Published online Mar 27, 2026. doi: 10.4240/wjgs.v18.i3.115484
Revised: December 24, 2025
Accepted: January 20, 2026
Published online: March 27, 2026
Processing time: 155 Days and 10.9 Hours
The standard natural orifice specimen extraction surgery (NOSES) type IV pro
To retrospectively compare postoperative outcomes of standard NOSES and mo
A retrospective analysis was performed on 40 patients who underwent NOSES type IV surgery for rectosigmoid cancer at Shenzhen People’s Hospital between July 2021 and October 2025. The patients were divided into two groups: 19 treated with the modified NOSES procedure (modified group) and 21 treated with the standard NOSES procedure (control group). The baseline characteristics, peri
The modified group experienced less intraoperative blood loss, shorter operative time, and lower operative cost compared with the control group (all P < 0.05), and achieved earlier first defecation. One Grade B anastomotic leak occurred in the control group. Baseline characteristics, lymph node yield, postoperative pain, inflammatory markers, complication rates, and other recovery outcomes did not differ significantly between groups (all P > 0.05). In multivariable analysis, the modified procedure was independently associated with reduced operative cost (β = -1307, P < 0.001) and operative time (β = -49.9 minutes, P = 0.019). Larger tumor size and greater distance from the anus were associated with higher operative cost.
The modified NOSES technique may reduce operative trauma, shorten procedure time, lower perioperative resource use and accelerate postoperative recovery, with similar outcomes to the standard approach. These results require confirmation in larger, prospective multicenter studies.
Core Tip: This study compared the conventional and modified natural orifice specimen extraction surgery (NOSES) type IV procedures for rectosigmoid cancer. Compared to the conventional technique, the modified technique had simplified operative steps and eliminated the need for a circular stapler, thereby reducing operative time, blood loss, and surgical costs without compromising oncological safety. Postoperative recovery, including bowel function and complication rates, was comparable between groups. These findings suggest that the modified NOSES IV approach is a safe, efficient, and cost-effective alternative for minimally invasive radical resection of rectosigmoid cancer.
- Citation: Li YB, Zhu C, Xia LG, Sun X, Zhong KL, Li Y. Modified natural orifice specimen extraction type IV surgery for rectosigmoid cancer: A retrospective clinical study. World J Gastrointest Surg 2026; 18(3): 115484
- URL: https://www.wjgnet.com/1948-9366/full/v18/i3/115484.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i3.115484
Natural orifice specimen extraction surgery (NOSES) is a surgical technique in which a specimen is removed through a natural orifice, thereby avoiding an auxiliary abdominal incision. Since 2015, standardized procedures for NOSES have been systematically summarized in China. Under the efforts of Guan et al[1], this technique has been progressively implemented in hundreds of hospitals nationwide[2]. Clinical studies in China have demonstrated that NOSES can effectively reduce postoperative pain, accelerate recovery, and improve the patient’s quality of life[3], indicating that it is a feasible, safe, and effective surgical approach[1,4]. However, the standard NOSES procedure involves extensive manipulation of the lower gastrointestinal tract, which may result in a prolonged operative time, increased consumption of surgical supplies, and delayed postoperative bowel function recovery. These limitations highlight the need for modifications to the NOSES technique[5]. We have implemented modifications to the standard NOSES type IV procedure and achieved promising preliminary results. In this study, we compare the postoperative outcomes of standard NOSES and modified NOSES type IV techniques for radical resection of rectosigmoid cancer.
According to the Guidelines for Natural Orifice Specimen Extraction Surgery for Colorectal Tumors, 2023 Edition[6], the inclusion criteria were as follows: (1) Age 18-75 years; (2) Tumor stage T1-T3; (3) Complete clinical records; (4) Body mass index (BMI) ≤ 30 kg/m²; (5) Tumor characteristics: Protruding tumors with a circumferential diameter ≤ 5 cm, or ulcerative-infiltrative tumors involving less than half of the bowel circumference; adequate rectal and sigmoid colon length without stenosis or proximal diverticular disease; (6) Tumor location: High rectal tumors (lower margin ≥ 10 cm from the dentate line), rectosigmoid tumors, or distal sigmoid colon tumors; and (7) Successful completion of postopera
Exclusion criteria were: (1) Distant metastases or receipt of preoperative neoadjuvant chemotherapy; (2) Excessively thick sigmoid colon rendering specimen extraction difficult; (3) Presence of other primary malignancies; (4) Severe dysfunction of vital organs precluding surgery; and (5) Psychiatric disorders preventing cooperation with treatment or follow-up.
