Published online Apr 18, 2026. doi: 10.5312/wjo.v17.i4.116521
Revised: January 4, 2026
Accepted: February 24, 2026
Published online: April 18, 2026
Processing time: 146 Days and 12.1 Hours
Motor imagery (MI) is a cognitive intervention that enhances post-operative recovery, particularly following anterior cruciate ligament reconstruction (ACLR).
To determine the effectiveness of MI-based psychological interventions on post
This systematic review evaluated the impact of MI on critical outcomes, including pain, knee function, kinesiophobia, and return-to-sport readiness in ACLR pati
Twelve studies including 526 individuals (266 in intervention groups, 118 in placebo groups, and 142 in control groups) were included in the qualitative synthesis. MI was most commonly administered three times per week following ACLR, with intervention durations ranging from 6 days to 24 weeks; a 24-week period was the most frequently reported. Several studies reported improvements in kinesiophobia and psychological readiness to return to sport in patients receiving imagery-based interventions compared with placebo or usual care; however, these effects were not consistent across all trials and should be interpreted with caution.
Given the psychological burden associated with ACLR, MI represents a promising adjunct to standard rehabilitation that warrants more rigorous evaluation.
Core Tip: This article examined the impact of motor imagery (MI), a cognitive strategy involving the mental rehearsal of movement, on recovery following anterior cruciate ligament reconstruction. Across 12 randomized controlled trials (526 patients), MI was associated with reductions in postoperative pain and kinesiophobia (fear of reinjury) and with improved psychological readiness to return to sport in several studies, although findings were not consistently statistically significant. Integrating MI into conventional rehabilitation may offer additional psychological benefits and, in some cases, functional improvements after anterior cruciate ligament reconstruction. Larger, high-quality trials with standardized MI protocols are needed to clarify its clinical efficacy and optimal application in postoperative care.
- Citation: Salimi M, Mafhoumi A, Mosalamiaghili S, Arvin A, Keshtkar A, Lowe W, Akbari H. Effectiveness of motor imagery in postoperative outcomes after anterior cruciate ligament reconstruction. World J Orthop 2026; 17(4): 116521
- URL: https://www.wjgnet.com/2218-5836/full/v17/i4/116521.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i4.116521
Rehabilitation following anterior cruciate ligament reconstruction (ACLR) is often prolonged and challenging for many patients. Although surgical intervention is effective in restoring knee stability, a substantial proportion of individuals fail to return to their preinjury level of function and report persistent psychological barriers, including lack of confidence in the reconstructed knee. Common postoperative challenges include pain, stiffness, and kinesiophobia (fear of reinjury), all of which may hinder participation in sport and activities of daily living[1,2].
Conventional postoperative rehabilitation protocols following ACLR primarily emphasize physical recovery, such as strength, range of motion (ROM), and neuromuscular control, with comparatively less attention to psychological and cognitive components of recovery. In recent years, motor imagery (MI) has been proposed as a cognitive intervention that may enhance rehabilitation outcomes. MI involves mentally rehearsing specific motor tasks without overt physical movement, activating neural networks associated with actual movement execution and potentially facilitating motor control and functional recovery while minimizing mechanical stress on healing tissues[3,4].
While MI has demonstrated beneficial effects in other areas of musculoskeletal rehabilitation, its application following ACLR remains inconsistently studied. Individual trials have reported variable effects on pain, psychological outcomes, and functional recovery, often limited by small sample sizes, heterogeneous intervention protocols, and inconsistent outcome measures. Moreover, previous systematic reviews addressing MI after ACLR were restricted by a limited number of included studies and did not incorporate more recent randomized trials or comprehensively synthesize emerging psychological outcomes such as kinesiophobia and readiness to return to sport (RTS)[3-5].
Accordingly, an updated systematic review was conducted to synthesize the current evidence on the effectiveness of MI following ACLR, with a specific focus on combining cognitive strategies, like MI, with traditional physical rehabilitation protocols holds the potential to enhance the patient’s psychological readiness, decrease the risk of subsequent injury, and improve RTS rates. By integrating newer studies and systematically addressing methodological heterogeneity, this review aims to clarify the existing evidence base and identify key gaps to inform both clinical practice and future research[6-9].
This systematic review (registered in the PROSPERO database, registration No. CRD420251272773) were conducted and reported in accordance with the PRISMA 2020 statement. A completed PRISMA checklist is provided as Supplementary Table 1[10].
A systematic literature search was conducted in PubMed, EMBASE, and Web of Science from database inception to 20 July 2024. The search strategy was developed using a combination of controlled vocabulary terms [Medical Subject Headings (MeSH) in PubMed] and free-text keywords related to three core concepts: Anterior cruciate ligament pathology, surgical or rehabilitative management, and psychological or MI-based interventions.
For the population component, the following MeSH terms and keywords were used: “Anterior Cruciate Ligament” (MeSH) and free-text terms including anterior cruciate ligament (ACL) and anterior cruciate ligament. For the rehabilitation and surgical context, keywords included rehabilita, reconstruct, surgery, and treatment. For the intervention component, psychological and imagery-related terms were applied, including psychologic intervention, imagery, imagined movement, mirror therapy, movement representative technique, video, relaxation, coping, modeling, self talk, goal setting, and counseling (Supplementary Table 1).
Within each concept, terms were combined using the Boolean operator “OR”, and the three concept blocks were combined using “AND”. Searches were limited to title and abstract fields where applicable. Database-specific syntax was adapted for each platform (e.g., MeSH terms in PubMed and Emtree-aligned free-text terms in EMBASE). The full electronic search strategies for all databases are provided in Supplementary Table 1. Reference lists of all included studies were manually screened to identify additional eligible articles.
All titles and abstracts to identify potentially relevant articles were reviewed. Two researchers (Seyedarad Mosa
The methodological quality of all included studies was independently assessed by two reviewers (Arvin A and Mosalamiaghili S). Any disagreements were resolved through discussion, with arbitration by a third reviewer (Salimi M) when necessary. The risk of bias in randomized controlled trials was evaluated using the Cochrane Risk of Bias 2 tool[11].
A narrative synthesis was undertaken because of substantial heterogeneity in intervention types, delivery methods, outcome measures, and follow-up time points across studies. Findings were synthesized descriptively and grouped according to outcome domains (pain, kinesiophobia, psychological readiness, SE, functional outcomes, and knee strength/Laxity). Where outcomes were reported using multiple instruments, the measure most frequently reported across studies was prioritized for comparison. Risk-of-bias assessments were incorporated into the interpretation of results, and differences in outcomes were considered in light of study quality and methodological characteristics. Due to the small number of studies reporting comparable outcomes, a quantitative meta-analysis and formal assessment of publication bias were not performed.
