Copyright: ©Author(s) 2026.
World J Cardiol. Mar 26, 2026; 18(3): 114077
Published online Mar 26, 2026. doi: 10.4330/wjc.v18.i3.114077
Published online Mar 26, 2026. doi: 10.4330/wjc.v18.i3.114077
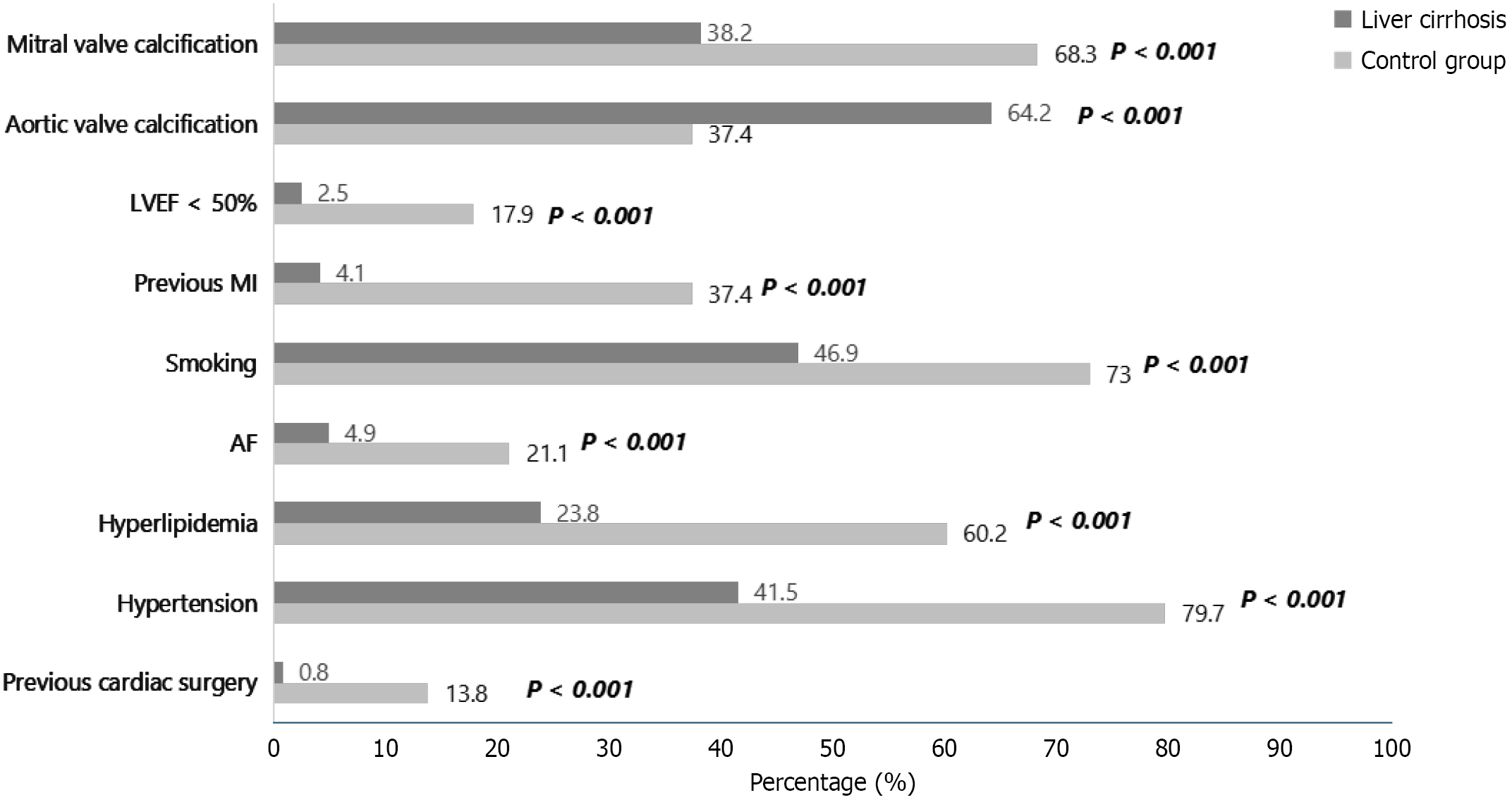
Figure 1 Comparison of cardiovascular comorbidities and valvular calcification between patients with liver cirrhosis and control sub
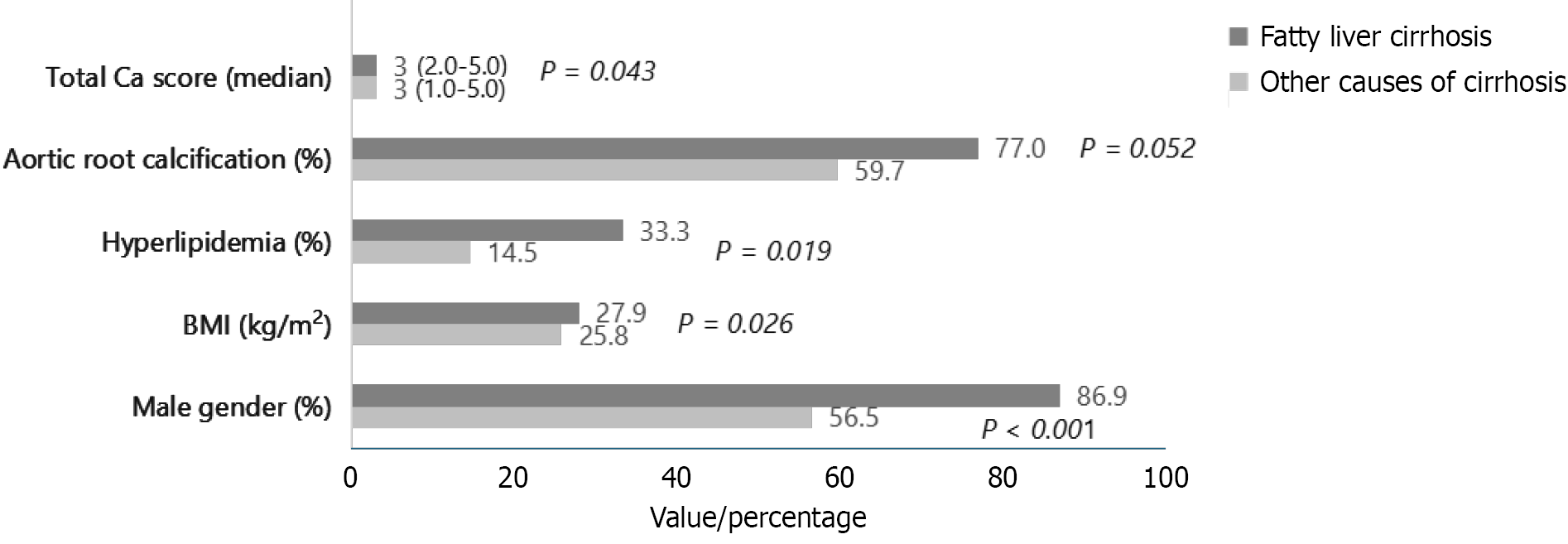
Figure 2 Comparison of demographic and clinical characteristics between patients with fatty liver cirrhosis and those with cirrhosis of other etiologies.
Horizontal bar chart illustrating differences in key variables between patients with fatty liver-related cirrhosis and those with cirrhosis due to other non-fatty etiologies. Displayed characteristics include male sex (%), body mass index (kg/m²), prevalence of hyperlipidemia (%), aortic root calcification (%), and median total calcium score. Patients with fatty liver cirrhosis showed a higher prevalence of hyperlipidemia and aortic root calcification, as well as a greater proportion of males, compared with patients with other etiologies, while body mass index and total calcium scores were similar between groups. P values are displayed to the right of each horizontal bar, adjacent to the corresponding group comparisons for every variable. Bold P values indicate statistical significance after Bonferroni correction. BMI: Body mass index; Ca: Calcium.
