Published online Mar 27, 2026. doi: 10.4240/wjgs.v18.i3.116575
Revised: December 13, 2025
Accepted: January 15, 2026
Published online: March 27, 2026
Processing time: 133 Days and 13.3 Hours
Obstructed defecation syndrome (ODS) frequently results from an internal rectal prolapse, which disrupts the rectal axis and impairs evacuation. Resectional transanal operations can remove redundant tissue, but fail to restore structural support, whereas abdominal mesh rectopexy involves prosthetic materials and has a higher operative burden. The sutured rectal lift (SuReL) was developed as a reconstructive, non-resective, and mesh-free transanal technique to restore rectal suspension while preserving continence in patients with ODS secondary to internal prolapse.
To describe the rationale, indications, and step-by-step operative technique of SuReL for Oxford grade II-III internal rectal prolapse causing obstructed defe
SuReL was performed using the Sylarum® transanal access device. The rectal wall was addressed sequentially in six circumferential sectors (11, 1, 9, 3, 7, and 5 o’clock). In each sector, a triphasic suture sequence with a barbed 0/0 monofilament (Filbloc®) was placed: (1) A mucosa-submucosa pass; (2) A deeper pass including the muscularis layer at the same level; and (3) A third pass 3 mm caudally, forming a semiloop for suspension. Cranial plications advanced distally to the upper limit of the prolapse. A deep circumferential reinforcement layer with a 2/0 Assuplus® monofilament consolidated the lift.
The procedure standardizes the reconstructive phase through sector-based rotation, allowing symmetric traction and full-thickness suspension without resection. Operative pearls consist of maintaining uniform exposure, ensuring precise semiloop depth for tension control, and verifying lumen patency with saline irrigation. Key technical advantages include the absence of stapling devices or prosthetic materials, minimal bleeding, a short operative time, and preservation of mucosal sensitivity. Postoperative recovery is typically rapid with early mobilization and minimal discomfort.
SuReL represents a technically reproducible and standardized approach for the treatment of internal rectal prolapse. This preclinical study demonstrated feasibility and mechanical consistency using anatomical simulators, while the clinical efficacy and physiological benefits remain to be validated in prospective trials.
Core Tip: Obstructed defecation syndrome due to internal rectal prolapse requires options beyond resection or mesh rectopexy. Sutured rectal lift is a physiological, mesh-free, sphincter-preserving transanal suspension. This basic study details the anatomic rationale, step-by-step standardization, and bench validation of suture-based lift to restore the rectal axis and compliance. By focusing on Oxford grade II–III prolapse and excluding multicompartmental descent, we provide reproducible technical guidance and implementation pearls that are distinct from the clinical outcomes reported elsewhere. The aim was to enable safe adoption, inform the study design, and avoid data overlap with prior clinical series.
- Citation: Pagano CE, Sarnari S, Favetta U, Picheo R, Gambarini F, Guttadauro A, Schiano di Visconte M. Sutured rectal lift for obstructed defecation: Mesh-free sphincter-preserving transanal technique for Oxford grade II-III prolapse. World J Gastrointest Surg 2026; 18(3): 116575
- URL: https://www.wjgnet.com/1948-9366/full/v18/i3/116575.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i3.116575
Obstructed defecation syndrome (ODS) is a multifactorial pelvic floor disorder that markedly impairs quality of life through chronic straining, incomplete evacuation, and the need for manual assistance or laxatives[1-3]. ODS results from a spectrum of structural (internal rectal prolapse, rectocele, multicompartment pelvic organ prolapse) and functional mechanisms (slow-transit constipation/rectal inertia, pelvic floor dyssynergia with spastic sphincter); therefore, accurate phenotyping is mandatory before selecting an anatomical repair[1]. Among the structural contributors, internal rectal prolapse and rectocele are the most clinically relevant because they distort the rectal axis and disrupt the coordinated defecation.
The Oxford classification system provides a reproducible framework for grading internal rectal prolapse and guiding therapeutic decision making[4]. Grades II–III defined as intussusception reaching or slightly exceeding the internal anal canal without externalization, usually represent the threshold for surgical intervention after the failure of conservative management.
Surgical strategies for ODS include stapled transanal rectal resection (STARR), laparoscopic ventral mesh rectopexy (LVMR), and abdominal suture rectopexy. STARR offers immediate mechanical correction through the resection of redundant tissue[5], however its circumferential staple line may compromise rectal compliance and sensory function, occasionally resulting in postoperative urgency or incontinence[5-9]. Conversely, LVMR provides durable anatomical correction and lower recurrence rates but entails the use of prosthetic mesh and an abdominal approach, with potential mesh-related complications such as erosion, chronic pelvic pain, or infection[10-13]. Abdominal rectopexy achieves stable fixation yet requires extensive dissection and carries the risk of postoperative constipation or autonomic nerve injury[14].
The ongoing debate between the transanal and ventral approaches underscores the need for a minimally invasive, sphincter-preserving, mesh-free alternative that restores the physiological rectal axis while maintaining compliance and continence[15]. The sutured rectal lift (SuReL) was developed to meet this requirement. It is a reconstructive, non-resective transanal technique that achieves cranial suspension of the rectal wall through full-thickness suturing, avoids prosthetic materials, and preserves the mucosal integrity.
The present basic study aimed to describe the anatomical rationale, operative concept, and standardized technical steps of SuReL for Oxford grade II-III internal rectal prolapse. This study focused exclusively on preclinical validation and procedural standardization, whereas the clinical outcomes will be addressed in future prospective studies.
The rectal wall serves as both a compliant reservoir and dynamic structure that supports coordinated evacuation. Internal rectal prolapse occurs when the mucosal and submucosal layers invaginate into the lumen as a result of weakened rectal wall and pelvic attachments[16,17]. In Oxford grade II-III prolapse, the redundant segment forms an intrarectal “sleeve” that impedes evacuation while remaining contained within the anal canal.