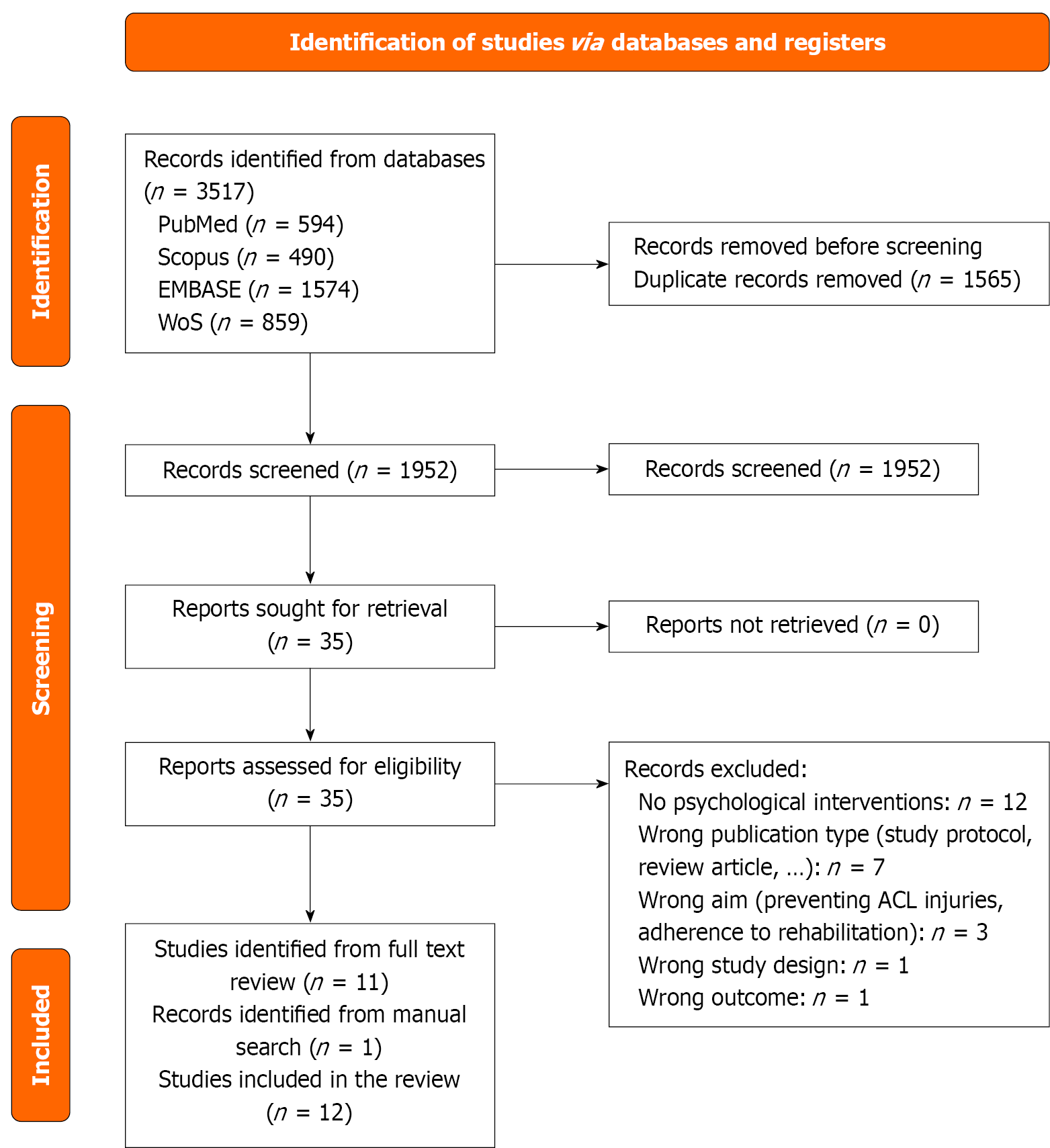
The electronic database search yielded 3517 records, including 594 from PubMed, 490 from Scopus, 1574 from EMBASE, and 859 from Web of Science. After removal of duplicates, 1952 records remained and underwent title and abstract screening, of which 1917 studies were excluded. Thirty-five articles were assessed for full-text eligibility, and 11 studies met the inclusion criteria. One additional study was identified through manual reference searching[4]. Ultimately, 12 studies[3,4,6-9,12-17] were included in the final qualitative synthesis (systematic review). The study selection process is illustrated in the PRISMA flow diagram (Figure 1).
The articles included were published between 2001 and 2023; all were randomized controlled trials. The sample sizes ranged from 12 to 101. Twelve studies comprised 526 individuals, including 266 participants undergoing the imagery interventions, 118 patients receiving the placebo, and 142 individuals in the control group (Table 1). All of the studies included in the analysis enrolled patients who had undergone isolated ACLR surgery[3,4,6-9,13-17], except for the study conducted by Almuhaya et al[12], which included patients undergoing either isolated ACLR or ACLR combined with meniscal repair. The gender distribution of participants was documented in eight studies[3,6-9,12,16,17]. Notably, in the study conducted by Almuhaya et al[12], the entire patient cohort consisted of males. The mean age of the patients ranged from 26 to 35.01. The participant demographics of the included studies are summarized in Table 1.