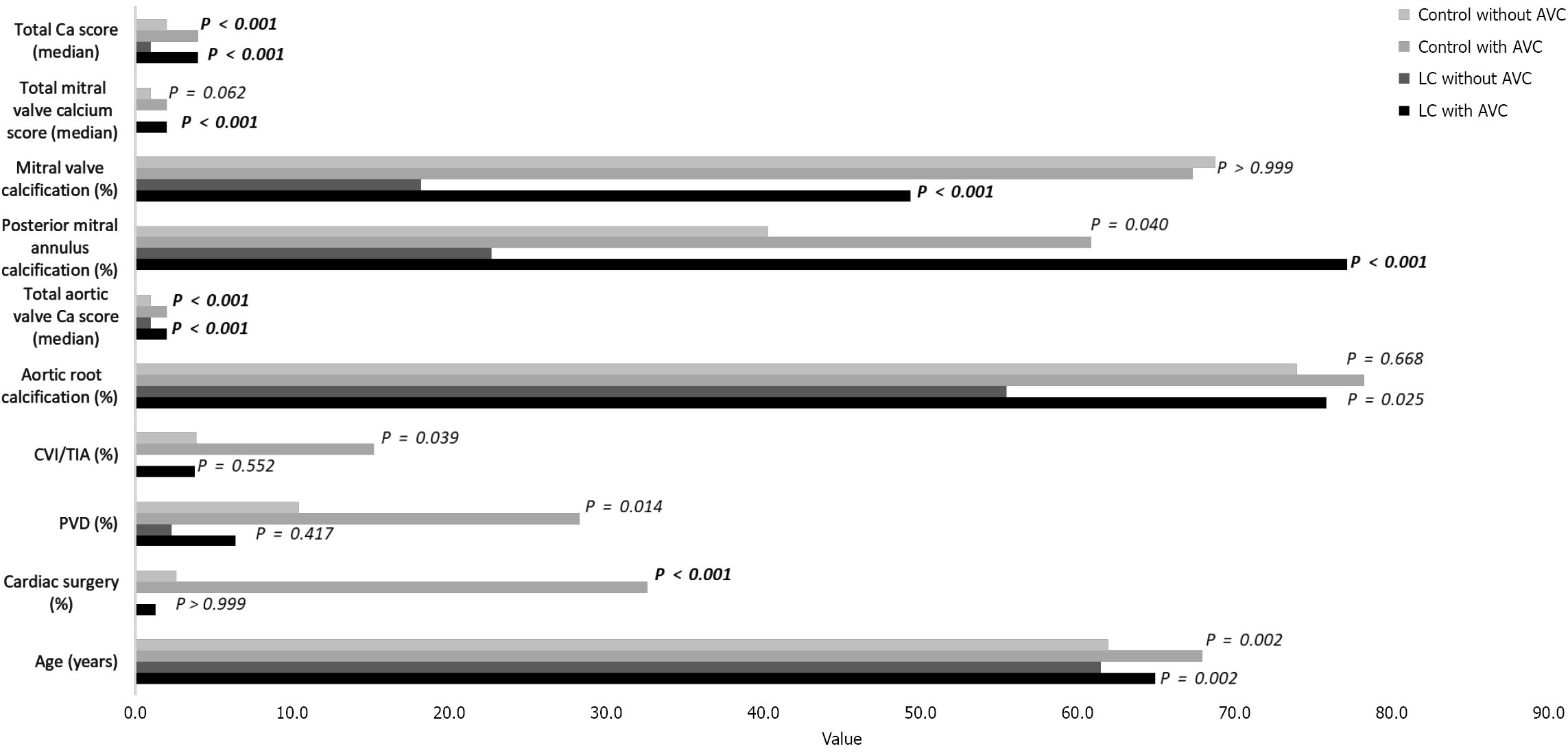
Figure 3 Demographic, clinical, and calcification characteristics in patients with and without aortic valve calcification, stratified by liver cirrhosis status.
Horizontal bar chart comparing key variables across four groups: Controls without aortic valve calcification (AVC), controls with AVC, patients with liver cirrhosis (LC) without AVC, and those with LC with AVC. Displayed parameters include age (years), prior cardiac surgery (%), peripheral vascular disease (%), cerebrovascular insult/transient ischemic attack (%), aortic root calcification (%), total aortic calcium score, posterior mitral annular calcium score, mitral valve calcification (%), total mitral calcium score, and total calcium score. The chart highlights substantial differences in both valvular and vascular calcification burden between groups, with patients exhibiting AVC - especially those with LC - showing markedly elevated calcium scores and higher prevalence of associated vascular comorbidities. P values are displayed to the right of each horizontal bar, adjacent to the corresponding group comparisons for every variable. Bold P values indicate statistical significance after Bonferroni correction. Ca: Calcium; PVD: Peripheral vascular disease; CVI: Cerebrovascular insult; TIA: Transient ischemic attack; AVC: Aortic valve calcification; LC: Liver cirrhosis.