Resectional procedures such as STARR mechanically correct the prolapse but compromise rectal compliance and sensory integrity[5]. Conversely, prosthetic suspensions such as LVMR restore anatomical alignment yet require foreign material and an abdominal approach, increasing operative complexity and potential for mesh-related complications[10]. Traditional suture-based abdominal rectopexy also achieves fixation, but involves extensive dissection and may impair pelvic nerve function, leading to postoperative constipation[14].
SuReL is conceived as a physiological suspension through intrinsic fixation. Rather than excising or reinforcing the tissue with a mesh, SuReL repositions and re-anchors the mucosa, submucosa, and muscular complex cranially using full-thickness barbed sutures. This creates a vertical “lift” that restores rectal alignment and relieves outlet obstruction while maintaining compliance.
The procedure employs a triphasic suture pattern: Superficial (mucosa–submucosa), deep (muscularis propria), and caudal anchoring semiloops, forming a self-stabilizing three-dimensional column. These sutures are evenly distributed across the six sectors and provide symmetric traction, prevent torsion, and preserve vascularity. Thus, this technique achieves immediate mechanical correction without resection or fibrosis, thereby minimizing ischemia, pain, and postoperative dysfunction.
In contrast to conventional mucopexy, which relies on reactive fibrosis for long-term fixation, the SuReL provides direct mechanical elevation and internal reinforcement. Its key conceptual advantages include sphincter preservation, mesh-free repair, potential preservation of rectal compliance, and suitability for short-stay surgery; however, these conceptual advantages require clinical validation.
This basic study was designed to describe and validate the technical developments in the SuReL procedure. No human or animal subjects were included in this study. The technique was conceptualized and standardized using synthetic an
Since no live tissues or identifiable data were used, Institutional Review Board approval was not required. Procedural validation focused exclusively on the reproducibility of the standardized six-sector suture sequence and mechanical integrity of the reconstructed rectal lumen. Each simulation was recorded using high-resolution imaging to document the sequence and assess luminal patency after reconstruction.
The simulators consisted of multilayered silicone composites engineered to reproduce the wall compliance, elasticity, and friction properties of a native rectum. Dimensional fidelity was verified by comparison with magnetic resonance imaging (MRI)-derived three-dimensional pelvic models, maintaining a ± 5% tolerance for the rectal curvature and canal diameter. Functional fidelity was assessed by measuring deformation and recoil under standardized traction loads (1-2 N) applied to the mucosa-muscularis complex, confirming linear elastic behavior analogous to that of native tissue.
This preclinical model ensured a controlled and reproducible environment for evaluating the technical feasibility and standardization of SuReL. Because no biological or clinical data were collected, statistical analyses were not performed.
The standardized six-sector suture sequence was consistently completed across all simulated models. The triphasic suture pattern and superficial, deep, and caudal anchoring passes were reproducibly performed in each sector to achieve uniform cranial plication without tissue tearing or luminal distortion.
Saline irrigation confirmed complete hemostasis and rectal patency throughout the reconstructed circumference. No disruption, suture slippage, or asymmetric traction occurred when the recommended tension protocol was applied.
The deep reinforcement layer could be applied circumferentially without narrowing the lumen, resulting in stable and symmetric elevation of the rectal wall. Overall, the bench simulations confirmed the technical feasibility and reproducibility of SuReL under controlled experimental conditions.
A comprehensive preoperative assessment encompassing detailed radiological, instrumental, and functional evaluations is essential for the management of internal rectal prolapse. Accurate preoperative characterization not only ensures proper indication and surgical planning but also enables exclusion of coexisting pelvic‐floor abnormalities that may otherwise compromise postoperative outcomes. The instrumental work-up should systematically include the following investigations:
Colonoscopy: This examination is essential to exclude alternative or concomitant causes of rectal bleeding or obstructive symptoms such as adenomatous polyps or colorectal neoplasia, particularly when a recent negative endoscopic report is unavailable.
Defecography or dynamic pelvic MRI: Conventional dynamic defecography remains the preferred diagnostic modality for quantifying the grade and type of internal rectal prolapse during near-physiological evacuation. When performed by an expert pelvic-floor radiologist, dynamic MRI offers superior multiplanar visualization of enterocele, sigmoidocele, rectocele, and other multicompartmental defects, thereby supporting an accurate differential diagnosis.
Anorectal manometry: Functional manometric assessment is particularly valuable for evaluating anal sphincter pressure, compliance, and rectoanal coordination in patients with reducible prolapse. The detection of paradoxical contractions or anismus requires preoperative biofeedback rehabilitation to restore coordinated evacuation before surgical intervention. High-resolution anorectal manometry allows quantification of the rectal propulsive pressure during simulated eva
Endoanal ultrasonography: This investigation is indicated when manometric findings suggest sphincter hypotonia or when a prior obstetric injury or iatrogenic lesion is suspected, allowing detailed assessment of internal and external sphincter integrity.
Colonic transit study: In patients with severe constipation, colonic transit time measurement helps differentiate slow-transit constipation from obstructed defecation. In cases where slow-transit constipation predominates, conservative management with targeted medical therapy and gastroenterological follow-up is essential before surgery. Fecal impaction, characterized by stool retention requiring manual or pharmacological disimpaction, must be differentiated from transient constipation, which reflects episodic stool hardness without outlet obstruction. Only patients with structural outlet obstruction (Oxford II-III internal prolapse) were considered candidates for SuReL.
Clinically, obstructed defecation is characterized by preserved rectal urge, excessive straining, a persistent sensation of incomplete evacuation, and the need for digital or vaginal assistance. Slow-transit constipation typically presents with infrequent bowel movements, reduced urge to defecate, and generalized stool retention, reflecting global colonic inertia rather than an evacuation disorder[18].