| Ref. | Study design | Trait of participants | Number of participants | Intervention | Type of imagery | Pre-op session | Duration | Frequency | Age (year) | Sex (male/total) | Mean follow-up |
| Almuhaya et al[12], 2023 | RCT | Cases: 13 ACLR only, 4 ACLR + MMR, 1 ACLR + both (MMR and LMR) | Cases: 16 | Cases: Structured education + standard physiotherapy | Virtual interactive structured educational session via Zoom platform including a series of topics related to the surgery and the rehabilitation process prepared with pictures and graphs | No | 1 week | 8 five days in a week, 2 four days, 8 three or less days | 26 (6) | 35/35 | 1 week |
| Controls: 12 ACLR only, 2 ACLR + MMR, 1 ACLR + LMR, 2 ACLR + both | Controls: 14 | Controls: Standard physiotherapy | |||||||||
| Lee et al[14], 2023 | RCT | ACL reconstruction | Cases: 55 | Cases: Smartphone app-based behavioral intervention + standard physiotherapy | A smartphone app delivering the intervention through text, pictorials, and videos on how post-surgery home-based exercises and rehabilitations will be done, behavior change techniques | No | 16 weeks | NR | 27.82 (8.73) | NR | 16 weeks |
| Controls: 41 | Controls: Standard physiotherapy | ||||||||||
| Brewer et al[6], 2022 | RCT | ACL reconstruction | Cases: 34 | Cases: Interactive cognitive-behavioral multimedia program + standard physiotherapy | Introductory information and instructions on: (1) General information; (2) Surgery; and (3) Rehabilitation. Videos in which an orthopedic surgeon discussed the sensory and procedural aspects associated with the corresponding section of the program. Anatomical and surgical animations, video and still images of preoperative and postoperative rehabilitation exercises, video clips of former ACL reconstruction patients describing their experiences with ACL surgery and rehabilitation, a graph of pain over the rehabilitation process, and written text were among the means by which procedural and sensory information and modeling of adaptive coping responses. Links to online resources, personal accounts of and recommendations for dealing with ACL surgery and rehabilitation from former patients | Yes | 24 weeks | Weekly | 35.01 (11.98) | 39/69 | 24 weeks |
| Placebos: 35 | Placebo: Printed educational materials + standard physiotherapy | ||||||||||
| D’Isanto et al[13], 2022 | RCT | ACL reconstruction | Cases: 15 | Cases: VRGI and MT + standard physiotherapy | Suggestions for imagining internal images related to the use of the affected limb in one or more functional tasks and also through the mirror box, working with the vision of a video in which, through a background voice, the subject was asked to visualize specific sports movements and gestures | No | 20 weeks | 3 times per week (training frequency was 5/week with a session length of 60 minutes, with MT added 3 times/week for 20-25 minutes after the end of the conventional physical therapy) | Cases: 33 (1.8) | NR | 20 weeks |
| Controls: 15 | Controls: Physiotherapy | Controls: 32 (1.6) | |||||||||
| Lyles et al[17], 2014 | RCT | ACL reconstruction | Cases: 15 | Cases: Mirror therapy + standard physiotherapy | Affected leg was placed behind a self-made mirror (non-reflecting side) and non-affected leg was placed in front of the mirror (reflecting side). Patients were instructed to observe the reflected leg into the mirror while performing the exercises and then attempt the same exercises with the involved leg | No | 6 days | Once a day | Cases: 33.13 (6.99) | Cases: 10/15 | 6 days |
| Controls: 15 | Controls: Standard physiotherapy | Controls: 32.4 (5.66) | Controls: 9/15 | ||||||||
| Rhim et al[8], 2020 | RCT | ACL reconstruction | Cases: 10 | Cases: Modeling intervention + standard physiotherapy | Cases: Six modeling videos of semi-structured interviews and models who discussed their injury experience, expectations, and recovery and performed postoperative time-matched | Yes | 24 weeks | NR | Cases: 27.1 (9.5), placebos: 32.2 (12.2), controls: 26.8 (7.9) | Cases: 9/10, placebos: 8/11, controls: 10/11 | 24 weeks |
| Placebos: 11 | Placebos: Placebo videos + standard physiotherapy | Tasks and rehabilitation exercises. Six videos were similar in length (5 minutes) | |||||||||
| Controls: 11 | Controls: Standard physiotherapy | Reflected 6 different time points: Preoperative period, from hospitalization to 2 weeks, 2 weeks to 6 weeks, 6 weeks to 3 months, 3 months to 6 months, and 6 months and beyond following ACLR; placebos: Videos of PowerPoint slides including epidemiology of ACL injuries, anatomy of ACL, and mechanisms of ACL injury, and describing rehabilitation exercises with words | |||||||||
| Levinger et al[7], 2017 | RCT | ACL reconstruction | Cases: 10 | Cases: Internet-based resource + usual rehabilitation | Video and images on ACL reconstruction, expected milestones during the recovery process, strategies to overcome distress associated with the injury, and recommended physiotherapy exercises | No | 12 weeks | On a daily basis for the first week following the surgery | Cases: 32.2 (10.2) | Cases: 6/10, placebos: 4/7 | 12 weeks |
| Placebos: 7 | Placebos: Restricted access to internet-based resource + usual rehabilitation | Three times per week for weeks 2-3 following the surgery | Placebos: 28.5 (9.1) | ||||||||
| Once a week for weeks 4-12 following the surgery | |||||||||||
| Zaffagnini et al[9], 2013 | RCT | ACL reconstruction | Cases: 51 | Cases: Therapeutic vision videos + standard physiotherapy | Cases: Art video producing therapeutic insight | No | 8 weeks | 3 times per week | 33 (17) | 80/101 | 12 weeks |
| Placebos: 50 | Placebos: Videos of unfavorable information + standard physiotherapy | Placebos: Art video with an insight unfavorable to the psychological recovery | |||||||||
| Maddison et al[16], 2012 | RCT | ACL reconstruction | Cases: 13 | Cases: Mental rehearsal of rehabilitation goals + standard physiotherapy | Nine individual sessions of mental rehearsal of activities to achieve physical rehabilitation goals including cognitive, motivational, and healing imagery; cognitive imagery was used to rehearse rehabilitation exercises, using both visual and kinaesthetic modalities. Motivational imagery was used to set goals, control arousal levels, and increase self-confidence. Healing imagery was used to imagine the physiological processes taking place during rehabilitation | No | 24 weeks | NR | 34.86 (8.84) | 13/21 | 24 weeks |
| Controls: 8 | Controls: Standard physiotherapy | ||||||||||
| Lebon et al[4], 2012 | RCT | ACL reconstruction | Cases: 7 | Cases: Imagining muscle contractions + standard physiotherapy | 3 blocks of 10 imagined contractions, with a 10-second rest period between rehearsals and 2-minute rest period between blocks | No | 5 weeks | Every 2 days | 28.5 (5) | NR | 5 weeks |
| Placebos: 5 | Placebos: Neutral mental task (crossword or calculation) + standard physiotherapy | ||||||||||
| Maddison et al[15], 2006 | RCT | ACL reconstruction | Cases: 30 | Cases: Coping-model video + standard physiotherapy | Two coping model videos of edited interviews and models performing rehabilitation exercises; first video pre-op to 2 weeks post-op (9-minute) and second video 2 weeks to 6 weeks post-op (7-minute) | Yes | 6 weeks | NR | 30 | NR | 6 weeks |
| Controls: 28 | Controls: Standard physiotherapy | ||||||||||
| Cupal and Brewer[3], 2001 | RCT | ACL reconstruction | Cases: 10 | Cases: Mental rehearsal of rehabilitation goals + standard physiotherapy | Videos of patient’s arthroscopic procedure, facilitating knee flexibility and ROM, edema reduction, knee strength, position sense, anxiety reduction, anatomical and neurological mental comparison | No | 24 weeks | Every 2 weeks | 28.2 (8.2) | 16/30 | 24 weeks |
| Placebos: 10 | Placebos: Peaceful scene imagery + attention, encouragement, and support + standard physiotherapy | ||||||||||
| Controls: 10 | Controls: Standard physiotherapy |
Six studies compared the intervention group with the placebo groups[3,4,6-9], while eight compared the intervention group with controls (Table 1)[3,8,12-17]. Research by Rhim et al[8] and Cupal and Brewer[3] contrasted the intervention groups with placebo and control groups (Table 1).
