Published online Apr 18, 2026. doi: 10.5312/wjo.v17.i4.115881
Revised: November 23, 2025
Accepted: February 4, 2026
Published online: April 18, 2026
Processing time: 164 Days and 18 Hours
Proximal tibial fractures (PTFs), including tibial plateau fractures (TPFs), are usually managed with osteosynthesis; however, in elderly patients with pre-injury knee osteoarthritis and osteoporotic bone, performing an acute total knee arthroplasty (aTKA) became a viable management option.
To explore the indications, patient characteristics, implant selection, and reported outcomes (functional, radiological, complications, and revision rates) after aTKA to manage traumatic PTFs.
A systematic literature search of English-language studies reporting on the aTKA for managing PTFs, including TPFs, was conducted across three major databases (EMBASE, PubMed, and Scopus) from inception to December 2024.
Of the 1055 reviewed articles, 14 studies with 174 patients met the inclusion criteria. The mean age was 71.3 years, and 60.9% were females. The incidence of pre-injury knee osteoarthritis ranged from 22.7% to 100%, and 90.8% were TPFs. A medial parapatellar approach was used in all cases, and a posterior-stabilized implant was most commonly used (49.4%). Of 103 patients in whom extras were used, 97.1% had a tibial stem, and 20.4% required metal augments for tibial bone defect reconstruction. After a mean follow up of 28.5 months, the maximum knee flexion as reported from 121 patients had a mean of 110.3 degrees, while the functional outcomes per the Knee Society Function and Knee Scores were reported in 129 patients and had good and fair outcomes, respectively. Complication incidence was 16.67%, with infection as the most common complication, and revision was required in only 3 (2.3%) patients.
The aTKA for managing PTFs is an appealing management option with acceptable functional, complication, and revision outcomes. Various implants and extras can be employed based on fracture type, collateral ligament status, and bone defect size. Better-designed studies with a larger number of patients and longer follow up are needed to validate the outcomes of such a management approach compared to other management options.
Core Tip: Managing proximal tibial fractures, particularly tibial plateau fractures, in elderly patients with osteoporotic bone and pre-existing knee osteoarthritis is challenging. This systematic review evaluated the role of acute total knee arthroplasty as a primary treatment option. Fourteen studies involving 174 patients were analyzed. Most were elderly females with total knee arthroplasty and pre-injury osteoarthritis. Posterior-stabilized implants were commonly used, often with tibial stems and metal augments. Outcomes were favorable, with a mean flexion of 110 degrees and generally good Knee Society Scores. Complications occurred in 16.7%, and revisions in 2.3%. Despite promising results, evidence quality was low, warranting larger comparative studies.
- Citation: Khalifa AA, Altahir A, AL-Harbi AM, Althaqafi RMM. Acute total knee arthroplasty for traumatic proximal tibial fractures: A systematic review. World J Orthop 2026; 17(4): 115881
- URL: https://www.wjgnet.com/2218-5836/full/v17/i4/115881.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i4.115881
Although proximal tibial fracture (PTFs) represents only about 1% of adult fractures, in the elderly population, they pose a specific challenge to the treating surgeons due to possible osteoporosis, soft tissue fragility, a higher incidence of concomitant pre-injury knee osteoarthritis (OA), and associated medical comorbidities[1-3]. Furthermore, the management becomes more challenging if these were tibial plateau fractures (TPFs), which have an incidence of about 24%, due to articular surface involvement and the possibility of injury-induced bone defects[1,4-6].
The main goal of treating PTFs or TPFs is to achieve anatomical fracture reduction and secure fixation to promote proper union and early patient mobilization for better functional recovery[2,4,7,8]. These goals could be achieved by various management strategies, including conservative management for minimally displaced fractures, open reduction and internal fixation (ORIF) for displaced fractures and those involving the articular surface, and total knee arthroplasty (TKA) either in an acute setting as a definitive management line or in a delayed (secondary) fashion to manage fracture sequelae[2,9-12]. It is worth noting that in the elderly population with PTFs, ORIF failure occurs in about 30% to 97% of the cases[10,13-16].
The TKA conversion rate after TPFs reaches up to 5%[17]. Furthermore, delayed TKA for managing sequelae of TPFs, such as post-traumatic OA, showed higher complication incidence reaching up to 60%[13,18,19]. Therefore, there has been increasing interest in performing acute TKA (aTKA) for managing PTFs in relatively older patients with osteoporotic bone or pre-injury knee OA, which has shown encouraging outcomes compared to other management modalities[13,17,20-22]. The current systematic review aimed to explore indications, patient characteristics, implant selection, and reported outcomes (functional, radiological, complications, and revision rates) following aTKA for traumatic PTFs.
The current systematic literature review was carried out following the Preferred Reporting Items for Systematic
The inclusion criteria were English language studies (randomized controlled trials, cohort studies, case series, and case reports) reporting the outcomes (clinical, radiological, and complications) of performing aTKA as the primary management of traumatic PTFs (intra-articular or extra-articular). We excluded studies not published in English, performed on animal models, other publication types (reviews, editorials, abstracts, technical notes, and commentaries), and studies not including the outcomes of interest, or if those outcomes could not be extracted (studies on femoral and tibial periarticular knee fracture where the outcomes could not be separated).
We developed a search strategy based on the predefined PICO (population, intervention, comparison, and outcome) model. The population of interest was patients with traumatic PTFs (intra-articular or extra-articular). The intervention was TKA as the primary intervention after trauma. Comparison with other management modalities (if present), such as ORIF or non-operative management. The main outcomes were functional, radiological, complications, and revision rate outcomes.
A comprehensive English literature search was performed on December 15, 2024 through three databases (EMBASE, PubMed, and Scopus), using various combinations of the following terms (TKA, total knee replacement, PTFs, and TPFs). The details of the search strategy are presented in Supplementary Table 1.
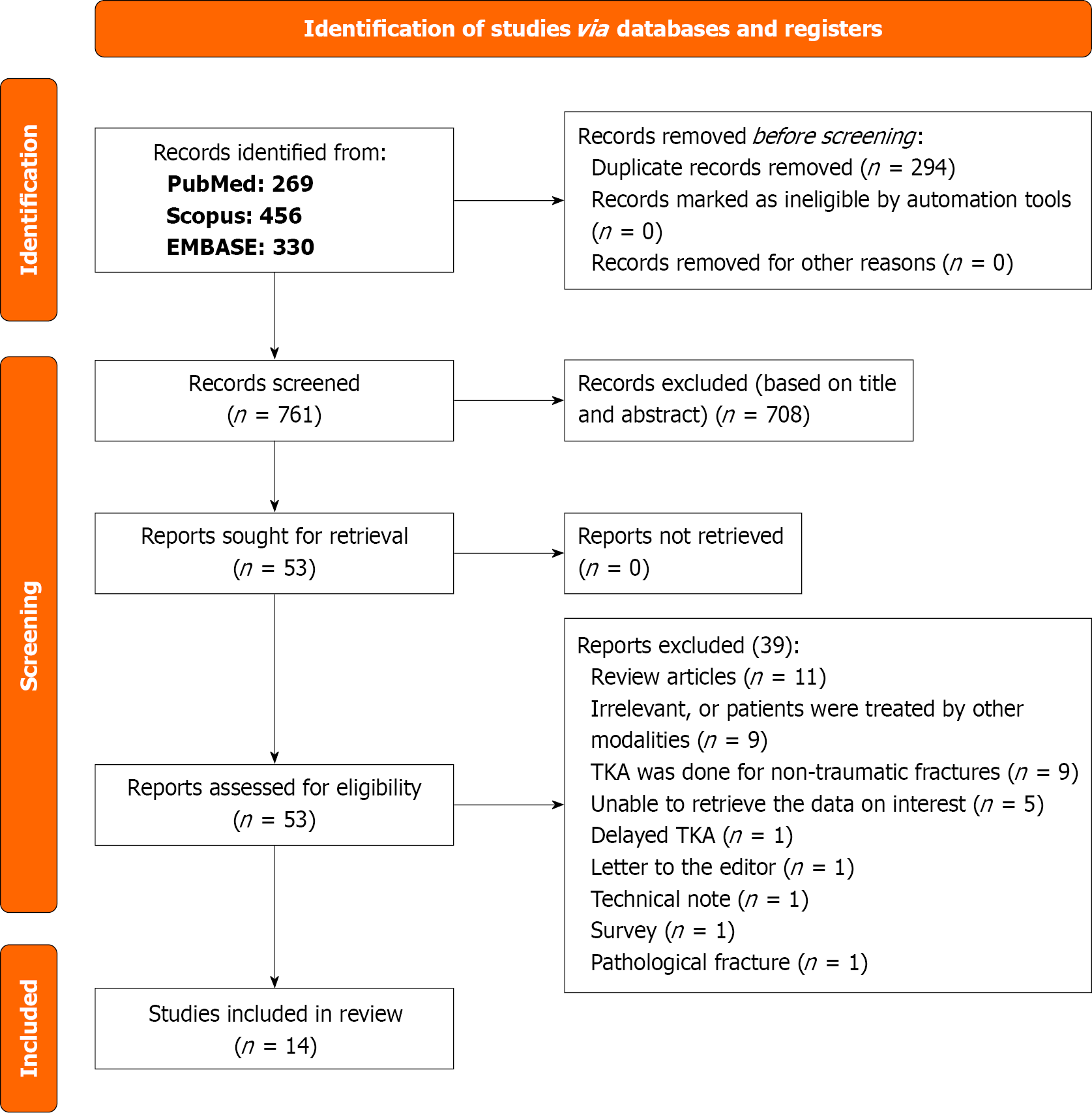
All the results (1055 articles) were downloaded to the EndNote 21 program. The first step was to identify and remove duplicates. Two authors (Althaqafi RMM and Altahir A) performed the screening and initial selection based on the predetermined criteria. Titles and abstracts of the retrieved eligible articles were screened, and their full text was reviewed for final inclusion. Any controversies were resolved through discussion among the authors, and the first author (Khalifa AA) was consulted as needed. The number of citations identified, included, and excluded at each screening step, along with the reasons for exclusion, is presented according to the PRISMA flowchart (Figure 1). The articles for final inclusion were divided equally among the authors; each extracted data from the assigned articles. After finishing data extraction, the authors exchanged their data, and each reviewed the data extracted by their colleague. If a controversy or missing data were present, a discussion between the authors was held to resolve any disagreement.
