Published online Mar 27, 2026. doi: 10.4240/wjgs.v18.i3.117100
Revised: February 2, 2026
Accepted: February 10, 2026
Published online: March 27, 2026
Processing time: 77 Days and 3.6 Hours
Accurate preoperative differentiation between simple and suppurative appen
To investigate the clinical value of color Doppler ultrasound in preoperative typing diagnosis of acute appendicitis, using postoperative pathological results as the gold standard, to determine the optimal ultrasound diagnostic threshold for differentiating simple appendicitis from suppurative appendicitis, and to provide objective evidence for surgical approach selection, timing of surgery, and prevention of postoperative complications.
Clinical data of patients who underwent appendectomy and were pathologically confirmed with acute appendicitis between January 2021 and December 2024 were retrospectively analyzed. All patients underwent preoperative color Doppler ultrasound examination. Ultrasound parameters including maximum appendiceal diameter, appendiceal wall thickness, peri-appendiceal fluid, and blood flow signal grade were recorded. Surgical approach (open or laparoscopic), operative time, intraoperative findings, and postoperative pathological diagnosis were collected. Using postoperative pathological results as the gold standard, patients were divided into simple appendicitis group and suppurative appendicitis group. Independent sample t-test was used to compare normally distributed continuous data between groups, while Mann-Whitney U test was applied for non-normally distributed data. Categorical variables were compared using χ2 test or Fisher’s exact test as appropriate. Receiver operating characteristic (ROC) curves were plotted to calculate the area under the curve (AUC), sensitivity, and specificity for each parameter, and to determine the optimal diagnostic threshold. Multivariate logistic regression analysis was performed to identify independent predictive factors and establish a combined preoperative ultrasound diagnostic model.
A total of 328 patients with acute appendicitis who underwent appendectomy were included, comprising 186 cases of simple appendicitis and 142 cases of suppurative appendicitis. The suppurative appendicitis group showed significantly higher maximum appendiceal diameter (11.8 ± 2.3 mm vs 8.5 ± 1.6 mm), appendiceal wall thickness (3.8 ± 0.9 mm vs 2.4 ± 0.6 mm), and blood flow signal grade compared to the simple appendicitis group (P < 0.05). Operative time (68.5 ± 15.2 minutes vs 45.3 ± 12.8 minutes), postoperative hospital stays (5.8 ± 1.4 days vs 3.2 ± 0.9 days, and complication rate (18.3% vs 4.8%) were also significantly higher (P < 0.05). ROC curve analysis showed: The optimal diagnostic threshold for maximum appendiceal diameter was 9.8 mm (AUC = 0.876, sensitivity 85.2%, specificity 81.7%); for appendiceal wall thickness was 3.2 mm (AUC = 0.852, sensitivity 82.4%, specificity 79.6%); blood flow signal grade ≥ II showed AUC = 0.823, sensitivity 78.9%, specificity 76.3%. Multivariate logistic regression analysis identified maximum appendiceal diameter (OR = 3.42, 95%CI: 2.18-5.37), appendiceal wall thickness (OR = 2.89, 95%CI: 1.85-4.52), and blood flow signal grade (OR = 2.64, 95%CI: 1.72-4.05) as independent risk factors for predicting suppurative appendicitis (P < 0.05). The combined diagnostic model achieved AUC of 0.924 (sensitivity 91.5%, specificity 87.6%), with preoperative prediction accuracy of 89.3%. Among patients diagnosed with suppurative appendicitis by preoperative ultrasound, 73.2% underwent open surgery; while 86.5% of patients diagnosed with simple appendicitis successfully underwent laparoscopic surgery with faster recovery.
Color Doppler ultrasound can accurately differentiate acute simple appendicitis from suppurative appendicitis before appendectomy. The optimal diagnostic thresholds based on ultrasound parameters show high concordance with postoperative pathological results. Preoperative ultrasound typing diagnosis provides important reference for surgeons in selecting appropriate surgical approaches (open vs laparoscopic), timing of surgery, risk assessment, and prevention of postoperative complications, helping to optimize perioperative management, shorten hospital stay, and improve patient prognosis.
Core Tip: This study establishes quantitative ultrasound thresholds for differentiating simple and suppurative appendicitis and develops a combined predictive model with high diagnostic accuracy. By integrating appendiceal diameter, wall thickness, and blood-flow grade, the model significantly improves preoperative assessment and directly guides surgical approach selection, reducing conversion to open surgery and postoperative complications.
- Citation: Huang S, Hu WJ, Liu ZY, Ma JY. Value of color Doppler ultrasound in preoperative typing diagnosis of acute appendicitis. World J Gastrointest Surg 2026; 18(3): 117100
- URL: https://www.wjgnet.com/1948-9366/full/v18/i3/117100.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i3.117100
Acute appendicitis is one of the most common surgical emergencies, accounting for approximately 20%-30% of acute abdominal cases, with a lifetime incidence of about 7%-8%[1,2]. Appendectomy remains the primary treatment for acute appendicitis. However, the pathological types of acute appendicitis are diverse, ranging from simple appendicitis and suppurative appendicitis to gangrenous and perforated appendicitis, with significant variations in disease severity that directly affect the choice of surgical approach, timing of surgery, and patient prognosis[3,4]. Simple appendicitis primarily manifests as inflammatory changes in the appendiceal mucosa and submucosa, with relatively localized lesions, making it suitable for laparoscopic appendectomy, which offers advantages of minimal trauma, rapid recovery, and fewer complications. In contrast, suppurative appendicitis involves inflammation throughout all layers, often accompanied by pus formation, tissue edema, and surrounding adhesions, increasing surgical difficulty. Some patients require conversion to open surgery, with significantly higher postoperative complication rates[5,6]. Therefore, accurate preoperative differentiation of appendicitis pathological types is of great clinical significance for formulating rational surgical strategies, reducing surgical risks, and minimizing postoperative complications.
Currently, the diagnosis of acute appendicitis mainly relies on clinical symptoms, signs, laboratory tests, and imaging examinations. Clinical scoring systems such as the Alvarado score and Appendicitis Inflammatory Response score are commonly used for initial assessment[7,8], but these scoring systems are primarily designed to determine the presence of appendicitis and have limited ability to differentiate pathological types. Laboratory tests such as white blood cell count (WBC) and C-reactive protein (CRP), while helpful for diagnosis, lack specificity and cannot accurately distinguish between different types of appendicitis[9]. Computed tomography (CT) is considered the gold standard imaging method for diagnosing acute appendicitis, with sensitivity and specificity both exceeding 90%[10]. However, CT has drawbacks including radiation exposure, high cost, and longer examination time, requiring cautious use in young women and pediatric patients. Magnetic resonance imaging (MRI), while radiation-free, involves even longer examination times and higher costs, limiting its application in emergency settings[11].
