visual Analogue Anxiety Scale (VAAS), which also took approximately one minute.
Three structured tools were used for data collection. Section A consisted of a demographic and clinical proforma designed to gather essential background information, including the child’s age, gender, religion, place of residence (rural or urban), birth order, presence of a primary caregiver, history of chronic illness, IV cannula site and size, number of hospitalization days, and types of medications administered.
Section B employed the WBFPRS[12], a widely recognized six-point pictorial tool for assessing self-reported pain intensity in children. The scale ranges from 0 (“no hurt”) to 5 (“hurts worst”) and demonstrated strong inter-rater reliability in this study, with a coefficient of 0.82.
Section C used the VAAS to measure the child’s level of anxiety. This tool consists of a 100 mm horizontal line anchored at 0 mm for “no anxiety” and 100 mm for “worst possible anxiety”. Children indicated their anxiety level by marking a point on the line, and the distance from the zero point was measured. Anxiety levels were categorized as follows: (1) 0-20 mm (mild); (2) 21-40 mm (mild to moderate); (3) 41-60 mm (moderate); (4) 61-80 mm (moderate to high); and (5) 81-100 mm (highest). The tool demonstrated high reliability, with an inter-rater reliability coefficient of 0.84[13].
The data supporting the findings of this study are available from the corresponding author upon reasonable request. All relevant data were collected and analyzed as part of the approved clinical research project.
The data collection tools were reviewed by a panel of 10 experts, comprising six pediatric nursing faculty members, three pediatricians, and one biostatistician. A content validity index was established to ensure content validity, and inter-rater reliability was assessed during the pilot phase.
Data analysis was conducted using Statistical Package for the Social Sciences software. Descriptive statistics, including frequency, percentage, mean, and standard deviation, were used to summarize demographic characteristics and outcome measures. Independent samples t-tests were employed to compare post-test pain and anxiety scores between the experimental and control groups. To examine the relationship between pain and anxiety levels within each group, Karl Pearson’s correlation coefficient (r) was calculated. χ2 were used to explore associations between categorized levels of pain and anxiety and various demographic and clinical variables. Data normality was confirmed using the Kolmogorov-Smirnov test for both pain (D = 0.072, P = 0.200) and anxiety (D = 0.068, P = 0.211), validating the use of parametric tests. Throughout the analysis, a P value of less than 0.05 was considered statistically significant.
Ethical approval for this study was obtained from the Institutional Ethics Committee of NAMO Medical Education and Research Institute and Shri Vinoba Bhave Civil Hospital (No. DMHS/IEC/2016/214/3953). Written informed consent was obtained from each child’s caregiver after the study’s purpose, procedures, and confidentiality safeguards were clearly explained. The study was conducted in full compliance with institutional and international ethical guidelines.
Table 1 presents the demographic and clinical characteristics of the two study groups (n = 300 each). Statistical significance was assessed using Pearson’s χ2 test for independence. The analysis revealed significant differences between groups in terms of age, place of residence, IV site, and cannula size. Children aged 3 years and 4 years were more prevalent in the experimental group (45.0%) than in the control group (35.3%), and the distributions for the 4 years and 5 years age and 5 years and 6 years age brackets also differed (χ2 = 6.72, P = 0.034), indicating a variation in age distribution across groups. Place of residence also showed a significant difference: 54.7% of children in the experimental group resided in rural areas compared with 64.0% in the control group (χ2 = 4.58, P = 0.032). Sex distribution did not differ significantly between groups (χ2 = 0.81, P = 0.369).
