Published online Nov 28, 2017. doi: 10.4329/wjr.v9.i11.405
Peer-review started: January 7, 2017
First decision: February 17, 2017
Revised: May 25, 2017
Accepted: June 12, 2017
Article in press: June 13, 2017
Published online: November 28, 2017
Processing time: 323 Days and 13.9 Hours
To comparatively evaluate Seldinger and Trocar techniques in the percutaneous treatment of hydatid disease.
Trocar and Seldinger techniques were used for 49 and 56 cysts, respectively, among 106 hydatid cysts in 88 patients. The number of males and females were 22 and 66, respectively with a mean age of 44.9 years (range, 15-87). Follow-up studies included cyst diameter, cyst contents, and morphological changes in the cyst wall, local recurrence, and secondary invasion, using ultrasound, computerized tomography and chest X-rays.
The positive criteria of healing were a decrease in cyst diameter, progressive solidification of the cyst contents, and disappearance of the cyst. Local recurrence was defined as an increase in the cyst diameter and contents, and appearance of daughter cysts in the primary cavity, while secondary dissemination was defined as the appearance of new cysts outside the treated cyst. Mean duration of follow-up was 19.23 mo (range, 18-26 mo). Follow-up results demonstrated that no significant differences were present between the Trocar and Seldinger techniques in the percentage of decrease in the cyst volume, rate of early complications, local recurrence and secondary dissemination (P = 0.384, 0.069, 0.215 and 0.533, respectively).
There are no differences between the Seldinger and Trocar techniques that gain entry to the cyst cavity in terms of the efficacy of the treatment and the rates of early and late complications.
Core tip: Although various methods have been developed as interventional procedures, there is no knowledge in the literature on which technique should be used when entering the cyst hydatid cavity. İn this study, no differences have been found between the Seldinger and Trocar techniques that gain entry to the cyst hydatid cavity in terms of the efficacy of the treatment and the rates of early and late complications. Although trocar technique is a practical method that is easier and more economical to apply compared with the drainage procedure conducted using Seldinger technique, it should not be considered in post-surgical and elderly patients.
- Citation: Turan HG, Özdemir M, Acu R, Küçükay F, Özdemir FAE, Hekimoğlu B, Yıldırım UM. Comparison of seldinger and trocar techniques in the percutaneous treatment of hydatid cysts. World J Radiol 2017; 9(11): 405-412
- URL: https://www.wjgnet.com/1949-8470/full/v9/i11/405.htm
- DOI: https://dx.doi.org/10.4329/wjr.v9.i11.405
Core tip: Although various methods have been developed as interventional procedures, there is no knowledge in the literature on which technique should be used when entering the cyst hydatid cavity. İn this study, no differences have been found between the Seldinger and Trocar techniques that gain entry to the cyst hydatid cavity in terms of the efficacy of the treatment and the rates of early and late complications. Although trocar technique is a practical method that is easier and more economical to apply compared with the drainage procedure conducted using Seldinger technique, it should not be considered in post-surgical and elderly patients.
Although surgery is a long-standing conventional treatment for the hydatid cysts, non-surgical alternative options have been used instead due to its remarkable rate of complications and the risk of recurrence[1,2]. Drugs containing benzimidazole constitute an alternative treatment, but the success rate is low and are not curative when used alone[3,4]. Endoscopic treatment is limited to hydatid cysts with biliary tract invasion[5].
Development in interventional radiology and the successful application of percutaneous methods for other intra-abdominal lesions resulted in the percutaneous approach being used for the treatment of cystic echinococcosis, and studies over the past 30 years have proved that these lesions could be successfully treated using the percutaneous approach[6-18].
Although various methods have been developed as interventional procedures, there is no knowledge in the literature on which technique should be used when entering the cyst cavity. The aim of this study is to compare two different techniques for percutaneous entry and to evaluate their efficacy.
