Published online Mar 18, 2026. doi: 10.5312/wjo.v17.i3.113562
Revised: October 9, 2025
Accepted: December 19, 2025
Published online: March 18, 2026
Processing time: 200 Days and 1.6 Hours
Despite being common in clinical practice, posterior calcaneal spur fractures in insertional Achilles tendinopathy (IAT) remain poorly studied.
To investigate spur fractures in patients with IAT.
Patients with IAT who underwent surgery at our institution were retrospectively evaluated. Demographics and spur length were compared between patients with and without spur fractures. The diagnostic cutoff value of spur length for pre
This study included 227 feet (59 females, 168 males). The mean age was 53.9 years, and the mean body mass index was 27.3. Spur fractures were observed in 87 cases (38.3%), including 11 of 59 females (18%) and 76 of 168 males (45%). Spur length was significantly greater in patients with spur fractures than in those without fractures (12.3 vs 5.7 mm, P < 0.001), whereas height, weight, and body mass index were comparable. The optimal cutoff value for spur length in predicting fracture was 9 mm (specificity: 0.857; sensitivity: 0.816; area under the curve: 0.902).
Spur fractures were present in 38.3% of feet with IAT, occurring more commonly in males. Spur length was significantly associated with fracture, with a 9-mm cutoff predicting spur fractures. Given their nature as stress fractures caused by sustained traction forces from the Achilles tendon, spur fractures may warrant surgical intervention.
Core Tip: Spur fractures were frequently identified in patients with insertional Achilles tendinopathy, more commonly among men. Cases with spur fractures had a longer mean spur length. A spur length of 9.0 mm demonstrated high sensitivity and specificity for predicting spur fractures. Spur fractures may require surgical intervention due to their nature as stress fractures caused by sustained traction forces from the Achilles tendon on the spur.
- Citation: Nakajima K. Characterizing posterior calcaneal spur fractures in insertional Achilles tendinopathy: A case control study. World J Orthop 2026; 17(3): 113562
- URL: https://www.wjgnet.com/2218-5836/full/v17/i3/113562.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i3.113562
Insertional Achilles tendinopathy (IAT) is characterized by posterior heel pain and degeneration of both the Achilles tendon and the calcaneal spur at its insertion[1]. Calcaneal spurs are classified into posterior heel spurs and plantar heel spurs, which are associated with IAT and plantar fasciitis, respectively[2]. Although plantar heel spurs are well documented, posterior heel spurs remain relatively underexplored[3]. A histological study by Zwirner et al[2] demon
Among cases of Achilles tendinopathy, ossification fractures in non-IAT patients have been well documented; however, no studies have specifically examined spur fractures in IAT[5], despite their frequent occurrence in clinical practice. To address this gap, the present study investigated and characterized spur fractures in patients with IAT. We hypothesized that larger spurs would be more prone to fracture.
This retrospective case control study reviewed demographic data and computed tomography (CT) images of patients with IAT and compared demographics and spur length between feet with and without spur fracture. Patients with IAT who underwent surgery at our hospital from April 2017 to August 2025 were included, while patients with incomplete data were excluded. Both feet from patients with bilateral IAT were included in the analysis. Demographic variables collected included sex, age, height, weight, and body mass index (BMI).
All sagittal plane slices and three-dimensional CT images were analyzed to measure spur length in all cases using a 320-row, 0.5-mm slice CT scanner (Aquilion ONE Nature Edition, Canon Medical Systems, Tochigi, Japan). Three-dimensional images were reconstructed with the Advanced intelligent Clear-IQ Engine Body Sharp Mild kernel. A spur was classified as fractured if the adjacent edges of two fragments were aligned and separated by a gap of ≤ 2 mm.