| Variable | Category | Experimental group (n = 300) | Control group (n = 300) | χ2 | P value |
| Age (years) | 3, 4 | 135 (45.0) | 106 (35.3) | 6.72 | 0.034 |
| 4, 5 | 68 (22.7) | 90 (30.0) | |||
| 5, 6 | 97 (32.3) | 104 (34.7) | |||
| Gender | Male | 187 (62.3) | 200 (66.7) | 0.81 | 0.369 |
| Female | 113 (37.7) | 100 (33.3) | |||
| Residence | Rural | 164 (54.7) | 192 (64.0) | 4.58 | 0.032 |
| Urban | 136 (45.3) | 108 (36.0) | |||
| IV site | Cephalic vein | 5 (1.7) | 21 (7.0) | 12.45 | 0.002 |
| Metacarpal vein | 259 (86.3) | 266 (88.7) | |||
| Median vein | 36 (12.0) | 13 (4.3) | |||
| IV cannula size | 22 G | 63 (21.0) | 98 (32.7) | 7.88 | 0.005 |
| 24 G | 237 (79.0) | 202 (67.3) |
Procedural variables also differed notably. IV site placement exhibited a significant difference (χ2 = 12.45, P = 0.002), with cephalic vein cannulation occurring more frequently in the control group (7.0%) than in the experimental group (1.7%). Cannula size usage varied as well: 22 G cannulas were used more often in the control group (32.7%) than in the experimental group (21.0%) (χ2 = 7.88, P = 0.005). Distributions for metacarpal and median vein use were otherwise comparable between groups. These findings indicate that several categorical demographic and clinical characteristics were associated with group allocation. Potential confounders such as age, IV site, and cannula size were adjusted for in subsequent analyses.
Table 2 presents the distribution of post-procedure pain scores, assessed using the WBFPRS, across the experimental and control groups, each consisting of 300 preschool children. The experimental group, which received the multimodal distraction intervention, exhibited significantly lower pain levels. More than half of the children (50.33%) reported a pain score of “hurts little more” (score 2), while 38.00% reported “hurts little bit” (score 1), and 6.67% reported “no hurt” (score 0). Only a small proportion (5.00%) experienced moderate pain (“hurts even more”; score 3). Importantly, none of the children in this group reported high-intensity pain (scores 4 or 5). In contrast, every child in the control group, which received only standard care, reported severe levels of pain. Specifically, 55.66% rated their pain as “hurts whole lot” (score 4), and 44.33% reported “hurts worst” (score 5). No child in the control group reported scores below 4, indicating a complete absence of mild or moderate pain experiences in the absence of distraction-based interventions. There was a statistically significant difference in pain score distribution between the two groups (P < 0.001).
| Pain level (Wong-Baker FACES Pain Rating Scale) | Experimental group (n = 300) | Control group (n = 300) | P value |
| No hurt (0) | 20 (6.67) | 0 (0.00) | < 0.001 |
| Hurts little bit (1) | 114 (38.00) | 0 (0.00) | |
| Hurts little more (2) | 151 (50.33) | 0 (0.00) | |
| Hurts even more (3) | 15 (5.00) | 0 (0.00) | |
| Hurts whole lot (4) | 0 (0.00) | 167 (55.66) | |
| Hurts worst (5) | 0 (0.00) | 133 (44.33) |
Table 3 summarizes the results of a binary logistic regression analysis conducted to identify demographic and clinical variables significantly associated with the likelihood of experiencing severe pain during IV cannulation. For this analysis, the outcome variable was dichotomized as “severe pain” (WBFPRS score ≥ 4) and “non-severe pain” (score < 4).