In addition to structural abnormalities, ODS may also arise from functional disorders such as rectal inertia and pelvic floor dyssynergia with a spastic anal sphincter. Anorectal manometry and colonic transit studies are therefore essential for distinguishing these pathophysiological mechanisms. Patients with markedly reduced rectal propulsive pressure consistent with rectal inertia and those with persistent dyssynergia or spastic anal sphincter despite optimized conservative treatment and biofeedback were not considered candidates for SuReL. Rectal inertia was specifically assessed through high-resolution anorectal manometry by evaluating rectal propulsive pressure during simulated evacuation, as fixation of a non-propulsive rectum would not correct and would even aggravate, obstructed defecation symptoms. This ensures that the SuReL is reserved exclusively for patients with preserved rectal propulsion. In such cases, suspending a non-propulsive rectum or an outlet obstructed by a functional spasm is unlikely to improve symptoms and may even exacerbate obstructed defecation. Instead, these patients are managed with motility-targeted medical therapy, neuromodulation, or alternative surgical strategies as appropriate, whereas SuReL is reserved for ODS driven predominantly by Oxford grade II-III internal rectal prolapse with preserved rectal propulsive function[19]. In selected refractory cases of anismus, temporary botulinum toxin injection may be used as an adjunctive functional therapy to facilitate pelvic floor rehabilitation, although this lies outside the anatomical scope of SuReL[20].
Neurophysiological testing: Evaluation of the pudendal nerve terminal motor latency and other relevant neuro
A rigorous multidisciplinary approach that integrates these diagnostic components refines patient selection, optimizes perioperative management, and maximizes functional benefits of the SuReL procedure.
Appropriate patient selection is essential to achieve optimal outcomes and prevent overtreatment. SuReL is indicated exclusively for patients with isolated Oxford grade II–III internal rectal prolapse in whom conservative management has failed. These individuals typically present with incomplete evacuation, excessive straining, or the need for digital assistance, while maintaining adequate sphincter function and preserving rectal propulsive activity.
Eligible patients are adults between 18 and 80 years of age with MRI-confirmed Oxford grade II-III internal rectal prolapse without external descent. Candidates must exhibit a Constipation Scoring System value of 12 or higher and an Obstructed Defecation Score of at least 10, with a Fecal Incontinence Severity Index below 10. All patients underwent optimized conservative therapy for at least 12 months, including dietary modification, pharmacological management, and pelvic floor rehabilitation, without sufficient symptom relief.
SuReL is contraindicated in the presence of multicompartmental pelvic organ prolapse, including rectocele greater than 3 cm, enterocele, cystocele, or uterine or vaginal vault descent. In these settings, combined or abdominal procedures such as laparoscopic/robotic ventral mesh rectopexy or synchronous perineal/posterior compartment repair are more appropriate than isolated transanal suspension. We deliberately excluded patients with clinically significant rectocele from the present conceptual and technical description to maintain a homogeneous model focused on isolated internal rectal prolapse and avoid undertreatment of complex multicompartmental defects[1].