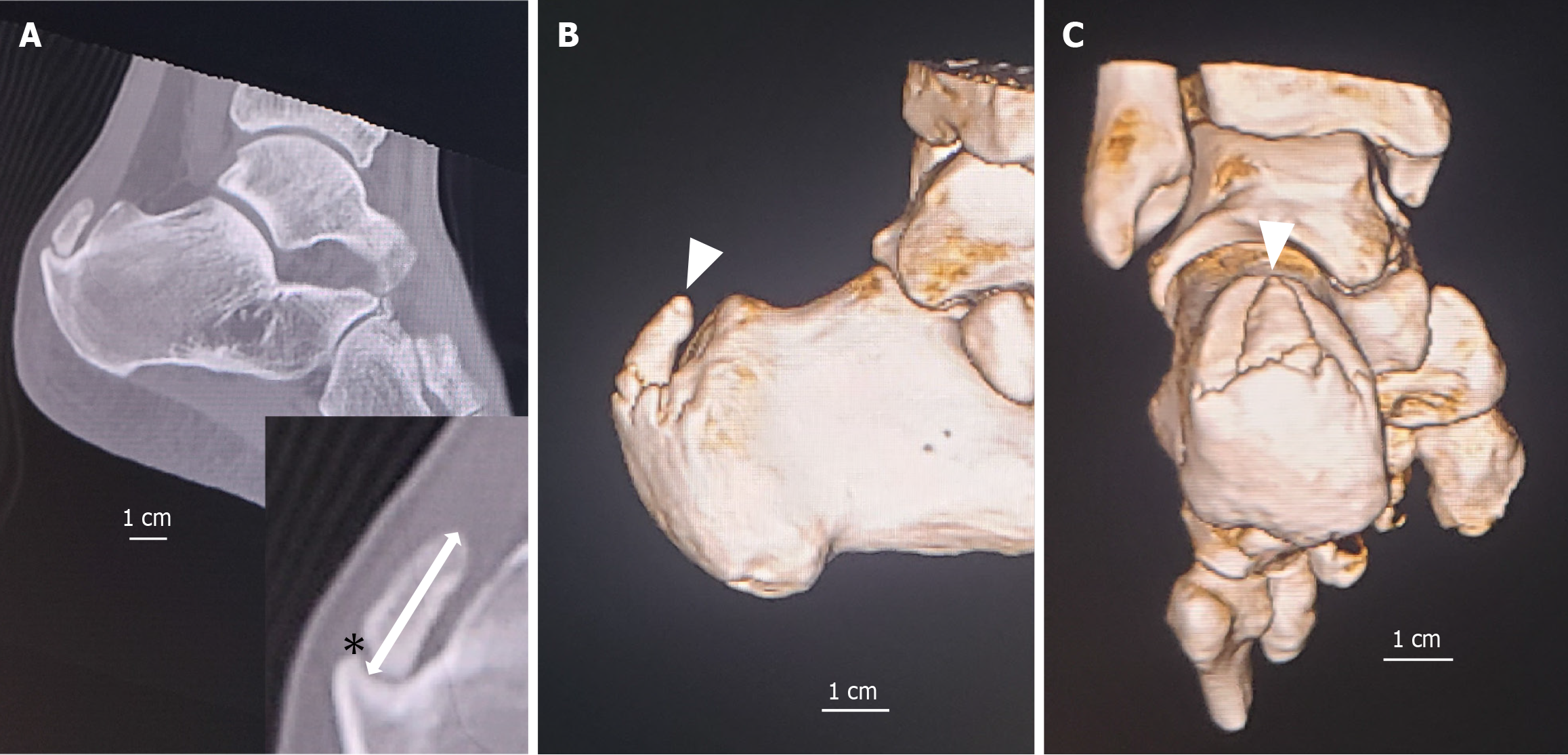
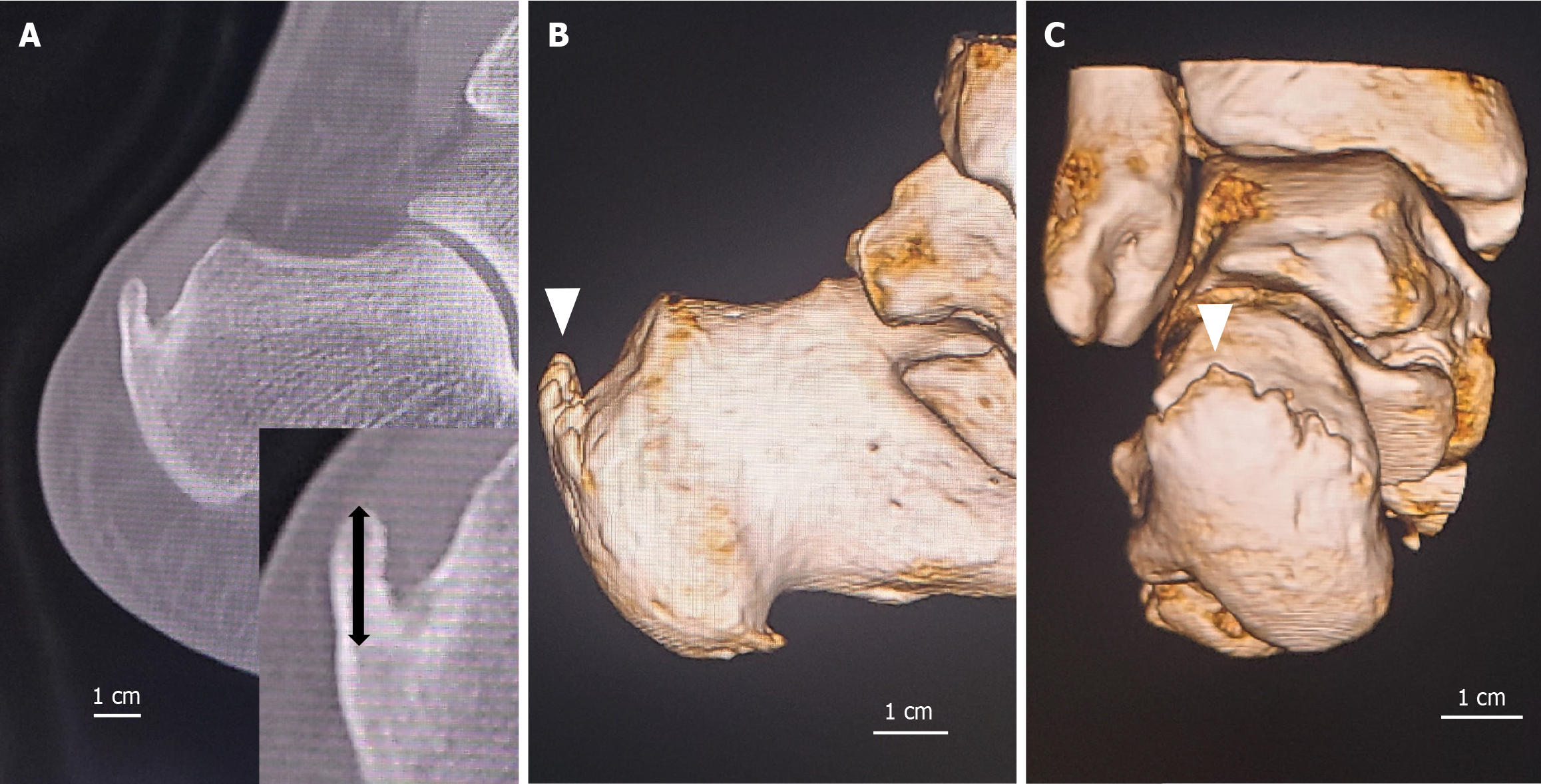
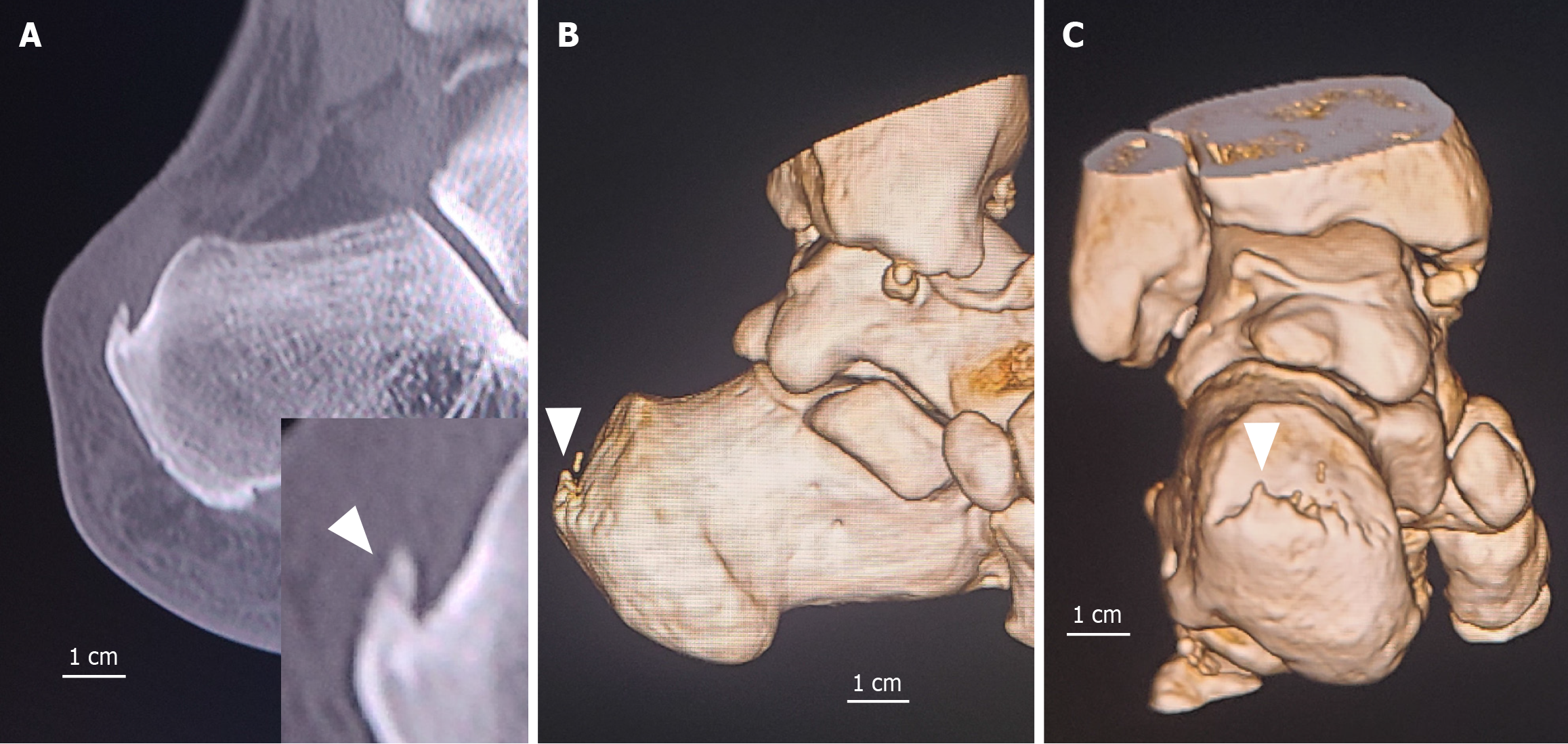
In nonfractured cases, spur length was defined as the distance from the base to the tip of the spur; the longest spur length observed on the sagittal plane was recorded (Figure 1). In fractured cases, spur length was calculated by subtracting the fracture gap from the total distance between the base and the tip of the spur; the length of the fractured spur was then recorded (Figure 2). If the presence of a fracture could not be clearly determined, the spur was classified as not fractured (Figure 3).