| Variable | Category | B | SE | Odds ratio (95%CI) | P value |
| Group | Control vs experimental | 5.98 | 0.58 | 396.4 (125.9-1247.7) | < 0.001 |
| Age (years) | 3, 4 (refence: 5, 6) | 0.64 | 0.28 | 1.89 (1.10-3.25) | 0.021 |
| Gender | Male vs female | 0.29 | 0.26 | 1.34 (0.80-2.23) | 0.263 |
| Residence | Rural vs urban | 0.41 | 0.25 | 1.51 (0.93-2.45) | 0.098 |
| Intravenous site | Cephalic vs metacarpal | 1.88 | 0.58 | 6.54 (2.08-20.54) | 0.001 |
| Median vs metacarpal) | 0.72 | 0.35 | 2.06 (1.05-4.06) | 0.036 | |
| Cannula size | 22 G vs 24 G | 0.86 | 0.26 | 2.36 (1.39-4.02) | 0.002 |
The most influential predictor was group assignment. Children in the control group had nearly 396 times greater odds of reporting severe pain compared with those in the experimental group who received the multimodal distraction intervention [odds ratio (OR) = 396.4; 95%CI: 125.9-1247.7; P < 0.001]. These results indicate a strong protective effect of the intervention against severe pain.
Age also emerged as a significant factor. Children aged 3 years and 4 years had nearly twice the odds of experiencing severe pain (OR = 1.89; P = 0.021) compared with those aged 5 years and 6 years, indicating that younger children are more susceptible to procedural pain. IV site placement showed a strong association with pain severity. Cannulation in the cephalic vein significantly increased the odds of severe pain (OR = 6.54; P = 0.001) compared with the metacarpal vein. Similarly, use of the median vein was associated with elevated risk (OR = 2.06; P = 0.036). Cannula size also played a notable role. Use of a 22 G cannula was associated with more than twice the risk of severe pain (OR = 2.36; P = 0.002) compared with a 24 G cannula. While male gender and rural residence were associated with higher odds of severe pain, these associations did not reach statistical significance. These findings underscore the importance of targeted clinical strategies, such as appropriate vein selection and equipment sizing, and further support the effectiveness of distraction-based interventions in reducing procedural pain in young children.
Table 4 presents the comparison of post-test pain scores between the experimental and control groups, assessed using an independent t-test. The mean pain score in the experimental group was 3.07 (SD = 1.390), while the control group recorded a significantly higher mean score of 8.80 (SD = 1.007). The calculated mean difference between the two groups was 5.73. This difference was statistically significant, as reflected by a high t-value of 58.56 and a P value of less than 0.001. These results indicate a substantial reduction in post-test pain levels among children who received the multimodal distraction intervention compared with those who received routine care (Figure 1A).
| Group | Mean (Wong-Baker FACES Pain Rating Scale) | SD | Mean difference | t value | P value |
| Experimental (n = 300) | 3.07 | 1.390 | 5.73 | 58.56 | < 0.001 |
| Control (n = 300) | 8.80 | 1.007 |
Table 5 presents the findings of a binary logistic regression analysis conducted to identify significant predictors of high procedural anxiety, defined as a VAAS score of 7 or higher, among preschool children undergoing IV cannulation. The most prominent predictor of high anxiety was intervention group status. Children in the control group, who did not receive the distraction intervention, were 129 times more likely to exhibit high anxiety compared with those in the experimental group who received the multimodal distraction intervention (OR = 129.2; 95%CI: 44.7-373.6; P < 0.001). Age also emerged as a significant factor. Children aged 3 years and 4 years had more than twice the odds of experiencing high anxiety compared with those aged 5 years and 6 years (OR = 2.06; P = 0.017), suggesting that younger children are more vulnerable to procedural stress.
| Variable | Category | B | SE | Odds ratio (95%CI) | P value |
| Group | Control vs experimental) | 4.86 | 0.55 | 129.2 (44.7-373.6) | < 0.001 |
| Age (years) | 3, 4 (refence: 5, 6) | 0.72 | 0.30 | 2.06 (1.14-3.72) | 0.017 |
| Gender | Male vs female | 0.33 | 0.27 | 1.39 (0.81-2.39) | 0.232 |
| Residence | Rural vs urban | 0.48 | 0.26 | 1.62 (0.97-2.71) | 0.066 |
| Intravenous site | Cephalic vs metacarpal | 1.55 | 0.53 | 4.72 (1.66-13.42) | 0.004 |
| Median vs metacarpal | 0.61 | 0.32 | 1.84 (0.98-3.43) | 0.057 | |
| Cannula size | 22 G vs 24 G | 0.91 | 0.27 | 2.48 (1.46-4.21) | 0.001 |
Among clinical variables, the IV cannula site was a significant predictor. Children who received cannulation in the cephalic vein had nearly five times higher odds of high anxiety (OR = 4.72; P = 0.004) compared with those with metacarpal vein access. The use of the median vein also showed a trend toward increased risk (OR = 1.84; P = 0.057), although this finding did not reach statistical significance.