Eighty-eight patients with hydatid cysts treated between January 2009 and February 2012, were retrospectively evaluated. One hundred and six hydatid cysts in these patients were treated using the percutaneous approach. The patients were followed up until February 2013. The mean duration of follow-up was 19.23 mo (range,18-26). The number of males and females were 22 and 66, respectively, with a mean age of 44.9 years (range, 15-87). Hydatid cysts were classified according to the criteria of Gharbi et al[19]. Type 1 and type 2 cysts were included in the study, while type 3 cysts were included only in cases where daughter cysts constituted a small part of the cyst. Type 4 and 5 cysts were excluded from the study. Also, three cysts that were initially diagnosed as hydatid cyst but were later detected to be non-parasitic cysts, were excluded from the study. Among these cysts, 99 had the appearance of type 1 cyst, four were type 2, and three were type 3 cysts. And 104 and two cases were located in the liver and the peritoneal cavity next to the liver, respectively. The volume of the cysts varied between 22.5 and 6840 mL (mean volume, 504.4 mL).
Oral albendazole at a dose of 10 mg/kg per day was administered to the patients for a week prior to the procedure in order to prevent secondary dissemination. Albendazole treatment was continued for prophylaxis for two further weeks following the procedure[9,20]. Catheter placement was performed using two different techniques: the Seldinger technique and the Trocar technique. An 18-22 G (gauge) Chiba needle, 6-10 F percutaneous drainage catheter or 5.7-8 F trocar tip (one-step) drainage catheter was used. The Seldinger technique was used in 56 cysts (53%) and the Trocar technique was used in 50 cysts (47%).
This is a two-step procedure. Standard wires and guide wires were used for drainage. The cyst was approached primarily through an intervention needle. Subsequently, a guide wire was sent through this needle and the needle was withdrawn. Thus, the guide wire could be located in the area of intervention. With dilators of various diameters sent through this guide wire, a hole was created that would permit the passage of the catheter through both the skin and the region of drainage. Finally, the drainage catheter was placed into the target area over the same guide wire, and the guide wire was withdrawn.
This is a single step procedure and a standard trocar tip drainage catheter is composed of a sheath needle and a catheter coaxial system. A catheter and a straightening cannula of the same size were placed in the catheter and a needle 2-3 mm longer than the catheter was placed one in the other. Through this system, a direct puncture was made and it was forwarded to the field of drainage. Subsequently, the cannula and needle was withdrawn with the catheter remaining inside.
Following the first puncture, the cyst fluid was sent for cytological examination. Mobile scolexes in the cyst, seen under direct microscopy, were accepted as evidence of viability. Cysts without presence of evidence of viability, such as that of laminar membrane fragments and scolex hooks in cytological exam-ination and separation of the endocyst in radiological evaluation, were excluded from the study.
We applied Puncture Aspiration Injection Reaspiration (PAIR) in cysts with a diameter of less than 6 cm and catheterization method in larger cysts[21-31]. Sixty-two cysts (58%) in 88 patients were treated using the PAIR technique, while the catheterization technique was used in the remaining 44 (42%) cysts[22].
Follow-up studies included the cyst diameter and morphological changes in the cyst wall, local recurrence and secondary dissemination. Follow-up with US was performed at the 1, 3, 6, 12, 18 and 24 mo after the procedure. Annual whole abdominal CT and chest X-ray examinations were also performed. Positive criteria of healing were accepted to be a decrease in cyst diameter, progressive solidification of the cyst contents and disappearance of the cyst. Local recurrence was defined as increased cyst diameter and contents, and the appearance of daughter cysts in the primary cavity, while secondary dissemination was defined as the appearance of new cysts outside the treated cyst.
SPSS 14.0 statistics software package program (SPSS Inc, Chicago, IL, United States) was used for statistical analysis. The analysis of difference in volume between Trocar and Seldinger methods was performed using Mann-Whitney U test. Differences between the two techniques in terms of the rates of complication, local recurrence and secondary dissemination were analyzed using the χ2 test. P < 0.05 was accepted as statistically significant.
Separation of the endocyst from the pericyst was observed in 104 out of 106 cysts following injection of the sclerosing agent. The cyst was drained without observation of membrane separation in one case, due to severe abdominal pain subsequent to hypertonic saline injection. In another patient, the procedure was terminated due to the development of anaphylaxis before the cyst contents could be aspirated, following catheter insertion.
Daughter cysts were ruptured following hypertonic saline injection in two type 3 cysts including daughter cysts among the three type 3 cysts in the total series and they were ruptured with the manipulation of the catheter/guide wire in one of the type 3 cysts. Cytological examination confirmed the diagnosis of hydatid cyst in 106 cysts, while viability was detected in 98 cysts.