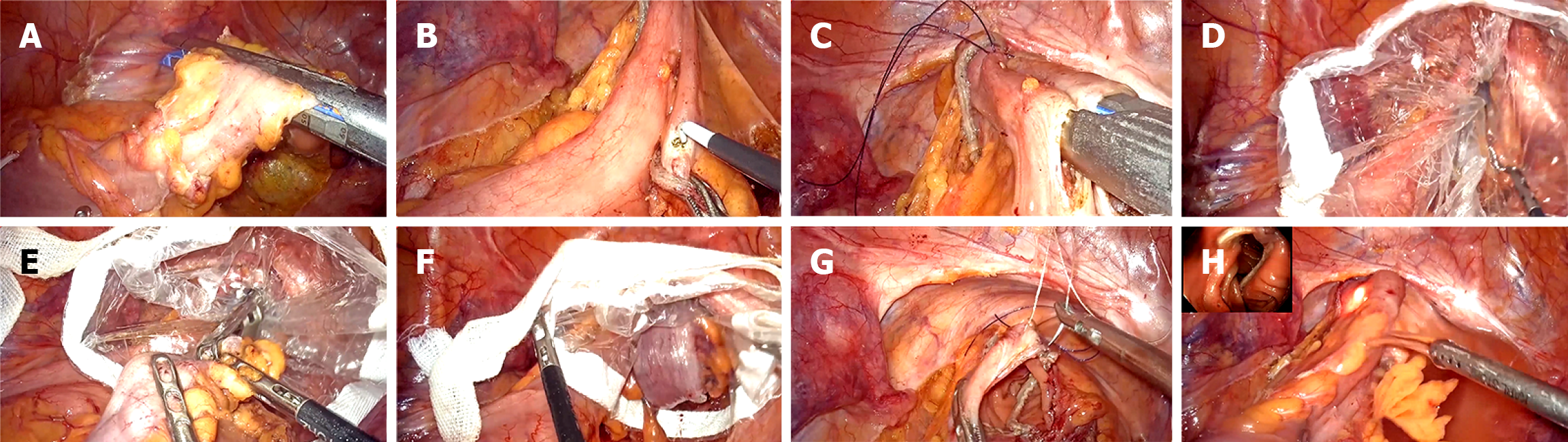
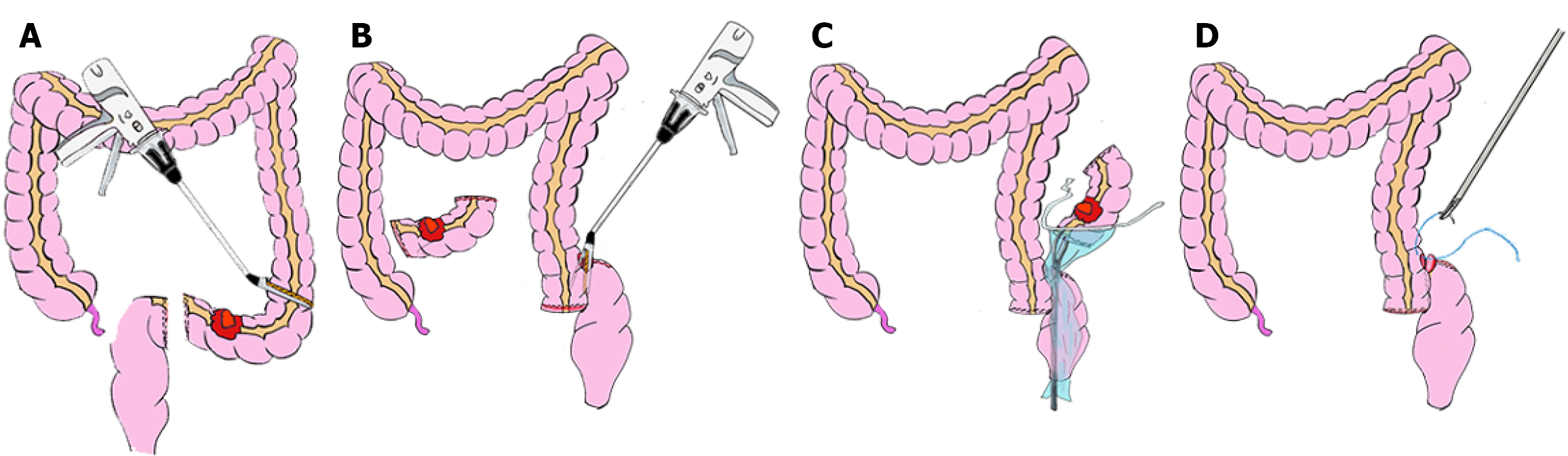
Patients in the modified NOSES group underwent radical resection of rectosigmoid cancer using the modified NOSES type IV procedure, with the intraoperative views shown in Figure 1 and the surgical steps illustrated in Figure 2. The procedure was performed as follows: (1) Radical resection was carried out following the principles of total mesorectal excision (TME)[7] to ensure oncological standards; (2) The proximal and distal bowel segments were aligned along the mesenteric edge, and the bowel wall was incised to insert the two jaws of a linear stapler. The stapler was fired to complete the overlapping anastomoses; (3) A wound protector was introduced through the common opening of the bowel, and the specimen was extracted transanally using grasping forceps. The common opening was closed with continuous 3-0 barbed sutures (Johnson & Johnson) and reinforced with seromuscular layer sutures; (4) Intraoperative colonoscopy was performed to confirm the integrity and quality of the anastomosis; and (5) Patients in the control group underwent radical resection of rectosigmoid cancer using the standard NOSES type IV procedure. The surgical steps were performed according to the following established protocols.
The procedure followed the principles of TME[7] to achieve radical resection with bloc mobilization of the tumor-bearing bowel segment.
The distal bowel was transected 5 cm beyond the tumor using a linear stapler. The bowel wall at the distal transection site was incised, and a wound protector was placed through this opening. After sufficient anal dilation, the anvil of the circular stapler was inserted transanally through the rectal opening into the abdominal cavity, and the wound protector was removed.