Cannula size was another important factor. Children cannulated with a 22 G needle were 2.48 times more likely to experience high anxiety compared with those with a 24 G needle (P = 0.001), possibly due to increased discomfort or invasiveness. Male gender and rural residence showed non-significant trends toward higher anxiety levels but did not reach statistical significance (P = 0.232 and P = 0.066, respectively). In summary, the absence of distraction, younger age, cephalic IV access, and use of larger cannula sizes were significant predictors of increased procedural anxiety in preschool children. These findings highlight the importance of developmentally appropriate, minimally invasive, and emotionally supportive strategies in pediatric clinical care.
Table 6 presents the comparison of post-test anxiety scores between the experimental and control groups, using an independent t-test. Anxiety was measured in millimeters using the VAAS. The experimental group recorded a mean anxiety score of 5.85 (SD = 1.560), while the control group had a significantly higher mean score of 9.39 (SD = 0.730). The mean difference between the groups was 3.54. The t-test yielded a value of 35.55, with a P value of less than 0.001. This statistically significant result indicates that children in the experimental group experienced lower anxiety levels following the intervention compared with those in the control group (Figure 1B).
| Group | Mean (Visual Analogue Anxiety Scale) | SD | Mean difference | t value | P value |
| Experimental (n = 300) | 5.85 | 1.560 | 3.54 | 35.55 | < 0.00001 |
| Control (n = 300) | 9.39 | 0.730 |
Table 7 shows the correlation between pain and anxiety scores within the experimental and control groups. In the experimental group, the mean pain score was 3.07 (SD = 1.39), and the mean anxiety score was 5.85 (SD = 1.56). A moderate positive correlation was observed between pain and anxiety scores, with a correlation coefficient of r = 0.67, which was statistically significant (P < 0.05). Similarly, in the control group, the mean pain score was higher at 8.80 (SD = 1.01), and the mean anxiety score was 9.39 (SD = 0.73). A comparable positive correlation was also observed in this group (r = 0.66, P < 0.05). These findings suggest a consistent and significant relationship between higher levels of pain and increased anxiety across both groups.
| Group | Pain, mean (SD) | Anxiety, mean (SD) | r value | P value |
| Experimental (n = 300) | 3.07 (1.39) | 5.85 (1.56) | 0.67 | < 0.05 |
| Control (n = 300) | 8.80 (1.01) | 9.39 (0.73) | 0.66 | < 0.05 |
This study demonstrates that a multimodal distraction approach, consisting of balloon blowing, art activities, and kaleidoscope viewing, significantly reduces pain and anxiety in hospitalized preschool children undergoing IV cannulation in resource-limited settings.
The neurocognitive basis for this effectiveness likely involves multisensory modulation of the hippocampus, a region that plays a central role in processing both pain and anxiety. Pate et al[22] found that distraction tools engaging multiple senses are more effective at reducing stress-related hippocampal activation than unimodal techniques. The moderate correlation observed in our study between pain and anxiety (r = 0.67) further supports the interdependent nature of these experiences and underscores the value of combining cognitive and emotional distraction methods. The success of the intervention can also be attributed to its developmental appropriateness for preschoolers, who are primarily kinesthetic and visual learners. Activities such as balloon blowing and coloring engage tactile and motor skills, while kaleidoscope viewing offers gentle visual stimulation. This contrasts with VR tools, which, although effective in older children, can overstimulate younger children, as noted by Gold and Mahrer[23].