Patients with predominant slow-transit constipation, rectal inertia, or unresolved pelvic floor dyssynergia (spastic anal sphincter) are excluded from SuReL candidacy, as functional obstruction due to impaired propulsion or persistent sphincteric spasm cannot be corrected using a structural suspension technique. In selected cases of refractory anismus, adjunctive nonsurgical therapies such as biofeedback or temporary botulinum toxin injection may be considered to improve sphincter relaxation. However, these modalities fall outside the anatomical scope of SuReL, which remains reserved for structural intrarectal prolapse with preserved rectoanal coordination. Additional exclusion criteria included previous pelvic-floor or rectal surgery, inflammatory bowel disease, malignancy, and active pelvic sepsis. Patients with neurological disorders, structural sphincter defects, pregnancy, contraindications to spinal anesthesia, or high-grade endometriosis were also deemed ineligible.
This strict anatomical definition clearly differentiates SuReL from operations designed for multicompartmental dysfunction, such as LVMR or posterior colporrhaphy. The absence of associated pelvic organ descent is a cornerstone of indication, confirming SuReL as a targeted solution for isolated intrarectal intussusception.
All patients underwent a complete preoperative proctologic evaluation, including high-resolution anorectal manometry and MRI defecography, to confirm Oxford grade II–III internal prolapse as the exclusive anatomical cause of ODS. The detection of a coexisting rectocele, cystocele, or uterine descent is an absolute contraindication to the procedure.
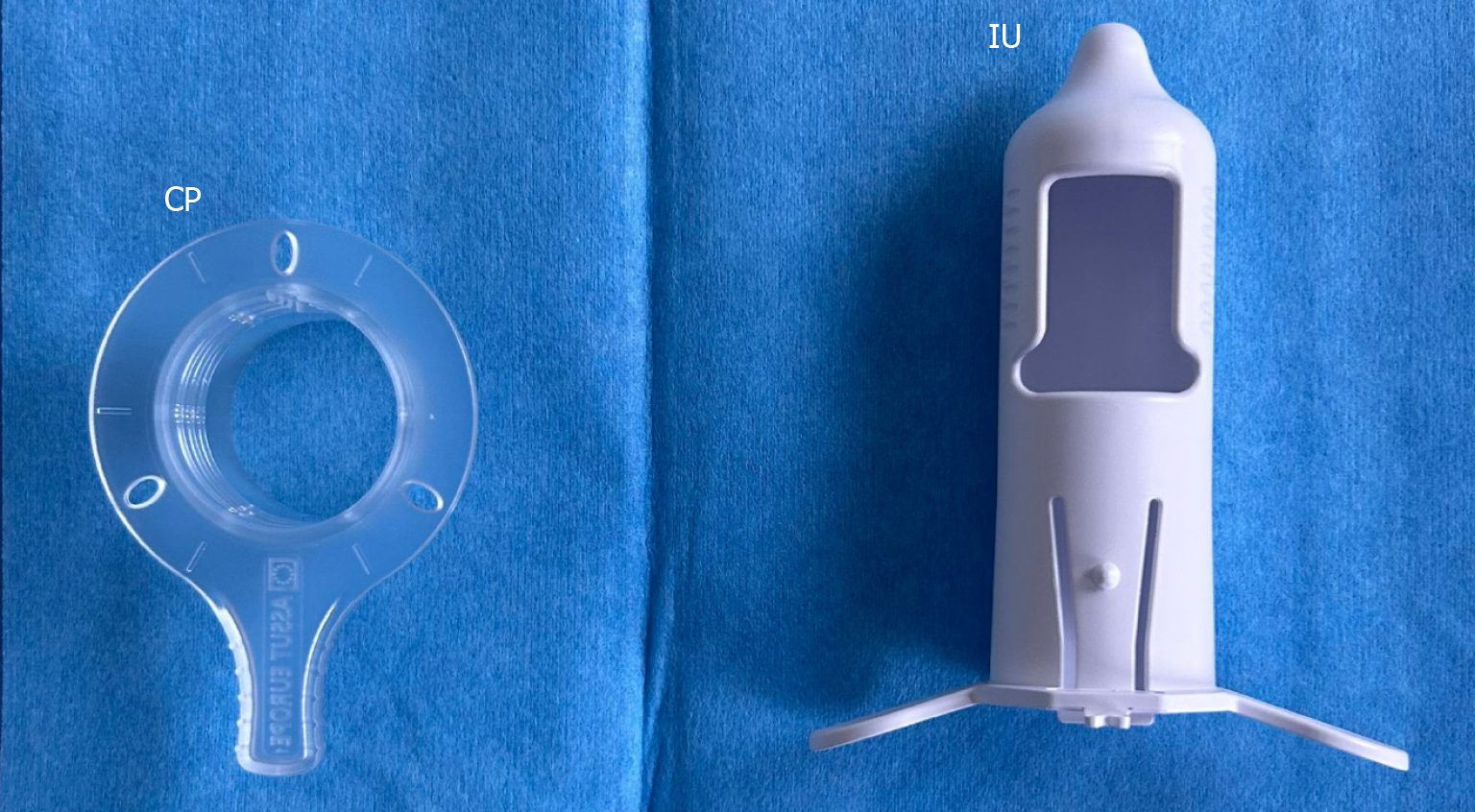
Bowel preparation consists of a low-residue diet for 48 hours and two cleansing enemas on the day before surgery. Prophylactic metronidazole (500 mg IV) is administered at induction. Mechanical bowel preparation is not required. The procedure is performed under spinal anesthesia with the patient in the lithotomy position. The anal verge is gently dilated, and a Sylarum® (Assut Europe SpA) is inserted and secured to the perineal skin using three natural non-absorbable braided sutures 1/0 (Perma-Hand Silk®; Ethicon Endo-Surgery, Inc., Pomezia, Italy) to ensure stable operative field exposure (Figure 1).
Each sector was approached using a standardized triphasic suture sequence using a synthetic barbed absorbable suture (Filbloc® 0/0, Assut Europe SpA).
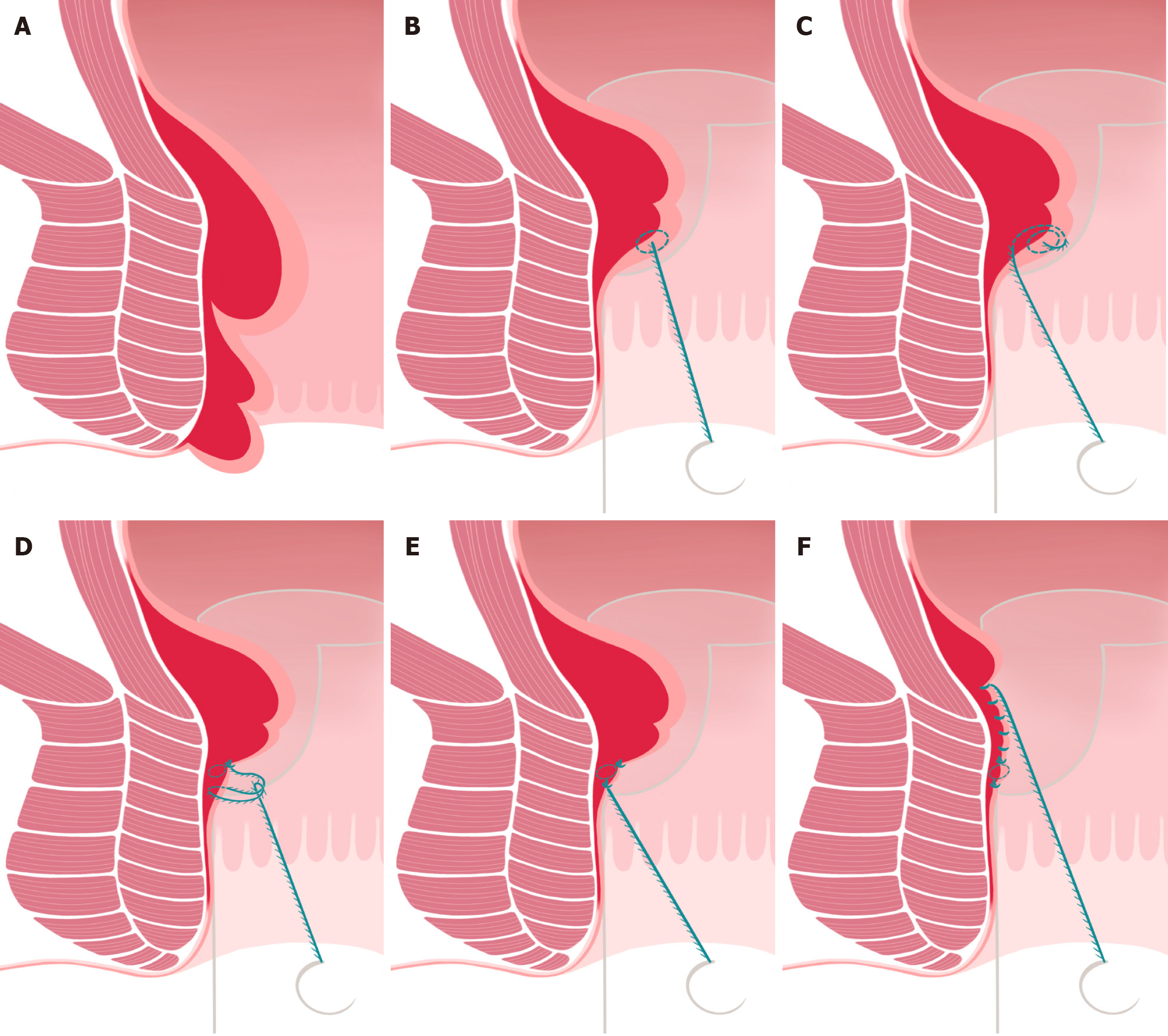
The operative window was first opened in the right anterolateral quadrant. Approximately 1.5-2 cm above the dentate line, a triphasic suture sequence was performed using a synthetic monofilament absorbable barbed suture 0/0 (Filbloc®; Assut Europe SpA). The first pass was superficial, involving the mucosa and submucosa, and was placed 1 cm above the lower edge of the operative window. The second pass, placed at the same level, was deeper and included the muscularis propria. The third pass was positioned 3 mm caudally, traversing the muscular layer, forming a semiloop to suspend the prolapsed tissue. The sutures were gently pulled cranially to elevate the rectal wall (Figure 2).