The Trocar technique was used in 50 cysts (47%) for entry to the cavity, while the Seldinger technique was used in 56 cysts (53%). Sclerotherapy was used in 98 cysts. Sclerotherapy was not performed in eight cysts, although they were catheterized due to contraindications of biliary fistula (n = 4), intra-abdominal extravasation (n = 2), anaphylaxis (n = 1), and absence of cellular elements in histopathological examination (n = 1). Mean duration of catheterization in 62 patients was 2.43 (range, 1- 45) d.
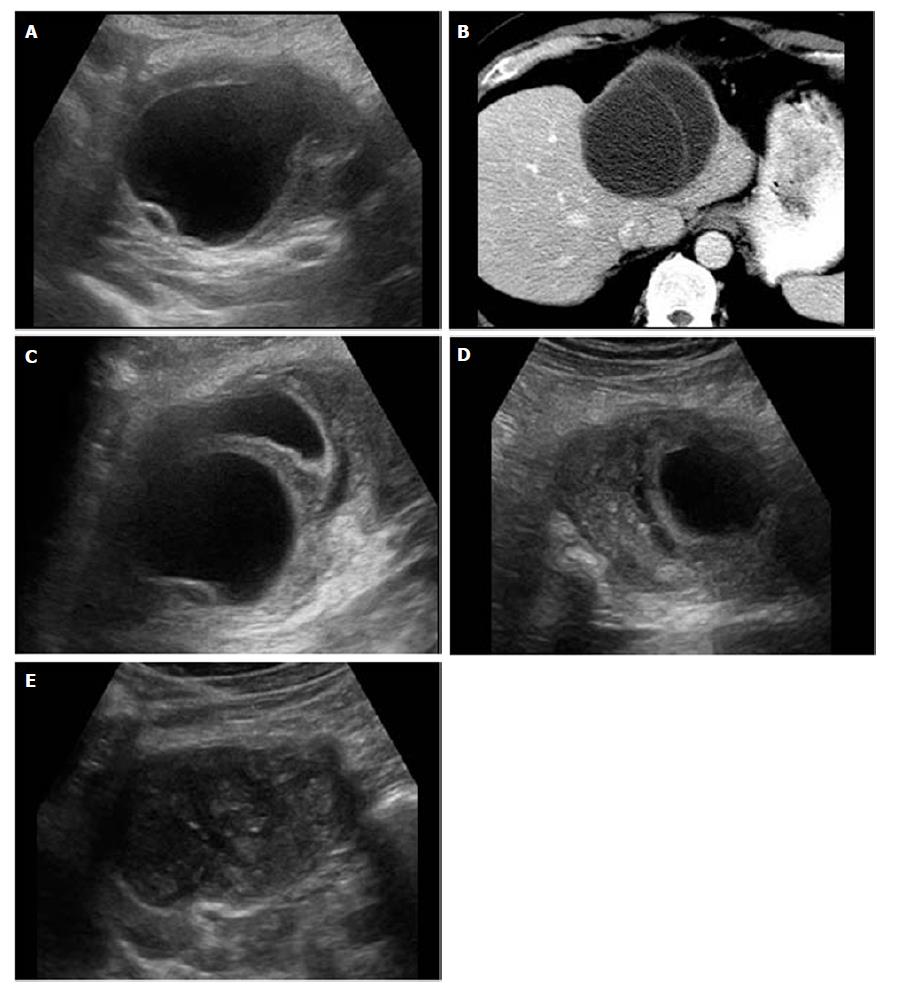
The mean duration of the follow-up of the 106 hydatid cysts in 88 patients was 19.23 mo (range, 18-26). Floating membranes were observed in the cyst fluid during the follow-up US examinations 12 mo after the percutaneous treatment, while none of the cysts had a pure anechoic image, which included dense internal echoes. At 12-14 mo follow-up, the cavity was seen to have collapsed, the cyst wall had thickened, and the cyst fluid was indiscernible. Finally, at the previous cyst, solid pseudotumors developed in many cases, which was seen to be iso- or hyperechoic with the liver parenchyma (Figure 1). No statistically significant difference was found in the cyst volume (P = 0.384) between the Trocar and Seldinger techniques (Table 1).