The present study demonstrated a significant reduction in pain levels among preschool children undergoing IV therapy when a multimodal distraction bundle, comprising balloon blowing, art activities, and kaleidoscope viewing, was implemented. Most children in the experimental group reported mild to moderate pain, with a mean pain score of 3.07 ± 1.39, compared with 8.80 ± 1.01 in the control group. These findings are consistent with those of Koç Özkan and Polat[14] who observed similar reductions using kaleidoscope distraction during venipuncture. They also align with studies by Birnie et al[6]and Uman et al[24] which established distraction as a reliable non-pharmacological strategy for pediatric pain management. Although VR has also shown strong efficacy, as noted by Gold and Mahrer[23] and Özalp Gerçeker et al[25], it requires financial investment, technical infrastructure, and staff training, factors that limit its feasibility in low-resource settings. In contrast, the strength of the present study lies in its accessibility and developmental appropriateness. By offering children a choice of simple activities, the intervention promoted a sense of agency and engagement. This study also revealed a marked reduction in procedural anxiety among children in the experimental group, as reflected by significantly lower mean VAAS scores (5.85 ± 1.56) compared with those in the control group (9.39 ± 0.73). A moderate positive correlation (r = 0.67) was observed between pain and anxiety, emphasizing their interconnected nature in pediatric patients. These results are supported by prior work from Won et al[26] who reported reduced anxiety in children using avatar-assisted VR interventions. However, unlike screen-based tools, the simple tactile and visual methods used in this study were better suited to the developmental and attentional capacities of preschool-aged children.
In another study, Gold et al[27] conducted a randomized controlled trial involving 20 pediatric patients undergoing IV placement. The VR group received a multisensory VR experience that included visual stimulation through a head-mounted display, tactile feedback, and music. This intervention was delivered for five minutes before and continued for five minutes after the IV procedure. The control group received only a local anesthetic spray and did not receive any VR intervention during the procedure, although they were allowed to use the VR equipment for three minutes after IV placement. Children in the control group experienced a four-fold increase in reported pain compared with those in the VR group.
Studies by Razmi et al[28] using cartoon-based distractions reported only modest reductions in anxiety, highlighting the greater effectiveness of active, child-led distraction strategies. A key strength of the present intervention is its alignment with cognitive-emotional engagement theory, which emphasizes the role of self-regulation in anxiety and pain management. However, one noted limitation was the limited involvement of parents during the procedures. Prior research by Ginsburg[29] has shown that active caregiver participation can significantly reduce anxiety in pediatric patients. Future interventions may benefit from incorporating structured roles for parental involvement during procedures.
The multimodal design of this study, which offered a choice among three low-cost, developmentally appropriate distraction activities, effectively addressed the diverse psychological and sensory needs of preschool children. Unlike VR tools, which may overstimulate younger children or require frequent adjustment, as noted by Gold and Mahrer[23], the interventions used in this study provided familiar, non-threatening experiences. Verhoeven et al[30] reported that children with high levels of pain catastrophizing respond more positively to emotionally engaging distractions than to purely sensory ones, further supporting the value of incorporating multiple modes of engagement. Pate et al[22] also emphasized that kinesthetic and multisensory activities are especially beneficial for preschool-aged children due to their enhanced ability to modulate stress cognitively. A notable strength of this intervention is its adaptability and cultural neutrality; materials such as balloons and kaleidoscopes transcend language and cultural boundaries. However, the absence of a formal assessment of temperament or individual coping styles limits the intervention’s potential for personalization. In addition, randomizing activity choices could have helped control for confounding variables related to individual preferences.