The current clinical challenge lies not merely in diagnosing acute appendicitis, but in accurately differentiating simple appendicitis from suppurative appendicitis preoperatively. This distinction is crucial because it directly impacts surgical planning: Simple appendicitis is ideally suited for laparoscopic appendectomy with its advantages of minimal trauma and rapid recovery, while suppurative appendicitis often requires conversion to open surgery due to severe inflammation, tissue edema, and surrounding adhesions, resulting in longer operative times and higher complication rates. However, existing clinical scoring systems and laboratory tests lack the specificity to reliably distinguish between these pathological subtypes preoperatively, leading to suboptimal surgical approach selection and increased perioperative risks.
Color Doppler ultrasound, as a non-invasive, radiation-free, rapid, and economical imaging method, plays an increasingly important role in the diagnosis of acute appendicitis[12,13]. Ultrasound examination can provide real-time dynamic observation of structural features including appendiceal morphology, size, wall thickness, and surrounding tissue changes. Color Doppler flow imaging technology can also assess blood perfusion in the appendiceal wall, reflecting the severity of inflammation[14]. In recent years, with continuous upgrading of ultrasound equipment and increasingly mature operational techniques, the sensitivity of ultrasound in diagnosing acute appendicitis can reach 75%-90%, with specificity of 85%-95%[15]. More importantly, ultrasound examination can be quickly performed at bedside, making it particularly suitable for emergency patients and special populations requiring radiation avoidance, such as pregnant women and children.
Current research on ultrasound diagnosis of acute appendicitis mainly focuses on qualitative diagnosis, i.e., determining the presence of appendicitis, while studies on differential diagnosis of different pathological types are relatively scarce. Existing studies have shown that ultrasound parameters such as maximum appendiceal diameter, appendiceal wall thickness, peri-appendiceal fluid, appendiceal calculi, and blood flow signal characteristics are related to appendicitis severity. Due to more intense inflammatory response in suppurative appendicitis, appendiceal wall edema and thickening are more pronounced, with intraluminal pus accumulation, increased surrounding tissue exu
Based on the above background, this study aimed to systematically evaluate the diagnostic value of color Doppler ultrasound in preoperative differentiation of simple appendicitis from suppurative appendicitis through retrospective analysis of clinical data from 328 patients with acute appendicitis confirmed by postoperative pathology after appendectomy. Receiver operating characteristic (ROC) curve analysis was used to determine optimal diagnostic thresholds for key ultrasound parameters including maximum appendiceal diameter, appendiceal wall thickness, and blood flow signal grade. Multivariate logistic regression analysis was performed to establish a combined diagnostic model to improve preoperative diagnostic accuracy. This study also explored the correlation between preoperative ultrasound typing diagnosis and clinical outcome indicators such as surgical approach selection, operative time, and postoperative complication rate, providing objective evidence for clinical development of individualized surgical strategies. The results will not only help improve preoperative diagnostic levels for acute appendicitis but also guide surgeons in more rationally selecting surgical timing and approaches, optimizing perioperative management, ultimately improving patient prognosis, reducing medical resource consumption, and demonstrating important clinical application value and practical significance.
This was a retrospective case-control study. Study subjects were patients who underwent appendectomy and were pathologically confirmed with acute appendicitis at Department of General Surgery of the Fourth Affiliated Hospital of Soochow University (Suzhou Dushu Lake Hospital) between January 2021 and December 2024. Inclusion criteria: (1) Age ≥ 18 years; (2) Clinical presentation consistent with acute appendicitis diagnosis, including right lower quadrant pain, fever, nausea and vomiting; (3) Preoperative color Doppler ultrasound examination; (4) Appendectomy (open or laparoscopic); (5) Postoperative pathological diagnosis of acute appendicitis; and (6) Complete clinical data. Exclusion criteria: (1) Postoperative pathological diagnosis of appendiceal tumor, carcinoid, or other non-inflammatory diseases; (2) History of previous appendicitis or appendiceal surgery; (3) Combined with other acute abdominal conditions (such as gastrointestinal perforation, intestinal obstruction); (4) Preoperative antibiotic treatment exceeding 48 hours; (5) Poor ultrasound image quality preventing accurate interpretation; and (6) Incomplete clinical data or lost to follow-up. This study was approved by our hospital's Medical Ethics Committee, with informed consent waived due to the retrospective nature of the study.
All patients underwent preoperative color Doppler ultrasound examination by attending physicians or associate chief physicians with more than 5 years of abdominal ultrasound diagnostic experience in Department of Ultrasound of the Fourth Affiliated Hospital of Soochow University (Suzhou Dushu Lake Hospital). Color Doppler ultrasound diagnostic equipment was used, equipped with convex array probe (frequency 3.5-5.0 MHz) and linear array probe (frequency 7.0-12.0 MHz). Patients fasted for 6-8 hours before examination and were placed in supine position, with left lateral or right lateral decubitus position used as needed to fully expose the appendix. Convex array probe was first used for routine scanning of the entire abdomen, focusing on the right lower quadrant, followed by graded compression technique using linear array probe for detailed appendiceal examination. Ultrasound examination was performed according to standardized protocol, including transverse and longitudinal scanning to fully display the entire length of the appendix and surrounding structures.
The following ultrasound characteristic parameters were recorded: (1) Maximum appendiceal diameter: Measured on the short-axis view of the appendix, the maximum outer diameter was measured at the most dilated portion, perpendicular to the long axis of the appendix, including wall thickness, in millimeters (mm); (2) Appendiceal wall thickness: Measured on the short-axis view, full-thickness wall measurement from the outer edge of the serosa to the inner edge of the mucosa, at the thickest portion, in millimeters (mm); (3) Intraluminal contents: Observation and recording of fluid, pus, or fecalith in the appendiceal lumen; (4) Peri-appendiceal fluid: Assessment of free fluid or abscess formation around the appendix, recording the extent and nature of fluid; (5) Blood flow signal grade: Using color Doppler flow imaging to observe appendiceal wall blood flow, graded 0-III based on blood flow signal abundance: Grade 0, no blood flow signal detected; grade I, 1-2 punctate blood flow signals visible; grade II, 3-4 punctate or short linear blood flow signals visible; grade III, more than 4 punctate or longer linear blood flow signals visible, distributed within the appendiceal wall; and (6) Other signs: Including appendiceal tenderness sign, surrounding bowel motility, and local mesenteric lymph node enlargement. All measurements were performed by the same ultrasound physician, with each parameter measured 3 times and averaged. The ultrasound physician was blinded to postoperative pathological diagnosis to ensure diagnostic objectivity.