The following data were extracted: (1) Articles’ characteristics [author(s), year of publication, country of origin, type of study]; (2) Patient characteristics (age, sex, comorbidities, status of knee OA, and bone quality assessment); (3) Fracture characteristics (mode of trauma, fracture location, and classification); (4) Surgery details (timing, surgical approach, implant type, and if extras were used); and (5) Outcomes (functional, radiological, complications, and revision data). Any further data deemed suitable for reporting was extracted.
A unified risk of bias (ROB) evaluation was performed for all included studies using the National Institutes of Health Quality Assessment Tool items for observational case series, cohort, and cross-sectional studies (https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools), to maintain methodological consistency across observational designs. Each study was assessed across five core domains: Patient selection, clarity of intervention description, validity of outcome measurement, adequacy of follow-up, and statistical/reporting transparency. All ROB items were independently evaluated by two authors (Altahir A and Althaqafi RMM), and all discrepancies were resolved by discussion to reach consensus or by consulting a third author (Khalifa AA).
Due to the heterogeneity of study designs and outcome measures, a meta-analysis was not feasible; therefore, only a qualitative (descriptive) synthesis was conducted. However, we used the Grading of Recommendations Assessment, Development and Evaluation (GRADE) system to generate the evidence certainty level.
Initially, we had 20 full texts for inclusion; however, in five articles, we could not isolate data on aTKA for managing PTFs because they combined other treatment modalities or distal femoral fractures[3,8,24-26]. In contrast, one article reported on delayed TKA (eight months from the trauma)[27]. We finally included 14 studies for analysis[28-41]. Two studies were published from each of Iran[35,37] and Malaysia[29,41], while one was published from each of the following: Belgium, China, Egypt, Finland, France, Germany, Italy, the Netherlands, Singapore, and the United Kingdom. Study types were as follows: Nine case series, two case reports, two retrospective cohort studies (one compared aTKA vs ORIF, the other compared acute vs delayed TKA), and one cross-sectional study. The 14 articles included 174 patients [68 (39.1%) males and 106 (60.9%) females], with an average age of 71.3 years, ranging from 53 years to 96 years, and all had unilateral fractures.
Seven studies (111 patients)[28,35-40] reported on concomitant preinjury knee OA, with an incidence ranging from 22.7% to 100%. Proper evaluation of the preoperative bone density profile was reported in one study (11 patients)[35], where the patients had an absorptiometry scan evaluation at least 6 months before the injury as a part of their routine rheumatology follow-up, and their mean T-score was -3.8 ± 0.7, the remaining articles reported comments on bone density based on either patients’ history, radiographic or intraoperative data (Table 1).
| Ref. | Country | Study type | Total number of patients included in the study | Number of patients who had aTKA | Age | Gender | Comorbidities | Concomitant knee OA | Evaluating abnormal bone profile (author’s remarks) | Fracture details | |||
| Male | Female | Trauma mechanism | Fracture location | Classification | |||||||||
| Abdelbadie et al[28], 2020 | Egypt | Retrospective cohort study | 43 (22 aTKA vs 21 ORIF) | 22 | 67.1 (60-73) | 8 | 14 | 86.4% of the patients [diabetes (36.4%), HT (35.5%), IHD (27.3%), CLD (4.5%)] | 5 (22.7) | NA [9 (40.9) patients were on bisphosphonates] | 14 high energy (6 falls, 2 RTA, 6 MCA) | TPFs | Schatzker type II (7, 31.8%), Schatzker type III (8, 36.4%), Schatzker type IV (7, 31.8%) |
| Asikin et al[29], 2022 | Malaysia | Case report | 1 | 1 | 75 | 1 | 0 | NR | NR | NA | High energy (MCA) | TPFs | Schatzker type V |
| Boureau et al[30], 2015 | France | Case series | 21 (10 distal femur fractures and 11 proximal tibia fractures) | 11 | 79 (68-96) | 8 | 3 | NR (ASA III: 6, ASA II: 5) | NR | NA (all patients showed radiologic osteopenia) | NR | TPFs | 5 Schatzker II, 2 Schatzker IV, 3 Schatzker V and 1 Schatzker VI |
| Haufe et al[31], 2016 | Germany | Case series | 30 | 30 | 78.4 (59-93) | 13 | 17 | NR | NR | NA | NR | TPFs | AO/OTA: Type B (13), type C fracture (17); 6: 41B2, 5: 41B3, 5: 41C1, 7: 41C2, and 7: 41C3 |
| Hesmerg et al[32], 2024 | Netherlands | Retrospective cohort study | 68 (34 matched pairs: 12 aTKA vs 22 late TKA) | 12 | 69.0 (65.3-79.5) (median) | 1 | 11 | NR [ASA I/II: 8 (66.7%)] | NR | NA | Traffic accident 2 (16.7%), fall from height 4 (33.3%), blunt trauma 1 (8.3%); other 4 (33.3%), unknown 1 (8.3%) | TPFs | Schatzker II (2, 16.7%). Type III (3, 25.0%). Type IV (1, 8.3%). Type V (4, 33.3%). Type VI (2, 16.7%) |
| Huang et al[33], 2016 | China | Case series | 6 | 6 | 69.5 (58-78) | 3 | 3 | NR | NR | NA | All were high energy (traffic accidents and falls from height) | TPFs | 4 Schatzker V and 2 Schatzker VI |
| Kadakia et al[34], 2007 | United Kingdom | Case report | 1 | 1 | 85 | 0 | 1 | NR: Patient’s chest radiograph showed evidence of previous scarring | NR | NA (operative findings revealed that the bone was mushy and porotic) | Low energy (fell on the knee from standing height) | TPFs | Schatzker type IV |
| Mirzatolooei et al[35], 2021 | Iran | Case series | 11 | 11 | 54.3 ± 4.7 | 0 | 11 | RA [all patients were on anti-RA agents, especially corticosteroid (prednisolone) for at least 5 years (range: 5-8)] | 11 (100) | It was evaluated by DXA scan 6 months before the surgery; the mean T-score was -3.8 ± 0.7 | All were low energy | PTFs | NR |
| Sabatini et al[36], 2023 | Italy | Case series | 11 | 11 | 76 ± 6 (65-84) | 4 | 7 | NR | 11 (100) | NA | 8 low energy (simple fall), 3 high energy (car accident) | TPFs | AO/OTA: Type B (8), type C fracture (3); one (41B1), 5 (41B3), 2 (41B2), 1 (41C1), 2 (41C2) |
| Sarzaeem et al[37], 2017 | Iran | Case series | 30 | 30 | 67.6 ± 4.2 (61-78) | 19 | 11 | NR | 23 (76.7) | NA (7 had osteoporosis) | 14 high energy | TPFs + PTFs | AO/OTA: Type A (5), type B (22), type C fracture (3); 5 (41A), 22 (41 B), 3 (41 C) |
| Sivasubramanian et al[38], 2016 | Singapore | Case series | 3 | 3 | 70.4 (59.2-79.0) | 1 | 2 | NR | 3 (100) | NA (poor bone stock) | All high energy | TPFs | 2 Schatzker II and one Schatzker III |
| Tapper et al[39], 2020 | Finland | Case series | 22 | 22 | 74 ± 12 (53-88) | 6 | 16 | NR | 5 (22.7) | NA (deficient bone stock) | 13 low energy, 9 high energy | TPFs | 6 Schatzker II, 7 Schatzker III, 2 Schatzker IV, 5 Schatzker V, 2 Schatzker VI |
| Vermeire and Scheerlinck[40], 2010 | Belgium | Case series | 12 | 12 | 73 (58-81) | 3 | 9 | NR | 5 (41.7) | NA | 6 low energy, 6 high energy | TPFs | AO/OTA: Type B (9), type C fracture (3); one 41-B1, 8: 41-B3, 3: 41-C3 |
| Wui et al[41], 2020 | Malaysia | Cross-sectional study | 10 (6 distal femur, 2 proximal tibial, and 2 combined distal femur and proximal tibial fractures) | 2 | 64 (55-76) | 1 | 1 | NR | NR | NA (poor bone quality) | NR | TPFs | AO/OTA: Type C fracture (2); one 41C3.1, one 41C3.3 |
The mechanism of injury was reported in 11 studies (126 patients)[28,29,32-40]. Of these, 62 (49.2%) had high-energy trauma, while 64 (50.8%) had low-energy trauma. The fracture location was reported in all studies, either by the authors or defined from the fracture classification. Twelve studies included TPFs only[28-34,36,38-41], one study had both PTFs (5 knees) and TPFs (25 knees)[37], and one study had only PTFs (11 knees)[35], giving a total of 158 (90.8%) TPFs and 16 (9.2%) PTFs. The fracture classification was reported in 13 studies[28-34,36-41] (163 patients), of which eight (78 patients) used the Schatzker classification (22 type II, 19 type III, 13 type IV, 17 type V, and 7 type VI). In contrast, five (85 patients) used the Arbeitsgemeinschaft für Osteosynthesefragen/Orthopaedic Trauma Association classification (5 type A, 52 type B, and 28 type C) (Table 1).