The implementation of this study in a tertiary care hospital without external funding underscores its relevance for resource-limited settings. All materials were provided by the investigators, and nurses received brief, structured training. This model demonstrates the feasibility of scaling simple, low-cost interventions in low-income and middle-income countries (LMICs), where nurse-to-patient ratios may reach as high as 1:40, as reported by Abebe et al[31]. While Ballard et al[32] have shown that hospital-supported distraction kits enhance sustainability and integration into routine care, the present study lacked institutional backing or policy integration, which limited the potential for long-term im
Globally, high-income countries have successfully integrated digital tools such as VR with custom avatars, achieving notable outcomes. For instance, Tas et al[33] reported anxiety rates as low as 27.3% using these technologies. However, such systems demand substantial financial and technical infrastructure, which is often unavailable in LMICs. In these settings, public health systems continue to struggle with high nurse-to-patient ratios, limited time resources, and the absence of formal pain management protocols.
This study demonstrates the effectiveness of a low-cost, multimodal distraction intervention in reducing pain and anxiety among preschool children undergoing IV therapy. Its strengths include a large sample size, statistically significant findings, and use of validated tools (WBFPRS and VAAS). The intervention is practical, child-friendly, and easily scalable in low-resource settings. Nurse-led implementation promotes workforce empowerment without requiring expensive technology. Ethical standards were upheld, and the approach offers strong potential for integration into routine pediatric care and policy frameworks.
This study was limited to a single tertiary care center, which may affect the generalizability of the findings. The use of subjective scales like WBFPRS and VAAS relies on children's ability to self-report, which may vary with age and understanding. Additionally, the long-term effects of the intervention were not assessed.
In summary, the present study aligns with international research on pediatric procedural pain and anxiety management while providing context-specific insights relevant to LMICs. The findings confirm that distraction techniques are both effective and feasible when tailored to the developmental stage of the child and the constraints of resource-limited healthcare environments. Key strengths of this study include its multisensory design, simplicity, and potential for scalability. However, future efforts could be enhanced by integrating structured caregiver involvement, assessing individual temperament, and securing institutional support to promote sustainable implementation.
| 1. | Bornstein MH, Britto PR, Nonoyama-Tarumi Y, Ota Y, Petrovic O, Putnick DL. Child development in developing countries: introduction and methods. Child Dev. 2012;83:16-31. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 62] [Article Influence: 4.4] [Reference Citation Analysis (1)] |
| 2. | Claridge AM, J Powell O. Children's experiences of stress and coping during hospitalization: A mixed-methods examination. J Child Health Care. 2023;27:531-546. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 25] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 3. | Debnath S, Das N, Sahoo P. Effectiveness of Distraction Therapy on Pain Relief among Children Undergoing Vein-Puncture in a Selected Hospital, Bhubaneswar. J Adv Res Med. 2020;7:15-21. [DOI] [Full Text] |
| 4. | Friedrichsdorf SJ, Goubert L. Pediatric pain treatment and prevention for hospitalized children. Pain Rep. 2020;5:e804. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 38] [Cited by in RCA: 111] [Article Influence: 15.9] [Reference Citation Analysis (0)] |
| 5. | Bakir E. Assessing Undergraduate Nursing Pediatric Pain Education in Turkey: A Content Analysis Study. Pain Manag Nurs. 2025;26:e405-e410. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 6. | Birnie KA, Noel M, Chambers CT, Uman LS, Parker JA. Psychological interventions for needle-related procedural pain and distress in children and adolescents. Cochrane Database Syst Rev. 2018;10:CD005179. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 132] [Article Influence: 16.5] [Reference Citation Analysis (0)] |