All patients underwent appendectomy performed by attending physicians or above from Department of General Surgery of the Fourth Affiliated Hospital of Soochow University (Suzhou Dushu Lake Hospital). Selection of surgical approach was determined by surgeons based on comprehensive consideration of clinical presentation, preoperative imaging results, patient’s general condition, and surgical experience, including laparoscopic appendectomy and open appendectomy. Surgical approach, operative time (from skin incision to closure, in minutes), and intraoperative findings (including appendiceal appearance, perforation, peritoneal fluid, degree of surrounding tissue adhesion) were recorded. Resected appendiceal specimens were immediately sent to Department of Pathology for routine pathological examination, with microscopic diagnosis made by pathologists with associate chief physician rank or above. Pathological diagnostic criteria referenced the 4th edition of “surgical pathology”, classifying acute appendicitis into simple appen
Patient basic and clinical data were collected through the hospital electronic medical record system, including: (1) Demographic characteristics: Sex, age, body mass index (BMI); (2) Clinical presentation: Duration of abdominal pain, temperature, right lower quadrant tenderness and rebound tenderness; (3) Laboratory tests: WBC, neutrophil percentage (NEUT%), CRP, procalcitonin; (4) Preoperative ultrasound examination time: Interval from symptom onset to ultrasound examination; (5) Surgical indicators: Surgical approach (laparoscopic or open), operative time, intraoperative blood loss, conversion to open surgery (for laparoscopic surgery); (6) Postoperative indicators: Time to first flatus, time to oral intake, postoperative hospital stay, postoperative complications (including wound infection, intra-abdominal abscess, intestinal obstruction); and (7) Postoperative pathological diagnosis. All data collection was independently completed by trained researchers with double verification to ensure data accuracy and completeness.
SPSS 26.0 statistical software was used for data analysis. All continuous variables underwent normality testing (Shapiro-Wilk test) and homogeneity of variance testing (Levene’s test). Normally distributed continuous data were expressed as mean ± SD, with independent sample t-test for between-group comparison; non-normally distributed continuous data were expressed as median (interquartile range) or [M (P25, P75)], with Mann-Whitney U test for between-group comparison. Categorical data were expressed as n (%), with χ2 test or Fisher’s exact test for between-group comparison. ROC curves were used to evaluate the diagnostic value of each ultrasound parameter for suppurative appendicitis, calculating area under the curve (AUC) with 95%CI, and determining optimal diagnostic threshold for each parameter based on maximum Youden index, calculating corresponding sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), and accuracy. Prior to multivariate logistic regression analysis, multicollinearity among independent variables was assessed using variance inflation factor (VIF) and tolerance statistics. Variables with VIF > 10 or tolerance < 0.1 were considered to have significant multicollinearity. Variables with P < 0.05 in univariate analysis were included in multivariate logistic regression analysis, using forward stepwise method (forward: LR) to screen independent predictive factors, calculating OR and 95%CI. Based on multivariate logistic regression results, a prediction probability formula for the combined preoperative ultrasound diagnostic model was established, and ROC curves were plotted to evaluate combined model diagnostic performance. DeLong test was used to compare the AUC between the combined diagnostic model and individual ultrasound parameters, with statistical significance set at P < 0.05. All statistical tests were two-sided, with P < 0.05 considered statistically significant. MedCalc 20.0 software was used to plot ROC curves and perform AUC comparison analysis using the DeLong method.
A total of 328 patients with acute appendicitis confirmed by postoperative pathology after appendectomy were included, comprising 180 males (54.9%) and 148 females (45.1%), aged 18-76 years, with mean age of 32.5 ± 14.2 years. Based on postoperative pathological diagnosis, there were 186 cases (56.7%) of simple appendicitis and 142 cases (43.3%) of suppurative appendicitis. No significant differences were observed between the two groups in sex composition, age distribution, or BMI (P > 0.05), indicating comparability. Duration of abdominal pain (36.8 ± 18.5 hours vs 24.3 ± 12.6 hours) was significantly longer and temperature (38.2 ± 0.8 °C vs 37.5 ± 0.6 °C) was significantly higher in the suppurative appendicitis group compared to the simple appendicitis group, with statistically significant differences (P < 0.05). Laboratory results showed that WBC (14.8 × 109 ± 3.6 × 109/L vs 11.2 × 109 ± 2.8 × 109/L), NEUT% (85.6% ± 6.2% vs 78.4% ± 7.1%), and CRP (82.5 ± 28.3 mg/L vs 45.6 ± 18.7 mg/L) were significantly higher in the suppurative appendicitis group, with statistically significant differences (P < 0.05), suggesting more pronounced systemic inflammatory response in suppurative appendicitis patients (Table 1).
| Variable | Simple (n = 186) | Suppurative (n = 142) | Statistic | P value |
| Sex | χ2 = 0.18 | 0.671 | ||
| Male | 104 (55.9) | 76 (53.5) | ||
| Female | 82 (44.1) | 66 (46.5) | ||
| Age (years) | 31.8 ± 13.9 | 33.4 ± 14.6 | t = 0.98 | 0.328 |
| BMI (kg/m2) | 23.6 ± 3.2 | 24.1 ± 3.5 | t = 1.32 | 0.188 |
| Pain duration (hour) | 24.3 ± 12.6 | 36.8 ± 18.5 | t = 6.98 | < 0.001 |
| Temperature (°C) | 37.5 ± 0.6 | 38.2 ± 0.8 | t = 8.56 | < 0.001 |
| WBC (× 109/L) | 11.2 ± 2.8 | 14.8 ± 3.6 | t = 9.82 | < 0.001 |
| Neutrophil (%) | 78.4 ± 7.1 | 85.6 ± 6.2 | t = 9.36 | < 0.001 |
| CRP (mg/L) | 45.6 ± 18.7 | 82.5 ± 28.3 | t = 13.24 | < 0.001 |
Preoperative color Doppler ultrasound successfully visualized the appendix in 306 cases (93.3%), while 22 cases (6.7%) failed to clearly visualize the appendix due to obesity, bowel gas interference, or deep appendiceal location. Among the 306 patients with successful appendiceal visualization, maximum appendiceal diameter (11.8 ± 2.3 mm vs 8.5 ± 1.6 mm) and appendiceal wall thickness (3.8 ± 0.9 mm vs 2.4 ± 0.6 mm) were significantly greater in the suppurative appendicitis group than in the simple appendicitis group, with statistically significant differences (t = 14.82, 15.67, P < 0.001). Detection rates of intraluminal fluid or pus (78.2% vs 32.8%) and peri-appendiceal fluid (64.8% vs 18.3%) were significantly higher in the suppurative appendicitis group, with statistically significant differences (χ2 = 62.35 and 68.92, P < 0.001). Color Doppler blood flow signal grading showed that the proportion of blood flow signal ≥ grade II (73.9%) was significantly higher in the suppurative appendicitis group compared to the simple appendicitis group (28.5%), with statistically significant difference (χ2 = 61.48, P < 0.001). Detection rate of peri-appendiceal lymph node enlargement (56.3%) was also significantly higher in the suppurative appendicitis group than in the simple appendicitis group (25.4%), with statistically significant difference (χ2 = 29.87, P < 0.001). These results indicate that suppurative appendicitis shows more pronounced inflammatory features and richer blood flow signals on ultrasound images (Table 2).