The frequency of intervention administration was documented in eight studies[3,4,6,7,9,12,13,17] with three-times-per-week schedule being the most commonly reported frequency, appearing in four of the studies[7,9,12,13]. With regard to the length of the program, the 24-week treatment period was the longest and most reported duration, having been found in four investigations[3,6,8,16]. The shortest treatment period, however, was found in the study by Lyles et al[17], which lasted only six days. The presence of preoperative treatment sessions was reported in three studies[6,8,15]. The mean follow-up duration ranged between 6 days to 24 weeks. Detailed information about the intervention characteristics is presented in Table 1.
Postoperative pain: A total of three articles compared the postoperative pain between the intervention and control groups[3,13,17] (Table 2). Quantitative analysis was impractical due to the disparate scales employed for reporting pain in the articles. However, studies by D’Isanto et al[13], Cupal and Brewer[3], and Lyles et al[17], all revealed significantly improved postoperative pain in the intervention group in comparison to control individuals (P value = 0.023, < 0.05, and 0.0018; respectively).
| Ref. | Measured outcomes | Results |
| Almuhaya et al[12], 2023 | Kinesiophobia (TSK) | Improved TSK (P = 0.026) and ACL-RSI (P = 0.009) in cases than controls, no significant difference in IKDC (P = 0.42) between groups |
| Return to sport (ACL-RSI) | ||
| Functional status (IKDC) | ||
| Lee et al[14], 2023 | Knee strength (biodex isokinetic dynamometer) | No significant difference in muscle strength (P = 0.25 to 0.96), knee laxity (P = 0.96), and subjective knee evaluation (P = 0.99) between groups |
| Knee laxity (KT1000) | ||
| Functional status (IKDC) | ||
| D’Isanto et al[13], 2022 | Pain (VAS score) | Greater psychological readiness (P < 0.01) and lower postoperative pain in cases than controls |
| Psychological readiness (ACL-RSI) | ||
| Lyles et al[17], 2014 | Pain (VAS score) | Improved postoperative pain (P = 0.0018), AROM (P = 0.0004), PROM (P = 0.0011), and Lysholm score (P = 0.044) |
| ROM (AROM and PROM in flexion) | ||
| Functional status (Lysholm) | ||
| Rhim et al[8], 2020 | Kinesiophobia (TSK) | No significant difference in self-efficacy (P = 0.808), return to sport (P = 0.574), kinesiophobia (P = 0.888), and KOOS subscales (P = 0.236 to 0.916) between groups |
| Return to sport (ACL-RSI) | ||
| Self-efficacy (K-SES) | ||
| Functional status (KOOS) | ||
| Maddison et al[16], 2012 | Self-efficacy (AISEQ) | Improved postoperative knee laxity (P < 0.05) favoring the intervention |
| Knee strength (180/second, 60/second) | No significant difference for knee strength for extension at 180/second (P = 0.67) or 60/second (P = 0.48) | |
| Knee laxity (KT1000) | Fairly stable self-efficacy between weeks 6 to weeks 12 in cases than controls | |
| Lebon et al[4], 2012 | Preoperative perception of pain (0-100 scale) | Improved crutches (P < 0.01), walking (P = 0.01), and exercise (P < 0.05) SE in cases than controls only at predischarge, better IKDC 6 weeks postop, less crutches use time in cases than controls (P < 0.01) |
| Preoperative anxiety (STAI) | ||
| Self-efficacy (CSE, WSE, ESE) | ||
| Functional status (IKDC subjective and objective) | No significant difference in preoperative anxiety reduction, preoperative perception of pain reduction (P = 0.52), and postoperative ROM (P = 0.36) between groups | |
| ROM by goniometry | ||
| Crutches use time | ||
| Maddison et al[15], 2006 | Pain (0-10 scale) | Improved pain in cases than controls (P < 0.05). Greater post-op knee strength in cases than controls (P < 0.02). Reduced re-injury anxiety in cases than controls (P < 0.05) |
| Reinjury anxiety (0-10 scale) | ||
| Knee strength (cybex 6000) | ||
| Isokinetic dynamometer) |
Comparing the MI and placebo groups, three studies documented the postoperative pain (Table 3)[3,4,6], of which studies by Brewer et al[6] and Cupal and Brewer[3] presented a significantly diminished postoperative pain in the imagery group in comparison to the placebo group (P value = 0.02 and < 0.05, respectively). However, the study by Lebon et al[4] found no significant difference in postoperative pain scores between groups (P value > 0.05).