Patient demographics and spur length were compared between groups with and without spur fractures. Because a significant difference in the male-to-female ratio was observed, additional sex-stratified analyses were performed. A post hoc analysis was conducted to calculate the required sample size. The diagnostic cutoff value of spur length for predicting spur fracture was determined using receiver operating characteristic curve. The spur length that resulted in the highest sum of sensitivity and specificity was used as the cutoff value.
Categorical variables were analyzed with Fisher’s exact test, and continuous variables with the Mann-Whitney U test. Because these tests were performed 25 times, a Bonferroni correction was applied, setting statistical significance at P < 0.002 (0.05/25). Each foot was treated as an independent case. All statistical analyses were performed using EZR version 1.54 (Saitama Medical Center, Jichi Medical University, Saitama, Japan), a modified version of R Commander 4.0.3 (The R Foundation for Statistical Computing, Vienna, Austria)[6].
After excluding 10 feet with incomplete data, 227 feet (59 from females and 168 from males) were analyzed. Of these, 16 feet from females and 40 feet from males belonged to patients with bilateral IAT. The study cohort consisted entirely of Asian patients. The mean age was 53.9 years, and the mean BMI was 27.3. Spur fractures were identified in 87 cases (38.3%) (Table 1).
| Parameter | Subclass | n (%)/mean ± SD (median, range) |
| Sex | Female | 59 (26.0) |
| Male | 168 (74.0) | |
| Age (years) | 53.9 ± 12.0 (54, 26-87) | |
| Height (cm) | 168.1 ± 8.7 (169, 146-189) | |
| Weight (kg) | 77.1 ± 15.7 (75.9, 38.5-147.5) | |
| Body mass index | 27.3 ± 5.1 (26.0, 16.4-43.7) | |
| Side | Left | 107 |
| Right | 120 | |
| Spur fracture | Yes | 87 (38.3) |
| No | 140 (61.7) | |
| Spur length (mm) | 8.2 ± 4.8 (7, 1-24) |
The demographics and spur lengths of patients with and without spur fractures are summarized in Table 2. Spur length was significantly greater in the fracture group than in the nonfracture group (P < 0.001). Because sex distribution differed significantly between the two groups (P < 0.001), additional analyses stratified by sex were performed (Tables 3 and 4). Spur fractures were identified in 11 of 59 female (18%) and 76 of 168 males (45%). For both sexes, spur length was significantly greater in the fracture group than in the nonfracture group (P < 0.001). Comparisons between female and male patients with spur fractures are presented in Table 5. Spur fractures occurred significantly more often in males than in females (P < 0.001). Males were significantly taller than females, but weight, BMI, and spur length did not differ significantly by sex (Table 5).