The proximal bowel was transected using a linear stapler. The proximal bowel wall was incised, and a circular stapler anvil was inserted. The anvil rod was removed through the bowel wall using the purse-string technique, and the proximal bowel opening was closed using a linear stapler.
The specimen was transanally extracted through the rectal opening using grasping forceps, and the distal bowel was closed using a linear stapler after removing the wound protector.
A circular stapler was introduced transanally, connecting the stapler guide tube and anvil rod. The stapler was fired to complete end-to-end bowel anastomosis.
Intraoperative colonoscopy was performed to confirm the integrity and quality of the anastomosis.
Perioperative parameters, including intraoperative blood loss, number of lymph nodes harvested, operative time, post
Postoperative pain was assessed using a 10-point Visual Analog Scale[8], with higher scores indicating greater pain. The pain scores at 24 hours postoperatively were collected for both the modified and standard NOSES groups.
All the statistical analyses were performed using SPSS version 26.0 (IBM Corp., Armonk, NY, United States). Continuous variables were expressed as the mean ± SD. For variables with homogeneity of variance, comparisons between groups were performed using independent-samples t tests; for variables with unequal variance, Welch’s t test or the Mann-Whitney U test was applied. Categorical variables were expressed as n (%) and compared using the χ2 test or continuity-corrected χ2 test. Ordinal data were analyzed using a rank-sum test. Statistical significance was defined as a two-sided P value of < 0.05. To control for potential confounding factors, this study performed multiple linear regression analysis to examine preoperative factors with a significant impact on surgical costs and surgical time. Postoperative complications were not included in the analysis because they directly mediated treatment costs.