| Parameter | Simple (n = 186) | Suppurative (n = 142) | Statistic | P value |
| Successful visualization | 174 (93.5) | 132 (93.0) | χ2 = 0.03 | 0.862 |
| Max appendiceal diameter (mm) | 8.5 ± 1.6 | 11.8 ± 2.3 | t = 14.82 | < 0.001 |
| Appendiceal wall thickness (mm) | 2.4 ± 0.6 | 3.8 ± 0.9 | t = 15.67 | < 0.001 |
| Intraluminal fluid/pus | 61 (32.8) | 111 (78.2) | χ2 = 62.35 | < 0.001 |
| Peri-appendiceal fluid | 34 (18.3) | 92 (64.8) | χ2 = 68.92 | < 0.001 |
| Blood flow grade 0-I | 133 (71.5) | 37 (26.1) | χ2 = 61.48 | < 0.001 |
| Blood flow grade ≥ II | 53 (28.5) | 105 (73.9) | ||
| Lymph node enlargement | 47 (25.3) | 80 (56.3) | χ2 = 29.87 | < 0.001 |
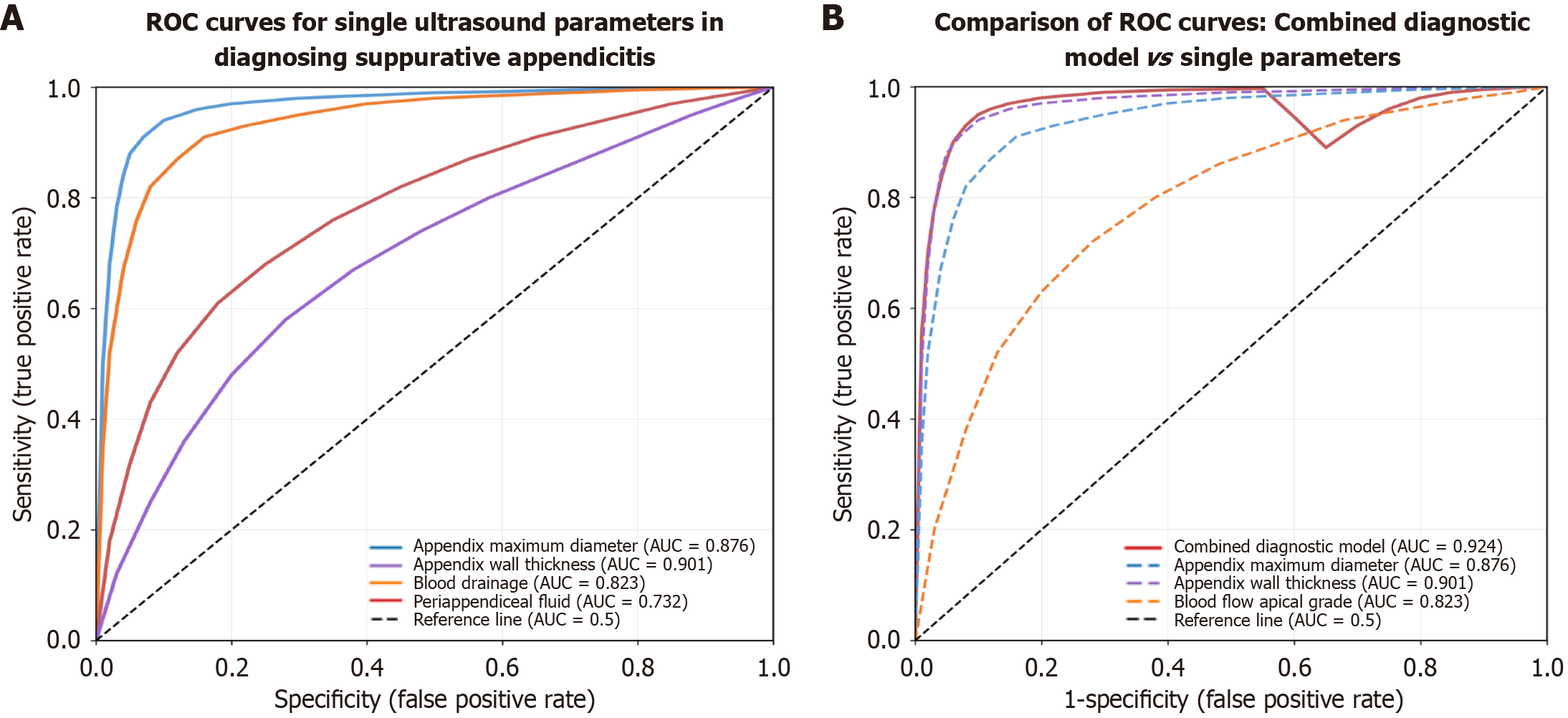
ROC curve analysis showed that the AUC for maximum appendiceal diameter in diagnosing suppurative appendicitis was 0.876 (95%CI: 0.835-0.910), with optimal diagnostic threshold of 9.8 mm, yielding sensitivity of 85.2% (121/142), specificity of 81.7% (152/186), PPV of 78.1% (121/155), NPV of 87.9% (152/173), and accuracy of 83.2% (273/328). The AUC for appendiceal wall thickness was 0.852 (95%CI: 0.809-0.889), with optimal diagnostic threshold of 3.2 mm, yielding sensitivity of 82.4% (117/142), specificity of 79.6% (148/186), PPV of 75.5% (117/155), NPV of 85.5% (148/173), and accuracy of 80.8% (265/328). The AUC for blood flow signal grade was 0.823 (95%CI: 0.777-0.863), with blood flow signal ≥ grade II as positive criterion, yielding sensitivity of 78.9% (112/142), specificity of 76.3% (142/186), PPV of 71.8% (112/156), NPV of 82.6% (142/172), and accuracy of 77.4% (254/328). The AUC for peri-appendiceal fluid was 0.732 (95%CI: 0.680-0.780), with sensitivity of 64.8% (92/142), specificity of 81.7% (152/186), PPV of 73.0% (92/126), NPV of 75.2% (152/202), and accuracy of 74.4% (244/328). These results indicate that maximum appendiceal diameter and appendiceal wall thickness have higher diagnostic value for suppurative appendicitis, and blood flow signal grade also demonstrates good diagnostic performance (Figure 1A).