| Parameter | With spur fracture | Without spur fracture | P value |
| Total number (female, male) | 87 (11, 76) | 140 (48, 92) | < 0.001c |
| Age (years) | 51.0 ± 10.5 (50, 32-87) | 55.7 ± 12.5 (55, 26-81) | 0.004 |
| Height (cm) | 171.5 ± 7.5 (172.2, 150-189.2) | 166.0 ± 8.7 (168, 146.5-185.3) | < 0.001c |
| Weight (kg) | 80.0 ± 14.5 (78.5, 39.5-147.5) | 75.3 ± 16.3 (72.2, 43.5-123.8) | 0.016 |
| Body mass index | 27.1 ± 4.2 (26.1, 16.4-41.2) | 27.4 ± 5.6 (25.8, 19.3-43.7) | 0.56 |
| Side (left, right) | 87 (39, 48) | 140 (68, 72) | 0.59 |
| Spur length (mm) | 12.3 ± 4.5 (11, 3-24) | 5.7± 3.0 (5.5, 1-19) | < 0.001c |
| Parameter | With spur fracture | Without spur fracture | P value |
| n | 11 (18.6) | 48 (81.4) | |
| Age (years) | 53.2 ± 11.3 (55, 35-69) | 56.4 ± 13.4 (54.5, 31-78) | 0.612 |
| Height (cm) | 161.1 ± 5.7 (161.9, 150-168) | 157.0 ± 6.8 (157, 146.5-175) | 0.051 |
| Weight (kg) | 73.3 ± 15.3 (76.1, 39.5-92.5) | 72.1 ± 20.4 (65.5, 43.5-110.8) | 0.532 |
| Body mass index | 28.3 ± 6.3 (27.9, 16.4-39.4) | 29.2 ± 7.0 (26.7, 19.6-43.7) | 0.984 |
| Side (left, right) | 11 (5, 6) | 48 (20, 28) | 1.00 |
| Spur length | 10.7 ± 4.0 (9, 6-17) | 4.8 ± 2.1 (5, 1-10) | < 0.001c |
| Parameter | With spur fracture | Without spur fracture | P value |
| n | 76 (45.2) | 92 (54.8) | |
| Age (years) | 50.8 ± 10.4 (49.5, 32-87) | 55.3 ± 12.1 (55.5, 26-81) | 0.003 |
| Height (cm) | 173.1 ± 6.4 (174, 156-189.2) | 171.0 ± 4.9 (170.8, 158-185.3) | 0.02 |
| Weight (kg) | 81.0 ± 14.2 (79.0, 58.0-147.5) | 77.2 ± 13.3 (74.8, 57.7-123.8) | 0.06 |
| Body mass index | 26.9 ± 3.6 (25.8, 19.9-41.2) | 26.5 ± 4.5 (25.4, 19.3-39.8) | 0.236 |
| Side (left, right) | 76 (34, 42) | 92 (48, 44) | 0.356 |
| Spur length | 12.5 ± 4.6 (11.5, 3-24) | 6.2 ± 3.3 (6, 1-19) | < 0.001c |
| Parameter | Female | Male | P value |
| n | 11 (18.6) | 76 (45.2) | |
| Age (years) | 53.2 ± 11.3 (55, 35-69) | 50.8 ± 10.4 (49.5, 32-87) | 0.467 |
| Height (cm) | 161.1 ± 5.7 (161.9, 150-168) | 173.1 ± 6.4 (174, 156-189.2) | < 0.001c |
| Weight (kg) | 73.3 ± 15.3 (76.1, 39.5-92.5) | 81.0 ± 14.2 (79.0, 58.0-147.5) | 0.106 |
| Body mass index | 28.3 ± 6.3 (27.9, 16.4-39.4) | 26.9 ± 3.6 (25.8, 19.9-41.2) | 0.311 |
| Side (left, right) | 11 (5, 6) | 76 (34, 42) | 1.00 |
| Spur length | 10.7 ± 4.0 (9, 6-17) | 12.5 ± 4.6 (11.5, 3-24) | 0.211 |
Post hoc power analyses were performed with a significance level of α = 0.05 (2-sided) and a statistical power of 80%. To detect differences in spur length between female patients with and without spur fractures, the required sample size was 8 per group (5.9 ± 4.0 mm). For male patients, the required sample size was 9 per group (6.3 ± 4.6 mm). These findings indicate that the analyses were conducted with a sufficient sample size to detect differences in spur length between fracture and nonfracture groups.