A retrospective analysis was conducted on 40 patients who underwent NOSES type IV surgery at the Shenzhen People’s Hospital between July 2021 and October 2025. Among them, 19 patients underwent the modified NOSES type IV pro
| Item | Modified NOSES (n = 19) | Standard NOSES (n = 21) | χ2/t/Z | P value | |
| Gender | Female | 12 (63.16) | 12 (57.14) | 0.15 | 0.755 |
| Male | 7 (36.84) | 9 (42.86) | |||
| Tumor staging | I | 12 (63.16) | 7 (33.33) | -1.435 | 0.151 |
| II | 3 (15.79) | 9 (42.86) | |||
| III | 4 (21.05) | 5 (23.81) | |||
| Tumor size (cm), mean ± SD | 2.26 ± 0.91 | 2.85 ± 1.06 | 1.878 | 0.068 | |
| Years, mean ± SD | 56.6 ± 13.55 | 55.19 ± 12.91 | 0.344 | 0.732 | |
| Distance of tumor from anus (cm) | 20.89 ± 7.34 | 17.95 ± 2.27 | -1.673 | 0.109 | |
| BMI (kg/m2), mean ± SD | 22.75 ± 3.09 | 21.85 ± 2.54 | -1.014 | 0.317 | |
Comparisons of the perioperative parameters between the two groups are summarized in Tables 2 and 3. Intraoperative blood loss was significantly lower in the modified NOSES group (8.79 ± 10.99 mL) than that in the standard NOSES group (26.9 ± 29.35 mL, P < 0.05). The operative time was also shorter in the modified NOSES group (174.37 ± 41.88 minutes) than that in the standard NOSES group (216.43 ± 69.35 minutes, P < 0.05). In addition, the total surgical cost was reduced in the modified NOSES group (¥32554.1 ± 9223.37) compared with that in the standard NOSES group (¥51975.26 ± 9223.37, P < 0.05).
| Item | Modified NOSES (n = 19) | Standard NOSES (n = 21) | t | P value |
| Intraoperative blood loss (mL) | 8.79 ± 10.99 | 26.9 ± 29.35 | 2.632 | 0.014a |
| Number of lymph nodes harvested | 13.89 ± 7.49 | 17.48 ± 5.72 | 1.709 | 0.096 |
| Operative time (minute) | 174.37 ± 41.88 | 216.43 ± 69.35 | 2.291 | 0.028a |
| 24-hour postoperative pain score (VAS) | 1.11 ± 0.81 | 1.38 ± 1.12 | 0.885 | 0.381 |
| Postoperative body temperature (°C) | 36.76 ± 0.39 | 36.74 ± 0.31 | -0.182 | 0.856 |
| Item | Modified NOSES (n = 19) | Standard NOSES (n = 21) | χ2/t/Z | P value | |
| Postoperative CRP (mg/L), mean ± SD | 49.33 ± 31.08 | 50.11 ± 33.35 | 0.076 | 0.94 | |
| Intra-abdominal infection | 2 (10.53) | 2 (9.52) | 0.011 | 0.658 | |
| Urinary retention | 2 (10.53) | 4 (19.05) | 0.568 | 0.664 | |
| Bowel obstruction | 1 (5.26) | 1 (5.26) | 0.731 | 1 | |
| Total surgical cost (¥), mean ± SD | 32554.1 ± 12022.29 | 51975.26 ± 10570.89 | 5.437 | < 0.001a | |
| Anastomotic leakage | Grade A | 1 (5.26) | 1 (5.26) | -0.534 | 0.593 |
| Grade B | 0 (0.00) | 1 (5.26) | |||
| Grade C | 0 (0.00) | 0 (0.00) | |||
One patient in the control group developed a grade B anastomotic leak.