| Method | n | Mean rank | Lower and upper- median | Mann-Whitney U | P value | Difference |
| Trocar | 50 | 50.23 | -165.00 and 97.00 | |||
| 61 | ||||||
| 1236.5 | 0.384 | None | ||||
| Seldinger | 56 | 55.42 | -29.00 and 100.00 | |||
| 70.5 |
Thirteen early complications developed in a total of 12 patients. The early complications were anaphylaxis in one patient, biliary fistula in four, minor reaction in one (chills and tachycardia), abdominal pain in three, fever without signs of infection, entry site infection in one patient, infection in the cyst cavity (abscess) in one patient, in whom a biliary fistula also developed, and intra-abdominal extravasation in one patient. Late complications developed in three patients that were secondary dissemination in one and local recurrence in two patients.
During entry to the cavity with the Seldinger technique, following catheter placement and before aspiration of the cyst contents, anaphylaxis developed in a 17-year-old male patient with a type 1 cyst. The patient’s vital signs returned to normal following immediate treatment. With the Seldinger technique, the catheter was placed in all cysts in which biliary fistula had developed. These cysts were big cysts with a mean diameter of 8 cm (range, 5-11.5 cm). Due to severe abdominal pain, the procedure was terminated in two patients treated with the Seldinger technique and in one patient treated with the Trocar technique. Fever, chills and tachycardia developed in one patient with the Seldinger technique; however these signs resolved spontaneously without any medical treatment. Entry site infection was seen in a patient using the Seldinger technique, and the patient was treated with antibiotics. Cystography revealed leakage into the peritoneal cavity in two cysts subcapsularly located at the dome of the right lobe of the liver in a patient using the Seldinger technique. This patient was treated with albendazole for three months and no peritoneal cysts were detected during the 24-mo follow-up period.
Local recurrence developed in two patients using the Seldinger technique, including the presence of multiple daughter cysts and increased dimensions in a cyst cavity that had collapsed and solidified. These two patients underwent surgical treatment. Two new lesions (secondary dissemination and recurrence) were found at the 12 mo follow-up visit in a patient using Seldinger technique. These lesions were also treated by percutaneous methods.
Complication rates, local recurrence and secondary dissemination were statistically similar between the patients using the Seldinger and Trocar techniques (Tables 2-4).
| Trocar | Seldinger | Total | χ2 | P value | ||
| Development of complications | Yes, n | 3 | 10 | 13 | ||
| (%) | 6.1 | 17.9 | 12.4 | |||
| No, n | 47 | 46 | 93 | 3317 | 0.069 | |
| (%) | 93.9 | 82.1 | 87.6 | |||
| Total | n | 50 | 56 | 106 | ||
| (%) | 100 | 100 |
| Trocar | Seldinger | Total | χ2 | P value | |
| Local recurrence, | |||||
| present, n | 2 | 0 | 2 | ||
| (%) | 4 | 0 | 1.9 | ||
| Local recurrence, | |||||
| none, n | 48 | 56 | 104 | ||
| (%) | 96 | 100 | 98.1 | 2330 | 0.215 |
| Total, | |||||
| n | 50 | 56 | 106 | ||
| (%) | 100 | 100 | 100 |
| Trocar | Seldinger | Total | χ2 | P value | |
| Secondary dissemination, present, n (%) | 0 0 | 1 1.8 | 1 1 | ||
| Secondary dissemination, none, n (%) | 50 100 | 55 98.2 | 105 99 | 0.883 | 0.533 |
| Total, n (%) | 50 100 | 56 100 | 106 100 |
Hydatid cyst disease should be treated, due to the risks of severe infection, invasion to the biliary system and peritoneum and dissemination into other organs. Although surgery is the gold standard treatment, various types of percutaneous treatment provide alternatives for the elimination of the parasite and preventing the disease from reoccurring[23-25,32]. In different series, the success rate of percutaneous procedures has been reported to be 95%-100%[6-19,23,26].