The time from injury to surgery was reported in nine studies[28,30,32,33,36,38-41], with a mean of 11.6 days, ranging from 1 day to 107 days. It should be noted that, across eight studies[28,30,33,36,38-41], the range was 1 day to 21 days, while in one study by Hesmerg et al[32], the range was from 15 days to 107 days. The surgical approach was reported in nine studies (108 patients)[28-30,33,35,37-39,41], all of which used a medial parapatellar approach; none reported an extensile approach. The knee prosthesis used in the surgeries were reported in all studies and were distributed according to their constraint level as follows: 86 (49.4%) posterior stabilized, 43 (24.7%) constraint condylar knee, 39 (22.4%) rotating hinge knee, and six (3.5%) cruciate retaining.
Details of the extras required during surgery were reported in 11 studies (103 patients)[28-30,32-34,36,38-41]. A tibial stem was inserted in 100 (97.1%) TKAs, and 26 (25.2%) had femoral stems. For bone defect reconstruction, the following were used on the tibial side: 21 (20.4%) metal augment (wedges or blocks), 15 (14.6%) metaphyseal cones, 14 (13.6%) bone graft, and three (2.9%) bone cement. The status of concomitant ORIF was reported in nine studies (89 knees)[28-30,33,34,36,38-40], of which 18 (20.2%) knees had a concomitant ORIF (Table 2).
| Ref. | Time from injury to surgery (days) | Surgical approach | Type of prosthesis | Bone defect assessment | Use of extras | Concomitant ORIF (number of knees) |
| Abdelbadie et al[28], 2020 | 6.5 (1-21) | Medial parapatellar | 22 PS | 10 (45.5%) contained defect and 12 (54.5%) non contained defect | 22 (100%) cementless long tibial stem, 6 (27.3%) bone graft and 4 (18.2%) metal wedge | 6 (the fracture fragment was fixed by screws to act as structural bone graft) |
| Asikin et al[29], 2022 | NR | Medial parapatellar | 1 PS | NR | 1 cementless tibial stem | Yes |
| Boureau et al[30], 2015 | 3.9 (1-11) | Medial parapatellar | 10 RHK, one CCK | NR | 11 cemented tibial stems | none |
| Haufe et al[31], 2016 | NR | NR | 24 RHK and 6 PS (MB) | NR | NR | NR |
| Hesmerg et al[32], 2024 | 58 (15-107) | NR | 8 PS (6 MB), 2 CR, 2 RHK | NR | 4 (33.3%) femoral stem, 12 (100%) tibial stem | NR |
| Huang et al[33], 2016 | 4 (2-6) | Medial parapatellar | 3 PS femur and 3 CCK tibia | 5 knees [3 contained and 2 non-contained (mean defect size was 3.2 mm)] | 3 (100%) cemented tibial stem, bone defect was filled with polymethyl methacrylate or autologous bone | None |
| Kadakia et al[34], 2007 | NR | NR | 1 RHK | NR | Cemented stems in femur and tibia | None |
| Mirzatolooei et al[35], 2021 | NR | Medial parapatellar | 11 CCK | NR | NR | NR |
| Sabatini et al[36], 2023 | 5 ± 2 (2-9) | NR | 6 PS and 5 CCK | NR | 11 (100%) tantalum cones, wedges, cementless tibial stems | None |
| Sarzaeem et al[37], 2017 | NR | Medial prepatellar | 27 PS and 3 CCK | NR | NR | NR |
| Sivasubramanian et al[38], 2016 | 9 (6-12) | Medial parapatellar | 2 PS and 1 LCCK | Intraoperatively, significant subchondral bone loss | 3 (100%) tibial stems and tantalum cones- one (33.3%) femoral stem | 2 |
| Tapper et al[39], 2020 | 5.8 (1-16) | Medial parapatellar | 2 RHK, 16 CCK, and 4 CR | NR | 22 (100%) tibial stem, 19 (86.4%) femoral stem; 4 (18.2%) lateral or medial tibial augment, 1 (4.5%) tantalum cone | 2 |
| Vermeire and Scheerlinck[40], 2010 | Three days (range: 1-6), one patient was operated upon after 2 weeks of trauma | NR | 11 PS and 1 CCK | NR | 12 (100%) tibial stem (cemented in two), 5 (41.7%) graft impaction, 2 (16.7%) augmentation blocks, one (8.3%) femoral stem | 7 |
| Wui et al[41], 2020 | 6 days and 15 days | Medial parapatellar | 2 CCK | NR | 2 (100%) tibia stem | NR |
All the studies demonstrated a high risk of bias, except for the two cohort studies, which showed a moderate risk of bias. This was mainly due to retrospective design, non-consecutive patient inclusion, limited follow-up, and incomplete reporting of complications or long-term outcomes (Table 3).
| Ref. | Patient selection | Outcome measures | Intervention description | Follow-up adequacy | Statistical clarity | Overall ROB |
| Abdelbadie et al[28], 2020 | Moderate | Low | Low | Moderate | Moderate | Moderate |
| Asikin et al[29], 2022 | High | Moderate | Moderate | High | Moderate | High |
| Boureau et al[30], 2015 | High | Moderate | Low | High | Low | High |
| Haufe et al[31], 2016 | High | Moderate | Low | High | Moderate | High |
| Hesmerg et al[32], 2024 | Moderate | Low | Low | Moderate | Moderate | Moderate |
| Huang et al[33], 2016 | High | Low | Low | High | Low | High |
| Kadakia et al[34], 2007 | High | Moderate | Moderate | High | Low | High |
| Mirzatolooei et al[35], 2021 | High | Low | Low | Moderate | Moderate | High |
| Sabatini et al[36], 2023 | High | Low | Low | Moderate | Low | High |
| Sarzaeem et al[37], 2017 | High | Low | Low | High | Low | High |
| Sivasubramanian et al[38], 2016 | High | Moderate | Moderate | High | Low | High |
| Tapper et al[39], 2020 | High | Moderate | Low | Moderate | Moderate | High |
| Vermeire and Scheerlinck[40], 2010 | High | Moderate | Moderate | Moderate | Low | High |
| Wui et al[41], 2020 | High | Moderate | Moderate | High | Moderate | High |
Postoperative weight-bearing status was reported in ten studies (120 patients)[28,30,31,33,35,37-41]. In seven studies, the authors allowed full weight-bearing (FWB) whenever tolerated[28,30,33,38-41], unless there was a reason for non-weight bearing, such as a concomitant skeletal injury. Meanwhile, in the remaining studies[29,35,37], the authors allowed immediate partial weight bearing. The mean follow-up for reporting the outcomes was 28.5 months, ranging from 1.3 months to 170.4 months.