The postoperative recovery data are presented in Table 4. The time to first defecation was significantly shorter in the modified NOSES group (3.37 ± 0.96 days) than that in the standard NOSES group (4.43 ± 1.96 days, P < 0.05).
| Item | Modified NOSES (n = 19) | Standard NOSES (n = 21) | t | P value |
| First oral intake (days) | 5.05 ± 2.20 | 4.48 ± 1.37 | -1.007 | 0.32 |
| First flatus (days) | 3.43 ± 1.36 | 2.84 ± 1.07 | 1.504 | 0.141 |
| First defecation (days) | 3.37 ± 0.96 | 4.43 ± 1.96 | 2.202 | 0.036a |
| Ambulation (days) | 4.43 ± 1.96 | 2.84 ± 1.07 | -0.286 | 0.174 |
| Hospital stay (days) | 9.58 ± 2.22 | 9.33 ± 3.09 | -1.4 | 0.71 |
| Drainage removal (days) | 6.21 ± 3.07 | 5.90 ± 2.05 | -0.374 | 0.32 |
No significant differences were observed between the groups in baseline characteristics, length of hospital stay, postoperative body temperature, CRP levels, time to drainage removal, time to first flatus, time to first oral intake, ambulation, incidence of bowel obstruction, intra-abdominal infection, urinary retention, and 24 hours postoperative pain scores (all P > 0.05).
Multivariable linear regression analysis, including preoperative and intraoperative variables, was performed to evaluate factors influencing operative cost. The modified surgical approach was associated with a significant reduction in operative cost after controlling for age, sex, BMI, tumor size, tumor distance from the anus, and intraoperative blood loss (β = -21307, standardized β = -0.726, P < 0.001).
Larger tumor size and a greater distance from the anus were both associated with increased operative cost (β = 3912 per cm, P = 0.024; β = 713 per cm, P = 0.025, respectively). No significant effects were observed for age, sex, or BMI. The detailed results are presented in Table 5.
| Variables | Unstandardized β (95%CI) | Standardized β | P value |
| Gender | -3452 (-10756 to 3852) | -0.115 | 0.341 |
| Age (years) | -129 (-401 to 143) | -0.113 | 0.334 |
| BMI (kg/m²) | 236 (-1153 to 1626) | 0.045 | 0.729 |
| Distance from the anus (cm) | 713 (88-1338) | 0.262 | 0.025a |
| Modified surgical approach | -21307 (-28742 to -13872) | -0.726 | < 0.001b |
| Intraoperative blood loss (mL) | -125 (-276 to 25) | -0.204 | 0.099 |
| Tumor size (cm) | 3912 (520-7304) | 0.270 | 0.024a |
Multivariable linear regression analysis was conducted to assess factors influencing operative time. After accounting for patient characteristics, tumor-related variables, and intraoperative factors, the modified surgical approach was asso
Tumor size showed a trend toward longer operative time (β = 17.5 minutes per cm increase, P = 0.067), although this did not reach statistical significance. Distance of the tumor from the anus and intraoperative blood loss were not signi
| Variables | Unstandardized β (95%CI) | Standardized β | P value |
| Gender | 5.0 (-35.3 to 45.4) | 0.041 | 0.803 |
| Age (years) | 0.4 (-1.1 to 1.9) | 0.088 | 0.582 |
| BMI (kg/m²) | 1.6 (-6.0 to 9.3) | 0.076 | 0.670 |
| Distance from the anus (cm) | 2.5 (-1.0 to 5.9) | 0.222 | 0.156 |
| Modified surgical approach | -49.9 (-90.8 to -9.0) | -0.415 | 0.019a |
| Intraoperative blood loss (mL) | -0.6 (-1.5 to 0.2) | -0.256 | 0.129 |
| Tumor size (cm) | 17.5 (-1.1 to 36.2) | 0.295 | 0.067 |
We observed a significantly lower intraoperative blood loss in the modified NOSES group. This can be attributed to two factors. First, in the standard procedure, following transection of the tumor-bearing segment, the proximal bowel wall must be opened to insert the circular stapler anvil, and the anvil must be secured using the in situ purse-string technique, which can contribute to additional bleeding. Second, after tumor excision, patients undergoing the standard procedure require a second incision in the distal bowel to extract the specimen, followed by closure of the distal bowel stump, which further increases blood loss. In contrast, the modified procedure employs an overlap anastomosis, avoiding repeated transection of the proximal and distal bowels and minimizing injury to the proximal segment, thereby reducing intraoperative bleeding.