The two step Seldinger technique or single step Trocar technique may be used for entry to the cyst cavity. The disadvantages in using the hydrophilic coated drainage catheters placed percutaneously with a guide wire, as required by the Seldinger technique, are the necessity for two individuals to perform the procedure and the relatively high cost of the technique. Trocar type catheters can be placed by a single individual and are more cost effective. However, secondary to aging, the pleura and peritoneum lose their elasticity after surgery, making the insertion of trocar type catheters difficult in such cases. There is no publication in the literature reporting whether a difference exists between the two techniques used for the entry to the cyst cavity in terms of the efficacy of treatment and the development of complications[15,31,32]. In the present study, Seldinger and Trocar techniques were used in 56 (53%) and 50 (47%) cysts, respectively, and the differences between the two techniques in terms of the efficacy of treatment and complications, if any, were evaluated.
A significant decrease was found in the cyst volume during the follow-up period. Furthermore, no statistically significant difference was found in the volume changes between the two techniques (P = 0.384).
The most frequently seen early complication of percutaneous treatment is fever without signs of infection and minor hypersensitivity reactions probably due to signs that develop secondary to the antigenic stimulus of the parasite, and are treated successfully with symptomatic treatment, as was the case in the present study and in other series previously reported in the literature[3,8,22]. Fistula may develop between the cavity and the biliary system, due to the percutaneous procedure or prolonged drainage. Some of the fistulae may close spontaneously, while some necessitate an endoscopic approach in the treatment[8,23,28]. In the present study, biliary fistula developed in four patients, all of whom had undergone percutaneous drainage with the Seldinger technique. In large patient series in the literature, the rate of development of anaphylaxis has been reported to be approximately 1%-2% with both percutaneous and surgical techniques[27-29]. When we looked into the cases reported in the literature, spontaneous rupture does not always result in anaphylaxis[30]. In thE present study, an anaphylactic reaction developed in one patient during the PAIR procedure following catheter placement with Seldinger technique, however the medical treatment was successful. No statistically significant differences between the two techniques used for the entry to the cyst were found in terms of the rates of development of early complications, such as anaphylaxis, biliary fistula, minor reactions, abdominal pain, entry site infection, infection in the cyst cavity and intraabdominal extravasation (P = 0.069).
Rates of local recurrence and secondary dissemination were reported to be 0%-4% in the literature[3,6,22]. In the present study, local recurrence and secondary dissemination occurred in two patients and one patient, respectively. No statistically significant association was found in the rates of local recurrence and secondary dissemination between the two techniques (P = 0.215, P = 0.533).
In conclusion, no differences were found between the Seldinger and Trocar techniques that might be used in the entry to cyst cavity, in terms of the efficacy of the treatment and the rates of early and late complications. Although percutaneous cyst drainage, conducted with a trocar type catheter, is a practical method that is easier and more economical to apply compared with the drainage procedure conducted using a Seldinger needle, guide wire and a catheter, it should be considered in post-surgical and elderly patients that the trocar type catheter placement might be more difficult to apply, due to decreased elasticity of the pleura and peritoneum in such cases.
Although various methods have been developed as interventional procedures, there is no knowledge in the literature on which technique should be used when entering the liver cyst hydatid cavity. Two step Seldinger technique or single step Trocar technique may be used for entry to the cavity. The objective of this study was to compare two different techniques of percutaneous entry and to evaluate their efficacy.
The weakness points are the small sample of patients and the retrospective design of the study but it can represent an interesting report for literature as first evaluation comparing two different techniques of percutaneous entry. Further studies with a larger number of patients will be needed to confirm the data.
No differences were found between the seldinger and Trocar techniques that might be used in the entry to cyst cavity, in terms of the efficacy of the treatment and the rates of early and late complications. Although percutaneous cyst drainage, conducted with a trocar type catheter, is a practical method that is easier and more economical to apply compared with the drainage procedure conducted using a Seldinger needle, guide wire and a catheter, it should be considered in post-surgical and elderly patients that the trocar type catheter placement might be more difficult to apply, due to decreased elasticity of the pleura and peritoneum, in such cases.
Seldinger technique is a two-step procedure, and standard wires and guide wires were used for drainage. Trocar technique is a single step procedure, and a standard trocar tip drainage catheter is composed of a sheath needle and a catheter coaxial system.
PAIR technique: The Puncture Aspiration Injection Reaspiration technique is performed using either ultrasound or CT guidance, involves aspiration of the cyst contents via a special cannula, followed by injection of a scolicidal agent and then reaspiration of the cystic contents. US: Ultrasound; CT: Computerized tomography.