Functional: The functional outcomes, including knee range of motion (ROM), were reported across all studies using various assessment tools. The knee ROM was reported in 11 studies (121 patients)[28,29,33-41], with a mean maximum knee flexion of 110.3 degrees (range, 90-140). The most commonly used tool for functional assessment was the Knee Society Score (KSS), including both components (knee and function), which was reported in eight studies (129 patients)[28,30,31,35-37,40,41]. Based on the definition of Miralles-Muñoz et al[42], a KSS ≥ 90 was an excellent outcome, 77-89 good, 76-65 fair, and < 65 poor. For the KS-Function Score: ≥ 85 was an excellent outcome, 73-84 good, 72-56 fair, and < 56 poor. The results from the eight studies[28,30,31,35-37,40,41] showed that the KSS component had a mean of 85.8 points (good outcome), with a range of 50 to 100. Meanwhile, the KS-Function Score component had a mean of 70.3 points (fair outcome), ranging from -20 to 100.
Radiological: Radiological outcomes were reported in eight studies (91 patients)[28-30,34,36-38,40]. In five studies (59 patients)[28,30,36,38,40], the final mechanical alignment was documented, and all knees achieved a mean mechanical alignment within the neutral range of ± 3 degrees at the hip-to-knee-to-ankle angle, except for three knees, which showed valgus alignment. In six studies (66 patients)[29,30,34,36,37,40], the authors reported no signs of radiolucencies or implant loosening. Fracture union status was reported in only two studies (4 patients)[29,38].
Complications: Complication incidents were reported in all studies, which occurred in 29 knees, giving an incidence of 16.7%. The most commonly occurring was periprosthetic joint infection (PJI) in 7 (4.02%) knees, followed by deep venous thrombosis in 4 (2.3%) knees, and each of the following occurred in three (1.7%) knees: Femoral periprosthetic fracture, limb malalignment, postoperative stiffness, wound healing issues, and hematoma formation. While implant loosening, retained cement particles, and extension lag occurred in one knee each (0.6%).
Revision: Data on revision were reported in 12 studies (132 patients)[28-30,33-41], and three (2.3%) patients required revision, two had a complete revision, one of them for stiffness and the other for PJI[39], while the third patient had only a debridement, antibiotics, and implant retention procedure for PJI[36] (Table 4).
| Ref. | Follow up (months) | Weight-bearing status postoperatively | Outcomes | ||||
| Functional | ROM | Radiological | Complication | Revision | |||
| Abdelbadie et al[28], 2020 | 27.2 (24-32) | 20 FWB (two NWB due to concomitant fractures) | Preoperative vs postoperative KS: 50.5 (42-64) vs 83 (50-100), preoperative vs postoperative KS Function Score: 62 (50-65) vs 84 (60-100) | Preoperative vs postoperative knee flexion: 32.6 degrees (20-40) vs 115 degrees (100-140); preoperative vs postoperative extension lag: 10.4 degrees (5-20) vs 1.4 degrees (0-5) | All were corrected to within a mean of ± 3 degrees neutral mechanical axis | Total of 4 (18.2%); 2 (9.1%) valgus alignment, 1 (4.5%) superficial wound infection, 1 (4.5%) femoral PPF | None |
| Asikin et al[29], 2022 | 6 | PWB (walking frame training started three days postoperatively) | NR | Painless knee ROM of 0 degree to 90 degrees | Complete bone union with no sign of loosening | None | None |
| Boureau et al[30], 2015 | 31 (6-9) | FWB | KSS: 127, KS: 84, KS Function Score: 43, OKS: 35.7, preoperative vs postoperative Parker Score: 7.4 vs 5 | NR (the authors reported the ROM for the whole group and did not report the ROM of tibia fracture patients separately) | There were no cases of radiolucency through the follow up period-mean HKA angle was 177 degrees (171 degrees to 180 degrees) | Total of 2: 1 stiffness required MUA, and 1 deep infection managed by irrigation drainage and prolonged antibiotic therapy | None |
| Haufe et al[31], 2016 | 27 (12-48) | NR | Mean KS: 81.1 (94-54), mean KS Function Score: 74.5 (100 to -20), and mean WOMAC score: 78.6 (96.2-36.7) | NR | NR | Total of 7: 3 wound healing deficit, 1 intraoperative PPF, 1 PJI, 1 retained intraarticular cement, 1 loosening | NR |
| Hesmerg et al[32], 2024 | 34.8 (16.8-170.4) | NR | KOOS-PS score 73 (59-93); OKS 43 (30-47), EQ-5D-5 L index 0.87 (0.69-1); EQ-5D VAS 80 (71-94) | NR | NR | One patient had stiffness requiring MUA | NR |
| Huang et al[33], 2016 | 32.3 (25-41) | 5 FWB and 1 PWB | HSS score: 89.8 (85-94) | Knee flexion: 119.2 degrees (105 degrees to 130 degrees) | NR | None | None |
| Kadakia et al[34], 2007 | 6 | NR | NR | Painless knee ROM 0 degree to 100 degrees | No loosening | PJI | None |
| Mirzatolooei et al[35], 2021 | 24 | PWB | Preoperative vs postoperative Tegner Activity Scale: 2.2 ± 1.4 vs 4.3 ± 1.4, KS: 88.7 ± 5.4, KS Function Score: 59.4 ± 8.2, preoperative vs postoperative median HSS scale: 42 (16-58) vs 78 (72-91); preoperative vs postoperative pain severity: 65.2 ± 12.3 vs 35.5 ± 11.3 | Preoperative vs postoperative median ROM: 85 degrees (55 degrees to 98 degrees) vs 97 degrees (95 degrees to 110 degrees) | NR | 2 DVT | None |
| Sabatini et al[36], 2023 | 28 ± 14 (12-48) | NR | KS: 83 ± 16 (48 to 97), KS Function Score: 74 ± 15 (32 to 88); preoperative vs postoperative Parker’s Scale was 7.5 ± 1.4 (5-9) vs 5.6 ± 1.3 (3-8) (P < 0.05); FJS: 66 ± 14, (42 to 94) | Knee flexion was 116 degrees ± 7 degrees (110 degrees to 130 degrees), 10 patients had full knee extension, one patient had an extension lag of 10 degrees | No radiolucency, all had neutral alignment (HKA between ± 3 degrees); based on patellar indices, there were no cases of patella alta; only one patient had a CDI and BPI consistent with a patella baja (CDI = 0.54 and BPI = 0.56) | 1 PJI, 1 extension lag of 10 degrees, 1 femoral PPF, 1 DVT | One required DAIR to treat PJI |
| Sarzaeem et al[37], 2017 | 54 ± 13 (36-72) | PWB | KS: 90.7 ± 6.5 (67-97), KS Function Score: 69.6 ± 8.8 (41-85); preoperative vs postoperative Tegner Activity Scale: 2.5 ± 1.2 (1-5) vs 3.5 ± 1.3 (2-6); the mean VAS for satisfaction: 8.1 ± 1 (6-10) and VAS Pain Score: 1.5 ± 1.2 | Knee flexion range was significantly higher than the contralateral uninjured side: 106 degrees ± 13 degrees vs 120 degrees ± 8 degrees | No case of septic or aseptic loosening | None | None |
| Sivasubramanian et al[38], 2016 | 56 (18-82) | FWB | KSS: 88, no pain | Knee flexion: 122 degrees (105 degrees to 132 degrees); no fixed flexion deformity or hyperextension | Radiological fracture union at a mean of 3 months (2 months to 5 months); alignment of within 3 degrees of the mechanical axis was achieved in 2 patients (2.8 varus and 3.0 valgus) | 1 valgus alignment of 7.2 degrees | None |
| Tapper et al[39], 2020 | 19 ± 16 | FWB | KSS score: 160 ± 39; OKS 27 ± 11 | Knee flexion: 109 degrees ± 16 degrees; extension deficit in three patients | NR | 1 stiffness, 1 PJI | 2 |
| Vermeire and Scheerlinck[40], 2010 | 31 (1.3-81) | 7 FWB, 3 PWB, 2 NWB (due to due to concomitant fractures) | Median KS: 78 (50-100), median KS Function Score: 58 (0-100); five patients had no pain at all | Knee flexion: 115.9 degrees (95 degrees to 130 degrees); no patients had hyperextension | Nine patients had a normal knee mechanical alignment (± 3 degrees HKA) and two showed a discrete valgus alignment compared to the contralateral side. No signs of loosening | 3 developed a hematoma, 1 DVT, 1 PJI | None |
| Wui et al[41], 2020 | 22.3 ± 13.9 | FWB | KS: 97 and 88; KS Function Score: 80 and 90 | One patient (0 degree to 90 degrees) the other (0 degree to 130 degrees) | NR | None | None |
The GRADE analysis showed that all evaluated outcomes, including functional results (KSS), postoperative knee flexion, complication rates, revision rates, and radiological alignment, were supported by very low-certainty evidence, downgraded primarily for serious risk of bias, imprecision, and inconsistency (Table 5).