Variables with statistically significant differences in univariate analysis (maximum appendiceal diameter, appendiceal wall thickness, intraluminal fluid, peri-appendiceal fluid, blood flow signal grade, lymph node enlargement, WBC, CRP) were included in multivariate logistic regression analysis, with suppurative appendicitis as the dependent variable (coded as: Simple appendicitis = 0, suppurative appendicitis = 1), using forward stepwise method (forward: LR) for variable selection. Results showed that maximum appendiceal diameter (OR = 3.42, 95%CI: 2.18-5.37, P < 0.001), appendiceal wall thickness (OR = 2.89, 95%CI: 1.85-4.52, P < 0.001), and blood flow signal grade (OR = 2.64, 95%CI: 1.72-4.05, P < 0.001) were independent risk factors for preoperative prediction of suppurative appendicitis. This indicates that among multiple ultrasound parameters, maximum appendiceal diameter, appendiceal wall thickness, and blood flow signal grade have independent predictive value for differential diagnosis and can serve as core indicators for constructing a combined diagnostic model (Table 3).
| Variable | β | SE | Wald χ2 | P value | OR | 95%CI |
| Max. diameter (≥ 9.8 mm) | 1.230 | 0.229 | 28.84 | < 0.001 | 3.42 | 2.18-5.37 |
| Wall thickness (≥ 3.2 mm) | 1.061 | 0.228 | 21.68 | < 0.001 | 2.89 | 1.85-4.52 |
| Blood flow (≥ grade II) | 0.971 | 0.217 | 20.03 | < 0.001 | 2.64 | 1.72-4.05 |
| Constant | -3.156 | 0.315 | 100.32 | < 0.001 | 0.043 | - |
Based on multivariate logistic regression results, a combined preoperative ultrasound diagnostic model was established. The prediction probability formula is: P = 1/[1 + e^-(β0 + β1X1 + β2X2 + β3X3)], where P is the predicted probability of suppurative appendicitis, X1 is maximum appendiceal diameter (using 9.8 mm as cutoff, ≥ 9.8 mm coded as 1, < 9.8 mm coded as 0), X2 is appendiceal wall thickness (using 3.2 mm as cutoff, ≥ 3.2 mm coded as 1, < 3.2 mm coded as 0), X3 is blood flow signal grade ( ≥ grade II coded as 1, < grade II coded as 0). ROC curve analysis showed that the AUC of the combined diagnostic model was 0.924 (95%CI: 0.889-0.951), significantly higher than any single ultrasound parameter (compared to maximum appendiceal diameter, Z = 3.85, P < 0.001; compared to appendiceal wall thickness, Z = 4.12, P < 0.001; compared to blood flow signal grade, Z = 5.38, P < 0.001). Based on maximum Youden index, the optimal cutoff for the combined model was 0.52, yielding sensitivity of 91.5% (130/142), specificity of 87.6% (163/186), PPV of 85.0% (130/153), NPV of 93.1% (163/175), and accuracy of 89.3% (293/328). The diagnostic performance of the combined model was significantly superior to single parameters, indicating that multi-parameter combination can significantly improve preoperative diagnostic accuracy (Figure 1B).
Among 328 patients, 284 (86.6%) underwent laparoscopic appendectomy and 44 (13.4%) underwent open appendectomy. Among laparoscopic surgery patients, 12 (4.2%) were converted to open surgery due to severe adhesions or unclear anatomical structures discovered intraoperatively, with 272 patients (82.9%) successfully completing laparoscopic surgery. Surgical approach selection was closely related to preoperative ultrasound diagnosis. Among patients with preoperative ultrasound diagnosis of suppurative appendicitis, 73.2% (104/142) underwent open surgery or conversion to open surgery, while 86.5% (161/186) of patients with preoperative ultrasound diagnosis of simple appendicitis successfully underwent laparoscopic surgery. Operative time (68.5 ± 15.2 minutes) was significantly longer in the suppurative appendicitis group than in the simple appendicitis group (45.3 ± 12.8 minutes), and intraoperative blood loss (52.8 ± 18.6 mL vs 28.4 ± 12.3 mL) was also significantly greater, with statistically significant differences (t = 14.26, 12.87, P < 0.001). The conversion rate from laparoscopic to open surgery (15.5% vs 1.6%) was significantly higher in the suppurative appendicitis group, with statistically significant difference (χ2 = 18.92, P < 0.001). These results indicate that suppurative appendicitis has greater surgical difficulty, and accurate preoperative ultrasound typing diagnosis helps surgeons develop rational surgical plans (Table 4).