| Ref. | Measured outcomes | Results |
| Brewer et al[6], 2022 | Pain (NRS) | Lower postoperative pain (P = 0.02), lower kinesiophobia (P = 0.77), improved postoperative symptoms (P = 0.002) in cases than controls |
| Kinesiophobia (TSK) | No significant difference in flexion ROM (P = 0.99), extension ROM (P = 0.18), and knee laxity (P = 0.09) between groups | |
| Subjective symptoms (KOS-SAS) | ||
| Knee laxity (KT1000) | ||
| ROM (flex and ext) | ||
| Rhim et al[8], 2020 | Kinesiophobia (TSK) | No significant difference in self-efficacy (P = 0.808), return to sport (P = 0.574), kinesiophobia (P = 0.888), and KOOS subscales (P = 0.236 to 0.916) between groups |
| Return to sport (ACL-RSI) | ||
| Self-efficacy (K-SES) | ||
| Functional status (KOOS) | ||
| Levinger et al[7], 2017 | Self-efficacy (K-SES) | No significant difference in KOOS subscales (P = 0.07-0.76), self-efficacy subscales (P = 0.42 and 0.71), kinesiophobia (P = 0.46), fear of activity (P = 0.96) between groups |
| Functional status (KOOS) | ||
| Kinesiophobia (TSK) | ||
| FABQ | ||
| Zaffagnini et al[9], 2013 | QOL (mental and physical SF-36) | Improved subjective IKDC (P = 0.047), TKS (P = 0.0141) and time to crutches discharge (P = 0.0012). No significant difference in Tegner score, and SF-36 mental and physical status between groups |
| Kinesiophobia (TSK) | ||
| Functional (subjective and objective IKDC, Tegner) | ||
| Crutches use time | ||
| Lebon et al[4], 2012 | Isometric activation of the medial musculature (EMG during maximum knee extension) | Greater postoperative musculature activity in cases than controls (P = 0.02). No significant difference in postoperative pain, ROM, effusion reduction, thigh circumference, LEFS score (P > 0.05) between groups |
| Pain (VAS score) | ||
| Ability to perform daily activities with lower extremity injury using the LEFS | ||
| Magnitude of surgical effusion and atrophy by the circumference of the knee above the kneecap and circumference of the thigh 15 cm above the kneecap | ||
| Knee ROM (goniometry) | ||
| Cupal and Brewer[3], 2001 | Pain (0-10 scale) | Improved pain in cases than placebos (P < 0.05). Reduced re-injury anxiety in cases than placebos (P < 0.05). Greater post-op knee strength in cases than placebos (P < 0.003) |
| Reinjury anxiety (0-10 scale) | ||
| Knee strength (cybex 6000) | ||
| Isokinetic dynamometer |
Postoperative kinesiophobia: Studies by Rhim et al[8] and Almuhaya et al[12] provided data on postoperative kinesiophobia (as measured by the Tampa Kinsiophobia Scale), comparing the imagery and control groups (Table 2). The study by Almuhaya et al[12] noted improved kinesiophobia following surgery in patients who received MI in comparison to the control group (P value = 0.026). In contrast, the study by Rhim et al[8] reported no significant difference between the study groups. Most studies reported a reduction in kinesiophobia following imagery-based interventions, although effect magnitude varied.
Postoperative knee laxity: Studies by Lee et al[14] and Maddison et al[16] provided data on postoperative knee laxity comparing case and control groups (Table 2). The study by Lee et al[14] found no significant difference in postoperative knee laxity between study groups (P value = 0.96). However, Maddison et al[16] reported significantly improved knee laxity after surgery in the imagery group compared to the controls (P value < 0.05).
Only one study by Brewer et al[6] compared postoperative knee laxity between patients who watched imagery videos and those who received placebo videos which reported no significant difference regarding the postoperative knee laxity between the two groups (P value = 0.09) (Table 3).
Postoperative knee ROM: Two studies compared the postoperative knee ROM between the intervention and control groups (Table 2)[15,17]. The study by Lyles et al[17] reported significant improvements in postoperative active and passive knee ROM in the imagery group in comparison to the control group (P value = 0.0004 and 0.0011, respectively). However, the study by Maddison et al[15] found no significant difference in postoperative knee ROM between the intervention and control groups (P value = 0.36).
Studies by Brewer et al[6] and Lebon et al[4] provided data on postoperative knee ROM in the imagery group compared to the placebo group, of which both presented no significantly improved postoperative knee ROM in patients who received imagery videos in comparison to the placebo group (P value > 0.05) (Table 3).
Postoperative strength: A total of three articles compared the postoperative knee strength between the intervention and control groups[3,14,16] (Table 2). Meta-analysis was unreasonable to conduct due to the heterogeneity in reported variables. Cupal and Brewer[3] showed significantly improved knee strength, which was measured with a Cybex 6000 isokinetic dynamometer, an instrument that assesses maximal torque during concentric-eccentric movements of a limb, following the surgery in imagery groups compared to the controls (P value < 0.02). However, studies by Lee et al[14] and Maddison et al[16] declared no significant difference in postoperative knee strength between the study groups (P value > 0.05).
Cupal and Brewer[3] study compared postoperative knee strength between patients who received imagery videos and those in the placebo group (Table 3). The study reported significantly higher knee strength in the imagery group compared to the placebo group (P value < 0.003).
Postoperative SE: Three studies provided information on comparing postoperative SE between the imagery and control groups[8,15,16] (Table 2). However, the variety of SE measurement scales prevented us from the conduction quantitative analysis. The study by Maddison et al[15] found improved SE in walking, using crutches, and exercise performance in patients who underwent imagery techniques than those who received only a standard physiotherapy program (P value = 0.01, < 0.01, < 0.05; respectively). Another study by Maddison et al[16] reported relatively stable SE between postoperative weeks 6 to weeks 12 in the imagery group than controls. Nonetheless, the survey by Rhim et al[8] represented no significant difference in postoperative SE between the study groups (P value = 0.808).
Two studies by Levinger et al[7] and Rhim et al[8] evaluated postoperative SE between the intervention and placebo groups. They exhibited no significant difference in postoperative SE between study groups (P value = 0.808, and P value = 0.42 and 0.71 for SE subscales, respectively) (Table 3).
Study by Rhim et al[8] compared postoperative RTS between imagery and placebo groups, which reported no significant difference in postoperative Anterior Cruciate Ligament-RTS after Injury (ACL-RSI) scale between the study groups (P value = 0.574) (Table 3).
Among the studies that compared intervention and control groups, the International Knee Documentation Committee (IKDC) score was assessed in three studies[12,14,15] (Table 2), showing no significant improvement postoperatively in two studies (P value = 0.42 and 0.99)[12,14], while one study reported a better score at 6 weeks post-operation[15]. The Knee Injury and Osteoarthritis Outcome Score (KOOS) subscales was examined in the study by Rhim et al[8] indicating no significant difference between groups (P value = 0.236 to 0.916). Additionally, the Lysholm score was evaluated in one study[17], demonstrating a significant improvement following surgery in the imagery group compared to the controls (P value = 0.044).