Compared with the standard NOSES procedure, the modified approach reduced both the number of surgical steps and the operative time. In the standard NOSES procedure, the circular stapler anvil is inserted transanally and secured proximally using the in situ purse-string technique. After distal specimen extraction, the distal bowel stump is closed using a linear stapler. These multiple steps increase the complexity of the procedure. In contrast, the modified technique omits the use of a circular stapler and proximal purse-string, requiring only closure of the common opening after overlap anastomosis, thereby simplifying the procedure and shortening the operative time.
Furthermore, unlike conventional laparoscopic rectosigmoid resection with transabdominal specimen extraction, which typically requires more linear staplers, the modified NOSES technique avoids repeated closures and trimming of the proximal and distal bowel walls after specimen extraction. By eliminating the need for a circular stapler, the modified procedure reduces operative costs and patient trauma while maintaining surgical efficacy.
One patient in the standard NOSES group developed a grade B anastomotic leak. Anastomotic leakage is a serious complication of gastrointestinal surgery, typically presenting as localized tenderness, peritonitis, and abnormal drainage, and it significantly affects postoperative outcomes[9]. Some studies have also suggested that postoperative anastomotic leakage may increase the risk of local recurrence and reduce overall survival[10]. The standard NOSES technique often employs a double-stapling technique for bowel reconstruction. In this method, overlapping staple lines from the circular and linear staplers create “dog ears”[11]. Compared to a single linear stapled area, these regions experience higher intramural pressure and are more prone to inflammatory edema, increasing the likelihood of postoperative anastomotic leakage. Repeated stapler application further increases the number of structurally weak sites[12]. Zhang and Xiao[13] emphasized the clinical importance of careful intraoperative handling to enhance patient safety and improve prognosis. By avoiding double-stapler techniques, the modified NOSES procedure eliminates “dog ears”. In our center, the use of overlapping anastomoses modifies the anastomotic configuration, preventing weak points at the staple intersections. Moreover, as reported by Sun and Tao[14], overlapping anastomoses create a wider anastomotic lumen with a longer contralateral mesenteric edge, providing better blood supply, which may optimize perfusion and vascular tension, further reducing the risk of postoperative leakage. In the present study, none of the patients in the modified NOSES group experienced anastomotic leakage, which supports the clinical advantages of this modification.
Patients in the modified NOSES group experienced postoperative bowel movements slightly earlier than those in the standard group. Previous studies have indicated that surgical trauma can significantly affect bowel function recovery. Compared to the modified procedure, the standard NOSES technique causes greater injury to the bowel, whereas re
Our center focused on modifying the NOSES procedure for specimen extraction and bowel anastomosis. The modified technique reduces the use of circular staplers and employs a colorectal overlap anastomosis, thereby simplifying the surgical steps and reducing intraoperative blood loss, operative time, and overall costs. Hu et al[19] demonstrated that total laparoscopic overlap anastomosis is safe and feasible, offering faster postoperative bowel function recovery and reduced surgical trauma without increasing the incidence of short-term complications. Building on the minimally invasive concept of NOSES, the modified procedure further minimizes surgical trauma through overlapping anastomosis, suggesting broader clinical applicability and potential advantages in patient recovery.
Considering current clinical practice, the modified surgical technique adopted in this study has been less frequently performed in clinical settings compared with the standard procedure. Furthermore, its outcomes may be influenced by the surgeon’s technical proficiency, potentially leading to differences in operative quality and material costs. To account for this factor, all surgeries in this study were performed by senior surgeons from our institution who had extensive experience with the procedure, assisted by physicians of comparable seniority level. In the control group, the operation of only one patient was performed by the regional pioneer of the NOSES technique. Otherwise, for most cases in this study, the operations were performed under consistent standards to ensure comparable surgical quality and minimize varia
This study had inherent limitations in the assessment of long-term outcomes. First, the sample size was relatively small, which restricted the statistical power to detect differences in survival or recurrence between the modified and standard NOSES procedures. Second, postoperative adjuvant treatments, including chemotherapy and radiotherapy, have not been fully standardized across patients, thereby introducing potential variability in the long-term prognosis. Consequently, while short-term perioperative outcomes and recovery were adequately evaluated, the current dataset was insufficient for drawing robust conclusions regarding long-term survival, disease-free survival, and tumor recurrence. Previous studies comparing NOSES with conventional laparoscopic rectosigmoid cancer surgery have provided insights into long-term outcomes[20]; however, whether the modifications introduced in the present procedure translate into differences in long-term efficacy remains unclear. Future research with larger, well-controlled cohorts and standardized postoperative management is required to validate these findings and clarify the impact of the modified NOSES procedure on patient prognosis over time.