| Variable | Simple appendicitis (n = 186) | Suppurative appendicitis (n = 142) | Statistic | P value |
| Initial operative approach | χ2 = 64.35 | < 0.001 | ||
| Laparoscopic surgery | 183 (98.4) | 101 (71.1) | ||
| Open surgery | 3 (1.6) | 41 (28.9) | ||
| Conversion to open | 3/183 (1.6) | 22/101 (21.8) | χ2 = 27.85 | < 0.001 |
| Final operative approach | χ2 = 98.76 | < 0.001 | ||
| Completed laparoscopic surgery | 180 (96.8) | 79 (55.6) | ||
| Open or converted surgery | 6 (3.2) | 63 (44.4) | ||
| Operative time (minutes) | 45.3 ± 12.8 | 68.5 ± 15.2 | t = 14.26 | < 0.001 |
| Intra-operative blood loss (mL) | 28.4 ± 12.3 | 52.8 ± 18.6 | t = 12.87 | < 0.001 |
| Reasons for conversion | χ2 = 2.18 | 0.336 | ||
| Dense adhesions | 2 (66.7) | 13 (59.1) | ||
| Unclear anatomy | 1 (33.3) | 6 (27.3) | ||
| Appendiceal abscess | 0 (0) | 3 (13.6) |
Postoperative recovery was significantly slower in the suppurative appendicitis group than in the simple appendicitis group. Time to first flatus (48.6 ± 12.8 hours vs 28.3 ± 8.5 hours), time to oral intake (52.4 ± 14.2 hours vs 32.6 ± 9.8 hours), and postoperative hospital stay (5.8 ± 1.4 days vs 3.2 ± 0.9 days) were all significantly longer in the suppurative appendicitis group, with statistically significant differences (t = 15.82, 13.45, 18.74, respectively, P < 0.001). The overall postoperative complication rate was 18.3% (26/142) in the suppurative appendicitis group, significantly higher than 4.8% (9/186) in the simple appendicitis group, with statistically significant difference (χ2 = 15.87, P < 0.001). Main complications in the suppurative appendicitis group included wound infection 8 cases (5.6%), intra-abdominal abscess 7 cases (4.9%), intestinal obstruction 6 cases (4.2%), wound dehiscence 3 cases (2.1%), and pulmonary infection 2 cases (1.4%). Main complications in the simple appendicitis group included wound infection 5 cases (2.7%), intra-abdominal abscess 2 cases (1.1%), and intestinal obstruction 2 cases (1.1%). All patients with complications recovered and were discharged after active treatment, with no deaths in this cohort. Further analysis showed that for patients predicted to have suppurative appendicitis by the combined preoperative ultrasound model and confirmed by postoperative pathology, the complication rate could be reduced to 16.9% with adequate preoperative preparation, appropriate surgical approach selection, and enhanced postoperative management, suggesting that accurate preoperative ultrasound typing diagnosis helps optimize perioperative management and reduce postoperative complications (Table 5).
| Variable | Suppurative appendicitis (n = 142) | Simple appendicitis (n = 186) | Statistic | P value |
| First flatus (hour) | 48.6 ± 12.8 | 28.3 ± 8.5 | t = 15.82 | < 0.001 |
| Oral intake resumed (hour) | 52.4 ± 14.2 | 32.6 ± 9.8 | t = 13.45 | < 0.001 |
| Post-operative LOS (day) | 5.8 ± 1.4 | 3.2 ± 0.9 | t = 18.74 | < 0.001 |
| Overall morbidity | 26 (18.3) | 9 (4.8) | χ2 = 15.87 | < 0.001 |
| Wound infection | 8 (5.6) | 5 (2.7) | ||
| Intra-abdominal abscess | 7 (4.9) | 2 (1.1) | ||
| Ileus | 6 (4.2) | 2 (1.1) | ||
| Wound dehiscence | 3 (2.1) | 0 (0) | ||
| Pneumonia | 2 (1.4) | 0 (0) |
Acute appendicitis, as one of the most common surgical emergencies, has always been a focus of clinical attention regarding its diagnosis and treatment strategy selection[17,18]. Traditional diagnostic approaches mainly rely on clinical symptoms, signs, and laboratory tests, but these methods have limited ability to differentiate appendicitis pathological types. With the development of minimally invasive surgical techniques, laparoscopic appendectomy has become the preferred treatment for acute appendicitis due to its advantages of minimal trauma and rapid recovery[19,20]. However, not all types of appendicitis are suitable for laparoscopic surgery. Suppurative appendicitis, with inflammation involving all layers, severe tissue edema, and obvious surrounding adhesions, significantly increases surgical difficulty, with some patients requiring conversion to open surgery or direct open surgery selection, and significantly higher postoperative complication rates[16,21]. Therefore, accurate preoperative differentiation of appendicitis pathological types is of great clinical significance for formulating individualized surgical plans, reducing surgical risks, and minimizing postoperative complications.
Imaging examinations play an increasingly important role in acute appendicitis diagnosis. Although CT is considered the gold standard imaging method for diagnosing acute appendicitis, it has drawbacks including radiation exposure, high cost, and long examination time, particularly for young women, pregnant women, and pediatric patients, where repeated radiation exposure should be avoided[22]. MRI, while radiation-free, involves even longer examination times and higher costs, limiting its application in emergency settings. In contrast, color Doppler ultrasound, as a non-invasive, radiation-free, rapid, and economical imaging method, has unique advantages in acute appendicitis diagnosis[17,23]. Ultrasound can provide real-time dynamic observation of morphological changes including appendiceal diameter, wall thickness, intraluminal contents, and peri-appendiceal fluid, while color Doppler flow imaging can assess blood perfusion in the appendiceal wall, reflecting inflammation severity. In recent years, with improvements in ultrasound equipment resolution and increasingly mature operational techniques, the value of ultrasound in acute appendicitis diagnosis has been widely recognized[24].
The innovation of this study lies not only in focusing on qualitative diagnosis of acute appendicitis by ultrasound, but more importantly in exploring the application value of ultrasound in preoperative differentiation of different pathological types of appendicitis. Through retrospective analysis of 328 patients with pathologically confirmed acute appendicitis, we systematically evaluated the diagnostic value of key ultrasound parameters including maximum appendiceal diameter, appendiceal wall thickness, and blood flow signal grade, and determined optimal diagnostic thresholds for each parameter through ROC curve analysis[25]. The study found that maximum appendiceal diameter ≥ 9.8 mm, appendiceal wall thickness ≥ 3.2 mm, and blood flow signal grade ≥ II were independent risk factors for predicting suppurative appendicitis, and the combined diagnostic model based on these three parameters demonstrated higher diagnostic performance. These quantitative indicators provide objective diagnostic evidence for clinicians, helping to accurately assess appendicitis severity preoperatively.
Our established diagnostic thresholds show both concordance and notable differences with previous studies. For maximum appendiceal diameter, our threshold of 9.8 mm aligns closely with Rettenbacher who reported 10 mm as the optimal cutoff for acute appendicitis, though their study did not differentiate pathological subtypes. However, our threshold is slightly higher than the 7-8 mm reported in some earlier studies using lower-resolution equipment, likely reflecting improvements in ultrasound technology that allow more precise measurements of wall edema and inflammation. For appendiceal wall thickness, our cutoff of 3.2 mm represents a more stringent threshold compared to the 2.5-3.0 mm ranges reported in previous literature. This difference may reflect our specific focus on differentiating suppurative from simple appendicitis, rather than distinguishing normal from inflamed appendix. Our blood flow grading system (grade II as the cutoff) is consistent with Quillin and Siegel’s work on color Doppler findings, though they used a less standardized grading approach. The innovation of our study lies in combining these three parameters into a unified diagnostic model with quantitative thresholds specifically validated for preoperative pathological type differentiation, which has not been systematically investigated in previous research.