| 7. | Orenius T, LicPsych, Säilä H, Mikola K, Ristolainen L. Fear of Injections and Needle Phobia Among Children and Adolescents: An Overview of Psychological, Behavioral, and Contextual Factors. SAGE Open Nurs. 2018;4:2377960818759442. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 51] [Cited by in RCA: 80] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 8. | Lerwick JL. Minimizing pediatric healthcare-induced anxiety and trauma. World J Clin Pediatr. 2016;5:143-150. [PubMed] [DOI] [Full Text] |
| 9. | Singh M, Bharti B, Bharti S, Gupta S. Needle Fear among Children during Mass Measles Rubella (MR) Injectable Vaccination Campaign in North India: an Observational Study. J Child Adolesc Trauma. 2022;15:47-52. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 10. | Makhlouf MM, Garibay ER, Jenkins BN, Kain ZN, Fortier MA. Postoperative pain: factors and tools to improve pain management in children. Pain Manag. 2019;9:389-397. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 19] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 11. | Stevens BJ, Abbott LK, Yamada J, Harrison D, Stinson J, Taddio A, Barwick M, Latimer M, Scott SD, Rashotte J, Campbell F, Finley GA; CIHR Team in Children's Pain. Epidemiology and management of painful procedures in children in Canadian hospitals. CMAJ. 2011;183:E403-E410. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 171] [Cited by in RCA: 221] [Article Influence: 14.7] [Reference Citation Analysis (0)] |
| 12. | Garra G, Singer AJ, Taira BR, Chohan J, Cardoz H, Chisena E, Thode HC Jr. Validation of the Wong-Baker FACES Pain Rating Scale in pediatric emergency department patients. Acad Emerg Med. 2010;17:50-54. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 282] [Cited by in RCA: 417] [Article Influence: 26.1] [Reference Citation Analysis (0)] |
| 13. | Davey HM, Barratt AL, Butow PN, Deeks JJ. A one-item question with a Likert or Visual Analog Scale adequately measured current anxiety. J Clin Epidemiol. 2007;60:356-360. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 214] [Cited by in RCA: 230] [Article Influence: 12.1] [Reference Citation Analysis (1)] |
| 14. | Koç Özkan T, Polat F. The Effect of Virtual Reality and Kaleidoscope on Pain and Anxiety Levels During Venipuncture in Children. J Perianesth Nurs. 2020;35:206-211. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 61] [Article Influence: 10.2] [Reference Citation Analysis (0)] |
| 15. | Semerci R, Akgün Kostak M. The Efficacy of Distraction Cards and Kaleidoscope for Reducing Pain During Phlebotomy: A Randomized Controlled Trial. J Perianesth Nurs. 2020;35:397-402. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 10] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 16. | Andersson V, Bergman S, Henoch I, Simonsson H, Ahlberg K. Pain and pain management in children and adolescents receiving hospital care: a cross-sectional study from Sweden. BMC Pediatr. 2022;22:252. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 41] [Reference Citation Analysis (0)] |
| 17. | Johnston CC, Abbott FV, Gray-Donald K, Jeans ME. A survey of pain in hospitalized patients aged 4-14 years. Clin J Pain. 1992;8:154-163. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 57] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 18. | Taylor EM, Boyer K, Campbell FA. Pain in hospitalized children: a prospective cross-sectional survey of pain prevalence, intensity, assessment and management in a Canadian pediatric teaching hospital. Pain Res Manag. 2008;13:25-32. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 159] [Cited by in RCA: 179] [Article Influence: 9.9] [Reference Citation Analysis (0)] |
| 19. | Bhadani U. Oral Presentation. Indian J Palliat Care. 2021;27:453-470. [RCA] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 20. | Eijlers R, Utens EMWJ, Staals LM, de Nijs PFA, Berghmans JM, Wijnen RMH, Hillegers MHJ, Dierckx B, Legerstee JS. Systematic Review and Meta-analysis of Virtual Reality in Pediatrics: Effects on Pain and Anxiety. Anesth Analg. 2019;129:1344-1353. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 517] [Cited by in RCA: 377] [Article Influence: 53.9] [Reference Citation Analysis (0)] |