In conclusion, our institutional cohort analysis finding indicates that the modified NOSES technique may be associated with reduced procedural trauma, shorter operative duration, lower perioperative resource utilization, and earlier post
| 1. | Guan X, Wang GY, Zhou ZQ, Zhou HT, Chen YG, Tang QC, Song JM, Cai JC, Bao CQ, Zhang H, Liu YJ, Xiong ZG, Wu M, Song C, Zheng YC, Jiang JR, Yan S, Wang Y, Hu QL, Ma D, Ren K, Xiong DH, Zhang XH, Yang MR, Bai YK, Fu W, Li SH, Zhang SF, Liu JG, Mo XW, Gong HY, Jiang B, Wang T, Zhang AP, Zhu P, Fu T, Hu JH, Jia WZ, Qin CJ, Su Q, Wang DR, Wu WQ, Zhao ZG, Zhu HB, Jin WY, Jing CQ, Li DG, Liu WZ, Liu ZC, Pang LM, Tang D, Wang XQ, Yang GS, Yao KH, Zhang XM, Zhao L, Zhong XG, Zhou L, Zhu Z, Bai XF, Chen CW, Chen SW, Chen ZH, Dai L, Fu ZB, Gao F, Gao H, Gao L, Gong JF, Jiang Y, Jie JZ, Jin WS, Li DC, Li J, Lin HW, Liu BL, Liu CQ, Liu M, Meng JB, Qiu J, Rao GA, Sun DH, Sun XJ, Tai JD, Wang ZG, Xie GW, Xie M, Wei Y, Yan J, Yan LK, Yang F, Yang HM, Yang WJ, Chen LC, Ye ZS, Yu ZG, Zhao ZH, Zhong M, Zhu YP, Fu CG, Wang XS. [Retrospective study of natural orifice specimen extraction surgery for colorectal tumors in 718 cases from 79 hospitals]. Zhonghua Jiezhichang Jibing Dianzi Zazhi. 2017;6:469-477. [DOI] [Full Text] |
| 2. | Xie HB, Yu JT, Wang HS, Jia C. [Comparison of the effects of NOSES and conventional laparoscopic surgery on postoperative recovery and complications in colorectal cancer]. Zhongguo Xiandai Putong Waike Jinzhan. 2023;26:194-196+201. |
| 3. | Guan X, Wang XS. [Advantages of organ protection in colorectal tumor specimen collection through natural orifice specimen extraction surgery]. Zhonghua Wei Chang Wai Ke Za Zhi. 2022;25:500-504. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 4. | Wang KJ, Fu CG, Zhu Z, Gao W, Du T, Liu MC, Zhang YY, Liu J. [Analysis of short-term clinical efficacy and quality of life after transrectal NOSES for colorectal cancer]. Tongji Daxue Xuebao (Yixueban). 2019;40:789-794. [DOI] [Full Text] |
| 5. | Wang XS. [Challenges and prospects of NOSES in China]. Zhonghua Jiezhichang Jibing Dianzi Zazhi. 2018;7:2-7. [DOI] [Full Text] |
| 6. | Colorectal Tumor Professional Committee of Chinese Medical Doctor Association; Colorectal Tumor Professional Committee of Chinese Medical Doctor Association; China NOSES Alliance. [Guidelines for natural orifice specimen extraction surgery for colorectal tumors (2023 edition)]. Zhonghua Jiezhichang Jibing Dianzi Zazhi. 2023;12:89-99. [DOI] [Full Text] |
| 7. | Kitaguchi D, Hasegawa H, Ando K, Ikeda K, Tsukada Y, Nishizawa Y, Ito M. Transanal Total Mesorectal Excision for Rectal Cancer: Toward Standardization of the Surgical Technique. J Anus Rectum Colon. 2023;7:225-231. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 8. | Bousquet PJ, Combescure C, Klossek JM, Daurès JP, Bousquet J. Change in visual analog scale score in a pragmatic randomized cluster trial of allergic rhinitis. J Allergy Clin Immunol. 2009;123:1349-1354. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 94] [Article Influence: 5.5] [Reference Citation Analysis (1)] |