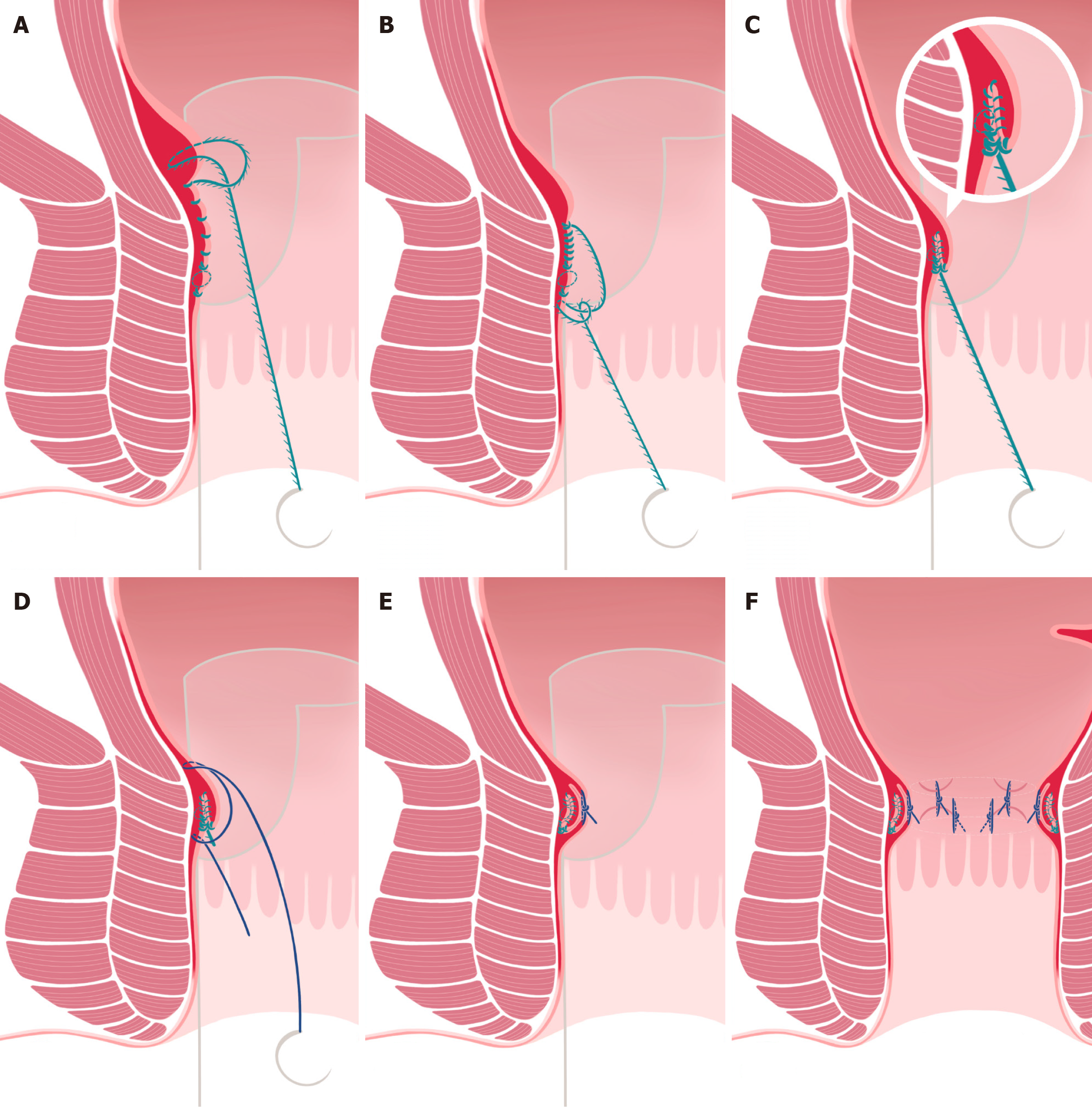
Subsequently, a structured cranial mucosal plication was performed. Additional stitches were placed at 3-5 mm intervals, starting 5 mm above the previous passes, incorporating the mucosa and submucosa and extending proximally to the upper margin of the prolapse. The final stitch in this series was secured as a second semiloop to complete the lift. A deep anchoring suture was placed 3 mm below the first stitch loop into the muscularis layer with another semiloop to reinforce the fixation, and the suture was trimmed to approximately 1 cm from the rectal wall. To strengthen the repair, a second layer of deep muscular reinforcement was applied using synthetic nonabsorbable monofilament sutures (Assuplus® 2/0, Assut Europe SpA). Deep stitches were placed 5 mm below and 5 mm above the existing suture line and then securely knotted to consolidate the rectal wall suspension (Figure 3).
This sequence is repeated for the remaining five sectors: Lateral right (9 o’clock), lateral left (3 o’clock), posterolateral right (7 o’clock), and posterolateral left (5 o’clock), according to a standardized rotational protocol. For each quadrant, the access device was rotated to allow optimal alignment and tension control.
After completing all six plications, the rectal ampulla was irrigated with normal saline to confirm hemostasis. Finally, the access device was withdrawn and a flat external dressing was applied for approximately one hour.