Preoperative ultrasound typing diagnosis has important guiding significance for surgical decision-making. Traditionally, surgical approach selection mainly depended on surgeons' clinical experience and intraoperative judgment, lacking objective preoperative assessment criteria[26]. This study found that among patients with preoperative ultrasound diagnosis of suppurative appendicitis, over 70% ultimately underwent open surgery or conversion to open surgery, while over 85% of patients with preoperative ultrasound diagnosis of simple appendicitis successfully com
The postoperative complication rate was significantly higher in suppurative appendicitis patients than in simple appendicitis patients, which is closely related to disease severity and increased surgical difficulty[16,21]. Due to inflammation involving all layers, severe tissue edema, and obvious surrounding adhesions in suppurative appendicitis, surgical manipulation is more difficult, with greater intraoperative tissue damage, making it prone to complications such as wound infection, intra-abdominal abscess, and intestinal obstruction. This study found that through accurate preoperative ultrasound typing diagnosis, high-risk patients can be identified, and targeted perioperative management measures can be taken, such as selecting appropriate surgical approaches, enhancing postoperative monitoring, and prophylactic antibiotic use, which helps reduce complication rates and improve patient prognosis.
It should be noted that the diagnostic accuracy of color Doppler ultrasound is affected by multiple factors[23]. First, ultrasound examination has certain operator dependence, with the examiner’s experience and technical level directly affecting diagnostic quality. This study minimized operator error by having experienced ultrasound physicians perform examinations according to standardized protocols and conducting repeated measurements of key parameters. Second, patient body habitus, bowel gas interference, and appendiceal position also affect ultrasound image quality, with approximately 6.7% of patients failing to clearly visualize the appendix due to various reasons. For these patients, other imaging methods may need to be combined for comprehensive judgment. Additionally, ultrasound examination should be performed by experienced operators and combined with clinical presentation and laboratory test results for comprehensive analysis, rather than relying solely on ultrasound findings for diagnosis[22,24].
To address the operator-dependent nature of ultrasound examination and enhance reproducibility across different centers and sonographers, we propose several concrete measures for future clinical implementation. First, we recommend the development and adoption of a standardized imaging protocol that specifies: (1) Patient positioning (supine with systematic graded compression technique); (2) Probe selection criteria (linear array 7-12 MHz for superficial structures, convex array 3.5-5 MHz for obese patients); (3) Standardized scanning planes (transverse and longitudinal views with complete appendiceal visualization); and (4) Measurement techniques with explicit anatomical landmarks (maximal outer diameter perpendicular to long axis, full-thickness wall measurement from outer serosa to inner mucosa).
This study also has certain limitations. First, as a retrospective study, there may be selection bias and information bias. Second, this study only included patients who ultimately received surgical treatment, excluding appendicitis patients treated conservatively, which may affect the generalizability of results. Third, this study did not include gangrenous and perforated appendicitis patients; these more severe pathological types also need accurate identification in clinical practice[27]. Future multicenter, large-sample prospective studies are needed to further validate ultrasound parameter diagnostic thresholds and explore the application value of ultrasound typing diagnosis in different appendicitis subtypes[25]. Additionally, with the development of artificial intelligence and machine learning technologies, applying these technologies to ultrasound image analysis may further improve diagnostic accuracy and objectivity, which is also an important direction for future research.
Color Doppler ultrasound can effectively differentiate acute simple appendicitis from suppurative appendicitis before appendectomy. Maximum appendiceal diameter ≥ 9.8 mm, appendiceal wall thickness ≥ 3.2 mm, and blood flow signal grade ≥ II are independent risk factors for predicting suppurative appendicitis. The combined diagnostic model based on these parameters demonstrates high diagnostic performance, with preoperative prediction accuracy reaching 89.3% and high concordance with postoperative pathological diagnosis. Accurate preoperative ultrasound typing diagnosis pro
| 1. | Addiss DG, Shaffer N, Fowler BS, Tauxe RV. The epidemiology of appendicitis and appendectomy in the United States. Am J Epidemiol. 1990;132:910-925. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1608] [Cited by in RCA: 1283] [Article Influence: 35.6] [Reference Citation Analysis (1)] |
| 2. | Ceresoli M, Zucchi A, Allievi N, Harbi A, Pisano M, Montori G, Heyer A, Nita GE, Ansaloni L, Coccolini F. Acute appendicitis: Epidemiology, treatment and outcomes- analysis of 16544 consecutive cases. World J Gastrointest Surg. 2016;8:693-699. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 46] [Cited by in RCA: 51] [Article Influence: 5.1] [Reference Citation Analysis (4)] |
| 3. | Bhangu A, Søreide K, Di Saverio S, Assarsson JH, Drake FT. Acute appendicitis: modern understanding of pathogenesis, diagnosis, and management. Lancet. 2015;386:1278-1287. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 949] [Cited by in RCA: 762] [Article Influence: 69.3] [Reference Citation Analysis (1)] |
| 4. | Di Saverio S, Podda M, De Simone B, Ceresoli M, Augustin G, Gori A, Boermeester M, Sartelli M, Coccolini F, Tarasconi A, De' Angelis N, Weber DG, Tolonen M, Birindelli A, Biffl W, Moore EE, Kelly M, Soreide K, Kashuk J, Ten Broek R, Gomes CA, Sugrue M, Davies RJ, Damaskos D, Leppäniemi A, Kirkpatrick A, Peitzman AB, Fraga GP, Maier RV, Coimbra R, Chiarugi M, Sganga G, Pisanu A, De' Angelis GL, Tan E, Van Goor H, Pata F, Di Carlo I, Chiara O, Litvin A, Campanile FC, Sakakushev B, Tomadze G, Demetrashvili Z, Latifi R, Abu-Zidan F, Romeo O, Segovia-Lohse H, Baiocchi G, Costa D, Rizoli S, Balogh ZJ, Bendinelli C, Scalea T, Ivatury R, Velmahos G, Andersson R, Kluger Y, Ansaloni L, Catena F. Diagnosis and treatment of acute appendicitis: 2020 update of the WSES Jerusalem guidelines. World J Emerg Surg. 2020;15:27. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 923] [Cited by in RCA: 728] [Article Influence: 121.3] [Reference Citation Analysis (3)] |