In studies comparing interventions with placebo groups, two investigations evaluated the KOOS score and found no significant differences[7,8]. Only Zaffagnini et al[9] evaluated IKDC and Tegner scores, showing a substantial improvement in IKDC (P value = 0.047) but no significant change in postoperative Tegner scores after treatment (Table 3). Due to the limited number of studies and heterogeneity of outcomes, a meta-analytic synthesis and formal assessment of publication bias were not performed.
This article evaluated the effects of mental imagery-based and other psychological interventions on postoperative outcomes following ACLR. Across the included randomized controlled trials, a wide range of interventions was examined, including MI, guided imagery, mirror therapy, educational and multimedia programs, and web-based or modeling approaches. Outcomes varied substantially and included postoperative pain, kinesiophobia, SE, psychological readiness to RTS, knee function, and strength. Intervention timing and duration also differed considerably, ranging from brief preoperative exposure to programs extending several months into postoperative rehabilitation.
Beyond physical impairment, ACL injuries are associated with substantial psychological consequences. Previous research has shown that only approximately 55% of athletes RTS after ACLR, often at a reduced level compared with preinjury status[18,19]. Psychological factors, particularly fear of reinjury and kinesiophobia, are common after ACL reconstruction and have been shown to hinder RTS, alter knee biomechanics, and potentially increase the risk of reinjury[20] targeted psychological interventions may therefore play a critical role in improving both psychological and functional recovery after ACLR[21].
Imagery-based interventions may help reduce fear of reinjury and postoperative discomfort. Addressing psychological factors during early rehabilitation may alleviate pain and improve ROM, while continued application throughout later rehabilitation phases may remain beneficial. However, findings across studies were not entirely consistent. Lebon et al[4] reported no significant benefit of MI, potentially due to the use of strong analgesic therapy during the early postoperative period, which may have influenced patients’ perception of imagery effects. Nevertheless, substantial evidence supports the role of imagery in pain reduction, both in ACLR and in sports-related injuries more broadly[22,23] with additional studies in this review reporting similar findings[3,6,13,17].
The proposed mechanism underlying pain reduction through MI and mirror therapy relates to modulation of sensory-motor integration within the central nervous system[24]. These techniques may reduce incongruence between motor intention and sensory feedback, which is thought to contribute to pain perception[25]. By influencing cognitive and emotional processing of pain, such interventions may alter the subjective pain experience[26]. Several studies reported reductions in pain across different mental training techniques suggests a shared underlying mechanism[27], although mirror therapy does not appear to provide superior immediate analgesia compared with MI alone[28].
Psychological readiness to RTS represents another important outcome following ACLR. Although many patients recover adequate physical function, a considerable proportion do not resume sport participation[29]. At the amateur level, approximately one-third of female football players fail to RTS, and those who do remain at increased risk of reinjury, particularly to the contralateral limb[30]. Across the included studies, findings for postoperative ACL-RSI were mixed, with some trials reporting improvement and others showing little or no change. Rhim et al[8] assessed multiple psychological measures and reported a significant effect only for knee SE at six months postoperatively. The inclusion of a placebo group in their study may partly explain discrepancies with other trials, as controlling for the effect of receiving video-based content - irrespective of its psychological focus - is important when evaluating modeling interventions[31]. While placebo-controlled designs enhance methodological rigor, they may not always be essential in future trials with limited resources[8,32].
Mirror therapy and structured educational interventions also demonstrated potential benefits. D’Isanto et al[13] reported improved Sport after Injury Scale scores in players receiving mirror therapy, accompanied by reduced pain and enhanced SE. Similarly, Almuhaya et al[12] found that structured educational sessions during rehabilitation significantly improved ACL-RSI scores and reduced kinesiophobia. These findings suggest that combining imagery techniques with educational components may further enhance psychological readiness during rehabilitation. Additionally, technology-based delivery methods, such as interactive multimedia programs, may improve accessibility and engagement, as demonstrated by Brewer et al[6].
Evidence regarding the effects of psychological interventions on biomechanical and functional outcomes remains mixed. Some studies reported improvements in knee laxity[16,33], while others found no significant differences[6,14], reflecting the ongoing controversy in the literature[34]. Psychological factors may influence knee laxity indirectly through rehabilitation adherence and neuromuscular control[35]. However, recovery outcomes are also affected by numerous moderators, including rehabilitation protocols, surgical factors, injury severity, and individual patient characteristics[36]. Short follow-up periods may further limit the ability to detect meaningful changes in objective clinical outcomes[14]. Longer follow-up durations may better capture recovery trajectories as patients progress to higher-intensity rehabilitation phases[37].
Functional outcomes were assessed using various instruments, including the IKDC, KOOS, and Lysholm scores. Each tool captures different dimensions of knee function, with the KOOS and Lysholm scores demonstrating high responsiveness over time[38-40], while the IKDC remains the most commonly used patient-reported outcome measure in ACL research due to its reliability and validity[41]. Results across studies were inconsistent, with some reporting short-term improvements[3,15,17], and others showing no significant difference[14]. Variability in intervention type and outcome selection likely contributed to these mixed findings.
Only 2 studies had more than 50 participants in our included studies, indicating a clear limitation in sample size across the reviewed literature. Additionally, 3 out of 12 studies used remote interventions while the rest relied on in-person methods[6,7,14]. Furthermore, the gender distribution was only reported in eight studies, and one study included only male participants, introducing potential bias. Only a small number of studies reported the same outcome measures, which limited comparability across trials.
The studies varied significantly in their intervention protocols, ranging from six days to 24 weeks, with most lacking follow-up with patients beyond 24 weeks, limiting the understanding of long-term outcomes. Differences in interventions, timing, and delivery likely contributed to variability in study findings. Another methodological limitation is the reliance on self-report measures, which may introduce bias, such as self-serving tendencies. Future research should consider integrating objective measures, such as clinic attendance or implicit association tests, to capture more objective data. Additionally, the lack of detailed data on intervention adherence, such as the frequency and duration of usage in remote interventions, limits the ability to evaluate the true impact of these methods. Finally, important confounding factors, such as the severity of ACL tears, socio-economic status, and leg dominance, were not consistently accounted for across the studies, which may have influenced the results. Larger sample sizes and better control of these variables are essential for future research to fully understand the effectiveness of psychological interventions in ACL reconstruction rehabilitation.