Meticulous adherence to specific technical details is fundamental to ensuring the safety, reproducibility, and long-term durability of the SuReL procedure. Stable exposure was achieved by securing the Sylarum® device, a transanal retractor (Assut Europe SpA) with three skin sutures, which provided optimal access and consistent visualization of all six operative sectors.
Each suture must include the muscularis propria to achieve durable traction and full-thickness suspension. Superficial sites are at risk of mucosal detachment or incomplete elevation. When handling barbed sutures, moderate and continuous tension should be maintained throughout the procedure, because excessive traction may compromise vascularity and tissue viability.
Sector symmetry is another crucial aspect of technical precision. The rectal wall should be approached sequentially in a clockwise fashion to guarantee uniform traction and to prevent torsion or asymmetric elevation of the rectal ampulla. A deep reinforcement layer using a nonabsorbable monofilament (Assuplus® 2/0) is mandatory to consolidate the lift and reduce the risk of late suture dehiscence.
Intraoperative hemostasis must be carefully verified using repeated saline irrigation and direct inspection after completing each sector. Electrocautery near the dentate line should be avoided to preserve the mucosal sensitivity and prevent postoperative discomfort. Common technical errors include over-resection, circumferential closure, or excessive cranial traction, all of which can lead to stenosis or distortion of the rectal lumen.
Ultimately, the key to reproducibility lies in controlled elevation, rather than excision. The surgeon must clearly visualize the upward shift of the mucosal plane while preserving the natural compliance of the rectal wall, thereby ensuring physiological and functionally effective reconstruction.
Postoperative care following SuReL is aimed at promoting early recovery and maintaining good functional outcomes. Analgesia is provided with paracetamol 1 g every eight hours for the first two days; ketoprofen is added if the visual analogue scale exceeds four. Routine antibiotic prophylaxis beyond induction is unnecessary because of the limited dissection and the aseptic nature of the procedure.
Patients resume oral intake on the first postoperative day, starting with a soft, fiber-rich diet to facilitate bowel movement. Early ambulation within six hours after surgery reduces thromboembolic risk and supports functional recovery.
A mild stool-regulating regimen, such as 10-15 mL of lactulose daily, is recommended for one week to avoid straining. The patients are discharged within 24-36 hours. Follow-up visits are scheduled at two weeks, three months, and subsequently every six months to assess healing, defecatory function, and long-term durability.
This study should be interpreted as a preclinical bench-validation study rather than a clinical investigation. These findings reflect technical feasibility and procedural standardization; therefore, their clinical applicability remains to be established through upcoming prospective trials.
SuReL introduces an alternative conceptual approach to the management of internal rectal prolapse by combining anatomical realignment through rectal suspension with the safety of a fully transanal, non-resective, and mesh-free technique. This procedure is based on the principle that rectal compliance is as critical as anatomical alignment for normal defecatory function. It is important to emphasize that this study does not include clinical, functional, or patient-reported outcomes. Consequently, any anticipated clinical advantages, such as improved compliance or reduced urgency, should be considered speculative until confirmed in future clinical investigations.
Unlike conventional mucopexy, which relies on reactive fibrosis for fixation, SuReL provides immediate mechanical support via full-thickness anchoring semiloops. This “autologous suspension” aims to preserve rectal elasticity and neurovascular integrity and may potentially reduce postoperative urgency, pain, and sensory impairment commonly observed after resective stapled procedures, although such benefits await clinical validation[5,6].
The STARR procedure remains a well-established transanal approach to ODS[16]. However, circumferential resection can alter the sensorimotor architecture of the rectal wall. Long-term studies report symptomatic recurrence rates of 30%-40%, postoperative urgency in 20%-30%, and new-onset fecal incontinence in up to 15% of patients[16,17]. Although refinements such as TST36HV® and Contour TRANSTAR® have improved resection precision, they have not eliminated the inherent drawbacks of tissue excision[9,21,22].
LVMR restores the physiological rectal axis and provides durable anatomical correction, with recurrence rates below 10% and sustained functional improvement[23-25]. Nevertheless, it requires prosthetic material and an abdominal approach, which increases the cost, complexity, and potential for mesh-related complications such as erosion or chronic pelvic pain.
Abdominal rectopexy, whether suture-based or resectional, offers reliable anatomic correction but at the cost of extensive dissection and higher morbidity. A meta-analysis of 1301 patients reported a 73.9% improvement in obstructed defecation, but a complication rate of 15% and recurrence rate of 5.8%[14]. New-onset constipation and delayed functional recovery occur in 10%-15% of cases, mainly due to autonomic nerve traction[14,26].
By contrast, SuReL achieves reconstructive suspension using full-thickness sutures alone, avoiding stapling devices or prosthetic materials. This technique aims to preserve rectal compliance, spare the dentate line and sphincter complex, and minimize ischemia by limiting dissection. Once standardized, the average operative time is 30 minutes, and patients are typically discharged within 24-36 hours. These characteristics make SuReL compatible with day surgery principles and potentially cost-effective in public healthcare systems. In our experience, the dedicated height-adjustable Sylarum™ transanal access platform facilitated reproducible 360° exposure and alignment with the dentate line, prevented mucosal prolapse into the working channel, and allowed the controlled placement of deep and superficial sutures in each sector, thereby supporting the standardization of the SuReL technique.
Preliminary preclinical simulations have demonstrated excellent correction of prolapse geometry and consistent restoration of rectal alignment, confirming technical feasibility and reproducibility under controlled conditions. Based on these findings, a multicenter randomized controlled trial, the SuReL-ODS Trial, is currently in preparation to compare SuReL with STARR and LVMR for the treatment of ODS caused by Oxford grade II-III internal prolapse. Formal ethics approval is pending before patient enrollment begins. The SuReL-ODS Trial is a planned multicenter randomized controlled trial designed to compare the efficacy and safety of SuReL vs STARR and LVMR in patients with Oxford grade II–III internal rectal prolapse and ODS. The study will include approximately 180 patients (60 per arm), randomized 1:1:1 to undergo SuReL, STARR, or LVMR, following the failure of standardized conservative management.