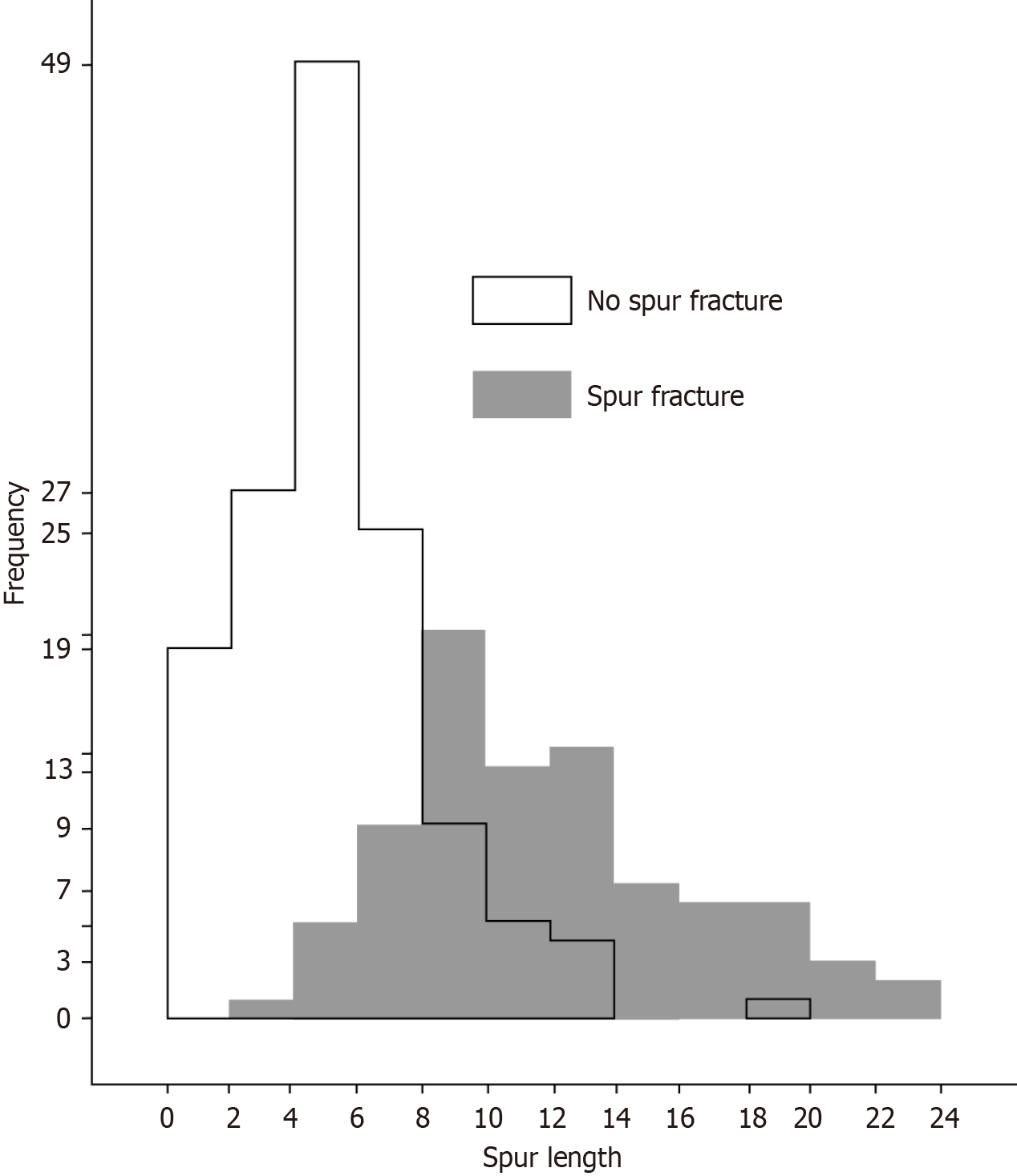
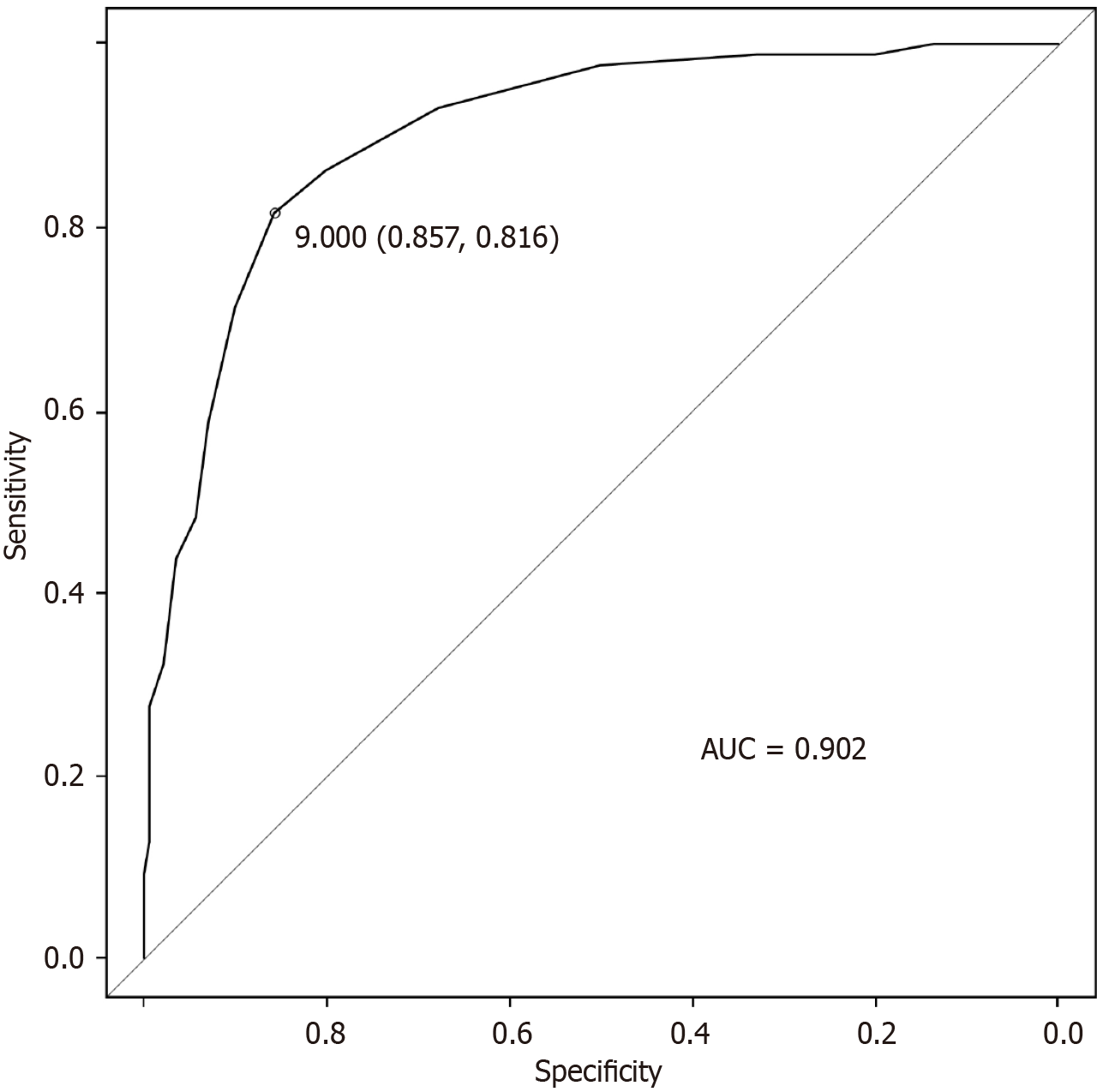
A histogram of patients with and without spur fractures is shown in Figure 4. The mean spur length was 5.7 mm in the nonfracture group and 12.3 mm in the fracture group (Table 2). The receiver operating characteristic curve used to determine the diagnostic cutoff value for predicting spur fractures is presented in Figure 5. The optimal cutoff was a spur length of 9 mm, yielding a specificity of 0.857 and a sensitivity of 0.816. The area under the curve was 0.902 (95% confidence interval: 0.862-0.942). This indicates an excellent discriminatory ability to spur length for predicting spur fractures.
This study evaluated spur fractures in patients with IAT who underwent surgery at our institution. Of 227 feet analyzed, spur fractures were identified in 38.3%. Patients with spur fractures had significantly longer spurs than those without fractures (12.3 mm vs 5.7 mm). Spur fractures were also more common in males than in females (45% vs 18%). A spur length of 9.0 mm showed high sensitivity and specificity for predicting spur fractures. That is, a spur length ≥ 9.0 mm may serve as a practical threshold to identify patients at higher risk of spur fracture.
Despite the higher prevalence of spur fractures in males than in females (45% vs 18%), the height, weight, and BMI were comparable between the fracture and nonfracture groups in the sex-stratified analysis (Tables 3 and 4). This disparity is likely due to greater tendon length and muscle strength in males, which may generate stronger traction forces on the Achilles tendon. Other factors, including bone mineral density, collagen structure, and activity level, may also contribute to this sex-based difference. Future studies examining these factors could elucidate the mechanisms underlying this disparity.