This study compared two percutaneous techniques on treatment of hydatid cysts.
| 1. | Rozanes I, Güven K, Acunaş B, Emre A. Cystic echinococcal liver disease: new insights into an old disease and an algorithm for therapy planning. Cardiovasc Intervent Radiol. 2007;30:1112-1116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 14] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 2. | Giorgio A, Tarantino L, Francica G, Mariniello N, Aloisio T, Soscia E, Pierri G. Unilocular hydatid liver cysts: treatment with US-guided, double percutaneous aspiration and alcohol injection. Radiology. 1992;184:705-710. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 52] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 3. | Khuroo MS, Dar MY, Yattoo GN, Zargar SA, Javaid G, Khan BA, Boda MI. Percutaneous drainage versus albendazole therapy in hepatic hydatidosis: a prospective, randomized study. Gastroenterology. 1993;104:1452-1459. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 142] [Cited by in RCA: 117] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 4. | Akkiz H, Akinoglu A, Colakoglu S, Demiryürek H, Yagmur O. Endoscopic management of biliary hydatid disease. Can J Surg. 1996;39:287-292. [PubMed] |
| 5. | Al Karawi MA, Mohamed AR, Yasawy I, Haleem A. Non-surgical endoscopic trans-papillary treatment of ruptured echinococcus liver cyst obstructing the biliary tree. Endoscopy. 1987;19:81-83. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 22] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 6. | Akhan O, Ozmen MN, Dinçer A, Sayek I, Göçmen A. Liver hydatid disease: long-term results of percutaneous treatment. Radiology. 1996;198:259-264. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 154] [Cited by in RCA: 145] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 7. | Men S, Hekimoğlu B, Yücesoy C, Arda IS, Baran I. Percutaneous treatment of hepatic hydatid cysts: an alternative to surgery. AJR Am J Roentgenol. 1999;172:83-89. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 100] [Cited by in RCA: 73] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 8. | Khuroo MS, Zargar SA, Mahajan R. Echinococcus granulosus cysts in the liver: management with percutaneous drainage. Radiology. 1991;180:141-145. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 91] [Cited by in RCA: 82] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 9. | Nasseri-Moghaddam S, Abrishami A. Percutaneous needle aspiration, injection, and reaspiration with or without benzimidazole coverage for uncomplicated hepatic hydatid cysts. The Cochrane Library. 2009;1:1-20. |
| 10. | Kabaalioğlu A, Ceken K, Alimoglu E, Apaydin A. Percutaneous imaging-guided treatment of hydatid liver cysts: do long-term results make it a first choice? Eur J Radiol. 2006;59:65-73. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 53] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 11. | Sayek I, Tirnaksiz MB, Dogan R. Cystic hydatid disease: current trends in diagnosis and management. Surg Today. 2004;34:987-996. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 113] [Cited by in RCA: 116] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 12. | Bosanac ZB, Lisanin L. Percutaneous drainage of hydatid cyst in the liver as a primary treatment: review of 52 consecutive cases with long-term follow-up. Clin Radiol. 2000;55:839-848. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 32] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 13. | Duţă C, Păscuţ M, Bordoş D. Percutaneous treatment of the liver hydatid cysts under sonographic guidance. Chirurgia (Bucur). 2002;97:173-177. [PubMed] |
| 14. | Peláez V, Kugler C, Correa D, Del Carpio M, Guangiroli M, Molina J, Marcos B, Lopez E. PAIR as percutaneous treatment of hydatid liver cysts. Acta Trop. 2000;75:197-202. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 36] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 15. | WHO Informal Working Group on Echinococcosis. Guidelines for treatment of cystic and alveolar echinococcosis in humans. WHO Informal Working Group on Echinococcosis. Bull World Health Organ. 1996;74:231-242. [PubMed] |
| 16. | Khuroo MS. Hydatid disease: current status and recent advances. Ann Saudi Med. 2002;22:56-64. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 57] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 17. | Eckert J, Gemmel MA, Meslin F-X, Pawlowski ZS (Eds). WHO/ OIE Manual on Echinococcosiss in Humans and Animals: a Public Health Problem of Global Concern. Genevan, Paris: WHO 2001; . |