| 5. | Southgate E, Vousden N, Karthikesalingam A, Markar SR, Black S, Zaidi A. Laparoscopic vs open appendectomy in older patients. Arch Surg. 2012;147:557-562. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 39] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 6. | Masoomi H, Nguyen NT, Dolich MO, Wikholm L, Naderi N, Mills S, Stamos MJ. Comparison of laparoscopic versus open appendectomy for acute nonperforated and perforated appendicitis in the obese population. Am J Surg. 2011;202:733-739. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 31] [Article Influence: 2.1] [Reference Citation Analysis (1)] |
| 7. | Alvarado A. A practical score for the early diagnosis of acute appendicitis. Ann Emerg Med. 1986;15:557-564. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 838] [Cited by in RCA: 809] [Article Influence: 20.2] [Reference Citation Analysis (2)] |
| 8. | Andersson M, Andersson RE. The appendicitis inflammatory response score: a tool for the diagnosis of acute appendicitis that outperforms the Alvarado score. World J Surg. 2008;32:1843-1849. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 219] [Cited by in RCA: 229] [Article Influence: 12.7] [Reference Citation Analysis (1)] |
| 9. | Ohmann C, Franke C, Kraemer M, Yang Q. [Status report on epidemiology of acute appendicitis]. Chirurg. 2002;73:769-776. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 41] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 10. | Pooler BD, Lawrence EM, Pickhardt PJ. Alternative diagnoses to suspected appendicitis at CT. Radiology. 2012;265:733-742. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 47] [Article Influence: 3.4] [Reference Citation Analysis (1)] |
| 11. | Duke E, Kalb B, Arif-Tiwari H, Daye ZJ, Gilbertson-Dahdal D, Keim SM, Martin DR. A Systematic Review and Meta-Analysis of Diagnostic Performance of MRI for Evaluation of Acute Appendicitis. AJR Am J Roentgenol. 2016;206:508-517. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 133] [Cited by in RCA: 100] [Article Influence: 10.0] [Reference Citation Analysis (1)] |
| 12. | Puylaert JB. Acute appendicitis: US evaluation using graded compression. Radiology. 1986;158:355-360. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 512] [Cited by in RCA: 382] [Article Influence: 9.6] [Reference Citation Analysis (1)] |
| 13. | Roberts K, Moore H, Raju M, Gent R, Piotto L, Taranath A, Ee M, Linke R, Goh DW. Diagnostic Ultrasound for Acute Appendicitis: The Gold Standard. J Pediatr Surg. 2024;59:235-239. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 14] [Reference Citation Analysis (1)] |
| 14. | Quillin SP, Siegel MJ. Appendicitis: efficacy of color Doppler sonography. Radiology. 1994;191:557-560. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 65] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 15. | Al-Ajerami Y. Sensitivity and specificity of ultrasound in the diagnosis of acute appendicitis. East Mediterr Health J. 2012;18:66-69. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 17] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 16. | Lin HF, Wu JM, Tseng LM, Chen KH, Huang SH, Lai IR. Laparoscopic versus open appendectomy for perforated appendicitis. J Gastrointest Surg. 2006;10:906-910. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 53] [Article Influence: 2.7] [Reference Citation Analysis (1)] |
| 17. | Puylaert JB. Mesenteric adenitis and acute terminal ileitis: US evaluation using graded compression. Radiology. 1986;161:691-695. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 100] [Cited by in RCA: 76] [Article Influence: 1.9] [Reference Citation Analysis (1)] |
| 18. | Ferris M, Quan S, Kaplan BS, Molodecky N, Ball CG, Chernoff GW, Bhala N, Ghosh S, Dixon E, Ng S, Kaplan GG. The Global Incidence of Appendicitis: A Systematic Review of Population-based Studies. Ann Surg. 2017;266:237-241. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 459] [Cited by in RCA: 389] [Article Influence: 43.2] [Reference Citation Analysis (1)] |
| 19. | Quah GS, Eslick GD, Cox MR. Laparoscopic appendicectomy is superior to open surgery for complicated appendicitis. Surg Endosc. 2019;33:2072-2082. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 60] [Article Influence: 8.6] [Reference Citation Analysis (1)] |
| 20. | Sauerland S, Jaschinski T, Neugebauer EA. Laparoscopic versus open surgery for suspected appendicitis. Cochrane Database Syst Rev. 2010;CD001546. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 209] [Cited by in RCA: 230] [Article Influence: 14.4] [Reference Citation Analysis (1)] |
| 21. | Wang X, Zhang W, Yang X, Shao J, Zhou X, Yuan J. Complicated appendicitis in children: is laparoscopic appendectomy appropriate? A comparative study with the open appendectomy--our experience. J Pediatr Surg. 2009;44:1924-1927. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 59] [Cited by in RCA: 47] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 22. | Moris D, Paulson EK, Pappas TN. Diagnosis and Management of Acute Appendicitis in Adults: A Review. JAMA. 2021;326:2299-2311. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 283] [Cited by in RCA: 221] [Article Influence: 44.2] [Reference Citation Analysis (1)] |
| 23. | Mostbeck G, Adam EJ, Nielsen MB, Claudon M, Clevert D, Nicolau C, Nyhsen C, Owens CM. How to diagnose acute appendicitis: ultrasound first. Insights Imaging. 2016;7:255-263. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 83] [Cited by in RCA: 103] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 24. | Giljaca V, Nadarevic T, Poropat G, Nadarevic VS, Stimac D. Diagnostic Accuracy of Abdominal Ultrasound for Diagnosis of Acute Appendicitis: Systematic Review and Meta-analysis. World J Surg. 2017;41:693-700. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 57] [Article Influence: 6.3] [Reference Citation Analysis (1)] |
| 25. | Rettenbacher T, Hollerweger A, Macheiner P, Rettenbacher L, Tomaselli F, Schneider B, Gritzmann N. Outer diameter of the vermiform appendix as a sign of acute appendicitis: evaluation at US. Radiology. 2001;218:757-762. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 98] [Cited by in RCA: 75] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 26. | Ebell MH, Shinholser J. What are the most clinically useful cutoffs for the Alvarado and Pediatric Appendicitis Scores? A systematic review. Ann Emerg Med. 2014;64:365-372.e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 89] [Cited by in RCA: 74] [Article Influence: 6.2] [Reference Citation Analysis (1)] |
| 27. | Simillis C, Symeonides P, Shorthouse AJ, Tekkis PP. A meta-analysis comparing conservative treatment versus acute appendectomy for complicated appendicitis (abscess or phlegmon). Surgery. 2010;147:818-829. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 280] [Cited by in RCA: 224] [Article Influence: 14.0] [Reference Citation Analysis (1)] |