| Outcome | Number of studies | Study design | Risk of bias | Inconsistency | Indirectness | Imprecision | Certainty |
| Functional outcomes (KSS) | 12 | 10 case series + 2 cohorts | Serious | Not serious | Not serious | Serious | ⊕◯◯◯: Very low |
| Range of motion (knee flexion) | 12 | 10 case series + 2 cohorts | Serious | Not serious | Not serious | Serious | ⊕◯◯◯: Very low |
| Complications (overall) | 14 | 10 case series + 2 cohorts | Serious | Serious | Not serious | Serious | ⊕◯◯◯: Very low |
| Revision rate | 14 | 10 case series + 2 cohorts | Serious | Not serious | Not serious | Very serious | ⊕◯◯◯: Very low |
| Radiological alignment | 5 | All were case series | Serious | Serious | Not serious | Very serious | ⊕◯◯◯: Very low |
The current systematic review reported the results of 174 patients who had aTKA as their initial treatment for either PTFs or TPFs. Such a procedure was performed when pre-injury knee OA or severe osteopenia jeopardized the stability of the ORIF option. Various knee implants and extras were successfully used, and selection was primarily based on fracture classification and collateral ligament integrity. The aTKA resulted in acceptable functional outcomes, relatively lower complications, and revision rates.
Before discussing the results in more detail, it is mandatory to mention that these results should be interpreted cautiously, given the considerable ROB among the included studies and the overall quality of the evidence generated from those studies.
In the elderly population, some authors recommend ORIF for isolated medial or lateral TPFs without articular surface depression, which revealed acceptable outcomes[4,8,28]. In contrast, a clear indication for performing aTKA to manage PTFs or TPFs is debatable; however, patients with pre-existing knee OA or rheumatoid arthritis, severe osteoporosis, those who cannot follow the restricted western blot instructions, and those with complex fracture patterns are suitable candidates for aTKA[10,20,43].
A scoring system (Total Knee Replacement Indication Scoring System for knee fractures) was proposed by Quattrini et al[8] based on Arbeitsgemeinschaft für Osteosynthesefragen fracture classification after considering the patient age, pre-injury knee OA, medical comorbidities including diabetes, smoking, and malnutrition, and lastly, the Clinical Frailty Scale. Specific points were assigned to each item, and based on the total points, the patient had low, moderate, or high indications for aTKA if the score was 0-5, 5-8, or > 9, respectively.
Gupta et al[3] retrospectively evaluated 182 displaced TPFs in patients older than 60 years; 95.6% were initially treated with ORIF; however, within five years, 12% required secondary TKA. The authors reported that pre-injury knee OA and the severity of articular surface depression were independent risk factors for developing post-traumatic osteoarthritis and requiring TKA, and in the presence of such factors, aTKA should be considered. Interestingly, based on the patient’s pre-injury mobility and independence, Parratte et al[44] proposed that aTKA should be performed in patients with a Parker Mobility Score greater than six points.
Another crucial and controversial issue is how we define an aTKA and when such a surgery should be done after injury. Acute TKA for PTFs or TPFs is agreed upon as if it was the definitive surgery for these fractures to be differentiated from secondary or delayed TKA, which is performed after these fractures were treated, regardless of the type of initial management[21]. In the current review, two studies reported their view on this timing, where the surgery is considered aTKA, if it was performed within three weeks of the injury, according to Vermeire and Scheerlinck[40], while Hesmerg et al[32] extended such an interval to within four months after the fracture.
Furthermore, the timing till surgery is usually measured as the interval between the injury and aTKA; this interval varied in the current review as reported from nine studies[28,30,32,33,36,38-41]. The mean interval was 11.6 days, ranging from 1 day to 107 days; however, in eight studies[28,30,33,36,38-41], the range was from 1 day to 21 days, while in one study by Hesmerg et al[32] the range was from 15 days to 107 days. It is worth noting that the extended interval by Hesmerg et al[32] compared to other studies originated from the fact that the authors grouped patients who had TKA acutely after the injury and those who had TKA as the primary line of management within the first four months, this was clear when looking at the lower limit of the injury to surgery interval, which was 15 days, similar to other studies reporting the time interval to define aTKA.
Such a waiting period might be due to the patient’s medical or local soft-tissue conditions. Although none of the studies reported assessing the soft-tissue envelope or the reason for waiting such an interval, except for the study by Abdelbadie et al[28], which noted that the delay was to allow soft tissue to heal. However, it is well known from the trauma literature that waiting for some time to let the soft tissue heal and settle down is practiced by many surgeons[45].
Many authors suggested that the fundamentals of TKA revision surgery apply to performing an aTKA for managing PTFs, including surgical approaches, implant choice, and the need for extras (such as stems, augments, bone grafts, and so on). Selecting the best surgical strategy primarily depends on fracture extension, collateral ligament status, and the need for bone defect reconstruction[14,20,36,46].
Surgical approach: In the current review, the nine studies[28-30,33,35,37-39,41], that mentioned the surgical approach used the medial parapatellar approach, and none reported the need for an extensile approach. Parratte et al[46] suggested using an extensile approach, namely the extended sub-vastus approach, which is usually used in their revision TKA cases. In contrast, Tampere et al[14] reported that one approach has no advantage over the other, and surgeons should use their familiar approach.
Type of knee prosthesis: Some goals of performing aTKA for managing PTFs are to achieve a stable, pain-free, and mobile joint, allowing the patient to bear weight early and mobilize. These goals should be considered when selecting the proper knee prosthesis to use, especially the constraint level: Non-constraint (posterior stabilized and cruciate retaining), semi-constraint (constraint condylar knee type), and fully constraint (rotating hinge knee)[14,20,21,47]. Although some of the included studies reported that the knee prosthesis constraint level was determined based on collateral ligament status, none reported the exact selection criteria or whether this correlated with the fracture classification. Furthermore, the level of implant constraints varied across studies, with posterior stabilized prostheses used in nearly 50% of patients, which is the implant most commonly used during primary TKA. However, it is generally accepted that the fracture nature is closely related to the integrity of the collateral ligaments, particularly if the fracture directly affects one or both of their attachments. Moreover, rotating hinge knee prosthesis might be suitable for fractures with metaphyseal comminution in osteoporotic bone, marked laxity, or if there is a large bone defect[36,46].
Need for extras: The need for extras while performing aTKA was mainly to support the stability of the tibial implant or bone defect reconstruction. For this issue, Scott et al[48] reported the need to adopt the zonal fixation concept (originally described during revision TKA[49]), where obtaining tibial metaphyseal and diaphyseal fixation should be considered if epiphyseal fixation could not be achieved.
In the current review, of the 11 studies[28-30,32-34,36,38-41] reporting the use of extras (103 knees), 97% inserted tibial stems regardless of stem fixation method (cemented, cementless, or hybrid). Tibial stems offload the metaphyseal area until the fracture fully unites and the bone regains its strength, and surgeons may choose between cemented or cementless stems based on fracture extension and remaining bone stock; however, both techniques seem to work well[29,46,50]. Moreover, to improve metaphyseal area stability or reconstruct fracture-associated bone defects, various reconstruction strategies were used in the current review, namely metal augments (20.4%), metaphyseal cones (14.6%), bone grafts (13.6%), and bone cement (2.91%). The previously used options are well described in the TKA revision literature[49,51].
To ease dealing with the possible fracture-associated bone defects and deciding the needed fixation extent, Scott et al[48] adapted bone defect classification according to the Anderson Orthopaedic Research Institute to the Schatzker fracture classification. They suggested that Schatzker types I, II, III, and IV fractures are considered Anderson Orthopaedic Research Institute type 2A defects (single-plateau, uncontained defect). Therefore, these are amenable to management by acute metaphyseal fixation. In contrast, more severe injuries (Schatzker V and VI fractures) involving both tibial condyles could be considered as type 2B (both plateaus uncontained affecting) or type 3 (severe metaphyseal deficiency) defects, where diaphyseal fixation using stems should be added to the metaphyseal augmentation if aTKA was considered as the management option.