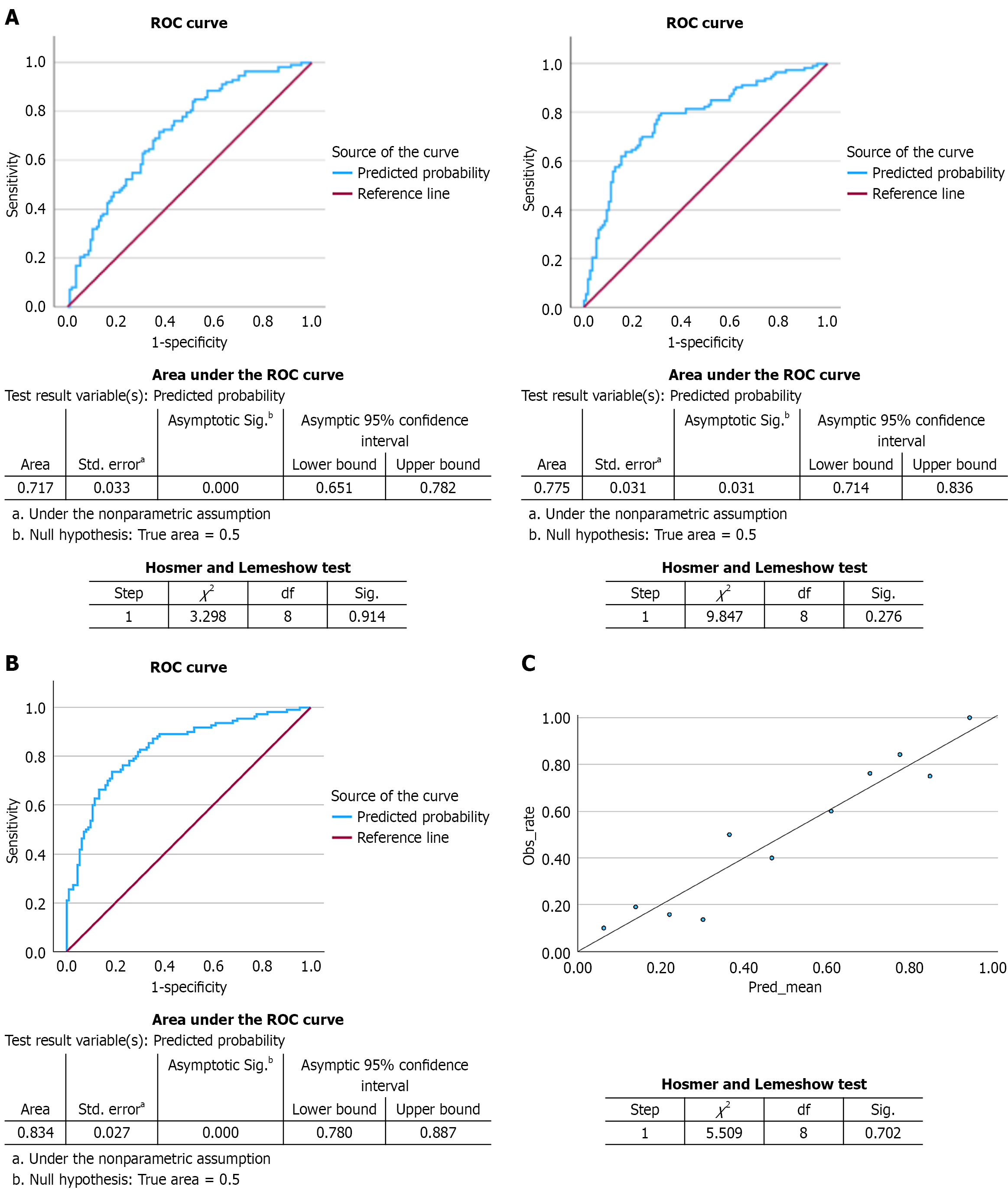
Figure 4 Discriminative performance, calibration, and receiver operating characteristic analysis of prediction models for aortic valve calcification.
