Published online Feb 28, 2026. doi: 10.4329/wjr.v18.i2.115741
Revised: November 25, 2025
Accepted: January 9, 2026
Published online: February 28, 2026
Processing time: 124 Days and 19 Hours
Non-contrast whole-heart coronary magnetic resonance angiography (CMRA) remains underutilized in clinical practice due to limited visualization of distal vessels and prolonged acquisition times.
To evaluate the performance of a coronal balanced turbo field echo (BTFE) sequence for CMRA at 3.0T in comparison with conventional axial turbo field echo (TFE) and modified Dixon (mDixon) sequences.
Healthy young volunteers were prospectively enrolled from January 2025 to April 2025. All participants underwent coronary artery imaging using BTFE, TFE, and mDixon sequences. Subjective image quality was assessed based on the society of cardiovascular computed tomography 18-segment model using a four-point scale (1 = non-assessable to 4 = excellent) across the three major coronary arteries and their side branches. The assessability rate was defined as the percentage of segments receiving a score ≥ 2. Objective evaluation of the main coronary arteries included measurements of signal-to-noise ratio, contrast-to-noise ratio, vessel edge sharpness, and visible vessel length. Acquisition time was recorded for each sequence. Statistical comparisons among the three sequences were performed using the Friedman test and one-way repeated measures analysis of variance.
A total of 22 participants (mean age ± SD, 23 ± 2 years; 12 men) were included in the study. BTFE significantly outperformed both TFE and mDixon in subjective image quality scores across all coronary segments (all P < 0.05), except for the left main coronary artery, the proximal and mid segments of the left anterior descending artery (LAD), the proximal and mid segments of the left circumflex artery (LCX), the proximal segment of the right coronary artery, and ramus intermedius, for which no significant differences were observed between BTFE and mDixon (P > 0.05). The BTFE sequence achieved the highest overall assessability (99.3%, 282/284), surpassing mDixon (95.4%, 271/284) and TFE (87.0%, 247/284). BTFE yielded significantly higher signal-to-noise ratio, contrast-to-noise ratio, and vessel edge sharpness compared with both TFE and mDixon (all P < 0.001). The measured lengths of the LAD and right coronary artery were also significantly greater with BTFE (P < 0.05 for both). The LCX length was significantly longer on BTFE than on TFE (77.5 ± 10.5 mm vs 75.1 ± 8.3 mm; P = 0.017), but not significantly different from that on mDixon (77.5 ± 10.5 mm vs 75.7 ± 8.8 mm; P = 0.074). Additionally, BTFE demonstrated a shorter and more consistent acquisition time compared with both TFE and mDixon (6.13 ± 1.00 minutes vs 7.15 ± 2.02 minutes vs 7.17 ± 1.72 minutes; P < 0.05).
Coronal BTFE-based non-contrast whole-heart CMRA at 3.0T offers superior image quality and reduced acquisition time compared with conventional axial TFE and mDixon sequences.
Core Tip: This study presents a focused technical evaluation of a newly implemented coronal-plane balanced turbo field echo (BTFE) sequence for non-contrast-enhanced coronary magnetic resonance angiography at 3.0T. Through a prospective intra-individual comparison with conventional axial turbo field echo and modified Dixon sequences, the coronal BTFE protocol demonstrated superior image quality - particularly in distal coronary segments - and a shorter acquisition time. These find
- Citation: Wei CW, Zhang RZ, Xu Y, Liu JY, Zhang N, Xu L, Wen ZY. Non-contrast 3.0T coronary magnetic resonance angiography: Image quality comparison of coronal balanced-turbo-field-echo, axial turbo-field-echo, and modified-Dixon sequences. World J Radiol 2026; 18(2): 115741
- URL: https://www.wjgnet.com/1949-8470/full/v18/i2/115741.htm
- DOI: https://dx.doi.org/10.4329/wjr.v18.i2.115741
Cardiovascular diseases, particularly coronary artery disease (CAD), remain the leading cause of mortality worldwide[1]. The current clinical assessment of CAD primarily relies on two imaging modalities: Invasive digital subtraction angiography[1] considered the diagnostic gold standard, and noninvasive coronary computed tomography angiography (CCTA). However, both techniques require iodinated contrast agents and expose patients to ionizing radiation, which poses potential risks. Non-contrast coronary magnetic resonance (MR) angiography (CMRA) has emerged as a safe, noninvasive, radiation-free alternative for imaging coronary artery stenosis without the need for iodinated contrast agents[2,3]. In addition to evaluating coronary arteries, CMRA can detect coronary artery aneurysms and assess coronary artery bypass grafts[4-6]. Furthermore, unlike CCTA, CMRA is not affected by calcification-induced artifacts[7,8].
Despite these advantages, the clinical adoption of CMRA remains limited due to technical challenges related to image quality and acquisition time. To address these limitations, various MR sequences have been developed and refined. The modified Dixon (mDixon) technique, based on water-fat separation, offers improved vessel-to-fat contrast and increased signal-to-noise ratio (SNR), along with enhanced tolerance to field inhomogeneity[9,10]. Previous studies have demon
Recently, a coronal-plane implementation of a balanced TFE (BTFE) sequence has been proposed as a promising alternative to non-contrast CMRA[15]. This SSFP-based approach is designed to optimize acquisition efficiency and enhance image quality by improving SNR and reducing scan time. Although previous studies have compared BTFE with mDixon at 3T and demonstrated its diagnostic accuracy in patients with suspected CAD using CCTA as the reference standard, these investigations primarily focused on clinical populations and diagnostic outcomes. In contrast, direct head-to-head technical comparisons among BTFE, TFE, and mDixon sequences under conditions free from disease-related variability remain limited. Therefore, the objective of this prospective study was to address this gap by systematically comparing the performance of BTFE, TFE, and mDixon sequences for non-contrast whole-heart CMRA at 3.0T.
This study was approved by the institutional review board of Beijing Anzhen Hospital, Capital Medical University, approval No. 2025232x. Written informed consent was obtained from all participants. Between January 2025 and April 2025, 22 healthy young volunteers were prospectively enrolled, all of whom underwent non-contrast, free-breathing, whole-heart CMRA. Each participant underwent scanning with three sequences, BTFE, TFE, and mDixon, on a 3.0T Philips system.