This article suggests that psychological interventions - particularly those incorporating MI - may help reduce postoperative pain following ACL reconstruction. However, evidence for effects on kinesiophobia, SE, functional recovery, and RTS remains inconsistent across studies. Interpretation is limited by small sample sizes, variability in intervention protocols, and short follow-up durations. Larger, well-designed randomized trials with standardized outcome measures are needed to clarify the role of psychological interventions in ACL rehabilitation.
| 1. | Zwolski CM, Paterno MV, Magnussen RA, Thomas SM, Goodway JD, Hand BN, Quatman-Yates CC, Schmitt LC. The Association of Physical Competence With Psychological Response Among Young Athletes at Time of Return to Sport After ACL Reconstruction. Am J Sports Med. 2023;51:2908-2917. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 2. | Xiao M, van Niekerk M, Trivedi NN, Hwang CE, Sherman SL, Safran MR, Abrams GD. Patients Who Return to Sport After Primary Anterior Cruciate Ligament Reconstruction Have Significantly Higher Psychological Readiness: A Systematic Review and Meta-analysis of 3744 Patients. Am J Sports Med. 2023;51:2774-2783. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 52] [Article Influence: 17.3] [Reference Citation Analysis (0)] |
| 3. | Cupal DD, Brewer BW. Effects of relaxation and guided imagery on knee strength, reinjury anxiety, and pain following anterior cruciate ligament reconstruction. Rehabil Psychol. 2001;46:28-43. [DOI] [Full Text] |
| 4. | Lebon F, Guillot A, Collet C. Increased muscle activation following motor imagery during the rehabilitation of the anterior cruciate ligament. Appl Psychophysiol Biofeedback. 2012;37:45-51. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 59] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 5. | Pastora-Bernal JM, Estebanez-Pérez MJ, Lucena-Anton D, García-López FJ, Bort-Carballo A, Martín-Valero R. The Effectiveness and Recommendation of Motor Imagery Techniques for Rehabilitation after Anterior Cruciate Ligament Reconstruction: A Systematic Review. J Clin Med. 2021;10:428. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 13] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 6. | Brewer BW, Van Raalte JL, Cornelius AE. An Interactive Cognitive-Behavioural Multimedia Program Favourably Affects Pain and Kinesiophobia During Rehabilitation After Anterior Cruciate Ligament Surgery: An Effectiveness Trial. Int J Sport Exerc Psychol. 2022;20:1133-1155. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 11] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 7. | Levinger P, Hallam K, Fraser D, Pile R, Ardern C, Moreira B, Talbot S. A novel web-support intervention to promote recovery following Anterior Cruciate Ligament reconstruction: A pilot randomised controlled trial. Phys Ther Sport. 2017;27:29-37. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 26] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 8. | Rhim HC, Lee SJ, Jeon JS, Kim G, Lee KY, Lee JH, Jang KM. Effectiveness of modeling videos on psychological responses of patients following anterior cruciate ligament reconstruction: A pilot randomized trial. Medicine (Baltimore). 2020;99:e23158. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 12] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 9. | Zaffagnini S, Russo RL, Marcheggiani Muccioli GM, Marcacci M. The Videoinsight® method: improving rehabilitation following anterior cruciate ligament reconstruction--a preliminary study. Knee Surg Sports Traumatol Arthrosc. 2013;21:851-858. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 32] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 10. | Higgins JPT, Green S. Cochrane Handbook for Systematic Reviews of Interventions. London: The Cochrane Collaboration, 2008. |
| 11. | Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng HY, Corbett MS, Eldridge SM, Emberson JR, Hernán MA, Hopewell S, Hróbjartsson A, Junqueira DR, Jüni P, Kirkham JJ, Lasserson T, Li T, McAleenan A, Reeves BC, Shepperd S, Shrier I, Stewart LA, Tilling K, White IR, Whiting PF, Higgins JPT. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ. 2019;366:l4898. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22257] [Cited by in RCA: 20296] [Article Influence: 2899.4] [Reference Citation Analysis (7)] |
| 12. | Almuhaya A, Albarrati A, Alhowimel A, Alodaibi F. Adding A Structured Educational Session to the Rehabilitation Program of Soccer Players Following Anterior Cruciate Ligament Reconstruction: A Feasibility Study. Int J Sports Phys Ther. 2023;18:81-91. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 13. | D’Isanto T, D'Elia F, Esposito G, Altavilla G, Raiola G. Examining the Effects of Mirror Therapy on Psychological Readiness and Perception of Pain in ACL-Injured Female Football Players. J Funct Morphol Kinesiol. 2022;7:113. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 14. | Lee ASY, Shu-Hang Yung P, Ong MT, Lonsdale C, Wong TWL, Siu PM, Hagger MS, Chan DKC. Effectiveness of a theory-driven mHealth intervention in promoting post-surgery rehabilitation adherence in patients who had anterior cruciate ligament reconstruction: A randomized clinical trial. Soc Sci Med. 2023;335:116219. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 15. | Maddison R, Prapavessis H, Clatworthy M. Modeling and rehabilitation following anterior cruciate ligament reconstruction. Ann Behav Med. 2006;31:89-98. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 55] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 16. | Maddison R, Prapavessis H, Clatworthy M, Hall C, Foley L, Harper T, Cupal D, Brewer B. Guided imagery to improve functional outcomes post-anterior cruciate ligament repair: randomized-controlled pilot trial. Scand J Med Sci Sports. 2012;22:816-821. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 42] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 17. | Lyles CR, Schafer AL, Seligman HK. Income, food insecurity, and osteoporosis among older adults in the 2007-2008 National Health and Nutrition Examination Survey (NHANES). J Health Care Poor Underserved. 2014;25:1530-1541. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 25] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 18. | Ardern CL, Taylor NF, Feller JA, Webster KE. Fifty-five per cent return to competitive sport following anterior cruciate ligament reconstruction surgery: an updated systematic review and meta-analysis including aspects of physical functioning and contextual factors. Br J Sports Med. 2014;48:1543-1552. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1184] [Cited by in RCA: 1022] [Article Influence: 85.2] [Reference Citation Analysis (0)] |
| 19. | Medvecky MJ, Nelson S. Kinesiophobia and Return to Sports After Anterior Cruciate Ligament Reconstruction. Conn Med. 2015;79:155-157. [PubMed] |