The primary endpoints will include changes in the Obstructed Defecation Score and Constipation Scoring System at 12 months. Secondary outcomes will include changes in anorectal manometry, patient-reported quality of life, continence, surgical morbidity, and recurrence rates.
As of manuscript submission, the protocol was finalized and is currently under review by the relevant ethics committees. Recruitment is expected to begin within the next 6-9 months, with results anticipated in 2027. This trial will provide the first clinical validation of the SuReL technique in a controlled comparative setting.
The conceptual framework of SuReL aligns with evidence from previous studies showing that procedures restoring anterior rectal support and the anorectal angle achieve superior pelvic floor function and long-term satisfaction compared with resective approaches[27-29]. Although preliminary bench simulations demonstrated consistent geometric correction and reproducibility, these results must be interpreted cautiously as they do not directly translate into clinical outcomes. The conceptual advantages of SuReL, its technical simplicity and potentially lower resource utilization compared with more extensive abdominal procedures, are strictly dependent on rigorous anatomical and functional patient selection. Only patients with isolated internal rectal prolapse and preserved rectal propulsion are likely to benefit from this minimally invasive concept, whereas its indiscriminate use outside this phenotype risks undertreatment and reduced clinical efficacy. The true functional impact and long-term safety of SuReL require validation through prospective multicenter trials.
In this context, prospective comparative studies against established transanal and transabdominal techniques are therefore warranted to define the relative efficacy and durability of SuReL.
The current SuReL concept applies exclusively to patients without associated vaginal, uterine, or bladder descent and without a clinically significant rectocele. It should not be used in cases of full-thickness external prolapse or complex multicompartmental disorders that require abdominal or combined pelvic reconstruction. Moreover, SuReL is not appropriate for patients with predominant slow-transit constipation, rectal inertia, or unresolved anismus, in whom a structural suspension cannot correct the underlying functional disturbance and may even exacerbate the symptoms. The present study is intentionally restricted to preclinical bench validation in synthetic anatomical models and therefore does not provide clinical, functional, or patient-reported outcomes. Future prospective and comparative clinical studies, including multicenter evaluations, are required to assess the safety, functional results, durability, and cost-effectiveness of SuReL and to determine how it performs in real patients relative to established techniques for ODS.
SuReL represents a promising sphincter-preserving and mesh-free reconstructive option for the treatment of Oxford grade II-III internal rectal prolapse. This Basic Study offers the first comprehensive technical standardization and preclinical bench validation of this procedure, demonstrating its feasibility, reproducibility, and geometric consistency in controlled simulated models. However, as no biological, functional, or patient-reported data were collected, these findings remain preliminary and should not be interpreted as evidence of clinical efficacy.
Future prospective studies, including the forthcoming multicenter SuReL-ODS Trial, are required to determine the long-term safety, functional performance, and comparative effectiveness of SuReL relative to established procedures such as STARR and LVMR. If validated, SuReL may emerge as a physiologically oriented and compliance-preserving alternative within the evolving landscape of transanal reconstructive surgery for obstructed defecation.
| 1. | Podzemny V, Pescatori LC, Pescatori M. Management of obstructed defecation. World J Gastroenterol. 2015;21:1053-1060. [PubMed] [DOI] [Full Text] |
| 2. | Bordeianou L, Ogilvie JW Jr, Saraidaridis JT, Olortegui KS, Ratto C, Ky AJ, Oliveira L, Vogler SA, Gurland BH; Steering Committee for the Pelvic Floor Disorders Consortium Quality Improvement in Rectal Prolapse Surgery Database Pilot. Durable Approaches to Recurrent Rectal Prolapse Repair May Require Avoidance of Index Procedure. Dis Colon Rectum. 2024;67:968-976. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 3. | Kim M, Meurette G, Ragu R, Lehur PA. Current surgical treatment of obstructed defecation among selected European opinion leaders in pelvic floor surgery. Tech Coloproctol. 2016;20:395-399. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 18] [Article Influence: 1.8] [Reference Citation Analysis (1)] |
| 4. | Pescatori M, Quondamcarlo C. A new grading of rectal internal mucosal prolapse and its correlation with diagnosis and treatment. Int J Colorectal Dis. 1999;14:245-249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 42] [Article Influence: 1.6] [Reference Citation Analysis (1)] |
| 5. | Schiano di Visconte M, Nicolì F, Pasquali A, Bellio G. Clinical outcomes of stapled transanal rectal resection for obstructed defaecation syndrome at 10-year follow-up. Colorectal Dis. 2018;20:614-622. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 15] [Article Influence: 1.9] [Reference Citation Analysis (1)] |
| 6. | Boccasanta P, Venturi M, Stuto A, Bottini C, Caviglia A, Carriero A, Mascagni D, Mauri R, Sofo L, Landolfi V. Stapled transanal rectal resection for outlet obstruction: a prospective, multicenter trial. Dis Colon Rectum. 2004;47:1285-96; discussion 1296. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 220] [Cited by in RCA: 164] [Article Influence: 7.5] [Reference Citation Analysis (1)] |
| 7. | Schwandner O, Fürst A; German STARR Registry Study Group. Assessing the safety, effectiveness, and quality of life after the STARR procedure for obstructed defecation: results of the German STARR registry. Langenbecks Arch Surg. 2010;395:505-513. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 43] [Article Influence: 2.7] [Reference Citation Analysis (1)] |
| 8. | Titu LV, Riyad K, Carter H, Dixon AR. Stapled transanal rectal resection for obstructed defecation: a cautionary tale. Dis Colon Rectum. 2009;52:1716-1722. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 22] [Article Influence: 1.3] [Reference Citation Analysis (2)] |