| 18. | Larrieu E, Del Carpio M, Salvitti JC, Mercapide C, Sustersic J, Panomarenko H, Costa M, Bigatti R, Labanchi J, Herrero E. Ultrasonographic diagnosis and medical treatment of human cystic echinococcosis in asymptomatic school age carriers: 5 years of follow-up. Acta Trop. 2004;91:5-13. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 34] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 19. | Gharbi HA, Hassine W, Brauner MW, Dupuch K. Ultrasound examination of the hydatic liver. Radiology. 1981;139:459-463. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 639] [Cited by in RCA: 481] [Article Influence: 10.7] [Reference Citation Analysis (2)] |
| 20. | El-On J. Benzimidazole treatment of cystic echinococcosis. Acta Trop. 2003;85:243-252. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 106] [Cited by in RCA: 110] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 21. | Ben Amor N, Gargouri M, Gharbi HA, Golvan YJ, Ayachi K, Kchouck H. [Trial therapy of inoperable abdominal hydatid cysts by puncture]. Ann Parasitol Hum Comp. 1986;61:689-692. [PubMed] |
| 22. | Akhan O, Dincer A, Gököz A, Sayek I, Havlioglu S, Abbasoglu O, Eryilmaz M, Besim A, Baris I. Percutaneous treatment of abdominal hydatid cysts with hypertonic saline and alcohol. An experimental study in sheep. Invest Radiol. 1993;28:121-127. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 68] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 23. | Smego RA, Sebanego P. Treatment options for hepatic cystic echinococcosis. Int J Infect Dis. 2005;9:69-76. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 159] [Cited by in RCA: 144] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 24. | Chautems R, Buhler L, Gold B, Chilcott M, Morel P, Mentha G. Long term results after complete or incomplete surgical resection of liver hydatid disease. Swiss Med Wkly. 2003;133:258-262. [PubMed] |
| 25. | Gupta N, Javed A, Puri S, Jain S, Singh S, Agarwal AK. Hepatic hydatid: PAIR, drain or resect? J Gastrointest Surg. 2011;15:1829-1836. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 49] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 26. | Odev K, Paksoy Y, Arslan A, Aygün E, Sahin M, Karaköse S, Baykan M, Arikoğlu H, Aksoy F. Sonographically guided percutaneous treatment of hepatic hydatid cysts: long-term results. J Clin Ultrasound. 2000;28:469-478. [PubMed] [DOI] [Full Text] |
| 27. | Ormeci N, Soykan I, Bektas A, Sanoğlu M, Palabiyikoğlu M, Hadi Yasa M, Dökmeci A, Uzunalimoğlu O. A new percutaneous approach for the treatment of hydatid cysts of the liver. Am J Gastroenterol. 2001;96:2225-2230. [PubMed] [DOI] [Full Text] |
| 28. | Etlik O, Arslan H, Bay A, Sakarya ME, Harman M, Temizoz O, Kayan M, Bakan V, Unal O. Abdominal hydatid disease: long-term results of percutaneous treatment. Acta Radiol. 2004;45:383-389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 18] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 29. | Hofstetter C, Segovia E, Vara-Thorbeck R. Treatment of uncomplicated hydatid cyst of the liver by closed marsupialization and fibrin glue obliteration. World J Surg. 2004;28:173-178. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 14] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 30. | Saenz de San Pedro B, Cazaña JL, Cobo J, Serrano CL, Quiralte J, Contreras J, Martinez F. Anaphylactic shock by rupture of hydatid hepatic cyst. Follow-up by specific IgE serum antibodies. Allergy. 1992;47:568-570. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 20] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 31. | WHO. PAIR: Puncture, Aspiration, Injection, ReAspiration. An option for the treatment of Cystic Echinococcosis. Available from: http://wholibdoc.who.int/hq/2001. |
| 32. | Gomez I Gavara C, López-Andújar R, Belda Ibáñez T, Ramia Ángel JM, Moya Herraiz Á, Orbis Castellanos F, Pareja Ibars E, San Juan Rodríguez F. Review of the treatment of liver hydatid cysts. World J Gastroenterol. 2015;21:124-131. [PubMed] [DOI] [Full Text] |
Manuscript source: Unsolicited manuscript
Specialty type: Radiology, nuclear medicine and medical imaging
Country of origin: Turkey
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
Open-Access: This article is an open-access article which was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/
P- Reviewer: Liu F S- Editor: Ji FF L- Editor: A E- Editor: Zhao LM