| 21. | Sharma SK, Rani R. Nurse-to-patient ratio and nurse staffing norms for hospitals in India: A critical analysis of national benchmarks. J Family Med Prim Care. 2020;9:2631-2637. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 48] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 22. | Pate JT, Blount RL, Cohen LL, Smith AJ. Childhood Medical Experience and Temperament as Predictors of Adult Functioning in Medical Situations. Child Health Care. 1996;25:281-298. [DOI] [Full Text] |
| 23. | Gold JI, Mahrer NE. Is Virtual Reality Ready for Prime Time in the Medical Space? A Randomized Control Trial of Pediatric Virtual Reality for Acute Procedural Pain Management. J Pediatr Psychol. 2018;43:266-275. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 143] [Cited by in RCA: 183] [Article Influence: 26.1] [Reference Citation Analysis (0)] |
| 24. | Uman LS, Birnie KA, Noel M, Parker JA, Chambers CT, McGrath PJ, Kisely SR. Psychological interventions for needle-related procedural pain and distress in children and adolescents. Cochrane Database Syst Rev. 2013;CD005179. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 84] [Cited by in RCA: 123] [Article Influence: 9.5] [Reference Citation Analysis (0)] |
| 25. | Özalp Gerçeker G, Ayar D, Özdemir EZ, Bektaş M. Effects of virtual reality on pain, fear and anxiety during blood draw in children aged 5-12 years old: A randomised controlled study. J Clin Nurs. 2020;29:1151-1161. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 113] [Article Influence: 18.8] [Reference Citation Analysis (0)] |
| 26. | Won AS, Bailey J, Bailenson J, Tataru C, Yoon IA, Golianu B. Immersive Virtual Reality for Pediatric Pain. Children (Basel). 2017;4:52. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 157] [Cited by in RCA: 134] [Article Influence: 14.9] [Reference Citation Analysis (0)] |
| 27. | Gold JI, Kim SH, Kant AJ, Joseph MH, Rizzo AS. Effectiveness of virtual reality for pediatric pain distraction during i.v. placement. Cyberpsychol Behav. 2006;9:207-212. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 230] [Cited by in RCA: 229] [Article Influence: 11.5] [Reference Citation Analysis (0)] |
| 28. | Razmi S, Karajizadeh M, Zarei Fard S, Pourahmad S, Fazeli P, Bordbar N. The Effect of Distraction on Pain Management in Children Aged 5 to 12 Years Old With Acute Leukemia Undergoing Bone Marrow Aspiration. Health Sci Rep. 2025;8:e70634. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 29. | Ginsburg GS. The Child Anxiety Prevention Study: intervention model and primary outcomes. J Consult Clin Psychol. 2009;77:580-587. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 95] [Cited by in RCA: 86] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 30. | Verhoeven K, Goubert L, Jaaniste T, Van Ryckeghem DM, Crombez G. Pain catastrophizing influences the use and the effectiveness of distraction in schoolchildren. Eur J Pain. 2012;16:256-267. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 36] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 31. | Abebe MT, Tegegne KT, Shiferaw DA, Gonete YA, Kebede YA, Fetene JC, Tibebu AT, Agimas MC. Knowledge and practice of pediatric pain management and associated factors among nurses in Ethiopia: a systematic review and meta-analysis. BMC Nurs. 2024;23:848. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 32. | Ballard A, Le May S, Khadra C, Lachance Fiola J, Charette S, Charest MC, Gagnon H, Bailey B, Villeneuve E, Tsimicalis A. Distraction Kits for Pain Management of Children Undergoing Painful Procedures in the Emergency Department: A Pilot Study. Pain Manag Nurs. 2017;18:418-426. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 23] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 33. | Tas FQ, van Eijk CAM, Staals LM, Legerstee JS, Dierckx B. Virtual reality in pediatrics, effects on pain and anxiety: A systematic review and meta-analysis update. Paediatr Anaesth. 2022;32:1292-1304. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 92] [Article Influence: 23.0] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/