According to Huang et al[33], bone defects < 5 mm could be filled with bone cement, defects between 5 mm and 10 mm could be augmented with autogenous bone graft (usually obtained from the bony cuts), and for defects larger than 10 mm, metal wedges are required, accompanied by bone grafts. Furthermore, bone defect reconstruction should be protected by using a tibial stem. We found that Schatzker type II fractures were the most commonly reported among the included studies, consistent with previous reports[4,52]. However, this type of injury poses a challenge during reconstruction of the lateral plateau bone defect through the medial parapatellar approach (the predominant surgical approach in most studies). To address such a challenge, Scott et al[48] reported that asymmetric metaphyseal cones were used to reconstruct the defect, with promising results.
The need for a concomitant ORIF: The status of concomitant fracture osteosynthesis was reported in nine studies[28-30,33,34,36,38-40] in the current review, including 89 knees; however, it was only performed in 20% of the TKAs. The main benefit of performing a concomitant ORIF using plate and screws or screws alone is most evident when the fracture extends to the metaphyseal segment, where obtaining fracture stability and union at this area will lower the shearing forces and provide future stability of the tibial implant[21,29]. Moreover, osteosynthesis of these fractures could be an alternative to the use of costly extras such as metaphyseal cones[29]. Bohm et al[10] described a stepwise decision-making algorithm for managing osteoporotic fractures around the knee. They suggested optional supplementary fracture fixation for Schatzker type I-II-IV fractures based on the fragment size. Still, they highly recommend fracture osteosynthesis in combination with the tibial stem for bicondylar fractures or metaphyseal involvement (as in Schatzker types V and VI).
Functional: What guards against draining a robust estimate of the functional outcomes in the current review is the diversity of tools used for assessment; however, given the commonly used tool, the KSS, the functional outcomes are considered good and fair per the KS knee and function components, respectively[42,53]. Moreover, a mean knee flexion reaching about 110 degrees was reported in the current review, comparable to the range of motion obtained with primary TKA for knee OA[54].
In a systematic review by Makaram et al[13] comparing outcomes of aTKA vs delayed or secondary TKA (regardless of the initial management) after TPFs, the authors compared 121 in the acute group to 202 in the delayed group. Patients who had secondary TKA were significantly younger than those with aTKA (mean age: 61.3 years vs 72.2 years, P < 0.001). The functional outcomes were better in the aTKA group than in the delayed TKA group; however, the difference did not reach statistical significance [85.2% vs 79.9%, P = 0.359, 95% confidence interval (CI): 16.7 to 6.1]. The same conclusion was found in the study by Hesmerg et al[32]; however, the authors reported comparable functional and patient-reported outcomes in the aTKA patients compared with a matched cohort of elective TKA (for primary knee OA). At the same time, the results were worse when a group of delayed TKA patients was compared with the elective group.
Although we did not include comparisons of aTKA with other management modalities due to a lack of such comparisons within the included studies, Abdelbadie et al[28] compared the results of aTKA with ORIF; they reported similar hospital stay length but significantly better outcomes in the aTKA group as follows: Postoperative knee flexion, 115 degrees vs 95 degrees (P = 0.003), postoperative extension lag, 1.4 degrees vs 5.7 degrees (P = 0.005), postoperative KS-Knee Score 83 vs 70 (P = 0.00), and postoperative KS-Function Score 84 vs 72 (P = 0.00).
In contrast, Gupta et al[6] evaluated outcomes after operative (47 knees) and nonoperative (20 knees) management of TPFs in patients older than 60 years. After a mean follow up of 3.5 years, regardless of their initial management, they reported lower outcomes than a matched cohort of the same age and gender. The TPFs cohort showed significantly worse EQ-5D-3 Utility Scores, although their scores were higher when comparing their pre-injury status. They found a significant decline in the Oxford Knee Score compared with pre-injury levels. The decrease in patient-reported outcomes and functional outcomes could be attributed to delayed weight-bearing, loss of independence, and complications associated with operative management, which are not encountered with aTKA for managing TPFs in this age group.
Radiological: Regarding radiological outcomes, only five studies[28,30,36,38,40] reported postoperative alignment, with most patients achieving neutral mechanical alignment within the accepted range of 180 degrees ± 3 degrees hip to knee to ankle; in contrast, none reported individual component (tibial and femoral) alignment. Furthermore, five studies reported no signs of radiolucencies or implant loosening until the last follow up. These outcomes align with those obtained during primary TKA and after TPFs’ operative management[4,54].
In a study by Donovan et al[4] evaluating the outcomes after managing TPFs in 220 patients having a mean age of 74 years (range 60-100). Low-energy trauma was the leading cause of fractures (71%), and 61% of the fractures involved the lateral tibial plateau. Interestingly, 60% of the patients were treated nonoperatively. Of the operatively managed patients, only 3% underwent aTKA, and the majority (91%) were treated by ORIF. The authors reported that the knee joint alignment, measured as the anatomical femorotibial angle, had a mean of 173.0 degrees ± 5.0 degrees for all patients, and was 173.0 degrees ± 5.3 degrees vs 173.1 degrees ± 4.7 degrees for operatively vs nonoperatively managed patients, respectively, which is comparable to the results shown in the current review.
Complications and revisions: Complication incidence was reported in all of the studies, where the total incidence was about 17%, with PJI and deep venous thrombosis being the most frequently occurring complications. Hematoma formation, reported in three knees, may be attributed to the amount of soft-tissue injury associated with TPFs.
Data on the need for revision surgeries and their indications were reported in 12 studies[28-30,33-41], and only three patients required revision, giving an overall revision incidence of 2.3%: One for PJI, one for knee stiffness, and the last patient had PJI but was managed by debridement, antibiotics, and implant retention. One patient had aseptic loosening, but until the last follow up, the patient required no revision.
A systematic review by Pander et al[22], who evaluated the outcomes of secondary TKA for post-traumatic osteoarthritis after TPFs, included 162 patients from five studies, where 77% of those patients were initially treated operatively; they reported a complication incidence reaching up to 36%, where postoperative stiffness and PJI were the most commonly occurring. Furthermore, revision TKA surgery was required in 14 (8.6%) patients, six for PJI and three for aseptic loosening. It is worth mentioning that 12 (7.4%) patients required manipulation under anesthesia for persistent postoperative stiffness.
A recent study by Wagener et al[55], based on data from the German Arthroplasty Registry comparing the risk and causes of revision after TKA in more than ten thousand patients who had previous osteosynthesis to those who had osteotomies, although the authors included osteosynthesis of fractures of the distal femur and patella besides PTFs, they reported a higher risk of revision in this group (hazard ratio = 1.81, 95%CI: 1.52-2.15; P < 0.001), furthermore, the PJI risk was also higher (hazard ratio = 1.62, 95% confidence interval: 1.21-2.19).
Abdelbadie et al[28] reported fewer complications with aTKA than ORIF (4 vs 8); however, the difference did not reach statistical significance (P = 0.15). According to Makaram et al[13], the complication rate was significantly lower in aTKA patients. Furthermore, the need for reoperation or revision surgery was also lower with aTKA, 10% compared to 19% in the secondary TKA group (odds ratio = 2.14, 95%CI: 1.08 to 4.25, P = 0.26).
Some advantages of performing aTKA for TPFs, especially in older patients, should be mentioned: First is overcoming the challenging issue of osteoporotic bone, where ORIF might fail. During aTKA, this issue was mitigated by using extras such as augments and stems to improve implant stability, leading to early rehabilitation and ambulation; second is early mobilization and weight bearing, which are beneficial for function and help prevent complications associated with prolonged recumbency, such as DVT. In the current systematic review, nearly all patients were allowed to start weight bearing as tolerated early postoperatively, and the incidence of DVT was reported at an incidence of 2.3%. In contrast, Donovan et al[4] reported that weight-bearing was limited for the first six weeks in 90% of operatively managed patients; third, early mobilization will partially prevent loss of autonomy, especially in geriatric patients, which was proven in two studies included in the current systematic review[30,36], where the authors showed that Parker’s Mobility Scale decreased in the last follow up compared to the preoperative values; and lastly, aTKA avoids the reported higher complications and revision rate associated with ORIF and secondary TKA[9,22,32].