aThe standard error of the area under the curve (AUC) was calculated under the non-parametric assumption; bStatistical significance of the AUC was assessed using an asymptotic test against the null hypothesis of an area equal to 0.5. A: Discriminative performance and calibration of models Ia and IIa for predicting aortic valve calcification (AVC). The receiver operating characteristic (ROC) curve on the left illustrates the discriminative ability of model Ia for identifying individuals with AVC, accompanied by the corresponding AUC statistics and Hosmer-Lemeshow (HL) goodness-of-fit results. The ROC curve on the right displays the performance of model IIa, an extended predictive model that includes additional covariates. AUC values with standard errors, significance levels, and 95% confidence intervals are shown directly beneath each ROC curve. Model calibration is summarized using the HL goodness-of-fit test, with nonsignificant P values indicating good agreement between predicted and observed outcomes; B: ROC curve for the fully adjusted multivariable prediction model (model IIIa) of AVC; C: Calibration plot for the fully adjusted multivariable prediction model (model IIIa) of AVC. The ROC curve shows good discrimination, with an AUC of 0.834 (standard error 0027; 95% confidence interval: 0.780-0.887; P < 0.001). The calibration plot compares observed and predicted probabilities of AVC across deciles of predicted risk, with the diagonal indicating perfect calibration. Model calibration was adequate, as indicated by the nonsignificant Hosmer-Lemeshow goodness-of-fit test (χ2 = 5.509, df = 8, P = 0.702). ROC: Receiver operating characteristic.
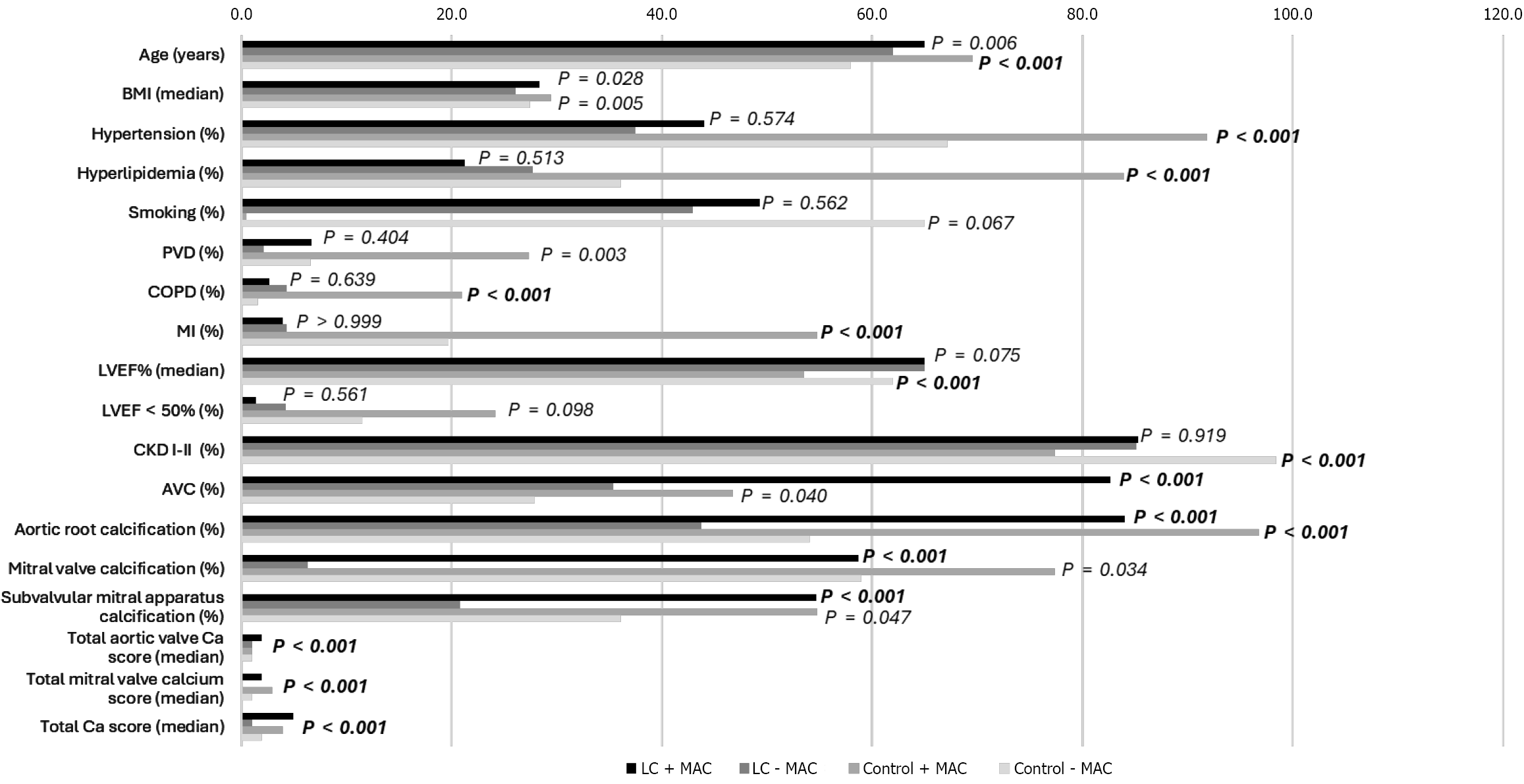