| 9. | Mari FS, Pezzatini M, Gasparrini M, Antonio B. STARR with Contour Transtar for Obstructed Defecation Syndrome: Long-Term Results. World J Surg. 2017;41:2906-2911. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 7] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 10. | D'Hoore A, Cadoni R, Penninckx F. Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg. 2004;91:1500-1505. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 463] [Cited by in RCA: 328] [Article Influence: 14.9] [Reference Citation Analysis (0)] |
| 11. | Consten EC, van Iersel JJ, Verheijen PM, Broeders IA, Wolthuis AM, D'Hoore A. Long-term Outcome After Laparoscopic Ventral Mesh Rectopexy: An Observational Study of 919 Consecutive Patients. Ann Surg. 2015;262:742-7; discussion 747. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 184] [Cited by in RCA: 136] [Article Influence: 12.4] [Reference Citation Analysis (1)] |
| 12. | Collinson R, Wijffels N, Cunningham C, Lindsey I. Laparoscopic ventral rectopexy for internal rectal prolapse: short-term functional results. Colorectal Dis. 2010;12:97-104. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 106] [Article Influence: 6.6] [Reference Citation Analysis (1)] |
| 13. | Emile SH, Elfeki H, Shalaby M, Sakr A, Sileri P, Wexner SD. Outcome of laparoscopic ventral mesh rectopexy for full-thickness external rectal prolapse: a systematic review, meta-analysis, and meta-regression analysis of the predictors for recurrence. Surg Endosc. 2019;33:2444-2455. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 54] [Article Influence: 7.7] [Reference Citation Analysis (0)] |
| 14. | Emile SH, Elfeki HA, Youssef M, Farid M, Wexner SD. Abdominal rectopexy for the treatment of internal rectal prolapse: a systematic review and meta-analysis. Colorectal Dis. 2017;19:O13-O24. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 42] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 15. | Schiano di Visconte M. Comparative clinical outcomes of ventral rectopexy versus STARR in the management of obstructed defecation syndrome: a clinical review. Updates Surg. 2025;77:1645-1655. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 16. | Ripamonti L, Guttadauro A, Lo Bianco G, Rennis M, Maternini M, Cioffi G, Chiarelli M, De Simone M, Cioffi U, Gabrielli F. Stapled Transanal Rectal Resection (Starr) in the Treatment of Obstructed Defecation: A Systematic Review. Front Surg. 2022;9:790287. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 10] [Article Influence: 2.5] [Reference Citation Analysis (1)] |
| 17. | Lian T, Wang N. Stapled trans-anal rectal resection can improve constipation symptoms and inflammatory reaction of patients with outlet obstructive constipation. Am J Transl Res. 2021;13:11472-11481. [PubMed] |
| 18. | Bunni J, Laugharne MJ. Pathophysiological basis, clinical assessment, investigation and management of patients with obstruction defecation syndrome. Langenbecks Arch Surg. 2023;408:75. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 19. | Ratuapli SK, Bharucha AE, Noelting J, Harvey DM, Zinsmeister AR. Phenotypic identification and classification of functional defecatory disorders using high-resolution anorectal manometry. Gastroenterology. 2013;144:314-322.e2. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 164] [Cited by in RCA: 140] [Article Influence: 10.8] [Reference Citation Analysis (1)] |
| 20. | Kaplan JA, Simianu VV. Pelvic Floor Nonrelaxation: Approach to Evaluation and Treatment. Clin Colon Rectal Surg. 2021;34:49-55. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 21. | Boccasanta P, Agradi S, Vergani C, Calabrò G, Bordoni L, Missaglia C, Venturi M. The evolution of transanal surgery for obstructed defecation syndrome: Mid-term results from a randomized study comparing double TST 36 HV and Contour TRANSTAR staplers. Am J Surg. 2018;216:893-899. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 8] [Article Influence: 1.0] [Reference Citation Analysis (2)] |
| 22. | Ribaric G, D'Hoore A, Schiffhorst G, Hempel E; TRANSTAR Registry Study Group. STARR with CONTOUR® TRANSTAR™ device for obstructed defecation syndrome: one-year real-world outcomes of the European TRANSTAR registry. Int J Colorectal Dis. 2014;29:611-622. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 42] [Cited by in RCA: 35] [Article Influence: 2.9] [Reference Citation Analysis (2)] |
| 23. | Barra M, Trilling B, Mastronicola G, Sage PY, Roudier A, Foote A, Tidadini F, Fournier J, Faucheron JL. Long-term outcome of laparoscopic ventral rectopexy for full-thickness rectal prolapse: the PEXITY study. Tech Coloproctol. 2025;29:68. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 9.0] [Reference Citation Analysis (1)] |
| 24. | Tsunoda A, Takahashi T, Matsuda S, Oka N, Kusanagi H. Midterm functional outcome after laparoscopic ventral rectopexy for external rectal prolapse. Asian J Endosc Surg. 2020;13:25-32. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 28] [Cited by in RCA: 19] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 25. | Lonne MLR, Cao AMY, Jenkin A, Convie LJ, Stevenson GE, Moloney JM, Stevenson ARL. Long-term Outcomes After Minimally Invasive Ventral Rectopexy for Rectal Prolapse Using Biological Graft Prosthesis: A 15-Year Retrospective Cohort Study. Dis Colon Rectum. 2025;68:608-615. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 26. | Graf W, Karlbom U, Påhlman L, Nilsson S, Ejerblad S. Functional results after abdominal suture rectopexy for rectal prolapse or intussusception. Eur J Surg. 1996;162:905-911. [PubMed] |
| 27. | Altomare DF, Picciariello A, Memeo R, Fanelli M, Digennaro R, Chetta N, De Fazio M. Pelvic floor function following ventral rectopexy versus STARR in the treatment of obstructed defecation. Tech Coloproctol. 2018;22:289-294. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 16] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 28. | Solari S, Martellucci J, Ascanelli S, Sturiale A, Annicchiarico A, Fabiani B, Prosperi P, Carcoforo P, Naldini G. Predictive factors for functional failure of ventral mesh rectopexy in the treatment of rectal prolapse and obstructed defecation. Tech Coloproctol. 2022;26:973-979. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 29. | Faucheron JL, Trilling B, Girard E, Sage PY, Barbois S, Reche F. Anterior rectopexy for full-thickness rectal prolapse: Technical and functional results. World J Gastroenterol. 2015;21:5049-5055. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 57] [Cited by in RCA: 62] [Article Influence: 5.6] [Reference Citation Analysis (1)] |