Although the data derived from the included studies seem encouraging, and some advantages are associated with selecting aTKA as the primary management option for selected patients and specific injury patterns, these data should be interpreted cautiously in light of the following limitations: First, the serious ROB across nearly all the included studies led to weak, less reliable evidence. This is mainly attributed to the nature of the study design, as most of the studies were either case series or reports lacking control or comparative groups, making it challenging to attribute the acceptable outcomes directly to the intervention (aTKA) rather than other confounding factors (e.g., patient selection, surgeon skill, post-operative protocol, and so on); second, the probable heterogeneity originating from variations in surgical technique, type of prosthesis used, the use of stems and other extras, and different techniques for bone defect reconstruction. This “performance bias” makes it difficult to pool results or identify a single best technique, rather than tailoring the decision after considering the patient and fracture factors; third, formulating clear indications for performing aTKA to treat PTFs rather than other management options was difficult, as most studies reported varied indications and perspectives based on the authors’ experience and clinical judgement; fourth, performing quantitative analysis and making robust recommendations based on the obtained results was not possible, which was also attributed to the study design and its relatively small sample sizes; fifth, few studies reported overall limb alignment postoperatively, and none reported on individual component alignment, especially on the tibial side, which is a crucial factor in predicting the risk of future failure or aseptic loosening[56]; sixth, we could not properly evaluate functional outcomes due to inconsistent reporting, particularly as different assessment scores were used; and last is the relatively short follow-up duration, which limits the ability to detect longer-term complications, revision rates, and implant longevity.
PTFs, either intra-articular or extra-articular, might pose a challenge to the treating surgeon, especially when occurring in older patients with concomitant knee OA, osteoporosis, and severe metaphyseal comminution. Performing aTKA as the primary management for such fractures is suitable after considering patient and fracture variables. Various levels of knee prosthesis constraint may be used depending on fracture type, collateral ligament integrity, and the extent of the bone defect. Furthermore, extras such as stems and augments are needed to improve initial implant stability and to reconstruct bone defects. The functional, complications, and revision outcomes are considered acceptable. However, while the included studies collectively suggest that aTKA may offer promising short-term outcomes for selected PTFs, the strength of the evidence remains limited and underscores the need for well-designed prospective studies with larger sample sizes and longer follow-up.
| 1. | Elsoe R, Larsen P, Nielsen NP, Swenne J, Rasmussen S, Ostgaard SE. Population-Based Epidemiology of Tibial Plateau Fractures. Orthopedics. 2015;38:e780-e786. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 105] [Cited by in RCA: 180] [Article Influence: 16.4] [Reference Citation Analysis (1)] |
| 2. | Sauhta R, Makkar D. Proximal Tibia Fractures in Osteoporosis. Indian J Orthop. 2025;59:326-345. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 3. | Gupta S, Sadczuk D, Riddoch FI, Oliver WM, Davidson E, White TO, Keating JF, Scott CEH. Pre-existing knee osteoarthritis and severe joint depression are associated with the need for total knee arthroplasty after tibial plateau fracture in patients aged over 60 years. Bone Joint J. 2024;106-B:28-37. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 4. | Donovan RL, Smith JRA, Yeomans D, Bennett F, Smallbones M, White P, Chesser TJS. Epidemiology and outcomes of tibial plateau fractures in adults aged 60 and over treated in the United Kingdom. Injury. 2022;53:2219-2225. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 21] [Article Influence: 5.3] [Reference Citation Analysis (1)] |
| 5. | Gálvez-Sirvent E, Ibarzábal-Gil A, Rodríguez-Merchán EC. Complications of the surgical treatment of fractures of the tibial plateau: prevalence, causes, and management. EFORT Open Rev. 2022;7:554-568. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 41] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 6. | Gupta S, Yapp LZ, Sadczuk D, MacDonald DJ, Clement ND, White TO, Keating JF, Scott CEH. Tibial plateau fractures in older adults are associated with a clinically significant deterioration in health-related quality of life. Bone Jt Open. 2023;4:273-282. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (1)] |
| 7. | Kim JK, Hwang KT, Soh HS, Shon OJ, Park KC. Comparison of tibial plateau fracture surgical outcomes between young and elderly patients: are outcomes really poorer in the elderly? Arch Orthop Trauma Surg. 2022;142:2419-2427. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 17] [Article Influence: 4.3] [Reference Citation Analysis (1)] |
| 8. | Quattrini F, Andriollo L, Ciatti C, Maniscalco P, Benazzo F, Rossi SMP. Fractures around the knee in elderly patients: Balancing fixation and arthroplasty approaches, a multicenter experience(). Injury. 2024;55 Suppl 4:111347. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 9. | Pinter Z, Jha AJ, McGee A, Paul K, Lee S, Dombrowsky A, Naranje S, Shah A. Outcomes of knee replacement in patients with posttraumatic arthritis due to previous tibial plateau fracture. Eur J Orthop Surg Traumatol. 2020;30:323-328. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 12] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 10. | Bohm ER, Tufescu TV, Marsh JP. The operative management of osteoporotic fractures of the knee: to fix or replace? J Bone Joint Surg Br. 2012;94:1160-1169. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 36] [Article Influence: 2.6] [Reference Citation Analysis (1)] |
| 11. | Wang Y, Wang Z, Dong Y, Zhao K, Zhu Y, Chen W, Zhang Y. Outcomes after ORIF are similar in young and elderly patients with tibial plateau fractures: A minimum 2-year follow-up study. J Orthop Sci. 2024;29:292-298. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 12. | Tapper V, Reito A, Pamilo K, Ylitalo A, Toom A, Paloneva J. Complications and secondary operations after non-operative and operative treatment of tibial plateau fractures: a population-based study of 562 patients with mean follow-up of 7 years. Arch Orthop Trauma Surg. 2024;144:269-280. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 13. | Makaram NS, Param A, Clement ND, Scott CEH. Primary Versus Secondary Total Knee Arthroplasty for Tibial Plateau Fractures in Patients Aged 55 or Over-A Systematic Review and Meta-Analysis. J Arthroplasty. 2024;39:559-567. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 13] [Article Influence: 6.5] [Reference Citation Analysis (1)] |
| 14. | Tampere T, Ollivier M, Jacquet C, Fabre-Aubrespy M, Parratte S. Knee arthroplasty for acute fractures around the knee. EFORT Open Rev. 2020;5:713-723. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 13] [Article Influence: 2.2] [Reference Citation Analysis (1)] |
| 15. | Ebied A, Zayda A, Marei S, Elsayed H. Medium term results of total knee arthroplasty as a primary treatment for knee fractures. SICOT J. 2018;4:6. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 14] [Article Influence: 1.8] [Reference Citation Analysis (1)] |
| 16. | Ali AM, El-Shafie M, Willett KM. Failure of fixation of tibial plateau fractures. J Orthop Trauma. 2002;16:323-329. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 146] [Cited by in RCA: 107] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 17. | Haslhofer DJ, Kraml N, Winkler PW, Gotterbarm T, Klasan A. Risk for total knee arthroplasty after tibial plateau fractures: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2023;31:5145-5153. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 32] [Article Influence: 10.7] [Reference Citation Analysis (1)] |
| 18. | Scott CE, Davidson E, MacDonald DJ, White TO, Keating JF. Total knee arthroplasty following tibial plateau fracture: a matched cohort study. Bone Joint J. 2015;97-B:532-538. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 83] [Article Influence: 7.5] [Reference Citation Analysis (1)] |
| 19. | Brockman BS, Maupin JJ, Thompson SF, Hollabaugh KM, Thakral R. Complication Rates in Total Knee Arthroplasty Performed for Osteoarthritis and Post-Traumatic Arthritis: A Comparison Study. J Arthroplasty. 2020;35:371-374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 39] [Article Influence: 6.5] [Reference Citation Analysis (1)] |
| 20. | Naylor B, Butler J, Bradham AA, Gresham N, Schwab JM, Garrett J. The Role of Immediate Arthroplasty in Elderly Tibial Plateau Fractures. Orthop Rev (Pavia). 2025;17:143563. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 21. | Stevenson I, McMillan TE, Baliga S, Schemitsch EH. Primary and Secondary Total Knee Arthroplasty for Tibial Plateau Fractures. J Am Acad Orthop Surg. 2018;26:386-395. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 30] [Article Influence: 3.8] [Reference Citation Analysis (1)] |
| 22. | Pander P, Fransen BL, Hagemans FJA, Keijser LCM. Functional outcome of total knee arthroplasty following tibial plateau fractures: a systematic review. Arch Orthop Trauma Surg. 2023;143:1265-1274. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 11] [Reference Citation Analysis (1)] |