Figure 5 Comparison of demographic, clinical, and echocardiographic characteristics among patients with liver cirrhosis and non-cirrhotic controls stratified by the presence or absence of mitral annular calcification.
Horizontal bars show the proportion of subjects (categorical variables, %) or median values (continuous variables) for each group: Liver cirrhosis + mitral annular calcification (MAC; black), Liver cirrhosis - MAC (dark gray), control + MAC (light gray), and control - MAC (very light gray). Displayed variables include age; body mass index; hypertension; hyperlipidemia; smoking; peripheral vascular disease; chronic obstructive pulmonary disease; myocardial infarction; left ventricular ejection fraction; left ventricular ejection fraction < 50%; chronic kidney disease stages I-II; aortic valve calcification; aortic root calcification; mitral valve calcification; subvalvular mitral apparatus calcification; and total aortic, mitral, and combined calcium scores. P values for between-group comparisons are indicated next to each characteristic. Bold P values indicate statistical significance after Bonferroni correction. For total aortic, mitral, and combined calcium scores, P values were identical across comparisons and are therefore shown only once. BMI: Body mass index; PVD: Peripheral vascular disease; COPD: Chronic obstructive pulmonary disease; LVEF: Left ventricular ejection fraction; CKD: Chronic kidney disease; AVC: Aortic valve calcification; LC: Liver cirrhosis; MAC: Mitral annular calcification; MI: Myocardial infarction; Ca: Calcium.
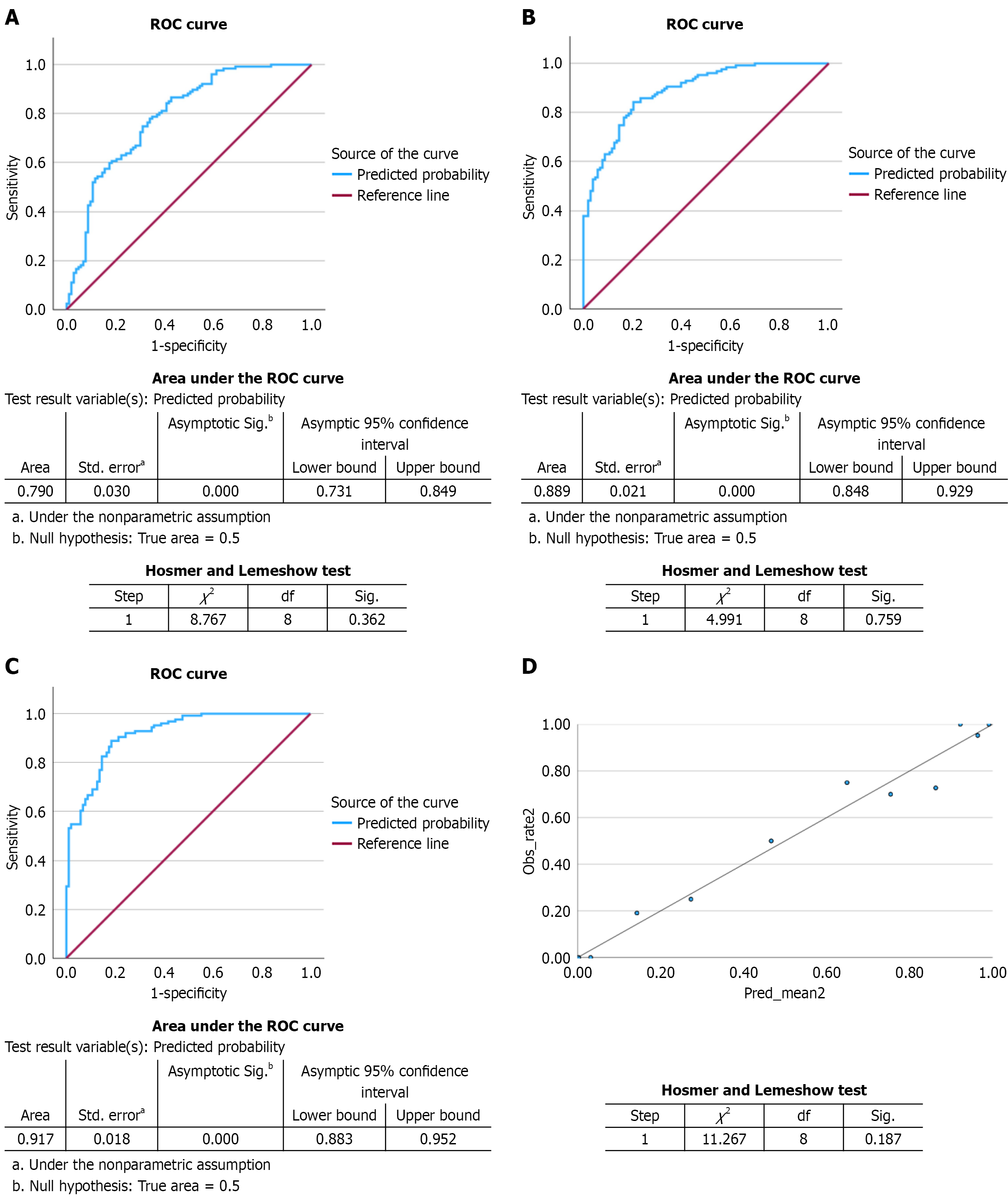