CMRA examinations were performed using a 3.0T MR scanner (Gyroscan Intera, Philips Medical Systems, Best, Netherlands) equipped with a dedicated cardiac software package, a synergy cardiac coil, and a vectorcardiogram. Acquisition parameters for the BTFE, TFE, and mDixon sequences are summarized in Table 1.
| Parameter | BTFE | TFE | mDixon |
| No. slices | 250 | 150 | 150 |
| Field of view (mm × mm) | 280 × 340 | 265 × 301 | 265 × 301 |
| Matrix | 208 × 234 | 212 × 201 | 176 × 201 |
| Repetition time (millisecond) | Shortest | Shortest | Shortest |
| Echo time (millisecond) | Shortest | Shortest | Shortest |
| Flip angle (degrees) | 70 | 20 | 10 |
| Number of signal averages | 1 | 1 | 1 |
| Fat/blood suppression | Spectral-attenuated inversion recovery | Spectral-attenuated inversion recovery | Water-fat separation |
| Acquired voxel (mm3) | 1.35 × 1.45 × 1.55 | 1.25 × 1.50 × 1.50 | 1.50 × 1.50 × 1.50 |
| Reconstructed voxel (mm3) | 0.75 × 0.75 × 0.75 | 0.75 × 0.75 × 0.75 | 0.75 × 0.75 × 0.75 |
Participants were positioned supine and head-first in the scanner. Survey images were obtained using the BTFE sequence to localize the heart. High-temporal-resolution cine imaging (100 phases per cardiac cycle) in the four-chamber view was then conducted. Subsequently, a BTFE sequence was used to determine the subject-specific trigger delay and the optimal data acquisition window, during which right coronary artery motion was minimal.
The same cardiac phase (diastole or systole) was selected for each participant across all three imaging protocols. A beam-shaped navigator was positioned at the dome of the right hemidiaphragm, with approximately one-third of the beam over the lung and two-thirds over the liver. The BTFE sequence was acquired in the coronal plane, whereas the TFE and mDixon sequences were acquired in the axial plane. All CMRA acquisitions were performed under free-breathing conditions. The total acquisition time varied according to navigator efficiency. Assuming 100% scan efficiency, the estimated acquisition times were 2 minutes 24 seconds for BTFE, 3 minutes 23 seconds for TFE, and 3 minutes 48 seconds for mDixon. For each CMRA scan, the participant’s heart rate and the actual acquisition time were recorded.
All examinations were independently evaluated by two radiologists with over 10 years of experience in cardiovascular imaging (Nan Zhang 15 years; Jia-Yi Liu 25 years). The names, dates, and sequences of each case were blinded to the readers. Image post-processing and evaluation were conducted using a Vitrea workstation (v8, Vital Images, Minnetonka, MN, United States). Image quality for all sequences was assessed from axial-plane images.
A total of 18 coronary artery segments were evaluated in each participant, following the society of cardiovascular computed tomography 18-segment model: Left main coronary artery (LM); left anterior descending artery LAD-proximal (pro), LAD-mid, LAD-distal (dis); first and second diagonal branches (D1, D2); left circumflex artery (LCX-pro, LCX-dis); first and second obtuse marginal branches (OM1, OM2); ramus intermedius; right coronary artery (RCA-pro, RCA-mid, RCA-dis); left and right posterior descending arteries (PDA); and left and right posterolateral branches (PLB). Because certain small vessels were present in only a subset of participants, D1 and D2 were pooled into a single diagonal branch (D) category, OM1 and OM2 into an OM category, left-PDA and right-PDA into a PDA category, and left-PLB and right-PLB into a PLB category to ensure adequate sample size for statistical analysis.
CMRA image quality was graded on a four-point scale: 1 = non-assessable (severe artifacts, poor vessel contrast); 2 = assessable (moderate artifacts, fair vessel contrast); 3 = assessable (minor artifacts, good vessel contrast); and 4 = assessable (no apparent artifacts, excellent vessel contrast)[16,17]. If either reader assigned a score of 1 (non-assessable), the segment was classified as non-assessable by consensus.
SNR and contrast-to-noise ratio (CNR) were measured on axial-plane images at four coronary locations: The LM, LAD-pro, LCX-pro, and RCA-pro. At each predefined measurement site, including the LM and the proximal segments (10 mm from the origin) of the RCA, LAD, and LCX, a circular region of interest (ROI) with an area of approximately 5 mm2 was manually placed at the center of the vessel lumen to measure mean blood signal intensity. A second ROI of similar size was placed in the anterior chest wall musculature at the same axial level to assess background noise. ROI placement was standardized across sequences and participants, thereby avoiding partial-volume effects, proximity to the vessel wall, and regions affected by motion or flow artifacts. SNR was defined as SNR = SIcoronary artery/SDmusculature, where SI denotes signal intensity, and SD represents the standard deviation. CNR was defined as CNR = (SIcoronary artery - SImusculature)/
Coronary MRA images were further processed using curved planar reformation on the Vitrea post-processing workstation, and the visible vessel lengths of the LAD, LCX, and RCA were measured. The LAD length measurement included the LM segment.
The reproducibility of the image analysis was assessed through intra- and interobserver studies. To assess intraobserver variability, one reader (Nan Zhang) reviewed the images twice, with a two-week interval to reduce bias. For interobserver agreement, the same CMRA scans were independently reviewed by another reader (Jia-Yi Liu) and compared with the initial reader’s first set of measurements.
Data were tested for normality using the Shapiro-Wilk test. Normally distributed variables are reported as mean ± SD, while non-normally distributed data are presented as median (interquartile range). To compare measurements across the BTFE, TFE, and mDixon sequences, the Friedman test and one-way repeated measures analysis of variance were applied. For normally distributed variables, a one-way repeated-measures analysis of variance with post hoc Bonferroni correction was used. For non-normally distributed variables, the Friedman test was followed by pairwise Wilcoxon signed-rank tests with Bonferroni adjustment.