Spur fractures were observed in a substantial proportion of cases (38.3% overall). A systematic review by Agyekum and Ma[7] identified retrocalcaneal bursitis, Achilles tendinitis, Haglund’s deformity, and degeneration of the Achilles tendon insertion as common causes of posterior heel pain. Our findings suggest that spur fractures should also be considered among these causes. Furthermore, a spur length of 9 mm demonstrated excellent sensitivity and specificity for predicting spur fractures. Therefore, in patients with IAT who have a spur length of at least 9 mm, the possibility of spur fracture should be strongly considered. In such cases, CT imaging is recommended to differentiate spur fractures from other sources of pain.
We believe that IAT with spur fractures warrants surgical intervention. By nature, spur fractures can be considered as stress fractures, arising from sustained traction forces exerted by the Achilles tendon on the spur and the limited mechanical resistance of its irregular trabeculae. Consequently, spur fractures are unlikely to respond to conservative treatment. Nakajima compared radiographs of symptomatic and asymptomatic heels and found that spur width and length were greater in symptomatic heels[8]. Similarly, McCahon et al[9] reported that spur width, spur length, and spur-to-skin distance were significant predictors of failed conservative management in IAT. Pringels et al[10] demonstrated that low tendon compression rehabilitation is significantly more effective than high tendon compression rehabilitation for the conservative treatment of IAT. However, we recommend confirming spur characteristics before initiating conservative treatment. In the present study, all 227 cases were managed with fluoroscopic spur resection combined with endoscopic Achilles tendon debridement, a minimally invasive surgical technique that we developed, which yielded favorable outcomes. Accordingly, we recommend this procedure for its effectiveness and low invasiveness[1,11].