| 20. | Rodriguez RM, Marroquin A, Cosby N. Reducing Fear of Reinjury and Pain Perception in Athletes With First-Time Anterior Cruciate Ligament Reconstructions by Implementing Imagery Training. J Sport Rehabil. 2019;28:385-389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 33] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 21. | Driediger M, Hall C, Callow N. Imagery use by injured athletes: a qualitative analysis. J Sports Sci. 2006;24:261-271. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 40] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 22. | Evans L, Hare R, Mullen R. Imagery Use During Rehabilitation from Injury. J Imag Res Sport Phys Act. 2006;1. [DOI] [Full Text] |
| 23. | Ol HS, Van Heng Y, Danielsson L, Husum H. Mirror therapy for phantom limb and stump pain: a randomized controlled clinical trial in landmine amputees in Cambodia. Scand J Pain. 2018;18:603-610. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 24] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 24. | Herrador Colmenero L, Perez Marmol JM, Martí-García C, Querol Zaldivar MLÁ, Tapia Haro RM, Castro Sánchez AM, Aguilar-Ferrándiz ME. Effectiveness of mirror therapy, motor imagery, and virtual feedback on phantom limb pain following amputation: A systematic review. Prosthet Orthot Int. 2018;42:288-298. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 118] [Cited by in RCA: 84] [Article Influence: 10.5] [Reference Citation Analysis (0)] |
| 25. | Wittkopf PG, Johnson MI. Mirror therapy: A potential intervention for pain management. Rev Assoc Med Bras (1992). 2017;63:1000-1005. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 34] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 26. | Thieme H, Morkisch N, Rietz C, Dohle C, Borgetto B. The Efficacy of Movement Representation Techniques for Treatment of Limb Pain--A Systematic Review and Meta-Analysis. J Pain. 2016;17:167-180. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 105] [Cited by in RCA: 87] [Article Influence: 8.7] [Reference Citation Analysis (0)] |
| 27. | Cuenca-Martínez F, Reina-Varona Á, Castillo-García J, La Touche R, Angulo-Díaz-Parreño S, Suso-Martí L. Pain relief by movement representation strategies: An umbrella and mapping review with meta-meta-analysis of motor imagery, action observation and mirror therapy. Eur J Pain. 2022;26:284-309. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 26] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 28. | Forsdyke D, Smith A, Jones M, Gledhill A. Psychosocial factors associated with outcomes of sports injury rehabilitation in competitive athletes: a mixed studies systematic review. Br J Sports Med. 2016;50:537-544. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 163] [Cited by in RCA: 134] [Article Influence: 13.4] [Reference Citation Analysis (0)] |
| 29. | Brophy RH, Schmitz L, Wright RW, Dunn WR, Parker RD, Andrish JT, McCarty EC, Spindler KP. Return to play and future ACL injury risk after ACL reconstruction in soccer athletes from the Multicenter Orthopaedic Outcomes Network (MOON) group. Am J Sports Med. 2012;40:2517-2522. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 337] [Cited by in RCA: 292] [Article Influence: 20.9] [Reference Citation Analysis (0)] |
| 30. | Everhart JS, Best TM, Flanigan DC. Psychological predictors of anterior cruciate ligament reconstruction outcomes: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2015;23:752-762. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 174] [Cited by in RCA: 192] [Article Influence: 17.5] [Reference Citation Analysis (0)] |
| 31. | Munnangi S, Sundjaja JH, Singh K, Dua A, Angus LD. Placebo Effect. 2023 Nov 13. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. [PubMed] |
| 32. | Brewer BW, Van Raalte JL, Cornelius AE, Petitpas AJ, Sklar JH, Pohlman MH, Krushell RJ, Ditmar TD. Psychological factors, rehabilitation adherence, and rehabilitation outcome after anterior cruciate ligament reconstruction. Rehabil Psychol. 2000;45:20-37. [DOI] [Full Text] |
| 33. | Zaffagnini S, Grassi A, Serra M, Marcacci M. Return to sport after ACL reconstruction: how, when and why? A narrative review of current evidence. Joints. 2015;3:25-30. [PubMed] |
| 34. | Mercurio M, Cerciello S, Corona K, Guerra G, Simonetta R, Familiari F, Galasso O, Gasparini G. Factors Associated With a Successful Return to Performance After Anterior Cruciate Ligament Reconstruction: A Multiparametric Evaluation in Soccer Players. Orthop J Sports Med. 2024;12:23259671241275663. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 12] [Reference Citation Analysis (0)] |
| 35. | Faleide AGH, Magnussen LH, Bogen BE, Strand T, Mo IF, Vervaat W, Inderhaug E. Association Between Psychological Readiness and Knee Laxity and Their Predictive Value for Return to Sport in Patients With Anterior Cruciate Ligament Reconstruction. Am J Sports Med. 2021;49:2599-2606. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 24] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 36. | Cronström A, Häger CK, Thorborg K, Ageberg E. Factors Associated With Sports Function and Psychological Readiness to Return to Sports at 12 Months After Anterior Cruciate Ligament Reconstruction: A Cross-sectional Study. Am J Sports Med. 2023;51:3112-3120. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 30] [Reference Citation Analysis (0)] |
| 37. | Briggs KK, Lysholm J, Tegner Y, Rodkey WG, Kocher MS, Steadman JR. The reliability, validity, and responsiveness of the Lysholm score and Tegner activity scale for anterior cruciate ligament injuries of the knee: 25 years later. Am J Sports Med. 2009;37:890-897. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 794] [Cited by in RCA: 729] [Article Influence: 42.9] [Reference Citation Analysis (0)] |
| 38. | Yang XG, Feng JT, He X, Wang F, Hu YC. The effect of knee bracing on the knee function and stability following anterior cruciate ligament reconstruction: A systematic review and meta-analysis of randomized controlled trials. Orthop Traumatol Surg Res. 2019;105:1107-1114. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 33] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 39. | Sakai M, Akasaki Y, Akiyama T, Horikawa T, Okazaki K, Hamai S, Tsushima H, Kawahara S, Kurakazu I, Kubota K, Mizu-Uchi H, Nakashima Y. Similar short-term KOOS between open-wedge high tibial osteotomy and total knee arthroplasty in patients over age 60: A propensity score-matched cohort study. Mod Rheumatol. 2023;33:623-628. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 40. | Abed V, Kapp S, Nichols M, Castle JP, Landy DC, Conley C, Stone AV. Lysholm and KOOS QoL Demonstrate High Responsiveness in Patients Undergoing Anterior Cruciate Ligament Reconstruction: A Systematic Review and Meta-analysis of Randomized Clinical Trials. Am J Sports Med. 2024;52:3161-3166. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 12] [Article Influence: 6.0] [Reference Citation Analysis (0)] |