Figure 6 Receiver operating characteristic curves and calibration analysis of logistic regression models for predicting mitral annular calcification.
aThe standard error of the area under the curve (AUC) was calculated under the non-parametric assumption; bStatistical significance of the AUC was assessed using an asymptotic test against the null hypothesis of an area equal to 0.5. A: Receiver operating characteristic (ROC) curves for multivariable logistic regression models Ib; B: ROC curves for multivariable logistic regression model IIb. Model Ib demonstrated moderate discrimination [AUC 0.790; 95% confidence interval (CI): 0.731-0.849, P < 0.001; Hosmer-Lemeshow (HL) χ2 = 8.767, df = 8, P = 0.362]. Model IIb showed improved discrimination (AUC 0.889; 95%CI: 0.848-0.929; P < 0.001) and good calibration (HL χ2 = 4.991, df = 8, P = 0.759). The diagonal line indicates the reference line (AUC = 0.5); C: The ROC curve for the fully adjusted multivariable prediction model (model IIIb) shows excellent discriminative performance, with an AUC of 0.917 (95%CI: 0.883-0.952; P < 0.001); D: The calibration plot compares observed event rates with predicted probabilities across deciles of predicted risk, with the diagonal line indicating perfect calibration. Model calibration was adequate, as indicated by the HL goodness-of-fit test: χ2 = 11.267, df = 8, P = 0.187. ROC: Receiver operating characteristic.
- Citation: Vuckovic M, Grgurić J, Paic F, Radonic V, Jurin I, Filipec Kanizaj T, Letilovic T. Valvular calcification in liver cirrhosis: A comparison with non-cirrhotic cardiovascular controls. World J Cardiol 2026; 18(3): 114077
- URL: https://www.wjgnet.com/1949-8462/full/v18/i3/114077.htm
- DOI: https://dx.doi.org/10.4330/wjc.v18.i3.114077