| 9. | Zou DP. [Experience in the prevention and management of anastomotic leakage after low anterior resection for rectal cancer]. Xiandai Xiaohua Ji Jieru Zhiliao. 2015;20:30-32. [DOI] [Full Text] |
| 10. | Teng XL, Yue K, Zhou JD, Chi Q. [Meta-analysis of the impact of anastomotic leakage on prognosis after colorectal cancer surgery]. Zhongguo Yishi Jinxiu Zazhi. 2015;38:5. [DOI] [Full Text] |
| 11. | Perez MM, Stoehr JR, Chwa E, Connor L, Gosain AK. Dog Ears in Wound Closure: Can They Be Minimized? Ann Plast Surg. 2022;89:581-590. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 12. | Chen SW, Xia SJ, Zhang SF. [Comparative study of two preventive ileostomy methods in low and mid-rectal cancer anterior resection]. Zhongguo Xiandai Yixue Zazhi. 2016;26:124-126. [DOI] [Full Text] |
| 13. | Zhang Y, Wang X. [Effect of reinforcing the "dog-ear area" on reducing anastomotic leakage after laparoscopic rectal cancer TME]. Jiezhichang Gangmen Waike. 2018;24:545-548. [DOI] [Full Text] |
| 14. | Sun JY, Zhang T. [Clinical study of overlap anastomosis in reconstruction during laparoscopic colorectal surgery]. Quanke Yixue Linchuang Yu Jiaoyu. 2024;22:518-21. [DOI] [Full Text] |
| 15. | Lu XR, Zhou XS. [Construction of a risk model for delayed postoperative intestinal paralysis in elderly patients after colorectal surgery based on logistic regression]. Yixue Lilun Yu Shijian. 2025;38:2276-2278. [DOI] [Full Text] |
| 16. | Mao H, Milne TGE, O'Grady G, Vather R, Edlin R, Bissett I. Prolonged Postoperative Ileus Significantly Increases the Cost of Inpatient Stay for Patients Undergoing Elective Colorectal Surgery: Results of a Multivariate Analysis of Prospective Data at a Single Institution. Dis Colon Rectum. 2019;62:631-637. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 74] [Article Influence: 10.6] [Reference Citation Analysis (1)] |
| 17. | Bragg D, El-Sharkawy AM, Psaltis E, Maxwell-Armstrong CA, Lobo DN. Postoperative ileus: Recent developments in pathophysiology and management. Clin Nutr. 2015;34:367-376. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 314] [Cited by in RCA: 253] [Article Influence: 23.0] [Reference Citation Analysis (4)] |
| 18. | Li XL, Yi FF, Qing CJ. [Effect of laparoscopic NOSES versus small-incision surgery for colorectal cancer and its impact on serum GAS and MTL levels]. Shiyong Aizheng Zazhi. 2024;39:1163-1166. |
| 19. | Hu BG, Zhang Z, Liu Y, Sun L. [Short-term efficacy and complication analysis of totally laparoscopic overlap anastomosis in right hemicolectomy for colon cancer]. Xiandai Zhongliu Yixue. 2024;32:4329-4333. [DOI] [Full Text] |
| 20. | Wang S, Tang J, Sun W, Yao H, Li Z. The natural orifice specimen extraction surgery compared with conventional laparoscopy for colorectal cancer: A meta-analysis of efficacy and long-term oncological outcomes. Int J Surg. 2022;97:106196. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 42] [Article Influence: 10.5] [Reference Citation Analysis (1)] |