Interreader reproducibility for SNR, CNR, VES, and vessel length measurements was assessed using intraclass correlation coefficients (range: 0-1.00, with 0.81-1.00 indicating excellent agreement). Interreader agreement for image quality scoring was evaluated using κ statistics (range: 0-1.00, with κ ≥ 0.80 indicating excellent agreement). All statistical analyses were performed using SPSS version 27.0 (IBM, New York, NY, United States). A P value < 0.05 was considered statistically significant.
A total of 22 healthy participants (12 men; mean age 23 ± 2 years) were prospectively enrolled. The mean heart rate (HR) was 67 ± 7 beats/minutes, and the mean body mass index was 21.2 ± 1.4 kg/m2. All participants completed non-contrast CMRA using the three sequences.
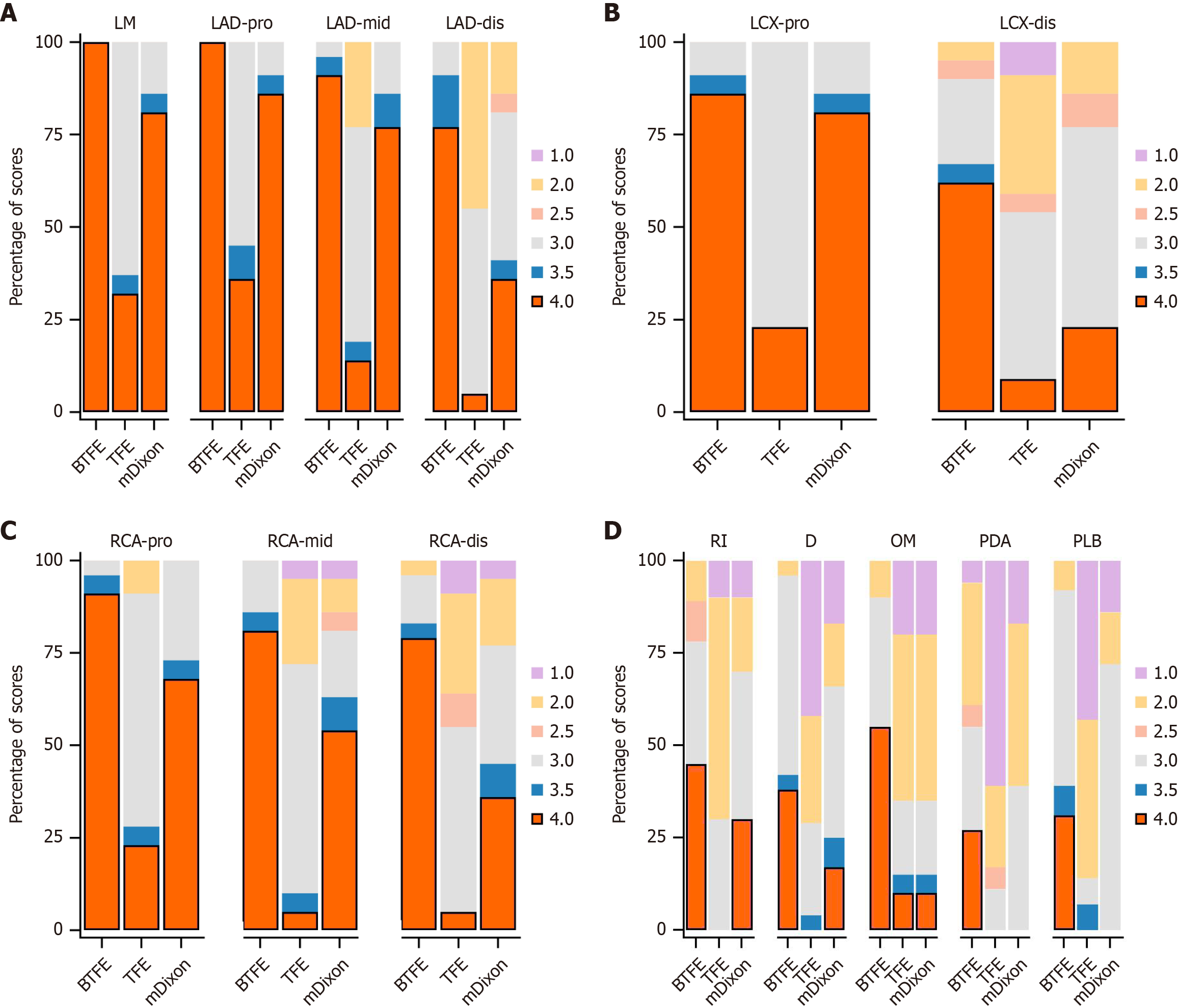
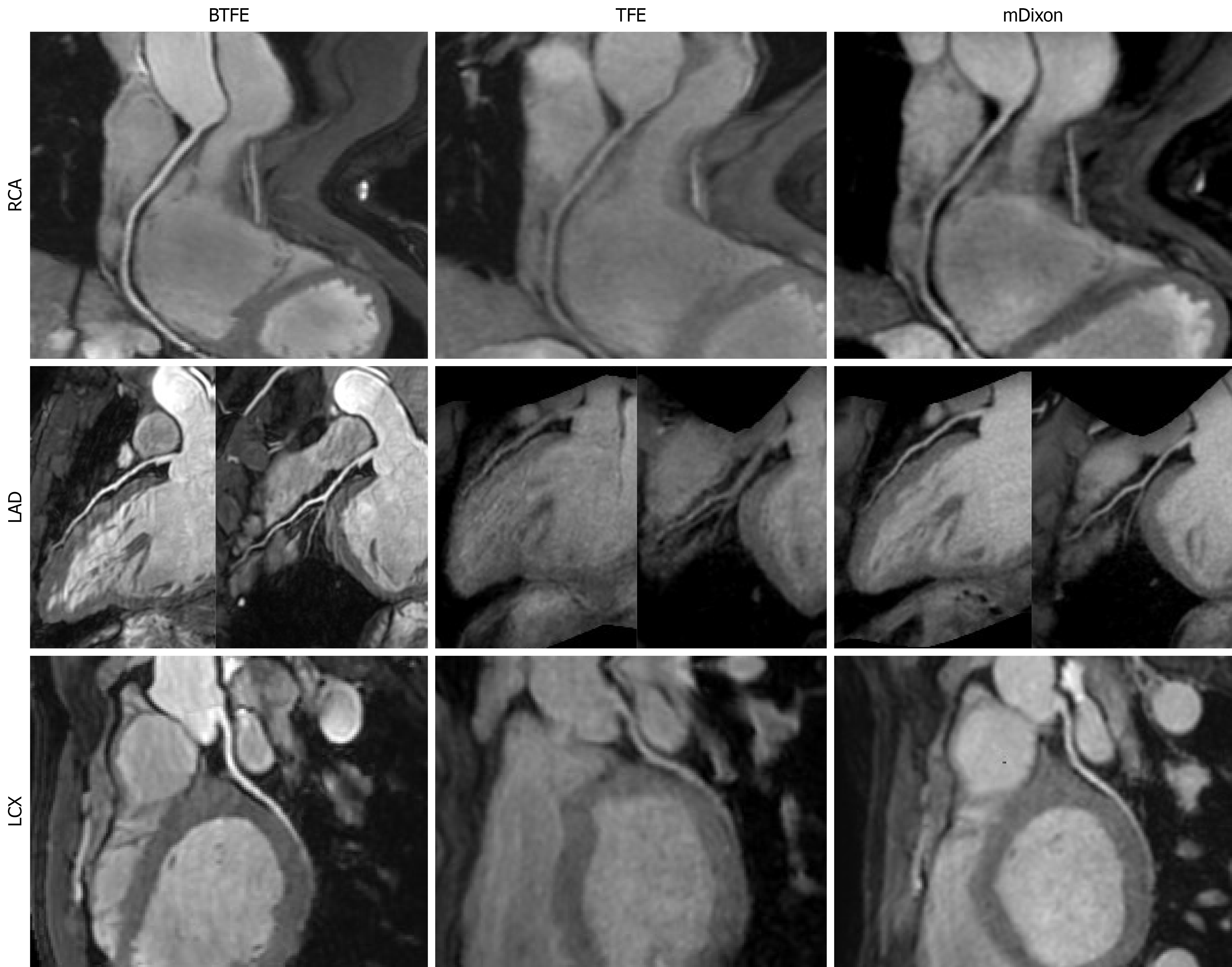
Subjective image quality score and vessel assessability rate: As summarized in Table 2, visualization scores for distal coronary segments, including LAD-dis, LCX-dis, RCA-mid, RCA-dis, D, OM, PDA, and PLB, were significantly higher with BTFE than with TFE or mDixon (P < 0.05 for all). For proximal segments - including the LM, LAD-pro, LAD-mid, LCX-pro, RCA-pro, and ramus intermedius, BTFE yielded significantly higher scores than TFE (P < 0.05 for all), but showed no significant differences from mDixon (P > 0.05 for all) (Figures 1 and 2). The BTFE sequence achieved the highest overall vessel assessability rate (99.3%, 282/284), outperforming mDixon (95.4%, 271/284) and TFE (87.0%, 247/284). BTFE achieved 100% assessability in all major segments and side branches (D and OM), and demonstrated superior rates in distal segments, including PDA (94.4% vs 38.9% for TFE vs 83.3% for mDixon) and PLB (92.9% vs 57.1% vs 85.7%) (Tables 2 and 3).
| Characteristic | BTFE | TFE | mDixon | Intergroups P value1 | P value (adjusted P value)2 | P value (adjusted P value)3 | P value (adjusted P value)4 |
| Sex | - | - | - | NA | NA | NA | NA |
| Male | 12 | 12 | 12 | - | - | - | - |
| Female | 10 | 10 | 10 | - | - | - | - |
| Age (year), mean ± SD | 23 ± 2 | 23 ± 2 | 23 ± 2 | NA | NA | NA | NA |
| HR (beats/minute), mean ± SD | 67 ± 7 | 67 ± 7 | 67 ± 7 | NA | NA | NA | NA |
| BMI, mean ± SD | 21.2 ± 1.4 | 21.2 ± 1.4 | 21.2 ± 1.4 | NA | NA | NA | NA |
| Image quality score | |||||||
| LM | 4.0 (4.0-4.0) | 3.0 (3.0-3.0) | 4.0 (4.0-4.0) | < 0.001 | < 0.001 | 0.177 | 0.009 |
| LAD-pro | 4.0 (4.0-4.0) | 3.0 (3.0-4.0) | 4.0 (4.0-4.0) | < 0.001 | < 0.001 | 0.306 | 0.003 |
| LCX-pro | 4.0 (4.0-4.0) | 3.0 (3.0-3.25) | 4.0 (4.0-4.0) | < 0.001 | < 0.001 | 0.583 | < 0.001 |
| RCA-pro | 4.0 (4.0-4.0) | 3.0 (3.0-3.25) | 4.0 (4.0-4.0) | < 0.001 | < 0.001 | 0.084 | < 0.001 |
| LAD-mid | 4.0 (4.0-4.0) | 3.0 (2.75-3.0) | 4.0 (3.875-4.0) | < 0.001 | < 0.001 | 0.489 | < 0.001 |
| RCA-mid | 4.0 (4.0-4.0) | 3.0 (2.5-3.0) | 3.75 (2.875-4.0) | < 0.001 | < 0.001 | 0.024 | < 0.001 |
| LAD-dis | 4.0 (3.875-4.0) | 3.0 (2.0-3.0) | 3.0 (3.0-4.0) | < 0.001 | < 0.001 | < 0.001 | 0.009 |
| LCX-dis | 4.0 (3.0-4.0) | 3.0 (2.0-3.0) | 3.0 (2.875-3.25) | < 0.001 | < 0.001 | 0.03 | < 0.001 |
| RCA-dis | 4.0 (3.375-4.0) | 3.0 (2.0-3.0) | 3.0 (2.75-4.0) | < 0.001 | < 0.001 | 0.03 | < 0.001 |
| RI | 3.5 (2.88-4.0) | 2.0 (2.0-2.63) | 3.0 (2.0-4.0) | 0.009 | 0.033 | 0.156 | 0.21 |
| D | 3.0 (3.0-4.0) | 2.0 (1.0-3.0) | 3.0 (2.0-3.375) | < 0.001 | < 0.001 | 0.009 | 0.006 |
| OM | 4.0 (3.0-4.0) | 2.0 (2.0-3.0) | 3.0 (2.0-4.0) | < 0.001 | < 0.001 | 0.015 | 0.09 |
| PDA | 3.0 (2.0-4.0) | 1.0 (1.0-2.0) | 2.0 (2.0-3.0) | < 0.001 | < 0.001 | 0.033 | 0.006 |
| PLB | 3.0 (3.0-4.0) | 2.0 (1.0-2.0) | 3.0 (2.0-3.0) | < 0.001 | 0.006 | 0.042 | 0.018 |
| Segment | No. of all segments | No. of assessable segment (score ≥ 2) | ||
| BTFE | TFE | mDixon | ||
| Overall | 284 | 282 (99.3) | 247 (87.0) | 271 (95.4) |
| LM | 22 | 22 (100) | 22 (100) | 22 (100) |
| LAD-pro | 22 | 22 (100) | 22 (100) | 22 (100) |
| LCX-pro | 22 | 22 (100) | 22 (100) | 22 (100) |
| RCA-pro | 22 | 22 (100) | 22 (100) | 22 (100) |
| LAD-mid | 22 | 22 (100) | 22 (100) | 22 (100) |
| RCA-mid | 22 | 22 (100) | 21 (95.5) | 21 (95.5) |
| LAD-dis | 22 | 22 (100) | 22 (100) | 22 (100) |
| LCX-dis | 22 | 22 (100) | 20 (90.9) | 22 (100) |
| RCA-dis | 22 | 22 (100) | 20 (90.9) | 21 (95.5) |
| RI | 10 | 10 (100) | 9 (90.0) | 9 (90.0) |
| D | 24 | 24 (100) | 14 (58.3) | 20 (83.3) |
| OM | 20 | 20 (100) | 16 (80) | 19 (95.0) |
| PDA | 18 | 17 (94.4) | 7 (38.9) | 15 (83.3) |
| PLB | 14 | 13 (92.9) | 8 (57.1) | 12 (85.7) |
Quantitative image quality assessment and acquisition time: BTFE significantly outperformed both TFE and mDixon across all quantitative metrics (P < 0.001 for all) (Table 4). Mean SNR values for BTFE ranged from 137 to 145, compared with 73 to 89 for TFE and 94 to 109 for mDixon (P < 0.001). Mean CNR values ranged from 75 to 84 for BTFE, 15 to 31 for TFE, and 35 to 50 for mDixon (P < 0.001). Mean VES was also significantly higher with BTFE, ranging from 257 to 284, compared with 141 to 150 for TFE and 77 to 82 for mDixon (P < 0.001).
| Parameter | BTFE | TFE | mDixon | Intergroups P value1 | P value (adjusted P value)2 | P value (adjusted P value)3 | P value (adjusted P value)4 |
| SNR | |||||||
| LM | 145.0 ± 12.9 | 88.68 ± 8.2 | 109.4 ± 12.2 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| LAD-pro | 139.7 ± 13.6 | 83.2 ± 7.9 | 109.4 ± 12.6 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| LCX-pro | 137.2 ± 14.5 | 80.4 ± 6.3 | 104.8 ± 12.5 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| RCA-pro | 135.4 ± 8.4 | 73.3 ± 9.2 | 94.3 ± 12.0 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| CNR | - | - | - | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| LM | 83.7 ± 13.6 | 30.7 ± 6.4 | 50.2 ± 10.6 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| LAD-pro | 78.2 ± 12.4 | 25.1 ± 5.8 | 50.1 ± 11.7 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| LCX-pro | 75.7 ± 14.0 | 22.2 ± 7.1 | 45.5 ± 14.0 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| RCA-pro | 74.1 ± 12.1 | 15.4 ± 6.7 | 35.1 ± 8.6 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| VES5 | - | - | - | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| LM | 257.3 ± 31.0 | 150.2 ± 19.3 | 80.5 ± 14.0 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| LAD-pro | 266.1 ± 34.9 | 149.6 ± 14.2 | 82.1 ± 10.8 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| LCX-pro | 276.6 ± 33.9 | 141.1 ± 13.0 | 76.9 ± 7.4 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| RCA-pro | 284.1 ± 35.8 | 143.4 ± 13.5 | 79.7 ± 9.8 | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
| Vessel length (mm) | |||||||
| LAD | 126 ± 10 | 114 ± 17 | 118 ± 17 | < 0.001 | < 0.001 | 0.016 | 0.017 |
| LCX | 77 ± 10 | 75 ± 8 | 76 ± 9 | 0.002 | 0.017 | 0.074 | 0.459 |
| RCA | 122 ± 7 | 120 ± 7 | 121 ± 7 | < 0.001 | 0.002 | 0.043 | 0.038 |
| Acquisition time (minute) | 6.13 ± 1.00 | 7.15 ± 2.02 | 7.17 ± 1.72 | 0.015 | 0.025 | 0.035 | 1.000 |
The measured lengths of the LAD and RCA were significantly greater with BTFE compared to the other sequences (P < 0.005 for all). The LCX length was significantly longer on BTFE than on TFE (77.5 ± 10.5 mm vs 75.1 ± 8.3 mm; P = 0.017), but not significantly different from mDixon (77.5 ± 10.5 mm vs 75.7 ± 8.8 mm; P = 0.074).
BTFE CMRA also demonstrated a shorter mean acquisition time and reduced variability in imaging time compared with TFE and mDixon (6.13 ± 1.00 minutes vs 7.15 ± 2.02 minutes vs 7.17 ± 1.72 minutes; P < 0.005).
Agreements of scoring and measurements: Inter- and intra-observer reproducibility was excellent for all assessments, including image quality scoring, quantitative image quality metrics (SNR, CNR, VES), and vessel length measurements across the BTFE, TFE, and mDixon sequences. κ values for categorical assessments and intraclass correlation coefficients for continuous variables are summarized in Tables 5 and 6.
| Score of vessel segments | Reader 1 | Reader 2 | Interobserver kappa (95%CI) | Reader 1 repeat | Intraobserver kappa (95%CI) |
| LM | 4.0 (3.0-4.0) | 4.0 (3.0-4.0) | 0.887 (0.763-1.012) | 4.0 (3.0-4.0) | 0.924 (0.819-1.028) |
| LAD-pro | 4.0 (3.75-4.0) | 4.0 (3.75-4.0) | 0.835 (0.679-0.991) | 4.0 (4.0-4.0) | 0.874 (0.734-1.013) |
| LCX-pro | 4.0 (3.0-4.0) | 4.0 (3.0-4.0) | 0.901 (0.792-1.010) | 4.0 (3.0-4.0) | 0.933 (0.843-1.024) |
| RCA-pro | 4.0 (3.0-4.0) | 4.0 (3.0-4.0) | 0.886 (0.776-0.996) | 4.0 (3.0-4.0) | 0.914 (0.817-1.010) |
| LAD-mid | 4.0 (3.0-4.0) | 4.0 (3.0-4.0) | 0.875 (0.766-0.985) | 4.0 (3.0-4.0) | 0.900 (0.802-0.998) |
| RCA-mid | 4.0 (3.0-4.0) | 3.0 (3.0-4.0) | 0.887 (0.797-0.978) | 3.0 (3.0-4.0) | 0.906 (0.824-0.988) |
| LAD-dis | 3.0 (3.0-4.0) | 3.0 (3.0-4.0) | 0.853 (0.743-0.963) | 3.0 (3.0-4.0) | 0.872 (0.768-0.976) |
| LCX-dis | 3.0 (2.75-4.0) | 3.0 (3.0-4.0) | 0.859 (0.753-0.965) | 3.0 (3.0-4.0) | 0.877 (0.777-0.977) |
| RCA-dis | 3.0 (3.0-4.0) | 3.0 (2.0-4.0) | 0.872 (0.774-0.969) | 3.0 (2.0-4.0) | 0.888 (0.796-0.980) |
| RI | 3.0 (2.0-4.0) | 3.0 (2.0-3.25) | 0.865 (0.740-0.991) | 3.0 (2.0-4.0) | 0.904 (0.797-1.011) |
| D | 3.0 (2.0-3.0) | 3.0 (2.0-3.0) | 0.924 (0.865-0.984) | 3.0 (2.0-3.0) | 0.950 (0.901-0.998) |
| OM | 3.0 (2.0-4.0) | 3.0 (2.0-4.0) | 0.891 (0.812-0.970) | 3.0 (2.0-4.0) | 0.938 (0.879-0.998) |
| PDA | 2.0 (1.0-3.0) | 2.0 (1.0-3.0) | 0.910 (0.836-0.984) | 2.0 (1.0-3.0) | 0.964 (0.915-1.014) |
| PLB | 3.0 (2.0-3.0) | 3.0 (2.0-3.0) | 0.884 (0.787-0.981) | 3.0 (2.0-3.0) | 0.954 (0.892-1.016) |
| Characteristic | Reader 1 | Reader 2 | Interobserver ICC (95%CI) | Reader 1 repeat | Intraobserver ICC (95%CI) |
| SNR | |||||
| LM | 114.4 ± 25.9 | 115.6 ± 23.0 | 0.957 (0.931-0.974) | 114.4 ± 24.0 | 0.989 (0.982-0.993) |
| LAD-pro | 110.8 ± 25.9 | 112.9 ± 30.7 | 0.966 (0.943-0.979) | 111.4 ± 23.7 | 0.985 (0.976-0.991) |
| LCX-pro | 107.4 ± 26.1 | 107.3 ± 22.4 | 0.956 (0.930-0.973) | 108.4 ± 23.6 | 0.986 (0.977-0.991) |
| RCA-pro | 103.6 ± 27.6 | 101.4 ± 26.6 | 0.975 (0.959-0.985) | 103.8 ± 24.6 | 0.989 (0.968-0.995) |
| CNR | |||||
| LM | 54.9 ± 24.2 | 57.2 ± 28.7 | 0.951 (0.918-0.970) | 55.9 ± 28.0 | 0.973 (0.956-0.983) |
| LAD-pro | 51.2 ± 24.1 | 51.1 ± 20.2 | 0.948 (0.916-0.968) | 52.1 ± 21.8 | 0.984 (0.973-0.990) |
| LCX-pro | 47.8 ± 25.1 | 50.1 ± 28.8 | 0.952 (0.920-0.971) | 48.8 ± 28.1 | 0.973 (0.957-0.984) |
| RCA-pro | 41.5 ± 26.3 | 43.3 ± 27.0 | 0.971 (0.951-0.982) | 43.3 ± 27.7 | 0.982 (0.967-0.990) |
| VES | |||||
| LM | 162.7 ± 76.6 | 155.7 ± 65.9 | 0.951 (0.917-0.971) | 159.6 ± 75.4 | 0.983 (0.972-0.989) |
| LAD-pro | 166.0 ± 79.8 | 159.0 ± 69.2 | 0.958 (0.927-0.975) | 162.9 ± 78.2 | 0.984 (0.974-0.990) |
| LCX-pro | 164.9 ± 86.5 | 161.5 ± 77.2 | 0.979 (0.966-0.987) | 161.2 ± 81.0 | 0.985 (0.975-0.991) |
| RCA-pro | 169.1 ± 88.9 | 162.0 ± 82.7 | 0.985 (0.964- 0.992) | 160.9 ± 84.6 | 0.989 (0.949-0.996) |
| Vessel length (mm) | |||||
| LAD | 119.2 ± 16.0 | 119.3 ± 16.0 | 0.997 (0.994-0.998) | 118.7 ± 16.2 | 0.999 (0.999-1.000) |
| LCX | 76.1 ± 9.1 | 75.9 ± 9.8 | 0.984 (0.975-0.990) | 76.2 ± 9.7 | 0.989 (0.982-0.993) |
| RCA | 121.4 ± 7.2 | 122.4 ± 7.2 | 0.978 (0.908-0.991) | 121.5 ± 7.2 | 0.996 (0.994-0.998) |
This study compared CMRA image quality and acquisition time across BTFE, TFE, and mDixon sequences. The main findings are as follows: (1) Radiologist evaluations revealed significantly improved coronary visualization with BTFE, particularly in distal segments, compared with the other sequences; (2) The coronal-plane BTFE CMRA sequence achieved higher SNR, CNR, and VES, along with a shorter acquisition time, relative to both TFE and mDixon; and (3) BTFE provided superior delineation of the LAD and RCA compared with the other two techniques.
Although the mDixon technique has gained broader application in 3.0T CMRA due to its robust fat suppression and improved tolerance to B0 inhomogeneity[9], it typically requires longer acquisition times and often relies on multiphase data acquisition within the same respiratory window to ensure accurate water-fat separation[15]. These requirements may reduce its efficiency for routine coronary imaging. TFE, while widely used in clinical settings, remains sensitive to flow-related artifacts and may exhibit less consistent blood-myocardium contrast, particularly in distal and branch vessels.
In contrast, the coronal BTFE sequence offers higher intrinsic SNR efficiency and more stable magnetization during free-breathing acquisition. This results in significantly improved SNR, CNR, and VES, along with shorter and more consistent scan times in our study cohort. These characteristics collectively account for the superior overall performance of BTFE compared with both TFE and mDixon in this direct technical comparison.
In this cohort of healthy volunteers, the BTFE sequence demonstrated superior image quality, particularly in visua
Quantitative analysis demonstrated that the coronal plane BTFE sequence significantly increased the visualized lengths of the LAD and RCA compared with the mDixon sequences, whereas measurements of the LCX showed no significant differences. The discrepancy observed in LAD measurements may be attributed to its distinct anatomical characteristics: Approximately 67%-98% of myocardial bridges are located in the LAD, most commonly in its proximal and mid seg
This study differs in scope and study population from a recent work by Yuan et al[15], who evaluated the coronal-plane BTFE sequence in patients with suspected CAD, using CCTA as the reference standard. Their investigation focused on diagnostic performance, including sensitivity and specificity for stenosis detection. It demonstrated superior image quality and diagnostic accuracy of BTFE compared with mDixon in a clinical setting. In contrast, the present study was conducted in healthy volunteers and focused on a technical comparison of three noncontrast CMRA sequences - BTFE, TFE, and mDixon - at 3.0T. Unlike Yuan et al[15] included TFE as a conventional sequence not evaluated in their work and conducted a more comprehensive technical assessment encompassing quantitative metrics (SNR, CNR, and VES), subjective image quality scores for both major coronary trunks and side branches, vessel assessability, and total scan time. These findings not only complement those of Yuan et al[15] by confirming the superior performance of BTFE over TFE and mDixon but also extend their conclusions by demonstrating excellent image quality and high assessability of distal segments and side branches. This is particularly relevant given that limited visualization of distal segments and side branches has long been a major constraint in the broader clinical adoption of CMRA.
The robust performance of BTFE in anatomically and diagnostically challenging segments suggests its potential to overcome current technical limitations and enhance diagnostic confidence in comprehensive coronary assessment. Accordingly, further investigation of patients with suspected CAD is warranted, particularly to evaluate the diagnostic utility of side branch imaging. Collectively, these findings highlight the clinical potential of BTFE as a technically reliable and diagnostically versatile sequence for non-contrast coronary MRA.
Additionally, ECG trigger delay and data acquisition windows were individually optimized for each subject based on the RCA’s relative quiescent phase during coronary MRA acquisition. Despite this tailored approach, RCA images exhibited lower SNR and CNR compared with those of other coronary arteries. This discrepancy is likely due to residual vessel motion and the RCA’s distinct flow dynamics, which may compromise image stability even during nominally motion-free periods.
Additionally, these observations indicate that in CMRA, performing high-temporal-resolution cine imaging under conditions of low HR variability to determine the trigger delay and data acquisition window is critical for ensuring the image quality of subsequent CMRA. For patients with a baseline HR exceeding 75 bpm, which may lead to suboptimal image quality, sublingual administration of nitroglycerin can be used to reduce the HR to the target range of 55-65 bpm[19,20]. Lu et al[12] demonstrated that sublingual administration of nitroglycerin significantly enhances coronary artery conspicuity and overall image quality, particularly in distal segments, and improves the diagnostic performance of non-contrast coronary MRA for CAD. Additionally, it is noteworthy that autonomic nervous system-mediated changes in breathing patterns during sleep can lead to increased diaphragm displacement, which results in decreased navigator gating efficiency and a significant prolongation of adequate acquisition time. Therefore, patients should be prevented from falling asleep during the scan.
This study has several limitations. First, the sample size was relatively small due to its single-center design. Inclusion of a larger number of participants, particularly through multicenter collaboration, is desirable. Second, the inclusion criteria were limited to young, healthy individuals, excluding elderly participants and those at high risk for CAD. Consequently, the applicability of these findings to the broader clinical population requires further validation. Future research is planned as a prospective, multicenter cohort study with a larger sample size and broader demographic stratification to assess the generalizability of this technique.
Compared with uncontrast CMRA using TFE and mDixon sequences, the BTFE-based approach demonstrated sig
| 1. | Virani SS, Alonso A, Aparicio HJ, Benjamin EJ, Bittencourt MS, Callaway CW, Carson AP, Chamberlain AM, Cheng S, Delling FN, Elkind MSV, Evenson KR, Ferguson JF, Gupta DK, Khan SS, Kissela BM, Knutson KL, Lee CD, Lewis TT, Liu J, Loop MS, Lutsey PL, Ma J, Mackey J, Martin SS, Matchar DB, Mussolino ME, Navaneethan SD, Perak AM, Roth GA, Samad Z, Satou GM, Schroeder EB, Shah SH, Shay CM, Stokes A, VanWagner LB, Wang NY, Tsao CW; American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee. Heart Disease and Stroke Statistics-2021 Update: A Report From the American Heart Association. Circulation. 2021;143:e254-e743. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4769] [Cited by in RCA: 4006] [Article Influence: 801.2] [Reference Citation Analysis (4)] |
| 2. | Lu H, Miao X, Wang D, Zheng X, Zhang S, Wang R, Li G, Qian X, Chen Y, Hu C, Jin H, Zeng M. Feasibility and Clinical Application of 5-T Noncontrast Dixon Whole-Heart Coronary MR Angiography: A Prospective Study. Radiology. 2024;313:e240389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 10] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 3. | Dweck MR, Puntman V, Vesey AT, Fayad ZA, Nagel E. MR Imaging of Coronary Arteries and Plaques. JACC Cardiovasc Imaging. 2016;9:306-316. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 59] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 4. | Rahsepar AA, Kim D. Advancing Cardiovascular Imaging: The Promise of High-Field-Strength MRI in Coronary Artery Disease Assessment. Radiology. 2024;313:e242499. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 5. | Zhou Z, Wei D, Azhe S, Fu C, Zhou X, An J, Piccini D, Bastiaansen J, Guo Y, Wen L. Self-navigated coronary MR angiography for coronary aneurysm detection in Kawasaki disease at 3T: comparison with conventional diaphragm-navigated coronary MR angiography. Eur Radiol. 2024;34:3400-3410. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 6. | Pahlavan PS, Niroomand F. Coronary artery aneurysm: a review. Clin Cardiol. 2006;29:439-443. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 163] [Cited by in RCA: 148] [Article Influence: 7.4] [Reference Citation Analysis (4)] |
| 7. | Liu X, Zhao X, Huang J, Francois CJ, Tuite D, Bi X, Li D, Carr JC. Comparison of 3D free-breathing coronary MR angiography and 64-MDCT angiography for detection of coronary stenosis in patients with high calcium scores. AJR Am J Roentgenol. 2007;189:1326-1332. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 65] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 8. | Hajhosseiny R, Bustin A, Munoz C, Rashid I, Cruz G, Manning WJ, Prieto C, Botnar RM. Coronary Magnetic Resonance Angiography: Technical Innovations Leading Us to the Promised Land? JACC Cardiovasc Imaging. 2020;13:2653-2672. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 43] [Article Influence: 7.2] [Reference Citation Analysis (0)] |
| 9. | Kourtidou S, Jones MR, Moore RA, Tretter JT, Ollberding NJ, Crotty EJ, Rattan MS, Fleck RJ, Taylor MD. mDixon ECG-gated 3-dimensional cardiovascular magnetic resonance angiography in patients with congenital cardiovascular disease. J Cardiovasc Magn Reson. 2019;21:52. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 23] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 10. | Kaul MG, Stork A, Bansmann PM, Nolte-Ernsting C, Lund GK, Weber C, Adam G. Evaluation of balanced steady-state free precession (TrueFISP) and K-space segmented gradient echo sequences for 3D coronary MR angiography with navigator gating at 3 Tesla. Rofo. 2004;176:1560-1565. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 35] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 11. | Nezafat M, Henningsson M, Ripley DP, Dedieu N, Greil G, Greenwood JP, Börnert P, Plein S, Botnar RM. Coronary MR angiography at 3T: fat suppression versus water-fat separation. MAGMA. 2016;29:733-738. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 20] [Cited by in RCA: 27] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 12. | Lu H, Zhao S, Tian D, Yang S, Ma J, Chen Y, Ge M, Zeng M, Jin H. Clinical Application of Non-Contrast-Enhanced Dixon Water-Fat Separation Compressed SENSE Whole-Heart Coronary MR Angiography at 3.0 T With and Without Nitroglycerin. J Magn Reson Imaging. 2022;55:579-591. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 12] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 13. | Lu H, Guo J, Zhao S, Yang S, Ma J, Ge M, Chen Y, Zeng M, Jin H. Assessment of Non-contrast-enhanced Dixon Water-fat Separation Compressed Sensing Whole-heart Coronary MR Angiography at 3.0 T: A Single-center Experience. Acad Radiol. 2022;29 Suppl 4:S82-S90. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 12] [Reference Citation Analysis (0)] |
| 14. | Zhao SH, Li CG, Chen YY, Yun H, Zeng MS, Jin H. Applying Nitroglycerin at Coronary MR Angiography at 1.5 T: Diagnostic Performance of Coronary Vasodilation in Patients with Coronary Artery Disease. Radiol Cardiothorac Imaging. 2020;2:e190018. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 8] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 15. | Yuan Y, Jiang Y, Lu GM, Jin D, Chen WB, Wang B, Chen T, Hu Q, Zhu J, Zhao Y. Performance of 3-T Nonenhanced Whole-Heart bSSFP Coronary MR Angiography: A Comparison with 3-T Modified Dixon Water-Fat Separation Sequence. Radiol Cardiothorac Imaging. 2025;7:e240162. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 16. | He Y, Pang J, Dai Q, Fan Z, An J, Li D. Diagnostic Performance of Self-navigated Whole-Heart Contrast-enhanced Coronary 3-T MR Angiography. Radiology. 2017;283:923. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 17. | Yang Q, Li K, Liu X, Du X, Bi X, Huang F, Jerecic R, Liu Z, An J, Xu D, Zheng H, Fan Z, Li D. 3.0T whole-heart coronary magnetic resonance angiography performed with 32-channel cardiac coils: a single-center experience. Circ Cardiovasc Imaging. 2012;5:573-579. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 39] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 18. | Sternheim D, Power DA, Samtani R, Kini A, Fuster V, Sharma S. Myocardial Bridging: Diagnosis, Functional Assessment, and Management: JACC State-of-the-Art Review. J Am Coll Cardiol. 2021;78:2196-2212. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 170] [Article Influence: 34.0] [Reference Citation Analysis (0)] |
| 19. | Heer T, Reiter S, Trißler M, Höfling B, von Knobelsdorff-Brenkenhoff F, Pilz G. Effect of Nitroglycerin on the Performance of MR Coronary Angiography. J Magn Reson Imaging. 2017;45:1419-1428. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 11] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 20. | Rajiah PS, François CJ, Leiner T. Cardiac MRI: State of the Art. Radiology. 2023;307:e223008. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 112] [Reference Citation Analysis (8)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/