| 23. | Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Syst Rev. 2021;10:89. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7414] [Cited by in RCA: 6034] [Article Influence: 1206.8] [Reference Citation Analysis (6)] |
| 24. | Malviya A, Reed MR, Partington PF. Acute primary total knee arthroplasty for peri-articular knee fractures in patients over 65 years of age. Injury. 2011;42:1368-1371. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 35] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 25. | Nau T, Pflegerl E, Erhart J, Vecsei V. Primary total knee arthroplasty for periarticular fractures. J Arthroplasty. 2003;18:968-971. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 35] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 26. | Shimizu T, Sawaguchi T, Sakagoshi D, Goshima K, Shigemoto K, Hatsuchi Y. Geriatric tibial plateau fractures: Clinical features and surgical outcomes. J Orthop Sci. 2016;21:68-73. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 26] [Article Influence: 2.6] [Reference Citation Analysis (1)] |
| 27. | McSorley M, Jabbal M, Walmsley P. The use of a metaphyseal sleeve total knee replacement as primary treatment for Schaztker VI tibial plateau fracture. J Surg Case Rep. 2022;2022:rjac561. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 28. | Abdelbadie A, El-Hennawy A, Sallam A. Primary Total knee Arthroplasty: A Viable Surgical Option for Complex Tibial Plateau Fractures in Elderly. J Knee Surg. 2020;33:496-503. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 14] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 29. | Asikin MZ, Hayyun MF, Yusof MF. A viable option for immediate mobilisation: Primary total knee replacement with supplementary osteosynthesis for acute complex tibial plateau fracture in elderly. J Orthop Trauma Rehabil. 2022;29:221049172210758. [DOI] [Full Text] |
| 30. | Boureau F, Benad K, Putman S, Dereudre G, Kern G, Chantelot C. Does primary total knee arthroplasty for acute knee joint fracture maintain autonomy in the elderly? A retrospective study of 21 cases. Orthop Traumatol Surg Res. 2015;101:947-951. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 28] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 31. | Haufe T, Förch S, Müller P, Plath J, Mayr E. The Role of a Primary Arthroplasty in the Treatment of Proximal Tibia Fractures in Orthogeriatric Patients. Biomed Res Int. 2016;2016:6047876. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 20] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 32. | Hesmerg MK, Benner JL, de Jong LD, Zuiderbaan HA, Somford MP, van der List JP, Keijser LCM; mProve Orthopaedics Research Group. Mid-term outcomes of acute and delayed total knee arthroplasty following tibial plateau fractures: A matched cohort study. Knee. 2024;50:33-40. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 33. | Huang JF, Shen JJ, Chen JJ, Tong PJ. Primary total knee arthroplasty for elderly complex tibial plateau fractures. Acta Orthop Traumatol Turc. 2016;50:702-705. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 28] [Cited by in RCA: 27] [Article Influence: 2.7] [Reference Citation Analysis (1)] |
| 34. | Kadakia AP, Williams R, Langkamer VG. Tuberculous infection in a total knee replacement performed for medial tibial plateau fracture: a case report. Acta Orthop Belg. 2007;73:661-664. [PubMed] |
| 35. | Mirzatolooei F, Tabrizi A, Safari MB, Shishavan SAMK. Acute Total Knee Replacement in Rheumatoid Arthritis Patients with Proximal Tibial Fractures: A Case Series. J Knee Surg. 2021;34:1587-1591. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (1)] |
| 36. | Sabatini L, Aprato A, Camazzola D, Bistolfi A, Capella M, Massè A. Primary total knee arthroplasty in tibial plateau fractures: Literature review and our institutional experience. Injury. 2023;54 Suppl 1:S15-S23. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 17] [Article Influence: 3.4] [Reference Citation Analysis (1)] |
| 37. | Sarzaeem MM, Omidian MM, Kazemian G, Manafi A. Acute Primary Total Knee Arthroplasty for Proximal Tibial Fractures in Elderly. Arch Bone Jt Surg. 2017;5:302-307. [PubMed] |
| 38. | Sivasubramanian H, Kini SG, Ang KY, Sathappan SS. Use of tantalum cones in primary arthroplasty of acute proximal tibial fractures. Acta Orthop Belg. 2016;82:593-598. [PubMed] |
| 39. | Tapper V, Toom A, Pesola M, Pamilo K, Paloneva J. Knee joint replacement as primary treatment for proximal tibial fractures: analysis of clinical results of twenty-two patients with mean follow-up of nineteen months. Int Orthop. 2020;44:85-93. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 13] [Article Influence: 1.9] [Reference Citation Analysis (1)] |
| 40. | Vermeire J, Scheerlinck T. Early primary total knee replacement for complex proximal tibia fractures in elderly and osteoarthritic patients. Acta Orthop Belg. 2010;76:785-793. [PubMed] |
| 41. | Wui NB, Ahmad Anuar MA, Abdul Wahid AM. Short-Term Outcome of Early Primary Total Knee Arthroplasty for Fractures Around the Knee in the Elderly Population: The Experience of a Secondary Healthcare Centre in Malaysia. Malays J Med Sci. 2020;27:64-71. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 42. | Miralles-Muñoz FA, Gonzalez-Parreño S, Martinez-Mendez D, Gonzalez-Navarro B, Ruiz-Lozano M, Lizaur-Utrilla A, Alonso-Montero C. A validated outcome categorization of the knee society score for total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2022;30:1266-1272. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 30] [Article Influence: 7.5] [Reference Citation Analysis (1)] |
| 43. | Rossi SMP, Andriollo L, Sangaletti R, Montagna A, Benazzo F. International, consensus-based, indications and treatment options for knee arthroplasty in acute fractures around the knee. Arch Orthop Trauma Surg. 2025;145:154. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 44. | Parratte S, Bonnevialle P, Pietu G, Saragaglia D, Cherrier B, Lafosse JM. Primary total knee arthroplasty in the management of epiphyseal fracture around the knee. Orthop Traumatol Surg Res. 2011;97:S87-S94. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 29] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 45. | Adams JDJ Jr, Loeffler MF. Soft Tissue Injury Considerations in the Treatment of Tibial Plateau Fractures. Orthop Clin North Am. 2020;51:471-479. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 17] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 46. | Parratte S, Ollivier M, Argenson JN. Primary total knee arthroplasty for acute fracture around the knee. Orthop Traumatol Surg Res. 2018;104:S71-S80. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 32] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 47. | Indelli PF, Giori N, Maloney W. Level of constraint in revision knee arthroplasty. Curr Rev Musculoskelet Med. 2015;8:390-397. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 23] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 48. | Scott CEH, Param A, Moran M, Makaram NS. Acute Total Knee Arthroplasty for Unicondylar Tibial Plateau Fracture Using Metaphyseal Cones. Arthroplast Today. 2023;23:101209. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 8] [Article Influence: 2.7] [Reference Citation Analysis (1)] |
| 49. | Morgan-Jones R, Oussedik SI, Graichen H, Haddad FS. Zonal fixation in revision total knee arthroplasty. Bone Joint J. 2015;97-B:147-149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 209] [Article Influence: 19.0] [Reference Citation Analysis (1)] |
| 50. | Darwich A, Jovanovic A, Dally FJ, Abd El Hai A, Baumgärtner T, Assaf E, Gravius S, Hetjens S, Bdeir M. Cemented versus Cementless Stem Fixation in Revision Total Knee Arthroplasty: A Systematic Review and Meta-Analysis. Antibiotics (Basel). 2023;12:1633. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 8] [Reference Citation Analysis (1)] |
| 51. | Khalifa AA, Said E, Refae H, Abdelaal AM. Knee Bony Defects Reconstruction in Revision Total Knee Arthroplasty for Aseptic Loosening. Ortho Res Online J. 2019;5:502-508. [DOI] [Full Text] |
| 52. | He QF, Sun H, Shu LY, Zhan Y, He CY, Zhu Y, Zhang BB, Luo CF. Tibial plateau fractures in elderly people: an institutional retrospective study. J Orthop Surg Res. 2018;13:276. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 25] [Article Influence: 3.1] [Reference Citation Analysis (1)] |
| 53. | Scuderi GR, Bourne RB, Noble PC, Benjamin JB, Lonner JH, Scott WN. The new Knee Society Knee Scoring System. Clin Orthop Relat Res. 2012;470:3-19. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 582] [Cited by in RCA: 544] [Article Influence: 38.9] [Reference Citation Analysis (1)] |
| 54. | Khalifa AA, Fayez M, Elkady H, Abdelaal AM, Elassal MA. The Outcome of Posterior-Stabilized, Rotating Platform Total Knee Arthroplasty at a Minimum Ten-Year Follow-Up, a Middle East Institution Experience. J Knee Surg. 2022;35:718-724. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 6] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 55. | Wagener N, Wu Y, Grimberg A, Hipfl C, Hardt S. Prior osteosynthesis-unlike osteotomy-raises revision risk after total knee arthroplasty, predominantly via periprosthetic infection. Knee Surg Sports Traumatol Arthrosc. 2025;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 56. | Silva JD, Nunes B, Duarte F, Raposo F, Valente L, Antunes A, Oliveira P, Sousa A. Effect of tibial alignment in early failure in total knee arthroplasties. Rev Chir Orthop Traumatol. 2016;102:S80. [DOI] [Full Text] |