This study has several limitations. First, because the analysis was restricted to patients who underwent surgery, the reported prevalence of spur fractures may have differed if patients treated conservatively had been included. Second, cases with small spurs in which fracture status was difficult to determine were classified as nonfractured (Figure 3). If some of these cases actually represented fractures, the true prevalence of spur fractures may be higher. Third, the number of female patients with spur fractures was small (n = 11), limiting the strength of sex-specific conclusions. Fourth, we could not completely avoid referencing patient demographic information when measuring spur length and assessing fracture status. However, the sex-based discrepancy was not recognized until revealed through statistical analysis, suggesting that knowledge of patient sex did not influence the assessments. Fifth, both feet from patients with bilateral IAT were included in the analysis. Although this approach risks a loss of statistical independence, IAT frequently occurs bilaterally, and excluding such patients could introduce selection bias. Nonetheless, their inclusion may still have influenced the results[12]. Finally, as this study was conducted at a single local hospital and all enrolled patients were Asian, the findings may not be generalizable to other populations.
Among 227 feet, spur fractures were identified in 38.3%, occurring more frequently in males. Patients with spur fractures had significantly longer spurs than those without fractures (12.3 mm vs 5.7 mm). A spur length of 9.0 mm demonstrated high sensitivity and specificity for predicting spur fractures. Given their nature as stress fractures caused by sustained traction forces from the Achilles tendon, spur fractures may warrant surgical intervention.
The author would like to thank Shigeaki Ohtsuki, PhD, the president of Japan Institute of Statistical Technology (Tokyo, Japan) for checking the statistical analyses.
| 1. | Nakajima K. Fluoroscopic and Endoscopic Calcaneal Exostosis Resection and Achilles Tendon Debridement for Insertional Achilles Tendinopathy Results in Good Outcomes, Early Return to Sports Activities, and Few Wound Complications. Arthrosc Sports Med Rehabil. 2022;4:e1385-e1395. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 9] [Reference Citation Analysis (0)] |
| 2. | Zwirner J, Singh A, Templer F, Ondruschka B, Hammer N. Why heel spurs are traction spurs after all. Sci Rep. 2021;11:13291. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 3. | Velagala VR, Velagala NR, Kumar T, Singh A, Mehendale AM. Calcaneal Spurs: A Potentially Debilitating Disorder. Cureus. 2022;14:e28497. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 4. | Chimenti RL, Bucklin M, Kelly M, Ketz J, Flemister AS, Richards MS, Buckley MR. Insertional achilles tendinopathy associated with altered transverse compressive and axial tensile strain during ankle dorsiflexion. J Orthop Res. 2017;35:910-915. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 38] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 5. | Sullivan D, Pabich A, Enslow R, Roe A, Borchert D, Barr K, Cook B, Brooks A. Extensive Ossification of the Achilles Tendon with and without Acute Fracture: A Scoping Review. J Clin Med. 2021;10:3480. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 6. | Kanda Y. Investigation of the freely available easy-to-use software 'EZR' for medical statistics. Bone Marrow Transplant. 2013;48:452-458. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16540] [Cited by in RCA: 14863] [Article Influence: 1143.3] [Reference Citation Analysis (5)] |
| 7. | Agyekum EK, Ma K. Heel pain: A systematic review. Chin J Traumatol. 2015;18:164-169. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 38] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 8. | Nakajima K. Insertional Achilles tendinopathy: A radiographic cross-sectional comparison between symptomatic and asymptomatic heel of 71 patients. Eur J Radiol Open. 2024;12:100568. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 9. | McCahon JAS, Kohring A, Schultz MJ, Massaglia J, Patrizio HA, Parekh SG, Pedowitz DI, Daniel JN. Retrocalcaneal Enthesophytes and Radiographic Predictors of Failing Nonoperative Management in Insertional Achilles Tendinopathy: A Retrospective Cohort Study. Foot Ankle Spec. 2025;19386400251331642. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 10. | Pringels L, Capelleman R, Van den Abeele A, Burssens A, Planckaert G, Wezenbeek E, Vanden Bossche L. Effectiveness of reducing tendon compression in the rehabilitation of insertional Achilles tendinopathy: a randomised clinical trial. Br J Sports Med. 2025;59:640-650. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 11. | Nakajima K. Fluoroscopic and Endoscopic Calcaneal Exostosis Resection and Achilles Tendon Debridement for Insertional Achilles Tendinopathy: Surgical Techniques. Arthrosc Tech. 2023;12:e855-e860. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |