Published online Apr 26, 2026. doi: 10.4330/wjc.v18.i4.117928
Revised: January 14, 2026
Accepted: March 9, 2026
Published online: April 26, 2026
Processing time: 116 Days and 15 Hours
Heart failure (HF) is prevalent worldwide; however, due to the absence of a dedicated monitoring system in India, an adequate assessment of epidemiological trends in HF remains unaccomplished. Determining the profile of patients with HF facilitates early detection and therapy, minimising the disease burden.
To describe the demographics, clinical characteristics, haematological and bio
This was an observational study conducted between May 2019 and December 2020 at a tertiary-care institution in North India. Consecutive adult patients with clinically stable chronic HF were enrolled. Demographic characteristics, clinical features, laboratory parameters, electrocardiographic findings, echocardiographic data, and HF etiology were recorded using a standardised questionnaire.
This study enrolled a total of 407 chronic HF patients with a mean age of 58.8 years, 64.4% of whom were male. The mean left ventricular ejection fraction was 38.47%. Ischemic heart disease is the leading cause of HF, accounting for 53.6% of the population. Diabetes was the most prevalent linked co-morbidity (28.6%), followed by hypertension (21.5%). The majority of individuals had HF with reduced ejection fraction (58.5%), and the most frequent pre
HF in this cohort occurred at a younger age and was predominantly ischemic in etiology, with most patients having HF with reduced ejection fraction. Despite reasonable guideline-directed medical therapy prescription rates, suboptimal dosing and low uptake of newer therapies highlight the need for structured HF care and im
Core Tip: Heart failure (HF) in India represents a growing public health challenge, affecting patients at a younger age and predominantly driven by ischemic heart disease. In this hospital-based study from North India, most patients had HF with reduced ejection fraction and a high burden of diabetes and hypertension. Although prescription rates of guideline-directed medical therapy were relatively high, only 64% of patients received all three foundational HF drugs, and uptake of newer therapies such as angiotensin receptor-neprilysin inhibitors was low. These findings highlight critical gaps in surveillance, early risk factor control, and optimisation of evidence-based HF care in India.
- Citation: Gailson L, Singh A, Pradhan A, Prajapathi S, Choudhary R, Bhandari M, Vishwakarma P, Shukla A, Sharma A, Chaudhary G, Chandra S, Sethi R, Dwivedi SK. Demographic and clinical profile of patients with heart failure at a tertiary care hospital. World J Cardiol 2026; 18(4): 117928
- URL: https://www.wjgnet.com/1949-8462/full/v18/i4/117928.htm
- DOI: https://dx.doi.org/10.4330/wjc.v18.i4.117928
Heart failure (HF) is a pervasive disease whose prevalence is projected to increase by 25% over the next two decades due to an ageing population and improved detection and treatment of acute cardiovascular events[1,2]. According to the Global Health Data Exchange registry, the current global prevalence of HF is 64.34 million cases, which accounts for 9.91 million years lost due to disability and 346.17 billion United States dollars in expenditures[3]. Based on left ventricular ejection fraction (LVEF), natriuretic peptide levels, and indications of cardiac structural and/or functional abnormalities and diastolic dysfunction, the European Society of Cardiology (ESC) Guidelines 2021 have divided HF into three subtypes[4]. Due to the presence of different demographics, etiologies, and co-morbidities, optimal care of HF patients requires classification based on LVEF. Globally, ischemic heart disease (IHD) was identified as the leading cause of HF (42.3%), followed by chronic obstructive pulmonary disease (37%), mitral valve disease (4.3%), aortic valve disease (3.4%), rheumatic heart disease (RHD) (3%), myocarditis (2.6%), and endocarditis (1.4%)[3]. If people with these disorders were detected, identified, and treated at an earlier stage, HF could be prevented.
In contrast to the Western world, India’s epidemiological data on HF are limited, with no large-scale investigations examining the burden of HF. Only a handful of hospital-based registries provide data on HF, such as the Trivandrum Heart Failure Registry (THFR)[5], Acute Failure Registry[6], Manipal Heart Failure Registry[7], Registry of Heart Failure at Medanta (Med-HFR)[8], India Ukieri Study[9], Heart Failure and Pan-arrhythmia Registry[10], the Srirama Chandra Bhanja Medical College Registry[11], and the International Congestive Heart Failure Registry[12]. Huffman and Prabhakaran[13] estimated that the prevalence of HF in India ranges from 1.3 million to 4.6 million (0.12% to 0.44%), with an incidence of 0.5 million per year to 1.8 million per year (0.05% to 0.17%), which may be an underestimation. In addition, there is no HF-specific surveillance mechanism in India. For the optimal allocation of healthcare resources and the reduction of disease burden, an accurate assessment of epidemiologic trends in HF is crucial. Consequently, the purpose of this study was to: (1) Describe the demographics and clinical characteristics; (2) Identify the various causes of HF; (3) Describe the haematological and biochemical parameters; (4) Electrocardiogram (ECG) findings; and (5) Echocardiogram findings in patients with HF in India.
This observational study was conducted between May 2019 and December 2020 at a tertiary-care institution in North India. Prior to the trial, written informed consent was obtained from all study participants. Consecutive adult patients (≥ 18 years) with an established diagnosis of chronic HF who were clinically stable at presentation were prospectively enrolled. Patients with acute decompensated HF, cardiogenic shock, recent hospitalisation for HF within the preceding four weeks, severe valvular heart disease requiring immediate surgical or interventional correction, and advanced non-cardiac terminal illnesses (e.g., advanced chronic kidney disease requiring dialysis, active malignancy with limited life expectancy) were excluded. Patients unwilling to provide informed consent were also excluded. Data were collected using a structured, standardised questionnaire designed for this study, incorporating routinely used variables in HF registries, including demographic characteristics, clinical features, co-morbidities, laboratory parameters, electrocardiographic findings, echocardiographic measurements, and HF aetiology. The questionnaire served as a data capture tool for objective clinical variables and was completed by trained physicians.
Sample size was calculated based on an expected prevalence of 62% derived from the THFR and an absolute precision of 5%. For a 95% confidence interval and a two-tailed test, the minimum required sample size was 362 patients. To account for exclusions and missing data, a target sample size of approximately 400 patients was deemed adequate. A total of 407 consecutive eligible patients were ultimately enrolled during the study period[14]. Chronic HF was diagnosed according to ESC guideline recommendations. Diagnosis required the presence of typical HF symptoms and/or signs, together with objective evidence of cardiac structural and/or functional abnormality on transthoracic echocardiography. N-terminal pro B-type natriuretic peptide (NT-proBNP) levels were used as supportive biomarkers where available. Patients were subsequently classified according to LVEF into HF with reduced (HFrEF), mildly reduced (HFmrEF), or preserved ejection fraction (HFpEF), in accordance with ESC guidelines[15].
Statistical analysis was performed using STATA version 12. Continuous variables are presented as mean ± SD or median (range), as appropriate, and categorical variables as n (%). Comparisons of continuous variables between HF phenotypes (HFrEF, HFmrEF, and HFpEF) were performed using one-way analysis of variance (ANOVA) for normally distributed data and the Kruskal-Wallis test for non-normally distributed data. A two-sided P-value < 0.05 was considered statistically significant.
During the study period, a total of 407 chronic HF patients were enrolled in our study. The mean age of the cohort was 58.8 years, with 262 males (64.4% of the group) and 145 females (35.6%). The comparison of demographic, clinical, haematological, and biochemical factors with other international registries[16-18] is shown in Table 1. The subjects’ mean ± SD heart rate was 91.19 ± 14.92 beats per minute, and their mean ± SD systolic and diastolic blood pressures were 122.37 ± 21.04 and 76.71 ± 11.54, respectively. Diabetes mellitus (DM) was the most prevalent comorbidity, present in 28.6% of patients (n = 117), encompassing both isolated diabetes and diabetes occurring in combination with other comorbidities; hypertension was the next most common comorbidity (21.5%, n = 88). The majority of the subjects presented with dyspnoea and belonged to New York Heart Association Class II (69%), followed by Class I (26.5%) and Class III (1.7%). Other symptoms and indicators included nocturnal cough, palpitations, orthopnea, basal rales, ankle edema, and pleural effusion.
| Parameter | King George’s Medical University (n = 407) | United States acute decompensated HF national registry (n = 105388) | Swedish HF registry (S-HFR PHC) (n = 631) | Italian registry on HF (n = 5610) |
| Mean age (years) | 58.8 | 72.4 | 76 | 72 |
| Male (%) | 64.4 | 48 | 56 | 60.2 |
| Female (%) | 35.6 | 52 | 44 | 39.8 |
| Mean heart rate (beats/minute) | 91.19 | NA | 73 | 93 |
| Mean SBP (mmHg) | 122.37 | 144 | < 100 (2.9%); 100-140 (63.8%); > 140 (33.3%) | 134 |
| Mean DBP (mmHg) | 76.71 | NA | NA | NA |
| HF phenotype distribution | HFmrEF: 25.6%; HFpEF: 16.0%; HFrEF: 58.5% | Mean EF: 34.4% | EF < 30%: 25%; EF 30%-40%: 23%; EF 40%-49%: 17%; EF ≥ 50%: 18% | HFpEF: 35% |
| Co-morbidities (%) | DM (overall): 28.6%; DM (isolated): 18.1%; HTN (overall): 21.5%; HTN + DM: 10.3%; HTN (isolated): 9.8%; HTN + CKD: 1.2%; CKD: 0.5%; HTN + DM + CKD: 0.2%; others: 3.2% | HTN: 73%; CAD: 57%; DM: 44%; MI: 31%; AF: 31%; renal insufficiency: 30%; VT: 8%; VF: 1% | IHD: 43.3%; AF: 43.3%; HTN: 51.5%; DM: 26.5%; valve disease: 11%; pulmonary disease: 30.3%; DCM: 4%; HCM: 0.3% | IHD: 42.3%; HTN: 57.8%; DM: 40.4%; renal dysfunction: 32.5%; AF: 37.7% |
| NYHA class (%) | I: 26.5; II: 69.0; III: 1.7; IV: - | I: 20; II: 44; III: 32; IV: NA | I: 8; II: 32; III: 28; IV: 4 | NA |
| Clinical features (%) | Major: Acute pulmonary edema (0.2%), rales (0.2%); minor: DOE (10.3%), DOE + ankle edema (0.5%), nocturnal cough (0.5%), ankle edema (0.2%), DOE + pleural effusion (0.2%) | Peripheral edema: 66%; dyspnea: 89%; rales: 68% | NA | Pulmonary congestion: 78.2%; peripheral congestion: 56.1%; either/both: 88.4%; peripheral hypoperfusion: 12%; cold: 10.8%; altered sensorium: 11.5% |
| Mean hemoglobin (g/dL) | 12.01 | NA | 13.5 | 12.5 |
| Serum creatinine (mg/dL) | 1.19 | 1.8; > 2: 21%; > 3: 9% | 1.157 | 1.21; > 1.5: 28.7% |
| RDW (%) | 16.49 | NA | NA | NA |
| NT-proBNP (pg/mL) | mean: 3377.39; HFrEF: 3926.88; HFpEF: 2745.73; HFmrEF: 2707.94 | NA | NA | 51681 |
IHD (53.6%; n = 218) and idiopathic dilated cardiomyopathy (34.2%; n = 139) were the two most prevalent causes of HF. Other causes were peripartum cardiomyopathy (2%), RHD (2%), non-rheumatic valvular heart disease (0.5%), che
| Modality | Parameter | Findings |
| ECG | Heart rhythm | Sinus rhythm: 95.6%; atrial fibrillation: 4.4% |
| Conduction abnormalities | Poor R-wave progression: 48.7%; LBBB: 21.1%; LAHB + RBBB: 10.2%; RBBB: 7.6% | |
| LBBB | Present: 2.2%; absent: 97.8% | |
| LVH | Present: 3.7%; absent: 96.3% | |
| ECHO | LVDD | Mild: 40.3%; moderate: 11.5%; severe: 0.7%; absent: 47.4% |
| Mitral regurgitation | Mild: 33.7%; moderate: 14.7%; severe: 11.1%; absent: 40.5% | |
| Tricuspid regurgitation | Mild: 27.5%; moderate: 9.1%; severe: 2.9%; absent: 60.4% | |
| RWMA | Present: 43%; absent: 57% | |
| LVEF | Mean LVEF: 38.47% | |
| FS | Mean: 19.32% | |
| LV dimensions | LVESD: 4.37 cm; LVEDD: 5.34 cm | |
| Left atrial size | Diameter 1: 4.49 cm; diameter 2: 4.22 cm |
The distribution of guideline-directed medical therapy (GDMT) prescriptions, including angiotensin-converting enzyme inhibitors (ACEIs), angiotensin receptor blockers (ARBs), aldosterone antagonists, angiotensin receptor-neprilysin inhibitor (ARNI), and beta blockers, is presented in Table 3. The most prescribed ACEI/ARB was ramipril (68.8%), followed by telmisartan (8.11%) and perindopril (3.19%), respectively. A cumulative of 325 (79.85%) out of 407 patients were on any ACEI/ARB. ARNI was prescribed to only 6.6% patients. Carvedilol (45.7%) and metoprolol (44.7%) were the most commonly prescribed β-blockers. About 368 (90.42%) of 407 patients were on any beta-blocker. Spironolactone was the most commonly prescribed mineralocorticoid receptor antagonist (MRA), and 335 (82.33%) of 407 patients were on any MRA. Sixty-four per cent of patients were prescribed GDMT (defined as any dose of all 3 pillars - ACE/ARB, beta-blocker and MRA). The distribution of doses of GDMT prescribed to the study population is summarised in Table 4.
| Population (n = 407) | n (%) |
| ACEI/ARB | 325 (79.85) |
| Ramipril | 280 (68.8) |
| Telmisartan | 33 (8.11) |
| Perindopril | 12 (2.94) |
| ARNI | 27 (6.63) |
| BB | 368 (90.42) |
| Metoprolol | 182 (44.7) |
| Carvedilol | 186 (45.7) |
| MRA | 335 (82.31) |
| Spironolactone | 277 (68.05) |
| Eplerenone | 58 (14.25) |
| GDMT (All 3 of ACE/ARB, BB and MRA) | 260 (63.8) |
| Drugs dose (mg/day) | mean ± SD | Median | Min | Max |
| Perindopril | 2.77 ± 1.01 | 2 | 2 | 4 |
| Ramipril | 2.86 ± 1.16 | 2.5 | 1.25 | 7.5 |
| Telmisartan | 36.97 ± 16.67 | 40 | 20 | 80 |
| Sacubitril valsartan | 88.89 ± 57.74 | 50 | 50 | 200 |
| Carvedilol | 6.4 ± 5.7 | 3.12 | 3.12 | 25 |
| Metoprolol | 50 ± 15.77 | 50 | 25 | 100 |
| Torsemide | 18.51 ± 4.08 | 20 | 5 | 50 |
| Spironolactone | 49.3 ± 4.14 | 50 | 25 | 50 |
| Furosemide | 17.69 ± 4.39 | 20 | 10 | 20 |
| Eplerenone | 25 ± 0 | 25 | 25 | 25 |
This hospital-based observational study provides important insights into the demographic and clinical profile of patients with chronic HF in India. A key and consistent finding is the younger mean age of HF patients compared with Western registries, a pattern also observed in other Indian and Asian cohorts. The mean age of the study population was 58.8 years, which is nearly identical to the mean ages of the THFR[5], Med-HFR[8], and India Ukieri Study[9] studies, which were 61.2 years, 59.1 years, and 58.3 years, respectively. Compared to other similar global studies involving patients with HF, the average age of the participants in this study was younger[16-20].
The younger age of HF presentation in India is likely multifactorial. First, the earlier onset and aggressive course of coronary artery disease in South Asian populations is well documented. Indians develop coronary artery disease nearly a decade earlier than Western populations, often with more extensive and diffuse disease, predisposing them to earlier ischemic cardiomyopathy and HF[21-23]. This is reflected in our cohort, where IHD accounted for over half of HF cases. Second, although RHD represented a smaller proportion of HF etiology in our study, its long-term sequelae continue to contribute to HF at a younger age in India. Inadequate early detection and delayed access to valve interventions allow progressive myocardial remodelling and eventual HF, particularly in socioeconomically disadvantaged populations[24,25]. Third, poor control of cardiovascular risk factors, particularly hypertension and diabetes, remains an important contributor. While the prevalence of these comorbidities in our cohort was lower than that reported in Western registries, national data indicate significant underdiagnosis, low treatment adherence, and poor long-term control in India[26,27]. Prolonged exposure to uncontrolled risk factors accelerates myocardial dysfunction, leading to HF at a younger age. Finally, delayed healthcare-seeking behaviour and limited access to specialized care play a significant role. Financial constraints, lack of symptom awareness, and uneven distribution of cardiac services often result in late presentation, when structural myocardial damage is already advanced[9,12,28]. This delayed diagnosis may explain why HF manifests at a younger chronological age but with significant disease severity. The majority of our study’s participants were male (64.4%). This is comparable to other studies, in which a greater number of patients were male: 83% in Med-HFR[8], 78.2% in the Asian Heart Failure Registry (AHFR)[17], 71.2% in the ESC HF Long-Term Registry[17], and 69.2% in the THFR[5].
In patients with HF, the presence of co-morbidities is another aspect that must be considered. DM increases the incidence of HF and adversely affects patient outcomes[29]. In our study, co-morbidities such as diabetes and hyper
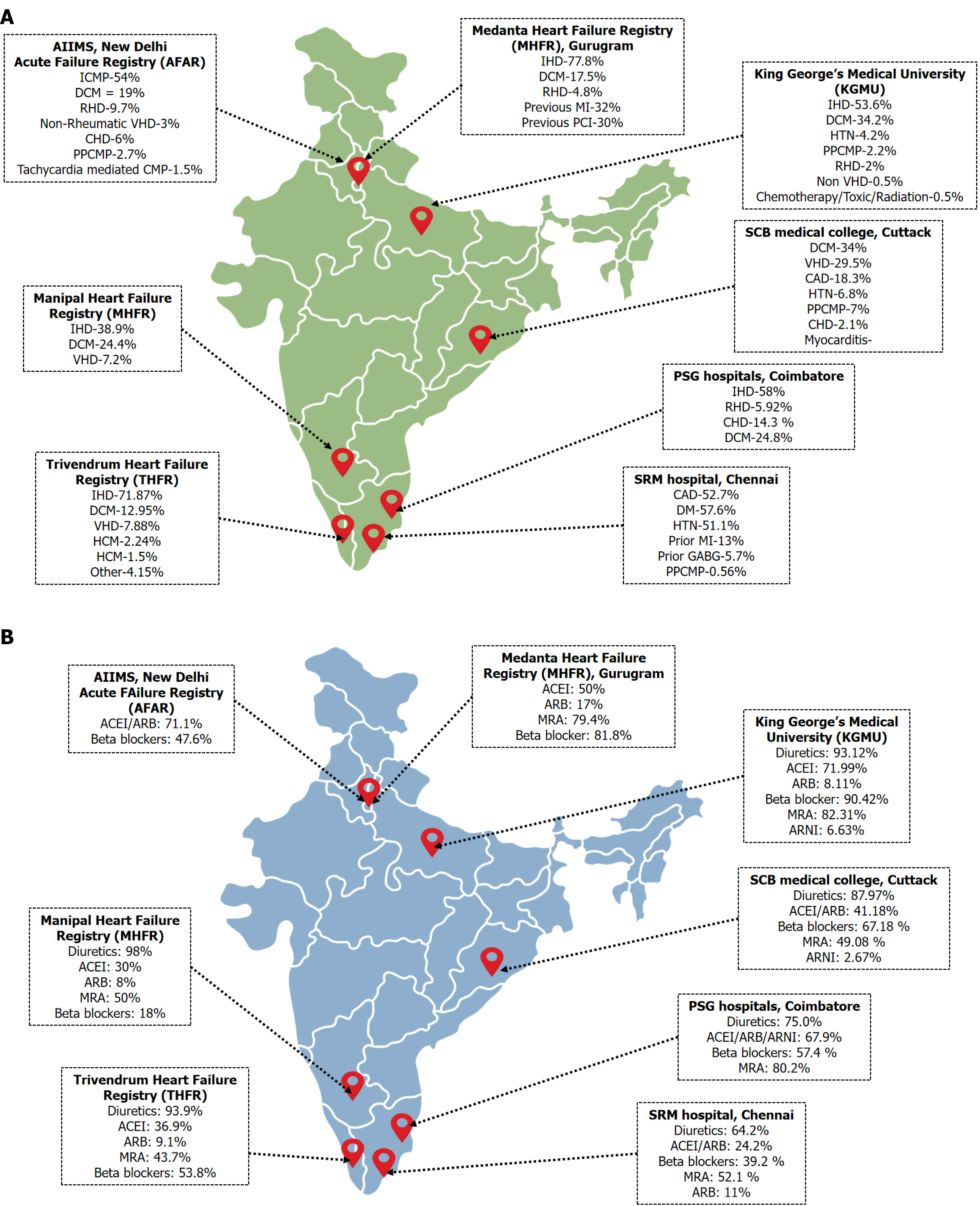
Identification of the etiology of HF, such as the underlying cardiac condition, is critical since it influences the therapeutic path. IHD was found to be the leading cause of HF, affecting 53.6% of the population, followed by idiopathic dilated cardiomyopathy (34.2%). Only 2% of individuals had HF as a result of RHD. IHD was also the leading cause of HF in other studies[5-8], contributing to a substantial number of HF cases in India. In contrast, Mishra et al[11] showed that dilated cardiomyopathy was present in 34% of cases, valvular heart disease was present in 29.5% of cases, and coronary artery disease was present in 18.3% of cases. Consistent with other Indian registries, the majority of patients in our study had HF with reduced ejection fraction (HFrEF). This predominance likely reflects the high burden of ischemic cardiomyopathy and delayed diagnosis of HF. Patients with HFpEF and HFmrEF may remain underdiagnosed due to nonspecific symptoms and limited access to advanced echocardiographic assessment, leading to underrepresentation in hospital-based cohorts. Figure 1A depicts the epidemiological profile of HF in India.
In order to evaluate the therapeutic response and long-term stability of patients with HF, it is crucial to evaluate their symptoms and signs. Signs such as elevated JVP, the hepatojugular reflex, the third heart sound, and lateral displacement of the apical impulse are more specific[4,30]. In individuals with obesity, advanced age, and chronic lung illness, it may be difficult to elicit symptoms and signs[15]. The persistence of symptoms despite treatment signals the need for further treatment, whereas the deterioration of symptoms necessitates prompt medical attention. In the present study, the most prevalent presenting symptom was dyspnea on exertion, classified as New York Heart Association Class II (69%). Other signs and symptoms, like bilateral ankle oedema, raised JVP, orthopnea, rales, and nocturnal cough, were less common. In comparison to prior studies[6,19,21], however, the symptoms and signs of HF were insufficient for its diagnosis; further tests, such as laboratory studies and cardiac imaging, were needed[1].
In conjunction with a clinical examination, biomarkers can provide more diagnostic precision than clinical examination alone. Natriuretic peptides are one of the most effective biomarkers for diagnosing HF. According to the American College of Cardiology/American Heart Association[31], HF may be prevented by natriuretic peptide screening and early management. Mant et al[32] found from a meta-analysis that BNP or NT-proBNP should be preferred over the ECG for the diagnosis of HF. To exclude HF, the 2021 ESC guideline proposes a cutoff of 35 pg/mL for BNP and 125 pg/mL for NT-proBNP in non-acute settings. In our study, nearly all patients showed elevated NT-proBNP, with a mean of 3377.39 pg/mL, which is much lower than IN-HFR (5168 pg/mL)[21]. It was observed that periodic measurement of NT-proBNP concentration is a better approach for risk stratification in patients with chronic and stable HF[33].
The latest ESC 2021 Guideline suggests renaming “HF with mid-range ejection fraction” to “HF with mildly reduced ejection fraction”. The majority of the individuals in our study had HFrEF (58.5%), followed by HFmrEF (25.6%) and HFpEF (16%)[4]. They propose a 12-lead ECG in all patients with chronic HF to evaluate the heart rhythm, heart rate, and to detect any cardiac abnormalities, allowing for treatment planning and patient monitoring 4.12% and 13.9% of participants in the AHFR were found to have AF and LBBB, respectively, compared to 4.4% and 21.1% in our study[18]. ECG recordings in the IN-HFR revealed 31.5% AF and 11% LBBB in patients with deteriorating HF, compared to 6.9% LBBB in individuals with newly diagnosed HF[21]. They demonstrated significant mitral regurgitation in 22.9% of cases, compared to 11.1% in our analysis. In the Swedish Heart Failure Registry, 38% had AF[20]. Echocardiography is the preferred diagnostic tool for patients suspected of having HF. In our study, the mean left ventricular end-systolic diameter and left ventricular end-diastolic diameter (LVEDD) were comparatively less (4.37 cm and 5.34 cm, respec
The use of GDMT in HF significantly reduces morbidity and mortality. However, despite strong evidence, the majority of patients do not receive or are not able to achieve the target dose of GDMT. The guidelines recommend ACEI/ARB/ARNI + beta blockers + MRAs in all HF patients. The latest guidelines also recommend sodium-glucose cotransporter 2 inhibitors, which are collectively known as the four pillars of HF management.
In our study, the percentages of patients who received diuretics, ACEI, ARB, MRAs, ARNI, and beta blockers were 93.12%, 71.99%, 8.11%, 82.31%, 6.63%, and 90.42%, respectively. A similar trend was seen in the Trivandrum HF study, where the percentages of patients who had received diuretics, ACEI, ARB, MRAs and beta blockers or treatment were 93.9%, 36.9%, 9.1%, 43.7% and 53.8%, respectively[5]. The respective percentages were 98%, 30%, 8%, 50%, and 18% in the group with reduced ejection fraction and 94%, 22%, 13%, 52%, and 11% in the group with preserved ejection fraction in the Manipal HF study[7]. The 63.88% of our patients received optimal guideline recommended therapy compared to only 21.41% in the Trivandrum HF registry. Although prescription rates of GDMT were relatively high compared with some Indian registries, substantial gaps remain in achieving target doses and adopting newer therapies. These gaps are influenced by cost, drug availability, tolerability, and limited structured follow-up for dose titration[34,35]. The younger age of HF onset further magnifies the economic and societal burden, as patients are often affected during their most productive years. Details of treatment in other HF registries are described in Table 3 and Figure 1B.
The Asian HF registry demonstrated a dose-dependent improvement in a 1-year composite outcome with adherence to GDMT[23]. The drugs that constitute guideline-based therapy have individually been shown to have a clear mortality benefit in HF through systematic review and meta-analysis of various well-designed, adequately powered randomised controlled trials. Since only 63.88% of patients were prescribed guideline-based therapy in our study, there is still a need to improve management and outcomes in patients with HF in our country.
The median prescribed dose for ACEI was around 25% of the guideline-recommended dose. For carvedilol and Metoprolol, the rates were roughly 12.5% and 25%, respectively. However, 13% of patients received more than 50% of the guideline-recommended doses. The reduced proportion of patients achieving target doses of guideline-recommended ACE inhibitors in our study compared with European cohorts is likely multifactorial. While a higher prevalence of ACE inhibitor-associated cough reported among Asian populations may contribute to early discontinuation or dose limitation[36], other systemic factors also play a substantial role. These include limited drug affordability and availability, absence of structured follow-up systems for systematic dose titration, challenges with long-term patient adherence, and physician-related factors such as therapeutic inertia and delays in the adoption of evolving guideline recommendations[23]. Together, these real-world constraints likely explain the persistent gap between prescription rates and achievement of target doses in routine HF care.
In our cohort, the prescription rates of foundational agents were encouraging compared to some Indian registries; yet, important gaps remain in the optimisation and uptake of newer therapies. In the Candesartan in Heart failure Asse
As a single-centre, hospital-based study, the generalizability may be limited. The lack of follow-up data and multivariate analyses restricts prognostic inference. The use of sodium-glucose cotransporter-2 inhibitors and vericiguat is minimal, as they were not approved for HF by licensing authorities during the study. ARNI was approved, though it was not off-patent, and hence generic versions were not available, limiting their use. Nevertheless, the study provides valuable real-world evidence on HF characteristics in India and identifies critical targets for prevention and healthcare planning.
This study demonstrates that HF in India affects patients at a younger age, is predominantly driven by IHD, and is characterized by a high burden of HFrEF. Although prescription rates of GDMT were substantial, achievement of target doses and uptake of newer therapies remain suboptimal. These findings call for structured HF care models that emphasize systematic GDMT titration and regular follow-up. At a public health level, the early onset of HF underscores the urgency of aggressive cardiovascular risk factor prevention and improved access to affordable evidence-based therapies. Future efforts should prioritize prospective multicenter studies and a national HF registry to inform policy, guide resource allocation, and improve outcomes in India.
| 1. | Metra M, Teerlink JR. Heart failure. Lancet. 2017;390:1981-1995. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 391] [Cited by in RCA: 496] [Article Influence: 55.1] [Reference Citation Analysis (4)] |
| 2. | Savarese G, Lund LH. Global Public Health Burden of Heart Failure. Card Fail Rev. 2017;3:7-11. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2169] [Cited by in RCA: 1866] [Article Influence: 207.3] [Reference Citation Analysis (1)] |
| 3. | Lippi G, Sanchis-gomar F. Global epidemiology and future trends of heart failure. AME Med J. 2020;5:15-15. [DOI] [Full Text] |
| 4. | McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, Böhm M, Burri H, Butler J, Čelutkienė J, Chioncel O, Cleland JGF, Coats AJS, Crespo-Leiro MG, Farmakis D, Gilard M, Heymans S, Hoes AW, Jaarsma T, Jankowska EA, Lainscak M, Lam CSP, Lyon AR, McMurray JJV, Mebazaa A, Mindham R, Muneretto C, Francesco Piepoli M, Price S, Rosano GMC, Ruschitzka F, Kathrine Skibelund A; ESC Scientific Document Group. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J. 2021;42:3599-3726. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10992] [Cited by in RCA: 9188] [Article Influence: 1837.6] [Reference Citation Analysis (4)] |
| 5. | Harikrishnan S, Sanjay G, Anees T, Viswanathan S, Vijayaraghavan G, Bahuleyan CG, Sreedharan M, Biju R, Nair T, Suresh K, Rao AC, Dalus D, Huffman MD, Jeemon P; Trivandrum Heart Failure Registry. Clinical presentation, management, in-hospital and 90-day outcomes of heart failure patients in Trivandrum, Kerala, India: the Trivandrum Heart Failure Registry. Eur J Heart Fail. 2015;17:794-800. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 85] [Cited by in RCA: 104] [Article Influence: 9.5] [Reference Citation Analysis (0)] |
| 6. | Seth S, Khanal S, Ramakrishnan S, Gupta N, Bahl V. Epidemiology of acute decompensated heart failure in India : The AFAR study (Acute failure registry study). J Pract Cardiovasc Sci. 2015;1:35. [RCA] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 12] [Article Influence: 1.1] [Reference Citation Analysis (1)] |
| 7. | Singh A, Chauhan S, Devasia T, Karkala YR, Paramasivam G, Shetty PN, Uppunda D, Kareem H. Financial burden of heart failure in a developing country: cost analysis from Manipal Heart Failure Registry, India. J Public Health (Berl). 2021;29:585-594. [RCA] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 16] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 8. | Chopra VK, Mittal S, Bansal M, Singh B, Trehan N. Clinical profile and one-year survival of patients with heart failure with reduced ejection fraction: The largest report from India. Indian Heart J. 2019;71:242-248. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 20] [Article Influence: 2.9] [Reference Citation Analysis (1)] |
| 9. | Chaturvedi V, Parakh N, Seth S, Bhargava B, Ramakrishnan S, Roy A, Saxena A, Gupta N, Misra P, Rai S, Anand K, Pandav C, Sharma R, Prasad S. Heart failure in India: The INDUS (INDia Ukieri Study) study. J Pract Cardiovasc Sci. 2016;2:28. [RCA] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 46] [Article Influence: 4.6] [Reference Citation Analysis (1)] |
| 10. | Vora A, Naik A, Lokhandwala Y, Chopra A, Varma J, Wander GS, Jaswal A, Srikanthan V, Singh B, Kahali D, Gupta A, Mantri RR, Mishra A, Pandurangi U, Ghosh D, Makkar JS, Sahu S, Radhakrishnan R. Profiling cardiac arrhythmia and heart failure patients in India: The Pan-arrhythmia and Heart Failure Observational Study. Indian Heart J. 2017;69:226-239. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 9] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 11. | Mishra TK, Das B, Routray S. Prevalence and short-term prognosis of heart failure: An in hospital prevalence study. J Indian Coll Cardiol. 2018;8:103-106. [RCA] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 12. | Dokainish H, Teo K, Zhu J, Roy A, AlHabib KF, ElSayed A, Palileo-Villaneuva L, Lopez-Jaramillo P, Karaye K, Yusoff K, Orlandini A, Sliwa K, Mondo C, Lanas F, Prabhakaran D, Badr A, Elmaghawry M, Damasceno A, Tibazarwa K, Belley-Cote E, Balasubramanian K, Yacoub MH, Huffman MD, Harkness K, Grinvalds A, McKelvie R, Yusuf S; INTER-CHF Investigators. Heart Failure in Africa, Asia, the Middle East and South America: The INTER-CHF study. Int J Cardiol. 2016;204:133-141. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 112] [Article Influence: 10.2] [Reference Citation Analysis (1)] |
| 13. | Huffman MD, Prabhakaran D. Heart failure: epidemiology and prevention in India. Natl Med J India. 2010;23:283-288. [PubMed] |
| 14. | Harikrishnan S, Jeemon P, Ganapathi S, Agarwal A, Viswanathan S, Sreedharan M, Vijayaraghavan G, Bahuleyan CG, Biju R, Nair T, Pratapkumar N, Krishnakumar K, Rajalekshmi N, Suresh K, Huffman MD. Five-year mortality and readmission rates in patients with heart failure in India: Results from the Trivandrum heart failure registry. Int J Cardiol. 2021;326:139-143. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 33] [Article Influence: 6.6] [Reference Citation Analysis (1)] |
| 15. | Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS, Falk V, González-Juanatey JR, Harjola VP, Jankowska EA, Jessup M, Linde C, Nihoyannopoulos P, Parissis JT, Pieske B, Riley JP, Rosano GMC, Ruilope LM, Ruschitzka F, Rutten FH, van der Meer P; ESC Scientific Document Group. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC)Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2016;37:2129-2200. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10909] [Cited by in RCA: 9411] [Article Influence: 941.1] [Reference Citation Analysis (4)] |
| 16. | Ibrahim NE, Song Y, Cannon CP, Doros G, Russo P, Ponirakis A, Alexanian C, Januzzi JL Jr. Heart failure with mid-range ejection fraction: characterization of patients from the PINNACLE Registry®. ESC Heart Fail. 2019;6:784-792. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 47] [Article Influence: 6.7] [Reference Citation Analysis (1)] |
| 17. | Crespo-Leiro MG, Anker SD, Maggioni AP, Coats AJ, Filippatos G, Ruschitzka F, Ferrari R, Piepoli MF, Delgado Jimenez JF, Metra M, Fonseca C, Hradec J, Amir O, Logeart D, Dahlström U, Merkely B, Drozdz J, Goncalvesova E, Hassanein M, Chioncel O, Lainscak M, Seferovic PM, Tousoulis D, Kavoliuniene A, Fruhwald F, Fazlibegovic E, Temizhan A, Gatzov P, Erglis A, Laroche C, Mebazaa A; Heart Failure Association (HFA) of the European Society of Cardiology (ESC). European Society of Cardiology Heart Failure Long-Term Registry (ESC-HF-LT): 1-year follow-up outcomes and differences across regions. Eur J Heart Fail. 2016;18:613-625. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 692] [Cited by in RCA: 609] [Article Influence: 60.9] [Reference Citation Analysis (3)] |
| 18. | Lam CS, Teng TK, Tay WT, Anand I, Zhang S, Shimizu W, Narasimhan C, Park SW, Yu CM, Ngarmukos T, Omar R, Reyes EB, Siswanto BB, Hung CL, Ling LH, Yap J, MacDonald M, Richards AM. Regional and ethnic differences among patients with heart failure in Asia: the Asian sudden cardiac death in heart failure registry. Eur Heart J. 2016;37:3141-3153. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 98] [Cited by in RCA: 144] [Article Influence: 14.4] [Reference Citation Analysis (1)] |
| 19. | Adams KF Jr, Fonarow GC, Emerman CL, LeJemtel TH, Costanzo MR, Abraham WT, Berkowitz RL, Galvao M, Horton DP; ADHERE Scientific Advisory Committee and Investigators. Characteristics and outcomes of patients hospitalized for heart failure in the United States: rationale, design, and preliminary observations from the first 100,000 cases in the Acute Decompensated Heart Failure National Registry (ADHERE). Am Heart J. 2005;149:209-216. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1466] [Cited by in RCA: 1496] [Article Influence: 71.2] [Reference Citation Analysis (4)] |
| 20. | Jonsson A, Edner M, Alehagen U, Dahlström U. Heart failure registry: a valuable tool for improving the management of patients with heart failure. Eur J Heart Fail. 2010;12:25-31. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 131] [Article Influence: 8.2] [Reference Citation Analysis (1)] |
| 21. | Oliva F, Mortara A, Cacciatore G, Chinaglia A, Di Lenarda A, Gorini M, Metra M, Senni M, Maggioni AP, Tavazzi L; IN-HF Outcome Investigators. Acute heart failure patient profiles, management and in-hospital outcome: results of the Italian Registry on Heart Failure Outcome. Eur J Heart Fail. 2012;14:1208-1217. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 96] [Cited by in RCA: 105] [Article Influence: 7.5] [Reference Citation Analysis (1)] |
| 22. | Pradhan A, Sharma P, Prajapathi S, Aracri M, Iellamo F, Perrone MA. Intensive Lipid-Lowering Therapy Following Acute Coronary Syndrome: The Earlier the Better. J Cardiovasc Dev Dis. 2025;12:300. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (1)] |
| 23. | Teng TK, Tromp J, Tay WT, Anand I, Ouwerkerk W, Chopra V, Wander GS, Yap JJ, MacDonald MR, Xu CF, Chia YM, Shimizu W; ASIAN-HF investigators, Richards AM, Voors A, Lam CS. Prescribing patterns of evidence-based heart failure pharmacotherapy and outcomes in the ASIAN-HF registry: a cohort study. Lancet Glob Health. 2018;6:e1008-e1018. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 139] [Article Influence: 19.9] [Reference Citation Analysis (1)] |
| 24. | Bhargav BRM, Sivasankaran S. Prevention and Control of Rheumatic Fever in India: An Achievable Health Target. Indian J Cardiovasc Dis Women. 2025;10:216-224. [DOI] [Full Text] |
| 25. | Negi PC, Sondhi S, Asotra S, Mahajan K, Mehta A. Current status of rheumatic heart disease in India. Indian Heart J. 2019;71:85-90. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 39] [Cited by in RCA: 35] [Article Influence: 5.0] [Reference Citation Analysis (1)] |
| 26. | Koya SF, Pilakkadavath Z, Chandran P, Wilson T, Kuriakose S, Akbar SK, Ali A. Hypertension control rate in India: systematic review and meta-analysis of population-level non-interventional studies, 2001-2022. Lancet Reg Health Southeast Asia. 2023;9:100113. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 33] [Article Influence: 11.0] [Reference Citation Analysis (1)] |
| 27. | Geldsetzer P, Manne-Goehler J, Theilmann M, Davies JI, Awasthi A, Vollmer S, Jaacks LM, Bärnighausen T, Atun R. Diabetes and Hypertension in India: A Nationally Representative Study of 1.3 Million Adults. JAMA Intern Med. 2018;178:363-372. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 169] [Cited by in RCA: 246] [Article Influence: 30.8] [Reference Citation Analysis (1)] |
| 28. | Haridoss M, Nandi D, Rajesh Lenin R, John SP, Anantharaman VV, Janardhanan R. Health-seeking behavior and its determinants for non-communicable diseases in India - a systematic review and meta-analysis. Front Public Health. 2025;13:1580824. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 29. | Benjamin EJ, Virani SS, Callaway CW, Chamberlain AM, Chang AR, Cheng S, Chiuve SE, Cushman M, Delling FN, Deo R, de Ferranti SD, Ferguson JF, Fornage M, Gillespie C, Isasi CR, Jiménez MC, Jordan LC, Judd SE, Lackland D, Lichtman JH, Lisabeth L, Liu S, Longenecker CT, Lutsey PL, Mackey JS, Matchar DB, Matsushita K, Mussolino ME, Nasir K, O'Flaherty M, Palaniappan LP, Pandey A, Pandey DK, Reeves MJ, Ritchey MD, Rodriguez CJ, Roth GA, Rosamond WD, Sampson UKA, Satou GM, Shah SH, Spartano NL, Tirschwell DL, Tsao CW, Voeks JH, Willey JZ, Wilkins JT, Wu JH, Alger HM, Wong SS, Muntner P; American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee. Heart Disease and Stroke Statistics-2018 Update: A Report From the American Heart Association. Circulation. 2018;137:e67-e492. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5445] [Cited by in RCA: 4934] [Article Influence: 616.8] [Reference Citation Analysis (2)] |
| 30. | Fonseca C, Morais H, Mota T, Matias F, Costa C, Gouveia-Oliveira A, Ceia F; EPICA Investigators. The diagnosis of heart failure in primary care: value of symptoms and signs. Eur J Heart Fail. 2004;6:795-800, 821. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 59] [Cited by in RCA: 59] [Article Influence: 2.7] [Reference Citation Analysis (1)] |
| 31. | Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE Jr, Colvin MM, Drazner MH, Filippatos GS, Fonarow GC, Givertz MM, Hollenberg SM, Lindenfeld J, Masoudi FA, McBride PE, Peterson PN, Stevenson LW, Westlake C. 2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of America. Circulation. 2017;136:e137-e161. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2303] [Cited by in RCA: 2028] [Article Influence: 225.3] [Reference Citation Analysis (4)] |
| 32. | Mant J, Doust J, Roalfe A, Barton P, Cowie MR, Glasziou P, Mant D, McManus RJ, Holder R, Deeks J, Fletcher K, Qume M, Sohanpal S, Sanders S, Hobbs FD. Systematic review and individual patient data meta-analysis of diagnosis of heart failure, with modelling of implications of different diagnostic strategies in primary care. Health Technol Assess. 2009;13:1-207, iii. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 310] [Cited by in RCA: 238] [Article Influence: 14.0] [Reference Citation Analysis (5)] |
| 33. | Masson S, Latini R, Anand IS, Barlera S, Angelici L, Vago T, Tognoni G, Cohn JN; Val-HeFT Investigators. Prognostic value of changes in N-terminal pro-brain natriuretic peptide in Val-HeFT (Valsartan Heart Failure Trial). J Am Coll Cardiol. 2008;52:997-1003. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 251] [Cited by in RCA: 261] [Article Influence: 14.5] [Reference Citation Analysis (1)] |
| 34. | George S, Selvaraj RJ, Satheesh S, Karthikeyan B. Usage of Guideline-directed Medical Therapy in Patients with Heart Failure and Reduced Ejection Fraction in a Tertiary Care Hospital. J Assoc Physicians India. 2025;73:62-65. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 35. | Ponde CK, Mohan JC, Oomman A, Kumar AS, Hazra PK, Jadhav UM. An Indian Expert Consensus on Patient-Profile-Based Implementation of Guideline-Directed Medical Therapy in the Management of Heart Failure With Reduced Ejection Fraction: APPROACH-HF. J Card Fail. 2025;31:1858-1875. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 36. | Ng LP, Goh PS. Incidence of discontinuation of angiotensin-converting enzyme inhibitors due to cough, in a primary healthcare centre in Singapore. Singapore Med J. 2014;55:146-149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 21] [Article Influence: 1.9] [Reference Citation Analysis (1)] |
| 37. | Pfeffer MA, Swedberg K, Granger CB, Held P, McMurray JJ, Michelson EL, Olofsson B, Ostergren J, Yusuf S, Pocock S; CHARM Investigators and Committees. Effects of candesartan on mortality and morbidity in patients with chronic heart failure: the CHARM-Overall programme. Lancet. 2003;362:759-766. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1518] [Cited by in RCA: 1217] [Article Influence: 52.9] [Reference Citation Analysis (0)] |
| 38. | McMurray JJ, Packer M, Desai AS, Gong J, Lefkowitz MP, Rizkala AR, Rouleau JL, Shi VC, Solomon SD, Swedberg K, Zile MR; PARADIGM-HF Investigators and Committees. Angiotensin-neprilysin inhibition versus enalapril in heart failure. N Engl J Med. 2014;371:993-1004. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5932] [Cited by in RCA: 4988] [Article Influence: 415.7] [Reference Citation Analysis (4)] |
| 39. | Konstam MA, Neaton JD, Dickstein K, Drexler H, Komajda M, Martinez FA, Riegger GA, Malbecq W, Smith RD, Guptha S, Poole-Wilson PA; HEAAL Investigators. Effects of high-dose versus low-dose losartan on clinical outcomes in patients with heart failure (HEAAL study): a randomised, double-blind trial. Lancet. 2009;374:1840-1848. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 541] [Cited by in RCA: 448] [Article Influence: 26.4] [Reference Citation Analysis (4)] |
| 40. | Devereux RB, Roman MJ, Liu JE, Welty TK, Lee ET, Rodeheffer R, Fabsitz RR, Howard BV. Congestive heart failure despite normal left ventricular systolic function in a population-based sample: the Strong Heart Study. Am J Cardiol. 2000;86:1090-1096. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 206] [Cited by in RCA: 189] [Article Influence: 7.3] [Reference Citation Analysis (2)] |